Skier's Thumb Case Study: Diagnosing Ulnar Collateral Ligament Rupture & Stener Lesion
Key Takeaway
Diagnosis of Skier's Thumb (UCL rupture) involves a detailed clinical examination, including valgus stress testing that reveals significant instability. A palpable firm mass near the MCP joint strongly suggests a Stener lesion. MRI imaging is crucial for confirming a complete UCL tear and identifying the Stener lesion's displacement, guiding appropriate surgical intervention.
Patient Presentation and History
Mechanism of Injury and Biomechanics
A 35-year-old right-hand dominant male presented to the orthopedic trauma bay following a high-velocity skiing accident. The specific mechanism of injury involved a fall while actively gripping a ski pole. As the patient fell, the ski pole planted into the snow, and the strap, which was wrapped around his wrist and thumb, acted as a fulcrum. This applied a violent, forced abduction and hyperextension moment to the right thumb metacarpophalangeal joint. The patient reported an immediate, distinct tactile and auditory pop, followed by an acute sensation of joint instability and profound weakness in his pinch grip.
The biomechanics of this injury pattern are classic for acute ulnar collateral ligament ruptures, historically differentiated from the chronic attenuation seen in Scottish gamekeepers. The forced radial deviation of the proximal phalanx relative to the metacarpal head places catastrophic tensile strain on the ulnar collateral ligament complex. When the metacarpophalangeal joint is in extension during the traumatic event, the accessory ulnar collateral ligament and volar plate bear the initial stress. However, as the joint is forced into flexion and abduction, the proper ulnar collateral ligament becomes the primary restraint and subsequently fails.
Demographic and Occupational Considerations
Prior medical history was entirely unremarkable, with no known drug allergies, previous surgical interventions, or significant medical comorbidities. The patient denied any prior trauma, fractures, or ligamentous injuries to the affected right hand or wrist. He is a highly active individual, participating in alpine skiing, rock climbing, and recreational tennis. Social history includes occasional ethanol consumption and strictly no tobacco or illicit substance use.
Crucially from a surgical decision-making standpoint, the patient is employed as a senior software engineer. His occupation demands high-level fine motor dexterity, rapid repetitive keyboard strikes, and sustained pinch grip for mouse utilization. The right thumb serves as the primary stabilizing digit for the spacebar and requires precise opposition for daily occupational tasks. Consequently, restoring absolute anatomic stability and preventing chronic metacarpophalangeal joint subluxation or early-onset osteoarthritis is paramount for his continued professional trajectory and quality of life.
Upon initial presentation, the patient reported severe, localized pain, rated 8 out of 10 on a visual analog scale. This pain was acutely exacerbated by any active movement, particularly attempts at key pinch or chuck grip. He noted a subjective, profound weakness when attempting to grasp his opposite hand. Rapid, progressive ecchymosis and significant soft tissue edema developed over the ulnar aspect of the thumb metacarpophalangeal joint within two hours of the traumatic event.
Clinical Examination Findings
Inspection and Palpation
Initial inspection of the right hand revealed significant, localized edema and pronounced ecchymosis over the ulnar aspect of the right thumb metacarpophalangeal joint, extending proximally toward the first web space. There was no gross angular deformity, step-off, or rotational malalignment of the digit at rest. The skin envelope was entirely intact, with no open wounds, abrasions, or impending skin necrosis.
Palpation was performed meticulously. Maximal point tenderness was elicited directly over the ulnar collateral ligament complex. The tenderness was most acute at the ligamentous insertion site onto the volar-ulnar base of the proximal phalanx, and to a slightly lesser degree at its origin on the metacarpal head.
During palpation of the ulnar joint line, a distinct, firm, highly tender, pea-sized mass was appreciated proximally and ulnarly to the metacarpophalangeal joint line. This palpable mass is the pathognomonic clinical hallmark of a Stener lesion. It represents the avulsed, retracted distal end of the ulnar collateral ligament that has displaced superficial to the proximal edge of the adductor pollicis aponeurosis. This anatomic interposition physically prevents the torn ligament ends from approximating, rendering non-operative management futile. Additional tenderness was noted along the adductor pollicis muscle belly, likely secondary to the traumatic displacement of the aponeurosis. No tenderness was appreciated over the radial collateral ligament, the volar plate, the carpometacarpal joint, or the anatomic snuffbox.
Range of Motion and Provocative Testing
Active and passive range of motion of the right thumb metacarpophalangeal joint was severely restricted secondary to pain, guarding, and acute hemarthrosis. Flexion was limited to approximately 30 degrees, compared to a normal physiological range of 50 to 70 degrees. Extension was limited to neutral, lacking the normal 10 to 20 degrees of hyperextension seen in the contralateral digit. Any attempt at active or passive abduction elicited severe apprehension and pain.
To accurately assess ligamentous integrity without the confounding factor of muscle guarding, a local intra-articular anesthetic block was administered using 2 milliliters of 1 percent lidocaine without epinephrine. Following appropriate anesthetic effect, valgus stress testing was performed.
Testing was conducted in two distinct positions to isolate the components of the ulnar collateral ligament complex. First, valgus stress was applied with the metacarpophalangeal joint in full extension. In this position, the volar plate and the accessory ulnar collateral ligament are the primary stabilizers. The injured thumb demonstrated approximately 20 degrees of valgus angulation with a soft, ill-defined endpoint, compared to 5 degrees of firm angulation on the contralateral uninjured thumb.
Subsequently, valgus stress was applied with the metacarpophalangeal joint flexed to 30 degrees. This position relaxes the volar plate and isolates the proper ulnar collateral ligament as the primary restraint to valgus stress. In 30 degrees of flexion, the injured thumb revealed gross instability, demonstrating approximately 40 degrees of valgus angulation. The endpoint was distinctly soft, and significant gapping of the ulnar joint line was visually and palpably perceived. The contralateral uninjured thumb demonstrated only 10 degrees of angulation with a firm, abrupt endpoint. The absolute angulation exceeding 35 degrees, combined with a side-to-side difference greater than 15 degrees, provided definitive clinical evidence of a complete, full-thickness rupture of the proper ulnar collateral ligament.
Neurological and Vascular Assessment
A comprehensive neurovascular examination of the right upper extremity was performed. Sensation was grossly intact to light touch and two-point discrimination in the distributions of the median, ulnar, and radial nerves. Specific attention was paid to the dorsal sensory branch of the radial nerve, which courses directly over the operative field; sensation in its distribution over the dorsoradial aspect of the thumb was entirely intact. Motor function of the intrinsic thumb musculature, including the thenar eminence (abductor pollicis brevis, opponens pollicis, flexor pollicis brevis) and the adductor pollicis, was intact, though strength testing was limited by pain.
Vascular assessment revealed brisk capillary refill of less than two seconds in the thumb and all adjacent digits. The radial and ulnar pulses at the wrist were strong, symmetric, and easily palpable. The Allen test demonstrated patent dual arterial supply to the hand. There were no signs of acute compartment syndrome or vascular compromise.
Imaging and Diagnostics
Standard and Specialized Radiography
Initial plain radiographs of the right thumb, including true anteroposterior, lateral, and oblique views, were obtained. The true anteroposterior view, often referred to as the Roberts view (obtained with the thumb in maximum internal rotation and the dorsum of the thumb resting on the cassette), is critical for evaluating the metacarpophalangeal joint space and the base of the proximal phalanx.
The radiographs revealed varying degrees of soft tissue swelling about the ulnar aspect of the metacarpophalangeal joint. Crucially, the imaging demonstrated no evidence of acute fracture, dislocation, or bony avulsion at the ulnar base of the proximal phalanx. The joint spaces were preserved, and there were no signs of pre-existing degenerative joint disease or chondrocalcinosis.
Historically, stress radiography was utilized to quantify the degree of valgus laxity objectively. However, in the modern clinical setting, stress radiography is largely contraindicated when a Stener lesion is suspected clinically. Applying forceful valgus stress to a partial tear can inadvertently convert it into a complete tear, or it can actively displace a non-displaced complete tear over the adductor aponeurosis, creating an iatrogenic Stener lesion. Given the definitive clinical exam under local anesthesia, stress radiographs were omitted.
Advanced Cross Sectional Imaging
While the clinical diagnosis of a complete ulnar collateral ligament rupture with a Stener lesion was highly probable based on the palpable mass and gross laxity, Magnetic Resonance Imaging was ordered to definitively map the pathoanatomy, confirm the Stener lesion, and assist in surgical templating.
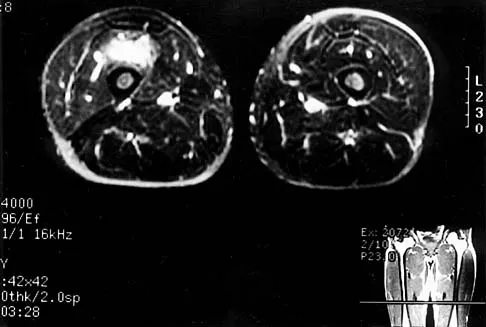
A high-resolution MRI of the right thumb without intravenous contrast was performed using a dedicated surface coil. The protocol included T1-weighted, T2-weighted, and proton density fat-saturated sequences in the axial, coronal, and sagittal planes relative to the thumb metacarpophalangeal joint.
The MRI findings were definitive. Coronal T2-weighted fat-suppressed images demonstrated a complete, full-thickness discontinuity of the proper and accessory ulnar collateral ligaments at their distal insertion onto the base of the proximal phalanx. The proximal stump of the ruptured ligament was visualized retracted proximally.
Crucially, the MRI demonstrated the classic yo yo on a string sign. The torn, retracted ulnar collateral ligament stump appeared as a balled-up, nodular mass of low signal intensity (the "yo-yo") resting superficial and proximal to the low-signal band of the adductor pollicis aponeurosis (the "string"). This confirmed the presence of a Stener lesion. Furthermore, the MRI confirmed the absence of occult trabecular microfractures, osteochondral shear injuries to the metacarpal head, or concomitant injuries to the radial collateral ligament or volar plate. The flexor pollicis longus tendon and extensor mechanism were intact and properly centralized.
Differential Diagnosis
When evaluating acute ulnar-sided thumb pain and instability following a traumatic abduction/extension injury, the differential diagnosis must distinguish between injuries that require immediate surgical intervention and those amenable to conservative management.
| Diagnostic Consideration | Mechanism of Injury | Key Clinical Findings | Imaging Characteristics |
|---|---|---|---|
| Complete UCL Rupture with Stener Lesion | Forced valgus/abduction of the thumb MCP joint. | >35° valgus laxity, >15° side-to-side difference. Palpable mass proximal to joint line. Lack of a firm endpoint. | MRI shows full-thickness tear, retracted proximal stump superficial to adductor aponeurosis (yo-yo on a string sign). |
| Partial UCL Sprain (Grade I/II) | Mild to moderate forced valgus/abduction. | Tenderness over UCL. Valgus laxity <30°, minimal side-to-side difference. Firm endpoint present. No palpable mass. | MRI shows ligamentous edema and thickening, but continuous fibers. No retraction. Adductor aponeurosis is superficial to the ligament. |
| Bony Avulsion Fracture (Gamekeeper's Fracture) | Forced valgus/abduction, often with a rotational component. | Tenderness localized to the volar-ulnar base of the proximal phalanx. Crepitus may be present. Variable laxity depending on displacement. | Plain radiographs demonstrate a fracture fragment at the ulnar base of the proximal phalanx. Fragment may be non-displaced, displaced, or rotated. |
| Radial Collateral Ligament (RCL) Rupture | Forced varus/adduction of the thumb MCP joint. | Tenderness over the radial aspect of the MCP joint. Instability with varus stress testing. Volar subluxation of the proximal phalanx. | MRI shows disruption of the RCL complex on the radial side of the joint. |
| Volar Plate Avulsion/Hyperextension Injury | Pure forced hyperextension of the thumb MCP joint. | Tenderness localized to the volar aspect of the MCP joint. Hyperextension laxity. Valgus/varus stability is typically preserved. | Lateral radiographs may show a small volar avulsion fragment. MRI confirms volar plate disruption at its distal insertion. |
Surgical Decision Making and Classification
Indications for Operative Intervention
The management of ulnar collateral ligament injuries is dictated by the precise pathoanatomy of the disruption. The primary goal of treatment is to restore a stable, painless metacarpophalangeal joint to allow for forceful pinch and grasp.
Non-operative management, consisting of rigid immobilization in a thumb spica cast or orthosis for four to six weeks, is strictly reserved for partial tears (Grade I and II sprains) or completely non-displaced bony avulsion fractures where the ligament remains anatomically reduced.
In this patient's case, the clinical examination demonstrating gross valgus instability lacking a firm endpoint, combined with the palpable mass and definitive MRI evidence of a Stener lesion, served as absolute indications for operative intervention.
The Stener lesion, first described by Bertil Stener in 1962, represents a mechanical barrier to healing. When the ulnar collateral ligament ruptures from its distal insertion, the adductor pollicis aponeurosis can slip beneath the torn ligament stump. The aponeurosis effectively interposes itself between the torn ligament and its anatomic footprint on the proximal phalanx. Because the ligament and the bone are physically separated by this aponeurotic sheet, spontaneous healing is biologically impossible, regardless of the duration of immobilization. Failure to surgically reduce and repair this lesion inevitably leads to chronic instability, profound pinch weakness, and the rapid onset of post-traumatic osteoarthritis of the metacarpophalangeal joint.
Pathoanatomic Classification
Ulnar collateral ligament injuries are broadly classified by chronicity and anatomic location.
Acute injuries (typically <3 weeks old) are amenable to direct primary repair. Chronic injuries (>3-4 weeks old) often present with retracted, scarred, and attenuated ligamentous tissue that is inadequate for primary repair, necessitating complex ligamentous reconstruction using autograft (e.g., palmaris longus or plantaris tendon). Given this patient presented within 48 hours of the injury, he was an ideal candidate for an acute primary repair.
Anatomically, the injury is classified as either a soft tissue avulsion, a mid-substance tear, or a bony avulsion. Mid-substance tears are relatively rare. The vast majority of complete ruptures occur as soft tissue avulsions directly from the distal insertion site at the base of the proximal phalanx. This patient presented with a classic distal soft tissue avulsion complicated by aponeurotic interposition, necessitating an open surgical approach for anatomic reduction and rigid internal fixation.
Surgical Technique and Intervention
Preoperative Preparation and Positioning
The patient was taken to the operating room and placed in the supine position on the operating table. A standard radiolucent hand table was attached to the operative side. Anesthesia was achieved via a regional supraclavicular brachial plexus block, supplemented with intravenous monitored anesthesia care for patient comfort.
A well-padded pneumatic tourniquet was applied to the proximal brachium. The right upper extremity was meticulously prepped and draped in a standard sterile surgical fashion. The limb was exsanguinated using an Esmarch bandage, and the tourniquet was inflated to 250 mmHg to ensure a bloodless surgical field. Intraoperative fluoroscopy was positioned and draped, ready for immediate use.
Surgical Approach and Dissection
A lazy-S or gently curved chevron incision was planned over the ulnar aspect of the thumb metacarpophalangeal joint. The incision was designed to avoid a straight longitudinal line crossing the flexion crease, which could lead to a restrictive postoperative scar contracture. The incision began mid-axially on the proximal phalanx, curved dorsally over the joint line, and extended proximally along the ulnar border of the first metacarpal.
Skin and subcutaneous tissues were incised sharply using a number 15 blade. Meticulous blunt dissection was performed using fine tenotomy scissors to identify and protect the terminal branches of the dorsal sensory radial nerve (Wartenberg's nerve). These delicate sensory branches are highly susceptible to iatrogenic injury or traction neuritis, which can result in debilitating postoperative neuromas. The nerve branches were gently mobilized and retracted dorsally using fine silastic vessel loops.
Deep dissection revealed the superficial fascia and the underlying adductor pollicis aponeurosis. At this stage, the pathoanatomy of the Stener lesion was directly visualized. The proximal stump of the ruptured ulnar collateral ligament was found lying superficial to the proximal edge of the adductor aponeurosis, appearing as a congested, bulbous mass of disorganized collagen.
To access the joint space and the ligament's anatomic footprint, the adductor aponeurosis was incised longitudinally, parallel to the extensor pollicis longus tendon. A 2 to 3 millimeter cuff of aponeurotic tissue was intentionally left attached to the extensor mechanism to facilitate a robust closure at the conclusion of the procedure. The aponeurosis was retracted volarly, exposing the underlying dorsal capsule and the metacarpophalangeal joint.
Ligament Reconstruction and Fixation
The joint capsule, which was found to be longitudinally torn as part of the injury complex, was opened further to allow for thorough intra-articular inspection. The articular surfaces of the metacarpal head and the base of the proximal phalanx were examined and found to be free of osteochondral defects. The joint was irrigated with sterile normal saline to evacuate the acute hemarthrosis.
Attention was then turned to the torn ulnar collateral ligament. The bulbous, retracted stump was mobilized. The degenerative, frayed edges of the ligament were sharply debrided back to healthy, organized collagenous tissue to optimize the biological healing environment.
The anatomic footprint of the ulnar collateral ligament on the volar-ulnar aspect of the proximal phalanx base was identified. Using a small curette and a fine surgical burr, the cortical bone at the footprint was decorticated to expose bleeding cancellous bone. This crucial step stimulates the local inflammatory cascade and provides marrow-derived osteoprogenitor cells to enhance ligament-to-bone healing.
For fixation, a 1.5 millimeter titanium suture anchor, double-loaded with high-strength non-absorbable ultra-high-molecular-weight polyethylene suture, was selected. The anchor was inserted into the prepared bony footprint at a 45-degree angle to the diaphyseal axis to maximize pullout strength. The anchor was seated flush with the cortical bone, and secure fixation was confirmed with manual traction.
The sutures were then passed through the distal stump of the ulnar collateral ligament using a modified Mason-Allen grasping stitch configuration. This specific suture technique provides superior biomechanical holding power and prevents the suture from pulling through the longitudinally oriented collagen fibers of the ligament under tension.
The thumb metacarpophalangeal joint was manually reduced and held in approximately 15 degrees of flexion and slight ulnar deviation to remove tension from the repair site. The sutures were then tied securely, bringing the ligament intimately down to the decorticated bony footprint.
Following knot tying, the joint was taken through a gentle range of motion. Direct visualization confirmed anatomic restoration of the ligamentous tension. Valgus stress testing was repeated intraoperatively and demonstrated complete restoration of joint stability, symmetric to the preoperative examination of the contralateral digit. Intraoperative fluoroscopy was utilized to confirm the precise placement of the suture anchor and ensure no intra-articular penetration of the hardware.
Closure and Immediate Postoperative Care
Once the ligament repair was deemed mechanically sound, the joint capsule was approximated using 4-0 absorbable braided sutures. The critical step of repairing the adductor aponeurosis was then performed. The aponeurosis was anatomically repaired over the reconstructed ulnar collateral ligament using 4-0 absorbable sutures, effectively restoring the dynamic stabilizing function of the adductor pollicis muscle.
The tourniquet was deflated, and meticulous hemostasis was achieved using bipolar electrocautery to prevent postoperative hematoma formation. The skin was closed using 5-0 non-absorbable monofilament nylon sutures in a simple interrupted fashion.
A sterile, non-adherent dressing was applied to the incision. The thumb was immediately immobilized in a custom-molded, fiberglass short-arm thumb spica splint. The splint positioned the wrist in 20 degrees of extension, the thumb carpometacarpal joint in slight palmar abduction, and the metacarpophalangeal joint in 15 degrees of flexion. Crucially, the thumb interphalangeal joint was left free to allow for immediate active range of motion, preventing flexor pollicis longus tendon adhesions. The patient was monitored in the post-anesthesia care unit and discharged home the same day with appropriate oral analgesics and strict instructions for elevation and neurovascular monitoring.
Post Operative Protocol and Rehabilitation
Acute Immobilization Phase
The initial postoperative phase, spanning from day zero to two weeks, prioritizes wound healing, edema control, and absolute protection of the surgical repair. The patient is instructed to maintain strict elevation of the operative extremity above the level of the heart to mitigate swelling. Active range of motion of the shoulder, elbow, and non-involved digits is strongly encouraged to prevent stiffness and promote venous return. The interphalangeal joint of the involved thumb must be actively flexed and extended multiple times daily to prevent tethering of the flexor pollicis longus tendon.
At the two-week postoperative mark, the patient returns to the clinic. The fiberglass surgical splint is removed, and the surgical incision is inspected. Suture removal is performed if the wound edges are fully epithelialized and stable. At this juncture, the patient is transitioned into a custom-fabricated thermoplastic thumb spica orthosis by a certified hand therapist. This orthosis continues to immobilize the metacarpophalangeal and carpometacarpal joints but is removable for hygiene and supervised therapy sessions.
Progressive Mobilization Phase
Between two and four weeks postoperatively, the goal shifts toward preventing capsular contracture while continuing to protect the healing ligament-to-bone interface. Under the direct supervision of a hand therapist, the patient initiates active range of motion exercises for the thumb metacarpophalangeal joint in the flexion and extension planes only. Absolute avoidance of any active or passive abduction or valgus stress is strictly enforced. The thermoplastic orthosis must be worn at all times outside of these dedicated therapy sessions, including during sleep.
From four to six weeks, the rehabilitation protocol advances. The patient may begin gentle passive range of motion in flexion and extension to address any residual joint stiffness. The weaning process from the rigid orthosis begins during light, non-stressful activities of daily living. However, the orthosis is still mandated for any activity involving lifting, gripping, or potential unpredictable trauma, as well as during sleep.
Strengthening and Return to Activity
At six weeks postoperatively, the ligament-to-bone healing is generally considered biologically mature enough to withstand mild to moderate physiological loads. The rigid thermoplastic orthosis is discontinued. The patient is transitioned to a soft neoprene thumb spica sleeve, which provides proprioceptive feedback and mild support during the transition to normal use.
Progressive strengthening exercises are initiated. This begins with isometric exercises for the thenar and adductor musculature, followed by dynamic strengthening using therapeutic putty and hand grippers. Specific focus is placed on restoring key pinch, chuck grip, and power grasp strength.
For this specific patient, occupational therapy focuses heavily on simulated keyboard and mouse utilization, ensuring the thumb can sustain the repetitive micro-impacts of typing and the static stabilization required for mouse control without pain or fatigue.
By eight to ten weeks, the patient is typically cleared for full, unrestricted activities of daily living and work. Return to high-impact sports, such as alpine skiing, is generally permitted at the ten to twelve-week mark. However, patients are strongly advised to utilize a prophylactic custom thumb brace during high-risk sporting activities for the first year following surgery to prevent recurrent catastrophic failure during the final phases of ligamentous remodeling.
Clinical Pearls and Pitfalls
Diagnostic Pearls
- The 30-Degree Flexion Rule: Valgus stress testing must be performed with the metacarpophalangeal joint in 30 degrees of flexion to accurately isolate the proper ulnar collateral ligament. Testing only in extension may yield a false negative if the volar plate and accessory ligament are intact.
- Local Anesthesia is Mandatory: Attempting to grade laxity in an acutely injured, unanesthetized thumb is highly unreliable due to involuntary muscle guarding by the adductor pollicis. A local intra-articular or digital block is essential for an accurate physical examination.
- Palpation Precedes Stress: Always palpate the ulnar joint line for a Stener lesion before applying valgus stress. Forceful stress testing of a non-displaced complete tear can iatrogenically displace the ligament superficial to the aponeurosis, converting a potentially non-operative injury into an operative one.
- Radiographic Scrutiny: Always obtain a true anteroposterior (Roberts) view to rule out a bony avulsion. A large, displaced bony fragment requires internal fixation (e.g., mini-screws or K-wires) rather than suture anchors.
Surgical Pitfalls
- Radial Sensory Nerve Injury: The dorsal sensory branches of the radial nerve are highly variable and course directly through the surgical field. Meticulous blunt dissection and gentle retraction are critical. A postoperative neuroma in this location is often
