Mastering Lower Extremity Deformity & Hip Pathology: Orthopaedic Board Review | Part 15

Key Takeaway
Lower extremity deformity correction in orthopaedics involves precise surgical planning using principles like the Center of Rotation of Angulation (CORA) and mechanical axis alignment. This includes managing conditions such as Slipped Capital Femoral Epiphysis (SCFE), septic hip sequelae, and rotational deformities through osteotomies and specialized fixation to restore biomechanics and limb function.
Question 1
A 26-year-old male has a distal femoral varus deformity. The surgeon plans to use an intramedullary nail. Due to the wide "bell-bottom" shape of the distal metaphysis, the surgeon is concerned about the nail migrating medially and leaving a residual varus. What adjunct fixation is used to prevent this?
View Answer & Explanation
Correct Answer: C
Rationale: The text specifically describes the use of Poller (blocking) screws for this purpose: "To prevent the nail from migrating in the wide distal metaphysis, surgeons must utilize Poller screws." These screws artificially narrow the canal and guide the nail to the desired central position.
Question 2
A surgeon is correcting a 15-degree valgus deformity in the distal femur using an intramedullary nail. To ensure the nail achieves a central position in the distal fragment and corrects the deformity, where should a Poller (blocking) screw be placed?
View Answer & Explanation
Correct Answer: B
Rationale: The text states that Poller screws should be "Placed on the concavity of the deformity." For a valgus deformity, the apex is medial, making the medial side the concavity. A screw placed here will block the nail from drifting medially and will force it laterally, thereby correcting the valgus.
Question 3
A 13-year-old obese male presents with a 4-month history of a painful limp. Radiographs of his left hip reveal a chronic Slipped Capital Femoral Epiphysis (SCFE). During preoperative planning for a corrective osteotomy, the surgeon defines a line from the center of the femoral head to the center of the ankle joint. What is this line called?
View Answer & Explanation
Correct Answer: B
Rationale: The mechanical axis of the lower extremity is defined as a straight line from the center of the femoral head to the center of the ankle. This axis is the cornerstone of lower extremity alignment analysis. The anatomic axis follows the mid-diaphyseal line of the femur.
Question 4
A surgeon is evaluating a 15-year-old female with a healed SCFE and persistent coxa vara. On a standing long-leg radiograph, the mechanical axis line passes 25 mm medial to the center of the knee joint. What does this measurement represent?
View Answer & Explanation
Correct Answer: C
Rationale: Mechanical Axis Deviation (MAD) is the quantified distance of the mechanical axis line from the center of the knee joint. A significant proximal femoral deformity, such as coxa vara from SCFE, will alter the limb's mechanical axis and induce a MAD.
Question 5
A 14-year-old boy undergoes preoperative planning for a proximal femoral osteotomy to correct a chronic SCFE deformity. The surgeon measures the lateral angle formed by the intersection of the femoral mechanical axis and a line from the tip of the greater trochanter to the center of the femoral head. The measured angle is 75 degrees. Which parameter has been measured?

View Answer & Explanation
Correct Answer: D
Rationale: The Mechanical Lateral Proximal Femoral Angle (mLPFA) is the lateral angle between the femoral mechanical axis and the proximal femoral joint line. A normal value is 85-95 degrees. A value of 75 degrees indicates significant mechanical varus (coxa vara).
Question 6
A 16-year-old patient with a healed, moderate SCFE has a measured Mechanical Lateral Proximal Femoral Angle (mLPFA) of 80 degrees. According to the provided text, what does this value indicate?
View Answer & Explanation
Correct Answer: C
Rationale: The normal range for the mLPFA is 85 to 95 degrees. An angle less than 85 degrees, such as the 80 degrees measured in this patient, indicates mechanical varus (coxa vara). An angle greater than 95 degrees would indicate mechanical valgus.
Question 7
During the analysis of a proximal femoral deformity on an AP radiograph, a surgeon measures the medial angle between the mid-diaphyseal line of the femur and the proximal femoral joint line. This angle is found to be 70 degrees. What is the normal value for this specific angle?

View Answer & Explanation
Correct Answer: A
Rationale: The angle described is the Anatomic Medial Proximal Femoral Angle (aMPFA). Its normal value is approximately 84 degrees (range 80-89 degrees). This measurement is useful for assessing the intrinsic deformity of the proximal femur, independent of distal deformities.
Question 8
A 14-year-old female presents with a chronic SCFE. Her radiographs demonstrate a classic deformity with a measured angle of 110 degrees between the femoral neck axis and the anatomic axis of the femoral shaft. Which parameter does this value represent?
View Answer & Explanation
Correct Answer: E
Rationale: The Neck Shaft Angle (NSA) measures the relationship between the femoral neck axis and the anatomic axis of the femoral shaft. A normal value is approximately 130 degrees. A value of 110 degrees indicates significant coxa vara, which is a hallmark of SCFE deformity.
Question 9
A 15-year-old boy with a severe, chronic SCFE presents with a profound lurching gait. Physical examination reveals a positive Trendelenburg sign. Which of the following radiographic measurements is most directly responsible for this biomechanical deficiency?

View Answer & Explanation
Correct Answer: D
Rationale: A decreased or negative Articular Trochanteric Distance (ATD), also known as a "high-riding trochanter," severely compromises the abductor muscle lever arm. This leads to abductor weakness, a positive Trendelenburg sign, and a lurching gait. The other parameters describe angulation but not the specific lever arm deficiency.
Question 10
In the Paley method of deformity analysis, what is the single most important step in planning a surgical correction for a proximal femoral deformity?
View Answer & Explanation
Correct Answer: C
Rationale: The text explicitly states, "Identifying the CORA is the single most important step in planning a deformity correction because its location dictates the entire surgical strategy, the choice of osteotomy level, and the expected outcome."
Question 11
A 12-year-old boy is diagnosed with an unstable, acute-on-chronic SCFE. According to the principles of deformity analysis described, where is the Center of Rotation of Angulation (CORA) for this deformity located?
View Answer & Explanation
Correct Answer: D
Rationale: In a classic SCFE, the femoral head remains in the acetabulum while the metaphysis displaces. The CORA, which is the intersection of the normal head/neck axis and the deformed neck axis, is therefore located precisely at the level of the proximal femoral physis.
Question 12
A surgeon is planning a corrective osteotomy for a chronic SCFE. They understand that the deformity is a complex, three-dimensional problem. What is the primary reason that a standard AP pelvis radiograph can be misleading when assessing the true deformity?
View Answer & Explanation
Correct Answer: B
Rationale: The text highlights that because SCFE involves external rotation of the femoral shaft relative to the head, a standard AP view does not show the true neck profile. A true AP of the femur (with internal rotation) or a cross-table lateral is required to unmask the full extent of the deformity.
Question 13
A resident is using the Paley box diagram to understand the three-dimensional nature of an SCFE deformity. The front wall of the box, representing the AP radiograph, primarily shows which components of the deformity?

View Answer & Explanation
Correct Answer: C
Rationale: The Paley box diagram analogizes the AP radiograph (coronal plane) to the front wall of the box. This view shows the "shadow" of the deformity in the superoinferior (SI) plane, revealing the SI components of angulation and translation.
Question 14
When analyzing a severe SCFE using the Paley box diagram concept, the side wall of the box represents the lateral radiograph (sagittal plane). Which components of the deformity are best visualized on this view?

View Answer & Explanation
Correct Answer: B
Rationale: The side wall of the box represents the lateral X-ray (sagittal plane). This view shows the anteroposterior (AP) components of the deformity, which typically include a significant apex anterior angulation and posterior displacement (translation) of the head relative to the neck.
Question 15
A 15-year-old has a chronic SCFE. Radiographic analysis reveals an apparent angulation of 10 degrees on the AP view and 30 degrees on the lateral view. According to the principles described, what is the relationship between these measured values and the true magnitude of the deformity?
View Answer & Explanation
Correct Answer: D
Rationale: The text states, "Crucially, the true magnitude of the deformity is always greater than what is measured on either individual X-ray." The true deformity exists in an oblique plane, and the AP and lateral views are merely its two-dimensional "shadows."
Question 16
A surgeon is planning a correction for an SCFE with a 30-degree angulation on the AP view (SI plane) and a 10-degree angulation on the lateral view (AP plane). Using the Pythagorean theorem as described in the text, what is the calculated true magnitude of the oblique plane angulation?

View Answer & Explanation
Correct Answer: C
Rationale: The text and accompanying diagram illustrate that the true angulation is calculated using the Pythagorean theorem on the component vectors. For the example given (which is slightly different from the question stem but illustrates the principle), an AP angulation of 30° and an SI angulation of 10° result in a true oblique angulation of 32° (sqrt(30^2 + 10^2) ≈ 31.6°).
Question 17
In the context of three-dimensional deformity correction, what is the geometric relationship between the Axis of Correction of Angulation (ACA) and the true plane of angulation?
View Answer & Explanation
Correct Answer: B
Rationale: The text explicitly states, "By geometric definition, the ACA is always perpendicular to the plane of true angulation." The ACA acts as the hinge pin around which the bone fragment is rotated to correct the deformity within its true plane.
Question 18
A surgeon is planning a capital realignment for a severe SCFE. They have correctly identified the CORA at the physis and calculated the ACA. According to Paley's Rule One, what is the ideal location for the osteotomy to achieve a perfect anatomic correction without secondary translation?
View Answer & Explanation
Correct Answer: D
Rationale: Paley's Rule One states that if the osteotomy is performed exactly at the CORA, the deformity will be corrected perfectly without any secondary translation. In SCFE, this means performing the osteotomy at the physis or immediate femoral neck base.
Question 19
A surgeon performs a corrective osteotomy for an SCFE precisely at the CORA, located at the base of the femoral neck. What is the primary and most feared risk associated with this specific osteotomy location?
View Answer & Explanation
Correct Answer: C
Rationale: The text warns that performing the osteotomy at the CORA (the anatomic ideal) "places the surgeon directly in the 'danger zone' of the femoral head's delicate blood supply (the medial femoral circumflex artery)," which carries a catastrophic risk of avascular necrosis (AVN).
Question 20
According to Paley's osteotomy rules, if a surgeon chooses to perform an osteotomy at a level different from the CORA (e.g., intertrochanteric), what must be done to achieve a correct final alignment?
View Answer & Explanation
Correct Answer: A
Rationale: Paley's Rule Two, described as the "pragmatic workhorse," states that if the osteotomy is performed at a level different from the CORA, the bone must still be rotated around an Axis of Correction of Angulation (ACA) that passes through the original CORA to achieve proper alignment.
Question 21
A 14-year-old boy with a chronic SCFE has a fixed external rotation deformity of his affected leg. During preoperative planning, the surgeon notes that the calculated Axis of Correction of Angulation (ACA) is inclined relative to the long anatomic axis of the femur. What is the direct surgical consequence of this inclination?

View Answer & Explanation
Correct Answer: B
Rationale: The text explicitly states that the inclination of the ACA relative to the femur's long axis means that failure to account for it will result in an unwanted rotational change. Therefore, "Proper surgical planning requires intentionally derotating the femur around its long axis as a calculated part of the correction."
Question 22
A 13-year-old female has a chronic SCFE. In this condition, what is the typical displacement pattern of the femoral neck (metaphysis) relative to the femoral head (epiphysis)?
View Answer & Explanation
Correct Answer: B
Rationale: The text clarifies a common misconception. The head remains in the acetabulum. It is the metaphysis (femoral neck) that displaces. The text states, "The metaphysis typically displaces anteriorly and superiorly while also externally rotating." This results in the head being in a relatively posterior and inferior position.
Question 23
A surgeon is reviewing the parameters for a normal proximal femur. What is the normal value range for the Neck Shaft Angle (NSA) in an adult?

View Answer & Explanation
Correct Answer: C
Rationale: The provided table and text state that a normal Neck Shaft Angle (NSA) in an adult is approximately 130 degrees, with a normal range of 124 to 136 degrees. An NSA below this range indicates coxa vara.
Question 24
A 16-year-old patient who had a previous SCFE pinning now presents with hip pain and impingement. Radiographs show a "high-riding trochanter." The vertical distance between the tip of the greater trochanter and the superior articular surface of the femoral head is measured to be -5 mm. What is the normal range for this measurement?
View Answer & Explanation
Correct Answer: D
Rationale: This measurement is the Articular Trochanteric Distance (ATD). The text and summary table indicate that a normal ATD is positive, typically 10 to 15 mm, meaning the trochanter is distal to the apex of the femoral head. A negative value indicates a significant biomechanical problem.
Question 25
A 9-year-old girl with a history of neonatal sepsis presents with a painless, lurching gait and a significant leg length discrepancy. Radiographs confirm the complete absence of the left femoral head and neck. What is the primary pathological event that leads to this condition?
View Answer & Explanation
Correct Answer: C
Rationale: The text explicitly states that untreated neonatal septic arthritis leads to "complete enzymatic and avascular destruction of the proximal femoral epiphysis," resulting in the absence of the femoral head and neck. The other options represent different pediatric hip pathologies not caused by neonatal infection.
Question 26
A 12-year-old boy with sequelae of right hip septic arthritis demonstrates a profound drop of the left side of his pelvis when standing on his right leg. His torso lurches to the right with each step. What is the fundamental biomechanical cause of this Trendelenburg gait?
View Answer & Explanation
Correct Answer: B
Rationale: The text explains that the foundation of normal hip biomechanics is the femoral head acting as a stable fulcrum. Its destruction eliminates this fulcrum, leading to superior migration of the femur, abductor incompetence, and the resultant Trendelenburg gait. The other options are not the primary cause in this specific pathology.
Question 27
A 15-year-old female with an "unhinged hip" from a childhood infection undergoes gait analysis. The superior migration of her proximal femur has rendered her abductor muscles slack and mechanically disadvantaged. This primarily affects which component of the hip's lever system?
View Answer & Explanation
Correct Answer: B
Rationale: The abductor lever arm extends from the femoral head (the fulcrum) to the greater trochanter (the point of muscle insertion). When the fulcrum is lost and the femur migrates superiorly, this lever arm becomes ineffective, and the muscles lose their resting tension, leading to functional incompetence.
Question 28
An 11-year-old boy with post-septic destruction of the right femoral head is observed walking. To prevent falling when he stands on his right leg, he instinctively lurches his torso laterally over the affected hip. What is the primary purpose of this compensatory maneuver?
View Answer & Explanation
Correct Answer: C
Rationale: The text describes the Trendelenburg gait as a compensatory maneuver that "shifts the center of gravity directly over the unstable femur to artificially balance the pelvis." This reduces the moment arm of the body weight, decreasing the need for abductor force that the patient cannot generate.
Question 29
A 14-year-old presents with severe pelvic instability and a 10 cm leg length discrepancy due to a destroyed left hip from infantile sepsis. Radiographs show the proximal femur articulating with the iliac wing. The inability of the abductor muscles to stabilize the pelvis is a direct result of:
View Answer & Explanation
Correct Answer: C
Rationale: The superior migration of the femur shortens the distance between the origin and insertion of the abductor muscles. This causes them to lose their resting tension, rendering them "slack, mechanically disadvantaged, and functionally incompetent."
Question 30
A 16-year-old patient with sequelae of neonatal septic arthritis of the right hip presents with right knee pain. A full-length standing radiograph is obtained. The diagram shown illustrates the patient's lower extremity alignment.

The image on the right demonstrates which of the following biomechanical phenomena?
View Answer & Explanation
Correct Answer: B
Rationale: The diagram on the right clearly shows the mechanical axis (line from the hip center to the ankle center) falling far medial to the center of the knee. This is the definition of medial Mechanical Axis Deviation (MAD), which creates a varus moment at the knee.
Question 31
A 22-year-old male with a history of a destroyed left hip from childhood infection now complains of progressive left knee pain and instability. His limb alignment is consistent with the diagram on the right.

The chronic varus force across the knee, as depicted, will most likely lead to which combination of secondary knee problems?
View Answer & Explanation
Correct Answer: C
Rationale: The text states that the varus moment leads to a "constellation of secondary problems," including stretching of the lateral collateral ligament (LCL) complex causing lateral laxity, and immense compressive forces on the medial femoral and tibial condyles, leading to medial compartment overload and osteoarthritis.
Question 32
A 19-year-old with a destroyed right hip from septic arthritis presents with worsening medial-sided right knee pain, especially with walking. On exam, he has a varus thrust at the knee during gait. What is the underlying biomechanical cause of his medial knee pain?
View Answer & Explanation
Correct Answer: B
Rationale: The lateral shift of the functional hip center causes the mechanical axis to deviate medially. This concentrates the load-bearing forces onto the medial compartment of the knee, causing overload, cartilage wear, and pain, which is consistent with the patient's symptoms.
Question 33
A surgeon is evaluating a full-length radiograph of a patient with post-septic hip destruction. The "functional hip joint" is identified as the unstable contact point between the proximal femur and the ilium. The mechanical axis is drawn. The resulting malalignment is best described as:
View Answer & Explanation
Correct Answer: B
Rationale: The text explains that the superior and lateral migration of the functional hip center causes the mechanical axis to fall far medial to the knee. This creates a massive varus moment, meaning the overall deformity originating from the hip malposition is a varus malalignment of the limb.
Question 34
A 17-year-old patient with a long-standing history of a destroyed left hip presents with a sensation of the knee "giving way" to the outside with each step. Physical examination reveals significant laxity with varus stress testing of the knee. This lateral knee instability is a direct consequence of:
View Answer & Explanation
Correct Answer: A
Rationale: The medial mechanical axis deviation creates a varus thrust during gait. This thrust acts as a "constant stretching force on the lateral collateral ligament (LCL) complex, leading to severe lateral laxity with every step."
Question 35
A 5-year-old child is diagnosed with complete destruction of the proximal femoral physis following neonatal septic arthritis. The surgeon is counseling the parents about the expected leg length discrepancy (LLD) at skeletal maturity. According to Shapiro's classification, which pattern of LLD progression is most typical for this type of large discrepancy from a complete epiphyseal arrest?
View Answer & Explanation
Correct Answer: A
Rationale: The text states that the Shapiro Type 1 pattern represents a "linear, predictable discrepancy, often seen in congenital hypoplasia or complete epiphyseal arrest," which is characteristic of the pathology described. While the text notes the LLD in septic hip is complex, the underlying physeal arrest component aligns best with Type 1.
Question 36
A pediatric orthopaedic surgeon is evaluating a 10-year-old with severe LLD from a destroyed hip. The discrepancy is noted to be progressive. The total LLD is a result of which two combined factors?
View Answer & Explanation
Correct Answer: B
Rationale: The text explicitly states that the severe, progressive LLD results from the "destruction of the proximal femoral growth plate (physis), combined with the continuous superior mechanical migration of the femur."
Question 37
A surgeon is using the Moseley straight-line graph to predict the LLD at maturity for a child with a complete distal femoral physeal arrest from trauma. This method is most accurate for which Shapiro pattern of LLD progression?
View Answer & Explanation
Correct Answer: A
Rationale: The text states, "Current methods for predicting LLD at skeletal maturity, such as the multiplier method or the Moseley straight-line graph, are primarily applicable to the Shapiro Type 1 proportionate progression pattern."
Question 38
When planning a limb lengthening for a child with post-septic hip destruction, why can't methods like the Moseley graph be used with absolute mathematical certainty?
View Answer & Explanation
Correct Answer: B
Rationale: The text explains that the LLD in this condition is complex, resembling a Type 2 pattern or a combination. It states, "Because types 2 through 5 have periods of acceleration or deceleration, they cannot always be predicted with absolute mathematical certainty."
Question 39
An orthopaedic resident is presenting a case of a 7-year-old with a complex limb deformity. The attending surgeon emphasizes that in addition to angular, rotational, and translational deformities, they must also consider the "fourth critical dimension of deformity." What is this fourth dimension?
View Answer & Explanation
Correct Answer: C
Rationale: The text explicitly states, "...in the growing child, there is a fourth critical dimension of deformity: time. The LLD changes over time, becoming gradually greater..."
Question 40
A surgeon is planning a corrective osteotomy for a femoral varus deformity. The proximal and distal mechanical axes of the deformed bone are drawn on a radiograph. The point where these two axes intersect is known as the:
View Answer & Explanation
Correct Answer: A
Rationale: The text defines the Center of Rotation of Angulation (CORA) as "the point where the proximal and distal anatomical (or mechanical) axes of a deformed bone intersect." This is the geometric center of the deformity.
Question 41
In the context of Paley's principles of deformity correction, where must an osteotomy be performed to achieve pure angular correction without inducing a secondary translational deformity?
View Answer & Explanation
Correct Answer: C
Rationale: This is the definition of Paley's Osteotomy Rule 1: "An osteotomy performed at the CORA allows for pure angular correction without any translation of the bone segments."
Question 42
A surgeon is planning an Ilizarov hip reconstruction for a patient with a completely absent femoral head and neck. Since there is no proximal anatomical landmark, a new functional hip center must be defined. This new center is strategically planned at the desired point of contact between the proximal femur and which pelvic structure?
View Answer & Explanation
Correct Answer: D
Rationale: The text states that the surgeon must define a new functional hip center by "determining the desired point of contact between the proximal femur and the lateral wall of the pelvis—specifically, the ischium." This creates the bony buttress.
Question 43
During preoperative planning for a pelvic support osteotomy, the surgeon defines a new hip center where the proximal femur will abut the ischium. What is the primary biomechanical goal of this strategic placement?
View Answer & Explanation
Correct Answer: B
Rationale: The text explains that this strategic placement "is the first step in creating a stable, bone-on-bone buttress to support the pelvis during the stance phase of gait," which is the core principle of the pelvic support osteotomy.
Question 44
A 35-year-old male undergoes a mid-diaphyseal derotational osteotomy of the femur for excessive anteversion. The surgeon performs the rotation around the anatomic axis of the femur. According to Paley's principles, what is the most likely iatrogenic consequence of this surgical maneuver?
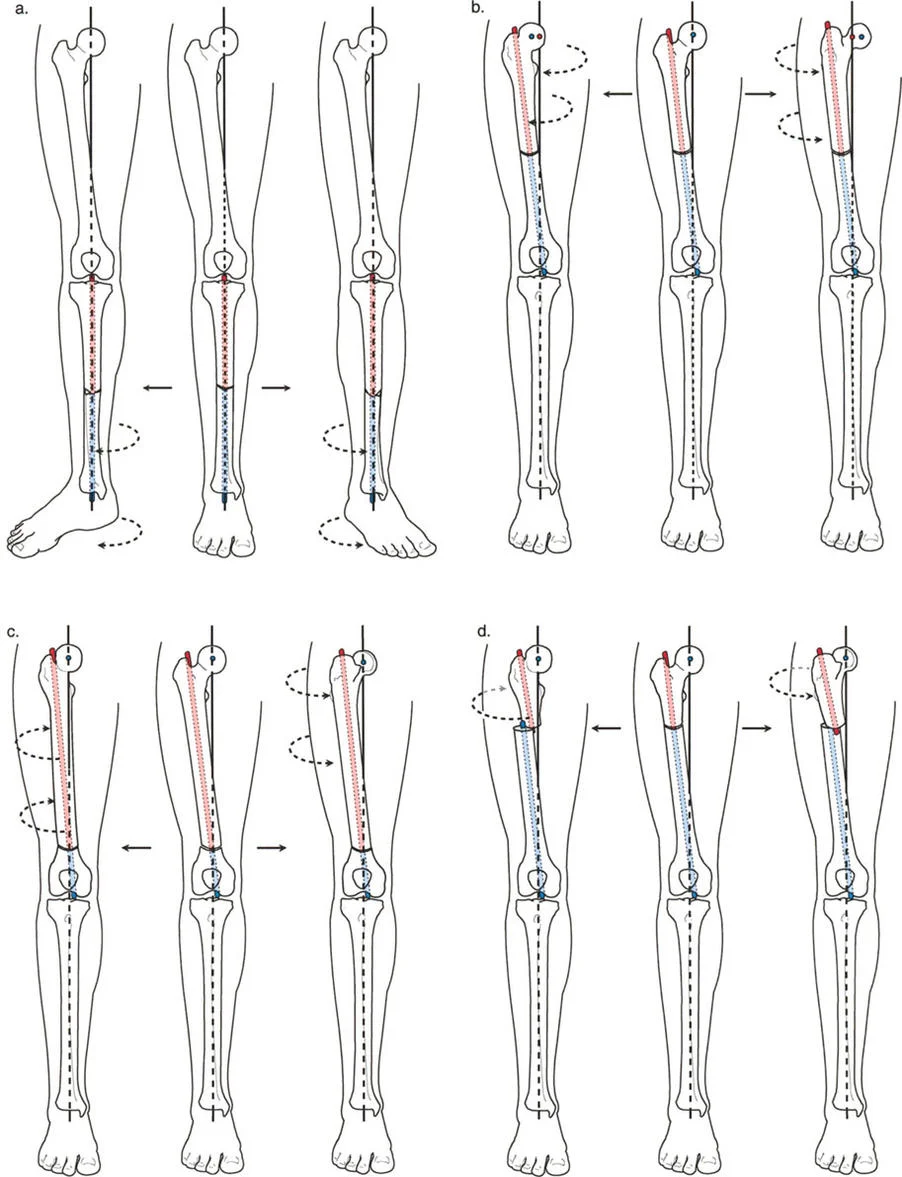
View Answer & Explanation
Correct Answer: B
Rationale: The anatomic and mechanical axes of the femur are not parallel. Rotating the femur around its anatomic axis causes the femoral head to swing medially or laterally, inducing an iatrogenic varus or valgus deformity, which is a form of Mechanical Axis Deviation (MAD). Rotation around the anatomic axis of the tibia (C) does not cause MAD because its axes are parallel.
Question 45
A 28-year-old female is undergoing a derotational osteotomy for symptomatic internal tibial torsion. The surgeon chooses a mid-diaphyseal location for the osteotomy and rotates the distal segment around the anatomic axis. What effect will this have on the lower limb's mechanical axis?

View Answer & Explanation
Correct Answer: D
Rationale: In the tibia, the anatomic and mechanical axes are essentially collinear and parallel. Therefore, a pure rotational osteotomy around the anatomic axis of the tibia does not displace the mechanical axis or produce any frontal plane deformity (MAD). This is in stark contrast to the femur.
Question 46
A surgeon is planning a femoral derotational osteotomy and wants to avoid inducing any mechanical axis deviation or significant fragment translation. Based on biomechanical principles, what is the ideal location and axis of rotation for this procedure?

View Answer & Explanation
Correct Answer: D
Rationale: The distal femur is the "sweet spot" for derotation because the mechanical and anatomic axes intersect in this region. Rotating around the mechanical axis in the distal femur is surgically practical, provides excellent bone contact, and does not induce MAD. Proximal rotation around the mechanical axis (B) is impractical due to massive translation, and diaphyseal rotation around the anatomic axis (C) causes MAD.
Question 47
A 15-year-old female presents with bilateral anterior knee pain and in-toeing gait. Her clinical examination reveals a foot progression angle of -15 degrees. Her hip rotation is 80 degrees internal and 10 degrees external. Her thigh-foot axis is measured at +5 degrees. What is the primary source of her in-toeing?
View Answer & Explanation
Correct Answer: D
Rationale: The clinical profile of significantly increased internal hip rotation (80 degrees) compared to external rotation (10 degrees) is the classic sign of increased femoral anteversion. The thigh-foot axis is normal, ruling out significant tibial torsion (A, B) as the primary cause of the in-toeing.
Question 48
A 17-year-old athlete presents with patellofemoral pain. On gait analysis, her foot progression angle is noted to be neutral (0 degrees). However, her clinical exam shows 75 degrees of internal hip rotation and 15 degrees of external rotation, and a thigh-foot axis of +35 degrees. This clinical picture is best described as:
View Answer & Explanation
Correct Answer: E
Rationale: Miserable malalignment syndrome is characterized by the combination of increased femoral anteversion (indicated by high internal hip rotation) and compensatory external tibial torsion (indicated by the high positive thigh-foot axis). These opposing deformities can neutralize the foot progression angle, masking the underlying pathology and making the gait appear deceptively normal in the axial plane.
Question 49
A resident is performing a clinical assessment for tibial torsion on a patient in the prone position with knees flexed to 90 degrees. They are measuring the angle between the long axis of the thigh and a line from the mid-heel through the second toe. What is this specific measurement called?
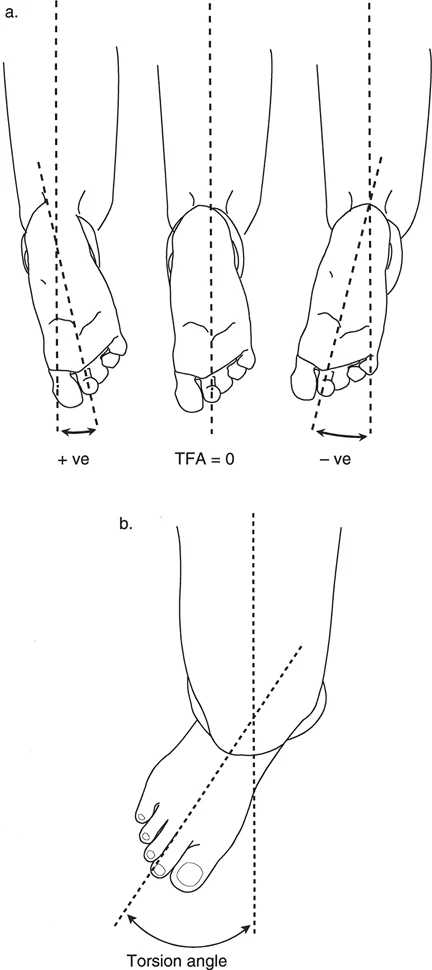
View Answer & Explanation
Correct Answer: C
Rationale: The thigh-foot axis (TFA) is the standard clinical measurement for tibial torsion performed with the patient prone and knees flexed. It quantifies the orientation of the foot relative to the thigh. The foot progression angle (A) is measured during gait.
Question 50
A 40-year-old male is being evaluated for a rotational deformity. During the standing examination, the surgeon manually orients the patient's patellae to face directly forward before assessing the angle of the feet. What is the primary purpose of this maneuver?
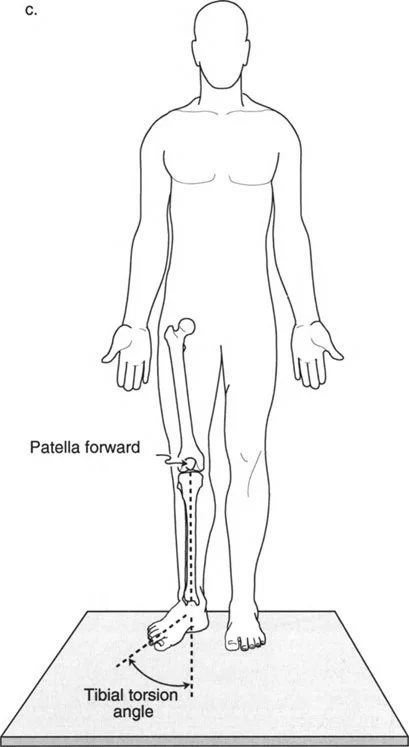
View Answer & Explanation
Correct Answer: B
Rationale: By fixing the knee's rotational position (patella forward), the surgeon effectively neutralizes the rotational influence of the femur. The resulting angle of the foot on the floor is therefore a direct clinical measure of the tibial torsion component of the limb's rotational profile.
Question 51
An orthopedic surgeon is assessing femoral version in a 20-year-old patient who has a 25-degree valgus deformity of the right tibia. The surgeon uses the shaft of the tibia as the vertical reference (plumb line) to measure hip rotation. How will the tibial valgus affect the perceived hip rotation measurements?
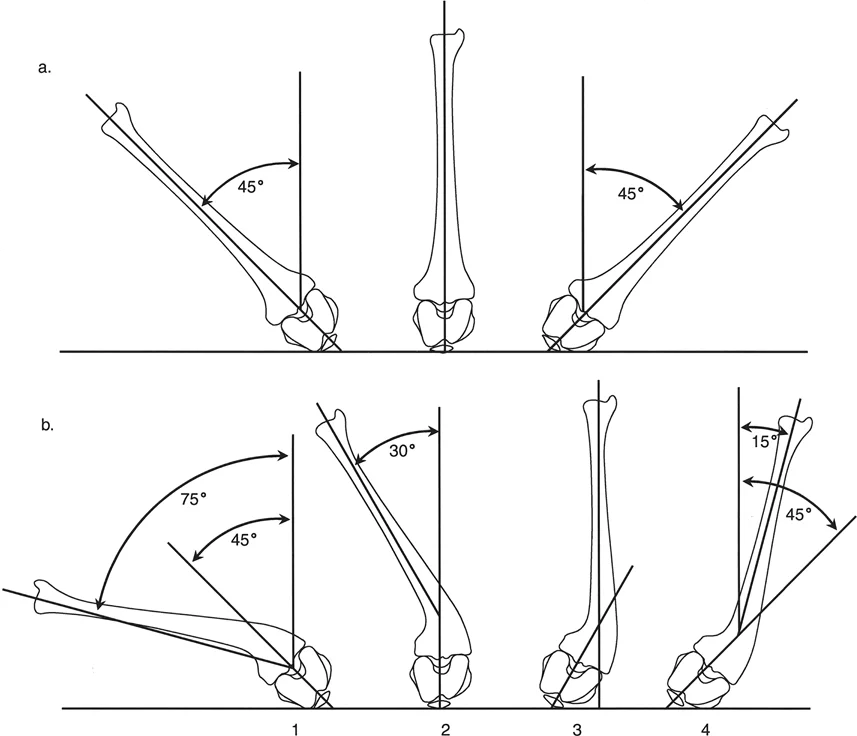
View Answer & Explanation
Correct Answer: A
Rationale: This scenario describes the "valgus/varus trap." A valgus tibia angles the lower leg outward. If the examiner incorrectly uses the tibial shaft as the vertical "zero" reference, the leg is already starting in a position of relative external rotation. This will lead to an underestimation (falsely decreased measurement) of the true internal rotation range and an overestimation of the external rotation range.
Question 52
To avoid the "valgus/varus trap" when clinically assessing femoral version in a patient with a tibial deformity, what is the most reliable method to establish the true zero-degree reference position for hip rotation?

View Answer & Explanation
Correct Answer: C
Rationale: The true zero position for assessing femoral rotation is defined by the femur itself, not the tibia. The most reliable clinical landmark is the patella, which should be pointed directly down at the examining table. This ensures the posterior femoral condyles are level and horizontal, establishing a true vertical reference for measuring hip rotation, regardless of any underlying tibial deformity.
Question 53
Which imaging modality is considered the gold standard for the precise quantification of femoral and tibial torsion?
View Answer & Explanation
Correct Answer: C
Rationale: Computed Tomography (CT) is the definitive modality for measuring rotational deformities. It eliminates the projectional errors inherent in plain radiography and provides exact, cross-sectional angular measurements of the femoral neck, femoral condyles, and tibial malleoli, which are necessary for accurate torsional profiling.
Question 54
A surgeon is planning a tibial derotational osteotomy for a 25-year-old patient and orders a CT scan. To measure tibial torsion, the angle between which two anatomical axes is calculated?
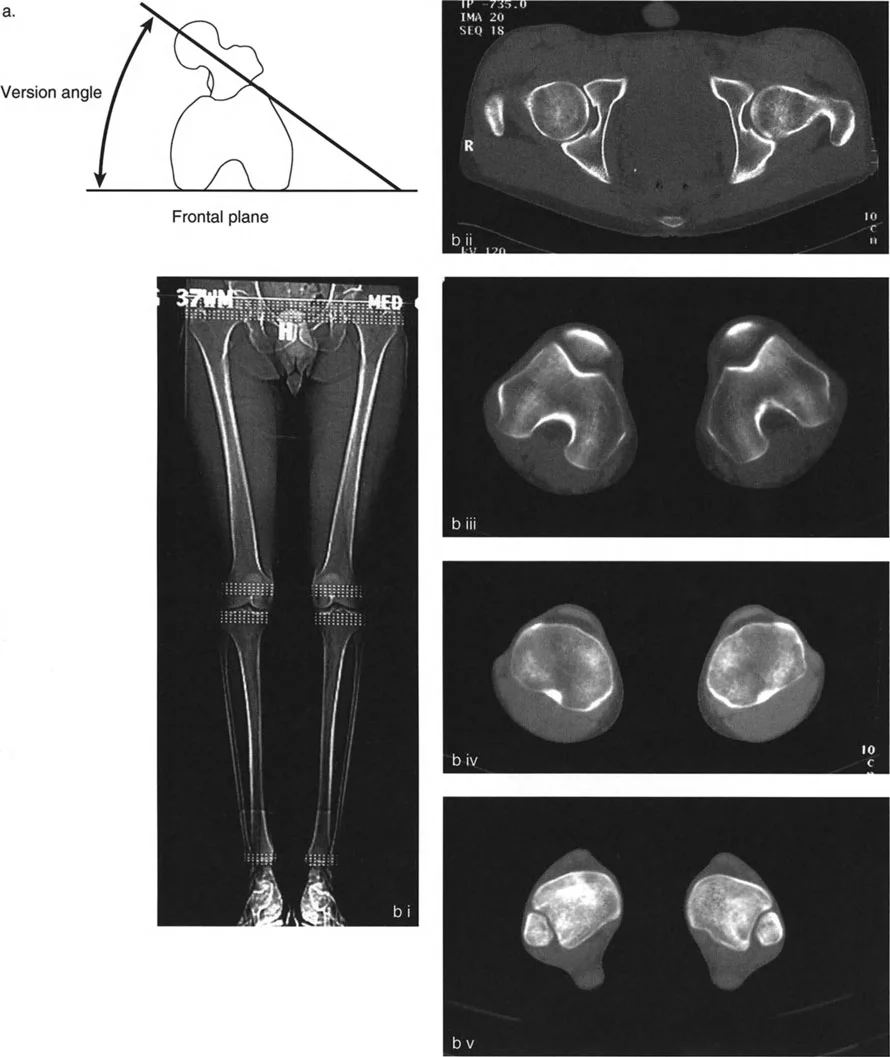
View Answer & Explanation
Correct Answer: C
Rationale: Tibial torsion is defined on CT as the angle between the axis of the proximal tibia (defined by the posterior aspect of the tibial condyles) and the axis of the distal tibia (defined by the transmalleolar axis, a line connecting the centers of the medial and lateral malleoli).
Question 55
According to the foundational normative data established by Strecker et al. using CT analysis, what is the approximate mean value for normal adult femoral anteversion?
View Answer & Explanation
Correct Answer: D
Rationale: The studies by Strecker et al. are the benchmark for CT-based torsional norms. They established the mean normal femoral anteversion in adults to be approximately 24.1 degrees. The mean normal external tibial torsion was found to be approximately 34.85 degrees (E).
Question 56
A 22-year-old is scheduled for a 30-degree external derotational osteotomy of the tibia. Which of the following is a mandatory adjunctive procedure to allow for this degree of correction and minimize the risk of non-union?
View Answer & Explanation
Correct Answer: D
Rationale: For tibial rotational corrections greater than 10-15 degrees, an intact fibula acts as a rigid tether, preventing the desired rotation and creating significant stress at the tibial osteotomy site, which increases the risk of non-union. A concurrent fibular osteotomy is therefore mandatory. While peroneal nerve decompression (C) is often considered for large external rotations, it is not as universally mandatory as the fibular osteotomy.
Question 57
During a tibial derotational osteotomy, after the bone is cut, the surgeon loses all reliable visual landmarks. What is the most crucial intraoperative step that should be performed *before* the osteotomy to ensure an accurate correction?
View Answer & Explanation
Correct Answer: B
Rationale: Placing two parallel reference pins (e.g., K-wires or Steinmann pins) proximal and distal to the planned osteotomy is the standard and most reliable method for intraoperative measurement. After the cut, the angle between these two pins directly and accurately reflects the amount of rotation that has been achieved.
Question 58
A surgeon is performing a 25-degree external derotation of the tibia. This maneuver places which neurovascular structure at the highest risk of a stretch injury?
View Answer & Explanation
Correct Answer: C
Rationale: The common peroneal nerve is at particular risk during external rotation of the tibia. As the tibia rotates externally, the nerve, which is tethered as it winds around the fibular neck, is stretched. Prophylactic decompression should be strongly considered for large corrections.
Question 59
A 19-year-old requires a derotational osteotomy of the femur. The surgeon is concerned about the biomechanical consequences of the osteotomy level. A rotation performed around the mechanical axis in the proximal femur is considered surgically impractical primarily due to what outcome?

View Answer & Explanation
Correct Answer: C
Rationale: In the proximal femur, the mechanical axis (center of head to center of knee) is highly eccentric and medial to the diaphysis. Attempting to rotate the shaft around this distant axis results in a large, unacceptable translational displacement of the bone fragments, making stable fixation and healing extremely difficult.
Question 60
A 21-year-old patient with cerebral palsy has a complex lower limb deformity consisting of 40 degrees of femoral anteversion and 20 degrees of genu valgum. According to the CORA principle applied to multi-planar deformities, where should the corrective osteotomy ideally be performed?
View Answer & Explanation
Correct Answer: C
Rationale: When a rotational deformity is combined with an angular deformity, the ideal surgical plan is to perform a single osteotomy at the Center of Rotation of Angulation (CORA) of the angular deformity. At this location, both the angular and rotational corrections can be performed simultaneously, often requiring advanced techniques like hexapod external fixators or custom guides.
Question 61
A surgeon is using the "goniometer technique" during a distal femoral derotational osteotomy. This technique involves placing two parallel Steinmann pins into the anterior femur before the cut. What is the primary function of these pins?
View Answer & Explanation
Correct Answer: E
Rationale: Similar to the reference pins used in tibial osteotomies, the two parallel Steinmann pins in the femur serve as an intraoperative measuring device. After the osteotomy, the surgeon rotates the distal fragment and uses a sterile goniometer to measure the angle created between the two pins, ensuring the planned amount of correction is accurately achieved.
Question 62
A 25-year-old undergoes a CT scan for torsional profiling. The report states the angle between the femoral neck axis and the posterior femoral condylar axis is 45 degrees. Based on normative data, this finding is best described as:

View Answer & Explanation
Correct Answer: B
Rationale: The angle described is the definition of femoral version (anteversion/retroversion). The normal mean value is approximately 24 degrees. A value of 45 degrees is significantly higher than the norm and represents excessive femoral anteversion.
Question 63
A resident is reviewing plain radiographs of a patient with suspected femoral retroversion. Which radiographic finding on an AP view of the hip is most suggestive of this condition?
View Answer & Explanation
Correct Answer: A
Rationale: The lesser trochanter is located posteromedially on the femur. In femoral retroversion, the femur is externally rotated relative to the neck, which brings the lesser trochanter into profile on a standard AP radiograph, making it appear more prominent. Conversely, in excessive anteversion, the lesser trochanter is rotated posteriorly and may be diminished or absent (D).
Question 64
A 14-year-old female with cerebral palsy presents with a progressive, scissoring gait and hip pain. Physical examination reveals a positive Trendelenburg sign. A standing long-leg radiograph is obtained for pre-operative planning. According to the principles of deformity correction, the mechanical axis of the lower limb is defined as a straight line drawn between which two points?
View Answer & Explanation
Correct Answer: C
Rationale: The mechanical axis of the lower limb is a fundamental concept in deformity correction, defined as a straight line from the center of the femoral head to the center of the ankle joint (tibial plafond). This line should pass slightly medial to the center of the knee in a normally aligned limb. The anatomical axis of the femur (a line down the diaphysis) is different and not used to define the overall limb alignment.
Question 65
A 22-year-old male presents with hip pain and a limp following a malunited intertrochanteric femur fracture. When planning a corrective osteotomy, the surgeon measures the angle between the anatomical axis of the femoral shaft and the axis of the femoral neck. What is this angle called, and what is its normal range?
View Answer & Explanation
Correct Answer: B
Rationale: The Neck-Shaft Angle (NSA) is the angle formed between the anatomical axis of the femoral shaft and the axis of the femoral neck. Its normal range is 125° to 135°. The LPFA relates the mechanical axis to the proximal joint line, and the mLDFA relates the mechanical axis to the distal joint line.
Question 66
A surgeon is templating a proximal femoral osteotomy for a 16-year-old with developmental coxa vara. The surgeon identifies the intersection point of the proximal anatomical axis and the distal anatomical axis of the deformed femur. According to Paley's principles, what is this critical point called?
View Answer & Explanation
Correct Answer: D
Rationale: The Center of Rotation of Angulation (CORA) is the foundational concept of the Paley Method. It is precisely defined as the point where the proximal and distal anatomical axes of a deformed bone intersect. Locating the CORA is the first step in planning the geometric correction of the deformity.
Question 67
During pre-operative planning for a proximal femoral osteotomy, a surgeon decides to perform the bone cut and place the corrective hinge exactly at the level of the CORA. According to Paley's Rule 1, what will be the result of this maneuver?
View Answer & Explanation
Correct Answer: B
Rationale: Paley's Rule 1 states that if the osteotomy and the hinge (axis of correction) are placed exactly at the CORA, the deformity is corrected purely by angulation, without any secondary translation. This is the most straightforward application of the CORA principle, though not always practical in the proximal femur.
Question 68
A 19-year-old patient with a history of Perthes disease presents with coxa vara and a 2.5 cm leg length discrepancy, with the affected leg being shorter. The planned procedure is a valgus-producing proximal femoral osteotomy. What is the expected effect of this angular correction on the overall limb length?
View Answer & Explanation
Correct Answer: C
Rationale: Correcting a varus deformity to a normal Neck-Shaft Angle inherently increases the length of the femur due to trigonometric principles. This is a critical consideration in pre-operative planning, as the osteotomy itself can partially or fully correct a pre-existing leg length discrepancy. Conversely, correcting a valgus deformity shortens the limb.
Question 69
A 12-year-old girl with developmental dysplasia of the hip (DDH) has a Neck-Shaft Angle of 145°. This condition is best described as which of the following?
View Answer & Explanation
Correct Answer: D
Rationale: Coxa valga is defined by a Neck-Shaft Angle (NSA) greater than the normal range of 125-135°. An NSA of 145° is characteristic of coxa valga. Coxa vara is an NSA less than 125°. The other terms refer to the size or shape of the femoral head, not the neck-shaft relationship.
Question 70
A 15-year-old boy with cerebral palsy and coxa valga demonstrates a significant Trendelenburg gait. What is the primary biomechanical reason for this gait abnormality in this patient?
View Answer & Explanation
Correct Answer: B
Rationale: In coxa valga, the greater trochanter is positioned more medially and superiorly relative to the center of the femoral head. This shortens the abductor lever arm, requiring the gluteus medius and minimus to generate significantly more force to stabilize the pelvis, leading to muscle fatigue and a Trendelenburg gait. A lengthened abductor lever arm is seen in coxa vara.
Question 71
A surgeon is planning a corrective osteotomy for a patient with severe coxa valga. The image shows the planned correction. What type of osteotomy is required to restore normal hip biomechanics in this case?

View Answer & Explanation
Correct Answer: B
Rationale: Coxa valga (increased Neck-Shaft Angle) is corrected with a varus-producing osteotomy. This procedure decreases the Neck-Shaft Angle, effectively lateralizing the greater trochanter to restore the abductor lever arm and improving the seating of the femoral head in the acetabulum. The image demonstrates a varus correction with medial translation.
Question 72
A 13-year-old male with a history of a slipped capital femoral epiphysis (SCFE) presents with a painful limp. Radiographs show a Neck-Shaft Angle of 110°. This deformity subjects the femoral neck to what type of unfavorable forces?
View Answer & Explanation
Correct Answer: C
Rationale: In coxa vara (NSA < 125°), the femoral neck becomes more horizontal. This orientation converts the normal compressive forces from weight-bearing into massive shear forces across the neck and physis (if open). These shear forces can lead to fatigue fractures or progression of the deformity. A valgus osteotomy is performed to convert these shear forces back into favorable compressive forces.
Question 73
A surgeon is planning a valgus-producing osteotomy for a patient with coxa vara. The osteotomy is planned to be performed distal to the lesser trochanter. What effect will this have on the iliopsoas tendon tension during the correction?
View Answer & Explanation
Correct Answer: A
Rationale: For a valgus osteotomy performed distal to the lesser trochanter, the correction medializes and proximally displaces the insertion point of the iliopsoas tendon. This geometric shift decreases the tension on the tendon, making the osteotomy easier to perform and close. Conversely, an osteotomy proximal to the lesser trochanter would increase tension.
Question 74
A surgeon is performing a varus-producing osteotomy for coxa valga and plans the cut distal to the lesser trochanter. Based on the principles of soft tissue dynamics described by Paley, what is the expected change in iliopsoas tendon tension, and why is this osteotomy considered more difficult?
View Answer & Explanation
Correct Answer: B
Rationale: For a varus osteotomy performed distal to the lesser trochanter, the correction lateralizes and distally displaces the insertion point of the tendon. This increases the tension on the iliopsoas tendon, making the correction more difficult to achieve and maintain without a concomitant psoas release. An osteotomy proximal to the lesser trochanter would decrease the tension.
Question 75
A 25-year-old patient requires an acute, single-stage correction of a proximal femoral varus deformity with no associated leg length discrepancy. The patient has good bone quality and desires a high level of post-operative comfort with no external hardware. Which fixation method is most appropriate?
View Answer & Explanation
Correct Answer: C
Rationale: Internal fixation, such as an angled blade plate or a proximal femoral locking plate, is the gold standard for acute, single-stage corrections where lengthening is not required. It provides rigid fixation and high patient comfort. External fixation is reserved for gradual corrections, lengthening, or cases with poor bone/soft tissue quality.
Question 76
A 17-year-old male has a complex, multi-planar proximal femoral deformity with a concurrent 5 cm leg length discrepancy following a severe physeal injury. The surgeon plans a gradual correction and simultaneous lengthening. Which fixation strategy is best suited for this clinical scenario?
View Answer & Explanation
Correct Answer: D
Rationale: External fixation, particularly a hexapod-based circular frame like the Taylor Spatial Frame, is the ideal choice for complex, multi-planar deformities that require gradual correction and simultaneous lengthening via distraction osteogenesis. Internal fixation devices cannot perform gradual correction or significant lengthening.
Question 77
When inserting a 130-degree angled blade plate for a proximal femoral osteotomy, what is the most critical step to avoid rotational malalignment of the femoral head and neck fragment?
View Answer & Explanation
Correct Answer: B
Rationale: The insertion of the seating chisel dictates the final position of the blade. It is crucial that the chisel is driven into the femoral neck perfectly parallel to the neck's axis in the axial (lateral) plane. Any deviation will induce a flexion or extension deformity (rotational malalignment in the sagittal plane) of the proximal fragment when the plate is fixed to the shaft.
Question 78
A surgeon is performing a proximal femoral osteotomy on a patient with a significant coronal plane deformity. To prevent inadvertently inducing a flexion or extension deformity during the bone cut, which surgical pearl is most effective?
View Answer & Explanation
Correct Answer: C
Rationale: Placing Schanz pins proximal and distal to the planned osteotomy site before making the cut provides excellent control over the bone fragments. These pins act as "joysticks," allowing the surgeon to maintain and verify the sagittal alignment and prevent unintended flexion or extension while the coronal plane correction is performed.
Question 79
During a proximal femoral osteotomy, the surgeon performs the bone cut at the subtrochanteric level, which is distal to the CORA. To restore the mechanical axis to the center of the knee, a medial translation of the distal fragment is required. This creates a step-off at the osteotomy site. What is this surgically created offset known as?
View Answer & Explanation
Correct Answer: C
Rationale: When an osteotomy is performed away from the CORA, a translation is required to realign the mechanical axis (Paley's Rule 2). This necessary translation creates a "dog leg" or step-off appearance on the radiograph. This is a planned and biomechanically correct outcome, not a technical error. The bone will remodel over time.
Question 80
A 28-year-old male undergoes a subtrochanteric osteotomy for a post-traumatic deformity. At 4 months post-operatively, he complains of persistent thigh pain. Radiographs show no callus formation at the osteotomy site and a broken screw in his locking plate. What is the most likely diagnosis?
View Answer & Explanation
Correct Answer: B
Rationale: The subtrochanteric region is prone to non-union due to high biomechanical stresses. The lack of callus indicates an atrophic non-union (poor biology). The hardware, subjected to continuous fatigue cycling because the bone has not healed, eventually fails. A hypertrophic non-union would show abundant but ineffective callus.
Question 81
A 16-year-old patient is 8 weeks post-operative from a proximal femoral osteotomy with blade plate fixation. Radiographs show early callus formation. According to a typical rehabilitation protocol, what is the most appropriate weight-bearing status and physical therapy focus at this stage?
View Answer & Explanation
Correct Answer: D
Rationale: Between 6 and 12 weeks post-operatively, as radiographic evidence of healing appears, weight-bearing is typically advanced from partial to full. This is also the critical time to begin active strengthening exercises, particularly for the abductors, to retrain the muscles and improve gait mechanics. Full weight-bearing is usually not achieved until closer to 3 months.
Question 82
A surgeon is templating a proximal femoral osteotomy using the image provided. The angle formed by the mechanical axis of the femur and the proximal joint line (from the tip of the greater trochanter to the center of the femoral head) is measured. What is this angle, and what is its normal value?

View Answer & Explanation
Correct Answer: C
Rationale: The Lateral Proximal Femoral Angle (LPFA) is the angle between the mechanical axis of the femur and the proximal femoral joint line. As shown in the diagram, its normal value is approximately 90°. This angle is crucial for assessing the orientation of the proximal femur relative to the limb's mechanical axis.
Question 83
A 20-year-old patient has a valgus deformity of the proximal femur with equal leg lengths. A varus-producing osteotomy is planned. What is the expected consequence of this procedure on limb length, and what might be a necessary consideration?
View Answer & Explanation
Correct Answer: B
Rationale: Correcting a valgus hip to a normal Neck-Shaft Angle (varusizing osteotomy) inherently shortens the femur. If the patient starts with equal leg lengths, this will create a leg length discrepancy. The surgeon must be aware of this and counsel the patient that a future lengthening procedure or a shoe lift may be necessary.
Question 84
A surgeon is planning a proximal femoral osteotomy and performs the osteotomy at a different level than the CORA, but keeps the hinge of correction at the CORA. According to Paley's principles, what will be the result?
View Answer & Explanation
Correct Answer: C
Rationale: This scenario describes Paley's Rule 2. When the osteotomy is performed away from the CORA but the correction is hinged around the CORA, the result is a combined angular correction and a translation of the bone fragments. This is often done intentionally in the proximal femur to improve bone contact or muscle tension while still correctly aligning the mechanical axis.
Question 85
A 30-year-old patient with a history of a malunited femoral fracture undergoes a corrective osteotomy. The surgeon performs the osteotomy and places the hinge of correction at a location remote from the CORA. What is the most likely consequence of this action?
View Answer & Explanation
Correct Answer: B
Rationale: This describes Paley's Rule 3. If both the osteotomy and the hinge are placed away from the CORA, the correction will induce a secondary, unplanned translation deformity. This will shift the mechanical axis unfavorably and fail to restore normal limb alignment.
Question 86
A 45-year-old male presents with progressive right hip pain. On physical examination, he has a positive Trendelenburg sign. When planning a proximal femoral osteotomy, the surgeon defines a line from the center of the femoral head to the center of the ankle joint. What is this critical reference line called?
View Answer & Explanation
Correct Answer: B
Rationale: The mechanical axis of the lower extremity, a line from the center of the femoral head to the center of the ankle, is the cornerstone of lower extremity deformity analysis. The anatomic axis (A) follows the intramedullary canal of the femur and is different from the mechanical axis.
Question 87
A 38-year-old female with developmental dysplasia of the hip (DDH) is evaluated for a corrective osteotomy. Her full-length standing radiograph shows the mechanical axis of her right leg passing 20 mm lateral to the center of the knee joint. What is the correct term for this finding?
View Answer & Explanation
Correct Answer: B
Rationale: Mechanical Axis Deviation (MAD) is any deviation of the mechanical axis from the center of the knee. A lateral shift is termed valgus MAD, which overloads the lateral compartment of the knee. A medial shift is termed varus MAD (A).
Question 88
A surgeon is templating a proximal femoral osteotomy for a 22-year-old with a post-traumatic deformity. The angle formed by the intersection of the femoral mechanical axis and a line from the tip of the greater trochanter to the center of the femoral head is measured. What is this paramount angle for assessing proximal femoral alignment?
View Answer & Explanation
Correct Answer: C
Rationale: The Mechanical Lateral Proximal Femoral Angle (mLPFA) is the primary indicator of proximal femoral alignment relative to the mechanical axis and is crucial for planning corrections and assessing abductor mechanics. The NSA (A) measures the intrinsic shape of the proximal femur but not its alignment relative to the entire bone's mechanical axis.
Question 89
A 14-year-old patient with a history of Legg-Calvé-Perthes disease presents with a painless limp. Radiographs reveal an anatomic Neck Shaft Angle (NSA) of 105 degrees. What is the correct term for this deformity?
View Answer & Explanation
Correct Answer: B
Rationale: A decreased anatomic Neck Shaft Angle (NSA) is termed coxa vara. The normal range is 124 to 136 degrees. Coxa valga (A) refers to an abnormally increased NSA.
Question 90
During a preoperative conference, a resident is asked for the normal value range for the Mechanical Lateral Proximal Femoral Angle (mLPFA). What is the correct range that indicates normal proximal femoral alignment?
View Answer & Explanation
Correct Answer: B
Rationale: The normal value range for the mLPFA is 85 to 95 degrees, with an average of 90 degrees. Values below this range indicate a valgus deformity, while values above indicate a varus deformity. The range of 124 to 136 degrees (D) corresponds to the normal anatomic Neck Shaft Angle (NSA).
Question 91
A 28-year-old patient has a significant varus deformity of the proximal femur following a malunited fracture. According to Paley's principles, what is the geometric point where the proximal and distal mechanical axis lines of the deformed femur intersect?
View Answer & Explanation
Correct Answer: B
Rationale: The CORA is the fundamental concept in Paley's deformity analysis, defined as the apex or fulcrum of the deformity where the axes of the proximal and distal fragments intersect. Correctly identifying the CORA is the most critical step in planning an osteotomy to avoid creating a secondary deformity.
Question 92
A 19-year-old female with a history of congenital hip dysplasia presents with an increased anatomic Neck Shaft Angle (coxa valga) and a decreased mLPFA of 78 degrees. What is the expected global alignment consequence of this proximal femoral deformity?
View Answer & Explanation
Correct Answer: B
Rationale: A coxa valga deformity (decreased mLPFA) shifts the global mechanical axis laterally, creating a valgus MAD at the knee. This chronically overloads the lateral compartment. Coxa vara (A) would cause a varus MAD.
Question 93
A 55-year-old male presents with medial-sided knee pain and is found to have a coxa vara deformity with an mLPFA of 100 degrees. How does this proximal femoral deformity contribute to his knee symptoms?
View Answer & Explanation
Correct Answer: B
Rationale: A coxa vara deformity (increased mLPFA) shifts the global mechanical axis medially, creating a varus MAD at the knee. This leads to increased load on the medial compartment and can cause or accelerate medial compartment osteoarthritis. A valgus deformity (A) would cause lateral overload.
Question 94
A 40-year-old patient with early hip osteoarthritis secondary to DDH undergoes a simple proximal femoral varus osteotomy. Preoperatively, her mLPFA was 90 degrees. Postoperatively, she complains of a severe limp. What is the most likely iatrogenic cause of her new gait disturbance?

View Answer & Explanation
Correct Answer: C
Rationale: As illustrated in the provided image, performing a varus osteotomy on a hip with a normal starting mLPFA inherently displaces the greater trochanter proximally. This shortens the abductor lever arm and creates muscle slack, leading to significant abductor weakness and a Trendelenburg gait. While other complications are possible, this is the most predictable biomechanical consequence.
Question 95
A 50-year-old woman undergoes a 20° varus osteotomy as depicted in the provided image (a-ii). During single-leg stance on the operative side, her contralateral pelvis drops significantly. What is this clinical sign called?

View Answer & Explanation
Correct Answer: C
Rationale: The Trendelenburg sign, depicted in (b-i), is the classic clinical manifestation of abductor muscle weakness. The weakened abductors fail to stabilize the pelvis during single-leg stance, causing the contralateral side to drop. The osteotomy shown in (a-ii) directly causes this weakness.
Question 96
Referring to the biomechanical model of the hip as a first-class lever, what component serves as the fulcrum during single-leg stance?
View Answer & Explanation
Correct Answer: C
Rationale: In the first-class lever system of the hip, the center of rotation of the femoral head acts as the fulcrum. The abductor force is the effort, and the body weight is the resistance.
Question 97
A patient who underwent a simple varus osteotomy now walks with a characteristic lurch, throwing their torso laterally over the affected hip during the stance phase. What is the primary biomechanical purpose of this compensatory movement?
View Answer & Explanation
Correct Answer: B
Rationale: The compensated Trendelenburg lurch is an instinctive maneuver to reduce the torque demand on the weakened abductors. By shifting the torso over the hip, the patient moves their body's center of gravity closer to the fulcrum (femoral head), which shortens and therefore reduces the body weight moment arm.
Question 98
A 42-year-old with DDH undergoes a varus osteotomy. According to Bombelli's theory, the resulting abductor weakness may lead to the formation of a specific type of osteophyte from the superior acetabular ridge. What is this osteophyte called?
View Answer & Explanation
Correct Answer: B
Rationale: Bombelli theorized that the weakened abductors could lead to the formation of a traction osteophyte from the superior acetabulum. This was thought to be a biological attempt to increase lateral coverage of the femoral head over time. A compression osteophyte (A) would form in an area of high load, not in response to muscle pull.
Question 99
When performing a proximal femoral varus osteotomy, what is the definitive surgical technique to prevent the iatrogenic abductor weakness and subsequent Trendelenburg gait?
View Answer & Explanation
Correct Answer: D
Rationale: The most effective and biomechanically sound solution is to perform a concurrent lateral and distal transfer of the greater trochanter. This compensatory procedure directly counteracts the proximal displacement caused by the varus osteotomy, restoring both abductor tension and the abductor lever arm. Postoperative therapy (E) cannot overcome a significant, surgically created mechanical disadvantage.
Question 100
A surgeon is performing a greater trochanteric transfer in conjunction with a varus osteotomy. What is the specific biomechanical goal of moving the trochanteric fragment in a distal direction?
View Answer & Explanation
Correct Answer: D
Rationale: The distal transfer of the greater trochanter is crucial for re-tensioning the gluteus medius and minimus muscles, which were put on slack by the varus correction. This restores their optimal length-tension relationship and force-generating capacity. The lateral transfer component (B) is what increases the abductor moment arm.
You Might Also Like
