ABOS Orthopedic Board Review: Bone Tumors, Alcohol-Related Musculoskeletal Issues & PJI | Part 24
Key Takeaway
This ABOS Board Review section offers multiple-choice questions on diverse orthopedic pathologies. Topics include Gorham's disease, avascular necrosis, septic arthritis, gout, nonossifying fibroma, and periprosthetic joint infection. It also covers alcohol-related musculoskeletal issues like osteoporosis and Charcot arthropathy, providing essential insights for exam preparation.
Question 1
A 28-year-old male is diagnosed with Gorham's disease affecting his pelvis. Initial radiographs show patchy lytic lesions. He is followed over several years. What radiographic change is expected to occur over time in the involved bone?
View Answer & Explanation
Correct Answer: C
Rationale: The disease is described as involving "massive, progressive osteolytic changes" and radiographs show "extensive osteolytic changes of the involved bone." Fig. 8.62 further illustrates "complete resorption of diaphysis," indicating the progressive and extensive nature of the osteolysis. Main Distractor: Option D is incorrect. While the text mentions "Over time, sclerotic bone may accompany healing," this refers to a later, potential healing phase, not the primary progressive change which is osteolysis. The initial and predominant radiographic feature is progressive bone destruction.
Question 2
A bone biopsy is performed on a 19-year-old patient suspected of having Gorham's disease in the distal femur. Upon gross examination of the specimen, what characteristic finding would the pathologist most likely report?
View Answer & Explanation
Correct Answer: C
Rationale: The case text explicitly states under "Pathology": "Gross specimens have a sponge-like consistency." Main Distractor: Option B, a soft, gelatinous texture, might seem plausible for a vascular lesion, but the specific and unique descriptor provided in the text for Gorham's disease is "sponge-like consistency," which is more precise.
Question 3
A 50-year-old male presents with chronic hip pain. Radiographs show significant lytic destruction in the proximal femur with concentric narrowing of the femoral neck. A biopsy is performed. Microscopic examination of the bone tissue would most likely reveal which of the following?

View Answer & Explanation
Correct Answer: C
Rationale: The text states, "Microscopic examination shows varying amounts of vascular changes... Note the cavernous angiomatous spaces." Fig. 8.63 further illustrates this. This is a hallmark microscopic feature of Gorham's disease. Main Distractor: Option A, abundant reactive bone formation, is incorrect because the text specifically states, "Microscopic examination shows varying amounts of vascular changes without reactive bone formation."
Question 4
A 30-year-old patient undergoes a bone biopsy for a progressive lytic lesion in the tibia. The pathologist notes vascular proliferation. To confirm a diagnosis of Gorham's disease and differentiate it from other vascular lesions, which microscopic feature is critical to observe or, more importantly, *not* observe?
View Answer & Explanation
Correct Answer: B
Rationale: The text and Fig. 8.63 specifically state, "Endothelial cells show no cytological atypia." This benign nature of the endothelial cells is crucial in distinguishing Gorham's disease from malignant vascular tumors. Main Distractor: Option A, presence of osteoid seams, is not directly mentioned as a distinguishing feature in the context of Gorham's pathology. The absence of reactive bone formation is mentioned, which is different from osteoid seams.
Question 5
A 17-year-old athlete presents with insidious onset of pain and swelling in his forearm, several months after a minor fall. Radiographs show progressive osteolysis of the radius. Given the potential diagnosis of Gorham's disease, what historical factor is frequently reported by patients?
View Answer & Explanation
Correct Answer: C
Rationale: The case description explicitly states, "Many patients report antecedent trauma." Main Distractor: Option A, family history, is incorrect as Gorham's disease is described as an "idiopathic process," implying no clear genetic predisposition or familial pattern.
Question 6
A 38-year-old female presents with a several-month history of worsening pain and swelling in her left thigh. Radiographs demonstrate complete resorption of the diaphysis of the left femur. What additional radiographic finding might be observed in the local region in Gorham's disease?
View Answer & Explanation
Correct Answer: B
Rationale: The text states, "Local soft tissues may also be involved." This indicates that the disease process is not always confined strictly to the bone. Main Distractor: Option A, periosteal new bone formation, is generally associated with reactive processes or infection, which is not characteristic of Gorham's disease; the text emphasizes the lack of reactive bone formation.
Question 7
A 25-year-old male is diagnosed with Gorham's disease after presenting with progressive bone loss in his humerus. Based on the provided description, how is Gorham's disease primarily classified?
View Answer & Explanation
Correct Answer: C
Rationale: The first sentence of the case description clearly states, "Gorham’s disease is an idiopathic process involving massive, progressive osteolytic changes." Main Distractor: Option A, a primary bone malignancy, is incorrect because the pathology explicitly states "Endothelial cells show no cytological atypia," indicating a benign process, not malignant.
Question 8
A 15-year-old patient is diagnosed with Gorham's disease affecting the scapula. The parents inquire about the long-term course of the disease. Which statement best describes the typical progression of the osteolytic changes?
View Answer & Explanation
Correct Answer: B
Rationale: The description states, "Gorham’s disease is an idiopathic process involving massive, progressive osteolytic changes." This highlights the key characteristic of the disease's progression. Main Distractor: Option C, stabilization after initial rapid bone loss, is incorrect as the disease is described as "progressive," implying ongoing rather than self-limiting or stabilizing destruction.
Question 9
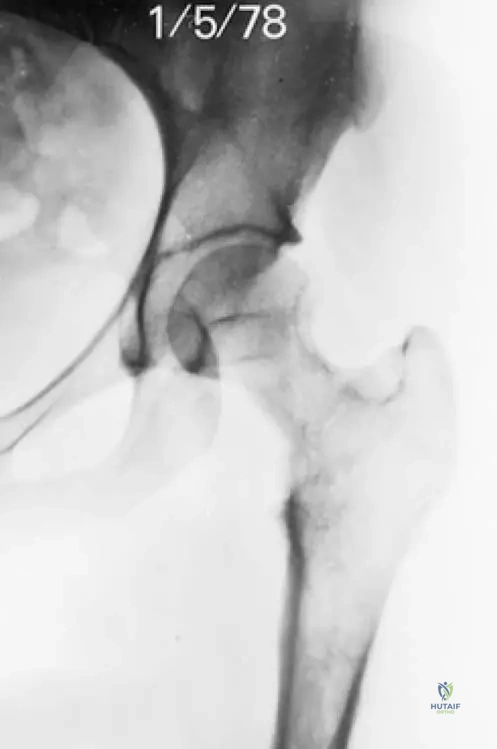
A 60-year-old patient presents with chronic hip pain. Radiographs show significant lytic destruction in the proximal femur with concentric narrowing of the femoral neck, as depicted in the image. This finding is characteristic of which aspect of Gorham's disease?

View Answer & Explanation
Correct Answer: C
Rationale: The image (Fig. 8.57) shows "Lytic destruction in the proximal femur with concentric narrowing of the femoral neck," which is a direct visual representation of the "massive, progressive osteolytic changes" that define Gorham's disease. Main Distractor: Option B, malignant bone tumor infiltration, is incorrect. While it can cause lytic lesions, Gorham's disease is a benign vascular process, and the pathology explicitly states no cytological atypia, ruling out malignancy.
Question 10
A 45-year-old male presents with a "vanishing bone" phenomenon in his left leg. An AP radiograph of the left femur, as shown, demonstrates complete resorption of the diaphysis. This radiographic appearance is a hallmark of Gorham's disease and signifies what?

View Answer & Explanation
Correct Answer: B
Rationale: The image (Fig. 8.62) shows "complete resorption of diaphysis," which is an extreme manifestation of the "massive, progressive osteolytic changes" characteristic of Gorham's disease. This represents extensive and advanced destruction. Main Distractor: Option D, early stages of bone healing, is incorrect. The image clearly shows severe bone loss, which is the opposite of early healing. While sclerotic bone may accompany healing later, complete resorption is a destructive phase.
Question 11
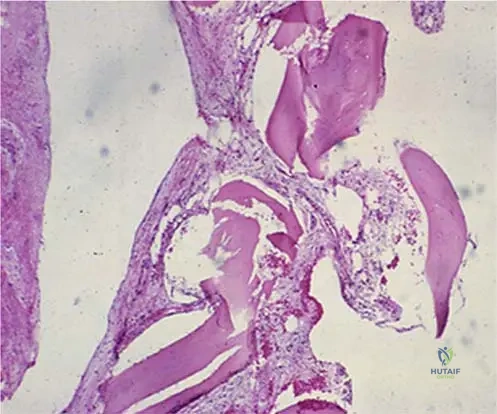
A bone biopsy from a patient with suspected Gorham's disease reveals the microscopic features shown in the image, characterized by cavernous angiomatous spaces. What is a key characteristic of the endothelial cells lining these spaces in Gorham's disease?
View Answer & Explanation
Correct Answer: C
Rationale: The text accompanying Fig. 8.63 explicitly states, "Endothelial cells show no cytological atypia." This benign nature is a defining feature of Gorham's disease. Main Distractor: Option A, they exhibit significant cytological atypia, is the direct opposite of the described pathology and would suggest a malignant vascular tumor rather than Gorham's disease.
Question 12
A pathologist is reviewing a bone biopsy from a patient with extensive osteolysis. The microscopic findings include vascular changes and cavernous angiomatous spaces. To support a diagnosis of Gorham's disease, the pathologist would specifically note the absence of which feature?
View Answer & Explanation
Correct Answer: B
Rationale: The text states, "Microscopic examination shows varying amounts of vascular changes without reactive bone formation." The absence of reactive bone formation is a key diagnostic characteristic. Main Distractor: Option A, endothelial cell proliferation, is incorrect because vascular changes and angiomatous spaces imply endothelial cell proliferation, which is a *present* feature, not an absent one.
Question 13
A 30-year-old patient presents with symptoms related to Gorham's disease. The specific complaints vary widely depending on the affected anatomical site. Which of the following is NOT listed as a general clinical symptom in the provided text?
View Answer & Explanation
Correct Answer: D
Rationale: The text states, "Clinical symptoms vary depending on the anatomic site, with many patients reporting pain, swelling, and mechanical symptoms. Lesions of the vertebral column may cause neurologic findings." Fever is not mentioned as a clinical symptom. Main Distractor: Option A, pain, is incorrect as it is explicitly listed as a common clinical symptom.
Question 14
A 22-year-old patient with Gorham's disease affecting the femur is being monitored with serial radiographs. While the disease is characterized by progressive osteolysis, what radiographic change is noted to potentially occur over time, suggesting a phase of resolution or healing?
View Answer & Explanation
Correct Answer: C
Rationale: The text states, "Over time, sclerotic bone may accompany healing." This indicates a potential late-stage radiographic finding distinct from the initial progressive osteolysis. Main Distractor: Option B, complete disappearance of the affected bone, is a description of the *progression* of osteolysis (as seen in Fig. 8.62), not a sign of healing or resolution.
Question 15
A 40-year-old male presents with a several-month history of worsening pain in his arm. Radiographs show extensive bone loss in the humerus. The primary characteristic of the osteolysis seen in Gorham's disease is described as:
View Answer & Explanation
Correct Answer: B
Rationale: The introductory sentence defines the disease: "Gorham’s disease is an idiopathic process involving massive, progressive osteolytic changes." Main Distractor: Option A, localized and self-limiting, is incorrect because the disease is described as "massive" and "progressive," indicating widespread and ongoing destruction, not a limited or resolving process.
Question 16
A microscopic examination of a bone biopsy from a patient with Gorham's disease reveals vascular changes within the bone marrow. Which specific cell type is primarily involved in forming these characteristic vascular structures?
View Answer & Explanation
Correct Answer: C
Rationale: The text mentions "vascular changes" and "cavernous angiomatous spaces," and specifically states, "Endothelial cells show no cytological atypia." Endothelial cells are the cells that line blood vessels and form vascular structures. Main Distractor: Option B, osteoblasts, are bone-forming cells, and the pathology of Gorham's disease is characterized by the *absence* of reactive bone formation, making osteoblasts not primarily involved in the characteristic vascular changes.
Question 17
A 29-year-old female undergoes a bone biopsy for a lytic lesion in her humerus. Microscopic examination reveals numerous vascular spaces. The image provided shows these spaces. What is the specific descriptive term used for these vascular spaces in the context of Gorham's disease?

View Answer & Explanation
Correct Answer: C
Rationale: The text accompanying Fig. 8.63 explicitly states, "Note the cavernous angiomatous spaces." This is the precise pathological description of the vascular lesions. Main Distractor: Option A, capillary hemangiomas, is a general term for a type of vascular lesion, but "cavernous angiomatous spaces" is the specific and more accurate descriptor provided in the case for Gorham's disease.
Question 18
A 45-year-old male with a history of chronic alcohol abuse presents with insidious onset of left hip pain over the past 3 months. The pain is worse with weight-bearing and activity, and he reports a dull ache even at rest. Physical examination reveals a painful limp, limited internal rotation, and pain with flexion and abduction of the left hip. Radiographs of the hip are initially unremarkable.
View Answer & Explanation
Correct Answer: C
Rationale: The clinical presentation of insidious hip pain, worse with weight-bearing, limited range of motion, and a history of chronic alcohol abuse, with initially normal radiographs, is highly suggestive of early avascular necrosis (AVN) of the femoral head. Alcoholism is a major risk factor for AVN. Early osteoarthritis typically shows radiographic changes, and stress fractures often have a more acute onset or specific activity-related history. Septic arthritis usually presents with more acute, severe pain, fever, and systemic signs. Trochanteric bursitis typically presents with lateral hip pain, tenderness over the greater trochanter, and pain with resisted abduction, not typically limited internal rotation.
Question 19
A 52-year-old male with a 20-year history of heavy alcohol consumption presents with severe right hip pain, significantly limiting his ambulation. He reports progressive pain over the past year. Physical examination shows a Trendelenburg gait, markedly restricted and painful range of motion in all planes of the right hip. Radiographs reveal flattening and sclerosis of the right femoral head with subchondral collapse and joint space narrowing.
View Answer & Explanation
Correct Answer: C
Rationale: The radiographic findings of femoral head collapse (subchondral collapse) and joint space narrowing in the setting of avascular necrosis (AVN) indicate advanced disease (e.g., Ficat Stage III or IV). At this stage, joint-preserving procedures like core decompression or osteotomy are generally not effective. Total hip arthroplasty is the most appropriate surgical treatment for advanced AVN with femoral head collapse and significant functional impairment. NSAIDs and activity modification are palliative and insufficient for advanced disease. Arthrodesis is rarely performed for hip AVN due to its significant functional limitations.
Question 20
A 48-year-old male with chronic alcohol abuse develops avascular necrosis (AVN) of both femoral heads. He asks about the underlying mechanism of how alcohol contributes to this condition. Which of the following is considered the primary pathophysiological mechanism linking chronic alcohol abuse to AVN?
View Answer & Explanation
Correct Answer: C
Rationale: The primary pathophysiological mechanism linking chronic alcohol abuse to avascular necrosis (AVN) is thought to involve hyperlipidemia and fat embolization. Chronic alcohol intake can lead to elevated serum lipid levels, resulting in the formation of fat emboli that occlude small vessels in the bone, particularly in the femoral head. This leads to ischemia and subsequent osteocyte death. While alcohol can affect bone health in other ways (e.g., osteoporosis), and septic emboli can occur, fat embolization is the most widely accepted and significant mechanism for alcoholic AVN. Direct chondrocyte toxicity and impaired calcium metabolism are not primary mechanisms for AVN.
Question 21
A 55-year-old male with a history of heavy alcohol consumption is diagnosed with avascular necrosis (AVN) of the right femoral head. Given his history, he is at increased risk for multifocal disease. Which of the following joints is most commonly affected by AVN in conjunction with the hip in alcoholic patients?
View Answer & Explanation
Correct Answer: C
Rationale: In patients with systemic risk factors for avascular necrosis (AVN), such as chronic alcohol abuse, the disease is often multifocal. After the hip, the knee and shoulder are the most commonly affected joints. The ankle, elbow, wrist, and small joints of the hand are less frequently involved in systemic AVN, although they can occur. Therefore, the shoulder is a common site for multifocal AVN in alcoholic patients.
Question 22
A 60-year-old male with a history of cirrhosis due to chronic alcohol abuse presents to the emergency department with acute onset of severe right knee pain, swelling, and redness. He reports chills and a fever of 101.5°F (38.6°C). Physical examination reveals a warm, erythematous, and exquisitely tender right knee with a large effusion. He is unable to bear weight. What is the most critical immediate diagnostic step?
View Answer & Explanation
Correct Answer: C
Rationale: The patient's presentation (acute, severe pain, swelling, redness, warmth, fever, chills, inability to bear weight) is highly suggestive of septic arthritis, which is a medical emergency. Chronic alcohol abuse and cirrhosis increase the risk of infection. The most critical immediate diagnostic step is to perform an aspiration of the knee joint to obtain synovial fluid for cell count, Gram stain, and culture. This is essential to confirm the diagnosis and identify the causative organism for targeted antibiotic therapy. While antibiotics may be started empirically, joint aspiration should precede them if possible to avoid masking the culture results. MRI is useful for soft tissue and bone assessment but is not the immediate diagnostic priority for septic arthritis. CBC and inflammatory markers are supportive but not definitive. NSAIDs and rest are inappropriate for a suspected infection.
Question 23
A 40-year-old male with a history of heavy beer consumption presents with sudden onset of excruciating pain, swelling, and redness in his right great toe. He describes the pain as the worst he has ever experienced. Physical examination reveals a warm, erythematous, and extremely tender metatarsophalangeal (MTP) joint of the right great toe. Serum uric acid levels are elevated. Which of the following is the most likely diagnosis?
View Answer & Explanation
Correct Answer: D
Rationale: The classic presentation of acute, severe pain, swelling, and redness in the great toe MTP joint (podagra), combined with a history of heavy beer consumption and elevated serum uric acid, is highly characteristic of gout. Alcohol, particularly beer, increases uric acid production and impairs its renal excretion, predisposing individuals to gout flares. While septic arthritis and cellulitis are in the differential for an acutely inflamed joint, the specific location and history strongly point to gout. Pseudogout typically affects larger joints (e.g., knee) and is caused by calcium pyrophosphate crystals. A bunion is a chronic deformity, not an acute inflammatory attack.
Question 24
A 68-year-old male with a history of chronic alcohol use and osteoarthritis presents with acute onset of pain and swelling in his left knee. Arthrocentesis is performed, and synovial fluid analysis reveals positively birefringent, rhomboid-shaped crystals. Which of the following is the most likely diagnosis?
View Answer & Explanation
Correct Answer: C
Rationale: The presence of positively birefringent, rhomboid-shaped crystals in synovial fluid is pathognomonic for calcium pyrophosphate deposition disease (CPPD), also known as pseudogout. While alcohol is more strongly associated with gout (negatively birefringent, needle-shaped urate crystals), CPPD can also occur in older individuals and may be exacerbated by metabolic stress, which can be seen in chronic alcoholics. Gout is ruled out by the crystal morphology. Septic arthritis would show bacteria and a very high white blood cell count. Rheumatoid arthritis is a chronic inflammatory condition with different synovial fluid findings. An osteoarthritis flare would not typically show crystals.
Question 25
A 50-year-old male with a history of chronic alcohol abuse, liver cirrhosis, and recent intravenous drug use presents with a several-day history of worsening right shoulder pain, swelling, and limited range of motion. He has a low-grade fever and appears unwell. What is the most important consideration in the differential diagnosis for his shoulder pain?
View Answer & Explanation
Correct Answer: D
Rationale: The combination of chronic alcohol abuse, liver cirrhosis (which impairs immune function), and intravenous drug use significantly increases the risk of septic arthritis. The acute onset of pain, swelling, limited range of motion, and systemic signs (low-grade fever, unwell appearance) are highly suspicious for septic arthritis. While AVN of the humeral head is a known complication of alcoholism, it typically has a more insidious onset. Rotator cuff tears, adhesive capsulitis, and bicipital tendonitis are less likely to present with acute systemic symptoms and significant swelling. Given the risk factors and acute presentation, septic arthritis must be ruled out urgently.
Question 26
A 58-year-old male with a long history of heavy alcohol intake complains of generalized muscle weakness and pain, particularly in his proximal extremities, making it difficult to rise from a chair or climb stairs. He denies specific joint swelling or redness. Physical examination reveals diffuse muscle tenderness and atrophy, with no specific joint effusions or warmth. Laboratory tests show elevated creatine kinase (CK) levels. What is the most likely diagnosis?
View Answer & Explanation
Correct Answer: B
Rationale: The patient's presentation of generalized proximal muscle weakness, pain, atrophy, and elevated creatine kinase (CK) levels in the context of chronic heavy alcohol intake is classic for alcoholic myopathy. This condition can be acute or chronic and is a direct toxic effect of alcohol on muscle tissue. While peripheral neuropathy can occur with alcoholism, it primarily causes sensory and distal motor deficits, not typically proximal weakness and elevated CK. Gouty arthritis affects joints, not muscles diffusely. Polymyalgia rheumatica typically affects older individuals and is associated with elevated inflammatory markers (ESR/CRP) but not typically high CK. Fibromyalgia is a diagnosis of exclusion with widespread pain but usually normal labs.
Question 27
A 42-year-old male with a history of chronic alcohol use presents with persistent left hip pain for 4 months. Initial radiographs of the hip are normal. Physical examination reveals pain with internal rotation and a mild antalgic gait. Given the strong suspicion for early avascular necrosis (AVN), what is the most sensitive imaging modality to confirm the diagnosis?
View Answer & Explanation
Correct Answer: D
Rationale: For early detection of avascular necrosis (AVN) when plain radiographs are normal, Magnetic Resonance Imaging (MRI) is the most sensitive and specific imaging modality. MRI can detect changes in bone marrow edema and fat necrosis before structural changes are visible on radiographs. CT scans are better for assessing bone architecture and collapse but less sensitive for early changes. Bone scintigraphy can show increased uptake but is less specific than MRI. Ultrasound is primarily used for soft tissue and effusion assessment. Waiting for repeat radiographs delays diagnosis and treatment, as radiographic changes only become apparent in later stages of AVN.
Question 28
A 38-year-old male with a history of alcohol abuse is diagnosed with Ficat Stage I avascular necrosis (AVN) of the right femoral head. He has mild pain with activity and no subchondral collapse on MRI. He is committed to abstaining from alcohol. Which of the following is the most appropriate initial non-surgical management strategy?
View Answer & Explanation
Correct Answer: C
Rationale: For early-stage avascular necrosis (Ficat Stage I or II) without subchondral collapse, especially in a patient committed to addressing the underlying risk factor (alcohol cessation), non-surgical management with protected weight-bearing and observation is a reasonable initial approach. This allows for potential spontaneous healing or stabilization. Core decompression and vascularized fibular grafts are surgical options for early to pre-collapse stages, but observation is often tried first. Bisphosphonates have shown some promise in slowing progression but are not typically first-line monotherapy. Total hip arthroplasty is reserved for advanced stages with collapse.
Question 29
A 47-year-old male with a history of chronic alcohol use presents with persistent left hip pain. MRI confirms Ficat Stage II avascular necrosis (AVN) of the femoral head with significant bone marrow edema but no subchondral collapse. He has failed conservative management including activity modification and protected weight-bearing. What is the most appropriate next step in management?
View Answer & Explanation
Correct Answer: C
Rationale: For Ficat Stage II avascular necrosis (AVN) of the femoral head, where there is significant bone marrow edema but no subchondral collapse, and conservative management has failed, core decompression is a commonly indicated joint-preserving surgical procedure. It aims to reduce intraosseous pressure, improve blood flow, and potentially prevent collapse. Total hip arthroplasty and hemiarthroplasty are typically reserved for more advanced stages (Ficat III and IV) with collapse. Resurfacing arthroplasty has specific indications and contraindications, and continued non-weight-bearing is not a definitive treatment for progressive AVN.
Question 30
A 62-year-old male with a long history of alcohol abuse and severe alcoholic liver disease (cirrhosis) requires a total hip arthroplasty for advanced avascular necrosis of the femoral head. What is a significant perioperative concern specific to this patient's medical history?
View Answer & Explanation
Correct Answer: C
Rationale: Patients with severe alcoholic liver disease (cirrhosis) have impaired synthetic function, leading to coagulopathies (decreased production of clotting factors) and increased risk of bleeding. They also have compromised immune function, making them more susceptible to perioperative infections. These are significant concerns that require careful preoperative optimization and intraoperative management. While alcohol abuse can contribute to decreased bone mineral density, and DVT risk is general to surgery, bleeding and infection are particularly heightened in patients with advanced liver disease. Heterotopic ossification and nerve injury are less specifically linked to alcoholic liver disease compared to bleeding and infection risks.
Question 31
A 50-year-old male with a history of chronic alcohol abuse presents with insidious onset of right knee pain, worse with weight-bearing. Radiographs show subchondral lucency and sclerosis in the medial femoral condyle, without significant joint space narrowing. MRI confirms avascular necrosis (AVN) of the medial femoral condyle. What is the most appropriate initial management for this patient?
View Answer & Explanation
Correct Answer: D
Rationale: For early-stage avascular necrosis (AVN) of the knee, particularly in the medial femoral condyle, and without significant collapse or advanced degenerative changes, conservative management with protected weight-bearing (e.g., crutches, cane) and activity modification is often the initial approach. This allows for potential healing or stabilization of the lesion. Surgical options like total or unicompartmental knee arthroplasty are reserved for more advanced disease with collapse or significant symptoms. High tibial osteotomy might be considered for unicompartmental disease with varus malalignment but is not typically the first step for AVN. Arthroscopic debridement is generally not effective for AVN.
Question 32
A 56-year-old male with a history of chronic alcohol abuse and corticosteroid use for an unrelated condition presents with progressive right shoulder pain and weakness over 6 months. Physical examination reveals painful and limited active and passive range of motion, particularly abduction and external rotation. Radiographs show flattening and sclerosis of the humeral head with some subchondral changes. What is the most likely diagnosis?
View Answer & Explanation
Correct Answer: D
Rationale: The patient's history of chronic alcohol abuse and corticosteroid use are significant risk factors for avascular necrosis (AVN). The progressive shoulder pain, weakness, limited range of motion, and radiographic findings of flattening and sclerosis of the humeral head are characteristic of AVN of the humeral head. While osteoarthritis can cause similar symptoms, the specific radiographic changes and risk factors point more strongly to AVN. Rotator cuff arthropathy typically involves a massive rotator cuff tear. Adhesive capsulitis (frozen shoulder) is characterized by global stiffness but usually normal radiographs. Calcific tendonitis is an acute inflammatory condition.
Question 33
A 49-year-old male with avascular necrosis (AVN) of the femoral head due to chronic alcohol abuse undergoes core decompression. Despite the procedure, his pain persists, and follow-up imaging shows progression of the AVN. He admits to continued heavy alcohol consumption. What is the most significant factor contributing to the failure of his treatment and disease progression?
View Answer & Explanation
Correct Answer: C
Rationale: For avascular necrosis (AVN) caused by chronic alcohol abuse, continued heavy alcohol consumption represents ongoing exposure to the primary risk factor. This significantly undermines the effectiveness of any treatment, surgical or non-surgical, by perpetuating the underlying pathophysiological mechanisms (e.g., fat embolization, hyperlipidemia). While other factors can influence outcomes, addressing and eliminating the primary risk factor is paramount for successful management and preventing disease progression. Inadequate surgical technique, new medical conditions, insufficient physical therapy, or genetic predisposition are less likely to be the *most significant* factor compared to continued alcohol abuse in this specific scenario.
Question 34
A 55-year-old male with a history of chronic alcohol abuse presents with polyarthralgias and fatigue. His physical exam is unremarkable for specific joint effusions or warmth. As part of his workup for alcoholic arthropathy, which of the following laboratory findings would be most indicative of underlying liver dysfunction related to his alcohol use?
View Answer & Explanation
Correct Answer: D
Rationale: Elevated liver transaminases (AST, ALT) are indicators of hepatocellular injury, and decreased albumin is a marker of impaired synthetic function of the liver, both commonly seen in alcoholic liver disease. These findings would directly indicate underlying liver dysfunction related to his alcohol use, which can contribute to various systemic manifestations, including arthropathy. Elevated CRP and ESR are general inflammatory markers. Elevated serum uric acid is associated with gout, a common comorbidity of alcoholism, but not directly indicative of liver dysfunction itself. A positive rheumatoid factor is associated with rheumatoid arthritis, which is not directly linked to alcoholic arthropathy.
Question 35
A 65-year-old male with a long history of poorly controlled diabetes and chronic alcohol abuse presents with progressive deformity and instability of his right ankle. He reports minimal pain despite significant joint destruction. Physical examination reveals a warm, swollen, and unstable ankle with palpable crepitus and rocker-bottom deformity. Radiographs show severe disorganization of the ankle joint, fragmentation, sclerosis, and new bone formation. What is the most likely diagnosis?
View Answer & Explanation
Correct Answer: C
Rationale: The patient's history of poorly controlled diabetes and chronic alcohol abuse are risk factors for peripheral neuropathy. The presentation of progressive joint deformity, instability, minimal pain despite significant destruction, warmth, swelling, and characteristic radiographic findings (fragmentation, sclerosis, new bone formation, rocker-bottom deformity) are classic for Charcot arthropathy (neuroarthropathy). This condition results from repetitive microtrauma to a denervated joint. While severe osteoarthritis can cause joint destruction, the lack of pain and specific radiographic features point away from it. Septic arthritis would typically be more acute and painful. Gout and rheumatoid arthritis have different clinical and radiographic presentations.
Question 36
A 58-year-old male with a history of severe alcoholic cirrhosis presents with clubbing of his fingers and toes, and painful swelling of his wrists and ankles. Radiographs show periostitis of the distal long bones. What is the most likely diagnosis?
View Answer & Explanation
Correct Answer: C
Rationale: The combination of clubbing, painful swelling of peripheral joints (wrists, ankles), and periostitis of the distal long bones in a patient with severe alcoholic cirrhosis is characteristic of hypertrophic osteoarthropathy (HOA). HOA is a paraneoplastic syndrome or can be associated with chronic systemic diseases, including liver cirrhosis. Gout, rheumatoid arthritis, psoriatic arthritis, and osteoarthritis have different clinical and radiographic features and are not typically associated with clubbing and periostitis in this manner.
Question 37
A 45-year-old male presenting with bilateral hip pain is diagnosed with avascular necrosis (AVN) of both femoral heads. He admits to daily alcohol consumption but denies it is problematic. As his orthopedic surgeon, what is the most appropriate initial step regarding his alcohol use?
Question 38
A 45-year-old male with a history of chronic alcohol abuse presents with insidious onset of right hip pain over the past 6 months. The pain is worse with weight-bearing and activity, and he reports a limp. On examination, he has a painful arc of motion, particularly with internal rotation and abduction. Radiographs of the hip are initially unremarkable, but an MRI is ordered. What is the most likely diagnosis?
View Answer & Explanation
Correct Answer: C
Rationale: Chronic alcohol abuse is a major risk factor for avascular necrosis (AVN) of the femoral head, which typically presents with insidious onset of groin pain, worse with weight-bearing, and restricted range of motion, especially internal rotation. Early radiographs can be normal, making MRI the most sensitive diagnostic tool. Osteoarthritis would typically show joint space narrowing and osteophytes on radiographs, and while possible, AVN is more specific to the history. Trochanteric bursitis causes lateral hip pain. Septic arthritis would present more acutely with systemic symptoms. Lumbar radiculopathy would typically have radiating pain and neurological signs.
Question 39
A 52-year-old male with a 20-year history of heavy alcohol consumption is diagnosed with Ficat Stage II avascular necrosis of the left femoral head. He asks about the mechanism by which alcohol contributes to this condition. Which of the following is the primary pathophysiological mechanism?
View Answer & Explanation
Correct Answer: C
Rationale: The primary pathophysiological mechanism linking chronic alcohol abuse to avascular necrosis (AVN) is the development of hyperlipidemia and the formation of fat emboli. These fat emboli occlude small vessels supplying the femoral head, leading to ischemia and osteocyte death. While alcohol can have other effects on bone, vascular occlusion via fat emboli is the most accepted mechanism for AVN. Direct osteocyte toxicity, neuropathy, metabolic acidosis, or impaired calcium absorption are not the primary mechanisms for AVN.
Question 40
A 48-year-old male with chronic alcoholism presents with right hip pain. MRI confirms Ficat Stage I avascular necrosis of the femoral head. He has no collapse of the femoral head and minimal symptoms. What is the most appropriate initial surgical management for this patient?
View Answer & Explanation
Correct Answer: C
Rationale: For early-stage avascular necrosis (Ficat Stage I or II) without femoral head collapse, core decompression is the most appropriate initial surgical intervention. It aims to reduce intraosseous pressure and stimulate revascularization, potentially halting disease progression and preserving the native hip joint. Total hip arthroplasty and hemiarthroplasty are reserved for later stages with significant collapse and joint destruction. Valgus osteotomy can be considered for specific lesions but is less common than core decompression for early stages. Arthrodesis is a salvage procedure for severe, painful arthritis in younger, active patients, not typically for early AVN.
Question 41
A 60-year-old male with a long history of alcohol abuse presents with severe, debilitating bilateral hip pain. Radiographs show Ficat Stage IV avascular necrosis of both femoral heads with significant collapse, joint space narrowing, and secondary degenerative changes. He has failed conservative management. What is the most appropriate surgical treatment?
View Answer & Explanation
Correct Answer: C
Rationale: For late-stage avascular necrosis (Ficat Stage III or IV) with femoral head collapse, significant pain, and secondary degenerative changes, total hip arthroplasty (THA) is the most effective treatment to relieve pain and restore function. Core decompression and osteotomy are indicated for earlier stages before collapse. Arthrodesis is a salvage procedure that sacrifices motion for pain relief and stability, generally not preferred for bilateral disease or in older patients. Non-weight-bearing and pain management are conservative measures that have failed in this scenario.
Question 42
A 55-year-old male with chronic alcohol use presents to the emergency department with acute onset of severe right knee pain, swelling, and erythema. He denies any trauma. On examination, the knee is exquisitely tender, warm, and swollen with a limited range of motion due to pain. He has a fever of 101.5°F (38.6°C) and chills. Radiographs show soft tissue swelling but no fractures or dislocations. What is the most critical immediate diagnostic step?
View Answer & Explanation
Correct Answer: C
Rationale: The presentation of acute monoarticular arthritis with systemic symptoms (fever, chills) in an immunocompromised patient (due to chronic alcohol use) is highly suspicious for septic arthritis. The most critical immediate diagnostic step is to perform an aspiration of the joint to obtain synovial fluid for analysis (cell count with differential, Gram stain, culture, crystal analysis). This allows for definitive diagnosis and guides appropriate antibiotic therapy. While CBC and inflammatory markers are important, they are not diagnostic. Empirical antibiotics should only be started after cultures are obtained. MRI is useful but not as immediate or definitive as aspiration for septic arthritis. NSAIDs are contraindicated if infection is suspected.
Question 43
A 40-year-old male with a history of heavy alcohol intake and occasional binge drinking presents with sudden, excruciating pain and swelling in his right great toe (podagra). The skin over the joint is red and shiny. He denies trauma or fever. His serum uric acid level is elevated. What is the most likely diagnosis?
View Answer & Explanation
Correct Answer: C
Rationale: The classic presentation of acute monoarticular arthritis in the great toe (podagra) with erythema, swelling, and exquisite pain, especially in a patient with heavy alcohol intake and elevated serum uric acid, is highly suggestive of gouty arthritis. Alcohol consumption is a known trigger for gout flares. While septic arthritis and cellulitis can present with similar inflammatory signs, the lack of fever and specific joint involvement make gout more likely. Pseudogout typically affects larger joints (e.g., knee) and involves calcium pyrophosphate crystals. A stress fracture would usually have a history of repetitive activity and different radiographic findings.
Question 44
A 50-year-old male with chronic alcohol abuse presents with an acutely swollen, painful left knee. Arthrocentesis is performed. Which synovial fluid finding is most characteristic of gout?
View Answer & Explanation
Correct Answer: A
Rationale: Gout is definitively diagnosed by the presence of negatively birefringent, needle-shaped urate crystals within neutrophils in the synovial fluid, visualized under polarized light microscopy. Positively birefringent, rhomboid-shaped crystals are characteristic of pseudogout (calcium pyrophosphate deposition disease). A high WBC count with neutrophils and no crystals could be septic arthritis or other inflammatory arthritides. Low WBC count with mononuclear cells is typical of non-inflammatory conditions. Milky, viscous fluid with high protein is not a specific diagnostic finding for gout.
Question 45
A 62-year-old male with a history of chronic alcohol-induced liver cirrhosis and a recent diagnosis of gout presents with an acute flare in his right ankle. He has significant renal impairment (eGFR 35 mL/min). Which medication is the most appropriate for acute management of his gout flare, considering his comorbidities?
View Answer & Explanation
Correct Answer: C
Rationale: In a patient with acute gout flare, NSAIDs (like indomethacin) are often first-line but are contraindicated or used with extreme caution in patients with significant renal impairment and liver disease due to increased risk of adverse effects. Colchicine is also a good option but requires dose adjustment in renal and hepatic impairment and can have significant GI side effects. Oral prednisone (corticosteroids) is a safe and effective option for acute gout flares in patients with renal or hepatic dysfunction, as it is less dependent on renal/hepatic clearance for efficacy and has a favorable risk profile in this context. Allopurinol and probenecid are for chronic uric acid lowering and are not used for acute flares; allopurinol also requires dose adjustment in renal impairment and can cause liver toxicity.
Question 46
A 58-year-old male with a history of chronic alcohol abuse and recurrent gout flares has a serum uric acid level consistently above 9 mg/dL. He has developed tophi in his elbows and feet. He is currently asymptomatic from a flare. What is the most appropriate long-term management strategy for his hyperuricemia?
View Answer & Explanation
Correct Answer: B
Rationale: For patients with recurrent gout flares, tophi, or evidence of gouty arthropathy and persistently elevated serum uric acid, urate-lowering therapy (ULT) is indicated. Allopurinol, a xanthine oxidase inhibitor, is the most commonly used first-line ULT to reduce uric acid production. NSAIDs and colchicine are for acute flare management or prophylaxis during ULT initiation, not for long-term uric acid lowering. Dietary changes are helpful but usually insufficient alone for severe hyperuricemia. Surgical removal of tophi is rarely indicated and does not address the underlying hyperuricemia.
Question 47
A 42-year-old male with a history of intravenous drug use and chronic alcohol abuse presents with a 2-day history of severe pain, swelling, and warmth in his right shoulder. He has a temperature of 102°F (38.9°C), chills, and appears acutely ill. On examination, the shoulder is held in adduction and internal rotation, and any attempt at passive or active motion causes excruciating pain. Radiographs show soft tissue swelling but no bony abnormalities. What is the most urgent diagnostic and therapeutic intervention?
View Answer & Explanation
Correct Answer: C
Rationale: The presentation of acute monoarticular arthritis with severe pain, systemic signs of infection (fever, chills, acutely ill appearance), and risk factors (IV drug use, chronic alcoholism leading to immunocompromise) is highly suggestive of septic arthritis. This is an orthopedic emergency. The most urgent diagnostic and therapeutic intervention is emergent aspiration of the joint for synovial fluid analysis (cell count, Gram stain, culture) and immediate initiation of empiric broad-spectrum intravenous antibiotics after cultures are obtained. Delay in diagnosis and treatment can lead to rapid joint destruction. Oral antibiotics are insufficient. MRI is helpful but not as urgent as aspiration. Analgesics alone are inadequate. Physical therapy is contraindicated in acute septic arthritis.
Question 48
A 38-year-old male with a history of chronic alcohol abuse and poor nutrition presents with acute onset of left hip pain, fever, and malaise. Arthrocentesis of the hip joint is performed. Which synovial fluid analysis result is most indicative of septic arthritis?
View Answer & Explanation
Correct Answer: A
Rationale: Septic arthritis is characterized by a highly inflammatory synovial fluid. The most indicative findings are a very high white blood cell (WBC) count, typically >50,000 cells/µL (often >100,000 cells/µL), with a predominance of neutrophils (>90%), and a positive Gram stain (though Gram stain is only positive in about 50-70% of cases). Option B describes non-inflammatory or mildly inflammatory fluid. Option C describes inflammatory fluid consistent with crystal arthropathy (gout). Option D describes non-inflammatory fluid. Option E describes hemorrhagic fluid, which could be traumatic or from a coagulopathy, but not typically septic arthritis.
Question 49
A 50-year-old male with a history of chronic alcohol abuse is diagnosed with septic arthritis of the right knee caused by Staphylococcus aureus. After initial joint aspiration and initiation of appropriate intravenous antibiotics, what is the next most critical step in management?
View Answer & Explanation
Correct Answer: C
Rationale: For septic arthritis, especially in large joints like the knee and particularly when caused by virulent organisms like S. aureus, surgical irrigation and debridement (arthroscopic or open) is often necessary in addition to intravenous antibiotics. This helps to remove purulent material, fibrin, and debris, reducing the bacterial load and preventing cartilage destruction. While immobilization can provide comfort, it's not the primary treatment. Daily physical therapy is contraindicated in the acute phase. Oral antibiotics are typically used after a period of IV antibiotics, not immediately. Repeat aspiration may be considered if surgical debridement is not performed or if there is concern for persistent infection, but surgical debridement is often preferred for definitive source control.
Question 50
A 45-year-old male with a history of chronic pancreatitis due to alcohol abuse presents with acute pain and swelling in his left ankle. He has a low-grade fever (100.2°F / 37.9°C) and elevated inflammatory markers. Synovial fluid analysis shows a WBC count of 35,000 cells/µL with 80% neutrophils, but Gram stain is negative and no crystals are seen. What is the most appropriate next step to differentiate between septic arthritis and a crystal-induced arthropathy?
View Answer & Explanation
Correct Answer: C
Rationale: The synovial fluid findings (high WBC, high neutrophils, negative Gram stain, no crystals) are ambiguous and could represent either septic arthritis (especially if Gram stain is falsely negative or organism is fastidious) or a highly inflammatory crystal arthropathy (e.g., pseudogout, or even gout where crystals were missed). Given the patient's risk factors (alcoholism, pancreatitis which can cause fat necrosis-induced arthritis), and the potential for severe consequences of untreated septic arthritis, the most appropriate next step is to repeat synovial fluid analysis (ensuring proper collection and immediate transport for culture) and to initiate empiric broad-spectrum antibiotics while awaiting culture results. A serum uric acid level is not diagnostic for acute gout. NSAIDs are contraindicated if infection is suspected. MRI is useful for osteomyelitis but less urgent than ruling out septic arthritis.
Question 51
A 65-year-old male with a 30-year history of heavy alcohol consumption presents with a low-energy distal radius fracture. A DEXA scan reveals osteoporosis. Which of the following is a primary mechanism by which chronic alcohol abuse contributes to osteoporosis?
View Answer & Explanation
Correct Answer: C
Rationale: Chronic alcohol abuse contributes to osteoporosis through multiple mechanisms, but a primary one is impaired calcium and vitamin D absorption and metabolism. Alcohol can damage the intestinal lining, leading to malabsorption, and can also impair liver and kidney function, which are crucial for vitamin D activation. Other mechanisms include direct toxic effects on osteoblasts, increased cortisol levels, hypogonadism, and malnutrition. Options A, B, D, and E describe mechanisms that would either increase bone density or are incorrect in the context of alcohol-induced osteoporosis.
Question 52
A 55-year-old male with chronic alcohol abuse and documented osteoporosis sustains a displaced intertrochanteric hip fracture after a ground-level fall. He has a history of liver cirrhosis and coagulopathy. What is the most important pre-operative consideration for this patient?
View Answer & Explanation
Correct Answer: C
Rationale: Patients with chronic alcohol abuse, especially those with liver cirrhosis, often have significant coagulopathy (due to impaired synthesis of clotting factors) and other systemic issues. Before any surgical intervention for a hip fracture, it is critical to correct any coagulopathy (e.g., with vitamin K, fresh frozen plasma, cryoprecipitate) and optimize liver function as much as possible to minimize perioperative bleeding risk and other complications. While hip fractures generally require timely fixation, addressing life-threatening comorbidities takes precedence. Nutritional supplementation is important but not the most immediate pre-operative concern. Bisphosphonates are for long-term osteoporosis management, not acute fracture care. Alcohol cessation counseling is vital but not an immediate pre-operative step.
Question 53
A 68-year-old male with a long history of alcohol dependence presents with recurrent falls and multiple fragility fractures over the past two years, despite a moderately osteopenic DEXA scan. Beyond bone mineral density, what other factor commonly associated with chronic alcoholism significantly increases his risk of fractures?
View Answer & Explanation
Correct Answer: C
Rationale: Chronic alcoholism is associated with several factors that increase fracture risk beyond just reduced bone mineral density. These include peripheral neuropathy (leading to impaired balance and gait instability), sarcopenia (muscle wasting and weakness), malnutrition, and an increased propensity for falls due to intoxication or withdrawal. Increased muscle mass, improved balance, enhanced vitamin D synthesis, and reduced inflammatory markers are not typically associated with chronic alcoholism and would not increase fracture risk.
Question 54
A 50-year-old male with a history of chronic alcohol-induced pancreatitis presents with acute, migratory polyarthralgia involving his knees and ankles, accompanied by subcutaneous nodules (panniculitis) and abdominal pain. Radiographs of the affected joints are unremarkable. What is the most likely cause of his arthropathy?
View Answer & Explanation
Correct Answer: C
Rationale: Pancreatitis-associated arthropathy is a recognized complication of acute or chronic pancreatitis, often seen in the context of alcohol abuse. It typically presents as an acute, migratory polyarthritis, often involving large joints, and can be accompanied by subcutaneous fat necrosis (panniculitis) and bone lesions. The release of pancreatic enzymes (lipase) into the circulation is thought to play a role. Gout and septic arthritis are less likely given the migratory nature and associated panniculitis. Psoriatic and rheumatoid arthritis have different clinical and serological profiles.
Question 55
A 60-year-old male with a long history of uncontrolled diabetes and chronic alcohol abuse presents with a severely deformed, swollen, and insensate right foot. Radiographs show extensive disorganization of the midfoot joints, fragmentation, subluxation, and osteolysis, consistent with a "rocker-bottom" deformity. He reports minimal pain despite the severe deformity. What is the most likely diagnosis?
View Answer & Explanation
Correct Answer: D
Rationale: The combination of uncontrolled diabetes (a major risk factor for neuropathy), chronic alcohol abuse (another cause of neuropathy), a severely deformed, swollen, and insensate foot with extensive joint disorganization, fragmentation, and subluxation on radiographs (classic "rocker-bottom" deformity) with minimal pain is highly characteristic of Charcot neuroarthropathy. This condition results from progressive joint destruction due to repetitive trauma in a neuropathic limb. Severe osteoarthritis would be painful and typically less destructive. Gout and septic arthritis would be acutely painful and have different radiographic features. Rheumatoid arthritis typically affects smaller joints symmetrically and has different deformities.
Question 56
A 12-year-old male presents for evaluation of knee pain following a minor fall. Radiographs of the knee are obtained, revealing an incidental, sharply marginated, eccentric, metaphyseal lesion in the distal femur. He denies any prior symptoms related to this area. Physical examination is unremarkable. What is the most likely diagnosis?

View Answer & Explanation
Correct Answer: C
Rationale: Nonossifying fibromas (metaphyseal fibrous defects) are commonly detected incidentally in the second decade, are eccentric and metaphyseal, often in the distal femur, and are sharply marginated. The patient's age, incidental finding, and radiographic characteristics are classic for a nonossifying fibroma. Osteosarcoma would typically present with pain, a more aggressive appearance, and often nuclear atypia on histology. Enchondroma is typically diaphyseal or metaphyseal but often central, and less common in the distal femur as an incidental finding with these specific features. Osteoid osteoma presents with characteristic nocturnal pain relieved by NSAIDs and a nidus. Fibrous dysplasia can be metaphyseal but often has a "ground glass" appearance and is less commonly sharply marginated in this context.
Question 57
A 14-year-old female undergoes radiographs for a sports physical, which incidentally reveal a well-defined, lobular lesion in the proximal tibia. She is asymptomatic and has no tenderness on palpation. Based on the typical characteristics of this lesion, what is its most common synonym?

View Answer & Explanation
Correct Answer: B
Rationale: The provided text explicitly states that "Metaphyseal fibrous defect" is a synonym for Nonossifying Fibroma. While "Fibrous Cortical Defect" is often used interchangeably or refers to a smaller version, "Metaphyseal Fibrous Defect" is the direct synonym given in the text. Unicameral bone cysts and aneurysmal bone cysts are distinct lesions with different radiographic and histological features. Osteochondroma is an exostosis.
Question 58
A 10-year-old male presents with an incidental finding of a nonossifying fibroma in the distal tibia. He is asymptomatic, and the lesion occupies less than 20% of the bone diameter. What is the expected physical examination finding for this patient?

View Answer & Explanation
Correct Answer: D
Rationale: The text states, "As they are asymptomatic, there are no common findings on physical examination." Local tenderness would only be expected for large lesions occupying more than half of the bone diameter, presenting with a pathologic fracture. The other options are not typical for an asymptomatic nonossifying fibroma.
Question 59
A 16-year-old male presents to the emergency department after sustaining a fall during a basketball game, resulting in a pathologic fracture through a large lesion in his distal femur. Radiographs show an eccentric, metaphyseal lesion with cortical thinning, occupying more than 60% of the bone diameter. Physical examination reveals local tenderness over the fracture site. What is the most likely underlying lesion?

View Answer & Explanation
Correct Answer: B
Rationale: The clinical scenario describes a patient in the second decade with a large, eccentric, metaphyseal lesion in the distal femur that has resulted in a pathologic fracture. The text explicitly states that "For large lesions occupying more than half of the bone diameter, patients may present with a pathologic fracture and have local tenderness," which is characteristic of a nonossifying fibroma. Osteochondroma is an exostosis and typically does not cause pathologic fractures through the bone shaft. Chondrosarcoma and Ewing sarcoma are malignant tumors with different typical presentations and radiographic features. Simple bone cysts are typically central and often in the proximal humerus or femur, and while they can fracture, the eccentric and lobular description points more towards NOF.
Question 60
A 13-year-old female is diagnosed with a nonossifying fibroma in the distal tibia. Histological examination of a biopsy specimen is performed. Which of the following findings is typically absent in a nonossifying fibroma?

View Answer & Explanation
Correct Answer: D
Rationale: The text states, "Histology shows a variable pattern of fibrous stroma with occasional clusters of giant cells and macrophages. There is no nuclear atypia, although mitotic figures may be present." Therefore, nuclear atypia is typically absent, distinguishing it from malignant lesions. Fibrous stroma, giant cells, macrophages, and even mitotic figures (without atypia) are all described as potentially present.
Question 61
A 15-year-old male presents with an incidental finding of a nonossifying fibroma in the proximal tibia. Radiographs demonstrate a sharply marginated lesion. What is the typical location of these lesions within the long bones?

View Answer & Explanation
Correct Answer: C
Rationale: The text explicitly states, "These lesions are usually eccentric and metaphyseal." The image captions also reinforce this, showing lesions in the distal femur, distal tibia, and proximal tibia, all metaphyseal regions. Diaphyseal, epiphyseal, articular, or purely cortical locations are not the typical presentation described.
Question 62
A 17-year-old female is found to have an asymptomatic nonossifying fibroma in her distal femur during an evaluation for an unrelated ankle sprain. What is the peak age range for the detection of these lesions?

View Answer & Explanation
Correct Answer: B
Rationale: The text states, "Peak age is the second decade." This makes the 17-year-old patient a typical presentation. The other age ranges are less common for the peak detection of nonossifying fibromas.
Question 63
A 10-year-old male presents with an incidental finding of a nonossifying fibroma in the distal tibia. Radiographs show a lesion with a lobular appearance. Which of the following bones is NOT specifically mentioned in the provided text as a common location for nonossifying fibromas?

View Answer & Explanation
Correct Answer: D
Rationale: The text and image captions state that these lesions "often occurring in the long bones of the lower extremity, including the distal femur (a) and distal (b) and proximal (c) tibia." The proximal humerus is a long bone but is not specifically mentioned in the provided text as a common location, whereas the other options are explicitly listed.
Question 64
A 13-year-old female is diagnosed with an asymptomatic nonossifying fibroma in her distal femur. Radiographs show a sharply marginated lesion. What is a characteristic radiographic feature regarding the overlying cortex?

View Answer & Explanation
Correct Answer: C
Rationale: The text states, "The overlying cortex may be thinned and/or expanded." This is a characteristic radiographic feature of nonossifying fibromas. Sclerotic and thickened cortex, erosion with periosteal reaction, or irregular/spiculated cortex would suggest other pathologies, often more aggressive ones. An intact cortex with no changes is less likely if the lesion is of significant size.
Question 65
A 16-year-old male presents with an incidental finding of a nonossifying fibroma in the distal tibia. Radiographs show a lesion with a septated appearance. What is the most common way these lesions are detected?

View Answer & Explanation
Correct Answer: C
Rationale: The text explicitly states, "These lesions most commonly are detected incidentally as part of an evaluation for other reasons, for example, knee pain." While a pathologic fracture can occur, it's not the most common detection method. Severe localized pain, a palpable mass, or systemic symptoms are not typical for the initial detection of an asymptomatic nonossifying fibroma.
Question 66
A 12-year-old female presents with an incidental finding of a nonossifying fibroma in the distal femur. Radiographs show a lesion with a lobular appearance. What is a characteristic radiographic feature regarding the margins of the lesion?

View Answer & Explanation
Correct Answer: C
Rationale: The text states, "Lesions may have a lobular or septated appearance and are usually sharply marginated." Sharply marginated indicates a benign, non-aggressive nature. Ill-defined, infiltrative, permeative, or aggressive margins would suggest a more malignant process. While "corticated with a narrow zone of transition" is often true for benign lesions, "sharply marginated" is the direct descriptor used in the text.
Question 67
A 14-year-old male presents with a pathologic fracture through a nonossifying fibroma in his distal tibia. The lesion is noted to occupy a significant portion of the bone diameter. What is the critical size threshold mentioned in the text that increases the risk of pathologic fracture?

View Answer & Explanation
Correct Answer: C
Rationale: The text states, "For large lesions occupying more than half of the bone diameter, patients may present with a pathologic fracture and have local tenderness." This is the specific threshold mentioned for increased fracture risk. Other percentages are not specified in the provided text.
Question 68
A 10-year-old male is found to have an incidental nonossifying fibroma in his distal femur. Histological analysis of a biopsy specimen is performed. Which of the following cellular components is typically found within the fibrous stroma?

View Answer & Explanation
Correct Answer: C
Rationale: The text states, "Histology shows a variable pattern of fibrous stroma with occasional clusters of giant cells and macrophages." Chondrocytes, osteoblasts, spindle cells with pleomorphism, or adipocytes with hematopoietic elements are not the primary or characteristic cellular components described for nonossifying fibromas in the provided text.
Question 69
A 15-year-old female presents with an incidental nonossifying fibroma in her proximal tibia. Histological examination of a biopsy reveals a fibrous stroma. Regarding mitotic activity, which of the following is true for nonossifying fibromas?

View Answer & Explanation
Correct Answer: C
Rationale: The text states, "There is no nuclear atypia, although mitotic figures may be present." This indicates that the presence of mitotic figures alone does not signify malignancy in nonossifying fibromas, as long as nuclear atypia is absent. The other options contradict this specific histological description.
Question 70
A 13-year-old male presents with an incidental finding of a nonossifying fibroma. The provided image, Fig. 11.16a, shows a characteristic location for these lesions. Which specific bone and region is depicted in Fig. 11.16a?

View Answer & Explanation
Correct Answer: C
Rationale: The image caption explicitly states, "Fig. 11.16 a–c These lesions are usually eccentric and metaphyseal, often occurring in the long bones of the lower extremity, including the distal femur (a) and distal (b) and proximal (c) tibia." Therefore, Fig. 11.16a depicts the distal femur.
Question 71
A 16-year-old female is diagnosed with an asymptomatic nonossifying fibroma. The provided image, Fig. 11.16b, illustrates another common location for these lesions. Which specific bone and region is depicted in Fig. 11.16b?

View Answer & Explanation
Correct Answer: B
Rationale: The image caption explicitly states, "Fig. 11.16 a–c These lesions are usually eccentric and metaphyseal, often occurring in the long bones of the lower extremity, including the distal femur (a) and distal (b) and proximal (c) tibia." Therefore, Fig. 11.16b depicts the distal tibia.
Question 72
A 10-year-old male presents with an incidental finding of a nonossifying fibroma. The provided image, Fig. 11.16c, demonstrates a third common location for these lesions. Which specific bone and region is depicted in Fig. 11.16c?

View Answer & Explanation
Correct Answer: C
Rationale: The image caption explicitly states, "Fig. 11.16 a–c These lesions are usually eccentric and metaphyseal, often occurring in the long bones of the lower extremity, including the distal femur (a) and distal (b) and proximal (c) tibia." Therefore, Fig. 11.16c depicts the proximal tibia.
Question 73
A 14-year-old male presents with an incidental finding of a nonossifying fibroma in the distal femur. Radiographs show a lesion with a lobular appearance. Which of the following radiographic characteristics is NOT typically associated with a nonossifying fibroma as described?

View Answer & Explanation
Correct Answer: E
Rationale: The text describes nonossifying fibromas as "usually eccentric and metaphyseal," with a "lobular or septated appearance" and "sharply marginated" borders. The overlying cortex may be thinned or expanded, but extensive periosteal reaction is not mentioned and would typically suggest a more aggressive or inflammatory process, which is not characteristic of an uncomplicated nonossifying fibroma.
Question 74
A 12-year-old female is diagnosed with a nonossifying fibroma in her distal tibia. She is asymptomatic, and the lesion is small. What is the most likely reason for her presentation to a physician?
<img atlas-113-nonossifying-fibroma-p219-aef92.webp'="" class="aaos-clinical-img" hutaiforthoatlas="" media="" src='/media/Hutaifortho
<div class="aaos-static-mcq" markdown="1">
<h3>Question 21</h3>
<p class="vignette">A 14-year-old male presents with chronic knee pain. Radiographs of the distal femur reveal a sharply marginated, eccentric, metaphyseal lesion with a lobular appearance. The overlying cortex is noted to be thinned. Which of the following is the most characteristic cortical finding associated with this lesion?</p>
<img src='/>
View Answer & Explanation
Correct Answer: C
Rationale: The clinical context describes a Nonossifying Fibroma (NOF). The provided image description explicitly states, "The overlying cortex may be thinned and/or expanded." This is a characteristic radiographic feature of NOFs. Options A, B (only thickened), D, and E describe features more typical of other bone lesions, such as osteoid osteoma, osteosarcoma, or aggressive tumors. The main distractor, B, is partially correct but incomplete as it omits "thinned," which is equally characteristic.
Question 75
A 12-year-old female undergoes biopsy of an incidentally discovered metaphyseal lesion in the proximal tibia. Histological examination reveals a variable pattern of fibrous stroma with occasional clusters of giant cells and macrophages. Mitotic figures are observed. What is the significance of these mitotic figures in the context of this lesion?
View Answer & Explanation
Correct Answer: C
Rationale: The case text states for Nonossifying Fibroma (NOF) histology, "There is no nuclear atypia, although mitotic figures may be present." This indicates that the presence of mitotic figures alone, without nuclear atypia, is a common and benign finding for NOFs and does not signify malignancy. Options A, B, D, and E are incorrect as they suggest malignancy or aggressive behavior, which is contrary to the nature of NOF. The main distractor, A, is incorrect because the text specifically mentions the absence of nuclear atypia, which is a key differentiator for malignancy.
Question 76
A 10-year-old boy presents with an incidental finding on a knee radiograph performed after a minor fall. The radiograph shows a well-defined, lucent lesion in the distal femoral metaphysis. Based on the typical characteristics of a Nonossifying Fibroma, what is the most likely location of this lesion within the bone?

View Answer & Explanation
Correct Answer: D
Rationale: The image description explicitly states that Nonossifying Fibromas (NOFs) "are usually eccentric and metaphyseal." This is a hallmark radiographic feature. Options A, B, C, and E describe locations not typical for NOFs. The main distractor, A, is incorrect as NOFs are metaphyseal, not diaphyseal, and eccentric, not central.
Question 77
A 16-year-old male presents to the emergency department with acute pain and swelling in his distal tibia after a minor trauma. Radiographs reveal a large, sharply marginated, lobulated lesion occupying approximately 60% of the bone diameter, with an associated cortical breach. What is the most likely acute presentation for this patient?
View Answer & Explanation
Correct Answer: A
Rationale: The clinical text states, "For large lesions occupying more than half of the bone diameter, patients may present with a pathologic fracture and have local tenderness." The lesion described (60% of bone diameter) fits this criterion. Options B, C, D, and E are not typical acute presentations for a Nonossifying Fibroma (NOF), especially given the specific size criterion mentioned. The main distractor, B, is incorrect as NOFs are benign lesions and malignant transformation is exceedingly rare and not the typical acute presentation.
Question 78
A 13-year-old girl undergoes a biopsy for a suspected Nonossifying Fibroma in her proximal tibia. The pathologist's report describes fibrous stroma, giant cells, and macrophages. Which of the following histological features, if present, would raise concern for a more aggressive or malignant process, deviating from a typical NOF?
View Answer & Explanation
Correct Answer: C
Rationale: The case text explicitly states for Nonossifying Fibroma (NOF) histology, "There is no nuclear atypia." The presence of nuclear atypia would be a significant finding suggesting a more aggressive or malignant lesion, differentiating it from a benign NOF. Options A, B, D, and E are all described as features that "may be present" or are characteristic of NOF histology. The main distractor, A, is incorrect because the text specifically notes that mitotic figures "may be present" in NOFs without indicating malignancy.
Question 79
A 15-year-old male is found to have an incidental bone lesion in his distal femur during evaluation for a sports injury. The lesion is consistent with a Nonossifying Fibroma. What is the peak age range for the detection of these lesions?
View Answer & Explanation
Correct Answer: B
Rationale: The clinical text explicitly states, "Peak age is the second decade." This makes option B the correct answer. The other age ranges are not the peak age for Nonossifying Fibromas (NOFs). The main distractor, A, is incorrect as the peak is the second decade, though they can be seen in the first.
Question 80
A 13-year-old girl presents with an incidental finding of a well-circumscribed, eccentric, metaphyseal lesion on a radiograph of her leg. Given the typical presentation of a Nonossifying Fibroma, which of the following bones is among the most common locations for this lesion?

View Answer & Explanation
Correct Answer: C
Rationale: The image description states that Nonossifying Fibromas (NOFs) "often occurring in the long bones of the lower extremity, including the distal femur (a) and distal (b) and proximal (c) tibia." Therefore, the distal femur is a very common location. Options A, B, D, and E are less common or atypical locations for NOFs. The main distractor, A, is incorrect as NOFs are predominantly found in the lower extremities.
Question 81
A 10-year-old boy has a radiograph of his leg for a minor injury, revealing an incidental metaphyseal lesion in the proximal tibia. The lesion is lucent, eccentric, and has a lobular appearance. What is the characteristic margin appearance of this lesion?

View Answer & Explanation
Correct Answer: C
Rationale: The image description explicitly states that Nonossifying Fibromas (NOFs) "are usually sharply marginated." This is a key radiographic feature indicating a benign, slow-growing lesion. Options A, B (partially), D, and E describe margins typically associated with more aggressive or malignant bone lesions. The main distractor, A, is incorrect as ill-defined margins suggest an aggressive process, which is not characteristic of NOF.
Question 82
A 14-year-old girl presents with knee pain after a sports injury. Radiographs reveal a small, asymptomatic, eccentric metaphyseal lesion in the distal femur, consistent with a Nonossifying Fibroma. What is the most common reason for the detection of these lesions?
View Answer & Explanation
Correct Answer: C
Rationale: The clinical text states, "Th ese lesions most commonly are detected incidentally as part of an evaluation for other reasons, for example, knee pain." This aligns with the vignette. Options A, D, and E describe symptomatic presentations that are less common or atypical for NOFs, especially for small lesions. Option B is not a standard practice. The main distractor, A, is incorrect because while pathologic fractures can occur with large lesions, incidental detection is the *most common* reason.
Question 83
A 12-year-old boy is referred for evaluation of an incidentally discovered Nonossifying Fibroma in his proximal tibia. He denies any pain or functional limitations related to the lesion. What are the expected physical examination findings for this patient?
View Answer & Explanation
Correct Answer: D
Rationale: The clinical text states, "As they are asymptomatic, there are no common fi ndings on physical examination." This applies to typical, asymptomatic Nonossifying Fibromas (NOFs). Options A, B, C, and E describe findings that might be present with a symptomatic lesion (e.g., pathologic fracture) or other conditions, but not typically with an asymptomatic NOF. The main distractor, A, is incorrect because tenderness and swelling are usually associated with a pathologic fracture, not an asymptomatic NOF.
Question 84
A 15-year-old male undergoes biopsy of a metaphyseal fibrous defect in his distal tibia. Which of the following combinations of histological components is most characteristic of this lesion?
View Answer & Explanation
Correct Answer: B
Rationale: The clinical text states for Nonossifying Fibroma (NOF) histology, "Histology shows a variable pattern of fi brous stroma with occasional clusters of giant cells and macrophages." This directly matches option B. The other options describe histological features characteristic of other bone lesions (e.g., enchondroma, osteosarcoma, normal bone marrow, eosinophilic granuloma). The main distractor, C, is incorrect because while fibrous stroma and spindle cells might be present, nuclear atypia and osteoid formation are indicative of malignancy (osteosarcoma), which is not characteristic of NOF.
Question 85
A 13-year-old athlete has an incidentally discovered Nonossifying Fibroma in his distal femur. The lesion is sharply marginated, eccentric, and measures 4 cm in diameter. The bone diameter at that level is 6 cm. What is the clinical significance of this lesion's size?
View Answer & Explanation
Correct Answer: C
Rationale: The clinical text states, "For large lesions occupying more than half of the bone diameter, patients may present with a pathologic fracture and have local tenderness." In this case, 4 cm / 6 cm = 0.66 or 66%, which is greater than half. Therefore, this lesion carries an increased risk of pathologic fracture. Options A, B, D, and E are incorrect as they misrepresent the natural history or management implications of NOFs. The main distractor, D, is incorrect. While large lesions with fracture risk may warrant intervention, "immediate surgical curettage" is not universally indicated, and observation or activity modification might be considered first, depending on the specific clinical scenario.
Question 86
A 10-year-old boy undergoes radiographs for knee pain, revealing a benign-appearing lesion in the distal femur metaphysis. The lesion is eccentric, sharply marginated, and shows internal divisions. Which descriptive term best characterizes the internal appearance of this Nonossifying Fibroma?

View Answer & Explanation
Correct Answer: C
Rationale: The image description states, "Lesions may have a lobular or septated appearance." This is a characteristic radiographic feature of Nonossifying Fibromas (NOFs). Options A, B, D, and E describe features more commonly associated with other bone lesions (e.g., fibrous dysplasia, enchondroma, Ewing sarcoma, osteosarcoma). The main distractor, A, is incorrect as ground-glass matrix is characteristic of fibrous dysplasia.
Question 87
A 14-year-old male presents with an incidental finding of a well-defined, eccentric, metaphyseal lesion in the distal tibia. The lesion is lucent and appears to have a sclerotic rim. Given the patient's age and the lesion's characteristics, which of the following is the most appropriate initial management strategy for an asymptomatic lesion?
View Answer & Explanation
Correct Answer: C
Rationale: Nonossifying Fibromas (NOFs) are benign, often asymptomatic, and frequently detected incidentally. For asymptomatic lesions, especially those not posing an immediate fracture risk (i.e., not occupying >50% of bone diameter), observation with follow-up radiographs is the standard initial management. They often spontaneously resolve or ossify. Options A, B, D, and E represent overly aggressive or inappropriate treatments for a typical asymptomatic NOF. The main distractor, A, is incorrect because immediate surgical excision is not indicated for an asymptomatic, benign lesion like NOF, unless there's a high risk of fracture or symptoms develop.
Question 88
A 16-year-old female has a Nonossifying Fibroma in her proximal tibia, discovered incidentally. The lesion is small, asymptomatic, and occupies less than 30% of the bone diameter. What is the most likely natural history of this lesion?
View Answer & Explanation
Correct Answer: B
Rationale: Nonossifying Fibromas (NOFs) are benign lesions that often undergo spontaneous regression and ossification, especially smaller, asymptomatic ones. The clinical text implies this by stating they are "most commonly detected incidentally" and "asymptomatic." Options A, C, D, and E describe outcomes that are not typical for NOFs. The main distractor, A, is incorrect as NOFs are benign and do not typically undergo malignant transformation.
Question 89
A 12-year-old boy is diagnosed with a Nonossifying Fibroma in his distal femur. His parents ask about other names for this condition. Which of the following is a recognized synonym for Nonossifying Fibroma?
View Answer & Explanation
Correct Answer: C
Rationale: The clinical text explicitly states, "(Synonym: Metaphyseal fi brous defect)." This makes option C the correct answer. Options A, B, D, and E are distinct benign bone lesions with different characteristics. The main distractor, B, is incorrect as fibrous dysplasia is a separate condition, though both involve fibrous tissue.
Question 90
A 15-year-old male presents with knee pain. Radiographs reveal a well-defined, lucent lesion in the distal femoral metaphysis. The lesion is located towards one side of the bone. Which combination of location descriptors best characterizes a Nonossifying Fibroma?

View Answer & Explanation
Correct Answer: C
Rationale: The image description explicitly states that Nonossifying Fibromas (NOFs) "are usually eccentric and metaphyseal." This combination is a key diagnostic feature. The other options describe locations not typical for NOFs. The main distractor, A, is incorrect as NOFs are metaphyseal, not diaphyseal, and eccentric, not central.
Question 91
A 13-year-old girl is found to have a small, sharply marginated Nonossifying Fibroma in her distal tibia during a workup for ankle sprain. She denies any pain or tenderness directly over the lesion. What is the most common symptomatic presentation of a typical, small Nonossifying Fibroma?
View Answer & Explanation
Correct Answer: D
Rationale: The clinical text states, "As they are asymptomatic, there are no common fi ndings on physical examination." This indicates that the most common presentation for a typical, small Nonossifying Fibroma (NOF) is asymptomatic. Symptomatic presentations (like pathologic fracture) are reserved for large lesions. Options A, B, C, and E describe symptoms not typically associated with a small, uncomplicated NOF. The main distractor, B, is incorrect as persistent pain is not characteristic of small, asymptomatic NOFs.
Question 92
A 10-year-old boy undergoes biopsy of a metaphyseal lesion. Histology reveals fibrous stroma, giant cells, and macrophages. Mitotic figures are present, but there is no nuclear atypia. What is the most appropriate interpretation of these histological findings for a suspected Nonossifying Fibroma?
View Answer & Explanation
Correct Answer: B
Rationale: The clinical text states that Nonossifying Fibroma (NOF) histology shows "fibrous stroma with occasional clusters of giant cells and macrophages. There is no nuclear atypia, although mitotic figures may be present." This combination of findings is entirely consistent with a benign fibrous lesion like an NOF. The absence of nuclear atypia is crucial for ruling out malignancy. Options A, C, D, and E suggest more aggressive, malignant, or infectious processes, which are not supported by the described histology for an NOF. The main distractor, A, is incorrect because the absence of nuclear atypia is a strong indicator against malignancy, even with mitotic figures.
Question 93
A 68-year-old male presents with increasing pain and swelling in his right hip, 3 years after undergoing a total hip arthroplasty. On examination, there is erythema and induration in the right gluteal region, and he reports systemic symptoms including fever. Pus appears to be breaking through the skin. Radiographs show signs of implant loosening.
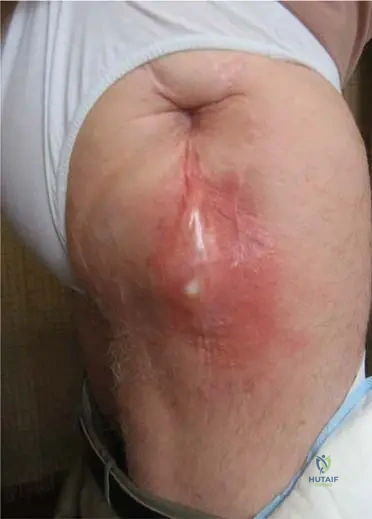
View Answer & Explanation
Correct Answer: C
Rationale: The clinical presentation of pain, swelling, erythema, induration, systemic fever, pus breaking through the skin, and radiographic signs of implant loosening several years post-THA are classic indicators of a chronic periprosthetic joint infection (PJI). The image directly illustrates these local signs of inflammation and pus formation in the gluteal region following THA. Aseptic loosening typically presents with pain but lacks the overt signs of infection (erythema, induration, fever, pus). Deep vein thrombosis would present with swelling and pain, but not typically erythema, induration, or pus in this specific location, nor fever as a primary symptom. Heterotopic ossification is a radiographic finding, not a primary cause of these acute inflammatory signs. Gluteal muscle strain would not cause systemic fever, pus, or implant loosening.
Question 94
A 72-year-old female undergoes revision total knee arthroplasty for suspected periprosthetic joint infection. Intraoperatively, the implant is found to be covered by a slimy material, and the soft tissues of the joint are covered by a pyogenic pseudomembrane. Cultures are sent for analysis. Based on the typical epidemiology of PJI, which group of organisms is most likely to be identified?
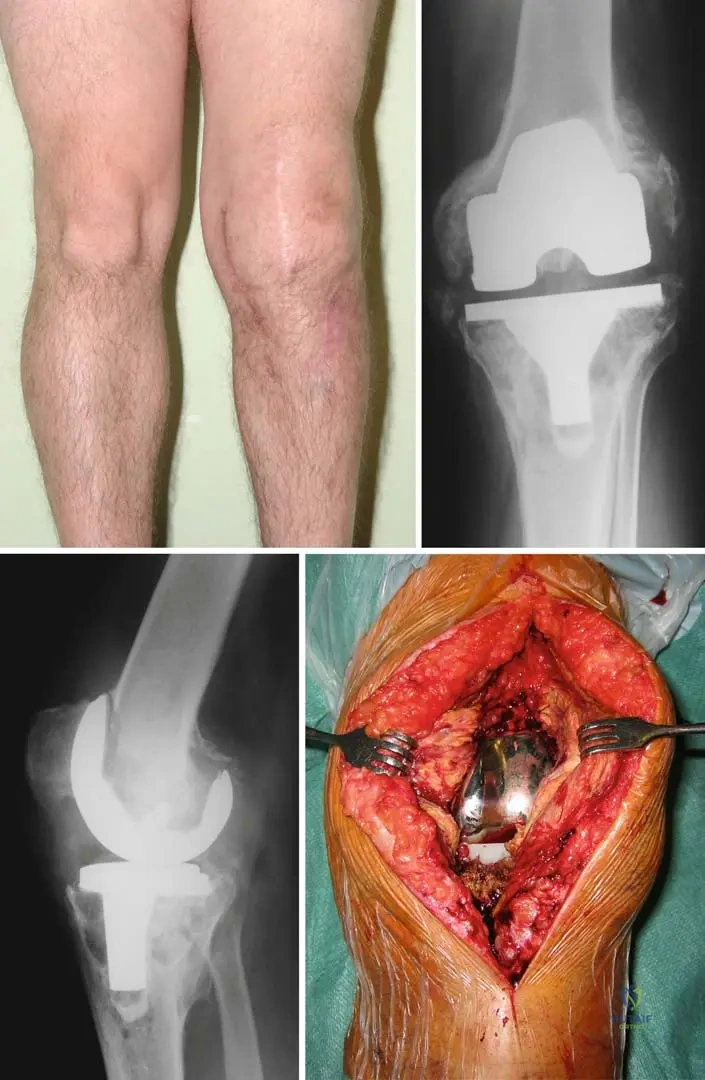
View Answer & Explanation
Correct Answer: D
Rationale: The provided text explicitly states that "The most important agents are Staphylococci (both coagulase-negative and Staphylococcus aureus), which are responsible for the infections in about 50% of all cases." The image context further reinforces this by mentioning "The implant is covered by slime, produced by coagulase-negative Staphylococci." While other organisms can cause PJI, Staphylococci are by far the most common. Gram-negative bacilli, anaerobes, fungi, and streptococci are less common causes of PJI compared to Staphylococci.
Question 95
A 65-year-old male presents with a small discharging sinus in his groin, 2 years after a total hip arthroplasty. He reports intermittent pain and mild swelling. Systemic symptoms are minimal. Physical examination reveals a small opening with seropurulent discharge. Radiographs show radiolucency around the femoral component. To further delineate the extent of the infection and its connection to the joint, which diagnostic procedure is most indicated?
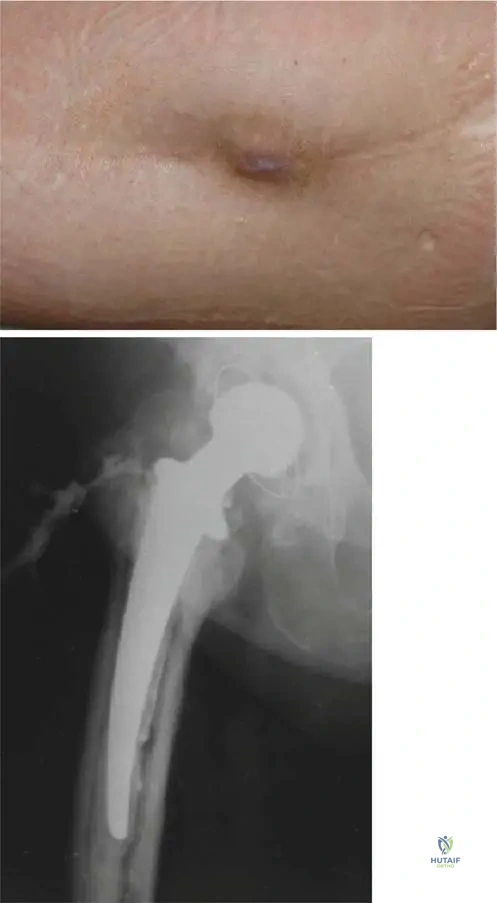
View Answer & Explanation
Correct Answer: C
Rationale: The text explicitly states, "In case of discharging sinuses fistulography is a useful tool." The image (Fig. 2.54 a, b) further demonstrates its utility, showing how the radiopaque fluid reveals the path of pus directly connecting to the infected joint. While aspiration for culture is crucial for identifying the organism, fistulography is specifically indicated to visualize the tract of a draining sinus and its connection to the implant, which is a key diagnostic step in this scenario. Bone scintigraphy and MRI can show inflammation but are not as specific for delineating a sinus tract. A CT scan would show bony changes but not the tract itself as clearly as fistulography.
Question 96
A 58-year-old female presents with a 3-month history of worsening knee pain, swelling, and warmth, 1 year after total knee arthroplasty. She denies fever but reports feeling generally unwell. Physical examination reveals a swollen, erythematous, and tender knee joint with limited range of motion. Radiographs show signs of loosening of the prosthetic components. Which of the following laboratory findings would be most consistent with a periprosthetic joint infection?
View Answer & Explanation
Correct Answer: C
Rationale: The text states that "The clinical symptoms of an infected orthopedic implant are pain, limited function of the prosthetic joint, erythema in the involved region, subfebrility, elevated levels of C-reactive protein, erythrocyte sedimentation rate and WBC counts." Therefore, elevated CRP, ESR, and WBC count are all consistent with a periprosthetic joint infection. While WBC count may not always be elevated in chronic PJI, the combination of elevated CRP and ESR is highly suggestive, and an elevated WBC count further supports the diagnosis. Normal inflammatory markers would argue against infection. Elevated CRP and ESR with a normal WBC count can occur, but the most comprehensive and typical finding includes all three.
Question 97
A 70-year-old male presents with chronic pain and instability in his right knee, 5 years after total knee arthroplasty. He has a history of multiple prior surgeries on the knee. On examination, the skin around the knee is reddish, and the joint is swollen. Radiographs reveal septic loosening of the total knee replacement, with the femoral component tilted and paraarticular ossification. Large osteolytic changes are also observed around the implants. What is the primary mechanism by which bacteria cause loosening of the implant in this scenario?

View Answer & Explanation
Correct Answer: B
Rationale: The text explicitly states, "The connection between the implant and the host bone is disturbed by bacterial pseudomembrane." This pseudomembrane, often composed of biofilm, acts as a barrier and inflammatory mediator, preventing osseointegration and promoting osteolysis, leading to septic loosening. While bacteria can cause inflammation and bone resorption, the direct mechanism described in the text for loosening is the pseudomembrane. Direct mechanical erosion is not the primary mechanism, nor is increased joint fluid pressure. Degradation of implant material by bacterial enzymes is less common than the biofilm-mediated loosening.
Question 98
A 45-year-old male, who underwent a modular tumor knee endoprosthesis placement 4 years ago, presents with progressive knee pain, swelling, and a grayish discoloration of the skin around the knee. Arthrocentesis reveals dark, metallic-appearing joint fluid. Surgical exploration shows a black synovial membrane full of wear particles. Cultures from the joint fluid are positive for Staphylococcus epidermidis. What is the most likely additional complication present in this patient?
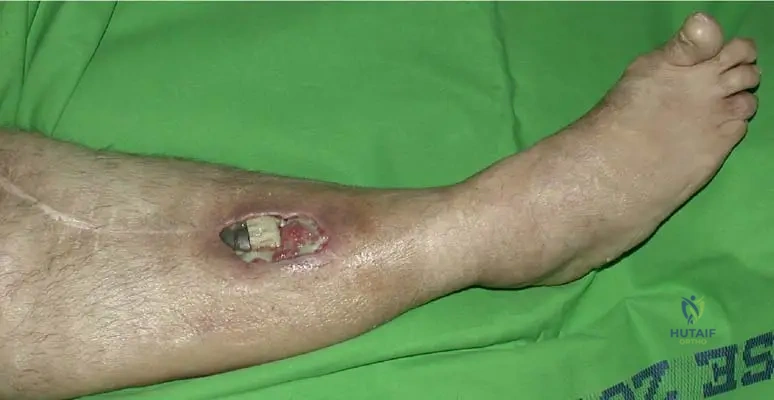
View Answer & Explanation
Correct Answer: C
Rationale: The vignette describes a patient with a modular tumor knee endoprosthesis, grayish skin discoloration, dark joint fluid, and black synovial membrane full of wear particles. The text and image (Fig. 2.60 a, b) specifically link these findings to "metallosis occurred (metal particles in the joint fluid from the implant)." While an infection is also present (positive cultures), the question asks for the *additional* complication described by the specific clinical and intraoperative findings related to metal particles. Aseptic loosening is a differential for pain but doesn't explain the metallosis signs. DVT, HO, and patellar fracture are unrelated to the described metal particle findings.
Question 99
A 60-year-old female presents with a chronic draining sinus in her thigh, 5 years after total hip arthroplasty. She has experienced intermittent fevers and pain. Fistulography is performed, which demonstrates a direct connection between the sinus tract and the infected joint. Radiographs show significant radiolucency around the entire implant. What is the significance of the radiolucency observed around the implant?

View Answer & Explanation
Correct Answer: C
Rationale: The text and image (Fig. 2.54 b) explicitly state, "Note the radiolucency around the entire implant (b)" in the context of an infected joint. This radiolucency represents osteolysis and loss of bone-implant interface, which is characteristic of septic loosening. It is not a normal finding, nor is it evidence of healthy bone remodeling or early osseointegration. Stress shielding refers to bone loss due to reduced mechanical loading, which can cause radiolucency, but in the context of a draining sinus and infection, septic loosening is the more specific and accurate diagnosis.
Question 100
A 75-year-old male presents with a severe deformity of his lower leg and limb length discrepancy, following a complicated open tibial fracture that was treated with internal fixation 2 years prior. He has a history of chronic wound drainage. Radiographs show a large bone defect and a pseudoarticulation. What is the most appropriate term to describe this complication?
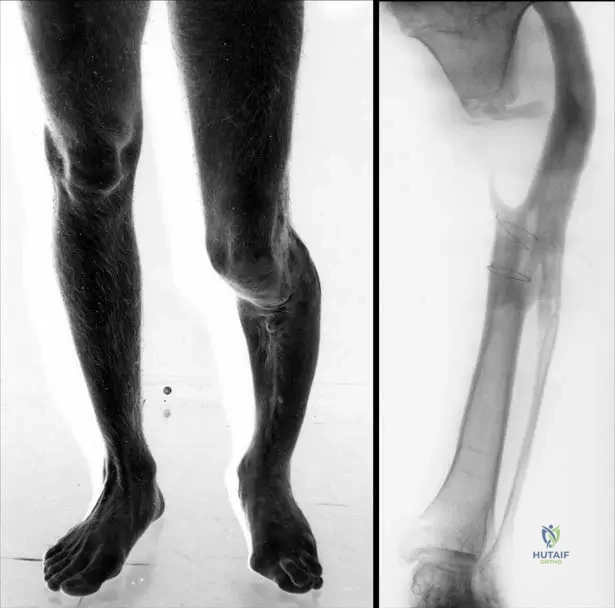
View Answer & Explanation
Correct Answer: C
Rationale: The text and images (Fig. 2.57 a, b) directly describe this scenario as "Septic defect tibial non-union (pseudoarticulation) with a severe deformity of the leg and limb length discrepancy (a). On the radiograph large bone defect is observed (b)." The presence of chronic wound drainage and the described radiographic findings clearly point to a septic non-union with a significant bone defect. Aseptic non-union would lack the infectious component. Malunion implies healing in an incorrect position, not a lack of healing with a defect. Stress fracture is an acute injury. Osteomyelitis without non-union does not fully capture the lack of bone healing and pseudoarticulation.
You Might Also Like

