Master ABOS Orthopedic Board Review: Bone Tumors, GIO & Neurofibromatosis | Part 1
Key Takeaway
This ABOS Board Review provides challenging multiple-choice questions on essential orthopedic topics. Master the diagnosis and management of diverse benign and malignant bone tumors, understand glucocorticoid-induced osteoporosis mechanisms and treatments, and review the clinical features and orthopedic complications of Neurofibromatosis Types 1 and 2 for exam success.
Question 1
A 12-year-old boy presents with a 6-month history of dull, aching pain in his right proximal femur, worse with activity. Physical examination reveals mild tenderness over the greater trochanter. Radiographs show a well-defined, lucent lesion in the intertrochanteric region with a sclerotic rim and a ground-glass matrix. There is no periosteal reaction or cortical breach. Bone scan shows increased uptake in the affected area.
View Answer & Explanation
Correct Answer: C
Rationale: The classic radiographic appearance of monostotic fibrous dysplasia includes a well-defined, lucent lesion with a sclerotic rim and a characteristic "ground-glass" matrix due to immature woven bone within a fibrous stroma. Pain is a common symptom, especially in weight-bearing bones. A unicameral bone cyst (A) would typically be purely lytic and often metaphyseal, without the ground-glass appearance. An aneurysmal bone cyst (B) would show expansile, lytic lesions with fluid-fluid levels on MRI. An enchondroma (D) typically has a chondroid matrix with rings and arcs calcification. A non-ossifying fibroma (E) is usually cortically based, eccentric, and has a scalloped sclerotic rim without a ground-glass matrix.
Question 2
A 15-year-old girl presents with a slowly growing, painless mass near her right knee for the past year. On examination, a firm, immobile mass is palpable on the medial aspect of the distal femur, just proximal to the physis. Radiographs reveal a bony exostosis arising from the metaphysis of the distal femur, pointing away from the joint, with continuity of the cortex and medullary canal with the parent bone. The lesion is capped by cartilage.
View Answer & Explanation
Correct Answer: D
Rationale: The description of a bony exostosis arising from the metaphysis, pointing away from the joint, with continuity of the cortex and medullary canal with the parent bone, and capped by cartilage, is pathognomonic for a solitary osteochondroma. Enchondromas (A) are intramedullary cartilaginous lesions. Osteoid osteomas (B) are small, painful lesions with a central nidus. Chondroblastomas (C) are epiphyseal lesions. Parosteal osteosarcoma (E) is a surface osteosarcoma that typically arises from the cortex and is densely ossified, lacking the medullary continuity of an osteochondroma.
Question 3
A 45-year-old man presents with a several-month history of mild, intermittent pain and swelling in his left index finger. He denies trauma. Physical examination reveals fusiform swelling of the proximal phalanx of the left index finger. Radiographs show an expansile, lytic lesion within the proximal phalanx, with endosteal scalloping and punctate calcifications within the matrix. There is no cortical breach or periosteal reaction.
View Answer & Explanation
Correct Answer: C
Rationale: The clinical presentation of an expansile, lytic lesion in a small tubular bone of the hand with punctate or "rings and arcs" calcifications is highly suggestive of an enchondroma. These are common in the phalanges and metacarpals. Giant cell tumors (A) are rare in the hands and typically epiphyseal. Aneurysmal bone cysts (B) are expansile but usually multiloculated with fluid-fluid levels. Osteomyelitis (D) would present with more acute pain, warmth, and signs of infection, often with sequestrum/involucrum. Chondrosarcoma (E) in the hand is rare and usually presents with more aggressive features, though malignant transformation of an enchondroma is a concern, the current description is benign.
Question 4
A 9-year-old boy is evaluated after an incidental finding on a knee radiograph obtained for a minor sports injury. The radiograph shows a well-defined, eccentric, lucent lesion in the metadiaphyseal cortex of the distal femur, with a scalloped sclerotic margin. The lesion is asymptomatic and measures approximately 3 cm in greatest dimension. There is no periosteal reaction or soft tissue mass.
View Answer & Explanation
Correct Answer: B
Rationale: The description of an asymptomatic, eccentric, lucent lesion in the metadiaphyseal cortex with a scalloped sclerotic margin is classic for a non-ossifying fibroma (NOF), also known as a fibrous cortical defect when smaller. These are common developmental lesions that typically resolve spontaneously. Osteosarcoma (A) would be aggressive with periosteal reaction and cortical destruction. Unicameral bone cysts (C) are typically centrally located, purely lytic, and metaphyseal. Fibrous dysplasia (D) has a ground-glass matrix. Osteoid osteoma (E) is typically painful and has a central nidus.
Question 5
A 7-year-old boy presents with a pathological fracture of his left proximal humerus after a fall from a bicycle. He denies prior pain or symptoms. Radiographs show a centrally located, expansile, lytic lesion in the metaphysis of the proximal humerus, with a "fallen leaf" sign visible within the lesion. The cortex is thinned but intact.
View Answer & Explanation
Correct Answer: B
Rationale: The "fallen leaf" sign, which refers to a fragment of cortical bone that has fractured and fallen to the dependent portion of a fluid-filled cavity, is pathognomonic for a unicameral bone cyst (UBC) or simple bone cyst (SBC). These are common causes of pathological fractures in children, often presenting asymptomatically until fracture. Aneurysmal bone cysts (A) are expansile and lytic but typically multiloculated with fluid-fluid levels. Fibrous dysplasia (C) has a ground-glass matrix. Chondroblastomas (D) are epiphyseal. Eosinophilic granulomas (E) are lytic but typically do not show a fallen leaf sign.
Question 6
A 14-year-old girl presents with progressive swelling and pain in her left distal tibia over 3 months. Physical examination reveals a tender, firm mass. Radiographs show an expansile, eccentric, multiloculated lytic lesion in the metadiaphyseal region of the distal tibia, with cortical thinning and a "soap bubble" appearance. MRI reveals multiple fluid-fluid levels within the lesion.
View Answer & Explanation
Correct Answer: C
Rationale: The combination of an expansile, multiloculated lytic lesion with a "soap bubble" appearance on radiographs and characteristic fluid-fluid levels on MRI is diagnostic for an aneurysmal bone cyst (ABC). These are often painful and can cause swelling. Unicameral bone cysts (A) are typically unilocular and lack fluid-fluid levels. Giant cell tumors (B) are typically epiphyseal and do not usually show fluid-fluid levels. Osteosarcoma (D) would show more aggressive features like periosteal reaction and matrix mineralization. Chondromyxoid fibroma (E) is a rare, benign cartilaginous tumor with a lobulated appearance but typically without fluid-fluid levels.
Question 7
A 22-year-old man complains of severe, localized pain in his right proximal tibia for 6 months, worse at night and relieved by aspirin. Physical examination reveals localized tenderness over the anterior aspect of the tibia. Radiographs show cortical thickening and sclerosis in the proximal tibia. A CT scan reveals a small, lucent nidus (approximately 8 mm) within the sclerotic cortex.
View Answer & Explanation
Correct Answer: D
Rationale: The classic presentation of severe nocturnal pain relieved by aspirin, combined with radiographic findings of cortical thickening/sclerosis and a small lucent nidus on CT, is diagnostic for an osteoid osteoma. Osteoblastomas (A) are larger (>1.5-2 cm) and less responsive to NSAIDs. Brodie's abscess (B) is a chronic osteomyelitis with a central lucency but typically presents with signs of infection. Stress fractures (C) cause pain with activity and have a linear lucency or callus formation. Fibrous dysplasia (E) has a ground-glass matrix and is typically not associated with such severe, aspirin-responsive pain.
Question 8
A 16-year-old boy presents with a 4-month history of dull, aching pain in his left distal femur, which is not significantly relieved by NSAIDs. Radiographs show a well-defined, eccentric, lytic lesion in the metaphysis of the distal femur, approximately 4 cm in size, with a thin sclerotic rim and some internal calcifications. There is no periosteal reaction or cortical destruction. Biopsy reveals sheets of benign chondroblasts with areas of myxoid change.
View Answer & Explanation
Correct Answer: C
Rationale: Chondromyxoid fibroma is a rare, benign cartilaginous tumor typically found in the metaphysis of long bones, often presenting with pain. Radiographically, it's a well-defined, eccentric lytic lesion with a sclerotic rim, and sometimes internal calcifications. The biopsy finding of sheets of benign chondroblasts with myxoid change is characteristic. Enchondromas (A) are intramedullary and typically have more distinct chondroid matrix calcifications. Chondroblastomas (B) are typically epiphyseal. Aneurysmal bone cysts (D) are expansile, multiloculated, and have fluid-fluid levels. Osteochondromas (E) are exostoses.
Question 9
A 10-year-old boy presents with a 2-month history of localized pain and swelling over his right mastoid process. He has no fever or other systemic symptoms. Radiographs show a well-defined, punched-out lytic lesion in the mastoid bone. A biopsy is performed, revealing a proliferation of Langerhans cells mixed with eosinophils, lymphocytes, and plasma cells.
View Answer & Explanation
Correct Answer: C
Rationale: The clinical presentation of a solitary, punched-out lytic lesion, especially in the skull or flat bones, in a child, combined with the characteristic histopathology of Langerhans cells mixed with eosinophils, is diagnostic for eosinophilic granuloma, which is the localized form of Langerhans Cell Histiocytosis (LCH). Osteomyelitis (A) would typically have more signs of infection. Ewing sarcoma (B) is a malignant tumor with a different histology and often more aggressive radiographic features. Osteoid osteoma (D) has a sclerotic rim and nidus. Fibrous dysplasia (E) has a ground-glass matrix.
Question 10
A 28-year-old woman presents with a 5-year history of progressive stiffness and pain in her right lower extremity. Physical examination reveals a thickened, sclerotic right tibia and fibula, with limited ankle and knee range of motion. Radiographs show irregular cortical thickening and undulating hyperostosis along the entire length of the right tibia and fibula, resembling "dripping candle wax."
View Answer & Explanation
Correct Answer: C
Rationale: The radiographic appearance of irregular cortical thickening and undulating hyperostosis along the length of a bone, described as "dripping candle wax," is pathognomonic for melorheostosis. This is a rare, non-hereditary sclerosing bone dysplasia that typically affects a single limb or segment. Paget's disease (A) involves bone remodeling with mixed lytic and sclerotic lesions. Osteopetrosis (B) is diffuse increased bone density. Progressive diaphyseal dysplasia (D) causes symmetrical cortical thickening of diaphyses. Osteosarcoma (E) is a malignant tumor with aggressive features.
Question 11
A 6-year-old boy presents with bowing of his left leg and a limp. Radiographs reveal multiple enchondromas predominantly affecting the bones of the left lower extremity, leading to significant deformity and limb length discrepancy. There are no associated soft tissue lesions.
View Answer & Explanation
Correct Answer: B
Rationale: The presence of multiple enchondromas, often with a unilateral or segmental distribution leading to deformity and limb length discrepancy, is characteristic of Ollier's disease (enchondromatosis). Maffucci syndrome (A) is similar but also includes soft tissue hemangiomas, which are absent here. Multiple hereditary exostoses (C) involves multiple osteochondromas, not enchondromas. Fibrous dysplasia (D) presents with ground-glass lesions. Osteogenesis imperfecta (E) is a generalized bone fragility disorder.
Question 12
A 35-year-old woman with a known history of Ollier's disease presents with increasing pain and swelling in her right proximal humerus over the past 6 months. She previously had a stable enchondroma in this location. Radiographs now show cortical destruction, periosteal reaction, and increased size of the lesion with more aggressive calcifications. What is the most likely diagnosis?
View Answer & Explanation
Correct Answer: C
Rationale: In patients with Ollier's disease, there is a significant risk of malignant transformation of enchondromas into chondrosarcomas, particularly with increasing age and in larger lesions. The new onset of pain, swelling, and aggressive radiographic features (cortical destruction, periosteal reaction, increased size) in a previously stable enchondroma is highly suspicious for malignant transformation. A pathological fracture (A) would cause acute pain and typically show a fracture line. Aneurysmal bone cyst formation (B) is less likely to show aggressive cortical destruction. Osteomyelitis (D) would have signs of infection. Giant cell tumors (E) are typically epiphyseal and not directly related to enchondromas.
Question 13
A 19-year-old man with a known solitary osteochondroma of the distal femur presents with acute, severe pain after a direct impact to the lesion. Physical examination reveals localized tenderness and swelling over the osteochondroma. Radiographs show a transverse lucency through the stalk of the osteochondroma. What is the most likely complication?
View Answer & Explanation
Correct Answer: C
Rationale: Acute, severe pain following trauma to an osteochondroma, especially with a radiographic lucency through its stalk, is highly indicative of a fracture of the osteochondroma. This is a common complication, particularly in pedunculated lesions. Malignant transformation (A) is a concern but typically presents with insidious pain and growth, not acute trauma. Bursal formation (B) can cause pain and swelling but usually without acute trauma or a fracture line. Nerve impingement (D) would present with neurological symptoms. Pseudoaneurysm formation (E) is rare and would involve vascular symptoms.
Question 14
A 13-year-old boy presents with chronic, mild pain in his right hip. Radiographs show a shepherd's crook deformity of the proximal femur, characterized by coxa vara and bowing of the femoral shaft, with a ground-glass appearance of the bone. What is the underlying skeletal dysplasia?
View Answer & Explanation
Correct Answer: C
Rationale: The "shepherd's crook" deformity of the proximal femur, characterized by coxa vara and bowing, is a classic and severe manifestation of fibrous dysplasia, particularly the polyostotic form affecting the femur. The ground-glass appearance on radiographs is also characteristic of fibrous dysplasia. Osteogenesis imperfecta (A) causes brittle bones and fractures. Achondroplasia (B) is a dwarfism with short limbs. Multiple hereditary exostoses (D) involves osteochondromas. Progressive diaphyseal dysplasia (E) causes diaphyseal cortical thickening.
Question 15
A 25-year-old man presents with a 3-month history of worsening pain in his left distal femur, near the knee. Physical examination reveals localized tenderness and warmth. Radiographs show an eccentric, lytic lesion in the epiphysis of the distal femur, extending to the subchondral bone, with a thin sclerotic rim and some punctate calcifications. MRI confirms an epiphyseal lesion with surrounding edema.
View Answer & Explanation
Correct Answer: B
Rationale: Chondroblastoma is a rare, benign cartilaginous tumor that characteristically arises in the epiphysis or apophysis of long bones in adolescents and young adults. It presents with pain and can have a lytic appearance with a sclerotic rim and occasional punctate calcifications. Giant cell tumors (A) are also epiphyseal but typically occur after physeal closure and are purely lytic without calcifications. Enchondromas (C) are metaphyseal/diaphyseal. Osteosarcoma (D) would show more aggressive features. Subchondral cysts (E) are typically smaller and associated with degenerative changes.
Question 16
A 4-year-old boy presents with a progressively enlarging mass on the medial aspect of his right knee. Radiographs show an irregular, lobulated cartilaginous mass arising from the medial femoral condyle, causing significant deformity and joint incongruity. The lesion appears to be an overgrowth of the epiphysis.
View Answer & Explanation
Correct Answer: C
Rationale: Dysplasia Epiphysealis Hemimelica (Trevor's Disease) is a rare, benign developmental disorder characterized by localized overgrowth of cartilage, typically affecting an epiphysis or apophysis, often unilateral and involving the knee or ankle. The description of an irregular, lobulated cartilaginous mass arising from the epiphysis causing deformity is classic. Solitary osteochondroma (A) arises from the metaphysis. Chondrosarcoma (B) is malignant. Enchondroma (D) is intramedullary. Synovial chondromatosis (E) involves cartilaginous loose bodies within the joint, not an epiphyseal overgrowth.
Question 17
A 30-year-old man undergoes radiographs for unrelated trauma. Incidental findings include multiple small, round, sclerotic foci scattered throughout the metaphyses and epiphyses of the long bones, particularly prominent in the distal femur. These lesions are asymptomatic and have a "spotty
Question 17
A 12-year-old boy presents with incidental finding of a well-defined, eccentric, lucent lesion in the metaphysis of the distal femur during evaluation for a sports injury. Radiographs show a lesion with a scalloped, sclerotic border, measuring 3 cm in greatest dimension. He is asymptomatic.
View Answer & Explanation
Correct Answer: A
Rationale: Non-ossifying fibromas (NOFs), also known as fibrous cortical defects when smaller, are common, benign, asymptomatic lesions typically found eccentrically in the metaphysis of long bones. They are characterized by a well-defined lucent appearance with a sclerotic, scalloped border. They often resolve spontaneously. Unicameral bone cysts are typically central, expansile, and may present with pathological fracture. Aneurysmal bone cysts are expansile, lytic, and often have fluid-fluid levels. Fibrous dysplasia has a "ground glass" appearance. Enchondromas are often in small bones of hands/feet or central in long bones, with chondroid matrix calcifications.
Question 17
A 16-year-old male complains of persistent, localized pain in his proximal tibia for 6 months. The pain is worse at night and is significantly relieved by over-the-counter NSAIDs. Physical examination reveals localized tenderness. Radiographs show a small, lucent nidus (less than 1.5 cm) surrounded by dense cortical sclerosis.
View Answer & Explanation
Correct Answer: A
Rationale: The classic presentation of an osteoid osteoma includes nocturnal pain relieved by NSAIDs, localized tenderness, and a small lucent nidus with surrounding sclerosis on radiographs. Osteoblastomas are similar but typically larger (greater than 2 cm) and less responsive to NSAIDs. Stress fractures lack a distinct nidus. Chronic osteomyelitis would likely have systemic symptoms and different radiographic features. Ewing sarcoma is a malignant tumor with aggressive features.
Question 17
A 7-year-old boy presents to the emergency department after falling on his arm, complaining of severe pain in his left shoulder. Radiographs reveal a pathological fracture through a large, centrally located, expansile, lytic lesion in the proximal humerus. A "fallen leaf" sign is noted within the lesion.
View Answer & Explanation
Correct Answer: A
Rationale: Unicameral bone cysts (UBCs) are common benign bone lesions in children, often presenting with pathological fractures, particularly in the proximal humerus or femur. They are typically centrally located, expansile, and lytic. The "fallen leaf" sign, representing a fragment of cortical bone that has fallen into the fluid-filled cyst, is pathognomonic for a UBC. Aneurysmal bone cysts are typically eccentric and may show fluid-fluid levels. Fibrous dysplasia has a "ground glass" appearance. Enchondromas are less common in this location and often have chondroid matrix. Langerhans cell histiocytosis can be lytic but less commonly presents with a "fallen leaf" sign.
Question 17
A 15-year-old girl presents with chronic knee pain, worse with activity. Radiographs show a well-defined, lytic lesion in the epiphysis of the distal femur, with some punctate calcifications. MRI confirms an epiphyseal lesion with surrounding edema.
View Answer & Explanation
Correct Answer: A
Rationale: Chondroblastoma is a rare, benign cartilaginous tumor that characteristically occurs in the epiphysis or apophysis of long bones in adolescents and young adults. It typically presents with pain and is seen as a lytic lesion with a sclerotic rim, often with punctate calcifications. Giant cell tumors are also epiphyseal but occur in skeletally mature individuals and lack chondroid matrix. Osteochondromas are exophytic lesions from the metaphysis. Enchondromas are typically metaphyseal or diaphyseal. Osteosarcoma is malignant and would show more aggressive features.
Question 17
A 14-year-old boy presents with a rapidly growing, painful mass in his proximal tibia. Radiographs show an eccentric, expansile, lytic lesion with a thin sclerotic rim and internal septations. MRI reveals multiple fluid-fluid levels within the lesion.
View Answer & Explanation
Correct Answer: A
Rationale: The clinical presentation of a rapidly growing, painful, eccentric, expansile lytic lesion with internal septations and, most importantly, fluid-fluid levels on MRI, is highly characteristic of an aneurysmal bone cyst (ABC). UBCs are typically central and lack fluid-fluid levels. Osteosarcoma is malignant and would show more aggressive features like cortical destruction and periosteal reaction. Fibrous dysplasia has a "ground glass" appearance. Chondromyxoid fibromas are eccentric, lytic, and septated but typically lack fluid-fluid levels.
Question 17
A 35-year-old woman presents with progressive pain and swelling around her knee for several months. Radiographs show a large, lytic lesion involving the distal femoral epiphysis and extending into the metaphysis, with no evidence of matrix calcification or periosteal reaction. She is skeletally mature.
View Answer & Explanation
Correct Answer: A
Rationale: Giant cell tumors (GCTs) are typically found in skeletally mature individuals (3rd-5th decades) and are characterized by their epiphyseal location, often extending into the metaphysis. They are purely lytic, aggressive lesions without matrix production. Chondroblastomas are epiphyseal but occur in adolescents. Aneurysmal bone cysts can be aggressive but often have fluid-fluid levels and occur in younger patients. Enchondromas are typically metaphyseal/diaphyseal and have chondroid matrix. Osteosarcoma would show aggressive features like periosteal reaction and osteoid matrix.
Question 17
A 4-year-old boy presents with a painful, palpable lump on his scalp. Radiographs of the skull reveal a well-demarcated, lytic lesion with a "punched-out" appearance and a "beveled edge." There are no other systemic symptoms.
View Answer & Explanation
Correct Answer: A
Rationale: Eosinophilic granuloma, the most benign form of Langerhans cell histiocytosis, commonly presents as a solitary lytic lesion in the skull of children. The "punched-out" appearance with a "beveled edge" (or "hole within a hole") is a classic radiographic finding. Epidermoid cysts are typically well-corticated and less aggressive. Osteomyelitis would have more ill-defined margins and possibly sequestra. Neuroblastoma metastases are usually multiple and less well-defined. Fibrous dysplasia has a "ground glass" appearance.
Question 17
A 9-year-old girl presents with progressive bowing of her right tibia and a limp. Radiographs show diffuse expansion and sclerosis of the tibial diaphysis with a "ground glass" appearance and cortical thickening. There is no evidence of periosteal reaction or soft tissue mass.
View Answer & Explanation
Correct Answer: A
Rationale: Fibrous dysplasia is a developmental anomaly where normal bone is replaced by fibrous tissue and immature woven bone. It often presents with bowing deformities and has a characteristic "ground glass" appearance on radiographs due to the immature woven bone. Osteofibrous dysplasia is similar but typically affects the anterior cortex of the tibia in younger children and is often self-limiting. Adamantinoma is a rare malignant tumor of the tibia, usually in adults. Paget's disease affects older adults. Rickets would show widened growth plates and generalized osteopenia.
Question 17
A 45-year-old man has an incidental finding of a well-circumscribed, lucent lesion with speckled calcifications in the proximal phalanx of his left index finger during a hand injury evaluation. He denies pain or swelling in the digit.
View Answer & Explanation
Correct Answer: A
Rationale: Enchondromas are common benign cartilaginous tumors, frequently found incidentally in the small bones of the hands and feet. They appear as well-circumscribed lucent lesions with characteristic punctate or speckled calcifications (chondroid matrix). Asymptomatic lesions are typically observed. Chondrosarcoma is a malignant tumor, but primary chondrosarcoma of the hand is rare, and this lesion lacks aggressive features. Glomus tumors are painful, subungual lesions. Epidermoid inclusion cysts are purely lytic. Giant cell tumors of the tendon sheath are soft tissue masses.
Question 17
A 10-year-old boy presents with a painless, hard mass near his right knee. Radiographs show a bony projection arising from the metaphysis of the distal femur, pointing away from the joint. The cortex and medullary cavity of the lesion are continuous with the host bone.
View Answer & Explanation
Correct Answer: A
Rationale: Osteochondroma is the most common benign bone tumor, characterized by a bony outgrowth from the metaphysis of a long bone, covered by a cartilaginous cap. The key diagnostic feature is the continuity of the cortex and medullary cavity of the lesion with the host bone. Parosteal osteosarcoma is a malignant surface lesion but lacks medullary continuity. Myositis ossificans is heterotopic ossification in soft tissues, not continuous with bone marrow. Juxtacortical chondroma is a cartilaginous lesion on the bone surface. Fibrous cortical defects are intraosseous lucent lesions.
Question 17
A 3-year-old boy presents with progressive anterior bowing of his left tibia. Radiographs show a well-defined, lytic lesion with a sclerotic rim, primarily involving the anterior cortex of the mid-diaphysis of the tibia. There is no evidence of a pathological fracture or other bone involvement.
View Answer & Explanation
Correct Answer: A
Rationale: Osteofibrous dysplasia (OFD) is a rare, benign fibro-osseous lesion almost exclusively found in the anterior cortex of the tibia in young children. It often presents with anterior bowing and can be mistaken for fibrous dysplasia, but OFD is typically more localized to the cortex and has a different histological appearance. Fibrous dysplasia is more diffuse and has a "ground glass" appearance. Congenital pseudarthrosis of the tibia is a distinct entity involving non-union. Adamantinoma is a malignant tumor of the tibia, typically in adults. Rickets would show generalized bone changes.
Question 17
A 48-year-old man presents with a slowly enlarging, painful mass in his anterior tibia. Radiographs show a large, eccentric, lytic lesion with cortical destruction and a "soap bubble" appearance. Biopsy reveals epithelial and osteofibrous components.
View Answer & Explanation
Correct Answer: A
Rationale: Adamantinoma is a rare, low-grade malignant tumor that almost exclusively affects the tibia, typically in adults. It is characterized by a lytic, often eccentric, lesion with a "soap bubble" appearance and cortical destruction. The biphasic histology (epithelial and osteofibrous components) is pathognomonic. Osteofibrous dysplasia occurs in younger patients and is benign. Fibrous dysplasia has a "ground glass" appearance. Chondrosarcoma would have chondroid matrix. Metastatic carcinoma is possible but less likely to be solitary in the tibia with this specific radiographic appearance.
Question 17
A 6-year-old boy undergoes radiographs for a minor knee injury. An incidental finding of a small, well-defined, lucent lesion with a sclerotic rim is noted in the metaphysis of the distal femur. The lesion is asymptomatic and measures 1.5 cm. On follow-up radiographs a year later, the lesion appears smaller and more sclerotic.
View Answer & Explanation
Correct Answer: A
Rationale: A fibrous cortical defect (FCD) is a common, asymptomatic, benign lesion found in the metaphysis of long bones in children. It is typically small, well-defined, lucent, and has a sclerotic rim. FCDs are known to spontaneously regress and ossify over time, which aligns with the follow-up finding. Osteoid osteoma causes pain relieved by NSAIDs. Unicameral bone cysts are larger and often present with fracture. Enchondromas have chondroid matrix. Chondroblastomas are epiphyseal and symptomatic.
Question 17
A 55-year-old woman with a history of chronic renal failure and secondary hyperparathyroidism presents with pain in her jaw. Radiographs reveal a lytic, expansile lesion in the mandible. Laboratory tests show elevated parathyroid hormone and calcium levels.
View Answer & Explanation
Correct Answer: A
Rationale: Brown tumors are non-neoplastic lesions that occur as a direct consequence of hyperparathyroidism, leading to increased osteoclastic activity and bone resorption. They are characterized by collections of osteoclast-like giant cells and fibrous stroma, appearing as lytic, expansile lesions on radiographs. The history of chronic renal failure and elevated PTH strongly points to this diagnosis. Giant cell tumors are true neoplasms. Ameloblastoma is an odontogenic tumor. Fibrous dysplasia has a "ground glass" appearance. Osteomyelitis would have different clinical and radiographic features.
Question 17
An 80-year-old man reports an increase in his hat size and deep, aching pain in his right femur. Radiographs of the femur show cortical thickening, trabecular coarsening, and a mixed lytic and sclerotic pattern, described as "cotton wool" appearance. Alkaline phosphatase levels are significantly elevated.
View Answer & Explanation
Correct Answer: A
Rationale: Paget's disease of bone (osteitis deformans) is a chronic disorder
Question 18
A 12-year-old boy presents with incidental finding of a well-defined, eccentric, lucent lesion in the metaphysis of the distal femur during evaluation for a sports injury. Radiographs show a lesion with a scalloped, sclerotic border, measuring 3 cm in greatest dimension. He is asymptomatic.
View Answer & Explanation
Correct Answer: A
Rationale: Non-ossifying fibromas (NOFs), also known as fibrous cortical defects when smaller, are common, benign, asymptomatic lesions typically found eccentrically in the metaphysis of long bones. They are characterized by a well-defined lucent appearance with a sclerotic, scalloped border. They often resolve spontaneously. Unicameral bone cysts are typically central, expansile, and may present with pathological fracture. Aneurysmal bone cysts are expansile, lytic, and often have fluid-fluid levels. Fibrous dysplasia has a "ground glass" appearance. Enchondromas are often in small bones of hands/feet or central in long bones, with chondroid matrix calcifications.
Question 19
A 16-year-old male complains of persistent, localized pain in his proximal tibia for 6 months. The pain is worse at night and is significantly relieved by over-the-counter NSAIDs. Physical examination reveals localized tenderness. Radiographs show a small, lucent nidus (less than 1.5 cm) surrounded by dense cortical sclerosis.
View Answer & Explanation
Correct Answer: A
Rationale: The classic presentation of an osteoid osteoma includes nocturnal pain relieved by NSAIDs, localized tenderness, and a small lucent nidus with surrounding sclerosis on radiographs. Osteoblastomas are similar but typically larger (greater than 2 cm) and less responsive to NSAIDs. Stress fractures lack a distinct nidus. Chronic osteomyelitis would likely have systemic symptoms and different radiographic features. Ewing sarcoma is a malignant tumor with aggressive features.
Question 20
A 7-year-old boy presents to the emergency department after falling on his arm, complaining of severe pain in his left shoulder. Radiographs reveal a pathological fracture through a large, centrally located, expansile, lytic lesion in the proximal humerus. A "fallen leaf" sign is noted within the lesion.
View Answer & Explanation
Correct Answer: A
Rationale: Unicameral bone cysts (UBCs) are common benign bone lesions in children, often presenting with pathological fractures, particularly in the proximal humerus or femur. They are typically centrally located, expansile, and lytic. The "fallen leaf" sign, representing a fragment of cortical bone that has fallen into the fluid-filled cyst, is pathognomonic for a UBC. Aneurysmal bone cysts are typically eccentric and may show fluid-fluid levels. Fibrous dysplasia has a "ground glass" appearance. Enchondromas are less common in this location and often have chondroid matrix. Langerhans cell histiocytosis can be lytic but less commonly presents with a "fallen leaf" sign.
Question 21
A 15-year-old girl presents with chronic knee pain, worse with activity. Radiographs show a well-defined, lytic lesion in the epiphysis of the distal femur, with some punctate calcifications. MRI confirms an epiphyseal lesion with surrounding edema.
View Answer & Explanation
Correct Answer: A
Rationale: Chondroblastoma is a rare, benign cartilaginous tumor that characteristically occurs in the epiphysis or apophysis of long bones in adolescents and young adults. It typically presents with pain and is seen as a lytic lesion with a sclerotic rim, often with punctate calcifications. Giant cell tumors are also epiphyseal but occur in skeletally mature individuals and lack chondroid matrix. Osteochondromas are exophytic lesions from the metaphysis. Enchondromas are typically metaphyseal or diaphyseal. Osteosarcoma is malignant and would show more aggressive features.
Question 22
A 14-year-old boy presents with a rapidly growing, painful mass in his proximal tibia. Radiographs show an eccentric, expansile, lytic lesion with a thin sclerotic rim and internal septations. MRI reveals multiple fluid-fluid levels within the lesion.
View Answer & Explanation
Correct Answer: A
Rationale: The clinical presentation of a rapidly growing, painful, eccentric, expansile lytic lesion with internal septations and, most importantly, fluid-fluid levels on MRI, is highly characteristic of an aneurysmal bone cyst (ABC). UBCs are typically central and lack fluid-fluid levels. Osteosarcoma is malignant and would show more aggressive features like cortical destruction and periosteal reaction. Fibrous dysplasia has a "ground glass" appearance. Chondromyxoid fibromas are eccentric, lytic, and septated but typically lack fluid-fluid levels.
Question 23
A 35-year-old woman presents with progressive pain and swelling around her knee for several months. Radiographs show a large, lytic lesion involving the distal femoral epiphysis and extending into the metaphysis, with no evidence of matrix calcification or periosteal reaction. She is skeletally mature.
View Answer & Explanation
Correct Answer: A
Rationale: Giant cell tumors (GCTs) are typically found in skeletally mature individuals (3rd-5th decades) and are characterized by their epiphyseal location, often extending into the metaphysis. They are purely lytic, aggressive lesions without matrix production. Chondroblastomas are epiphyseal but occur in adolescents. Aneurysmal bone cysts can be aggressive but often have fluid-fluid levels and occur in younger patients. Enchondromas are typically metaphyseal/diaphyseal and have chondroid matrix. Osteosarcoma would show aggressive features like periosteal reaction and osteoid matrix.
Question 24
A 4-year-old boy presents with a painful, palpable lump on his scalp. Radiographs of the skull reveal a well-demarcated, lytic lesion with a "punched-out" appearance and a "beveled edge." There are no other systemic symptoms.
View Answer & Explanation
Correct Answer: A
Rationale: Eosinophilic granuloma, the most benign form of Langerhans cell histiocytosis, commonly presents as a solitary lytic lesion in the skull of children. The "punched-out" appearance with a "beveled edge" (or "hole within a hole") is a classic radiographic finding. Epidermoid cysts are typically well-corticated and less aggressive. Osteomyelitis would have more ill-defined margins and possibly sequestra. Neuroblastoma metastases are usually multiple and less well-defined. Fibrous dysplasia has a "ground glass" appearance.
Question 25
A 9-year-old girl presents with progressive bowing of her right tibia and a limp. Radiographs show diffuse expansion and sclerosis of the tibial diaphysis with a "ground glass" appearance and cortical thickening. There is no evidence of periosteal reaction or soft tissue mass.
View Answer & Explanation
Correct Answer: A
Rationale: Fibrous dysplasia is a developmental anomaly where normal bone is replaced by fibrous tissue and immature woven bone. It often presents with bowing deformities and has a characteristic "ground glass" appearance on radiographs due to the immature woven bone. Osteofibrous dysplasia is similar but typically affects the anterior cortex of the tibia in younger children and is often self-limiting. Adamantinoma is a rare malignant tumor of the tibia, usually in adults. Paget's disease affects older adults. Rickets would show widened growth plates and generalized osteopenia.
Question 26
A 45-year-old man has an incidental finding of a well-circumscribed, lucent lesion with speckled calcifications in the proximal phalanx of his left index finger during a hand injury evaluation. He denies pain or swelling in the digit.
View Answer & Explanation
Correct Answer: A
Rationale: Enchondromas are common benign cartilaginous tumors, frequently found incidentally in the small bones of the hands and feet. They appear as well-circumscribed lucent lesions with characteristic punctate or speckled calcifications (chondroid matrix). Asymptomatic lesions are typically observed. Chondrosarcoma is a malignant tumor, but primary chondrosarcoma of the hand is rare, and this lesion lacks aggressive features. Glomus tumors are painful, subungual lesions. Epidermoid inclusion cysts are purely lytic. Giant cell tumors of the tendon sheath are soft tissue masses.
Question 27
A 10-year-old boy presents with a painless, hard mass near his right knee. Radiographs show a bony projection arising from the metaphysis of the distal femur, pointing away from the joint. The cortex and medullary cavity of the lesion are continuous with the host bone.
View Answer & Explanation
Correct Answer: A
Rationale: Osteochondroma is the most common benign bone tumor, characterized by a bony outgrowth from the metaphysis of a long bone, covered by a cartilaginous cap. The key diagnostic feature is the continuity of the cortex and medullary cavity of the lesion with the host bone. Parosteal osteosarcoma is a malignant surface lesion but lacks medullary continuity. Myositis ossificans is heterotopic ossification in soft tissues, not continuous with bone marrow. Juxtacortical chondroma is a cartilaginous lesion on the bone surface. Fibrous cortical defects are intraosseous lucent lesions.
Question 28
A 3-year-old boy presents with progressive anterior bowing of his left tibia. Radiographs show a well-defined, lytic lesion with a sclerotic rim, primarily involving the anterior cortex of the mid-diaphysis of the tibia. There is no evidence of a pathological fracture or other bone involvement.
View Answer & Explanation
Correct Answer: A
Rationale: Osteofibrous dysplasia (OFD) is a rare, benign fibro-osseous lesion almost exclusively found in the anterior cortex of the tibia in young children. It often presents with anterior bowing and can be mistaken for fibrous dysplasia, but OFD is typically more localized to the cortex and has a different histological appearance. Fibrous dysplasia is more diffuse and has a "ground glass" appearance. Congenital pseudarthrosis of the tibia is a distinct entity involving non-union. Adamantinoma is a malignant tumor of the tibia, typically in adults. Rickets would show generalized bone changes.
Question 29
A 48-year-old man presents with a slowly enlarging, painful mass in his anterior tibia. Radiographs show a large, eccentric, lytic lesion with cortical destruction and a "soap bubble" appearance. Biopsy reveals epithelial and osteofibrous components.
View Answer & Explanation
Correct Answer: A
Rationale: Adamantinoma is a rare, low-grade malignant tumor that almost exclusively affects the tibia, typically in adults. It is characterized by a lytic, often eccentric, lesion with a "soap bubble" appearance and cortical destruction. The biphasic histology (epithelial and osteofibrous components) is pathognomonic. Osteofibrous dysplasia occurs in younger patients and is benign. Fibrous dysplasia has a "ground glass" appearance. Chondrosarcoma would have chondroid matrix. Metastatic carcinoma is possible but less likely to be solitary in the tibia with this specific radiographic appearance.
Question 30
A 6-year-old boy undergoes radiographs for a minor knee injury. An incidental finding of a small, well-defined, lucent lesion with a sclerotic rim is noted in the metaphysis of the distal femur. The lesion is asymptomatic and measures 1.5 cm. On follow-up radiographs a year later, the lesion appears smaller and more sclerotic.
View Answer & Explanation
Correct Answer: A
Rationale: A fibrous cortical defect (FCD) is a common, asymptomatic, benign lesion found in the metaphysis of long bones in children. It is typically small, well-defined, lucent, and has a sclerotic rim. FCDs are known to spontaneously regress and ossify over time, which aligns with the follow-up finding. Osteoid osteoma causes pain relieved by NSAIDs. Unicameral bone cysts are larger and often present with fracture. Enchondromas have chondroid matrix. Chondroblastomas are epiphyseal and symptomatic.
Question 31
A 55-year-old woman with a history of chronic renal failure and secondary hyperparathyroidism presents with pain in her jaw. Radiographs reveal a lytic, expansile lesion in the mandible. Laboratory tests show elevated parathyroid hormone and calcium levels.
View Answer & Explanation
Correct Answer: A
Rationale: Brown tumors are non-neoplastic lesions that occur as a direct consequence of hyperparathyroidism, leading to increased osteoclastic activity and bone resorption. They are characterized by collections of osteoclast-like giant cells and fibrous stroma, appearing as lytic, expansile lesions on radiographs. The history of chronic renal failure and elevated PTH strongly points to this diagnosis. Giant cell tumors are true neoplasms. Ameloblastoma is an odontogenic tumor. Fibrous dysplasia has a "ground glass" appearance. Osteomyelitis would have different clinical and radiographic features.
Question 32
A 62-year-old female on chronic prednisone for rheumatoid arthritis presents with new onset back pain. A DEXA scan shows a T-score of -2.8 at the lumbar spine.
View Answer & Explanation
Correct Answer: B
Rationale: Glucocorticoids primarily induce osteoporosis by directly inhibiting osteoblast differentiation and activity, leading to decreased bone formation. They also increase osteocyte apoptosis, impairing bone maintenance and repair, and prolong the lifespan of osteoclasts, leading to increased bone resorption. Option A is incorrect as glucocorticoids tend to prolong osteoclast lifespan, not increase their apoptosis. Option C is incorrect as glucocorticoids decrease, rather than enhance, intestinal calcium absorption. Option D is incorrect as glucocorticoids can suppress PTH secretion initially, though chronic use can lead to secondary hyperparathyroidism due to hypocalcemia. Option E is incorrect as glucocorticoids can increase RANKL expression, promoting osteoclastogenesis.
Question 33
A 55-year-old male with Crohn's disease is starting a new course of prednisone 20 mg daily. He has no prior history of fractures.
View Answer & Explanation
Correct Answer: C
Rationale: The daily dose of glucocorticoids is the most significant independent risk factor for glucocorticoid-induced osteoporosis (GIO), with higher doses conferring a greater risk. A prednisone dose of 20 mg daily is considered a high dose. While age over 50 (B), underlying Crohn's disease (D), and smoking (E) are all risk factors for osteoporosis, the dose of glucocorticoids is the primary driver of GIO risk. Male gender (A) is generally a lower risk factor for osteoporosis compared to female gender, but men on glucocorticoids are still at significant risk.
Question 34
A 48-year-old female has been on prednisone 10 mg daily for 6 months for systemic lupus erythematosus. She has no prior fractures.
View Answer & Explanation
Correct Answer: D
Rationale: A Dual-energy X-ray absorptiometry (DEXA) scan is the gold standard for diagnosing osteoporosis and monitoring bone mineral density (BMD). It is recommended for all patients initiating or on long-term glucocorticoid therapy. While serum calcium and phosphate levels (A) are important for general bone health, they do not directly assess BMD or fracture risk. Bone turnover markers (B) can provide insights into bone remodeling but are not primary diagnostic tools for osteoporosis. Lateral spine radiographs (C) are used to identify vertebral fractures, but not for initial diagnosis of osteoporosis in the absence of symptoms or high risk. QCT (E) can assess volumetric BMD but is less commonly used than DEXA due to higher cost and radiation exposure.
Question 35
A 35-year-old male is initiated on prednisone 7.5 mg daily for severe asthma. He has no history of fractures and a normal baseline DEXA scan.
View Answer & Explanation
Correct Answer: C
Rationale: For patients initiating glucocorticoid therapy with a moderate to high risk of fracture (e.g., prednisone ≥ 7.5 mg/day for ≥ 3 months), oral bisphosphonates like alendronate are generally the first-line pharmacologic agents for prevention and treatment of GIO. Teriparatide (A), denosumab (B), and romosozumab (D) are typically reserved for patients with severe osteoporosis, very high fracture risk, or those who have failed or are intolerant to bisphosphonates. Calcitonin (E) has limited efficacy and is not a first-line agent for GIO.
Question 36
A 68-year-old female on chronic prednisone 15 mg daily for polymyalgia rheumatica presents with a new vertebral compression fracture. Her DEXA T-score is -3.2 at the lumbar spine.
View Answer & Explanation
Correct Answer: D
Rationale: This patient has severe glucocorticoid-induced osteoporosis (T-score < -2.5 and a fragility fracture) and is on a high dose of prednisone. Oral bisphosphonates like risedronate are the recommended first-line treatment for GIO. Intravenous zoledronic acid (B) is an option, especially if oral bisphosphonates are not tolerated or contraindicated, but oral agents are typically tried first. Raloxifene (A) is a selective estrogen receptor modulator (SERM) primarily used in postmenopausal women for prevention and treatment, but less effective than bisphosphonates for GIO. Estrogen replacement therapy (C) is generally not recommended as a primary osteoporosis treatment due to potential risks. Calcitonin (E) has weak anti-fracture efficacy and is not a first-line treatment.
Question 37
A 72-year-old male with severe glucocorticoid-induced osteoporosis (T-score -3.5, multiple vertebral fractures) has failed oral bisphosphonate therapy due to persistent fractures and declining BMD. He is still on prednisone 10 mg daily.
View Answer & Explanation
Correct Answer: B
Rationale: This patient has severe GIO with persistent fractures despite bisphosphonate therapy, indicating a need for a more potent agent, particularly an anabolic one. Romosozumab is an anabolic agent that both increases bone formation and decreases bone resorption, making it highly effective for severe osteoporosis and those with very high fracture risk or treatment failure. Denosumab (A) is a potent antiresorptive agent, but anabolic agents are often preferred in cases of severe osteoporosis with treatment failure. Ibandronate (C) is an oral bisphosphonate, which the patient has already failed. Strontium ranelate (D) is not approved in the US and has safety concerns. Vitamin K2 supplementation (E) is not a primary treatment for severe osteoporosis.
Question 38
A 58-year-old female is starting prednisone 10 mg daily for giant cell arteritis. Her baseline serum 25-hydroxyvitamin D level is 22 ng/mL.
View Answer & Explanation
Correct Answer: C
Rationale: For adults at risk of osteoporosis, including those on glucocorticoids, the recommended daily intake of elemental calcium is 1000-1200 mg and vitamin D is 800-1000 IU. Her baseline vitamin D level of 22 ng/mL indicates insufficiency, further supporting the need for adequate supplementation. Options A and B provide insufficient amounts. Options D and E provide higher doses that may be used in cases of severe deficiency or specific conditions but are generally above the standard recommendation for initial prevention in this context.
Question 39
A 60-year-old female is on prednisone 7.5 mg daily for 3 months. Her DEXA T-score is -1.8 at the femoral neck. She has no prior fractures.
View Answer & Explanation
Correct Answer: C
Rationale: The Fracture Risk Assessment Tool (FRAX) is widely used to estimate the 10-year probability of major osteoporotic fracture and hip fracture, incorporating clinical risk factors (including glucocorticoid use) and femoral neck BMD. This patient has osteopenia (T-score -1.8) and is on glucocorticoids, making FRAX an appropriate tool to guide treatment decisions. TBS (A) assesses bone microarchitecture but is not a primary risk assessment tool. QCT (B) and HR-pQCT (E) are advanced imaging techniques not routinely used for initial risk assessment. BTMs (D) reflect bone remodeling rates but do not directly predict fracture risk.
Question 40
A 28-year-old pre-menopausal female with systemic lupus erythematosus requires long-term prednisone 10 mg daily. Her baseline DEXA T-score is -1.5 at the lumbar spine. She desires future pregnancy.
View Answer & Explanation
Correct Answer: E
Rationale: In pre-menopausal women, especially those desiring future pregnancy, bisphosphonates (A, B) and denosumab (C) are generally avoided due to their long half-lives and potential teratogenicity. Teriparatide (D) is also contraindicated in pregnancy. For pre-menopausal women on glucocorticoids with osteopenia (T-score -1.5) and no prior fractures, the initial approach often involves optimizing calcium and vitamin D intake, addressing secondary causes, and monitoring. Pharmacologic therapy is usually reserved for those with a history of fragility fracture or very low BMD (Z-score < -2.0) and then with careful consideration of reproductive plans. Given her desire for future pregnancy, avoiding medications with long-term fetal risks is paramount.
Question 41
A 65-year-old male has been on alendronate for 5 years for glucocorticoid-induced osteoporosis, initiated after a vertebral fracture. His prednisone dose has been tapered to 2.5 mg daily for the past year, and his DEXA T-score has improved from -3.0 to -2.2.
View Answer & Explanation
Correct Answer: C
Rationale: For patients on bisphosphonates for 3-5 years with stable or improved BMD, no recent fractures, and a lower fracture risk (e.g., T-score > -2.5), a drug holiday can be considered. This patient has been on alendronate for 5 years, his prednisone dose is low, and his T-score has improved to osteopenia. While he had a prior vertebral fracture, the overall risk profile has improved. A drug holiday allows for a reduction in potential long-term bisphosphonate side effects (e.g., atypical femoral fractures, osteonecrosis of the jaw) while retaining some residual bone protection. Discontinuing immediately (A) might be too abrupt. Continuing indefinitely (B) increases long-term risks. Switching to denosumab (D) or teriparatide (E) is typically for escalating therapy, not de-escalation.
Question 42
A 70-year-old female on chronic prednisone for polymyalgia rheumatica and alendronate for 8 years for GIO presents with new onset dull, aching pain in her right thigh. Radiographs show cortical thickening of the lateral subtrochanteric femur.
View Answer & Explanation
Correct Answer: C
Rationale: The clinical presentation of dull, aching thigh pain, especially in a patient on long-term bisphosphonate therapy (8 years of alendronate), combined with radiographic findings of cortical thickening of the lateral subtrochanteric femur, is highly suggestive of an impending or complete atypical femoral fracture (AFF). AFFs are a rare but serious complication associated with long-term bisphosphonate use. Stress fractures of the femoral neck (A) typically occur with repetitive stress and may not show the characteristic cortical thickening. Metastatic bone disease (B) would be less likely to present with this specific radiographic finding in the absence of a known primary malignancy. Osteonecrosis of the femoral head (D) is a known complication of glucocorticoid use but typically presents with groin pain and characteristic MRI findings, not usually cortical thickening. Trochanteric bursitis (E) is soft tissue inflammation and would not show bone changes.
Question 43
A 45-year-old male on high-dose prednisone for 1 year following renal transplant develops severe left hip pain. Radiographs are initially normal, but MRI shows subchondral collapse and marrow edema in the femoral head.
Question 44
A 45-year-old male with a history of Crohn's disease has been on chronic oral prednisone 20 mg daily for the past 3 years. He presents for routine follow-up. A recent DEXA scan shows a T-score of -2.8 at the lumbar spine. Which of the following is the primary mechanism by which glucocorticoids contribute to osteoporosis?
View Answer & Explanation
Correct Answer: C
Rationale: Glucocorticoids primarily induce osteoporosis by directly inhibiting osteoblast differentiation and promoting their apoptosis, leading to decreased bone formation. They also increase osteoclastogenesis indirectly by affecting osteoblast/stromal cell production of RANKL and OPG, and prolong osteoclast lifespan. Option A is incorrect because glucocorticoids primarily increase osteoclast activity indirectly. Option B and D are incorrect as glucocorticoids decrease intestinal calcium absorption and increase renal calcium excretion, respectively, leading to secondary hyperparathyroidism.
Question 45
A 62-year-old female with rheumatoid arthritis has been on prednisone 7.5 mg daily for 5 years. She has a history of a distal radius fracture 2 years ago. Her current DEXA scan shows a T-score of -2.0 at the femoral neck. Which of the following factors is most strongly associated with an increased risk of glucocorticoid-induced osteoporosis (GIO) and fracture?
View Answer & Explanation
Correct Answer: C
Rationale: The cumulative dose of glucocorticoids over time is a critical determinant of GIO risk, even more so than the daily dose alone, especially when considering long-term use. While a daily dose >5 mg is a risk factor, the total exposure is key. Short-term use carries less risk. Female gender and older age are generally associated with higher osteoporosis risk, not lower. Option A is incorrect as doses >5mg/day are generally considered high risk. Option B is incorrect as long-term use is the primary concern. Option D and E are incorrect as female gender and older age are generally higher risk factors for osteoporosis.
Question 46
A 38-year-old female is initiated on high-dose oral prednisone (40 mg daily) for severe systemic lupus erythematosus. She has no prior history of fractures or osteoporosis. What is the most appropriate initial diagnostic test and timing for assessing her bone health in the context of glucocorticoid therapy?
View Answer & Explanation
Correct Answer: E
Rationale: A baseline DEXA scan is recommended for all patients initiating long-term glucocorticoid therapy (defined as ≥3 months at a prednisone equivalent dose of ≥2.5 mg/day) to establish baseline bone mineral density (BMD) and assess fracture risk. This should ideally be performed within 6 weeks of starting therapy. Subsequent scans are typically performed annually. Option A is important but not the primary diagnostic test for bone density. Options B and C are too late for a baseline assessment. Option D is not the standard initial diagnostic test for osteoporosis.
Question 47
A 55-year-old male is prescribed prednisone 10 mg daily for 6 months due to polymyalgia rheumatica. He has no prior history of osteoporosis or fractures. His baseline DEXA scan shows a T-score of -1.2 at the lumbar spine. Which of the following non-pharmacologic interventions is universally recommended for all patients starting long-term glucocorticoid therapy?
View Answer & Explanation
Correct Answer: B
Rationale: Adequate intake of calcium and vitamin D is a cornerstone of osteoporosis prevention and treatment, and it is universally recommended for all patients initiating long-term glucocorticoid therapy, regardless of their baseline bone density or fracture risk. Options A, C, D, and E are important lifestyle modifications that should be encouraged, but calcium and vitamin D supplementation are considered a mandatory baseline intervention for all patients on chronic steroids.
Question 48
A 70-year-old female with chronic obstructive pulmonary disease (COPD) has been on prednisone 15 mg daily for 2 years. Her recent DEXA scan reveals a T-score of -2.7 at the lumbar spine and -2.5 at the femoral neck. She has no history of prior fractures. Her serum calcium and vitamin D levels are within normal limits with supplementation. Which of the following is the most appropriate first-line pharmacologic treatment for her glucocorticoid-induced osteoporosis?
View Answer & Explanation
Correct Answer: C
Rationale: Oral bisphosphonates (e.g., alendronate, risedronate) are generally considered the first-line pharmacologic treatment for glucocorticoid-induced osteoporosis in patients with a high fracture risk (T-score ≤ -2.5 or T-score between -1.0 and -2.5 with additional risk factors like prior fracture or high FRAX score). They are effective, well-studied, and generally well-tolerated. Teriparatide, denosumab, and romosozumab are typically reserved for patients with severe osteoporosis, very high fracture risk, or intolerance/failure of bisphosphonates. Raloxifene is a selective estrogen receptor modulator (SERM) primarily used in postmenopausal women for prevention and treatment, but not first-line for GIO.
Question 49
A 58-year-old male with a history of severe asthma has been on chronic oral glucocorticoids for 10 years. He has developed severe glucocorticoid-induced osteoporosis, evidenced by a T-score of -3.5 at the lumbar spine and two new vertebral compression fractures despite 2 years of consistent oral alendronate therapy and adequate calcium/vitamin D supplementation. He has normal renal function. Which of the following is the most appropriate next-line pharmacologic treatment?
View Answer & Explanation
Correct Answer: B
Rationale: Teriparatide, a recombinant human parathyroid hormone, is an anabolic agent that stimulates new bone formation. It is indicated for patients with severe osteoporosis, very high fracture risk, or those who have failed or are intolerant to antiresorptive therapies like bisphosphonates, especially in the context of multiple fractures. Switching to IV zoledronic acid (another bisphosphonate) might be considered if compliance or absorption was an issue with oral alendronate, but given new fractures on therapy, an anabolic agent is preferred. Increasing the alendronate dose is not standard practice. Calcitonin is less effective and not a first-line agent for severe osteoporosis. Estrogen replacement therapy is not indicated for men and has other risks.
Question 50
A 42-year-old female with systemic lupus erythematosus has been on prednisone 10 mg daily for 4 years. She was diagnosed with GIO (T-score -2.6) and initiated on risedronate 35 mg weekly, along with calcium and vitamin D. She has been compliant with her medication. What is the most appropriate method to monitor the efficacy of her treatment for GIO?
View Answer & Explanation
Correct Answer: B
Rationale: The most appropriate and standard method to monitor the efficacy of treatment for GIO is an annual DEXA scan of the lumbar spine and hip. This allows for assessment of changes in bone mineral density (BMD) over time, which is a key indicator of treatment response. While bone turnover markers (Option A) can provide an early indication of drug effect, they are not routinely used as the primary monitoring tool for treatment efficacy in GIO. X-rays (Option C) are used to diagnose fractures, not to monitor treatment efficacy. Serum calcium and phosphate (Option D) are important for general bone health but do not directly assess treatment efficacy for GIO. Pain levels (Option E) are subjective and not a direct measure of bone health improvement.
Question 51
A 68-year-old male with a history of severe asthma has been on chronic oral prednisone 10 mg daily for 7 years. He presents with new-onset, severe back pain that started after a minor fall. Physical examination reveals tenderness over the mid-thoracic spine. Radiographs show a wedge compression fracture of T8. Which type of fracture is most commonly associated with glucocorticoid-induced osteoporosis?
View Answer & Explanation
Correct Answer: D
Rationale: Vertebral compression fractures are the most common type of fracture associated with glucocorticoid-induced osteoporosis. These fractures often occur with minimal trauma or even spontaneously and can lead to significant pain, height loss, and kyphosis. While hip, distal radius, and proximal humerus fractures can also occur, vertebral fractures are particularly characteristic of GIO.
Question 52
A 48-year-old female with inflammatory bowel disease has been on varying doses of oral prednisone for 10 years. Her recent DEXA scan shows a T-score of -2.9 at the lumbar spine. Before initiating specific GIO treatment, her physician orders a comprehensive workup to rule out other causes of bone loss. Which of the following conditions is most important to exclude as a potential contributor to her low bone mineral density?
View Answer & Explanation
Correct Answer: D
Rationale: Osteomalacia (defective mineralization of bone) is a critical condition to exclude, especially in patients with inflammatory bowel disease who may have malabsorption of vitamin D. Treating osteoporosis with antiresorptive agents in the presence of severe osteomalacia can worsen bone quality. Primary hyperparathyroidism (Option A) can cause bone loss but is less common in this context. Hypothyroidism (Option B) is generally associated with increased bone density, not loss. Paget's disease (Option C) is a localized disorder of bone remodeling, not generalized osteoporosis. Hyperthyroidism (Option E) can cause bone loss but osteomalacia is a more direct and critical consideration in this specific patient profile.
Question 53
A 35-year-old male recently underwent a kidney transplant and is now on a regimen including high-dose prednisone (30 mg daily). He has no prior history of osteoporosis. Given the high risk of bone loss in transplant recipients on glucocorticoids, what is the most appropriate initial management strategy for preventing GIO in this patient?
View Answer & Explanation
Correct Answer: E
Rationale: Transplant recipients on glucocorticoids are at very high risk for rapid bone loss and fractures, particularly in the first 6-12 months post-transplant. Prophylactic treatment with an oral bisphosphonate (or intravenous if oral is not tolerated/contraindicated) along with calcium and vitamin D is often recommended immediately post-transplant, regardless of baseline DEXA, due to the high and immediate risk. Option A and B are typically reserved for higher risk or intolerance. Option C is insufficient given the high risk. Option D is a reactive approach and would miss the critical window for prevention.
Question 54
A 65-year-old female with severe GIO (T-score -3.0 at lumbar spine) and a history of a vertebral fracture is unable to tolerate oral bisphosphonates due to severe gastroesophageal reflux. She also has moderate chronic kidney disease (eGFR 35 mL/min/1.73m²), which contraindicates intravenous bisphosphonates. Which of the following is the most appropriate alternative pharmacologic treatment for her GIO?
View Answer & Explanation
Correct Answer: B
Rationale: Denosumab is a fully human monoclonal antibody that inhibits RANKL, thereby reducing osteoclast activity. It is administered subcutaneously every 6 months and is not renally cleared, making it a suitable option for patients with renal impairment who cannot take bisphosphonates. Teriparatide (Option A) is an anabolic agent, also a good option for severe GIO, but denosumab is often considered first in cases of bisphosphonate intolerance with renal impairment. Raloxifene (Option C) is less potent and not first-line for severe GIO. Calcitonin (Option D) is generally not recommended for long-term treatment of osteoporosis due to limited efficacy. Romosozumab (Option E) is a newer anabolic agent but denosumab is a well-established alternative in this specific scenario.
Question 55
A 50-year-old male is receiving high-dose glucocorticoids for a severe autoimmune condition. From a cellular perspective, what is the primary direct effect of glucocorticoids on osteoblasts that contributes to bone loss?
View Answer & Explanation
Correct Answer: B
Rationale: Glucocorticoids directly promote the apoptosis (programmed cell death) of osteoblasts and osteocytes, leading to a reduction in the number of bone-forming cells and a decrease in bone formation. They also inhibit osteoblast differentiation. Options A, C, and D describe effects that would promote bone formation, which is contrary to the action of glucocorticoids. Option E is incorrect; glucocorticoids tend to decrease OPG and increase RANKL production by osteoblasts, indirectly promoting osteoclast activity.
Question 56
A 40-year-old female is on long-term oral prednisone for systemic lupus erythematosus. While glucocorticoids primarily affect osteoblasts directly, they also have indirect effects on osteoclasts. Which of the following describes an indirect effect of glucocorticoids on osteoclasts that contributes to bone resorption?
View Answer & Explanation
Correct Answer: D
Rationale: Glucocorticoids indirectly contribute to increased bone resorption by prolonging the lifespan of osteoclasts and by altering the RANKL/OPG ratio in favor of increased osteoclastogenesis. Specifically, they increase the production of RANKL and decrease the production of OPG by osteoblasts/stromal cells, thereby promoting osteoclast differentiation and activity. Option A and B are incorrect as glucocorticoids promote osteoclast differentiation and increase RANKL. Option C is incorrect as glucocorticoids decrease OPG. Option E is incorrect as the effect on osteoclasts is primarily indirect.
Question 57
A 28-year-old male is starting a 6-month course of high-dose oral methylprednisolone for optic neuritis. He has no known bone health issues. What is the most important initial adjunctive therapy to recommend to mitigate the risk of glucocorticoid-induced osteoporosis?
View Answer & Explanation
Correct Answer: C
Rationale: Calcium and vitamin D supplementation are universally recommended for all patients initiating long-term glucocorticoid therapy, regardless of their baseline bone mineral density or fracture risk. Glucocorticoids impair intestinal calcium absorption and increase renal calcium excretion, leading to secondary hyperparathyroidism and increased bone resorption. Adequate calcium and vitamin D intake helps to counteract these effects. Bisphosphonates (Option A) or teriparatide (Option B) are typically reserved for patients with higher fracture risk or established osteoporosis. Estrogen replacement therapy (Option D) is not indicated for men. While weight-bearing exercise (Option E) is beneficial, it is not the most important initial adjunctive therapy compared to calcium and vitamin D.
Question 58
A 52-year-old female with Crohn's disease has been on prednisone 7.5 mg daily for 2 years. Her recent DEXA scan shows a T-score of -1.8 at the lumbar spine. She has no history of prior fractures. Her physician is considering initiating pharmacologic treatment for GIO. What is the role of the FRAX tool in guiding management for this patient?
View Answer & Explanation
Correct Answer: B
Rationale: The FRAX (Fracture Risk Assessment Tool) is a valuable tool that estimates the 10-year probability of hip fracture and major osteoporotic fracture (clinical spine, forearm, hip, or shoulder). It incorporates several clinical risk factors, including current oral glucocorticoid use, along with age, BMI, prior fracture, parental hip fracture, smoking, alcohol intake, and secondary osteoporosis causes. For patients with osteopenia (T-score between -1.0 and -2.5), FRAX helps to identify those who would benefit from pharmacologic intervention. Option A is incorrect as FRAX specifically includes glucocorticoid use. Option C is incorrect as DEXA diagnoses osteoporosis, FRAX assesses risk. Option D and E are incorrect as FRAX is for risk assessment, not dose determination or monitoring.
Question 59
A 68-year-old female with severe, refractory glucocorticoid-induced osteoporosis (T-score -3.8 at the lumbar spine) has experienced two new vertebral fractures in the past year despite sequential therapy with alendronate for 5 years and then teriparatide for 2 years. She has no contraindications to anabolic agents. Which of the following newer agents, with a dual mechanism of action (anabolic and antiresorptive), might be considered for this patient?
View Answer & Explanation
Correct Answer: C
Rationale: Romosozumab is a monoclonal antibody that inhibits sclerostin, a protein that negatively regulates bone formation. By inhibiting sclerostin, romosozumab simultaneously increases bone formation and decreases bone resorption, offering a dual anabolic and antiresorptive effect. It is indicated for postmenopausal women at high risk for fracture, including those with a history of osteoporotic fracture, or who have failed or are intolerant to other available osteoporosis therapy. Given the patient's severe, refractory GIO and multiple fractures despite prior therapies, romosozumab would be a strong consideration. Denosumab (Option A) and Zoledronic acid (Option D) are antiresorptive agents. Abaloparatide (Option B) is another anabolic agent similar to teriparatide, but romosozumab has a unique dual mechanism. Calcitonin (Option E) is not a potent agent for severe osteoporosis.
Question 60
A 60-year-old female with a history of rheumatoid arthritis has been on alendronate 70 mg weekly for 5 years for glucocorticoid-induced osteoporosis. Her initial T-score was -2.8 at the lumbar spine, and her most recent DEXA scan shows improvement to -1.9. She has had no new fractures. Her prednisone dose has been tapered to 2.5 mg daily. When considering a "drug holiday" from bisphosphonate therapy, what is the most important factor to assess?
View Answer & Explanation
Correct Answer: C
Rationale: The decision to take a "drug holiday" from bisphosphonates is primarily based on the patient's current fracture risk and bone mineral density (BMD). For patients with GIO, if the glucocorticoid dose has been significantly reduced or discontinued, and BMD has improved or stabilized with a low fracture risk, a drug holiday may be considered after 3-5 years of oral bisphosphonate therapy. However, if the patient remains on high-dose glucocorticoids or has persistent high fracture risk, continuous therapy is often preferred. Options A, B, D, and E are important considerations for overall management but not the primary determinant for a drug holiday decision.
Question 61
A 40-year-old male with inflammatory bowel disease is being managed with varying doses of oral prednisone. His physician is concerned about the risk of glucocorticoid-induced osteoporosis. What is the approximate daily prednisone equivalent dose that is generally considered to significantly increase the risk of GIO when used for 3 months or longer?
View Answer & Explanation
Correct Answer: B
Rationale: A daily prednisone equivalent dose of 2.5 mg or more, when used for 3 months or longer, is generally considered to significantly increase the risk of glucocorticoid-induced osteoporosis. The risk is dose-dependent, with higher doses conferring greater risk, but even relatively low doses can be detrimental over time. Option A is generally considered low risk. Options C and D are very high doses that carry extremely high risk, but the threshold for significant risk is lower. Option E is incorrect as very low doses or very short courses may not pose significant risk.
Question 62
A 9-year-old boy presents to the clinic with his parents due to a noticeable curvature of his spine. On physical examination, multiple café-au-lait spots are observed on his trunk, along with a large nodule on his forehead. Radiographs confirm a structural scoliosis. This clinical presentation is most consistent with which of the following conditions?
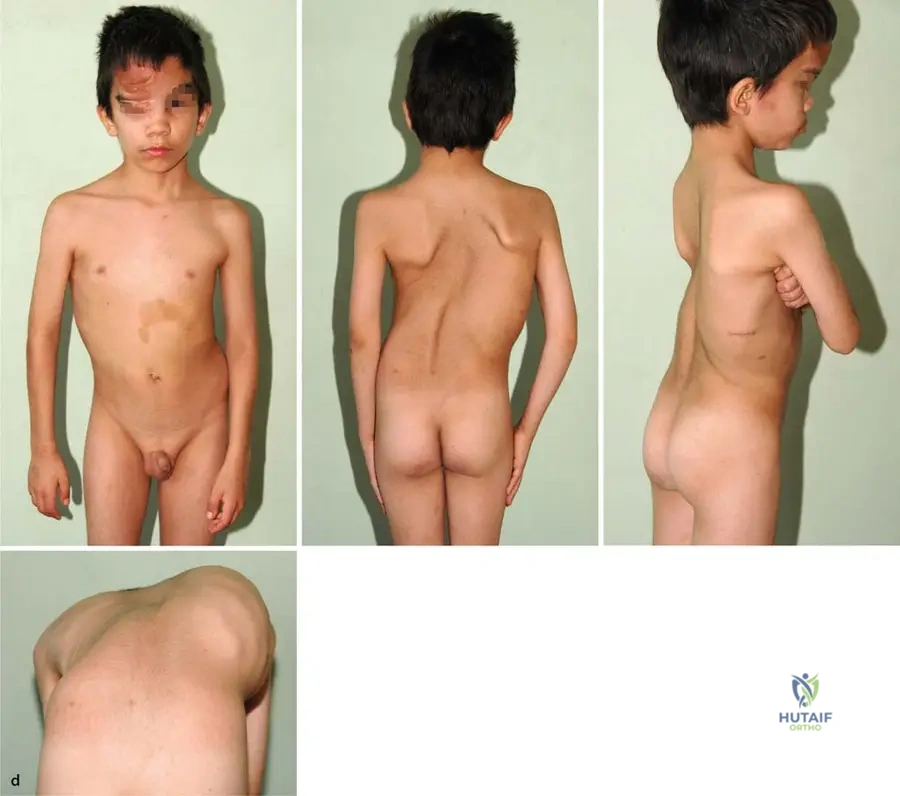
View Answer & Explanation
Correct Answer: C
Rationale: The presence of café-au-lait spots, neurofibromatic nodes (as seen on the forehead), and structural scoliosis in a child are classic features of Neurofibromatosis Type 1 (NF1), also known as von Recklinghausen's disease. Marfan syndrome and Ehlers-Danlos syndrome can present with scoliosis but typically lack café-au-lait spots and neurofibromas. Osteogenesis imperfecta is characterized by brittle bones and blue sclera, while spinal muscular atrophy involves muscle weakness and atrophy.
Question 63
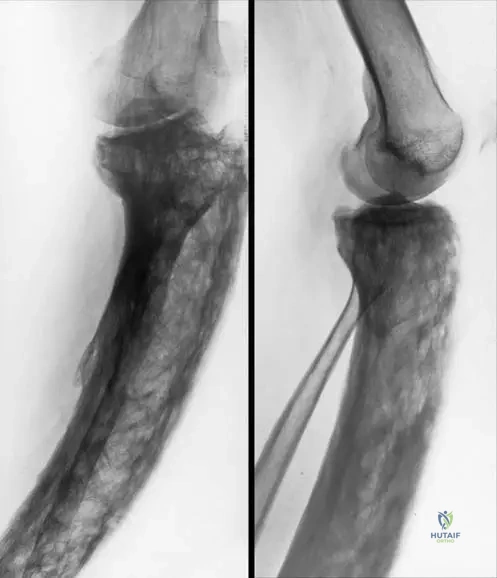
A 2-year-old boy is brought to the orthopedic clinic with a bowing deformity of his left tibia. Three years later, at age 5, he develops a non-union at the site of the previous angulation, consistent with a pseudoarthrosis. This progression is a known complication of which genetic disorder?
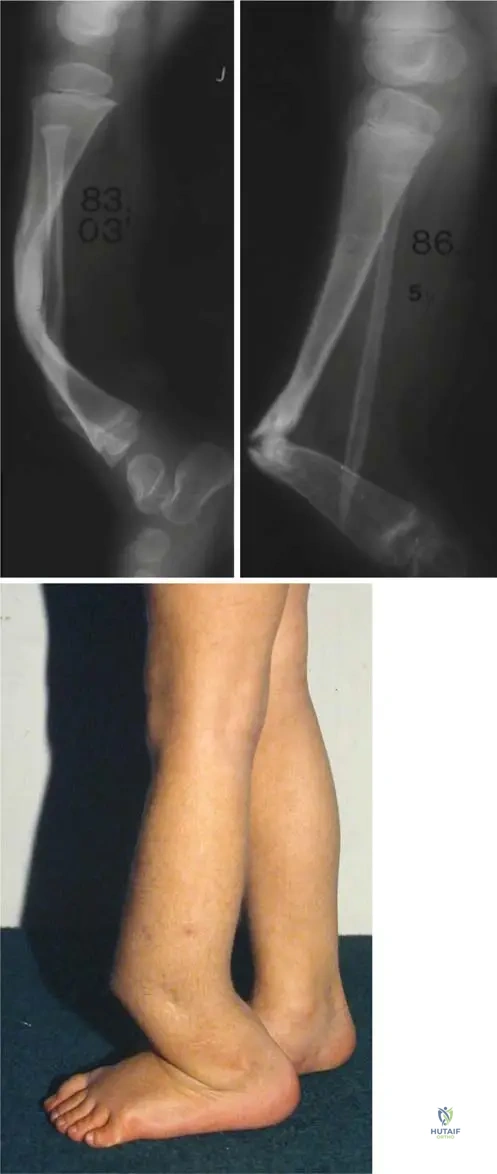
View Answer & Explanation
Correct Answer: C
Rationale: The development of an angulation of the tibia in early childhood progressing to a typical pseudoarthrosis at the same site is a characteristic orthopedic manifestation of Neurofibromatosis Type 1 (NF1). While other conditions can cause bowing or non-union, this specific progression in early childhood is highly suggestive of NF1. Fibrous dysplasia can cause bowing but pseudoarthrosis is less typical in this manner. Achondroplasia and Rickets have distinct radiographic features and clinical presentations.
Question 64
An 18-year-old male with a known history of von Recklinghausen's disease presents with a rapidly enlarging, painful mass in his thigh. MRI reveals a large, heterogeneous mass with features concerning for malignancy. A biopsy confirms a malignant schwannoma. What is the approximate lifetime risk of developing a malignant schwannoma in patients with von Recklinghausen's disease?
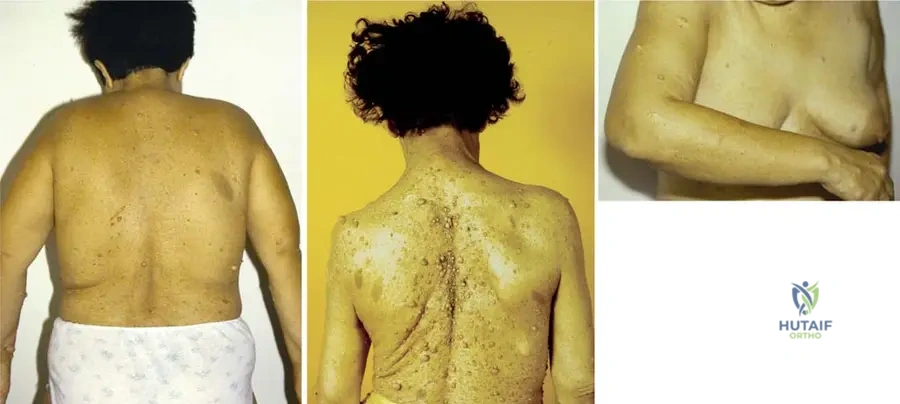
View Answer & Explanation
Correct Answer: B
Rationale: The provided clinical context explicitly states that "Between 3 and 13% of patients with von Recklinghausen’s disease will develop a malignant schwannoma." This makes option B the correct answer. The risk is significant but not as high as options C, D, or E, and not as low as option A.
Question 65
A 6-year-old girl is diagnosed with Neurofibromatosis Type 1 (NF1). Her parents ask about the inheritance pattern of the disease. Which of the following best describes the genetic transmission of NF1?
View Answer & Explanation
Correct Answer: C
Rationale: The teaching case explicitly states that neurofibromatosis is "one of the most frequent inheritable disorders, with autosomal dominant transmission." This is a fundamental characteristic of NF1. X-linked, autosomal recessive, mitochondrial, and polygenic inheritance patterns are incorrect for NF1.
Question 66
A 10-year-old boy with Neurofibromatosis Type 1 (NF1) presents for a routine follow-up. During the ophthalmologic examination, pigmented iris hamartomas are noted. What is the common name for these specific lesions?
View Answer & Explanation
Correct Answer: B
Rationale: The clinical context mentions "pigmented iris hamartomes – called also Lish’s nodule –" as a characteristic feature of Neurofibromatosis Type 1. Schwannomas are nerve sheath tumors, optic gliomas are brain tumors, and café-au-lait spots are skin pigmentations, all of which can be associated with NF1 but are not pigmented iris hamartomas. Horner's nodules are not a recognized term in this context.
Question 67
A 35-year-old female with a family history of neurofibromatosis presents with progressive hearing loss and balance issues. MRI of the brain reveals bilateral vestibular schwannomas. This presentation is most characteristic of which type of neurofibromatosis?
View Answer & Explanation
Correct Answer: B
Rationale: The teaching case explicitly states that "Type II is characterized by the central involvement as neurinomes of acoustic nerve," which are also known as vestibular schwannomas. Bilateral vestibular schwannomas are the hallmark diagnostic criterion for Neurofibromatosis Type 2 (NF2). NF1 primarily involves peripheral manifestations. Schwannomatosis is a distinct condition, and Legius and Proteus syndromes are other genetic disorders with different primary features.
Question 68
A 9-year-old boy with Neurofibromatosis Type 1 (NF1) is being evaluated for his scoliosis. The image shows an early onset structural scoliosis. What is a common characteristic of scoliosis associated with NF1 that distinguishes it from idiopathic scoliosis?

View Answer & Explanation
Correct Answer: C
Rationale: Scoliosis in NF1 can be either non-dystrophic (similar to idiopathic) or dystrophic. Dystrophic curves are often characterized by sharp, angular curves, vertebral scalloping, rib penciling, and dural ectasia, making them more aggressive and challenging to treat than typical idiopathic scoliosis. They are often progressive and frequently require surgical intervention. Options A, B, D, and E are generally incorrect for NF1-associated scoliosis, especially the dystrophic type.
Question 69
A 4-year-old child with multiple café-au-lait spots is suspected of having Neurofibromatosis Type 1. Which of the following is NOT considered a typical peripheral manifestation of NF1 according to the provided text?
View Answer & Explanation
Correct Answer: D
Rationale: The text explicitly lists "cutaneous fibromata, 'café au lait' pigmentation disorders, pigmented iris hamartomes – called also Lish’s nodule –, scoliosis, and thin long bones" as features of Type I (peripheral involvement). "Neurinomes of acoustic nerve" are listed under Type II (central involvement). Therefore, neurinomas of the acoustic nerve are not a typical peripheral manifestation of NF1.
Question 70
An 18-year-old male with Neurofibromatosis Type 1 (NF1) presents with a large, rapidly growing mass in his thigh. An MRI (as shown in Fig. 1.132 b) confirms a huge malignant schwannoma. What is the primary concern regarding the management of such a lesion?

View Answer & Explanation
Correct Answer: C
Rationale: Malignant schwannomas (also known as malignant peripheral nerve sheath tumors, MPNSTs) are aggressive sarcomas with a high propensity for local recurrence and distant metastasis, particularly to the lungs. While other issues like cosmetic disfigurement, nerve compression, and joint impairment can occur, the primary concern for a malignant tumor is its oncologic potential. Pathological fracture is less common for soft tissue sarcomas unless there is bone involvement.
Question 71
A 5-year-old boy with Neurofibromatosis Type 1 (NF1) is found to have multiple café-au-lait spots. To meet the diagnostic criteria for NF1, how many café-au-lait spots, typically, must be present in a prepubertal child?
View Answer & Explanation
Correct Answer: E
Rationale: While not explicitly stated in the provided text, standard diagnostic criteria for NF1 (NIH Consensus Conference) include six or more café-au-lait macules over 5 mm in greatest diameter in prepubertal individuals (or over 15 mm in postpubertal individuals). This is a common board-level question related to NF1 diagnosis. Options A-D are insufficient for diagnosis based on café-au-lait spots alone.
Question 72
A 2-year-old patient with Neurofibromatosis Type 1 (NF1) presents with an angulation of the tibia. What is the most likely long-term orthopedic complication if this angulation is left untreated or inadequately managed?

View Answer & Explanation
Correct Answer: C
Rationale: The clinical context specifically highlights that "Three years later a typical pseudoarthrosis developed at the same site of the tibia" following an initial angulation at age 2. This progression to pseudoarthrosis (a false joint or non-union) is a well-known and severe complication of NF1-related long bone dysplasia, particularly in the tibia. While leg length discrepancy can occur, pseudoarthrosis is the more specific and severe complication described. Osteomyelitis and avascular necrosis are less typical direct complications of the angulation itself in NF1.
Question 73
A 40-year-old male with Neurofibromatosis Type 1 (NF1) undergoes an MRI of the pelvis, which reveals multiple neurofibromata on enlarged nerves (as shown in Fig. 1.132 d). These lesions are benign nerve sheath tumors. What is the primary cell type from which these neurofibromas originate?
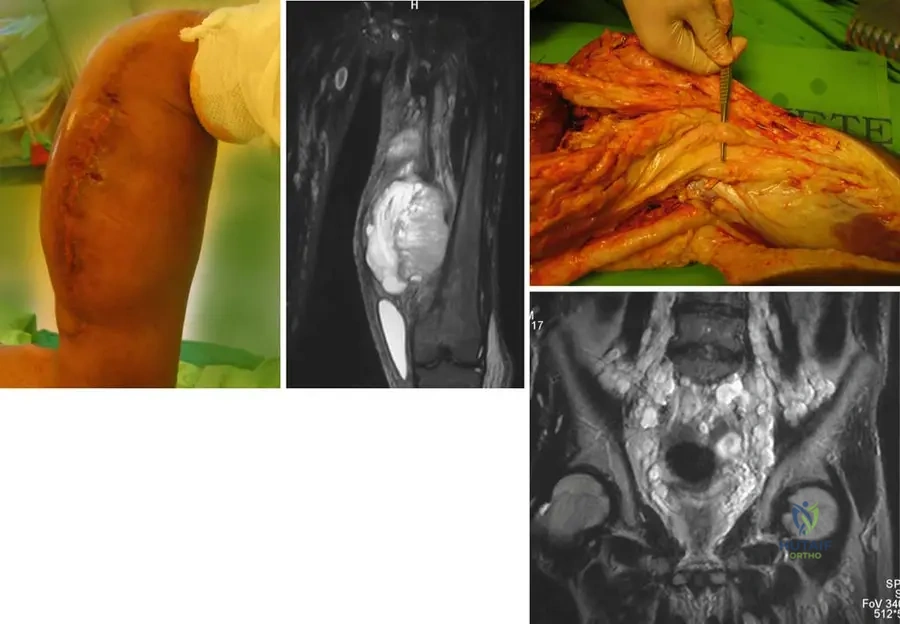
View Answer & Explanation
Correct Answer: D
Rationale: Neurofibromas are benign tumors of peripheral nerves, composed of a mixture of Schwann cells, fibroblasts, mast cells, and perineurial cells. Schwann cells are the primary neoplastic component. Malignant schwannomas (MPNSTs) also arise from Schwann cells or their precursors. Neurons, astrocytes, oligodendrocytes are central nervous system cells, and endothelial cells form blood vessels.
Question 74
A 7-year-old boy with Neurofibromatosis Type 1 (NF1) is noted to have thin long bones. This skeletal manifestation contributes to an increased risk of which orthopedic complication?
View Answer & Explanation
Correct Answer: D
Rationale: The "thin long bones" described in NF1 are often dysplastic, meaning they have abnormal development and structure. This inherent weakness makes them highly susceptible to pathological fractures, which are fractures occurring through bone weakened by an underlying disease process, often with minimal or no trauma. This is distinct from stress fractures (due to repetitive loading in otherwise normal bone) or general osteoporosis (reduced bone density). Osteoarthritis and bone cysts are less directly linked to the "thin long bones" description in NF1.
Question 75
A 15-year-old female with Neurofibromatosis Type 2 (NF2) presents with progressive weakness and numbness in her lower extremities. An MRI of the spine reveals a mass compressing the spinal cord. This finding is consistent with which of the following?
View Answer & Explanation
Correct Answer: B
Rationale: The text states that NF2 "may compress the spinal cord, giving the typical picture of spinal cord tumor." While NF1 can be associated with dural ectasia, and other conditions can cause spinal cord compression, the specific mention of NF2 and spinal cord compression leading to a "spinal cord tumor" picture directly points to option B. These tumors are often schwannomas or meningiomas in NF2. Syringomyelia is a fluid-filled cavity within the spinal cord, and vertebral hemangioma/spinal lipoma are other types of spinal lesions.
Question 76
A 25-year-old male with Neurofibromatosis Type 1 (NF1) is undergoing surveillance. Given the risk of malignant transformation, which of the following clinical signs would raise the highest suspicion for a malignant schwannoma?
View Answer & Explanation
Correct Answer: C
Rationale: The most concerning signs for malignant transformation of a neurofibroma into a malignant schwannoma (MPNST) are rapid growth, new or increasing pain, and neurological deficits. A new small, painless neurofibroma (A) or stable plexiform neurofibroma (B) are typically benign. New café-au-lait spots (D) are a diagnostic feature but not indicative of malignancy. Mild, non-progressive scoliosis (E) is an orthopedic manifestation, not a sign of malignant transformation.
Question 77
A 9-year-old boy with Neurofibromatosis Type 1 (NF1) presents with scoliosis. The image shows a typical café-au-lait spot. What is the approximate frequency of neurofibromatosis in the general population?

View Answer & Explanation
Correct Answer: B
Rationale: The teaching case states that "the frequency is approximately 33/100,000." This directly corresponds to option B. This is a factual recall question from the provided text.
Question 78
A 2-year-old patient is diagnosed with Neurofibromatosis Type 1 (NF1) after presenting with an angulation of the tibia. Given the high risk of pseudoarthrosis, what is a common initial orthopedic management strategy for this specific bone deformity in NF1?

View Answer & Explanation
Correct Answer: C
Rationale: While the text describes the progression to pseudoarthrosis, it doesn't detail management. However, in the context of early angulation in NF1, prophylactic bracing or casting is often attempted to prevent or delay the progression to pseudoarthrosis, especially in very young children. Immediate amputation (A) is too aggressive. Observation (B) alone is often insufficient given the high risk of progression. Intramedullary nailing with bone grafting (D) and external fixation (E) are surgical treatments typically reserved for established pseudoarthrosis, not initial angulation prevention.
Question 79
A 30-year-old male with Neurofibromatosis Type 1 (NF1) presents with a large, palpable mass in his thigh. An MRI (Fig. 1.132 b) shows a huge malignant schwannoma. The amputated specimen (Fig. 1.132 c) reveals a neurofibroma of the enlarged peroneal nerve. What is the most appropriate initial surgical approach for a confirmed malignant schwannoma?

View Answer & Explanation
Correct Answer: C
Rationale: Malignant schwannomas (MPNSTs) are high-grade sarcomas. The cornerstone of treatment is wide local excision with clear surgical margins to minimize local recurrence and improve survival. Marginal excision (B) or intralesional debulking (D) would have unacceptably high recurrence rates. While radiation therapy (A) may be used adjunctively, it is not the primary surgical approach. Amputation (E) is reserved for cases where wide local excision with limb salvage is not feasible due to tumor size, location, or involvement of critical structures, or for recurrent disease, as depicted in the image as a consequence of the disease, not necessarily the initial approach.
Question 80
A 9-year-old boy with Neurofibromatosis Type 1 (NF1) has a structural scoliosis. In addition to the visible café-au-lait spots and neurofibromatic node, what other skeletal manifestation is commonly associated with NF1 and can contribute to spinal deformity?

View Answer & Explanation
Correct Answer: C
Rationale: While not explicitly detailed in the provided text, dural ectasia (ballooning of the dural sac, often with associated vertebral scalloping) is a well-recognized skeletal manifestation of NF1, particularly in the spine. It can contribute to spinal instability and the progression of scoliosis or kyphosis. Osteopetrosis is a condition of increased bone density. Vertebral body fusion anomalies are more typical of congenital scoliosis. Spondylolisthesis and Scheuermann's kyphosis are distinct spinal conditions not primarily associated with NF1.
Question 81
A 5-year-old child is diagnosed with Neurofibromatosis Type 1 (NF1). The parents are concerned about the long-term prognosis. Which of the following statements regarding the prognosis of NF1 is most accurate?
View Answer & Explanation
Correct Answer: C
Rationale: NF1 is known for its highly variable expressivity, even within the same family. While some individuals have mild cutaneous manifestations, others develop severe complications like progressive scoliosis, tibial pseudoarthrosis, optic pathway gliomas, and malignant peripheral nerve sheath tumors (MPNSTs), which can significantly impact morbidity and mortality. Not all patients develop malignant transformation (A), and it is not uniformly mild (B). Amputation (D) is a severe outcome for specific complications like pseudoarthrosis or malignant tumors, but not for most patients. NF1 affects multiple organ systems, not just cosmetic appearance (E).
Question 82
A 19-year-old male with a known history of Neurofibromatosis Type 1 (NF1) presents with a rapidly enlarging, painful mass in his left thigh over the past 3 months. Physical examination reveals a firm, fixed, and tender mass. MRI of the thigh shows a large, heterogeneous mass with areas of necrosis and invasion into surrounding muscle. Biopsy confirms a malignant schwannoma.

View Answer & Explanation
Correct Answer: C
Rationale: The clinical context explicitly states that "Between 3 and 13% of patients with von Recklinghausen’s disease will develop a malignant schwannoma." This directly answers the question regarding the risk of malignant transformation. Main Distractor: Option D (15-25%) is incorrect as it significantly overestimates the reported risk in the provided text.
Question 83
A 2-year-old boy is diagnosed with Neurofibromatosis Type 1 (NF1) after presenting with multiple café-au-lait spots and a family history of the disorder. His parents are concerned about potential orthopedic manifestations. At what age does the provided clinical context suggest that lower extremity deformities, such as tibial angulation, can typically begin to develop?

View Answer & Explanation
Correct Answer: B
Rationale: The clinical context for Fig. 1.130 a–c states, "In this patient the disease started with an angulation of the tibia at age 2 (a)." This directly indicates that lower extremity deformities can manifest in early childhood, specifically around age 2. Main Distractor: Option C (Preschool age) is incorrect because the case explicitly mentions the onset at age 2, which is earlier than typical preschool age.
Question 84
An 18-year-old male with Neurofibromatosis Type 1 (NF1) undergoes amputation for a large malignant schwannoma of the thigh. During pathological examination of the amputated specimen, the surgeon points to a neurofibroma of an enlarged nerve. Which specific nerve is identified in the provided image as being affected by a neurofibroma in this context?

View Answer & Explanation
Correct Answer: D
Rationale: The clinical context for Fig. 1.132 a–d explicitly states, "The forceps points to a neurofibroma of the enlarged peroneal nerve in the amputated specimen (c)." Main Distractor: Option B (Sciatic nerve) is incorrect, although the peroneal nerve is a branch of the sciatic nerve, the specific nerve identified in the image context is the peroneal nerve.
Question 85
A 9-year-old boy with Neurofibromatosis (NF) presents with a structural scoliosis. On physical examination, a typical café-au-lait spot is noted on his trunk, and a large neurofibromatic node is visible on his forehead. Which type of Neurofibromatosis is most consistent with these findings?

View Answer & Explanation
Correct Answer: A
Rationale: The clinical text describes Type I (NF1) as being known especially for "peripheral involvement: cutaneous fibromata, 'café au lait' pigmentation disorders... scoliosis." The vignette's findings of café-au-lait spots, neurofibromatic nodes (cutaneous fibromata), and scoliosis in a child are classic presentations of NF1. Main Distractor: Option B (Neurofibromatosis Type 2) is incorrect because NF2 is characterized by central involvement such as acoustic neurinomas and cataracts, not typically by widespread cutaneous fibromata or café-au-lait spots as primary diagnostic features.
Question 86
A 5-year-old child with Neurofibromatosis Type 1 (NF1) is noted to have developed a pseudoarthrosis of the tibia, which began as an angulation at age 2. Given the progressive nature of this condition in NF1, what is the most likely long-term orthopedic complication if this pseudoarthrosis is not successfully treated?

View Answer & Explanation
Correct Answer: C
Rationale: The clinical context for Fig. 1.130 a–c shows the progression from tibial angulation to a "typical pseudoarthrosis." Pseudoarthrosis, by definition, is a false joint formed at the site of a nonunion, leading to persistent instability, pain, and often significant limb length discrepancy if not successfully treated. The text highlights the development of pseudoarthrosis as a significant deformity. Main Distractor: Option A (Spontaneous resolution) is incorrect; pseudoarthrosis in NF1 is notoriously difficult to treat and rarely resolves spontaneously. Option B (Development of osteosarcoma) is incorrect; while NF1 patients have an increased risk of certain malignancies, osteosarcoma is not the direct or most likely complication of a tibial pseudoarthrosis itself.
Question 87
A 30-year-old female with a known history of Neurofibromatosis Type 2 (NF2) presents with progressive hearing loss and balance issues. MRI of the brain reveals bilateral acoustic neurinomas. Which other ocular finding is specifically mentioned in the provided text as a characteristic feature of NF2?
View Answer & Explanation
Correct Answer: D
Rationale: The clinical text explicitly states that Type II (NF2) is characterized by "neurinomes of acoustic nerve, cataract and it may compress the spinal cord." Main Distractor: Option A (Lisch's nodules) is incorrect as the text specifically associates Lisch's nodules (pigmented iris hamartomas) with Neurofibromatosis Type 1 (NF1).
Question 88
A 9-year-old boy with Neurofibromatosis Type 1 (NF1) is being evaluated for scoliosis. In addition to the spinal deformity, he exhibits multiple café-au-lait spots and a large neurofibromatic node on his forehead. What is the genetic inheritance pattern of Neurofibromatosis, as described in the provided text?

View Answer & Explanation
Correct Answer: B
Rationale: The clinical text states, "The neurofibromatosis is one of the most frequent inheritable disorders, with autosomal dominant transmission." Main Distractor: Option A (Autosomal recessive) is incorrect as the text clearly specifies autosomal dominant inheritance.
Question 89
An 18-year-old male with Neurofibromatosis (NF) presents with a large, rapidly growing mass in his thigh, which is later confirmed to be a malignant schwannoma. MRI of the pelvis also reveals multiple neurofibromata on enlarged nerves. What is the term used in the provided text to refer to Neurofibromatosis, particularly Type 1?

View Answer & Explanation
Correct Answer: C
Rationale: The clinical text explicitly states, "It is called also von Recklinghausen’s disease." Main Distractor: Option D (Tuberous sclerosis) is incorrect; while it is also a neurocutaneous disorder, the text specifically identifies von Recklinghausen's disease as another name for neurofibromatosis.
Question 90
A 9-year-old boy with Neurofibromatosis Type 1 (NF1) is diagnosed with structural scoliosis. His physical exam also reveals multiple café-au-lait spots and a large neurofibroma on his forehead. What is a characteristic feature of the long bones in patients with NF1, as mentioned in the provided text?

View Answer & Explanation
Correct Answer: C
Rationale: The clinical text, when describing Type I (NF1), lists "scoliosis, and thin long bones" as characteristic features. Main Distractor: Option B (Shortened length) is incorrect; while limb length discrepancy can occur due to pseudoarthrosis, the general characteristic mentioned for long bones in NF1 is thinness, not necessarily uniform shortening.
Question 91
A 2-year-old child with Neurofibromatosis Type 1 (NF1) presents with an angulation of the tibia. Three years later, at age 5, this angulation has progressed to a typical pseudoarthrosis. This progression highlights the need for careful monitoring in NF1 patients. What is the approximate frequency of Neurofibromatosis in the general population, according to the provided text?

View Answer & Explanation
Correct Answer: B
Rationale: The clinical text states, "the frequency is approximately 33/100,000." Main Distractor: Option C (1/10,000) is incorrect; while it represents a similar order of magnitude, it is not the precise frequency stated in the text.
Question 92
A 45-year-old male with a long-standing diagnosis of Neurofibromatosis Type 2 (NF2) presents with new onset weakness and numbness in his lower extremities. Neurological examination reveals signs consistent with spinal cord compression. What is the primary pathological finding in the spine that is characteristic of NF2 and can lead to such compression, as described in the provided text?
View Answer & Explanation
Correct Answer: C
Rationale: The clinical text states that NF2 "may compress the spinal cord, giving the typical picture of spinal cord tumor." This refers to neurinomas (schwannomas) affecting the spinal nerves or cord. Main Distractor: Option B (Spinal stenosis) is incorrect; while spinal stenosis can cause compression, the specific etiology in NF2 leading to compression is described as a "spinal cord tumor," which are typically neurinomas/schwannomas.
Question 93
A 9-year-old boy with Neurofibromatosis Type 1 (NF1) is noted to have a structural scoliosis, multiple café-au-lait spots, and a large neurofibroma on his forehead. His parents are concerned about the progression of his scoliosis. Which of the following is a key feature distinguishing NF1 from NF2, based on the provided text?

View Answer & Explanation
Correct Answer: D
Rationale: The text clearly differentiates NF1 and NF2 by their primary involvement: "Type I. is known especially for peripheral involvement... Type II is characterized by the central involvement as neurinomes of acoustic nerve, cataract and it may compress the spinal cord." While NF1 can have some CNS manifestations (e.g., optic gliomas, not mentioned here), NF2 is *characterized* by central involvement. The question asks for a *key distinguishing feature*. Main Distractor: Option E (Peripheral nervous system involvement) is incorrect because this is characteristic of NF1, not NF2, and therefore does not distinguish NF2 from NF1 in the way central involvement distinguishes NF2.
Question 94
An 18-year-old male with Neurofibromatosis (NF) presents with a large, painful mass in his thigh, which is later identified as a malignant schwannoma. MRI of the pelvis also reveals multiple neurofibromata on enlarged nerves. What is the typical age range when malignant transformation of lesions in NF patients often occurs, as suggested by the provided clinical context?

View Answer & Explanation
Correct Answer: C
Rationale: The clinical context for Fig. 1.132 a–d states, "In adult life the lesions often undergo malignant transformation and malignant schwannoma develops, as in this case. Preoperative photograph from the thigh of a 18-year-old male patient (a) and the MRI picture (b) present a huge malignant schwannoma." This indicates that malignant transformation is typically an adult phenomenon, exemplified by the 18-year-old patient. Main Distractor: Option B (Adolescence) is incorrect because while 18 is technically the end of adolescence, the text specifically uses the term "adult life" and the case example is 18, indicating the onset is typically in adulthood rather than predominantly in younger adolescence.
Question 95
A 9-year-old boy with Neurofibromatosis Type 1 (NF1) is being evaluated for scoliosis. He also has multiple café-au-lait spots and a large neurofibroma on his forehead. In addition to these findings, what other ocular manifestation is specifically associated with NF1 in the provided text?

View Answer & Explanation
Correct Answer: C
Rationale: The clinical text, when describing Type I (NF1), lists "pigmented iris hamartomes – called also Lish’s nodule" as a characteristic feature. Main Distractor: Option E (Early-onset cataracts) is incorrect because the text specifically associates cataracts with Neurofibromatosis Type 2 (NF2).
Question 96
A 2-year-old child with Neurofibromatosis Type 1 (NF1) develops an angulation of the tibia, which progresses to a pseudoarthrosis by age 5. This condition is a significant orthopedic challenge in NF1. Which of the following statements about the gender prevalence of Neurofibromatosis is accurate, according to the provided text?

View Answer & Explanation
Correct Answer: C
Rationale: The clinical text states, "Both genders are affected with equal severity." Main Distractor: Options A and B are incorrect as the text explicitly states equal severity for both genders.
Question 97
An 18-year-old male with Neurofibromatosis (NF) presents with a large malignant schwannoma in his thigh, requiring amputation. MRI of the pelvis also shows multiple neurofibromata on enlarged nerves. Which imaging modality is specifically mentioned in the provided text as useful for visualizing these neurofibromata on enlarged nerves in the pelvis?

View Answer & Explanation
Correct Answer: D
Rationale: The clinical context for Fig. 1.132 a–d states, "MRI picture of the pelvis (d) reveals neurofibromata on the enlarged nerves." This directly indicates MRI as the modality used for this purpose. Main Distractor: Option A (X-ray) is incorrect; while X-rays are used for bone deformities, they are not suitable for visualizing soft tissue neurofibromata on nerves in the pelvis.
Question 98
A 9-year-old boy with Neurofibromatosis Type 1 (NF1) presents with structural scoliosis. He also has multiple café-au-lait spots and a prominent neurofibromatic node on his forehead. What is the primary type of involvement that characterizes Neurofibromatosis Type 1 (NF1), according to the provided text?

View Answer & Explanation
Correct Answer: B
Rationale: The clinical text states, "Type I. is known especially for peripheral involvement: cutaneous fibromata, 'café au lait' pigmentation disorders, pigmented iris hamartomes – called also Lish’s nodule –, scoliosis, and thin long bones." Main Distractor: Option A (Central nervous system involvement) is incorrect because the text explicitly states that central involvement characterizes Type II (NF2), not NF1.
Question 99
A 2-year-old child with Neurofibromatosis Type 1 (NF1) develops an angulation of the tibia, which progresses to a pseudoarthrosis by age 5. This progression is a common orthopedic challenge in NF1. What is the term used for the pigmented iris hamartomas that are a characteristic feature of NF1?

View Answer & Explanation
Correct Answer: C
Rationale: The clinical text, when describing Type I (NF1), lists "pigmented iris hamartomes – called also Lish’s nodule" as a characteristic feature. Main Distractor: Option A (Café-au-lait spots) is incorrect; while also a feature of NF1, they are skin pigmentations, not iris hamartomas.
Question 100
A 9-year-old boy with Neurofibromatosis (NF) presents with early-onset structural scoliosis. He also has multiple café-au-lait spots on his trunk and a large neurofibromatic node on his forehead. Based on the provided images, what is the appearance of the café-au-lait spot on the trunk?

View Answer & Explanation
Correct Answer: C
Rationale: The image Fig. 1.128 a shows a "Typical café-au-lait spot... visible on the trunk." Visually, it is a light brown, flat, and relatively uniformly pigmented macule, consistent with the classic description of café-au-lait spots. Main Distractor: Option B (A dark brown, irregular patch of skin) is incorrect; while café-au-lait spots are pigmented, they are typically light brown and often have relatively smooth borders, not necessarily dark or highly irregular as described in this option.
You Might Also Like