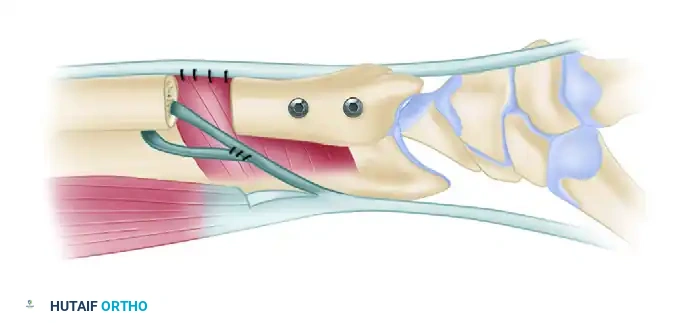
Mastering Flexor and Extensor Tenosynovectomy: An Intraoperative Masterclass for Rheumatoid Hand Surgery
Key Takeaway
Join us in the OR for a comprehensive masterclass on flexor and extensor tenosynovectomy. This guide provides fellows with detailed surgical anatomy, meticulous step-by-step intraoperative execution, critical pearls, and robust postoperative management strategies for inflammatory tenosynovitis, particularly in rheumatoid arthritis. Master precise dissection, hardware application, and complication avoidance for optimal patient outcomes.
Welcome, fellows, to the operating theater. Today, we're tackling a crucial procedure in the management of rheumatoid arthritis: flexor and extensor tenosynovectomy. This isn't just about removing inflamed tissue; it's about preserving tendon function, preventing rupture, and restoring quality of life for our patients. You'll gain a deep understanding of the intricate anatomy, the meticulous surgical steps, and the critical decision-making required to achieve optimal outcomes. Let's scrub in.
Understanding Tenosynovitis: Definitions and Pathophysiology
Before we make our first incision, let's review the fundamentals.
Definition:
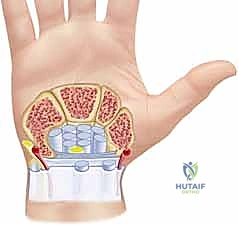
The synovium is a specialized membrane that lines joint spaces and, critically for our purposes today, tendon sheaths. Its primary role is to secrete synovial fluid, a viscous lubricant essential for smooth tendon gliding and reducing friction within synovial joints.
- Tendon Classification: Tendons can be broadly classified as either extrasynovial or intrasynovial.
- Extrasynovial tendons: These tendons, such as the wrist flexors (flexor carpi radialis (FCR), palmaris longus, flexor carpi ulnaris (FCU)), are enveloped by a tendon sheath but lack a true synovial lining. Inflammation here is termed tenosynovitis.
- Intrasynovial tendons: These tendons, like the digital flexors within the carpal tunnel and the extensor tendons beneath the dorsal retinaculum, possess a true synovial lining. Inflammation in these cases involves the synovial lining itself.
- Unique Features:
- The extensor digitorum quinti (EDQ) in the fifth extensor compartment is often the sole motor for small finger metacarpophalangeal (MCP) joint extension. Its health is paramount for small finger function.
- The extensor carpi ulnaris (ECU) tendon in the sixth compartment resides within a fibro-osseous tunnel and is intimately secured in the ulnar groove by a subsheath. This subsheath is absolutely critical for distal radioulnar joint (DRUJ) stability. Compromise here can lead to significant wrist dysfunction.
- Flexor tendons within the carpal tunnel have an additional feature: subsynovial connective tissue, which can also become inflamed, contributing to compression and dysfunction.
Pathogenesis:
Today's primary indication is often rheumatoid arthritis (RA), a systemic inflammatory disease characterized by chronic synovial tissue inflammation.
- Hypertrophic Synovium: In RA, the synovial tissue undergoes significant hypertrophy, forming a destructive pannus that invades both joint spaces and tendon sheaths. This hypertrophic synovium, rich in inflammatory mediators, directly attacks the tendon substance.
- Mechanical Impingement: The proliferating synovium occupies space within the confined tendon sheaths, leading to mechanical impingement and increased friction during tendon excursion.
- Tendon Weakening and Rupture: The chronic inflammation and mechanical stress progressively weaken the tendon collagen fibers. The end result, if untreated, is often tendon rupture, a devastating complication that can severely impair hand function.
- Specific Susceptibilities:
- The extensor pollicis longus (EPL) in the third extensor compartment is particularly vulnerable due to its acute angle around Lister's tubercle, making it susceptible to attrition rupture from chronic synovitis or bony spurs.
- The flexor pollicis longus (FPL) is the most common flexor tendon to rupture in RA, a condition known as the Mannerfelt lesion, resulting in the loss of thumb interphalangeal (IP) joint flexion.
Natural History:
Inflammatory tenosynovitis, especially in RA, can often be surprisingly painless in its early stages. It may even be the initial presenting sign of the disease. The dorsal and volar wrist, as well as the volar digits, are the most commonly affected areas.
Comprehensive Surgical Anatomy: Navigating the Wrist and Hand
Understanding the intricate anatomy is paramount. We must respect neurovascular structures and appreciate the biomechanics of each compartment.
Extensor Tendons and Compartments
The extensor tendons of the wrist and hand are organized into six distinct fibro-osseous compartments beneath the dorsal retinaculum. Each compartment is lined with a synovial sheath.
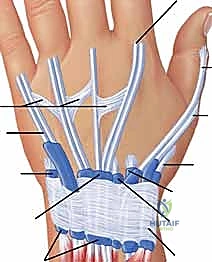
- First Extensor Compartment (Radial Side):
- Tendons: Abductor Pollicis Longus (APL) and Extensor Pollicis Brevis (EPB) – the "outcropper muscles."
- Origin/Course: These muscles originate from the distal third of the forearm and cross over the second extensor compartment tendons (ECRL/ECRB) distally, approximately 4 cm proximal to the radial styloid.
- Action: Abduct the thumb radially.
- Neurovascular Risks: The superficial branch of the radial nerve courses in close proximity, particularly radial to the first compartment. Care must be taken during incision and flap elevation to avoid injury.
- Second Extensor Compartment:
- Tendons: Extensor Carpi Radialis Longus (ECRL) and Extensor Carpi Radialis Brevis (ECRB).
- Action: Extend and radially deviate the wrist.
- Third Extensor Compartment:
- Tendon: Extensor Pollicis Longus (EPL).
- Course: Makes an acute turn around Lister's tubercle at the level of the wrist, making it susceptible to attrition.
- Action: Extends the thumb, particularly raising it off a flat surface.
- Fourth Extensor Compartment:
- Tendons: Extensor Digitorum Communis (EDC) and Extensor Indicis Proprius (EIP).
- Course: Lies under a broad retinaculum.
- Action: EDC extends the fingers at the MCP joints; EIP extends the index finger independently.
- Neurovascular Risks: The deep branch of the posterior interosseous nerve (PIN) courses deep to this compartment. While typically not in the surgical field for a superficial synovectomy, awareness is crucial if deeper dissection is required or if a mass effect is present.
- Fifth Extensor Compartment:
- Tendon: Extensor Digitorum Quinti (EDQ).
- Action: Extends the small finger at the MCP joint, often as the sole motor.
- Sixth Extensor Compartment (Ulnar Side):
- Tendon: Extensor Carpi Ulnaris (ECU).
- Course: Lies within a fibro-osseous tunnel and is held intimately in the ulnar groove by a critical subsheath.
- Action: Extends and ulnarly deviates the wrist.
- Neurovascular Risks: The dorsal cutaneous branch of the ulnar nerve can be found in the vicinity, particularly when dissecting near the ulnar styloid.
Flexor Tendons and Compartments
Unlike the extensors, digital flexor tendons are almost entirely intrasynovial.
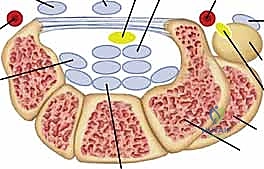
- Carpal Tunnel:
- Contents: Flexor Digitorum Superficialis (FDS) (4 tendons), Flexor Digitorum Profundus (FDP) (4 tendons), Flexor Pollicis Longus (FPL) (1 tendon), and the Median Nerve.
- Course: These tendons lie under the transverse carpal ligament.
- Neurovascular Risks: The median nerve is the most critical structure. The palmar cutaneous branch of the median nerve arises proximally and courses superficially over the transverse carpal ligament, making it vulnerable during the initial incision. The ulnar nerve and artery are adjacent, within Guyon's canal, medial to the carpal tunnel.
- Wrist Flexors (Extrasynovial):
- Tendons: Flexor Carpi Radialis (FCR), Palmaris Longus, Flexor Carpi Ulnaris (FCU).
- Course: The FCR passes through a tight fibro-osseous tunnel in the trapezium before inserting on the base of the second metacarpal.
- Neurovascular Risks: The radial artery is lateral to the FCR tendon.
- Digital Flexors:
- Course: Lie within a fibro-osseous canal formed by the annular (A1-A5) and cruciate (C1-C3) pulleys.
- Critical Structures: The A2 and A4 pulleys are essential for maintaining the mechanical advantage of the flexor tendons and preventing bowstringing. Their preservation is paramount.
Patient History and Physical Findings: The Diagnostic Foundation
A thorough history and physical exam are the cornerstones of diagnosis. Tenosynovitis is primarily a clinical diagnosis.
Patient History:
* Onset, duration, and progression of swelling.
* Pain characteristics (often painless initially in RA).
* Functional limitations (difficulty with grip, pinch, extension).
* Any "triggering" or "catching" sensation.
* History of rheumatoid arthritis or other inflammatory conditions.
* Previous nonoperative treatments and their efficacy.
Physical Findings:
- Inspection: Look for visible swelling, erythema, and deformities.
* Palpation: Tenderness, crepitus, and thickening of tendon sheaths.
* Range of Motion (ROM): Assess active and passive ROM for all digits and the wrist. Note any discrepancies.
* Specific Compartment Findings:
* First Extensor Compartment: Thickening of the APL and EPB tendon sheaths at the radial styloid. A positive Finkelstein's test (ulnar wrist abduction with the thumb in a fist) will elicit pain along this compartment.
* Second Extensor Compartment: Often presents with painless swelling on the dorsum of the wrist, approximately 4 cm proximal to the radial styloid. Focal tenderness may be present. A positive Tinel sign over the sensory branch of the radial nerve may indicate nerve irritation due to the swelling.
* Third Extensor Compartment: Typically presents with EPL tendon rupture, leading to an inability to actively raise the thumb when the hand is placed flat on a table (positive "tabletop test").
* Fourth Extensor Compartment: Focal swelling in extensor zone 7, often accompanied by multiple tendon ruptures of the EDC and EIP.
* Fifth Extensor Compartment: Usually associated with dorsal distal ulna instability and EDQ tendon rupture.
* Sixth Extensor Compartment: Manifests as ECU instability (subluxation/dislocation) in addition to significant intrasynovial inflammation at the ulnar styloid level.
* Flexor Tenosynovitis (Wrist): Can cause median nerve compression within the carpal tunnel, leading to numbness, tingling, and weakness. Decreased active and passive range of motion of the fingers may also be noted.
* Flexor Tenosynovitis (Digits): Commonly causes triggering or "catching" of the finger, indicating a nodule or thickened synovium impeding tendon gliding at the A1 pulley.
* Flexor Tendon Rupture: The FPL rupture (Mannerfelt lesion) results in loss of thumb IP joint flexion.
* Strength Testing: Grade muscle strength on a scale of 0 to 5 for each tendon group:
* First Dorsal Compartment (APL/EPB): Abduct the thumb radially.
* Second Extensor Compartment (ECRL/ECRB): Extend and radially deviate the wrist.
* Third Extensor Compartment (EPL): With the hand flat on the table, extend the thumb (lift it off the surface).
* Fourth Extensor Compartment (EDC): Extend the fingers at the MCP joints.
* Extensor Indicis Proprius (EIP): Extend the index finger at the MCP joint
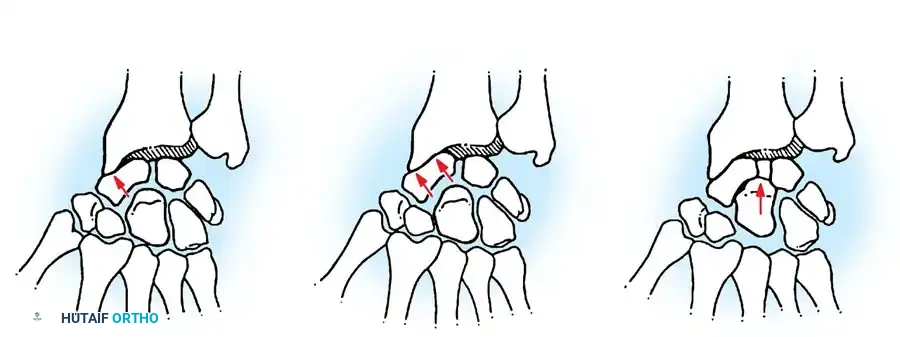
Additional Intraoperative Imaging & Surgical Steps
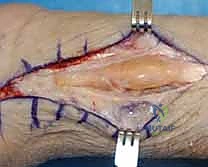
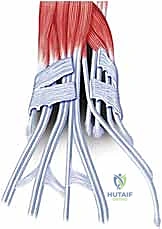
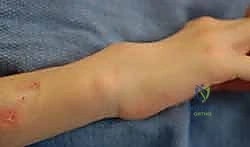
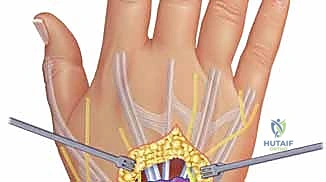
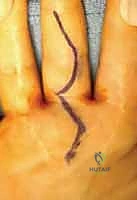
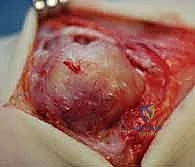
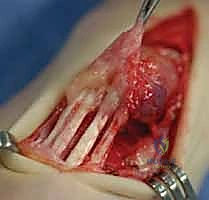
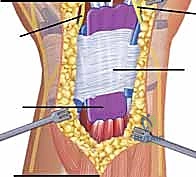
REFERENCES
References
- Splint The Wrist In Neutral Position.
- Early (within 48 hours) active and passive digit range of motion exercise is key to maintaining motion. 1
OUTCOMES
- Long-term studies show less than 10% tendon rupture and recurrent tenosynovitis at 5 years.
COMPLICATIONS
- Wound dehiscence
-
Tendon adhesions
-
Tendon rupture 1
-
Brown FE, Brown ML. Long-term results after tenosynovectomy to treat the rheumatoid hand. J Hand Surg Am 1998;13:704–708.
-
Feldon P, Terrano A, Nalebuff E, et al: Rheumatoid arthritis and other connective tissue disease. In Green DP, Hotchkiss R, Pederson WC, eds. Green’s Operative Hand Surgery, ed
-
New York: Churchill Livingstone, 2005:2060–2068.
-
Millender L, Nalebuff E, Albin R, et al. Dorsal tenosynovectomy and tendon transfer in the rheumatoid hand. J Bone Joint Surg Am 1974;56A:601–610.
-
Ryu J, Patel S. Rheumatoid arthritis: Soft tissue reconstruction. In: Trumble T, ed: Hand Surgery Update
-
Rosemont, IL: American Society for Surgery of the Hand, 2003:535–536.
-
Thirupathi R, Ferlic D, Clayton M. Dorsal wrist synovectomy in rheumatoid arthritis: A long-term study. J Hand Surg Am 1983;8:848–856.

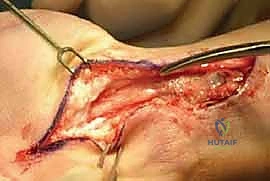
You Might Also Like