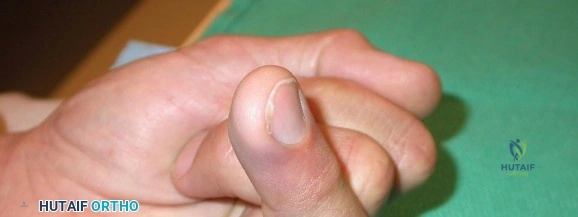
Orthopedic Hand Cases: A Patient's Journey, Is a Year Old a Factor?
Key Takeaway
For anyone wondering about Orthopedic Hand Cases: A Patient's Journey, Is a Year Old a Factor?, For multiple displaced metacarpal fractures, open reduction and internal fixation (ORIF) is the most appropriate management, particularly in high-energy trauma. When the patient is a 28-year-old male, ORIF restores anatomy, including longitudinal and transverse arches, decompresses interosseous muscles, and stabilizes the hand. This enables earlier rehabilitation, significantly optimizing the patient's functional outcome.
Detailed Patient Presentation and Mechanism of Injury
The case before us involves a 28-year-old, right-hand-dominant male who presented to our orthopedic trauma clinic on the fourth day following a high-energy trauma sustained while snowboarding. The patient, a novice to the sport, reported catching "big air" off a terrain park jump, losing control in mid-air, and landing catastrophically. In an attempt to break his fall, he landed awkwardly on his non-dominant left hand, with the wrist in extension and the digits likely caught in a hyperflexed or torsionally loaded position against the compacted snow and ice. He experienced an immediate, profound onset of pain, accompanied by rapid swelling and an obvious clinical deformity of the dorsal hand.

The mechanism of injury here is paramount to understanding the fracture personality and the soft tissue envelope's status. High-energy axial loading combined with torsional forces on a closed or partially closed hand bypasses the typical energy-absorbing mechanisms of the wrist (which usually result in distal radius or scaphoid fractures). Instead, the force is propagated directly through the metacarpal shafts. When multiple contiguous metacarpals fracture simultaneously, the intrinsic stability of the hand is entirely compromised. The adjacent intact metacarpals, which typically act as internal splints to prevent severe shortening and angulation in isolated fractures, are no longer available to provide structural support.

Furthermore, the delayed presentation of four days introduces a significant clinical variable. The patient had been evaluated slope-side, where initial radiographs confirmed multiple metacarpal fractures. He was placed in a non-custom, temporary short-arm splint and advised to seek definitive orthopedic care. Over the intervening 96 hours, the inflammatory cascade has peaked. Hematoma formation, fracture site mobility, and unmitigated edema have led to profound swelling within the tight fascial compartments of the hand. This temporal factor—the "year old" or chronic/delayed aspect of presentation—drastically alters our surgical timing, soft tissue management, and approach to anatomic restoration.

The initial slope-side splinting, while well-intentioned, often fails to place the hand in a true intrinsic-plus position (metacarpophalangeal joints flexed to 70-90 degrees, interphalangeal joints fully extended). Consequently, the collateral ligaments of the metacarpophalangeal (MCP) joints may have already begun to contract in a shortened position, and the interosseous muscles are subjected to sustained hemorrhage and edema. This presentation mandates a high index of suspicion for impending or established compartment syndrome of the hand, specifically within the interosseous compartments, and sets the stage for a complex reconstructive effort rather than a simple fracture fixation.
Comprehensive Clinical Examination Findings
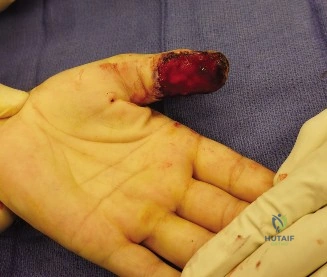
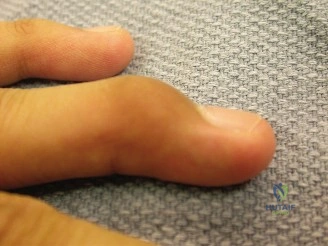
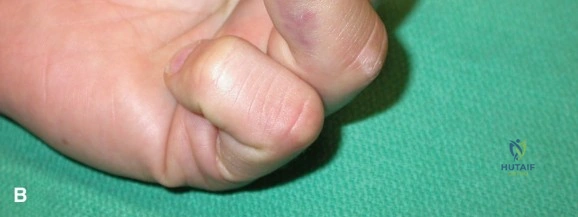
Upon removal of the temporary splint in the clinic, the physical examination immediately revealed a grossly swollen, ecchymotic left hand. The dorsal soft tissue envelope was tense, with loss of the normal dorsal skin wrinkles and obliteration of the venous architecture. The normal dorsal longitudinal and transverse arches of the hand were clinically absent, replaced by a flattened, widened, and shortened metacarpal profile. A prominent dorsal mass was palpable, representing the apex-dorsal angulation of the fractured metacarpal shafts, driven by the deforming forces of the intrinsic muscles (interossei and lumbricals) and the extrinsic flexor tendons.
Careful assessment of the digital cascade was performed. In a normal resting posture, the digits should exhibit a progressive increase in flexion from the index to the small finger, pointing toward the scaphoid tubercle. In this patient, the cascade was entirely disrupted. Passive extension of the wrist did not produce the expected tenodesis effect of digital flexion, indicating profound mechanical disruption and guarding. Furthermore, when the patient was asked to actively flex his fingers (which was severely limited by pain and edema), frank scissoring of the middle and ring fingers was observed. This rotational malalignment is a hallmark of displaced metacarpal fractures and is clinically intolerable, as it severely impairs grip strength and function.

Palpation elicited exquisite point tenderness over the shafts of the second, third, and fourth metacarpals. Crepitus was evident, though manipulation was kept to an absolute minimum to prevent further soft tissue trauma. Crucially, the intrinsic compartments were assessed for tightness. The interosseous muscles occupy the spaces between the metacarpals; with multiple fractures, the bleeding into these confined spaces can dramatically increase intracompartmental pressures. Passive stretch of the interossei (achieved by extending the MCP joints while flexing the PIP joints) elicited severe pain out of proportion to the fractures themselves, highly suggestive of elevated compartment pressures necessitating eventual surgical decompression.

A rigorous neurovascular examination was documented. Despite the massive swelling, capillary refill remained brisk (under 2 seconds) in all digits, and the radial and ulnar pulses were palpable. Two-point discrimination was intact and symmetric across all dermatomes of the median, ulnar, and radial nerves, measuring approximately 4-5 mm at the volar fingertips. However, the patient reported subjective paresthesias over the dorsal sensory branch of the ulnar nerve, likely secondary to traction or compression from the massive dorsal hematoma. This baseline neurovascular status is critical to document prior to any surgical intervention, especially in the setting of extreme edema.
Advanced Imaging and Diagnostics (X-ray, CT, MRI, Templating)
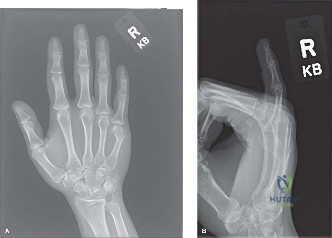
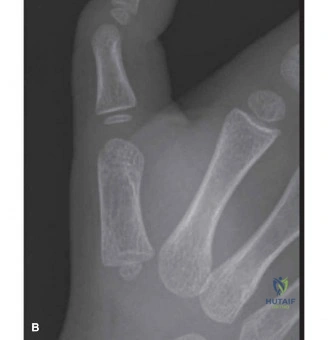
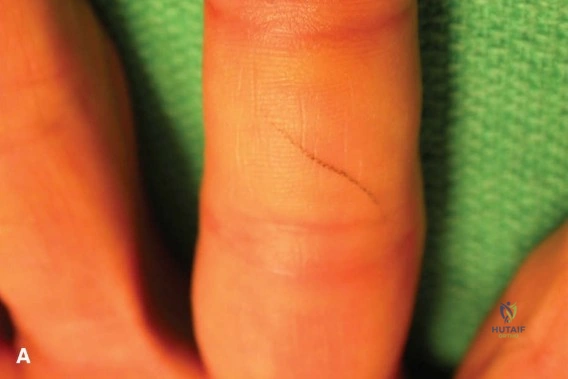
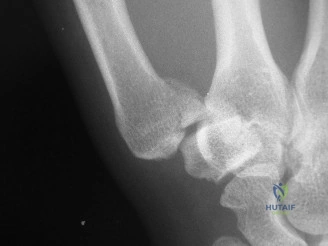
Standard orthogonal radiographs of the left hand—comprising posteroanterior (PA), lateral, and oblique views—were obtained to definitively characterize the skeletal injury. The radiographs confirmed the presence of multiple, displaced metacarpal shaft fractures involving the index, long, and ring fingers (metacarpals II, III, and IV).
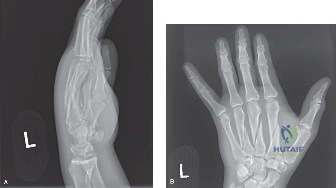
The PA view demonstrated significant shortening of the affected rays. The second metacarpal exhibited a long, spiral fracture pattern, while the third and fourth metacarpals demonstrated transverse to short-oblique fracture patterns with comminution at the volar cortices. The loss of longitudinal length was readily apparent when compared to the intact fifth metacarpal. This shortening directly alters the length-tension relationship of the intrinsic musculature, which, if left uncorrected, leads to profound weakness and intrinsic minus posturing.

The lateral and oblique views were critical for assessing the degree of apex-dorsal angulation. The third and fourth metacarpals demonstrated approximately 40 degrees of apex-dorsal angulation. While the ring and small fingers can tolerate up to 30-40 degrees of angulation due to the compensatory mobility of the 4th and 5th carpometacarpal (CMC) joints, the index and long fingers (2nd and 3rd metacarpals) form the fixed, rigid central pillar of the hand. Any angulation greater than 10-15 degrees in these central rays is poorly tolerated, leading to a prominent palmar metacarpal head that causes pain with gripping and a pseudo-clawing effect due to relative extensor tendon lengthening.
While standard radiographs are often sufficient for diaphyseal metacarpal fractures, the high-energy nature of this injury and the degree of comminution prompted the acquisition of a non-contrast Computed Tomography (CT) scan of the hand. The CT scan, utilizing 1mm fine cuts with 3D reconstructions, allowed for meticulous pre-operative templating. It confirmed that the CMC joints were congruent and free of intra-articular extension. Furthermore, the 3D reconstructions provided a spatial roadmap of the rotational deformity, aiding in the selection of appropriate implants. Pre-operative templating determined the need for a combination of 1.5mm/2.0mm lag screws for the spiral fracture and low-profile titanium locking plates for the transverse/comminuted fractures.
Exhaustive Differential Diagnosis
When evaluating a patient with a grossly swollen hand and severe pain following a high-energy axial load, the differential diagnosis must encompass a spectrum of osseous, ligamentous, and soft tissue pathologies. While the radiographs in this case readily identified the metacarpal fractures, a systematic approach ensures no concomitant injuries are missed.
| Differential Diagnosis | Key Clinical Findings | Radiographic Hallmarks | Management Implications |
|---|---|---|---|
| Multiple Metacarpal Shaft Fractures | Severe dorsal swelling, loss of knuckle prominence, scissoring of digits, point tenderness over shafts. | Disruption of diaphyseal continuity, apex-dorsal angulation, shortening, rotational malalignment. | ORIF mandated for contiguous fractures to restore arches, length, and allow early motion. |
| Carpometacarpal (CMC) Fracture-Dislocations | Pain localized proximally at the CMC joints, apparent shortening of the hand, swelling at the wrist crease. | Loss of parallelism at CMC joints on PA view, dorsal/volar displacement on true lateral view. | High risk of missed diagnosis. Requires closed reduction + CRPP or open reduction if unstable. |
| Phalanx Fractures (Proximal/Middle) | Deformity localized to the digit itself, rotational malalignment easily visible at the nail beds. | Fractures distal to the MCP joint. Apex-volar angulation common due to intrinsic/extrinsic pulls. | Non-operative if stable/minimally displaced; operative if rotated, shortened, or intra-articular. |
| Compartment Syndrome of the Hand | Pain out of proportion, tense swelling, severe pain with passive stretch of intrinsic muscles (intrinsic minus position). | Normal radiographs (if isolated), or presence of high-energy crush/fractures. | Surgical emergency. Requires immediate dorsal and volar fasciotomies to prevent ischemic contracture. |
Multiple Metacarpal Shaft Fractures
As confirmed in our patient, contiguous metacarpal fractures represent a severe disruption of the hand's structural integrity. The hand relies on a delicate balance between the fixed central unit (2nd and 3rd metacarpals) and the mobile border units (1st, 4th, and 5th metacarpals). When multiple adjacent metacarpals are fractured, the mutual soft-tissue support (the deep transverse metacarpal ligaments and interosseous fascia) is lost. This results in independent displacement, severe shortening, and rotation. The primary differentiator here is the contiguous nature; an isolated 3rd metacarpal fracture might be managed conservatively due to the splinting effect of the 2nd and 4th rays, but multiple fractures demand surgical stabilization.
Carpometacarpal (CMC) Fracture-Dislocations
Often missed in the emergency department, CMC fracture-dislocations occur from similar high-energy axial loads. The force is transmitted proximally, disrupting the strong dorsal carpometacarpal ligaments. Clinically, the swelling is more proximal than diaphyseal fractures. Radiographically, the key is evaluating the "M" lines of the CMC joints on the PA view and ensuring no dorsal step-off on the lateral view. In our patient, the CT scan definitively ruled this out, localizing the pathology entirely to the diaphysis.
Compartment Syndrome of the Hand
While technically a complication rather than a primary osseous diagnosis, compartment syndrome must be considered a primary differential for the source of the patient's severe pain. The hand contains 10 fascial compartments: 4 dorsal interosseous, 3 volar interosseous, the adductor pollicis, the thenar, and the hypothenar compartments. The massive swelling and pain with passive intrinsic stretch in our patient strongly suggested impending compartment syndrome. This dictates not only the need for surgery but the specific surgical approach—utilizing longitudinal dorsal incisions that allow for thorough fascial release and decompression of the interosseous muscles.
Complex Surgical Decision Making and Classifications
The decision to proceed with operative intervention in this case is absolute. While a single, minimally displaced metacarpal fracture might be managed with a short-arm cast or splint in the intrinsic-plus position (MCPs flexed, PIPs/DIPs extended), this non-operative modality is entirely inappropriate for multiple contiguous displaced fractures. The literature unequivocally supports Open Reduction and Internal Fixation (ORIF) for this injury pattern.

The rationale for open treatment is multifaceted and addresses both the skeletal and soft tissue envelopes. First, ORIF allows for the precise restoration of anatomy. The metacarpals possess a natural longitudinal arch (concave on the volar surface) and form a transverse arch at the level of the metacarpal heads. Restoring these arches is critical for grip strength and the mechanical advantage of the flexor tendons. Second, open treatment facilitates the direct decompression of the interosseous muscles. The surgical approach inherently opens the fascial compartments, evacuating the fracture hematoma and mitigating the risk of intrinsic contracture.
Third, ORIF restores the longitudinal length of the metacarpals. The intrinsic muscles originate on the metacarpal shafts; shortening of the bone leads to a slackening of these muscles, altering their length-tension relationship and resulting in profound weakness. Finally, rigid internal fixation provides skeletal stability that permits immediate, early active rehabilitation. In a hand subjected to such trauma, prolonged immobilization in a cast would guarantee severe tendon adhesions, joint stiffness, and a devastating functional outcome.

The classification of these fractures dictates the specific implant choice. The second metacarpal exhibited a long spiral fracture. Biomechanically, if the length of the fracture line is greater than twice the diameter of the bone at that level, the fracture is amenable to fixation with multiple interfragmentary lag screws alone. Lag screws provide absolute stability through interfragmentary compression, promoting primary bone healing without callus formation. Conversely, the third and fourth metacarpals demonstrated transverse and short-oblique patterns with volar comminution. These cannot be managed with lag screws alone; they require dorsal plating to act as a tension band against the displacing forces of the flexor tendons, neutralizing bending and torsional loads.
Step-by-Step Surgical Technique and Intervention
The patient was taken to the operating room and placed supine on the operating table with the left arm extended on a radiolucent hand table. General anesthesia was induced, supplemented by an ultrasound-guided supraclavicular brachial plexus block for optimal intra-operative muscle relaxation and post-operative pain control. A well-padded pneumatic tourniquet was applied to the proximal arm and inflated to 250 mmHg after exsanguination with an Esmarch bandage.

Surgical access was achieved via two longitudinal dorsal incisions. The first incision was placed in the second intermetacarpal space to access the second and third metacarpals, and the second incision was placed in the fourth intermetacarpal space to access the fourth metacarpal. This dual-incision technique is preferred over a single large transverse or serpentine incision, as it preserves the dorsal venous lymphatic drainage, minimizes skin flap necrosis, and provides direct access to the dorsal interosseous fascial compartments for decompression.

Careful blunt dissection was utilized to identify and protect the dorsal sensory branches of the radial and ulnar nerves. The extensor tendons (extensor digitorum communis, extensor indicis proprius) were identified, mobilized, and retracted. The dorsal interosseous fascia was incised longitudinally, immediately releasing a large volume of dark, organized hematoma and decompressing the engorged muscle bellies. The periosteum over the fracture sites was incised longitudinally and elevated minimally—only 1-2 mm from the fracture edges—to preserve the crucial periosteal blood supply while allowing direct visualization of the fracture reduction.

Attention was first directed to the second metacarpal. The long spiral fracture was anatomically reduced using pointed reduction forceps. Once rotational and longitudinal alignment was confirmed clinically and fluoroscopically, three 1.5mm titanium lag screws were placed perpendicular to the fracture plane. The sequence of over-drilling the near cortex (glide hole), drilling the far cortex (thread hole), countersinking, measuring, and screw insertion was meticulously followed to achieve robust interfragmentary compression.
Next, the third and fourth metacarpals were addressed. Due to the transverse/comminuted nature of these fractures, low-profile 2.0mm titanium locking plates were selected. The fractures were reduced and held with K-wires temporarily. The plates were contoured to match the normal dorsal concavity of the metacarpals. Non-locking screws were used first to pull the bone to the plate and achieve compression where possible, followed by locking screws in the comminuted segments to function as an internal fixator. Throughout the procedure, the tenodesis effect was repeatedly checked, and the digits were flexed into the palm to ensure no rotational malalignment (scissoring) was present. After copious irrigation and confirmation of hemostasis upon tourniquet deflation, the wounds were closed loosely with non-absorbable sutures to accommodate anticipated post-operative swelling.
Strict Post-Operative Protocol and Rehabilitation Stages
The success of complex hand trauma surgery is intrinsically linked to the rigor and execution of the post-operative rehabilitation protocol. The primary goal of rigid internal fixation is not merely bone healing, but the facilitation of early active motion to prevent the devastating complications of tendon adhesions and joint contracture. Immediately post-operatively, the patient was placed in a bulky, non-compressive soft dressing reinforced with a volar plaster splint. The hand was immobilized in the intrinsic-plus, or "safe," position: wrist extended 30 degrees, MCP joints flexed 70-90 degrees, and PIP/DIP joints in full extension. This position maintains the collateral ligaments of the MCP joints at their maximal length, preventing extension contractures.
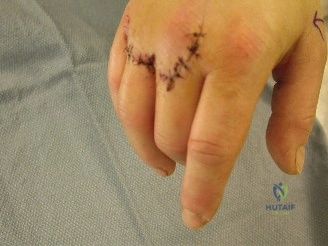
At post-operative day 3 to 5, the bulky surgical dressing was removed by the certified hand therapist (CHT). Wound care was initiated, and a custom thermoplastic splint was fabricated. Crucially, because rigid internal fixation was achieved (lag screws and locking plates), the patient was immediately cleared for Early Active Motion (EAM) protocols. The patient was instructed to perform active composite flexion and extension, as well as isolated intrinsic and extrinsic tendon gliding exercises, for 10 minutes every hour while awake. The splint was worn at all times between exercise sessions and at night.
Weeks 2 through 6 focus heavily on edema control and maximizing tendon excursion. Suture removal occurred at day 14. Edema was managed with compressive wraps (Coban), retrograde massage, and strict elevation. The hand therapist guided the patient through differential tendon gliding (hook fist, straight fist, composite fist) to ensure the extensor tendons did not adhere to the underlying dorsal plates or fracture callus. Passive range of motion and dynamic splinting were strictly avoided during this phase to prevent hardware failure or loss of reduction.

From week 6 to 12, following radiographic confirmation of bridging callus and clinical stability, the protective splint was progressively weaned. The rehabilitation focus shifted toward strengthening, grip endurance, and work-hardening. Putty exercises, grip dynamometer training, and simulated snowboarding/weight-bearing activities were integrated. By 12 weeks, the patient is expected to achieve near-normal grip strength and full, painless range of motion, allowing a safe return to high-impact activities.
High-Yield Clinical Pearls and Pitfalls
In the management of multiple metacarpal fractures, several high-yield pearls and dangerous pitfalls must be recognized by the operating surgeon. The most unforgiving pitfall is the failure to recognize and correct rotational malalignment. Unlike angulation or shortening, the hand has zero tolerance for rotational deformity. Even 5 degrees of metacarpal malrotation can result in 1.5 cm of digital overlap at the level of the distal phalanx. Surgeons must rely on clinical evaluation of the digital cascade during surgery, flexing the fingers passively into the palm to ensure they all point synchronously toward the scaphoid tubercle.

Another critical pearl involves the management of the soft tissue envelope. The dorsal skin of the hand is thin and highly mobile, while the extensor tendons lie directly beneath it, separated only by a thin paratenon. Excessive periosteal stripping or the use of overly thick, non-contoured plates will inevitably lead to hardware prominence, extensor tendon irritation, and potential tendon rupture. Utilizing low-profile mini-fragment sets, burying screw heads, and meticulously repairing the periosteum or paratenon over the hardware (when possible) are vital steps to minimize these complications.

Finally, surgeons must remain hyper-vigilant regarding compartment syndrome, particularly in delayed presentations or high-energy crush injuries. The threshold for performing dorsal and volar fasciotomies should be exceedingly low. If the interosseous muscles appear pale, non-contractile, or bulge excessively upon fascial release, thorough decompression is mandatory. Failing to decompress the hand compartments will lead to ischemic necrosis of the intrinsic musculature, resulting in a fibrotic, contracted, and functionally useless "intrinsic minus" hand, a catastrophic outcome that overshadows any successful osseous fixation.
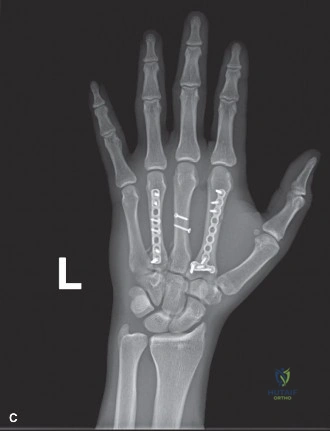
Clinical & Radiographic Imaging Archive