Comprehensive Introduction and Patho-Epidemiology
The advent and subsequent evolution of wrist arthroscopy have fundamentally revolutionized the diagnostic and therapeutic paradigms within orthopedic hand and upper extremity surgery. Historically, the intricate and compact nature of the radiocarpal and midcarpal articulations relegated surgeons to extensive open arthrotomies, which inherently carried significant morbidity, including profound postoperative stiffness, dense capsular scarring, and prolonged rehabilitation trajectories. Today, wrist arthroscopy is universally recognized as the gold standard for evaluating intra-articular pathology, offering unparalleled magnification and illumination of the chondral surfaces, intrinsic interosseous ligaments, and the triangular fibrocartilage complex (TFCC). This minimally invasive approach not only mitigates the iatrogenic trauma associated with open surgical dissection but also facilitates a more rapid return to pre-injury functional baselines for patients.


Understanding the patho-epidemiology of wrist disorders is paramount for the operating surgeon, as it directly informs the clinical index of suspicion and subsequent operative planning. Ulnar-sided wrist pain, often colloquially referred to as the "low back pain of the wrist," represents a significant proportion of pathology encountered in clinical practice. The TFCC is the primary stabilizer of the distal radioulnar joint (DRUJ) and the ulnar carpus, bearing approximately 20% of the axial load transmitted across the wrist. Traumatic tears (Palmer Class 1) typically occur in young, active individuals following an axial load applied to an extended, pronated wrist, whereas degenerative tears (Palmer Class 2) manifest in older populations, frequently exacerbated by positive ulnar variance and ulnocarpal impaction syndrome.


Furthermore, carpal instability patterns, particularly scapholunate (SL) and lunotriquetral (LT) ligament disruptions, are critical patho-epidemiological entities that demand precise arthroscopic evaluation. The SL ligament is the most frequently injured intrinsic ligament, often resulting from a fall on an outstretched hand (FOOSH) with the wrist in extension, ulnar deviation, and intercarpal supination. Unrecognized SL dissociation predictably progresses to scapholunate advanced collapse (SLAC), a devastating degenerative condition characterized by sequential chondral wear. Arthroscopy allows for the dynamic assessment of these interosseous ligaments, enabling the surgeon to grade the instability (e.g., using the Geissler classification) and execute timely, appropriate interventions before irreversible arthrosis ensues.
Evolution of Minimally Invasive Wrist Surgery
The historical trajectory of wrist arthroscopy traces back to the late 1970s and early 1980s, pioneered by visionary surgeons who adapted small-joint arthroscopes initially designed for temporomandibular and ankle joints. Early iterations were plagued by inadequate instrumentation, poor fiber-optic illumination, and a steep learning curve that deterred widespread adoption. However, the subsequent development of dedicated 2.4 mm and 1.9 mm high-definition, 30-degree angled arthroscopes, coupled with specialized traction towers, provided the necessary joint distraction and visual clarity to safely navigate the radiocarpal and midcarpal spaces.


As instrumentation evolved, so too did the scope of arthroscopic interventions. What began strictly as a diagnostic modality rapidly transitioned into a robust therapeutic platform. The development of specialized motorized shavers, radiofrequency ablation wands, and micro-suture passing devices allowed surgeons to perform complex procedures such as TFCC repairs, limited synovectomies, and thermal shrinkage of attenuated ligaments. This transition from open to arthroscopic techniques has drastically reduced the incidence of postoperative complications, particularly infection and debilitating joint stiffness, which were once accepted risks of wrist surgery.
Today, the integration of wrist arthroscopy with fracture management represents a critical frontier in orthopedic trauma. Arthroscopically assisted reduction and internal fixation (ARIF) of distal radius fractures and scaphoid nonunions provides real-time, magnified visualization of the articular surface, ensuring anatomic reduction and identifying concomitant soft-tissue injuries that are entirely missed by standard fluoroscopy. This dual diagnostic and therapeutic capability underscores the indispensable nature of wrist arthroscopy in the modern orthopedic armamentarium.
Detailed Surgical Anatomy and Biomechanics
A profound, three-dimensional comprehension of wrist anatomy is the absolute prerequisite for safe and effective arthroscopic surgery. The wrist is not a single joint but a highly complex, multi-articulated biomechanical linkage comprising the radiocarpal joint, the midcarpal joint, and the distal radioulnar joint (DRUJ). The radiocarpal articulation is formed by the biconcave distal articular surface of the radius, the TFCC, and the convex proximal surfaces of the scaphoid, lunate, and triquetrum. This joint is inherently unstable due to its osseous geometry and relies heavily on a robust network of extrinsic palmar and dorsal capsular ligaments to maintain alignment under physiological loads.


The midcarpal joint, situated between the proximal and distal carpal rows, functions as a complex hinge that accommodates approximately half of the total flexion-extension arc of the wrist. Unlike the radiocarpal joint, the midcarpal joint does not possess direct tendinous insertions; instead, the proximal row functions as an intercalated segment, governed entirely by the mechanical forces exerted by the surrounding ligaments and the geometric constraints of the adjacent bones. The intrinsic ligaments, primarily the scapholunate interosseous ligament (SLIL) and the lunotriquetral interosseous ligament (LTIL), are critical for synchronizing the complex kinematics of the carpal rows during global wrist motion.


Biomechanically, load transmission across the normal wrist is distributed asymmetrically, with approximately 80% of the axial load traversing the radiocarpal joint (predominantly through the radioscaphoid and radiolunate fossae) and 20% traversing the ulnocarpal joint via the TFCC. Alterations in ulnar variance significantly perturb this load distribution; for instance, a 2.5 mm increase in ulnar length (positive ulnar variance) can increase the load transmitted through the ulnocarpal joint to over 40%, precipitating ulnocarpal impaction syndrome, central TFCC perforations, and chondromalacia of the lunate and ulnar head.
The Triangular Fibrocartilage Complex (TFCC)
The TFCC is a highly specialized, heterogeneous structure that serves as the primary stabilizer of the DRUJ and a critical load-bearing cushion for the ulnar carpus. Anatomically, it is composed of the articular disc proper, the dorsal and volar radioulnar ligaments, the meniscus homologue, the ulnar collateral ligament, and the extensor carpi ulnaris (ECU) tendon subsheath. The articular disc is centrally avascular and hypocellular, rendering it incapable of intrinsic healing following traumatic perforation or degenerative wear (Palmer Class 1A or 2 lesions).


Conversely, the peripheral margins of the TFCC, particularly its ulnar attachments to the fovea and the base of the ulnar styloid, possess a robust vascular supply derived from the ulnar artery and the anterior and posterior interosseous arteries. This rich vascularity allows for the successful surgical repair of peripheral tears (Palmer Class 1B). The foveal attachment of the TFCC is mechanically the most critical component for DRUJ stability; disruption here leads to gross instability of the ulnar head relative to the sigmoid notch of the radius, necessitating anatomic reattachment using transosseous tunnels or suture anchors.

The biomechanical function of the TFCC extends beyond simple load distribution; it acts as a dynamic ligamentous sling that guides the complex rotational kinematics of the forearm. During pronation, the dorsal radioulnar ligament becomes taut, preventing dorsal subluxation of the ulna, while in supination, the volar radioulnar ligament tightens to prevent volar subluxation. Arthroscopic evaluation of the TFCC must therefore include dynamic testing—the "trampoline test" and the "hook test"—to accurately assess the structural integrity and functional tension of these critical ligamentous components.
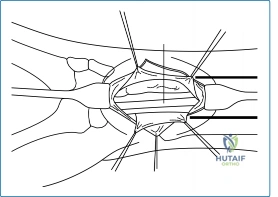
Neurovascular Topography and Extensor Compartments
Safe establishment of arthroscopic portals demands an intimate knowledge of the dorsal wrist's neurovascular topography and the precise locations of the six extensor compartments. The extensor retinaculum acts as a pulley system, dividing the dorsal tendons into distinct compartments that serve as reliable anatomical landmarks. The primary viewing portal, the 3-4 portal, is established between the extensor pollicis longus (EPL, 3rd compartment) and the extensor digitorum communis (EDC, 4th compartment), just distal to Lister's tubercle.


The superficial branch of the radial nerve (SBRN) and the dorsal cutaneous branch of the ulnar nerve (DCBUN) represent the structures at highest risk during portal placement. The SBRN courses distally along the radial aspect of the wrist, arborizing into multiple branches that cross the anatomic snuffbox and the 1-2 portal region. Injury to these branches can result in debilitating neuromas and complex regional pain syndrome (CRPS). Consequently, the 1-2 portal, located between the first compartment (APL/EPB) and the second compartment (ECRL/ECRB), is utilized less frequently and requires meticulous blunt dissection to avoid the radial artery and SBRN branches.
Similarly, the DCBUN crosses the ulnar aspect of the wrist, placing it at significant risk during the establishment of the 6U portal (ulnar to the ECU tendon). To mitigate neurovascular injury, surgeons must employ a strict "nick and spread" technique: incising only the epidermis with a #15 blade, followed by blunt spreading of the subcutaneous tissues down to the capsule using a fine hemostat. This technique gently displaces the cutaneous nerves and dorsal venous network, ensuring safe passage of the trocar and cannula into the joint space.
Exhaustive Indications and Contraindications
The clinical utility of wrist arthroscopy spans a broad spectrum of diagnostic and therapeutic applications. Diagnostically, it remains the gold standard for evaluating patients with chronic, recalcitrant wrist pain of ambiguous etiology, particularly when advanced imaging modalities such as high-resolution MRI or MR arthrography yield equivocal results. Arthroscopy allows for the direct, magnified visualization and dynamic probing of the chondral surfaces, interosseous ligaments, and the TFCC, providing a definitive diagnosis in cases of occult carpal instability or subtle chondromalacia that elude standard radiographic detection.


Therapeutically, the indications for wrist arthroscopy have expanded exponentially. It is routinely employed for the debridement or repair of TFCC tears, the management of localized chondral defects, and the excision of dorsal wrist ganglions via a capsular window. In the realm of trauma, arthroscopically assisted reduction of distal radius fractures allows for the meticulous restoration of articular congruity and the concurrent management of associated soft-tissue injuries, which are present in up to 70% of intra-articular distal radius fractures. Furthermore, arthroscopy is invaluable in the assessment and treatment of Kienböck’s disease (evaluating lunate articular cartilage to guide surgical staging), the irrigation and debridement of septic arthritis, and the retrieval of intra-articular loose bodies.


Despite its minimally invasive nature, wrist arthroscopy is not without its limitations, and careful patient selection is paramount. Absolute contraindications are relatively few but include active, persistent bacterial infection of the overlying skin or soft tissues (cellulitis), which risks inoculating the sterile joint space. Additionally, severe distortion of the normal capsular anatomy—whether due to massive trauma, extensive prior surgical interventions, or advanced inflammatory arthropathy—can obliterate the joint space, making safe portal placement impossible and significantly increasing the risk of iatrogenic neurovascular or chondral injury.
Table of Indications and Contraindications
| Category | Specific Conditions | Clinical Rationale |
|---|---|---|
| Diagnostic Indications | Chronic unexplained wrist pain | Direct visualization and dynamic probing of occult pathology missed by MRI. |
| Suspected carpal instability | Geissler grading of SL/LT ligaments via midcarpal and radiocarpal evaluation. | |
| Unexplained mechanical symptoms | Identification of loose bodies, subtle chondral flaps, or meniscoid lesions. | |
| Therapeutic Indications | TFCC Tears (Palmer 1B, 1C, 1D) | Arthroscopic debridement or anatomic repair utilizing inside-out/outside-in techniques. |
| Distal Radius Fractures | ARIF to ensure anatomic articular reduction (<1mm step-off) and treat concomitant soft tissue injuries. | |
| Scaphoid Fractures/Nonunions | Assessment of vascularity, assistance with percutaneous screw fixation, and bone grafting. | |
| Dorsal Wrist Ganglions | Resection of the ganglion stalk and a portion of the dorsal capsule to prevent recurrence. | |
| Septic Arthritis | Voluminous irrigation and thorough mechanical debridement of purulent loculations. | |
| Absolute Contraindications | Overlying skin infection | High risk of iatrogenic intra-articular inoculation and subsequent septic arthritis. |
| Inadequate instrumentation | Attempting the procedure without appropriate 2.4/1.9mm scopes or traction towers is unsafe. | |
| Relative Contraindications | Severe capsular scarring | Prior open surgery or severe trauma obliterates the joint space, preventing safe portal entry. |
| Advanced radiocarpal arthrosis | Complete loss of joint space makes scope insertion highly traumatic to residual cartilage. | |
| Shoulder/Elbow stiffness | Inability to position the arm in the traction tower (requires 90° shoulder abduction/elbow flexion). |
Pre-Operative Planning, Templating, and Patient Positioning
Meticulous preoperative planning is the cornerstone of a successful wrist arthroscopy. The process begins with a comprehensive clinical history and a targeted physical examination, focusing on provocative maneuvers such as the Watson scaphoid shift test, the shuck test for lunotriquetral instability, and the foveal sign or DRUJ ballottement for TFCC pathology. These clinical findings must be correlated with recent, high-quality radiographic investigations. Standard posteroanterior, lateral, and specialized views (e.g., clenched fist, scaphoid views) are mandatory to assess carpal alignment, ulnar variance, and degenerative changes. Advanced imaging, particularly 3-Tesla MRI or MR arthrography, is frequently employed to delineate soft-tissue pathology and guide the specific clinical questions that the arthroscopy aims to answer.


Equipment selection must be finalized prior to bringing the patient into the operating theater. The standard instrumentation includes a 2.4 mm or 2.7 mm, 30-degree angled arthroscope, which provides an optimal balance of structural rigidity, field of view, and maneuverability within the tight confines of the wrist. For smaller patients or for navigating the midcarpal joint, a 1.9 mm arthroscope may be advantageous, though it is inherently more fragile. A dedicated wrist arthroscopy traction tower is an absolute necessity, as manual traction is insufficient to maintain the consistent joint distraction required for safe instrument passage. Additional procedure-specific equipment, such as motorized shavers (2.0 mm or 2.9 mm), radiofrequency probes, and specialized suture passers, must be readily available on the sterile back table.


Informed consent must be obtained with a detailed discussion of the specific risks associated with wrist arthroscopy. While minimally invasive, patients must be counseled on the potential for iatrogenic nerve injury (specifically the superficial radial nerve and the dorsal cutaneous branch of the ulnar nerve), postoperative infection, hematoma formation, and vascular injury. Furthermore, the risk of extensor tendon injury from aberrant portal placement and the possibility of persistent postoperative stiffness must be explicitly documented. Setting realistic preoperative expectations regarding the timeline for recovery and the potential need for subsequent open procedures is critical for patient satisfaction.
Anesthesia and Patient Setup
The procedure is typically performed under regional anesthesia (supraclavicular or axillary brachial plexus block) combined with intravenous sedation, or under general anesthesia, depending on patient preference and the anticipated duration of the surgery. The patient is positioned supine on the operating table. A well-padded, above-elbow pneumatic tourniquet is applied and typically inflated to 250 mm Hg following exsanguination of the limb to ensure a bloodless surgical field, which is critical for maintaining arthroscopic visibility.


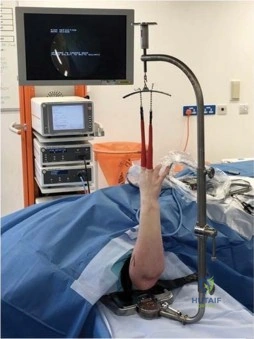
Positioning the upper extremity requires specialized equipment. The shoulder is abducted to 90 degrees, and the arm is placed on a radiolucent hand table or side extension. A dedicated wrist arthroscopy traction tower is then assembled. Sterile finger traps are applied securely to the index and middle fingers. The arm is anchored to the base of the tower using a padded counter-traction strap placed proximally to the elbow joint. The elbow is flexed to precisely 90 degrees, and longitudinal traction of approximately 10 lbs (4.5 kg) is applied through the finger traps. This specific vector of traction is essential for distracting the radiocarpal and midcarpal joints, creating a sufficient working space to introduce the arthroscopic trocars without scoring the delicate articular cartilage.


Once the arm is suspended, the surgical site is meticulously prepped and draped in a standard sterile fashion. The surgeon must then palpate and mark the critical osseous landmarks: the radial styloid, the ulnar styloid, Lister's tubercle, and the extensor tendons. Marking these landmarks prior to joint distension is crucial, as the infusion of fluid will rapidly obscure the surface anatomy. Joint distension is achieved by injecting 5 to 10 mL of sterile saline or lactated Ringer's solution into the radiocarpal joint, typically at the site of the planned 3-4 portal. This distension not only facilitates easier trocar entry but also pushes the dorsal capsule and associated neurovascular structures away from the underlying carpal bones, adding an extra layer of safety during portal creation.
Step-by-Step Surgical Approach and Fixation Technique
The execution of a successful wrist arthroscopy relies heavily on the precise establishment of standard portals. The nomenclature for these portals is derived from their anatomical relationship to the six dorsal extensor compartments. The 3-4 portal, located between the extensor pollicis longus (EPL) and the extensor digitorum communis (EDC), serves as the primary viewing portal. To establish this portal, the surgeon palpates Lister’s tubercle and rolls the thumb distally over the dorsal rim of the radius into the soft "divot" of the radiocarpal joint. A longitudinal incision through the dermis is made, followed by blunt dissection with a mosquito hemostat down to the capsule. The blunt trocar and cannula are then introduced with a firm, twisting motion, angled approximately 10 to 15 degrees proximally to match the volar tilt of the distal radius articular surface.

Once the arthroscope is introduced through the 3-4 portal, a systematic diagnostic tour of the radiocarpal joint is initiated. The surgeon evaluates the volar capsular ligaments (radioscaphocapitate, long radiolunate, short radiolunate), the articular surfaces of the scaphoid and lunate, and the intrinsic scapholunate ligament. The arthroscope is then swept ulnarly to inspect the lunotriquetral ligament and the expansive surface of the TFCC. To facilitate probing and therapeutic intervention, a working portal must be established. The 4-5 portal (between the EDC and extensor digiti minimi) or the 6R portal (radial to the extensor carpi ulnaris) are most commonly utilized. These portals are established under direct intra-articular visualization using a spinal needle to localize the optimal trajectory before making the skin incision.


Evaluation of the midcarpal joint is equally critical, particularly for assessing dynamic carpal instability. The midcarpal radial (MCR) and midcarpal ulnar (MCU) portals are utilized for this purpose. The MCR portal is located approximately 1 cm distal to the 3-4 portal, aligning with the scapholunate interval, while the MCU portal is located 1 cm distal to the 4-5 portal, aligning with the lunotriquetral interval. Within the midcarpal joint, the surgeon assesses the articular surfaces of the proximal and distal carpal rows and utilizes a probe to test the integrity of the SL and LT ligaments from their distal aspect. The Geissler classification is employed here to grade any abnormal gapping or step-off between the carpal bones, dictating the need for subsequent pinning or repair.
Specific Therapeutic Techniques
For the management of peripheral TFCC tears (Palmer 1B), arthroscopic repair is the treatment of choice. Following meticulous debridement of the tear edges and the ulnar capsule to stimulate a bleeding, healing response, an "outside-in" or "inside-out" suturing technique is employed. In the outside-in technique, specialized PDS sutures are passed through the dorsal ulnar capsule, capturing the peripheral edge of the TFCC, and tied blindly over the capsule through a small accessory incision. For more complex foveal avulsions, an arthroscopically assisted transosseous repair or the use of knotless suture anchors placed directly into the fovea via the DRUJ or 6U portal is required to restore the biomechanical tether of the ulnar head.









































































































































Detailed Chapters & Topics
Dive deeper into specialized chapters regarding surgery-of-the-wrist
