Chronic Achilles Tendon Rupture Reconstruction: An Intraoperative Masterclass in Tendon Transfer and Grafting
Key Takeaway
Join us in the OR for a detailed masterclass on chronic Achilles tendon rupture reconstruction. We'll meticulously cover patient positioning, surgical anatomy, and step-by-step techniques for peroneus brevis or gracilis tendon transfer, emphasizing critical pearls, pitfalls, and comprehensive postoperative management to ensure optimal patient outcomes.
Welcome, esteemed colleagues and surgical fellows, to the operating theater. Today, we are undertaking a masterclass in a pathology that is as intellectually demanding as it is technically challenging: the reconstruction of the chronic Achilles tendon rupture. Unlike the straightforward primary repair of an acute rupture, the chronic or neglected Achilles tear presents a formidable reconstructive conundrum. These cases demand meticulous preoperative planning, a profound understanding of lower extremity biomechanics, and a versatile armamentarium of advanced reconstructive techniques, including tendon transfers and autologous grafting. Our ultimate objective is not merely anatomical continuity, but the restoration of robust plantarflexion power, physiologic resting tension, and functional independence for our patients.
Comprehensive Introduction and Patho-Epidemiology
The Achilles tendon is the largest and most powerful tendinous structure in the human body, yet it remains highly susceptible to rupture. While acute ruptures are frequently encountered in emergency departments and sports medicine clinics, a staggering 20% to 25% of these injuries are initially misdiagnosed. This diagnostic failure invariably leads to a chronic or neglected rupture, universally defined in the orthopaedic literature as a rupture with a delay in diagnosis or definitive treatment exceeding four weeks.
The Pathogenesis of Chronicity and the Watershed Zone
The pathogenesis of Achilles tendon ruptures is intimately linked to its unique vascular anatomy. The tendon receives its blood supply from the musculotendinous junction proximally, the osteotendinous insertion distally, and the surrounding paratenon. However, microangiographic studies have consistently demonstrated a distinct "watershed" zone of relative hypovascularity located approximately 2 to 6 centimeters proximal to the calcaneal insertion. This precarious blood supply diminishes further with advancing age, making this specific segment highly vulnerable to degenerative tendinosis and subsequent mechanical failure.
When an acute rupture is missed, the normal cascade of tendon healing is severely disrupted. The hematoma that initially fills the rupture gap is gradually replaced by disorganized, non-contractile fibrovascular scar tissue. As the proximal gastrocnemius-soleus complex undergoes unopposed retraction, this scar tissue elongates, resulting in a functionally lengthened and mechanically incompetent musculotendinous unit. Furthermore, the proximal muscle belly rapidly undergoes fatty infiltration and atrophy, significantly compromising its contractile potential even if anatomical continuity is eventually restored.
Clinical Presentation and the Deception of Compensatory Mechanisms
The clinical diagnosis of a chronic Achilles rupture is notoriously treacherous. The classic acute presentation—a sudden "pop," immediate weakness, and a palpable defect—is often absent or forgotten by the patient. Instead, these individuals typically present weeks or months later complaining of a vague, persistent ache, a noticeable limp, and profound difficulty with unilateral heel raises or ascending stairs.
The physical examination requires a high index of suspicion. The palpable gap, a hallmark of acute injuries, is frequently obliterated by the interposition of thick, hypertrophic scar tissue. More deceptively, patients often demonstrate preserved active plantarflexion. This is a critical diagnostic pitfall; this movement is driven by the compensatory hypertrophy and action of the tibialis posterior, the peroneal tendons (longus and brevis), and the long toe flexors (flexor hallucis longus and flexor digitorum longus).
To unmask the deficit, we rely on specific provocative maneuvers. The Calf Squeeze Test (Simmonds/Thompson Test) remains a staple; however, the surgeon must be aware that an intact, hypertrophied plantaris tendon can occasionally yield a false-negative result. The Knee Flexion Test (Matles Test) is highly sensitive; with the patient prone and knees actively flexed to 90 degrees, the affected foot will invariably fall into neutral or slight dorsiflexion due to the loss of resting Achilles tension, contrasting sharply with the physiologic plantarflexion of the contralateral intact limb.
Advanced Imaging and Diagnostic Adjuncts
Given the unreliability of the clinical exam in chronic settings, advanced imaging is an absolute prerequisite for both definitive diagnosis and surgical templating. Plain lateral weight-bearing radiographs are the initial step. We must critically evaluate Kager’s triangle—the pre-Achilles fat pad. In a chronic rupture, the normal radiolucent geometry of this fat pad is obliterated by edema, hemorrhage, and fibrotic infiltration. Furthermore, radiographs help rule out avulsion fractures of the calcaneal tuberosity.
Ultrasonography provides a dynamic, cost-effective evaluation. In the hands of an experienced musculoskeletal sonographer, a chronic rupture manifests as an "acoustic vacuum" or a heterogeneous mass of disorganized echogenic scar tissue bridging the retracted tendon stumps.
However, Magnetic Resonance Imaging (MRI) remains the undisputed gold standard for preoperative templating. T1-weighted sagittal and axial sequences are paramount for quantifying the exact length of the tendon gap after accounting for the interposed scar tissue. Furthermore, MRI allows us to assess the degree of fatty infiltration and atrophy within the gastrocnemius and soleus muscle bellies (Goutallier classification), which directly influences our expectations for postoperative functional recovery and helps dictate whether a local tendon transfer is sufficient or if more extensive reconstruction is warranted.
Detailed Surgical Anatomy and Biomechanics
A masterful reconstruction requires an intimate, three-dimensional understanding of the posterior leg and ankle anatomy. The surgical approach, graft harvest, and final fixation are all dictated by the intricate relationships of the musculotendinous and neurovascular structures.
The Gastrocnemius-Soleus-Achilles Complex
The Achilles tendon is the conjoint tendon of the gastrocnemius and soleus muscles. The gastrocnemius, a biarticular muscle crossing both the knee and ankle, provides explosive plantarflexion power. The soleus, a monoarticular muscle originating from the tibia and fibula, is rich in slow-twitch type I muscle fibers, providing crucial postural control and sustained plantarflexion endurance.
As the aponeuroses of these two muscles merge to form the Achilles tendon, the fibers undergo a complex, spiraling rotation. The fibers from the medial head of the gastrocnemius rotate laterally, while the soleus fibers rotate medially to insert on the posteromedial aspect of the calcaneal tuberosity. This spiraling architecture is biomechanically brilliant, allowing the tendon to elongate and store elastic strain energy during the stance phase of gait, which is subsequently released during push-off. Recreating this physiologic tensioning is the crux of a successful reconstruction.
Critical Neurovascular Topography
The posterior surgical approach to the ankle is fraught with potential neurovascular hazards. The most vulnerable structure is the sural nerve. Formed by the convergence of the medial sural cutaneous nerve (a branch of the tibial nerve) and the sural communicating branch (from the common peroneal nerve), it courses distally down the posterior calf.
Crucially, the sural nerve crosses the lateral border of the Achilles tendon from medial to lateral at an average distance of 9.8 centimeters proximal to the calcaneal insertion. It then runs distally along the lateral aspect of the tendon, accompanied by the small saphenous vein, to provide sensation to the lateral hindfoot and midfoot. To mitigate the risk of iatrogenic neuroma or sensory deficit, our primary longitudinal incision must be placed strictly medial to the medial border of the Achilles tendon.
Deep to the superficial posterior compartment lies the tibial nerve and posterior tibial artery, safely sequestered within the deep posterior compartment behind the transverse intermuscular septum. While generally safe during a standard Achilles approach, these structures become highly relevant if a flexor hallucis longus (FHL) tendon transfer is planned.
Graft Harvest Anatomy: The Peroneus Brevis
For moderate tendon gaps (typically 3 to 9 centimeters), the peroneus brevis (PB) tendon transfer is a highly reliable and biomechanically sound reconstructive option. The peroneus brevis originates from the distal two-thirds of the lateral fibular shaft and the adjacent intermuscular septa. It courses distally through the retromalleolar groove, deep and anterior to the peroneus longus, to insert onto the tuberosity at the base of the fifth metatarsal.
Harvesting the PB requires a thorough understanding of the lateral compartment's neurovascular supply. The superficial peroneal nerve provides innervation, while the blood supply is segmental. A major advantage of the PB transfer is that when the tendon is detached distally and mobilized proximally, its proximal muscular blood supply via the lateral intermuscular septum is preserved, effectively making it a vascularized local tendon transfer. This robust vascularity dramatically enhances the healing potential when woven through the avascular scar tissue of the chronic Achilles defect.
Exhaustive Indications and Contraindications
The decision to proceed with operative reconstruction for a chronic Achilles tendon rupture is generally straightforward, as conservative management yields uniformly poor functional outcomes. However, patient selection must be rigorous, balancing the significant functional benefits against the inherent risks of complex soft tissue surgery in a watershed vascular zone.
| Category | Specific Criteria | Clinical Rationale |
|---|---|---|
| Absolute Indications | Symptomatic chronic rupture (>4 weeks old) | Persistent weakness, altered gait mechanics, inability to perform unilateral heel raise. |
| MRI-confirmed gap > 3 cm after debridement | Primary end-to-end repair is impossible under physiologic tension; requires augmentation/transfer. | |
| Failed conservative management | Persistent pain and functional limitation despite aggressive physical therapy and bracing. | |
| Relative Indications | High-demand athlete with a smaller gap | May require augmentation (e.g., plantaris weave) even for smaller gaps to ensure robust construct strength. |
| Absolute Contraindications | Severe Peripheral Vascular Disease (PVD) | High risk of catastrophic wound necrosis, infection, and subsequent amputation. |
| Active local or systemic infection | Risk of deep space seeding and osteomyelitis. | |
| Non-ambulatory patient | The risks of surgery outweigh the negligible functional benefits. | |
| Severe medical comorbidities | Unacceptable perioperative mortality risk (e.g., recent MI, severe COPD). | |
| Relative Contraindications | Uncontrolled Diabetes Mellitus | Significantly elevated risk of wound dehiscence and deep infection. Requires strict glycemic optimization prior to surgery. |
| Chronic high-dose corticosteroid use | Poor tissue quality, impaired healing, and high risk of construct failure or wound breakdown. | |
| Active smoking | Nicotine-induced vasoconstriction severely compromises the already tenuous microvascular supply of the posterior skin flaps. |
Pre-Operative Planning, Templating, and Patient Positioning
Preoperative planning is the foundation of a successful reconstruction. We utilize the Kuwada classification system to categorize the defect and dictate our surgical algorithm. This classification is based on the intraoperative gap measured after the radical debridement of all interposed scar tissue.
- Type I (Partial tear): Excision of scar tissue and primary repair.
- Type II (Complete tear, gap < 3 cm): End-to-end repair, often facilitated by a V-Y advancement flap of the proximal gastrocnemius aponeurosis.
- Type III (Complete tear, gap 3 to 6 cm): Requires tendon transfer (Peroneus Brevis or FHL) or synthetic/allograft interposition.
- Type IV (Complete tear, gap > 6 cm): Requires complex reconstruction, often combining a V-Y advancement with a tendon transfer, or utilizing a free autologous graft (e.g., Gracilis or Semitendinosus).
For the purpose of this masterclass, we are templating for a Kuwada Type III defect, utilizing a Peroneus Brevis tendon transfer.
Patient Positioning and Anesthesia
The procedure is typically performed under general anesthesia, though a robust regional neuraxial block (spinal or epidural) is an acceptable alternative, provided the patient can tolerate the prone position.
The patient is carefully transitioned onto the operating table in the prone position. It is absolutely critical that the patient is positioned such that the knees are at the break of the table and the feet and ankles hang completely free and clear of the mattress. This allows the surgeon to freely manipulate the ankle through a full arc of motion, from maximal dorsiflexion to maximal plantarflexion. This unrestricted motion is non-negotiable, as it is required to accurately set the resting tension of the reconstructed tendon.
A well-padded pneumatic tourniquet is applied to the proximal thigh. The operative limb is exsanguinated using an Esmarch bandage, and the tourniquet is inflated to 250 to 300 mmHg. A bloodless field is essential for meticulous dissection, identifying the sural nerve, and ensuring thorough debridement of the fibrotic tendon ends.
Step-by-Step Surgical Approach and Fixation Technique
We are now ready to commence the reconstruction. The room must be quiet, and the surgical team focused. The margin for error in soft tissue handling in this region is zero.
The Surgical Incision and Exposure
We begin with a 10- to 12-centimeter longitudinal, slightly curvilinear incision. The placement is critical: it must be positioned exactly 1 centimeter medial to the palpable medial border of the Achilles tendon. This medial trajectory is our primary defense against iatrogenic injury to the sural nerve.
The initial incision is carried sharply through the epidermis and dermis. From this point forward, dissection must be deliberate and respectful of the tenuous local vascularity. We must elevate full-thickness fasciocutaneous flaps. Skiving into the subcutaneous fat or creating thin skin flaps is the most common technical error leading to catastrophic postoperative wound necrosis. The dissection proceeds directly down to the crural fascia and the underlying paratenon.
If the paratenon is identifiable and viable, it is incised longitudinally in the midline and carefully reflected. In many chronic cases, however, the paratenon is densely adherent, scarred, or entirely obliterated by the chronic inflammatory process.
Radical Debridement: Establishing Healthy Tissue
Upon exposing the tendon, the extent of the pathology becomes visually apparent. The rupture gap is typically bridged by a dense, bulbous mass of yellowish, disorganized fibrocartilaginous scar tissue. This tissue lacks the organized collagen bundles required for tensile strength.
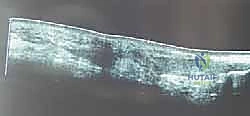
Using a #15 scalpel blade and heavy tissue scissors, we perform a radical and unapologetic debridement of both the proximal and distal tendon stumps. We must resect all fibrotic, devitalized tissue until we encounter normal, pearly-white tendon bundles that exhibit punctate bleeding—the "paprika sign" of healthy tissue.
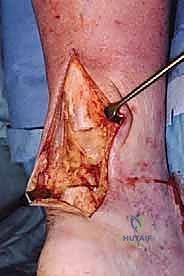
Once the debridement is complete, we apply heavy traction sutures (e.g., #2 FiberWire) to the proximal stump and pull distally to overcome muscle retraction. With the ankle held in neutral dorsiflexion, we measure the true defect gap. In this case, we measure a 5-centimeter gap, confirming our preoperative plan for a Peroneus Brevis transfer.
Harvesting the Peroneus Brevis Tendon
Attention is now directed to the lateral aspect of the foot. We make a separate 2.5-centimeter longitudinal incision directly over the palpable base of the fifth metatarsal.
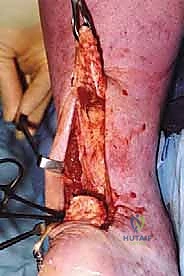
Blunt dissection through the subcutaneous tissue exposes the peroneal sheath. The sheath is incised, revealing the peroneus brevis tendon inserting onto the tuberosity, with the peroneus longus tendon diving plantarward into the cuboid groove.
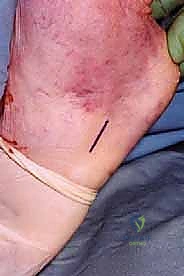
We place a locking whipstitch (using a #2 non-absorbable suture) into the distal 2 centimeters of the peroneus brevis tendon to secure control. Using a scalpel, the tendon is sharply detached directly from its bony insertion on the fifth metatarsal base.
Returning to our primary posterior incision, we identify the peroneus brevis muscle belly and tendon proximal to the lateral malleolus. Applying gentle traction to our distal whipstitch, we carefully pull the detached tendon proximally into the primary posterior wound. We must ensure that the tendon glides freely and that all fascial adhesions within the retromalleolar groove are released, while strictly preserving the muscular branches from the lateral intermuscular septum.
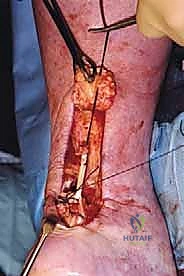
The Reconstructive Weave and Tensioning
With the robust peroneus brevis tendon now mobilized into the posterior wound, we prepare for the reconstructive weave. The goal is to bridge the defect while creating a biomechanically superior construct that allows for early postoperative mobilization.
We utilize a modified Pulvertaft weave technique. Using a #11 blade, we create a transverse slit through the center of the healthy proximal Achilles tendon stump, approximately 2 centimeters proximal to its debrided edge.
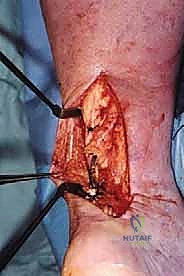
The peroneus brevis tendon is passed through this slit from lateral to medial.
Next, we create a corresponding transverse or oblique slit in the distal Achilles stump (or directly through the calcaneal tuberosity if the distal stump is inadequate).
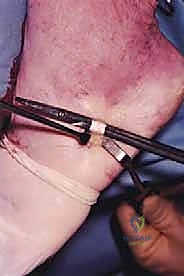
The peroneus brevis is then routed distally and passed through this distal slit.
Now comes the most critical step of the entire procedure: Setting the Tension. The ankle must be placed into approximately 15 to 20 degrees of plantarflexion (equinus). This position matches the resting tension of the contralateral, uninjured limb.
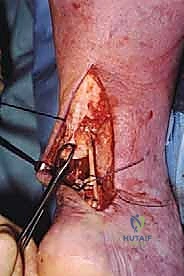
While an assistant holds the ankle rigidly in this equinus position, maximal distal traction is applied to the proximal Achilles stump, and the peroneus brevis tendon is pulled taut through the distal slit.
While maintaining this strict tension, the weave is secured. We use multiple figure-of-eight and horizontal mattress sutures of #2 non-absorbable braided suture (e.g., FiberWire or Ethibond) at every intersection of the peroneus brevis and the Achilles stumps.
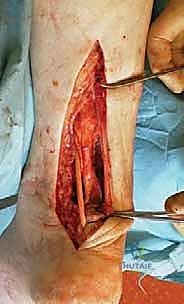
To augment the construct and prevent any micromotion at the transfer site, additional fixation can be employed. If the distal stump was short and the PB was routed through a calcaneal bone tunnel, a biocomposite interference screw is deployed to achieve aperture fixation. Alternatively, robust suture anchors can be placed into the calcaneal tuberosity to tie down the distal aspect of the weave.
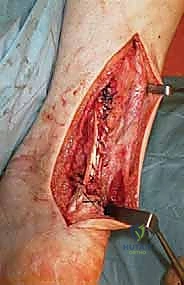
The final construct is rigorously tested. The surgeon takes the ankle through a gentle arc of motion, confirming that the resting equinus is maintained and that the construct moves as a single, cohesive, and mechanically sound unit.

Meticulous Closure
Closure is just as critical as the reconstruction itself. The tourniquet is deflated, and meticulous hemostasis is achieved using bipolar electrocautery. Hematoma formation in this dead space is a primary catalyst for deep infection and wound breakdown.
If the paratenon was preserved, it is meticulously closed over the reconstruction using a 3-0 absorbable suture. The subcutaneous tissue is closed in multiple layers using 2-0 and 3-0 absorbable sutures, ensuring that no tension is transmitted to the skin edges.
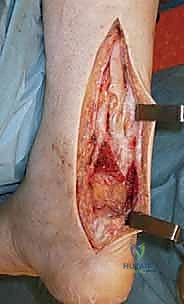
The skin is closed using a non-tension-producing technique, such as vertical mattress sutures or a running subcuticular closure with nylon or prolene.
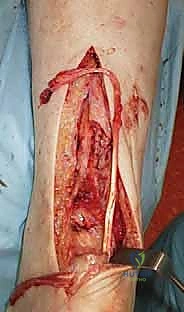
The leg is cleaned, sterile dressings are applied, and the limb is immobilized in a well-padded short-leg splint with the ankle locked in the exact degree of equinus (15-20 degrees) that was set during the reconstructive weave.
Complications, Incidence Rates, and Salvage Management
Despite meticulous surgical technique, chronic Achilles reconstruction carries a significantly higher complication profile compared to acute primary repair. The surgeon must be prepared to identify and aggressively manage these sequelae.
| Complication | Estimated Incidence | Pathophysiology & Prevention | Salvage & Management Strategy |
|---|---|---|---|
| Wound Necrosis / Dehiscence | 5% - 15% | Caused by thin skin flaps, excessive retraction, or smoking. Prevent via strict medial incision, full-thickness flaps, and atraumatic handling. | Minor: Local wound care, negative pressure wound therapy (NPWT). Major: Plastic surgery consultation for sural artery fasciocutaneous flap or free tissue transfer. |
| Sural Nerve Injury (Neuroma) | 3% - 10% | Iatrogenic transection or entrapment in scar tissue. Prevent by maintaining a strict medial surgical approach. | Initial: Gabapentinoids, desensitization. Refractory: Surgical exploration, neuroma excision, and burying the proximal nerve stump into deep muscle. |
| Deep Infection | 2% - 5% | Hematoma formation or contiguous spread from superficial wound breakdown. | Aggressive surgical irrigation and debridement (I&D), retention of viable graft if possible, infectious disease consultation for culture-directed IV antibiotics. |
| Construct Re-Rupture | 2% - 4% | Patient non-compliance with bracing, premature weight-bearing, or inadequate initial fixation strength. | Revision surgery utilizing a more robust graft (e.g., free Gracilis autograft or Achilles allograft with calcaneal bone block). |
| Deep Vein Thrombosis (DVT) / PE | 1% - 5% | Prolonged immobilization and prone positioning. | Chemical prophylaxis (LMWH or DOACs) based on patient risk stratification (Caprini score), early mobilization. |
Phased Post-Operative Rehabilitation Protocols
The surgical reconstruction is only half the battle; the postoperative rehabilitation protocol is equally critical to the final functional outcome. The protocol must delicately balance the need to protect the healing tendon transfer with the necessity of early mobilization to prevent debilitating arthrofibrosis and muscle atrophy.
Phase I: Maximum Protection (Weeks 0 to 2)
Immediately postoperative, the patient is strictly non-weight-bearing. The limb is immobilized in the well-padded, rigid short-leg splint applied in the operating room, maintaining the ankle in 15 to 20 degrees of plantarflexion. The primary goals during this phase are strict elevation to minimize edema, strict adherence to non-weight-bearing status, and monitoring for any signs of wound compromise or deep vein thrombosis.
Phase II: Controlled Mobilization (Weeks 2 to 6)
At the two-week mark, the surgical splint is removed, and the incision is meticulously inspected. Sutures are removed if the wound is fully healed. The patient is transitioned into a controlled ankle motion (CAM) boot equipped with 3 to 4 heel wedges to maintain the equinus position and eliminate tension on the reconstruction.
During this phase, the patient remains non-weight-bearing or touch-down weight-bearing with crutches. Under the guidance of a physical therapist, the patient begins active range of motion (ROM) out of the boot, focusing strictly on active plantarflexion and active dorsiflexion only to the neutral position. Stretching into dorsiflexion past neutral is strictly prohibited, as it risks elongating the healing construct.
Phase III: Progressive Weight-Bearing and Strengthening (Weeks 6 to 12)
At six weeks, radiographic and clinical healing of the soft tissues is generally sufficient to initiate progressive mechanical loading. The heel wedges in the CAM boot are sequentially removed—typically one wedge every 1 to 2 weeks—slowly bringing the ankle towards neutral.
Weight-bearing is progressively advanced from partial to full weight-bearing within the CAM boot. Physical therapy intensifies, focusing on isometric and concentric strengthening of the gastrocnemius-soleus complex. Proprioceptive training and closed-kinetic-chain exercises (e.g., seated calf raises, double-leg stance on unstable surfaces) are initiated.
Phase IV: Return to Function (Months 3 to 6+)
By the third month, the patient is typically transitioned out of the CAM boot and into a supportive athletic shoe, often utilizing a small silicone heel lift for an additional month to prevent sudden stretching.
Therapy now focuses on eccentric strengthening, which is vital for collagen remodeling and restoring the tendon's ability to store and release elastic energy. Patients progress to single-leg heel raises, plyometrics, and sport-specific agility drills. The operating surgeon must counsel the patient that maximal functional recovery, particularly the restoration of explosive push-off power, may take up to 12 to 18 months following a chronic reconstruction.
Summary of Landmark Literature and Clinical Guidelines
The evolution of chronic Achilles reconstruction is deeply rooted in landmark orthopaedic literature. A thorough understanding of these foundational texts is essential for any reconstructive surgeon.
- Perez-Teuffer (1974): Pioneered the use of the peroneus brevis tendon transfer for Achilles reconstruction. His original description highlighted the robust vascularity of the PB and its biomechanical suitability for bridging moderate defects, establishing it as a workhorse technique.
- Wapner et al. (1993): Revolutionized the approach to larger defects and older, less active patients by popularizing the Flexor Hallucis Longus (FHL) tendon transfer. Wapner demonstrated that the FHL is stronger than the PB, its axis of pull more closely replicates the Achilles, and its muscle belly provides excellent vascularized coverage for compromised posterior skin.
- Kuwada (1990): Developed the definitive classification system for Achilles tendon defects. By categorizing ruptures based on the intraoperative gap size after debridement, Kuwada provided the surgical
