Master ABOS Orthopedic Board Review: Paget's, Gout, Hyperparathyroidism | Part 5
Key Takeaway
This ABOS Orthopedic Board Review provides multiple-choice questions covering key musculoskeletal pathologies. Topics include Paget's Disease, Gout, Hyperparathyroidism, and Newborn's Septic Arthritis of the Hip, focusing on diagnosis, pathophysiology, and clinical management crucial for board exam preparation.
Question 1
A 70-year-old male with known Paget's disease of the femur experiences a sudden onset of severe thigh pain after a minor fall. Radiographs confirm a transverse fracture. Despite the bone appearing robust on previous imaging, it fractured easily. What characteristic of Pagetic bone explains its susceptibility to fracture?
View Answer & Explanation
Correct Answer: C
Rationale: The introductory text states that Paget's disease "results in producing robust, however, often fragile bone tissue." This explains why bone that appears dense or enlarged can still be prone to fracture due to its disorganized internal structure. Option A is partially true (increased density) but doesn't explain fragility. Option B is incorrect as remodeling is abnormal. Option E is incorrect as osteoclast activity is pathologically increased.
Question 2
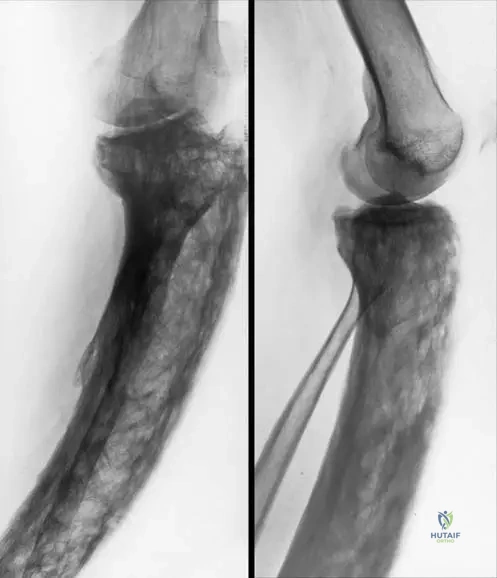
A 69-year-old male with long-standing Paget's disease affecting his distal femur presents with insidious onset of right knee pain, stiffness, and swelling. Physical examination reveals crepitus and reduced range of motion.

Based on the provided image and clinical scenario, what common musculoskeletal complication is frequently observed in patients with Paget's disease, particularly in adjacent joints?
View Answer & Explanation
Correct Answer: C
Rationale: The clinical context for Fig. 7.55 a, b specifically mentions "Early osteoarthritis of the knee in a patient with Paget’s disease." The altered biomechanics and bone deformity associated with Paget's disease can predispose adjacent joints to premature degenerative changes. The other options are inflammatory or infectious arthritides not directly linked as a common complication of Paget's disease in the provided text.
Question 3
A 78-year-old female with extensive Paget's disease affecting her left pelvis and proximal femur presents with a progressive limp and difficulty walking. On examination, a significant discrepancy in leg length is noted.
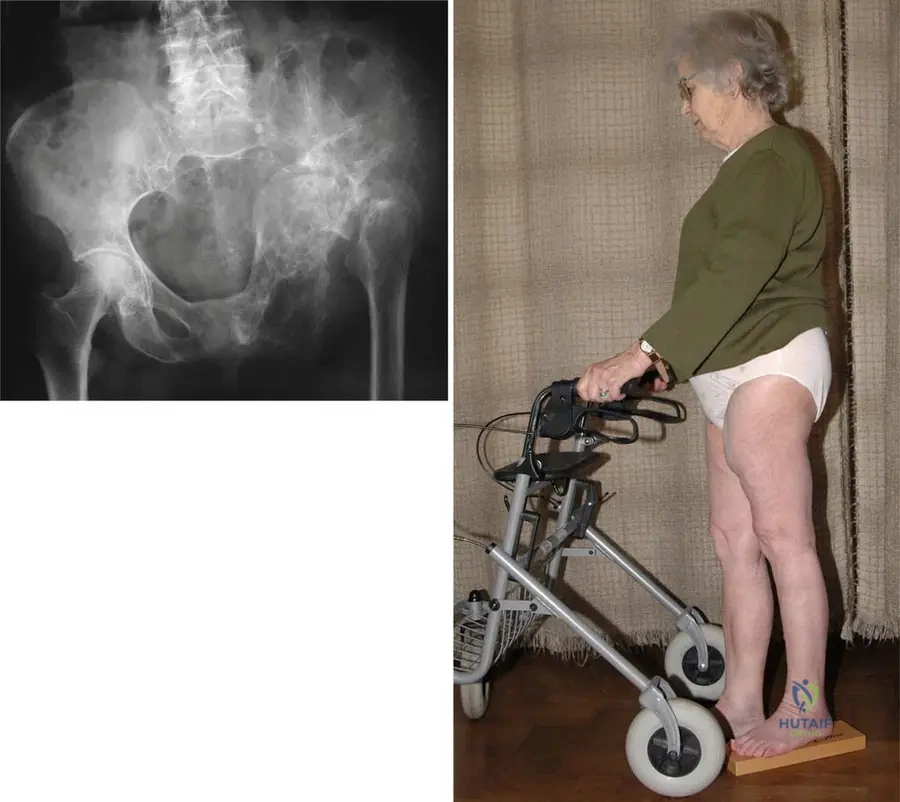
Based on the provided image and clinical context, what is the measured absolute shortening of the affected extremity in this patient?
View Answer & Explanation
Correct Answer: D
Rationale: The clinical context for Fig. 7.58 a, b explicitly states, "The patient has 4-cm absolute shortening of the left extremity and required support for walking." This is a direct factual recall from the provided case description. Other options are incorrect values.
Question 4
A 71-year-old male presents with severe left hip and pelvic pain. Radiographs show marked osteopenia and extensive destruction of the left pelvic bone and proximal femur, raising concern for malignancy.
Based on the provided image and clinical context, what condition does this presentation of Paget's disease mimic, particularly in its florid lytic phase?
View Answer & Explanation
Correct Answer: C
Rationale: The clinical context for Fig. 7.58 a, b states, "Florid lytic phase of the disease aff ecting the innominate bone and vertebra. Note the marked osteopenia, the extensive destruction of the left pelvic bone, and proximal femur that mimics metastatic carcinoma (a)." This highlights a critical differential diagnosis for the lytic phase of Paget's. The other options are less likely to present with such extensive destruction mimicking malignancy.
Question 5
A 67-year-old male is diagnosed with Paget's disease. His physician explains that the disease involves a fundamental disruption in the normal process of bone maintenance. What is the core disturbance in bone physiology characteristic of Paget's disease?
View Answer & Explanation
Correct Answer: B
Rationale: The introductory text states, "Th is is a disease of unknown etiology, which is characterized by the disturbance of bone remodeling..." This is the overarching physiological problem in Paget's disease, leading to the cellular and structural abnormalities. The other options describe different metabolic bone disorders or related physiological processes not identified as the primary disturbance in Paget's.
Question 6
A 70-year-old male presents with isolated right femur pain and bowing, confirmed as Paget's disease. This presentation, affecting only a single bone, is referred to as:
View Answer & Explanation
Correct Answer: B
Rationale: The clinical context for Fig. 7.51 a, b and Fig. 7.52 a, b both refer to "Patient with monostotic Paget’s disease aff ecting the right femur" and "monostotic form" for the tibia. Monostotic refers to involvement of a single bone. Polyostotic Paget's disease involves multiple bones. The other options are incorrect terms for this specific presentation.
Question 7
In the active phase of Paget's disease, a 66-year-old patient's bone turnover is significantly elevated. This high turnover is characterized by specific cellular activities. Which statement accurately describes the cellular events in the active phase?
View Answer & Explanation
Correct Answer: B
Rationale: The text states, "In the active phase with high turnover, the abnormal osteoclast activity creates lytic cavities, and the consequent increased bone production by active osteoblasts produces abnormal growth of the bone cortex." This accurately describes the sequence of events. Option A is incorrect as osteoclast activity is increased, not decreased. Option C is incorrect as the activity is unbalanced and abnormal.
Question 8
A 73-year-old male with Paget's disease of the tibia undergoes a follow-up radiograph. The image shows significant enlargement of the bone with a thickened cortex. This cortical change is a direct result of which pathological process in Paget's disease?
View Answer & Explanation
Correct Answer: C
Rationale: The text explains that in the active phase, "the consequent increased bone production by active osteoblasts produces abnormal growth of the bone cortex." This increased, but disorganized, bone formation leads to the characteristic cortical thickening and enlargement. Option A is incorrect as osteoblast function is increased. Option B is incorrect as remodeling is abnormal.
Question 9
A 60-year-old male presents with new onset of deep, aching pain in his right femur, which is worse with weight-bearing. Radiographs show cortical thickening and bowing consistent with Paget's disease. What is the most likely cause of his pain?
View Answer & Explanation
Correct Answer: B
Rationale: While not explicitly stated as "pain," the text describes "pathologically active osteoclast cell activity," "increased osteoblast function," "deformed bone is fragile," and "lytic cavities." These processes, especially the rapid bone turnover, microfractures, and bone expansion, are well-known causes of bone pain in Paget's disease. The other options are less direct or primary causes of bone pain in this context.
Question 10
A 74-year-old patient with a history of prostate cancer presents with new onset of severe back pain. Imaging reveals extensive lytic lesions in the lumbar vertebrae and pelvis. While metastatic disease is a primary concern, the patient also has elevated alkaline phosphatase. Given the radiographic appearance, what other bone disease should be considered in the differential diagnosis?
View Answer & Explanation
Correct Answer: C
Rationale: The text for Fig. 7.58 a, b explicitly states that the "Florid lytic phase of the disease aff ecting the innominate bone and vertebra... mimics metastatic carcinoma." The presence of extensive lytic lesions in the spine and pelvis, combined with elevated alkaline phosphatase (a marker of bone turnover, often high in Paget's), makes Paget's disease a crucial differential diagnosis for metastatic carcinoma. Multiple myeloma can also present with lytic lesions but typically has normal alkaline phosphatase.
Question 11
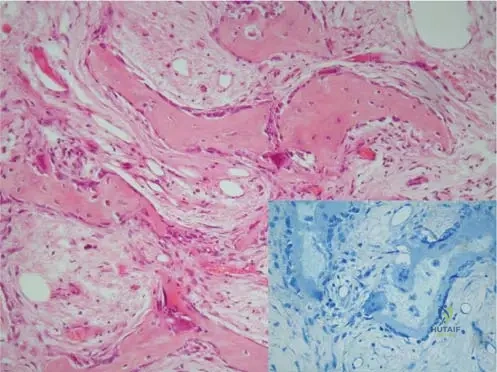
A 63-year-old male is diagnosed with Paget's disease based on clinical and radiographic findings. A bone biopsy is performed. The microscopic examination reveals a disorganized, haphazard arrangement of collagen fibers within the bone matrix. This characteristic structure is best described as:
View Answer & Explanation
Correct Answer: B
Rationale: The text states, "Bone changes in Paget’s disease are characterized by the development of “woven” bone and lamellar pattern of collagen." Woven bone is immature, disorganized bone, which is rapidly laid down in Paget's disease. Lamellar bone is mature, organized bone. While lamellar bone is also present, the *development* of woven bone is the key pathological feature. Option A is incorrect as woven bone is the characteristic feature of Paget's, not predominantly lamellar bone.
Question 12
A 71-year-old female presents with a progressive increase in hat size and difficulty fitting her eyeglasses. On examination, her skull appears enlarged. Radiographs confirm thickening of the calvarium. This type of bone enlargement and deformity is a direct consequence of which aspect of Paget's disease?
View Answer & Explanation
Correct Answer: B
Rationale: The text states, "the consequent increased bone production by active osteoblasts produces abnormal growth of the bone cortex." This abnormal growth leads to the characteristic enlargement and deformity seen in affected bones, such as the skull. Option A is incorrect as bone resorption is pathologically active. Option E is incorrect as osteoblast activity is increased.
Question 13
A 65-year-old male is diagnosed with Paget's disease. His family asks about the typical demographic affected by this condition. Which statement accurately describes the typical patient population for Paget's disease?
View Answer & Explanation
Correct Answer: C
Rationale: The introductory text states, "Paget’s disease involves 2–8% of the population aged over 60. Male to female ratio is 2:1." This directly matches option C. Options A, B, D, and E contradict the provided epidemiological data.
Question 14
A 68-year-old male presents with new onset left hip pain. Radiographs reveal marked osteopenia and extensive destruction of the left pelvic bone and proximal femur, mimicking metastatic carcinoma. He reports a 4-cm absolute shortening of the left extremity and requires support for walking. His medical history is otherwise unremarkable.

View Answer & Explanation
Correct Answer: C
Rationale: Paget's disease is characterized by a disturbance of bone remodeling with pathologically active osteoclast cell activity and accordingly increased osteoblast function. This leads to the production of robust, yet often fragile, bone tissue. Option A is incorrect because osteoblast function is increased, not decreased. Option D describes a different metabolic bone disease.
Question 15
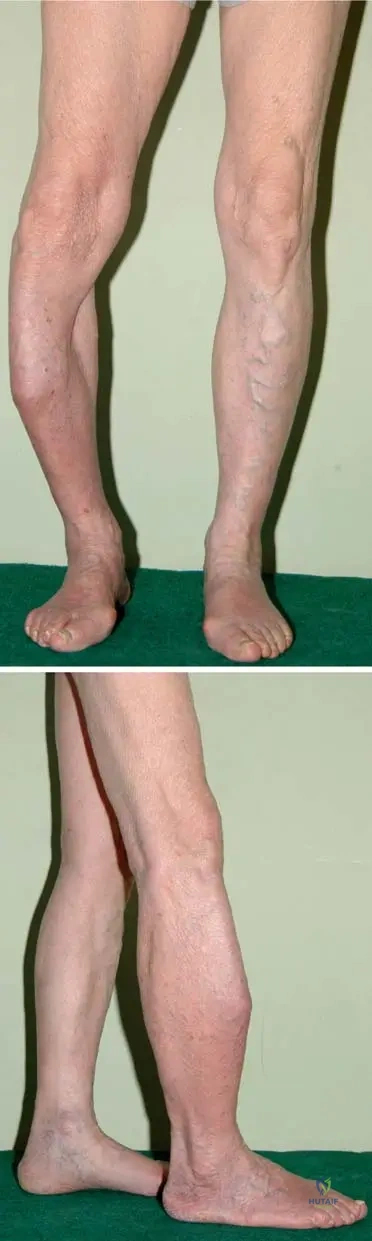
A 72-year-old male presents with progressive bowing of his right lower leg. Physical examination reveals an enlarged right tibia with anterior bowing. Radiographs confirm the characteristic "sabre tibia" deformity. He denies any history of trauma.
View Answer & Explanation
Correct Answer: D
Rationale: The clinical presentation of an enlarged tibia with anterior bowing, known as "sabre tibia," is highly characteristic of Paget's disease, especially in its monostotic form affecting the tibia. Osteoporosis (A) primarily involves bone density loss without significant bowing or enlargement. Osteomalacia (B) can cause bowing but typically presents with diffuse bone pain and muscle weakness, and the bone enlargement is not as characteristic. Fibrous dysplasia (C) can cause deformities but "sabre tibia" is not its classic presentation. Chronic osteomyelitis (E) would typically involve signs of infection.
Question 16
A 65-year-old female is found to have an elevated alkaline phosphatase level during a routine check-up. She denies any bone pain or other symptoms. Subsequent skeletal survey reveals changes consistent with Paget's disease. Which of the following bones is LEAST likely to be involved in Paget's disease?
View Answer & Explanation
Correct Answer: E
Rationale: The provided text states that the most often involved bones are the pelvis, spinal column, skull, femur, and tibia. While Paget's disease "may be present in any bone," the phalanges of the hand are not listed among the commonly affected sites, making them the least likely among the given options. The other options (A, B, C, D) are explicitly mentioned as commonly involved bones.
Question 17
A 70-year-old male presents with a history of progressive hearing loss and increasing hat size. A skull radiograph is performed. Which of the following radiographic findings would be most characteristic of the acute phase of Paget's disease in the skull?
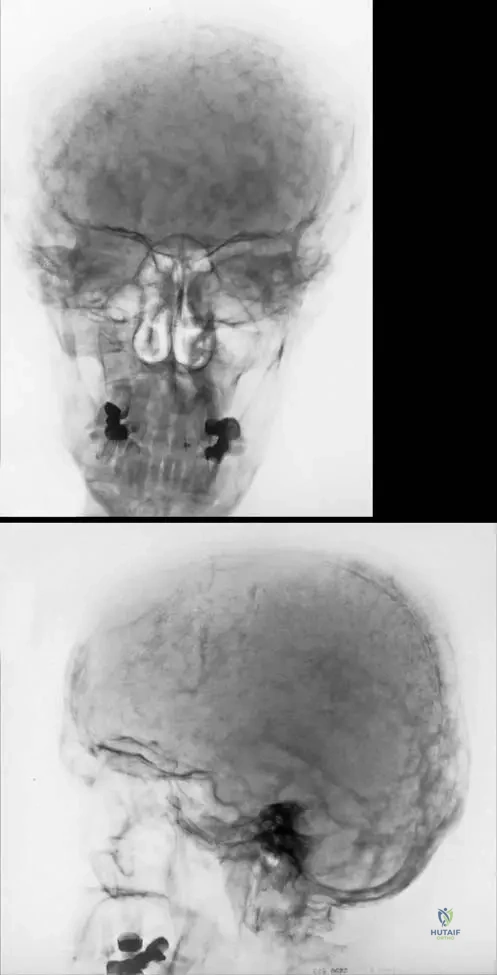
View Answer & Explanation
Correct Answer: C
Rationale: The image caption (Fig. 7.54 a, b) explicitly states, "The skull shows typical changes in the acute phase known as osteoporosis circumscripta." This refers to well-demarcated lytic lesions in the skull. While "cotton wool appearance" (A) and sclerotic patches (D) are also seen in Paget's, they are typically associated with later, mixed, or sclerotic phases. Punched-out lytic lesions (B) are more characteristic of multiple myeloma. Hair-on-end appearance (E) is seen in conditions like thalassemia.
Question 18
A 62-year-old male is diagnosed with monostotic Paget's disease affecting his right femur. Radiographs show a laterally and anteriorly bowed long bone. Histological examination of a bone biopsy from the affected area would most likely reveal which of the following?
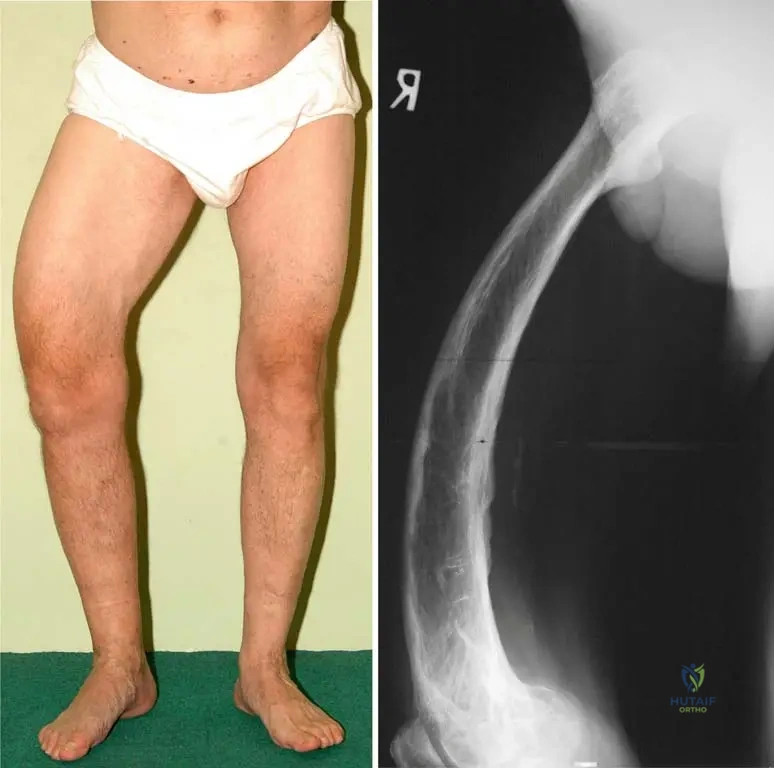
View Answer & Explanation
Correct Answer: C
Rationale: The text states, "Bone changes in Paget’s disease are characterized by the development of “woven” bone and lamellar pattern of collagen." This is the hallmark histological finding. Option A is incorrect as the bone is abnormal. Option B describes osteomalacia. Options D and E are not characteristic histological features of Paget's disease.
Question 19
A 75-year-old male presents with chronic right knee pain and stiffness. Radiographs show early osteoarthritis of the knee. His medical history includes a diagnosis of Paget's disease affecting the distal femur and proximal tibia. What is the most likely relationship between his Paget's disease and his knee osteoarthritis?

View Answer & Explanation
Correct Answer: B
Rationale: The image caption (Fig. 7.55 a, b) shows "Early osteoarthritis of the knee in a patient with Paget’s disease." This implies a connection. Paget's disease causes bone enlargement, deformity (like bowing of the femur and tibia), and altered bone mechanics, which can lead to abnormal joint loading and accelerate the development of secondary osteoarthritis in adjacent joints. Option A is too direct; the effect is indirect through altered mechanics. Option C is incorrect as it's a known complication. Options D and E are incorrect.
Question 20
A 60-year-old male is diagnosed with Paget's disease. He asks about the typical demographic profile of this condition. Which of the following statements regarding the epidemiology of Paget's disease is most accurate?
View Answer & Explanation
Correct Answer: B
Rationale: The text explicitly states, "Paget’s disease involves 2–8% of the population aged over 60. Male to female ratio is 2:1." This directly matches option B. All other options present incorrect demographic data.
Question 21
A 70-year-old male presents with severe left hip and lower back pain. Radiographs reveal extensive destruction of the left pelvic bone and proximal femur, along with vertebral involvement, mimicking metastatic carcinoma. The patient also has a 4-cm absolute shortening of the left extremity. This presentation is characteristic of which phase of Paget's disease?

View Answer & Explanation
Correct Answer: C
Rationale: The image caption (Fig. 7.58 a, b) describes this exact scenario as "Florid lytic phase of the disease affecting the innominate bone and vertebra. Note the marked osteopenia, the extensive destruction of the left pelvic bone, and proximal femur that mimics metastatic carcinoma." This directly identifies the phase as florid lytic. The other options describe different phases or are not supported by the description of extensive destruction and osteopenia.
Question 22
A 67-year-old male is diagnosed with Paget's disease affecting his right femur. He is concerned about the strength of the affected bone. Which of the following statements best describes the nature of the bone tissue produced in Paget's disease?

View Answer & Explanation
Correct Answer: B
Rationale: The text states that the increased osteoblast function "results in producing robust, however, often fragile bone tissue." This is a key characteristic of Pagetic bone, which, despite its increased mass, is structurally disorganized and prone to fracture. Option A is incorrect because it is fragile. Option C describes osteomalacia. Option D describes osteoporosis. Option E is incorrect as it is histologically distinct.
Question 23
A 71-year-old male presents with a 3-month history of dull aching pain in his right lower extremity. Physical examination reveals an enlarged and bowed right tibia. Radiographs confirm the presence of a "sabre tibia" deformity. What is the primary pathological process leading to the abnormal growth of the bone cortex in Paget's disease?

View Answer & Explanation
Correct Answer: C
Rationale: The text explains, "In the active phase with high turnover, the abnormal osteoclast activity creates lytic cavities, and the consequent increased bone production by active osteoblasts produces abnormal growth of the bone cortex." This describes the coupled but disorganized remodeling process. Option A is incorrect because osteoclast activity is increased. Options B, D, and E do not accurately describe the primary pathological process in Paget's disease.
Question 24
A 69-year-old male presents with a new fracture of his right femur after a low-energy fall. He has a known history of monostotic Paget's disease affecting the right femur, which exhibits significant bowing. The fragility of the bone in Paget's disease is primarily due to which of the following?

View Answer & Explanation
Correct Answer: B
Rationale: The text states, "Bone changes in Paget’s disease are characterized by the development of “woven” bone and lamellar pattern of collagen... The deformed bone is fragile." The disorganized "woven" bone, which is immature and structurally inferior to normal lamellar bone, is the primary reason for the fragility, despite the bone often appearing robust or enlarged. Option C is incorrect as the bone mass is often increased, not decreased, though it may appear osteopenic in the lytic phase. Option A is incorrect as the issue is disorganization, not just excessive mineralization. Options D and E are not the primary reasons for fragility in Paget's.
Question 25
A 73-year-old female presents with severe left hip pain and difficulty walking, requiring support. Radiographs show extensive destruction of the left pelvic bone and proximal femur, with marked osteopenia, raising suspicion for metastatic carcinoma. What is the most significant functional impairment directly resulting from the bone changes seen in this patient?

View Answer & Explanation
Correct Answer: C
Rationale: The image caption (Fig. 7.58 a, b) explicitly states, "The patient has 4-cm absolute shortening of the left extremity and required support for walking." This directly describes a significant functional impairment. While pathological fracture risk (A) is also present due to bone fragility, the vignette specifically mentions the shortening and need for support, making C the most direct answer to "functional impairment directly resulting from the bone changes seen in this patient." Cranial nerve compression (D) occurs with skull involvement, and hypercalcemia (E) is rare unless immobilized. Osteosarcoma (B) is a rare complication, not a direct functional impairment.
Question 26
A 66-year-old male presents with a new onset of right thigh pain. Radiographs reveal an enlarged and bowed right femur. The patient's serum alkaline phosphatase is significantly elevated. This presentation is most consistent with which of the following conditions?

View Answer & Explanation
Correct Answer: C
Rationale: The clinical vignette describes an enlarged and bowed femur, which is a classic presentation of Paget's disease, as shown in Fig. 7.51 a, b. Elevated alkaline phosphatase is a common biochemical marker reflecting increased osteoblast activity in Paget's disease. Osteogenesis Imperfecta (A) involves brittle bones but typically presents earlier in life and with different radiographic features. Renal Osteodystrophy (B) and Hyperparathyroidism (E) can cause bone changes but typically have different clinical contexts and radiographic patterns. Multiple Myeloma (D) presents with punched-out lytic lesions and is not associated with bone enlargement or bowing in this manner.
Question 27
A 78-year-old female is undergoing a workup for unexplained bone pain. Her radiographs show areas of both osteolysis and osteosclerosis in the spine and pelvis. A bone biopsy reveals a mosaic pattern of lamellar and woven bone. This histological finding is characteristic of which disease?
View Answer & Explanation
Correct Answer: C
Rationale: The text explicitly states, "Bone changes in Paget’s disease are characterized by the development of “woven” bone and lamellar pattern of collagen." The description of a mosaic pattern of lamellar and woven bone is a classic histological feature of Paget's disease. Osteoporosis (A) involves reduced bone mass but normal histology. Osteomalacia (B) shows increased unmineralized osteoid. Fibrous dysplasia (D) shows immature woven bone within a fibrous stroma. Metastatic carcinoma (E) would show malignant cells.
Question 28
A 63-year-old male presents with a 6-month history of progressive anterior bowing of his left tibia. Physical examination reveals an enlarged and warm left tibia. Radiographs confirm the "sabre tibia" deformity. Given the typical progression of Paget's disease, what is the most likely long-term complication in this affected limb?

View Answer & Explanation
Correct Answer: C
Rationale: The text states, "The deformed bone is fragile." This inherent fragility, combined with the abnormal architecture and bowing, significantly increases the risk of pathological fractures in Pagetic bone. While malignant transformation (D) to osteosarcoma (not chondrosarcoma) is a rare but serious complication, pathological fracture (C) is a more common and direct consequence of the fragile, deformed bone. Spontaneous resolution (A) does not occur. Avascular necrosis (B) is not a typical complication of Paget's in the tibia. Progressive decrease in bone size (E) is incorrect; the bone typically enlarges.
Question 29
A 70-year-old male presents with chronic pain in his right hip and knee. Radiographs show significant osteoarthritis in the right knee and changes consistent with Paget's disease in the distal femur and proximal tibia. The presence of Paget's disease in these locations contributes to the development of osteoarthritis primarily by:

View Answer & Explanation
Correct Answer: B
Rationale: As indicated by Fig. 7.55 a, b, osteoarthritis is a known complication of Paget's disease. The abnormal bone remodeling in Paget's disease leads to bone enlargement and deformity (e.g., bowing of the femur or tibia), which alters the normal biomechanics of adjacent joints. This abnormal loading and stress on the articular cartilage accelerate its degeneration, leading to secondary osteoarthritis. Option A is incorrect as Paget's is not primarily an inflammatory arthritis. Option D is incorrect as Paget's often involves increased bone mass, not severe osteoporosis. Options C and E are not mechanisms by which Paget's causes osteoarthritis.
Question 30
A 65-year-old male presents with a 5-cm limb length discrepancy in his left leg, requiring a cane for ambulation. Radiographs show extensive lytic and sclerotic changes in the left innominate bone and proximal femur, mimicking metastatic disease. This patient's condition is best described as:

View Answer & Explanation
Correct Answer: B
Rationale: The image caption (Fig. 7.58 a, b) describes "Florid lytic phase of the disease affecting the innominate bone and vertebra." The vignette mentions involvement of the left innominate bone and proximal femur, and the image shows vertebral involvement, indicating multiple bones are affected (polyostotic). The description of "extensive destruction" and "mimics metastatic carcinoma" aligns with the "florid lytic phase." Osteoporosis circumscripta (E) is specific to the skull in the acute phase. Monostotic (A, C) is incorrect due to multiple bone involvement. Sclerotic (C) and quiescent (A) phases do not typically present with extensive destruction and limb shortening.
Question 31
A 70-year-old male is diagnosed with Paget's disease. He asks about the underlying cause. Based on the provided information, what is the current understanding of the etiology of Paget's disease?
View Answer & Explanation
Correct Answer: C
Rationale: The very first sentence of the provided text states, "This is a disease of unknown etiology." While genetic factors and viral associations (like measles) have been investigated, the text explicitly states the etiology is unknown. Therefore, options A, B, D, and E are not supported by the provided text as the primary or definitive cause.
Question 32
A 68-year-old male presents with a 4-cm absolute shortening of his left extremity and requires support for walking due to severe left hip and lower back pain. Radiographs show marked osteopenia and extensive destruction of the left pelvic bone and proximal femur, mimicking metastatic carcinoma. Which of the following conditions is most likely to be considered in the differential diagnosis given the radiographic findings?

View Answer & Explanation
Correct Answer: D
Rationale: The image caption (Fig. 7.58 a, b) explicitly states that the "marked osteopenia, the extensive destruction of the left pelvic bone, and proximal femur... mimics metastatic carcinoma." This makes metastatic carcinoma the most likely differential diagnosis mentioned in the provided text. While other conditions might be considered, metastatic carcinoma is specifically highlighted as a mimicker. Osteoarthritis (A) would not typically present with extensive destruction mimicking cancer. Osteomyelitis (B) would usually have signs of infection. Multiple myeloma (C) can cause lytic lesions but the description of extensive destruction and osteopenia in Paget's can be very similar to metastatic disease. Fibrous dysplasia (E) has different radiographic characteristics.
Question 33
A 55-year-old male presents with acute onset of severe pain, swelling, and redness in his great toe. Synovial fluid aspiration is performed.
View Answer & Explanation
Correct Answer: B
Rationale: The clinical text explicitly states that gout (arthritis urica) is inflammation of joints caused by the deposit of mononatrium-urate-monohydrate (MNU) crystals in the tissues. This is the defining characteristic of gout. Calcium pyrophosphate dihydrate crystals are associated with pseudogout, a common differential diagnosis.
Question 34
A 60-year-old male presents with recurrent episodes of acute inflammatory arthritis. His serum uric acid levels are elevated.
View Answer & Explanation
Correct Answer: B
Rationale: The provided text states that the prevalence of gout is 5–28‰ in males. Option E (1-6‰) refers to the prevalence in females, which is significantly lower.
Question 35
A 48-year-old male with a family history of gout presents with his first episode of acute monoarticular arthritis. Laboratory tests reveal hyperuricemia without any other identifiable systemic illness or medication use.
View Answer & Explanation
Correct Answer: C
Rationale: The clinical text defines primary gout as being caused by hyperuricemia, which is the consequence of a hereditary disorder of metabolism. The patient's family history and absence of other systemic causes align with this definition. Secondary gout is associated with hyperuricemia triggered by other identifiable causes like myeloproliferative disease or kidney malfunction.
Question 36
A 65-year-old female presents with a swollen, painful knee. Arthrocentesis is performed.
View Answer & Explanation
Correct Answer: D
Rationale: The clinical text explicitly states, "The presence of MNU crystals in the tophus specimen or in the synovial fluid leads to a safe diagnosis." This is the gold standard for diagnosing gout. Elevated WBC count can be seen in various inflammatory conditions, and negative bacterial culture rules out septic arthritis but doesn't confirm gout. Calcium pyrophosphate crystals indicate pseudogout.
Question 37
A 70-year-old male presents with chronic, progressively worsening hand deformities. On examination, his fingers are deformed, and the phalangeal joints are swollen with tight, hot, and dark-red skin. He also reports occasional low-grade fever.
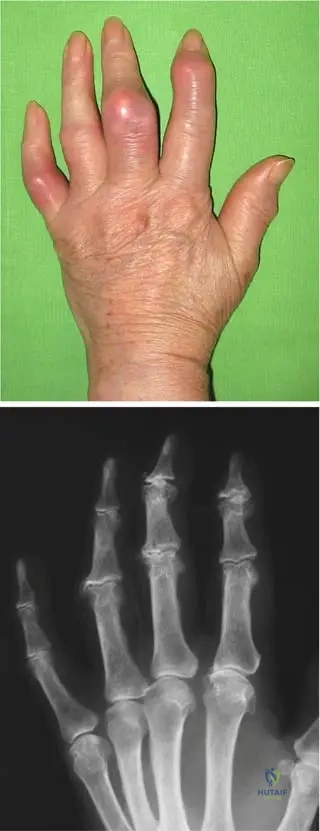
View Answer & Explanation
Correct Answer: C
Rationale: The clinical context for Fig. 7.2 a, b directly describes this scenario as "Exacerbation of a chronic gout process in the hand: the fingers are deformed, the joints of the phalanges are swollen, with tight, hot, and dark-red skin, frequently accompanied by some general symptoms (fever, higher sedimentation rate, increased number of white blood cells)." While acute symptoms are present, the underlying chronicity and deformities point to an exacerbation of a chronic condition.
Question 38
A 68-year-old male with a long history of gout presents with chronic hand pain and deformities. A radiograph of his hand is obtained.

View Answer & Explanation
Correct Answer: C
Rationale: The clinical context for Fig. 7.2 b states that the radiograph of a patient with chronic gout presents "narrowed joint spaces, and typical punched-out periarticular lytic lesions." These are classic radiographic findings for chronic gouty arthropathy. Option B describes some features that can be seen, but "punched-out lytic lesions" are highly characteristic.
Question 39
A 75-year-old male with poorly controlled gout for several decades presents with multiple firm, non-tender nodules in his palmar region.
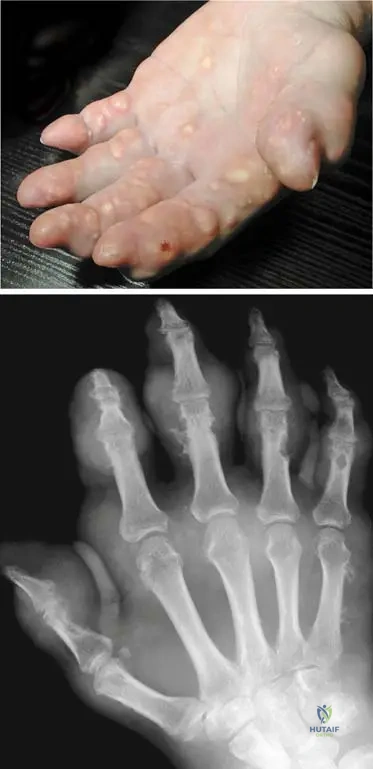
View Answer & Explanation
Correct Answer: C
Rationale: The clinical context for Fig. 7.3 a, b explicitly states, "Late stage of gout: numerous subcutaneous tophi are present in the palmar region." Tophi are characteristic subcutaneous deposits of urate crystals in chronic, uncontrolled gout. Heberden's and Bouchard's nodes are associated with osteoarthritis, and rheumatoid nodules with rheumatoid arthritis.
Question 40
A 72-year-old male with a history of chronic gout presents with hand pain. Radiographs reveal soft tissue masses around the small joints of the hand.

View Answer & Explanation
Correct Answer: C
Rationale: The clinical context for Fig. 7.3 b states, "These tophaceus gouty deposits are also visible in the radiograph around the small joints of the hand." Tophi are the hallmark of late-stage chronic gout and can appear as soft tissue masses on radiographs. Chondrocalcinosis is calcification of cartilage, typically associated with pseudogout.
Question 41
A 58-year-old male presents to the emergency department with sudden, excruciating pain and swelling in his left knee. Examination reveals a hot, erythematous, and exquisitely tender knee joint.
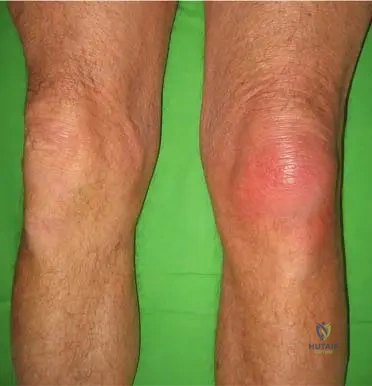
View Answer & Explanation
Correct Answer: D
Rationale: While the first metatarsophalangeal joint (podagra) is the most common site for acute gout, the clinical context for Fig. 7.4 explicitly shows an "Acute gout spasm of the left knee," indicating that the knee is another frequently affected large joint. The ankle is also a common site, but the image specifically depicts the knee.
Question 42
A 62-year-old male undergoes arthroscopy for chronic knee pain and suspected inflammatory arthritis. During the procedure, white, chalky deposits are noted within the joint.
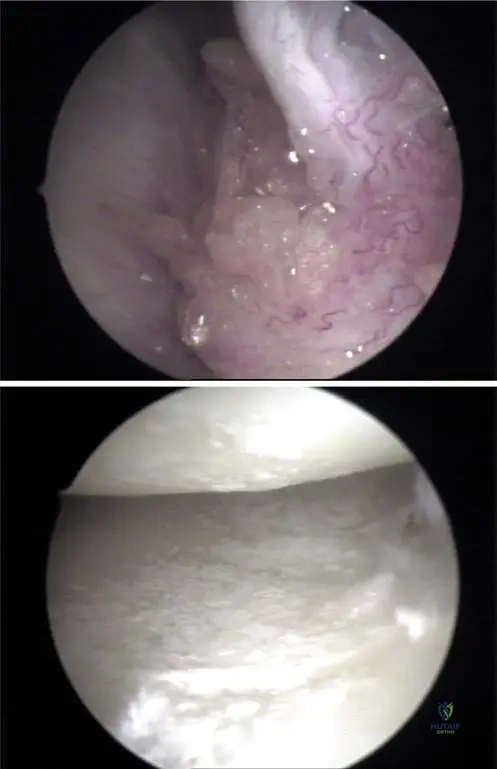
View Answer & Explanation
Correct Answer: C
Rationale: The clinical context for Fig. 7.5 a, b states, "Deposits of urate crystals may occur in the synovium (a) and in the cartilage of the knee joint (b) as visualized by arthroscopy." This indicates that both these tissues are common sites for urate crystal deposition within the joint. While menisci are cartilaginous structures, the description is more encompassing of the joint's cartilage and synovium.
Question 43
A 55-year-old male presents with sudden onset of severe pain, swelling, and redness in his right great toe. Examination reveals a hot, exquisitely tender, and swollen metatarsophalangeal joint. Radiographs show soft tissue swelling without acute bony changes. The most likely underlying cause of this condition is the deposition of which of the following?
View Answer & Explanation
Correct Answer: C
Rationale: The clinical presentation is classic for gout. The provided text explicitly states that gout is inflammation of joints caused by the deposit of mononatrium-urate-monohydrate (MNU) crystals in the tissues. Calcium pyrophosphate dihydrate crystals cause pseudogout, which is a common distractor but incorrect for gout.
Question 43
A 60-year-old male presents with a history of recurrent painful joint swelling. He asks about the general prevalence of his condition. Based on epidemiological data, the prevalence of gout is significantly higher in which demographic group?
View Answer & Explanation
Correct Answer: B
Rationale: The text states that the prevalence of gout is 5–28‰ in males and 1–6‰ in females, indicating a significantly higher prevalence in males. While age is not specified for the prevalence rates, gout is generally a disease of older adults, making males aged 50-60 years the most appropriate answer reflecting the higher male prevalence. Females aged 60-70 years would have a lower prevalence than males of similar age, and younger individuals (20-30 years) generally have lower rates.
Question 43
A 45-year-old male is diagnosed with gout. His workup reveals no obvious secondary causes such as myeloproliferative disease or kidney malfunction. His hyperuricemia is attributed to a hereditary metabolic disorder. This specific type of gout is best classified as:
View Answer & Explanation
Correct Answer: C
Rationale: The text explicitly defines primary gout as being caused by hyperuricemia, which is the consequence of a hereditary disorder of metabolism. Secondary gout is associated with hyperuricemia triggered by other causes, which are ruled out in this vignette. Idiopathic gout is not a classification mentioned, and pseudogout and septic arthritis are distinct conditions.
Question 43
A 70-year-old male with a known history of myeloproliferative disease develops acute, severe pain and swelling in his left knee. Arthrocentesis is performed, and synovial fluid analysis confirms the presence of mononatrium-urate-monohydrate crystals. Given his medical history, this presentation is most consistent with which type of gout?
View Answer & Explanation
Correct Answer: D
Rationale: The text states that secondary gout is associated with hyperuricemia triggered by other causes, such as increased disintegration of cells because of myeloproliferative disease. The patient's myeloproliferative disease is a direct cause of hyperuricemia, leading to secondary gout. Primary gout is due to hereditary metabolic disorder, and the other options are not classifications based on etiology.
Question 43
A 62-year-old female presents with chronic pain and swelling in her hands and feet. Multiple small, firm nodules are noted around her finger joints. To confirm the diagnosis of gout, which of the following findings would provide the most definitive diagnosis?
View Answer & Explanation
Correct Answer: C
Rationale: The text explicitly states, "The presence of MNU crystals in the tophus specimen or in the synovial fluid leads to a safe diagnosis." While elevated serum uric acid, radiographic changes, and family history are supportive, they are not definitive. Response to therapy is also not a definitive diagnostic criterion.
Question 43
A 68-year-old male presents with a long history of recurrent painful episodes in his hands. Examination reveals deformed fingers, swollen phalangeal joints, and areas of tight, hot, and dark-red skin over the affected joints. He also reports recent fever and fatigue. Which image best illustrates the clinical presentation of this patient's chronic condition?

View Answer & Explanation
Correct Answer: A
Rationale: Fig. 7.2 a is described as "Exacerbation of a chronic gout process in the hand: the fi ngers are deformed, the joints of the phalanges are swollen, with tight, hot, and dark-red skin, frequently accompanied by some general symptoms (fever, higher sedimentation rate, increased number of white blood cells)." This perfectly matches the clinical vignette. Fig. 7.3 a shows subcutaneous tophi in the palmar region, Fig. 7.4 shows acute knee gout, Fig. 7.9 shows olecranon bursitis, and Fig. 7.10 a shows intraoperative tophi, none of which fully capture the described chronic hand presentation with acute exacerbation symptoms.
Question 43
A 72-year-old male with a 20-year history of gout presents with progressively worsening hand pain and stiffness. Radiographs of his hands are obtained. Which of the following radiographic findings is characteristic of chronic gouty arthropathy?

View Answer & Explanation
Correct Answer: C
Rationale: The clinical context for Fig. 7.2 b explicitly states, "The radiograph of the same patient presents the characteristics of chronic gouty arthropathy, narrowed joint spaces, and typical punched-out periarticular lytic lesions." This directly matches option C. The other options describe features of other arthropathies (e.g., osteoarthritis, psoriatic arthritis, rheumatoid arthritis).
Question 43
A 75-year-old male with long-standing, poorly controlled gout presents with multiple firm, painless nodules under the skin of his palms and around his finger joints. These nodules are consistent with the late stage of gout. Which image best depicts this clinical finding?

View Answer & Explanation
Correct Answer: B
Rationale: Fig. 7.3 a is described as "Late stage of gout: numerous subcutaneous tophi are present in the palmar region." This directly corresponds to the patient's presentation of firm, painless nodules (tophi) in the palmar region. Fig. 7.2 a shows an acute exacerbation, Fig. 7.4 shows acute knee gout, Fig. 7.9 shows olecranon bursitis, and Fig. 7.10 a shows intraoperative tophi, none of which are the primary clinical depiction of subcutaneous tophi in the hand.
Question 43
A 65-year-old male with a history of chronic gout presents with significant deformities in his hands. Radiographs are ordered to assess the extent of his disease. In the late stage of gout, what specific radiographic finding related to deposits would be expected around the small joints of the hand?

View Answer & Explanation
Correct Answer: C
Rationale: The clinical context for Fig. 7.3 b states, "These tophaceus gouty deposits are also visible in the radiograph around the small joints of the hand." This directly answers the question. While other findings like joint effusions or subchondral cysts might be present, tophaceous deposits are a specific characteristic of late-stage gout visible on radiographs.
Question 43
A 58-year-old male presents to the emergency department with sudden, excruciating pain and swelling in his left knee, making it impossible to bear weight. Examination reveals a hot, red, and swollen knee joint with limited range of motion. This presentation is most consistent with an acute gout attack. Which image best illustrates this specific clinical scenario?

View Answer & Explanation
Correct Answer: C
Rationale: Fig. 7.4 is explicitly labeled "Acute gout spasm of the left knee," which perfectly matches the clinical vignette describing an acute gout attack in the knee. The other images depict chronic hand gout, subcutaneous tophi, olecranon bursitis, or intraoperative findings, not an acute knee presentation.
Question 43
A 50-year-old male undergoes arthroscopy for chronic knee pain and suspected gout. During the procedure, the surgeon observes white, chalky deposits within the joint. According to the provided information, where might these urate crystals be found within the knee joint during arthroscopy?

View Answer & Explanation
Correct Answer: C
Rationale: The clinical context for Fig. 7.5 a states, "Deposits of urate crystals may occur in the synovium (a) and in the cartilage of the knee joint (b) as visualized by arthroscopy." Therefore, finding crystals within the synovium is a correct arthroscopic observation. While they can also be in cartilage, "only" options are often incorrect, and synovium is a distinct location mentioned.
Question 43
During an arthroscopic examination of a 60-year-old male's knee, the surgeon notes glistening white deposits on the joint surfaces. These deposits are consistent with urate crystals. Based on the provided images and context, where else within the knee joint might these urate crystals be visualized arthroscopically?

View Answer & Explanation
Correct Answer: B
Rationale: The clinical context for Fig. 7.5 b states, "Deposits of urate crystals may occur in the synovium (a) and in the cartilage of the knee joint (b) as visualized by arthroscopy." Therefore, finding crystals on the articular cartilage is a correct arthroscopic observation. The other options are not mentioned as specific arthroscopic locations for urate crystal deposits in the provided text.
Question 43
A biopsy of a subcutaneous nodule from a 70-year-old male with chronic gout is sent for histopathological examination. Under the microscope, a characteristic feature of tophus formation is observed. What does the eosinophile-stained amorphous central area of a tophus represent?
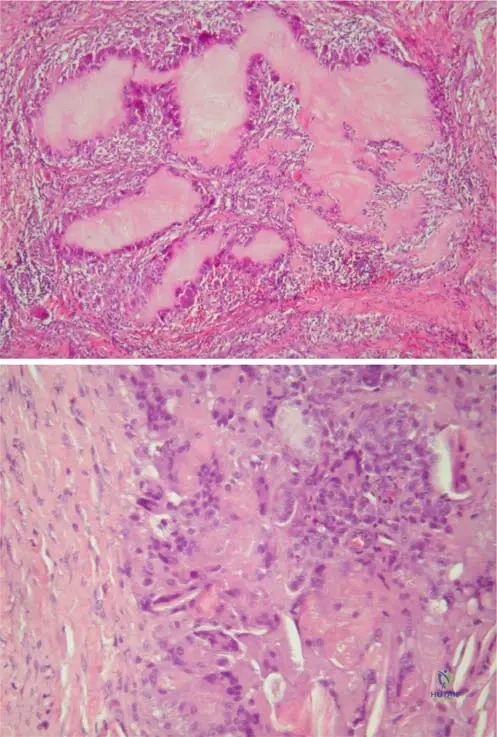
View Answer & Explanation
Correct Answer: C
Rationale: The clinical context for Fig. 7.6 a states, "Tophus formation is characteristic of gout: eosinophile-stained amorphous central area represents the urate crystals, which dissolved in processing through waterbased solutions." This directly identifies the nature of the central amorphous area. Fibrinoid necrosis is associated with rheumatoid nodules, and calcium deposits with pseudogout or other calcific conditions.
Question 43
Histopathological examination of a tophus from a 65-year-old male reveals a characteristic cellular reaction surrounding the central amorphous area. What type of cellular reaction is typically observed in response to urate deposits in a tophus?

View Answer & Explanation
Correct Answer: D
Rationale: The clinical context for Fig. 7.6 b states, "Higher magnifi cation illustrates the histiocytic and giant cell reaction to urate deposits (slit-like space) in tophus." This directly describes the characteristic cellular response. Neutrophilic infiltration is more typical of acute gout, while lymphocytic/plasma cell infiltration is seen in chronic inflammatory conditions like rheumatoid arthritis, but not specifically described for tophi in the text.
Question 43
A 70-year-old male with a long history of gout presents with a large, firm, non-tender mass over his left elbow. Examination reveals significant swelling and a palpable nodule in the olecranon region. This finding is consistent with a massive tophaceous deposit of urate crystals. Which image best illustrates this specific presentation?
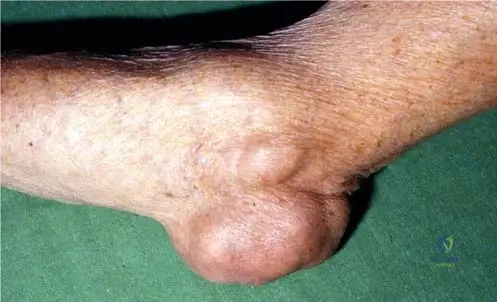
View Answer & Explanation
Correct Answer: D
Rationale: Fig. 7.9 is explicitly labeled "Bursitis olecrani due to the massive tophaceus deposit of urate crystals." This perfectly matches the clinical vignette describing a tophaceous mass over the olecranon. The other images depict chronic hand gout, subcutaneous tophi in the palm, acute knee gout, or intraoperative findings, not specifically olecranon bursitis.
Question 43
During surgical excision of a large tophus from the elbow of a 68-year-old male with chronic gout, the surgeon encounters a distinctive mass. What is the characteristic gross appearance of a gouty tophus as observed intraoperatively?
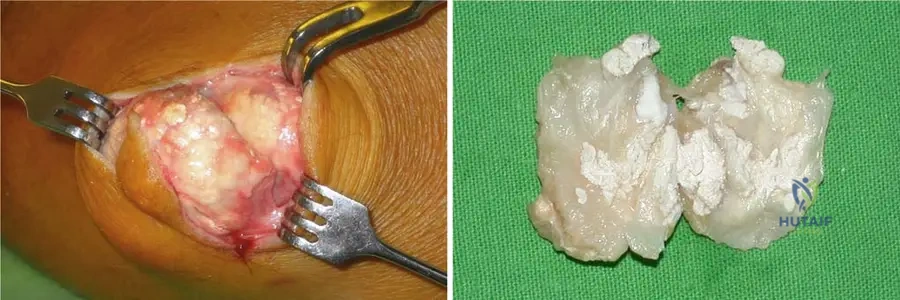
View Answer & Explanation
Correct Answer: B
Rationale: The clinical context for Fig. 7.10 a states, "The intraoperative picture demonstrates the encapsulated yellow chalky mass of gouty tophi." This directly describes the gross appearance. The other options describe features inconsistent with gouty tophi.
Question 43
A 52-year-old male presents with recurrent episodes of acute inflammatory arthritis. Synovial fluid analysis confirms the presence of crystals characteristic of gout. These crystals are composed of which specific chemical substance?
View Answer & Explanation
Correct Answer: C
Rationale: The introductory text states, "The gout (arthritis urica) is infl ammation of joints caused by the deposit of mononatrium-urate-monohydrate (MNU) crystals in the tissues." This identifies the specific chemical composition of the crystals responsible for gout. Calcium pyrophosphate dihydrate causes pseudogout.
Question 43
A 60-year-old male with chronic gout experiences an acute exacerbation in his hand, presenting with deformed fingers, swollen joints, and hot, dark-red skin. In addition to these local symptoms, what general systemic symptoms are frequently observed during such an exacerbation?

View Answer & Explanation
Correct Answer: B
Rationale: The clinical context for Fig. 7.2 a states that exacerbations are "frequently accompanied by some general symptoms (fever, higher sedimentation rate, increased number of white blood cells)." This directly matches option B. The other options describe physiological states inconsistent with an acute inflammatory process.
Question 43
A 48-year-old male is diagnosed with gout. His physician discusses the multifactorial nature of the disease. Beyond the direct deposit of mononatrium-urate-monohydrate crystals, the manifestation of gout is also influenced by which combination of factors?
View Answer & Explanation
Correct Answer: B
Rationale: The introductory text states, "Th e manifestation of the illness is also due to environmental as well as genetic, sexual, and ethnic factors." This directly matches option B. While dietary habits can influence gout, the provided text specifically lists the broader categories in option B as influencing manifestation.
Question 43
A researcher is studying the ultrastructure of sodium urate crystals found in gout patients. To visualize these crystals at a very high magnification, which imaging technique would be most appropriate, as demonstrated in the provided clinical images?

View Answer & Explanation
Correct Answer: C
Rationale: Fig. 7.13 is explicitly labeled "The electron microscope image of sodium urate crystals (magnifi cation: ×6,600)." This indicates that electron microscopy is the technique used for high-magnification visualization of these crystals in the provided context. While polarized light microscopy is used for routine crystal identification in synovial fluid, the question refers to the provided image and high magnification, making electron microscopy the correct answer.
Question 43
A 55-year-old male presents with sudden onset of severe pain, swelling, and redness in his right great toe. Examination reveals a hot, exquisitely tender, and swollen metatarsophalangeal joint. Radiographs show soft tissue swelling without acute bony changes. The most likely underlying cause of this condition is the deposition of which of the following?
View Answer & Explanation
Correct Answer: C
Rationale: The clinical presentation is classic for gout. The provided text explicitly states that gout is inflammation of joints caused by the deposit of mononatrium-urate-monohydrate (MNU) crystals in the tissues. Calcium pyrophosphate dihydrate crystals cause pseudogout, which is a common distractor but incorrect for gout.
Question 43
A 60-year-old male presents with a history of recurrent painful joint swelling. He asks about the general prevalence of his condition. Based on epidemiological data, the prevalence of gout is significantly higher in which demographic group?
View Answer & Explanation
Correct Answer: B
Rationale: The text states that the prevalence of gout is 5–28‰ in males and 1–6‰ in females, indicating a significantly higher prevalence in males. While age is not specified for the prevalence rates, gout is generally a disease of older adults, making males aged 50-60 years the most appropriate answer reflecting the higher male prevalence. Females aged 60-70 years would have a lower prevalence than males of similar age, and younger individuals (20-30 years) generally have lower rates.
Question 43
A 45-year-old male is diagnosed with gout. His workup reveals no obvious secondary causes such as myeloproliferative disease or kidney malfunction. His hyperuricemia is attributed to a hereditary metabolic disorder. This specific type of gout is best classified as:
View Answer & Explanation
Correct Answer: CRationale: The text explicitly defines primary gout as being caused by hyperuricemia, which is the consequence of a hereditary disorder of metabolism. Secondary gout is associated with hyperuricemia triggered by other causes, which are ruled out in this vignette. Idiopathic gout is not a classification mentioned, and pseudogout and septic arthritis are distinct conditions.
Question 43
A 70-year-old male with a known history of myeloproliferative disease develops acute, severe pain and swelling in his left knee. Arthrocentesis is performed, and synovial fluid analysis confirms the presence of mononatrium-urate-monohydrate crystals. Given his medical history, this presentation is most consistent with which type of gout?
View Answer & Explanation
Correct Answer: D
Rationale: The text states that secondary gout is associated with hyperuricemia triggered by other causes, such as increased disintegration of cells because of myeloproliferative disease. The patient's myeloproliferative disease is a direct cause of hyperuricemia, leading to secondary gout. Primary gout is due to hereditary metabolic disorder, and the other options are not classifications based on etiology.
Question 43
A 62-year-old female presents with chronic pain and swelling in her hands and feet. Multiple small, firm nodules are noted around her finger joints. To confirm the diagnosis of gout, which of the following findings would provide the most definitive diagnosis?
View Answer & Explanation
Correct Answer: C
Rationale: The text explicitly states, "The presence of MNU crystals in the tophus specimen or in the synovial fluid leads to a safe diagnosis." While elevated serum uric acid, radiographic changes, and family history are supportive, they are not definitive. Response to therapy is also not a definitive diagnostic criterion.
Question 43
A 68-year-old male presents with a long history of recurrent painful episodes in his hands. Examination reveals deformed fingers, swollen phalangeal joints, and areas of tight, hot, and dark-red skin over the affected joints. He also reports recent fever and fatigue. Which image best illustrates the clinical presentation of this patient's chronic condition?

View Answer & Explanation
Correct Answer: A
Rationale: Fig. 7.2 a is described as "Exacerbation of a chronic gout process in the hand: the fi ngers are deformed, the joints of the phalanges are swollen, with tight, hot, and dark-red skin, frequently accompanied by some general symptoms (fever, higher sedimentation rate, increased number of white blood cells)." This perfectly matches the clinical vignette. Fig. 7.3 a shows subcutaneous tophi in the palmar region, Fig. 7.4 shows acute knee gout, Fig. 7.9 shows olecranon bursitis, and Fig. 7.10 a shows intraoperative tophi, none of which fully capture the described chronic hand presentation with acute exacerbation symptoms.
Question 43
A 72-year-old male with a 20-year history of gout presents with progressively worsening hand pain and stiffness. Radiographs of his hands are obtained. Which of the following radiographic findings is characteristic of chronic gouty arthropathy?

View Answer & Explanation
Correct Answer: C
Rationale: The clinical context for Fig. 7.2 b explicitly states, "The radiograph of the same patient presents the characteristics of chronic gouty arthropathy, narrowed joint spaces, and typical punched-out periarticular lytic lesions." This directly matches option C. The other options describe features of other arthropathies (e.g., osteoarthritis, psoriatic arthritis, rheumatoid arthritis).
Question 43
A 75-year-old male with long-standing, poorly controlled gout presents with multiple firm, painless nodules under the skin of his palms and around his finger joints. These nodules are consistent with the late stage of gout. Which image best depicts this clinical finding?

View Answer & Explanation
Correct Answer: B
Rationale: Fig. 7.3 a is described as "Late stage of gout: numerous subcutaneous tophi are present in the palmar region." This directly corresponds to the patient's presentation of firm, painless nodules (tophi) in the palmar region. Fig. 7.2 a shows an acute exacerbation, Fig. 7.4 shows acute knee gout, Fig. 7.9 shows olecranon bursitis, and Fig. 7.10 a shows intraoperative tophi, none of which are the primary clinical depiction of subcutaneous tophi in the hand.
Question 43
A 65-year-old male with a history of chronic gout presents with significant deformities in his hands. Radiographs are ordered to assess the extent of his disease. In the late stage of gout, what specific radiographic finding related to deposits would be expected around the small joints of the hand?

View Answer & Explanation
Correct Answer: C
Rationale: The clinical context for Fig. 7.3 b states, "These tophaceus gouty deposits are also visible in the radiograph around the small joints of the hand." This directly answers the question. While other findings like joint effusions or subchondral cysts might be present, tophaceous deposits are a specific characteristic of late-stage gout visible on radiographs.
Question 43
A 58-year-old male presents to the emergency department with sudden, excruciating pain and swelling in his left knee, making it impossible to bear weight. Examination reveals a hot, red, and swollen knee joint with limited range of motion. This presentation is most consistent with an acute gout attack. Which image best illustrates this specific clinical scenario?

View Answer & Explanation
Correct Answer: C
Rationale: Fig. 7.4 is explicitly labeled "Acute gout spasm of the left knee," which perfectly matches the clinical vignette describing an acute gout attack in the knee. The other images depict chronic hand gout, subcutaneous tophi, olecranon bursitis, or intraoperative findings, not an acute knee presentation.
Question 43
A 50-year-old male undergoes arthroscopy for chronic knee pain and suspected gout. During the procedure, the surgeon observes white, chalky deposits within the joint. According to the provided information, where might these urate crystals be found within the knee joint during arthroscopy?

View Answer & Explanation
Correct Answer: C
Rationale: The clinical context for Fig. 7.5 a states, "Deposits of urate crystals may occur in the synovium (a) and in the cartilage of the knee joint (b) as visualized by arthroscopy." Therefore, finding crystals within the synovium is a correct arthroscopic observation. While they can also be in cartilage, "only" options are often incorrect, and synovium is a distinct location mentioned.
Question 43
During an arthroscopic examination of a 60-year-old male's knee, the surgeon notes glistening white deposits on the joint surfaces. These deposits are consistent with urate crystals. Based on the provided images and context, where else within the knee joint might these urate crystals be visualized arthroscopically?

View Answer & Explanation
Correct Answer: B
Rationale: The clinical context for Fig. 7.5 b states, "Deposits of urate crystals may occur in the synovium (a) and in the cartilage of the knee joint (b) as visualized by arthroscopy." Therefore, finding crystals on the articular cartilage is a correct arthroscopic observation. The other options are not mentioned as specific arthroscopic locations for urate crystal deposits in the provided text.
Question 43
A biopsy of a subcutaneous nodule from a 70-year-old male with chronic gout is sent for histopathological examination. Under the microscope, a characteristic feature of tophus formation is observed. What does the eosinophile-stained amorphous central area of a tophus represent?

View Answer & Explanation
Correct Answer: C
Rationale: The clinical context for Fig. 7.6 a states, "Tophus formation is characteristic of gout: eosinophile-stained amorphous central area represents the urate crystals, which dissolved in processing through waterbased solutions." This directly identifies the nature of the central amorphous area. Fibrinoid necrosis is associated with rheumatoid nodules, and calcium deposits with pseudogout or other calcific conditions.
Question 43
Histopathological examination of a tophus from a 65-year-old male reveals a characteristic cellular reaction surrounding the central amorphous area. What type of cellular reaction is typically observed in response to urate deposits in a tophus?

View Answer & Explanation
Correct Answer: D
Rationale: The clinical context for Fig. 7.6 b states, "Higher magnifi cation illustrates the histiocytic and giant cell reaction to urate deposits (slit-like space) in tophus." This directly describes the characteristic cellular response. Neutrophilic infiltration is more typical of acute gout, while lymphocytic/plasma cell infiltration is seen in chronic inflammatory conditions like rheumatoid arthritis, but not specifically described for tophi in the text.
Question 43
A 70-year-old male with a long history of gout presents with a large, firm, non-tender mass over his left elbow. Examination reveals significant swelling and a palpable nodule in the olecranon region. This finding is consistent with a massive tophaceous deposit of urate crystals. Which image best illustrates this specific presentation?

View Answer & Explanation
Correct Answer: D
Rationale: Fig. 7.9 is explicitly labeled "Bursitis olecrani due to the massive tophaceus deposit of urate crystals." This perfectly matches the clinical vignette describing a tophaceous mass over the olecranon. The other images depict chronic hand gout, subcutaneous tophi in the palm, acute knee gout, or intraoperative findings, not specifically olecranon bursitis.
Question 43
During surgical excision of a large tophus from the elbow of a 68-year-old male with chronic gout, the surgeon encounters a distinctive mass. What is the characteristic gross appearance of a gouty tophus as observed intraoperatively?

View Answer & Explanation
Correct Answer: B
Rationale: The clinical context for Fig. 7.10 a states, "The intraoperative picture demonstrates the encapsulated yellow chalky mass of gouty tophi." This directly describes the gross appearance. The other options describe features inconsistent with gouty tophi.
Question 43
A 52-year-old male presents with recurrent episodes of acute inflammatory arthritis. Synovial fluid analysis confirms the presence of crystals characteristic of gout. These crystals are composed of which specific chemical substance?
View Answer & Explanation
Correct Answer: C
Rationale: The introductory text states, "The gout (arthritis urica) is infl ammation of joints caused by the deposit of mononatrium-urate-monohydrate (MNU) crystals in the tissues." This identifies the specific chemical composition of the crystals responsible for gout. Calcium pyrophosphate dihydrate causes pseudogout.
Question 43
A 60-year-old male with chronic gout experiences an acute exacerbation in his hand, presenting with deformed fingers, swollen joints, and hot, dark-red skin. In addition to these local symptoms, what general systemic symptoms are frequently observed during such an exacerbation?

View Answer & Explanation
Correct Answer: B
Rationale: The clinical context for Fig. 7.2 a states that exacerbations are "frequently accompanied by some general symptoms (fever, higher sedimentation rate, increased number of white blood cells)." This directly matches option B. The other options describe physiological states inconsistent with an acute inflammatory process.
Question 43
A 48-year-old male is diagnosed with gout. His physician discusses the multifactorial nature of the disease. Beyond the direct deposit of mononatrium-urate-monohydrate crystals, the manifestation of gout is also influenced by which combination of factors?
View Answer & Explanation
Correct Answer: B
Rationale: The introductory text states, "Th e manifestation of the illness is also due to environmental as well as genetic, sexual, and ethnic factors." This directly matches option B. While dietary habits can influence gout, the provided text specifically lists the broader categories in option B as influencing manifestation.
Question 43
A researcher is studying the ultrastructure of sodium urate crystals found in gout patients. To visualize these crystals at a very high magnification, which imaging technique would be most appropriate, as demonstrated in the provided clinical images?

View Answer & Explanation
Correct Answer: C
Rationale: Fig. 7.13 is explicitly labeled "The electron microscope image of sodium urate crystals (magnifi cation: ×6,600)." This indicates that electron microscopy is the technique used for high-magnification visualization of these crystals in the provided context. While polarized light microscopy is used for routine crystal identification in synovial fluid, the question refers to the provided image and high magnification, making electron microscopy the correct answer.
Question 44
A 55-year-old male presents with sudden onset of severe pain, swelling, and redness in his right great toe. Examination reveals a hot, exquisitely tender, and swollen metatarsophalangeal joint. Radiographs show soft tissue swelling without acute bony changes. The most likely underlying cause of this condition is the deposition of which of the following?
View Answer & Explanation
Correct Answer: C
Rationale: The clinical presentation is classic for gout. The provided text explicitly states that gout is inflammation of joints caused by the deposit of mononatrium-urate-monohydrate (MNU) crystals in the tissues. Calcium pyrophosphate dihydrate crystals cause pseudogout, which is a common distractor but incorrect for gout.
Question 45
A 60-year-old male presents with a history of recurrent painful joint swelling. He asks about the general prevalence of his condition. Based on epidemiological data, the prevalence of gout is significantly higher in which demographic group?
View Answer & Explanation
Correct Answer: B
Rationale: The text states that the prevalence of gout is 5–28‰ in males and 1–6‰ in females, indicating a significantly higher prevalence in males. While age is not specified for the prevalence rates, gout is generally a disease of older adults, making males aged 50-60 years the most appropriate answer reflecting the higher male prevalence. Females aged 60-70 years would have a lower prevalence than males of similar age, and younger individuals (20-30 years) generally have lower rates.
Question 46
A 45-year-old male is diagnosed with gout. His workup reveals no obvious secondary causes such as myeloproliferative disease or kidney malfunction. His hyperuricemia is attributed to a hereditary metabolic disorder. This specific type of gout is best classified as:
View Answer & Explanation
Correct Answer: CRationale: The text explicitly defines primary gout as being caused by hyperuricemia, which is the consequence of a hereditary disorder of metabolism. Secondary gout is associated with hyperuricemia triggered by other causes, which are ruled out in this vignette. Idiopathic gout is not a classification mentioned, and pseudogout and septic arthritis are distinct conditions.
Question 47
A 70-year-old male with a known history of myeloproliferative disease develops acute, severe pain and swelling in his left knee. Arthrocentesis is performed, and synovial fluid analysis confirms the presence of mononatrium-urate-monohydrate crystals. Given his medical history, this presentation is most consistent with which type of gout?
View Answer & Explanation
Correct Answer: D
Rationale: The text states that secondary gout is associated with hyperuricemia triggered by other causes, such as increased disintegration of cells because of myeloproliferative disease. The patient's myeloproliferative disease is a direct cause of hyperuricemia, leading to secondary gout. Primary gout is due to hereditary metabolic disorder, and the other options are not classifications based on etiology.
Question 48
A 62-year-old female presents with chronic pain and swelling in her hands and feet. Multiple small, firm nodules are noted around her finger joints. To confirm the diagnosis of gout, which of the following findings would provide the most definitive diagnosis?
View Answer & Explanation
Correct Answer: C
Rationale: The text explicitly states, "The presence of MNU crystals in the tophus specimen or in the synovial fluid leads to a safe diagnosis." While elevated serum uric acid, radiographic changes, and family history are supportive, they are not definitive. Response to therapy is also not a definitive diagnostic criterion.
Question 49
A 68-year-old male presents with a long history of recurrent painful episodes in his hands. Examination reveals deformed fingers, swollen phalangeal joints, and areas of tight, hot, and dark-red skin over the affected joints. He also reports recent fever and fatigue. Which image best illustrates the clinical presentation of this patient's chronic condition?

View Answer & Explanation
Correct Answer: A
Rationale: Fig. 7.2 a is described as "Exacerbation of a chronic gout process in the hand: the fi ngers are deformed, the joints of the phalanges are swollen, with tight, hot, and dark-red skin, frequently accompanied by some general symptoms (fever, higher sedimentation rate, increased number of white blood cells)." This perfectly matches the clinical vignette. Fig. 7.3 a shows subcutaneous tophi in the palmar region, Fig. 7.4 shows acute knee gout, Fig. 7.9 shows olecranon bursitis, and Fig. 7.10 a shows intraoperative tophi, none of which fully capture the described chronic hand presentation with acute exacerbation symptoms.
Question 50
A 72-year-old male with a 20-year history of gout presents with progressively worsening hand pain and stiffness. Radiographs of his hands are obtained. Which of the following radiographic findings is characteristic of chronic gouty arthropathy?

View Answer & Explanation
Correct Answer: C
Rationale: The clinical context for Fig. 7.2 b explicitly states, "The radiograph of the same patient presents the characteristics of chronic gouty arthropathy, narrowed joint spaces, and typical punched-out periarticular lytic lesions." This directly matches option C. The other options describe features of other arthropathies (e.g., osteoarthritis, psoriatic arthritis, rheumatoid arthritis).
Question 51
A 75-year-old male with long-standing, poorly controlled gout presents with multiple firm, painless nodules under the skin of his palms and around his finger joints. These nodules are consistent with the late stage of gout. Which image best depicts this clinical finding?

View Answer & Explanation
Correct Answer: B
Rationale: Fig. 7.3 a is described as "Late stage of gout: numerous subcutaneous tophi are present in the palmar region." This directly corresponds to the patient's presentation of firm, painless nodules (tophi) in the palmar region. Fig. 7.2 a shows an acute exacerbation, Fig. 7.4 shows acute knee gout, Fig. 7.9 shows olecranon bursitis, and Fig. 7.10 a shows intraoperative tophi, none of which are the primary clinical depiction of subcutaneous tophi in the hand.
Question 52
A 65-year-old male with a history of chronic gout presents with significant deformities in his hands. Radiographs are ordered to assess the extent of his disease. In the late stage of gout, what specific radiographic finding related to deposits would be expected around the small joints of the hand?

View Answer & Explanation
Correct Answer: C
Rationale: The clinical context for Fig. 7.3 b states, "These tophaceus gouty deposits are also visible in the radiograph around the small joints of the hand." This directly answers the question. While other findings like joint effusions or subchondral cysts might be present, tophaceous deposits are a specific characteristic of late-stage gout visible on radiographs.
Question 53
A 58-year-old male presents to the emergency department with sudden, excruciating pain and swelling in his left knee, making it impossible to bear weight. Examination reveals a hot, red, and swollen knee joint with limited range of motion. This presentation is most consistent with an acute gout attack. Which image best illustrates this specific clinical scenario?

View Answer & Explanation
Correct Answer: C
Rationale: Fig. 7.4 is explicitly labeled "Acute gout spasm of the left knee," which perfectly matches the clinical vignette describing an acute gout attack in the knee. The other images depict chronic hand gout, subcutaneous tophi, olecranon bursitis, or intraoperative findings, not an acute knee presentation.
Question 54
A 50-year-old male undergoes arthroscopy for chronic knee pain and suspected gout. During the procedure, the surgeon observes white, chalky deposits within the joint. According to the provided information, where might these urate crystals be found within the knee joint during arthroscopy?

View Answer & Explanation
Correct Answer: C
Rationale: The clinical context for Fig. 7.5 a states, "Deposits of urate crystals may occur in the synovium (a) and in the cartilage of the knee joint (b) as visualized by arthroscopy." Therefore, finding crystals within the synovium is a correct arthroscopic observation. While they can also be in cartilage, "only" options are often incorrect, and synovium is a distinct location mentioned.
Question 55
During an arthroscopic examination of a 60-year-old male's knee, the surgeon notes glistening white deposits on the joint surfaces. These deposits are consistent with urate crystals. Based on the provided images and context, where else within the knee joint might these urate crystals be visualized arthroscopically?

View Answer & Explanation
Correct Answer: B
Rationale: The clinical context for Fig. 7.5 b states, "Deposits of urate crystals may occur in the synovium (a) and in the cartilage of the knee joint (b) as visualized by arthroscopy." Therefore, finding crystals on the articular cartilage is a correct arthroscopic observation. The other options are not mentioned as specific arthroscopic locations for urate crystal deposits in the provided text.
Question 56
A biopsy of a subcutaneous nodule from a 70-year-old male with chronic gout is sent for histopathological examination. Under the microscope, a characteristic feature of tophus formation is observed. What does the eosinophile-stained amorphous central area of a tophus represent?

View Answer & Explanation
Correct Answer: C
Rationale: The clinical context for Fig. 7.6 a states, "Tophus formation is characteristic of gout: eosinophile-stained amorphous central area represents the urate crystals, which dissolved in processing through waterbased solutions." This directly identifies the nature of the central amorphous area. Fibrinoid necrosis is associated with rheumatoid nodules, and calcium deposits with pseudogout or other calcific conditions.
Question 57
Histopathological examination of a tophus from a 65-year-old male reveals a characteristic cellular reaction surrounding the central amorphous area. What type of cellular reaction is typically observed in response to urate deposits in a tophus?

View Answer & Explanation
Correct Answer: D
Rationale: The clinical context for Fig. 7.6 b states, "Higher magnifi cation illustrates the histiocytic and giant cell reaction to urate deposits (slit-like space) in tophus." This directly describes the characteristic cellular response. Neutrophilic infiltration is more typical of acute gout, while lymphocytic/plasma cell infiltration is seen in chronic inflammatory conditions like rheumatoid arthritis, but not specifically described for tophi in the text.
Question 58
A 70-year-old male with a long history of gout presents with a large, firm, non-tender mass over his left elbow. Examination reveals significant swelling and a palpable nodule in the olecranon region. This finding is consistent with a massive tophaceous deposit of urate crystals. Which image best illustrates this specific presentation?

View Answer & Explanation
Correct Answer: D
Rationale: Fig. 7.9 is explicitly labeled "Bursitis olecrani due to the massive tophaceus deposit of urate crystals." This perfectly matches the clinical vignette describing a tophaceous mass over the olecranon. The other images depict chronic hand gout, subcutaneous tophi in the palm, acute knee gout, or intraoperative findings, not specifically olecranon bursitis.
Question 59
During surgical excision of a large tophus from the elbow of a 68-year-old male with chronic gout, the surgeon encounters a distinctive mass. What is the characteristic gross appearance of a gouty tophus as observed intraoperatively?

View Answer & Explanation
Correct Answer: B
Rationale: The clinical context for Fig. 7.10 a states, "The intraoperative picture demonstrates the encapsulated yellow chalky mass of gouty tophi." This directly describes the gross appearance. The other options describe features inconsistent with gouty tophi.
Question 60
A 52-year-old male presents with recurrent episodes of acute inflammatory arthritis. Synovial fluid analysis confirms the presence of crystals characteristic of gout. These crystals are composed of which specific chemical substance?
View Answer & Explanation
Correct Answer: C
Rationale: The introductory text states, "The gout (arthritis urica) is infl ammation of joints caused by the deposit of mononatrium-urate-monohydrate (MNU) crystals in the tissues." This identifies the specific chemical composition of the crystals responsible for gout. Calcium pyrophosphate dihydrate causes pseudogout.
Question 61
A 60-year-old male with chronic gout experiences an acute exacerbation in his hand, presenting with deformed fingers, swollen joints, and hot, dark-red skin. In addition to these local symptoms, what general systemic symptoms are frequently observed during such an exacerbation?

View Answer & Explanation
Correct Answer: B
Rationale: The clinical context for Fig. 7.2 a states that exacerbations are "frequently accompanied by some general symptoms (fever, higher sedimentation rate, increased number of white blood cells)." This directly matches option B. The other options describe physiological states inconsistent with an acute inflammatory process.
Question 62
A 48-year-old male is diagnosed with gout. His physician discusses the multifactorial nature of the disease. Beyond the direct deposit of mononatrium-urate-monohydrate crystals, the manifestation of gout is also influenced by which combination of factors?
View Answer & Explanation
Correct Answer: B
Rationale: The introductory text states, "Th e manifestation of the illness is also due to environmental as well as genetic, sexual, and ethnic factors." This directly matches option B. While dietary habits can influence gout, the provided text specifically lists the broader categories in option B as influencing manifestation.
Question 63
A 55-year-old female presents with generalized fatigue. Laboratory workup reveals elevated serum calcium and elevated parathyroid hormone (PTH) levels.
View Answer & Explanation
Correct Answer: C
Rationale: The provided text states that increased PTH consequently leads to increased bone resorption, allowing flow of calcium from bone to blood. This is a primary mechanism by which PTH elevates serum calcium. Option A is incorrect as PTH increases serum calcium. Options B and D are incorrect as PTH reduces renal clearance of calcium and increases intestinal calcium absorption, respectively.
Question 64
A 62-year-old male is diagnosed with primary hyperparathyroidism after presenting with recurrent kidney stones and elevated serum calcium.
View Answer & Explanation
Correct Answer: D
Rationale: The text explicitly states, "The most common cause [of primary hyperparathyroidism] is a benign parathyroid adenoma that loses its sensitivity to circulating calcium levels." Options A and B are less common causes of primary hyperparathyroidism. Options C and E are causes of secondary hyperparathyroidism.
Question 65
A 48-year-old female with a history of elevated PTH and hypercalcemia undergoes hand radiographs due to chronic hand pain.
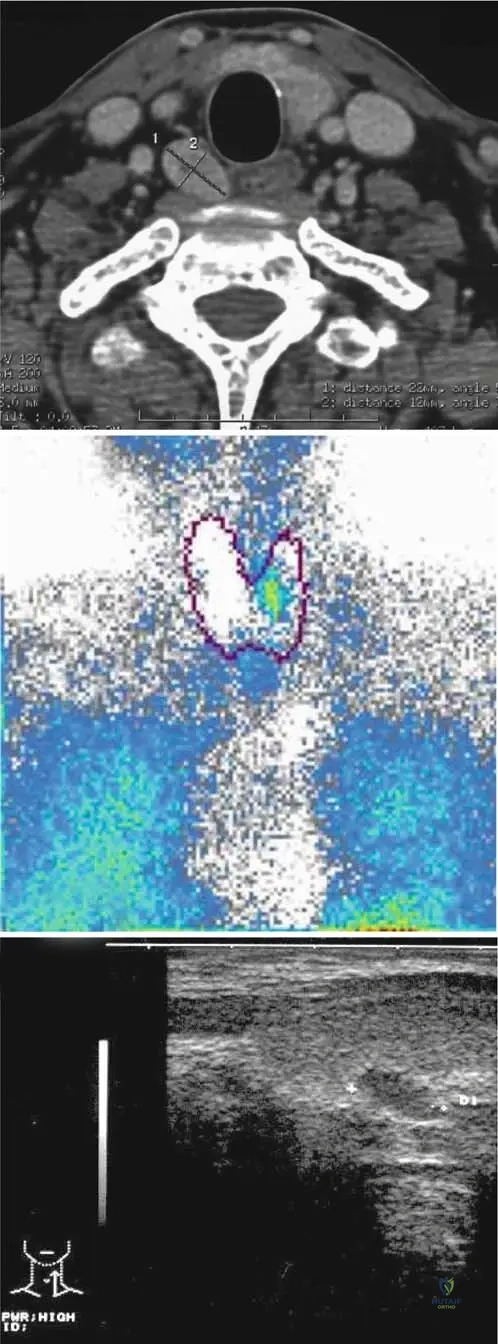
View Answer & Explanation
Correct Answer: C
Rationale: Fig. 7.43 and its accompanying description clearly state, "Primary hyperparathyroidism with subtle subperiostal bone resorption and local osteopenia of the phalanges." Options A and B are more characteristic of osteoarthritis. Options D and E are not the primary radiographic findings described for hyperparathyroidism in the phalanges.
Question 66
A 70-year-old patient with long-standing hyperparathyroidism presents for follow-up. A skull radiograph is obtained.
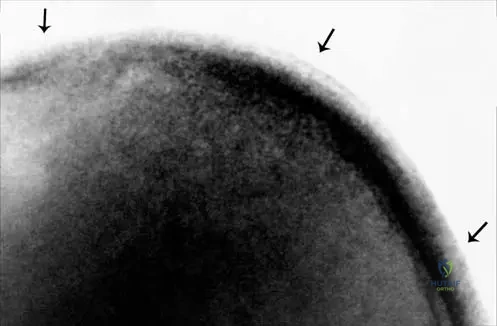
View Answer & Explanation
Correct Answer: B
Rationale: Fig. 7.49 and its description indicate "Bone resorptions in the skull – dominantly in the external cortical region (arrows)." Options A, C, D, and E are not the specific radiographic findings described for the skull in hyperparathyroidism in the provided text.
Question 67
A 58-year-old male with primary hyperparathyroidism undergoes biopsy of a lytic bone lesion.
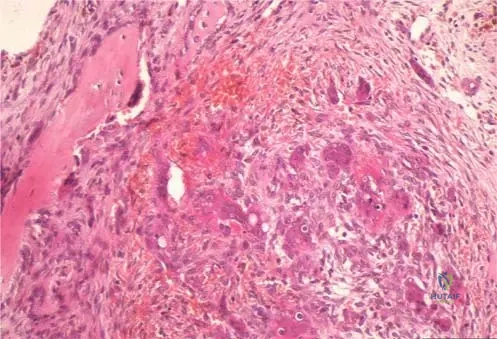
View Answer & Explanation
Correct Answer: C
Rationale: Fig. 7.50's description states, "This photomicrograph illustrates the characteristic histological feature of a brown tumor in hyperparathyroidism. Note the relative clustering of the osteoclast-type giant cells in fi brous tissue and reactive bone formation." Option D describes a malignant process, which is not characteristic of a benign brown tumor.
Question 68
A 45-year-old male with end-stage renal disease on hemodialysis develops elevated PTH and hypercalcemia.
View Answer & Explanation
Correct Answer: B
Rationale: The text defines, "Secondary hyperparathyroidism is due to resistance to the actions of PTH, usually because of chronic renal failure or malabsorption." Option A, primary hyperparathyroidism, results from dysfunction within the parathyroid glands themselves.
Question 69
A 60-year-old female presents with chronic bone pain and lytic lesions on radiographs, confirmed to be due to hyperparathyroidism.
View Answer & Explanation
Correct Answer: C
Rationale: The text states that manifestations of hyperparathyroidism involve "the skeletal system (bone pain due to fi brous tissue replacement, termed osteitis fi brosa cystica)." Options A, B, D, and E are distinct bone pathologies not specifically described as the fibrous tissue replacement seen in hyperparathyroidism.
Question 70
A 52-year-old male with newly diagnosed hyperparathyroidism reports a history of recurrent flank pain.
View Answer & Explanation
Correct Answer: C
Rationale: The text mentions, "Manifestations of hyperparathyroidism usually involve the kidney (stones)." Recurrent flank pain is a common symptom of kidney stones. Options A, B, D, and E are other renal conditions not directly linked to hyperparathyroidism in the provided text.
Question 71
A 65-year-old patient with primary hyperparathyroidism is being evaluated for hypercalcemia.
View Answer & Explanation
Correct Answer: B
Rationale: The text states, "Increased PTH consequently leads to... increases intestinal calcium absorption." This is one of the mechanisms by which PTH contributes to hypercalcemia. Option A is the opposite effect. Options C and D are also incorrect as PTH reduces renal clearance of calcium and increases bone resorption.
Question 72
A 59-year-old female presents with hypercalcemia and inappropriately elevated PTH levels. Imaging reveals a solitary parathyroid adenoma.
View Answer & Explanation
Correct Answer: B
Rationale: The text defines primary hyperparathyroidism as resulting "from dysfunction in the parathyroid glands themselves, with oversecretion of PTH." Option A describes secondary hyperparathyroidism. Options C, D, and E are not the primary defect in primary hyperparathyroidism.
Question 73
A 50-year-old female is diagnosed with primary hyperparathyroidism.
View Answer & Explanation
Correct Answer: D
Rationale: The text lists benign parathyroid adenoma, hyperplasia, and rarely carcinoma as causes of primary hyperparathyroidism. Chronic renal failure, however, is specifically mentioned as a cause of secondary hyperparathyroidism. Loss of sensitivity to circulating calcium levels is a characteristic of the adenoma causing primary hyperparathyroidism.
Question 74
A 72-year-old male is found to have elevated serum calcium and PTH
Question 74
A 55-year-old female presents with chronic fatigue and generalized bone pain. Laboratory tests reveal elevated serum calcium and parathyroid hormone (PTH) levels. Radiographs of her hands show subtle subperiosteal bone resorption and local osteopenia of the phalanges.

View Answer & Explanation
Correct Answer: D
Rationale: Increased parathyroid hormone (PTH) leads to increased serum calcium, increased bone resorption, reduced renal clearance of calcium, and increased intestinal calcium absorption. Therefore, increased intestinal calcium absorption is a direct consequence of excess PTH. Decreased serum calcium, decreased bone resorption, increased renal clearance of calcium, and decreased PTH production are all contrary to the effects of hyperparathyroidism.
Question 74
A 62-year-old male presents with recurrent kidney stones and a history of chronic generalized bone pain. Laboratory findings indicate elevated serum calcium and parathyroid hormone (PTH). Imaging reveals a solitary adenoma in the neck region. What is the most common cause of this patient's condition?
View Answer & Explanation
Correct Answer: C
Rationale: The most common cause of primary hyperparathyroidism, as described in the vignette with an adenoma and elevated PTH/calcium, is a benign parathyroid adenoma that loses its sensitivity to circulating calcium levels. Parathyroid hyperplasia and carcinoma are less common causes of primary hyperparathyroidism. Chronic renal failure and malabsorption syndrome are causes of secondary hyperparathyroidism, not primary.
Question 74
A 48-year-old female undergoes routine blood work which reveals hypercalcemia and elevated parathyroid hormone (PTH) levels. She reports no specific symptoms. Which of the following is a direct consequence of the excess PTH in her system?
View Answer & Explanation
Correct Answer: E
Rationale: Increased PTH consequently leads to increased serum calcium and increased bone resorption, allowing flow of calcium from bone to blood. While PTH does affect phosphate, the text specifically highlights calcium regulation. Increased bone formation, reduced calcium absorption, and enhanced renal clearance of calcium are all incorrect effects of PTH in hyperparathyroidism.
Question 74
A 70-year-old male presents with severe bone pain and multiple pathological fractures. Imaging studies reveal widespread lytic lesions and areas of fibrous tissue replacement within the bone. Histological examination of a bone biopsy shows osteoclast-type giant cells in fibrous tissue. What is the specific term for the skeletal involvement characterized by fibrous tissue replacement due to hyperparathyroidism?
View Answer & Explanation
Correct Answer: D
Rationale: The skeletal system manifestations of hyperparathyroidism, characterized by bone pain due to fibrous tissue replacement, are termed osteitis fibrosa cystica. Osteoporosis, osteomalacia, Paget's disease, and rickets are distinct bone disorders not specifically described as fibrous tissue replacement due to hyperparathyroidism in the provided text.
Question 74
A 58-year-old female with a known history of primary hyperparathyroidism presents to the emergency department with acute flank pain and hematuria. A CT scan reveals a 4 mm calculus in the left ureter. Which of the following is the most common renal manifestation of hyperparathyroidism?
View Answer & Explanation
Correct Answer: C
Rationale: Manifestations of hyperparathyroidism usually involve the kidney (stones) and the skeletal system. The patient's presentation with flank pain and a ureteral calculus directly points to kidney stones as the most common renal manifestation. While severe hyperparathyroidism can eventually lead to renal failure, kidney stones are the primary and most common renal manifestation mentioned.
Question 74
A 65-year-old male with a history of elevated serum calcium and PTH undergoes a skeletal survey. Radiographs of his hands, specifically the phalanges, show subtle changes. Which of the following radiographic findings is characteristic of primary hyperparathyroidism in the phalanges?

View Answer & Explanation
Correct Answer: C
Rationale: Fig. 7.43 illustrates "Primary hyperparathyroidism with subtle subperiosteal bone resorption and local osteopenia of the phalanges." This is a classic radiographic sign of hyperparathyroidism. The other options are characteristic of other conditions or not specifically mentioned as typical findings for hyperparathyroidism in the phalanges.
Question 74
A 50-year-old female with long-standing hyperparathyroidism undergoes a skull radiograph as part of her workup for bone pain. The radiograph reveals specific changes in the cranial vault. Which of the following describes the characteristic bone resorption pattern seen in the skull in hyperparathyroidism?

View Answer & Explanation
Correct Answer: C
Rationale: Fig. 7.49 shows "Bone resorptions in the skull – dominantly in the external cortical region (arrows)." This is a specific radiographic finding associated with hyperparathyroidism. The other options do not accurately describe the characteristic pattern of bone resorption in the skull as per the provided image and context.
Question 74
A 35-year-old male presents with a painful swelling in his tibia. Biopsy of the lesion is performed, and the photomicrograph reveals a characteristic histological feature associated with hyperparathyroidism. What is the key histological feature of a brown tumor?

View Answer & Explanation
Correct Answer: C
Rationale: Fig. 7.50 states: "This photomicrograph illustrates the characteristic histological feature of a brown tumor in hyperparathyroidism. Note the relative clustering of the osteoclast-type giant cells in fibrous tissue and reactive bone formation." This directly matches option C. The other options describe features not characteristic of a brown tumor in hyperparathyroidism.
Question 74
A 52-year-old female with a history of chronic renal failure develops elevated parathyroid hormone (PTH) levels and hypercalcemia. Her condition is diagnosed as secondary hyperparathyroidism. What is the underlying mechanism for secondary hyperparathyroidism in this patient?
View Answer & Explanation
Correct Answer: C
Rationale: Secondary hyperparathyroidism is due to resistance to the actions of PTH, usually because of chronic renal failure or malabsorption. Options A, B, and D are causes of primary hyperparathyroidism. Option E describes primary hyperparathyroidism, not secondary.
Question 74
A 68-year-old male is diagnosed with primary hyperparathyroidism. His laboratory results show elevated serum calcium and PTH. Regarding renal function, how does increased PTH affect calcium handling in the kidneys?
View Answer & Explanation
Correct Answer: C
Rationale: Increased PTH consequently leads to increased serum calcium, increased bone resorption, and reduces renal clearance of calcium. This means less calcium is excreted in the urine, contributing to hypercalcemia. Options A, B, and E are incorrect as they describe increased calcium excretion or decreased reabsorption. Option D is incorrect as PTH has a significant effect.
Question 74
A 45-year-old female undergoes a routine health check-up. Blood tests reveal mildly elevated serum calcium and parathyroid hormone (PTH) levels. She denies any symptoms such as bone pain, kidney stones, or fatigue. What is a common characteristic of patients with hyperparathyroidism regarding their symptomatic status?
View Answer & Explanation
Correct Answer: C
Rationale: The text explicitly states: "The majority of patients with hyperparathyroidism are asymptomatic." This makes option C the correct answer. Options A, B, D, and E are incorrect as they describe universal or specific severe symptoms, which contradicts the asymptomatic nature in most cases.
Question 74
A 60-year-old male with a long history of end-stage renal disease on dialysis develops persistently elevated parathyroid hormone (PTH) levels and progressive bone disease. His condition is diagnosed as secondary hyperparathyroidism. Which of the following is the most common underlying cause of secondary hyperparathyroidism?
View Answer & Explanation
Correct Answer: C
Rationale: Secondary hyperparathyroidism is due to resistance to the actions of PTH, usually because of chronic renal failure or malabsorption. Given the patient's history of end-stage renal disease, chronic renal failure is the most common underlying cause. Parathyroid adenoma and carcinoma are causes of primary hyperparathyroidism. Vitamin D toxicity and hyperthyroidism are not listed as causes of secondary hyperparathyroidism in the provided text.
Question 74
A 40-year-old female with primary hyperparathyroidism develops a lytic lesion in her femur. A biopsy confirms the diagnosis of a "brown tumor." What is the nature of these bony involvements in hyperparathyroidism?
View Answer & Explanation
Correct Answer: C
Rationale: The text states: "The bony involvements are also named as brown tumors." And further, Fig. 7.50 describes the histology as "relative clustering of the osteoclast-type giant cells in fibrous tissue and reactive bone formation." This confirms that brown tumors are areas of fibrous tissue replacement and reactive bone formation, not true neoplasms, infections, or metastases.
Question 74
A 50-year-old male presents with generalized weakness and polyuria. Initial laboratory tests show elevated parathyroid hormone (PTH) levels. What is the expected serum calcium level in a patient with hyperparathyroidism?
View Answer & Explanation
Correct Answer: C
Rationale: Hyperparathyroidism is overactivity of the parathyroid glands resulting in excess production of parathyroid hormone (PTH). Increased PTH consequently leads to increased serum calcium. Therefore, an increased serum calcium level is expected.
Question 74
A 65-year-old female with a long history of hyperparathyroidism presents with progressive bone pain and fragility fractures. Her radiographs show diffuse osteopenia. What is the primary effect of excess parathyroid hormone (PTH) on bone?
View Answer & Explanation
Correct Answer: D
Rationale: Increased PTH consequently leads to increased serum calcium and increased bone resorption, allowing flow of calcium from bone to blood. This is the primary effect of excess PTH on bone. The other options describe effects contrary to hyperparathyroidism or no effect.
Question 74
A 58-year-old female is diagnosed with primary hyperparathyroidism due to a parathyroid adenoma. What is the key characteristic of this adenoma that leads to oversecretion of PTH?
View Answer & Explanation
Correct Answer: C
Rationale: The text states: "The most common cause [of primary hyperparathyroidism] is a benign parathyroid adenoma that loses its sensitivity to circulating calcium levels." This loss of sensitivity leads to autonomous PTH secretion despite high calcium levels. Increased sensitivity, decreased proliferation, calcitonin production, or inhibition of PTH synthesis are all incorrect.
Question 74
A 72-year-old male with long-standing, untreated hyperparathyroidism presents with severe bone pain and multiple lytic lesions on radiographs. A bone biopsy reveals fibrous tissue replacement. What is the term for this specific skeletal manifestation?
View Answer & Explanation
Correct Answer: C
Rationale: The text states that manifestations of hyperparathyroidism involve the skeletal system (bone pain due to fibrous tissue replacement, termed osteitis fibrosa cystica). The patient's symptoms and biopsy findings directly match this description. The other options are distinct bone pathologies not specifically described as fibrous tissue replacement due to hyperparathyroidism.
Question 74
A 60-year-old female is diagnosed with primary hyperparathyroidism. While a benign adenoma is the most common cause, what are other less frequent causes of primary hyperparathyroidism mentioned in the clinical context?
View Answer & Explanation
Correct Answer: C
Rationale: The text states: "The most common cause is a benign parathyroid adenoma... The other causes are hyperplasia and rarely carcinoma." Options A are causes of secondary hyperparathyroidism. Options B, D, and E are unrelated conditions or incorrect causes of primary hyperparathyroidism.
Question 74
A 45-year-old male with hyperparathyroidism develops a lytic lesion in his humerus, diagnosed as a brown tumor. Histological examination of this lesion would predominantly show which type of cell?

View Answer & Explanation
Correct Answer: C
Rationale: Fig. 7.50 states: "Note the relative clustering of the osteoclast-type giant cells in fibrous tissue and reactive bone formation." This directly identifies osteoclast-type giant cells as a characteristic feature of brown tumors. Osteoblasts are involved in bone formation, chondrocytes in cartilage, adipocytes in fat, and plasma cells in immune responses, none of which are the predominant characteristic cell type of a brown tumor.
Question 74
A 55-year-old female presents with hypercalcemia and elevated parathyroid hormone (PTH) levels. Further investigation confirms that the dysfunction originates within the parathyroid glands themselves, leading to oversecretion of PTH. What type of hyperparathyroidism is this?
View Answer & Explanation
Correct Answer: C
Rationale: Primary hyperparathyroidism results from dysfunction in the parathyroid glands themselves, with oversecretion of PTH. Secondary hyperparathyroidism is due to resistance to PTH actions, usually from chronic renal failure or malabsorption. Tertiary hyperparathyroidism is not mentioned in the text. Pseudohyperparathyroidism and ectopic PTH production are not described as the primary classification in the provided context.
Question 75
A 55-year-old female presents with chronic fatigue and generalized bone pain. Laboratory tests reveal elevated serum calcium and parathyroid hormone (PTH) levels. Radiographs of her hands show subtle subperiosteal bone resorption and local osteopenia of the phalanges.

View Answer & Explanation
Correct Answer: D
Rationale: Increased parathyroid hormone (PTH) leads to increased serum calcium, increased bone resorption, reduced renal clearance of calcium, and increased intestinal calcium absorption. Therefore, increased intestinal calcium absorption is a direct consequence of excess PTH. Decreased serum calcium, decreased bone resorption, increased renal clearance of calcium, and decreased PTH production are all contrary to the effects of hyperparathyroidism.
Question 76
A 62-year-old male presents with recurrent kidney stones and a history of chronic generalized bone pain. Laboratory findings indicate elevated serum calcium and parathyroid hormone (PTH). Imaging reveals a solitary adenoma in the neck region. What is the most common cause of this patient's condition?
View Answer & Explanation
Correct Answer: C
Rationale: The most common cause of primary hyperparathyroidism, as described in the vignette with an adenoma and elevated PTH/calcium, is a benign parathyroid adenoma that loses its sensitivity to circulating calcium levels. Parathyroid hyperplasia and carcinoma are less common causes of primary hyperparathyroidism. Chronic renal failure and malabsorption syndrome are causes of secondary hyperparathyroidism, not primary.
Question 77
A 48-year-old female undergoes routine blood work which reveals hypercalcemia and elevated parathyroid hormone (PTH) levels. She reports no specific symptoms. Which of the following is a direct consequence of the excess PTH in her system?
View Answer & Explanation
Correct Answer: E
Rationale: Increased PTH consequently leads to increased serum calcium and increased bone resorption, allowing flow of calcium from bone to blood. While PTH does affect phosphate, the text specifically highlights calcium regulation. Increased bone formation, reduced calcium absorption, and enhanced renal clearance of calcium are all incorrect effects of PTH in hyperparathyroidism.
Question 78
A 70-year-old male presents with severe bone pain and multiple pathological fractures. Imaging studies reveal widespread lytic lesions and areas of fibrous tissue replacement within the bone. Histological examination of a bone biopsy shows osteoclast-type giant cells in fibrous tissue. What is the specific term for the skeletal involvement characterized by fibrous tissue replacement due to hyperparathyroidism?
View Answer & Explanation
Correct Answer: D
Rationale: The skeletal system manifestations of hyperparathyroidism, characterized by bone pain due to fibrous tissue replacement, are termed osteitis fibrosa cystica. Osteoporosis, osteomalacia, Paget's disease, and rickets are distinct bone disorders not specifically described as fibrous tissue replacement due to hyperparathyroidism in the provided text.
Question 79
A 58-year-old female with a known history of primary hyperparathyroidism presents to the emergency department with acute flank pain and hematuria. A CT scan reveals a 4 mm calculus in the left ureter. Which of the following is the most common renal manifestation of hyperparathyroidism?
View Answer & Explanation
Correct Answer: C
Rationale: Manifestations of hyperparathyroidism usually involve the kidney (stones) and the skeletal system. The patient's presentation with flank pain and a ureteral calculus directly points to kidney stones as the most common renal manifestation. While severe hyperparathyroidism can eventually lead to renal failure, kidney stones are the primary and most common renal manifestation mentioned.
Question 80
A 65-year-old male with a history of elevated serum calcium and PTH undergoes a skeletal survey. Radiographs of his hands, specifically the phalanges, show subtle changes. Which of the following radiographic findings is characteristic of primary hyperparathyroidism in the phalanges?

View Answer & Explanation
Correct Answer: C
Rationale: Fig. 7.43 illustrates "Primary hyperparathyroidism with subtle subperiosteal bone resorption and local osteopenia of the phalanges." This is a classic radiographic sign of hyperparathyroidism. The other options are characteristic of other conditions or not specifically mentioned as typical findings for hyperparathyroidism in the phalanges.
Question 81
A 50-year-old female with long-standing hyperparathyroidism undergoes a skull radiograph as part of her workup for bone pain. The radiograph reveals specific changes in the cranial vault. Which of the following describes the characteristic bone resorption pattern seen in the skull in hyperparathyroidism?

View Answer & Explanation
Correct Answer: C
Rationale: Fig. 7.49 shows "Bone resorptions in the skull – dominantly in the external cortical region (arrows)." This is a specific radiographic finding associated with hyperparathyroidism. The other options do not accurately describe the characteristic pattern of bone resorption in the skull as per the provided image and context.
Question 82
A 35-year-old male presents with a painful swelling in his tibia. Biopsy of the lesion is performed, and the photomicrograph reveals a characteristic histological feature associated with hyperparathyroidism. What is the key histological feature of a brown tumor?

View Answer & Explanation
Correct Answer: C
Rationale: Fig. 7.50 states: "This photomicrograph illustrates the characteristic histological feature of a brown tumor in hyperparathyroidism. Note the relative clustering of the osteoclast-type giant cells in fibrous tissue and reactive bone formation." This directly matches option C. The other options describe features not characteristic of a brown tumor in hyperparathyroidism.
Question 83
A 52-year-old female with a history of chronic renal failure develops elevated parathyroid hormone (PTH) levels and hypercalcemia. Her condition is diagnosed as secondary hyperparathyroidism. What is the underlying mechanism for secondary hyperparathyroidism in this patient?
View Answer & Explanation
Correct Answer: C
Rationale: Secondary hyperparathyroidism is due to resistance to the actions of PTH, usually because of chronic renal failure or malabsorption. Options A, B, and D are causes of primary hyperparathyroidism. Option E describes primary hyperparathyroidism, not secondary.
Question 84
A 68-year-old male is diagnosed with primary hyperparathyroidism. His laboratory results show elevated serum calcium and PTH. Regarding renal function, how does increased PTH affect calcium handling in the kidneys?
View Answer & Explanation
Correct Answer: C
Rationale: Increased PTH consequently leads to increased serum calcium, increased bone resorption, and reduces renal clearance of calcium. This means less calcium is excreted in the urine, contributing to hypercalcemia. Options A, B, and E are incorrect as they describe increased calcium excretion or decreased reabsorption. Option D is incorrect as PTH has a significant effect.
Question 85
A 45-year-old female undergoes a routine health check-up. Blood tests reveal mildly elevated serum calcium and parathyroid hormone (PTH) levels. She denies any symptoms such as bone pain, kidney stones, or fatigue. What is a common characteristic of patients with hyperparathyroidism regarding their symptomatic status?
View Answer & Explanation
Correct Answer: C
Rationale: The text explicitly states: "The majority of patients with hyperparathyroidism are asymptomatic." This makes option C the correct answer. Options A, B, D, and E are incorrect as they describe universal or specific severe symptoms, which contradicts the asymptomatic nature in most cases.
Question 86
A 60-year-old male with a long history of end-stage renal disease on dialysis develops persistently elevated parathyroid hormone (PTH) levels and progressive bone disease. His condition is diagnosed as secondary hyperparathyroidism. Which of the following is the most common underlying cause of secondary hyperparathyroidism?
View Answer & Explanation
Correct Answer: C
Rationale: Secondary hyperparathyroidism is due to resistance to the actions of PTH, usually because of chronic renal failure or malabsorption. Given the patient's history of end-stage renal disease, chronic renal failure is the most common underlying cause. Parathyroid adenoma and carcinoma are causes of primary hyperparathyroidism. Vitamin D toxicity and hyperthyroidism are not listed as causes of secondary hyperparathyroidism in the provided text.
Question 87
A 40-year-old female with primary hyperparathyroidism develops a lytic lesion in her femur. A biopsy confirms the diagnosis of a "brown tumor." What is the nature of these bony involvements in hyperparathyroidism?
View Answer & Explanation
Correct Answer: C
Rationale: The text states: "The bony involvements are also named as brown tumors." And further, Fig. 7.50 describes the histology as "relative clustering of the osteoclast-type giant cells in fibrous tissue and reactive bone formation." This confirms that brown tumors are areas of fibrous tissue replacement and reactive bone formation, not true neoplasms, infections, or metastases.
Question 88
A 50-year-old male presents with generalized weakness and polyuria. Initial laboratory tests show elevated parathyroid hormone (PTH) levels. What is the expected serum calcium level in a patient with hyperparathyroidism?
View Answer & Explanation
Correct Answer: C
Rationale: Hyperparathyroidism is overactivity of the parathyroid glands resulting in excess production of parathyroid hormone (PTH). Increased PTH consequently leads to increased serum calcium. Therefore, an increased serum calcium level is expected.
Question 89
A 65-year-old female with a long history of hyperparathyroidism presents with progressive bone pain and fragility fractures. Her radiographs show diffuse osteopenia. What is the primary effect of excess parathyroid hormone (PTH) on bone?
View Answer & Explanation
Correct Answer: D
Rationale: Increased PTH consequently leads to increased serum calcium and increased bone resorption, allowing flow of calcium from bone to blood. This is the primary effect of excess PTH on bone. The other options describe effects contrary to hyperparathyroidism or no effect.
Question 90
A 58-year-old female is diagnosed with primary hyperparathyroidism due to a parathyroid adenoma. What is the key characteristic of this adenoma that leads to oversecretion of PTH?
View Answer & Explanation
Correct Answer: C
Rationale: The text states: "The most common cause [of primary hyperparathyroidism] is a benign parathyroid adenoma that loses its sensitivity to circulating calcium levels." This loss of sensitivity leads to autonomous PTH secretion despite high calcium levels. Increased sensitivity, decreased proliferation, calcitonin production, or inhibition of PTH synthesis are all incorrect.
Question 91
A 72-year-old male with long-standing, untreated hyperparathyroidism presents with severe bone pain and multiple lytic lesions on radiographs. A bone biopsy reveals fibrous tissue replacement. What is the term for this specific skeletal manifestation?
View Answer & Explanation
Correct Answer: C
Rationale: The text states that manifestations of hyperparathyroidism involve the skeletal system (bone pain due to fibrous tissue replacement, termed osteitis fibrosa cystica). The patient's symptoms and biopsy findings directly match this description. The other options are distinct bone pathologies not specifically described as fibrous tissue replacement due to hyperparathyroidism.
Question 92
A 60-year-old female is diagnosed with primary hyperparathyroidism. While a benign adenoma is the most common cause, what are other less frequent causes of primary hyperparathyroidism mentioned in the clinical context?
View Answer & Explanation
Correct Answer: C
Rationale: The text states: "The most common cause is a benign parathyroid adenoma... The other causes are hyperplasia and rarely carcinoma." Options A are causes of secondary hyperparathyroidism. Options B, D, and E are unrelated conditions or incorrect causes of primary hyperparathyroidism.
Question 93
A 45-year-old male with hyperparathyroidism develops a lytic lesion in his humerus, diagnosed as a brown tumor. Histological examination of this lesion would predominantly show which type of cell?

View Answer & Explanation
Correct Answer: C
Rationale: Fig. 7.50 states: "Note the relative clustering of the osteoclast-type giant cells in fibrous tissue and reactive bone formation." This directly identifies osteoclast-type giant cells as a characteristic feature of brown tumors. Osteoblasts are involved in bone formation, chondrocytes in cartilage, adipocytes in fat, and plasma cells in immune responses, none of which are the predominant characteristic cell type of a brown tumor.
Question 94
A 1-month-old male infant presents with high fever, irritability, and refusal to move his left leg. On examination, the left hip is held in a flexed, abducted, and externally rotated position, with significant pain on passive movement. Laboratory tests show elevated white blood cell count and Westergreen sedimentation rate. Which of the following organisms is the most common bacterial cause of this condition?
View Answer & Explanation
Correct Answer: B
Rationale: The clinical vignette describes septic coxitis (Säuglings-coxitis) in a newborn. The provided text explicitly states that *S. aureus* and *Haemophilus influenzae* are the most common bacteria causing coxitis in newborns. Among the given options, *Staphylococcus aureus* is listed as a primary pathogen. While other bacteria can cause infections, *S. pneumoniae* is less common in this specific context for hip coxitis.
Question 95
A 2-month-old female infant is brought to the emergency department by her parents due to persistent crying, fever, and decreased movement of her right leg. Physical examination reveals a painful right hip held in a characteristic position. Which of the following describes the typical resting position of the affected hip in a newborn with coxitis?
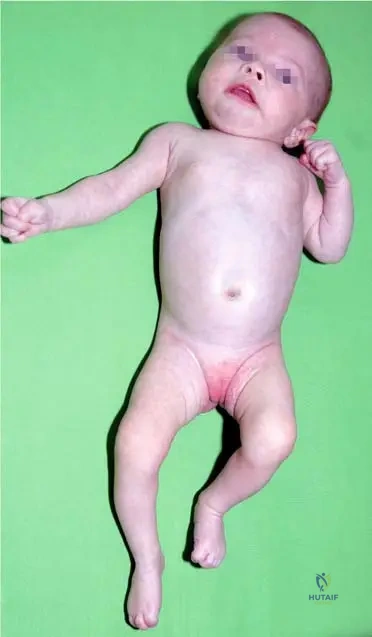
View Answer & Explanation
Correct Answer: D
Rationale: The clinical text and Fig. 2.7 explicitly state that the characteristic position of the newborn's hip in coxitis is flexion–abduction–external rotation. This position minimizes intra-articular pressure and pain. Adduction, extension, and internal rotation (A) would typically increase pain and pressure in a septic hip.
Question 96
A 3-week-old male infant presents with signs of sepsis and a painful, swollen left hip. Imaging reveals septic arthritis of the hip. The pathophysiology of osteomyelitis in newborns and infants under 1 year often involves the spread of infection to the epiphyses and joints. Which anatomical feature contributes to this pattern of involvement in the hip?
View Answer & Explanation
Correct Answer: B
Rationale: The provided text states, "The metaphyseal vessels of the femur contain bacteria, which may penetrate into the epiphysis and the hip joint, thus the metaphysis is localized intra-articular." This unique anatomical relationship in newborns allows for direct spread of infection from the metaphysis into the joint space. The epiphyseal growth plate is indeed vascularized, but the key factor for joint involvement is the intra-articular metaphysis (C is a distractor as it's not the primary reason for *joint* involvement from osteomyelitis).
Question 97
A 1-month-old infant presents with a high fever, irritability, and a swollen, painful right hip. Physical examination shows limited range of motion and an antalgic posture. Initial laboratory tests are consistent with a septic process. Given the age and clinical presentation, which imaging modality is most sensitive for detecting early signs of hip joint effusion and potential dislocation?
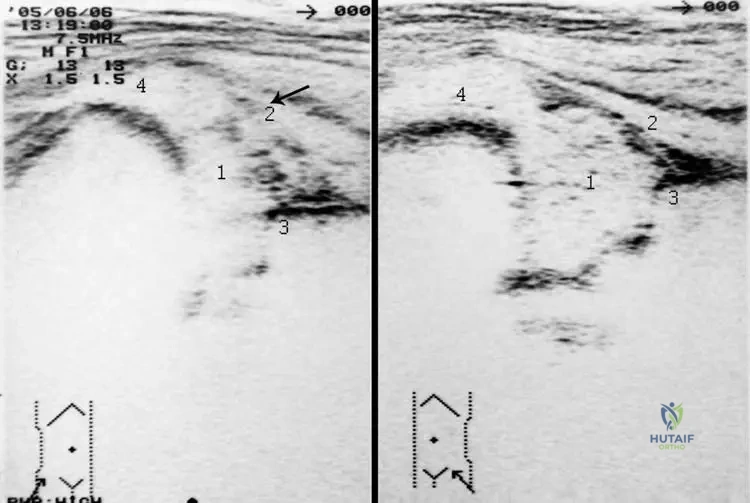
View Answer & Explanation
Correct Answer: D
Rationale: Fig. 2.8 a, b demonstrates bilateral ultrasound images of the hips in a baby with septic coxitis, showing a dilated capsule, fluid formation, and femoral head dislocation. Ultrasound is highly sensitive for detecting joint effusions, capsular distention, and early signs of dislocation in the cartilaginous hips of newborns and infants, making it the initial imaging modality of choice. Plain radiographs (A) are often normal in early septic arthritis and are less sensitive for soft tissue and fluid. MRI (B) and CT (C) are more detailed but typically reserved for complex cases or when ultrasound is inconclusive, and bone scintigraphy (E) is less specific for joint fluid.
Question 98
A 6-week-old infant is diagnosed with septic coxitis of the left hip. An ultrasound is performed to assess the joint. Which of the following findings would be characteristic of septic coxitis on ultrasound?

View Answer & Explanation
Correct Answer: C
Rationale: Fig. 2.8a explicitly describes the ultrasound findings in septic coxitis: "in the left hip joint the capsule is dilated (arrow); below a less echo dense area (tip of arrow), which indicates a thick fluid formation, femoral head is dislocated (1), the cartilaginous acetabulum is lifted (2), the osseous acetabulum is intact (3), the greater trochanter is in high position (4)." Therefore, a dilated capsule with thick fluid and potential femoral head dislocation are characteristic findings. Sclerotic changes (D) are typically seen on later radiographs, and an intact capsule with minimal fluid (B) or normal trochanter position (E) would indicate a normal or less severe condition.
Question 99
A 1-month-old infant presents with high fever, poor feeding, and a painful, limited range of motion in the left hip. Blood tests are ordered to evaluate for a septic process. Which combination of laboratory findings is most characteristic of newborn's coxitis?
View Answer & Explanation
Correct Answer: B
Rationale: The clinical text states: "Newborn’s coxitis is at highly septic condition, and the lab tests show high Westergreen and white blood cell levels and a left shift in the qualitative blood test." Westergreen refers to the erythrocyte sedimentation rate (ESR). These findings are indicative of an acute bacterial infection and systemic inflammation.
Question 100
A 2-week-old infant is diagnosed with septic coxitis. The parents deny any recent trauma or obvious skin infections. Upon further questioning and examination, the physician identifies a potential primary source of infection. Which of the following is a common primary site for hematogenous bacterial transmission leading to newborn's coxitis?
View Answer & Explanation
Correct Answer: C
Rationale: The provided text explicitly states: "The bacteria are transmitted hematogenously, and the primary infection is mostly in a discharging (“wet”) umbilicus, bacterial skin inflammation or otitis." Among the options, a discharging umbilicus is a direct match. While other conditions might occur in infants, they are not listed as common primary sources for hematogenous spread to the hip in this context.
You Might Also Like
