Introduction and Epidemiology
Total hip arthroplasty (THA) stands as a monumental achievement in modern orthopedic surgery, consistently demonstrating unparalleled efficacy in pain eradication, functional restoration, and the enhancement of health-related quality of life for patients afflicted with end-stage hip pathology. The procedure necessitates the meticulous surgical extirpation of the diseased articular surfaces and their substitution with highly engineered prosthetic components. The historical trajectory of THA spans over a century, evolving from rudimentary interpositional arthroplasties (utilizing materials ranging from fascia lata to glass and vitalium) to the sophisticated modular systems employed today. Sir John Charnley’s introduction of the "low-friction arthroplasty" concept in the early 1960s—combining a small-diameter metallic femoral head, a polytetrafluoroethylene (later ultra-high-molecular-weight polyethylene, UHMWPE) acetabular component, and polymethylmethacrylate (PMMA) bone cement—established the biomechanical and tribological paradigm that underpins contemporary joint replacement.
Epidemiologically, the global incidence of hip osteoarthritis (OA), the predominant indication for THA, exhibits a relentless upward trajectory. The prevalence of symptomatic hip OA is estimated to afflict 1% to 2% of the adult population in industrialized nations, with a markedly higher penetrance in cohorts exceeding 65 years of age. Demographic shifts, characterized by an aging population, increasing life expectancy, and a rising prevalence of obesity, are catalyzing a profound surge in THA utilization. Epidemiological forecasting in the United States projects annual THA volumes to exceed 1.4 million by 2040, representing an exponential increase from the roughly 400,000 procedures performed annually in the early 2020s. Furthermore, there is a discernible demographic shift toward younger, higher-demand patients undergoing THA, placing unprecedented demands on implant survivorship and bearing surface tribology.
Beyond primary OA, other significant etiologies necessitating THA include inflammatory arthropathies (e.g., rheumatoid arthritis, ankylosing spondylitis), osteonecrosis (avascular necrosis, AVN) of the femoral head, post-traumatic osteoarthritis, developmental dysplasia of the hip (DDH), and displaced intracapsular femoral neck fractures in physiologically robust, active elderly patients.
The health economics of THA are compelling. While the index procedural costs, inpatient hospitalization, and post-acute care represent substantial initial expenditures, these are overwhelmingly eclipsed by the long-term societal dividends. THA yields a highly favorable cost-per-Quality-Adjusted Life Year (QALY) ratio. It restores workforce participation, mitigates the systemic sequelae of chronic immobility, and drastically reduces the reliance on chronic analgesic pharmacotherapy, cementing its status as one of the most cost-effective interventions in the entire medical armamentarium.
Surgical Anatomy and Biomechanics
A profound, three-dimensional comprehension of hip osteology, myology, and neurovascular topography is the sine qua non of successful THA. The hip is an inherently stable, multiaxial enarthrodial (ball-and-socket) joint engineered for simultaneous weight-bearing and extensive spatial mobility.
Osteology and Articular Anatomy
- Proximal Femur: The proximal femur comprises the femoral head, neck, greater and lesser trochanters, and the intertrochanteric region. The native femoral head represents approximately two-thirds of a true sphere. The femoral neck projects from the diaphysis at an angle of inclination (neck-shaft angle) typically ranging between 120° and 135°, and exhibits an anterior version (anteversion) of 10° to 15° relative to the trans-epicondylar axis of the distal femur. The greater trochanter acts as the critical lever arm for the abductor mechanism (gluteus medius and minimus), while the lesser trochanter serves as the apophysis for the iliopsoas tendon. The calcar femorale is a dense, vertically oriented plate of cortical bone originating from the posteromedial diaphysis and radiating proximally into the femoral neck, serving as a primary load-transfer conduit.
- Acetabulum: The acetabulum is a hemispherical concavity situated at the confluence of the ilium, ischium, and pubis (the triradiate cartilage in the skeletally immature). The articular surface is the horseshoe-shaped facies lunata, which surrounds the central, non-articular acetabular fossa containing the ligamentum teres and the pulvinar (fat pad). The structural integrity of the acetabulum relies on the anterior and posterior columns. The native acetabulum is typically oriented with 40° to 45° of inclination and 15° to 20° of anteversion. The transverse acetabular ligament, spanning the inferior acetabular notch, serves as a critical intraoperative landmark for determining the inferior border of the definitive component and establishing true anatomical anteversion.
Musculature and Dynamic Stabilizers
The periarticular musculature dictates joint stability, gait mechanics, and the selection of surgical internervous planes.
* Abductors: The gluteus medius and minimus, innervated by the superior gluteal nerve, are the primary abductors. They originate from the external ilium and insert onto the greater trochanter. Their functional integrity is paramount for maintaining a level pelvis during the single-leg stance phase of gait (preventing a Trendelenburg lurch).
* External Rotators: The piriformis, superior and inferior gemelli, obturator internus, obturator externus, and quadratus femoris provide dynamic posterior stability. These are routinely encountered and often released during the posterolateral approach.
* Flexors and Extensors: The iliopsoas and rectus femoris serve as primary flexors. The gluteus maximus (inferior gluteal nerve) is the primary extensor, crucial for rising from a seated position and stair climbing.
Neurovascular Topography
- Sciatic Nerve: Arising from the lumbosacral plexus (L4-S3), it exits the greater sciatic foramen typically inferior to the piriformis. It lies in close proximity to the posterior acetabular column and is highly vulnerable to iatrogenic injury during posterior retractory placement, excessive leg lengthening, or thermal necrosis from extruded PMMA.
- Femoral Nerve and Vessels: Situated in the anterior compartment. The femoral nerve lies lateral to the femoral artery. These structures are at risk during anterior approaches, particularly with aberrant retractor placement over the anterior acetabular rim.
- Superior Gluteal Nerve: Exits the greater sciatic notch superior to the piriformis and courses anteriorly between the gluteus medius and minimus. It is at risk during direct lateral or anterolateral approaches if the proximal fascial split extends more than 3 to 5 cm proximal to the greater trochanter.
- Vascular Supply to the Femoral Head: Primarily derived from the medial and lateral circumflex femoral arteries (branches of the profunda femoris), which form an extracapsular arterial ring. Ascending cervical branches pierce the capsule to form the subsynovial intra-articular ring, terminating in the lateral epiphyseal vessels.
Biomechanics and Tribology
The biomechanical imperative of THA is the precise restoration of the hip's center of rotation (COR), femoral offset, and leg length to optimize abductor mechanics and minimize joint reactive forces.
- Static Equilibrium and Lever Arms: During single-leg stance, the hip acts as a class I lever. The fulcrum is the femoral head. The body weight (acting through the center of gravity) creates a moment arm that must be counterbalanced by the abductor musculature. Because the body weight lever arm is typically 2.5 to 3 times longer than the abductor lever arm, the abductor muscles must generate a force significantly greater than body weight. Consequently, the joint reactive force across the hip can reach 3 to 5 times body weight during normal gait, and up to 10 times during strenuous activity.
- Femoral Offset: Defined as the perpendicular distance from the center of rotation of the femoral head to the longitudinal axis of the femoral diaphysis. Restoring or slightly increasing offset improves the abductor lever arm, thereby decreasing the required abductor force and the resultant joint reactive force. Failure to restore offset leads to abductor weakness, increased energy expenditure during gait, and potential impingement.
- Center of Rotation (COR): The anatomical COR must be restored. Superior and lateral displacement of the acetabular component shortens the abductor lever arm and increases joint reactive forces, accelerating wear and increasing the risk of mechanical failure.
- Implant Tribology: The science of interacting surfaces in relative motion (friction, wear, and lubrication).
- Metal-on-Polyethylene (MoP): The historical gold standard. Modern highly cross-linked polyethylene (HXLPE), often infused with antioxidants like Vitamin E to prevent in vivo oxidation, has dramatically reduced wear rates (osteolysis threshold is typically considered >0.1 mm/year; modern HXLPE wear is often <0.05 mm/year).
- Ceramic-on-Ceramic (CoC): Offers the lowest wear rates and is highly scratch-resistant. However, it carries risks of catastrophic component fracture and audible "squeaking."
- Ceramic-on-Polyethylene (CoP): Currently the most widely utilized bearing couple, combining the excellent wear characteristics and scratch resistance of a ceramic head with the forgiving mechanical properties of HXLPE.
- Jump Distance: The vertical distance the femoral head must translate before frank dislocation occurs. Larger femoral heads (e.g., 32mm, 36mm) increase the jump distance and the head-to-neck ratio, significantly improving range of motion prior to impingement and reducing the risk of dislocation.
Indications and Contraindications
The decision to proceed with THA must be predicated on a rigorous clinical and radiographic evaluation, balancing the severity of the pathology against the patient's physiological reserves and operative risk profile.
Indications for Total Hip Arthroplasty
The primary indication is recalcitrant, debilitating pain and functional impairment secondary to structural hip disease that has proven refractory to a comprehensive regimen of conservative modalities (e.g., weight optimization, activity modification, NSAIDs, intra-articular corticosteroid injections, physical therapy).
- Primary Osteoarthritis (OA): Radiographically characterized by asymmetric joint space narrowing, subchondral sclerosis, osteophytosis, and subchondral cyst formation (Kellgren-Lawrence Grade III-IV).
- Inflammatory Arthropathies: Rheumatoid arthritis, ankylosing spondylitis, and systemic lupus erythematosus. These patients often present with concentric joint space loss, severe osteopenia, and protrusio acetabuli. THA in this cohort may require specialized techniques to address bone loss and soft tissue contractures.
- Osteonecrosis (AVN): Ficat/Steinberg Stage III (subchondral collapse/crescent sign) and Stage IV (secondary degenerative changes). AVN often affects younger patients and necessitates meticulous preoperative planning regarding stem fixation in potentially compromised metaphyseal bone.
- Developmental Dysplasia of the Hip (DDH): Classified by the Crowe or Hartofilakidis systems. High-grade DDH presents complex reconstructive challenges, including a shallow, lateralized true acetabulum, excessive femoral anteversion, a narrow femoral canal, and significant leg length discrepancies often requiring subtrochanteric shortening osteotomies.
- Post-Traumatic Osteoarthritis: Sequelae of acetabular fractures, femoral head fractures, or traumatic dislocations. These cases are frequently complicated by retained hardware, heterotopic ossification, and distorted anatomy.
- Acute Femoral Neck Fractures: Displaced intracapsular fractures (Garden III/IV) in physiologically active, independent community ambulators. THA yields superior functional outcomes and lower revision rates compared to hemiarthroplasty in this specific demographic.
Contraindications for Total Hip Arthroplasty
- Absolute Contraindications:
- Active Sepsis or Periprosthetic Joint Infection (PJI): Any active local or systemic infection (e.g., florid urinary tract infection, untreated dental abscess, cellulitis) is an absolute contraindication due to the catastrophic risk of hematogenous seeding of the implant.
- Neuropathic Arthropathy (Charcot Joint): Profound sensory loss and proprioceptive deficits lead to rapid, massive bone destruction and inevitable early implant failure.
- Severe Neurological Deficits: Conditions precluding active participation in rehabilitation or resulting in a flail, non-functional limb (e.g., profound quadriplegia, advanced myopathies).
- Relative Contraindications:
- Severe Medical Comorbidities: Unstable angina, recent myocardial infarction (<6 months), uncompensated congestive heart failure, severe pulmonary hypertension, or end-stage renal disease. These require rigorous preoperative medical optimization.
- Morbid Obesity (BMI > 40 kg/m²): Significantly elevates the risk of PJI, dislocation, venous thromboembolism, and early mechanical failure. Many institutions implement strict BMI cutoffs (e.g., <40 or <35) prior to elective THA.
- Poor Dentition: Requires dental clearance prior to surgery to mitigate hematogenous seeding.
- Inadequate Bone Stock: Severe osteopenia or massive structural defects that preclude stable implant fixation, though custom triflange components and advanced augments have expanded the reconstructive envelope.
Operative vs. Non-Operative Paradigm
| Parameter | Operative Candidacy (THA) | Non-Operative Optimization |
|---|---|---|
| Clinical Presentation | Intractable rest pain, severe night pain, ambulatory capacity < 1 block, failure of >6 months conservative care. | Mild/intermittent pain, functional ADLs maintained, responsive to NSAIDs/injections. |
| Radiographic Findings | Bone-on-bone articulation, severe structural collapse, large osteophytic impingement. | Mild joint space narrowing, preserved spherical congruency. |
| Patient Optimization | HbA1c < 7.5%, BMI < 40, smoking cessation > 4-6 weeks, optimized nutritional status (Albumin > 3.5 g/dL). | Uncontrolled diabetes, active nicotine use, profound malnutrition. |
Pre Operative Planning and Patient Positioning
Surgical execution is only as robust as the preoperative plan. Advanced templating and a nuanced understanding of spinopelvic mechanics are mandatory in contemporary arthroplasty.
Clinical and Radiographic Assessment
- Spinopelvic Biomechanics: The relationship between the lumbar spine and the pelvis dictates the functional orientation of the acetabulum during positional changes (sitting to standing). Patients with a stiff lumbar spine (e.g., multi-level spinal fusion, severe spondylosis) fail to increase their pelvic tilt when sitting, leading to functional retroversion of the acetabulum and a high risk of anterior impingement and posterior dislocation. These patients require customized cup positioning (often increased anteversion and inclination).
- Digital Templating: Utilizing calibrated digital radiographs (typically with a 25mm spherical marker).
- Acetabular Templating: The center of rotation is established relative to the teardrop and Kohler's line. The goal is to place the cup at the level of the true acetabulum, restoring the anatomical COR without excessive medialization or superior migration.
- Femoral Templating: Determines the optimal stem size to achieve diaphyseal or metaphyseal fill (depending on stem design). The neck cut level is calculated to restore leg length (measured from the lesser trochanter to the inter-teardrop line) and femoral offset.
- Leg Length Discrepancy (LLD): Preoperative LLD must be quantified objectively (radiographically) and subjectively (clinical block testing). The surgeon must distinguish between true LLD (bony asymmetry) and apparent LLD (due to pelvic obliquity from adduction/abduction contractures).
Patient Positioning
Impeccable positioning dictates surgical exposure and mitigates iatrogenic complications.
- Lateral Decubitus Position (Posterior and Direct Lateral Approaches):
- The patient is positioned laterally with the operative hip superior. Rigid pelvic fixation using anterior (pubic symphysis) and posterior (sacrum) supports is critical. If the pelvis rolls anteriorly or posteriorly during acetabular reaming, the surgeon's spatial orientation is compromised, leading to malpositioned components (excessive retroversion or anteversion).
- An axillary roll is mandatory to prevent brachial plexus neuropraxia. The dependent fibular head must be padded to protect the common peroneal nerve.
- Supine Position (Direct Anterior Approach - DAA):
- Often performed on a specialized radiolucent traction table (e.g., Hana table) to allow independent manipulation, traction, and rotation of the operative limb.
- Facilitates intraoperative fluoroscopy to objectively assess cup positioning, offset, and leg length in real-time.
- Care must be taken to avoid hyperextension of the contralateral hip, and the perineal post must be adequately padded to prevent pudendal nerve injury.
Detailed Surgical Approach and Technique
While the direct anterior approach (DAA) and anterolateral approaches have seen a surge in popularity, the posterolateral approach remains the most universally taught and highly versatile technique, offering extensile exposure for both primary and complex revision scenarios.
The Posterolateral (Moore/Southern) Approach
This approach exploits the anatomical interval posterior to the gluteus medius and minimus, preserving the critical abductor mechanism.
- Incision and Superficial Dissection:
- A curvilinear incision is centered over the posterior third of the greater trochanter.
- The subcutaneous tissue is incised to expose the fascia lata distally and the gluteus maximus fascia proximally.
- The fascia lata is incised longitudinally. Proximally, the gluteus maximus fibers are bluntly split in line with their orientation. This is not a true internervous plane, as the gluteus maximus is innervated by the inferior gluteal nerve, but splitting the fibers minimizes denervation.
- Deep Dissection and External Rotator Takedown:
- A Charnley or self-retaining retractor is placed beneath the gluteus maximus. The bursa overlying the external rotators is excised.
- The posterior border of the gluteus medius is identified and retracted anteriorly.
- The short external rotators (piriformis, superior gemellus, obturator internus, inferior gemellus) are identified. The piriformis tendon is isolated. A stay suture is placed through the conjoined insertion of these tendons on the greater trochanter, and they are sharply detached close to their insertion.
- The quadratus femoris is identified distally; its proximal half may be released, taking care to coagulate the ascending branch of the medial circumflex femoral artery located at its distal border to prevent postoperative hematoma.
- Neurovascular Alert: The sciatic nerve lies immediately deep to the gluteus maximus and posterior to the short external rotators. It must be protected from direct trauma and excessive traction.
- Capsulotomy and Dislocation:
- A robust capsulotomy (T-shaped, H-shaped, or complete capsulectomy) is performed to expose the femoral head and neck.
- The hip is dislocated via controlled flexion, adduction, and internal rotation. If the hip is ankylosed or severe protrusio is present, an in situ femoral neck osteotomy may be required prior to head extraction.
- Femoral Neck Osteotomy:
- Utilizing preoperative templating, the osteotomy is performed with an oscillating saw at the appropriate level above the lesser trochanter, maintaining the planned version.
- Acetabular Preparation and Implantation:
- Retractors are placed to expose the entire acetabular rim (anterior, posterior, and inferiorly over the transverse acetabular ligament).
- The labrum and peripheral osteophytes are excised to identify the true bony rim.
- Sequential reaming is performed, directing the reamer in 40° of inclination and 15°-20° of anteversion, medializing down to the medial wall (cotyloid fossa) without breaching the quadrilateral plate.
- A cementless, porous-coated hemispherical titanium shell is press-fit into the prepared bed. Supplemental cancellous screws may be placed in the posterosuperior quadrant (the safe zone) to augment primary stability.
- The polyethylene or ceramic liner is impacted into the shell.
- Femoral Preparation and Implantation:
- The operative leg is placed in flexion, adduction, and marked internal rotation.
- The femoral canal is accessed with a box osteotome laterally to avoid varus malpositioning.
- Sequential broaching is performed to shape the metaphysis and diaphysis. For cementless stems, broaching continues until rotational stability and cortical chatter are achieved.
- The trial stem and neck/head components are inserted.
- Trial Reduction and Biomechanical Assessment:
- The hip is reduced. The surgeon rigorously assesses:
- Leg Length: Comparing the level of the medial malleoli or utilizing intraoperative pin measurements.
- Offset: Assessing abductor tension (the "shuck" test).
- Stability: The hip is taken through dynamic ranges of motion. For a posterior approach, stability is tested in 90° of flexion, adduction, and internal rotation. Impingement (bony or component) is identified and addressed.
- The hip is reduced. The surgeon rigorously assesses:
- Definitive Implantation and Closure:
- Trial components are removed, and the definitive stem and head are implanted.
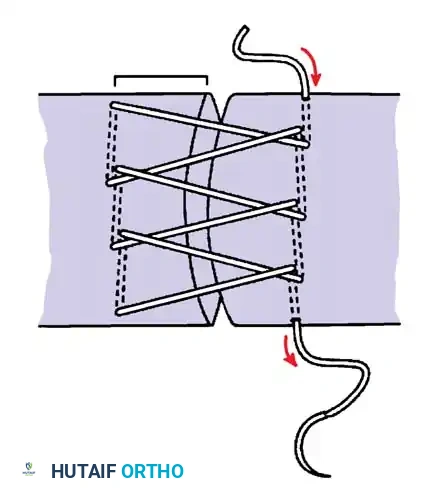
- Enhanced Posterior Soft Tissue Repair (EPSTR): The capsule and short external rotators are meticulously repaired back to the greater trochanter through transosseous drill holes. This step is critical and has drastically reduced the dislocation rate of the posterior approach to levels comparable with anterior approaches.
- Layered closure of the fascia lata, subcutaneous tissue, and skin.
Alternative Approaches
- Direct Anterior Approach (DAA): Utilizes the true internervous plane between the tensor fasciae latae (superior gluteal nerve) and the sartorius/rectus femoris (femoral nerve). It is highly touted for preserving the posterior capsule and abductors, theoretically accelerating early mobilization. Challenges include a steep learning curve, risk to the lateral femoral cutaneous nerve (meralgia paresthetica), and difficulty addressing severe femoral deformity or complex revisions.
- Direct Lateral (Hardinge) Approach: Splits the gluteus medius and vastus lateralis. Provides excellent acetabular exposure and carries a very low dislocation rate. The primary drawback is the risk of iatrogenic injury to the superior gluteal nerve or failure of the abductor repair, leading to a permanent Trendelenburg gait.
Complications and Management
The mitigation of complications requires obsessive attention to detail, rigorous patient optimization, and precise surgical execution.
1. Periprosthetic Joint Infection (PJI)
PJI is the most devastating complication in arthroplasty, carrying substantial morbidity and mortality.
* Pathogenesis: Can occur via direct intraoperative inoculation or delayed hematogenous seeding. Biofilm formation on the inert implant surface renders systemic antibiotics largely ineffective without surgical intervention.
* Diagnosis: Relies on the Musculoskeletal Infection Society (MSIS) or International Consensus Meeting (ICM) criteria. Workup includes serum ESR/CRP, joint aspiration for synovial fluid cell count (>3,000 WBC/µL and >80% PMNs in chronic PJI), alpha-defensin, and aerobic/anaerobic/fungal/AFB cultures.
* Management:
* Acute PJI (<4 weeks post-op or <3 weeks symptom duration): Debridement, Antibiotics, and Implant Retention (DAIR) with exchange of modular components.
* Chronic PJI: Two-stage revision is the gold standard. Stage 1: Explantation of all components, radical debridement, and placement of an antibiotic-eluting PMMA spacer. Stage 2: Reimplantation of definitive components after 6-12 weeks of targeted IV antibiotics and normalization of inflammatory markers.
2. Instability and Dislocation
- Etiology: Multifactorial, including component malposition (failure to adhere to the Lewinnek safe zone of 40°±10° inclination and 15°±10° anteversion, though this is now modified by spinopelvic parameters), inadequate restoration of offset (lax abductors), impingement, and patient non-compliance.
- Management: Acute dislocations are managed with closed reduction under conscious sedation. Recurrent instability necessitates comprehensive radiographic and CT evaluation to assess component version. Surgical revision may involve repositioning malaligned components, increasing head size, utilizing dual-mobility constructs, or employing constrained liners in salvage scenarios.
3. Periprosthetic Fracture (PPF)
- Classification: The Vancouver Classification dictates management for femoral fractures.
- Type A: Trochanteric (usually non-operative or cerclage).
- Type B1: Around or just below the stem, stem is well-fixed (ORIF with locking plates and cables).
- Type B2: Around or just below the stem, stem is loose (Revision to a long, distally fixing bypass stem).
- Type B3: Stem is loose with severe bone stock loss (Revision with proximal femoral replacement or allograft-prosthesis composite).
- Type C: Well below the stem (ORIF).
4. Venous Thromboembolism (VTE)
- Prophylaxis: Modern protocols favor risk-stratified approaches. For standard-risk patients, early mobilization combined with chemical prophylaxis (e.g., Aspirin 81mg BID for 4 weeks) has proven highly efficacious. High-risk patients (history of VTE, known thrombophilia) require more aggressive anticoagulation (LMWH, DOACs, or Warfarin).
5. Leg Length Discrepancy (LLD)
- Iatrogenic lengthening is the most common cause of post-THA litigation. Lengthening is often inadvertently performed to achieve soft-tissue stability if offset is not adequately restored. Management is primarily preventative through meticulous templating and intraoperative measurement. Symptomatic LLD postoperatively is initially managed with shoe lifts; severe, disabling LLD may require revision.
6. Neurovascular Injury
- Sciatic Nerve Palsy: Most common nerve injury (0.5-2%). Usually presents as a peroneal division deficit (foot drop). Causes include direct trauma, retractor compression, excessive lengthening (>3-4 cm), or hematoma. Management includes immediate removal of compressive dressings, maintaining the hip in extension and knee in flexion to reduce tension, and surgical exploration if a compressive hematoma is identified.
Post Operative Rehabilitation Protocols
Modern THA rehabilitation is governed by Enhanced Recovery After Surgery (ERAS) pathways, which have fundamentally shifted the paradigm from prolonged bed rest to immediate, aggressive mobilization.
Immediate Post-Operative Phase (Days 0-1)
- Multimodal Analgesia: Opioid-sparing protocols are standard. This includes preoperative administration of gabapentinoids and acetaminophen, intraoperative periarticular injections (PAI) of local anesthetics (e.g., bupivacaine, ropivacaine mixed with epinephrine and ketorolac), and postoperative scheduled NSAIDs.
- Mobilization: Patients are mobilized out of bed and initiate weight-bearing as tolerated (WBAT) on postoperative day zero under the supervision of physical therapy.
- Discharge Criteria: Many patients are now discharged within 24 hours (outpatient THA). Criteria include independent transfers, ability to ambulate household distances with an assistive device, ability to negotiate stairs, adequate pain control on oral medications, and spontaneous voiding.
Acute to Subacute Phase (Weeks 1-6)
- Precautions: Depending on the surgical approach, specific hip precautions may be enforced (e.g., avoiding flexion >90°, internal rotation, and adduction for posterior approaches) for 4 to 6 weeks to allow capsular healing.
- Physical Therapy: Focuses on gait normalization, weaning from assistive devices (walker to cane to independent), and progressive resistance exercises targeting the hip abductors, extensors, and core musculature.
Long-Term Management
- Patients are encouraged to return to low-impact aerobic activities (cycling, swimming, golf, doubles tennis). High-impact loading (running, jumping sports) is
Detailed Chapters & Topics
Dive deeper into specialized chapters regarding form
