Lower Extremity Deformity Correction & TKA Biomechanics for ABOS Board Review | Part 4

Key Takeaway
Lower extremity deformity correction involves restoring a neutral mechanical axis and balanced joint lines. Utilizing Paley's principles, surgeons identify the Center of Rotation of Angulation (CORA) and apply specific osteotomy rules or TKA techniques to address angular and translational deformities, ensuring optimal load distribution and functional outcomes.
Question 1
A 50-year-old patient underwent a TKA for knee arthritis secondary to a long-standing 20-degree varus deformity from a femoral malunion. The surgeon attempted to correct the alignment solely with intra-articular bone resections. Two years later, the patient presents with instability and pain. What is the most likely mode of failure?
View Answer & Explanation
Correct Answer: C
Rationale: Correcting a large extra-articular deformity with intra-articular cuts creates an oblique joint line relative to the mechanical axis. This leads to obligatory collateral ligament imbalance, abnormal shear stresses on the polyethylene, and eccentric loading, all of which precipitate aseptic loosening and instability.
Question 2
A 68-year-old male presents with debilitating right knee pain and a severe varus deformity. On examination, he has a 20-degree varus thrust. When planning for a total knee arthroplasty (TKA), which of the following imaging studies is considered non-negotiable for accurately calculating the Mechanical Axis Deviation (MAD) and formulating a corrective strategy?
View Answer & Explanation
Correct Answer: C
Rationale: The provided text explicitly states that a full-length standing radiograph is "non-negotiable" to accurately calculate the MAD and identify any extra-articular deformities. Relying solely on short knee films (A) will inevitably lead to miscalculations in the magnitude of the deformity.
Question 3
A 72-year-old female with end-stage osteoarthritis is being evaluated for a TKA. A full-length standing radiograph reveals her mechanical axis passes 25 mm medial to the center of her knee joint. How is this finding best described?
View Answer & Explanation
Correct Answer: B
Rationale: Mechanical Axis Deviation (MAD) is the measurement of how far the mechanical axis deviates from the knee's center. When the axis passes medial to the knee center, it is defined as varus malalignment. Therefore, this represents 25 mm of varus MAD. Valgus MAD (A) would occur if the axis passed lateral to the knee center.
Question 4
A 58-year-old male with a history of a malunited mid-shaft femoral fracture presents with severe knee arthritis. Preoperative planning for TKA reveals a significant extra-articular deformity. What is the single most important step in determining the surgical plan for this patient?
View Answer & Explanation
Correct Answer: B
Rationale: The text emphasizes that identifying the CORA's location is the "single most important step" in surgical planning. When the CORA is extra-articular (outside the joint), attempting to correct the deformity with intra-articular cuts alone will lead to an oblique joint line and profound ligamentous imbalance, necessitating a combined osteotomy and arthroplasty.
Question 5
A 65-year-old female presents for a primary TKA due to osteoarthritis. Her deformity is primarily intra-articular, resulting from cartilage and subchondral bone loss. Based on Paley principles, where is the Center of Rotation of Angulation (CORA) most likely located?
View Answer & Explanation
Correct Answer: C
Rationale: The text states that in common cases of TKA where the deformity is from intra-articular loss, the CORA is conveniently located "at the joint line." This allows for correction of the deformity through standard intra-articular bone resections and soft tissue balancing.
Question 6
A surgeon is planning a TKA for a patient with a 15-degree varus deformity and a malunited proximal tibia fracture from 20 years ago. The CORA is identified in the tibial metaphysis, 5 cm distal to the joint line. What is the most likely consequence of attempting to correct this deformity with intra-articular cuts alone?
View Answer & Explanation
Correct Answer: B
Rationale: The text warns that for an extra-articular deformity (CORA outside the joint), correcting with intra-articular cuts alone is a "recipe for disaster." It will lead to an oblique joint line, profound ligamentous imbalance, and a translated mechanical axis, dooming the arthroplasty to early failure.
Question 7
During preoperative templating for a TKA, a surgeon measures the angle between the femoral mechanical axis and the distal femoral joint line. What is this angle called, and what is its average normal value?
View Answer & Explanation
Correct Answer: B
Rationale: The Mechanical Lateral Distal Femoral Angle (mLDFA) is defined as the angle between the mechanical axis and the distal femoral joint line. Its normal average value is 88° (range 85°-90°). The aLDFA (A) relates to the anatomic axis of the femur.
Question 8
A surgeon is performing a TKA using an intramedullary (IM) femoral guide. To achieve a neutral mechanical axis, a "valgus cut angle" of 6 degrees is set on the jig. This cut angle is primarily determined by which of the following preoperative measurements?
View Answer & Explanation
Correct Answer: C
Rationale: An IM guide follows the femoral anatomic axis. The valgus cut angle is set to compensate for the natural bow of the femur (the angle between the anatomic and mechanical axes) to make the final bone cut perpendicular to the mechanical axis. The aLDFA is a related concept that guides this cut.
Question 9
A 70-year-old female undergoes TKA. The surgeon's goal is to achieve the "Classical Alignment Schema." What are the target angles for the mLDFA and MPTA, respectively, with this philosophy?

View Answer & Explanation
Correct Answer: B
Rationale: The Classical, or mechanical, alignment philosophy aims for biomechanical purity by creating a joint line perfectly perpendicular to the mechanical axis. As shown in the provided image (b), this results in a target mLDFA of 90° and a target MPTA of 90°.
Question 10
A surgeon advocates for an "Anatomic Alignment Schema" during TKA, arguing it better replicates native knee kinematics. To achieve a neutral overall mechanical axis with this philosophy, what is the target Mechanical Proximal Tibial Angle (MPTA)?

View Answer & Explanation
Correct Answer: C
Rationale: The Anatomic Alignment Schema, shown in the image (a), aims to recreate the native 3° joint line obliquity. To balance the valgus femoral cut and maintain a neutral limb axis, the proximal tibia is intentionally cut into 3° of varus, yielding a target MPTA of 87°.
Question 11
A preoperative weight-bearing radiograph of a patient with severe varus osteoarthritis shows the distal femoral and proximal tibial joint lines converging medially at an angle of 8 degrees. What is this angle called, and what does it primarily indicate?
View Answer & Explanation
Correct Answer: C
Rationale: The Joint Line Convergence Angle (JLCA) is the angle between the femoral and tibial joint lines. A large JLCA (>2°) on a weight-bearing film indicates that a significant portion of the deformity is driven by ligamentous issues (contracture on the concave side, laxity on the convex side), not just bone loss.
Question 12
A resident is asked to assess the sagittal alignment of the tibia on a preoperative lateral radiograph. Which angle defines the posterior slope of the tibia, and what is its normal range?
View Answer & Explanation
Correct Answer: D
Rationale: The Posterior Proximal Tibial Angle (PPTA) defines the posterior slope of the tibia. Its normal range is 77° to 84°. This angle is critical for sagittal plane balance, flexion, and extension after TKA.
Question 13
A 69-year-old male with a severe, fixed varus deformity is undergoing TKA. The surgeon has made the initial bone cuts. During gap assessment, the medial side is extremely tight in both flexion and extension. According to the sequential medial release algorithm, what is the first step in balancing?
View Answer & Explanation
Correct Answer: D
Rationale: The text outlines a stepwise medial release algorithm. The first step is to remove large medial osteophytes and then release the deep MCL from its tibial attachment. This often provides significant correction before proceeding to more aggressive releases like elevating the superficial MCL (A).
Question 14
During a TKA for a fixed varus knee, after removing osteophytes and releasing the deep MCL, the knee remains tight, particularly in extension. What is the next logical step in the medial release sequence?
View Answer & Explanation
Correct Answer: C
Rationale: The described algorithm states that if the knee remains tight in extension after the initial steps, the next release is the posteromedial capsule from the tibia, along with the tendinous insertions of the semimembranosus. Elevating the entire superficial MCL (B) is a more powerful, subsequent step.
Question 15
A surgeon is performing a TKA on an extremely rigid, long-standing varus knee. After performing releases of the deep MCL, posteromedial corner, and a subperiosteal elevation of the superficial MCL, the medial gap remains unacceptably tight. What is the final soft-tissue release option on the medial side?
View Answer & Explanation
Correct Answer: B
Rationale: The text specifies that in the "most extreme, rigid varus deformities," the final step in the sequential medial release is the elevation of the pes anserinus tendon insertions. This is reserved for the most severe cases after other releases have been performed.
Question 16
A 75-year-old female presents with a severe, fixed valgus deformity and lateral compartment arthritis. During TKA, what is considered a primary deforming force, especially in extension, that must be addressed?
View Answer & Explanation
Correct Answer: C
Rationale: For a valgus knee, the text identifies the IT band as a "primary deforming force, especially in extension." It can be addressed by releasing it from Gerdy's tubercle or by "pie-crusting." The other structures listed are on the medial side and are relevant to varus deformities.
Question 17
A surgeon is planning a TKA for a patient with a significant valgus deformity. Preoperative valgus stress radiographs show the medial joint space opening to 20 degrees. What is the most important implication of this finding for implant selection?
View Answer & Explanation
Correct Answer: C
Rationale: The text states that an opening of greater than 15° on stressed views delineates clear collateral ligament incompetency. In this case, the medial collateral ligament is incompetent. Standard soft tissue balancing may be insufficient, and the surgeon must be prepared to use a more constrained prosthesis (e.g., varus-valgus constrained or rotating hinge) to provide stability.
Question 18
A 66-year-old patient has a TKA performed. Postoperatively, the patient has difficulty achieving deep flexion and reports a sensation of anterior impingement. The surgeon suspects an issue with the sagittal alignment of the tibial component. Which of the following is the most likely technical error?
View Answer & Explanation
Correct Answer: B
Rationale: The text warns that an "improperly sloped tibia can block flexion, cause anterior impingement, or lead to paradoxical instability in flexion." Insufficient posterior slope (or an anteriorly sloped cut) reduces the space available for the femur to roll back in deep flexion, leading to impingement.
Question 19
What is the foundational principle of ligament balancing in TKA for a fixed coronal plane deformity?
View Answer & Explanation
Correct Answer: B
Rationale: The text states the "cardinal rule" and "foundational principle" is simple: "releases are performed on the concave side, while preserving the convex side." For a varus knee, this means releasing medial structures; for a valgus knee, it means releasing lateral structures.
Question 20
A 62-year-old patient with a history of a healed tibial shaft fracture with retained intramedullary nail presents for TKA. During preoperative planning, what is the most critical consideration regarding the existing hardware?
View Answer & Explanation
Correct Answer: C
Rationale: The text advises surgeons to assess retained hardware to "determine if it crosses your planned osteotomy or stem trajectory." An IM nail in the tibia would directly block the placement of a standard stemmed tibial component, requiring either hardware removal or an alternative implant strategy.
Question 21
A surgeon is performing a clinical examination on a patient with a severe varus deformity. The surgeon applies firm, longitudinal traction to the leg while assessing the alignment. What is this maneuver called, and what is its primary purpose?
View Answer & Explanation
Correct Answer: C
Rationale: The text describes the "tension" test, where the joint is tensed by pulling on the leg. Its purpose is to tense both collateral ligaments simultaneously, allowing the surgeon to "assess the degree of fixed, osseous deformity versus the correctable, soft-tissue component."
Question 22
The ultimate goal of restoring the mechanical axis in TKA is to ensure optimal load distribution across the prosthetic components. In a perfectly aligned limb, where should the mechanical axis line pass relative to the knee's center?
View Answer & Explanation
Correct Answer: C
Rationale: The text states that in a perfectly aligned limb, the mechanical axis "passes slightly medial to the knee's center, typically around the 8 mm mark." This ensures proper load distribution and longevity of the prosthesis.
Question 23
A 71-year-old male with a history of developmental bowing of his femur presents with severe knee arthritis. Preoperative planning reveals the CORA is located in the distal femoral diaphysis. Which surgical approach is most appropriate to avoid early arthroplasty failure?
View Answer & Explanation
Correct Answer: C
Rationale: The text is unequivocal that when the CORA is located outside the joint (extra-articular deformity), attempting correction with intra-articular cuts alone is incorrect. It states that these "severe cases often dictate a simultaneous extra-articular corrective osteotomy combined with the arthroplasty."
Question 24
A surgeon is templating a TKA and measures the angle between the anatomic axis of the femur and the distal femoral joint line. The value is 81°. Which angle has been measured?
View Answer & Explanation
Correct Answer: E
Rationale: The Anatomic Lateral Distal Femoral Angle (aLDFA) is defined as the angle between the femoral shaft (anatomic axis) and the distal femoral joint line. Its average value is 81°. This is distinct from the mLDFA (A), which uses the mechanical axis.
Question 25
In the Classical Alignment philosophy for TKA, the proximal tibial cut is made perpendicular to the tibial mechanical axis. What is the target Mechanical Proximal Tibial Angle (MPTA) in this schema?
View Answer & Explanation
Correct Answer: C
Rationale: The Classical Alignment Schema aims for a joint line perpendicular to the limb's mechanical axis. This is achieved with a distal femoral cut (mLDFA) of 90° and a proximal tibial cut (MPTA) of 90°.
Question 26
A 25-year-old male presents with a healed diaphyseal femur fracture. Radiographs show the proximal and distal anatomical axis lines are perfectly parallel but not collinear. The mechanical Lateral Distal Femoral Angle (mLDFA) is normal relative to the distal fragment. Which term best describes this deformity?
View Answer & Explanation
Correct Answer: C
Rationale: The definition of a pure translation deformity is that the proximal and distal axis lines are parallel but not collinear. The joint orientation angles (like mLDFA) remain normal because there is no angulation. An angulation-translation deformity (D) would have non-parallel, intersecting axes.
Question 27
A 30-year-old female has a tibial malunion characterized by pure medial translation. On long-leg standing radiographs, the mechanical axis is deviated medially, but the Medial Proximal Tibial Angle (MPTA) and Lateral Distal Tibial Angle (LDTA) are within normal limits. Where is the Center of Rotation of Angulation (CORA) for this deformity located?
View Answer & Explanation
Correct Answer: E
Rationale: In a pure translation deformity, the proximal and distal axes are parallel and never intersect. Mathematically, parallel lines are said to intersect at infinity. Therefore, the CORA for a pure translation deformity is located at infinity. The apex of the translation (A) is the physical location of the deformity, not the geometric CORA.
Question 28
A 40-year-old male sustains a mid-shaft humeral fracture that heals with a pure 2 cm anterior translation. There is no associated angulation or shortening. What is the most significant clinical consequence of this deformity on the limb's overall alignment?
View Answer & Explanation
Correct Answer: B
Rationale: Even without angulation, a pure translation deformity shifts the overall mechanical axis of the limb, resulting in Mechanical Axis Deviation (MAD). This alters weight-bearing forces and can lead to long-term joint degeneration. Joint orientation angles (A) remain normal in a pure translation deformity.
Question 29
A surgeon is planning an acute correction of a 1.5 cm pure translational deformity in the diaphysis of the tibia using a plate and screws. What is the primary limiting factor that must be considered to ensure biomechanical stability and successful healing?
View Answer & Explanation
Correct Answer: D
Rationale: The text explicitly states that the primary limiting factor in translating a bone is the preservation of adequate bone-to-bone contact. A significant translation in a narrow diaphysis can reduce cortical contact to less than 50%, compromising stability and healing. While soft tissue compliance (C) is a concern, especially with lengthening, bone contact is the key biomechanical factor for a pure translation correction.
Question 30
A 28-year-old patient has a femoral malunion with 2 cm of pure lateral translation and no shortening. The surgeon is planning a single-level osteotomy for correction. Which type of osteotomy is most appropriate for this specific situation?
View Answer & Explanation
Correct Answer: B
Rationale: The text states that a transverse osteotomy is the "workhorse for pure translational correction when there is no need to add length." An oblique osteotomy (A) is used when simultaneous lengthening is required. Wedge osteotomies (C, D) are used to correct angular deformities.
Question 31
A surgeon performs a transverse osteotomy in the narrow diaphysis of the femur to correct a pure translation deformity. The bone diameter is 30 mm. To achieve full correction, a translation of 15 mm is required. What percentage of cortical bone-to-bone contact will remain after the correction?
View Answer & Explanation
Correct Answer: C
Rationale: The text explains that in a narrow diaphysis, the cross-sectional bone-to-bone contact decreases linearly with translation. A 15 mm translation on a 30 mm diameter bone represents a 50% translation, which leaves only 50% cortical contact. This level of contact significantly compromises intrinsic stability.
Question 32
A 35-year-old patient presents with a tibial malunion characterized by 15 mm of medial translation and 15 mm of shortening. The surgeon plans a single osteotomy to correct both deformities simultaneously. What is the ideal angle for this oblique osteotomy?
View Answer & Explanation
Correct Answer: C
Rationale: The text specifies that the angle of an oblique osteotomy is determined by the required length and translation. When the required lengthening and translation are equal (in this case, 15 mm each), a 45-degree oblique cut is required. This geometry allows the bone to slide distally and medially/laterally at an equal rate.
Question 33
During an acute correction of a combined translation and shortening deformity using an oblique osteotomy, the surgeon achieves 2.5 cm of length. Post-operatively, the patient develops a foot drop. This complication is most likely due to exceeding the safe limit for acute stretch of which structure?
View Answer & Explanation
Correct Answer: E
Rationale: The text warns that stretching neurovascular structures acutely beyond 1.5 to 2 centimeters can lead to neurapraxia, compartment syndrome, or vascular compromise. A foot drop indicates an injury to the peroneal nerve, which is part of the neurovascular bundle and is highly susceptible to stretch.
Question 34
A surgeon is correcting a translational malunion where a large, mature callus is physically blocking the bone ends from sliding into the corrected position. According to the principles outlined, what is the most appropriate next step?
View Answer & Explanation
Correct Answer: C
Rationale: The text and accompanying image (c) explicitly state that in cases of mature malunions, the surgeon must perform a careful decortication or trimming of the obstructing callus. This must be done judiciously to preserve the surrounding periosteal blood supply while creating a flat track for the bone ends to glide along.
Question 35
A 45-year-old patient has a severe, 4 cm pure translational deformity in the narrow diaphysis of the humerus. A single sliding transverse osteotomy would result in zero bone-to-bone contact. What is the most appropriate alternative surgical technique to correct this deformity while maximizing bone contact?
View Answer & Explanation
Correct Answer: C
Rationale: The text describes the two-level angulation technique as particularly useful in severe diaphyseal translations where a single sliding cut would result in zero bone-to-bone contact. By creating a controlled "Z-deformity" with two osteotomies, the axis is corrected while maintaining cortical contact at both osteotomy sites.
Question 36
When using the two-level angulation technique to correct a pure translation deformity, which of the following geometric rules must be followed to avoid creating a new angular deformity?
View Answer & Explanation
Correct Answer: C
Rationale: The text lists three strict rules for this technique: 1) The angulation must be in opposite directions. 2) The angulation must be of the exact same magnitude. 3) The angulation must occur in the exact same plane. This ensures that the net effect is pure translation of the axis without any residual angulation.
Question 37
A 22-year-old has a femoral malunion with both varus angulation and medial translation. How do the proximal and distal anatomical axis lines behave geometrically in this type of deformity?
View Answer & Explanation
Correct Answer: D
Rationale: The text clearly distinguishes between pure translation (parallel axes) and angulation-translation deformities. When angulation is present, the proximal and distal axis lines are no longer parallel; they are on a collision course and will intersect at a point in space defined as the Center of Rotation of Angulation (CORA).
Question 38
When analyzing a long bone deformity with both angulation and translation, the perpendicular distance between the proximal and distal axis lines changes depending on the level of measurement. Why is a standardized measurement convention, such as the Paley convention, critically important?
View Answer & Explanation
Correct Answer: B
Rationale: The text emphasizes that because the translation distance changes at every level in an angulated bone, measuring it arbitrarily leads to irreproducible results and surgical planning errors. A standardized convention is essential for consistency and accuracy in planning the correction.
Question 39
A surgeon is evaluating a tibial malunion with both angulation and translation. According to the universally accepted Paley measurement convention, how is the magnitude of translation defined?
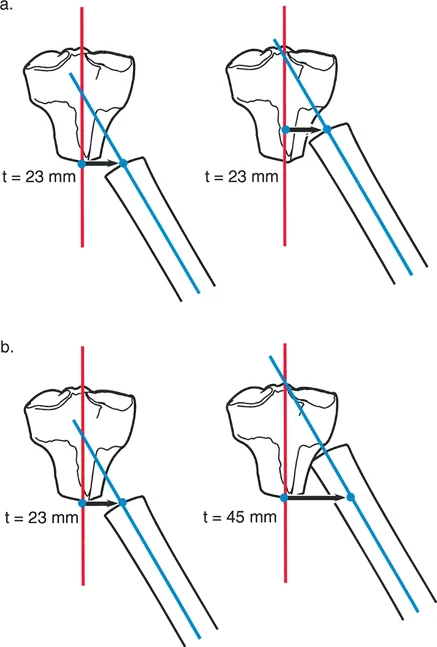
View Answer & Explanation
Correct Answer: B
Rationale: The text explicitly defines the Paley convention: "The magnitude of translation is defined as the perpendicular distance from the proximal axis line to the distal axis line at the level of the proximal end of the distal fragment." This is the gold standard for consistent measurement.
Question 40
What is the primary rationale for adopting the Paley convention of measuring translation relative to the proximal axis at the start of the distal fragment?
View Answer & Explanation
Correct Answer: C
Rationale: The text explains that this convention is preferred because deformities are often associated with shortening. By referencing the proximal axis (contiguous with the axial skeleton) and measuring where the distal fragment begins, we accurately capture how far the distal limb has shifted away from the body's central alignment.
Question 41
A surgeon is analyzing an oblique plane deformity of the femur using AP and lateral radiographs. The AP view shows 10 mm of medial translation, and the lateral view shows 24 mm of posterior translation. What is the true magnitude of the translation in the oblique plane?
View Answer & Explanation
Correct Answer: C
Rationale: The true magnitude is calculated using the Pythagorean theorem (a² + b² = c²). Here, c = √(10² + 24²) = √(100 + 576) = √676 = 26 mm. The AP and lateral measurements are vector components of the true deformity.
Question 42
According to Paley's Osteotomy Rule 1, what is the result if an osteotomy is performed directly through the CORA and the Angulation Correction Axis (ACA) is also placed at the CORA?
View Answer & Explanation
Correct Answer: B
Rationale: Paley's Rule 1 is the fundamental principle for correcting a simple angular deformity. When the osteotomy and the hinge (ACA) are both at the CORA, the bone ends pivot perfectly, correcting the angle without any shift or translation at the osteotomy site.
Question 43
A surgeon is correcting a femoral malunion that has both 15 degrees of varus and 20 mm of medial translation. The surgeon performs the osteotomy at the level of the old fracture, which is anatomically distal to the true CORA. To correct both deformities simultaneously, where should the Angulation Correction Axis (ACA) or hinge be placed?
View Answer & Explanation
Correct Answer: B
Rationale: This scenario describes the application of Paley's Osteotomy Rule 2. By performing the osteotomy at a level away from the CORA but hinging the correction around the true CORA, the bone segments will both angulate and translate, allowing for simultaneous correction of the combined deformity.
Question 44
Which of Paley's Osteotomy Rules is considered the "secret weapon" for correcting combined angulation-translation deformities with a single osteotomy?
View Answer & Explanation
Correct Answer: B
Rationale: The text explicitly refers to Rule 2 as the "secret weapon for correcting angulation-translation deformities." This principle explains how a single, well-planned osteotomy can resolve a complex multi-planar problem by strategically separating the osteotomy level from the center of rotation.
Question 45
A 15-year-old female with a history of treated developmental dysplasia of the hip (DDH) presents with a painful limp. Radiographs of the affected hip show a neck-shaft angle (NSA) of 108° and a mechanical-proximal femoral angle (MPFA) of 48°. The contralateral normal hip has an NSA of 136° and an MPFA of 90°. If a surgeon performs a subtrochanteric osteotomy to correct only the NSA deformity of 28°, what will be the resulting MPFA?
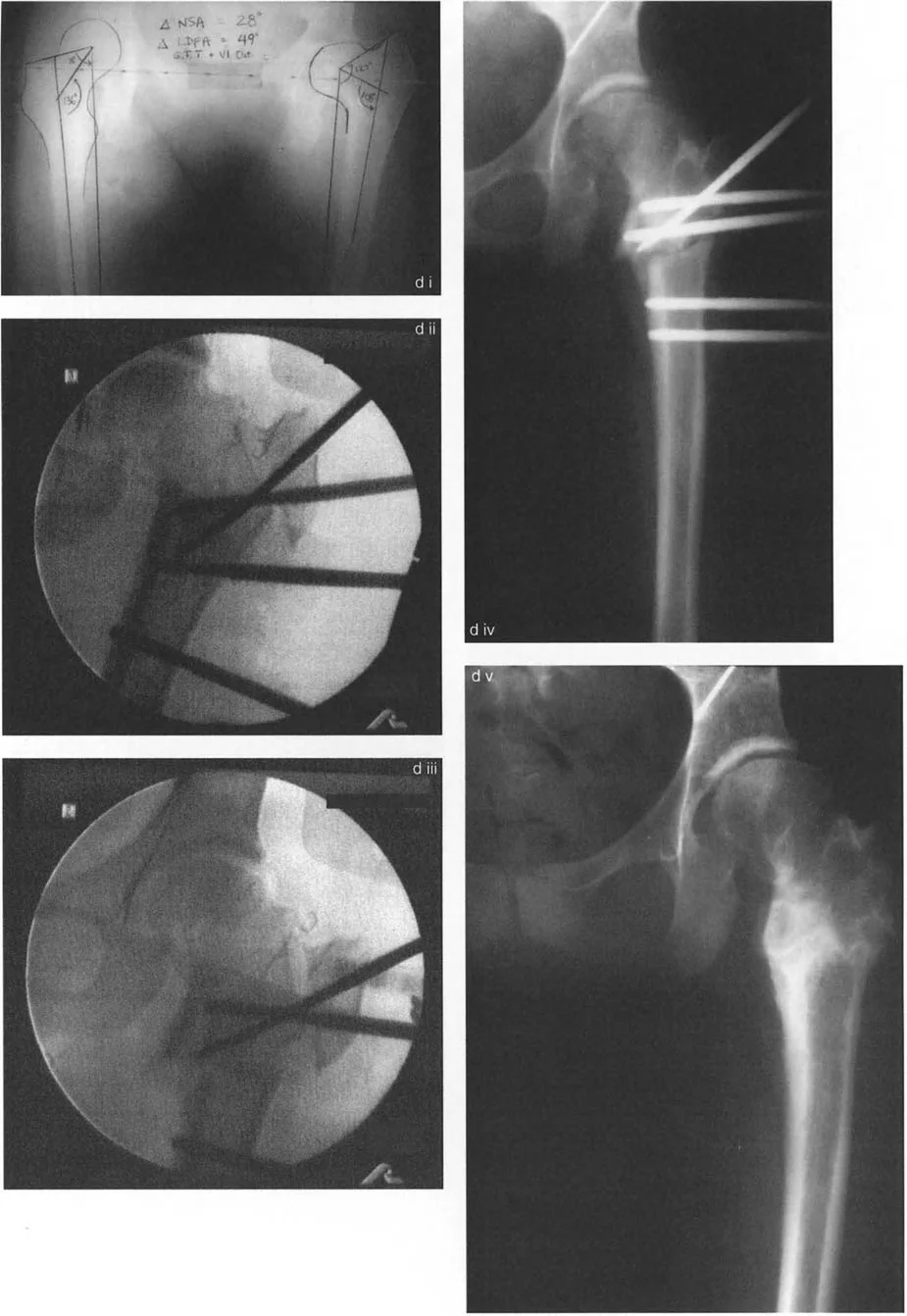
View Answer & Explanation
Correct Answer: B
Rationale: The total MPFA deformity is 42° (90°-48°), while the NSA deformity is 28° (136°-108°). The difference is due to greater trochanteric overgrowth. Correcting only the 28° of NSA varus will leave the MPFA in residual varus at 76° (48° + 28°), as shown in Figure 19-9c, panel ii. A full correction to 90° would require addressing the trochanteric component as well.
Question 46
A 16-year-old male presents with a Trendelenburg gait and hip pain secondary to coxa vara and breva from previous DDH treatment. Radiographs reveal significant greater trochanteric overgrowth, a varus NSA, and an abnormal MPFA. To achieve an anatomic correction that normalizes both the NSA and the MPFA, which of the following procedures is most appropriate?
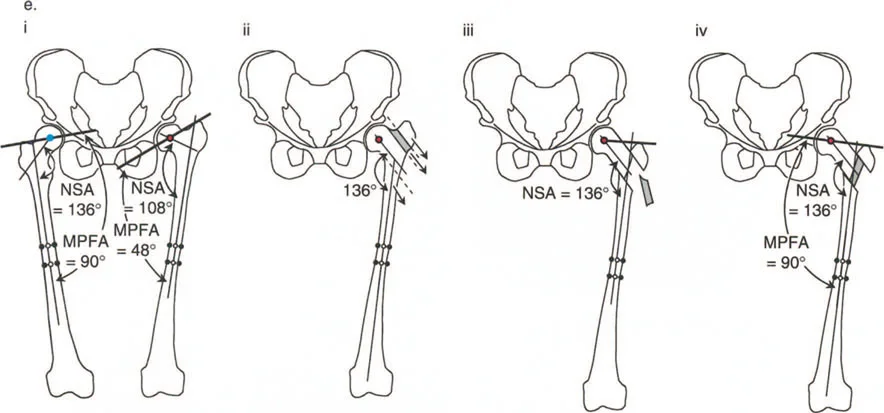
View Answer & Explanation
Correct Answer: C
Rationale: As described by Wagner and illustrated in Figure 19-9c and 19-9d, an anatomic correction for combined coxa vara and trochanteric overgrowth requires addressing both deformities. A subtrochanteric valgus osteotomy corrects the NSA, while a distal and lateral transfer of the greater trochanter corrects the trochanteric overgrowth and normalizes the MPFA. An isolated procedure (A or B) would only partially correct the overall deformity.
Question 47
A 14-year-old with sequelae of Perthes disease has coxa vara and significant trochanteric overgrowth. The surgeon plans a Morscher osteotomy. What is the key characteristic of the Morscher osteotomy that distinguishes it from the Wagner osteotomy?
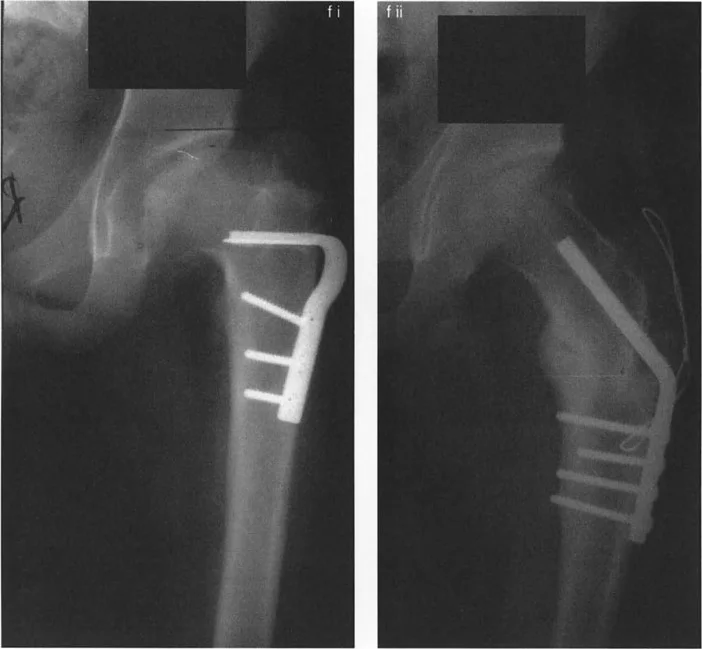
View Answer & Explanation
Correct Answer: B
Rationale: The text explicitly states that the Morscher osteotomy corrects both the NSA and the MPFA but "does not change the orientation of the femoral head in the acetabulum." This is a key difference from the Wagner method, which is preferred when reorientation of the femoral head is also required.
Question 48
During a Morscher osteotomy for coxa vara, a cylinder of bone is harvested from the base of the greater trochanter. What is the intended use for this bone cylinder?

View Answer & Explanation
Correct Answer: C
Rationale: As described in the text for Figure 19-9e, the harvested bone cylinder is "interposed between the trochanter and the femoral shaft to fill the lateral space." This maneuver achieves the desired distal and lateral transfer of the trochanter, lengthening the abductor mechanism.
Question 49
A 17-year-old patient with hypochondroplasia presents with a waddling gait. Examination reveals a positive Trendelenburg sign. Radiographs show a normal NSA of 130° but an abnormal lateral proximal femoral angle (LPFA) of 100°, indicating an overgrown greater trochanter. What is the most appropriate surgical intervention?
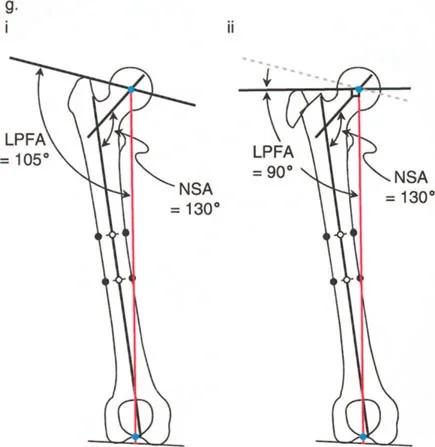
View Answer & Explanation
Correct Answer: D
Rationale: The text accompanying Figure 19-9g states that for an overgrown trochanter with a normal NSA, "The ideal treatment in this case is transfer of the greater trochanter." A subtrochanteric osteotomy (A or B) is not indicated because the neck-shaft relationship is already normal.
Question 50
A surgeon is performing a percutaneous transfer of the greater trochanter. After completing the osteotomy, scissors are inserted into the osteotomy site. What is the primary purpose of this step?
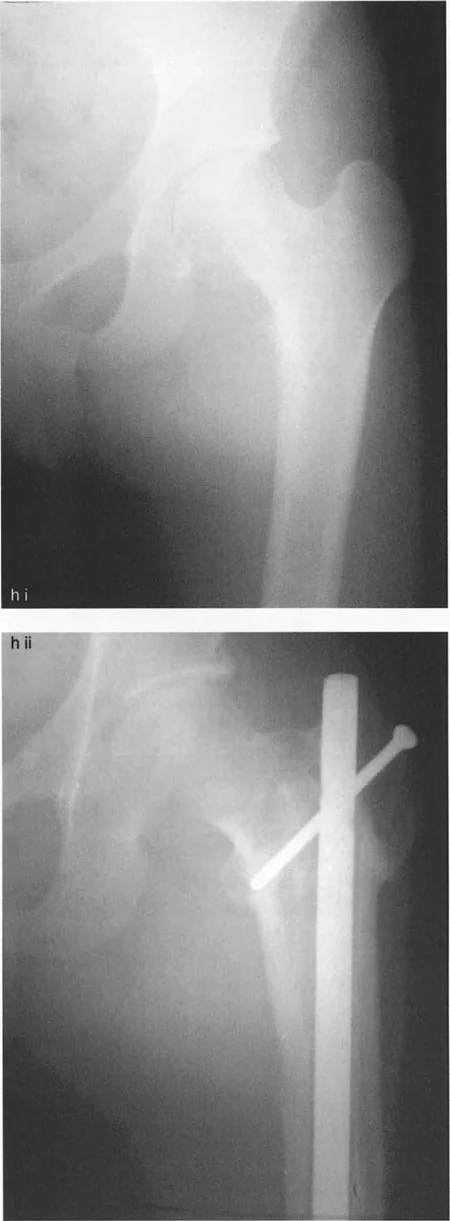
View Answer & Explanation
Correct Answer: B
Rationale: Figure 19-9i, panel iii, explicitly shows this step and the caption states, "scissors are inserted to release the soft tissue attachments around the trochanter." This mobilization is crucial to allow for distal traction and repositioning of the trochanteric fragment.
Question 51
A 58-year-old male with hip osteoarthritis undergoes a subtrochanteric varus osteotomy without a concomitant trochanteric procedure. Postoperatively, what is the most likely new clinical finding related to his gait?
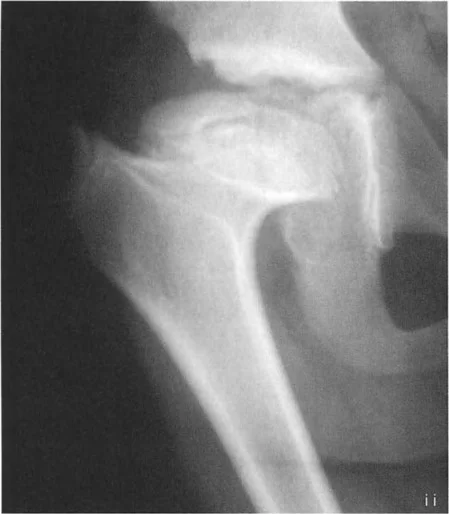
View Answer & Explanation
Correct Answer: B
Rationale: As illustrated in Figure 19-10a, a simple varus osteotomy proximalizes the greater trochanter. This shortens the abductor lever arm, weakens the hip abductors, and leads to a Trendelenburg gait. While the antalgic component may improve, the new biomechanical deficit often produces a Trendelenburg lurch.
Question 52
A 68-year-old male presents with severe right knee pain and a visible varus deformity. A full-length standing radiograph reveals the mechanical axis, a line from the center of the femoral head to the center of the ankle, passes 35 mm medial to the center of the knee joint. What does this measurement represent?
View Answer & Explanation
Correct Answer: C
Rationale: The Mechanical Axis Deviation (MAD) is the perpendicular distance from the center of the knee to the mechanical axis of the lower extremity. A medially shifted MAD, as described, indicates a varus deformity. The mLDFA and MPTA are joint orientation angles, not a measure of overall limb alignment.
Question 53
A 55-year-old female with a history of a malunited mid-shaft femur fracture presents for total knee arthroplasty (TKA) evaluation. Her surgeon is planning the procedure based on Paley's principles. According to the text, what is the precise definition of the lower extremity mechanical axis?
View Answer & Explanation
Correct Answer: C
Rationale: The mechanical axis of the lower extremity is the weight-bearing line, defined as a straight line from the center of the femoral head to the center of the ankle talus. This is the foundational concept for all lower limb alignment analysis. The other options describe anatomical axes or reference lines for bone cuts.
Question 54
A 72-year-old woman with end-stage osteoarthritis is being evaluated for a TKA. Her preoperative deformity analysis reveals a significant varus deformity originating from the tibia. Her Medial Proximal Tibial Angle (MPTA) is measured to be 78°. What is the normal range for the MPTA?
View Answer & Explanation
Correct Answer: C
Rationale: The normal Medial Proximal Tibial Angle (MPTA) is between 85° and 90°, with an average target of 87°. An MPTA of 78° indicates a significant tibial varus deformity. The goal of TKA is to restore this angle to approximately 90° relative to the tibial mechanical axis.
Question 55
A 65-year-old male with a history of Paget's disease has a severe valgus deformity of his left knee. Preoperative planning radiographs show that the deformity is primarily located in the distal femur. Which joint orientation angle would be most affected and is used to quantify this specific deformity?
View Answer & Explanation
Correct Answer: D
Rationale: The Mechanical Lateral Distal Femoral Angle (mLDFA) defines the relationship between the femoral mechanical axis and the distal femoral articular surface. A valgus deformity of the distal femur would result in an mLDFA less than the normal 85°-90°. The MPTA and LDTA relate to the tibia.
Question 56
A surgeon is planning a corrective osteotomy for a 45-year-old patient with a post-traumatic tibial malunion. On the long-leg radiograph, the surgeon draws the proximal and distal mechanical axes of the tibia and notes their intersection point. According to Paley's principles, what is this intersection point called?
View Answer & Explanation
Correct Answer: C
Rationale: The Center of Rotation of Angulation (CORA) is the precise geometric point where the proximal mechanical axis and the distal mechanical axis of a deformed bone intersect. Identifying the CORA is the most critical step in planning a surgical correction, as it represents the epicenter of the deformity.
Question 57
A 66-year-old female presents with severe knee arthritis and a 20° varus deformity secondary to a healed mid-diaphyseal femur fracture. According to Paley's principles, where is the CORA of this deformity located, and what is the implication for treatment?
View Answer & Explanation
Correct Answer: B
Rationale: When the CORA is located in the diaphysis (shaft) of the bone, it is an extraarticular deformity. Paley's First Osteotomy Rule states that the most biomechanically sound correction is an osteotomy performed at the level of the CORA. Attempting to correct this with intraarticular cuts alone would lead to severe complications.
Question 58
A 75-year-old male presents with classic medial compartment osteoarthritis, bone-on-bone changes, and a 15° varus deformity. Long-leg films show no diaphyseal bowing of the femur or tibia. Where is the CORA of his deformity most likely located?
View Answer & Explanation
Correct Answer: C
Rationale: In standard osteoarthritis without extraarticular bowing, the deformity is driven by asymmetric cartilage wear, bone collapse, and ligament laxity. Therefore, the CORA is located at or near the joint line (intraarticular). This type of deformity is appropriately corrected with standard TKA bone cuts and soft-tissue balancing.
Question 59
A surgeon identifies a single, extraarticular CORA in the mid-shaft of the femur in a patient needing a TKA. To achieve the most anatomically and biomechanically sound correction without creating a secondary translational deformity, where should the corrective osteotomy be performed?
View Answer & Explanation
Correct Answer: D
Rationale: Paley's First Osteotomy Rule states that executing the correction of a deformity exactly at the level of the CORA allows for pure angular correction without creating a secondary translational deformity. This is the most efficient and anatomically correct method to resolve a structural deformity before or during arthroplasty.
Question 60
A surgeon attempts to correct a 20° varus deformity originating from the femoral diaphysis solely with intraarticular bone cuts during a TKA. While the immediate post-operative radiograph may show a straight mechanical axis, what is the most significant iatrogenic consequence of this compensatory approach?
View Answer & Explanation
Correct Answer: D
Rationale: Correcting a deformity away from its CORA inherently induces a new, secondary deformity. Correcting a mid-shaft femoral varus at the knee tilts the entire proximal femur into valgus, altering the LPFA and hip biomechanics. Similarly, correcting a tibial deformity at the knee will tilt the ankle plafond, altering the LDTA.
Question 61
A 62-year-old female has a 15° valgus deformity with an extraarticular CORA in the distal femoral diaphysis. If a surgeon attempts to correct this deformity entirely with intraarticular TKA cuts to achieve a neutral mechanical axis, which of the following will be required?
View Answer & Explanation
Correct Answer: A
Rationale: To correct a valgus (knock-knee) deformity originating in the femur using only intraarticular cuts, an enormous, non-anatomic wedge of bone must be removed from the convex side of the deformity, which is the medial femoral condyle. This leads to joint line elevation and potential MCL compromise.
Question 62
A 69-year-old male presents with a 20° varus deformity with a CORA in the proximal tibial diaphysis. During TKA, the surgeon decides against an osteotomy and plans to correct the deformity with compensatory bone cuts. This approach will necessitate which of the following?
View Answer & Explanation
Correct Answer: D
Rationale: To correct a varus (bow-leg) deformity originating in the tibia using only intraarticular cuts, a large wedge of bone must be removed from the convex side of the deformity, which is the lateral tibial plateau. This creates a large gap medially and risks joint line alteration.
Question 63
A 58-year-old female has a severe valgus deformity of the knee secondary to a malunited proximal tibia fracture. The surgeon plans to correct the deformity entirely with an aggressive intraarticular tibial cut. Which ligament is at the highest risk of iatrogenic injury with this approach?

View Answer & Explanation
Correct Answer: C
Rationale: As shown in the provided diagram, correcting a valgus tibial deformity with an intraarticular cut requires a massive medial tibial resection. This aggressive cut can completely obliterate the broad insertion footprint of the Medial Collateral Ligament (MCL), leading to gross coronal plane instability.
Question 64
During a TKA for a severe valgus deformity with an extraarticular tibial CORA, a surgeon performs a large compensatory medial tibial bone cut, which inadvertently detaches the MCL insertion. The knee is now grossly unstable in the coronal plane. What is the most likely implant choice the surgeon will be forced to make?
View Answer & Explanation
Correct Answer: D
Rationale: Iatrogenic detachment of a collateral ligament creates gross instability that cannot be managed by standard primary implants (CR or PS). The surgeon must escalate to a highly constrained or hinged prosthesis to provide the stability that was lost. These salvage implants transfer immense stress to the bone-cement interface, increasing the risk of aseptic loosening.
Question 65
A 60-year-old male with a 20° varus deformity from a mid-shaft femoral malunion undergoes a TKA where the deformity is corrected entirely with intraarticular cuts. Postoperatively, he has a neutral mechanical axis but develops a Trendelenburg gait. This is most likely due to an iatrogenic alteration of which joint orientation angle?
View Answer & Explanation
Correct Answer: E
Rationale: Correcting a mid-shaft femoral varus deformity at the knee forces the entire proximal femur into a valgus orientation relative to the ground. This pathologically alters the Lateral Proximal Femoral Angle (LPFA), which changes abductor muscle tension and can lead to abductor dysfunction and a Trendelenburg gait.
Question 66
A patient with a significant valgus deformity originating in the mid-tibia undergoes a TKA with intraarticular correction only. Postoperatively, the knee is well-aligned, but the patient develops progressive ankle pain and arthropathy. This complication is a direct result of altering which angle?
View Answer & Explanation
Correct Answer: A
Rationale: Correcting a mid-shaft tibial deformity at the knee joint will tilt the ankle plafond relative to the ground. This alters the Lateral Distal Tibial Angle (LDTA), creating an abnormal mechanical environment for the tibiotalar joint, which can lead to premature ankle arthropathy.
Question 67
A 67-year-old male has a severe valgus knee deformity due to a distal femoral malunion. Preoperative digital templating for a TKA reveals that the necessary compensatory medial femoral condyle cut will completely resect the origin footprint of the MCL. According to the provided text, what does this finding represent?
View Answer & Explanation
Correct Answer: C
Rationale: The text explicitly states that any deformity where the planned compensatory cut would resect the origin or insertion of the MCL or LCL is a strict, absolute indication for an extraarticular osteotomy. Proceeding with the cut would lead to catastrophic instability.
Question 68
A 64-year-old man presents with a 10-year history of progressive bilateral knee pain and difficulty walking. His medical history is significant for a childhood bone disorder that was not treated. A clinical photograph of his lower extremities is shown. On examination, he has a palpable varus thrust bilaterally and crepitus with a limited range of motion. What is the most critical next step in his diagnostic workup?

View Answer & Explanation
Correct Answer: C
Rationale: In a patient with severe extra-articular deformity, a full-length standing radiograph is essential to assess the overall limb alignment, identify the location of the deformity (femoral vs. tibial), and measure critical angles for surgical planning. An MRI (A) is useful for soft tissues but does not provide the necessary alignment information for deformity correction.
Question 69
A 58-year-old woman with end-stage knee arthritis and a long-standing "bow-legged" deformity undergoes evaluation. A preoperative standing hip-to-ankle radiograph is obtained. Based on this image, where is the primary apex of the varus deformity located?

View Answer & Explanation
Correct Answer: C
Rationale: The radiograph clearly shows that the distal femur has relatively normal alignment, while there is a sharp varus angulation in the proximal tibia, just below the joint line. This indicates the Center of Rotation of Angulation (CORA), or apex of the deformity, is in the proximal tibial metaphysis. The intra-articular space (B) shows arthritic changes but is not the source of the major structural deformity.
Question 70
A 66-year-old male presents for evaluation of severe knee pain. His preoperative standing radiograph is shown. A line is drawn from the center of the femoral head to the center of the ankle. Where does this line pass relative to the knee joint, and what is its significance?

View Answer & Explanation
Correct Answer: B
Rationale: The line described is the mechanical axis of the lower limb. In this severe varus deformity, the axis passes significantly medial to the center of the knee joint. This medial deviation shifts the weight-bearing load onto the medial compartment, accelerating its degeneration and causing pain. A line lateral to the knee (D) would indicate a valgus deformity.
Question 71
A surgeon is analyzing the preoperative radiograph of a patient with severe varus deformity and knee arthritis. The Medial Proximal Tibial Angle (MPTA) is a critical measurement for planning. Based on the image, which of the following is the most likely MPTA value for this patient's right tibia?

View Answer & Explanation
Correct Answer: D
Rationale: The normal MPTA is approximately 87 degrees. The image shows a severe varus deformity originating in the proximal tibia, which results in a significantly decreased MPTA. A value of 65 degrees reflects this severe angulation. An MPTA of 87 degrees (B) would be normal, and 95 degrees (A) would indicate a valgus tibia.
Question 72
During preoperative planning for a patient with multi-apical lower limb deformity, the mechanical Lateral Distal Femoral Angle (mLDFA) is measured on the standing radiograph shown. What is the approximate mLDFA, and what does it imply about the location of the deformity?

View Answer & Explanation
Correct Answer: B
Rationale: The normal mLDFA is approximately 87 degrees. Visually, the distal femur in the radiograph does not have a significant deformity; its joint line is relatively parallel to the ground compared to the severe tilt of the tibial plateau. Therefore, an mLDFA near 87 degrees is expected, indicating the primary deformity is not in the femur but in the tibia. A value of 75 degrees (C) would indicate severe femoral varus.
Question 73
A 60-year-old patient presents with the clinical and radiographic findings shown. He reports having had "bowed legs" since adolescence, which have worsened over time, along with severe knee pain. Given the severe, bilateral, symmetric extra-articular varus deformity originating in the proximal tibia, what is the most likely underlying etiology?

View Answer & Explanation
Correct Answer: C
Rationale: Blount's disease is a developmental disorder characterized by disordered ossification of the medial proximal tibial physis, leading to a progressive varus deformity. The appearance of a sharp angulation in the proximal tibial metaphysis is classic for this condition. Severe primary osteoarthritis (B) typically causes intra-articular deformity, not the significant extra-articular bowing seen here.
Question 74
A surgeon contemplates performing a standard total knee arthroplasty (TKA) on the patient shown, attempting to correct the alignment with soft-tissue releases and asymmetric bone cuts alone, without an extra-articular osteotomy. What is the most predictable and detrimental consequence of this approach?

View Answer & Explanation
Correct Answer: A
Rationale: Attempting to correct a large extra-articular deformity through intra-articular means forces the surgeon to make highly asymmetric bone cuts. This results in a joint line that is not perpendicular to the mechanical axis (an oblique joint line), leading to abnormal kinematics, severe ligamentous imbalance, and ultimately, early failure of the arthroplasty. Peroneal nerve palsy (D) is a risk of the correction itself, but the primary technical failure of avoiding the osteotomy is joint line obliquity and instability.
Question 75
The provided image shows a preoperative plan for deformity correction. The solid line drawn from the center of the femoral head to the center of the talus, which is planned to pass through the center of the knee postoperatively, is known as the:

View Answer & Explanation
Correct Answer: D
Rationale: The mechanical axis of the lower limb is a straight line connecting the center of the femoral head to the center of the ankle. It represents the true weight-bearing axis of the leg. The goal of deformity correction is to realign this axis to pass through the center of the knee. The anatomic axes (A, B) follow the intramedullary canals of the bones and are not straight lines.
Question 76
The preoperative plan for the patient with severe tibial varus includes a proximal tibial osteotomy. According to the principles of deformity correction popularized by Paley, the ideal location for a single, angular corrective osteotomy is at the:

View Answer & Explanation
Correct Answer: B
Rationale: A fundamental principle of deformity correction is that an angular correction performed at the CORA (the apex of the deformity) will realign the bone's axes without inducing an additional translational deformity. Placing the osteotomy away from the CORA requires both angulation and translation to achieve proper alignment, which is more complex and less ideal. In this case, the CORA is in the proximal tibial metaphysis.
Question 77
A 68-year-old female presents with debilitating medial-sided knee pain and a varus thrust. She has end-stage osteoarthritis. According to the principles outlined, viewing a total knee arthroplasty (TKA) in this patient with severe malalignment is most accurately described as which of the following?
View Answer & Explanation
Correct Answer: B
Rationale: The provided text explicitly states, "When viewed through the lens of Paley's principles, a standard TKA is, in its purest form, an intra-articular corrective osteotomy." This reframes the procedure from simple resurfacing to a complex biomechanical reconstruction aimed at correcting deformity. Option A is incorrect because the text emphasizes that TKA in severe malalignment is *not* a standard resurfacing procedure.
Question 78
A 72-year-old male with a history of a healed femoral shaft fracture presents for evaluation of severe knee arthritis. You are planning a total knee arthroplasty. Which of the following imaging studies is considered non-negotiable for preoperative planning in this patient?
View Answer & Explanation
Correct Answer: C
Rationale: The text emphasizes that full-length, standing, weight-bearing, bipedal hip-to-ankle radiographs are "non-negotiable" and the "only accurate method to calculate the true Mechanical Axis Deviation (MAD)." This is especially critical in a patient with a prior femoral fracture to identify any extra-articular deformity. Option B is explicitly stated as a common and preventable error that can lead to iatrogenic deformity.
Question 79
A 65-year-old female presents with a significant valgus deformity and lateral compartment osteoarthritis. A long-leg standing radiograph is obtained. The line drawn from the center of the femoral head to the center of the talus, as shown in the provided diagram, is known as what?

View Answer & Explanation
Correct Answer: D
Rationale: The text and the diagram define the mechanical axis as "a line drawn from the center of the femoral head to the center of the talus." This line is fundamental for assessing overall limb alignment. Options A and B refer to the axes within the medullary canals of the individual bones, not the overall limb alignment.
Question 80
A 70-year-old male is being evaluated for a TKA for severe varus osteoarthritis. His preoperative long-leg radiograph shows the mechanical axis passing significantly medial to the center of the knee joint. This finding is defined as the:

View Answer & Explanation
Correct Answer: B
Rationale: The text defines Mechanical Axis Deviation (MAD) as the deviation of the mechanical axis from the center of the knee joint. The image shown illustrates a varus deformity where the mechanical axis passes medial to the knee, representing a medial MAD. The other options are specific angles or points used to analyze the source of the deformity, but MAD describes the overall deviation.
Question 81
During preoperative planning for a TKA in a patient with severe malalignment, the surgeon asks, "Where is the Center of Rotation of Angulation (CORA)?" According to Paley's principles, why is this the single most important question?
View Answer & Explanation
Correct Answer: B
Rationale: The text states, "The single most important question in planning a TKA for malalignment is: *Where is the Center of Rotation of Angulation (CORA)?* The location of the CORA dictates the entire surgical strategy." Whether the CORA is intra-articular or extra-articular determines if a TKA alone is sufficient or if an additional osteotomy is required. The other options are secondary considerations not directly determined by the CORA's location.
Question 82
A 67-year-old female has severe varus osteoarthritis. Preoperative analysis of her long-leg radiograph reveals an mLDFA of 88°, an MPTA of 87°, and a JLCA of 8°. Based on these findings, where is the Center of Rotation of Angulation (CORA) most likely located?
View Answer & Explanation
Correct Answer: C
Rationale: The text indicates that a normal mLDFA and MPTA are between 85-90°. In this case, both are normal. An abnormal Joint Line Convergence Angle (JLCA), which is normally 0-2°, with normal bone orientation angles indicates an intra-articular CORA due to cartilage/bone loss or ligamentous issues. An 8° JLCA is significantly abnormal, localizing the deformity to the joint itself.
Question 83
A 58-year-old male with a history of a malunited proximal tibial fracture presents with knee pain. His long-leg radiograph shows a significant varus deformity. The mLDFA is 89°, but the MPTA is 75°. Where is the CORA for this patient's deformity?
View Answer & Explanation
Correct Answer: B
Rationale: According to the provided table, a normal MPTA is 85-90°. An MPTA of 75° is abnormally varus. With a normal mLDFA (89°), the deformity's CORA is located in the proximal tibia. This indicates an extra-articular deformity originating from the old fracture. Option A is incorrect because the mLDFA is normal.
Question 84
A 62-year-old female has a severe valgus deformity of her knee. Preoperative analysis reveals an mLDFA of 95° and an MPTA of 88°. Based on these angles, the primary source of her deformity is located in the:
View Answer & Explanation
Correct Answer: C
Rationale: The normal mLDFA is 85-90°. An mLDFA of 95° indicates a valgus deformity originating from the distal femur. The MPTA of 88° is within the normal range. Therefore, the CORA is in the distal femur. Option A is incorrect because the MPTA is normal.
Question 85
A surgeon attempts to correct a 15° varus deformity originating from a tibial diaphyseal malunion (extra-articular CORA) solely with intra-articular bone cuts during a TKA. According to the text, what is the most likely catastrophic outcome of this approach?
View Answer & Explanation
Correct Answer: C
Rationale: The text explicitly warns against this scenario: "Attempting to correct the limb's mechanical axis solely with asymmetric intra-articular TKA bone cuts is a critical biomechanical error. This approach will create severe joint line obliquity, leading to catastrophic mid-flexion instability, abnormal patellofemoral tracking, and accelerated polyethylene wear." The other options are potential TKA complications but not the specific biomechanical failure described.
Question 86
A 75-year-old male with Paget's disease has a bowed tibia and severe varus knee arthritis. Deformity analysis confirms an extra-articular CORA in the tibial diaphysis. What is the most appropriate surgical plan to restore a neutral mechanical axis?
View Answer & Explanation
Correct Answer: C
Rationale: The text states that cases with an extra-articular CORA "require a two-level correction: an extra-articular osteotomy to correct the diaphyseal deformity, combined with a TKA to address the intra-articular arthritis." Attempting to correct the diaphyseal bow with TKA cuts or releases alone (Options A, B, D) would lead to joint line obliquity and instability.
Question 87
A 66-year-old female presents with the clinical deformity shown. A long-leg radiograph is planned. What is the ultimate goal of the bone cuts during the subsequent TKA regarding the limb's alignment?

View Answer & Explanation
Correct Answer: D
Rationale: The text clearly states, "The ultimate goal of any lower extremity arthroplasty is the restoration of a neutral mechanical axis, creating parallel joint lines in the hip, knee, and ankle." This ensures optimal load distribution across the prosthesis. The other options are incorrect goals; for example, a horizontal joint line may not be correct if there is pelvic obliquity, and matching a potentially deformed contralateral limb is not the goal.
Question 88
A surgeon is analyzing the provided radiograph for a patient with severe valgus knee arthritis. The angle labeled "mLDFA" is being measured. What does this angle represent?

View Answer & Explanation
Correct Answer: B
Rationale: The table and diagram define the mLDFA as the Mechanical Lateral Distal Femoral Angle. It is measured between the mechanical axis of the femur and the joint line of the distal femur. A normal value is 85-90°. Option A describes the MPTA (Medial Proximal Tibial Angle).
Question 89
A 71-year-old male has severe medial compartment osteoarthritis. His preoperative long-leg radiograph shows an MPTA of 80°. According to the provided text, this value indicates a deformity primarily located in the:
View Answer & Explanation
Correct Answer: B
Rationale: The normal range for the Medial Proximal Tibial Angle (MPTA) is 85-90°. An MPTA less than 85° (in this case, 80°) indicates a varus deformity originating from the proximal tibia. Option D is incorrect because a value less than 85° signifies varus, not valgus.
Question 90
A 69-year-old female with a severe valgus knee is shown. Her mechanical axis passes far lateral to the knee center. This finding on a long-leg radiograph is best described as:

View Answer & Explanation
Correct Answer: C
Rationale: The diagram and clinical context describe a valgus knee, where the mechanical axis (line from hip to ankle) falls lateral to the center of the knee joint. This is termed a lateral Mechanical Axis Deviation (MAD). Medial MAD (Option A) is seen in varus deformities.
Question 91
Planning a TKA on a short knee film in a patient with an unrecognized femoral diaphyseal deformity is described as a "recipe for catastrophic" failure. What specific postoperative complication is most directly caused by this planning error?
View Answer & Explanation
Correct Answer: D
Rationale: The text explicitly states, "Planning a TKA on a short knee film in a patient with an unrecognized diaphyseal deformity is a recipe for catastrophic joint line obliquity and severe mid-flexion instability post-operatively." The short film hides the extra-articular deformity, leading the surgeon to make incorrect intra-articular cuts that malorient the joint line.
Question 92
A 64-year-old male has a painful knee with a significant angular deformity. A long-leg radiograph is obtained, and the Joint Line Convergence Angle (JLCA) is measured. What does an abnormal JLCA with normal mLDFA and MPTA signify?
View Answer & Explanation
Correct Answer: C
Rationale: The table in the text specifies that an abnormal JLCA with normal mLDFA and MPTA indicates an intra-articular CORA. This means the source of the malalignment is within the joint itself (asymmetric wear, ligament issues) and not from the bones outside the joint. Option D is incorrect because an intra-articular CORA can typically be corrected with TKA alone.
Question 93
A 77-year-old female presents with the severe valgus deformity shown. Preoperative planning is being performed using Paley's principles. The normal range for the Mechanical Lateral Distal Femoral Angle (mLDFA) is:

View Answer & Explanation
Correct Answer: B
Rationale: The provided table of joint orientation angles clearly lists the normal range for the mLDFA as 85° to 90°. Values greater than 90° would indicate a valgus deformity originating in the femur, as is likely in this patient.
Question 94
A 63-year-old male has a varus knee deformity. His long-leg radiograph is analyzed. The Medial Proximal Tibial Angle (MPTA) is measured to be 88°. What is the clinical significance of this finding?
View Answer & Explanation
Correct Answer: C
Rationale: The normal range for the MPTA is 85-90°. A value of 88° falls squarely within this normal range, indicating that the proximal tibia is not the source of the patient's overall varus deformity. The surgeon must then look to the femur (mLDFA) or the joint space (JLCA) to find the CORA. Options A and B are incorrect because the angle is normal.
Question 95
A surgeon is performing a TKA on a patient with a severe intra-articular varus deformity. The bone cuts are made to reorient the joint surfaces. This process of realigning the limb via TKA is biomechanically analogous to what procedure?
View Answer & Explanation
Correct Answer: B
Rationale: The text's central theme is that a TKA for deformity is not simple resurfacing but rather an "intra-articular corrective osteotomy." The bone cuts are not just removing arthritic surfaces; they are strategically planned to change the alignment of the limb, which is the fundamental purpose of a corrective osteotomy.
Question 96
A 70-year-old female has a long-standing valgus deformity. Her long-leg radiograph shows an mLDFA of 96°, an MPTA of 92°, and a JLCA of 2°. Where are the CORAs for this patient's deformity located?
View Answer & Explanation
Correct Answer: D
Rationale: A normal mLDFA is 85-90°; 96° indicates femoral valgus. A normal MPTA is 85-90°; 92° indicates tibial valgus. The JLCA is normal (0-2°). Therefore, this patient has a complex deformity with two extra-articular CORAs, one in the distal femur and one in the proximal tibia. Option A is incorrect because the MPTA is also abnormal.
Question 97
A 45-year-old male undergoes a corrective osteotomy for a varus knee deformity. Postoperatively, his radiographs show perfect restoration of the mechanical axis. However, he continues to report significant fatigue with walking and demonstrates a persistent limp. According to the provided text, what is the most likely overarching reason for this discrepancy between radiographic success and functional outcome?
View Answer & Explanation
Correct Answer: B
Rationale: The text emphasizes that the true objective of deformity correction is the optimization of dynamic biomechanical function (gait), which extends beyond the restoration of static radiographic alignment. A persistent limp despite a corrected axis suggests an unaddressed dynamic or neuromuscular issue. While other options are possible complications, the core philosophy presented is that gait is the ultimate outcome.
Question 98
A 14-year-old female with a complex lower extremity deformity ambulates with a circumduction gait. The text states that such compensatory mechanisms are initiated by the body to adapt to structural malalignment. What is the primary negative consequence of these adaptations?
View Answer & Explanation
Correct Answer: C
Rationale: The text explicitly states that compensatory mechanisms, while clever, are "metabolically expensive." They "drastically increase energy expenditure, induce rapid fatigue, and impose pathologic, asymmetrical stress on adjacent joints." The other options describe the opposite of what occurs.
Question 99
A 50-year-old woman with severe coxa vara presents with a painful, lurching gait. Physical examination reveals a positive Trendelenburg sign. According to the principles described, this gait abnormality is a direct result of which biomechanical problem?
View Answer & Explanation
Correct Answer: C
Rationale: The text uses coxa vara as a classic example of a condition that causes a "significantly shortened" abductor muscle lever arm. This reduction in the lever arm requires the abductor muscles to generate a massively increased force to stabilize the pelvis, leading to fatigue, dysfunction, and a Trendelenburg gait. Lengthening the lever arm (B) would improve abductor efficiency.
Question 100
A surgeon is planning a derotational osteotomy for a patient with excessive femoral anteversion and a symptomatic in-toeing gait. The text suggests that the primary goal of this surgical intervention, in terms of muscle function, is to:
View Answer & Explanation
Correct Answer: D
Rationale: The text states, "While little can be done surgically to increase the intrinsic power generated by a muscle, the magnitude of the moment acting on the joint can be dramatically improved simply by correcting the lever arm dysfunction." A derotational osteotomy instantly restores the anatomical lever arm, allowing the muscle to function at optimal efficiency.
You Might Also Like
