Orthopaedic Board Exam Review: JIA, Bone Tumors, Syringomyelia & Charcot Joints | Part 8
Key Takeaway
This ABOS Orthopaedic Review covers critical topics for board exam preparation. Learn about Juvenile Idiopathic Arthritis (JIA) management, diverse bone tumor pathology including osteosarcoma and chondrosarcoma, and the diagnosis and treatment of syringomyelia with associated Charcot joint complications. Essential knowledge for orthopaedic specialists.
Question 1
A 12-year-old girl with a long-standing history of polyarticular JIA (RF positive) presents with increasing pain and stiffness in her right hip. Radiographs show significant joint space narrowing, subchondral sclerosis, and early erosions. She has failed multiple DMARDs and biologics. What is the most definitive surgical intervention for her hip pain and dysfunction?
View Answer & Explanation
Correct Answer: C
Rationale: For end-stage arthropathy in JIA, characterized by significant joint destruction, pain, and functional limitation refractory to medical management, total hip arthroplasty (THA) is the most definitive surgical intervention to restore function and relieve pain. Arthroscopic debridement and synovectomy are for earlier stages of disease or specific indications. Core decompression is for avascular necrosis. Femoral osteotomy might be considered for deformity correction but not for end-stage arthritis with significant joint destruction.
Question 2
A 3-year-old girl with oligoarticular JIA of the left knee is being managed with intra-articular corticosteroid injections. Her parents are concerned about potential complications. Which of the following is a common local complication of repeated intra-articular corticosteroid injections in children?
View Answer & Explanation
Correct Answer: C
Rationale: Subcutaneous fat atrophy and skin depigmentation at the injection site are common local complications of intra-articular corticosteroid injections, especially in children due to their thinner skin and subcutaneous tissue. While septic arthritis is a rare but serious complication, and adrenal suppression is possible with very frequent or high-dose injections, fat atrophy and skin changes are more frequently observed local issues. Systemic growth retardation and avascular necrosis are not typical local complications of intra-articular injections.
Question 3
A 15-year-old boy with a history of enthesitis-related JIA presents with worsening back pain and stiffness, particularly in the morning. Radiographs of the lumbar spine show squaring of vertebral bodies and syndesmophytes. Which laboratory marker is most likely to be positive in this patient?
View Answer & Explanation
Correct Answer: D
Rationale: Enthesitis-related JIA is strongly associated with the HLA-B27 allele, similar to adult ankylosing spondylitis. The clinical presentation of axial involvement (back pain, stiffness, syndesmophytes) further supports this association. RF and anti-CCP are characteristic of RF-positive polyarticular JIA. ANA is common in oligoarticular JIA. Anti-dsDNA is associated with Systemic Lupus Erythematosus.
Question 4
A 7-year-old girl with oligoarticular JIA is being monitored for chronic anterior uveitis. She is currently asymptomatic, but a recent slit-lamp examination revealed active inflammation. What is the primary goal of treatment for JIA-associated uveitis?
View Answer & Explanation
Correct Answer: C
Rationale: The primary goal of treating JIA-associated uveitis is to preserve vision and prevent complications such as cataracts, glaucoma, synechiae, and band keratopathy, which can lead to permanent vision loss. Uveitis often runs an independent course from joint disease and requires specific ophthalmologic management, typically with topical corticosteroids and cycloplegics, and sometimes systemic immunosuppressants. While the other options are goals for JIA management in general, they are not the primary goal specifically for uveitis.
Question 5
A 13-year-old boy with systemic JIA is admitted to the hospital with high fever, rash, hepatosplenomegaly, and new onset pancytopenia, coagulopathy, and elevated liver enzymes. His ferritin level is extremely high. What is the most likely acute and life-threatening complication he is experiencing?
View Answer & Explanation
Correct Answer: C
Rationale: The constellation of high fever, rash, hepatosplenomegaly, pancytopenia, coagulopathy, elevated liver enzymes, and extremely high ferritin in a patient with systemic JIA is highly suggestive of Macrophage Activation Syndrome (MAS). MAS is a severe, life-threatening complication of sJIA characterized by uncontrolled activation and proliferation of macrophages and T lymphocytes, leading to a cytokine storm. Septic shock, acute renal failure, drug-induced hepatitis, and myocarditis are less likely to present with this specific combination of findings, especially the pancytopenia and extremely high ferritin.
Question 6
A 6-year-old girl with polyarticular JIA (RF negative) has developed significant flexion contractures in both knees and elbows despite medical management. Her rheumatologist recommends a comprehensive rehabilitation program. Which of the following is a primary goal of physical therapy in JIA?
View Answer & Explanation
Correct Answer: C
Rationale: Physical therapy plays a crucial role in the multidisciplinary management of JIA. Its primary goals are to maintain or improve joint range of motion, prevent contractures, strengthen muscles, improve functional abilities, and reduce pain. While medical treatments aim to reduce inflammation and control the autoimmune process, physical therapy focuses on the musculoskeletal consequences of the disease. The other options are either goals of medical therapy or not a direct goal of physical therapy.
Question 7
A 10-year-old boy with a 1-year history of JIA affecting his right knee and ankle presents with persistent pain and swelling in these joints despite treatment with methotrexate. His rheumatologist is considering initiating a biologic agent. Which class of biologic agents is commonly used as a first-line biologic for JIA?
View Answer & Explanation
Correct Answer: D
Rationale: TNF-alpha inhibitors (e.g., etanercept, adalimumab) are generally considered the first-line biologic agents for JIA that is refractory to conventional DMARDs like methotrexate, particularly for oligoarticular and polyarticular subtypes. IL-1 and IL-6 inhibitors are often used for systemic JIA. T-cell costimulation modulators (abatacept) and B-cell depleting agents (rituximab) are typically reserved for specific situations or as second-line biologics.
Question 8
A 16-year-old girl with a history of polyarticular JIA (RF positive) presents with severe pain and limited motion in her temporomandibular joints (TMJs). Radiographs show condylar erosion and flattening. What is the most appropriate initial management strategy for JIA-related TMJ arthritis?
View Answer & Explanation
Correct Answer: B
Rationale: JIA-related TMJ arthritis is common and can lead to significant pain, dysfunction, and growth disturbances. Initial management typically involves conservative measures such as intra-articular corticosteroid injections to reduce inflammation, along with physical therapy to maintain range of motion and prevent ankylosis. Systemic medications for JIA also play a role. Surgical interventions like condylectomy, distraction osteogenesis, or total TMJ replacement are reserved for severe, refractory cases with significant deformity or ankylosis after failure of conservative and medical management. Long-term oral corticosteroids are not ideal due to systemic side effects.
Question 9
A 2-year-old boy presents with a swollen, warm, and painful right knee. He has no fever or other systemic symptoms. Arthrocentesis reveals cloudy synovial fluid with a white blood cell count of 60,000/mm³ (85% neutrophils) and a glucose level significantly lower than serum. Gram stain is negative. What is the most important differential diagnosis to rule out before considering JIA?
View Answer & Explanation
Correct Answer: C
Rationale: In a young child presenting with acute monoarthritis, especially with inflammatory synovial fluid findings (high WBC count, high neutrophils, low glucose), septic arthritis is a surgical emergency and the most critical diagnosis to rule out immediately. While JIA can present as monoarthritis, the inflammatory markers in the synovial fluid are highly suspicious for infection. Transient synovitis typically has less inflammatory fluid. Lyme arthritis and leukemia are important considerations but less immediately life-threatening than septic arthritis. Hemarthrosis would typically show blood in the joint fluid.
Question 10
A 14-year-old girl with a 5-year history of polyarticular JIA (RF negative) has developed significant wrist deformities, including ulnar deviation and carpal collapse. Which of the following surgical procedures might be considered to improve wrist function and stability in this patient?
View Answer & Explanation
Correct Answer: C
Rationale: For severe, painful, and unstable wrist deformities in JIA that have failed medical management, wrist arthrodesis (fusion) can provide significant pain relief and stability, albeit at the cost of motion. This is a common reconstructive procedure for end-stage JIA wrist involvement. Carpal tunnel release addresses nerve compression. DRUJ fusion might be part of a larger wrist reconstruction but not the primary procedure for overall wrist deformity. MCP joint arthroplasty addresses finger deformities. Tendon transfers are for specific muscle imbalances or ruptures.
Question 11
A 9-year-old boy with systemic JIA is on long-term oral corticosteroids. His parents are concerned about the potential side effects. Which of the following is a well-known musculoskeletal complication of chronic corticosteroid use in children?
View Answer & Explanation
Correct Answer: C
Rationale: Avascular necrosis (AVN), particularly of the femoral head, is a serious and well-known musculoskeletal complication of chronic systemic corticosteroid use in children, especially in conditions like systemic JIA where high doses may be required. Corticosteroids can also lead to osteoporosis and growth retardation, not accelerated bone maturation or increased bone mineral density. Joint hypermobility and ligamentous laxity are not typical complications of corticosteroids.
Question 12
A 5-year-old girl is diagnosed with oligoarticular JIA affecting her left knee. Her ANA test is positive. What is the recommended frequency for ophthalmologic screening for uveitis in this patient?
View Answer & Explanation
Correct Answer: C
Rationale: For children with oligoarticular JIA who are ANA positive, the risk of chronic anterior uveitis is significantly elevated. Due to the often asymptomatic nature of uveitis in children, frequent ophthalmologic screening (slit-lamp examination) is crucial. Guidelines typically recommend screening every 3-4 months for ANA-positive oligoarticular JIA patients. Less frequent screening or waiting for symptoms can lead to delayed diagnosis and irreversible vision loss. ANA-negative oligoarticular JIA or older children might have less frequent screening.
Question 13
A 12-year-old girl with a 3-year history of polyarticular JIA (RF negative) presents with increasing pain and stiffness in her cervical spine. Radiographs show atlantoaxial subluxation. What is the most critical concern regarding this finding?
View Answer & Explanation
Correct Answer: C
Rationale: Atlantoaxial subluxation in JIA, particularly in polyarticular forms, is a serious complication due to inflammation and laxity of the transverse ligament. The most critical concern is the potential for spinal cord compression, which can lead to devastating neurological deficits, including paralysis or even death. While the other options (kyphosis, radiculopathy, limited motion, dysphagia) can occur, spinal cord compression represents the most immediate and severe threat requiring urgent evaluation and potentially surgical stabilization.
Question 14
A 14-year-old girl with a history of polyarticular, RF-negative juvenile idiopathic arthritis presents with severe bilateral hip pain and stiffness, significantly limiting her ambulation. Physical examination reveals severely restricted range of motion in both hips, with flexion contractures and pain at the extremes. Radiographs show advanced bilateral hip destruction with joint space narrowing, subchondral erosions, and acetabular protrusion. She has failed maximal medical therapy, including biologics.
View Answer & Explanation
Correct Answer: C
Rationale: For a young patient with advanced, symptomatic hip destruction due to JIA who has failed maximal medical therapy, bilateral total hip arthroplasty (THA) is the most appropriate surgical intervention to restore function and alleviate pain. JIA patients often have bilateral involvement, and addressing both hips simultaneously or in a staged manner (often simultaneously if feasible) is common. Arthrodesis is generally avoided in JIA due to the high likelihood of multi-joint involvement and the need to preserve motion. Osteotomy is typically for earlier stages of disease or specific deformities, not advanced destruction. Continued medical management is not appropriate given the failure of previous treatments and severe functional limitation.
Question 15
A 7-year-old boy with systemic juvenile idiopathic arthritis (sJIA) is admitted to the hospital with a high fever, rash, and polyarthritis. Over the past 24 hours, he develops increasing lethargy, hepatosplenomegaly, lymphadenopathy, and laboratory findings show pancytopenia, elevated ferritin (markedly high), elevated triglycerides, and low fibrinogen. His ESR and CRP, previously very high, are now paradoxically decreasing.
View Answer & Explanation
Correct Answer: C
Rationale: The constellation of symptoms including high fever, hepatosplenomegaly, lymphadenopathy, pancytopenia, markedly elevated ferritin, elevated triglycerides, low fibrinogen, and a paradoxical decrease in ESR/CRP in a patient with sJIA is highly suggestive of Macrophage Activation Syndrome (MAS). MAS is a severe and potentially life-threatening complication of sJIA, characterized by uncontrolled activation and proliferation of macrophages and T lymphocytes. While some features overlap with septic shock or DIC, the specific lab profile (especially ferritin and the paradoxical ESR/CRP) points to MAS. Worsening sJIA flare would typically show continued high inflammatory markers.
Question 16
A 4-year-old girl presents with a 3-month history of swelling and limited range of motion in her right knee. Physical examination reveals a warm, effused right knee with mild flexion contracture. The remainder of her joints are normal. Laboratory tests show a positive ANA, negative RF, and normal ESR/CRP. Radiographs of the knee are unremarkable except for soft tissue swelling. She is diagnosed with oligoarticular JIA.
View Answer & Explanation
Correct Answer: C
Rationale: For oligoarticular JIA with active synovitis in one or a few joints, intra-articular corticosteroid injection is the first-line treatment. It effectively reduces inflammation locally with minimal systemic side effects. NSAIDs alone may provide symptomatic relief but often do not control the underlying synovitis. Oral methotrexate and systemic corticosteroids are typically reserved for more widespread disease or failure of intra-articular injections. Surgical synovectomy is a last resort for persistent synovitis unresponsive to medical management.
Question 17
A 16-year-old boy with a long-standing history of polyarticular JIA presents with severe pain and stiffness in multiple joints, particularly his wrists, knees, and ankles. He has experienced multiple flares and has been on various DMARDs and biologics. Radiographs of his affected joints are obtained.
View Answer & Explanation
Correct Answer: C
Rationale: In advanced JIA, characteristic radiographic findings include subchondral erosions (due to chronic synovitis), joint space narrowing (due to cartilage destruction), and epiphyseal overgrowth (due to chronic inflammation and hyperemia near growth plates). Other findings can include periarticular osteopenia, growth disturbances (e.g., leg length discrepancy, micrognathia), and in severe cases, joint ankylosis. Diffuse osteopenia alone or isolated soft tissue swelling are seen in earlier stages. Joint space widening and osteophytes are more typical of osteoarthritis, while chondrocalcinosis is associated with crystal arthropathies.
Question 18
A 10-year-old girl with a 5-year history of polyarticular JIA complains of persistent neck pain and stiffness, especially with rotation. Physical examination reveals limited cervical range of motion, particularly in rotation and extension. Neurological examination is normal. Radiographs of the cervical spine show C1-C2 instability with atlantoaxial subluxation and fusion of the posterior elements of the cervical spine.
View Answer & Explanation
Correct Answer: D
Rationale: Atlantoaxial subluxation with C1-C2 instability in JIA, especially when symptomatic or progressive, carries a significant risk of spinal cord compression. Given the radiographic findings of instability and posterior element fusion (which can exacerbate instability by limiting compensatory motion), surgical stabilization of the cervical spine is indicated to prevent neurological compromise. Aggressive physical therapy could worsen instability. Oral corticosteroids might reduce inflammation but won't address mechanical instability. A cervical collar provides temporary support but is not a definitive treatment for instability. MRI of the brain is not indicated for this specific presentation of cervical instability.
Question 19
A 6-year-old boy presents to the emergency department with acute onset of severe pain, swelling, and warmth in his right knee, accompanied by a fever of 102°F (38.9°C). He refuses to bear weight on the leg. There is no prior history of joint pain. Physical examination reveals a markedly tender, erythematous, and swollen right knee with severely restricted, painful range of motion. Laboratory tests show elevated white blood cell count, ESR, and CRP. Radiographs show a joint effusion without bony abnormalities.
View Answer & Explanation
Correct Answer: C
Rationale: The acute onset of severe monoarticular pain, swelling, warmth, fever, and refusal to bear weight, along with elevated inflammatory markers, is highly suspicious for septic arthritis. Septic arthritis is a surgical emergency that requires urgent diagnosis and treatment to prevent rapid joint destruction. An urgent aspiration of the knee joint is critical to obtain synovial fluid for cell count, Gram stain, and culture to confirm the diagnosis and identify the causative organism. Delaying aspiration and treatment can lead to irreversible cartilage damage. While JIA can present with acute flares, the acute, severe, monoarticular presentation with high fever makes septic arthritis the primary concern. NSAIDs, ANA/RF, or systemic corticosteroids are not appropriate initial steps in this emergent situation. Discharging with antibiotics without aspiration is dangerous.
Question 20
A 3-year-old girl was diagnosed with oligoarticular JIA affecting her left knee. She received intra-articular corticosteroid injections and has been well controlled for the past 2 years, with no new joint involvement. Her ANA was positive at diagnosis. Her parents ask about her long-term prognosis.
View Answer & Explanation
Correct Answer: C
Rationale: Oligoarticular JIA, especially with a positive ANA, has the best prognosis among JIA subtypes, with a high rate of remission and good long-term functional outcomes. However, these patients are at increased risk for chronic anterior uveitis, which can lead to blindness if not detected and treated early. Therefore, regular ophthalmologic screening (slit-lamp examination) is crucial. Systemic complications, polyarticular disease in adulthood, lifelong immunosuppression, or severe hip/spine involvement are less common in this subtype compared to others.
Question 21
A 9-year-old boy with a history of oligoarticular JIA affecting his right knee since age 3 presents for follow-up. His knee disease is well-controlled with intra-articular injections. His parents notice that his right leg appears longer than his left. Physical examination confirms a measurable leg length discrepancy, with the right leg being 1.5 cm longer than the left.
View Answer & Explanation
Correct Answer: A
Rationale: Leg length discrepancy (LLD) is a common growth disturbance in JIA, particularly in oligoarticular forms affecting a single lower extremity joint. Chronic inflammation and hyperemia around the affected joint (e.g., knee) can stimulate growth at the adjacent physis, leading to overgrowth of the affected limb. While corticosteroids can have systemic effects on growth, intra-articular injections are less likely to cause this specific LLD. It is a known complication of JIA, not an unrelated anomaly or an indication of worsening systemic disease. Management depends on the severity of the discrepancy and can range from shoe lifts to epiphysiodesis.
Question 22
A 12-year-old girl with polyarticular JIA has persistent synovitis in her right wrist despite optimal medical management, including methotrexate and a TNF-alpha inhibitor. She experiences significant pain, swelling, and limited range of motion, impacting her ability to perform daily activities. Radiographs show persistent soft tissue swelling but no significant erosions or joint destruction.
View Answer & Explanation
Correct Answer: C
Rationale: Surgical synovectomy is indicated for persistent, symptomatic synovitis that has failed to respond to maximal medical management (including DMARDs and biologics), especially when there is no significant joint destruction yet. The goal is to remove the inflamed synovium to reduce pain, swelling, and prevent further cartilage and bone damage. While trying a different biologic (E) might be considered, surgical synovectomy is a direct intervention for localized, refractory synovitis. Continuing current management (A) or increasing the dose (B) is unlikely to be effective given the failure. Systemic corticosteroids (D) are typically for acute flares or systemic symptoms, not localized refractory synovitis.
Question 23
A 15-year-old boy with polyarticular JIA, well-controlled on methotrexate, requires an elective total knee arthroplasty due to severe joint destruction and pain. His rheumatologist has cleared him for surgery. As the orthopaedic surgeon, what is a key consideration regarding his methotrexate therapy in the perioperative period?
View Answer & Explanation
Correct Answer: B
Rationale: Current recommendations from rheumatology and orthopaedic societies generally advise continuing methotrexate throughout the perioperative period for patients undergoing elective surgery. Studies have shown that discontinuing methotrexate can increase the risk of disease flare without significantly reducing the risk of infection or wound complications. Maintaining disease control is crucial for optimal surgical outcomes. Discontinuing methotrexate (A, D) is outdated advice. Switching to a biologic (C) or corticosteroids (E) is not the standard approach for perioperative management of methotrexate.
Question 24
A 13-year-old girl with a history of polyarticular JIA presents with progressive difficulty chewing, jaw pain, and facial asymmetry. Physical examination reveals limited mouth opening, crepitus in both temporomandibular joints (TMJs), and a retrognathic mandible. Radiographs and MRI confirm bilateral TMJ arthritis with condylar erosion and hypoplasia.
View Answer & Explanation
Correct Answer: C
Rationale: TMJ involvement is common in JIA and can lead to significant functional and cosmetic issues. Initial management for active TMJ arthritis typically involves conservative measures, including intra-articular corticosteroid injections, physical therapy, and splinting. These aim to reduce inflammation and preserve joint function. While surgical reconstruction (D) may be necessary for severe, end-stage disease with significant deformity and functional impairment, it is not the first-line treatment. Orthodontics (A) may be part of a comprehensive plan but won't address the active inflammation. Aggressive physical therapy (B) without addressing inflammation can be painful. A soft diet and NSAIDs (E) are supportive but often insufficient to control active arthritis.
Question 25
A 5-year-old boy is diagnosed with polyarticular JIA affecting his knees, ankles, and wrists. He has significant pain, stiffness, and limited range of motion in these joints. His medical treatment includes methotrexate. What non-pharmacological intervention is crucial for optimizing his long-term functional outcome?
View Answer & Explanation
Correct Answer: C
Rationale: Regular physical and occupational therapy is a cornerstone of JIA management. It helps maintain or improve joint range of motion, strengthen muscles, prevent contractures, improve functional independence, and educate the child and family on joint protection. Complete bed rest (A) can lead to joint stiffness and muscle atrophy. High-impact exercises (B) can exacerbate joint inflammation and damage. Strict immobilization (D) can lead to contractures and loss of function. Nutritional counseling (E) is important for overall health but not the primary non-pharmacological intervention for joint function.
Question 26
A 16-year-old girl with long-standing polyarticular JIA presents with a severe, fixed flexion contracture of her right knee (45 degrees), significantly impairing her ambulation. She has failed extensive physical therapy and serial casting. Radiographs show significant joint space narrowing and early erosions but no complete ankylosis.
View Answer & Explanation
Correct Answer: D
Rationale: For a severe, fixed flexion contracture of the knee in a skeletally mature adolescent with significant joint destruction due to JIA, total knee arthroplasty (TKA) is often the most effective surgical option to correct the deformity, relieve pain, and restore function. While osteotomy (C) can correct angular deformities, it is less effective for severe fixed flexion contractures with significant joint destruction. Continued conservative measures (A, B) are unlikely to be effective given the severity and chronicity. Arthrodesis (E) is generally avoided in JIA due to multi-joint involvement and the need to preserve motion.
Question 27
A 17-year-old boy with a history of systemic JIA, currently on a biologic agent, is scheduled for a total hip arthroplasty due to severe bilateral hip destruction. What is a critical pre-operative consideration for this patient from an orthopaedic perspective?
View Answer & Explanation
Correct Answer: B
Rationale: Patients with JIA, especially those with systemic disease or long-term corticosteroid use, are at high risk for osteoporosis and poor bone quality. This can significantly impact implant fixation and increase the risk of periprosthetic fractures during and after total hip arthroplasty. Therefore, a thorough assessment of bone quality (e.g., DEXA scan) and optimization of bone health pre-operatively is crucial. Discontinuation of all JIA medications (A) is generally not recommended as it can lead to disease flares. Immediate full weight-bearing (C) may not be appropriate given potential bone fragility. Recovery (D) can be prolonged and challenging. JIA patients have unique challenges that require specific pre-operative considerations (E is incorrect).
Question 28
A 10-year-old boy presents with a 6-month history of pain and swelling in his right knee and left ankle. He also reports intermittent low back pain and has a family history of psoriasis. Physical examination reveals enthesitis at the Achilles tendon insertion bilaterally and dactylitis of the right second toe. Radiographs show mild joint effusions in the knee and ankle, and sacroiliac joint sclerosis.
View Answer & Explanation
Correct Answer: D
Rationale: The presence of enthesitis (inflammation at tendon/ligament insertions), dactylitis (sausage digits), low back pain suggestive of sacroiliitis, and lower extremity arthritis in a male child is highly characteristic of Enthesitis-Related Arthritis (ERA), a subtype of JIA. ERA is strongly associated with HLA-B27 and often progresses to ankylosing spondylitis in adulthood. While psoriasis is in the family history, the primary features described (enthesitis, dactylitis, sacroiliitis) fit ERA more precisely, though PsA can also have these features. Oligoarticular and polyarticular JIA typically do not present with prominent enthesitis or sacroiliitis. Systemic JIA has distinct systemic features like fever and rash.
Question 29
A 7-year-old girl is diagnosed with polyarticular JIA. Her rheumatologist explains that JIA is an autoimmune disease. Which of the following best describes the underlying pathophysiology of JIA?
View Answer & Explanation
Correct Answer: C
Rationale: JIA is an autoimmune disease characterized by chronic inflammation of the synovial membrane, driven by dysregulation of the immune system. This leads to the infiltration of immune cells into the joint, release of pro-inflammatory cytokines, and ultimately, damage to articular cartilage and subchondral bone. Bacterial infection (A) describes septic arthritis. Degenerative wear and tear (B) describes osteoarthritis. Crystal deposition (D) describes gout or pseudogout. Traumatic injury (E) describes acute trauma, not chronic inflammatory arthritis.
Question 30
A 14-year-old boy with long-standing polyarticular JIA presents with severe pain and deformity in both feet and ankles. He has developed rigid pes planovalgus deformities, hallux valgus, and painful callosities. His ambulation is significantly impaired. Radiographs show severe hindfoot valgus, midfoot collapse, and forefoot deformities with joint destruction.
View Answer & Explanation
Correct Answer: C
Rationale: For severe, rigid, painful foot and ankle deformities with significant joint destruction in JIA that impair ambulation and have failed conservative management, surgical arthrodesis (fusion) of the affected joints (e.g., triple arthrodesis for hindfoot deformity) is often necessary to correct the deformity, stabilize the foot, and relieve pain. While orthotics (A) and physical therapy (B) are important conservative measures, they are unlikely to correct rigid deformities with joint destruction. Injections (D) and NSAIDs (E) address inflammation and pain but not the structural deformities or instability.
Question 31
A 6-year-old girl is newly diagnosed with systemic JIA. Her treatment plan involves a combination of medications, physical therapy, and regular monitoring. Her parents are overwhelmed and ask about the best approach to her care.
View Answer & Explanation
Correct Answer: C
Rationale: JIA is a complex chronic disease that often affects multiple organ systems and requires a comprehensive approach to care. A multidisciplinary team, typically including a pediatric rheumatologist, orthopaedic surgeon, physical therapist, occupational therapist, ophthalmologist, dentist, social worker, and psychologist, is essential for optimal management. This ensures all aspects of the disease (medical, musculoskeletal, ocular, psychosocial) are addressed. Relying solely on a single physician (A, B) or pharmacotherapy (D) is insufficient. Homeopathic remedies (E) are not evidence-based for JIA.
Question 32
A 16-year-old male presents with a 3-month history of progressive right distal femur pain, worse with activity and at night. Physical examination reveals a palpable mass and tenderness over the distal femur. Radiographs show a destructive lesion in the distal femoral metaphysis with a sunburst periosteal reaction and Codman's triangle. There is evidence of cortical breach. A chest CT reveals multiple bilateral pulmonary nodules.
View Answer & Explanation
Correct Answer: E
Rationale: The clinical presentation and radiographic findings are highly suggestive of osteosarcoma with pulmonary metastases. The initial diagnostic step for a suspected malignant bone tumor is an image-guided core needle biopsy. This provides tissue for definitive diagnosis, grading, and molecular studies while minimizing contamination of surrounding tissues, which is crucial for subsequent limb salvage planning. An open biopsy is generally avoided due to increased risk of contamination and potential compromise of future surgical margins. Neoadjuvant chemotherapy is indicated after a definitive diagnosis is made. Excisional biopsy of lung nodules is not the primary diagnostic step for the bone lesion. Palliative radiation is not the initial treatment for potentially curable metastatic osteosarcoma.
Question 33
A 12-year-old female presents with left proximal humerus pain and swelling for 2 months, accompanied by intermittent fever and weight loss. Physical examination reveals a warm, tender, palpable mass. Radiographs show a lytic lesion in the diaphysis of the proximal humerus with an "onion-skin" periosteal reaction. MRI demonstrates a large soft tissue component. A bone scan shows increased uptake in the proximal humerus and a focal area in the left iliac wing.
View Answer & Explanation
Correct Answer: C
Rationale: The patient's age (adolescent), diaphyseal location, "onion-skin" periosteal reaction, large soft tissue component, and systemic symptoms (fever, weight loss) are classic features of Ewing sarcoma. Osteosarcoma typically presents in the metaphysis with a sunburst pattern. Chondrosarcoma is more common in older adults. Giant cell tumor is typically epiphyseal in young adults. Osteoid osteoma is a benign lesion with a characteristic nidus and pain relieved by NSAIDs, without systemic symptoms or a large soft tissue mass.
Question 34
A 65-year-old male presents with dull, aching pain in his right hip and groin for 6 months, which has been gradually worsening. He denies any history of trauma. Radiographs of the pelvis show an ill-defined, expansile lesion in the right ilium with punctate and ring-and-arc calcifications and endosteal scalloping. A core needle biopsy reveals atypical chondrocytes within a myxoid matrix.
Correct Answer: D
Rationale: The patient's age (older adult), location (pelvis), radiographic findings (expansile lesion, punctate/ring-and-arc calcifications, endosteal scalloping), and biopsy results (atypical chondrocytes in myxoid matrix) are all characteristic of chondrosarcoma. Enchondromas are typically asymptomatic, smaller, and lack significant endosteal scalloping or atypical features. Osteochondromas are exostoses. Chondroblastoma occurs in younger patients and is epiphyseal. Osteosarcoma would show osteoid matrix, not chondroid.
Question 35
A 28-year-old female presents with left distal femur pain and swelling for 4 months. Radiographs show a lytic, expansile lesion involving the epiphysis and extending into the metaphysis of the distal femur, with a "soap-bubble" appearance and no sclerotic rim. MRI confirms the epiphyseal involvement and shows no significant matrix mineralization.
View Answer & Explanation
Correct Answer: C
Rationale: The patient's age (young adult), epiphyseal location (extending into metaphysis), lytic and expansile "soap-bubble" appearance without a sclerotic rim or significant matrix mineralization are classic features of a giant cell tumor (GCT). Aneurysmal bone cysts can be expansile and lytic but typically have fluid-fluid levels on MRI and are often metaphyseal. Chondroblastoma is epiphyseal but usually has a sclerotic rim and calcified matrix. Unicameral bone cysts are typically metaphyseal in children. Osteosarcoma usually has a more aggressive appearance with periosteal reaction and osteoid matrix.
Question 36
A 14-year-old male presents with a 6-month history of localized right proximal tibia pain, worse at night and consistently relieved by over-the-counter NSAIDs. Physical examination is unremarkable except for mild tenderness over the anterior aspect of the proximal tibia. Radiographs show cortical thickening with a small, lucent nidus surrounded by reactive sclerosis in the proximal tibia.
View Answer & Explanation
Correct Answer: B
Rationale: The clinical presentation (nocturnal pain relieved by NSAIDs) and radiographic findings (lucent nidus with reactive sclerosis) are pathognomonic for osteoid osteoma. Percutaneous radiofrequency ablation (RFA) is the preferred treatment due to its minimally invasive nature, high success rate, and lower morbidity compared to surgical excision. Surgical excision is an alternative but more invasive. Observation is an option for asymptomatic or mildly symptomatic lesions, but this patient has significant pain. Chemotherapy and radiation are not indicated for benign osteoid osteoma.
Question 37
A 7-year-old boy falls during soccer and sustains a pathologic fracture of his left proximal humerus. Radiographs show a well-circumscribed, centrally located, lytic lesion in the metaphysis of the proximal humerus with a "fallen leaf" sign. The lesion is slightly expansile with a thin cortex.
View Answer & Explanation
Correct Answer: C
Rationale: The patient's age (child), metaphyseal location, lytic and well-circumscribed nature, and the presence of a "fallen leaf" sign (a fragment of cortical bone that has fallen to the bottom of the cyst) are classic for a unicameral bone cyst (UBC). Aneurysmal bone cysts are typically expansile and eccentric with fluid-fluid levels. Fibrous dysplasia has a "ground glass" appearance. Non-ossifying fibromas are eccentric cortical lesions with a sclerotic rim. Chondroblastomas are epiphyseal.
Question 38
An 11-year-old girl is evaluated for knee pain after a minor fall. Radiographs of the distal femur, obtained to rule out fracture, incidentally reveal an eccentric, lobulated, lucent lesion in the metaphysis with a thin sclerotic rim. The lesion is located in the cortex and does not involve the medullary canal. She denies any prior symptoms related to this area.
View Answer & Explanation
Correct Answer: C
Rationale: The patient's age (adolescent), asymptomatic presentation, eccentric cortical location, lobulated lucency, and sclerotic rim are characteristic of a non-ossifying fibroma (NOF), also known as a fibrous cortical defect if smaller. These are benign, self-limiting lesions that typically resolve spontaneously with cortical remodeling. Asymptomatic lesions do not require intervention and can be observed with serial radiographs to confirm resolution. Surgical intervention is reserved for large, symptomatic lesions or those at risk of pathologic fracture. Biopsy is not needed for classic radiographic appearance.
Question 39
A 35-year-old male presents with a 1-year history of progressive right hip pain and a limp. He has a history of multiple fractures in childhood. Physical examination reveals a shepherd's crook deformity of the proximal femur. Radiographs show an expansile, ground-glass lesion involving the proximal femur and acetabulum, with cortical thinning.
View Answer & Explanation
Correct Answer: C
Rationale: The patient's history of multiple fractures, "shepherd's crook" deformity, and radiographic "ground-glass" appearance are classic for fibrous dysplasia. This is a developmental anomaly where normal bone is replaced by immature woven bone and fibrous tissue. Osteogenesis imperfecta is characterized by brittle bones but typically presents with diffuse osteopenia and blue sclera. Paget's disease affects older adults and shows mixed lytic and blastic lesions. Enchondromatosis involves multiple enchondromas. Multiple myeloma presents with punched-out lytic lesions in older adults.
Question 40
A 55-year-old male presents with persistent, dull pain in his left proximal humerus for 8 months. He denies any trauma. Radiographs show an intramedullary lesion with punctate calcifications and endosteal scalloping greater than 2/3 of the cortical thickness. A previous radiograph from 2 years ago showed a similar lesion, but it was smaller and had less endosteal scalloping.
View Answer & Explanation
Correct Answer: B
Rationale: The patient's age, persistent pain, intramedullary location, punctate calcifications, and especially the progressive endosteal scalloping (greater than 2/3 cortical thickness) and interval growth are highly suspicious for a low-grade chondrosarcoma. While enchondromas can have similar calcifications, they are typically asymptomatic, stable, and have minimal to no endosteal scalloping. Osteochondromas are exostoses. Chondroblastomas are epiphyseal and occur in younger patients. Fibrous dysplasia has a "ground glass" appearance.
Question 41
A 45-year-old male presents with a rapidly growing, painful mass in his right distal femur. Radiographs and MRI suggest a high-grade malignant bone tumor. A biopsy is planned. Which of the following is the most critical principle to adhere to during the biopsy procedure?
View Answer & Explanation
Correct Answer: B
Rationale: For suspected malignant bone tumors, the biopsy tract must be planned meticulously so that it can be completely excised en bloc with the definitive tumor resection. This prevents tumor cell seeding along the tract, which could compromise limb salvage or require a wider resection. Biopsying through the largest soft tissue component is not always the best approach; the tract should be direct and surgically excisable. While adequate tissue is needed, the primary concern is the excisability of the tract. Anesthesia choice depends on the patient and procedure. Multiple biopsies are often performed, but the *most critical* principle is the excisability of the tract.
Question 42
A 19-year-old male is diagnosed with a high-grade osteosarcoma of the proximal tibia. Imaging reveals that the tumor has breached the cortex and extended into the surrounding soft tissues, but there is no evidence of skip lesions or distant metastases. According to the Enneking surgical staging system, what is the appropriate stage for this tumor?
View Answer & Explanation
Correct Answer: D
Rationale: The Enneking surgical staging system classifies musculoskeletal sarcomas based on grade (G), local extent (T), and presence of metastases (M). * Grade (G): G1 (low), G2 (high). This is a high-grade osteosarcoma (G2). * Local Extent (T): T0 (intracapsular), T1 (intracompartmental), T2 (extracompartmental). Breaching the cortex and extending into surrounding soft tissues indicates extracompartmental spread (T2). * Metastases (M): M0 (no metastases), M1 (regional or distant metastases). No skip lesions or distant metastases (M0). Therefore, a high-grade (G2), extracompartmental (T2) tumor without metastases (M0) is classified as Stage IIB. Stage III would indicate distant metastases (M1).
Question 43
A 40-year-old male presents with a 2-year history of progressive swelling and mild pain in his right anterior tibia. Radiographs show a lytic, expansile lesion in the mid-diaphysis of the tibia, with a "soap-bubble" appearance and cortical thickening. A biopsy reveals epithelial cells arranged in nests and cords within a fibrous stroma.
View Answer & Explanation
Correct Answer: C
Rationale: The patient's age (adult), chronic presentation, characteristic location (anterior tibia diaphysis), radiographic appearance (lytic, expansile, "soap-bubble," cortical thickening), and biopsy findings (epithelial cells in nests/cords) are pathognomonic for adamantinoma. Adamantinoma is a rare, low-grade malignant tumor almost exclusively found in the tibia. Osteosarcoma and Ewing sarcoma are typically more aggressive and have different histologies. Chondrosarcoma has a chondroid matrix. Fibrous dysplasia has a "ground glass" appearance.
Question 44
A 68-year-old female presents with a 9-month history of progressive lower back pain, radiating to her buttocks and perineum, accompanied by bowel and bladder dysfunction. MRI of the sacrum reveals a large, destructive lesion involving the S2-S4 vertebral bodies, with significant soft tissue extension. A biopsy confirms a malignant tumor composed of physaliferous cells.
View Answer & Explanation
Correct Answer: D
Rationale: The patient's age (older adult), location (sacrum, clivus, or vertebral bodies), destructive nature, and the presence of physaliferous cells (vacuolated cells with bubbly cytoplasm) on biopsy are classic for chordoma. Chordomas arise from remnants of the notochord. Osteosarcoma and chondrosarcoma are less common in this location and have different histologies. Multiple myeloma presents with punched-out lytic lesions and plasma cells. Metastatic carcinoma is a possibility but the specific cell type points to chordoma.
Question 45
A 4-year-old boy presents with a 3-month history of localized pain and swelling over his left parietal skull. Radiographs show a well-defined, lytic lesion in the parietal bone with a "beveled edge" appearance. A bone scan shows no other areas of increased uptake. Laboratory tests are unremarkable.
View Answer & Explanation
Correct Answer: C
Rationale: The patient's age (young child), lytic skull lesion, and "beveled edge" appearance are highly suggestive of Langerhans cell histiocytosis (LCH), specifically eosinophilic granuloma. LCH is a spectrum of disorders characterized by proliferation of Langerhans cells. While Ewing sarcoma and osteosarcoma can occur in children, they are less common in the skull and have different radiographic features. Neuroblastoma metastasis can cause lytic lesions but usually presents with systemic symptoms and multiple lesions. Chronic osteomyelitis would typically show sequestrum, involucrum, and periosteal reaction.
Question 46
A 15-year-old male presents with acute onset of severe pain and swelling in his right distal femur after a minor fall. Radiographs show a large, purely lytic, expansile lesion in the distal femoral metaphysis with cortical destruction. MRI reveals multiple fluid-fluid levels within the lesion. A biopsy confirms a high-grade malignant tumor with osteoid production.
View Answer & Explanation
Correct Answer: B
Rationale: The presence of multiple fluid-fluid levels on MRI within a purely lytic, expansile, and destructive lesion, combined with a biopsy showing osteoid production, is characteristic of telangiectatic osteosarcoma. This is a rare, aggressive variant of osteosarcoma that can mimic an aneurysmal bone cyst due to its hemorrhagic and cystic nature. While aneurysmal bone cysts also show fluid-fluid levels, they are benign and do not produce osteoid. Conventional osteosarcoma typically has a more solid appearance with varying degrees of osteoid matrix. Giant cell tumors are epiphyseal and lack osteoid. Chondrosarcoma has a chondroid matrix.
Question 47
A 30-year-old female presents with a slowly growing, painless mass on the posterior aspect of her left distal femur for several years. Radiographs show a densely ossified, lobulated mass arising from the posterior cortex of the distal femur, with a clear cleavage plane between the tumor and the underlying cortex. There is no involvement of the medullary canal.
View Answer & Explanation
Correct Answer: C
Rationale: The patient's age (adult), slow growth, posterior distal femur location, dense ossification, lobulated appearance, and clear cleavage plane from the underlying cortex without medullary involvement are classic features of parosteal osteosarcoma. This is a low-grade surface osteosarcoma. Osteochondromas have a cartilaginous cap and continuity with the medullary canal. Conventional osteosarcoma is intramedullary. Myositis ossificans is typically post-traumatic and matures from periphery to center. Juxtacortical chondroma is cartilaginous.
Question 48
A 17-year-old male presents with chronic knee pain, worse with activity. Radiographs show a well-defined, lytic lesion in the lateral femoral condyle epiphysis, with a sclerotic rim and punctate calcifications within the matrix. MRI confirms the epiphyseal location and shows no significant soft tissue extension.
View Answer & Explanation
Correct Answer: B
Rationale: The patient's age (adolescent), epiphyseal location, lytic lesion with a sclerotic rim, and punctate calcifications are characteristic of chondroblastoma. Giant cell tumors are also epiphyseal but typically occur in young adults, are purely lytic, and lack calcifications or a sclerotic rim. Unicameral bone cysts are metaphyseal. Osteoid osteomas have a nidus and reactive sclerosis. Subchondral cysts are typically associated with degenerative joint disease and are smaller.
Question 49
A 22-year-old male presents with persistent, dull back pain that is not significantly relieved by NSAIDs. Physical examination reveals localized tenderness over the L4 spinous process. Radiographs and CT show a lucent lesion in the posterior elements of L4, approximately 2.5 cm in diameter, with a central nidus and surrounding reactive sclerosis. The nidus is larger than 1.5 cm.
View Answer & Explanation
Correct Answer: B
Rationale: The patient's age (young adult), location (spine, posterior elements), and radiographic findings (lucent lesion with a central nidus and reactive sclerosis, nidus >1.5 cm) are characteristic of osteoblastoma. Osteoblastoma is often considered a "giant osteoid osteoma" as it shares similar histological features but is typically larger (>1.5-2 cm), less painful, and less responsive to NSAIDs compared to osteoid osteoma. Aneurysmal bone cysts are expansile and lytic with fluid levels. Ewing sarcoma is more aggressive with systemic symptoms. Spinal tuberculosis would show disc space narrowing and paravertebral abscesses.
Question 50
A 10-year-old girl presents with a 2-month history of progressive swelling and mild pain in her left distal tibia. Radiographs show an expansile, lytic lesion in the metaphysis of the distal tibia, with a thin cortex and septations. MRI reveals multiple fluid-fluid levels within the lesion.
View Answer & Explanation
Correct Answer: C
Rationale: The patient's age (child), metaphyseal location, expansile lytic lesion with septations, and characteristic fluid-fluid levels on MRI are diagnostic for an aneurysmal bone cyst (ABC). While telangiectatic osteosarcoma can also have fluid-fluid levels, it is a malignant tumor with osteoid production on biopsy, and the clinical presentation is often more aggressive. Unicameral bone cysts are typically unilocular and lack fluid-fluid levels. Fibrous dysplasia has a "ground glass" appearance. Chondroblastoma is epiphyseal.
Question 51
A 5-year-old boy presents with a limp and mild pain in his right hip. Radiographs of the hip show a well-defined, lytic lesion in the femoral neck metaphysis, with a sclerotic border. There is no periosteal reaction or soft tissue mass. The lesion is approximately 1.5 cm in diameter.
View Answer & Explanation
Correct Answer: C
Question 51
A 16-year-old male presents with 3 months of progressive right distal femur pain, worse at night and with activity. He denies trauma. Physical examination reveals a tender, warm, and swollen area over the distal femur. Radiographs show a destructive lesion in the metaphysis of the distal femur with a sunburst periosteal reaction and Codman's triangle. There is also evidence of soft tissue extension.
View Answer & Explanation
Correct Answer: C
Rationale: The classic presentation of an adolescent with progressive pain, a destructive metaphyseal lesion, sunburst periosteal reaction, Codman's triangle, and soft tissue extension is highly characteristic of osteosarcoma. Ewing sarcoma typically presents in a younger age group, often with an "onion skin" periosteal reaction and diaphyseal involvement. Chondrosarcoma is more common in older adults and typically shows chondroid matrix calcification. Giant cell tumor is epiphyseal/meta-epiphyseal and lytic. Aneurysmal bone cyst is expansile and lytic, lacking the aggressive periosteal reaction and soft tissue mass.
Question 51
An 8-year-old boy presents with left proximal tibia pain and swelling for 2 months, accompanied by intermittent fever and malaise. Physical examination reveals a tender, warm mass. Laboratory studies show elevated ESR and CRP. Radiographs demonstrate a large, lytic lesion in the diaphysis of the proximal tibia with an "onion skin" periosteal reaction and cortical destruction. There is also a large associated soft tissue mass.
View Answer & Explanation
Correct Answer: B
Rationale: The clinical picture of a young child with pain, swelling, systemic symptoms (fever, malaise, elevated inflammatory markers), a diaphyseal lytic lesion, "onion skin" periosteal reaction, and a large soft tissue mass is classic for Ewing sarcoma. While osteomyelitis can present with similar systemic symptoms and lytic lesions, the "onion skin" periosteal reaction and large soft tissue mass are more indicative of Ewing sarcoma. Osteosarcoma typically presents in adolescents with a sunburst reaction and metaphyseal involvement. Unicameral bone cysts are usually asymptomatic until fracture and lack aggressive features. Fibrous dysplasia has a characteristic "ground glass" appearance.
Question 51
A 65-year-old male presents with chronic, dull left hip pain that has progressively worsened over the past year. He has a history of multiple enchondromas in his left femur diagnosed 20 years ago. Radiographs show an ill-defined, destructive lesion in the proximal femur with mottled calcifications and cortical erosion. MRI reveals a large intramedullary lesion with lobulated contours, high signal on T2-weighted images, and cortical breakthrough.
View Answer & Explanation
Correct Answer: C
Rationale: The patient's age, chronic worsening pain, history of enchondromas, and radiographic findings of a destructive lesion with mottled calcifications and cortical erosion are highly suggestive of chondrosarcoma, likely arising from a pre-existing enchondroma. Enchondromas are typically asymptomatic unless fractured and do not show cortical erosion or progressive pain. Osteosarcoma would typically show osteoid matrix, not mottled calcifications. Fibrous dysplasia has a "ground glass" appearance. Metastatic carcinoma is a possibility in this age group but the chondroid matrix calcifications point towards chondrosarcoma.
Question 51
A 30-year-old female presents with progressive pain and swelling around her right knee for 6 months. Physical examination reveals a palpable mass over the distal femur. Radiographs show an expansile, purely lytic lesion in the meta-epiphyseal region of the distal femur, extending to the subchondral bone, with a narrow zone of transition and no significant periosteal reaction. CT scan confirms the lytic nature and absence of matrix mineralization.
View Answer & Explanation
Correct Answer: C
Rationale: The classic presentation of a young adult (20-40 years old) with a purely lytic, expansile lesion in the meta-epiphyseal region, extending to the subchondral bone, is highly characteristic of a Giant Cell Tumor (GCT). Chondroblastoma also occurs in the epiphysis but typically in younger patients (10-20s) and often has a sclerotic rim. Aneurysmal bone cysts can be expansile and lytic but are more common in younger patients and often have fluid-fluid levels. Unicameral bone cysts are typically metaphyseal and do not extend to the subchondral bone. Osteosarcoma would typically show osteoid matrix and an aggressive periosteal reaction.
Question 51
A 45-year-old male presents with incidental finding of a lesion in his left proximal humerus on a shoulder X-ray obtained for rotator cuff evaluation. He denies pain or other symptoms related to the lesion. Radiographs show a well-circumscribed, intramedullary lesion with punctate and ring-and-arc calcifications, located in the diaphysis. There is no cortical destruction, periosteal reaction, or soft tissue mass. MRI confirms the lesion is contained within the bone.
View Answer & Explanation
Correct Answer: B
Rationale: The asymptomatic nature, well-circumscribed intramedullary location, and characteristic punctate and ring-and-arc calcifications (chondroid matrix) without cortical destruction or periosteal reaction are classic features of an enchondroma. Chondrosarcoma would typically present with pain, cortical erosion, or soft tissue extension. Osteochondroma is an exostosis arising from the bone surface. Fibrous dysplasia has a "ground glass" appearance. Bone infarcts can calcify but usually have a serpiginous pattern and are often subchondral.
Question 51
A 12-year-old girl presents with a painless, hard bump near her right knee that she has had for several years. The bump has grown slowly with her. Physical examination reveals a firm, immobile mass arising from the metaphysis of the distal femur, pointing away from the joint. Radiographs confirm an exostosis with a continuous cortical and medullary canal connection to the underlying bone.
View Answer & Explanation
Correct Answer: D
Rationale: The presentation of a painless, slow-growing exostosis in a child or adolescent, arising from the metaphysis and pointing away from the joint, with cortical and medullary continuity with the parent bone, is pathognomonic for an osteochondroma. Osteosarcoma is malignant and would present with pain and aggressive features. Chondrosarcoma can arise from an osteochondroma but would typically present with new pain or growth after skeletal maturity. Osteoid osteoma causes nocturnal pain relieved by NSAIDs and has a nidus. Fibrous dysplasia is an intramedullary lesion.
Question 51
A 25-year-old female presents with a several-year history of progressive bowing deformity of her left tibia and recurrent pathological fractures. She denies pain at rest. Radiographs show an expansile, intramedullary lesion in the diaphysis of the tibia with a characteristic "ground glass" matrix, thinned cortex, and shepherd's crook deformity. There is no periosteal reaction or soft tissue mass.
View Answer & Explanation
Correct Answer: C
Rationale: The "ground glass" matrix, expansile intramedullary lesion, thinned cortex, and shepherd's crook deformity (especially in the proximal femur, though tibia is also common) are classic features of fibrous dysplasia. Adamantinoma is also a tibial lesion but is typically more aggressive and lytic/sclerotic. Osteofibrous dysplasia is a benign lesion of the tibia in children, but fibrous dysplasia is more common in adults with these specific radiographic features. Non-ossifying fibromas are typically smaller, cortical, and metaphyseal. Unicameral bone cysts are purely lytic and fluid-filled.
Question 51
A 14-year-old boy presents with sudden onset of severe right proximal humerus pain after a minor fall. Radiographs reveal an expansile, lytic lesion in the metaphysis of the proximal humerus with a "blown-out" appearance and cortical thinning. MRI shows multiple fluid-fluid levels within the lesion.
View Answer & Explanation
Correct Answer: C
Rationale: The expansile, lytic, "blown-out" appearance in the metaphysis of a child or adolescent, especially with characteristic fluid-fluid levels on MRI, is diagnostic of an Aneurysmal Bone Cyst (ABC). Unicameral bone cysts are also lytic and metaphyseal but typically do not show fluid-fluid levels and are more often centrally located. Telangiectatic osteosarcoma can also have fluid-fluid levels but is a malignant tumor with more aggressive features and osteoid matrix. Giant cell tumors are meta-epiphyseal and typically in young adults. Chondroblastoma is epiphyseal.
Question 51
A 7-year-old boy presents with a pathological fracture of his left proximal humerus after falling off his bicycle. He had no prior symptoms. Radiographs show a well-circumscribed, centrally located, lytic lesion in the metaphysis of the proximal humerus, with a "fallen leaf" sign visible within the lesion.
View Answer & Explanation
Correct Answer: C
Rationale: The "fallen leaf" sign (a fragment of cortical bone that has fallen to the bottom of a fluid-filled cavity) in a child with a pathological fracture through a centrally located, lytic metaphyseal lesion is pathognomonic for a Unicameral Bone Cyst (UBC), also known as a simple bone cyst. Aneurysmal bone cysts are typically expansile and often have fluid-fluid levels. Fibrous dysplasia has a "ground glass" appearance. Non-ossifying fibromas are usually cortical and eccentric. Enchondromas have chondroid matrix calcifications.
Question 51
A 22-year-old male presents with 6 months of progressively worsening right hip pain, particularly severe at night, which is reliably relieved by over-the-counter NSAIDs. Physical examination is unremarkable. Radiographs of the proximal femur are initially normal, but a subsequent CT scan reveals a small, lucent nidus (less than 1.5 cm) surrounded by dense cortical sclerosis in the femoral neck.
View Answer & Explanation
Correct Answer: C
Rationale: The classic presentation of nocturnal pain relieved by NSAIDs, along with a small lucent nidus (typically <1.5-2 cm) surrounded by reactive sclerosis, is diagnostic of an osteoid osteoma. Osteoblastoma is similar but has a larger nidus (>2 cm) and less reactive sclerosis, and pain is less reliably relieved by NSAIDs. Osteosarcoma is malignant and would have aggressive features. Stress fractures can cause pain but lack a nidus. Brodie's abscess (chronic osteomyelitis) can cause sclerosis but usually has a more irregular lytic center and may have systemic symptoms.
Question 51
A 17-year-old male presents with chronic left knee pain, worse with activity. Radiographs show a well-defined, lytic lesion in the epiphysis of the distal femur with a sclerotic rim and punctate calcifications. MRI confirms the epiphyseal location and shows surrounding bone marrow edema.
View Answer & Explanation
Correct Answer: C
Rationale: Chondroblastoma is a benign cartilaginous tumor typically found in the epiphysis or apophysis of long bones in adolescents and young adults. The radiographic features of a well-defined, lytic epiphyseal lesion with a sclerotic rim and punctate calcifications are characteristic. Giant cell tumor is also epiphyseal but typically occurs in slightly older patients (20-40s) and is purely lytic without calcifications or a sclerotic rim. Aneurysmal bone cysts are metaphyseal. Osteoid osteoma has a nidus and reactive sclerosis. Subchondral cysts are typically associated with degenerative joint disease.
Question 51
A 55-year-old male presents with progressive low back pain, radiating down his left leg, and recent onset of bowel and bladder dysfunction. Neurological examination reveals saddle anesthesia and diminished anal tone. MRI of the spine shows a destructive lesion involving the S2 vertebral body, extending into the sacral canal, with a lobulated appearance and high signal on T2-weighted images.
View Answer & Explanation
Correct Answer: D
Rationale: Chordoma is a rare, slow-growing malignant tumor arising from notochordal remnants, most commonly found in the sacrococcygeal region (50-60%), followed by the spheno-occipital region (30-40%) and cervical spine (10-15%). The patient's age, location (sacrum), progressive neurological deficits, and MRI findings of a destructive, lobulated lesion with high T2 signal are highly suggestive of chordoma. Chondrosarcoma can occur in the spine but is less common in the sacrum and typically has chondroid matrix. Metastatic carcinoma is a possibility but chordoma is the most likely primary bone tumor in this specific location and presentation. Giant cell tumor is rare in the sacrum and Ewing sarcoma is typically in younger patients.
Question 51
A 40-year-old male presents with a 2-year history of progressive swelling and mild pain in his left lower leg. Physical examination reveals a firm, non-tender mass in the mid-tibia. Radiographs show a well-defined, eccentric, lytic lesion in the diaphysis of the tibia with areas of sclerosis and a "soap bubble" appearance. There is cortical thickening and some periosteal reaction.
View Answer & Explanation
Correct Answer: C
Rationale: Adamantinoma is a rare, low-grade malignant tumor almost exclusively found in the tibia. It typically presents in young to middle-aged adults with slow-growing pain and swelling. Radiographically, it appears as an eccentric, lytic lesion with a "soap bubble" appearance, often with sclerotic areas, cortical thickening, and sometimes periosteal reaction. Fibrous dysplasia has a "ground glass" appearance. Osteofibrous dysplasia is a benign lesion of the tibia in children. Chondrosarcoma would show chondroid matrix. Non-ossifying fibromas are typically smaller, cortical, and asymptomatic.
Question 51
A 35-year-old male presents with new onset of dull, aching pain in his left hip, which has been present for 3 months. He has a known history of multiple hereditary exostoses, and a large osteochondroma has been present on his left ilium since childhood. Radiographs now show irregular enlargement of the cartilaginous cap of the iliac osteochondroma, with focal areas of lucency and cortical erosion. MRI confirms a cartilaginous cap thickness greater than 2 cm.
View Answer & Explanation
Correct Answer: C
Rationale: Malignant transformation of an osteochondroma to a secondary peripheral chondrosarcoma is a known complication, especially in patients with multiple hereditary exostoses. Key indicators of malignant transformation in an adult include new onset or worsening pain, continued growth after skeletal maturity, and radiographic findings such as irregular enlargement of the cartilaginous cap (especially >2 cm in adults), focal lucencies, and cortical erosion. A new osteochondroma would not typically cause pain or show these aggressive features. Traumatic injury might cause acute pain but not cap thickening. Inflammatory reactions are less common and would not explain cap thickening. Benign growth spurts do not occur after skeletal maturity.
Question 51
A 15-year-old male presents with a rapidly growing, painful mass in his distal femur. Radiographs show an expansile, lytic lesion with cortical destruction and a "sunburst" periosteal reaction. MRI reveals multiple fluid-fluid levels within the lesion, mimicking an aneurysmal bone cyst. Biopsy is performed.
View Answer & Explanation
Correct Answer: C
Rationale: Telangiectatic osteosarcoma is a highly aggressive variant of osteosarcoma that can mimic an aneurysmal bone cyst (ABC) due to its expansile lytic nature and the presence of fluid-fluid levels on MRI. However, the rapid growth, significant pain, cortical destruction, and "sunburst" periosteal reaction are aggressive features more consistent with osteosarcoma. Aneurysmal bone cysts are benign and typically lack the aggressive periosteal reaction and rapid growth. Giant cell tumors are meta-epiphyseal. Unicameral bone cysts are typically asymptomatic until fracture. Chondroblastoma is epiphyseal.
Question 51
A 10-year-old boy presents with left thigh pain and swelling. Radiographs show a lytic lesion in the mid-diaphysis of the femur with multiple concentric layers of new bone formation, giving an "onion skin" appearance. This type of periosteal reaction is most commonly associated with which of the following primary bone tumors?
View Answer & Explanation
Correct Answer: C
Rationale: The "onion skin" (lamellated) periosteal reaction, characterized by multiple concentric layers of new bone, is a classic radiographic feature most commonly associated with Ewing sarcoma, particularly in diaphyseal lesions. It represents intermittent growth of the tumor, lifting the periosteum. Osteosarcoma typically presents with a "sunburst" or Codman's triangle periosteal reaction. Chondrosarcoma usually has little to no periosteal reaction unless aggressive. Osteoid osteoma causes dense reactive sclerosis. Giant cell tumors are purely lytic and lack significant periosteal reaction.
Question 51
A 45-year-old male is diagnosed with a suspected high-grade chondrosarcoma of the proximal humerus based on imaging. The orthopedic oncologist plans a biopsy. Which of the following is the most critical principle to adhere to during the biopsy procedure?
View Answer & Explanation
Correct Answer: C
Rationale: For suspected malignant bone tumors, the biopsy tract must be meticulously planned so that it can be completely excised en bloc with the tumor during the definitive surgical resection. This minimizes the risk of tumor cell contamination of surrounding tissues, which could compromise limb salvage or local recurrence rates. Excisional biopsy is generally contraindicated for suspected malignancies as it can spread tumor cells. While ample tissue is needed, the incision must be planned for definitive surgery. Avoiding biopsy is incorrect; histological confirmation is crucial. Fine-needle aspiration may not provide sufficient tissue for accurate grading and diagnosis of bone sarcomas.
Question 51
A 16-year-old male is diagnosed with a high-grade osteosarcoma of the distal femur. Staging studies, including MRI of the femur, CT chest, and bone scan, show no evidence of metastatic disease. According to the Enneking surgical staging system for musculoskeletal sarcomas, what is the appropriate stage for this tumor?
View Answer & Explanation
Correct Answer: D
Rationale: The Enneking surgical staging system classifies musculoskeletal sarcomas based on grade (G), local extent (T), and presence of metastases (M). - Grade (G): G1 (low grade), G2 (high grade). Osteosarcoma is inherently high grade (G2). - Local Extent (T): T1 (intracompartmental), T2 (extracompartmental). Distal femur osteosarcoma often extends extracompartmentally (T2). - Metastases (M): M0 (no metastases), M1 (metastases present). Given a high-grade osteosarcoma (G2) without metastatic disease (M0), the stage depends on local extent. Assuming it's extracompartmental (as most osteosarcomas are), it would be Stage IIB (G2, T2, M0). If it were strictly intracompartmental, it would be Stage IIA. However, high-grade osteosarcomas are rarely truly intracompartmental. Stage III indicates metastatic disease (M1).
Question 51
A 6-year-old boy presents with a pathological fracture of the proximal humerus. Radiographs show a large, expansile, purely lytic lesion in the metaphysis. There is no periosteal reaction or matrix mineralization. Which of the following is the most likely diagnosis?
View Answer & Explanation
Correct Answer: C
Rationale: In a young child (under 10-12 years old) with a pathological fracture through a purely lytic, metaphyseal lesion without aggressive features like periosteal reaction or matrix, a unicameral bone cyst (UBC) is the most common diagnosis. Aneurysmal bone cysts (ABCs) are also lytic and expansile but typically occur in slightly older children/adolescents and often show fluid-fluid levels. Osteosarcoma and Ewing sarcoma are malignant and would typically show aggressive features (periosteal reaction, soft tissue mass, rapid growth). Chondroblastoma is epiphyseal.
Question 51
A 70-year-old male presents with new onset of severe, unremitting back pain. Radiographs of the lumbar spine show a dense, sclerotic lesion involving a vertebral body, with associated cortical thickening and no obvious lytic component. A bone scan shows increased uptake in the affected vertebra. Which of the following is the most likely diagnosis?
View Answer & Explanation
Correct Answer: D
Rationale: In an elderly male with a new, dense sclerotic vertebral lesion and increased uptake on bone scan, metastatic prostate carcinoma is the most likely diagnosis. Prostate cancer is notorious for causing osteoblastic (sclerotic) metastases. While Paget's disease can cause sclerotic lesions, it often has mixed lytic/sclerotic features and is typically asymptomatic until complications arise. Osteoid osteoma is typically in younger patients and much smaller. Osteosarcoma is rare in this age group as a primary tumor and usually has a lytic component. Chondrosarcoma is typically lytic with chondroid matrix.
Question 52
A 16-year-old male presents with 3 months of progressive right distal femur pain, worse at night and with activity. He denies trauma. Physical examination reveals a tender, warm, and swollen area over the distal femur. Radiographs show a destructive lesion in the metaphysis of the distal femur with a sunburst periosteal reaction and Codman's triangle. There is also evidence of soft tissue extension.
View Answer & Explanation
Correct Answer: C
Rationale: The classic presentation of an adolescent with progressive pain, a destructive metaphyseal lesion, sunburst periosteal reaction, Codman's triangle, and soft tissue extension is highly characteristic of osteosarcoma. Ewing sarcoma typically presents in a younger age group, often with an "onion skin" periosteal reaction and diaphyseal involvement. Chondrosarcoma is more common in older adults and typically shows chondroid matrix calcification. Giant cell tumor is epiphyseal/meta-epiphyseal and lytic. Aneurysmal bone cyst is expansile and lytic, lacking the aggressive periosteal reaction and soft tissue mass.
Question 53
An 8-year-old boy presents with left proximal tibia pain and swelling for 2 months, accompanied by intermittent fever and malaise. Physical examination reveals a tender, warm mass. Laboratory studies show elevated ESR and CRP. Radiographs demonstrate a large, lytic lesion in the diaphysis of the proximal tibia with an "onion skin" periosteal reaction and cortical destruction. There is also a large associated soft tissue mass.
View Answer & Explanation
Correct Answer: B
Rationale: The clinical picture of a young child with pain, swelling, systemic symptoms (fever, malaise, elevated inflammatory markers), a diaphyseal lytic lesion, "onion skin" periosteal reaction, and a large soft tissue mass is classic for Ewing sarcoma. While osteomyelitis can present with similar systemic symptoms and lytic lesions, the "onion skin" periosteal reaction and large soft tissue mass are more indicative of Ewing sarcoma. Osteosarcoma typically presents in adolescents with a sunburst reaction and metaphyseal involvement. Unicameral bone cysts are usually asymptomatic until fracture and lack aggressive features. Fibrous dysplasia has a characteristic "ground glass" appearance.
Question 54
A 65-year-old male presents with chronic, dull left hip pain that has progressively worsened over the past year. He has a history of multiple enchondromas in his left femur diagnosed 20 years ago. Radiographs show an ill-defined, destructive lesion in the proximal femur with mottled calcifications and cortical erosion. MRI reveals a large intramedullary lesion with lobulated contours, high signal on T2-weighted images, and cortical breakthrough.
View Answer & Explanation
Correct Answer: C
Rationale: The patient's age, chronic worsening pain, history of enchondromas, and radiographic findings of a destructive lesion with mottled calcifications and cortical erosion are highly suggestive of chondrosarcoma, likely arising from a pre-existing enchondroma. Enchondromas are typically asymptomatic unless fractured and do not show cortical erosion or progressive pain. Osteosarcoma would typically show osteoid matrix, not mottled calcifications. Fibrous dysplasia has a "ground glass" appearance. Metastatic carcinoma is a possibility in this age group but the chondroid matrix calcifications point towards chondrosarcoma.
Question 55
A 30-year-old female presents with progressive pain and swelling around her right knee for 6 months. Physical examination reveals a palpable mass over the distal femur. Radiographs show an expansile, purely lytic lesion in the meta-epiphyseal region of the distal femur, extending to the subchondral bone, with a narrow zone of transition and no significant periosteal reaction. CT scan confirms the lytic nature and absence of matrix mineralization.
View Answer & Explanation
Correct Answer: C
Rationale: The classic presentation of a young adult (20-40 years old) with a purely lytic, expansile lesion in the meta-epiphyseal region, extending to the subchondral bone, is highly characteristic of a Giant Cell Tumor (GCT). Chondroblastoma also occurs in the epiphysis but typically in younger patients (10-20s) and often has a sclerotic rim. Aneurysmal bone cysts can be expansile and lytic but are more common in younger patients and often have fluid-fluid levels. Unicameral bone cysts are typically metaphyseal and do not extend to the subchondral bone. Osteosarcoma would typically show osteoid matrix and an aggressive periosteal reaction.
Question 56
A 45-year-old male presents with incidental finding of a lesion in his left proximal humerus on a shoulder X-ray obtained for rotator cuff evaluation. He denies pain or other symptoms related to the lesion. Radiographs show a well-circumscribed, intramedullary lesion with punctate and ring-and-arc calcifications, located in the diaphysis. There is no cortical destruction, periosteal reaction, or soft tissue mass. MRI confirms the lesion is contained within the bone.
View Answer & Explanation
Correct Answer: B
Rationale: The asymptomatic nature, well-circumscribed intramedullary location, and characteristic punctate and ring-and-arc calcifications (chondroid matrix) without cortical destruction or periosteal reaction are classic features of an enchondroma. Chondrosarcoma would typically present with pain, cortical erosion, or soft tissue extension. Osteochondroma is an exostosis arising from the bone surface. Fibrous dysplasia has a "ground glass" appearance. Bone infarcts can calcify but usually have a serpiginous pattern and are often subchondral.
Question 57
A 12-year-old girl presents with a painless, hard bump near her right knee that she has had for several years. The bump has grown slowly with her. Physical examination reveals a firm, immobile mass arising from the metaphysis of the distal femur, pointing away from the joint. Radiographs confirm an exostosis with a continuous cortical and medullary canal connection to the underlying bone.
View Answer & Explanation
Correct Answer: D
Rationale: The presentation of a painless, slow-growing exostosis in a child or adolescent, arising from the metaphysis and pointing away from the joint, with cortical and medullary continuity with the parent bone, is pathognomonic for an osteochondroma. Osteosarcoma is malignant and would present with pain and aggressive features. Chondrosarcoma can arise from an osteochondroma but would typically present with new pain or growth after skeletal maturity. Osteoid osteoma causes nocturnal pain relieved by NSAIDs and has a nidus. Fibrous dysplasia is an intramedullary lesion.
Question 58
A 25-year-old female presents with a several-year history of progressive bowing deformity of her left tibia and recurrent pathological fractures. She denies pain at rest. Radiographs show an expansile, intramedullary lesion in the diaphysis of the tibia with a characteristic "ground glass" matrix, thinned cortex, and shepherd's crook deformity. There is no periosteal reaction or soft tissue mass.
View Answer & Explanation
Correct Answer: C
Rationale: The "ground glass" matrix, expansile intramedullary lesion, thinned cortex, and shepherd's crook deformity (especially in the proximal femur, though tibia is also common) are classic features of fibrous dysplasia. Adamantinoma is also a tibial lesion but is typically more aggressive and lytic/sclerotic. Osteofibrous dysplasia is a benign lesion of the tibia in children, but fibrous dysplasia is more common in adults with these specific radiographic features. Non-ossifying fibromas are typically smaller, cortical, and metaphyseal. Unicameral bone cysts are purely lytic and fluid-filled.
Question 59
A 14-year-old boy presents with sudden onset of severe right proximal humerus pain after a minor fall. Radiographs reveal an expansile, lytic lesion in the metaphysis of the proximal humerus with a "blown-out" appearance and cortical thinning. MRI shows multiple fluid-fluid levels within the lesion.
View Answer & Explanation
Correct Answer: C
Rationale: The expansile, lytic, "blown-out" appearance in the metaphysis of a child or adolescent, especially with characteristic fluid-fluid levels on MRI, is diagnostic of an Aneurysmal Bone Cyst (ABC). Unicameral bone cysts are also lytic and metaphyseal but typically do not show fluid-fluid levels and are more often centrally located. Telangiectatic osteosarcoma can also have fluid-fluid levels but is a malignant tumor with more aggressive features and osteoid matrix. Giant cell tumors are meta-epiphyseal and typically in young adults. Chondroblastoma is epiphyseal.
Question 60
A 7-year-old boy presents with a pathological fracture of his left proximal humerus after falling off his bicycle. He had no prior symptoms. Radiographs show a well-circumscribed, centrally located, lytic lesion in the metaphysis of the proximal humerus, with a "fallen leaf" sign visible within the lesion.
View Answer & Explanation
Correct Answer: C
Rationale: The "fallen leaf" sign (a fragment of cortical bone that has fallen to the bottom of a fluid-filled cavity) in a child with a pathological fracture through a centrally located, lytic metaphyseal lesion is pathognomonic for a Unicameral Bone Cyst (UBC), also known as a simple bone cyst. Aneurysmal bone cysts are typically expansile and often have fluid-fluid levels. Fibrous dysplasia has a "ground glass" appearance. Non-ossifying fibromas are usually cortical and eccentric. Enchondromas have chondroid matrix calcifications.
Question 61
A 22-year-old male presents with 6 months of progressively worsening right hip pain, particularly severe at night, which is reliably relieved by over-the-counter NSAIDs. Physical examination is unremarkable. Radiographs of the proximal femur are initially normal, but a subsequent CT scan reveals a small, lucent nidus (less than 1.5 cm) surrounded by dense cortical sclerosis in the femoral neck.
View Answer & Explanation
Correct Answer: C
Rationale: The classic presentation of nocturnal pain relieved by NSAIDs, along with a small lucent nidus (typically <1.5-2 cm) surrounded by reactive sclerosis, is diagnostic of an osteoid osteoma. Osteoblastoma is similar but has a larger nidus (>2 cm) and less reactive sclerosis, and pain is less reliably relieved by NSAIDs. Osteosarcoma is malignant and would have aggressive features. Stress fractures can cause pain but lack a nidus. Brodie's abscess (chronic osteomyelitis) can cause sclerosis but usually has a more irregular lytic center and may have systemic symptoms.
Question 62
A 17-year-old male presents with chronic left knee pain, worse with activity. Radiographs show a well-defined, lytic lesion in the epiphysis of the distal femur with a sclerotic rim and punctate calcifications. MRI confirms the epiphyseal location and shows surrounding bone marrow edema.
View Answer & Explanation
Correct Answer: C
Rationale: Chondroblastoma is a benign cartilaginous tumor typically found in the epiphysis or apophysis of long bones in adolescents and young adults. The radiographic features of a well-defined, lytic epiphyseal lesion with a sclerotic rim and punctate calcifications are characteristic. Giant cell tumor is also epiphyseal but typically occurs in slightly older patients (20-40s) and is purely lytic without calcifications or a sclerotic rim. Aneurysmal bone cysts are metaphyseal. Osteoid osteoma has a nidus and reactive sclerosis. Subchondral cysts are typically associated with degenerative joint disease.
Question 63
A 55-year-old male presents with progressive low back pain, radiating down his left leg, and recent onset of bowel and bladder dysfunction. Neurological examination reveals saddle anesthesia and diminished anal tone. MRI of the spine shows a destructive lesion involving the S2 vertebral body, extending into the sacral canal, with a lobulated appearance and high signal on T2-weighted images.
View Answer & Explanation
Correct Answer: D
Rationale: Chordoma is a rare, slow-growing malignant tumor arising from notochordal remnants, most commonly found in the sacrococcygeal region (50-60%), followed by the spheno-occipital region (30-40%) and cervical spine (10-15%). The patient's age, location (sacrum), progressive neurological deficits, and MRI findings of a destructive, lobulated lesion with high T2 signal are highly suggestive of chordoma. Chondrosarcoma can occur in the spine but is less common in the sacrum and typically has chondroid matrix. Metastatic carcinoma is a possibility but chordoma is the most likely primary bone tumor in this specific location and presentation. Giant cell tumor is rare in the sacrum and Ewing sarcoma is typically in younger patients.
Question 64
A 40-year-old male presents with a 2-year history of progressive swelling and mild pain in his left lower leg. Physical examination reveals a firm, non-tender mass in the mid-tibia. Radiographs show a well-defined, eccentric, lytic lesion in the diaphysis of the tibia with areas of sclerosis and a "soap bubble" appearance. There is cortical thickening and some periosteal reaction.
View Answer & Explanation
Correct Answer: C
Rationale: Adamantinoma is a rare, low-grade malignant tumor almost exclusively found in the tibia. It typically presents in young to middle-aged adults with slow-growing pain and swelling. Radiographically, it appears as an eccentric, lytic lesion with a "soap bubble" appearance, often with sclerotic areas, cortical thickening, and sometimes periosteal reaction. Fibrous dysplasia has a "ground glass" appearance. Osteofibrous dysplasia is a benign lesion of the tibia in children. Chondrosarcoma would show chondroid matrix. Non-ossifying fibromas are typically smaller, cortical, and asymptomatic.
Question 65
A 35-year-old male presents with new onset of dull, aching pain in his left hip, which has been present for 3 months. He has a known history of multiple hereditary exostoses, and a large osteochondroma has been present on his left ilium since childhood. Radiographs now show irregular enlargement of the cartilaginous cap of the iliac osteochondroma, with focal areas of lucency and cortical erosion. MRI confirms a cartilaginous cap thickness greater than 2 cm.
View Answer & Explanation
Correct Answer: C
Rationale: Malignant transformation of an osteochondroma to a secondary peripheral chondrosarcoma is a known complication, especially in patients with multiple hereditary exostoses. Key indicators of malignant transformation in an adult include new onset or worsening pain, continued growth after skeletal maturity, and radiographic findings such as irregular enlargement of the cartilaginous cap (especially >2 cm in adults), focal lucencies, and cortical erosion. A new osteochondroma would not typically cause pain or show these aggressive features. Traumatic injury might cause acute pain but not cap thickening. Inflammatory reactions are less common and would not explain cap thickening. Benign growth spurts do not occur after skeletal maturity.
Question 66
A 15-year-old male presents with a rapidly growing, painful mass in his distal femur. Radiographs show an expansile, lytic lesion with cortical destruction and a "sunburst" periosteal reaction. MRI reveals multiple fluid-fluid levels within the lesion, mimicking an aneurysmal bone cyst. Biopsy is performed.
View Answer & Explanation
Correct Answer: C
Rationale: Telangiectatic osteosarcoma is a highly aggressive variant of osteosarcoma that can mimic an aneurysmal bone cyst (ABC) due to its expansile lytic nature and the presence of fluid-fluid levels on MRI. However, the rapid growth, significant pain, cortical destruction, and "sunburst" periosteal reaction are aggressive features more consistent with osteosarcoma. Aneurysmal bone cysts are benign and typically lack the aggressive periosteal reaction and rapid growth. Giant cell tumors are meta-epiphyseal. Unicameral bone cysts are typically asymptomatic until fracture. Chondroblastoma is epiphyseal.
Question 67
A 10-year-old boy presents with left thigh pain and swelling. Radiographs show a lytic lesion in the mid-diaphysis of the femur with multiple concentric layers of new bone formation, giving an "onion skin" appearance. This type of periosteal reaction is most commonly associated with which of the following primary bone tumors?
View Answer & Explanation
Correct Answer: C
Rationale: The "onion skin" (lamellated) periosteal reaction, characterized by multiple concentric layers of new bone, is a classic radiographic feature most commonly associated with Ewing sarcoma, particularly in diaphyseal lesions. It represents intermittent growth of the tumor, lifting the periosteum. Osteosarcoma typically presents with a "sunburst" or Codman's triangle periosteal reaction. Chondrosarcoma usually has little to no periosteal reaction unless aggressive. Osteoid osteoma causes dense reactive sclerosis. Giant cell tumors are purely lytic and lack significant periosteal reaction.
Question 68
A 45-year-old male is diagnosed with a suspected high-grade chondrosarcoma of the proximal humerus based on imaging. The orthopedic oncologist plans a biopsy. Which of the following is the most critical principle to adhere to during the biopsy procedure?
View Answer & Explanation
Correct Answer: C
Rationale: For suspected malignant bone tumors, the biopsy tract must be meticulously planned so that it can be completely excised en bloc with the tumor during the definitive surgical resection. This minimizes the risk of tumor cell contamination of surrounding tissues, which could compromise limb salvage or local recurrence rates. Excisional biopsy is generally contraindicated for suspected malignancies as it can spread tumor cells. While ample tissue is needed, the incision must be planned for definitive surgery. Avoiding biopsy is incorrect; histological confirmation is crucial. Fine-needle aspiration may not provide sufficient tissue for accurate grading and diagnosis of bone sarcomas.
Question 69
A 16-year-old male is diagnosed with a high-grade osteosarcoma of the distal femur. Staging studies, including MRI of the femur, CT chest, and bone scan, show no evidence of metastatic disease. According to the Enneking surgical staging system for musculoskeletal sarcomas, what is the appropriate stage for this tumor?
View Answer & Explanation
Correct Answer: D
Rationale: The Enneking surgical staging system classifies musculoskeletal sarcomas based on grade (G), local extent (T), and presence of metastases (M). - Grade (G): G1 (low grade), G2 (high grade). Osteosarcoma is inherently high grade (G2). - Local Extent (T): T1 (intracompartmental), T2 (extracompartmental). Distal femur osteosarcoma often extends extracompartmentally (T2). - Metastases (M): M0 (no metastases), M1 (metastases present). Given a high-grade osteosarcoma (G2) without metastatic disease (M0), the stage depends on local extent. Assuming it's extracompartmental (as most osteosarcomas are), it would be Stage IIB (G2, T2, M0). If it were strictly intracompartmental, it would be Stage IIA. However, high-grade osteosarcomas are rarely truly intracompartmental. Stage III indicates metastatic disease (M1).
Question 70
A 6-year-old boy presents with a pathological fracture of the proximal humerus. Radiographs show a large, expansile, purely lytic lesion in the metaphysis. There is no periosteal reaction or matrix mineralization. Which of the following is the most likely diagnosis?
View Answer & Explanation
Correct Answer: C
Rationale: In a young child (under 10-12 years old) with a pathological fracture through a purely lytic, metaphyseal lesion without aggressive features like periosteal reaction or matrix, a unicameral bone cyst (UBC) is the most common diagnosis. Aneurysmal bone cysts (ABCs) are also lytic and expansile but typically occur in slightly older children/adolescents and often show fluid-fluid levels. Osteosarcoma and Ewing sarcoma are malignant and would typically show aggressive features (periosteal reaction, soft tissue mass, rapid growth). Chondroblastoma is epiphyseal.
Question 71
A 48-year-old male presents with progressive weakness and sensory changes in his upper extremities. Imaging reveals a fluid-filled cavity within his cervical spinal cord.
View Answer & Explanation
Correct Answer: C
Rationale: Syringomyelia is defined as a disorder in which a cyst or tubular cavity (syrinx) forms within the spinal cord, expanding and destroying the central cord. This is the primary pathological process. Demyelination (A) is characteristic of conditions like multiple sclerosis, while primary spinal cord tumors (D) are distinct entities. Ischemic necrosis (B) or autoimmune inflammation (E) are not the defining features of syringomyelia.
Question 72
A 55-year-old female reports a several-month history of burning pain and numbness in her hands, particularly noticing she can't feel extreme temperatures. Neurological exam confirms diminished pain and temperature sensation in a cape-like distribution.
View Answer & Explanation
Correct Answer: D
Rationale: A classic symptom of syringomyelia, due to damage to the spinothalamic tracts crossing in the central cord, is the loss of the ability to feel extremes of hot or cold, especially in the hands, often in a "cape-like" distribution. Loss of proprioception (A), vibration sense (B), and two-point discrimination (C) are associated with dorsal column damage. Glove-and-stocking neuropathy (E) is more typical of peripheral neuropathies.
Question 73
A 62-year-old male with a known history of syringomyelia presents with significant swelling, instability, and crepitus in his right shoulder. Radiographs show extensive joint destruction.
View Answer & Explanation
Correct Answer: D
Rationale: In syringomyelia, neuropathic changes (Charcot's joint) are most common in the shoulder joint, followed by the elbow and wrist. The knee (A), hip (B), and ankle (C) are more commonly affected in other causes of Charcot arthropathy, such as diabetes or tabes dorsalis.
Question 74
A 39-year-old female presents with progressive neck stiffness, arm weakness, and a dissociated sensory loss. Syringomyelia is suspected.
View Answer & Explanation
Correct Answer: C
Rationale: MRI is the gold standard for diagnosing syringomyelia as it clearly visualizes the syrinx formation within the spinal cord. X-rays (A) and CT scans (B) are less effective for visualizing soft tissue structures like the spinal cord and syrinx. EMG (D) and nerve conduction studies (E) assess nerve and muscle function but do not directly visualize the syrinx.
Question 75
A 50-year-old male presents with chronic neck pain and upper extremity weakness. An MRI of the cervical spine is performed.

View Answer & Explanation
Correct Answer: C
Rationale: The provided image caption explicitly states, "The MRI finding – the syrinx formation in the cervical cord – confirms the correct diagnosis of syringomyelia." This is the characteristic and diagnostic finding. While other conditions like spinal stenosis (D) or disc herniation (B) can cause similar symptoms, they are not the primary pathology of syringomyelia. Spinal cord atrophy (A) can be a secondary finding but not the primary diagnostic feature.
Question 76
A 68-year-old male with a long-standing history of syringomyelia presents with a grossly enlarged and unstable left shoulder joint, with minimal pain despite significant deformity.
View Answer & Explanation
Correct Answer: D
Rationale: The description of a significantly enlarged, unstable, and deformed joint with minimal pain despite extensive destruction, in the context of syringomyelia, is classic for neurogenic osteoarthropathy, also known as Charcot's joint. This condition results from repetitive microtrauma due to loss of protective sensation. Septic arthritis (C) would typically be acutely painful and associated with systemic signs of infection. Rotator cuff tear (A) and adhesive capsulitis (B) present differently and do not typically lead to such gross joint destruction. Avascular necrosis (E) involves bone death but not the same pattern of joint disorganization and enlargement.
Question 77
A 70-year-old female with syringomyelia presents with progressive destruction of her right shoulder. A CT scan is performed.
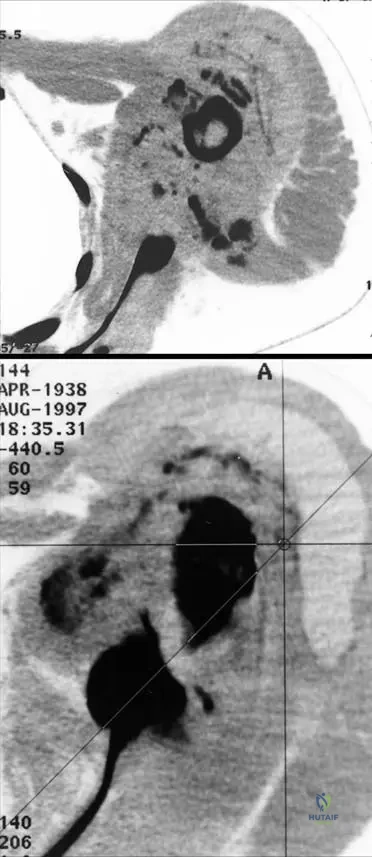
View Answer & Explanation
Correct Answer: D
Rationale: The image caption for Fig. 4.7 explicitly states, "3D CT visualizes better the destruction of the shoulder joint and the extensive soft tissue ossification." This is a hallmark finding of severe neurogenic osteoarthropathy. Options A, B, C, and E describe findings inconsistent with advanced Charcot arthropathy.
Question 78
A 58-year-old male with syringomyelia develops a Charcot joint in his elbow.
View Answer & Explanation
Correct Answer: C
Rationale: The joint destruction in neurogenic osteoarthropathy (Charcot's joint) is primarily attributed to the loss of protective sensation, leading to unrecognized and repetitive microtrauma. This constant stress on the joint, without the normal pain signals to limit activity, results in progressive destruction. While inflammation can be present, it is secondary to the trauma, not the primary cause (A). Bacterial infection (B) is septic arthritis, a different condition. Metabolic bone disease (D) or primary ligamentous laxity (E) are not the underlying mechanisms for Charcot arthropathy.
Question 79
A 42-year-old female is diagnosed with syringomyelia after presenting with a cape-like sensory loss and upper extremity weakness.
View Answer & Explanation
Correct Answer: C
Rationale: The clinical context provided, including symptoms like neck stiffness, arm weakness, and cape-like sensory loss, points to a cervical spinal cord lesion. The text also mentions that the MRI finding of syrinx formation in the cervical cord confirms the diagnosis. While a syrinx can theoretically occur at any level, the cervical region is the most common location for syringomyelia, especially when associated with Chiari malformations.
Question 80
A 53-year-old male with syringomyelia reports difficulty discerning hot from cold water with his hands.
View Answer & Explanation
Correct Answer: C
Rationale: The spinothalamic tract carries pain and temperature sensation. In syringomyelia, the syrinx expands centrally, damaging the decussating fibers of the spinothalamic tract, leading to a dissociated sensory loss where pain and temperature are affected, but touch, vibration, and proprioception (carried by the dorsal columns, A) are preserved. The corticospinal tract (B) is involved in motor control, while rubrospinal (D) and vestibulospinal (E) tracts are also motor pathways.
Question 81
A 65-year-old female with syringomyelia has developed neurogenic osteoarthropathy in her left shoulder. She is concerned about other joints.
View Answer & Explanation
Correct Answer: C
Rationale: The clinical text explicitly states that in syringomyelia, neuropathic changes are common in the shoulder joint, followed by the elbow and wrist. This pattern reflects the typical distribution of sensory loss and neurological deficits in cervical syringomyelia. Hip and knee (A) or ankle and foot (B) are more commonly affected in Charcot arthropathy due to other conditions like diabetes or tabes dorsalis, which primarily affect lower extremity sensation.
Question 82
A 60-year-old male with suspected Charcot arthropathy of the shoulder undergoes bone scintigraphy.
View Answer & Explanation
Correct Answer: D
Question 82
A 45-year-old male presents with progressive weakness and stiffness in his left arm and shoulder over the past year. He also reports a peculiar inability to feel extreme temperatures, particularly in his hands, but touch sensation seems relatively preserved. Physical examination reveals atrophy of intrinsic hand muscles and a significantly enlarged, unstable left shoulder joint with crepitus. Radiographs show severe destruction of the glenohumeral joint with extensive periarticular ossification. An MRI of the cervical spine is ordered.

View Answer & Explanation
Correct Answer: C
Rationale: The constellation of symptoms including progressive weakness, stiffness, loss of temperature sensation (dissociated sensory loss), muscle atrophy, and a neuropathic (Charcot) joint in the shoulder is highly characteristic of syringomyelia. The MRI finding of a syrinx in the cervical cord would confirm this diagnosis. Cervical disc herniation might cause weakness and sensory changes but typically not dissociated sensory loss or Charcot joint. ALS primarily affects motor neurons without significant sensory loss. Rotator cuff arthropathy and rheumatoid arthritis do not typically present with dissociated sensory loss or extensive spinal cord symptoms.
Question 82
A 38-year-old female presents with a 6-month history of burning pain and numbness in her right hand, along with difficulty distinguishing hot from cold water. She also notes increasing weakness in her right arm. Physical examination reveals diminished pain and temperature sensation in a cape-like distribution over her shoulders and arms, with preserved light touch and proprioception. Which of the following spinal cord tracts is primarily affected by the expanding syrinx in this patient?
View Answer & Explanation
Correct Answer: C
Rationale: The classic dissociated sensory loss (loss of pain and temperature sensation with preserved light touch and proprioception) in syringomyelia is due to the expansion of the syrinx into the central gray matter, where the spinothalamic tracts decussate. The dorsal columns carry light touch, vibration, and proprioception. Corticospinal tracts are motor pathways. Rubrospinal and vestibulospinal tracts are also motor pathways involved in posture and movement, not primary sensory perception of pain and temperature.
Question 82
A patient diagnosed with syringomyelia presents with advanced neuropathic arthropathy. Based on the typical progression and prevalence of Charcot joints in syringomyelia, which of the following joints is most commonly affected?
View Answer & Explanation
Correct Answer: D
Rationale: The clinical text explicitly states, "In syringomyelia, neuropathic changes are common in the shoulder joint, followed by the elbow and wrist." This reflects the cervical location of most syringomyelia, affecting the innervation of the upper extremities. While other joints can be affected, the shoulder is the most common site for Charcot arthropathy in syringomyelia.
Question 82
A 55-year-old male presents with chronic neck pain, upper extremity weakness, and a history of recurrent shoulder dislocations. Clinical suspicion for syringomyelia is high. Which imaging modality is considered the gold standard for confirming the diagnosis by visualizing the characteristic spinal cord abnormality?

View Answer & Explanation
Correct Answer: D
Rationale: The clinical context and Fig. 4.3 explicitly state, "The MRI finding – the syrinx formation in the cervical cord – confirms the correct diagnosis of syringomyelia." MRI provides superior soft tissue contrast, allowing direct visualization of the syrinx (fluid-filled cavity) within the spinal cord. X-rays and CT scans are less effective for visualizing the syrinx itself, though CT can show bony changes. Myelography is an invasive procedure largely replaced by MRI for this diagnosis.
Question 82
A 62-year-old patient with a known history of syringomyelia presents with severe, painless destruction of the right elbow joint, characterized by effusions, instability, and osteophyte formation. This condition is best described as a neuropathic osteoarthropathy (Charcot joint). What is the primary underlying mechanism leading to this joint destruction in syringomyelia?
View Answer & Explanation
Correct Answer: C
Rationale: The text describes Charcot's joint as a neurogenic osteoarthropathy, directly linking it to "spinal cord damage; decreased sensation of touch and pain, weakness, and loss of muscle tissue." The loss of protective sensation (pain) and proprioception prevents the patient from recognizing and protecting the joint from repetitive microtrauma, leading to progressive destruction. While hypervascularization (Fig 4.4) can be a feature, it's a secondary phenomenon, not the primary cause of joint destruction. The syrinx does not directly invade the joint, and it's not primarily an autoimmune or metabolic process.
Question 82
A 49-year-old patient with a long-standing diagnosis of syringomyelia reports increasing difficulty with fine motor tasks, such as buttoning shirts and writing. On examination, there is noticeable atrophy of the intrinsic hand muscles and weakness in the upper extremities. These motor symptoms are a direct consequence of the syrinx's expansion and destruction of which part of the spinal cord?
View Answer & Explanation
Correct Answer: B
Rationale: The text mentions "weakness, and loss of muscle tissue" as symptoms of spinal cord damage in syringomyelia. The anterior horn cells, located in the central gray matter of the spinal cord, contain the motor neurons that innervate skeletal muscles. Damage to these cells by an expanding syrinx directly leads to lower motor neuron signs such as weakness and muscle atrophy. While lateral corticospinal tracts (upper motor neurons) can also be affected, the specific mention of muscle atrophy points more directly to anterior horn cell involvement. Posterior columns and Lissauer's tract are sensory pathways, and dorsal root ganglia are peripheral sensory structures.
Question 82
A 58-year-old patient with syringomyelia presents with a severely disorganized and destructive left glenohumeral joint, as visualized on CT scan, along with extensive soft tissue ossification. This presentation is consistent with a Charcot joint. When considering the differential diagnosis for such severe joint destruction in the absence of trauma, which of the following conditions is least likely to cause a similar degree of painless, destructive arthropathy with extensive ossification?

View Answer & Explanation
Correct Answer: D
Rationale: Rheumatoid arthritis is an inflammatory arthropathy that causes joint destruction, but it is typically painful, symmetrical, and characterized by synovitis, erosions, and pannus formation, not the extensive, often painless, disorganized destruction with massive osteophyte formation and soft tissue ossification seen in Charcot arthropathy. Diabetes mellitus, tabes dorsalis, chronic alcoholism, and spinal cord injury can all cause neuropathic arthropathy due to peripheral or central nervous system damage leading to loss of protective sensation and proprioception, similar to syringomyelia.
Question 82
A patient with suspected Charcot arthropathy secondary to syringomyelia undergoes digital subtractive angiography of the affected shoulder. The angiography demonstrates hypervascularization in the parenchymal phase around the glenohumeral joint. What is the significance of this finding in the context of Charcot arthropathy?
View Answer & Explanation
Correct Answer: C
Rationale: Fig. 4.4 shows "Digital subtractive angiography demonstrates hypervascularization in the parenchymal phase around the glenohumeral joint." This hypervascularization is a recognized feature of the "hypertrophic" phase of Charcot arthropathy, reflecting increased blood flow, inflammation, and bone turnover associated with the rapid destructive process. It is not indicative of infection, autoimmune vasculitis, malignancy, or acute trauma as a primary cause, although these should be considered in a broader differential.
Question 82
A 50-year-old patient with syringomyelia and a severely damaged right shoulder joint undergoes bone scintigraphy. The scan reveals increased isotope uptake above periarticular ossification. What does this finding primarily indicate in the context of Charcot arthropathy?

View Answer & Explanation
Correct Answer: C
Rationale: Fig. 4.5 shows "Bone scintigraphy: increased isotope uptake above periarticular ossification." Increased isotope uptake on bone scintigraphy reflects areas of increased bone turnover and osteoblastic activity. In Charcot arthropathy, this is consistent with the ongoing destructive and reparative processes, including periarticular ossification and new bone formation, which are hallmarks of the condition. While infection can also cause increased uptake, in the absence of other signs, it primarily indicates active bone remodeling. Reduced metabolism, tumor, or normal physiology are inconsistent with increased uptake.
Question 82
A 65-year-old patient with a history of syringomyelia presents with a grossly deformed and unstable left shoulder. A CT scan is performed to further evaluate the joint. Which of the following findings would be most characteristic of a Charcot joint secondary to syringomyelia on this CT scan?

View Answer & Explanation
Correct Answer: C
Rationale: The text for Fig. 4.7 (and 4.6) explicitly describes CT findings: "3D CT visualizes better the destruction of the shoulder joint and the extensive soft tissue ossification" and "CT scan shows destroyed humeral head and disorganized gleno-humeral joint, ossification in the soft tissues." These features, including severe disorganization, bone destruction, and extensive periarticular new bone formation/ossification, are classic for Charcot arthropathy. Options A and B are more typical of osteoarthritis and rheumatoid arthritis, respectively. Option D describes rotator cuff arthropathy, and E describes conditions like synovial chondromatosis or advanced inflammatory arthritis, which are distinct from Charcot joint.
Question 82
A 42-year-old patient is diagnosed with syringomyelia after presenting with progressive weakness and sensory deficits. The patient asks about the natural history of the condition. Based on the provided clinical information, how does a syrinx typically behave over time?
View Answer & Explanation
Correct Answer: C
Rationale: The introductory paragraph of the case explicitly states: "This syrinx expands and elongates over time, destroying the center of the spinal cord." This describes the progressive nature of untreated syringomyelia, leading to worsening neurological deficits. Spontaneous resolution, stability, calcification, or migration are not characteristic of the natural history described.
Question 82
A 30-year-old patient is newly diagnosed with a symptomatic cervical syrinx causing progressive pain, weakness, and sensory loss. The syrinx is associated with a Chiari malformation (though not explicitly stated in the text, it's a common association for board-level knowledge). What is the primary goal of surgical management for symptomatic syringomyelia?
View Answer & Explanation
Correct Answer: C
Rationale: While the provided text does not explicitly detail surgical management, board-level knowledge of syringomyelia (often associated with Chiari I malformation) dictates that the primary surgical goal is to address the underlying cause of CSF flow obstruction, typically at the craniocervical junction. This aims to restore normal CSF dynamics, which can lead to syrinx collapse or stabilization, thereby halting or reversing neurological deficits. Direct excision of the syrinx is generally avoided due to spinal cord damage. Spinal fusion is not the primary treatment for the syrinx itself. Nerve transfers are for peripheral nerve injuries, and joint replacement is for end-stage Charcot arthropathy, not the syrinx itself.
Question 82
A 52-year-old patient with syringomyelia presents with a "cape-like" distribution of pain and temperature loss over the shoulders and upper arms, along with weakness in the hands. The syrinx is located in the cervical spinal cord. This specific pattern of sensory loss is due to the involvement of which part of the spinal cord's gray matter?
View Answer & Explanation
Correct Answer: A
Rationale: The syrinx typically expands in the central gray matter. The spinothalamic tracts, which carry pain and temperature sensation, decussate (cross) in the anterior white commissure, just anterior to the central canal, and then ascend in the anterolateral funiculus. The posterior horns of the gray matter are where sensory neurons synapse. As the syrinx expands centrally, it damages these decussating fibers and the posterior horns, leading to the characteristic dissociated sensory loss. Anterior horns are motor, lateral horns contain autonomic neurons, and dorsal/ventral root zones are for nerve root entry/exit.
Question 82
A patient with long-standing syringomyelia is noted to have trophic skin changes, such as dry, cracked skin, and poor wound healing on the affected upper extremity, in addition to the neuropathic joint. These findings are indicative of damage to which component of the nervous system due to the syrinx?
View Answer & Explanation
Correct Answer: C
Rationale: While not explicitly detailed in the provided text, the symptoms of syringomyelia (pain, weakness, stiffness, loss of hot/cold sensation) are due to spinal cord damage. Trophic changes in the skin, such as those described, are often associated with damage to the autonomic nervous system fibers within the spinal cord, which regulate blood flow, sweating, and skin nutrition. Pyramidal and extrapyramidal tracts are motor pathways. Cranial nerves are in the brainstem, and cerebellar pathways are for coordination, neither directly explaining skin trophic changes in the extremities.
Question 82
A 40-year-old patient with syringomyelia is being evaluated for surgical intervention due to progressive neurological deficits. The primary goal of surgery for syringomyelia is to:
View Answer & Explanation
Correct Answer: C
Rationale: The text states that the syrinx "expands and elongates over time, destroying the center of the spinal cord," leading to various symptoms. The primary goal of surgical intervention is to halt this progression by addressing the underlying cause (e.g., Chiari malformation, arachnoiditis) or by shunting the syrinx, thereby preventing further expansion and stabilizing or improving neurological function. Replacing damaged spinal cord tissue is not currently possible. Permanent drainage is a technique, but the goal is broader. Repairing the Charcot joint is a secondary orthopedic concern, and complete elimination of pain is often difficult to achieve.
Question 82
A 60-year-old patient with long-standing syringomyelia has developed severe Charcot arthropathy of the shoulder, characterized by extensive joint destruction and instability. Despite conservative management, the joint continues to deteriorate, leading to significant functional impairment. What is a major long-term orthopedic complication associated with advanced Charcot arthropathy in syringomyelia?
View Answer & Explanation
Correct Answer: B
Rationale: Charcot arthropathy, due to the loss of protective sensation and proprioception, leads to repetitive microtrauma and progressive joint destruction. This severe structural damage, coupled with bone resorption and disorganization, significantly increases the risk of pathological fractures through the weakened and disorganized bone, even with minimal trauma. While other conditions listed can occur, pathological fractures are a direct and severe consequence of the advanced bone destruction characteristic of Charcot joints. The text mentions "destroyed humeral head" and "disorganized gleno-humeral joint" which predisposes to such fractures.
Question 82
A 48-year-old patient with syringomyelia presents with a unique pattern of sensory loss. She describes a loss of pain and temperature sensation that starts in her hands and extends up her arms and across her shoulders, resembling a "cape" or "shawl." This specific distribution of sensory deficit is most accurately explained by the syrinx's effect on which of the following?
View Answer & Explanation
Correct Answer: C
Rationale: The "cape-like" or "shawl" distribution of dissociated sensory loss (pain and temperature) is a classic presentation of syringomyelia. It results from the syrinx expanding within the central gray matter of the cervical spinal cord, specifically damaging the decussating spinothalamic fibers that cross at each spinal level to ascend to the brain. This central lesion affects sensory input from dermatomes corresponding to the cervical levels involved. Peripheral nerve entrapment or brachial plexus compression would typically cause more localized or dermatomal/myotomal patterns, not a cape-like distribution. Cortical lesions would present differently, and while ischemia can affect the spinal cord, the specific pattern points to a central cavity.
Question 82
A 55-year-old patient with a known cervical syrinx presents with worsening symptoms including severe headaches, visual disturbances, and dysphagia, in addition to her existing upper extremity weakness and sensory loss. These new symptoms suggest the syrinx has likely extended to involve which anatomical region?
View Answer & Explanation
Correct Answer: C
Rationale: While the provided text focuses on the spinal cord, board-level knowledge recognizes that a syrinx can extend rostrally into the brainstem, a condition known as syringobulbia. Symptoms like headaches, visual disturbances, and dysphagia (difficulty swallowing) are indicative of brainstem involvement, as cranial nerve nuclei and vital centers are located there. Extension to the thoracic or lumbar spinal cord would cause lower extremity or truncal symptoms, not cranial nerve-related issues. Cauda equina and peripheral nerves are distal to the spinal cord.
Question 82
A 70-year-old patient with a history of syringomyelia presents with severe, painless destruction of the right shoulder joint. Radiographs show extensive disorganization, fragmentation, and periarticular ossification. When differentiating this Charcot arthropathy from severe osteoarthritis, which of the following features is most characteristic of Charcot arthropathy?
View Answer & Explanation
Correct Answer: C
Rationale: Charcot arthropathy is characterized by severe joint destruction, fragmentation, and disorganization that is often disproportionately painless due to the underlying neuropathy. The text describes "destroyed humeral head and disorganized gleno-humeral joint" and "extensive soft tissue ossification." While osteoarthritis can have osteophytes, joint space narrowing, and subchondral cysts, it is typically painful and does not usually present with the extreme disorganization and instability seen in Charcot joints, especially with minimal pain. Symmetrical involvement is more characteristic of inflammatory arthropathies like rheumatoid arthritis, not typically Charcot.
Question 82
A 50-year-old patient with syringomyelia has developed a rapidly progressive Charcot arthropathy of the left shoulder, leading to significant instability and functional loss. The underlying syrinx has been surgically stabilized. What is the most appropriate initial orthopedic management strategy for this progressive Charcot joint?
View Answer & Explanation
Correct Answer: B
Rationale: The primary goal in managing Charcot arthropathy, especially in its progressive phase, is to protect the joint from further destruction. This is achieved through long-term immobilization, protective bracing, and activity modification to offload the affected joint. Surgical options like arthroplasty are generally reserved for very specific cases, often after the acute destructive phase has subsided, and outcomes can be poor due to the underlying neuropathy and bone quality. Aggressive physical therapy without protection would exacerbate destruction. Corticosteroid injections are generally contraindicated due to their catabolic effects on cartilage and bone, and diagnostic arthroscopy is not a primary management strategy for progressive destruction.
Question 83
A 45-year-old male presents with progressive weakness and stiffness in his left arm and shoulder over the past year. He also reports a peculiar inability to feel extreme temperatures, particularly in his hands, but touch sensation seems relatively preserved. Physical examination reveals atrophy of intrinsic hand muscles and a significantly enlarged, unstable left shoulder joint with crepitus. Radiographs show severe destruction of the glenohumeral joint with extensive periarticular ossification. An MRI of the cervical spine is ordered.

View Answer & Explanation
Correct Answer: C
Rationale: The constellation of symptoms including progressive weakness, stiffness, loss of temperature sensation (dissociated sensory loss), muscle atrophy, and a neuropathic (Charcot) joint in the shoulder is highly characteristic of syringomyelia. The MRI finding of a syrinx in the cervical cord would confirm this diagnosis. Cervical disc herniation might cause weakness and sensory changes but typically not dissociated sensory loss or Charcot joint. ALS primarily affects motor neurons without significant sensory loss. Rotator cuff arthropathy and rheumatoid arthritis do not typically present with dissociated sensory loss or extensive spinal cord symptoms.
Question 84
A 38-year-old female presents with a 6-month history of burning pain and numbness in her right hand, along with difficulty distinguishing hot from cold water. She also notes increasing weakness in her right arm. Physical examination reveals diminished pain and temperature sensation in a cape-like distribution over her shoulders and arms, with preserved light touch and proprioception. Which of the following spinal cord tracts is primarily affected by the expanding syrinx in this patient?
View Answer & Explanation
Correct Answer: C
Rationale: The classic dissociated sensory loss (loss of pain and temperature sensation with preserved light touch and proprioception) in syringomyelia is due to the expansion of the syrinx into the central gray matter, where the spinothalamic tracts decussate. The dorsal columns carry light touch, vibration, and proprioception. Corticospinal tracts are motor pathways. Rubrospinal and vestibulospinal tracts are also motor pathways involved in posture and movement, not primary sensory perception of pain and temperature.
Question 85
A patient diagnosed with syringomyelia presents with advanced neuropathic arthropathy. Based on the typical progression and prevalence of Charcot joints in syringomyelia, which of the following joints is most commonly affected?
View Answer & Explanation
Correct Answer: D
Rationale: The clinical text explicitly states, "In syringomyelia, neuropathic changes are common in the shoulder joint, followed by the elbow and wrist." This reflects the cervical location of most syringomyelia, affecting the innervation of the upper extremities. While other joints can be affected, the shoulder is the most common site for Charcot arthropathy in syringomyelia.
Question 86
A 55-year-old male presents with chronic neck pain, upper extremity weakness, and a history of recurrent shoulder dislocations. Clinical suspicion for syringomyelia is high. Which imaging modality is considered the gold standard for confirming the diagnosis by visualizing the characteristic spinal cord abnormality?

View Answer & Explanation
Correct Answer: D
Rationale: The clinical context and Fig. 4.3 explicitly state, "The MRI finding – the syrinx formation in the cervical cord – confirms the correct diagnosis of syringomyelia." MRI provides superior soft tissue contrast, allowing direct visualization of the syrinx (fluid-filled cavity) within the spinal cord. X-rays and CT scans are less effective for visualizing the syrinx itself, though CT can show bony changes. Myelography is an invasive procedure largely replaced by MRI for this diagnosis.
Question 87
A 62-year-old patient with a known history of syringomyelia presents with severe, painless destruction of the right elbow joint, characterized by effusions, instability, and osteophyte formation. This condition is best described as a neuropathic osteoarthropathy (Charcot joint). What is the primary underlying mechanism leading to this joint destruction in syringomyelia?
View Answer & Explanation
Correct Answer: C
Rationale: The text describes Charcot's joint as a neurogenic osteoarthropathy, directly linking it to "spinal cord damage; decreased sensation of touch and pain, weakness, and loss of muscle tissue." The loss of protective sensation (pain) and proprioception prevents the patient from recognizing and protecting the joint from repetitive microtrauma, leading to progressive destruction. While hypervascularization (Fig 4.4) can be a feature, it's a secondary phenomenon, not the primary cause of joint destruction. The syrinx does not directly invade the joint, and it's not primarily an autoimmune or metabolic process.
Question 88
A 49-year-old patient with a long-standing diagnosis of syringomyelia reports increasing difficulty with fine motor tasks, such as buttoning shirts and writing. On examination, there is noticeable atrophy of the intrinsic hand muscles and weakness in the upper extremities. These motor symptoms are a direct consequence of the syrinx's expansion and destruction of which part of the spinal cord?
View Answer & Explanation
Correct Answer: B
Rationale: The text mentions "weakness, and loss of muscle tissue" as symptoms of spinal cord damage in syringomyelia. The anterior horn cells, located in the central gray matter of the spinal cord, contain the motor neurons that innervate skeletal muscles. Damage to these cells by an expanding syrinx directly leads to lower motor neuron signs such as weakness and muscle atrophy. While lateral corticospinal tracts (upper motor neurons) can also be affected, the specific mention of muscle atrophy points more directly to anterior horn cell involvement. Posterior columns and Lissauer's tract are sensory pathways, and dorsal root ganglia are peripheral sensory structures.
Question 89
A 58-year-old patient with syringomyelia presents with a severely disorganized and destructive left glenohumeral joint, as visualized on CT scan, along with extensive soft tissue ossification. This presentation is consistent with a Charcot joint. When considering the differential diagnosis for such severe joint destruction in the absence of trauma, which of the following conditions is least likely to cause a similar degree of painless, destructive arthropathy with extensive ossification?

View Answer & Explanation
Correct Answer: D
Rationale: Rheumatoid arthritis is an inflammatory arthropathy that causes joint destruction, but it is typically painful, symmetrical, and characterized by synovitis, erosions, and pannus formation, not the extensive, often painless, disorganized destruction with massive osteophyte formation and soft tissue ossification seen in Charcot arthropathy. Diabetes mellitus, tabes dorsalis, chronic alcoholism, and spinal cord injury can all cause neuropathic arthropathy due to peripheral or central nervous system damage leading to loss of protective sensation and proprioception, similar to syringomyelia.
Question 90
A patient with suspected Charcot arthropathy secondary to syringomyelia undergoes digital subtractive angiography of the affected shoulder. The angiography demonstrates hypervascularization in the parenchymal phase around the glenohumeral joint. What is the significance of this finding in the context of Charcot arthropathy?

View Answer & Explanation
Correct Answer: C
Rationale: Fig. 4.4 shows "Digital subtractive angiography demonstrates hypervascularization in the parenchymal phase around the glenohumeral joint." This hypervascularization is a recognized feature of the "hypertrophic" phase of Charcot arthropathy, reflecting increased blood flow, inflammation, and bone turnover associated with the rapid destructive process. It is not indicative of infection, autoimmune vasculitis, malignancy, or acute trauma as a primary cause, although these should be considered in a broader differential.
Question 91
A 50-year-old patient with syringomyelia and a severely damaged right shoulder joint undergoes bone scintigraphy. The scan reveals increased isotope uptake above periarticular ossification. What does this finding primarily indicate in the context of Charcot arthropathy?

View Answer & Explanation
Correct Answer: C
Rationale: Fig. 4.5 shows "Bone scintigraphy: increased isotope uptake above periarticular ossification." Increased isotope uptake on bone scintigraphy reflects areas of increased bone turnover and osteoblastic activity. In Charcot arthropathy, this is consistent with the ongoing destructive and reparative processes, including periarticular ossification and new bone formation, which are hallmarks of the condition. While infection can also cause increased uptake, in the absence of other signs, it primarily indicates active bone remodeling. Reduced metabolism, tumor, or normal physiology are inconsistent with increased uptake.
Question 92
A 65-year-old patient with a history of syringomyelia presents with a grossly deformed and unstable left shoulder. A CT scan is performed to further evaluate the joint. Which of the following findings would be most characteristic of a Charcot joint secondary to syringomyelia on this CT scan?

View Answer & Explanation
Correct Answer: C
Rationale: The text for Fig. 4.7 (and 4.6) explicitly describes CT findings: "3D CT visualizes better the destruction of the shoulder joint and the extensive soft tissue ossification" and "CT scan shows destroyed humeral head and disorganized gleno-humeral joint, ossification in the soft tissues." These features, including severe disorganization, bone destruction, and extensive periarticular new bone formation/ossification, are classic for Charcot arthropathy. Options A and B are more typical of osteoarthritis and rheumatoid arthritis, respectively. Option D describes rotator cuff arthropathy, and E describes conditions like synovial chondromatosis or advanced inflammatory arthritis, which are distinct from Charcot joint.
Question 93
A 42-year-old patient is diagnosed with syringomyelia after presenting with progressive weakness and sensory deficits. The patient asks about the natural history of the condition. Based on the provided clinical information, how does a syrinx typically behave over time?
View Answer & Explanation
Correct Answer: C
Rationale: The introductory paragraph of the case explicitly states: "This syrinx expands and elongates over time, destroying the center of the spinal cord." This describes the progressive nature of untreated syringomyelia, leading to worsening neurological deficits. Spontaneous resolution, stability, calcification, or migration are not characteristic of the natural history described.
Question 94
A 30-year-old patient is newly diagnosed with a symptomatic cervical syrinx causing progressive pain, weakness, and sensory loss. The syrinx is associated with a Chiari malformation (though not explicitly stated in the text, it's a common association for board-level knowledge). What is the primary goal of surgical management for symptomatic syringomyelia?
View Answer & Explanation
Correct Answer: C
Rationale: While the provided text does not explicitly detail surgical management, board-level knowledge of syringomyelia (often associated with Chiari I malformation) dictates that the primary surgical goal is to address the underlying cause of CSF flow obstruction, typically at the craniocervical junction. This aims to restore normal CSF dynamics, which can lead to syrinx collapse or stabilization, thereby halting or reversing neurological deficits. Direct excision of the syrinx is generally avoided due to spinal cord damage. Spinal fusion is not the primary treatment for the syrinx itself. Nerve transfers are for peripheral nerve injuries, and joint replacement is for end-stage Charcot arthropathy, not the syrinx itself.
Question 95
A 52-year-old patient with syringomyelia presents with a "cape-like" distribution of pain and temperature loss over the shoulders and upper arms, along with weakness in the hands. The syrinx is located in the cervical spinal cord. This specific pattern of sensory loss is due to the involvement of which part of the spinal cord's gray matter?
View Answer & Explanation
Correct Answer: A
Rationale: The syrinx typically expands in the central gray matter. The spinothalamic tracts, which carry pain and temperature sensation, decussate (cross) in the anterior white commissure, just anterior to the central canal, and then ascend in the anterolateral funiculus. The posterior horns of the gray matter are where sensory neurons synapse. As the syrinx expands centrally, it damages these decussating fibers and the posterior horns, leading to the characteristic dissociated sensory loss. Anterior horns are motor, lateral horns contain autonomic neurons, and dorsal/ventral root zones are for nerve root entry/exit.
Question 96
A patient with long-standing syringomyelia is noted to have trophic skin changes, such as dry, cracked skin, and poor wound healing on the affected upper extremity, in addition to the neuropathic joint. These findings are indicative of damage to which component of the nervous system due to the syrinx?
View Answer & Explanation
Correct Answer: C
Rationale: While not explicitly detailed in the provided text, the symptoms of syringomyelia (pain, weakness, stiffness, loss of hot/cold sensation) are due to spinal cord damage. Trophic changes in the skin, such as those described, are often associated with damage to the autonomic nervous system fibers within the spinal cord, which regulate blood flow, sweating, and skin nutrition. Pyramidal and extrapyramidal tracts are motor pathways. Cranial nerves are in the brainstem, and cerebellar pathways are for coordination, neither directly explaining skin trophic changes in the extremities.
Question 97
A 40-year-old patient with syringomyelia is being evaluated for surgical intervention due to progressive neurological deficits. The primary goal of surgery for syringomyelia is to:
View Answer & Explanation
Correct Answer: C
Rationale: The text states that the syrinx "expands and elongates over time, destroying the center of the spinal cord," leading to various symptoms. The primary goal of surgical intervention is to halt this progression by addressing the underlying cause (e.g., Chiari malformation, arachnoiditis) or by shunting the syrinx, thereby preventing further expansion and stabilizing or improving neurological function. Replacing damaged spinal cord tissue is not currently possible. Permanent drainage is a technique, but the goal is broader. Repairing the Charcot joint is a secondary orthopedic concern, and complete elimination of pain is often difficult to achieve.
Question 98
A 60-year-old patient with long-standing syringomyelia has developed severe Charcot arthropathy of the shoulder, characterized by extensive joint destruction and instability. Despite conservative management, the joint continues to deteriorate, leading to significant functional impairment. What is a major long-term orthopedic complication associated with advanced Charcot arthropathy in syringomyelia?
View Answer & Explanation
Correct Answer: B
Rationale: Charcot arthropathy, due to the loss of protective sensation and proprioception, leads to repetitive microtrauma and progressive joint destruction. This severe structural damage, coupled with bone resorption and disorganization, significantly increases the risk of pathological fractures through the weakened and disorganized bone, even with minimal trauma. While other conditions listed can occur, pathological fractures are a direct and severe consequence of the advanced bone destruction characteristic of Charcot joints. The text mentions "destroyed humeral head" and "disorganized gleno-humeral joint" which predisposes to such fractures.
Question 99
A 48-year-old patient with syringomyelia presents with a unique pattern of sensory loss. She describes a loss of pain and temperature sensation that starts in her hands and extends up her arms and across her shoulders, resembling a "cape" or "shawl." This specific distribution of sensory deficit is most accurately explained by the syrinx's effect on which of the following?
View Answer & Explanation
Correct Answer: C
Rationale: The "cape-like" or "shawl" distribution of dissociated sensory loss (pain and temperature) is a classic presentation of syringomyelia. It results from the syrinx expanding within the central gray matter of the cervical spinal cord, specifically damaging the decussating spinothalamic fibers that cross at each spinal level to ascend to the brain. This central lesion affects sensory input from dermatomes corresponding to the cervical levels involved. Peripheral nerve entrapment or brachial plexus compression would typically cause more localized or dermatomal/myotomal patterns, not a cape-like distribution. Cortical lesions would present differently, and while ischemia can affect the spinal cord, the specific pattern points to a central cavity.
Question 100
A 55-year-old patient with a known cervical syrinx presents with worsening symptoms including severe headaches, visual disturbances, and dysphagia, in addition to her existing upper extremity weakness and sensory loss. These new symptoms suggest the syrinx has likely extended to involve which anatomical region?
View Answer & Explanation
Correct Answer: C
Rationale: While the provided text focuses on the spinal cord, board-level knowledge recognizes that a syrinx can extend rostrally into the brainstem, a condition known as syringobulbia. Symptoms like headaches, visual disturbances, and dysphagia (difficulty swallowing) are indicative of brainstem involvement, as cranial nerve nuclei and vital centers are located there. Extension to the thoracic or lumbar spinal cord would cause lower extremity or truncal symptoms, not cranial nerve-related issues. Cauda equina and peripheral nerves are distal to the spinal cord.
You Might Also Like