Adult Acquired Flatfoot Reconstruction: FDL Transfer & Medial Displacement Calcaneal Osteotomy Masterclass
Key Takeaway
This masterclass details the surgical management of adult acquired flatfoot deformity with flexor digitorum longus (FDL) transfer and medial displacement calcaneal osteotomy. We cover comprehensive anatomy, meticulous preoperative planning, and a granular, step-by-step intraoperative execution, emphasizing critical pearls, potential pitfalls, and robust postoperative rehabilitation strategies for optimal patient outcomes.
Introduction and Epidemiology
The posterior tibial tendon undergoes tearing and degeneration, and as it fails, the foot falls into a planovalgus configuration. Posterior tibial tendon dysfunction (PTTD), increasingly referred to in contemporary literature as Progressive Collapsing Foot Deformity (PCFD), is the most common cause of an adult acquired flatfoot deformity. The medial displacement calcaneal osteotomy (MDCO) serves as a workhorse skeletal procedure to restore hindfoot alignment and protect soft-tissue reconstructions in flexible deformities.

Most cases occur spontaneously without known antecedent trauma. Women are much more commonly affected than men, with a typical age range older than 50 years. With time, a rigid deformity develops. The degree and flexibility of the deformity play a key role in determining treatment, specifically dictating whether joint-sparing osteotomies like the MDCO are viable or if arthrodesis is mandated.

Dysfunction of the posterior tibialis is thought to be the initiating event in the collapse of the arch. Early in the course of the disease, pain along the course of the posterior tibialis or weakness of its function will be present without any arch collapse. This is classified as stage I disease. With time, a planovalgus foot deformity develops. Initially, this deformity is flexible and is classified as stage II disease. A fixed deformity eventually results, classified as stage III disease. The first component of the deformity to become fixed is usually an elevation of the first ray relative to the fifth ray. This is the result of a compensation of the forefoot for the hindfoot valgus and is defined as a fixed forefoot varus. Later, the valgus alignment of the calcaneus through the subtalar joint becomes contracted and irreducible. Rarely, a secondary failure of the deltoid ligament along the medial aspect of the hindfoot develops as the mechanical stresses placed on it by the flattened arch increase, culminating in a stage IV deformity.
Surgical Anatomy and Biomechanics
The posterior tibialis typically degenerates in an area underneath the medial malleolus and distally to its insertion. The process is not inflammatory but is rather characterized by replacement of the normal collagen fibers with amorphous scar and mucinous degeneration.

As the arch falls, the hindfoot will fall into valgus relative to the leg, whereas the forefoot will abduct through the talonavicular joint. Uncovering of the talar head results as the forefoot pivots laterally. The sag of the arch and the abduction of the forefoot can be described in terms of the loss of alignment of the first metatarsal and the talus. The long axes of these bones should normally be colinear (Meary's line). A sag of the arch is seen by an angulation in this line on the standing lateral radiograph, whereas abduction of the forefoot is seen by lateral angulation of this line on the anteroposterior view.

In most cases, the cause of PTTD is unknown and is not associated with a clear antecedent trauma. The collapse of the arch is the result of a tendon imbalance. The antagonists to the posterior tibialis are the peroneals (peroneus brevis and longus), and they must be functional for the deformity to develop. A single study has suggested a correlation of PTTD with the human leukocyte antigen B27 genotype, typically associated with seronegative arthropathies. Cumulative mechanical factors likely play a role in the development of the disorder; a preexisting planovalgus deformity presumably places extra stress on the tendon and is thought to be a risk factor for degeneration. The presence of an accessory navicular ossicle within the tendon substance at its insertion into the medial pole of the navicular is also a risk factor for tendon degeneration, likely from local mechanical stress.

Biomechanical Rationale for Medial Displacement Calcaneal Osteotomy
The primary biomechanical goal of the MDCO is to correct the valgus thrust of the hindfoot by shifting the mechanical axis of the calcaneus medially. In a normal foot, the Achilles tendon inserts slightly medial to the axis of the subtalar joint, acting as a primary plantarflexor and a secondary hindfoot invertor. In the planovalgus foot, the calcaneus everts, shifting the insertion of the Achilles tendon lateral to the subtalar joint axis. This pathologic shift converts the powerful gastrocnemius-soleus complex into a hindfoot evertor, exacerbating the deformity with every step.
By performing a transverse osteotomy of the calcaneal tuberosity and translating the posterior fragment medially (typically 8 to 10 millimeters), the Achilles tendon insertion is repositioned medial to the subtalar axis. This restores its function as a hindfoot invertor, neutralizes the deforming valgus force, and protects the medial soft tissue reconstruction (such as the flexor digitorum longus transfer and spring ligament repair) from excessive tension.
Indications and Contraindications
The medial displacement calcaneal osteotomy is primarily indicated for flexible adult acquired flatfoot deformity, specifically Stage II PTTD. It is rarely performed in isolation; it is almost universally combined with soft tissue procedures (flexor digitorum longus tendon transfer) and often with other bony procedures (Cotton osteotomy, lateral column lengthening) depending on the specific multiplanar components of the deformity.

A rigid deformity (Stage III) is an absolute contraindication for a joint-sparing osteotomy like the MDCO. Attempting to correct a rigid subtalar joint with an extra-articular osteotomy will fail to restore alignment and will lead to persistent pain and hardware failure. In such cases, arthrodesis (subtalar, talonavicular, or triple arthrodesis) is required.

Operative Versus Non Operative Management
| Management Strategy | Indications | Modalities and Procedures |
|---|---|---|
| Non-Operative | Stage I disease; Early Stage II disease; Poor surgical candidates (severe medical comorbidities, non-ambulatory). | High-top lace-up orthotics (Arizona brace); Custom UCBL inserts; Physical therapy (eccentric strengthening); NSAIDs. |
| Operative (Joint-Sparing) | Stage IIa and IIb flexible deformities; Failure of 3-6 months of conservative management. | Medial Displacement Calcaneal Osteotomy (MDCO); FDL transfer; Spring ligament repair; Achilles lengthening; Cotton osteotomy. |
| Operative (Arthrodesis) | Stage III (rigid hindfoot); Severe subtalar or talonavicular osteoarthritis; Stage IV (deltoid failure with ankle valgus). | Subtalar arthrodesis; Triple arthrodesis; Tibiotalocalcaneal (TTC) arthrodesis for Stage IV. |
Pre Operative Planning and Patient Positioning
Thorough clinical evaluation is paramount. Most, but not all, patients present with pain along the medial arch. In some cases, lateral impingement develops as the valgus posture of the hindfoot becomes extreme. The calcaneus impinges against the inferior tip of the lateral malleolus, causing severe lateral pain that can overshadow the medial tendon pain.

The physical examination must assess the flexibility of the hindfoot. The single heel rise test is the hallmark clinical assessment. A patient with normal posterior tibial tendon function will invert the hindfoot when rising onto the toes. In Stage II disease, the patient may be able to perform a single heel rise, but the hindfoot will remain in valgus. In advanced stages, the patient cannot perform the maneuver at all. The Silfverskiöld test must be performed to evaluate for isolated gastrocnemius contracture versus Achilles tendon contracture, as addressing the equinus contracture is a mandatory component of the surgical reconstruction.

Radiographic Evaluation
Standard weight-bearing radiographs of the foot and ankle (anteroposterior, lateral, and mortise views) are required. A Harris heel view is highly beneficial to quantify the degree of hindfoot valgus.
Key radiographic parameters to evaluate include:
* Talonavicular Uncoverage: Measured on the AP view; greater than 30% uncoverage indicates significant forefoot abduction.
* Meary's Angle: The angle between the longitudinal axis of the talus and the first metatarsal on the lateral view.
* Calcaneal Pitch: Often decreased in planovalgus deformities.
* Talo-calcaneal Angle (Kite's Angle): Increased on the AP view in flatfoot deformities.

Patient Positioning
The patient is typically placed in the supine position on a radiolucent operating table. A large bump is placed under the ipsilateral hip to internally rotate the leg, bringing the lateral aspect of the hindfoot into clear view for the MDCO. This bump can be removed later in the case when the surgeon transitions to the medial side of the foot for the flexor digitorum longus transfer and spring ligament repair. A thigh tourniquet is applied to provide a bloodless surgical field. Fluoroscopy must be readily available and positioned to allow for intraoperative axial, AP, and lateral imaging of the hindfoot.
Detailed Surgical Approach and Technique
The surgical sequence for Stage II flatfoot reconstruction typically follows a specific order: 1) Equinus correction (gastrocnemius recession or Achilles lengthening), 2) Medial Displacement Calcaneal Osteotomy, 3) Medial soft tissue reconstruction (FDL transfer), and 4) Medial column stabilization (Cotton osteotomy) if residual forefoot supination exists.

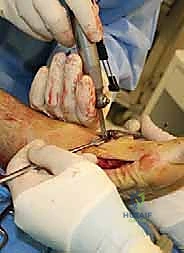
Incision and Dissection
The approach for the MDCO utilizes an oblique incision on the lateral aspect of the calcaneus. The incision is approximately 4 to 5 centimeters long, oriented parallel and just posterior to the peroneal tendons, extending from the superior aspect of the calcaneal tuberosity angling inferiorly toward the plantar aspect of the heel.

Careful subcutaneous dissection is critical to avoid injury to the sural nerve, which typically courses just anterior and superior to the incision but often has branching patterns that cross the surgical field. The lesser saphenous vein should be identified and protected or ligated. The periosteum over the lateral wall of the calcaneus is incised in line with the skin incision. Subperiosteal flaps are elevated anteriorly and posteriorly to expose the lateral wall of the calcaneus. Retractors are placed superiorly to protect the peroneal tendons and inferiorly to protect the plantar fascia and neurovascular structures.

Osteotomy Execution
Using a sagittal saw, the osteotomy is initiated on the lateral calcaneal wall. The cut is oriented perpendicular to the lateral wall of the calcaneus and angled approximately 45 degrees relative to the plantar surface of the foot. The trajectory should aim just posterior to the posterior facet of the subtalar joint to avoid intra-articular penetration.

The saw blade is advanced through the cancellous bone of the calcaneal body. It is imperative to stop the saw blade just short of the medial cortex. Plunging through the medial cortex with the saw risks catastrophic injury to the tibial neurovascular bundle, the flexor hallucis longus, and the flexor digitorum longus tendons. The medial cortex is instead carefully breached using a broad osteotome. The osteotome is gently levered to complete the osteotomy and mobilize the posterior tuberosity fragment.

Medial Displacement and Translation
Once the osteotomy is complete and the posterior fragment is fully mobile, the tuberosity is translated medially. This is typically achieved by inserting a lamina spreader or a smooth periosteal elevator into the osteotomy site to glide the posterior fragment medially along the osteotomy plane. The required translation is generally 8 to 10 millimeters, or approximately one-third to one-half the width of the calcaneus.

The surgeon must ensure that the fragment translates purely medially without unwanted dorsal or plantar translation, or varus/valgus tilting, unless intentionally modifying the pitch. A temporary stout Kirschner wire (K-wire) is driven from the posterior inferior aspect of the tuberosity, across the osteotomy site, and into the anterior calcaneal body to hold the reduction. Intraoperative fluoroscopy (lateral and Harris heel views) is utilized to confirm the medial shift, ensure the subtalar joint has not been violated, and verify that the hardware trajectory is appropriate.

Hardware Fixation
Definitive fixation of the MDCO is most commonly achieved with one or two large-fragment cannulated screws (6.5 mm or 7.0 mm). The screws are placed from the posterior-inferior heel, directed anteriorly, superiorly, and slightly laterally into the dense bone of the anterior calcaneus or the subchondral bone of the posterior facet.

Alternatively, specialized calcaneal step-plates can be utilized. These plates are applied to the lateral wall and feature a pre-contoured step (typically 8mm or 10mm) that inherently holds the medialized position of the tuberosity. Plate fixation can provide robust rotational stability and may reduce the incidence of symptomatic hardware at the posterior heel, which is a known complication of screw fixation.
Adjunctive Procedures
The MDCO addresses only the hindfoot valgus component of the PCFD. Comprehensive reconstruction requires addressing all components of the deformity:
* Flexor Digitorum Longus (FDL) Transfer: The diseased posterior tibial tendon is excised, and the FDL is harvested and transferred into the navicular to restore active inversion and support the medial arch.
* Spring Ligament Repair: The superomedial calcaneonavicular ligament is often attenuated or torn and must be imbricated or repaired with suture anchors.
* Medial Column Stabilization (Cotton Osteotomy): After hindfoot valgus is corrected, a residual fixed forefoot supinatus may become apparent. If the first ray does not rest on the floor when the hindfoot is reduced, an opening wedge osteotomy of the medial cuneiform (Cotton osteotomy) is performed to plantarflex the first ray.
* Gastrocnemius Recession / Achilles Lengthening: Essential to address the equinus contracture, which forces the midfoot to break down during the stance phase of gait.
Complications and Management
While the MDCO is highly effective, it carries a distinct complication profile. Careful surgical technique and appropriate patient selection mitigate these risks, but surgeons must be prepared to manage them.

Sural nerve injury is one of the most frequently reported complications, presenting as numbness, paresthesias, or painful neuromas along the lateral foot. The nerve is at risk during the initial incision, during retraction, and from hardware placement.

Symptomatic hardware is also common, particularly when large headed screws are used at the posterior heel. The thin soft tissue envelope over the posterior calcaneus makes screw heads prone to irritation from footwear.

Common Complications and Salvage Strategies
| Complication | Estimated Incidence | Etiology / Risk Factors | Management and Salvage Strategies |
|---|---|---|---|
| Sural Nerve Neuritis / Neuroma | 5% - 15% | Direct laceration, stretch injury from retraction, or entrapment in scar tissue. | Initial: Gabapentinoids, desensitization, targeted steroid injections. Salvage: Surgical exploration, neurolysis, or neurectomy with proximal burying in muscle. |
| Symptomatic Hardware | 10% - 20% | Prominent screw heads at the posterior heel; thin soft tissue envelope. | Conservative: Shoe wear modification, heel padding. Operative: Hardware removal after radiographic confirmation of complete bony union (typically > 6 months). |
| Delayed Union / Nonunion | 1% - 3% | Smoking, diabetes, poor fixation, thermal necrosis from saw blade. | Prolonged immobilization, bone stimulators. Surgical revision with bone grafting and robust plate fixation if nonunion is symptomatic and persistent. |
| Overcorrection (Varus Hindfoot) | < 5% | Excessive medial translation (>10-12mm); failure to recognize rigid components. | A rigid varus hindfoot is highly symptomatic. Salvage requires revision osteotomy (lateralizing calcaneal osteotomy) or subtalar arthrodesis. |
| Undercorrection (Persistent Valgus) | 5% - 10% | Insufficient medial shift; failure to address severe forefoot abduction or medial column instability. | Orthotics bracing. If symptomatic, revision surgery may require lateral column lengthening (Evans osteotomy) or subtalar fusion. |
Post Operative Rehabilitation Protocols
Rehabilitation following an MDCO and associated soft tissue reconstructions is prolonged and requires strict adherence to biomechanical offloading to allow both bony union and tendon healing.

Phase 1: Maximum Protection (Weeks 0-6)
The patient is placed in a well-padded short leg splint in the operating room. The foot is typically immobilized in slight plantarflexion and inversion to remove tension from the FDL transfer and spring ligament repair. The patient is strictly non-weight-bearing. At 2 weeks, sutures are removed, and the patient is transitioned to a short leg cast or a locked controlled ankle motion (CAM) boot, continuing strict non-weight-bearing precautions.
Phase 2: Progressive Loading (Weeks 6-12)
Radiographs are obtained at 6 weeks to assess early callus formation at the osteotomy site. If clinical and radiographic healing is progressing appropriately, the patient is transitioned to a CAM boot and allowed to begin progressive partial weight-bearing, advancing to full weight-bearing as tolerated. Active and active-assisted range of motion exercises for the ankle and subtalar joints are initiated. Inversion and eversion strengthening are delayed to protect the tendon transfer.
Phase 3: Strengthening and Proprioception (Weeks 12+)
The patient transitions from the CAM boot to supportive athletic shoes, often with a custom orthotic or an over-the-counter arch support. Physical therapy focuses on aggressive calf stretching, eccentric strengthening of the posterior tibialis/FDL complex, and proprioceptive retraining. Return
Clinical & Radiographic Imaging























You Might Also Like
