Orthopaedic Board Review: Synovial Chondromatosis, Charcot Joint, Fibrous Dysplasia, Bone Metastases | Part 21
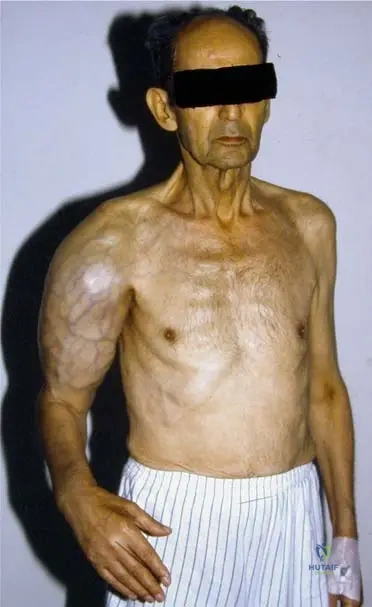
Key Takeaway
This ABOS Board Review covers key orthopaedic pathologies: synovial chondromatosis, neurogenic osteoarthropathy (Charcot joint), fibrous dysplasia, and metastatic bone disease. It details their clinical presentations, diagnostic features, and management principles, providing essential knowledge for orthopaedic surgeons preparing for their board examinations.
Orthopaedic Board Review: Synovial Chondromatosis, Charcot Joint, Fibrous Dysplasia, Bone Metastases | Part 21
Comprehensive 100-Question Exam
00:00
Start Quiz
Question 1
A 12-year-old girl presents with a chronic limp and mild thigh pain. Radiographs reveal a ground-glass expansile lesion in the proximal femur with a characteristic shepherd's crook deformity. What is the underlying molecular pathogenesis of this condition?
Explanation
Question 2
A 60-year-old man with metastatic lung cancer complains of severe, unrelenting pain in his right thigh. Radiographs reveal a 4 cm lytic lesion in the femoral diaphysis that involves approximately 50% of the cortical diameter. According to Mirels' criteria, what is his score and the corresponding recommendation?
Explanation
Question 3
A 45-year-old man undergoes an arthroscopic procedure for chronic knee locking. The surgeon removes dozens of uniformly sized, loose cartilaginous bodies. Which of the following histologic findings is classically associated with the primary form of this disease and must not be misdiagnosed as malignancy?
Explanation
Question 4
A 50-year-old man presents with rapid, painless swelling and severe radiographic destruction of the right shoulder joint over the past 3 months. Neurological exam reveals a loss of pain and temperature sensation in a cape-like distribution over the upper extremities. What is the most appropriate next step in diagnosis?
Explanation
Question 5
A 15-year-old boy with polyostotic fibrous dysplasia presents with a progressing proximal femur deformity.
Surgical management is planned to restore mechanical alignment. Which of the following is the most appropriate biomechanical approach for reconstruction?
Explanation
Question 6
A 65-year-old man is scheduled for prophylactic intramedullary nailing of a solitary, painful lytic lesion in the right humerus.
Biopsy confirmed metastatic renal cell carcinoma. To prevent a catastrophic intraoperative complication, what critical intervention should be performed 24 to 48 hours prior to surgery?
Explanation
Question 7
A 60-year-old woman with a 15-year history of primary synovial chondromatosis of the hip presents with acute worsening of pain and a rapidly enlarging soft tissue mass. Imaging reveals new cortical destruction and marrow invasion. What is the most likely diagnosis?
Explanation
Question 8
The pathogenesis of Charcot arthropathy is debated between the neurotraumatic and neurovascular theories. Which of the following best describes the fundamental mechanism proposed by the neurovascular theory?
Explanation
Question 9
A 35-year-old woman with polyostotic fibrous dysplasia
complains of a painless, deep-seated soft tissue mass in her right thigh. If this mass is associated with her skeletal condition, a biopsy would most likely reveal which of the following?
Explanation
Question 10
A patient is evaluated for surgical stabilization of an impending pathologic femur fracture due to metastatic disease. Among the following options, which primary tumor generally carries the most favorable long-term survival prognosis after bony metastasis?
Explanation
Question 11
A diabetic patient presents with a warm, erythematous, and swollen midfoot. Radiographs demonstrate periarticular fragmentation, bony debris, and subluxation at the tarsometatarsal joints, but no signs of coalescence. According to the Eichenholtz classification, what is the stage and best initial management?
Explanation
Question 12
When surgically managing an impending pathologic fracture of the femoral shaft due to metastatic breast cancer
, which biomechanical principle must guide the choice of implant?
Explanation
Question 13
Which of the following is the primary pathophysiologic mechanism underlying primary synovial chondromatosis?
Explanation
Question 14
A 45-year-old male with a long-standing history of recurrent synovial chondromatosis of the knee presents with sudden, rapidly increasing pain and swelling. MRI reveals a large soft tissue mass eroding into the distal femur. What is the most likely diagnosis?
Explanation
Question 15
According to the Eichenholtz classification of Charcot arthropathy, which of the following radiographic findings is hallmark for the Coalescence stage (Stage 2)?
Explanation
Question 16
The neurovascular theory of Charcot arthropathy suggests that autonomic neuropathy leads to which of the following physiological changes?
Explanation
Question 17
Fibrous dysplasia is caused by a somatic activating mutation in which of the following genes?
Explanation
Question 18
When evaluating a patient with metastatic bone disease of the femur, which of the following factors would contribute the highest point value in Mirels' scoring system for prophylactic fixation?
Explanation
Question 19
Which histological feature helps differentiate primary synovial chondromatosis from secondary synovial chondromatosis?
Explanation
Question 20
A diabetic patient presents with a hot, swollen, erythematous foot without an open ulceration. X-rays show acute periarticular fragmentation at the midfoot. What is the most appropriate initial management?
Explanation
Question 21
A 9-year-old girl presents with a limp and a shepherd's crook deformity of the proximal femur. She also has large, irregularly bordered hyperpigmented skin macules. What endocrine abnormality is most commonly associated with this syndrome?
Explanation
Question 22
A 65-year-old male presents with a purely blastic metastatic lesion in his lumbar spine. Which primary malignancy is the most likely source?
Explanation
Question 23
Which joint is most frequently affected by primary synovial chondromatosis, and what is the typical patient demographic?
Explanation
Question 24
Which imaging modality or technique is most specific for differentiating an acute Charcot neuroarthropathy from pedal osteomyelitis in a diabetic foot with an overlying ulcer?
Explanation
Question 25
A routine radiograph of a 25-year-old patient reveals an expansile, intramedullary lesion in the proximal femur with a hazy, 'ground-glass' appearance and endosteal scalloping. What is the recommended surgical management if the lesion is completely asymptomatic and structurally stable?
Explanation
Question 26
A patient with a known history of renal cell carcinoma requires intramedullary nailing for an impending pathologic fracture of the femur. Which preoperative intervention is strongly recommended?
Explanation
Question 27
What is the surgical treatment of choice for symptomatic primary synovial chondromatosis of the knee to minimize the risk of recurrence?
Explanation
Question 28
In a patient with established Charcot arthropathy of the foot and ankle, which of the following is the most widely accepted indication for surgical reconstruction or arthrodesis?
Explanation
Question 29
Which pharmacological agent has shown efficacy in reducing bone pain and potentially decreasing the rate of abnormal bone turnover in patients with polyostotic fibrous dysplasia?
Explanation
Question 30
Which of the following factors is considered in the Spinal Instability Neoplastic Score (SINS) to determine the need for surgical stabilization in spinal metastases?
Explanation
Question 31
A 12-year-old girl presents with a persistent limp. Radiographs demonstrate an expansile proximal femur lesion with a "ground-glass" appearance.
What is the underlying molecular pathogenesis of this condition?
Explanation
Question 32
A 40-year-old male presents with mechanical knee pain, clicking, and intermittent locking. MRI shows multiple intra-articular loose bodies of uniform size with a "ring and arc" enhancement pattern. What is the primary histological process driving this condition?
Explanation
Question 33
A 62-year-old female with known breast cancer presents with moderate thigh pain. Radiographs reveal a lytic lesion in the femoral diaphysis involving 75% of the cortical diameter.
According to Mirels' criteria, what is her score and the most appropriate recommendation?
Explanation
Question 34
A 55-year-old diabetic male presents with a swollen, erythematous, and warm foot without skin ulceration. Radiographs show extensive bone fragmentation, periarticular debris, and joint subluxation. Which stage of the Eichenholtz classification does this represent, and what is the primary initial treatment?
Explanation
Question 35
A 35-year-old female with known polyostotic fibrous dysplasia presents with a painless, deep-seated soft tissue mass in her right thigh.
Excisional biopsy of the mass reveals an intramuscular myxoma. Which syndrome is this patient exhibiting?
Explanation
Question 36
A 68-year-old male with a history of renal cell carcinoma presents with a solitary lytic metastasis in the proximal humerus and an impending fracture.
What is an essential step prior to surgical stabilization of this lesion?
Explanation
Question 37
The pathogenesis of Charcot arthropathy involves multiple factors. The 'French theory' of Charcot pathogenesis specifically emphasizes which of the following mechanisms?
Explanation
Question 38
A 50-year-old male with a long-standing history of primary synovial chondromatosis of the hip presents with acute worsening of pain and rapid joint swelling. MRI demonstrates a new, aggressive soft tissue mass with marrow invasion. What is the most likely diagnosis?
Explanation
Question 39
A 72-year-old male presents with severe back pain. Radiographs show multiple dense, blastic lesions in the lumbar spine and pelvis.
Which of the following combinations of tumor marker and primary cellular mechanism is characteristic of this malignancy?
Explanation
Question 40
A 22-year-old male with polyostotic fibrous dysplasia presents with a severe Shepherd's crook deformity of the proximal femur.
When planning corrective osteotomy and fixation, which biomechanical principle is most critical to prevent mechanical failure?
Explanation
Question 41
Which of the following best describes the underlying molecular pathophysiology of fibrous dysplasia?
Explanation
Question 42
A 45-year-old male with a long-standing history of primary synovial chondromatosis of the hip presents with acutely worsening pain and rapid swelling. Radiographs show new cortical erosion and marrow involvement. Which of the following is the most likely diagnosis?
Explanation
Question 43
A diabetic patient presents with a red, hot, swollen foot. Radiographs show joint debris, fragmentation of subchondral bone, and subluxation, but no signs of consolidation. According to the Eichenholtz classification, what is the most appropriate initial management?
Explanation
Question 44
When evaluating a patient with a metastatic lesion to the long bone, the Mirels' scoring system is used to predict the risk of pathologic fracture. Which of the following combinations yields the highest score (3 points) for each respective category?
Explanation
Question 45
A 9-year-old girl presents with a limp and a history of early-onset puberty. Radiographs reveal multiple expansile ground-glass lesions in the femur and tibia. Physical exam notes large, irregular hyperpigmented skin macules. What is the classic term for these skin lesions?
Explanation
Question 46
Primary synovial chondromatosis is fundamentally a disease driven by which of the following pathophysiological processes?
Explanation
Question 47
A 62-year-old male presents with a purely lytic impending pathologic fracture of the proximal femur secondary to metastatic renal cell carcinoma. Before proceeding with prophylactic intramedullary nailing, what critical step should be taken to minimize perioperative complications?
Explanation
Question 48
The "neurovascular theory" of Charcot neuropathic arthropathy pathogenesis primarily implicates which of the following mechanisms?
Explanation
Question 49
A 25-year-old patient with polyostotic fibrous dysplasia presents with increasing hip pain and a progressive varus deformity of the proximal femur. What is the most appropriate surgical management for this characteristic "shepherd's crook" deformity?
Explanation
Question 50
A 55-year-old female with a history of breast cancer presents with severe thoracic back pain. Imaging demonstrates a blastic and lytic lesion at T8 with posterior element involvement but no spinal cord compression. In addition to localized radiation, what pharmacological agent is indicated to reduce skeletal-related events?
Explanation
Question 51
Differentiating primary from secondary synovial chondromatosis on imaging can sometimes be challenging. Which of the following features is most characteristic of PRIMARY synovial chondromatosis?
Explanation
Question 52
A 42-year-old male presents with chronic knee pain and mechanical catching. Radiographs demonstrate multiple radiopaque bodies within the joint space. MRI reveals a large effusion with numerous uniform-sized, intra-articular nodules. Which of the following best describes the pathophysiology of this condition?
Explanation
Question 53
A 45-year-old man with a known history of primary synovial chondromatosis of the hip presents with sudden, rapidly progressive pain and a new palpable mass. Plain radiographs demonstrate cortical destruction and extension into the surrounding soft tissues. Which of the following is the most reliable histologic indicator of malignant transformation in this condition?
Explanation
Question 54
Primary synovial chondromatosis is a benign neoplastic process rather than a purely reactive metaplasia. Which of the following cytogenetic abnormalities is most frequently associated with the primary form of this disease?
Explanation
Question 55
A 35-year-old woman presents with a 2-year history of episodic knee pain and mechanical catching. MRI reveals a large joint effusion with multiple intra-articular nodules that are isointense to muscle on T1-weighted images and hyperintense on T2-weighted images, but show no mineralization on plain radiographs. What is the most appropriate management for the primary underlying pathology?
Explanation
Question 56
A 55-year-old man with poorly controlled type 2 diabetes presents with a red, hot, swollen right foot. He denies fevers or chills. Plain radiographs show early fragmentation of the tarsometatarsal joints without frank dislocation. Elevating the leg for 10 minutes leads to a significant decrease in erythema. What is the most appropriate next step in management?
Explanation
Question 57
Differentiating between acute Charcot arthropathy and osteomyelitis in a diabetic foot can be challenging. Which of the following imaging modalities or combinations provides the highest specificity for diagnosing superimposed osteomyelitis in a patient with an active midfoot Charcot joint?
Explanation
Question 58
The pathogenesis of Charcot neuroarthropathy is multifactorial, involving both neurotraumatic and neurovascular pathways. Which of the following best describes the neurovascular theory (French theory) of this disease?
Explanation
Question 59
A 14-year-old boy presents with progressive bowing and pain in his right femur. Radiographs display an expansile ground-glass lesion in the diaphysis. Biopsy confirms fibrous dysplasia. What is the precise genetic etiology of this condition?
Explanation
Question 60
A 65-year-old man with a history of radical nephrectomy presents with severe right thigh pain. Radiographs reveal a large, impending pathologic fracture of the proximal femur due to a lytic lesion. What is the most critical intervention to perform prior to intramedullary nailing?
Explanation
Question 61
A 55-year-old diabetic male presents with an acutely swollen, erythematous, and warm right foot. He is afebrile and his pedal pulses are bounding. Radiographs show soft tissue swelling and early bony fragmentation of the midfoot without ulceration. What is the best initial management?
Explanation
Question 62
Which radiographic feature is most characteristic for differentiating primary synovial chondromatosis from secondary synovial chondromatosis?
Explanation
Question 63
A 25-year-old woman with known fibrous dysplasia presents with increasing thigh pain and a progressive shepherd's crook deformity. What is the most appropriate surgical management to address her symptoms and deformity?
Explanation
Question 64
A 50-year-old woman with metastatic breast cancer presents with a newly discovered lytic lesion in the peritrochanteric region of her femur. The lesion involves 50% of the cortical diameter. She reports severe pain with weight-bearing. What is her Mirels' score?
Explanation
Question 65
A 42-year-old man presents with painless, massive swelling and crepitus of his right shoulder. Radiographs demonstrate severe destruction of the humeral head and glenoid with multiple bony fragments. Which underlying condition is most likely responsible?
Explanation
Question 66
A 50-year-old man with long-standing primary synovial chondromatosis of the hip presents with rapid worsening of pain and swelling. MRI reveals a new, large soft tissue mass invading the adjacent marrow cavity with cortical destruction. What is the most likely diagnosis?
Explanation
Question 67
A 35-year-old female is diagnosed with polyostotic fibrous dysplasia. During her workup, an MRI of her thigh unexpectedly reveals multiple well-circumscribed, T2-hyperintense soft tissue masses within her skeletal muscle. What is the correct diagnosis for this presentation?
Explanation
Question 68
A 72-year-old man with metastatic prostate cancer has multiple dense, osteoblastic lesions in his lumbar spine and pelvis. Which of the following factors, secreted by the tumor cells, is primarily responsible for the osteoblastic nature of these metastases?
Explanation
Question 69
According to the neurovascular theory of Charcot arthropathy, which mechanism directly contributes to bone resorption and subsequent joint destruction?
Explanation
Question 70
Which classic histologic feature clearly distinguishes fibrous dysplasia from normal bone and other reactive fibro-osseous lesions?
Explanation
Question 71
A 60-year-old woman presents with a destructive humeral diaphyseal lesion. Biopsy confirms metastatic follicular thyroid carcinoma. What defines the most appropriate operative strategy for this patient?
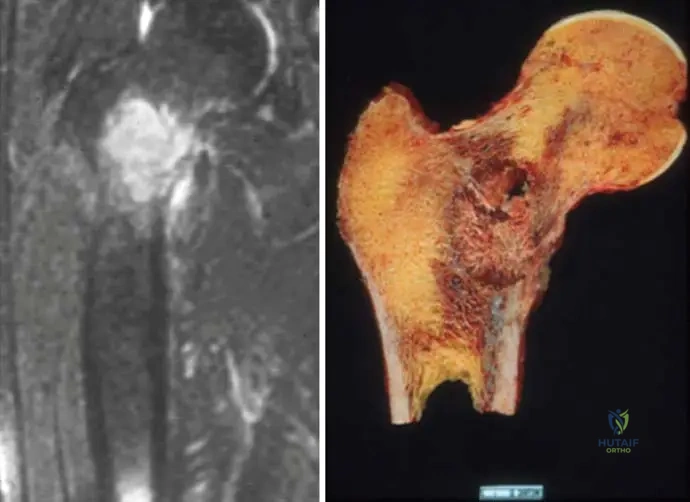
Explanation
Question 72
Primary synovial chondromatosis is considered a benign neoplastic process. Which of the following genetic fusions or chromosomal abnormalities is frequently implicated in its pathogenesis?
Explanation
Question 73
A 24-year-old with polyostotic fibrous dysplasia presents with a progressively painful Shepherd's crook deformity of the proximal femur.
If surgical intervention is elected to correct the deformity and prevent fracture, which of the following is the most appropriate biomechanical and biological strategy?
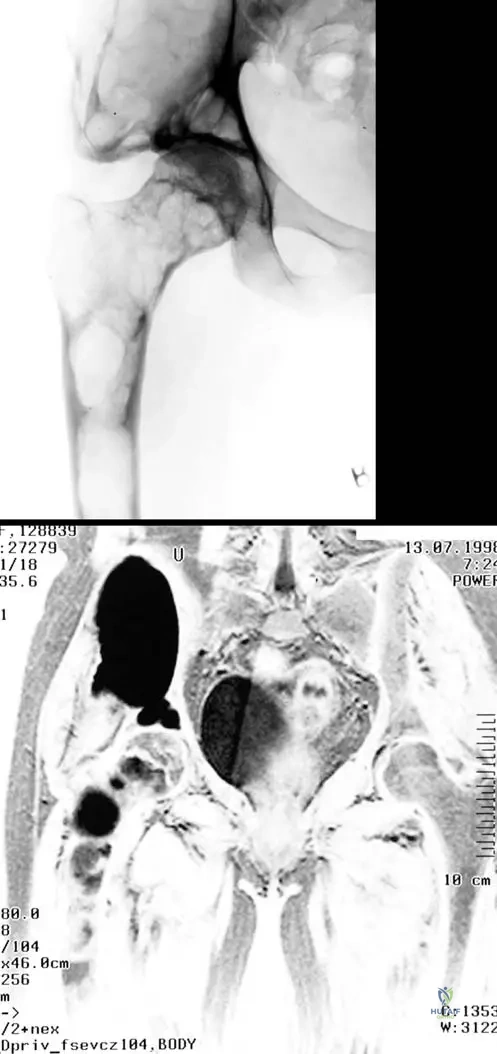
Explanation
Question 74
A 45-year-old male with a long-standing history of primary synovial chondromatosis of the hip presents with acute worsening of pain and a rapidly enlarging mass. Which of the following is the most reliable histologic or clinical indicator of malignant transformation to secondary chondrosarcoma in this specific setting?
Explanation
Question 75
A 55-year-old diabetic patient presents with a warm, swollen, erythematous foot. Radiographs show periarticular debris, fragmentation, and joint subluxation. According to the Eichenholtz classification, what is the current stage of this neuropathic arthropathy and the corresponding initial management?
Explanation
Question 76
A 62-year-old man presents with a pathologic fracture of the proximal humerus secondary to a metastatic renal cell carcinoma lesion.
Prior to surgical stabilization, which of the following interventions is most strongly recommended to minimize intraoperative morbidity?

Explanation
Question 77
A 9-year-old girl is evaluated for precocious puberty and café-au-lait spots with irregular "coast of Maine" borders. Radiographs of her lower extremities demonstrate multiple lucent, ground-glass bone lesions.
Which of the following best describes the underlying genetic anomaly in this patient?
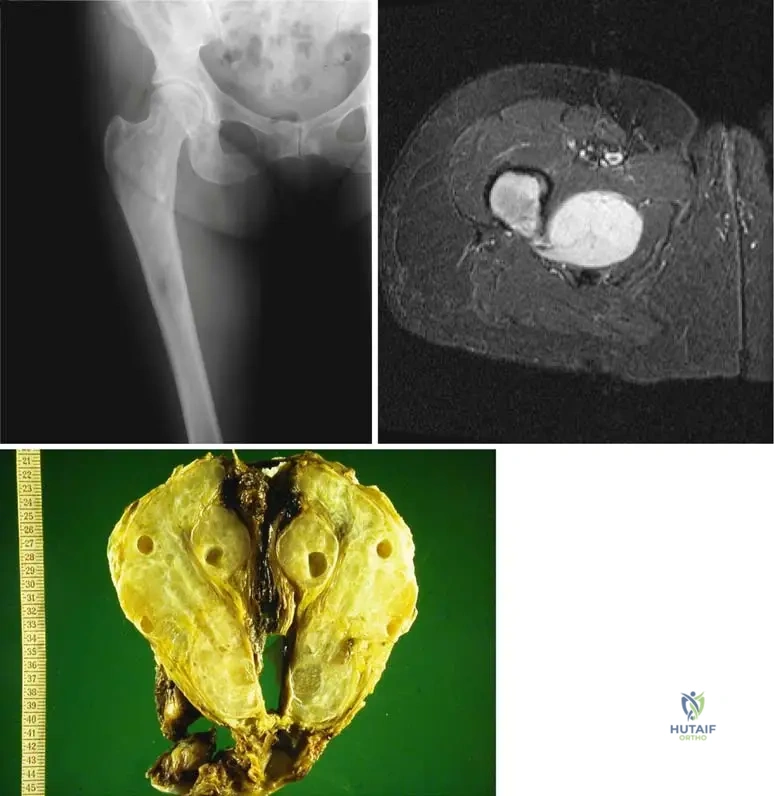
Explanation
Question 78
Differentiating between acute Charcot neuroarthropathy and osteomyelitis in a diabetic foot can be challenging. Which of the following MRI findings is most specific for diagnosing osteomyelitis over acute Charcot arthropathy?
Explanation
Question 79
A 72-year-old man presents with severe back pain. Radiographs reveal multiple osteoblastic lesions in the lumbar spine and pelvis. Laboratory studies show elevated alkaline phosphatase. Which of the following pathophysiologic mechanisms best explains the osteoblastic nature of these specific metastatic bone lesions?
Explanation
Question 80
A 38-year-old woman undergoes arthroscopic removal of dozens of uniformly sized cartilaginous loose bodies from her knee for primary synovial chondromatosis. To minimize the risk of disease recurrence, which of the following additional intraoperative steps is strictly indicated?
Explanation
Question 81
A 35-year-old woman with known polyostotic fibrous dysplasia presents with a painless, deep-seated soft tissue mass in her right thigh. Biopsy of the mass reveals an intramuscular myxoma. This patient is at an increased risk of developing which of the following?
Explanation
Question 82
A 65-year-old man presents with a pathologic fracture of the proximal humerus. Workup reveals a solitary large, destructive lytic lesion. Biopsy confirms metastatic clear cell renal cell carcinoma. What is the most critical step prior to operative stabilization?
Explanation
Question 83
A 55-year-old man with long-standing, poorly controlled diabetes presents with a swollen, erythematous, and warm left foot. He denies pain or recent trauma. Radiographs show osseous fragmentation, joint subluxation, and debris around the midfoot. What is the most appropriate initial management?
Explanation
Question 84
A 40-year-old man with a 10-year history of recurrent primary synovial chondromatosis of the hip presents with a sudden, rapid increase in pain and joint swelling. Imaging shows a large new soft tissue mass with 'ring and arc' calcifications invading the surrounding acetabulum. What is the most likely diagnosis?
Explanation
Question 85
A 55-year-old woman with metastatic breast cancer presents with mild hip pain. Radiographs reveal a lytic lesion involving 75% of the cortex in the peritrochanteric region of the right femur. According to Mirels' criteria, what is her score and recommended treatment?
Explanation
Question 86
A biopsy of a ground-glass rib lesion in a 14-year-old boy reveals fibrous stroma with irregular, woven bone trabeculae lacking osteoblastic rimming. The pathogenesis of this disease is linked to a somatic mutation leading to the substitution of arginine by histidine or cysteine. Which signaling pathway is directly upregulated by this mutation?
Explanation
Question 87
Which of the following best describes the 'neurovascular theory' in the pathogenesis of Charcot neuropathic arthropathy?
Explanation
Question 88
A 62-year-old woman undergoes intramedullary nailing for a pathologic fracture of the femur secondary to metastatic follicular thyroid carcinoma. Following surgical stabilization and appropriate wound healing, what is the preferred adjuvant treatment to specifically address the remaining microscopic disease at the bone metastasis site?
Explanation
None
