ABOS Orthopedic Board Review: Paget's Disease, Gout, Hyperparathyroidism, Septic Coxitis | Part 5
Key Takeaway
Orthopedic Board Review Pathology covers Paget's disease (bone remodeling, fragility, diagnosis), Gout (urate crystals, tophi, diagnosis), Hyperparathyroidism (PTH, bone resorption, kidney stones, brown tumors), and Newborn Septic Coxitis (S. aureus, hip position, ultrasound). This section provides essential knowledge for ABOS exam preparation.
ABOS Orthopedic Board Review: Paget's Disease, Gout, Hyperparathyroidism, Septic Coxitis | Part 5
Comprehensive 100-Question Exam
00:00
Start Quiz
Question 1
A 70-year-old male with a known history of Paget's disease presents with a 2-month history of new, severe, and unrelenting pain in his right thigh. Radiographs reveal a mixed lytic and sclerotic lesion in the mid-diaphysis of the femur with cortical destruction and a soft tissue mass. What is the most likely diagnosis?
Explanation
Question 2
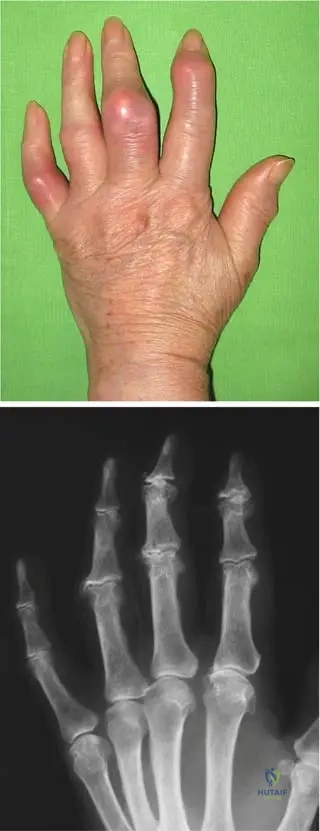
A 55-year-old female with end-stage renal disease presents with diffuse bone pain. Radiographs of her hands are obtained to evaluate for secondary hyperparathyroidism. What is the classic and earliest radiographic hallmark of this condition in the hand?
Explanation
Question 3
A 45-year-old male presents with an acutely swollen, red, and painful knee. Aspiration yields turbid fluid. Synovial fluid analysis confirms the diagnosis of gout. Which of the following describes the characteristic microscopic findings under polarized light?
Explanation
Question 4
A 4-year-old boy refuses to bear weight on his right leg. His temperature is 38.8°C, WBC is 13,500/mm3, and ESR is 45 mm/hr. An ultrasound of the right hip demonstrates a significant joint effusion. What is the most appropriate next step in management?
Explanation
Question 5
A patient with symptomatic Paget's disease of the tibia is prescribed the first-line pharmacologic treatment to reduce bone pain and turnover. What is the primary cellular mechanism of action of this medication class?
Explanation
Question 6
A 40-year-old female with a history of recurrent nephrolithiasis presents with a well-circumscribed lytic lesion in her distal femur. Biopsy reveals localized accumulations of giant cells, hemosiderin-laden macrophages, and spindle cells. Laboratory workup shows elevated serum calcium and low serum phosphorus. What is the most likely diagnosis of the bone lesion?
Explanation
Question 7
A neonate in the NICU develops irritability, fever, and pseudoparalysis of the left lower extremity. Physical examination reveals the left hip is held in a specific resting posture to minimize intracapsular pressure. Which position is most characteristic of a hip joint effusion in septic coxitis?
Explanation
Question 8
A 60-year-old male with a history of recurrent painful joint attacks presents with chronic deformities of his toes. Radiographs are obtained. What is the radiologic hallmark of this condition?

Explanation
Question 9
Routine laboratory testing in an asymptomatic 65-year-old male reveals an isolated, marked elevation of serum alkaline phosphatase. Calcium, phosphorus, and GGT levels are completely normal. Radiographs of the pelvis show coarse trabeculations and cortical thickening. What phase of Paget's disease does this presentation most likely represent?
Explanation
Question 10
A 60-year-old male on long-term hemodialysis presents with diffuse bone pain. Radiographs demonstrate a 'rugger jersey' appearance of the spine. His labs show elevated PTH, low calcium, and high phosphorus. What is the primary pathophysiologic trigger for his skeletal disease?
Explanation
Question 11
A 5-year-old child presents with a severe limp and a 3 cm limb length discrepancy. History reveals a prolonged NICU stay for sepsis as a neonate. Radiographs show complete absence of the femoral head and neck with proximal migration of the femoral shaft. This severe deformity is a known sequela of delayed treatment for which of the following?
Explanation
Question 12
A 72-year-old male with a long history of polyostotic Paget's disease presents with progressive bilateral lower extremity weakness, numbness, and neurogenic claudication. What is the most likely cause of his neurologic symptoms?
Explanation
Question 13
A 55-year-old male presents with an acute gout flare in his first metatarsophalangeal joint. He has a history of a recent severe upper gastrointestinal bleed and end-stage renal disease on dialysis. Which of the following is the most appropriate acute pharmacologic treatment?
Explanation
Question 14
A 2-year-old, fully immunized child is brought to the emergency department with a 2-day history of fever, refusal to walk, and left hip pain. Joint aspiration yields purulent fluid with a WBC count of 85,000/mm3. What is the most common causative organism overall for this condition?
Explanation
Question 15
Which of the following laboratory profiles most accurately differentiates primary hyperparathyroidism from secondary hyperparathyroidism?
Explanation
Question 16
A bone biopsy from the thickened, bowed tibia of a patient with Paget's disease demonstrates a characteristic mosaic pattern of lamellar bone with prominent, disorganized cement lines. What is the underlying primary cellular abnormality driving this disease process?
Explanation
Question 17
A 65-year-old male presents with massive, ulcerated, chalky white tophaceous deposits over his olecranon and PIP joints, causing severe mechanical restriction and recurrent secondary infections. Initial surgical management of these symptomatic lesions primarily involves:
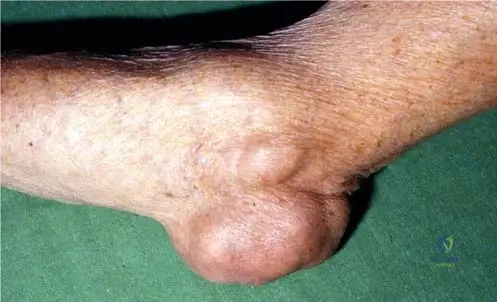
Explanation
Question 18
A 58-year-old male with a history of prolonged hemodialysis followed by a successful renal transplant 3 years ago presents to the clinic. Routine labs show persistent, severe hypercalcemia and markedly elevated PTH levels despite normal renal graft function. What is the most likely diagnosis?
Explanation
Question 19
A 55-year-old man presents with a swollen, erythematous first metatarsophalangeal joint. Joint aspiration is performed to confirm the diagnosis of acute gout.
Which of the following describes the characteristic crystal findings under polarized light microscopy?

Explanation
Question 20
What is the primary cellular defect that initiates the pathogenesis of Paget's disease of bone?
Explanation
Question 21
A 62-year-old woman with chronic kidney disease presents with diffuse bone pain. Radiographs of her hands show subperiosteal bone resorption on the radial aspect of the middle phalanges.
What is the most likely primary driving mechanism for these osseous changes?
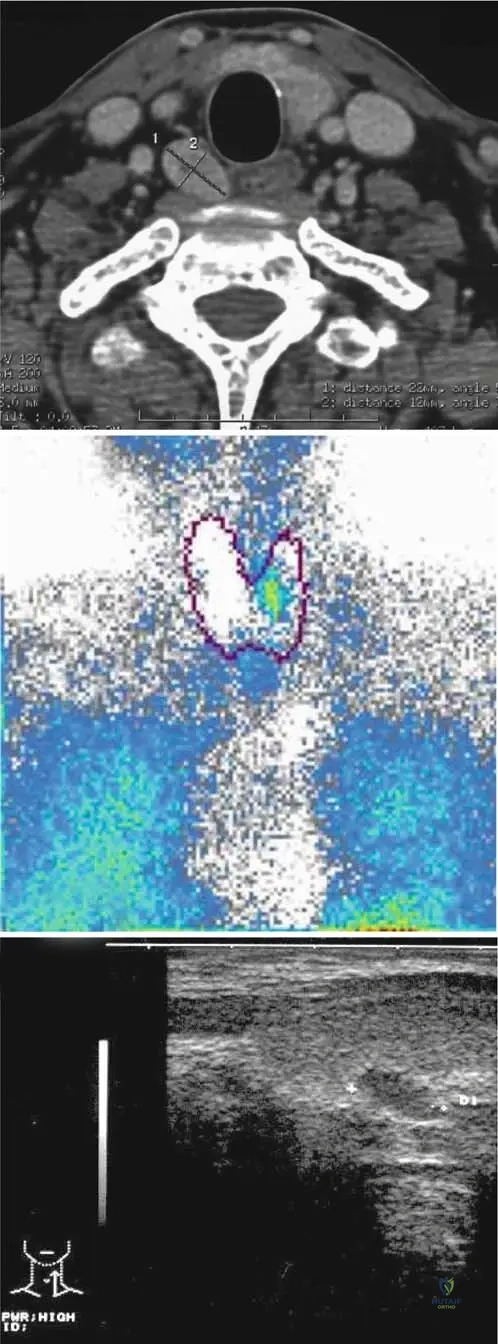
Explanation
Question 22
A 10-day-old neonate presents with irritability, fever, and asymmetric active leg movement. The affected hip is held in flexion, abduction, and external rotation.
What is the physiologic reason for this classic posture?
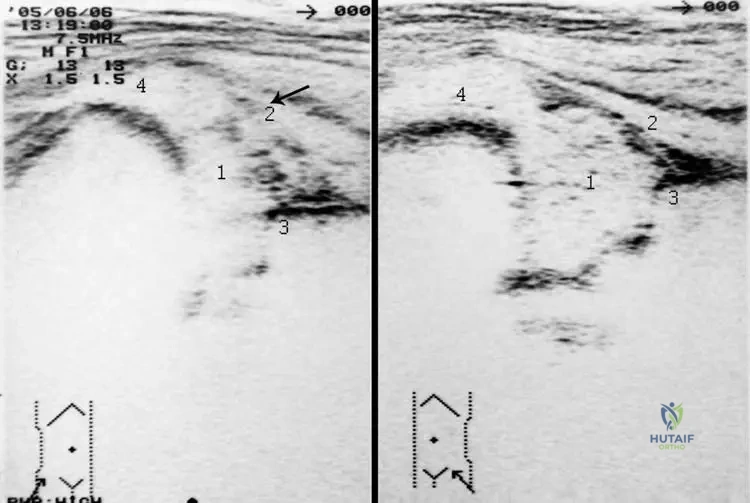
Explanation
Question 23
A 70-year-old man with a long-standing history of enlarged skull and bowed tibias presents with a sudden onset of severe, unrelenting pain in his right proximal femur, which was previously asymptomatic. His serum alkaline phosphatase is notably higher than his baseline.
What is the most likely diagnosis?
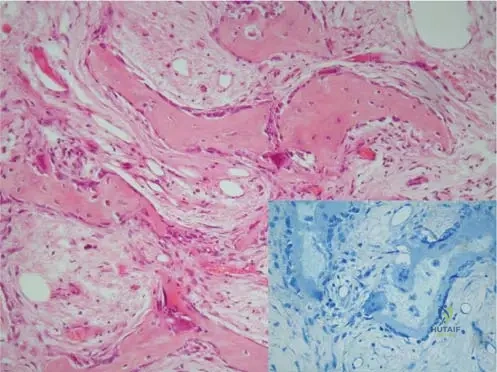
Explanation
Question 24
A 45-year-old man with a history of recurrent acute podagra and visible tophi on his elbows is started on long-term medical therapy to lower his serum uric acid. He is prescribed a medication that inhibits xanthine oxidase. Which of the following drugs fits this mechanism?
Explanation
Question 25
Which of the following laboratory profiles is most characteristic of an untreated patient with primary hyperparathyroidism?
Explanation
Question 26
A 68-year-old woman with active Paget's disease of the right hemipelvis and femur is scheduled for a total hip arthroplasty due to severe secondary osteoarthritis. Which preoperative pharmacological intervention is highly recommended to reduce intraoperative blood loss?
Explanation
Question 27
A 4-year-old boy presents with right hip pain and a limp. He refuses to bear weight. His temperature is 38.8°C (101.8°F), ESR is 45 mm/hr, and peripheral WBC count is 14,000/mm³. According to the Kocher criteria, what is the approximate probability that this child has septic arthritis of the hip?
Explanation
Question 28
A 68-year-old male presents with a painful, swollen great toe. Radiographs demonstrate punched-out periarticular erosions with overhanging edges.
Synovial fluid analysis of the affected joint is most likely to reveal which of the following?

Explanation
Question 29
A 74-year-old male with a long-standing history of bone pain and enlarging skull size presents with a new, severe, and unrelenting pain in his right thigh. Radiographs reveal a destructive, lytic lesion with cortical breakthrough in the diaphysis of the femur.
What is the most likely diagnosis?
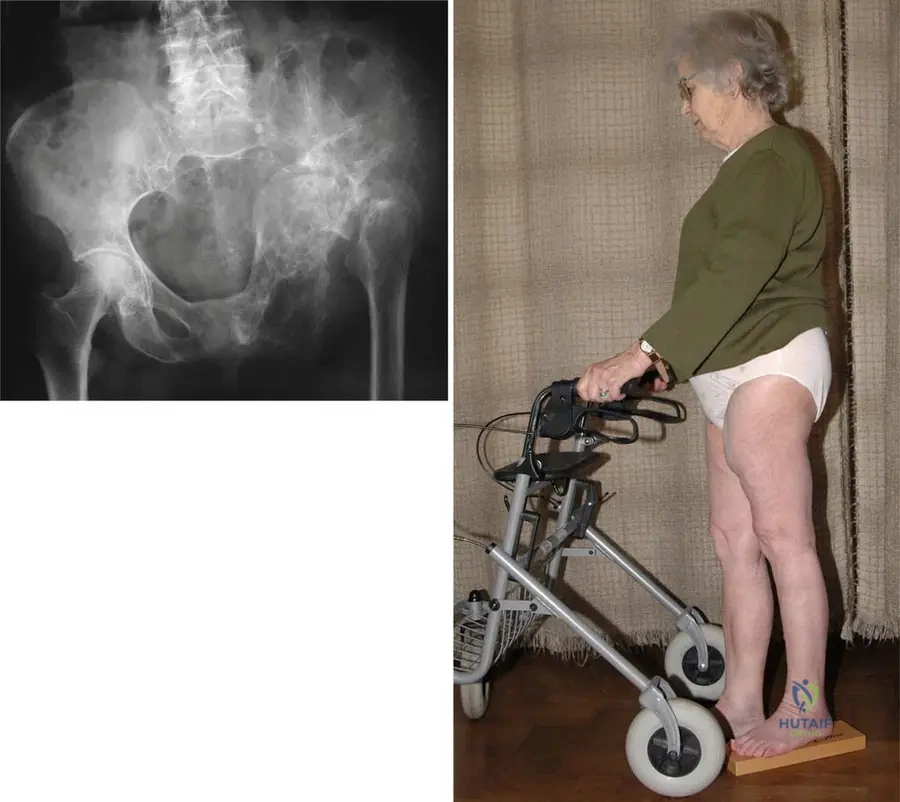
Explanation
Question 30
A 45-year-old female presents with diffuse bone pain and a history of recurrent nephrolithiasis. Radiographs demonstrate a lytic lesion in her proximal femur. Biopsy of the lesion reveals spindle cells, multinucleated giant cells, and abundant hemosiderin deposits. Which of the following laboratory profiles is most consistent with her diagnosis?
Explanation
Question 31
A 2-week-old neonate is brought to the emergency department for irritability and decreased spontaneous movement of the right lower extremity. Ultrasound reveals a significant hip effusion.
What is the most appropriate next step in management?
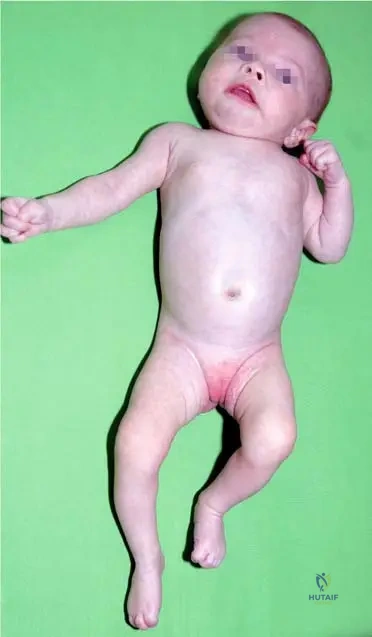
Explanation
Question 32
A 65-year-old male presents with enlarging hat size, hearing loss, and bowing of the tibiae. Laboratory evaluation reveals an isolated, markedly elevated alkaline phosphatase with normal serum calcium and phosphorus. What is the primary cellular abnormality initiating this disease process?
Explanation
Question 33
A 72-year-old male with a known history of Paget's disease presents with new-onset, severe, and unrelenting left thigh pain. Radiographs demonstrate a destructive lytic lesion in the femur with cortical breakthrough and soft tissue extension.
What is the most likely diagnosis?

Explanation
Question 34
A 68-year-old male with symptomatic Paget's disease of the right hip is scheduled for a total hip arthroplasty due to severe secondary osteoarthritis. To minimize severe intraoperative hemorrhage, which medical management is recommended prior to surgery?
Explanation
Question 35
In a patient diagnosed with asymptomatic Paget's disease incidentally on radiographs, which of the following represents an absolute indication for initiating bisphosphonate therapy?
Explanation
Question 36
A 55-year-old male presents with acute, severe pain, swelling, and erythema of the first metatarsophalangeal joint. Joint aspiration is performed. What is the expected crystal analysis result under polarized light microscopy?
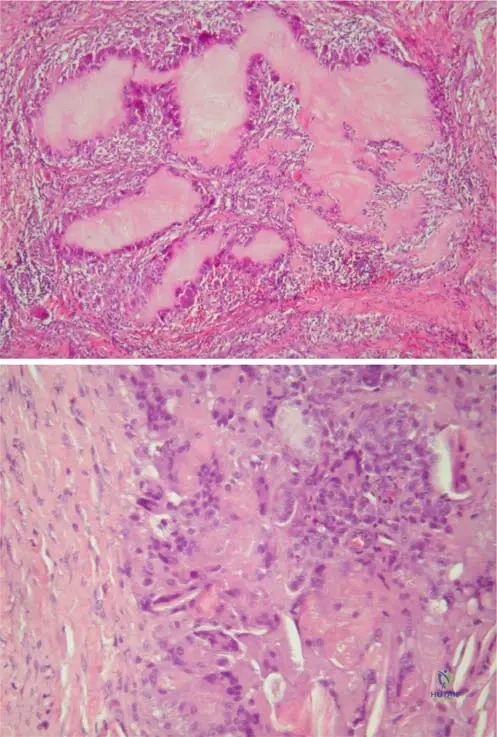
Explanation
Question 37
A 60-year-old male has a history of recurrent joint pain. Radiographs of his hands demonstrate periarticular erosions with overhanging sclerotic margins and preserved joint spaces.
What is the primary etiology of this disease process?
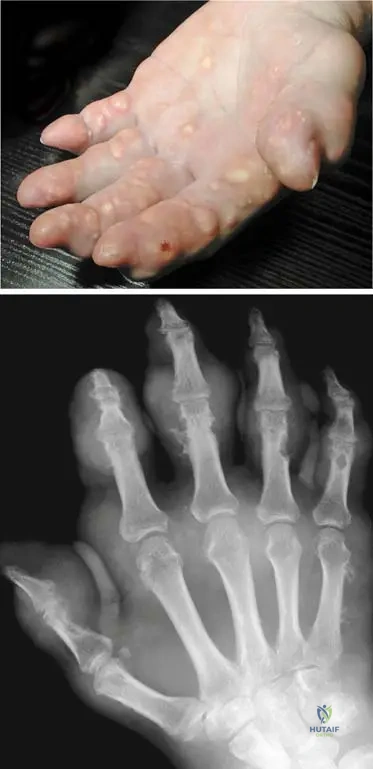
Explanation
Question 38
A patient with an acute gout flare is evaluated in the emergency department. He has a history of severe chronic kidney disease (Stage IV). Which of the following is the most appropriate initial treatment for his acute flare?
Explanation
Question 39
A 45-year-old female with chronic renal failure complains of diffuse bone pain. Laboratory evaluation shows elevated parathyroid hormone (PTH), low serum calcium, and high serum phosphate. Radiographs show subperiosteal resorption in the phalanges. What is the most likely diagnosis?
Explanation
Question 40
A 50-year-old female presents with a pathological fracture of the humerus. Radiographs show a well-defined, expansile, lytic lesion. Labs reveal hypercalcemia, hypophosphatemia, and elevated PTH.
Biopsy of the lesion would most likely show:

Explanation
Question 41
A 4-year-old boy presents with a sudden onset limp and refuses to bear weight on his right leg. He has a temperature of 38.8 C. Labs show an ESR of 45 mm/h and a WBC count of 13,500/mm3. According to the Kocher criteria, what is the probability that he has septic arthritis of the hip?
Explanation
Question 42
A 3-week-old neonate in the NICU develops swelling of the left thigh and pseudoparalysis of the left leg. The hip is held in flexion, abduction, and external rotation.
What is the most common causative organism for this condition in this age group?

Explanation
Question 43
A delay in the surgical drainage of septic coxitis in an infant can lead to devastating sequelae due to increased intra-articular pressure and bacterial chondrolysis. Which of the following structures is at highest immediate risk of irreversible ischemic necrosis?
Explanation
Question 44
A 55-year-old patient on hemodialysis presents with mechanical back pain. Lateral radiographs of the lumbar spine demonstrate alternating bands of dense sclerosis at the superior and inferior vertebral body endplates with central lucency.
What is this characteristic radiographic sign called?
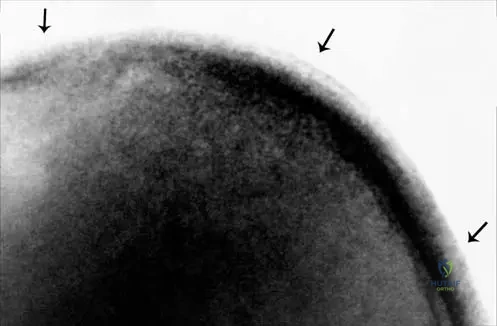
Explanation
Question 45
A 70-year-old female with active Paget's disease is treated with zoledronic acid. What is the primary cellular mechanism of action of this medication?
Explanation
Question 46
A 62-year-old male with a history of gout undergoes an elective total knee arthroplasty. On postoperative day 3, he develops acute, severe pain, swelling, and erythema of the operated knee. Aspiration yields cloudy fluid with 35,000 WBCs/mm3 and negatively birefringent crystals. Gram stain is negative. What is the most appropriate next step?
Explanation
Question 47
A 6-year-old child presents with atraumatic hip pain and fever. An ultrasound is performed, which reveals an asymmetry in the anterior capsular distance of 3 mm compared to the contralateral hip. Which of the following is the most appropriate next step to confirm the diagnosis?
Explanation
Question 48
A patient with refractory secondary hyperparathyroidism due to end-stage renal disease requires medical optimization. Which of the following medications functions as a calcimimetic to directly lower PTH levels?
Explanation
Question 49
An 70-year-old man with a long-standing history of Paget's disease presents with a sudden, progressive increase in thigh pain and swelling. Radiographs show a destructive, permeative lesion in the proximal femur with cortical breakthrough. What is the most common malignant transformation in this patient population?
Explanation
Question 50
A 3-week-old neonate presents with fever, irritability, and decreased spontaneous movement of the right lower extremity. Clinical examination reveals pain upon passive range of motion of the right hip. Ultrasound shows a joint effusion. What is the most appropriate next step in management?

Explanation
Question 51
A 55-year-old man presents with an acute, exquisitely tender, swollen first metatarsophalangeal joint. Joint aspiration yields cloudy fluid. Which of the following best describes the microscopic appearance of the crystals pathognomonic for this condition?
Explanation
Question 52
A 48-year-old woman with end-stage renal disease presents with diffuse bone pain. Radiographs of her hands reveal pathognomonic subperiosteal bone resorption on the radial aspect of the middle phalanges. What are the expected serum laboratory findings in this patient?
Explanation
Question 53
A 65-year-old man is incidentally diagnosed with a thickened calvarium and bowing of the tibia. His serum alkaline phosphatase is significantly elevated, but calcium and phosphate are normal. If a biopsy of the affected bone were performed, what would be the characteristic histological finding?
Explanation
Question 54
A 62-year-old man with a history of recurrent monoarticular arthritis presents with chronic pain and deformity in his foot. Radiographs display well-defined, "punched-out" erosions with sclerotic margins and overhanging edges in the first metatarsophalangeal joint. What is the underlying pathophysiology of this condition?

Explanation
Question 55
A 35-year-old woman presents with a pathological fracture of the proximal humerus. Radiographs reveal a large, purely lytic lesion. Laboratory tests demonstrate elevated serum calcium and elevated parathyroid hormone levels. A biopsy of the lesion shows abundant multinucleated giant cells in a fibrovascular stroma with hemosiderin deposition. What is the most appropriate definitive management for the underlying cause of this bone lesion?

Explanation
Question 56
A 72-year-old man with symptomatic Paget's disease involving the pelvis and femur is scheduled for a total hip arthroplasty due to severe secondary osteoarthritis. Which preoperative medication should be considered to reduce intraoperative blood loss and disease activity?
Explanation
Question 57
A 4-year-old child presents with a severe limp and limb length discrepancy. His mother reports he had a severe febrile illness requiring an operation on his hip shortly after birth. Radiographs show a completely absent femoral head and neck with proximal migration of the femoral shaft. What was the most likely diagnosis during the neonatal period?

Explanation
Question 58
A 50-year-old man presents with an acute flare of gout in his knee. He is prescribed colchicine. What is the mechanism of action of this medication in the treatment of acute gout?
Explanation
Question 59
A 55-year-old man on hemodialysis presents with chronic back pain. Lateral radiographs of the lumbar spine demonstrate dense sclerotic bands at the superior and inferior endplates of the vertebral bodies, with central radiolucency. What is this classic radiographic sign called?
Explanation
Question 60
An 80-year-old woman with advanced Paget's disease of the skull presents with gradual hearing loss and tinnitus. What is the primary cause of hearing loss in this patient?
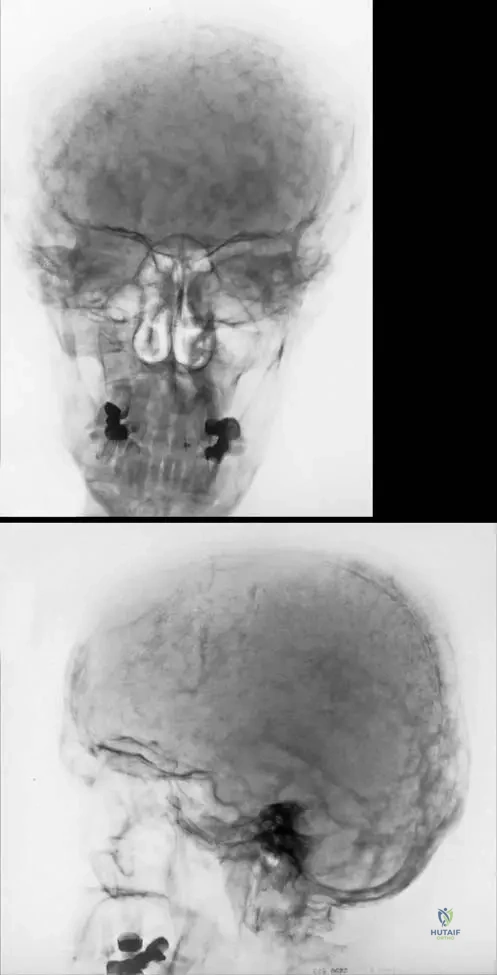
Explanation
Question 61
A patient with a chronic history of gouty arthritis presents with multiple, painless, firm, yellowish nodules over the olecranon bursa and Achilles tendon. Chalky white material is extruded from one of the nodules. Which of the following conditions is most strongly associated with this disease process?

Explanation
Question 62
A 65-year-old man with Paget's disease presents for a routine follow-up complaining of progressive hearing loss. Which of the following is the primary mechanism of action of the first-line medication used to treat the symptomatic manifestations of this condition?
Explanation
Question 63
A 52-year-old male with a history of recurrent podagra presents with a painful, nodular mass on his first metatarsophalangeal joint.
Radiographs are obtained. Which of the following radiographic features is most characteristic of chronic tophaceous gout?

Explanation
Question 64
A 48-year-old female with chronic kidney disease presents with diffuse back pain. Spine radiographs reveal alternating bands of radiolucency and radiodensity in the vertebral bodies. Which of the following underlying pathophysiologic processes is most directly responsible for this radiographic finding?
Explanation
Question 65
A 4-year-old boy presents with a limp, a temperature of 38.8°C, and refusal to bear weight on his right leg. Lab work shows a WBC of 13,000/mm³ and an ESR of 55 mm/hr. Which of the following represents the most appropriate next step in management?
Explanation
Question 66
A 72-year-old man undergoes a biopsy of a thickened, enlarged tibia exhibiting a bowing deformity. Histological examination of the bone reveals a mosaic pattern of lamellar bone with prominent cement lines. Which of the following cell types is initially responsible for the pathogenesis of this disease?
Explanation
Question 67
A 60-year-old man with a history of severe peptic ulcer disease and chronic kidney disease (eGFR 25 mL/min) presents with an acute gout flare in his left knee. Which of the following is the most appropriate initial pharmacological treatment for this acute flare?
Explanation
Question 68
A 50-year-old woman is found to have an expansive, lytic lesion in her distal femur.
Serum calcium is 11.5 mg/dL (Normal: 8.5-10.5) and PTH is significantly elevated. Biopsy reveals highly vascular fibroblastic stroma containing numerous multinucleated giant cells and hemosiderin. What is the most appropriate definitive management for the bone lesion?

Explanation
Question 69
A 2-week-old neonate presents with irritability, poor feeding, and pseudoparalysis of the left lower extremity.
Examination shows pain with passive range of motion of the left hip. If left untreated, which of the following is the most likely catastrophic complication specific to this joint in this age group?

Explanation
Question 70
A 75-year-old male with long-standing polyostotic Paget's disease is scheduled for an elective total hip arthroplasty. To minimize perioperative blood loss associated with the hypervascular pagetic bone, which of the following preoperative interventions is most appropriate?
Explanation
Question 71
A 45-year-old male with chronic tophaceous gout is started on long-term urate-lowering therapy. Six weeks later, his serum uric acid levels are significantly reduced. What is the mechanism of action of the most commonly prescribed first-line medication for this purpose?
Explanation
Question 72
A 55-year-old male with chronic renal failure presents with knee pain. Labs reveal hypocalcemia, hyperphosphatemia, and an extremely high PTH level. Radiographs show subperiosteal resorption. Which of the following combinations of laboratory findings is most characteristic of primary hyperparathyroidism, distinguishing it from this patient's condition?
Explanation
Question 73
A 3-week-old infant in the NICU develops an acutely swollen and erythematous right hip. Aspiration of the joint reveals purulent fluid. While Staphylococcus aureus is the most common pathogen overall, which of the following organisms is particularly unique to this age group and must be covered empirically?
Explanation
Question 74
A 68-year-old male with known Paget's disease presents with slowly progressive bilateral lower extremity weakness, numbness, and difficulty walking. Radiographs of the lumbar spine show an enlarged, dense vertebral body (ivory vertebra). What is the most likely cause of his neurological symptoms?
Explanation
Question 75
A mass is excised from the olecranon bursa of a 55-year-old male. Gross examination reveals chalky white deposits. Histological examination using H&E staining shows large amorphous granular pink material surrounded by macrophages and multinucleated giant cells, but no distinct crystals are seen. Why are the crystals not visible on standard H&E preparation?
Explanation
Question 76
A 65-year-old man undergoes a biopsy for an expansile diaphyseal tibial lesion. Pathology shows a chaotic pattern of woven and lamellar bone with prominent and irregular cement lines. Based on this histological description, what is the most likely diagnosis?
Explanation
Question 77
A 54-year-old woman with chronic kidney disease presents with diffuse skeletal pain. Radiographs of her hand show characteristic lesions
. Where is the classic earliest location of the subperiosteal resorption associated with this condition?

Explanation
Question 78
A 3-year-old child presents with a limp, refusal to bear weight, a temperature of 38.8 C, an ESR of 45 mm/hr, and a peripheral WBC of 13,000/mm^3. According to the Kocher criteria, what is the probability that this child has septic arthritis of the hip?
Explanation
Question 79
A 50-year-old man presents with a painful, swollen first MTP joint. Joint aspirate reveals needle-shaped crystals. When aligned parallel to the axis of the compensator under polarized light microscopy, what color do these crystals typically appear?
Explanation
Question 80
A 72-year-old man with active Paget's disease of the proximal femur is scheduled for an elective total hip arthroplasty due to severe secondary osteoarthritis. His alkaline phosphatase is markedly elevated. Which preoperative intervention is most appropriate to reduce surgical complications?
Explanation
Question 81
A 48-year-old woman presents with a lytic lesion in her distal radius. Biopsy reveals sheets of osteoclast-like multinucleated giant cells in a background of spindle cells and abundant hemosiderin. Lab evaluation shows elevated serum calcium and intact PTH. What is the underlying pathogenesis of this bone lesion?
Explanation
Question 82
A 4-week-old infant is diagnosed with a delayed presentation of septic coxitis
. Which of the following is the most devastating, yet common, complication of delayed surgical decompression in this specific age group?

Explanation
Question 83
A 60-year-old man presents with chronic foot pain and the following radiographic findings
. What is the classic radiographic description of the erosions associated with this disease process?

Explanation
Question 84
First-line medical therapy for symptomatic Paget's disease involves a class of drugs that potently inhibit bone resorption. What is the primary molecular target of the nitrogen-containing agents in this class?
Explanation
Question 85
A 42-year-old male with end-stage renal disease presents with chronic back pain. Radiographs of the lumbar spine demonstrate dense sclerotic bands at the superior and inferior endplates of the vertebral bodies. This "Rugger-Jersey" spine appearance is a hallmark of which condition?
Explanation
Question 86
Septic arthritis of the hip in infants is frequently complicated by concurrent osteomyelitis of the proximal femur. What anatomical feature of the infant hip uniquely predisposes to this rapid contiguous spread?
Explanation
Question 87
A 78-year-old patient with longstanding polyostotic Paget's disease notes rapid enlargement and extreme pain over his right humerus. Radiographs show a destructive lytic lesion with cortical breakthrough
. What is the generally accepted prognosis for this complication?

Explanation
Question 88
A patient undergoes surgical excision of a large chalky mass over the olecranon bursa
. To optimally preserve the diagnostic crystals for histological examination, which specific processing method must the pathologist utilize?

Explanation
Question 89
Which of the following serum laboratory profiles is most characteristic of PRIMARY hyperparathyroidism?
Explanation
Question 90
A 2-week-old premature infant in the neonatal intensive care unit develops an acutely swollen left thigh and holds the hip in a flexed and externally rotated position. In addition to Staphylococcus aureus, which organism is a leading cause of septic coxitis in this age group and requires empirical coverage?
Explanation
None
