Master ABOS Board Review: Scleroderma, Dwarfism, Infections, Osteomalacia | Part 26
Key Takeaway
This ABOS Board Review covers critical topics for orthopaedic surgeons, including systemic sclerosis manifestations, mesomelic dwarfism types and genetics, iatrogenic orthopaedic infection diagnosis and management, and the pathophysiology and clinical features of osteomalacia and rickets. Prepare for your board exam with these essential questions and explanations.
Question 1
A 52-year-old female with diffuse systemic sclerosis is being evaluated for elective carpal tunnel release. During her preoperative workup, she reports increasing shortness of breath with exertion and a persistent dry cough. Physical examination reveals fine crackles at the lung bases. Pulmonary function tests show a restrictive pattern. Radiographs of the chest show interstitial infiltrates.
View Answer & Explanation
Correct Answer: C
Rationale: Interstitial lung disease (ILD) is a common and serious complication of systemic sclerosis, often presenting with progressive dyspnea, dry cough, and restrictive lung disease on PFTs. Fine crackles and interstitial infiltrates on chest imaging are characteristic findings. Pulmonary hypertension can develop secondary to ILD but is a distinct entity. Pericardial effusion is a cardiac complication. Scleroderma renal crisis is a hypertensive emergency. GERD is a common GI manifestation but does not explain the pulmonary symptoms. Main Distractor: B) Pulmonary hypertension is a severe complication of systemic sclerosis and can cause dyspnea, but the presence of fine crackles, restrictive PFTs, and interstitial infiltrates on chest radiographs points more directly to interstitial lung disease as the primary pulmonary pathology.
Question 2
A 39-year-old male with recently diagnosed diffuse systemic sclerosis presents to the emergency department with sudden onset severe headache, blurred vision, and rapidly rising blood pressure (200/110 mmHg). He also reports decreased urine output. Laboratory tests reveal new-onset microangiopathic hemolytic anemia and acute kidney injury. Radiographs are not relevant to this acute presentation.
View Answer & Explanation
Correct Answer: C
Rationale: Scleroderma renal crisis (SRC) is a life-threatening complication characterized by abrupt onset of severe hypertension, rapidly progressive renal failure, and often microangiopathic hemolytic anemia and thrombocytopenia. It is a medical emergency requiring prompt treatment with ACE inhibitors. The described symptoms and lab findings are classic for SRC. While the patient has severe hypertension, it's more than just a hypertensive urgency; it's a specific organ-threatening complication of scleroderma. Main Distractor: E) Hypertensive urgency describes severe hypertension without acute end-organ damage. However, this patient presents with acute kidney injury, microangiopathic hemolytic anemia, and neurological symptoms, indicating end-organ damage and a specific scleroderma-related emergency (Scleroderma Renal Crisis).
Question 3
A 60-year-old female with long-standing systemic sclerosis is scheduled for a hand surgery procedure. During her pre-operative assessment, she reports chronic dysphagia, heartburn, and early satiety. She often regurgitates food and has lost weight. Physical examination reveals no acute abdominal findings. Radiographs of the chest show no acute cardiopulmonary pathology.
View Answer & Explanation
Correct Answer: C
Rationale: Gastrointestinal involvement is very common in systemic sclerosis, with esophageal dysmotility and severe gastroesophageal reflux disease (GERD) being prominent features. The dysphagia, heartburn, regurgitation, and early satiety are classic symptoms resulting from smooth muscle atrophy and fibrosis in the esophagus and stomach. This is a critical consideration for anesthesia due to aspiration risk. The other options are less specific or less common primary GI manifestations of scleroderma. Main Distractor: A) Peptic ulcer disease can cause heartburn and epigastric pain, but the primary dysphagia and regurgitation, along with early satiety, point more strongly to esophageal dysmotility and severe GERD, which are direct consequences of scleroderma's effect on smooth muscle.
Question 4
A 40-year-old female presents with Raynaud's phenomenon, telangiectasias, and calcinosis cutis on her fingers. She has mild sclerodactyly but no significant internal organ involvement. Her ANA is positive. Which of the following autoantibodies is most likely to be positive in this patient, indicating a limited cutaneous form of systemic sclerosis?
View Answer & Explanation
Correct Answer: C
Rationale: The clinical features described (Raynaud's, telangiectasias, calcinosis cutis, mild sclerodactyly, and absence of significant internal organ involvement) are characteristic of CREST syndrome, which is a limited cutaneous form of systemic sclerosis. Anti-centromere antibody is strongly associated with CREST syndrome and limited cutaneous systemic sclerosis. Anti-Scl-70 is associated with diffuse cutaneous systemic sclerosis and pulmonary fibrosis. Anti-RNA polymerase III is associated with diffuse cutaneous systemic sclerosis and renal crisis. Anti-Jo-1 is associated with myositis. Anti-dsDNA is associated with systemic lupus erythematosus. Main Distractor: A) Anti-Scl-70 is associated with diffuse cutaneous systemic sclerosis and a higher risk of interstitial lung disease, which is not consistent with the patient's limited cutaneous presentation and lack of significant internal organ involvement.
Question 5
A 50-year-old male presents with rapidly progressive skin thickening involving his trunk and proximal extremities, along with new-onset dyspnea and a dry cough. His ANA is positive. Which of the following autoantibodies is most likely to be positive in this patient, indicating a diffuse cutaneous form of systemic sclerosis with a higher risk of interstitial lung disease?
View Answer & Explanation
Correct Answer: C
Rationale: The rapidly progressive and widespread skin thickening (trunk and proximal extremities) indicates diffuse cutaneous systemic sclerosis. The presence of dyspnea and dry cough suggests interstitial lung disease. Anti-Scl-70 (anti-topoisomerase I) is strongly associated with diffuse cutaneous systemic sclerosis and a higher risk of interstitial lung disease. Anti-centromere antibody is associated with limited cutaneous systemic sclerosis. Anti-Ro/SSA, Anti-La/SSB, and Anti-Sm are associated with Sjögren's syndrome and systemic lupus erythematosus, respectively. Main Distractor: A) Anti-centromere antibody is characteristic of limited cutaneous systemic sclerosis (CREST syndrome), which typically presents with less widespread skin involvement and a different internal organ risk profile than described.
Question 6
A 65-year-old female with long-standing systemic sclerosis is scheduled for an elective total knee arthroplasty due to severe osteoarthritis. Her medical history includes esophageal dysmotility, pulmonary hypertension, and mild renal insufficiency. Which of the following is the MOST critical consideration for the orthopaedic surgeon and anesthesiologist during the perioperative period?
View Answer & Explanation
Correct Answer: C
Rationale: Patients with systemic sclerosis often have significant esophageal dysmotility and gastroesophageal reflux disease (GERD), which increases the risk of aspiration during induction of anesthesia and in the postoperative period. This is a life-threatening complication. While wound healing, DVT, pain, and infection are important considerations in any surgery, the specific combination of esophageal dysmotility and pulmonary hypertension makes airway management and aspiration risk paramount in scleroderma patients. Pulmonary hypertension also increases anesthetic risk. Main Distractor: B) Difficulty with wound healing is a significant concern in scleroderma due to microvascular disease and skin fibrosis, but aspiration during anesthesia can be acutely life-threatening, making it a more immediate and critical perioperative consideration.
Question 7
A 50-year-old female with systemic sclerosis undergoes a carpal tunnel release. Postoperatively, she develops delayed wound healing, with persistent erythema, induration, and partial dehiscence of the incision despite appropriate surgical technique and infection prophylaxis. Radiographs are not relevant to this complication.
View Answer & Explanation
Correct Answer: C
Rationale: Patients with systemic sclerosis have impaired microvascular circulation and extensive skin fibrosis, which significantly compromises wound healing. This leads to delayed healing, increased risk of dehiscence, and poor scar formation. While infection, tension, and nutrition can affect wound healing, the underlying pathology of scleroderma directly impacts the vascularity and elasticity of the skin, making it a primary cause of healing complications. Main Distractor: A) Surgical site infection is a common cause of delayed wound healing, but in a patient with systemic sclerosis, the underlying disease pathology (impaired microvascular circulation and skin fibrosis) predisposes to poor healing even in the absence of infection, and the description does not explicitly state purulence or systemic signs of infection.
Question 8
A 47-year-old female with severe sclerodactyly and flexion contractures of her PIP joints, secondary to systemic sclerosis, is considering surgical release to improve hand function. She has tried extensive physical and occupational therapy without significant improvement. What is the MOST important counseling point regarding surgical outcomes for contracture release in systemic sclerosis?
View Answer & Explanation
Correct Answer: C
Rationale: Due to the ongoing fibrotic process characteristic of systemic sclerosis, contractures often recur after surgical release. While surgery can provide temporary improvement in range of motion and function, it does not address the underlying disease, and the fibrotic process continues. Patients must be counseled about the high likelihood of recurrence and the need for continued therapy. Wound healing complications are common, not rare. Main Distractor: A) While some functional improvement can be achieved, the expectation of "excellent long-term functional improvement" is often unrealistic due to the high rate of contracture recurrence and ongoing disease progression.
Question 9
A 53-year-old female with systemic sclerosis presents with a painful, non-healing ulcer on her fingertip, which developed after a minor trauma. She has a history of severe Raynaud's phenomenon. On examination, the ulcer is small, punched-out, and surrounded by ischemic skin. Radiographs show no acute osteomyelitis.
View Answer & Explanation
Correct Answer: D
Rationale: Digital ulcers are a common and debilitating complication of systemic sclerosis, primarily due to severe Raynaud's phenomenon and underlying microvascular disease leading to ischemia. These ulcers are often painful, slow to heal, and prone to infection. The description of a painful, punched-out ulcer on the fingertip with surrounding ischemia in a patient with Raynaud's is classic for an ischemic digital ulcer in scleroderma. The other ulcer types have different etiologies and typical locations. Main Distractor: A) Diabetic ulcers are typically neuropathic or neuro-ischemic, often found on the plantar surface of the foot, and while they can be ischemic, the specific context of severe Raynaud's and fingertip location points more directly to a digital ulcer of scleroderma.
Question 10
Question 10
A 45-year-old female presents with a 10-year history of Raynaud's phenomenon, telangiectasias, and dysphagia. On examination, she has thickened skin limited to her fingers and face, and small, firm, subcutaneous nodules on her fingertips. Radiographs show soft tissue calcifications around the distal interphalangeal joints. Systemic workup reveals no significant lung or renal involvement. Which subtype of systemic sclerosis is most consistent with this presentation?
View Answer & Explanation
Correct Answer: B
Rationale: The patient's presentation with a long history of Raynaud's, telangiectasias, dysphagia, calcinosis (subcutaneous nodules and radiographic findings), and skin thickening limited to the fingers and face (sclerodactyly) is classic for Limited Cutaneous Systemic Sclerosis, often referred to as CREST syndrome (Calcinosis, Raynaud's, Esophageal dysmotility, Sclerodactyly, Telangiectasias). Diffuse cutaneous systemic sclerosis involves skin thickening proximal to the elbows and knees and often has more rapid progression and severe internal organ involvement. Systemic sclerosis sine scleroderma lacks skin involvement. Overlap syndrome involves features of SSc and another connective tissue disease. Undifferentiated connective tissue disease is used when criteria for a specific disease are not fully met.
Question 10
A 58-year-old male with a recent diagnosis of systemic sclerosis presents for evaluation of progressive hand stiffness. He has significant sclerodactyly and flexion contractures of his fingers. The underlying pathophysiology of systemic sclerosis involves an imbalance in which of the following cellular processes?
View Answer & Explanation
Correct Answer: B
Rationale: Systemic sclerosis is characterized by widespread vascular damage and excessive deposition of collagen and other extracellular matrix components in the skin and internal organs. This fibrosis is primarily driven by the overproduction of collagen by activated fibroblasts. While other connective tissue diseases involve different mechanisms, the hallmark of scleroderma is this fibrotic process. Increased osteoclast activity is seen in osteoporosis, autoimmune destruction of synovial cells in rheumatoid arthritis, impaired proteoglycan synthesis in osteoarthritis, and elastin degradation in conditions like Marfan syndrome or emphysema.
Question 10
A 38-year-old female with newly diagnosed systemic sclerosis complains of episodic digital pallor, cyanosis, and rubor, particularly when exposed to cold temperatures. This phenomenon is often the earliest symptom of systemic sclerosis. Which of the following is the most appropriate initial management strategy for this symptom?
View Answer & Explanation
Correct Answer: C
Rationale: The described symptoms are classic for Raynaud's phenomenon, which is a prominent feature of systemic sclerosis and often the presenting symptom. Initial management typically involves conservative measures like avoiding cold exposure and smoking cessation. Pharmacologically, calcium channel blockers (e.g., nifedipine, amlodipine) are the first-line agents to reduce the frequency and severity of vasospastic attacks. Corticosteroids and cyclophosphamide are immunosuppressants used for inflammatory or fibrotic organ involvement, not primarily for Raynaud's. Surgical sympathectomy is a more invasive option reserved for severe, refractory cases with critical ischemia. Amputation is a last resort for irreversible tissue loss.
Question 10
A 62-year-old female with limited cutaneous systemic sclerosis presents with painful, firm nodules on her fingertips and elbows. Examination reveals white, chalky material extruding from some of these lesions. Radiographs confirm extensive soft tissue calcifications. What is the most appropriate term for these calcifications?
View Answer & Explanation
Correct Answer: C
Rationale: The presence of firm, painful nodules with chalky material extruding, confirmed by radiographs as soft tissue calcifications, is characteristic of calcinosis cutis, a common feature of systemic sclerosis, particularly the limited cutaneous subtype (CREST). Tophi are urate crystal deposits seen in gout. Osteophytes are bony spurs associated with osteoarthritis. Heterotopic ossification is bone formation in soft tissues, often post-trauma or surgery. Gouty nodules are another term for tophi.
Question 10
A 50-year-old female with diffuse cutaneous systemic sclerosis presents with progressive difficulty making a fist and performing fine motor tasks. On examination, her fingers appear shiny, taut, and tapered, with reduced range of motion at the interphalangeal joints. This characteristic skin change is known as:
View Answer & Explanation
Correct Answer: C
Rationale: Sclerodactyly refers to the localized thickening and tightening of the skin of the fingers and toes, leading to a shiny, taut, and often tapered appearance, with associated joint contractures. It is a hallmark feature of systemic sclerosis. Livedo reticularis is a mottled, reticulated vascular pattern. Erythema nodosum is an inflammatory condition characterized by tender red nodules. Psoriatic plaques are scaly, erythematous lesions seen in psoriasis. Dermatofibroma is a benign skin lesion.
Question 10
A 48-year-old male with long-standing systemic sclerosis complains of chronic pain in his fingertips. Radiographs of his hands reveal resorption of the distal phalangeal tufts. This specific radiographic finding is termed:
View Answer & Explanation
Correct Answer: C
Rationale: Acro-osteolysis is the pathological resorption of the distal phalangeal tufts (terminal phalanges) and is a characteristic radiographic finding in systemic sclerosis, often associated with severe Raynaud's phenomenon and digital ischemia. Osteopenia is generalized bone thinning. Erosions are bone defects typically seen in inflammatory arthritis. Joint space narrowing indicates cartilage loss. Periarticular calcifications can be seen but are distinct from bone resorption.
Question 10
A 55-year-old female with systemic sclerosis presents with widespread arthralgias and morning stiffness affecting her hands, wrists, and knees. On examination, she has mild synovitis in several metacarpophalangeal joints and developing flexion contractures of her fingers. Which of the following is the most common musculoskeletal manifestation in systemic sclerosis?
View Answer & Explanation
Correct Answer: C
Rationale: Arthralgias (joint pain) and non-erosive polyarthritis are very common musculoskeletal manifestations in systemic sclerosis, affecting a significant percentage of patients. While some patients may develop mild synovitis, destructive erosive arthritis is rare and not typical of SSc (more common in RA). Gouty arthritis is unrelated to SSc. Septic arthritis is an infection. Avascular necrosis is not a primary musculoskeletal manifestation of SSc, though it can occur from other causes (e.g., corticosteroid use).
Question 10
A 42-year-old male with diffuse cutaneous systemic sclerosis reports a grating sensation and pain with movement around his wrists and ankles. On physical examination, palpable and audible friction rubs are noted over the extensor tendons of his wrists and the Achilles tendons. This finding is highly suggestive of:
View Answer & Explanation
Correct Answer: A
Rationale: Tendon friction rubs, described as a palpable and audible grating sensation over tendons, are a characteristic and often early sign of tenosynovitis in diffuse cutaneous systemic sclerosis. They are caused by the inflammatory and fibrotic process affecting the tendon sheaths. This finding is highly specific for SSc and can indicate more severe disease. Carpal tunnel syndrome is nerve compression. Gouty tendinitis involves urate crystals. Rheumatoid nodules are subcutaneous nodules in RA. Septic tenosynovitis would present with more acute signs of infection.
Question 10
A 60-year-old female with systemic sclerosis complains of severe heartburn, regurgitation, and difficulty swallowing solid foods. Barium swallow studies reveal decreased peristalsis in the distal two-thirds of the esophagus and a patulous lower esophageal sphincter. These symptoms are indicative of which common systemic manifestation?
View Answer & Explanation
Correct Answer: C
Rationale: Esophageal dysmotility, leading to dysphagia, heartburn, and reflux, is one of the most common gastrointestinal manifestations of systemic sclerosis, affecting nearly all patients. It results from fibrosis and atrophy of the smooth muscle in the esophagus. Scleroderma renal crisis, interstitial lung disease, pulmonary hypertension, and cardiac fibrosis are other serious systemic complications but do not directly explain the described GI symptoms.
Question 10
A 52-year-old male with diffuse cutaneous systemic sclerosis presents with progressive dyspnea on exertion and a persistent dry cough. High-resolution computed tomography (HRCT) of the chest shows ground-glass opacities and honeycombing, predominantly in the lung bases. This finding is most consistent with which severe complication of systemic sclerosis?
View Answer & Explanation
Correct Answer: B
Rationale: Progressive dyspnea, dry cough, and HRCT findings of ground-glass opacities and honeycombing are classic for interstitial lung disease (ILD), a major cause of morbidity and mortality in systemic sclerosis. ILD involves inflammation and fibrosis of the lung parenchyma. Bronchiectasis is abnormal widening of the airways. Pulmonary embolism is a blood clot in the lungs. Pleural effusion is fluid around the lungs. Asthma exacerbation involves airway hyperresponsiveness and bronchospasm.
Question 10
A 65-year-old female with limited cutaneous systemic sclerosis, who previously had stable disease, develops increasing fatigue, exertional dyspnea, and peripheral edema. Echocardiography reveals elevated right ventricular systolic pressure and right heart enlargement. These findings are most concerning for the development of:
View Answer & Explanation
Correct Answer: C
Rationale: The symptoms of progressive dyspnea, fatigue, peripheral edema, and echocardiographic evidence of elevated right ventricular pressure are highly suggestive of pulmonary hypertension (PH). PH is a serious and common complication of systemic sclerosis, particularly in the limited cutaneous subtype, and is a leading cause of death. Congestive heart failure is a broader term, and while PH can lead to right-sided heart failure, PH itself is the primary diagnosis here. Myocardial infarction, pericardial effusion, and aortic stenosis are other cardiac conditions but do not fit the specific findings as well as PH.
Question 10
A 35-year-old female with diffuse cutaneous systemic sclerosis presents to the emergency department with sudden onset of severe headache, blurred vision, and rapidly rising blood pressure (200/110 mmHg). Laboratory tests show new-onset microangiopathic hemolytic anemia and acute kidney injury. This constellation of symptoms is characteristic of which life-threatening complication?
View Answer & Explanation
Correct Answer: B
Rationale: Scleroderma renal crisis (SRC) is a medical emergency characterized by abrupt onset of severe hypertension, rapidly progressive renal failure, and often microangiopathic hemolytic anemia and thrombocytopenia. It is a life-threatening complication of systemic sclerosis, particularly in the diffuse subtype. While it involves hypertension, it is distinct from essential hypertension. Acute glomerulonephritis and drug-induced nephropathy have different etiologies. TTP shares some features but is a primary hematologic disorder, whereas SRC is a systemic sclerosis-specific complication.
Question 10
A 50-year-old female with systemic sclerosis is undergoing a preoperative evaluation for carpal tunnel release. Her medical history includes Raynaud's phenomenon, esophageal dysmotility, and mild sclerodactyly. During the cardiac workup, she is found to have evidence of myocardial fibrosis and conduction abnormalities. Which of the following cardiac manifestations is most commonly associated with systemic sclerosis?
View Answer & Explanation
Correct Answer: C
Rationale: Cardiac involvement in systemic sclerosis commonly includes myocardial fibrosis (leading to diastolic dysfunction, arrhythmias, and conduction abnormalities) and pericardial disease (pericardial effusions, pericarditis). While other cardiac issues can occur, these are the most characteristic direct cardiac manifestations of SSc. Valvular disease, primary coronary artery disease, and congenital defects are not typically primary features of SSc, though patients can develop them independently. Atrial fibrillation is a common arrhythmia but not specific to SSc pathology.
Question 10
A 40-year-old female presents with a 5-year history of Raynaud's phenomenon, telangiectasias, and sclerodactyly limited to her hands. Her rheumatologist orders a panel of autoantibodies to aid in diagnosis and prognosis. Which autoantibody is most strongly associated with limited cutaneous systemic sclerosis (CREST syndrome)?
View Answer & Explanation
Correct Answer: B
Rationale: Anti-centromere antibody (ACA) is highly specific for limited cutaneous systemic sclerosis (CREST syndrome) and is found in 50-90% of these patients. Anti-Scl-70 (anti-topoisomerase I) is associated with diffuse cutaneous systemic sclerosis and interstitial lung disease. Anti-RNA polymerase III is associated with diffuse cutaneous systemic sclerosis and scleroderma renal crisis. Anti-dsDNA is characteristic of systemic lupus erythematosus. Anti-Jo-1 is associated with polymyositis/dermatomyositis.
Question 10
A 50-year-old male presents with rapidly progressive skin thickening involving his trunk and proximal extremities, new-onset dysphagia, and recent development of interstitial lung disease. His rheumatologist suspects diffuse cutaneous systemic sclerosis. Which autoantibody is most commonly associated with this presentation and a higher risk of interstitial lung disease?
View Answer & Explanation
Correct Answer: C
Rationale: Anti-Scl-70 (anti-topoisomerase I) is strongly associated with diffuse cutaneous systemic sclerosis and is a marker for increased risk of interstitial lung disease. Anti-centromere antibody is associated with limited cutaneous SSc. Anti-Ro/SSA and Anti-La/SSB are associated with Sjögren's syndrome and lupus. Anti-U1 RNP is associated with mixed connective tissue disease.
Question 10
A 45-year-old female with systemic sclerosis develops painful digital ulcers on her fingertips, which are slow to heal and prone to infection. She has severe Raynaud's phenomenon. Which of the following is a key component in the management of these digital ulcers?
View Answer & Explanation
Correct Answer: C
Rationale: Digital ulcers in systemic sclerosis are primarily caused by severe microvascular ischemia due to Raynaud's phenomenon and vasculopathy. Therefore, treatment focuses on improving blood flow. Vasodilators such as prostacyclin analogs (e.g., iloprost, epoprostenol) or endothelin receptor antagonists (e.g., bosentan) are crucial for healing existing ulcers and preventing new ones. High-dose corticosteroids are generally avoided in SSc due to the risk of scleroderma renal crisis. Surgical debridement may be necessary for necrotic tissue but primary closure is often difficult due to poor vascularity. Physical therapy is for contractures, not ulcers. Methotrexate is an immunosuppressant, not a primary treatment for ischemic ulcers.
Question 10
A 58-year-old female with long-standing systemic sclerosis presents with severe flexion contractures of her fingers, making it difficult to perform daily activities. Her skin is taut and thickened over her hands. What is the primary non-pharmacological intervention for managing these joint contractures?
View Answer & Explanation
Correct Answer: C
Rationale: Joint contractures in systemic sclerosis are primarily due to skin and periarticular fibrosis. Regular physical and occupational therapy, focusing on stretching exercises, range of motion, and splinting, is the cornerstone of non-pharmacological management to maintain joint mobility and prevent further contractures. Surgical release is a last resort for severe, debilitating contractures. Immobilization in extension can be part of a splinting program but not as the sole intervention. Corticosteroid injections are for inflammation, not fibrosis. Topical retinoids are for skin conditions, not joint contractures.
Question 10
An orthopaedic surgeon is evaluating a 60-year-old female with diffuse cutaneous systemic sclerosis for elective total knee arthroplasty. Her medical history includes interstitial lung disease, Raynaud's phenomenon, and esophageal dysmotility. Which of the following is the most critical preoperative consideration for this patient?
View Answer & Explanation
Correct Answer: B
Rationale: Patients with systemic sclerosis, especially diffuse cutaneous SSc, have thickened, taut, and fragile skin with impaired microcirculation. This significantly increases the risk of skin breakdown, delayed wound healing, and infection post-surgery, making it a critical preoperative consideration for any elective procedure. While DVT prophylaxis, antibiotics, and pain management are standard, the unique skin and vascular pathology in SSc makes wound complications particularly challenging. Heterotopic ossification is not a primary concern specific to SSc in this context.
Question 10
A 30-year-old female presents with isolated Raynaud's phenomenon for 2 years, without any other symptoms of skin thickening, telangiectasias, or internal organ involvement. Her ANA is negative, and other autoantibodies are absent. She is concerned about developing systemic sclerosis. What is the most likely diagnosis in this patient?
View Answer & Explanation
Correct Answer: C
Rationale: Primary Raynaud's phenomenon (also known as Raynaud's disease) is characterized by isolated Raynaud's symptoms without evidence of an underlying connective tissue disease or other secondary cause. It typically has a benign course, no digital ulcers, and negative autoantibodies. The absence of skin thickening, telangiectasias, internal organ involvement, and negative autoantibodies differentiates it from systemic sclerosis and other connective tissue diseases. Limited and diffuse SSc would have other characteristic features and autoantibodies. Mixed connective tissue disease and SLE would also have specific autoantibodies and other systemic manifestations.
Question 10
A 68-year-old male with long-standing diffuse cutaneous systemic sclerosis has experienced progressive decline in his health. He has severe interstitial lung disease and recently developed pulmonary hypertension. What are the two leading causes of mortality in patients with systemic sclerosis?
View Answer & Explanation
Correct Answer: C
Rationale: Pulmonary hypertension and interstitial lung disease are the two most common and significant causes of mortality in patients with systemic sclerosis. These pulmonary complications lead to progressive respiratory failure and right heart failure. While renal crisis and cardiac involvement (including arrhythmias) are serious, and digital gangrene/sepsis can occur, PH and ILD are consistently identified as the leading causes of death. Malignancy risk is slightly increased, but not a leading cause of mortality compared to the pulmonary complications. Liver failure is not a typical direct complication of SSc.
Question 11
A 45-year-old female presents with a 10-year history of Raynaud's phenomenon, telangiectasias, and dysphagia. On examination, she has thickened skin limited to her fingers and face, and small, firm, subcutaneous nodules on her fingertips. Radiographs show soft tissue calcifications around the distal interphalangeal joints. Systemic workup reveals no significant lung or renal involvement. Which subtype of systemic sclerosis is most consistent with this presentation?
View Answer & Explanation
Correct Answer: B
Rationale: The patient's presentation with a long history of Raynaud's, telangiectasias, dysphagia, calcinosis (subcutaneous nodules and radiographic findings), and skin thickening limited to the fingers and face (sclerodactyly) is classic for Limited Cutaneous Systemic Sclerosis, often referred to as CREST syndrome (Calcinosis, Raynaud's, Esophageal dysmotility, Sclerodactyly, Telangiectasias). Diffuse cutaneous systemic sclerosis involves skin thickening proximal to the elbows and knees and often has more rapid progression and severe internal organ involvement. Systemic sclerosis sine scleroderma lacks skin involvement. Overlap syndrome involves features of SSc and another connective tissue disease. Undifferentiated connective tissue disease is used when criteria for a specific disease are not fully met.
Question 12
A 58-year-old male with a recent diagnosis of systemic sclerosis presents for evaluation of progressive hand stiffness. He has significant sclerodactyly and flexion contractures of his fingers. The underlying pathophysiology of systemic sclerosis involves an imbalance in which of the following cellular processes?
View Answer & Explanation
Correct Answer: B
Rationale: Systemic sclerosis is characterized by widespread vascular damage and excessive deposition of collagen and other extracellular matrix components in the skin and internal organs. This fibrosis is primarily driven by the overproduction of collagen by activated fibroblasts. While other connective tissue diseases involve different mechanisms, the hallmark of scleroderma is this fibrotic process. Increased osteoclast activity is seen in osteoporosis, autoimmune destruction of synovial cells in rheumatoid arthritis, impaired proteoglycan synthesis in osteoarthritis, and elastin degradation in conditions like Marfan syndrome or emphysema.
Question 13
A 38-year-old female with newly diagnosed systemic sclerosis complains of episodic digital pallor, cyanosis, and rubor, particularly when exposed to cold temperatures. This phenomenon is often the earliest symptom of systemic sclerosis. Which of the following is the most appropriate initial management strategy for this symptom?
View Answer & Explanation
Correct Answer: C
Rationale: The described symptoms are classic for Raynaud's phenomenon, which is a prominent feature of systemic sclerosis and often the presenting symptom. Initial management typically involves conservative measures like avoiding cold exposure and smoking cessation. Pharmacologically, calcium channel blockers (e.g., nifedipine, amlodipine) are the first-line agents to reduce the frequency and severity of vasospastic attacks. Corticosteroids and cyclophosphamide are immunosuppressants used for inflammatory or fibrotic organ involvement, not primarily for Raynaud's. Surgical sympathectomy is a more invasive option reserved for severe, refractory cases with critical ischemia. Amputation is a last resort for irreversible tissue loss.
Question 14
A 62-year-old female with limited cutaneous systemic sclerosis presents with painful, firm nodules on her fingertips and elbows. Examination reveals white, chalky material extruding from some of these lesions. Radiographs confirm extensive soft tissue calcifications. What is the most appropriate term for these calcifications?
View Answer & Explanation
Correct Answer: C
Rationale: The presence of firm, painful nodules with chalky material extruding, confirmed by radiographs as soft tissue calcifications, is characteristic of calcinosis cutis, a common feature of systemic sclerosis, particularly the limited cutaneous subtype (CREST). Tophi are urate crystal deposits seen in gout. Osteophytes are bony spurs associated with osteoarthritis. Heterotopic ossification is bone formation in soft tissues, often post-trauma or surgery. Gouty nodules are another term for tophi.
Question 15
A 50-year-old female with diffuse cutaneous systemic sclerosis presents with progressive difficulty making a fist and performing fine motor tasks. On examination, her fingers appear shiny, taut, and tapered, with reduced range of motion at the interphalangeal joints. This characteristic skin change is known as:
View Answer & Explanation
Correct Answer: C
Rationale: Sclerodactyly refers to the localized thickening and tightening of the skin of the fingers and toes, leading to a shiny, taut, and often tapered appearance, with associated joint contractures. It is a hallmark feature of systemic sclerosis. Livedo reticularis is a mottled, reticulated vascular pattern. Erythema nodosum is an inflammatory condition characterized by tender red nodules. Psoriatic plaques are scaly, erythematous lesions seen in psoriasis. Dermatofibroma is a benign skin lesion.
Question 16
A 48-year-old male with long-standing systemic sclerosis complains of chronic pain in his fingertips. Radiographs of his hands reveal resorption of the distal phalangeal tufts. This specific radiographic finding is termed:
View Answer & Explanation
Correct Answer: C
Rationale: Acro-osteolysis is the pathological resorption of the distal phalangeal tufts (terminal phalanges) and is a characteristic radiographic finding in systemic sclerosis, often associated with severe Raynaud's phenomenon and digital ischemia. Osteopenia is generalized bone thinning. Erosions are bone defects typically seen in inflammatory arthritis. Joint space narrowing indicates cartilage loss. Periarticular calcifications can be seen but are distinct from bone resorption.
Question 17
A 55-year-old female with systemic sclerosis presents with widespread arthralgias and morning stiffness affecting her hands, wrists, and knees. On examination, she has mild synovitis in several metacarpophalangeal joints and developing flexion contractures of her fingers. Which of the following is the most common musculoskeletal manifestation in systemic sclerosis?
View Answer & Explanation
Correct Answer: C
Rationale: Arthralgias (joint pain) and non-erosive polyarthritis are very common musculoskeletal manifestations in systemic sclerosis, affecting a significant percentage of patients. While some patients may develop mild synovitis, destructive erosive arthritis is rare and not typical of SSc (more common in RA). Gouty arthritis is unrelated to SSc. Septic arthritis is an infection. Avascular necrosis is not a primary musculoskeletal manifestation of SSc, though it can occur from other causes (e.g., corticosteroid use).
Question 18
A 42-year-old male with diffuse cutaneous systemic sclerosis reports a grating sensation and pain with movement around his wrists and ankles. On physical examination, palpable and audible friction rubs are noted over the extensor tendons of his wrists and the Achilles tendons. This finding is highly suggestive of:
View Answer & Explanation
Correct Answer: A
Rationale: Tendon friction rubs, described as a palpable and audible grating sensation over tendons, are a characteristic and often early sign of tenosynovitis in diffuse cutaneous systemic sclerosis. They are caused by the inflammatory and fibrotic process affecting the tendon sheaths. This finding is highly specific for SSc and can indicate more severe disease. Carpal tunnel syndrome is nerve compression. Gouty tendinitis involves urate crystals. Rheumatoid nodules are subcutaneous nodules in RA. Septic tenosynovitis would present with more acute signs of infection.
Question 19
A 60-year-old female with systemic sclerosis complains of severe heartburn, regurgitation, and difficulty swallowing solid foods. Barium swallow studies reveal decreased peristalsis in the distal two-thirds of the esophagus and a patulous lower esophageal sphincter. These symptoms are indicative of which common systemic manifestation?
View Answer & Explanation
Correct Answer: C
Rationale: Esophageal dysmotility, leading to dysphagia, heartburn, and reflux, is one of the most common gastrointestinal manifestations of systemic sclerosis, affecting nearly all patients. It results from fibrosis and atrophy of the smooth muscle in the esophagus. Scleroderma renal crisis, interstitial lung disease, pulmonary hypertension, and cardiac fibrosis are other serious systemic complications but do not directly explain the described GI symptoms.
Question 20
A 52-year-old male with diffuse cutaneous systemic sclerosis presents with progressive dyspnea on exertion and a persistent dry cough. High-resolution computed tomography (HRCT) of the chest shows ground-glass opacities and honeycombing, predominantly in the lung bases. This finding is most consistent with which severe complication of systemic sclerosis?
View Answer & Explanation
Correct Answer: B
Rationale: Progressive dyspnea, dry cough, and HRCT findings of ground-glass opacities and honeycombing are classic for interstitial lung disease (ILD), a major cause of morbidity and mortality in systemic sclerosis. ILD involves inflammation and fibrosis of the lung parenchyma. Bronchiectasis is abnormal widening of the airways. Pulmonary embolism is a blood clot in the lungs. Pleural effusion is fluid around the lungs. Asthma exacerbation involves airway hyperresponsiveness and bronchospasm.
Question 21
A 65-year-old female with limited cutaneous systemic sclerosis, who previously had stable disease, develops increasing fatigue, exertional dyspnea, and peripheral edema. Echocardiography reveals elevated right ventricular systolic pressure and right heart enlargement. These findings are most concerning for the development of:
View Answer & Explanation
Correct Answer: C
Rationale: The symptoms of progressive dyspnea, fatigue, peripheral edema, and echocardiographic evidence of elevated right ventricular pressure are highly suggestive of pulmonary hypertension (PH). PH is a serious and common complication of systemic sclerosis, particularly in the limited cutaneous subtype, and is a leading cause of death. Congestive heart failure is a broader term, and while PH can lead to right-sided heart failure, PH itself is the primary diagnosis here. Myocardial infarction, pericardial effusion, and aortic stenosis are other cardiac conditions but do not fit the specific findings as well as PH.
Question 22
A 35-year-old female with diffuse cutaneous systemic sclerosis presents to the emergency department with sudden onset of severe headache, blurred vision, and rapidly rising blood pressure (200/110 mmHg). Laboratory tests show new-onset microangiopathic hemolytic anemia and acute kidney injury. This constellation of symptoms is characteristic of which life-threatening complication?
View Answer & Explanation
Correct Answer: B
Rationale: Scleroderma renal crisis (SRC) is a medical emergency characterized by abrupt onset of severe hypertension, rapidly progressive renal failure, and often microangiopathic hemolytic anemia and thrombocytopenia. It is a life-threatening complication of systemic sclerosis, particularly in the diffuse subtype. While it involves hypertension, it is distinct from essential hypertension. Acute glomerulonephritis and drug-induced nephropathy have different etiologies. TTP shares some features but is a primary hematologic disorder, whereas SRC is a systemic sclerosis-specific complication.
Question 23
A 50-year-old female with systemic sclerosis is undergoing a preoperative evaluation for carpal tunnel release. Her medical history includes Raynaud's phenomenon, esophageal dysmotility, and mild sclerodactyly. During the cardiac workup, she is found to have evidence of myocardial fibrosis and conduction abnormalities. Which of the following cardiac manifestations is most commonly associated with systemic sclerosis?
View Answer & Explanation
Correct Answer: C
Rationale: Cardiac involvement in systemic sclerosis commonly includes myocardial fibrosis (leading to diastolic dysfunction, arrhythmias, and conduction abnormalities) and pericardial disease (pericardial effusions, pericarditis). While other cardiac issues can occur, these are the most characteristic direct cardiac manifestations of SSc. Valvular disease, primary coronary artery disease, and congenital defects are not typically primary features of SSc, though patients can develop them independently. Atrial fibrillation is a common arrhythmia but not specific to SSc pathology.
Question 24
A 40-year-old female presents with a 5-year history of Raynaud's phenomenon, telangiectasias, and sclerodactyly limited to her hands. Her rheumatologist orders a panel of autoantibodies to aid in diagnosis and prognosis. Which autoantibody is most strongly associated with limited cutaneous systemic sclerosis (CREST syndrome)?
View Answer & Explanation
Correct Answer: B
Rationale: Anti-centromere antibody (ACA) is highly specific for limited cutaneous systemic sclerosis (CREST syndrome) and is found in 50-90% of these patients. Anti-Scl-70 (anti-topoisomerase I) is associated with diffuse cutaneous systemic sclerosis and interstitial lung disease. Anti-RNA polymerase III is associated with diffuse cutaneous systemic sclerosis and scleroderma renal crisis. Anti-dsDNA is characteristic of systemic lupus erythematosus. Anti-Jo-1 is associated with polymyositis/dermatomyositis.
Question 25
A 50-year-old male presents with rapidly progressive skin thickening involving his trunk and proximal extremities, new-onset dysphagia, and recent development of interstitial lung disease. His rheumatologist suspects diffuse cutaneous systemic sclerosis. Which autoantibody is most commonly associated with this presentation and a higher risk of interstitial lung disease?
View Answer & Explanation
Correct Answer: C
Rationale: Anti-Scl-70 (anti-topoisomerase I) is strongly associated with diffuse cutaneous systemic sclerosis and is a marker for increased risk of interstitial lung disease. Anti-centromere antibody is associated with limited cutaneous SSc. Anti-Ro/SSA and Anti-La/SSB are associated with Sjögren's syndrome and lupus. Anti-U1 RNP is associated with mixed connective tissue disease.
Question 26
A 45-year-old female with systemic sclerosis develops painful digital ulcers on her fingertips, which are slow to heal and prone to infection. She has severe Raynaud's phenomenon. Which of the following is a key component in the management of these digital ulcers?
View Answer & Explanation
Correct Answer: C
Rationale: Digital ulcers in systemic sclerosis are primarily caused by severe microvascular ischemia due to Raynaud's phenomenon and vasculopathy. Therefore, treatment focuses on improving blood flow. Vasodilators such as prostacyclin analogs (e.g., iloprost, epoprostenol) or endothelin receptor antagonists (e.g., bosentan) are crucial for healing existing ulcers and preventing new ones. High-dose corticosteroids are generally avoided in SSc due to the risk of scleroderma renal crisis. Surgical debridement may be necessary for necrotic tissue but primary closure is often difficult due to poor vascularity. Physical therapy is for contractures, not ulcers. Methotrexate is an immunosuppressant, not a primary treatment for ischemic ulcers.
Question 27
A 58-year-old female with long-standing systemic sclerosis presents with severe flexion contractures of her fingers, making it difficult to perform daily activities. Her skin is taut and thickened over her hands. What is the primary non-pharmacological intervention for managing these joint contractures?
View Answer & Explanation
Correct Answer: C
Rationale: Joint contractures in systemic sclerosis are primarily due to skin and periarticular fibrosis. Regular physical and occupational therapy, focusing on stretching exercises, range of motion, and splinting, is the cornerstone of non-pharmacological management to maintain joint mobility and prevent further contractures. Surgical release is a last resort for severe, debilitating contractures. Immobilization in extension can be part of a splinting program but not as the sole intervention. Corticosteroid injections are for inflammation, not fibrosis. Topical retinoids are for skin conditions, not joint contractures.
Question 28
An orthopaedic surgeon is evaluating a 60-year-old female with diffuse cutaneous systemic sclerosis for elective total knee arthroplasty. Her medical history includes interstitial lung disease, Raynaud's phenomenon, and esophageal dysmotility. Which of the following is the most critical preoperative consideration for this patient?
View Answer & Explanation
Correct Answer: B
Rationale: Patients with systemic sclerosis, especially diffuse cutaneous SSc, have thickened, taut, and fragile skin with impaired microcirculation. This significantly increases the risk of skin breakdown, delayed wound healing, and infection post-surgery, making it a critical preoperative consideration for any elective procedure. While DVT prophylaxis, antibiotics, and pain management are standard, the unique skin and vascular pathology in SSc makes wound complications particularly challenging. Heterotopic ossification is not a primary concern specific to SSc in this context.
Question 29
A 30-year-old female presents with isolated Raynaud's phenomenon for 2 years, without any other symptoms of skin thickening, telangiectasias, or internal organ involvement. Her ANA is negative, and other autoantibodies are absent. She is concerned about developing systemic sclerosis. What is the most likely diagnosis in this patient?
View Answer & Explanation
Correct Answer: C
Rationale: Primary Raynaud's phenomenon (also known as Raynaud's disease) is characterized by isolated Raynaud's symptoms without evidence of an underlying connective tissue disease or other secondary cause. It typically has a benign course, no digital ulcers, and negative autoantibodies. The absence of skin thickening, telangiectasias, internal organ involvement, and negative autoantibodies differentiates it from systemic sclerosis and other connective tissue diseases. Limited and diffuse SSc would have other characteristic features and autoantibodies. Mixed connective tissue disease and SLE would also have specific autoantibodies and other systemic manifestations.
Question 30
A 5-year-old boy presents with disproportionately short forearms and shins. Physical examination reveals significant shortening of the middle segments of his limbs. Radiographs confirm a chondrodysplasia primarily affecting these regions.
View Answer & Explanation
Correct Answer: C
Rationale: Mesomelic dwarfism is defined as a rare mesomelic chondrodysplasia with an elective defect of the mesial segments of the limbs, which correspond to the middle segments (forearms and shins). Rhizomelic dwarfism affects the proximal segments, and acromelic dwarfism affects the distal segments.
Question 31
A 10-year-old girl is diagnosed with Nievergelt type mesomelic dwarfism. Her father also has the condition, and her paternal grandfather had similar features.
View Answer & Explanation
Correct Answer: C
Rationale: The provided text explicitly states that Nievergelt and Langer type mesomelic dwarfism is a "high penetrating autosomal dominant" condition. The family history provided in the vignette supports this inheritance pattern.
Question 32
A 7-year-old boy presents with short stature, bowing of the forearms, and atypical clubfeet. Genetic testing is performed to confirm the diagnosis of Nievergelt type mesomelic dwarfism.
View Answer & Explanation
Correct Answer: C
Rationale: The text states that Nievergelt and Langer type mesomelic dwarfism is "caused by mutations in the SHOX gene." FGFR3 mutations are associated with achondroplasia, a common rhizomelic dwarfism, making it a plausible distractor for general dwarfism knowledge.
Question 33
A 12-year-old male with a known diagnosis of Nievergelt type mesomelic dwarfism undergoes a routine orthopedic evaluation. Physical examination reveals limited forearm rotation. Radiographs of the forearm are ordered.
View Answer & Explanation
Correct Answer: C
Rationale: The text lists "radio-ulnar...synostosis" as a specific feature of Nievergelt and Langer type mesomelic dwarfism. This fusion would directly explain limited forearm rotation. Radial head subluxation can occur in other conditions but is not specifically mentioned as a primary feature of this type of mesomelic dwarfism.
Question 34
A 9-year-old girl with mesomelic dwarfism, Nievergelt type, presents with progressive bowing of her lower legs and difficulty with ambulation. Radiographs of her tibias and fibulas are obtained.
View Answer & Explanation
Correct Answer: B
Rationale: The text explicitly mentions "tibio-fibular...synostosis" as a characteristic feature of Nievergelt and Langer type mesomelic dwarfism. Talo-calcaneal synostosis is a type of intertarsal synostosis, which is also a feature, but tibio-fibular synostosis directly addresses the long bones of the lower leg.
Question 35
A 6-year-old boy with a family history of mesomelic dwarfism presents with bilateral foot deformities. On examination, his feet appear rigid and malformed, consistent with atypical clubfeet. Radiographs are performed.
View Answer & Explanation
Correct Answer: D
Rationale: The text lists "atypical clubfeet" and "intertarsal synostosis" as features of Nievergelt and Langer type mesomelic dwarfism. Calcaneal-cuboid synostosis is a specific example of an intertarsal synostosis, but "intertarsal synostosis" is the broader, directly stated term in the provided text.
Question 36
A 14-year-old patient with Nievergelt type mesomelic dwarfism reports chronic elbow pain and limited range of motion. Physical examination confirms significant restriction in flexion and extension.
View Answer & Explanation
Correct Answer: C
Rationale: The text explicitly mentions "deformities of the elbow joints" as a characteristic feature of Nievergelt and Langer type mesomelic dwarfism. These deformities would naturally lead to limited range of motion and potential pain.
Question 37
A genetic counselor is discussing the prognosis and recurrence risk for a couple whose child has a form of mesomelic dwarfism. The child presents with hip dislocation, clubhand, and short malformed fingers, and genetic testing reveals an autosomal recessive inheritance pattern.
View Answer & Explanation
Correct Answer: D
Rationale: The text describes Acro–coxo–mesomelic dwarfism as "autosomal recessive dwarfi sm, with hip dislocation, clubhand and foot, short malformed fi ngers, reduced articular mobility of elbows, clinodactyly, brachyrhizophalangia." This matches the clinical picture and inheritance pattern in the vignette. Nievergelt's and Langer types are autosomal dominant.
Question 38
A 3-year-old girl is diagnosed with a mesomelic dwarfism. Her parents are concerned about potential hip problems. On examination, she has short, malformed fingers and reduced elbow mobility. Radiographs show bilateral hip dislocations.
View Answer & Explanation
Correct Answer: D
Rationale: The text specifically lists "hip dislocation" as a feature of Acro–coxo–mesomelic dwarfism, which is distinct from the features listed for Nievergelt and Langer type. While "reduced articular mobility of elbows" is mentioned for Acro-coxo-mesomelic, "deformities of the elbow joints" is listed for Nievergelt/Langer, making hip dislocation a clearer distinguishing feature.
Question 39
A pediatrician observes a 2-year-old child with disproportionate short stature. The child's forearms and lower legs appear significantly shorter than the upper arms and thighs.
View Answer & Explanation
Correct Answer: C
Rationale: The term "mesomelic" refers to the middle segments of the limbs, specifically the forearms (radius and ulna) and the lower legs (tibia and fibula). This is consistent with the definition of mesomelic dwarfism as an elective defect of the mesial segments.
Question 40
A 10-year-old boy presents with disproportionate short stature. Physical examination reveals significantly shortened forearms and lower legs compared to his upper arms and thighs. Radiographs confirm a chondrodysplasia primarily affecting the middle segments of the limbs.
View Answer & Explanation
Correct Answer: B
Rationale: The case text explicitly defines mesomelic dwarfism as having an "elective defect of the mesial segments of the limbs," which refers to the middle segments (forearms and lower legs). This is consistent with the clinical presentation.
Main Distractor: A) Proximal (rhizomelic) - Rhizomelic dwarfism affects the proximal segments (humerus and femur), which is not consistent with the description of shortened forearms and lower legs.
Question 41
A 7-year-old girl is diagnosed with mesomelic dwarfism, Nievergelt type, characterized by severe shortening of the forearms and lower legs, radio-ulnar synostosis, and atypical clubfeet. Genetic testing is recommended.
View Answer & Explanation
Correct Answer: C
Rationale: The case text explicitly states that mesomelic dwarfism (Nievergelt and Langer Type) is "caused by mutations in the SHOX gene."
Main Distractor: A) FGFR3 - FGFR3 mutations are associated with achondroplasia and hypochondroplasia, which are different types of skeletal dysplasias, not mesomelic dwarfism.
Question 42
A 5-year-old boy presents with mesomelic dwarfism, Nievergelt type. His mother also has mild disproportionate short stature with similar limb segment involvement.
View Answer & Explanation
Correct Answer: B
Rationale: The case text explicitly states, "This disease is high penetrating autosomal dominant with pleiotropic expression syndrome." The involvement of the mother and child is consistent with an autosomal dominant inheritance pattern.
Main Distractor: A) Autosomal recessive - While acro-coxo-mesomelic dwarfism is described as autosomal recessive, the Nievergelt and Langer type, which is the primary focus of the text, is autosomal dominant.
Question 43
A 12-year-old male with a known diagnosis of mesomelic dwarfism (Nievergelt type) presents for orthopedic evaluation. Clinical examination reveals limited forearm rotation. Radiographs of the forearm are obtained.
View Answer & Explanation
Correct Answer: C
Rationale: The case text lists "radio-ulnar... synostosis" as a characteristic feature of mesomelic dwarfism (Nievergelt and Langer Type). Radio-ulnar synostosis directly causes limited forearm rotation (pronation/supination).
Main Distractor: A) Radial head dislocation - While possible in some skeletal dysplasias, radio-ulnar synostosis is specifically mentioned as a defining feature in the text and directly explains the limited rotation.
Question 44
A 9-year-old girl with mesomelic dwarfism (Langer type) undergoes a lower extremity radiographic series due to progressive bowing of her lower legs and difficulty with ambulation.
View Answer & Explanation
Correct Answer: C
Rationale: The case text lists "tibio-fibular... synostosis" as a characteristic feature of mesomelic dwarfism (Nievergelt and Langer Type), affecting the lower limbs.
Main Distractor: D) Talo-calcaneal synostosis - While intertarsal synostosis is mentioned, tibio-fibular synostosis is a more prominent and specific long bone synostosis described in the lower leg, directly contributing to lower leg deformities.
Question 45
A 6-year-old boy with mesomelic dwarfism is evaluated for foot deformities. His parents report difficulty finding shoes that fit and observe an unusual foot shape since birth.
View Answer & Explanation
Correct Answer: C
Rationale: The case text explicitly mentions "atypical clubfeet" as a feature of mesomelic dwarfism (Nievergelt and Langer Type).
Main Distractor: A) Pes planus - While foot deformities can vary, "atypical clubfeet" is the specific and characteristic description provided in the teaching case for this condition.
Question 46
A 13-year-old girl with mesomelic dwarfism, Nievergelt type, presents with limited range of motion in her elbows. She struggles with activities requiring full extension or flexion.
View Answer & Explanation
Correct Answer: C
Rationale: The case text explicitly lists "deformities of the elbow joints" as a feature of mesomelic dwarfism (Nievergelt and Langer Type), which would account for limited range of motion.
Main Distractor: B) Recurrent dislocation of the radial head - While this can be a type of elbow deformity, the text uses the broader term "deformities of the elbow joints," which encompasses various issues, and does not specify dislocation as the sole or primary deformity.
Question 47
A 68-year-old male undergoes an elective total knee arthroplasty. He has a history of type 2 diabetes mellitus, obesity (BMI 35), and active smoking. On post-operative day 7, he develops fever, increasing knee pain, and purulent drainage from the incision. Which of the following is the most significant modifiable risk factor for surgical site infection in this patient?
View Answer & Explanation
Correct Answer: D
Rationale: Active smoking is a significant modifiable risk factor for surgical site infections due to its detrimental effects on wound healing, tissue oxygenation, and immune function. While diabetes and obesity are also modifiable risk factors, smoking cessation pre-operatively has a more immediate and profound impact on reducing SSI risk. Age and the elective nature of surgery are non-modifiable or less directly impactful on SSI risk compared to the patient's systemic health factors. The main distractor, B (Type 2 diabetes mellitus), is also a significant modifiable risk factor, but smoking cessation often yields a more rapid and substantial reduction in SSI risk when implemented pre-operatively.
Question 48
A 55-year-old female presents with acute onset pain, swelling, and erythema around her right hip, 3 weeks after undergoing a total hip arthroplasty. Laboratory tests reveal an elevated ESR and CRP. Aspiration of the joint yields purulent fluid. Gram stain shows gram-positive cocci in clusters. Which organism is the most likely causative agent?
View Answer & Explanation
Correct Answer: C
Rationale: Staphylococcus aureus is the most common causative organism for acute prosthetic joint infections, especially those occurring within the first few weeks to months post-operatively, and is characterized by gram-positive cocci in clusters on Gram stain. Coagulase-negative Staphylococci (like S. epidermidis) are also common but typically present as more indolent, chronic infections. Pseudomonas and E. coli are gram-negative organisms and less common in acute PJI. Streptococcus pyogenes is less common than S. aureus in this setting. The main distractor, D (Coagulase-negative Staphylococcus), is a common cause of PJI but typically presents with a more subacute or chronic course, rather than the acute onset described.
Question 49
A 72-year-old male is scheduled for a primary total shoulder arthroplasty. He has no known drug allergies. To minimize the risk of surgical site infection, what is the most appropriate prophylactic antibiotic regimen?
View Answer & Explanation
Correct Answer: C
Rationale: Intravenous Cefazolin (a first-generation cephalosporin) administered 30-60 minutes prior to incision is the standard prophylactic antibiotic for most orthopaedic surgeries. It provides excellent coverage against common skin flora, particularly Staphylococcus species, which are the most frequent cause of surgical site infections. Oral antibiotics are generally not used for surgical prophylaxis. Vancomycin is reserved for patients with penicillin allergies or in settings with high MRSA prevalence. Post-operative antibiotics are not routinely recommended for prophylaxis beyond the immediate perioperative period. The main distractor, B (Intravenous Vancomycin), is appropriate for patients with severe penicillin allergy or in high-risk MRSA settings, but Cefazolin is the first-line choice for general prophylaxis.
Question 50
A 60-year-old female presents with persistent pain and stiffness in her left hip, 18 months after a total hip arthroplasty. She denies fever or chills. ESR is 45 mm/hr (normal <20) and CRP is 15 mg/L (normal <5). Aspiration of the hip joint is performed. Which of the following synovial fluid findings is most indicative of a prosthetic joint infection?
View Answer & Explanation
Correct Answer: C
Rationale: For chronic prosthetic joint infections (PJI), a synovial fluid WBC count >2,000 cells/µL and a PMN percentage >70% (or >80% for hip/knee) are highly suggestive of infection. A WBC count of 3,000 cells/µL with 80% PMN meets these criteria. Options A and B are below the typical thresholds for PJI. A negative Gram stain does not rule out infection, as it has low sensitivity. Synovial fluid glucose is less reliable than cell count and differential for diagnosing PJI. The main distractor, B (PMN percentage of 60%), is below the typical threshold for PJI, which is usually >70-80% for chronic infections.
Question 51
A 45-year-old male develops an acute prosthetic joint infection (PJI) of his knee 4 weeks after total knee arthroplasty, caused by methicillin-sensitive Staphylococcus aureus (MSSA). He is otherwise healthy. What is the most appropriate initial management strategy?
View Answer & Explanation
Correct Answer: B
Rationale: For acute PJI (onset within 3-4 weeks of surgery) caused by a susceptible organism, in a patient with a well-fixed prosthesis and no sinus tract, irrigation and debridement (I&D) with exchange of modular components (e.g., polyethylene liner) followed by a prolonged course of culture-specific intravenous antibiotics is the preferred initial management. This approach aims to eradicate the infection while preserving the prosthesis. Two-stage revision is typically reserved for chronic infections or failed I&D. Arthrodesis and amputation are salvage procedures for intractable infections. Suppressive antibiotics alone are generally not curative for acute PJI. The main distractor, C (Two-stage revision arthroplasty), is the gold standard for chronic PJI, but for acute infections, prosthesis retention via I&D and component exchange is often successful.
Question 52
A 70-year-old female presents with a chronic prosthetic joint infection of her hip, 2 years after total hip arthroplasty. Cultures have repeatedly grown methicillin-resistant Staphylococcus aureus (MRSA). She has a draining sinus tract and significant bone loss around the femoral component. What is the most appropriate definitive surgical management?
View Answer & Explanation
Correct Answer: C
Rationale: For chronic PJI, especially with resistant organisms like MRSA, a draining sinus tract, or significant bone loss, a two-stage revision arthroplasty is the gold standard. This involves removal of all components, thorough debridement, placement of an antibiotic-laden cement spacer, a period of intravenous antibiotics, and then reimplantation of new components after infection markers normalize. I&D with component exchange is unlikely to be successful for chronic infections. One-stage revision is considered in highly selected cases without resistant organisms or extensive tissue damage. Suppressive antibiotics are not curative. Excision arthroplasty is a salvage procedure, not a definitive reconstructive solution. The main distractor, A (Irrigation and debridement with polyethylene exchange), is appropriate for acute infections but has a very low success rate for chronic PJI, especially with MRSA and a sinus tract.
Question 53
A 50-year-old male receives a corticosteroid injection for shoulder impingement. Three days later, he develops severe pain, swelling, and warmth in the injected shoulder, accompanied by fever. Aspiration reveals purulent fluid. Which of the following is the most likely cause of this iatrogenic infection?
View Answer & Explanation
Correct Answer: A
Rationale: The most common cause of iatrogenic joint infection following an injection is direct contamination during the procedure, introducing skin flora into the joint space. While corticosteroids can cause local immune suppression, this typically facilitates the growth of introduced bacteria rather than being the primary cause of infection itself. Hematogenous spread is less likely given the direct temporal and anatomical relationship to the injection. Reactivation of latent infection is rare. An allergic reaction would typically present with rash, itching, or anaphylaxis, not purulent arthritis. The main distractor, B (Steroid-induced immune suppression), is a contributing factor that can worsen an infection, but the initial introduction of bacteria is almost always due to contamination during the procedure.
Question 54
A 65-year-old female undergoes a lumbar laminectomy and fusion. On post-operative day 10, she develops increasing back pain, fever, and purulent drainage from the surgical incision. Cultures grow Staphylococcus epidermidis. What is the most appropriate initial management for this superficial surgical site infection?
View Answer & Explanation
Correct Answer: B
Rationale: For a superficial surgical site infection with purulent drainage, incision and drainage (I&D) with wound debridement is crucial to remove infected tissue and biofilm, followed by culture-specific antibiotics. Oral antibiotics alone are often insufficient for purulent infections. Removal of instrumentation is typically reserved for deep infections involving the hardware or failed I&D. Long-term suppressive antibiotics are not curative. Observation alone risks progression to a deeper infection. The main distractor, A (Oral antibiotics alone), is insufficient for a purulent infection, as source control (I&D) is paramount.
Question 55
A 30-year-old male sustains a Gustilo-Anderson Type IIIA open tibia fracture after a motor vehicle accident. He arrives in the emergency department 2 hours after injury. Which of the following interventions is most critical in preventing iatrogenic infection in this setting?
View Answer & Explanation
Correct Answer: B
Rationale: Early and thorough surgical debridement and irrigation of open fractures are the most critical steps in preventing infection. This removes devitalized tissue and contaminants, reducing the bacterial load. While immediate antibiotics are important, they are adjunctive to surgical debridement. Tetanus prophylaxis is standard but not the primary infection prevention strategy. Primary wound closure is often delayed in open fractures, especially Type IIIA, to allow for repeat debridement and reduce infection risk. NPWT can be used but is not the initial critical step. The main distractor, A (Immediate intravenous broad-spectrum antibiotics), is essential but serves as an adjunct to the primary mechanical removal of contaminants and devitalized tissue through surgical debridement.
Question 56
A 68-year-old female develops a chronic prosthetic joint infection of her knee. Cultures repeatedly grow Coagulase-negative Staphylococcus. The persistence of infection despite multiple antibiotic courses is most likely attributed to which characteristic of the bacteria?
View Answer & Explanation
Correct Answer: C
Rationale: Coagulase-negative Staphylococci (e.g., S. epidermidis) are notorious for their ability to form biofilms on orthopaedic implant surfaces. Biofilms are communities of bacteria encased in an extracellular polymeric substance, which provides a protective barrier against antibiotics and host immune defenses, making eradication extremely difficult without implant removal. While some strains may have intrinsic resistance, biofilm formation is the primary reason for persistent infection. Rapid replication, exotoxin production, and high virulence are more characteristic of acute, aggressive infections. The main distractor, A (Intrinsic antibiotic resistance), can contribute, but the physical protection and altered metabolic state within a biofilm are the primary mechanisms for antibiotic treatment failure in implant-associated infections.
Question 57
A 58-year-old male develops a deep surgical site infection following an open reduction and internal fixation of a distal femur fracture. He presents with wound dehiscence, purulent drainage, and exposed hardware. What is the primary goal of surgical debridement in this scenario?
View Answer & Explanation
Correct Answer: C
Rationale: The primary goal of surgical debridement in an infected wound is to remove all devitalized (necrotic) and infected tissue. This reduces the bacterial load, removes a nidus for infection, and promotes healthy tissue growth. While hardware removal may be necessary in some cases (especially if the infection is chronic or hardware is loose), it's not always the initial primary goal. Primary wound closure is often delayed until the infection is controlled. Obtaining tissue for culture is important, but it's a secondary goal to the therapeutic removal of infected tissue. Topical antibiotics are adjunctive, not the primary surgical goal. The main distractor, A (To remove all foreign material including the hardware), is sometimes necessary but not the *primary* goal of debridement itself, which focuses on tissue viability. Hardware removal is a separate decision based on the infection's nature and chronicity.
Question 58
A 40-year-old female develops a post-operative wound infection after an anterior cruciate ligament reconstruction. Cultures grow Methicillin-resistant Staphylococcus aureus (MRSA). Which of the following antibiotics is the most appropriate initial treatment?
View Answer & Explanation
Correct Answer: C
Rationale: Vancomycin is the drug of choice for treating infections caused by Methicillin-resistant Staphylococcus aureus (MRSA). Cefazolin and Amoxicillin-clavulanate are beta-lactam antibiotics that are ineffective against MRSA. Piperacillin-tazobactam has broad-spectrum activity but is not reliably effective against MRSA. Ciprofloxacin is a fluoroquinolone, which may have some activity but is not the first-line agent for MRSA. The main distractor, A (Cefazolin), is a first-generation cephalosporin and the standard prophylactic antibiotic, but it is ineffective against MRSA.
Question 59
A 75-year-old male undergoes a hip hemiarthroplasty for a femoral neck fracture. He receives perioperative antibiotics and a prolonged course of post-operative antibiotics for a suspected urinary tract infection. Two weeks later, he develops severe diarrhea and abdominal pain. Stool studies confirm Clostridioides difficile infection (CDI). Which of the following is the most significant risk factor for developing CDI in this patient?
View Answer & Explanation
Correct Answer: C
Rationale: Prolonged or broad-spectrum antibiotic use is the most significant risk factor for Clostridioides difficile infection (CDI). Antibiotics disrupt the normal gut flora, allowing C. difficile to proliferate and produce toxins. While advanced age and recent surgery are also risk factors, antibiotic exposure is the primary trigger. A hip fracture itself is not a direct risk factor for CDI. A suspected UTI might lead to antibiotic use, but the antibiotics themselves are the direct cause. The main distractor, A (Advanced age), is a significant risk factor for severe CDI and poor outcomes, but the direct precipitating factor for the infection itself is almost always antibiotic exposure.
Question 60
A 60-year-old female, 5 days post-total knee arthroplasty, presents with erythema and warmth around the incision, but no purulent drainage or systemic signs of infection. Her ESR and CRP are mildly elevated but trending down from post-operative peaks. What is the most likely diagnosis?
View Answer & Explanation
Correct Answer: B
Rationale: Erythema and warmth around an incision without purulent drainage or systemic signs of infection, especially with improving inflammatory markers, are most consistent with a superficial surgical site infection (cellulitis). Deep PJI would typically involve more severe pain, purulent drainage, and persistently elevated inflammatory markers. Normal post-operative inflammation should be resolving by day 5, and while some erythema is normal, increasing warmth suggests infection. A hematoma would typically present with swelling and ecchymosis, not necessarily increasing warmth. An allergic reaction would usually involve itching and a rash. The main distractor, C (Normal post-operative inflammation), is plausible, but the description of "erythema and warmth around the incision" suggests something beyond typical inflammation, leaning towards a superficial infection, especially if these symptoms are new or worsening.
Question 61
A 55-year-old male with poorly controlled type 2 diabetes (HbA1c 9.5%) is scheduled for an elective ankle fusion. To reduce the risk of surgical site infection, which pre-operative intervention is most important?
View Answer & Explanation
Correct Answer: B
Rationale: For diabetic patients, optimization of glycemic control (aiming for an HbA1c <7% and blood glucose <180 mg/dL perioperatively) is paramount in reducing the risk of surgical site infection. Hyperglycemia impairs neutrophil function, wound healing, and increases infection susceptibility. While all other options are important for SSI prevention, glycemic control is uniquely critical for diabetic patients. Smoking cessation is important but not specific to diabetes. The main distractor, C (Administration of prophylactic antibiotics), is standard for all surgeries, but for a diabetic patient with poor control, optimizing their metabolic state is a more fundamental and impactful intervention for infection prevention.
Question 62
A 28-year-old male undergoes an arthroscopic meniscectomy. Three days later, he develops increasing knee pain, swelling, and a low-grade fever. Physical examination reveals a warm, tender, effused knee joint. Which of the following is the most appropriate next step in management?
View Answer & Explanation
Correct Answer: C
Rationale: Given the signs and symptoms suggestive of septic arthritis following arthroscopy, immediate aspiration of the knee joint is the most appropriate next step. This diagnostic procedure provides crucial information (cell count, Gram stain, culture) to confirm the diagnosis, identify the causative organism, and guide antibiotic therapy. Oral antibiotics alone are insufficient for septic arthritis. RICE is for inflammatory conditions, not infection. MRI might show effusion but is not diagnostic for infection and delays definitive treatment. Immediate surgical debridement is often necessary *after* diagnosis is confirmed by aspiration. The main distractor, E (Immediate surgical debridement), is a likely subsequent step if septic arthritis is confirmed, but aspiration is necessary first to confirm the diagnosis and guide treatment.
Question 63
A 50-year-old male, 3 days post-operative from an open reduction internal fixation of an ankle fracture, presents with increasing redness and warmth extending from the incision, but no purulent drainage. He has no fever, and his white blood cell count is normal. What is the most likely diagnosis?
View Answer & Explanation
Correct Answer: B
Rationale: Increasing redness and warmth extending from an incision without purulent drainage, systemic signs of infection (fever, elevated WBC), or severe pain/toxicity is most consistent with cellulitis, a superficial surgical site infection. Deep SSI would typically involve more severe pain, purulent drainage, and often systemic signs. Necrotizing fasciitis is a rapidly progressive, severe infection with disproportionate pain, skin changes (bullae, crepitus), and systemic toxicity. Sterile inflammation would typically be resolving by day 3, not increasing. Allergic contact dermatitis would usually involve itching and a rash pattern related to the allergen. The main distractor, D (Sterile inflammation), is possible, but "increasing redness and warmth" suggests a progression beyond typical sterile inflammation, making cellulitis more likely.
Question 64
A 62-year-old female develops a chronic non-healing wound with exposed bone after surgical debridement for a deep infection following an open tibia fracture. The wound is clean but has persistent exudate. Which adjunctive therapy is most appropriate to promote wound healing and manage exudate?
View Answer & Explanation
Correct Answer: C
Rationale: Negative pressure wound therapy (NPWT) is highly effective for managing chronic, complex wounds with exposed bone and persistent exudate. It promotes granulation tissue formation, reduces edema, removes exudate, and increases local blood flow, thereby facilitating wound closure. Hyperbaric oxygen therapy is used for specific indications like osteomyelitis or compromised flaps. Topical silver sulfadiazine is primarily for burn wounds. Systemic antibiotics are for treating active infection, not primarily for wound healing in a clean wound. Wet-to-dry dressings are less efficient at managing exudate and promoting granulation than NPWT. The main distractor, E (Daily wet-to-dry dressings), is a traditional wound care method but is less effective and more labor-intensive than NPWT for complex, exudative wounds with exposed bone.
Question 65
A 48-year-old male develops septic shock secondary to a severe post-operative orthopaedic infection. He presents with hypotension, tachycardia, tachypnea, and altered mental status. Which of the following is a key component of the initial management of septic shock?
View Answer & Explanation
Correct Answer: B
Rationale: Aggressive fluid resuscitation with intravenous crystalloids is a cornerstone of initial management for septic shock to restore intravascular volume and improve tissue perfusion. While vasopressors may be needed if fluids are insufficient, they are not the sole initial treatment. Immediate surgical debridement is critical but should follow initial stabilization. High-dose corticosteroids are not routinely recommended for all septic shock patients. Delayed antibiotic administration significantly increases mortality; broad-spectrum antibiotics should be given within the first hour of recognition. The main distractor, A (Administration of vasopressors only), is incorrect because fluid resuscitation is the initial step to address hypovolemia before or in conjunction with vasopressors.
Question 66
A 70-year-old male with a history of multiple hospitalizations and prolonged antibiotic use develops a prosthetic joint infection caused by a carbapenem-resistant Enterobacteriaceae (CRE). This organism is classified as a multidrug-resistant organism (MD
Question 66
A 68-year-old male undergoes a total knee arthroplasty. He has a history of diabetes mellitus, obesity (BMI 35), and active smoking. Postoperatively, he develops fever, increasing knee pain, and purulent drainage from the incision. Radiographs show no acute changes in implant position. Which of the following is the MOST significant modifiable risk factor for iatrogenic infection in this patient?
View Answer & Explanation
Correct Answer: D
Rationale: Active smoking is a significant modifiable risk factor for surgical site infections, including periprosthetic joint infections. Smoking cessation, ideally several weeks prior to surgery, can significantly reduce this risk. While diabetes and obesity are also modifiable, smoking cessation often has a more immediate and profound impact on wound healing and infection risk. Age and the type of surgery are non-modifiable factors in this context.
Question 66
A 55-year-old female is scheduled for elective anterior cruciate ligament reconstruction. To minimize the risk of iatrogenic infection, which of the following prophylactic antibiotic regimens is generally recommended?
View Answer & Explanation
Correct Answer: C
Rationale: For most orthopaedic procedures, including ACL reconstruction, intravenous cefazolin (a first-generation cephalosporin) administered 30-60 minutes prior to skin incision is the recommended prophylactic antibiotic. This timing ensures adequate tissue levels at the time of incision. Vancomycin is typically reserved for patients with penicillin allergies or in settings with high MRSA prevalence. Oral antibiotics are generally not sufficient for surgical prophylaxis.
Question 66
A 42-year-old male is undergoing open reduction and internal fixation of a distal tibia fracture. Prior to incision, the surgical site is prepared. Which of the following skin preparation agents is generally considered superior for reducing the risk of iatrogenic surgical site infection?
View Answer & Explanation
Correct Answer: B
Rationale: Chlorhexidine gluconate (CHG) in an alcohol solution has demonstrated superior efficacy in reducing surgical site infections compared to povidone-iodine. CHG has a broader spectrum of activity, a faster kill time, and a longer residual effect. Povidone-iodine is still effective but generally considered less potent than CHG-alcohol. Alcohol alone has a rapid kill but no residual effect. Hydrogen peroxide and sterile saline are not primary surgical skin prep agents.
Question 66
During a total hip arthroplasty, a 72-year-old female patient experiences an iatrogenic surgical site infection. Which of the following intraoperative practices is MOST critical in minimizing the risk of such an infection?
View Answer & Explanation
Correct Answer: E
Rationale: While all listed options contribute to infection prevention, meticulous hemostasis and thorough wound irrigation are paramount intraoperatively. Hematoma formation provides an excellent culture medium, and retained devitalized tissue or foreign bodies can harbor bacteria. Prophylactic antibiotics (D) are critical but are pre-operative/intra-operative timing. Maintaining normothermia (A), laminar flow (B), and limiting traffic (C) are important environmental and systemic factors, but direct surgical technique regarding the wound itself is arguably the most critical intraoperative factor.
Question 66
A 60-year-old male develops a superficial surgical site infection following an elective carpal tunnel release. A wound culture is obtained. Which of the following organisms is the MOST common cause of iatrogenic surgical site infections in orthopaedic surgery?
View Answer & Explanation
Correct Answer: C
Rationale: Staphylococcus aureus, including both methicillin-sensitive (MSSA) and methicillin-resistant (MRSA) strains, is the most common pathogen responsible for surgical site infections and periprosthetic joint infections in orthopaedic surgery. Coagulase-negative Staphylococci (D) are also common, especially in implant-related infections, but S. aureus generally has a higher overall incidence and virulence in acute infections. Pseudomonas and E. coli are more common in specific scenarios (e.g., open fractures, genitourinary source). Candida is rare.
Question 66
A 70-year-old female presents with increasing pain, swelling, and warmth in her left knee 3 months after total knee arthroplasty. She has a low-grade fever. Radiographs show no loosening. Which of the following laboratory markers is typically MOST sensitive for diagnosing a periprosthetic joint infection?
View Answer & Explanation
Correct Answer: C
Rationale: C-reactive protein (CRP) is generally considered the most sensitive and rapidly responding inflammatory marker for diagnosing periprosthetic joint infections. It rises quickly with infection and falls quickly with successful treatment. ESR (B) is also sensitive but less specific and slower to respond. WBC (A) is often normal in chronic or low-grade infections. Procalcitonin (D) is useful for systemic sepsis but less specific for localized PJI. Blood cultures (E) are often negative in localized PJI.
Question 66
A 65-year-old male with a history of total hip arthroplasty 6 months prior presents with chronic groin pain and a draining sinus tract. Plain radiographs show no obvious loosening. To confirm the diagnosis of iatrogenic periprosthetic joint infection, which diagnostic study is considered the gold standard?
View Answer & Explanation
Correct Answer: C
Rationale: Aspiration of the joint for synovial fluid analysis (cell count, differential, and culture) is considered the gold standard for diagnosing periprosthetic joint infection. It provides direct evidence of infection and identifies the causative organism, guiding targeted antibiotic therapy. While ESR/CRP (D) are useful screening tools, they are not diagnostic. Imaging studies (A, B, E) can suggest infection but are not definitive for microbiological diagnosis.
Question 66
A 58-year-old female develops an acute periprosthetic joint infection (PJI) 3 weeks after total shoulder arthroplasty. Synovial fluid aspiration confirms methicillin-sensitive Staphylococcus aureus (MSSA). The implant is well-fixed. What is the MOST appropriate initial management strategy?
View Answer & Explanation
Correct Answer: B
Rationale: For acute PJI (typically within 3-6 weeks of surgery) with a well-fixed implant and susceptible organism, irrigation and debridement with implant retention (DAIR) combined with appropriate intravenous antibiotics is the preferred initial management. This approach aims to eradicate the infection while preserving the functional implant. Two-stage revision (C) is reserved for chronic infections or failed DAIR. One-stage revision (D) is less common for acute infections. Suppressive antibiotics (A) are for patients who cannot tolerate surgery or have chronic, incurable infections. Arthrodesis (E) is a salvage procedure.
Question 66
A 75-year-old male presents with chronic pain, swelling, and stiffness in his knee, 18 months after a total knee arthroplasty. ESR is 70 mm/hr and CRP is 45 mg/L. Joint aspiration reveals a high leukocyte count and positive culture for methicillin-resistant Staphylococcus epidermidis (MRSE). Radiographs show evidence of loosening. What is the MOST appropriate management strategy for this chronic iatrogenic PJI?
View Answer & Explanation
Correct Answer: C
Rationale: For chronic PJI (onset >3-6 weeks, often with implant loosening or resistant organisms), a two-stage revision arthroplasty is generally considered the gold standard. This involves removal of all implants, thorough debridement, placement of an antibiotic-loaded cement spacer, and a prolonged course of antibiotics, followed by reimplantation of new components once the infection is controlled. DAIR (A) is unlikely to be successful in chronic infections with loosening. One-stage revision (D) is less commonly performed for chronic infections due to higher failure rates. Suppressive antibiotics (B) are not curative. Amputation (E) is a last resort.
Question 66
A 30-year-old male develops a deep surgical site infection following open reduction and internal fixation of a tibia shaft fracture with an intramedullary nail. Cultures grow Pseudomonas aeruginosa. The fracture is healed, and the patient has completed a 6-week course of appropriate intravenous antibiotics, but inflammatory markers remain elevated. What is the MOST appropriate next step in managing this iatrogenic infection?
View Answer & Explanation
Correct Answer: C
Rationale: In cases of hardware-related infection where the fracture is healed, and despite appropriate antibiotic therapy, the infection persists (indicated by elevated inflammatory markers), removal of the hardware is often necessary to eradicate the biofilm and achieve infection control. Biofilm on implants makes complete eradication with antibiotics alone very difficult. Continuing antibiotics (A, B) without addressing the hardware is unlikely to be curative. Repeat debridement with retention (D) is less likely to succeed if the initial course failed and the fracture is healed. Hyperbaric oxygen (E) is an adjunctive therapy, not a primary treatment for persistent hardware infection.
Question 66
A 48-year-old recreational runner receives an intra-articular corticosteroid injection for knee osteoarthritis. One week later, he develops severe knee pain, swelling, warmth, and inability to bear weight. Aspiration reveals purulent fluid with a high leukocyte count. This iatrogenic infection is most likely due to:
View Answer & Explanation
Correct Answer: B
Rationale: Septic arthritis following an intra-articular injection is an iatrogenic infection almost always caused by direct contamination of the joint during the injection procedure. This can be due to inadequate skin preparation, non-sterile technique, or contaminated injectate. While corticosteroids can cause some local immunosuppression (D), the primary mechanism for acute septic arthritis post-injection is direct bacterial inoculation. Systemic bacteremia (A) is less common as a direct cause of post-injection septic arthritis. Reactivation of latent infection (C) is rare. Allergic reactions (E) would present differently.
Question 66
A 62-year-old male undergoes a femoral nerve block prior to knee arthroscopy. Two days later, he develops localized pain, redness, and swelling at the injection site, along with a fever. Imaging reveals a collection consistent with an abscess. Which of the following is the MOST important step to prevent such iatrogenic infections during regional anesthesia?
View Answer & Explanation
Correct Answer: B
Rationale: Strict aseptic technique, including thorough skin preparation, sterile gloves, and drapes, is the single most important measure to prevent iatrogenic infections associated with regional nerve blocks. While ultrasound guidance (A) can improve accuracy and reduce complications like nerve injury, it does not directly prevent infection if aseptic technique is compromised. Prophylactic antibiotics (C) are generally not indicated for routine nerve blocks. Limiting anesthetic volume (D) is not directly related to infection prevention. Performing the block in a dedicated room (E) is good practice but secondary to aseptic technique.
Question 66
A 25-year-old male is treated with an external fixator for an open tibia fracture. Three weeks post-application, he develops erythema, purulent drainage, and pain around one of the pin sites. Radiographs show no osteolysis around the pin. What is the MOST appropriate initial management for this iatrogenic pin tract infection?
View Answer & Explanation
Correct Answer: B
Rationale: For superficial pin tract infections without evidence of osteolysis or deep infection, initial management typically involves oral antibiotics (guided by culture if available, otherwise empiric for skin flora) and meticulous local wound care, including daily cleaning and dressing changes. Removal of the fixator (A) is premature unless the infection is severe or deep. Intravenous antibiotics and debridement (C) are for more severe or deep infections. Pin exchange (D) or antibiotic beads (E) are for more refractory or osteomyelitic infections.
Question 66
A 50-year-old female undergoes a lumbar microdiscectomy for a herniated disc. Two weeks postoperatively, she develops severe back pain, fever, and elevated inflammatory markers. MRI shows disc space inflammation and fluid collection. This iatrogenic infection, likely discitis, is most commonly caused by which pathogen?
View Answer & Explanation
Correct Answer: B
Rationale: Staphylococcus aureus is the most common pathogen causing iatrogenic discitis and vertebral osteomyelitis following spinal surgery. While coagulase-negative Staphylococci (D) and Propionibacterium acnes (E) can be involved, especially in more indolent or delayed infections, S. aureus is the predominant cause of acute, symptomatic post-surgical spinal infections. Streptococcus pneumoniae (A) and Enterococcus faecalis (C) are less common in this context.
Question 66
A 35-year-old male sustains a Gustilo-Anderson Type IIIA open tibia fracture. He undergoes emergent irrigation and debridement and intramedullary nailing. To reduce the risk of iatrogenic infection, which of the following is the MOST critical factor in the initial management?
View Answer & Explanation
Correct Answer: A
Rationale: For open fractures, the early administration of broad-spectrum intravenous antibiotics (within 3 hours of injury) is the single most critical factor in reducing the risk of iatrogenic infection. This helps to prevent bacterial proliferation in contaminated tissues. While thorough debridement is also crucial, antibiotics are a systemic measure. Primary wound closure (B) is often avoided in open fractures to allow for drainage and prevent compartment syndrome. Antibiotic cement (C) and NPWT (D) are adjunctive. Delayed definitive fixation (E) is not generally preferred if immediate fixation is feasible and safe.
Question 66
A 68-year-old female develops a chronic periprosthetic joint infection (PJI) 1 year after total hip arthroplasty. Despite multiple courses of antibiotics, the infection persists. This persistence is largely attributed to the formation of bacterial biofilms on the implant surface. Which characteristic of biofilm makes it particularly challenging to treat?
View Answer & Explanation
Correct Answer: C
Rationale: Biofilms are communities of bacteria encased in an extracellular polymeric substance (EPS) matrix. This matrix acts as a physical barrier, significantly reducing the penetration and efficacy of antibiotics, making bacteria within biofilms up to 1000 times more resistant to antibiotics than planktonic bacteria. Bacteria within biofilms also have reduced metabolic activity (A), making them less susceptible to antibiotics that target active growth. Biofilms also evade host immune defenses (B) and are formed by both Gram-positive and Gram-negative bacteria (E). While bacteria can disseminate (D), the primary challenge is local eradication.
Question 66
A 40-year-old male develops a surgical site infection following internal fixation of a calcaneus fracture. Wound cultures grow Methicillin-resistant Staphylococcus aureus (MRSA). Which of the following antibiotics is a first-line agent for treating MRSA iatrogenic infections in orthopaedics?
View Answer & Explanation
Correct Answer: C
Rationale: Vancomycin is the cornerstone and first-line intravenous antibiotic for treating confirmed or suspected MRSA infections in orthopaedics. Cefazolin (A) is a first-generation cephalosporin and is ineffective against MRSA. Piperacillin-tazobactam (B) has broad-spectrum activity but is not typically first-line for MRSA. Ciprofloxacin (D) is a fluoroquinolone, which may have some MRSA activity but is not preferred first-line. Clindamycin (E) can be used for some MRSA strains but requires D-test to confirm susceptibility and is generally not first-line for serious infections.
Question 66
A 55-year-old immunocompromised patient develops a persistent periprosthetic joint infection after total knee arthroplasty, despite multiple debridements and broad-spectrum antibacterial antibiotics. Fungal cultures from synovial fluid eventually grow Candida albicans. What is the MOST appropriate initial treatment for this iatrogenic fungal PJI?
View Answer & Explanation
Correct Answer: C
Rationale: Fungal periprosthetic joint infections are notoriously difficult to treat and typically require aggressive surgical management combined with prolonged systemic antifungal therapy. A two-stage revision arthroplasty, similar to chronic bacterial PJI, is generally recommended, involving removal of all hardware, thorough debridement, and systemic antifungals (e.g., fluconazole, echinocandins, or amphotericin B depending on species and severity). Implant retention (B) is rarely successful for fungal PJI. Continuing antibacterial antibiotics (A, D) is ineffective. Amphotericin B (E) is a potent antifungal but usually part of a broader strategy, not used alone, and often has significant side effects.
Question 66
A 60-year-old female presents 5 days after total hip arthroplasty with localized redness, warmth, and mild tenderness around the incision. Her temperature is 37.8°C (100.0°F), and WBC count is 9,500/µL. There is no purulent drainage. Radiographs are unremarkable. What is the MOST likely diagnosis?
View Answer & Explanation
Correct Answer: B
Rationale: The clinical presentation of localized redness, warmth, mild tenderness, low-grade fever, and normal WBC count without purulent drainage or systemic signs of severe infection is most consistent with superficial cellulitis, a type of superficial surgical site infection. Deep PJI (A) would typically present with more severe pain, higher fever, and often purulent drainage or systemic signs. Hematoma (C) would cause swelling and ecchymosis but typically not significant warmth or fever. Allergic reaction (D) is possible but less common and usually presents with itching and rash. Aseptic loosening (E) would not occur this early post-op and would not present with acute inflammatory signs.
Question 66
A 70-year-old male develops a complex, recurrent periprosthetic joint infection of the knee, requiring multiple surgical interventions and prolonged antibiotic courses. To optimize his care and improve outcomes, which of the following approaches is MOST beneficial in managing such a challenging iatrogenic infection?
View Answer & Explanation
Correct Answer: C
Rationale: Complex and recurrent periprosthetic joint infections are best managed with a multidisciplinary team approach. This typically involves orthopaedic surgeons (for surgical debridement, revision), infectious disease specialists (for antibiotic selection, duration, and monitoring), and often plastic surgeons (for soft tissue coverage), as well as physical therapists and social workers. This collaborative approach ensures comprehensive care, optimizes treatment strategies, and improves patient outcomes. Relying solely on a primary care physician (A) or a single surgeon (B) is insufficient for complex cases. While imaging (D) is important, it's part of a larger strategy. Amputation (E) is a last resort.
Question 67
A 68-year-old male undergoes a total knee arthroplasty. He has a history of diabetes mellitus, obesity (BMI 35), and active smoking. Postoperatively, he develops fever, increasing knee pain, and purulent drainage from the incision. Radiographs show no acute changes in implant position. Which of the following is the MOST significant modifiable risk factor for iatrogenic infection in this patient?
View Answer & Explanation
Correct Answer: D
Rationale: Active smoking is a significant modifiable risk factor for surgical site infections, including periprosthetic joint infections. Smoking cessation, ideally several weeks prior to surgery, can significantly reduce this risk. While diabetes and obesity are also modifiable, smoking cessation often has a more immediate and profound impact on wound healing and infection risk. Age and the type of surgery are non-modifiable factors in this context.
Question 68
A 55-year-old female is scheduled for elective anterior cruciate ligament reconstruction. To minimize the risk of iatrogenic infection, which of the following prophylactic antibiotic regimens is generally recommended?
View Answer & Explanation
Correct Answer: C
Rationale: For most orthopaedic procedures, including ACL reconstruction, intravenous cefazolin (a first-generation cephalosporin) administered 30-60 minutes prior to skin incision is the recommended prophylactic antibiotic. This timing ensures adequate tissue levels at the time of incision. Vancomycin is typically reserved for patients with penicillin allergies or in settings with high MRSA prevalence. Oral antibiotics are generally not sufficient for surgical prophylaxis.
Question 69
A 42-year-old male is undergoing open reduction and internal fixation of a distal tibia fracture. Prior to incision, the surgical site is prepared. Which of the following skin preparation agents is generally considered superior for reducing the risk of iatrogenic surgical site infection?
View Answer & Explanation
Correct Answer: B
Rationale: Chlorhexidine gluconate (CHG) in an alcohol solution has demonstrated superior efficacy in reducing surgical site infections compared to povidone-iodine. CHG has a broader spectrum of activity, a faster kill time, and a longer residual effect. Povidone-iodine is still effective but generally considered less potent than CHG-alcohol. Alcohol alone has a rapid kill but no residual effect. Hydrogen peroxide and sterile saline are not primary surgical skin prep agents.
Question 70
During a total hip arthroplasty, a 72-year-old female patient experiences an iatrogenic surgical site infection. Which of the following intraoperative practices is MOST critical in minimizing the risk of such an infection?
View Answer & Explanation
Correct Answer: E
Rationale: While all listed options contribute to infection prevention, meticulous hemostasis and thorough wound irrigation are paramount intraoperatively. Hematoma formation provides an excellent culture medium, and retained devitalized tissue or foreign bodies can harbor bacteria. Prophylactic antibiotics (D) are critical but are pre-operative/intra-operative timing. Maintaining normothermia (A), laminar flow (B), and limiting traffic (C) are important environmental and systemic factors, but direct surgical technique regarding the wound itself is arguably the most critical intraoperative factor.
Question 71
A 60-year-old male develops a superficial surgical site infection following an elective carpal tunnel release. A wound culture is obtained. Which of the following organisms is the MOST common cause of iatrogenic surgical site infections in orthopaedic surgery?
View Answer & Explanation
Correct Answer: C
Rationale: Staphylococcus aureus, including both methicillin-sensitive (MSSA) and methicillin-resistant (MRSA) strains, is the most common pathogen responsible for surgical site infections and periprosthetic joint infections in orthopaedic surgery. Coagulase-negative Staphylococci (D) are also common, especially in implant-related infections, but S. aureus generally has a higher overall incidence and virulence in acute infections. Pseudomonas and E. coli are more common in specific scenarios (e.g., open fractures, genitourinary source). Candida is rare.
Question 72
A 70-year-old female presents with increasing pain, swelling, and warmth in her left knee 3 months after total knee arthroplasty. She has a low-grade fever. Radiographs show no loosening. Which of the following laboratory markers is typically MOST sensitive for diagnosing a periprosthetic joint infection?
View Answer & Explanation
Correct Answer: C
Rationale: C-reactive protein (CRP) is generally considered the most sensitive and rapidly responding inflammatory marker for diagnosing periprosthetic joint infections. It rises quickly with infection and falls quickly with successful treatment. ESR (B) is also sensitive but less specific and slower to respond. WBC (A) is often normal in chronic or low-grade infections. Procalcitonin (D) is useful for systemic sepsis but less specific for localized PJI. Blood cultures (E) are often negative in localized PJI.
Question 73
A 65-year-old male with a history of total hip arthroplasty 6 months prior presents with chronic groin pain and a draining sinus tract. Plain radiographs show no obvious loosening. To confirm the diagnosis of iatrogenic periprosthetic joint infection, which diagnostic study is considered the gold standard?
View Answer & Explanation
Correct Answer: C
Rationale: Aspiration of the joint for synovial fluid analysis (cell count, differential, and culture) is considered the gold standard for diagnosing periprosthetic joint infection. It provides direct evidence of infection and identifies the causative organism, guiding targeted antibiotic therapy. While ESR/CRP (D) are useful screening tools, they are not diagnostic. Imaging studies (A, B, E) can suggest infection but are not definitive for microbiological diagnosis.
Question 74
A 58-year-old female develops an acute periprosthetic joint infection (PJI) 3 weeks after total shoulder arthroplasty. Synovial fluid aspiration confirms methicillin-sensitive Staphylococcus aureus (MSSA). The implant is well-fixed. What is the MOST appropriate initial management strategy?
View Answer & Explanation
Correct Answer: B
Rationale: For acute PJI (typically within 3-6 weeks of surgery) with a well-fixed implant and susceptible organism, irrigation and debridement with implant retention (DAIR) combined with appropriate intravenous antibiotics is the preferred initial management. This approach aims to eradicate the infection while preserving the functional implant. Two-stage revision (C) is reserved for chronic infections or failed DAIR. One-stage revision (D) is less common for acute infections. Suppressive antibiotics (A) are for patients who cannot tolerate surgery or have chronic, incurable infections. Arthrodesis (E) is a salvage procedure.
Question 75
A 75-year-old male presents with chronic pain, swelling, and stiffness in his knee, 18 months after a total knee arthroplasty. ESR is 70 mm/hr and CRP is 45 mg/L. Joint aspiration reveals a high leukocyte count and positive culture for methicillin-resistant Staphylococcus epidermidis (MRSE). Radiographs show evidence of loosening. What is the MOST appropriate management strategy for this chronic iatrogenic PJI?
View Answer & Explanation
Correct Answer: C
Rationale: For chronic PJI (onset >3-6 weeks, often with implant loosening or resistant organisms), a two-stage revision arthroplasty is generally considered the gold standard. This involves removal of all implants, thorough debridement, placement of an antibiotic-loaded cement spacer, and a prolonged course of antibiotics, followed by reimplantation of new components once the infection is controlled. DAIR (A) is unlikely to be successful in chronic infections with loosening. One-stage revision (D) is less commonly performed for chronic infections due to higher failure rates. Suppressive antibiotics (B) are not curative. Amputation (E) is a last resort.
Question 76
A 30-year-old male develops a deep surgical site infection following open reduction and internal fixation of a tibia shaft fracture with an intramedullary nail. Cultures grow Pseudomonas aeruginosa. The fracture is healed, and the patient has completed a 6-week course of appropriate intravenous antibiotics, but inflammatory markers remain elevated. What is the MOST appropriate next step in managing this iatrogenic infection?
View Answer & Explanation
Correct Answer: C
Rationale: In cases of hardware-related infection where the fracture is healed, and despite appropriate antibiotic therapy, the infection persists (indicated by elevated inflammatory markers), removal of the hardware is often necessary to eradicate the biofilm and achieve infection control. Biofilm on implants makes complete eradication with antibiotics alone very difficult. Continuing antibiotics (A, B) without addressing the hardware is unlikely to be curative. Repeat debridement with retention (D) is less likely to succeed if the initial course failed and the fracture is healed. Hyperbaric oxygen (E) is an adjunctive therapy, not a primary treatment for persistent hardware infection.
Question 77
A 48-year-old recreational runner receives an intra-articular corticosteroid injection for knee osteoarthritis. One week later, he develops severe knee pain, swelling, warmth, and inability to bear weight. Aspiration reveals purulent fluid with a high leukocyte count. This iatrogenic infection is most likely due to:
View Answer & Explanation
Correct Answer: B
Rationale: Septic arthritis following an intra-articular injection is an iatrogenic infection almost always caused by direct contamination of the joint during the injection procedure. This can be due to inadequate skin preparation, non-sterile technique, or contaminated injectate. While corticosteroids can cause some local immunosuppression (D), the primary mechanism for acute septic arthritis post-injection is direct bacterial inoculation. Systemic bacteremia (A) is less common as a direct cause of post-injection septic arthritis. Reactivation of latent infection (C) is rare. Allergic reactions (E) would present differently.
Question 78
A 62-year-old male undergoes a femoral nerve block prior to knee arthroscopy. Two days later, he develops localized pain, redness, and swelling at the injection site, along with a fever. Imaging reveals a collection consistent with an abscess. Which of the following is the MOST important step to prevent such iatrogenic infections during regional anesthesia?
View Answer & Explanation
Correct Answer: B
Rationale: Strict aseptic technique, including thorough skin preparation, sterile gloves, and drapes, is the single most important measure to prevent iatrogenic infections associated with regional nerve blocks. While ultrasound guidance (A) can improve accuracy and reduce complications like nerve injury, it does not directly prevent infection if aseptic technique is compromised. Prophylactic antibiotics (C) are generally not indicated for routine nerve blocks. Limiting anesthetic volume (D) is not directly related to infection prevention. Performing the block in a dedicated room (E) is good practice but secondary to aseptic technique.
Question 79
A 25-year-old male is treated with an external fixator for an open tibia fracture. Three weeks post-application, he develops erythema, purulent drainage, and pain around one of the pin sites. Radiographs show no osteolysis around the pin. What is the MOST appropriate initial management for this iatrogenic pin tract infection?
View Answer & Explanation
Correct Answer: B
Rationale: For superficial pin tract infections without evidence of osteolysis or deep infection, initial management typically involves oral antibiotics (guided by culture if available, otherwise empiric for skin flora) and meticulous local wound care, including daily cleaning and dressing changes. Removal of the fixator (A) is premature unless the infection is severe or deep. Intravenous antibiotics and debridement (C) are for more severe or deep infections. Pin exchange (D) or antibiotic beads (E) are for more refractory or osteomyelitic infections.
Question 80
A 50-year-old female undergoes a lumbar microdiscectomy for a herniated disc. Two weeks postoperatively, she develops severe back pain, fever, and elevated inflammatory markers. MRI shows disc space inflammation and fluid collection. This iatrogenic infection, likely discitis, is most commonly caused by which pathogen?
View Answer & Explanation
Correct Answer: B
Rationale: Staphylococcus aureus is the most common pathogen causing iatrogenic discitis and vertebral osteomyelitis following spinal surgery. While coagulase-negative Staphylococci (D) and Propionibacterium acnes (E) can be involved, especially in more indolent or delayed infections, S. aureus is the predominant cause of acute, symptomatic post-surgical spinal infections. Streptococcus pneumoniae (A) and Enterococcus faecalis (C) are less common in this context.
Question 81
A 35-year-old male sustains a Gustilo-Anderson Type IIIA open tibia fracture. He undergoes emergent irrigation and debridement and intramedullary nailing. To reduce the risk of iatrogenic infection, which of the following is the MOST critical factor in the initial management?
View Answer & Explanation
Correct Answer: A
Rationale: For open fractures, the early administration of broad-spectrum intravenous antibiotics (within 3 hours of injury) is the single most critical factor in reducing the risk of iatrogenic infection. This helps to prevent bacterial proliferation in contaminated tissues. While thorough debridement is also crucial, antibiotics are a systemic measure. Primary wound closure (B) is often avoided in open fractures to allow for drainage and prevent compartment syndrome. Antibiotic cement (C) and NPWT (D) are adjunctive. Delayed definitive fixation (E) is not generally preferred if immediate fixation is feasible and safe.
Question 82
A 68-year-old female develops a chronic periprosthetic joint infection (PJI) 1 year after total hip arthroplasty. Despite multiple courses of antibiotics, the infection persists. This persistence is largely attributed to the formation of bacterial biofilms on the implant surface. Which characteristic of biofilm makes it particularly challenging to treat?
View Answer & Explanation
Correct Answer: C
Rationale: Biofilms are communities of bacteria encased in an extracellular polymeric substance (EPS) matrix. This matrix acts as a physical barrier, significantly reducing the penetration and efficacy of antibiotics, making bacteria within biofilms up to 1000 times more resistant to antibiotics than planktonic bacteria. Bacteria within biofilms also have reduced metabolic activity (A), making them less susceptible to antibiotics that target active growth. Biofilms also evade host immune defenses (B) and are formed by both Gram-positive and Gram-negative bacteria (E). While bacteria can disseminate (D), the primary challenge is local eradication.
Question 83
A 40-year-old male develops a surgical site infection following internal fixation of a calcaneus fracture. Wound cultures grow Methicillin-resistant Staphylococcus aureus (MRSA). Which of the following antibiotics is a first-line agent for treating MRSA iatrogenic infections in orthopaedics?
View Answer & Explanation
Correct Answer: C
Rationale: Vancomycin is the cornerstone and first-line intravenous antibiotic for treating confirmed or suspected MRSA infections in orthopaedics. Cefazolin (A) is a first-generation cephalosporin and is ineffective against MRSA. Piperacillin-tazobactam (B) has broad-spectrum activity but is not typically first-line for MRSA. Ciprofloxacin (D) is a fluoroquinolone, which may have some MRSA activity but is not preferred first-line. Clindamycin (E) can be used for some MRSA strains but requires D-test to confirm susceptibility and is generally not first-line for serious infections.
Question 84
A 55-year-old immunocompromised patient develops a persistent periprosthetic joint infection after total knee arthroplasty, despite multiple debridements and broad-spectrum antibacterial antibiotics. Fungal cultures from synovial fluid eventually grow Candida albicans. What is the MOST appropriate initial treatment for this iatrogenic fungal PJI?
View Answer & Explanation
Correct Answer: C
Rationale: Fungal periprosthetic joint infections are notoriously difficult to treat and typically require aggressive surgical management combined with prolonged systemic antifungal therapy. A two-stage revision arthroplasty, similar to chronic bacterial PJI, is generally recommended, involving removal of all hardware, thorough debridement, and systemic antifungals (e.g., fluconazole, echinocandins, or amphotericin B depending on species and severity). Implant retention (B) is rarely successful for fungal PJI. Continuing antibacterial antibiotics (A, D) is ineffective. Amphotericin B (E) is a potent antifungal but usually part of a broader strategy, not used alone, and often has significant side effects.
Question 85
A 60-year-old female presents 5 days after total hip arthroplasty with localized redness, warmth, and mild tenderness around the incision. Her temperature is 37.8°C (100.0°F), and WBC count is 9,500/µL. There is no purulent drainage. Radiographs are unremarkable. What is the MOST likely diagnosis?
View Answer & Explanation
Correct Answer: B
Rationale: The clinical presentation of localized redness, warmth, mild tenderness, low-grade fever, and normal WBC count without purulent drainage or systemic signs of severe infection is most consistent with superficial cellulitis, a type of superficial surgical site infection. Deep PJI (A) would typically present with more severe pain, higher fever, and often purulent drainage or systemic signs. Hematoma (C) would cause swelling and ecchymosis but typically not significant warmth or fever. Allergic reaction (D) is possible but less common and usually presents with itching and rash. Aseptic loosening (E) would not occur this early post-op and would not present with acute inflammatory signs.
Question 86
A 45-year-old female presents with diffuse bone pain and muscle weakness. A bone biopsy is performed to investigate the underlying pathology.
View Answer & Explanation
Correct Answer: C
Rationale: The image (Fig. 7.41) and accompanying text explicitly state that osteomalacia is characterized by an increased amount of nonmineralized osteoid (orange) covering the normal mineralized trabeculae (green) on trichrome stain. This reflects the fundamental defect in mineralization.
Main Distractor Rationale: Option A, increased bone resorption, is characteristic of osteoporosis, where bone mass is reduced, but the remaining bone is normally mineralized. Osteomalacia's primary defect is in the quality of mineralization, not primarily the quantity of bone removed.
Question 87
A 3-year-old boy is brought to the clinic by his parents due to progressive bowing of his legs and difficulty walking. On examination, he has a prominent forehead and a cubical-shaped skull.
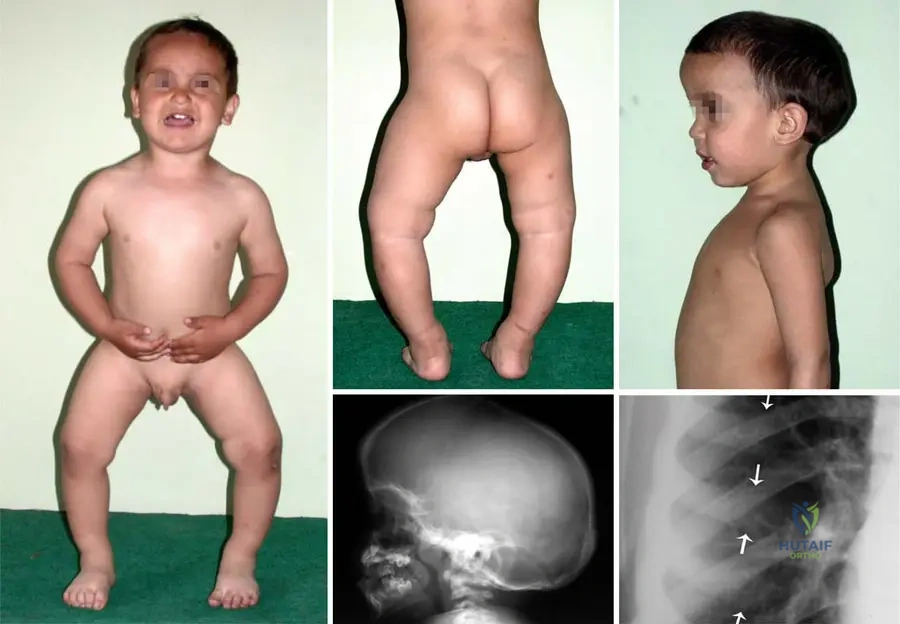
View Answer & Explanation
Correct Answer: C
Rationale: The clinical presentation of bowing of legs, difficulty walking (delayed milestones), and a cubical skull ("caput quadratum") are classic characteristics of rickets in children, as described and depicted in Fig. 7.32 a–e.
Main Distractor Rationale: Option A, osteogenesis imperfecta, is characterized by brittle bones and recurrent fractures, often with blue sclera, but typically does not present with the specific skull deformity or bowing of legs as the primary manifestation of a mineralization defect.
Question 88
A 2-year-old girl presents with a waddling gait and bilateral genu varum. Radiographs of her knees are obtained.
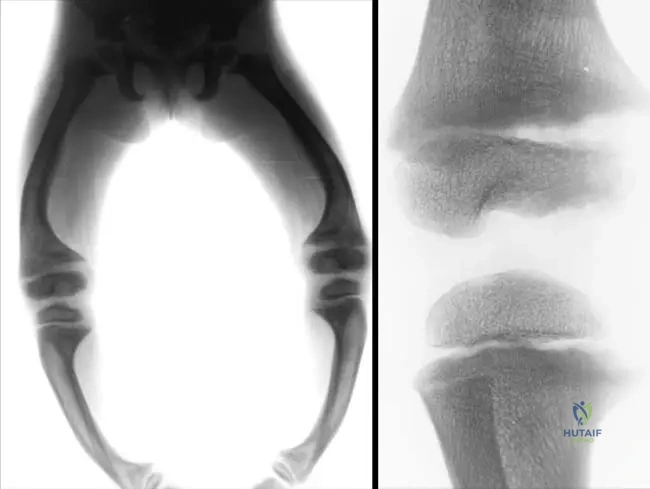
View Answer & Explanation
Correct Answer: C
Rationale: The image (Fig. 7.33 a, b) and text describe rickets in the knee as demonstrating diffuse osteopenia, an "O" curvature (varus deformation), and specifically, widened growth plates that protrude into the soft and weakened metaphyseal region.
Main Distractor Rationale: Option A, premature physeal closure, is not characteristic of rickets; instead, the growth plates remain open and are abnormally widened and irregular due to the mineralization defect.
Question 89
A 1-year-old boy presents with delayed walking and wrist deformities. Radiographs of his wrists are performed.
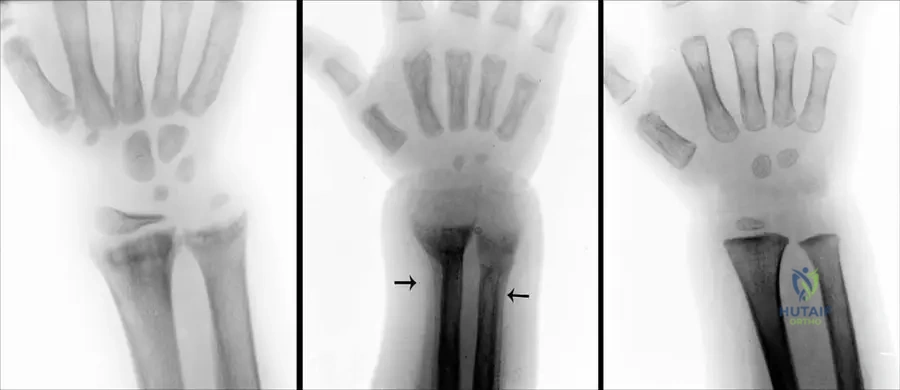
View Answer & Explanation
Correct Answer: B
Rationale: The image (Fig. 7.34 a–c) and its caption clearly illustrate and describe the characteristic radiological appearance of rickets at the wrist, which includes an enlarged and widened growth plate with cupping and fraying of the metaphyseal region.
Main Distractor Rationale: Option A, subperiosteal new bone formation, is more commonly associated with conditions like scurvy, trauma, or infection, rather than the primary mineralization defect seen in rickets.
Question 90
A 78-year-old female presents with increasing back pain, loss of height, and difficulty with ambulation due to generalized weakness. On examination, she exhibits marked kyphosis and a bulging abdomen.
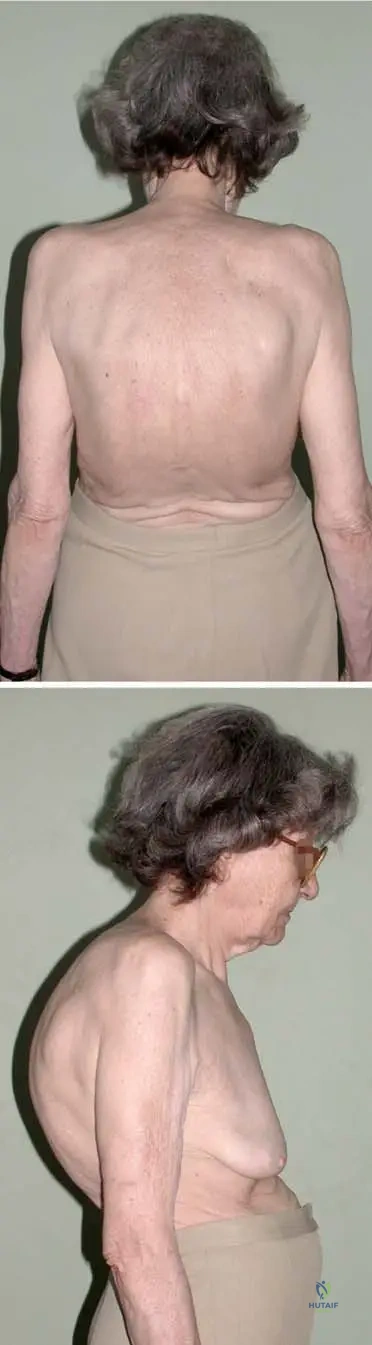
View Answer & Explanation
Correct Answer: C
Rationale: The image (Fig. 7.36 a, b) and its caption explicitly identify this clinical presentation (loss of height, kyphosis, bulging abdomen) in an elderly female as characteristic of osteoporomalacia, which is the co-occurrence of osteomalacia and osteoporosis.
Main Distractor Rationale: Option A, senile osteoporosis, can cause kyphosis and height loss. However, the term "osteoporomalacia" is more precise given the context of the teaching case, indicating the combined presence of both conditions, which is often seen in osteomalacia in adults.
Question 91
A 65-year-old male with a history of chronic malabsorption presents with severe, diffuse back pain. Radiographs of his lumbar spine are obtained.
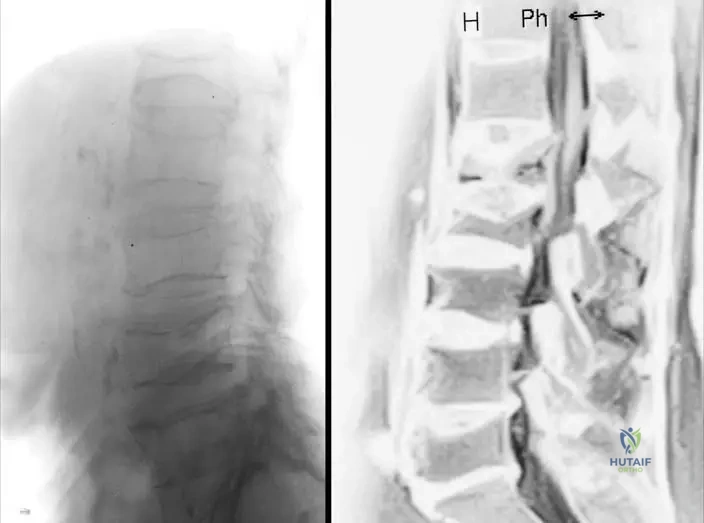
View Answer & Explanation
Correct Answer: C
Rationale: The image (Fig. 7.40 a, b) and its description state that radiographs of the lumbar vertebral column in patients with osteomalacia demonstrate fractures, biconcave vertebral bodies, and that the trabeculae appear indistinct or blurred with evidence of bone softening and bowing of the endplates.
Main Distractor Rationale: Option A, increased bone density, is incorrect. Osteomalacia is characterized by insufficient mineralization, leading to reduced bone density (osteopenia) and softening, not increased density.
Question 92
A 55-year-old female with a history of bariatric surgery presents to the emergency department after a low-energy fall, complaining of severe groin pain. An AP radiograph of the pelvis is performed.
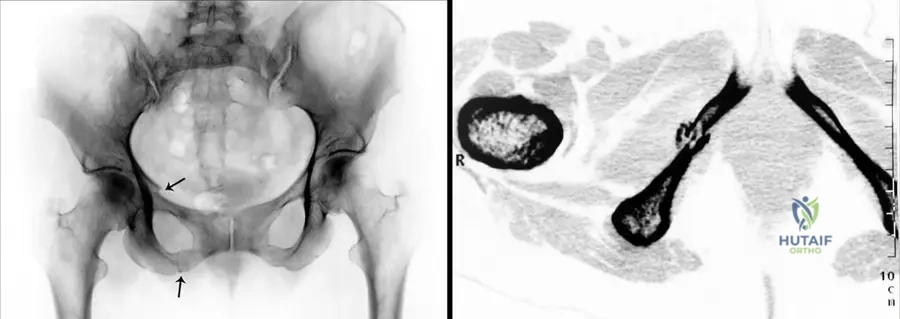
View Answer & Explanation
Correct Answer: B
Rationale: The image (Fig. 7.39 a, b) and its caption explicitly state, "Fracture of right pubic bone (arrows) because of the weakened pelvic ring in a patient with osteoporomalacia." This indicates a pathological fracture resulting from the underlying bone softening and fragility due to osteomalacia (often combined with osteoporosis).
Main Distractor Rationale: Option A, stress fracture from overuse, is less likely to be the primary cause in a patient with known osteoporomalacia, where generalized bone weakening is the predominant factor, even with low-energy trauma.
Question 93
A 4-year-old child from a low-income family presents with bowed legs and delayed motor milestones. Laboratory tests are ordered.
View Answer & Explanation
Correct Answer: C
Rationale: The text explicitly states, "Usually, this is caused by a deficiency of vitamin D, which reduces bone formation by altering calcium and phosphorus metabolism." This makes vitamin D deficiency the most common underlying cause of rickets.
Main Distractor Rationale: Option B, insufficient dietary calcium intake, can contribute to bone health issues, but vitamin D deficiency is the primary driver of the mineralization defect in most cases of rickets/
Question 93
A 45-year-old female presents with diffuse bone pain and easy fatigability. A bone biopsy is performed to investigate the underlying pathology. Histological examination reveals an increased amount of nonmineralized osteoid covering the normal mineralized trabeculae.

View Answer & Explanation
Correct Answer: C
Rationale: The clinical presentation of diffuse bone pain and easy fatigability in an adult, combined with the histological finding of increased nonmineralized osteoid covering mineralized trabeculae, is pathognomonic for osteomalacia. This condition is characterized by insufficient mineralization of bone matrix. Main Distractor Rationale: Osteoporosis is characterized by a reduction in bone mass and microarchitectural deterioration, but the mineralization of the remaining bone is normal. Histologically, there would not be an excess of unmineralized osteoid.
Question 93
A 78-year-old female presents with progressive loss of height, increasing kyphosis, and a bulging abdomen. She reports generalized malaise and diffuse bone pain that has worsened over the past year. Radiographs show biconcave vertebral bodies and indistinct trabeculae.

View Answer & Explanation
Correct Answer: C
Rationale: The patient's age, loss of height, kyphosis, malaise, diffuse bone pain, and radiographic findings of biconcave vertebral bodies and indistinct trabeculae are characteristic of osteomalacia. The term "osteoporomalacia" is used when osteomalacia and osteoporosis coexist, which is common in elderly patients presenting with these symptoms and signs. Main Distractor Rationale: While senile osteoporosis can cause loss of height and kyphosis due to vertebral compression fractures, the diffuse bone pain, malaise, and specific radiographic findings of indistinct trabeculae and biconcave vertebral bodies (suggesting bone softening) point more strongly towards osteomalacia, often coexisting with osteoporosis in this age group.
Question 93
A 2-year-old boy is brought to the clinic by his parents due to progressive bowing of his legs and difficulty walking. Physical examination reveals an "O" curvature of the lower limbs. An AP radiograph of the knee is obtained.

View Answer & Explanation
Correct Answer: B
Rationale: In rickets, which is osteomalacia in children, the characteristic radiographic findings at the knee include diffuse osteopenia, an "O" curvature (varus deformation), and importantly, widened growth plates that protrude into the soft and weakened metaphyseal region. This reflects the impaired mineralization of cartilage at the growth plate. Main Distractor Rationale: Normal growth plates with metaphyseal sclerosis would indicate a different pathology, such as osteopetrosis or a healing fracture, and is not consistent with the clinical presentation or typical radiographic findings of rickets.
Question 93
A 1-year-old girl presents with delayed walking and knobby enlargements at the ends of her long bones. Radiographs of the wrist are obtained to evaluate her skeletal development.

View Answer & Explanation
Correct Answer: B
Rationale: The characteristic radiological appearance of rickets at the wrist includes enlarged and widened growth plates and metaphyses, with cupping and fraying of the metaphyseal region. These findings are due to the impaired mineralization of the growing cartilage and bone. Main Distractor Rationale: Sclerotic metaphyses with normal growth plates are not characteristic of rickets; rickets involves impaired mineralization leading to lucency and disorganization, not sclerosis.
Question 93
A 35-year-old male presents with chronic, diffuse musculoskeletal pain and muscle weakness. Laboratory tests reveal low serum calcium and phosphate levels, with elevated alkaline phosphatase. A bone biopsy confirms osteomalacia.
View Answer & Explanation
Correct Answer: B
Rationale: Osteomalacia is fundamentally a disease characterized by insufficient mineralization of the osteoid (unmineralized bone matrix). This leads to the accumulation of soft, unmineralized bone, resulting in bone softening and pain. Main Distractor Rationale: Excessive bone resorption by osteoclasts is characteristic of conditions like osteoporosis or hyperparathyroidism, where bone mass is lost, but the remaining bone is typically well-mineralized. This is distinct from the mineralization defect seen in osteomalacia.
Question 93
A 9-month-old infant is noted by the pediatrician to have a disproportionately large head with a flattened occiput and prominent frontal bossing. The child also exhibits delayed motor milestones. These skull findings are clinically referred to as:
View Answer & Explanation
Correct Answer: C
Rationale: The description of a cubical skull, often with prominent frontal bossing, in a child with delayed motor milestones and other signs of rickets, is specifically referred to as "caput quadratum." This is a characteristic feature of rickets. Main Distractor Rationale: Plagiocephaly refers to an asymmetrical flattening of the skull, often due to positional molding, and does not specifically describe the cubical shape or frontal bossing associated with rickets.
Question 93
A 1-year-old child presents with a history of delayed crawling and walking. On physical examination, the pediatrician notes palpable, knobby enlargements at the costochondral junctions of the ribs, often described as a "rachitic rosary." This finding is indicative of:
View Answer & Explanation
Correct Answer: C
Rationale: The presence of knobby enlargements at the rib-breastbone joint (costochondral junctions), known as a "rachitic rosary," is a classic clinical sign of rickets. This, along with delayed motor milestones, strongly points to rickets. Main Distractor Rationale: Scurvy can cause bone pain and subperiosteal hemorrhages, but the "rachitic rosary" is not a characteristic feature of scurvy. Osteogenesis imperfecta involves brittle bones due to collagen defects, not specifically costochondral enlargements.
Question 93
A 15-month-old infant is brought to the clinic because he is not yet walking and struggles to pull himself to a standing position. His parents also report that he only recently started crawling at 12 months. These delayed motor milestones, along with other skeletal deformities, are common in children with:
View Answer & Explanation
Correct Answer: C
Rationale: Delayed sitting, crawling, and walking are explicitly mentioned as symptoms of rickets in children. The proximal muscle weakness associated with rickets contributes to these motor delays. Main Distractor Rationale: While cerebral palsy and muscular dystrophy can cause delayed motor milestones, the context of "other skeletal deformities" and the overall clinical picture points more specifically to rickets, which directly affects bone development and muscle function due to metabolic derangements.
Question 93
A 65-year-old male presents with chronic back pain and a recent history of a low-energy compression fracture of a lumbar vertebra. Radiographs of the lumbar spine reveal multiple biconcave vertebral bodies and indistinct, blurred trabeculae.

View Answer & Explanation
Correct Answer: C
Rationale: The radiographic findings of fractures, biconcave vertebral bodies, indistinct or blurred trabeculae, and bowing of the endplates are characteristic signs of bone softening and impaired mineralization seen in osteomalacia. Main Distractor Rationale: While osteoporosis can lead to vertebral compression fractures, these are typically wedge-shaped or crush fractures, and the trabeculae, though sparse, are usually distinct. The biconcave shape and blurred trabeculae are more indicative of the bone softening of osteomalacia.
Question 93
A 70-year-old female with a history of malabsorption syndrome presents with severe groin pain after a minor fall. An AP radiograph of the pelvis reveals a fracture of the right pubic bone. Further imaging and workup suggest a weakened pelvic ring due to metabolic bone disease.

View Answer & Explanation
Correct Answer: C
Rationale: The clinical context of malabsorption (a risk factor for vitamin D deficiency and osteomalacia), a low-energy fracture of the pubic bone, and evidence of a weakened pelvic ring are highly suggestive of osteomalacia, often coexisting with osteoporosis (osteoporomalacia) in older adults. The text specifically mentions pubic bone fractures due to a weakened pelvic ring in osteoporomalacia. Main Distractor Rationale: While severe osteoporosis can lead to insufficiency fractures, the underlying malabsorption and the specific mention of a "weakened pelvic ring" in the context of the provided text points more directly to osteomalacia, which often presents with osteoporosis in older patients as "osteoporomalacia."
Question 93
A 40-year-old male presents with progressive muscle weakness, bone pain, and multiple pseudofractures (Looser's zones) on radiographs. Laboratory tests show hypophosphatemia, phosphaturia, and normal serum calcium. Further investigation reveals a small, benign mesenchymal tumor. This presentation is most consistent with:
View Answer & Explanation
Correct Answer: C
Rationale: The combination of osteomalacia symptoms (bone pain, muscle weakness, pseudofractures), hypophosphatemia, phosphaturia, and the presence of a tumor (often mesenchymal) is characteristic of oncogenic osteomalacia. This condition is caused by tumors that secrete fibroblast growth factor 23 (FGF23), leading to renal phosphate wasting and impaired vitamin D activation. Main Distractor Rationale: While vitamin D deficiency osteomalacia shares many symptoms, the specific findings of hypophosphatemia, phosphaturia, normal serum calcium, and the presence of a tumor distinguish oncogenic osteomalacia from simple nutritional vitamin D deficiency.
Question 93
A 75-year-old female is diagnosed with a metabolic bone disorder. Her bone mineral density (BMD) T-score is -3.0 at the hip, indicating osteoporosis. Additionally, a bone biopsy shows evidence of impaired mineralization. The coexistence of these two conditions is best described as:
View Answer & Explanation
Correct Answer: C
Rationale: The text explicitly states that "Very often the osteomalacia and the osteoporosis are together" and refers to this combined condition as "osteoporomalacia." This term accurately describes the coexistence of reduced bone mass (osteoporosis) and impaired bone mineralization (osteomalacia). Main Distractor Rationale: Osteopenia refers to bone density that is lower than normal but not as severe as osteoporosis (T-score between -1.0 and -2.5). It does not specifically imply a mineralization defect, which is central to osteomalacia.
Question 93
A 2-year-old boy with rickets demonstrates characteristic cupping and fraying of the metaphyseal region of the wrist on initial radiographs. After 1 year of adequate vitamin D substitution treatment, follow-up radiographs are obtained.

View Answer & Explanation
Correct Answer: C
Rationale: The provided image and text (Fig. 7.34 c) clearly demonstrate that after 1 year of adequate substitution vitamin-D treatment, there is significant improvement in the characteristic radiological appearance of rickets at the wrist, including resolution of cupping and fraying. This indicates the effectiveness of treatment in promoting mineralization. Main Distractor Rationale: Worsening of metaphyseal cupping and fraying would indicate treatment failure or progression of the disease, which is contrary to the expected outcome of adequate vitamin D substitution.
Question 93
A 50-year-old male is diagnosed with osteomalacia secondary to chronic kidney disease. The primary metabolic derangement directly leading to the insufficient mineralization of bone in this patient is:
View Answer & Explanation
Correct Answer: B
Rationale: The text states that osteomalacia "is caused by a deficiency of vitamin D, which reduces bone formation by altering calcium and phosphorus metabolism." Regardless of the underlying cause (vitamin D deficiency, renal disorders, etc.), the final common pathway leading to insufficient mineralization is the disruption of calcium and phosphorus homeostasis, which are essential for bone mineralization. Main Distractor Rationale: While excessive parathyroid hormone secretion can occur in chronic kidney disease (secondary hyperparathyroidism) and contribute to bone disease (renal osteodystrophy), the direct mechanism for insufficient mineralization in osteomalacia is the altered calcium and phosphorus metabolism, which PTH dysregulation can exacerbate but is not the sole primary derangement causing the mineralization defect itself.
Question 93
A 3-year-old child presents with a waddling gait and difficulty climbing stairs. Physical examination reveals proximal muscle weakness and bowing of the legs. These findings, in the context of skeletal deformities, suggest:
View Answer & Explanation
Correct Answer: C
Rationale: Proximal muscle weakness, bowing of the legs, and bone pain are explicitly listed as characteristics of rickets in children. The waddling gait and difficulty climbing stairs are direct consequences of proximal muscle weakness. Main Distractor Rationale: While Duchenne muscular dystrophy also causes progressive proximal muscle weakness and a waddling gait, it is a primary muscle disorder without the characteristic skeletal deformities (like bowing of legs) or the underlying mineralization defect seen in rickets.
Question 93
A 78-year-old female patient is evaluated for chronic back pain and progressive stooping. Clinical examination reveals significant kyphosis and a noticeable loss of height. Her abdomen appears bulging. These clinical features are consistent with advanced:

View Answer & Explanation
Correct Answer: B
Rationale: The clinical description of loss of height, kyphosis, and a bulging abdomen in an elderly female is specifically highlighted in the text and image (Fig. 7.36) as characteristic of osteoporomalacia. These features result from vertebral compression fractures and spinal deformities caused by weakened, poorly mineralized bone. Main Distractor Rationale: While spondylolisthesis can cause back pain, it does not typically present with generalized loss of height, kyphosis, and a bulging abdomen as primary features of the condition itself, nor does it involve the systemic bone softening seen in osteoporomalacia.
Question 93
A 6-month-old infant presents with delayed motor development and bowing of the legs. A 40-year-old adult presents with diffuse bone pain and muscle weakness. Both patients are diagnosed with a disease characterized by insufficient mineralization of bone. The term used to distinguish the disease in the infant from that in the adult is:
View Answer & Explanation
Correct Answer: C
Rationale: The text explicitly states, "This disease [osteomalacia] causes the bending and misshaping of bones, such as bow-legging of the lower limbs, and is called rickets when it occurs in children." Rickets is essentially osteomalacia occurring before epiphyseal closure, affecting growth plates. Main Distractor Rationale: Osteoporosis is a distinct condition characterized by reduced bone mass but normal mineralization, and it is not the term used to differentiate osteomalacia in children from adults.
Question 93
A 55-year-old female is diagnosed with osteomalacia. Her physician is investigating the cause. Which of the following is NOT listed as a common cause of vitamin D deficiency leading to osteomalacia?
View Answer & Explanation
Correct Answer: D
Rationale: The text lists reduced exposure to sunlight, insufficient intake of vitamin D-enriched foods, and improper digestion and absorption of food with vitamin D as common causes of vitamin D deficiency. Renal tubular disorders (like Fanconi's syndrome) are also mentioned as a cause of osteomalacia, but they are not a cause of vitamin D *deficiency* itself, rather a cause of phosphate wasting leading to osteomalacia. Excessive intake of calcium supplements is not listed as a cause of vitamin D deficiency or osteomalacia; in fact, calcium is often supplemented in treatment. Main Distractor Rationale: Renal tubular disorders are a cause of osteomalacia, but not by causing vitamin D *deficiency*. They cause phosphate wasting, which leads to impaired mineralization. However, the question specifically asks for what is NOT a cause of vitamin D deficiency leading to osteomalacia. Excessive calcium intake is the most incorrect option as it does not cause vitamin D deficiency or osteomalacia.
Question 93
A 48-year-old male presents with chronic, widespread bone pain that is described as a dull ache, particularly in the spine, pelvis, and lower extremities. He also reports general malaise and easy fatigability. These symptoms, when delayed until the disorder has advanced, are characteristic of:
View Answer & Explanation
Correct Answer: C
Rationale: The text explicitly states that in adults, symptoms of osteomalacia are "often delayed until the disorder has advanced. These include easy fatigability, malaise, diffuse bone pain, and spasms." This directly matches the clinical vignette. Main Distractor Rationale: Fibromyalgia is characterized by widespread musculoskeletal pain, fatigue, and tenderness in specific points, but it is a soft tissue pain disorder and does not involve the underlying bone softening or specific radiographic findings of osteomalacia.
Question 93
A 60-year-old female presents with a history of recurrent fractures and generalized bone weakness. Her condition is attributed to osteomalacia. The fundamental effect of osteomalacia on bone structure is best described as:
View Answer & Explanation
Correct Answer: B
Rationale: The very first sentence of the text defines osteomalacia as "a disease in which insufficient mineralization leads to a softening of the bones." This is the core pathological feature of the condition, leading to bone weakness and susceptibility to fractures. Main Distractor Rationale: A primary defect in bone matrix formation (collagen synthesis) is characteristic of conditions like osteogenesis imperfecta, not osteomalacia. In osteomalacia, the matrix is formed, but it fails to mineralize adequately.
Question 94
A 45-year-old female presents with diffuse bone pain and easy fatigability. A bone biopsy is performed to investigate the underlying pathology. Histological examination reveals an increased amount of nonmineralized osteoid covering the normal mineralized trabeculae.

View Answer & Explanation
Correct Answer: C
Rationale: The clinical presentation of diffuse bone pain and easy fatigability in an adult, combined with the histological finding of increased nonmineralized osteoid covering mineralized trabeculae, is pathognomonic for osteomalacia. This condition is characterized by insufficient mineralization of bone matrix. Main Distractor Rationale: Osteoporosis is characterized by a reduction in bone mass and microarchitectural deterioration, but the mineralization of the remaining bone is normal. Histologically, there would not be an excess of unmineralized osteoid.
Question 95
A 78-year-old female presents with progressive loss of height, increasing kyphosis, and a bulging abdomen. She reports generalized malaise and diffuse bone pain that has worsened over the past year. Radiographs show biconcave vertebral bodies and indistinct trabeculae.

View Answer & Explanation
Correct Answer: C
Rationale: The patient's age, loss of height, kyphosis, malaise, diffuse bone pain, and radiographic findings of biconcave vertebral bodies and indistinct trabeculae are characteristic of osteomalacia. The term "osteoporomalacia" is used when osteomalacia and osteoporosis coexist, which is common in elderly patients presenting with these symptoms and signs. Main Distractor Rationale: While senile osteoporosis can cause loss of height and kyphosis due to vertebral compression fractures, the diffuse bone pain, malaise, and specific radiographic findings of indistinct trabeculae and biconcave vertebral bodies (suggesting bone softening) point more strongly towards osteomalacia, often coexisting with osteoporosis in this age group.
Question 96
A 2-year-old boy is brought to the clinic by his parents due to progressive bowing of his legs and difficulty walking. Physical examination reveals an "O" curvature of the lower limbs. An AP radiograph of the knee is obtained.

View Answer & Explanation
Correct Answer: B
Rationale: In rickets, which is osteomalacia in children, the characteristic radiographic findings at the knee include diffuse osteopenia, an "O" curvature (varus deformation), and importantly, widened growth plates that protrude into the soft and weakened metaphyseal region. This reflects the impaired mineralization of cartilage at the growth plate. Main Distractor Rationale: Normal growth plates with metaphyseal sclerosis would indicate a different pathology, such as osteopetrosis or a healing fracture, and is not consistent with the clinical presentation or typical radiographic findings of rickets.
Question 97
A 1-year-old girl presents with delayed walking and knobby enlargements at the ends of her long bones. Radiographs of the wrist are obtained to evaluate her skeletal development.

View Answer & Explanation
Correct Answer: B
Rationale: The characteristic radiological appearance of rickets at the wrist includes enlarged and widened growth plates and metaphyses, with cupping and fraying of the metaphyseal region. These findings are due to the impaired mineralization of the growing cartilage and bone. Main Distractor Rationale: Sclerotic metaphyses with normal growth plates are not characteristic of rickets; rickets involves impaired mineralization leading to lucency and disorganization, not sclerosis.
Question 98
A 35-year-old male presents with chronic, diffuse musculoskeletal pain and muscle weakness. Laboratory tests reveal low serum calcium and phosphate levels, with elevated alkaline phosphatase. A bone biopsy confirms osteomalacia.
View Answer & Explanation
Correct Answer: B
Rationale: Osteomalacia is fundamentally a disease characterized by insufficient mineralization of the osteoid (unmineralized bone matrix). This leads to the accumulation of soft, unmineralized bone, resulting in bone softening and pain. Main Distractor Rationale: Excessive bone resorption by osteoclasts is characteristic of conditions like osteoporosis or hyperparathyroidism, where bone mass is lost, but the remaining bone is typically well-mineralized. This is distinct from the mineralization defect seen in osteomalacia.
Question 99
A 9-month-old infant is noted by the pediatrician to have a disproportionately large head with a flattened occiput and prominent frontal bossing. The child also exhibits delayed motor milestones. These skull findings are clinically referred to as:
View Answer & Explanation
Correct Answer: C
Rationale: The description of a cubical skull, often with prominent frontal bossing, in a child with delayed motor milestones and other signs of rickets, is specifically referred to as "caput quadratum." This is a characteristic feature of rickets. Main Distractor Rationale: Plagiocephaly refers to an asymmetrical flattening of the skull, often due to positional molding, and does not specifically describe the cubical shape or frontal bossing associated with rickets.
Question 100
A 1-year-old child presents with a history of delayed crawling and walking. On physical examination, the pediatrician notes palpable, knobby enlargements at the costochondral junctions of the ribs, often described as a "rachitic rosary." This finding is indicative of:
View Answer & Explanation
Correct Answer: C
Rationale: The presence of knobby enlargements at the rib-breastbone joint (costochondral junctions), known as a "rachitic rosary," is a classic clinical sign of rickets. This, along with delayed motor milestones, strongly points to rickets. Main Distractor Rationale: Scurvy can cause bone pain and subperiosteal hemorrhages, but the "rachitic rosary" is not a characteristic feature of scurvy. Osteogenesis imperfecta involves brittle bones due to collagen defects, not specifically costochondral enlargements.
You Might Also Like
