Wrist Recovery Guide: Mastering Degrees with Forearm Movement
Key Takeaway
Here are the crucial details you must know about Wrist Recovery Guide: Mastering Degrees with Forearm Movement. Initial treatment for a transverse pisiform fracture includes short arm splinting. Should this fail, surgical excision of the pisiform is the preferred procedure for chronic pain, generally without major functional deficit. Post-operative rehabilitation aims to restore full wrist motion, progressing through various degrees with forearm support and stability to ensure optimal recovery and function.
Comprehensive Introduction and Patho-Epidemiology
The intricate biomechanics of the human wrist and forearm rely upon a delicate, perfectly orchestrated interplay between carpal osseous architecture, capsuloligamentous constraints, and dynamic musculotendinous units. When authoring a definitive guide to wrist recovery—specifically focusing on the mastery of functional degrees of forearm movement—one must address the entire kinematic chain. Forearm pronation and supination are not isolated events occurring solely at the proximal and distal radioulnar joints; they are intrinsically linked to the stability and pain-free motion of the radiocarpal, midcarpal, and carpometacarpal (CMC) articulations. Pathology at either the extreme ulnar border or the extreme radial border of the wrist can severely truncate the functional arc of motion, leading to profound disability in both elite athletes and the aging population.

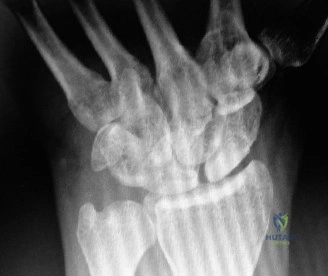
On the ulnar aspect of the wrist, the pisiform bone represents a unique anatomical and biomechanical entity. Fractures of the pisiform are relatively rare, comprising approximately 1% to 2% of all carpal fractures. They are most frequently encountered in the athletic population, particularly among football players, rugby athletes, and racket sports enthusiasts. The mechanism of injury typically involves a direct, high-energy blow to the hypothenar eminence during a fall on an outstretched hand, or a violent, resisted avulsion force transmitted through the flexor carpi ulnaris (FCU) tendon. Patients acutely present with severe, localized ulnar-sided wrist pain that is exacerbated by active wrist flexion and ulnar deviation. Because the pisiform acts as a dynamic fulcrum, any disruption to its integrity directly impairs the dart-thrower’s motion—a coupled kinematic arc essential for throwing, striking, and complex occupational tasks.
Conversely, on the radial aspect of the wrist, pathology of the first carpometacarpal joint presents a vastly different epidemiological profile but an equally devastating impact on forearm and wrist function. First CMC joint osteoarthritis is a progressive, degenerative condition that disproportionately affects post-menopausal females. Patients typically present with an insidious onset of base-of-thumb pain, independent of any acute traumatic event. The progressive loss of articular cartilage at the trapeziometacarpal joint leads to dorsal subluxation of the metacarpal base, secondary adduction contracture of the thumb web space, and compensatory hyperextension of the metacarpophalangeal (MCP) joint. This cascade of deformity severely compromises grip strength, key pinch, and the ability to perform forceful supination tasks, such as turning a key or opening a jar.
To master the degrees of wrist and forearm recovery, the orthopedic surgeon must possess an exhaustive understanding of these disparate yet functionally connected pathologies. Whether managing the acute trauma of a pisiform fracture in a young athlete or the chronic, debilitating pain of first CMC arthritis in an elderly patient, the ultimate goal remains the same: the restoration of a stable, painless, and kinematically sound wrist. This chapter will provide an uncompromising, highly technical exploration of the surgical anatomy, operative indications, meticulous surgical techniques, and advanced rehabilitation protocols required to achieve optimal clinical outcomes in the management of these complex wrist disorders.
Detailed Surgical Anatomy and Biomechanics
The pisiform is embryologically and anatomically classified as a sesamoid bone, distinguishing it from the other seven intercalated carpal bones. It develops entirely within the substance of the flexor carpi ulnaris (FCU) tendon and articulates exclusively with the volar surface of the triquetrum via a flat, synovial articulation. The primary biomechanical function of the pisiform is to serve as an anterior fulcrum, effectively displacing the FCU tendon away from the axis of rotation of the radiocarpal joint. This volar displacement significantly increases the moment arm of the FCU, enhancing its mechanical advantage during forceful wrist flexion and ulnar deviation. The stability of the pisiform is maintained by the robust pisohamate and pisometacarpal ligaments, which are functional distal extensions of the FCU tendon, inserting into the hook of the hamate and the base of the fifth metacarpal, respectively.
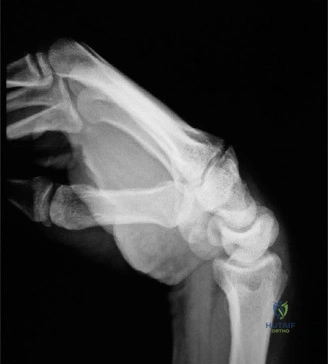
Clinically, the anatomical relationships of the pisiform are of paramount importance, particularly regarding the ulnar neurovascular bundle. The pisiform forms the medial (ulnar) wall of Guyon’s canal. The ulnar nerve and artery pass immediately radial to the pisiform, bifurcating into their superficial (sensory) and deep (motor) branches just distal to the bone. The deep motor branch of the ulnar nerve dives between the abductor digiti minimi and the flexor digiti minimi, passing in close proximity to the pisohamate ligament. Any trauma to the pisiform, hypertrophic non-union, or surgical intervention in this area carries a high risk of iatrogenic injury or compression to the ulnar nerve. Furthermore, the pisiform is not an isolated static structure; its dynamic excursion during wrist motion is critical. During wrist flexion, the FCU contracts, pulling the pisiform proximally, while during wrist extension, it glides distally.
On the radial side, the trapeziometacarpal (first CMC) joint is a highly specialized biconcave-biconvex saddle joint (articulatio sellaris). This unique geometric configuration allows for a vast degree of freedom, enabling flexion, extension, abduction, adduction, and the critical coupled motion of opposition. However, this extensive mobility comes at the cost of inherent osseous instability. Stability is heavily reliant on a complex network of capsuloligamentous structures, the most critical being the anterior oblique ligament (AOL), often referred to as the "beak ligament." The AOL originates from the volar tubercle of the trapezium and inserts onto the volar-ulnar beak of the first metacarpal base. It is the primary restraint against dorsal and radial subluxation of the metacarpal during functional pinch.
The biomechanical forces transmitted across the first CMC joint during normal daily activities are staggering. Due to the lever arm mechanics of the thumb, a simple pinch force of 1 kilogram at the thumb tip translates to approximately 12 to 13 kilograms of compressive force across the articular surface of the trapezium. Over decades of use, particularly in individuals with subtle ligamentous laxity or unfavorable joint morphology, this exponential force amplification leads to the predictable degradation of the articular cartilage. As the AOL attenuates, the metacarpal base subluxates dorsally, altering the contact mechanics and accelerating the arthritic cascade. Understanding these precise biomechanical principles is non-negotiable for the orthopedic surgeon attempting to reconstruct the joint or salvage wrist function.
Exhaustive Indications and Contraindications
The decision-making algorithm for surgical intervention in wrist pathology requires a nuanced evaluation of patient demographics, functional demands, chronicity of symptoms, and radiographic findings. For acute pisiform fractures, the initial approach is almost universally non-operative. A short arm splint or cast, applied with the wrist in approximately 30 degrees of flexion and slight ulnar deviation, is indicated to relax the deforming forces of the FCU tendon. This conservative management is maintained for 4 to 6 weeks. However, surgical intervention is strictly indicated in cases of chronic non-union, intractable pain persisting beyond 3 to 6 months despite appropriate immobilization, or in acute fractures presenting with concomitant severe ulnar neuropathy secondary to hematoma or displaced fracture fragments. The preferred and most reliable surgical procedure is excision of the pisiform.
Contraindications for pisiform excision are relatively few but must be respected. Absolute contraindications include active local soft tissue infection or osteomyelitis. Relative contraindications include the presence of advanced, untreated Complex Regional Pain Syndrome (CRPS) of the upper extremity, which can be catastrophically exacerbated by surgical trauma. Additionally, in the extremely rare scenario where the pisiform fracture is associated with massive volar carpal instability or a highly complex perilunate fracture-dislocation pattern, isolated excision of the pisiform without addressing the global carpal architecture is contraindicated and will lead to profound midcarpal collapse.
Comparative Indications and Contraindications
| Pathology / Procedure | Primary Surgical Indications | Absolute Contraindications | Relative Contraindications |
|---|---|---|---|
| Pisiform Excision | Chronic painful non-union; Acute fracture with ulnar motor neuropathy; Intractable pisotriquetral arthritis. | Active local infection; Untreated CRPS; Isolated excision in global volar carpal instability. | High-demand laborers requiring absolute maximal FCU strength (controversial). |
| 1st CMC Arthroplasty (Trapeziectomy ± LRTI) | Eaton-Littler Stage III/IV arthritis; Failure of 6 months conservative Rx; Severe rest pain and functional pinch deficit. | Active infection; Medically unfit for anesthesia; Paralyzed thumb lacking motor control. | Concomitant STT arthritis (requires modified approach); Young, heavy manual laborers (consider fusion). |
| 1st CMC Arthrodesis | Young, high-demand manual laborers; Post-traumatic arthritis in patients < 50 years old. | Eaton-Littler Stage IV (pan-trapezial arthritis); Elderly, low-demand patients. | Non-compliant patients unable to tolerate prolonged cast immobilization. |
For first CMC joint osteoarthritis, indications for surgery are dictated by the Eaton-Littler radiographic staging system combined with the patient's clinical symptomology. Early stages (I and II) are managed with NSAIDs, rigid thumb spica splinting, and intra-articular corticosteroid or hyaluronic acid injections. Surgical intervention—most commonly trapeziectomy with or without Ligament Reconstruction and Tendon Interposition (LRTI)—is indicated for Stage III (advanced joint space narrowing, subchondral sclerosis, osteophytes) and Stage IV (pan-trapezial involvement including the scaphotrapezial-trapezoid joint) disease when conservative measures have failed. Contraindications for standard LRTI include isolated STT arthritis without CMC involvement, or a severely paralyzed hand where the thumb lacks the dynamic musculature required to stabilize a reconstructed joint.
Pre-Operative Planning, Templating, and Patient Positioning
Thorough pre-operative planning begins with a meticulous clinical examination. In the case of suspected pisiform pathology, the surgeon must localize tenderness precisely over the volar-ulnar aspect of the wrist. Provocative testing includes the pisotriquetral shear test, where the examiner translates the pisiform radioulnarly against the triquetrum while the wrist is held in extension. Pain with resisted wrist flexion and ulnar deviation further implicates the FCU-pisiform complex. A comprehensive neurological examination of the ulnar nerve, testing both two-point discrimination in the small finger and the motor strength of the intrinsic muscles (e.g., first dorsal interosseous, abductor digiti minimi), is absolutely mandatory to document baseline function prior to any surgical intervention near Guyon's canal.
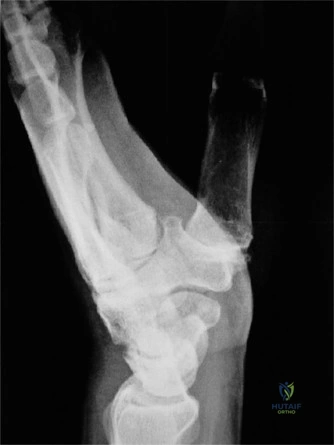
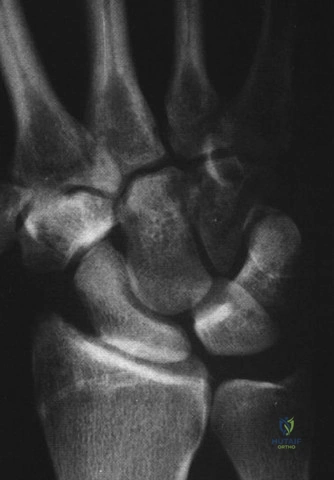
Radiographic evaluation requires specific, non-standard views. A standard PA and lateral of the wrist will often obscure the pisiform due to bony overlap. Therefore, a 30-degree supinated lateral view or a carpal tunnel view is essential to profile the pisiform and evaluate the pisotriquetral joint space. In cases of delayed union or subtle comminution, a fine-cut non-contrast Computed Tomography (CT) scan provides invaluable three-dimensional mapping. For the elderly patient presenting with progressive, non-traumatic base of thumb pain, standard radiographs must include a Robert's view (a true AP of the first CMC joint) and stress views to evaluate the degree of radial subluxation. The image above clearly demonstrates advanced 1st CMC arthritis, characterized by complete loss of joint space, subchondral sclerosis, and osteophyte formation, confirming the diagnosis.
Once the operative plan is established, patient positioning and anesthesia are standardized to ensure optimal surgical conditions. The patient is placed supine on the operating table with the operative extremity extended onto a radiolucent hand table. Regional anesthesia, typically an ultrasound-guided supraclavicular or axillary brachial plexus block, is highly preferred over general anesthesia, as it provides excellent intra-operative muscle relaxation and superior post-operative analgesia. A well-padded pneumatic tourniquet is applied to the proximal arm. Prior to inflation, the limb is strictly exsanguinated using an Esmarch bandage to provide a bloodless surgical field, which is critical for the micro-dissection required around the delicate neurovascular structures of the wrist.
Step-by-Step Surgical Approach and Fixation Technique
Pisiform Excision Technique
The surgical excision of the pisiform demands meticulous soft tissue handling and an intimate knowledge of ulnar-sided neurovascular anatomy. An expansile, zig-zag or lazy-S incision is made over the volar-ulnar aspect of the wrist, crossing the distal wrist flexion crease obliquely to prevent post-operative scar contracture. The incision is centered directly over the palpable mass of the pisiform. Subcutaneous tissues are bluntly dissected to protect the palmar cutaneous branches of the ulnar nerve. The antebrachial fascia is incised, and the FCU tendon is identified. The ulnar neurovascular bundle, located immediately radial to the FCU and pisiform, is identified, isolated with vessel loops, and gently retracted radially.
A longitudinal incision is made directly through the substance of the FCU tendon over the volar prominence of the pisiform. Using a #15 blade and a small periosteal elevator, a subperiosteal (or more accurately, sub-tendinous) dissection is performed to shell the pisiform out of its tendinous envelope. Sharp dissection is required distally to release the stout pisohamate and pisometacarpal ligaments. Extreme caution must be exercised during the deep and radial dissection to avoid penetrating the pisotriquetral joint capsule excessively or injuring the deep motor branch of the ulnar nerve as it dives around the hook of the hamate. Once the bone is excised en bloc, the residual defect in the FCU tendon is repaired using heavy, non-absorbable figure-of-eight sutures (e.g., 2-0 Ethibond or FiberWire) to restore the tendinous continuity and maintain the mechanical tension of the FCU.
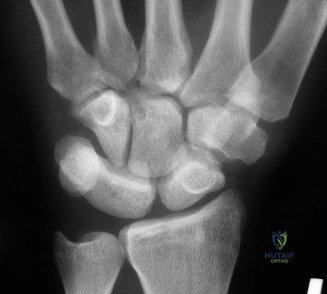
First CMC Arthroplasty (Trapeziectomy with LRTI)
For the surgical management of advanced first CMC arthritis, the trapeziectomy with Ligament Reconstruction and Tendon Interposition (LRTI) remains a gold-standard benchmark. A dorsal-radial (Wagner) incision is utilized, curving along the border of the first metacarpal and extending proximally over the anatomic snuffbox. Meticulous blunt dissection is utilized to identify and protect the superficial sensory branches of the radial nerve, which are highly susceptible to traction neuritis. The abductor pollicis brevis (APB) and opponens pollicis are elevated off the first metacarpal and joint capsule. A longitudinal capsulotomy is performed, exposing the degenerative trapeziometacarpal joint.
The trapezium is excised either en bloc or piecemeal using a combination of osteotomes, rongeurs, and a high-speed burr. The surgeon must remain vigilant during the deep volar resection to avoid injuring the flexor carpi radialis (FCR) tendon, which runs in a distinct groove on the volar aspect of the trapezium. Once the trapezium is entirely removed, the distal half of the FCR tendon is harvested via step-cut incisions proximally in the forearm. A drill hole is created in the dorsal-radial base of the first metacarpal. The harvested FCR tendon slip is passed through the metacarpal base, tensioned to reduce the dorsal subluxation, and sutured back onto itself or secured with a tenodesis screw. The remaining tendon is fashioned into an "anchovy" and interposed into the trapezial void to act as a biological spacer, preventing proximal subsidence of the metacarpal. The capsule is meticulously repaired, and the thumb is pinned in a position of palmar abduction and opposition using a smooth Kirschner wire.
Complications, Incidence Rates, and Salvage Management
Despite meticulous surgical technique, procedures addressing the extremes of the wrist are fraught with potential complications. Following pisiform excision, the most frequent complication is transient neurapraxia of the ulnar nerve, occurring in up to 5% to 10% of cases. This is typically secondary to intra-operative traction or post-operative hematoma within Guyon's canal. Most cases resolve spontaneously within 6 to 12 weeks. A more insidious complication is the development of a painful neuroma of the palmar cutaneous branch of the ulnar nerve, which can lead to severe, debilitating pain and hyperalgesia over the hypothenar eminence. Biomechanically, patients may experience a mild, often subclinical, loss of terminal wrist flexion power due to the alteration of the FCU moment arm, though this rarely affects functional outcomes.
Complications following first CMC arthroplasty are well-documented in the literature. Proximal subsidence of the first metacarpal into the trapezial void is radiographically ubiquitous, occurring in up to 30% to 40% of patients over time. However, it is paramount to understand that radiographic subsidence correlates poorly with clinical symptoms; many patients with severe subsidence remain completely asymptomatic with excellent pinch strength. A more concerning complication is injury to the superficial radial sensory nerve (Wartenberg's syndrome), which can cause profound dysesthesia. Complex Regional Pain Syndrome (CRPS) is a catastrophic complication that can occur in 1% to 3% of cases, requiring aggressive multidisciplinary pain management and aggressive hand therapy.
Complications, Incidence, and Salvage Strategies
| Complication | Estimated Incidence | Primary Prevention Strategy | Salvage / Management Strategy |
|---|---|---|---|
| Ulnar Neurapraxia (Pisiform) | 5% - 10% | Direct visualization; Avoid excessive radial retraction. | Observation; Gabapentin; Neurolysis if no recovery > 3 months. |
| Sural/Radial Nerve Neuroma | 2% - 5% | Blunt subcutaneous dissection; Loupe magnification. | Surgical excision of neuroma and burying proximal stump into muscle. |
| Metacarpal Subsidence (CMC) | 30% (Radiographic) | Robust LRTI construct; K-wire pinning for 4 weeks. | Revision suspensionplasty (e.g., Mini TightRope) or CMC Arthrodesis. |
| CRPS Type I | 1% - 3% | Adequate post-op analgesia; Early digit mobilization. | Aggressive OT; Stellate ganglion blocks; Neuromodulating agents. |
Salvage management requires a highly individualized approach. For a failed pisiform excision presenting with persistent pain, the surgeon must obtain advanced imaging (MRI or CT) to rule out retained osseous fragments, pisotriquetral joint loose bodies, or an organized neuroma. Revision surgery to excise neuromas and bury the nerve stump deep into the pronator quadratus may be necessary. For a failed first CMC arthroplasty with symptomatic subsidence and impingement against the scaphoid, salvage options include revision suspensionplasty using synthetic suture-button constructs, interposition of costochondral allograft, or conversion to a formal first metacarpal-to-scaphoid arthrodesis to provide a stable, albeit stiff, pillar for pinch.
Phased Post-Operative Rehabilitation Protocols
The ultimate success of any wrist surgery is inextricably linked to the quality and adherence to a phased post-operative rehabilitation protocol. The concept of "Mastering Degrees" is realized in the therapy clinic. The initial phase (Weeks 0-2) is the immobilization phase. Following pisiform excision, the wrist is immobilized in a short arm bulky dressing or splint in 20 degrees of flexion to minimize tension on the FCU repair. Following CMC arthroplasty, the thumb is immobilized in a rigid thumb spica cast. During this phase, the absolute priority is edema control and the immediate initiation of active range of motion (AROM) of the uninvolved digits (fingers and elbow) to prevent tendon adhesions and mitigate the risk of CRPS.
The early protective motion phase (Weeks 2-6) marks the transition to custom thermoplastic orthoses. For the pisiform patient, the splint is removed for supervised therapy sessions focusing on gentle, gravity-eliminated active wrist flexion and extension. Passive stretching and resisted FCU firing are strictly prohibited to protect the tendinous repair. For the CMC patient, if a K-wire was used, it is typically removed at 4 weeks. A custom forearm-based thumb spica splint is fabricated. Gentle AROM of the thumb CMC and MCP joints is initiated, focusing on palmar abduction and opposition. Key pinch and forceful grip are entirely avoided to prevent early subsidence of the metacarpal.
The intermediate phase (Weeks 6-10) focuses on restoring the complex kinematic arcs of the wrist. Weaning from the splint begins. For both patient populations, therapists introduce the "dart-thrower's motion" (coupled radial extension and ulnar flexion). This specific arc of motion is biomechanically advantageous as it occurs primarily at the midcarpal joint, minimizing stress on the radiocarpal and pisotriquetral articulations while maximizing functional return for activities of daily living. Gentle isometric strengthening is introduced.
The advanced strengthening and return-to-play phase (Weeks 10-16+) is tailored to the patient's specific demands. For the athlete recovering from a pisiform excision, plyometric exercises, eccentric FCU strengthening, and sport-specific drills (e.g., racket swings, football blocking techniques) are aggressively pursued. For the elderly patient recovering from CMC arthroplasty, work-hardening focuses on sustained grip, forceful key pinch, and unrestricted forearm pronation/supination to restore complete functional independence. Maximum medical improvement is typically achieved between 6 and 12 months post-operatively.
Summary of Landmark Literature and Clinical Guidelines
The evolution of surgical management for ulnar and radial-sided wrist pathology is deeply rooted in landmark orthopedic literature. Regarding pisiform fractures, the seminal work by Rayan and Stringer established the foundational classification system and highlighted that while conservative management is appropriate for non-displaced fractures, excision is the definitive treatment for chronic non-unions. Long-term biomechanical studies have consistently demonstrated that isolated excision of the pisiform does not significantly alter global wrist kinematics or significantly diminish grip strength, provided the FCU tendon is meticulously repaired and tensioned. This evidence solidifies pisiform excision as a safe and highly effective procedure that does not result in measurable functional deficits.
In the realm of first CMC joint arthritis, the Eaton and Littler classification, published in 1973, remains the cornerstone of radiographic evaluation and surgical decision-making. Their staging system accurately correlates the progressive loss of the anterior oblique ligament with articular degradation. However, the surgical treatment of CMC arthritis has been the subject of intense academic debate. The landmark Cochrane Review by Wajon et al. analyzed numerous randomized controlled trials comparing simple trapeziectomy, trapeziectomy with tendon interposition, and trapeziectomy with LRTI.
Surprisingly, the literature demonstrates that there is no statistically significant long-term difference in pain relief, grip strength, or functional outcomes between simple trapeziectomy and the more complex LRTI procedures, despite the higher incidence of radiographic subsidence in the simple trapeziectomy group. Furthermore, LRTI procedures carry a higher risk of adverse events, including tendon harvest site morbidity and nerve injury. Consequently, modern clinical guidelines advocate for a patient-specific approach. While
