Christine M Kleinert Discussion: Solving Difficult Wrist Fractures
Key Takeaway
For anyone wondering about Christine M Kleinert Discussion: Solving Difficult Wrist Fractures, Scaphoid fractures require suspicion with anatomical snuff box tenderness, even if initial X-rays are negative; treat with splinting and re-imaging in 2-4 weeks. The christine m kleinert discussion highlights CT scans as more reliable for assessing healing than X-rays. For persistent non-healing, Open Reduction Internal Fixation (ORIF) with cancellous bone graft and headless compression screws is the recommended treatment.
Comprehensive Introduction and Patho-Epidemiology
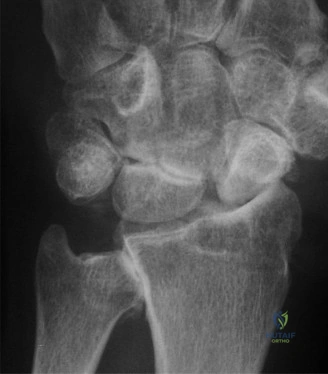
The management of complex wrist fractures remains one of the most intellectually demanding and technically unforgiving arenas in orthopedic surgery. Among these, injuries to the carpus—specifically scaphoid fractures—present a unique diagnostic and therapeutic paradigm. Consider the classic clinical scenario: a 14-year-old patient presents with acute wrist pain following a fall on an outstretched hand (FOOSH). Clinical examination reveals focal tenderness over the anatomical snuff box, yet the initial radiographic series is entirely unremarkable. This presentation epitomizes the "occult scaphoid fracture," a diagnostic trap that has historically confounded clinicians and led to devastating long-term sequelae if mismanaged.
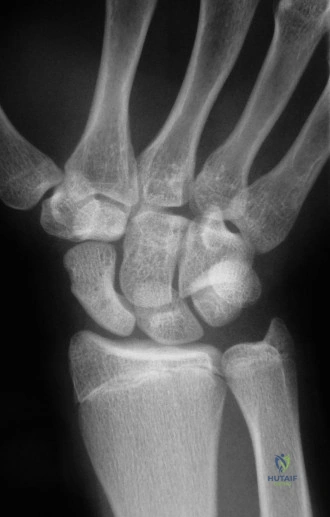
The epidemiology of scaphoid fractures dictates a high index of suspicion. They account for approximately 15% of all acute wrist injuries and represent nearly 60% to 70% of all carpal fractures. The incidence peaks in young, active males, typically between the ages of 15 and 30, often resulting from high-energy sporting activities or motor vehicle collisions. In the pediatric and adolescent populations, the incidence is lower but steadily rising due to increased participation in competitive athletics. The cartilaginous nature of the pediatric carpus provides some resilience, but as ossification completes, the biomechanical vulnerabilities mirror those of the adult.
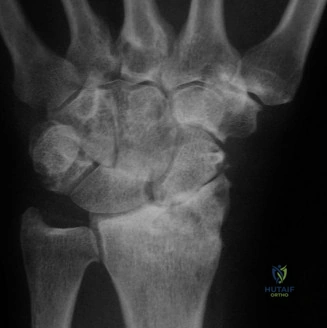
The pathophysiology of these fractures is intimately linked to the unique position of the scaphoid, which acts as a vital mechanical bridge between the proximal and distal carpal rows. During a FOOSH injury, the wrist is forced into extreme dorsiflexion, ulnar deviation, and intercarpal supination. The scaphoid impacts against the dorsal rim of the radius, creating a bending moment that concentrates stress at the waist of the scaphoid. If the applied force exceeds the ultimate tensile strength of the trabecular bone, a fracture ensues. The challenge lies not only in the initial diagnosis but in the high propensity for delayed union, non-union, and avascular necrosis (AVN) due to the tenuous retrograde blood supply.
The Diagnostic Paradox of the Occult Fracture
The occult scaphoid fracture is a well-documented phenomenon where initial plain radiographs fail to demonstrate a fracture line despite a high-energy mechanism and positive clinical signs (snuff box tenderness, scaphoid tubercle tenderness, and pain with axial loading of the thumb). In such instances, the standard of care dictates that the clinician must assume a fracture is present. The patient is universally placed in a thumb spica splint, and a follow-up evaluation is mandated at 10 to 14 days.
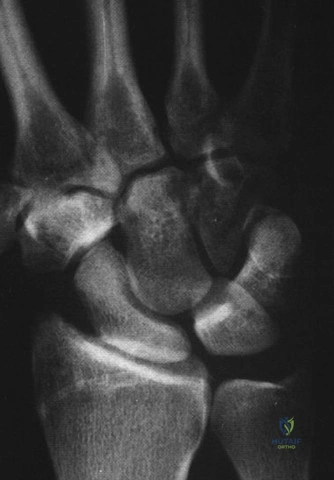
By the second or third week post-injury, osteoclastic resorption at the fracture site widens the gap, often rendering the previously invisible fracture apparent on repeat radiographs. If the patient returns at 4 weeks with persistent pain and a newly visible fracture line, the orthopedic surgeon is faced with a critical decision regarding the continuation of conservative management versus surgical intervention. In adolescent patients, where healing potential is robust, continuing cast immobilization for an additional 4 to 6 weeks is often the most prudent course, contrasting with the adult population where early surgical fixation is increasingly favored to minimize immobilization time and accelerate return to function.
Detailed Surgical Anatomy and Biomechanics
A profound understanding of carpal anatomy and kinematics is the bedrock upon which successful surgical intervention is built. The scaphoid is a complex, boat-shaped bone entirely covered by articular cartilage on 80% of its surface area. This extensive articular coverage severely limits the available surface area for vascular ingress and ligamentous attachment, rendering the bone uniquely susceptible to ischemic complications following trauma.
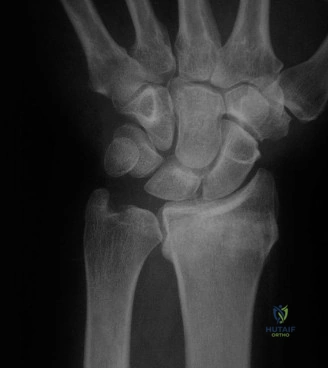
Vascular Anatomy and Ischemic Vulnerability
The vascular supply to the scaphoid is the single most critical anatomical factor dictating fracture healing. The primary arterial supply is derived from the radial artery. As the radial artery traverses the anatomic snuff box, it gives off dorsal carpal branches that enter the scaphoid through the dorsal ridge, supplying the proximal 70% to 80% of the bone via a retrograde intraosseous network. A secondary, minor volar vascular contribution enters the distal pole via branches from the superficial palmar arch.
Because the blood supply to the proximal pole is entirely dependent on retrograde flow from the distal intraosseous vessels, fractures occurring at the waist or proximal third of the scaphoid abruptly sever this vascular tether. Consequently, proximal pole fractures carry an exceptionally high risk of avascular necrosis (approaching 100% in very proximal lesions) and non-union, necessitating aggressive surgical management and often vascularized bone grafting.
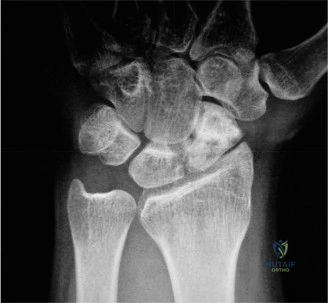
Carpal Kinematics and the Intercalated Segment
Biomechanically, the proximal carpal row (scaphoid, lunate, triquetrum) functions as an intercalated segment. It has no direct tendinous insertions; its movement is entirely passive, dictated by the geometry of the articular surfaces and the complex capsuloligamentous constraints during motion of the distal carpal row and radius. The scaphoid bridges the proximal and distal rows, stabilizing the midcarpal joint.
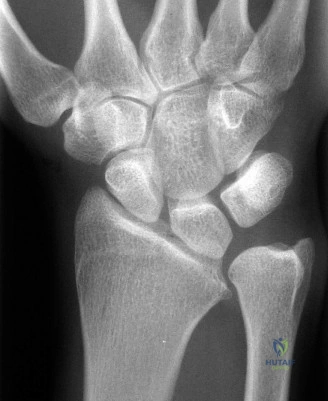
When the scaphoid fractures, this vital mechanical link is disrupted. The distal fragment flexes with the distal carpal row, while the proximal fragment extends with the lunate (due to the intact scapholunate interosseous ligament). This opposing motion results in the classic "humpback" deformity—a volar angular collapse of the scaphoid that alters carpal kinematics, reduces the carpal height, and leads to a dorsal intercalated segment instability (DISI) pattern. Failure to correct this anatomical collapse during surgical fixation inevitably leads to altered contact mechanics, progressive articular wear, and eventual scaphoid non-union advanced collapse (SNAC).
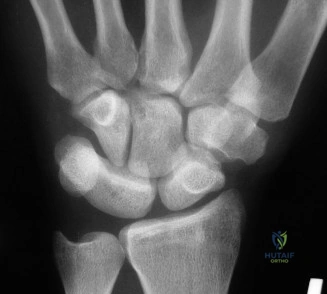
Ligamentous Constraints
The scaphoid is stabilized by a stout network of intrinsic and extrinsic ligaments. The radioscaphocapitate (RSC) ligament acts as a crucial volar sling, supporting the waist of the scaphoid. The scapholunate interosseous ligament (SLIL) is the primary intrinsic stabilizer, divided into dorsal, proximal, and volar regions, with the dorsal region being the thickest and most biomechanically significant. Surgical approaches must meticulously preserve these ligamentous structures to prevent iatrogenic carpal instability.
Exhaustive Indications and Contraindications
The decision-making algorithm for wrist fractures, particularly scaphoid fractures, hinges on patient age, fracture location, degree of displacement, and the chronicity of the injury. While conservative management has historically been the mainstay, the pendulum has swung toward operative fixation in specific cohorts to mitigate the socioeconomic burden of prolonged immobilization and reduce non-union rates.
Defining Operative Thresholds
In the adult population, any scaphoid fracture demonstrating greater than 1 mm of displacement is an absolute indication for surgical fixation. Displacement signifies disruption of the cartilaginous envelope and a higher energy injury, correlating with a non-union rate exceeding 50% if treated non-operatively. Furthermore, an intrascaphoid angle greater than 35 degrees or a radiolunate angle greater than 15 degrees indicates a humpback deformity and DISI collapse, respectively, mandating open reduction and internal fixation (ORIF).

Conversely, in the pediatric and adolescent populations, the robust osteogenic potential often allows for successful conservative management even in the setting of delayed presentation. As highlighted in the introductory case, a 14-year-old presenting with a visible fracture at 4 weeks post-injury, having been initially treated as an occult fracture, is often best served by continuing cast immobilization. The healing rates for non-displaced scaphoid waist fractures in adolescents approach 95% with cast immobilization alone.
Table of Indications and Contraindications
| Clinical Scenario | Primary Indication | Relative Contraindications | Preferred Management Strategy |
|---|---|---|---|
| Acute Non-displaced Waist Fracture (Adult) | Patient preference for early return to work/sport | Poor soft tissue envelope, severe osteopenia | Percutaneous Headless Compression Screw |
| Acute Non-displaced Waist Fracture (Adolescent) | Preserved carpal alignment, <1mm displacement | Polytrauma requiring early mobilization | Long-arm to short-arm thumb spica casting |
| Displaced Waist Fracture (>1mm) | Restoration of anatomy, prevention of non-union | Active local infection | Open Reduction Internal Fixation (ORIF) |
| Proximal Pole Fracture | High risk of AVN and non-union | Extreme comminution precluding fixation | Dorsal approach ORIF +/- vascularized graft |
| Humpback Deformity / DISI | Volar angular collapse, carpal instability | Advanced radiocarpal arthritis (SNAC III) | Volar approach ORIF with structural bone graft |
| Chronic Non-union without Arthritis | Prevention of progressive carpal collapse | Patient medically unfit for surgery | ORIF with iliac crest or distal radius bone graft |
Pre-Operative Planning, Templating, and Patient Positioning
Meticulous pre-operative planning is the sine qua non of successful orthopedic surgery. In the context of difficult wrist fractures, this begins with an exhaustive imaging protocol to define fracture geometry, assess vascularity, and map out the surgical trajectory.
Advanced Imaging Modalities
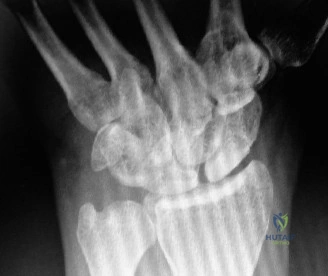
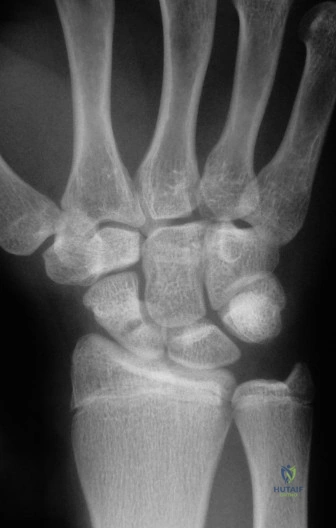
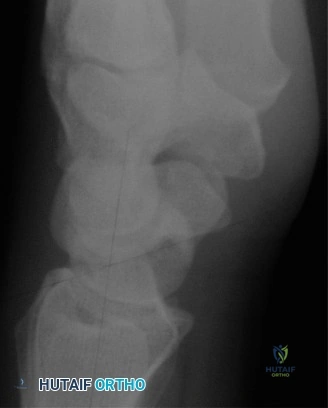
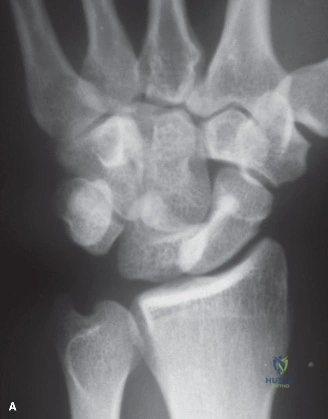
Plain radiography remains the initial screening tool. A dedicated scaphoid series must include posteroanterior (PA), true lateral, pronated oblique, and ulnar deviated (scaphoid) views. The ulnar deviated view extends the scaphoid, bringing its longitudinal axis parallel to the image receptor and unmasking subtle waist fractures.
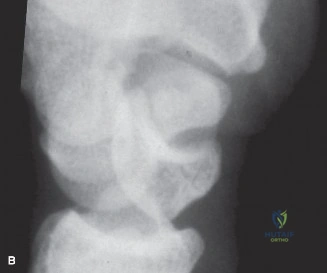
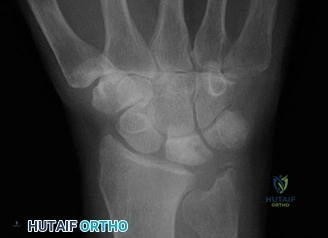
However, plain films are notoriously inadequate for assessing fracture union or complex comminution. As demonstrated in the clinical scenario, when a patient returns at 8 weeks post-injury and the clinician must determine whether the fracture has definitively healed, a Computed Tomography (CT) scan is the gold standard. CT scans oriented along the longitudinal axis of the scaphoid provide unparalleled visualization of trabecular bridging. A fracture is generally considered healed when greater than 50% trabecular bridging is observed across the fracture site.
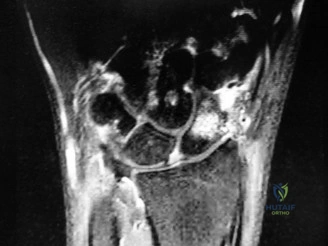
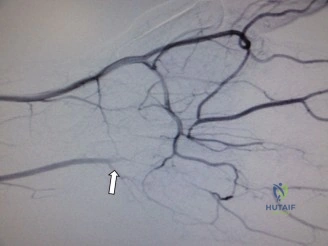
Magnetic Resonance Imaging (MRI) plays a distinct but equally critical role. It is the most sensitive modality for detecting acute occult fractures within the first 48 hours of injury. Furthermore, in the setting of established non-union, gadolinium-enhanced MRI is utilized to assess the vascularity of the proximal pole, which directly dictates the choice of bone graft (vascularized versus non-vascularized) during reconstructive procedures.
Patient Positioning and Fluoroscopic Setup
The patient is positioned supine on the operating table with the operative extremity extended on a radiolucent hand table. A high-arm tourniquet is applied over copious padding. The positioning of the fluoroscopy C-arm is critical; the surgeon must be able to obtain perfect PA and lateral views of the carpus without compromising the sterile field. Often, the C-arm is brought in perpendicular to the axis of the limb, allowing the surgeon to rotate the wrist rather than the machine to obtain orthogonal views.
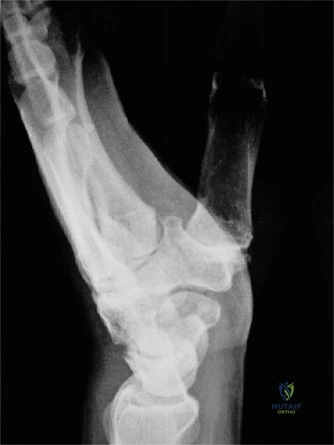
Pre-operative templating involves measuring the anticipated screw length. The ideal headless compression screw should engage the dense subchondral bone of both the proximal and distal poles without penetrating the articular surface. The surgeon must plan for a screw that is approximately 2 to 4 mm shorter than the measured total length of the scaphoid to ensure it remains completely buried within the bone.
Step-by-Step Surgical Approach and Fixation Technique
The surgical approach to the scaphoid is dictated by the location of the fracture and the presence of deformity. Broadly, volar approaches are utilized for waist and distal pole fractures, particularly when a humpback deformity requires correction. Dorsal approaches are reserved for proximal pole fractures to allow direct, perpendicular access to the small proximal fragment.
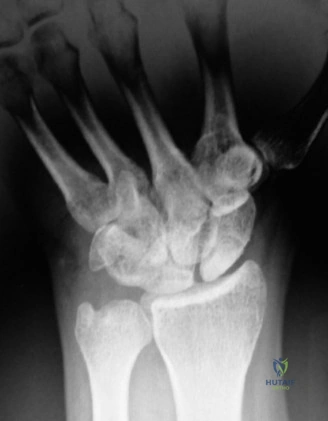
The Volar Approach (Russe)
The traditional volar approach utilizes a longitudinal or slightly curvilinear incision over the flexor carpi radialis (FCR) tendon.
1. Superficial Dissection: The FCR sheath is incised, and the tendon is retracted ulnarly. This protects the palmar cutaneous branch of the median nerve.
2. Deep Dissection: The floor of the FCR sheath is incised to expose the underlying radiocarpal capsule. The radial artery is carefully identified and retracted radially.
3. Capsulotomy: A longitudinal or T-shaped capsulotomy is performed, exposing the radioscaphocapitate (RSC) and long radiolunate (LRL) ligaments. These ligaments are carefully split or reflected to expose the scaphoid waist.
4. Deformity Correction: If a humpback deformity is present, the fracture site is debrided of fibrous tissue. The wrist is extended, and a small lamina spreader or a K-wire is used as a joystick to correct the volar flexion of the distal pole. A structural bone graft (often harvested from the iliac crest or distal radius) is impacted into the volar defect to restore the anatomical length and alignment.
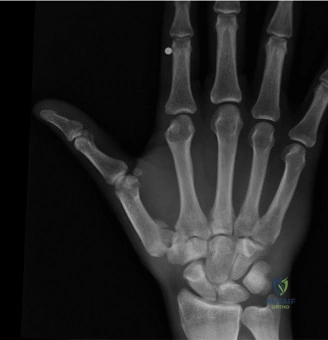
The Dorsal Approach
For proximal pole fractures, a dorsal approach provides optimal trajectory for screw placement along the central axis of the scaphoid.
1. Incision: A longitudinal incision is made over the Lister's tubercle.
2. Interval: The extensor retinaculum is incised over the third dorsal compartment, and the extensor pollicis longus (EPL) tendon is transposed radially.
3. Capsulotomy: A ligament-sparing dorsal capsulotomy is performed, taking care not to disrupt the dorsal portion of the scapholunate interosseous ligament.
4. Exposure: The proximal pole of the scaphoid is identified. The wrist is acutely flexed to bring the proximal pole into view and allow for a straight-line trajectory down the anatomic axis of the scaphoid.
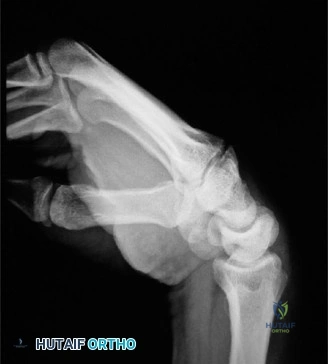
Fixation with Headless Compression Screws
Regardless of the approach, the biomechanical goal is rigid, interfragmentary compression. Modern fixation relies on headless, variable-pitch compression screws.
1. Guide Wire Placement: A 0.045-inch K-wire is advanced from the proximal to the distal pole (or vice versa) under strict fluoroscopic guidance. The wire must be positioned in the central-central axis of the scaphoid on both PA and lateral views. Eccentric placement significantly reduces the biomechanical strength of the construct.
2. Measurement and Drilling: The depth is measured, and an appropriate length screw is selected. The near cortex is over-drilled, and the far fragment is tapped if necessary.
3. Screw Insertion: The headless screw is inserted. The variable pitch design (wider threads distally, tighter threads proximally) ensures that as the screw is seated, the fracture fragments are drawn together, generating robust compression.
4. Confirmation: Fluoroscopy is utilized in multiple planes to confirm that the screw is entirely intraosseous and that no threads are proud within the radioscaphoid or scaphotrapezial joints.
Complications, Incidence Rates, and Salvage Management
Despite meticulous surgical technique, scaphoid fractures are fraught with complications. The surgeon must be intimately familiar with the natural history of failed fixation and the salvage options available.
Non-Union and Avascular Necrosis
Scaphoid non-union occurs in approximately 5% to 10% of treated fractures, but this rate skyrockets to over 50% in displaced or proximal pole fractures. AVN of the proximal pole complicates up to 30% of waist fractures and nearly 100% of proximal fifth fractures. When non-union occurs with a viable proximal pole, revision ORIF with non-vascularized structural bone grafting (e.g., iliac crest) is indicated. However, if the proximal pole is necrotic (as evidenced by lack of punctate bleeding intraoperatively or absent enhancement on MRI), a vascularized bone graft is mandatory. The 1,2-Intercompartmental Supraretinacular Artery (1,2-ICSRA) graft, pedicled from the distal radius, or a free medial femoral condyle vascularized graft are the procedures of choice.
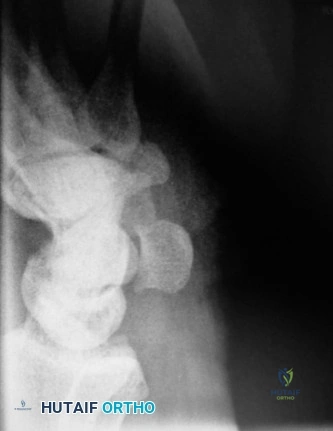
Scaphoid Non-Union Advanced Collapse (SNAC)
Untreated scaphoid non-union inevitably alters carpal kinematics, leading to a predictable pattern of degenerative arthritis known as SNAC wrist.
* Stage I: Arthritis localized to the radial styloid and the distal scaphoid fragment.
* Stage II: Progressive arthritis involving the entire radioscaphoid articulation.
* Stage III: Arthritis extending to the capitolunate joint. The radiolunate joint is characteristically spared due to the congruent spherical articulation and lack of shear forces.
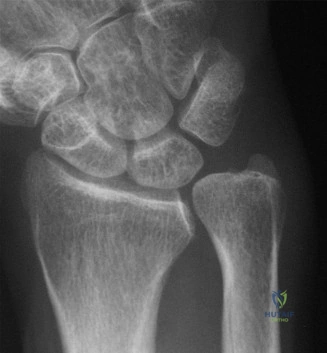
Salvage Procedures
When reconstructive efforts fail or advanced arthritis (SNAC II/III) is present, salvage procedures are required to alleviate pain while preserving a functional arc of motion.
| Complication Stage | Pathoanatomy | Recommended Salvage Procedure | Expected Functional Outcome |
|---|---|---|---|
| SNAC Stage I | Radial styloid arthritis | Radial styloidectomy + Scaphoid ORIF/Graft | Preserved grip strength, near-normal ROM |
| SNAC Stage II | Radioscaphoid arthritis | Proximal Row Carpectomy (PRC) OR Scaphoid Excision + 4-Corner Fusion | 60% normal ROM, 70-80% grip strength |
| SNAC Stage III | Capitolunate arthritis | Scaphoid Excision + 4-Corner Fusion | 50% normal ROM, 80% grip strength |
| SNAC Stage IV | Pancarpal arthritis | Total Wrist Arthrodesis | Pain-free, rigid wrist, strong grip |
For a Proximal Row Carpectomy (PRC) to be successful, the capitate head and the lunate fossa of the radius must have preserved articular cartilage, as they will form the new radiocarpal articulation. If the capitate is arthritic (SNAC III), a four-corner fusion (capitate, hamate, lunate, triquetrum) with scaphoid excision is the preferred motion-preserving salvage operation.
Phased Post-Operative Rehabilitation Protocols
The post-operative rehabilitation following scaphoid fixation is a delicate balance between protecting the surgical construct and preventing disabling wrist stiffness. The protocol is highly individualized based on the security of fixation, bone quality, and patient compliance.
Phase I: Maximum Protection (Weeks 0-2)
Immediately post-operatively, the patient is placed in a bulky soft dressing reinforced with a volar plaster splint, immobilizing the wrist in neutral and the thumb in slight abduction. Elevation and active digital range of motion (ROM) are aggressively encouraged to mitigate edema and prevent extensor tendon adhesions. At the two-week mark, sutures are removed. If fixation is deemed exceptionally rigid in a young, compliant adult, the patient may be transitioned to a removable custom thermoplastic thumb spica orthosis.
Phase II: Early Mobilization (Weeks 2-6)
During this phase, the patient begins gentle, active range of motion of the wrist and thumb out of the splint under the guidance of a certified hand therapist. Passive stretching and forceful mobilization are strictly contraindicated. The "dart-thrower's motion" (coupled radial extension and ulnar flexion) is emphasized, as this motion occurs primarily at the midcarpal joint and minimizes shear stress across the scaphoid fracture site. The splint is worn at all times between exercise sessions and at night.
Phase III: Strengthening and Consolidation (Weeks 6-12)
At 6 to 8 weeks, advanced imaging—ideally a CT scan, as discussed in the clinical case—is obtained to objectively assess trabecular bridging. Once bridging is confirmed, the splint is gradually weaned. Progressive resistive exercises are initiated, focusing on grip strength and dynamic stabilization of the carpus by the flexor carpi radialis and extensor carpi ulnaris. Return to contact sports or heavy manual labor is typically delayed until 12 to 16 weeks post-operatively, contingent upon full radiographic union and restoration of at least 80% of contralateral grip strength.
Summary of Landmark Literature and Clinical Guidelines
The evolution of scaphoid fracture management is deeply rooted in evidence-based medicine. The historical reliance on prolonged casting has been challenged by modern surgical techniques, yet the literature demands a nuanced approach rather than universal operative intervention.
The SWIFFT (Scaphoid Waist Internal Fixation for Fractures Trial) by Dias et al. is a landmark multicenter randomized controlled trial that profoundly influenced contemporary guidelines. The study compared early surgical fixation versus cast immobilization for acute, non-displaced scaphoid waist fractures in adults. The findings demonstrated no significant difference in long-term functional outcomes, grip strength, or non-union rates between the two groups. However, the surgical cohort experienced a higher rate of early complications, while the conservative cohort required a longer duration of immobilization. This trial underscores the principle that non-displaced fractures can be managed effectively with casting, reserving surgery for displaced fractures or patients prioritizing immediate mobilization.
Regarding imaging, the American Academy of Orthopaedic Surgeons (AAOS) clinical practice guidelines strongly advocate for the use of MRI in the acute setting for suspected occult fractures. The cost-effectiveness of an early MRI outweighs the socioeconomic burden of unnecessary prolonged casting and lost productivity. Furthermore, the literature unequivocally supports the use of multi-planar CT scanning for the evaluation of fracture union at the 8-to-12-week mark, as plain radiographs have a notoriously low positive predictive value for assessing trabecular continuity across the complex three-dimensional geometry of the scaphoid.
In conclusion, solving difficult wrist fractures requires a mastery of carpal anatomy, a deep respect for the tenuous vascularity of the scaphoid, and a technically precise surgical execution. Whether managing a 14-year-old with a delayed presentation or a high-performance athlete with an acute displaced fracture, the orthopedic surgeon must synthesize clinical acumen, advanced imaging, and evidence-based literature to restore the intricate mechanics of the human hand.
