Unlock Wrist Diagnosis: Cases Guided by Figure Sunil Thirkannad
Key Takeaway
Discover the latest medical recommendations for Unlock Wrist Diagnosis: Cases Guided by Figure Sunil Thirkannad. Radiographic findings, such as those in a figure sunil thirkannad, can diagnose pisotriquetral arthritis, a cause of ulnar-sided wrist pain. The article also covers the pisiform bone's anatomy, Watson's test for SLAC wrist (Scapholunate Advanced Collapse), and SNAC wrist (Scaphoid Nonunion Advanced Collapse) management. Understanding these conditions is crucial for accurate wrist assessments.
Welcome to this Grand Rounds presentation. Today, we are undertaking a deep, comprehensive exploration of complex wrist pathologies, utilizing specific clinical scenarios to guide our diagnostic and surgical rationale. The wrist is arguably the most biomechanically intricate joint in the human body, relying on a delicate interplay of ligamentous tethers, intercalated bone segments, and precise articular congruency. Even minor disruptions in this micro-environment can lead to profound functional deficits, chronic pain, and progressive arthropathy.
In this session, we will dissect two distinct but highly illustrative clinical presentations. The first involves the often-overlooked ulnar aspect of the wrist—specifically, the pisotriquetral articulation. The second transitions to the radial side, focusing on chronic scapholunate instability and the biomechanical collapse that inevitably follows. By mastering these two ends of the carpal spectrum, you will elevate your diagnostic acumen and refine your surgical decision-making.
Detailed Patient Presentation and Mechanism of Injury
We begin our analysis with two distinct clinical vignettes that highlight the diverse nature of carpal pathology.
Case 1: The Ulnar-Sided Conundrum
A 55-year-old male, an avid golfer and amateur tennis player, presents to your orthopedic clinic complaining of chronic, insidious-onset ulnar-sided wrist pain. He denies any acute traumatic event, fall on an outstretched hand (FOOSH), or sudden twisting injury. The pain has been progressively worsening over the past eighteen months. He notes that the pain is particularly exacerbated during the follow-through phase of his golf swing and when executing a forehand in tennis—motions that require forceful grip combined with extreme ulnar deviation and flexion. He reports a deep, aching discomfort localized to the volar-ulnar aspect of the wrist, occasionally radiating proximally along the forearm. Previous conservative management, including generic wrist splinting and oral non-steroidal anti-inflammatory drugs (NSAIDs), has yielded minimal relief.
Case 2: The Radial-Sided Collapse
In stark contrast, our second patient is a 68-year-old retired farmer who presents with a chief complaint of profound, activity-limiting pain in his dominant right wrist. He states that the discomfort began as an intermittent, dull ache approximately a decade ago but has recently escalated to the point where he can no longer perform basic daily activities, such as opening jars or lifting a coffee mug, without experiencing sharp, debilitating pain. When pressed about his history, he vaguely recalls a severe wrist sprain after a fall from a tractor in his late thirties, which was never formally evaluated or treated. He complains of significant weakness, a perceived loss of grip strength, and a sensation of "grinding" within the wrist during circumduction.
These two presentations represent classic endpoints of specific biomechanical failures. The first case directs our attention to the flexor carpi ulnaris (FCU) and its terminal sesamoid, the pisiform. The second case is a textbook presentation of chronic carpal instability leading to advanced degenerative changes, necessitating a thorough evaluation of the proximal carpal row's integrity.
Comprehensive Clinical Examination Findings
A meticulous physical examination is the cornerstone of wrist diagnosis. The wrist cannot be evaluated with a cursory glance; it requires a systematic, palpation-driven approach, isolating individual articulations and ligamentous intervals.
Evaluating the Pisotriquetral Articulation
In our first patient, inspection reveals no gross deformity, erythema, or significant effusion. Range of motion (ROM) is relatively preserved, though terminal flexion and ulnar deviation provoke sharp pain. The critical finding during palpation is exquisite point tenderness directly over the pisiform.
To isolate the pisotriquetral joint, we perform the Pisotriquetral Shear Test (or Grind Test). The examiner stabilizes the patient's wrist in a neutral position, grasps the pisiform between the thumb and index finger, and translates it medially and laterally (radially and ulnarly) against the triquetrum. In this patient, the maneuver elicits severe pain and palpable crepitus, pathognomonic for pisotriquetral arthritis. Furthermore, resisted activation of the flexor carpi ulnaris (FCU)—achieved by asking the patient to actively flex and ulnarly deviate the wrist against resistance—reproduces the patient's volar-ulnar pain. It is vital during this examination to rule out other ulnar-sided pathologies. We assess the triangular fibrocartilage complex (TFCC) via the fovea sign and ulnar impaction testing, both of which are negative in this patient. The extensor carpi ulnaris (ECU) tendon is stable within its subsheath, and the distal radioulnar joint (DRUJ) exhibits normal translation without instability.
Evaluating Scapholunate Competence
For the 68-year-old farmer, the examination focuses on the radial and central columns. There is visible swelling over the dorsal radiocarpal joint. Palpation reveals tenderness over the anatomic snuffbox and the dorsal scapholunate (SL) interval. Grip strength is objectively reduced to 40% of the contralateral side via Jamar dynamometry.
The most critical provocative maneuver in this scenario is the Watson’s Scaphoid Shift Test. To perform this test correctly, the examiner sits facing the patient. The examiner's thumb is placed firmly over the volar prominence of the scaphoid tuberosity, while the fingers wrap around the distal radius. The patient's wrist is initially placed in ulnar deviation and slight extension—a position where the scaphoid is normally extended and collinear with the forearm. The examiner then applies firm dorsal pressure to the scaphoid tuberosity while passively moving the patient's wrist into radial deviation and slight flexion.
In a normal wrist, the scaphoid flexes to accommodate the radial styloid, pushing the examiner's thumb volarly. However, in the setting of an incompetent scapholunate interosseous ligament (SLIL), the scaphoid cannot flex synchronously with the rest of the proximal row. Instead, the dorsal pressure forces the proximal pole of the scaphoid to subluxate dorsally over the dorsal rim of the radius. As the examiner releases thumb pressure, the scaphoid abruptly reduces back into the elliptical fossa with a palpable and audible "clunk." This positive Watson's test strongly indicates scapholunate instability, which, given the chronicity of this patient's symptoms, likely signifies advanced collapse.
Advanced Imaging and Diagnostics (X-ray, CT, MRI, Templating)
Radiographic evaluation must be tailored to the suspected pathology, utilizing specific views to unmask hidden arthrosis or subtle dynamic instability.
Imaging the Pisiform
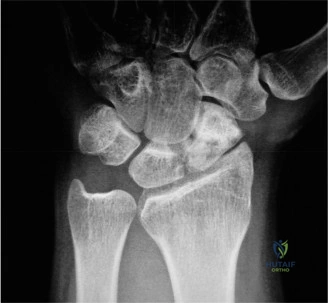
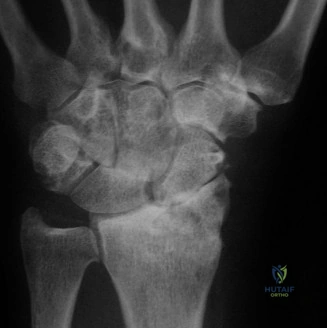
Standard posteroanterior (PA) and lateral radiographs of the wrist often fail to adequately visualize the pisotriquetral joint due to bony overlap from the distal pole of the scaphoid, the capitate, and the triquetrum itself. To properly assess this articulation, a 30-degree supinated AP view (the pisotriquetral view) is mandatory. In our first patient (referencing the classic Figure 3-10), this specific view reveals profound joint space narrowing, subchondral sclerosis, and prominent osteophyte formation at the pisotriquetral interface.
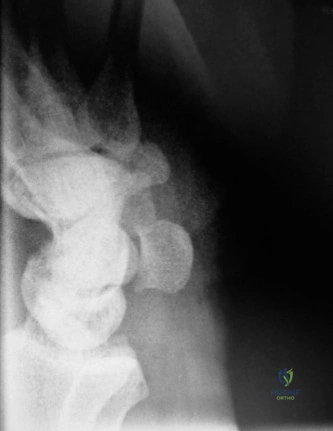
It is crucial to understand the osteology here. The pisiform is an atavistic, sesamoid bone. It is the only carpal bone that does not participate in the complex intercarpal kinematics of the proximal or distal rows. Instead, it lies entirely within the tendon of the flexor carpi ulnaris (FCU). The FCU-pisiform complex extends distally via robust ligamentous attachments: the pisotriquetral ligament, the pisohamate ligament, and the piso-5th metacarpal ligament. Notably, there is no piso-scaphoid ligament; the scaphoid resides on the entirely opposite side of the carpus.
Imaging Carpal Collapse
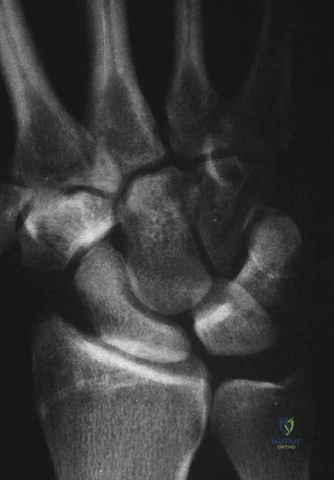
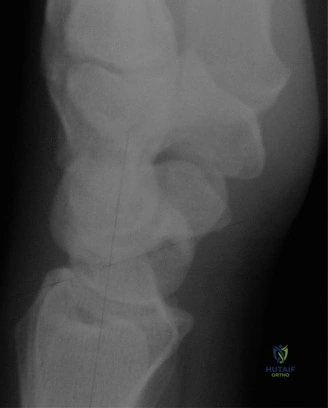
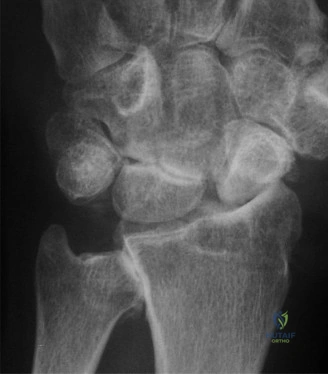
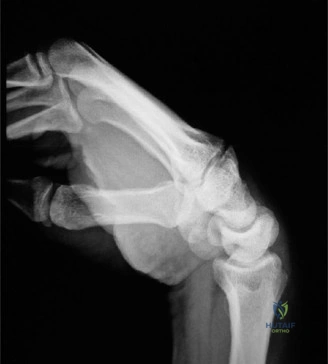
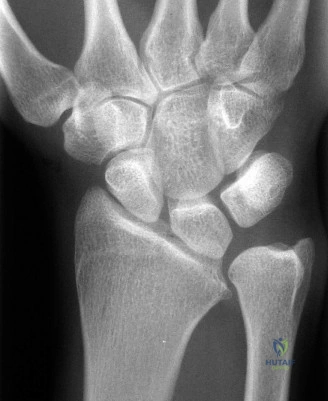
For the second patient, standard PA radiographs immediately reveal the diagnosis. We observe the classic Terry Thomas sign—a widening of the scapholunate interval greater than 3 mm. Furthermore, the lateral radiograph demonstrates a Dorsal Intercalated Segment Instability (DISI) deformity, characterized by a radiolunate angle greater than 15 degrees (lunate extended) and a scapholunate angle greater than 60 degrees.
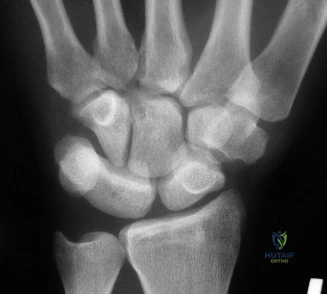
Advanced imaging, particularly Computed Tomography (CT), is highly beneficial for preoperative templating. A fine-cut CT scan accurately maps the extent of the degenerative changes. In scapholunate advanced collapse (SLAC), arthritis follows a highly predictable, sequential pattern. It begins at the radial styloid-scaphoid articulation (Stage I), progresses to involve the entire radioscaphoid fossa (Stage II), and eventually encompasses the capitolunate joint as the capitate migrates proximally into the widened SL gap (Stage III). Notably, the radiolunate joint is universally spared in SLAC wrist due to the concentric, congruent nature of the lunate fossa and the preservation of the short radiolunate ligaments.
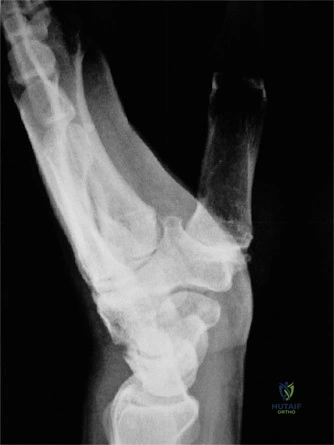
Magnetic Resonance Imaging (MRI) is less critical when advanced bony changes are visible on plain films, but it remains the gold standard for evaluating acute ligamentous injuries, TFCC tears, and the vascular status of the scaphoid (ruling out avascular necrosis or Preiser's disease).
Exhaustive Differential Diagnosis
When approaching wrist pain, the differential diagnosis must be anatomically compartmentalized. Below is a comprehensive breakdown of competing diagnoses for both ulnar and radial-sided wrist pain.
| Condition | Primary Location | Key Clinical Exam Finding | Radiographic Hallmark |
|---|---|---|---|
| Pisotriquetral Arthritis | Volar-Ulnar | Positive PT Grind Test; Pain with resisted FCU firing. | Joint space narrowing/osteophytes on 30° supinated view. |
| TFCC Tear | Dorsal-Ulnar | Positive Fovea sign; Pain with ulnar deviation and axial load. | Often normal X-ray; MRI shows articular disc disruption. |
| Ulnar Impaction Syndrome | Central-Ulnar | Pain with forceful grip and pronation; positive ulnar variance. | Ulnar positive variance; cystic changes in lunate/ulnar head. |
| ECU Tendinopathy/Subluxation | Dorsal-Ulnar | Palpable snapping over distal ulna during supination/pronation. | Normal X-ray; Ultrasound/MRI shows fluid in ECU sheath. |
| SLAC Wrist | Radial-Central | Positive Watson's Scaphoid Shift Test; reduced grip strength. | SL gap >3mm; radioscaphoid/capitolunate arthrosis. |
| De Quervain's Tenosynovitis | Radial Styloid | Positive Finkelstein's Test; pain over first dorsal compartment. | Normal X-ray; soft tissue swelling over radial styloid. |
| STT Arthritis | Volar-Radial | Pain at base of thenar eminence; positive STT grind. | Scaphotrapeziotrapezoidal joint space narrowing. |
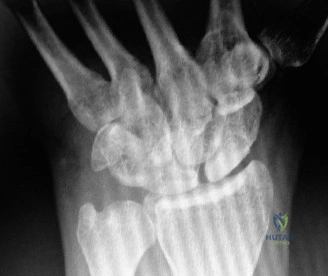
Differentiating these pathologies requires a nuanced understanding of wrist biomechanics. For instance, while both pisotriquetral arthritis and a TFCC tear present with ulnar-sided pain, the former is exacerbated by FCU loading (flexion/ulnar deviation), whereas the latter is aggravated by axial loading and rotation (pronation/supination) of the radiocarpal joint.
Complex Surgical Decision Making and Classifications
The decision to operate on the wrist is dictated by the failure of conservative management, the patient's functional demands, and the precise stage of the pathology.
Managing Pisotriquetral Arthritis
In the case of our 55-year-old golfer, conservative measures (steroid injections into the PT joint, splinting, activity modification) have failed. The surgical gold standard for isolated, refractory pisotriquetral arthritis is Pisiform Excision.
The biomechanical implications of removing the pisiform must be considered. The pisiform acts as a fulcrum, increasing the moment arm of the FCU tendon. Excision theoretically reduces the mechanical advantage of the FCU. However, extensive clinical outcome studies have demonstrated that patients tolerate this procedure exceptionally well, with no clinically significant loss of grip strength or wrist flexion power, provided the FCU tendon is meticulously repaired and stabilized during the closure.
Managing the SLAC Wrist
Surgical decision-making for the SLAC wrist is strictly guided by the Watson and Ballet classification of carpal collapse.
- Stage I: Arthritis isolated to the radial styloid. (Treatment: Radial styloidectomy and SL ligament reconstruction or PIN neurectomy).
- Stage II: Arthritis involving the entire scaphoid fossa of the radius. (Treatment: Proximal Row Carpectomy (PRC) or Scaphoid Excision and Four-Corner Fusion (4CF)).
- Stage III: Arthritis extending to the capitolunate articulation. (Treatment: 4CF is preferred over PRC, as PRC requires a pristine capitate head to articulate with the lunate fossa).
- Stage IV: Pancarpal arthritis, including the radiolunate joint. (Treatment: Total Wrist Arthrodesis).

For our 68-year-old farmer, CT imaging reveals Stage III SLAC wrist. The capitate head exhibits significant chondromalacia and subchondral cysts. Therefore, a Proximal Row Carpectomy is contraindicated. The procedure of choice is a Scaphoid Excision and Four-Corner Arthrodesis (Capitate, Lunate, Hamate, Triquetrum).
Step-by-Step Surgical Technique and Intervention
Technique 1: Pisiform Excision
- Positioning and Approach: The patient is positioned supine with a hand table. A tourniquet is applied. A 4 cm longitudinal or slightly zig-zag incision is made directly over the palpable FCU tendon, extending distally to the distal flexion crease.
- Neuromascular Protection: The most critical step is the identification and protection of the ulnar nerve and artery. These structures run immediately radial and deep to the FCU tendon and pisiform within Guyon's canal. The ulnar nerve bifurcates into superficial (sensory) and deep (motor) branches just distal to the pisiform.
- Subperiosteal Dissection: The FCU tendon sheath is incised. A longitudinal incision is made directly through the tendon fibers overlying the pisiform. Using a sharp scalpel and a small periosteal elevator, the pisiform is carefully shelled out of its tendinous envelope in a subperiosteal fashion.
- Excision and Inspection: The bone is excised, and the underlying triquetral articular surface is inspected to confirm the diagnosis of severe chondral wear.
- Reconstruction: The empty tendinous sleeve of the FCU is repaired using non-absorbable figure-of-eight sutures. It is imperative to suture the proximal FCU stump to the distal ligamentous extensions (pisohamate and pisotriquetral ligaments) to maintain the resting tension of the musculotendinous unit.
Technique 2: Scaphoid Excision and Four-Corner Fusion (4CF)
- Approach: A dorsal longitudinal incision is made centered over the Lister's tubercle. The extensor retinaculum is incised, typically elevating the third compartment (EPL) and opening the fourth compartment.
- Neurectomy: A posterior interosseous nerve (PIN) neurectomy is routinely performed at the floor of the fourth compartment to provide partial denervation and pain relief.
- Capsulotomy: A ligament-sparing dorsal capsulotomy (e.g., Berger's Mayo approach) is utilized to expose the carpus.
- Scaphoid Excision: The scaphoid is fragmented using an osteotome or rongeur and completely excised. Care is taken to preserve the volar radiocarpal ligaments.
- Decortication: The articular surfaces between the capitate, lunate, hamate, and triquetrum are meticulously denuded of all cartilage down to bleeding subchondral bone using a high-speed burr and curettes.
- Reduction and Fixation: The lunate, which is typically in a DISI posture (extended), must be reduced to a neutral position. The capitate is then reduced onto the lunate. Temporary K-wires hold the four bones in strict anatomic alignment.
- Hardware Application: Rigid internal fixation is achieved using a dorsal circular "spider" plate, headless compression screws, or memory-metal staples. Bone graft, harvested from the excised scaphoid or distal radius, is packed tightly into the interstices.
Strict Post-Operative Protocol and Rehabilitation Stages
Rehabilitation is heavily dependent on the nature of the surgical intervention. Soft tissue repairs (FCU reconstruction) require different pacing than bony fusions (4CF).
Post-Operative Protocol: Pisiform Excision
- Phase 1 (0-2 Weeks): The wrist is immobilized in a volar splint in 10-15 degrees of flexion to remove tension from the FCU repair. Digital motion is encouraged immediately to prevent tendon adhesions.
- Phase 2 (2-6 Weeks): Sutures are removed. The patient is transitioned to a removable custom orthosis. Active range of motion (AROM) of the wrist is initiated, focusing on flexion and extension. Passive stretching and resisted FCU firing are strictly avoided.
- Phase 3 (6-10 Weeks): Progressive strengthening begins. Grip strengthening and gentle resisted ulnar deviation are introduced. The patient can typically return to golf or racket sports by weeks 10-12.
Post-Operative Protocol: Four-Corner Fusion
- Phase 1 (0-2 Weeks): The wrist is immobilized in a bulky surgical dressing and volar splint. Elevation and strict digital AROM are mandatory to mitigate edema and prevent intrinsic tightness.
- Phase 2 (2-6 Weeks): The patient is placed in a short-arm fiberglass cast or a rigid custom thermoplastic splint. No wrist motion is permitted. Radiographs are obtained at 6 weeks to assess early trabecular bridging.
- Phase 3 (6-12 Weeks): Once clinical and radiographic signs of union are evident, the splint is weaned. AROM and active-assisted ROM (AAROM) of the wrist commence. Patients must be counseled that a 4CF will permanently reduce their wrist flexion/extension arc by approximately 50% compared to the normal contralateral side.
- Phase 4 (12+ Weeks): Heavy lifting and impact activities are gradually reintroduced once solid bony fusion is confirmed on a CT scan or high-quality radiographs.
High-Yield Clinical Pearls and Pitfalls
To conclude this Grand Rounds presentation, let us review the critical takeaways that will keep you out of trouble in the operating room and the clinic.
Pearls
- Anatomic Reality: Never forget that the pisiform is a sesamoid bone. It lives inside the FCU. When excising it, you are performing an intratendinous procedure.
- Ligamentous Distinctions: The distal extensions of the FCU-pisiform complex include the pisotriquetral, pisohamate, and piso-5th metacarpal ligaments. There is no piso-scaphoid ligament. Do not let this trap you on board examinations.
- The Watson Test Nuance: A positive Watson test is not just pain; it is the palpable, mechanical clunk of the scaphoid reducing from a subluxated position. Pain alone may simply indicate radioscaphoid arthrosis or synovitis.
- SLAC Spares the Lunate: The radiolunate joint is the "safe harbor" of the SLAC wrist. Because the lunate fossa is spherical and concentric, it does not undergo the shear forces seen in the elliptical scaphoid fossa. This is the entire biomechanical basis for allowing a Proximal Row Carpectomy or Four-Corner Fusion to succeed.
Pitfalls
- Guyon's Canal Injury: The most devastating complication of a pisiform excision is iatrogenic injury to the ulnar nerve. Always dissect on the radial aspect of the FCU with extreme caution. Subperiosteal dissection of the pisiform is your safest plane.
- Missed Capitate Arthrosis: Performing a Proximal Row Carpectomy (PRC) in a Stage III SLAC wrist is a catastrophic error. If the capitate head is devoid of cartilage, placing it into the lunate fossa of the radius will result in immediate, painful capitoradial arthritis, necessitating a salvage total wrist fusion. Always inspect the capitate head intraoperatively, or rely on a high-quality preoperative MRI/CT.
- Inadequate Lunate Reduction: During a Four-Corner Fusion, failing to correct the DISI posture of the lunate before applying the fixation plate will result in a dorsal impingement syndrome and severely restricted wrist extension. The lunate must be levered out of extension and pinned in neutral alignment prior to decortication and fixation.
By mastering the intricate anatomy of the ulnar sesamoids and the progressive biomechanical collapse of the radial column, you equip yourself to handle the vast majority of chronic wrist pathologies. Thank you for your attention to this exhaustive review of wrist diagnosis and surgical management.
