Conservative Hip Surgery: Relief for Bilateral Dysplasia
Key Takeaway
Learn more about Conservative Hip Surgery: Relief for Bilateral Dysplasia and how to manage it. Conservative hip surgery addresses conditions like Developmental Dysplasia of the Hip (DDH) in patients such as a 47-year-old female experiencing severe bilateral groin pain and activity limitations. This joint-preserving approach targets underlying anatomical abnormalities, evident from positive impingement tests, to reduce pain, improve hip function, and potentially avoid or postpone total hip replacement, considering the patient's specific health profile.
Introduction and Epidemiology
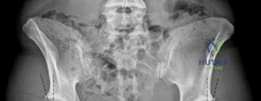
Developmental Dysplasia of the Hip represents a spectrum of abnormalities in hip joint development, ranging from mild acetabular dysplasia to frank dislocation. While often presenting unilaterally, a significant proportion of cases, up to 30 to 50 percent in some series, manifest bilaterally. Bilateral acetabular dysplasia poses unique challenges, often delaying diagnosis due to a lack of contralateral asymmetry on physical examination and requiring comprehensive, staged management strategies. The inherent biomechanical instability and altered load distribution in dysplastic hips predispose patients to premature degenerative changes, labral tears, and eventual osteoarthritis, particularly in the weight-bearing zones.
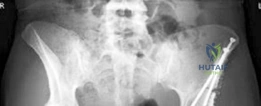
Conservative hip surgery, primarily encompassing joint-preserving osteotomies, aims to restore normal hip anatomy, optimize joint congruency, and redistribute articular contact pressures, thereby mitigating the progression of degenerative disease. The periacetabular osteotomy, initially described by Ganz, has become the gold standard for acetabular reorientation in skeletally mature adolescents and young adults with symptomatic hip dysplasia, demonstrating excellent long-term outcomes in preserving native hip function. Other osteotomies, such as the Dega, Pemberton, and triple osteotomy, are typically reserved for skeletally immature patients or specific pediatric deformity patterns. This review focuses on the current understanding, surgical principles, and outcomes of conservative hip surgery, with particular emphasis on the management of bilateral dysplasia in the adult and near-adult population.
Epidemiologically, the incidence of developmental dysplasia of the hip varies widely based on geographic and genetic factors, with higher prevalence noted in Native American and Eastern European populations. Female sex, breech presentation, and a positive family history remain the most robust risk factors. In the context of bilateral disease, patients frequently present with a waddling gait, hyperlordosis, and insidious onset of bilateral groin pain. Because both hips are structurally deficient, the compensatory mechanisms typically available to unilateral dysplasia patients are absent, often leading to accelerated bilateral chondral wear and earlier clinical presentation in early adulthood.
Surgical Anatomy and Biomechanics
A thorough understanding of the regional anatomy and the biomechanical sequelae of acetabular dysplasia is paramount for successful surgical planning and execution. The normal acetabulum provides comprehensive coverage of the femoral head, with a spherical articulation that distributes loads across a wide surface area.

Key radiographic parameters are critical in quantifying the degree and pattern of dysplasia. These include the lateral center-edge angle of Wiberg (normal >25 degrees), the anterior center-edge angle of Lequesne (normal >20 degrees), the Tönnis angle or acetabular index (normal <10 degrees), and the femoral epiphyseal acetabular roof index.
In acetabular dysplasia, the acetabulum is typically shallow, anteverted, and laterally displaced, leading to inadequate femoral head coverage. This morphological deficiency results in profound biomechanical consequences.
Pathomechanics of Dysplasia
The primary biomechanical failure in dysplasia is the drastic reduction in articular contact area. This concentrates stress on a smaller region of articular cartilage, predominantly in the superolateral and anterior aspects of the femoral head and acetabulum. This edge-loading phenomenon generates increased shear forces due to the more vertical orientation of the superior acetabulum. Over time, this leads to labral hypertrophy, subsequent labral tearing, and cartilage delamination at the chondrolabral junction.

Furthermore, the femoral head may migrate superolaterally, altering the lever arm mechanics of the abductor musculature. The shortened abductor lever arm necessitates increased muscle force to maintain pelvic level during the single-leg stance phase of gait, increasing the overall joint reaction force. Ligamentous laxity of the capsule and ligamentum teres further contributes to microinstability.
The goals of acetabular reorientation via periacetabular osteotomy are to normalize these parameters, increase the weight-bearing surface, improve abductor muscle mechanics by medializing the hip center of rotation, and protect the labrum and articular cartilage. The osteotomies performed in a periacetabular osteotomy selectively detach the acetabular fragment while preserving the posterior column and the blood supply via the superior gluteal vessels and obturator artery branches, allowing for precise three-dimensional reorientation without compromising pelvic ring stability.
Indications and Contraindications
The decision to proceed with conservative hip surgery for bilateral dysplasia is multifaceted, weighing patient symptoms, radiographic findings, skeletal maturity, and the potential for long-term joint preservation. The ideal candidate is a skeletally mature young adult with symptomatic, radiographically confirmed acetabular dysplasia and preserved articular cartilage space.
Patient Selection Criteria
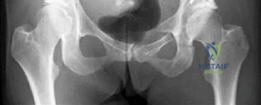
Symptomatic presentation typically involves activity-related groin pain, mechanical symptoms such as catching or clicking (indicative of concomitant labral pathology), and fatigue in the hip abductors. Radiographically, a lateral center-edge angle of less than 20 degrees, an anterior center-edge angle of less than 20 degrees, and an elevated Tönnis angle confirm the diagnosis.
Crucially, the joint space must be preserved. Patients with Tönnis grade 0 or 1 osteoarthritic changes are optimal candidates. Those with Tönnis grade 2 changes represent a grey area where joint preservation may be attempted but carries a higher risk of early conversion to total hip arthroplasty. Tönnis grade 3 changes, characterized by severe joint space narrowing, subchondral cysts, and large osteophytes, are an absolute contraindication to periacetabular osteotomy.
In bilateral cases, the decision regarding surgical timing is critical. Simultaneous bilateral periacetabular osteotomies have been described but carry significantly higher risks of blood loss, prolonged operative times, and complex postoperative rehabilitation. Staged bilateral periacetabular osteotomies, typically separated by an interval of 3 to 6 months to allow for adequate bony healing and rehabilitation of the first side, are the preferred approach in most high-volume centers.
| Parameter | Operative Indications (PAO) | Non-Operative / Alternative Management |
|---|---|---|
| Skeletal Maturity | Closed triradiate cartilage | Open triradiate cartilage (Dega/Pemberton) |
| Symptoms | Persistent groin pain, mechanical symptoms | Asymptomatic, incidental finding |
| Joint Space (Tönnis Grade) | Grade 0 or 1 (Preserved cartilage) | Grade 2 (Relative contraindication), Grade 3 (THA indicated) |
| LCE Angle | < 20 degrees | > 25 degrees (Consider isolated arthroscopy if symptomatic) |
| Hip Range of Motion | Preserved functional ROM | Stiff hip, severe contractures |
| Patient Age | Generally < 40-45 years | > 50 years (Higher risk of failure, lean toward THA) |
| Systemic Factors | Normal bone quality, medically optimized | Inflammatory arthropathy, severe osteoporosis |
Pre Operative Planning and Patient Positioning
Meticulous preoperative planning is essential for achieving optimal acetabular reorientation while avoiding neurovascular injury and intra-articular fracture.
Radiographic Evaluation
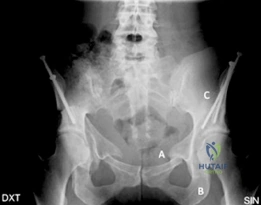
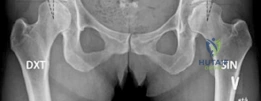
Standard radiographic evaluation includes an anteroposterior pelvis radiograph, a false profile view of Lequesne, and a Dunn lateral or cross-table lateral view. The AP pelvis allows for the measurement of the LCE angle, Tönnis angle, extrusion index, and evaluation of the Shenton line. The false profile view is critical for assessing anterior femoral head coverage (ACE angle) and evaluating the anterior joint space.
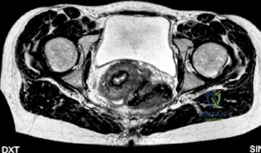
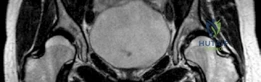
Advanced imaging with computed tomography (CT) with 3D reconstruction is increasingly utilized. 3D CT allows for precise mapping of the bony anatomy, evaluation of acetabular version, and virtual surgical planning. Magnetic resonance imaging (MRI) or MR arthrography is routinely obtained to evaluate the integrity of the labrum, articular cartilage, and ligamentum teres. Concomitant intra-articular pathology is highly prevalent in dysplastic hips and must be factored into the surgical plan, often necessitating a combined approach with hip arthroscopy or open arthrotomy.
Surgical Positioning and Setup
The patient is positioned supine on a radiolucent operating table to facilitate unimpeded intraoperative fluoroscopy. A bump may be placed under the ipsilateral hemipelvis to slightly elevate the operative side. The entire lower extremity is prepped and draped free to allow for dynamic assessment of hip range of motion and intraoperative manipulation of the limb during osteotomy execution and fragment reorientation.
A sterile tourniquet is not utilized. Intraoperative cell salvage is highly recommended due to the vascular nature of the pelvic cancellous bone. The fluoroscopy C-arm is positioned on the contralateral side of the table, ensuring that perfect AP, obturator oblique, and iliac oblique views of the pelvis can be obtained seamlessly throughout the procedure.
Detailed Surgical Approach and Technique
The Bernese periacetabular osteotomy remains the standard technique for conservative hip surgery in mature dysplasia. The procedure involves a series of four precise osteotomies that free the acetabulum from the pelvic ring while preserving the posterior column.
Surgical Approach
The procedure is typically performed via a modified Smith-Petersen approach or an anterior intrapelvic (Stoppa) approach. For the modified Smith-Petersen approach, the skin incision begins along the anterior iliac crest and extends distally toward the anterior superior iliac spine, curving distally along the interval between the tensor fasciae latae and the sartorius.
The superficial internervous plane is between the sartorius (femoral nerve) and the tensor fasciae latae (superior gluteal nerve). The deep internervous plane lies between the rectus femoris (femoral nerve) and the gluteus medius (superior gluteal nerve). The lateral femoral cutaneous nerve must be identified and protected, as it frequently crosses the operative field. The abdominal obliques and iliacus are elevated off the inner table of the ilium, exposing the quadrilateral plate and the pelvic brim.
The Four Osteotomies
The success of the periacetabular osteotomy relies on the precise execution of four distinct bone cuts.
1. Ischial Osteotomy:
The first cut is an incomplete osteotomy of the ischium. Access is gained by dissecting medial to the joint capsule and lateral to the psoas tendon. A specialized angled Ganz osteotome is directed infracotyloidally, starting just below the inferior acetabular rim and directed toward the ischial spine. This cut must not violate the posterior column or penetrate the joint.

2. Pubic Osteotomy:
The superior pubic ramus is exposed subperiosteally. Retractors are placed to protect the obturator neurovascular bundle inferiorly and the femoral neurovascular bundle superiorly. The osteotomy is performed using an oscillating saw or osteotomes just medial to the iliopectineal eminence, excising a small wedge of bone to allow for subsequent medialization and rotation of the acetabular fragment.
3. Iliac Osteotomy:
The iliac osteotomy begins at the anterior superior iliac spine (or just distal to it) and extends posteriorly. It is performed with an oscillating saw, stopping short of the pelvic brim. The cut is directed toward the greater sciatic notch but terminates approximately 1 to 2 centimeters short of the notch to preserve the structural integrity of the posterior column.
4. Retroacetabular Osteotomy:
The final and most technically demanding cut connects the iliac osteotomy to the ischial osteotomy. This is performed using an angled osteotome directed down the posterior column, remaining posterior to the articular surface. Fluoroscopic guidance (obturator oblique view) is critical to ensure the osteotome remains extra-articular and safely anterior to the posterior cortex of the posterior column.
Fragment Mobilization and Fixation
Once the osteotomies are complete, a Schanz pin is inserted into the supra-acetabular region of the mobilized fragment. The fragment is manipulated using a combination of flexion, internal rotation, and medialization to achieve optimal coverage. The goal is to achieve an LCE angle of 25 to 30 degrees, a neutral Tönnis angle, and slight anteversion of the acetabulum, while medializing the hip center.
Provisional fixation is achieved with Kirschner wires. The hip is then taken through a full range of motion to ensure there is no anterior impingement (which can occur if the fragment is over-rotated anteriorly) and that joint congruity is optimized. Fluoroscopy confirms the correction. Definitive fixation is typically achieved with three or four 3.5mm or 4.5mm fully threaded cortical screws directed from the stable ilium into the reoriented acetabular fragment.
Complications and Management
Periacetabular osteotomy is a technically demanding procedure with a steep learning curve. Complications can be significant and are generally categorized into intraoperative and postoperative events.
Intraoperative complications largely revolve around aberrant osteotomy trajectories. Intra-articular fracture is the most devastating, potentially leading to rapid joint degeneration. This is avoided by strict adherence to fluoroscopic landmarks, particularly during the retroacetabular cut. Neurovascular injuries can occur due to aggressive retraction or errant osteotome placement. The lateral femoral cutaneous nerve is most frequently affected, resulting in lateral thigh numbness. Injury to the sciatic nerve, femoral nerve, or obturator nerve is rare but morbid.
Postoperative complications include delayed union or nonunion, particularly at the pubic osteotomy site. Heterotopic ossification can restrict range of motion and is often mitigated with prophylactic nonsteroidal anti-inflammatory drugs. Overcorrection or retroversion of the acetabular fragment can induce secondary femoroacetabular impingement (pincer morphology), necessitating subsequent arthroscopic or open osteochondroplasty.
| Complication | Estimated Incidence | Etiology / Mechanism | Prevention and Salvage Strategies |
|---|---|---|---|
| LFCN Neuropraxia | 15% - 30% | Traction or direct injury during superficial dissection | Careful identification and mobilization; usually resolves spontaneously; gabapentin for neuropathic pain. |
| Intra-articular Fracture | 1% - 3% | Errant retroacetabular or ischial osteotome trajectory | Strict fluoroscopic guidance; if occurs, requires immediate anatomic reduction and screw fixation. |
| Heterotopic Ossification | 5% - 10% | Extensively stripped bone, muscle trauma | Indomethacin or localized radiation prophylaxis; surgical excision if mature and restricting ROM. |
| Nonunion (Pubic/Ischial) | 2% - 5% | Inadequate contact, thermal necrosis | Often asymptomatic; if symptomatic, may require bone grafting and revision plating. |
| Overcorrection (Impingement) | 3% - 8% | Excessive anterior/lateral rotation | Intraoperative ROM check; postoperative arthroscopic rim trimming if symptomatic FAI develops. |
| Major Vascular Injury | < 1% | Penetration of external iliac or obturator vessels | Retractor placement beneath iliopsoas; immediate vascular surgery consultation if pulsatile bleeding occurs. |
Post Operative Rehabilitation Protocols
Rehabilitation following conservative hip surgery is critical for achieving optimal functional outcomes, particularly in patients undergoing staged bilateral procedures. The protocol is designed to protect the osteotomy sites while promoting early mobility and preventing stiffness.
Phase 1 Protection Phase
The initial 6 to 8 weeks postoperatively focus on bone healing. Patients are restricted to toe-touch weight-bearing (approximately 20 pounds) on the operative extremity. Crutches or a walker are mandatory. In cases of staged bilateral dysplasia, if the interval between surgeries is short, wheelchair use may be temporarily required to protect both hemipelves. Continuous passive motion machines or early active-assisted range of motion exercises are initiated immediately to prevent capsular adhesions and nourish the articular cartilage. Active hip abduction is strictly avoided to prevent displacement of the osteotomy fragment prior to early consolidation.
Phase 2 Early Strengthening
Upon radiographic confirmation of early bridging callus (typically at the 6 to 8-week mark), patients transition to partial, and eventually full, weight-bearing. Aquatic therapy is highly beneficial during this transition. Rehabilitation focuses on restoring isometric abductor strength, core stability, and normalizing gait mechanics. Given the chronicity of abductor weakness in bilateral dysplasia, intensive pelvic drop exercises and closed-chain kinetic strengthening are emphasized.
Phase 3 Advanced Function
From 3 to 6 months postoperatively, therapy progresses to dynamic strengthening, proprioceptive training, and eventual return to sport-specific or high-demand occupational activities. For patients undergoing staged bilateral periacetabular osteotomies, the second surgery is typically scheduled during this phase, once the first hip has achieved pain-free full weight-bearing and sufficient abductor strength to support the contralateral rehabilitation process.
Summary of Key Literature and Guidelines
The academic foundation of the periacetabular osteotomy is rooted in the seminal work by Ganz et al. in 1988, which first detailed the surgical technique and its theoretical advantages over previous pelvic osteotomies. Subsequent literature has focused on long-term survivorship and the identification of prognostic variables.
Long-term follow-up studies, notably by Steppacher et al., have demonstrated remarkable joint preservation rates, with 20-year survivorship free of total hip arthroplasty exceeding 60 percent in properly selected patients. Predictors of failure, leading to early conversion to arthroplasty, consistently include advanced preoperative age (typically over 40 years), the presence of preoperative osteoarthritis (Tönnis grade 2 or greater), and a postoperative joint space width of less than 2 millimeters.
The Academic Network of Conservational Hip Outcomes Research (ANCHOR) registry has provided robust multicenter data regarding the safety and efficacy of the procedure. ANCHOR data corroborates that while concomitant labral pathology is nearly universal in symptomatic dysplasia, the primary driver of long-term success is the accurate biomechanical reorientation of the acetabulum.
In the context of bilateral dysplasia, contemporary guidelines recommend staged procedures over simultaneous bilateral surgery. Studies comparing the two approaches indicate that while simultaneous surgery reduces total hospital admissions, it is associated with significantly higher rates of allogeneic blood transfusion, longer intensive care unit stays, and a higher incidence of major complications. Consequently, the staged approach, allowing 3 to 6 months between interventions, remains the standard of care for bilateral conservative hip surgery.
