ABOS Part I Orthopedic Review: Ankle & Calcaneal Fractures, Surgical Management & Rehabilitation | Part 22208
Key Takeaway
This module offers a comprehensive review for the ABOS Part I exam, focusing on advanced orthopedic topics. It covers the diagnosis, surgical management, complications, and rehabilitation of complex ankle fractures (pilon, posterior malleolus) and intra-articular calcaneal fractures. Key areas include surgical approaches, anatomical considerations, classification systems like Sanders and Essex-Lopresti, and critical pre/post-operative patient management.
ABOS Part I Orthopedic Review: Ankle & Calcaneal Fractures, Surgical Management & Rehabilitation | Part 22208
Comprehensive 100-Question Exam
00:00
Start Quiz
Question 1
A 38-year-old male presents with a displaced posterior malleolus fracture involving 35% of the distal tibial articular surface, as confirmed by pre-operative CT scan. The fracture is associated with a fibula fracture and suspected syndesmotic instability. The orthopedic surgeon plans a posterolateral approach for direct reduction and internal fixation. During the initial dissection, which of the following neurovascular structures is most vulnerable and requires meticulous identification and protection?
Explanation
Correct Answer: C - Sural Nerve
The case explicitly states under 'Surgical Anatomy & Biomechanics' that the Sural Nerve runs superficially along the posterolateral aspect of the lower leg, typically coursing with the small saphenous vein. It is vulnerable during the skin incision and initial dissection, especially at the level of the ankle joint, and should be identified and protected, usually retracted anteriorly with the peroneal tendons.
- Option A (Posterior Tibial Nerve): This nerve is located more medially and deep, within the tarsal tunnel. It is generally not at direct risk with a strictly posterolateral approach.
- Option B (Peroneal Artery): This artery is located deep in the posterior compartment, more medially, and is not typically at risk with the posterolateral approach.
- Option D (Flexor Hallucis Longus Tendon): While the FHL tendon is in the surgical field, it is a muscular/tendinous structure, not a neurovascular structure, and is retracted medially with the Achilles tendon. It is not considered 'most vulnerable' in the same sense as a superficial nerve during initial dissection.
- Option E (Small Saphenous Artery): The case mentions the Small Saphenous Vein, which accompanies the sural nerve and is vulnerable. There is no mention of a 'Small Saphenous Artery' in the context of vulnerability during this approach.
Question 2
A 55-year-old diabetic patient sustains a high-energy ankle injury. Initial radiographs show a complex distal tibia fracture. A CT scan is obtained, revealing a comminuted posterolateral pilon fracture with significant articular impaction and a 4mm articular step-off. The soft tissue envelope is swollen but without blistering or open wounds. Based on the case, which of the following statements regarding pre-operative planning and indications is most accurate?
Explanation
Correct Answer: D - A CT scan is absolutely essential for this fracture pattern to plan the surgical approach and assess fragment morphology.
The case explicitly states under 'Pre-Operative Planning & Patient Positioning' that a Computed Tomography (CT) Scan is absolutely essential for posterolateral pilon and posterior malleolus fractures. It provides invaluable information on fracture morphology, fragment size, number, location, articular surface details, and helps confirm the appropriateness of the posterolateral approach.
- Option A (MRI is essential): The case states that MRI is 'Rarely indicated acutely for fracture assessment' and 'not routinely needed for acute fracture planning.'
- Option B (The posterolateral approach is contraindicated): While diabetes is listed as a relative contraindication due to increased risk of wound complications, it is not an absolute contraindication, especially for a significantly displaced articular fracture like a pilon fracture. The case notes that 'uncontrolled diabetes mellitus' is a relative contraindication, implying that with control, surgery is possible.
- Option C (Immediate surgical fixation is indicated): The case highlights that 'High-energy pilon fractures or those with severe soft tissue compromise often require staged management, beginning with external fixation and delaying definitive internal fixation until the soft tissue swelling has subsided (e.g., 7-14 days).' While the soft tissue is currently 'swollen but without blistering,' the high-energy nature of a pilon fracture often necessitates waiting for the 'wrinkle sign' to return, making immediate fixation potentially risky for wound complications.
- Option E (Non-operative management with casting is a viable option): The case clearly states that for posterolateral pilon fractures, non-operative management is 'Extremely rare (e.g., minimally displaced, stable fissure fracture without articular step-off). Typically requires operative stabilization due to high-energy mechanism and articular involvement.' A 4mm articular step-off unequivocally indicates operative management.
Question 3
A 28-year-old athlete presents with an ankle fracture. CT imaging reveals a posterior malleolus fracture involving 28% of the distal tibial articular surface with 3mm of posterior displacement and evidence of PITFL disruption. The fibula is intact. Based on the biomechanical principles and indications outlined in the case, what is the most appropriate management strategy?
Explanation
Correct Answer: C - Direct reduction and stable internal fixation of the posterior malleolus via a posterolateral approach.
The case emphasizes that 'Displaced posterior malleolus fractures' with 'Fragment Size: Generally accepted threshold is >25-30% of the distal tibial articular surface involved' or 'Displacement: Any articular step-off or gap greater than 2mm' are indications for operative intervention. The patient's fracture involves 28% of the articular surface and has 3mm of displacement, meeting these criteria. Furthermore, the case states that 'The posterolateral approach offers direct visualization and facilitates anatomical reduction and stable internal fixation of these difficult-to-access fragments, crucial for restoring articular congruity and overall ankle stability.' PITFL disruption further supports the need for direct stabilization.
- Option A (Non-operative management): This is incorrect. The fragment size (28%) and displacement (3mm) exceed the thresholds for non-operative management (<10-15% and <2mm displacement).
- Option B (Indirect reduction and syndesmotic screw fixation): The case highlights that 'indirect reduction techniques... are often unreliable in achieving and maintaining anatomical congruity.' While syndesmotic instability is present, direct fixation of the posterior malleolus (which is the PITFL attachment site) is the primary goal, and often restores syndesmotic stability. An anterolateral approach would not provide direct access to the posterior malleolus.
- Option D (External fixation as a definitive treatment): External fixation is typically used as a temporizing measure for severe soft tissue compromise or highly comminuted pilon fractures, not as a definitive treatment for a posterior malleolus fracture requiring articular reduction.
- Option E (Medial approach for deltoid ligament repair and indirect reduction): A medial approach would address the deltoid ligament (if injured, though not specified here) but would not provide direct access for anatomical reduction of a posterior malleolus fracture. Indirect reduction is generally discouraged for displaced articular fragments.
Question 4
A 62-year-old female undergoes a posterolateral approach for a complex pilon fracture. Post-operatively, she complains of numbness and tingling along the lateral aspect of her foot and ankle, extending to her little toe. On examination, she has diminished sensation in the distribution of the sural nerve. Which of the following is the most appropriate initial management strategy for this complication?
Explanation
Correct Answer: C - Observation, NSAIDs, and reassurance, as most neurapraxias resolve spontaneously.
The case discusses 'Sural Nerve Injury' under 'Complications & Management,' stating that it can range from temporary neurapraxia to permanent transection. For 'Post-operative' management, it advises 'Conservative management for neurapraxia (observation, NSAIDs).' The symptoms described are consistent with a neurapraxia (stretch or contusion injury) rather than a complete transection, which typically presents with immediate and complete loss of sensation. Most neurapraxias improve over weeks to months.
- Option A (Immediate surgical exploration and nerve repair): This is too aggressive for an initial presentation of sensory deficit, which is likely neurapraxia. Surgical exploration is reserved for persistent symptoms or clear evidence of transection.
- Option B (Referral for EMG and NCS within 48 hours): While EMG/NCS can be useful, they are typically not performed acutely (within 48 hours) as nerve degeneration takes time to manifest on these studies. They are more useful for assessing nerve recovery or persistent deficits after several weeks to months.
- Option D (Application of a nerve block): A nerve block might temporarily alleviate symptoms but does not address the underlying issue or aid in recovery. It's not an initial management strategy for the nerve injury itself.
- Option E (Initiation of high-dose oral corticosteroids): There is no evidence presented in the case, nor is it standard practice, to use high-dose oral corticosteroids for sural nerve neurapraxia following ankle surgery.
Question 5
During a posterolateral approach for a displaced posterior malleolus fracture, the surgeon has successfully exposed the posterior aspect of the distal tibia. The posterior malleolus fragment is large and impacted. Which of the following is the most appropriate sequence of steps for reduction and temporary fixation of this fragment?
Explanation
Correct Answer: B - Use a small osteotome to disimpact and elevate the articular surface, then manipulate the fragment with a ball-spiked pusher, and secure with temporary K-wires.
The case describes 'Reduction Techniques for Posterior Malleolus' under 'Detailed Surgical Approach Technique.' For impacted fragments, it states: 'For impacted fragments, a small osteotome or Freer elevator can be used to disimpact and elevate the articular surface.' For large fragments, it advises: 'If the posterior malleolus is a single, large fragment, use a ball-spiked pusher or a small pointed reduction clamp to manipulate it directly back into anatomical position.' Finally, for temporary fixation: 'Once anatomical reduction is achieved, maintain it with temporary K-wires (e.g., 1.2-1.6mm) drilled from posterior to anterior into the distal tibia.'
- Option A (Apply a posterior antiglide plate, then use lag screws, and finally assess syndesmotic stability): This sequence is incorrect. Fixation (plates and lag screws) comes after reduction and temporary fixation. Syndesmotic stability is assessed after posterior malleolus fixation.
- Option C (Perform indirect reduction by external rotation of the foot, followed by syndesmotic screw placement): Indirect reduction is generally discouraged for displaced articular fragments, and syndesmotic screw placement is not the primary step for posterior malleolus reduction.
- Option D (Immediately insert two 4.0mm lag screws): Lag screws are for definitive fixation after reduction and temporary stabilization, not as an immediate reduction step.
- Option E (Debride the fracture site, then apply a reduction clamp, and proceed directly to definitive plate fixation): While debridement is correct, proceeding directly to definitive plate fixation without temporary stabilization (K-wires) and fluoroscopic confirmation of reduction is not the safest or most precise method.
Question 6
A 45-year-old construction worker undergoes a posterolateral approach for a comminuted posterolateral pilon fracture with significant metaphyseal bone loss. After achieving anatomical reduction of the articular fragments, the surgeon notes a substantial underlying metaphyseal defect. According to the case, what is the most appropriate next step in managing this defect?
Explanation
Correct Answer: B - Fill the defect with autograft or allograft to provide structural support and prevent collapse.
Under 'Internal Fixation' for 'Posterolateral Pilon Fixation,' the case states: 'If significant metaphyseal bone loss or impaction exists beneath reduced articular fragments, bone graft (autograft or allograft) should be placed to provide structural support and prevent collapse. This is particularly important in high-energy pilon fractures.'
- Option A (Proceed directly to locking plate fixation without addressing the defect): This is incorrect. Without addressing the metaphyseal defect, the reduced articular fragments lack underlying support and are prone to collapse, leading to malunion and post-traumatic arthritis, even with locking plate fixation.
- Option C (Apply a non-locking 1/3 tubular plate): While a 1/3 tubular plate can be used for posterior malleolus, for a comminuted pilon fracture with bone loss, locking plates are generally preferred for their stability, and the plate alone does not address the bone defect.
- Option D (Perform a primary ankle arthrodesis): Primary arthrodesis is a salvage procedure for severe, end-stage arthritis or irreconstructible fractures, not typically the initial treatment for a pilon fracture where reconstruction is possible. The case mentions it as a consideration for 'severe bone loss' but 'rare for primary treatment of posterior malleolus,' implying reconstruction is preferred for pilon fractures if feasible.
- Option E (Use a syndesmotic screw to compress the articular fragments): A syndesmotic screw is used to stabilize the syndesmosis, not to compress articular fragments into a metaphyseal defect. This would be an inappropriate use of the implant.
Question 7
A 70-year-old patient with a history of peripheral vascular disease and well-controlled diabetes undergoes a posterolateral approach for a displaced posterior malleolus fracture. Post-operatively, the patient develops increasing pain, erythema, and purulent discharge from the wound. Despite oral antibiotics, the infection progresses, and deep tissue involvement is suspected. Based on the case, what is the most appropriate next step in managing this deep surgical site infection?
Explanation
Correct Answer: B - Initiate intravenous antibiotics and consider surgical debridement.
Under 'Complications & Management,' for 'Wound Complications,' the case states: 'Deep Infection: Surgical debridement, intravenous antibiotics, potentially hardware removal (once fracture is healed), antibiotic beads, or negative pressure wound therapy.' The patient's symptoms (increasing pain, erythema, purulent discharge, suspected deep tissue involvement) indicate a deep infection requiring aggressive management.
- Option A (Continue oral antibiotics): Oral antibiotics are typically for superficial infections. A deep infection requires intravenous antibiotics and often surgical intervention.
- Option C (Remove all hardware immediately): Hardware removal is generally considered once the fracture is healed, as immediate removal in an acute setting can lead to fracture instability and nonunion. It's not the first step for a deep infection unless the hardware itself is the source of infection and stability can be maintained.
- Option D (Apply negative pressure wound therapy as the sole treatment): Negative pressure wound therapy (NPWT) is a valuable adjunct for wound management but is not a sole treatment for a deep infection; it must be combined with debridement and antibiotics.
- Option E (Perform a skin graft): A skin graft is used to cover a clean wound defect after infection has been controlled and viable tissue is present, not as an initial treatment for an active deep infection.
Question 8
A 42-year-old male undergoes a posterolateral approach for a stable fixation of a posterior malleolus fracture. The surgeon confirms anatomical reduction and stable fixation intraoperatively. According to the post-operative rehabilitation protocols outlined in the case, what is the typical initial weight-bearing status and duration for this patient?
Explanation
Correct Answer: C - Non-weight bearing for 6-8 weeks in a posterior splint, then walking boot.
Under 'Post-Operative Rehabilitation Protocols,' in 'Phase 1 Immobilization & Early Healing,' the case states for 'Weight Bearing': 'Non-Weight Bearing (NWB): Essential for 6-8 weeks, or longer for complex pilon fractures or if significant comminution/bone graft was utilized.' It also mentions 'Immediately post-op: Well-padded posterior splint (neutral dorsiflexion/plantarflexion) for 2-3 weeks. Transition to: Removable walking boot (CAM walker) at 2-3 weeks.'
- Option A (Full weight bearing immediately): This is incorrect. Full weight bearing is not allowed immediately after stable fixation of an ankle fracture via this approach.
- Option B (Partial weight bearing (25%) in a cast for 2-3 weeks): Partial weight bearing typically begins at 6-8 weeks, not 2-3 weeks, and the initial immobilization is a splint, then a boot, not necessarily a cast.
- Option D (Touch-down weight bearing for 4 weeks, then full weight bearing): While touch-down weight bearing is for balance, the NWB period is longer (6-8 weeks), and progression to FWB is gradual, not immediately after 4 weeks.
- Option E (Non-weight bearing for 2 weeks, then transition to full weight bearing): The NWB period is typically 6-8 weeks, not just 2 weeks, and the transition to FWB is gradual, not immediate.
Question 9
A 50-year-old male presents with a high-energy ankle injury. CT scan reveals a comminuted posterolateral pilon fracture with significant articular impaction and a large metaphyseal defect. The fibula is also fractured. During the posterolateral approach, after debridement and initial reduction of the articular fragments, what is the most appropriate sequence of fixation steps, considering the principles outlined in the case?
Explanation
Correct Answer: A - Fix the fibula first to restore length, then address the pilon fracture with lag screws and a locking plate, and finally bone graft the metaphyseal defect.
The case states under 'Reduction Techniques for Posterolateral Pilon Fractures': 'Restoration of Fibular Length: If a fibula fracture is present, ensure its length and rotation are restored first, as this can help guide the reduction of the posterior tibial fragments (often performed via the same posterolateral incision, plating the posterior aspect of the fibula).' It then discusses 'Lag Screws' for articular reduction and 'Locking Plate Fixation' for buttressing and stability. Finally, for 'Bone Grafting,' it states: 'If significant metaphyseal bone loss or impaction exists beneath reduced articular fragments, bone graft (autograft or allograft) should be placed to provide structural support and prevent collapse.'
- Option B (Address the pilon fracture first): This is incorrect. The fibula should be fixed first to restore length and guide tibial reduction. Bone grafting is essential for significant defects, not just if instability persists.
- Option C (Perform a primary ankle arthrodesis): This is a salvage procedure, not the primary treatment for a reconstructible pilon fracture.
- Option D (Apply an external fixator as definitive treatment): External fixation is typically a temporizing measure for complex pilon fractures with severe soft tissue compromise, not a definitive treatment for articular reconstruction.
- Option E (Fix the fibula, then apply a posterior antiglide plate to the pilon, and use syndesmotic screws to compress the articular fragments): While fibula fixation is correct, a posterior antiglide plate is more commonly for posterior malleolus, and for pilon, specialized locking plates are often used. Syndesmotic screws are for syndesmotic stability, not for compressing articular fragments into a defect.
Question 10
A surgeon is preparing for a posterolateral approach to fix a posterior malleolus fracture. The patient has a history of severe obesity and sleep apnea, making prone positioning challenging for anesthetic access. Which alternative patient positioning, as described in the case, offers easier anesthetic access while still allowing for the posterolateral approach?
Explanation
Correct Answer: B - Lateral decubitus position on the contralateral side of the injured ankle.
Under 'Pre-Operative Planning & Patient Positioning,' the case discusses 'Patient Positioning.' For the 'Lateral Decubitus Position,' it lists 'Advantages' including 'Easier anesthetic access to the airway.' It specifies the setup: 'Patient is placed in a lateral decubitus position on the contralateral side of the injured ankle (e.g., right ankle injury, left lateral decubitus). '
- Option A (Supine position): A supine position does not provide adequate direct access to the posterolateral aspect of the ankle for this approach.
- Option C (Beach chair position): The beach chair position is typically used for shoulder or elbow surgery and is not suitable for a posterolateral ankle approach.
- Option D (Lithotomy position): The lithotomy position is used for perineal or lower extremity procedures but does not provide optimal exposure for a posterolateral ankle approach.
- Option E (Prone position with the patient's head turned to the side): While the head is turned in prone, the case explicitly states 'More challenging for anesthetic access to the airway if intubated' as a disadvantage of the prone position, making it less ideal for a patient with sleep apnea.
Question 11
A 32-year-old male presents with an ankle fracture. Initial radiographs show a posterior malleolus fracture. A subsequent CT scan reveals a posterior malleolus fragment involving 12% of the distal tibial articular surface with 2.5mm of posterior displacement. The syndesmosis appears stable on initial clinical examination. Based on the evolving literature guidelines summarized in the case, what is the most appropriate management decision?
Explanation
Correct Answer: C - Direct reduction and stable internal fixation of the posterior malleolus via a posterolateral approach, given the displacement.
Under 'Summary of Key Literature Guidelines,' the case states: 'While historically a 25-30% involvement of the articular surface was the most common threshold for posterior malleolus fixation, recent literature suggests that smaller fragments may warrant fixation if they are displaced (>2mm step-off/gap) or contribute to syndesmotic instability.' The patient's fracture, despite being 12% (below the traditional threshold), has 2.5mm of displacement, which exceeds the 2mm displacement threshold for operative intervention. The posterolateral approach is the preferred method for direct reduction and stable fixation.
- Option A (Non-operative management): This is incorrect. While the fragment size is below the traditional threshold, the significant displacement (>2mm) is a clear indication for operative management according to current literature.
- Option B (Indirect reduction and syndesmotic screw fixation): Indirect reduction is generally unreliable for displaced articular fragments. While syndesmotic instability can be associated, the primary issue here is the displaced articular fragment, which requires direct reduction.
- Option D (External fixation as a temporizing measure): External fixation is typically reserved for severe soft tissue compromise or highly comminuted pilon fractures, not for an isolated posterior malleolus fracture requiring articular reduction.
- Option E (Medial approach): A medial approach does not provide direct access to the posterior malleolus for anatomical reduction.
Question 12
A 38-year-old male presents to the emergency department after a 10-foot fall from a ladder onto both feet, experiencing severe bilateral heel pain and inability to bear weight. Given the high-energy axial loading mechanism of injury, which of the following associated injuries is MOST crucial to rule out during the initial assessment?
Explanation
Correct Answer: C
Explanation:
The case explicitly states, 'Upon initial assessment, specific inquiry was made regarding other potential injuries, especially those associated with high-energy axial loading. This included symptoms referable to the lumbar spine, which is crucial given the incidence of concomitant spinal fractures (up to 10-15% in calcaneal fractures).' High-energy axial load injuries, such as falls from height, transmit significant force through the entire kinetic chain, making the lumbar spine particularly vulnerable to compression fractures. Therefore, ruling out a lumbar spine fracture is a critical initial step.
Incorrect Options:
- A. Contralateral talar neck fracture: While talar fractures can occur with high-energy mechanisms, and a contralateral injury is possible, the incidence of concomitant spinal fractures with calcaneal fractures is higher and carries greater potential for neurological deficit, making it a more critical initial screen.
- B. Tibial pilon fracture: Pilon fractures are also high-energy injuries, but the primary mechanism for calcaneal fractures (axial load through the heel) is distinct from the typical mechanism for pilon fractures (axial load driving the talus into the distal tibia). While possible, it's not as commonly associated as lumbar spine fractures.
- D. Midfoot compartment syndrome: Compartment syndrome of the foot is a serious complication that must be monitored, but it is a consequence of the foot injury itself rather than a distinct associated injury in a different anatomical region. The initial assessment focuses on ruling out injuries that might be overlooked due to the obvious foot pain.
- E. Achilles tendon avulsion: While avulsion fractures of the calcaneal tuberosity can occur, a pure Achilles tendon avulsion is less common with a direct axial load mechanism that causes intra-articular calcaneal fractures. The case notes the Achilles tendon was intact.
Question 13
The patient's mechanism of injury involved a direct axial load. According to the biomechanics described in the case, what is the primary event that initiates the typical intra-articular calcaneal fracture pattern?
Explanation
Correct Answer: B
Explanation:
The case explicitly states, 'The biomechanics of this injury pattern involve a high-energy axial load where the body weight is driven downward while the ground reaction force is transmitted upward through the heel. In this scenario, the lateral process of the talus acts as a wedge, driving into the crucial angle of Gissane of the calcaneus. This sheer force typically creates a primary fracture line extending from the proximal-medial aspect to the distal-lateral aspect of the calcaneus...' This describes the classic mechanism for intra-articular calcaneal fractures.
Incorrect Options:
- A. Hyperplantarflexion causing avulsion of the anterior process: While anterior process fractures can occur, they are typically extra-articular and often result from hyperplantarflexion with inversion, not the primary mechanism for a complex intra-articular fracture.
- C. Direct impact of the calcaneal tuberosity on the ground causing a crush injury: While the tuberosity is impacted, the critical internal mechanism involves the talus acting as a wedge, not just a direct crush. The comminution is a secondary effect of the energy dissipation.
- D. Eversion injury leading to disruption of the calcaneocuboid joint: Eversion injuries are less common for calcaneal fractures and typically involve different ligamentous or bony structures. While the calcaneocuboid joint can be involved, it's not the primary initiating event for the intra-articular pattern.
- E. Inversion injury causing a stress fracture of the sustentaculum tali: Inversion injuries are more associated with lateral ankle sprains or talar dome injuries. The sustentaculum tali is a robust structure, and its fracture is usually part of a larger intra-articular pattern, not an isolated stress fracture from inversion.
Question 14
During the clinical examination, the patient exhibited Mondor's sign on the left foot. What is the significance of this finding in the context of a calcaneal fracture?
Explanation
Correct Answer: B
Explanation:
The case states, 'The presence of Mondor's sign—a plantar ecchymosis extending along the plantar fascia—is pathognomonic for a calcaneal fracture and indicates significant deep hematoma tracking along fascial planes.' This sign is a classic indicator of a calcaneal fracture due to the extensive cancellous bone and the deep location of the injury.
Incorrect Options:
- A. It indicates impending compartment syndrome of the foot: While compartment syndrome is a concern, Mondor's sign itself is not a direct indicator of impending compartment syndrome. It signifies deep bleeding, which can contribute to swelling, but compartment syndrome has specific clinical signs like pain out of proportion and pain with passive stretch.
- C. It suggests a concomitant sural nerve injury requiring immediate exploration: Mondor's sign is related to hematoma, not directly to nerve injury. Sural nerve injury is a risk with these fractures and surgical approaches, but it's assessed by sensory examination, not ecchymosis.
- D. It is a sign of an open fracture with communication to the skin: Mondor's sign is subcutaneous ecchymosis, indicating a closed injury with deep bleeding, not an open fracture.
- E. It implies a severe talar body fracture rather than a calcaneal fracture: Mondor's sign is specifically associated with calcaneal fractures due to the unique anatomy and mechanism of injury, not talar fractures.
Question 15
Initial radiographs of the left calcaneus revealed a Bohler's angle of 5 degrees (normal 20-40 degrees) and a Gissane's angle of 140 degrees (normal 100-120 degrees). What do these specific radiographic findings collectively indicate?
Explanation
Correct Answer: B
Explanation:
The case states, 'X-ray Findings (Left Calcaneus): Lateral View: Demonstrated a significant decrease in Bohler's angle (measured at 5 degrees, normal 20-40 degrees), indicative of substantial collapse of the posterior facet and loss of calcaneal height. Gissane's angle (Crucial angle) was increased to 140 degrees (normal 100-120 degrees), reflecting the disruption of the lateral process of the talus and the primary fracture line.' These two angles are critical for assessing the severity and intra-articular nature of calcaneal fractures.
Incorrect Options:
- A. An isolated anterior process fracture with minimal displacement: Anterior process fractures typically do not significantly alter Bohler's or Gissane's angles.
- C. A non-displaced extra-articular fracture of the calcaneal tuberosity: While a tuberosity fracture can affect calcaneal height, a non-displaced extra-articular fracture would not typically cause such a drastic reduction in Bohler's angle or increase in Gissane's angle, which are hallmarks of intra-articular collapse.
- D. A subtalar dislocation with intact calcaneal morphology: Subtalar dislocations involve disruption of the talocalcaneal and talonavicular joints, but the calcaneal bone itself may be intact. The described angle changes are specific to calcaneal bone collapse.
- E. A talar neck fracture with secondary involvement of the calcaneus: Talar neck fractures primarily affect the talus and its relationship with the tibia and navicular, not directly the calcaneal angles in this manner.
Question 16
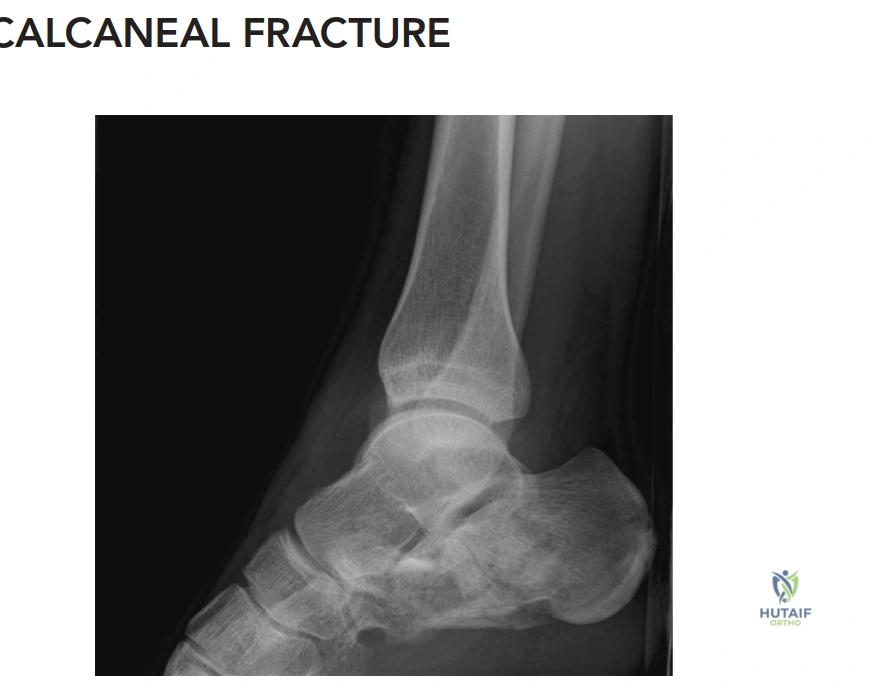
Based on the CT analysis described in the case and the provided coronal CT image of the left calcaneus, what is the most appropriate Sanders classification for this fracture?

Explanation
Correct Answer: D
Explanation:
The case explicitly states, 'The CT analysis of the left calcaneus revealed a highly comminuted posterior facet. The coronal cuts demonstrated three distinct articular fragments with fracture lines located centrally and laterally within the posterior facet, consistent with a Sanders Type IIIBC classification.' The image provided shows two fracture lines through the posterior facet, creating three articular fragments. One fracture line is central (B) and the other is lateral (C), with the medial fragment (A) remaining attached to the sustentaculum. This precisely matches the definition of a Sanders Type IIIBC fracture.
Incorrect Options:
- A. Sanders Type I: Type I fractures are non-displaced articular fractures. This fracture is clearly displaced and comminuted.
- B. Sanders Type IIA: Type II fractures are two-part articular fractures (one fracture line). This fracture has two fracture lines and three fragments.
- C. Sanders Type IIIAB: Type IIIAB would indicate two fracture lines, one medial (A) and one central (B), creating three fragments. The case and image show central (B) and lateral (C) fracture lines.
- E. Sanders Type IV: Type IV fractures are highly comminuted, four-part articular fractures. While this fracture is comminuted, the description and image specifically identify three distinct articular fragments, not four.
Question 17
The case describes the patient's fracture as a 'tongue-type variant' according to the Essex-Lopresti classification. What is the defining characteristic that distinguishes a tongue-type calcaneal fracture from a joint depression type?
Explanation
Correct Answer: C
Explanation:
The case clearly defines the Essex-Lopresti classification: 'Tongue Type: The secondary fracture line exits posteriorly through the calcaneal tuberosity. The posterior facet remains attached to the posterior tuberosity fragment.' This distinction is crucial for understanding the fracture morphology and guiding reduction maneuvers.
Incorrect Options:
- A. The presence of significant comminution of the posterior facet: Both tongue-type and joint depression type fractures can have significant posterior facet comminution. This is not the distinguishing feature between the two Essex-Lopresti types.
- B. The secondary fracture line exits superiorly, just posterior to the posterior facet: This describes the joint depression type, not the tongue type. The case explicitly contrasts this with the tongue type.
- D. Involvement of the calcaneocuboid joint with an anterior process fracture: Calcaneocuboid joint involvement can occur with either type but is not the defining characteristic of the Essex-Lopresti classification, which focuses on the posterior aspect of the calcaneus.
- E. The degree of varus deformity of the calcaneal tuberosity: Varus deformity is a common feature of displaced intra-articular calcaneal fractures in general, regardless of whether they are tongue-type or joint depression type.
Question 18
The patient is an active smoker with a 15 pack-year history, and clinical examination revealed a negative wrinkle test on the left hindfoot. Considering the surgical decision-making process for this Sanders IIIBC fracture, what is the MOST appropriate next step regarding the timing of open reduction and internal fixation (ORIF)?
Explanation
Correct Answer: B
Explanation:
The case emphasizes the critical importance of soft tissue status and the patient's smoking history: 'To mitigate the soft tissue risk, surgery must be delayed until the swelling has completely subsided and the "wrinkle test" is positive, typically 10 to 21 days post-injury.' A negative wrinkle test indicates severe interstitial edema, and proceeding with an extensile lateral approach in this state carries an unacceptably high risk of postoperative wound dehiscence and necrosis, especially in a smoker.
Incorrect Options:
- A. Proceed with immediate ORIF to prevent further soft tissue compromise: Immediate ORIF is contraindicated in the presence of severe swelling and a negative wrinkle test due to the high risk of wound complications. Delaying surgery allows for soft tissue recovery.
- C. Perform percutaneous fixation immediately to minimize soft tissue dissection: While percutaneous fixation has a role in some calcaneal fractures, it is generally not suitable for complex Sanders IIIBC fractures requiring anatomical reduction of the posterior facet and restoration of calcaneal morphology. Moreover, even percutaneous approaches carry risks in severely swollen tissues.
- D. Consider primary subtalar arthrodesis due to the high risk of complications: While the patient's smoking history increases complication risk, a primary arthrodesis is typically reserved for severe Type IV fractures or failed ORIF, not as a first-line treatment for a Sanders IIIBC in an active 38-year-old, especially when anatomical reduction is still achievable. The goal is to preserve the joint if possible.
- E. Initiate a course of antibiotics and proceed with ORIF within 24 hours: Antibiotics are not indicated unless there is an open fracture or signs of infection. Proceeding within 24 hours is too early given the soft tissue status and smoking history.
Question 19
During the extensile lateral approach for this calcaneal fracture, the case describes a specific technique for retracting the full-thickness soft tissue flap to minimize microvascular compromise. What is this technique?
Explanation
Correct Answer: C
Explanation:
The case details the specific, meticulous technique for flap retraction: 'To retract the flap without causing crush injury to the microvasculature, self-retaining retractors are strictly avoided. Instead, three 1.6 mm Kirschner wires (K-wires) are driven into the lateral talus, the talar neck, and the cuboid. The full-thickness flap is then gently retracted superiorly and held in place by bending the K-wires over the soft tissue. This technique eliminates continuous point pressure on the flap edges, significantly reducing the risk of postoperative marginal necrosis.'
Incorrect Options:
- A. Using self-retaining retractors to maintain constant tension on the flap: The case explicitly states that self-retaining retractors are 'strictly avoided' due to the risk of crush injury to the microvasculature.
- B. Employing multiple blunt Hohmann retractors placed directly on the bone: While Hohmanns are used in orthopedic surgery, using them for continuous flap retraction in this context can still cause pressure necrosis, and the K-wire technique is specifically highlighted for its gentleness.
- D. Utilizing skin hooks to apply continuous traction to the flap edges: Skin hooks, especially with continuous traction, can cause localized pressure and compromise the delicate flap edges, increasing the risk of necrosis.
- E. Performing a separate medial incision for counter-traction and flap elevation: A separate medial incision is not part of the extensile lateral approach for flap retraction; it would be a different surgical approach entirely, typically used for medial column fractures or specific medial fragment reduction.
Question 20
For this Sanders IIIBC tongue-type calcaneal fracture, the surgical technique outlines a specific sequence for reduction. What is the initial step in reconstructing the calcaneus?
Explanation
Correct Answer: C
Explanation:
The case describes the fracture reduction sequence: '1. Tuberosity Reduction: A 5.0 mm Schanz pin is inserted percutaneously from posterior to anterior into the dense bone of the calcaneal tuberosity fragment. Using this pin as a joystick, axial traction is applied to restore calcaneal length. The tuberosity is then translated medially and rotated out of varus to restore the mechanical axis of the hindfoot.' This establishes the overall length and alignment before addressing the articular surface.
Incorrect Options:
- A. Elevation and provisional fixation of the posterior facet fragments: While crucial, this step follows the initial tuberosity reduction, as the tuberosity provides a stable base for subsequent articular reconstruction.
- B. Reduction of the lateral wall blowout to decompress the subfibular space: Lateral wall reduction is typically performed after the posterior facet has been elevated and provisionally fixed, as the lateral wall often acts as a cortical shell over the cancellous void.
- D. Fixation of the sustentacular fragment to the anterior process: The sustentacular fragment is considered the 'constant' fragment and is used as a reference. Its fixation to the anterior process is not the initial step in the overall calcaneal reconstruction.
- E. Direct reduction of the calcaneocuboid joint: While calcaneocuboid joint involvement is noted, its reduction is usually addressed later in the sequence, often as part of the anterior process fixation, after the main body and subtalar joint are reconstructed.
Question 21
Following provisional reduction of this Sanders IIIBC fracture, a low-profile, anatomically contoured calcaneal perimeter plate is applied. What is the primary biomechanical goal of this plate in the fixation construct?
Explanation
Correct Answer: B
Explanation:
The case states, 'The primary biomechanical goal of the plate is to act as a lateral buttress, maintaining the restored calcaneal height, length, and neutral alignment of the tuberosity, while supporting the elevated posterior facet.' This buttress function is critical for preventing collapse of the reconstructed calcaneus.
Incorrect Options:
- A. To provide dynamic compression across the posterior facet: While lag screws can provide compression, the perimeter plate's primary role is buttressing, not dynamic compression across the articular surface.
- C. To distract the subtalar joint, preventing post-traumatic arthritis: The goal is anatomical reduction and restoration of height, not distraction. Distraction would lead to incongruity.
- D. To neutralize the pull of the Achilles tendon on the tuberosity: While the plate helps maintain tuberosity position, neutralizing Achilles pull is more about the overall stability of the construct and the initial tuberosity reduction, not the primary biomechanical role of the plate itself.
- E. To provide absolute stability to the calcaneocuboid joint only: While the plate extends to the anterior process and helps stabilize the calcaneocuboid joint, its primary role encompasses the entire calcaneal morphology, including height, length, width, and subtalar joint support, not just the calcaneocuboid joint.
Question 22
The patient's smoking history is a significant comorbidity. According to the landmark Buckley trial (JBJS 2002) referenced in the case, how does smoking status impact outcomes following operative intervention for displaced intra-articular calcaneal fractures?
Explanation
Correct Answer: B
Explanation:
The case directly references the Buckley trial: 'The Buckley trial (JBJS 2002), a landmark prospective randomized controlled trial comparing operative versus non-operative management of calcaneal fractures, demonstrated that while young, healthy, non-workers' compensation patients had significantly better outcomes with surgery, patients who smoked or were receiving workers' compensation had outcomes that were not significantly different from, or were worse than, those managed non-operatively. Furthermore, smokers had a drastically higher rate of wound complications.' This highlights the critical impact of smoking on surgical outcomes and complication rates.
Incorrect Options:
- A. Smokers consistently have significantly better outcomes with surgery due to enhanced bone healing: This is incorrect. Smoking is detrimental to bone healing and significantly increases complication rates.
- C. Smoking primarily affects long-term subtalar joint arthritis rates but not acute wound complications: This is incorrect. Smoking significantly increases the risk of acute wound complications, including marginal flap necrosis and deep infection, as stated in the case.
- D. The Buckley trial found no significant correlation between smoking and surgical outcomes: This is incorrect. The trial found a strong negative correlation, indicating worse outcomes and higher complication rates for smokers.
- E. Smokers require a shorter period of non-weight-bearing post-surgery due to faster soft tissue healing: This is incorrect. Smoking impairs soft tissue healing, necessitating careful postoperative management and often a longer recovery period, not shorter.
Question 23
A 45-year-old male sustains a closed, displaced, intra-articular calcaneus fracture after a fall from a roof. The foot is severely swollen with fracture blisters. The surgeon plans an extensile lateral approach for open reduction and internal fixation. Which of the following is the most reliable clinical indicator that the soft tissue envelope is safe for surgical incision?
Explanation
Question 24
During an extensile lateral approach to the calcaneus, a full-thickness fasciocutaneous flap is developed. To minimize the risk of flap necrosis, the surgeon must preserve the primary blood supply to this flap. Which of the following vessels provides the primary arterial supply to the lateral calcaneal flap?
Explanation
Question 25
A 50-year-old female presents with a closed tongue-type calcaneus fracture. On examination, the skin over the posterior heel is blanched and non-blanching on pressure, though intact. What is the most appropriate initial management?
Explanation
Question 26
A 35-year-old male presents with chronic lateral hindfoot pain 18 months after non-operative management of an intra-articular calcaneus fracture. Clinical exam reveals pain localized inferior to the lateral malleolus. Radiographs show a healed calcaneus fracture with loss of Bohler's angle and a widened hindfoot. What is the most likely cause of his pain?
Explanation
Question 27
A 28-year-old male sustains an ankle injury during a rugby tackle. Radiographs reveal an irreducible fracture-dislocation of the ankle. The lateral radiograph shows the proximal fragment of the fractured fibula entrapped behind the posterior tubercle of the distal tibia. What is the correct eponym for this injury?
Explanation
Question 28
When utilizing the Sanders classification for intra-articular calcaneus fractures, which imaging modality and specific anatomical view/location are required to determine the fracture type?
Explanation
Question 29
A 62-year-old male with long-standing, poorly controlled diabetes mellitus type 2 sustains a displaced bimalleolar equivalent ankle fracture. He undergoes ORIF. Compared to a non-diabetic patient, which modification in postoperative management is most appropriate?
Explanation
Question 30
A 40-year-old construction worker falls 20 feet from scaffolding, landing on both heels. He sustains bilateral intra-articular calcaneus fractures. Which of the following concomitant injuries is most critical to rule out during the primary and secondary surveys?
Explanation
Question 31
A 22-year-old male develops severe foot pain out of proportion to injury following a high-energy calcaneus fracture. Compartment syndrome of the foot is suspected but treated non-operatively due to delayed diagnosis. What is the classic long-term clinical deformity expected from untreated foot compartment syndrome?
Explanation
Question 32
According to the Lauge-Hansen classification, what is the initial anatomical structure to fail in a Pronation-External Rotation (PER) ankle injury?
Explanation
Question 33
A surgeon chooses a sinus tarsi approach instead of an extensile lateral approach for ORIF of a displaced intra-articular calcaneus fracture. Which of the following is the primary established advantage of the sinus tarsi approach?
Explanation
Question 34
A 55-year-old male presents with severe pain and functional limitation two years after an open reduction and internal fixation of a Sanders type IV calcaneus fracture. Radiographs and CT demonstrate end-stage subtalar arthritis, loss of calcaneal height, and decreased talocalcaneal angle. What is the most appropriate surgical intervention?
Explanation
Question 35
A 30-year-old athlete undergoes ORIF for a syndesmotic injury associated with an ankle fracture. Postoperatively, what is the most sensitive and specific imaging modality to assess the accuracy of the syndesmotic reduction?
Explanation
Question 36
A 45-year-old female sustains an ankle fracture. Radiographs demonstrate a transverse fracture of the medial malleolus and a comminuted fracture of the fibula at the level of the syndesmosis. According to the Lauge-Hansen classification, what is the mechanism of injury?
Explanation
Question 37
During open reduction and internal fixation of a medial malleolus fracture, a longitudinal incision is made directly over the medial malleolus. Which neurological structure is most at risk of injury during the superficial dissection in this area?
Explanation
Question 38
A surgeon uses a posterolateral approach to the ankle for fixation of a large posterior malleolus fragment. The surgical interval to access the posterior tibia is developed between which two muscle groups?
Explanation
Question 39
A 28-year-old patient had two cortical screws placed across the syndesmosis for a Maisonneuve fracture. At 10 weeks postoperatively, the patient is asymptomatic but asks about routine removal of the screws before initiating full weight-bearing. Based on current orthopedic literature, what is the recommended management regarding syndesmotic screw removal?
Explanation
Question 40
On a normal lateral radiograph of the calcaneus, Bohler's angle typically ranges from 20 to 40 degrees. Which specific pathoanatomical feature of a calcaneus fracture is primarily responsible for the reduction or flattening of this angle?
Explanation
Question 41
A 32-year-old female sustains a twisting injury to her ankle. Non-weight-bearing radiographs show a distal fibula fracture with an intact medial malleolus. A gravity stress view is obtained. What measurement of the medial clear space on the stress view is generally accepted as diagnostic for deltoid ligament incompetence?
Explanation
Question 42
During ankle fracture surgery, after rigid fixation of the fibula and medial malleolus, the surgeon suspects a syndesmotic injury. An intra-operative 'hook test' (Cotton test) is performed. What is the primary purpose of this test?
Explanation
Question 43
A 65-year-old diabetic female presents with acute posterior heel pain after a low-energy fall. Radiographs demonstrate a displaced avulsion fracture of the calcaneal tuberosity with proximal retraction. The skin overlying the posterior heel is visibly blanched and tense. What is the most appropriate next step in management?

Explanation
Question 44
The Sanders classification for intra-articular calcaneal fractures is based on the number of articular fracture lines extending through the posterior facet. Which of the following imaging modalities and views is strictly utilized to determine this classification?
Explanation
Question 45
Which of the following imaging planes and landmarks is strictly utilized to determine the Sanders classification of an intra-articular calcaneus fracture?
Explanation
Question 46
During an extensile lateral approach for open reduction and internal fixation of a calcaneus fracture, the vertical limb of the incision is placed anterior to the Achilles tendon. Which nerve is at greatest risk of iatrogenic injury if this vertical limb is carried too proximally or carelessly dissected?
Explanation
Question 47
A 24-year-old athlete sustains a severe external rotation ankle injury. Intraoperatively, after rigid fixation of the fibula, a Cotton test demonstrates 4 mm of lateral displacement of the fibula relative to the tibia. What is the most appropriate next step in management?
Explanation
Question 48
A 40-year-old construction worker falls from a ladder and sustains an intra-articular calcaneus fracture. On the lateral radiograph, Bohler's angle is measured at 5 degrees. What does a decreased Bohler's angle primarily indicate in the setting of a calcaneal fracture?
Explanation
Question 49
A 35-year-old woman requires fixation of a large, displaced posterior malleolus fracture via a standard posterolateral approach. The surgeon develops the primary intermuscular plane. What are the key tendinous/muscular boundaries of this surgical interval?
Explanation
Question 50
Which of the following is considered a primary advantage of early functional rehabilitation (early active range of motion) following rigid internal fixation of a bimalleolar ankle fracture in a healthy, compliant patient?
Explanation
Question 51
Which of the following patients presenting with a closed, displaced intra-articular calcaneus fracture is the most appropriate candidate for definitive non-operative management?
Explanation
Question 52
In a high-energy intra-articular calcaneus fracture, which fragment classically remains anatomically aligned with the talus due to strong ligamentous attachments, serving as the 'constant' fragment during surgical reconstruction?
Explanation
Question 53
During open reduction and internal fixation of a transverse medial malleolus fracture, the surgeon elects to use two partially threaded cancellous lag screws. To achieve optimal interfragmentary compression and avoid joint penetration, what is the recommended trajectory of the screws?
Explanation
Question 54
A 42-year-old male presents with persistent lateral hindfoot pain one year after non-operative management of a displaced intra-articular calcaneus fracture. Physical examination reveals focal tenderness just inferior to the lateral malleolus and limited subtalar motion. Radiographs demonstrate a widened calcaneus. Which of the following conditions is the most likely primary source of his focal lateral pain?
Explanation
Question 55
According to the Lauge-Hansen classification, what is the expected sequence of structural failure in a Supination-External Rotation (SER) type IV ankle injury?
Explanation
Question 56
A 38-year-old male sustains a closed intra-articular calcaneus fracture. The foot is massively swollen with multiple clear fracture blisters on presentation. What is the most reliable clinical indicator that the soft tissue envelope has recovered sufficiently to safely permit an extensile lateral surgical approach?
Explanation
Question 57
A 55-year-old patient with poorly controlled diabetes mellitus and peripheral neuropathy sustains an unstable bimalleolar ankle fracture. When planning operative fixation, what modification in surgical technique is most critical to minimize catastrophic postoperative complications?
Explanation
Question 58
A surgeon elects to use a minimally invasive sinus tarsi approach rather than a traditional extensile lateral approach for a Sanders Type II calcaneus fracture. Which of the following represents the primary proven advantage of the sinus tarsi approach?
Explanation
Question 59
Following uncomplicated open reduction and internal fixation of an intra-articular calcaneus fracture, what is the most appropriate initial rehabilitation protocol for the patient, assuming a stable fixation construct and healthy soft tissues?
Explanation
Question 60
A 29-year-old male presents with severe medial ankle pain after a twisting injury playing soccer. Radiographs show a widened medial clear space, but no fractures are visible around the ankle mortise. What is the most critical next step in the clinical and radiographic evaluation?
Explanation
Question 61
A 42-year-old male sustains a high-energy ankle injury. Closed reduction in the emergency department is unsuccessful. Radiographs demonstrate a fracture-dislocation with the proximal fragment of the fractured fibula entrapped posterior to the posterior tubercle of the distal tibia. Which of the following is the most accurate diagnosis and required immediate management?
Explanation
Question 62
A 35-year-old female is scheduled for open reduction and internal fixation of a displaced intra-articular calcaneus fracture via an extensile lateral approach. To minimize the risk of wound edge necrosis, the full-thickness subperiosteal flap must be developed carefully. The vascular supply to the apex of this flap is primarily derived from which of the following arteries?
Explanation
Question 63
A 28-year-old male sustains an ankle fracture involving 30% of the posterior malleolus along with a distal fibula fracture. Biomechanical studies indicate that anatomic reduction and rigid fixation of the posterior malleolus provides superior syndesmotic stability compared to a trans-syndesmotic screw. This stability is primarily achieved through the restoration of which of the following structures?
Explanation
Question 64
A 60-year-old smoker with diabetes presents to the emergency department after a fall from a ladder. Examination reveals a swollen heel with severe posterior skin blanching over the Achilles insertion. Radiographs demonstrate a tongue-type calcaneus fracture with superior displacement of the posterior tuberosity. What is the most appropriate next step in management?
Explanation
Question 65
A 68-year-old patient with long-standing, poorly controlled diabetes mellitus and peripheral neuropathy sustains an unstable bimalleolar ankle fracture. Which of the following modifications to standard surgical and post-operative protocols is most strongly supported by current literature to prevent catastrophic failure?
Explanation
Question 66
A 45-year-old male presents with persistent lateral hindfoot pain and limited ankle dorsiflexion two years after non-operative management of a displaced intra-articular calcaneus fracture. Radiographs show a healed fracture with significant loss of calcaneal height and a flattened Bohler's angle. The limitation in ankle dorsiflexion is most directly caused by which of the following anatomic alterations?
Explanation
Question 67
A 32-year-old patient underwent open reduction and internal fixation of a pronation-external rotation ankle fracture, which included the placement of two quadricortical syndesmotic screws. At 4 months post-operatively, the patient is asymptomatic, has full range of motion, and radiographs show intact hardware. Based on current orthopedic evidence, what is the best recommendation regarding the syndesmotic screws?
Explanation
Question 68
When evaluating a patient with a closed, displaced intra-articular calcaneus fracture, a computed tomography (CT) scan is obtained for pre-operative planning. The Sanders classification system is universally utilized for these fractures. On which specific CT view and anatomic location is the Sanders classification based?
Explanation
Question 69
A 24-year-old gymnast sustains an ankle injury upon landing. Radiographs reveal a transverse fracture of the medial malleolus and a short oblique, comminuted fracture of the fibula exactly at the level of the tibial plafond. According to the Lauge-Hansen classification, what is the mechanism of this injury?
Explanation
Question 70
During open reduction and internal fixation of a calcaneus fracture via an extensile lateral approach, the surgeon places screws directed from lateral to medial to capture the sustentaculum tali fragment. If these screws are overly long and penetrate the medial cortex of the sustentaculum tali, which structure is at highest risk of iatrogenic injury?
Explanation
Question 71
A surgeon opts for a posteromedial approach to directly reduce and fix a displaced posteromedial fragment of the distal tibia (pilon fracture). To safely access this fragment while minimizing neurovascular risk, the deepest dissection interval is typically developed between which of the following structures?
Explanation
Question 72
In the surgical management of displaced intra-articular calcaneus fractures (Sanders Type II and III), recent literature comparing the minimally invasive sinus tarsi approach to the traditional extensile lateral approach demonstrates which of the following relative outcomes?
Explanation
Question 73
A 29-year-old athlete presents with an isolated Weber B distal fibula fracture. A gravity stress radiograph is obtained to evaluate the integrity of the deltoid ligament and syndesmosis. At what threshold of medial clear space widening on the stress radiograph is the deep deltoid ligament considered incompetent, necessitating operative intervention?

Explanation
Question 74
A 55-year-old female sustains a Rowe Type I calcaneal fracture (avulsion of the calcaneal tuberosity) following a trip and fall. The fragment is proximally displaced by 2 cm and the skin overlying the posterior heel is visibly tented but intact. What is the most significant clinical consequence of failing to adequately treat this specific injury pattern?
Explanation
Question 75
A healthy 30-year-old male undergoes rigid open reduction and internal fixation of an uncomminuted, bimalleolar equivalent ankle fracture. The surgeon considers initiating early active range of motion and early weight-bearing (at 2-3 weeks post-operatively) in a controlled fracture boot. According to recent prospective studies, what is the expected outcome of this rehabilitation protocol compared to 6 weeks of non-weight-bearing cast immobilization?
Explanation
Question 76
In the evaluation of a Lauge-Hansen Supination-External Rotation (SER) Type IV ankle injury, understanding the primary stabilizers of the ankle mortise is crucial. Which of the following ligaments acts as the primary restraint to lateral talar excursion?
Explanation
None
