Master ABOS Board Review: Deformity Correction, Arthroplasty & Pediatric Orthopedics | Part 12

Key Takeaway
ABOS Orthopedic Board Review Part 12 covers advanced principles of limb deformity correction, including guided growth, osteotomies, and external fixation. It details biomechanics of THR and TKR, LLD prediction (Shapiro, Moseley), and pediatric conditions like SCFE and Perthes disease, emphasizing Paley's rules and surgical planning for complex cases.
Master ABOS Board Review: Deformity Correction, Arthroplasty & Pediatric Orthopedics | Part 12
Comprehensive 100-Question Exam
00:00
Start Quiz
Question 1
When planning a deformity correction, an osteotomy is performed at a level different from the center of rotation of angulation (CORA), but the mechanical axis is aligned using the CORA as the hinge point. What is the expected geometric outcome according to established osteotomy rules?
Explanation
Question 2
A 45-year-old active male underwent a total hip arthroplasty with a ceramic-on-ceramic bearing. Two years postoperatively, he complains of an audible squeaking sound from the hip during deep flexion. What is the most common mechanical etiology for this phenomenon?
Explanation
Question 3
An 11-year-old obese male presents with acute severe groin pain and inability to bear weight on his right leg after a minor fall. Radiographs reveal an unstable slipped capital femoral epiphysis (SCFE). Which of the following interventions has the highest risk of causing avascular necrosis (AVN) of the femoral head in this setting?
Explanation
Question 4
During treatment of a complex tibial deformity with a hexapod circular external fixator, the surgeon notes a residual varus and procurvatum deformity after completing the initial correction schedule. What is the most appropriate next step to correct the residual deformity?
Explanation
Question 5
During a primary total knee arthroplasty in a patient with a severe, unyielding 20-degree varus deformity, what is the widely accepted standard sequence for sequential medial soft tissue release?
Explanation
Question 6
A 5-month-old female with developmental dysplasia of the hip (DDH) has been treated in a Pavlik harness for 4 weeks. Ultrasound demonstrates continued complete dislocation of the left hip with no signs of reduction. What is the most appropriate next step in management?
Explanation
Question 7
A newborn is diagnosed with Proximal Focal Femoral Deficiency (PFFD). Radiographs demonstrate absence of the proximal femur, but an MRI confirms a cartilaginous connection between the present femoral head and the femoral shaft. According to the Aitken classification, this represents which class, and what is the typical long-term functional procedure if a severe leg-length discrepancy is expected?
Explanation
Question 8
A 55-year-old female with a metal-on-metal total hip arthroplasty presents with groin pain and a palpable mass 6 years postoperatively. Aspiration yields thick, dark fluid with a low nucleated cell count. MRI shows a large periarticular cystic collection. Histology of this tissue would most likely demonstrate:
Explanation
Question 9
Which of the following radiographic findings in Legg-Calvé-Perthes disease is considered one of Catterall's 'head-at-risk' signs, indicating a potentially poorer prognosis?
Explanation
Question 10
When applying an Ilizarov circular frame for tibial lengthening, which frame modification most effectively increases the axial stiffness of the construct?
Explanation
Question 11
During a primary total knee arthroplasty, the surgeon inadvertently places the femoral component in 5 degrees of internal rotation. What is the most likely biomechanical consequence of this specific error?
Explanation
Question 12
In the Ponseti method for the treatment of idiopathic clubfoot, what is the strictly required sequence of deformity correction during serial casting?
Explanation
Question 13
A 12-year-old boy presents with a proximal tibial deformity. Radiographic analysis reveals the center of rotation of angulation (CORA) is located at the level of the physis. To prevent growth arrest, the surgeon plans to perform a diaphyseal osteotomy distal to the CORA. To fully correct the mechanical axis without creating a secondary translation deformity, where should the hinge axis be placed?
Explanation
Question 14
A 14-year-old obese male presents with acute onset of severe hip pain and inability to bear weight. Radiographs confirm an unstable slipped capital femoral epiphysis (SCFE). He undergoes urgent in situ single-screw fixation. Which of the following complications is most highly associated with this specific presentation?
Explanation
Question 15
During a primary total knee arthroplasty for a patient with a severe fixed varus deformity, the surgeon removes medial osteophytes and releases the deep medial collateral ligament, but the medial compartment remains significantly tight in extension. Which structure should typically be sequentially released next to balance the extension gap?
Explanation
Question 16
A 4-year-old girl is diagnosed with developmental dysplasia of the hip (DDH). Radiographs demonstrate an acetabular index of 40 degrees with anterolateral acetabular deficiency. The surgeon decides to perform a Pemberton osteotomy. What is the primary hinge point for this specific pelvic osteotomy?
Explanation
Question 17
A 45-year-old highly active male undergoes a total hip arthroplasty using a ceramic-on-ceramic bearing surface. At his 2-year follow-up, he complains of an audible squeaking sound during certain movements. Which of the following factors is most strongly associated with this phenomenon?
Explanation
Question 18
When utilizing a hexapod circular external fixator (e.g., Taylor Spatial Frame) for complex lower extremity deformity correction, what is its primary biomechanical and software advantage over a traditional Ilizarov frame?
Explanation
Question 19
A 9-year-old girl presents with severe, progressive infantile Blount's disease. Radiographs reveal a Langenskiöld stage VI lesion with a complete medial physeal bar and severe depression of the medial tibial plateau. Which of the following surgical strategies is most appropriate?
Explanation
Question 20
During a total knee arthroplasty for a patient with a severe fixed valgus deformity, the surgeon plans a lateral soft tissue release. To avoid iatrogenic injury, what structure must be carefully protected during the release of the posterolateral capsule and popliteus tendon?
Explanation
Question 21
An infant with a severe idiopathic clubfoot is being treated with the Ponseti method of serial casting. The physician is manipulating the foot to correct the sequence of deformities. What is the final deformity to be corrected, often requiring a percutaneous tenotomy?
Explanation
Question 22
In distraction osteogenesis for limb lengthening, a latency period is strictly observed before starting distraction. Following latency, what is the generally accepted optimal rate and rhythm of distraction to promote high-quality bone regenerate while preventing premature consolidation?
Explanation
Question 23
A 6-year-old boy is diagnosed with Legg-Calvé-Perthes disease. Which of the following radiographic classifications is most reliable for determining the long-term prognosis and likelihood of a spherical femoral head?
Explanation
Question 24
A surgeon is performing a primary total hip arthroplasty using the direct anterior approach (Smith-Petersen). The superficial internervous plane lies between which two muscles?
Explanation
Question 25
In deformity correction principles, if an osteotomy is performed at a level different from the Center of Rotation of Angulation (CORA), but the hinge is placed exactly at the CORA, what is the geometric result of the correction?
Explanation
Question 26
According to the 2018 International Consensus Meeting (ICM) criteria, which of the following is considered a major criterion for the diagnosis of chronic periprosthetic joint infection (PJI)?
Explanation
Question 27
A 2-year-old child presents with bilateral genu varum. Radiographs reveal a metaphyseal-diaphyseal angle (MDA) of 18 degrees bilaterally. Which of the following is the most appropriate management?
Explanation
Question 28
What is the primary advantage of the 'lengthening over a nail' (LON) technique compared to traditional Ilizarov lengthening?
Explanation
Question 29
During a total knee arthroplasty, trial reduction reveals that the knee is tight in full extension but appropriately balanced in 90 degrees of flexion. Which of the following is the most appropriate next step to balance the knee?
Explanation
Question 30
Which of the following findings is the most reliable determinant of 'instability' in a slipped capital femoral epiphysis (SCFE) according to the Loder classification?
Explanation
Question 31
In distraction osteogenesis of the tibia, what is the primary physiological rationale for maintaining a latency period of 7 to 10 days prior to initiating distraction?
Explanation
Question 32
A 72-year-old female sustains a periprosthetic femur fracture around her cementless total hip arthroplasty. Radiographs show a fracture at the tip of the stem. The stem is radiographically loose, but she has excellent proximal bone stock. According to the Vancouver classification, what is the most appropriate treatment?
Explanation
Question 33
During the Ponseti method for correcting idiopathic clubfoot, the cavus deformity must be addressed first. Which of the following describes the correct initial manipulation?
Explanation
Question 34
When planning an opening wedge osteotomy to correct an angular deformity, placing the hinge on the convex cortex precisely at the level of the Center of Rotation of Angulation (CORA) will result in:
Explanation
Question 35
A patient with a ceramic-on-ceramic total hip arthroplasty complains of a new-onset audible 'squeaking' during walking. Radiographic evaluation is most likely to show which of the following component positions?
Explanation
Question 36
According to the Herring Lateral Pillar Classification for Legg-Calvé-Perthes disease, a patient whose lateral pillar height is maintained at 40% of its normal height falls into which group, and what is the general prognosis?
Explanation
Question 37
When utilizing a hexapod external fixator (e.g., Taylor Spatial Frame) for deformity correction, the concept of 'chronic' parameters primarily refers to:
Explanation
Question 38
According to Paley's osteotomy rules, if the osteotomy and the hinge of the correction are both located at the Center of Rotation of Angulation (CORA), what is the resultant effect on the mechanical axis?
Explanation
Question 39
A 65-year-old patient presents with end-stage knee osteoarthritis and a 25-degree extra-articular diaphyseal varus deformity of the femur. What is the most appropriate management?
Explanation
Question 40
In the Ponseti method for clubfoot casting, which of the following represents the correct sequential order of deformity correction?
Explanation
Question 41
When planning a deformity correction, if the osteotomy is performed at a level different from the CORA but the hinge remains exactly at the CORA, what is the expected outcome according to Paley's Rule 2?
Explanation
Question 42
A 45-year-old female with developmental dysplasia of the hip (DDH) Crowe type IV undergoes a total hip arthroplasty. To safely reduce the hip to the true acetabulum and minimize the risk of sciatic nerve palsy, which surgical maneuver is most frequently required?
Explanation
Question 43
Which patient with Legg-Calvé-Perthes disease would show the most significant radiographic benefit from a surgical containment procedure (e.g., proximal femoral or pelvic osteotomy)?
Explanation
Question 44
In a medial opening wedge high tibial osteotomy (HTO) for a varus knee, how does the correction typically alter the sagittal plane alignment if the anterior and posterior gaps are opened equally?
Explanation
Question 45
A 12-year-old obese male presents with acute-on-chronic hip pain and inability to bear weight. Radiographs show a severe slipped capital femoral epiphysis (SCFE). Intraoperatively, a capsulotomy is performed before pinning. What is the primary rationale for this capsulotomy?
Explanation
Question 46
A 72-year-old woman with a history of a malunited midshaft femur fracture (30 degrees of apex anterior bowing) presents for a total knee arthroplasty (TKA). If standard intra-articular cuts are used, which adjustment to the distal femoral cut is required to avoid anterior notching and knee component hyperextension?
Explanation
Question 47
You are evaluating a 2-year-old with infantile tibia vara (Blount's disease). During radiographic follow-up, which finding according to the Langenskiöld classification indicates an irreversible physeal injury that typically requires surgical intervention?
Explanation
Question 48
When performing an extensive external fixation lengthening of the tibia, what is the most common adjacent joint complication that often necessitates extending the frame across the joint?
Explanation
Question 49
A 6-year-old child weighing 25 kg sustains a completely displaced, isolated diaphyseal femur fracture. What is the standard of care for definitive surgical fixation?
Explanation
Question 50
A patient with a significant post-traumatic valgus deformity of the proximal tibia is undergoing a primary TKA. Through a standard medial parapatellar arthrotomy, which structure is most commonly released first to balance the fixed valgus knee?
Explanation
Question 51
A 10-year-old child is treated with eight-Plates (tension band constructs) for bilateral genu valgum. Eighteen months later, the deformity is fully corrected, and the hardware is removed. The parents should be counseled on which common post-removal phenomenon?
Explanation
Question 52
During a femoral lengthening procedure utilizing the Lengthening Over a Nail (LON) technique, what is the primary advantage compared to lengthening with an external fixator alone?
Explanation
Question 53
According to the principles of deformity correction, if an opening wedge osteotomy is performed with the axis of the hinge placed exactly at the Center of Rotation of Angulation (CORA), which of the following best describes the resulting correction?
Explanation
Question 54
A 65-year-old patient with a 25-degree coronal plane extra-articular bowing deformity of the midshaft femur presents for a Total Knee Arthroplasty. Which of the following is the most appropriate management?
Explanation
Question 55
An infant with developmental dysplasia of the hip (DDH) is being treated with a Pavlik harness. During a follow-up visit, the parents report the infant is not kicking the affected leg. Examination reveals lack of knee extension. Which of the following harness adjustments is required?
Explanation
Question 56
A 4-year-old girl with severe infantile Blount's disease undergoes a proximal tibial osteotomy. During preoperative planning, you note Langenskiöld stage V changes. What additional procedure is most commonly required in this stage compared to stage II?
Explanation
Question 57
A 13-year-old obese male presents to the ED with a 2-day history of severe left hip pain and inability to bear weight. Radiographs demonstrate a Slipped Capital Femoral Epiphysis (SCFE). Which of the following factors best defines this as an 'unstable' SCFE?
Explanation
Question 58
During a total hip arthroplasty for a patient with Crowe IV developmental dysplasia of the hip, a subtrochanteric shortening osteotomy is planned. Which nerve is at the highest risk of injury during the reduction of the hip into the true acetabulum?
Explanation
Question 59
A 55-year-old female with a metal-on-metal total hip arthroplasty presents with groin pain and a pseudotumor. Histological examination of the periprosthetic tissue is most likely to reveal which of the following?
Explanation
Question 60
A 7-year-old child presents with a 'gunstock' deformity of the right elbow following a supracondylar humerus fracture treated conservatively 2 years ago. The deformity is primarily caused by malunion in which plane?
Explanation
Question 61
When applying the Ponseti method for the treatment of idiopathic clubfoot, what is the correct sequence of deformity correction?
Explanation
Question 62
During a Total Knee Arthroplasty in a patient with a severe fixed varus deformity, what is the standard sequential soft tissue release performed on the medial side?
Explanation
Question 63
A 15-year-old male is undergoing femoral lengthening with a unilateral external fixator. If the bone is lengthened along the anatomical axis of the femur rather than the mechanical axis, what secondary deformity will be induced?
Explanation
Question 64
According to Rule 2 of deformity correction, if an osteotomy is performed at a level different from the CORA, but the axis of the hinge is placed exactly at the CORA, what is the geometric result?
Explanation
Question 65
A 70-year-old patient presents with a painful total knee arthroplasty 3 years postoperatively. Joint aspiration yields synovial fluid with a WBC count of 4,500 cells/uL and 85% PMNs. According to the MSIS criteria, how should this be interpreted?
Explanation
Question 66
When placing the acetabular component during a Total Hip Arthroplasty, what is the Lewinnek 'safe zone' to minimize the risk of dislocation?
Explanation
Question 67
According to Paley's rules of deformity correction, if an osteotomy and the hinge (axis of rotation) are both placed at a level outside the center of rotation of angulation (CORA), what is the resulting geometric effect on the bone?
Explanation
Question 68
A 64-year-old man presents with a painful swelling in his right groin 5 years after a primary total hip arthroplasty using a titanium stem, cobalt-chromium modular head, and highly cross-linked polyethylene liner. Aspiration yields sterile, cloudy, yellowish fluid. Blood tests reveal elevated serum cobalt levels with normal chromium levels. Which of the following is the most likely source of the problem?
Explanation
Question 69
In a 5-year-old child with spastic quadriplegic cerebral palsy, routine radiographic surveillance shows a Reimers migration percentage of 45% in the left hip. The child is symptomatic with limited hip abduction. Which of the following interventions is most appropriate?
Explanation
Question 70
During a primary total knee arthroplasty, the surgeon evaluates the gaps and finds the knee is well-balanced and stable in extension, but exceptionally tight in 90 degrees of flexion. Which of the following maneuvers is the most appropriate next step to balance the knee?
Explanation
Question 71
A 6-week-old infant is being treated with a Pavlik harness for developmental dysplasia of the hip (DDH). During follow-up, the mother notes the infant has stopped kicking her right leg, and clinical examination reveals decreased active knee extension on that side. Which of the following harness adjustments should have been avoided to prevent this complication?
Explanation
Question 72
A 3-year-old overweight boy presents with progressive bilateral genu varum. Standing radiographs demonstrate an abrupt varus angulation at the proximal medial tibial metaphysis with a metaphyseal-diaphyseal angle (MDA) of 18 degrees. What is the most appropriate management?
Explanation
Question 73
A patient develops patellar subluxation postoperatively following a total knee arthroplasty. On CT scan evaluation, which of the following component malpositions is most likely responsible for lateral patellar maltracking?
Explanation
Question 74
A 10-year-old girl is diagnosed with a unilateral slipped capital femoral epiphysis (SCFE). Which of the following patient profiles represents the strongest indication for prophylactic in situ pinning of the contralateral, asymptomatic hip?
Explanation
Question 75
According to the principles of deformity correction, if the center of rotation of angulation (CORA) is identified, but both the osteotomy and the hinge are placed at a level proximal to the CORA, what is the expected geometric outcome upon alignment of the mechanical axes?
Explanation
Question 76
During a posterior-stabilized total knee arthroplasty, the surgeon notes that the joint is symmetrically balanced in extension but excessively tight in flexion. Which of the following is the most appropriate next step to balance the knee?
Explanation
Question 77
A 7-year-old boy presents with an insidious onset of a painless limp. Radiographs demonstrate fragmentation of the capital femoral epiphysis with exactly 50% maintenance of the lateral pillar height. According to the Herring lateral pillar classification, what is the most appropriate management?
Explanation
Question 78
When constructing a circular external fixator (Ilizarov) for tibial lengthening, which of the following modifications most significantly increases the axial stiffness of the construct?
Explanation
Question 79
A 62-year-old female with a metal-on-polyethylene total hip arthroplasty presents with new-onset groin pain 5 years postoperatively. Radiographs show well-fixed components. Laboratory workup reveals an elevated serum cobalt-to-chromium ratio of 5:1. What is the most likely source of the elevated metal ions?
Explanation
Question 80
During the Ponseti casting treatment for a rigid idiopathic clubfoot in a 4-week-old infant, the midfoot has been fully abducted. The heel varus has resolved, and the forefoot is abducted to 70 degrees. However, ankle dorsiflexion remains at -10 degrees. What is the correct next step in management?
Explanation
Question 81
A patient requires correction of a valgus deformity of the proximal tibia.
To accurately plan the correction, the surgeon must map the normal mechanical axis. Where does the mechanical axis line (MAD) typically fall in relation to the center of the knee joint in a normal patient?
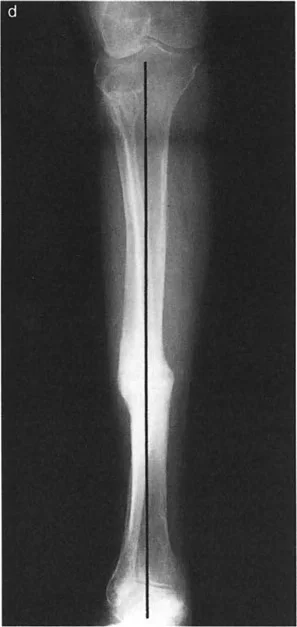
Explanation
Question 82
Which of the following pediatric patients presenting with a unilateral slipped capital femoral epiphysis (SCFE) has the strongest indication for prophylactic in situ pinning of the contralateral hip?
Explanation
Question 83
A 55-year-old male with a metal-on-metal total hip arthroplasty presents with a palpable groin mass and neuropathic pain radiating down the anterior thigh. MARS-MRI demonstrates a large cystic mass. Intraoperatively, the mass shows extensive tissue necrosis and an aseptic lymphocytic infiltrate. This reaction is best classified as:
Explanation
Question 84
When utilizing a hexapod circular frame (e.g., Taylor Spatial Frame) for simultaneous six-axis deformity correction, what does the concept of the "virtual hinge" represent?
Explanation
Question 85
A 2-year-old girl presents with bilateral bowing of the lower extremities.
Radiographs show medial beaking of the proximal tibial metaphysis. Which radiographic measurement is most reliable in differentiating infantile Blount's disease from physiologic genu varum?

Explanation
Question 86
A surgeon is performing a primary total hip arthroplasty utilizing the direct anterior approach. Which two nerves supply the muscles defining the superficial internervous plane of this approach?
Explanation
Question 87
A 15-year-old male presents with a predicted leg length discrepancy of 6.5 cm at skeletal maturity secondary to a physeal arrest of the distal femur. What is the most appropriate definitive management to equalize leg lengths?
Explanation
Question 88
A 6-week-old female infant born in breech presentation undergoes a screening ultrasound for developmental dysplasia of the hip (DDH). The alpha angle is reported as 45 degrees. According to Graf's classification, what is the most appropriate management?
Explanation
Question 89
In lower extremity deformity correction, an osteotomy is planned to correct a significant angular deformity. According to established osteotomy rules, if both the osteotomy cut and the hinge axis are placed away from the Center of Rotation of Angulation (CORA), what is the resultant geometric effect on the bone segments after angular correction?
Explanation
Question 90
An 8-year-old boy is diagnosed with Legg-Calvé-Perthes disease. According to the Herring Lateral Pillar classification, which of the following radiographic findings places him in Group C and predicts the poorest long-term prognosis?
Explanation
Question 91
A 62-year-old female presents with groin pain and a palpable anterior mass 6 years after a metal-on-polyethylene total hip arthroplasty utilizing a large-diameter cobalt-chromium femoral head on a titanium stem. Blood tests reveal elevated serum cobalt levels with normal chromium levels. What is the most likely etiology of her symptoms?
Explanation
Question 92
A 6-week-old infant with developmental dysplasia of the hip is being treated with a Pavlik harness. During a follow-up visit, the parents report the child has stopped actively extending the knee on the treated side. What is the most appropriate next step in management?
Explanation
Question 93
A 4-year-old girl presents with progressive genu varum. Radiographs demonstrate a sharp varus angulation at the proximal tibial metaphysis with a metaphyseal-diaphyseal angle of 18 degrees and profound medial physeal depression. She is diagnosed with infantile Blount's disease (Langenskiold stage III). What is the most appropriate management?
Explanation
Question 94
During a cruciate-retaining total knee arthroplasty, the surgeon finds that the knee is well balanced and symmetric in full extension, but tight symmetrically in 90 degrees of flexion. Which of the following is the most appropriate intervention to balance the knee?
Explanation
Question 95
A 13-year-old boy with a BMI of 38 presents with a stable slipped capital femoral epiphysis (SCFE) of the left hip. Routine preoperative blood work reveals untreated hypothyroidism. After in situ pinning of the left hip, what is the most appropriate recommendation regarding the right hip?
Explanation
Question 96
A 24-year-old male is undergoing femoral lengthening over a nail (LON) using a monoplanar external fixator. During the consolidation phase after achieving 4 cm of length, the fixator is removed prematurely before the intramedullary nail is proximally locked. What is the most likely complication?
Explanation
Question 97
A 72-year-old female sustains a fall 5 years after an uncemented total hip arthroplasty. Radiographs show a spiral periprosthetic femur fracture occurring around the stem. The stem is visibly subsided by 1 cm compared to previous films, but there is excellent bone stock proximally and distally. What is the appropriate Vancouver classification and standard treatment?
Explanation
Question 98
A 14-year-old boy is undergoing complex multiplanar tibial deformity correction using a hexapod circular external fixator. Midway through the strut adjustment schedule, orthogonal radiographs demonstrate that angular correction is proceeding appropriately, but a new unintended 5 mm medial translation has developed at the osteotomy site. What is the most appropriate management?

Explanation
Question 99
A 68-year-old male presents with inability to perform a straight leg raise 3 months following a primary total knee arthroplasty. Ultrasound confirms a complete avulsion of the patellar tendon from the tibial tubercle. Given the chronic nature of the tear and poor native tissue quality, reconstructive surgery is planned. Which of the following techniques provides the most reliable long-term functional outcome?
Explanation
Question 100
A 5-year-old girl is evaluated for a congenital femoral deficiency. Her current absolute femoral length discrepancy is 3 cm. Using the Paley multiplier method to estimate her discrepancy at skeletal maturity, which specific patient demographic factor is strictly required to select the correct multiplier coefficient?
Explanation
None
