Mastering Lower Limb Deformity, LLD & Biomechanics: ABOS Board Review | Part 2
Key Takeaway
This ABOS board review covers comprehensive lower limb deformity analysis, leg length discrepancy (LLD) management, and gait biomechanics. It details Shapiro's classification, Moseley graph, Paley Multiplier Method, and Paley's osteotomy rules for surgical correction, alongside TKA alignment principles. Essential for orthopedic exam preparation.
Question 1
A 6-year-old boy with congenital short femur presents for evaluation. Serial scanograms over the past 3 years show that his leg length discrepancy (LLD) has increased from 2.0 cm to 3.5 cm, with the percentage of growth inhibition remaining constant. According to Shapiro's classification, which pattern of LLD progression does this represent?
View Answer & Explanation
Correct Answer: A
Rationale: The vignette describes a discrepancy that increases at a constant, linear rate proportionate to the child's growth. This is the definition of a Shapiro Type 1 (Upward Slope) pattern, which is characteristic of congenital conditions like short femur. This is the only pattern accurately predicted by standard multiplier or graphing methods.
Question 2
A 10-year-old girl with a history of Juvenile Idiopathic Arthritis (JIA) in her right knee is evaluated for LLD. Initially, her right leg was longer due to hyperemia. Now, her right leg is shorter than her left, and the discrepancy is increasing. This complex progression, where an initial overgrowth is followed by premature physeal closure and relative shortening, is best described by which Shapiro pattern?
View Answer & Explanation
Correct Answer: E
Rationale: The clinical scenario of initial overgrowth (hyperemia) followed by premature physeal closure and subsequent shortening is the classic example of a Shapiro Type 5 pattern. The "downward slope" refers to the LLD decreasing after an initial period of increase (when the affected leg was longer).
Question 3
An 8-year-old boy is being followed for Legg-Calvé-Perthes disease of the left hip. His LLD initially increased due to femoral head collapse. For the past two years, the discrepancy has remained stable. However, you counsel the parents that premature arrest of the capital femoral physis is likely, which will cause the discrepancy to begin increasing again. This describes which Shapiro pattern?
View Answer & Explanation
Correct Answer: D
Rationale: Legg-Calvé-Perthes disease is the classic example of a Shapiro Type 4 pattern. It involves an initial increase in LLD (upward slope), a period of stabilization (plateau), and a subsequent increase in LLD due to premature physeal arrest (second upward slope).
Question 4
A 7-year-old boy sustained a femoral shaft fracture that was treated with flexible nails. The fracture healed with 1 cm of shortening. Over the next 4 years of follow-up, the LLD remains static at 1 cm, with both limbs growing at the same rate. This clinical course is an example of which Shapiro pattern of LLD progression?
View Answer & Explanation
Correct Answer: C
Rationale: This scenario describes an initial event causing a discrepancy (the fracture shortening), followed by a period where the affected and normal limbs grow at the same rate, causing the LLD to remain static. This is the definition of a Shapiro Type 3 (Upward Slope-Plateau) pattern.
Question 5
A pediatric orthopedic surgeon is using the Moseley straight-line graph to predict LLD at maturity for a child with fibular hemimelia. The surgeon notes that this method is only accurate for a specific type of LLD progression. For which Shapiro pattern are the Moseley, Amstutz, and Paley Multiplier methods most reliable?
View Answer & Explanation
Correct Answer: A
Rationale: All standard mathematical and graphical prediction methods are based on the assumption that the percentage of growth inhibition remains constant over time. This is only true for the Shapiro Type 1 (Upward Slope) pattern. Applying these methods to other patterns will lead to inaccurate predictions.
Question 6
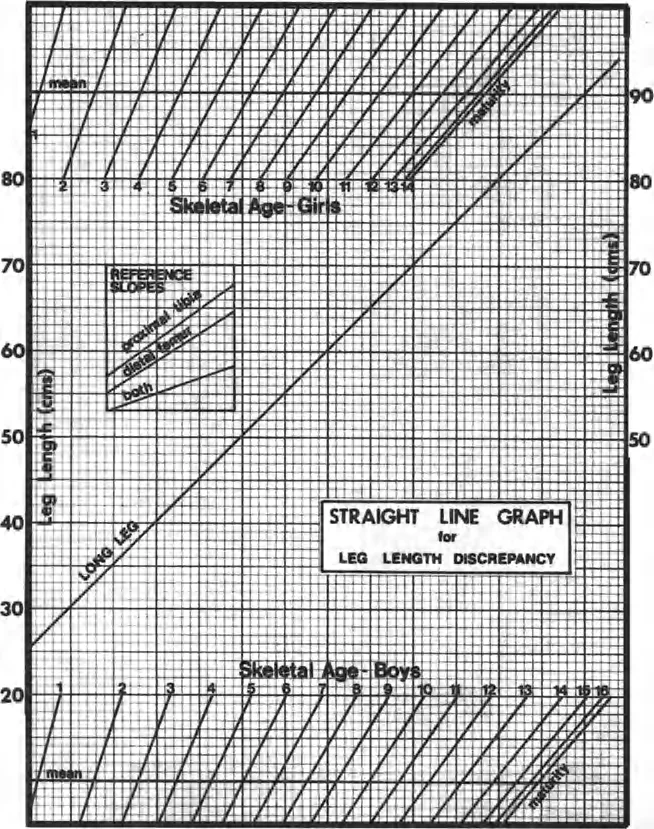
A 9-year-old boy with a 3 cm LLD is being evaluated. His surgeon uses the Moseley straight-line graph for prediction. The foundational genius of Moseley's graph is its ability to convert the normal S-shaped growth curve into a straight line. How is this accomplished?

View Answer & Explanation
Correct Answer: C
Rationale: Moseley's key insight was to create a nonlinear x-axis (age) where the physical distance between years is adjusted to reflect growth velocity. This manipulation forces the curved plot of normal growth into a straight 45° line, simplifying the prediction process for the affected limb.
Question 7
A resident is preparing to plot a patient's limb lengths on a Moseley straight-line graph for the first time. The attending surgeon emphasizes the importance of using the correct type of age for the x-axis to ensure accuracy, as recommended by Anderson and Green. Which type of age should be used?
View Answer & Explanation
Correct Answer: C
Rationale: The Moseley method's accuracy is highly dependent on biological maturity, not chronological time. Anderson and Green strongly recommended using skeletal age, typically determined from a left hand/wrist radiograph compared to the Greulich and Pyle atlas, for plotting on the x-axis.
Question 8
A 4-year-old girl presents to your clinic for the first time with a noticeable LLD due to hemihypertrophy. The parents are anxious and want to know the predicted discrepancy at maturity. You explain that the Moseley straight-line graph method has a significant limitation in this initial consultation. What is this primary limitation?
View Answer & Explanation
Correct Answer: C
Rationale: The Moseley graph relies on establishing the slope of the short leg's growth line. To accurately draw this line, a minimum of two, and preferably three, data points spaced over time (e.g., one year apart) are required. Therefore, it is not useful for prediction at the very first clinic visit.
Question 9
A 3-year-old boy presents with a 2.5 cm LLD from a congenital short tibia. The surgeon wishes to provide an immediate prediction of the LLD at maturity without waiting for serial radiographs. Which of the following methods was specifically developed to overcome the limitations of the Moseley graph and allow for prediction at the initial visit?
View Answer & Explanation
Correct Answer: B
Rationale: The Paley Multiplier Method was developed to simplify LLD prediction and eliminate the need for serial data, skeletal age determination, and complex graphing. It allows for an immediate prediction at the first clinic visit using the formula: Predicted LLD = Current LLD × Multiplier.
Question 10
A 5-year-old boy has a current LLD of 2 cm. Using the Paley Multiplier Method, the surgeon determines the multiplier for a boy of this age is 1.8. What is the predicted LLD at skeletal maturity?
View Answer & Explanation
Correct Answer: C
Rationale: The formula for the Paley Multiplier Method is: Predicted LLD at Maturity = Current LLD × Multiplier. In this case, 2 cm (Current LLD) × 1.8 (Multiplier) = 3.6 cm (Predicted LLD at Maturity).
Question 11
A 12-year-old girl is predicted to have a 4 cm LLD at skeletal maturity. Her predicted adult height is normal. According to the surgical decision-making matrix based on Paley's principles, what is the most appropriate intervention?
View Answer & Explanation
Correct Answer: B
Rationale: For a predicted LLD between 2 cm and 5 cm in a patient with adequate predicted height, a timed epiphysiodesis is the recommended treatment. This procedure halts the growth of the longer leg, allowing the shorter leg to "catch up" by the time of skeletal maturity.
Question 12
A 10-year-old boy is expected to have a 7 cm LLD at maturity. The family is concerned about him losing height. Which surgical option would best address the LLD while preserving or increasing his overall height?
View Answer & Explanation
Correct Answer: D
Rationale: For predicted discrepancies between 5 cm and 15 cm, limb lengthening is the preferred treatment. This technique involves an osteotomy and gradual distraction, which stimulates new bone formation (distraction osteogenesis) to make the shorter limb longer, thereby preserving the patient's final adult height.
Question 13
A 14-year-old boy presents with a fixed LLD of 1.5 cm. He is asymptomatic but his mother is concerned. He is approaching skeletal maturity. What is the most appropriate management for this patient?
View Answer & Explanation
Correct Answer: C
Rationale: A predicted LLD of 0-2 cm is generally well-tolerated and does not cause significant biomechanical alterations. The recommended intervention is non-operative, with a shoe lift used as needed for comfort or to address minor symptoms. Surgical intervention is typically not warranted for discrepancies of this magnitude.
Question 14
A 9-year-old boy has a short tibia with a significant varus deformity. Standing long-leg films show a mechanical axis deviation (MAD) medially and an abnormal medial proximal tibial angle (MPTA). The surgeon plans a limb lengthening procedure. To correct both the LLD and the angular deformity simultaneously, the osteotomy should ideally be performed at what location?
View Answer & Explanation
Correct Answer: D
Rationale: According to Paley's principles of deformity correction, when length and angular deformities coexist, the corrective osteotomy should be performed at the CORA. This allows for simultaneous correction of length through distraction and angulation through hinging of the fixation device, restoring a neutral mechanical axis.
Question 15
A surgeon is planning a distal femoral epiphysiodesis for a boy who needs to have 2 cm of growth arrested. Using the "rule of thumb" for growth, approximately how much does the distal femoral physis contribute to longitudinal growth per year?
View Answer & Explanation
Correct Answer: D
Rationale: The "rule of thumb" for growth states that the distal femur grows approximately 10 mm/year (or 1 cm/year). The proximal tibia grows at about 6 mm/year. Therefore, to arrest 2 cm of growth, the epiphysiodesis should be performed about 2 years before skeletal maturity.
Question 16
The foundational longitudinal data that underpins both the Moseley straight-line graph and the Amstutz arithmetic method was meticulously collected and published in 1964. This seminal work was authored by which group of researchers?
View Answer & Explanation
Correct Answer: E
Rationale: The text explicitly states that all historically validated methods of predicting LLD are built upon the monumental longitudinal data published by Anderson, Green, and Messner in 1964. This data provides the baseline "normal" growth curves against which pathological limbs are compared.
Question 17
A 7-year-old boy with fibular hemimelia has a significant LLD and a valgus ankle. The surgeon plans a tibial lengthening. According to the provided surgical pearls, what critical associated problem must be addressed before or during the lengthening to prevent a catastrophic complication?
View Answer & Explanation
Correct Answer: C
Rationale: A key surgical pearl is to "Always check the joints." In fibular hemimelia, the ankle is often unstable and in equinovalgus. Lengthening a limb without stabilizing the adjacent joint can lead to progressive subluxation or dislocation, which is a catastrophic complication.
Question 18
In the context of pediatric deformity, the text emphasizes a "critical fourth dimension" that surgeons must account for, which is absent in adults with static bone morphology. What is this fourth dimension?
View Answer & Explanation
Correct Answer: D
Rationale: The text explicitly states, "...when dealing with the pediatric population, orthopedic surgeons must account for a critical fourth dimension of deformity: Time." This refers to the fact that active physes cause deformities to change and progress as the child grows, unlike in adults.
Question 19
The Amstutz arithmetic method for predicting LLD is based on a key clinical observation about congenital deformities. What is the fundamental principle of this method?
View Answer & Explanation
Correct Answer: B
Rationale: The Amstutz method is built on the principle that for Type 1 progressions (common in congenital LLD), the affected limb grows at a constantly inhibited rate compared to the normal limb. Therefore, the ratio of the short leg length to the long leg length remains constant, allowing for arithmetic prediction.
Question 20
A 1-year-old boy is evaluated for proximal femoral focal deficiency (PFFD), with a predicted LLD greater than 20 cm at maturity. According to the provided surgical decision-making matrix, which of the following is a primary treatment consideration for a discrepancy of this magnitude?
View Answer & Explanation
Correct Answer: D
Rationale: The table indicates that for a predicted LLD greater than 15 cm, the discrepancy is too severe for a standard lengthening. The primary treatment options become multi-stage lengthening procedures spread across childhood or consideration of an amputation and prosthetic fitting to achieve a functional limb.
Question 21
A 13-year-old boy with a syndromic condition has a significant LLD. His chronological age is 13, but he is short for his age and has delayed puberty. The surgeon plans to use the Moseley graph for surgical planning. What is the most critical piece of information to obtain to ensure an accurate prediction?
View Answer & Explanation
Correct Answer: B
Rationale: The surgical pearl emphasizes that in patients with syndromic conditions, chronological age is often useless for growth prediction. Skeletal age, determined from a bone age radiograph, reflects the true biological maturity of the physes and is essential for accurate timing of interventions using methods like the Moseley graph.
Question 22
When evaluating a long-leg standing radiograph for deformity analysis, surgeons assess joint orientation angles to plan correction. The normal angle for the medial proximal tibia, which is a key target during deformity correction, is approximately what value?
View Answer & Explanation
Correct Answer: C
Rationale: The text mentions that a goal of deformity correction is restoring a normal Medial Proximal Tibial Angle (MPTA) of 87°. This angle, along with the mLDFA, defines the orientation of the knee joint relative to the mechanical axes of the tibia and femur.
Question 23
A 2-year-old girl is seen for the first time with fibular hemimelia. The parents ask for a prediction of the final LLD. The surgeon explains that both the Amstutz and Moseley methods have a major drawback when used for patients this young. What is this shared limitation?
View Answer & Explanation
Correct Answer: C
Rationale: The text explicitly states that a major drawback of both the Amstutz and Moseley methods is their inapplicability for infants and reduced reliability in very young children. This is a significant limitation as many congenital deformities present in infancy.
Question 24
A 9-year-old girl with a history of a physeal injury to her distal femur now has a 2 cm LLD and a progressive valgus deformity. This combined deformity is a direct result of an insult to which structure?
View Answer & Explanation
Correct Answer: D
Rationale: The physis is the biological engine for longitudinal growth. An asymmetrical insult, such as a physeal bar, will impair growth on one side, leading to both progressive shortening (LLD) and progressive angular deformity (valgus or varus).
Question 25
A 58-year-old male with a history of knee osteoarthritis presents with anterior thigh pain and a feeling of instability when walking. Examination reveals a 10° fixed flexion deformity (FFD) of the knee. During the stance phase of his gait, what is the most likely position of the Ground Reaction Vector (GRV) relative to his knee joint center?
View Answer & Explanation
Correct Answer: B
Rationale: In a knee with an FFD, the joint cannot achieve full extension. This forces the GRV to pass posterior to the knee joint center throughout the entire stance phase, generating a continuous flexion moment that must be counteracted by constant quadriceps firing. Option A describes a normal knee in mid-to-terminal stance.
Question 26
A 25-year-old physical therapy student is analyzing normal gait. She observes that during mid-stance, the tibia advances smoothly over the plantigrade foot. This action is characteristic of which mechanical rocker of the stance phase?
View Answer & Explanation
Correct Answer: B
Rationale: The second rocker, or ankle rocker, occurs during mid-stance. It is defined by the tibia advancing over the fixed, plantigrade foot, with the ankle joint acting as the fulcrum. This phase is critical for energy-efficient forward progression. The first rocker is at heel strike, and the third rocker is at toe-off.
Question 27
A 45-year-old male with a post-traumatic ankle arthrodesis in neutral position undergoes pedobarographic analysis. The force-versus-time graph for the affected limb is compared to the normal contralateral limb. What finding is most expected on the affected side?
View Answer & Explanation
Correct Answer: B
Rationale: A stiff or fused ankle creates a mechanically disadvantaged limb. The central nervous system instinctively minimizes the time spent weight-bearing on this limb to reduce pain and instability. This results in a quantifiable reduction in total stance time and an asymmetric gait. Stance time would not be increased (A) as this would prolong loading on the pathologic limb.
Question 28
A 62-year-old female presents with a 20° knee flexion deformity. On physical exam, she has a full passive range of motion of the knee joint from 20° to 110° of flexion. Full-length standing lateral radiographs are obtained. Which of the following radiographic findings would be most consistent with her clinical presentation?
View Answer & Explanation
Correct Answer: B
Rationale: The patient has a fixed flexion deformity but a normal arc of motion *within* the joint itself. This strongly suggests the deformity is extra-articular, located in the bone. An abnormal mPDFA would pinpoint the deformity to a procurvatum (anterior bowing) of the distal femur. If the angles were normal (A), the cause would likely be intra-articular or soft tissue, which contradicts the exam finding of a preserved motion arc.
Question 29
A 50-year-old long-distance runner develops a 15° knee flexion contracture after a hamstring injury. He complains of debilitating anterior thigh pain after walking only a few blocks. This pain is primarily due to the fatigue of which muscle group?
View Answer & Explanation
Correct Answer: C
Rationale: A 15° FFD forces the Ground Reaction Vector (GRV) to remain posterior to the knee joint throughout stance. This creates a constant flexion moment that must be counteracted by continuous, forceful firing of the quadriceps to prevent the knee from buckling. This relentless demand leads to rapid quadriceps fatigue and anterior thigh pain. The hamstrings (A) are the cause of the contracture but not the primary source of fatigue-related pain during gait.
Question 30
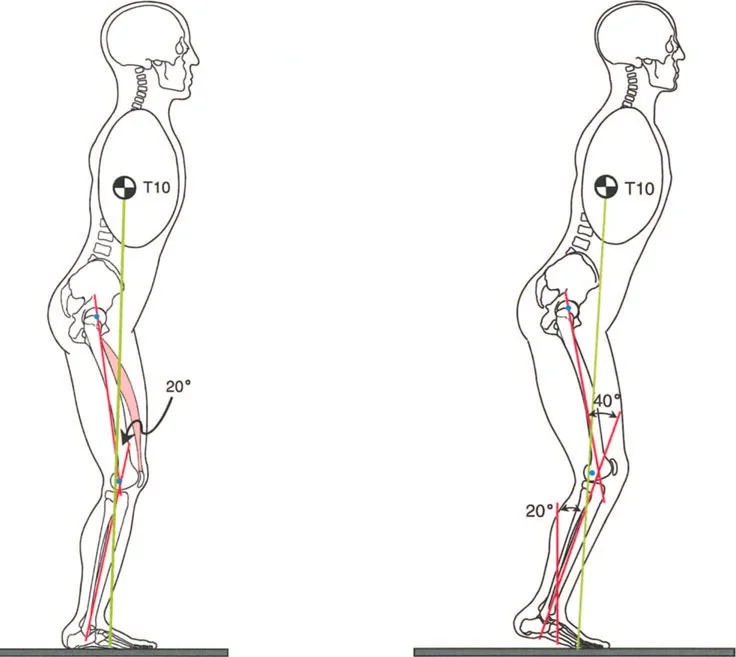
A 35-year-old patient with a chronic, untreated 40° knee flexion deformity is observed walking. Which compensatory gait pattern is most characteristic of this severe deformity?
View Answer & Explanation
Correct Answer: C
Rationale: A knee flexion deformity greater than 20° completely exhausts the ankle's compensatory dorsiflexion reserve (approx. 15-20°). To achieve a plantigrade foot would require more dorsiflexion than is available. Therefore, the heel is mechanically forced off the ground, resulting in an obligatory equinus posture. The patient walks on their toes ("toe-to-toe gait") to compensate for the severe functional limb shortening.
Question 31
A surgeon is planning a distal femoral extension osteotomy to correct a procurvatum deformity. During preoperative planning on a full-length standing lateral radiograph, they measure the angle between the femoral mechanical axis and the distal femoral joint line. What is the normal value for the mechanical posterior distal femoral angle (mPDFA)?
View Answer & Explanation
Correct Answer: C
Rationale: According to Paley's principles of deformity correction, the normal mechanical posterior distal femoral angle (mPDFA) is 83°. An angle less than this indicates a procurvatum (flexion) deformity of the distal femur. 81° (D) is the normal value for the mechanical posterior proximal tibial angle (mPPTA).
Question 32
An orthopedic surgeon identifies a simple, mid-diaphyseal procurvatum deformity of the femur. They plan to perform an osteotomy to correct the angulation. According to Paley's rules, how can pure angular correction be achieved without inducing any translation?
View Answer & Explanation
Correct Answer: C
Rationale: Paley's Rule 1 states that if the osteotomy and the hinge for angular correction are both located at the Center of Rotation of Angulation (CORA), the deformity will be corrected without creating any secondary translation. This results in perfect realignment of the mechanical axis. Option B describes Rule 2, which corrects the axis but intentionally creates translation at the osteotomy site.
Question 33
A 65-year-old male presents with difficulty walking and a crouched gait. On examination, he has a 20° knee flexion deformity. The surgeon is concerned about a co-existing hip flexion contracture. Which physical examination maneuver is essential to isolate and measure a hip flexion contracture?
View Answer & Explanation
Correct Answer: D
Rationale: The Thomas test is the classic and essential maneuver to assess for a hip flexion contracture (iliopsoas tightness). By maximally flexing the contralateral hip, the pelvis is locked in a neutral position, and the lumbar lordosis is flattened, revealing the true extension deficit of the hip being tested. The Prone Hang Test (A) and Popliteal Angle (B) assess the knee and hamstrings, respectively.
Question 34
A 40-year-old female is scheduled for an acute surgical correction of a severe, 35° post-traumatic knee flexion deformity via posterior capsulotomy and osteotomy. Which of the following is a critical prophylactic step to minimize the risk of iatrogenic nerve injury?
View Answer & Explanation
Correct Answer: B
Rationale: Acute correction of severe flexion deformities places the peroneal nerve under significant tension as it courses around the fibular head. Prophylactic decompression of the nerve at this site is highly recommended to reduce the risk of a traction neuropraxia or permanent palsy, which is a devastating complication. While SSEP monitoring (C) is useful, it is a monitoring tool, not a prophylactic surgical step.
Question 35
During a normal gait cycle, what is the primary biomechanical advantage of the Ground Reaction Vector (GRV) passing anterior to the knee joint center during mid-to-terminal stance?
View Answer & Explanation
Correct Answer: B
Rationale: When the GRV passes anterior to the knee joint in full extension, it creates a passive extension moment. This locks the knee in extension, allowing the massive quadriceps muscle to completely "turn off." Stability is provided passively by the posterior capsule and ligaments, which is a highly energy-efficient mechanism. A flexion moment (A) would require active muscle contraction to oppose it.
Question 36
A 28-year-old patient has an isolated paralysis of the gastrocnemius-soleus complex. During gait analysis, a deficit would be most pronounced during which phase, which is dependent on the eccentric contraction of this muscle group?
View Answer & Explanation
Correct Answer: C
Rationale: During mid-stance (the second rocker), the tibia advances over the foot. The eccentric contraction of the gastrocnemius-soleus complex is crucial for controlling the rate of this forward tibial progression. Without it, the tibia would advance too quickly, leading to knee instability. While the complex is also critical for concentric contraction at toe-off (D), its eccentric role is key to the second rocker.
Question 37
A 55-year-old woman with a 15° knee flexion deformity is observed to walk with a forward-leaning trunk and flexed hip. What is the primary biomechanical purpose of this postural compensation?
View Answer & Explanation
Correct Answer: C
Rationale: The FFD creates a persistent posterior GRV and a powerful knee flexion moment. By flexing the hip and leaning the trunk forward, the patient shifts their overall center of mass anteriorly. This is a desperate attempt to move the GRV more anteriorly, thereby reducing the flexion moment on the knee and lessening the extreme demand on the already fatigued quadriceps.
Question 38
A 38-year-old male presents with a severe, 40° knee flexion deformity following a crush injury. Based on the provided biomechanical diagram, what is the obligatory position of the ankle and hip required for him to maintain an upright posture?

View Answer & Explanation
Correct Answer: B
Rationale: The diagram (right figure) clearly illustrates that a 40° knee flexion deformity completely overwhelms the ankle's ability to dorsiflex. The heel is forced off the ground into an equinus position. To keep the trunk upright over the feet, the hip must adopt a compensatory flexion angle that is nearly equal to the knee flexion angle, in this case, 40°.
Question 39
A 14-year-old boy with cerebral palsy has a crouched gait with knee flexion and an equinus foot posture. On examination, his ankle dorsiflexion is limited to -10° with the knee extended, but improves to +10° with the knee flexed. What does this finding indicate?
View Answer & Explanation
Correct Answer: C
Rationale: This is the classic Silfverskiöld test. The gastrocnemius muscle crosses both the knee and ankle joints, while the soleus only crosses the ankle. When the knee is extended, the gastrocnemius is under tension, limiting dorsiflexion. When the knee is flexed, the gastrocnemius is relaxed, and if dorsiflexion improves, the contracture is isolated to the gastrocnemius. If it remained limited, it would indicate a combined or isolated Achilles/soleus contracture (A).
Question 40
An orthopedic surgeon is evaluating a 22-year-old patient with a complex multi-apical sagittal plane deformity of the femur and tibia. To accurately identify the CORA(s) and plan the necessary osteotomies, which radiographic study is most critical?
View Answer & Explanation
Correct Answer: C
Rationale: Comprehensive sagittal plane deformity planning requires visualization of the entire mechanical axis from the hip to the ankle. A full-length, standing lateral radiograph is the only study that allows for the drawing of the sagittal mechanical axes of the femur and tibia, measurement of joint orientation angles (mPDFA, mPPTA), and precise localization of the CORA.
Question 41
A 45-year-old patient has a severe, chronic 50° knee flexion contracture with associated skin changes and subjective paresthesias on examination. The surgeon is concerned about the neurovascular risk of an acute correction. What is the most appropriate surgical strategy?
View Answer & Explanation
Correct Answer: D
Rationale: For severe (>20-30°), chronic deformities, acute correction carries a massive risk of stretching the popliteal artery and peroneal/tibial nerves, leading to catastrophic complications. The safest method is gradual correction using a circular external fixator. An osteotomy is performed, and the deformity is corrected slowly (1 degree/day), allowing the soft tissues and neurovascular structures to accommodate safely.
Question 42
A surgeon is correcting a juxta-articular procurvatum deformity of the distal femur. The CORA is located in an area with poor bone quality, making fixation at that level impossible. The surgeon plans to perform the osteotomy more proximally in the diaphysis. To ensure the mechanical axis is perfectly restored, where must the hinge of the corrective device be placed?
View Answer & Explanation
Correct Answer: B
Rationale: This scenario describes Paley's Rule 2. When the osteotomy cannot be performed at the CORA, the mechanical axis can still be perfectly restored if the hinge of correction is placed at the CORA. This will intentionally create a translation of the bone fragments at the osteotomy site, but the final alignment of the limb will be correct.
Question 43
A 60-year-old male has a 12° fixed flexion deformity of his right knee. Compared to his normal left knee, the biomechanical consequence during the stance phase on the right side is a persistent flexion moment. This is caused by what alteration in the Ground Reaction Vector (GRV)?
View Answer & Explanation
Correct Answer: B
Rationale: The key to energy-efficient gait is allowing the GRV to pass anterior to the knee joint during mid-to-late stance, which creates a passive extension moment and allows the quadriceps to rest. A 12° FFD prevents the knee from ever reaching the full extension needed for this to occur. Thus, the GRV remains posterior to the joint center, creating the flexion moment.
Question 44
A 45-year-old male presents with progressive left knee pain. A full-length standing radiograph is obtained for deformity analysis. When defining the overall mechanical axis of the lower extremity, a line should be drawn connecting which two points?
View Answer & Explanation
Correct Answer: B
Rationale: The mechanical axis of the entire lower limb is the true load-bearing line and is defined by a straight line from the center of the femoral head to the center of the ankle joint. Option A describes a line related to the femoral anatomic axis proximally. Options D and E describe the individual mechanical axes of the femur and tibia, respectively, not the overall limb.
Question 45
A 22-year-old female sustains a mid-shaft femur fracture. During preoperative planning for an intramedullary nail, the surgeon identifies the anatomic axis of the femur. This axis is best described as a line that:
View Answer & Explanation
Correct Answer: C
Rationale: The anatomic axis is defined by the physical structure of the bone, specifically the mid-diaphyseal line or the center of the medullary canal. This is the axis around which intramedullary nails are designed. Option A describes the femoral mechanical axis. The femoral anatomic and mechanical axes are not collinear; they diverge.
Question 46
A 30-year-old patient has a varus deformity of the tibia. During preoperative planning, the surgeon draws both the anatomic and mechanical axes of the tibia. In the frontal plane, what is the typical relationship between these two axes in the tibia?
View Answer & Explanation
Correct Answer: C
Rationale: Unlike the femur, the tibia is a relatively straight bone. For all clinical and surgical planning purposes, the mechanical axis (center of knee to center of ankle) and the anatomic axis (mid-diaphyseal line) of the tibia are considered to be the same line (parallel and collinear). The 7-degree divergence (Option A) is characteristic of the femur.
Question 47
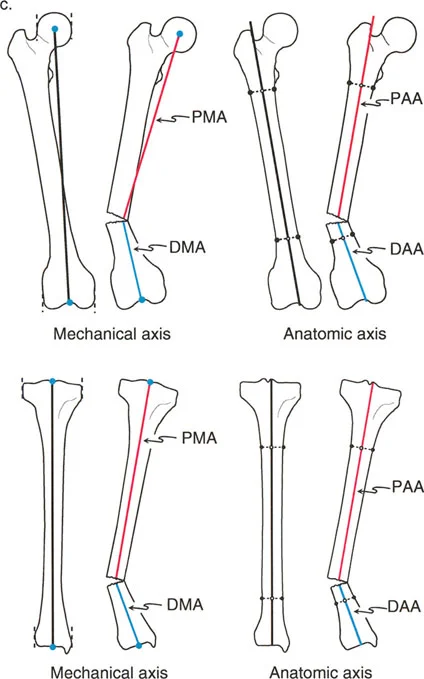
A 58-year-old female is being evaluated for a distal femur valgus deformity. The surgeon is explaining the difference between the femoral mechanical and anatomic axes. In the frontal plane, these two axes diverge by approximately how many degrees?
View Answer & Explanation
Correct Answer: C
Rationale: Due to the offset of the femoral head and neck, the mechanical axis (center of head to center of knee) and the anatomic axis (mid-diaphyseal line) of the femur are not parallel. They diverge by an average of 7 degrees (± 2°). This is a critical concept for distal femoral osteotomy planning.
Question 48
A 60-year-old male with a long-standing 15-degree varus tibial deformity presents with severe medial-sided knee pain and radiographic evidence of joint space narrowing. The underlying biomechanical principle explaining his condition is that the angular deformity has caused:
View Answer & Explanation
Correct Answer: B
Rationale: A varus (bow-legged) deformity shifts the mechanical axis of the limb medially. This deviation concentrates the load-bearing forces onto the medial compartment of the knee, leading to accelerated wear of the articular cartilage and premature osteoarthritis. Option C describes a valgus deformity. Option E is a consequence of the varus deformity, but the primary cause of the cartilage wear is the increased contact stress.
Question 49
A surgeon is planning an osteotomy for a 19-year-old with a femoral malunion. The surgeon draws the proximal mechanical axis and the distal mechanical axis on a radiograph. The point where these two lines intersect is known as the:
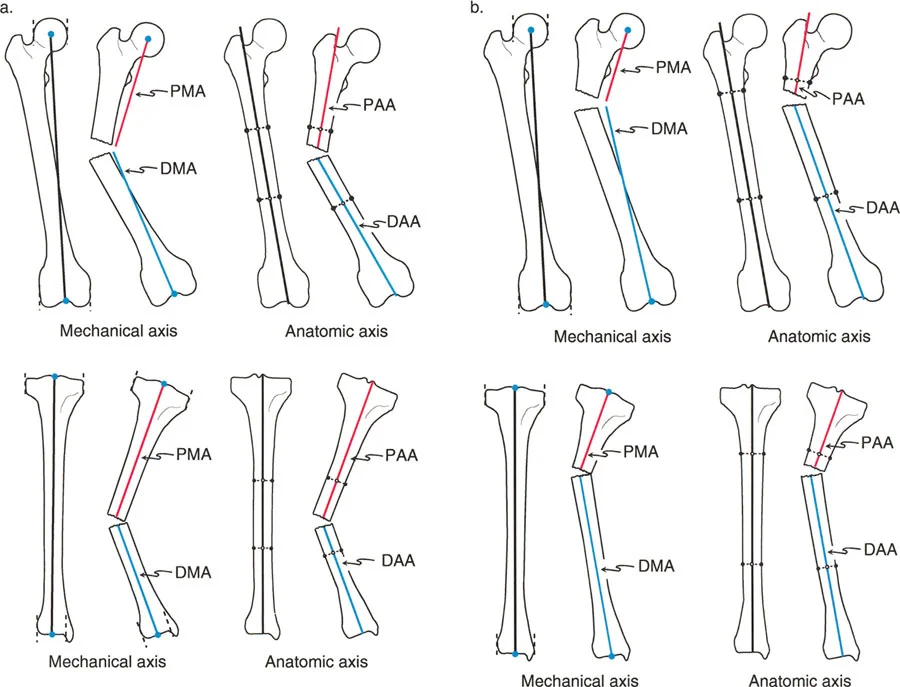
View Answer & Explanation
Correct Answer: A
Rationale: The Center of Rotation of Angulation (CORA) is the geometric point representing the apex of an angular deformity. It is precisely located at the intersection of the proximal and distal axes of the deformed bone. This point is the ideal location for the hinge of correction to avoid iatrogenic translation.
Question 50
A 25-year-old patient undergoes a tibial osteotomy for a varus malunion. The surgeon makes the bone cut 4 cm distal to the deformity's CORA and performs an angular correction without translation. Post-operative radiographs will most likely demonstrate:
View Answer & Explanation
Correct Answer: D
Rationale: According to Paley's Osteotomy Rules, if an osteotomy is performed at a level other than the CORA and a pure angular correction is applied, an iatrogenic translation (a "dog-leg" deformity) will be created. To avoid this, the osteotomy and the hinge of correction must both be at the CORA (Rule 1), or a planned translation must be added to the angular correction (Rule 2).
Question 51
During preoperative planning for a tibial deformity, a surgeon identifies the CORA by intersecting the proximal and distal mechanical axes. The angle formed at this intersection represents the:
View Answer & Explanation
Correct Answer: B
Rationale: The angle created by the intersection of the proximal and distal axes at the CORA is the mathematical representation of the true magnitude of the angular deformity. This angle dictates the amount of angular correction (e.g., the size of the opening or closing wedge) required to realign the bone.
Question 52
A 33-year-old male has a simple, uniapical varus deformity in the mid-diaphysis of his tibia. What is the most straightforward method to identify the CORA using anatomic axis planning?
View Answer & Explanation
Correct Answer: C
Rationale: For a pure diaphyseal deformity, anatomic axis planning is highly intuitive. The Proximal Anatomic Axis (PAA) is found by drawing a line through the middle of the proximal shaft, and the Distal Anatomic Axis (DAA) is found by drawing a line through the middle of the distal shaft. Their intersection point is the CORA.
Question 53
A surgeon is planning a correction for a valgus deformity located in the distal tibial metaphysis, 2 cm from the ankle joint. The primary challenge in drawing the distal axis line for this short juxta-articular segment is that:
View Answer & Explanation
Correct Answer: B
Rationale: When a deformity is very close to a joint (juxta-articular), the remaining bone segment is short and metaphyseal. It lacks a true diaphysis, making it impossible to accurately draw a mid-diaphyseal line. In these cases, the axis must be reconstructed by referencing the joint orientation line and using known angles (e.g., LDTA).
Question 54
A 40-year-old patient has a tibial deformity. The surgeon draws the anatomic axis of the distal tibia based on the mid-diaphyseal line, which appears straight. As a mandatory cross-check, the surgeon then measures the angle between this axis and the ankle joint line. This cross-check is known as the:
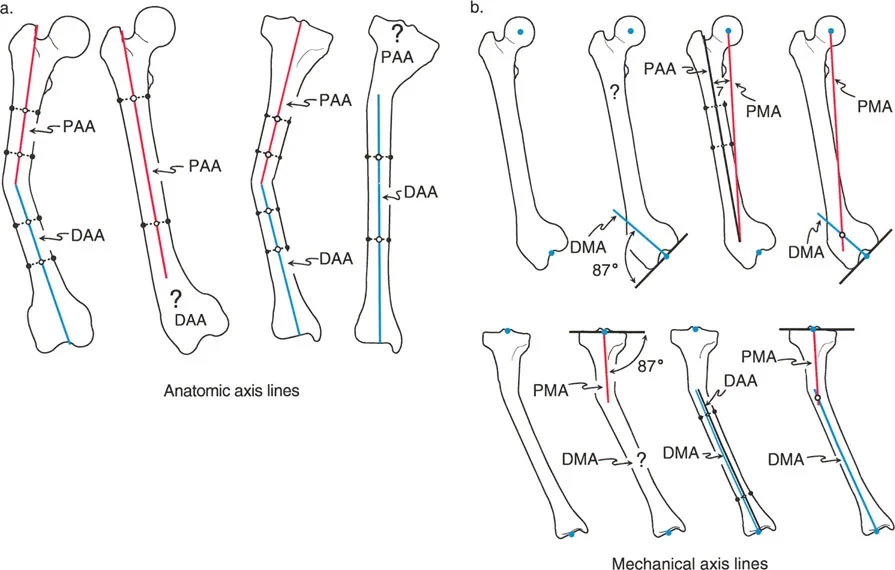
View Answer & Explanation
Correct Answer: B
Rationale: The Malorientation Test (MOT) is a critical step to ensure there is no hidden juxta-articular deformity. It involves measuring the joint orientation angle (like LDTA or MPTA) to confirm that the joint line is correctly oriented relative to its corresponding shaft axis. A normal-looking diaphysis can still have a maloriented joint.
Question 55
A surgeon performs a single-level osteotomy for a uniapical femoral deformity. The bone cut and the corrective hinge are both placed precisely at the CORA. According to Paley's Osteotomy Rule 1, the expected outcome is:
View Answer & Explanation
Correct Answer: C
Rationale: Paley's Osteotomy Rule 1 states that when the osteotomy and the hinge for correction are both located at the CORA, a pure angular correction is achieved. This restores the mechanical axis perfectly without creating any secondary translational deformity. The bone ends pivot perfectly around the apex.
Question 56
A 55-year-old female is undergoing planning for a corrective osteotomy. The surgeon measures the angle between the mechanical axis of the femur and the knee joint line on the lateral side. What is the normal average value for this angle, the mechanical Lateral Distal Femoral Angle (mLDFA)?
View Answer & Explanation
Correct Answer: B
Rationale: The normal average value for the mechanical Lateral Distal Femoral Angle (mLDFA) is 87° (range 85°-90°). This angle is a cornerstone of deformity planning around the knee. An angle less than 85° indicates valgus, while an angle greater than 90° indicates varus of the distal femur.
Question 57
A 28-year-old male presents with a proximal tibial varus deformity after a malunited fracture. During the Malalignment Test, the surgeon measures the angle between the mechanical axis of the tibia and the knee joint line on the medial side. The normal population average for this Medial Proximal Tibial Angle (MPTA) is:
View Answer & Explanation
Correct Answer: C
Rationale: The normal average value for the Medial Proximal Tibial Angle (MPTA) is 87° (range 85°-90°). This angle is critical for assessing proximal tibial alignment. An MPTA less than 85° indicates a varus deformity of the proximal tibia.
Question 58
A 42-year-old patient has a painful ankle deformity. As part of the workup, the surgeon measures the Lateral Distal Tibial Angle (LDTA). What is the accepted normal average value for the LDTA used in deformity planning?
View Answer & Explanation
Correct Answer: C
Rationale: The normal average value for the Lateral Distal Tibial Angle (LDTA) is 89° (range 86°-92°). While there is more population variability in this angle compared to knee angles, 89°-90° is the standard used for planning, especially when a contralateral template is unavailable.
Question 59
A 65-year-old male with hip pain is being evaluated. A full-length radiograph is obtained. The surgeon measures the angle between the mechanical axis of the femur and the hip joint line, which is defined by a line connecting the center of the femoral head to the tip of the greater trochanter. This angle is the Lateral Proximal Femoral Angle (LPFA). Its normal average is approximately:
View Answer & Explanation
Correct Answer: C
Rationale: The normal average value for the Lateral Proximal Femoral Angle (LPFA) is 90° (range 85°-95°). Similar to the LDTA, it has more population variability than the knee angles (mLDFA and MPTA).
Question 60
A 68-year-old female with severe knee varus has a full-length standing radiograph. The surgeon draws the distal femoral joint line and the proximal tibial joint line. The angle between these two lines is measured. This angle, which reflects ligamentous laxity or asymmetric cartilage wear, is the:
View Answer & Explanation
Correct Answer: D
Rationale: The Joint Line Convergence Angle (JLCA) is the angle between the femoral and tibial articular surfaces in the frontal plane on a weight-bearing radiograph. A normal JLCA is 0°-2°. An increased angle indicates either cartilage loss on one side (e.g., medial compartment in varus) or ligamentous laxity, causing the joint to "open up."
Question 61
A surgeon is planning a corrective osteotomy for a deformity near the knee. Due to the low population variability and reliability of the joint orientation angles in this region, the preferred reference line for drawing the mechanical axes of the distal femur and proximal tibia is the:
View Answer & Explanation
Correct Answer: C
Rationale: The mLDFA and MPTA have very little variability across the population. Therefore, the knee joint orientation line is the most reliable and preferred reference line for reconstructing the mechanical axes of the distal femur and proximal tibia during deformity planning.
Question 62
A 35-year-old has a proximal femoral varus deformity, but the femoral diaphysis is perfectly straight. When drawing the Proximal Mechanical Axis (PMA) of the femur, what is the preferred reference line, given the high variability of the LPFA?
View Answer & Explanation
Correct Answer: B
Rationale: Because the joint orientation angles at the hip (LPFA) and ankle (LDTA) have greater population variability, the preferred reference line is the adjacent mid-diaphyseal line, *if* a sufficient length of straight diaphysis is available. This provides a more patient-specific reference than a population average angle.
Question 63
A 35-year-old male presents for evaluation of lower limb alignment. When planning a full-limb deformity correction, the surgeon defines the mechanical axis of the entire lower limb. How is this axis correctly drawn on a full-length standing radiograph?
View Answer & Explanation
Correct Answer: B
Rationale: The mechanical axis of the entire lower limb is a fundamental reference line defined as a straight line from the center of the femoral head to the center of the ankle mortise. Option A describes the mechanical axis of the femur only. Option C describes the anatomic axes.
Question 64
A 45-year-old female with medial compartment knee osteoarthritis is being evaluated. Her full-length radiograph shows the mechanical axis of the lower limb passing 20 mm medial to the center of the knee. What is this finding called?
View Answer & Explanation
Correct Answer: C
Rationale: Mechanical Axis Deviation (MAD) is the measurement of how far the mechanical axis of the lower limb deviates from the center of the knee joint. Medial deviation indicates a varus deformity. JLCA refers to the angle between the knee joint lines, not the overall limb axis deviation.
Question 65
A surgeon is planning a distal femoral osteotomy and needs to assess the frontal plane alignment of the distal femur. The mechanical Lateral Distal Femoral Angle (mLDFA) is measured. What is the normal range for this angle?
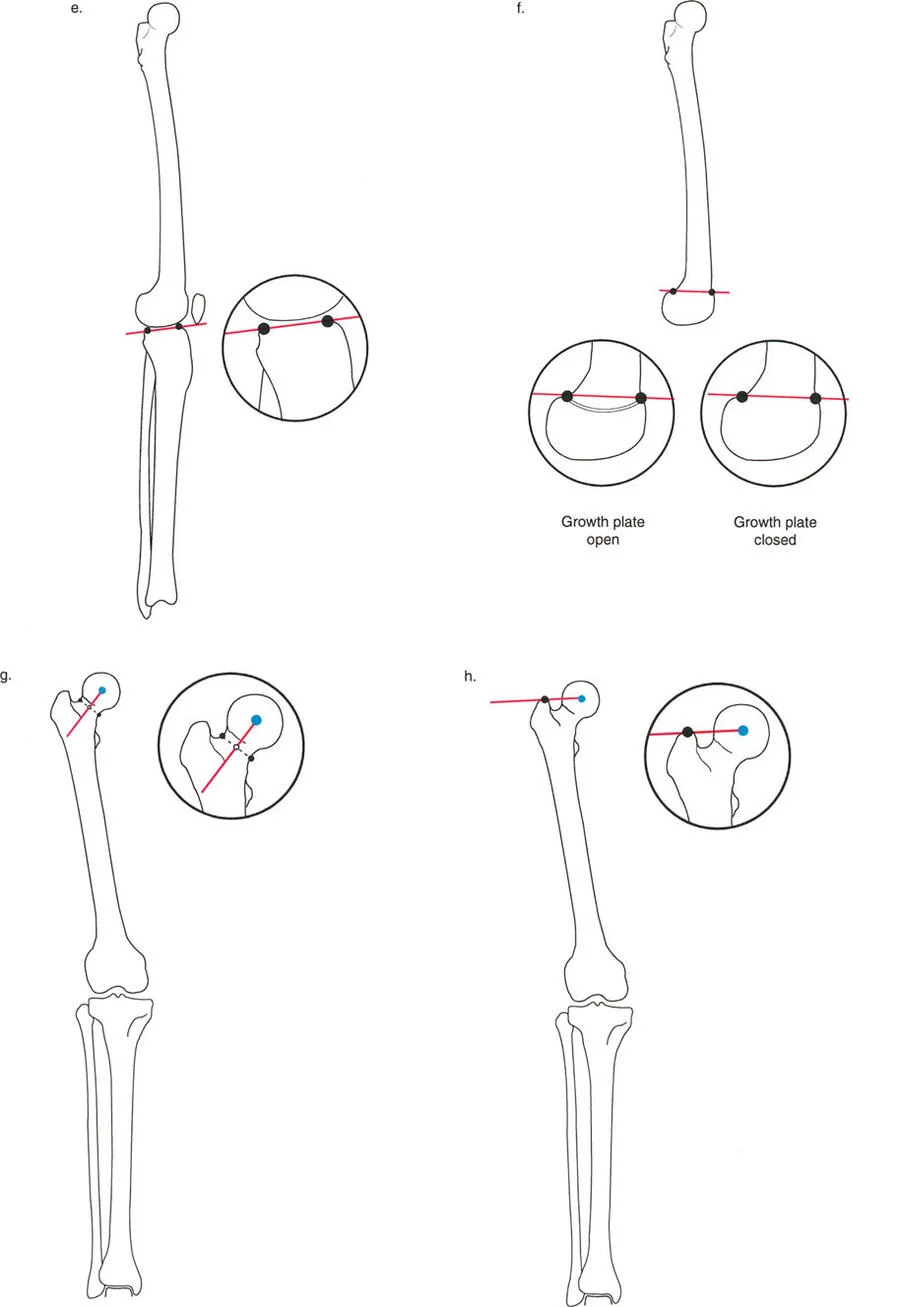
View Answer & Explanation
Correct Answer: B
Rationale: The normal mechanical Lateral Distal Femoral Angle (mLDFA) is 85° to 90°, with an average of 88°. This angle is critical for assessing distal femoral varus or valgus. Option A represents the normal PPTA, and option E represents the normal LDTA.
Question 66
A 22-year-old patient with a history of a tibial shaft fracture malunion presents with knee pain. Radiographic analysis reveals a Medial Proximal Tibial Angle (MPTA) of 82°. What deformity does this represent?

View Answer & Explanation
Correct Answer: B
Rationale: The normal MPTA is 85° to 90°. An MPTA less than 85° indicates tibia vara, which places increased stress on the medial compartment of the knee. Tibia valga would be represented by an MPTA greater than 90°.
Question 67
A 58-year-old male is undergoing a high tibial osteotomy (HTO) for medial compartment arthritis and a varus deformity. The preoperative MPTA is 80°. To offload the medial compartment, what is the typical target MPTA post-correction?
View Answer & Explanation
Correct Answer: D
Rationale: In an HTO for varus deformity, the goal is to correct the MPTA to a normal or slightly valgus alignment to shift the mechanical axis laterally. A common target is 89-90°, which slightly overcorrects the limb into valgus to effectively offload the diseased medial cartilage. Correcting to 87° would only restore neutral alignment, not provide the desired offloading effect.
Question 68
A resident is evaluating a lateral radiograph of the ankle to plan for a supramalleolar osteotomy. They draw a line from the distal tip of the posterior lip to the distal tip of the anterior lip of the tibia. What angle is measured using this line?
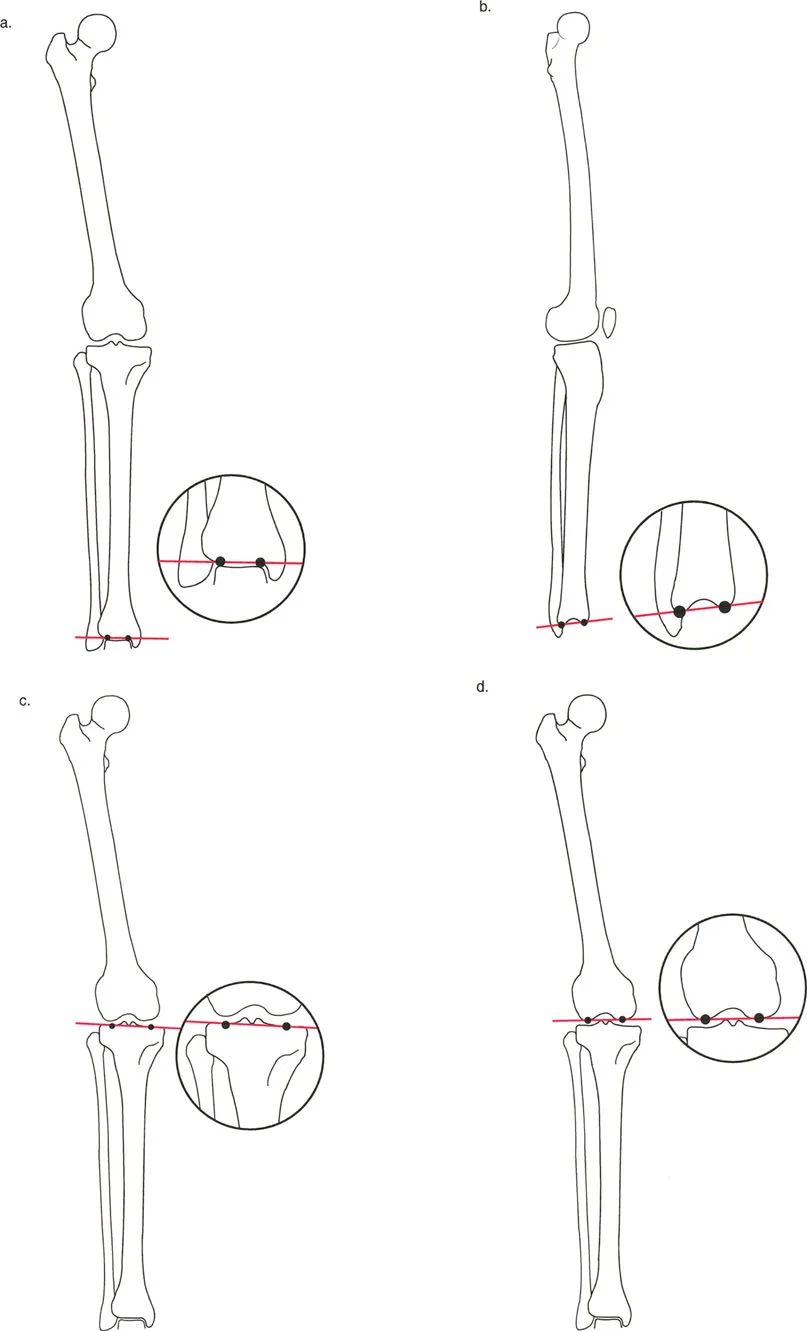
View Answer & Explanation
Correct Answer: B
Rationale: The Anterior Distal Tibial Angle (ADTA) is measured in the sagittal plane. The joint orientation line is drawn from the anterior to the posterior lip of the tibial plafond, and its angle with the tibial axis is the ADTA. The LDTA is a frontal plane measurement.
Question 69
A 28-year-old patient presents with anterior ankle impingement and limited dorsiflexion following a pilon fracture. A lateral radiograph reveals an Anterior Distal Tibial Angle (ADTA) of 88°. What deformity does this value indicate?

View Answer & Explanation
Correct Answer: B
Rationale: The normal ADTA is 78° to 82°. An increased ADTA (e.g., >85°) indicates a procurvatum deformity, where the distal tibia is angled excessively forward (anteriorly). This leads to anterior impingement. Recurvatum would be indicated by a decreased ADTA.
Question 70
During a preoperative planning session for a complex lower limb deformity, a fellow is asked to describe the anatomic axis of the femur. Which of the following is the correct definition?
View Answer & Explanation
Correct Answer: C
Rationale: The anatomic axis is defined as the mid-diaphyseal line of the bone. For the femur, this line is distinct from the mechanical axis (Option A) due to the offset of the femoral head and neck.
Question 71
A 60-year-old female with genu valgum is being evaluated. Her radiographs show a mechanical Lateral Distal Femoral Angle (mLDFA) of 82°. What is the primary deformity?
View Answer & Explanation
Correct Answer: B
Rationale: The normal mLDFA is 85° to 90°. An mLDFA less than 85° indicates a distal femoral valgus deformity (knock-knees). An mLDFA greater than 90° would indicate distal femoral varus.
Question 72
A surgeon is assessing the sagittal alignment of the knee in a patient with PCL insufficiency. Which measurement is most critical for evaluating the posterior tibial slope and its effect on the PCL?

View Answer & Explanation
Correct Answer: C
Rationale: The Posterior Proximal Tibial Angle (PPTA) is the measurement used to quantify the posterior tibial slope. A decreased slope (increased PPTA) places excessive strain on the PCL. The other angles measure alignment in different locations or planes.
Question 73
A 19-year-old athlete sustained an ACL tear. Preoperative planning includes a careful assessment of the posterior tibial slope. An increased posterior slope is a risk factor for ACL graft failure. Which of the following PPTA values would represent an increased posterior slope?
View Answer & Explanation
Correct Answer: D
Rationale: The normal PPTA is 77° to 84° (average 81°). The posterior slope is calculated as (90° - PPTA). Therefore, a lower PPTA value corresponds to a higher posterior slope. A PPTA of 75° would equate to a 15° slope, which is significantly increased and places greater strain on the ACL.
Question 74
A 65-year-old male with a painful hip has a radiograph showing a Neck-Shaft Angle (NSA) of 115°. What is the term for this condition, and what is a common clinical finding?
View Answer & Explanation
Correct Answer: B
Rationale: The normal NSA is 124° to 136°. An NSA less than 120° is termed coxa vara. This condition shortens the limb and decreases the efficiency of the abductor muscles by reducing their resting tension, which can lead to a Trendelenburg gait.
Question 75
A surgeon is evaluating a patient with abductor weakness after a proximal femur fracture fixation. The mechanical Lateral Proximal Femoral Angle (mLPFA) is measured to be 78°. What does this low mLPFA indicate?
View Answer & Explanation
Correct Answer: A
Rationale: The normal mLPFA is 85° to 95°. A decreased mLPFA indicates that the tip of the greater trochanter is positioned too high relative to the center of the femoral head. This high-riding trochanter reduces the articulotrochanteric distance (ATD) and leads to functional abductor weakness.
Question 76
According to Paley's principles, what is the first step in the "Malalignment Test" when evaluating a full-length standing AP radiograph of the lower extremities?
View Answer & Explanation
Correct Answer: B
Rationale: The Malalignment Test begins by drawing the primary reference line, which is the mechanical axis of the entire lower limb (center of hip to center of ankle). The position of this line relative to the knee determines if Mechanical Axis Deviation (MAD) is present, which then triggers further analysis.
Question 77
In deformity analysis, the Center of Rotation of Angulation (CORA) is a critical concept. How is the CORA identified on a radiograph?
View Answer & Explanation
Correct Answer: C
Rationale: The CORA is the geometric apex of a deformity. It is found by drawing the normal mechanical (or anatomic) axis of the proximal segment and the normal mechanical (or anatomic) axis of the distal segment of the deformed bone. The point where these two lines intersect is the CORA.
Question 78
A surgeon is planning a total knee arthroplasty (TKA) using a traditional Mechanical Alignment (MA) philosophy. What will the target mLDFA and MPTA be after the bone cuts are made?
View Answer & Explanation
Correct Answer: D
Rationale: The goal of traditional Mechanical Alignment TKA is to create a neutral mechanical axis for the limb. This is achieved by cutting both the distal femur and proximal tibia perpendicular (at 90°) to their respective mechanical axes, resulting in an mLDFA of 90° and an MPTA of 90°.
Question 79
A proponent of Kinematic Alignment (KA) for total knee arthroplasty (TKA) argues for restoring the patient's native joint line. What is the primary goal of KA regarding the mLDFA and MPTA?
View Answer & Explanation
Correct Answer: B
Rationale: Kinematic Alignment's philosophy is to resurface the knee by making bone cuts that restore the patient's pre-arthritic joint orientation lines (e.g., MPTA of ~87°, mLDFA of ~88°). This aims to preserve the natural ligamentous tension and knee kinematics, contrasting with Mechanical Alignment's goal of making both angles 90°.
Question 80
During radiographic evaluation for a varus knee, the surgeon measures the angle between the distal femoral joint line and the proximal tibial joint line. This angle is found to be 5°. What is this measurement called, and what does it signify?
View Answer & Explanation
Correct Answer: B
Rationale: The Joint Line Convergence Angle (JLCA) is the angle between the femoral and tibial joint lines. A normal JLCA is 0-2°. A widened JLCA (e.g., 5°) indicates that part of the deformity is intra-articular, due to factors like cartilage loss or ligamentous laxity, which must be considered during osteotomy planning.
Question 81
A surgeon is obtaining a full-length standing AP radiograph for deformity analysis. Why is it critical to ensure the patella is pointing straight forward during the imaging?
View Answer & Explanation
Correct Answer: B
Rationale: Rotational malalignment of the limb during radiography will project the three-dimensional anatomy onto a two-dimensional film in a distorted way. This can make angles like the mLDFA or MPTA appear falsely varus or valgus, leading to incorrect surgical planning. A patella-forward view standardizes the rotational position.
Question 82
When performing a medial opening wedge high tibial osteotomy, the surgeon places a hinge pin on the lateral cortex. To avoid inducing a secondary deformity in the sagittal plane, how should this hinge pin be oriented?
View Answer & Explanation
Correct Answer: B
Rationale: The axis of correction for an osteotomy is determined by the hinge. To achieve a pure uniplanar correction (e.g., only frontal plane correction), the hinge pin must be perfectly parallel to the joint orientation line. If the hinge is not parallel, it will induce an unwanted deformity in the orthogonal plane (e.g., altering the posterior slope).
Question 83
A 40-year-old patient has a varus ankle deformity. Preoperative planning on an AP radiograph shows a Lateral Distal Tibial Angle (LDTA) of 84°. What is the deformity, and what is the goal of a supramalleolar osteotomy (SMOT)?

View Answer & Explanation
Correct Answer: B
Rationale: The normal LDTA is 86° to 92°. An LDTA less than 86° indicates distal tibial varus. A supramalleolar osteotomy would aim to correct this by increasing the LDTA back into the normal range, typically around the average of 89°.
Question 84
In the tibia, what is the relationship between the anatomic axis and the mechanical axis?
View Answer & Explanation
Correct Answer: C
Rationale: Unlike the femur, the tibia is a relatively straight bone. Therefore, its mid-diaphyseal line (anatomic axis) and the line from the center of the knee to the center of the ankle (mechanical axis) are nearly identical and considered parallel for clinical purposes.
Question 85
A 68-year-old male with a history of a malunited mid-shaft femur fracture undergoes a total knee arthroplasty (TKR) using standard intramedullary guides. Postoperatively, his full-length radiograph shows a neutral mechanical axis, but he complains of severe instability and patellar subluxation. According to the principles outlined, what is the most likely underlying cause of his implant failure?
View Answer & Explanation
Correct Answer: C
Rationale: The text explicitly states that attempting to correct an extra-articular deformity (like a mid-shaft malunion) solely with intra-articular cuts creates a new translation deformity, leading to severe ligamentous imbalance and patellofemoral maltracking, even if the overall mechanical axis is corrected.
Question 86
A 72-year-old female with severe, long-standing genu varum undergoes a TKR. Postoperatively, she experiences rapid medial polyethylene wear and recurrent effusions. Examination reveals persistent medial joint line tenderness. This pattern of failure is most characteristic of which uncorrected postoperative parameter?
View Answer & Explanation
Correct Answer: B
Rationale: The text states that failure to neutralize the MAD leads to eccentric loading. In a varus knee, a residual medial MAD overloads the medial compartment, causing accelerated eccentric polyethylene wear and clinical failure.
Question 87
A surgeon is planning a TKR for a patient with a severe valgus deformity. According to the Paley philosophy described, the bone cuts made during the joint replacement should be primarily considered as what?
View Answer & Explanation
Correct Answer: B
Rationale: The text emphasizes a paradigm shift where the surgeon must recognize that "the bone cuts made during joint replacement are, in essence, corrective osteotomies." They are geometric resections designed to realign the entire lower extremity.
Question 88
A 65-year-old male presents with severe bilateral genu varum and knee pain. A full-length standing radiograph is obtained for preoperative planning. What is the single most important radiographic measurement for quantifying the overall limb alignment and the severity of load-bearing disruption?

View Answer & Explanation
Correct Answer: D
Rationale: The text defines Mechanical Axis Deviation (MAD) as "the single most important radiographic measurement for quantifying overall limb alignment and assessing the severity of the load-bearing disruption."
Question 89
A 58-year-old patient with a history of Blount's disease presents for TKR evaluation. Preoperative analysis reveals the apex of their varus deformity is located in the proximal tibial metaphysis. What is the correct term for this geometric point?
View Answer & Explanation
Correct Answer: C
Rationale: The Center of Rotation of Angulation (CORA) is defined as the precise geometric point where the deformity originates, found at the intersection of the proximal and distal mechanical axis lines of the deformed bone.
Question 90
During preoperative planning for a complex TKR, the surgeon determines that the CORA of a patient's varus deformity is located at the joint line, resulting from severe medial compartment bone loss. Based on Paley's principles, what is the most appropriate surgical strategy?
View Answer & Explanation
Correct Answer: B
Rationale: The text clearly states that if the CORA is intra-articular (at or very near the joint line), the deformity can typically be corrected entirely through the standard intra-articular bone cuts and soft tissue releases of the arthroplasty.
Question 91
A 45-year-old patient with a varus malunion of the distal femur requires a TKR. The surgeon identifies that the CORA is located 8 cm proximal to the knee joint. What is the primary risk of attempting to correct the entire limb alignment solely through intra-articular TKR cuts?
View Answer & Explanation
Correct Answer: A
Rationale: The text warns that for an extra-articular CORA, correcting solely through intra-articular cuts is a critical error that "will create a new, secondary 'translation' deformity at the joint line, leading to severe ligamentous imbalance."
Question 92
A surgeon is evaluating a full-length standing radiograph of a patient with a valgus knee. The line from the center of the femoral head to the center of the ankle joint passes 25 mm lateral to the center of the knee. How is this finding properly described?

View Answer & Explanation
Correct Answer: B
Rationale: The text and accompanying diagram define a valgus deformity as the mechanical axis passing lateral to the knee center. The perpendicular distance is the Mechanical Axis Deviation (MAD). Therefore, this is a 25 mm lateral MAD.
Question 93
According to the provided text, what is the primary biomechanical goal of a TKR in relation to the Mechanical Axis Deviation (MAD)?
View Answer & Explanation
Correct Answer: B
Rationale: The text states, "In the context of standard arthroplasty, correcting the MAD to zero (or near-zero...) is the primary biomechanical goal." This ensures symmetric distribution of forces across the prosthesis.
Question 94
A 69-year-old female presents for a TKR with a severe varus deformity. Preoperative planning reveals a Mechanical Lateral Distal Femoral Angle (mLDFA) of 95 degrees. What does this measurement indicate?
View Answer & Explanation
Correct Answer: C
Rationale: The normal mLDFA is 85-90 degrees. An angle greater than 90 degrees indicates a varus deformity of the distal femur. This measurement is crucial for determining the source of the overall limb malalignment.
Question 95
During preoperative templating for a TKR, the Medial Proximal Tibial Angle (MPTA) is measured to be 80 degrees. The normal range is 85-90 degrees. This finding suggests the presence of what deformity?
View Answer & Explanation
Correct Answer: A
Rationale: The MPTA is measured on the medial side. A normal angle is 87 degrees. An angle less than 85 degrees (more acute) indicates a varus deformity originating from the proximal tibia.
Question 96
A surgeon performs an osteotomy for a diaphyseal deformity. The bone cut is made at the CORA, and the hinge of correction is also placed at the CORA. According to Paley's Rule 1, what is the expected result of this correction?
View Answer & Explanation
Correct Answer: C
Rationale: The text explicitly states Paley's Rule 1: "When the osteotomy (bone cut) is made exactly at the CORA, and the hinge of correction is also placed at the CORA, the deformity corrects with angulation only. There is no translation."
Question 97
A TKR is performed for a patient with a mid-shaft femoral malunion (extra-articular CORA). The surgeon corrects the overall limb alignment using only intra-articular cuts. This scenario, where the "osteotomy" (the TKR cuts) and the "hinge" (the joint space) are both located away from the CORA, is a clinical application of which of Paley's rules?
View Answer & Explanation
Correct Answer: C
Rationale: The text explains this exact scenario as an application of Rule 3: "When both the osteotomy (bone cut) and the hinge of correction are placed away from the CORA, a new, complex translational and angular deformity is inadvertently created."
Question 98
A 62-year-old female with a painful valgus knee is being evaluated for a TKR. What is the primary purpose of measuring the joint orientation angles, such as the mLDFA and MPTA, during preoperative planning?
View Answer & Explanation
Correct Answer: D
Rationale: The text states that by measuring the mLDFA and MPTA, "the surgeon can precisely determine how many degrees of the total deformity originate from the femur versus the tibia," which prevents errors like over-resecting one bone to compensate for a deformity in the other.
Question 99
A surgeon is planning a total hip arthroplasty (THA) in a patient with a proximal femoral deformity. Which joint orientation angle is most critical for planning the femoral neck cut and restoring global offset to optimize abductor tension?
View Answer & Explanation
Correct Answer: E
Rationale: The table of joint orientation angles clearly identifies the Lateral Proximal Femoral Angle (LPFA) as being "Critical for planning the femoral neck cut, restoring global offset, and optimizing abductor tension in THA."
Question 100
A 70-year-old male has a varus knee deformity. On his standing radiograph, the medial joint space is obliterated, while the lateral joint space appears widened. The angle formed by lines drawn across the distal femoral condyles and the tibial plateau is 4 degrees. What does this angle represent?
View Answer & Explanation
Correct Answer: B
Rationale: The Joint Line Convergence Angle (JLCA) is defined in the text as quantifying "intra-articular deformity arising from asymmetric cartilage loss or severe collateral ligament laxity." A value of 4 degrees is outside the normal 0-2 degree range, indicating significant intra-articular pathology.
You Might Also Like