Primary Uncemented Total Hip Arthroplasty: A Case Study Title
Key Takeaway
This topic focuses on Primary Uncemented Total Hip Arthroplasty: A Case Study Title, The **case title uncemented** primary total hip arthroplasty addresses severe right hip osteoarthritis in a 61-year-old female. This procedure utilizes an extensively porous-coated femoral stem to achieve immediate diaphyseal cortical fixation without cement. This implant choice offers high long-term survivorship, providing a durable solution for debilitating hip pain when non-surgical treatments are exhausted.
Detailed Patient Presentation and Mechanism of Pathology
Demographic Profile and Chief Complaint
The patient is a 61-year-old female who presents to the orthopedic adult reconstruction clinic with a primary chief complaint of insidious, progressively worsening right hip pain that has been present for approximately one year. Her body mass index (BMI) is 34.1 kg/m², placing her in the Class I obesity category, bordering on Class II. This elevated BMI is a critical biomechanical and surgical factor, as it exponentially increases the joint reactive forces across the hip articulation during the stance phase of gait and necessitates meticulous surgical planning regarding the surgical approach, retractor placement, and soft-tissue management to minimize the risk of postoperative infection and component malposition.
The pain is predominantly localized to the right anterior groin, which is the classic dermatomal referral pattern for true intra-articular hip pathology, mediated primarily by the obturator and femoral nerves. The patient describes the pain as a deep, aching sensation that transforms into a sharp, stabbing pain precipitated by weight-bearing activities, specifically walking and transitioning from a seated to a standing position. Functionally, she reports profound difficulty with activities of daily living (ADLs) that require significant hip flexion and internal rotation, most notably putting on her shoes and socks. This functional deficit is a hallmark of the capsular contracture and osteophytic impingement characteristic of advanced degenerative joint disease.
Medical History and Systemic Considerations
A comprehensive evaluation of the patient's past medical history reveals a complex systemic profile that significantly elevates her perioperative risk and requires rigorous multidisciplinary optimization. Her principal medical pathologies include essential hypertension, hyperlipidemia, and, most critically, coronary artery disease (CAD) with a documented history of a previous myocardial infarction (MI). This cardiovascular profile mandates a thorough preoperative cardiac risk stratification, likely utilizing the Revised Cardiac Risk Index (RCRI), and necessitates formal clearance from her primary cardiologist.
Her current pharmacological regimen includes Lisinopril 10 mg daily for blood pressure control and Crestor (rosuvastatin) 4 mg nightly for lipid management. The history of a prior MI raises critical considerations regarding her perioperative antithrombotic and anticoagulant management. The orthopedic surgeon must carefully balance the risk of a secondary acute coronary syndrome against the risk of postoperative venous thromboembolism (VTE) and the potential for catastrophic surgical site bleeding or hematoma formation, which could subsequently lead to a periprosthetic joint infection (PJI).
Conservative management modalities have been exhaustively trialed and have ultimately failed to provide sustained symptomatic relief. The patient has utilized oral analgesics, specifically acetaminophen (Tylenol), with negligible benefit. She previously underwent a fluoroscopically guided intra-articular right hip corticosteroid injection, which provided profound but highly transient relief lasting only a single day—a diagnostic confirmation of the intra-articular source of her pain, but a therapeutic failure. Furthermore, a prolonged course of targeted physical therapy aimed at strengthening the abductor complex and core musculature yielded limited functional benefit, confirming that her pathology has surpassed the threshold for non-operative management.
Comprehensive Clinical Examination Findings
Inspection and Gait Analysis
Upon observation of the patient ambulating into the examination room, a pronounced antalgic gait is immediately evident. The patient demonstrates a significantly shortened stance phase on the affected right lower extremity, an involuntary compensatory mechanism designed to minimize the duration of peak joint reactive forces across the degenerated articular surface. Additionally, a subtle abductor lurch (uncompensated Trendelenburg gait) is noted, characterized by a lateral shift of the trunk over the right hip during the stance phase. This biomechanical adaptation reduces the moment arm of the body's center of gravity relative to the hip center of rotation, thereby decreasing the force required by the gluteus medius and minimus to maintain a level pelvis, effectively unloading the painful joint.
Range of Motion and Provocative Testing
Objective assessment of the right hip's range of motion (ROM) reveals severe, multidirectional restriction secondary to capsular fibrosis, osteophyte formation, and loss of the congruent articular spherical geometry. Active and passive ROM measurements are as follows:
* Extension: 0° (Normal is typically 10-15°). The lack of extension indicates a flexion contracture, which contributes to increased lumbar lordosis during standing and walking.
* Flexion: 70° (Normal is approximately 110-120°). This profound limitation directly correlates with her inability to perform ADLs such as donning footwear.
* Abduction: 20° (Normal is 40-50°).
* Adduction: 10° (Normal is 20-30°).
* External Rotation: 20° (Normal is 40-50°).
* Internal Rotation: 10° (Normal is 30-40°). The early loss of internal rotation is one of the most sensitive clinical indicators of hip osteoarthritis, reflecting the tensioning of the anterior capsule and the presence of anterior femoral neck osteophytes.
Provocative maneuvers, including the Stinchfield test (resisted straight leg raise) and the FADIR (Flexion, Adduction, Internal Rotation) test, elicit severe, reproducible anterior groin pain, further localizing the pathology to the intra-articular space.
Neurovascular and Musculoskeletal Integrity
A meticulous neurovascular examination of the bilateral lower extremities is performed to rule out concomitant spinal stenosis or peripheral neuropathy, which can frequently masquerade as or coexist with hip osteoarthritis. Motor function is grossly intact, graded at 5/5 for dorsiflexion (DF), plantarflexion (PF), extensor hallucis longus (EHL), and flexor hallucis longus (FHL). Sensation is intact to light touch in all major dermatomal distributions (L2-S1). Vascular examination reveals palpable, symmetric, and robust 2+ dorsalis pedis (DP) and posterior tibial (PT) pulses bilaterally, with brisk capillary refill, indicating adequate distal perfusion.
Advanced Imaging and Diagnostics
Radiographic Evaluation of the Hip
Standardized radiographic evaluation is the cornerstone of diagnosing and templating for total hip arthroplasty. A complete hip series was obtained, including a weight-bearing anteroposterior (AP) view of the pelvis, an AP view of the right hip, and a lateral view of the right hip.
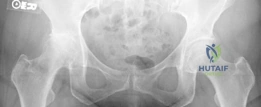
The preoperative AP radiograph of the pelvis demonstrates end-stage, Kellgren-Lawrence Grade IV osteoarthritis of the right hip. There is complete obliteration of the superior and axial articular joint space, indicating full-thickness chondral loss.
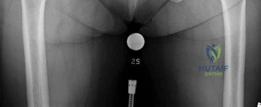
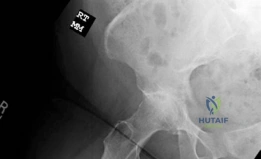
Focusing on the AP view of the right hip, profound subchondral sclerosis is visible on both the acetabular and femoral sides, representing Wolff's law in action as the bone hypertrophies in response to abnormal, unbuffered mechanical stress. Large, marginal osteophytes are present at the lateral acetabular rim and the femoral head-neck junction, contributing to the patient's mechanical block to motion. Subchondral cystic changes (geodes) are also noted within the acetabular roof, resulting from the intrusion of pressurized synovial fluid through microfractures in the denuded subchondral bone plate.

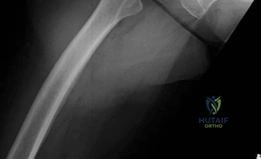
The preoperative lateral radiographs confirm the extensive circumferential nature of the osteophytic rim and the posterior loss of joint space. The femoral head has lost its normal spherical geometry, taking on a flattened, "mushroom" appearance due to the advanced degenerative remodeling. The proximal femoral diaphysis appears to have a robust cortical thickness, consistent with a Dorr Type A or B bone morphology, which is highly favorable for an uncemented, diaphyseal-engaging femoral stem.
Preoperative Templating and Biomechanical Considerations
Preoperative templating is a non-negotiable step in modern arthroplasty to predict component sizing, restore the anatomic center of rotation, optimize femoral offset, and equalize leg lengths.

Digital templating was performed on the AP pelvis radiograph. The horizontal line of Köhler (ilioischial line) and the radiographic teardrop were utilized to determine the true floor of the acetabulum. The goal is to medialize the acetabular component to the teardrop to decrease the body weight moment arm, while simultaneously restoring the femoral offset to optimize the abductor moment arm. Based on the templating, an extensively porous-coated, cylindrical Anatomic Medullary Locking (AML) stem was selected. The AML stem relies on a tight "scratch fit" at the femoral isthmus for initial mechanical stability, requiring precise cylindrical reaming of the diaphysis.
Exhaustive Differential Diagnosis
While the clinical and radiographic picture overwhelmingly points to primary osteoarthritis, a rigorous orthopedic surgeon must always consider and systematically exclude other pathologies that can present with groin pain and functional limitation.
Diagnostic Matrix for Adult Hip Pain
| Diagnostic Entity | Primary Clinical Presentation | Key Radiographic/Imaging Findings | Pathophysiological Mechanism |
|---|---|---|---|
| Primary Osteoarthritis (Current Diagnosis) | Insidious onset groin pain, worse with weight-bearing, profound loss of IR and flexion. | Joint space narrowing, subchondral sclerosis, osteophytes, subchondral cysts. | Mechanical wear and tear leading to progressive articular cartilage degradation and reactive bone formation. |
| Avascular Necrosis (AVN) / Osteonecrosis | Groin pain, often with a history of steroid use, alcohol abuse, or trauma. Pain may be present at rest. | Crescent sign (subchondral collapse), patchy sclerosis/lucency. MRI is highly sensitive (double-line sign). | Interruption of the vascular supply to the femoral head leading to osteocyte death and subsequent structural collapse. |
| Lumbar Radiculopathy (L2-L3) | Groin/anterior thigh pain, often radiating below the knee. Positive straight leg raise. | Degenerative disc disease, foraminal stenosis on MRI. Hip radiographs may be normal. | Mechanical compression or chemical irritation of the upper lumbar nerve roots. |
| Femoroacetabular Impingement (FAI) | Groin pain in younger patients, sharp pain with pivoting or deep flexion. Positive FADIR test. | Cam lesion (alpha angle >55°), Pincer lesion (coxa profunda, retroversion), crossover sign. | Abnormal morphological contact between the proximal femur and acetabular rim leading to labral tears and early chondral damage. |
Rationale for Excluding Mimickers
In this patient, the diagnosis of AVN is less likely given the lack of typical risk factors (no chronic corticosteroid use, no profound alcohol abuse) and the radiographic presence of widespread joint space loss and osteophytosis rather than isolated focal collapse of the femoral head. Lumbar radiculopathy is excluded by the entirely normal neurovascular examination, the absence of radicular symptoms extending below the knee, and the profound restriction in passive hip range of motion, which points directly to the joint capsule and articulation. FAI is typically a disease of the younger, more active demographic, and while this patient may have had asymptomatic impingement morphology in her youth, she has now progressed to end-stage degenerative joint disease.
Complex Surgical Decision Making and Classifications
Implant Selection and the AML Stem Rationale
The decision to proceed with an uncemented, extensively porous-coated Anatomic Medullary Locking (AML) stem represents a specific philosophical approach to femoral fixation. The AML stem is manufactured from a cobalt-chromium (CoCr) alloy, which possesses a high modulus of elasticity (stiffness). The stem is entirely coated with sintered CoCr beads, creating a porous surface with pore sizes ranging from 50 to 400 micrometers—the optimal dimension for osteoprogenitor cells to migrate and deposit woven bone, which eventually remodels into lamellar bone (osteointegration).
The rationale for utilizing an extensively coated stem in this 61-year-old patient is to achieve rigid, long-term biologic fixation in the diaphysis. This is particularly useful when the metaphyseal bone quality is questionable, although in this patient's case, her Dorr A/B morphology provides excellent bone stock throughout. The cylindrical geometry of the AML stem requires the femoral diaphysis to be reamed to a perfect cylinder. The stem is then driven into the canal, achieving an interference fit (scratch fit) over a distance of at least 1.5 to 2.0 inches within the isthmus.
Fixation Principles in Uncemented Arthroplasty
For successful uncemented fixation, two absolute prerequisites must be met:
1. Initial Mechanical Stability: The micromotion between the implant and the host bone must be kept strictly below 50 to 150 micrometers. Excessive micromotion leads to the formation of a fibrous tissue interface rather than true osseous integration, ultimately resulting in aseptic loosening and clinical failure. The AML stem achieves this via the aggressive diaphyseal scratch fit.
2. Biologic Environment: The host bone must be viable, and the implant surface must be osteoconductive. The sintered bead coating of the AML stem provides a highly textured, three-dimensional scaffold for bone ingrowth.
One of the known biomechanical trade-offs of the extensively porous-coated CoCr stem is "stress shielding." Because the stiff CoCr stem is rigidly fixed distally in the diaphysis, the load of body weight bypasses the proximal femur (calcar region). According to Wolff's law, this lack of mechanical stress leads to proximal bone resorption over time. While radiographically alarming, this proximal stress shielding is rarely clinically symptomatic if the distal diaphyseal fixation remains robust.
Step-by-Step Surgical Technique and Intervention
Patient Positioning and Surgical Approach
The patient was brought to the operating theater, and following the induction of general endotracheal anesthesia, she was positioned in the lateral decubitus position on a rigid peg board. Meticulous padding of all bony prominences, including the dependent axilla and peroneal nerve, was verified. A standard posterior (Moore/Southern) approach to the hip was utilized.
An incision was made centered over the greater trochanter, extending proximally in line with the gluteus maximus fibers and distally along the femoral shaft. The fascia lata was incised, and the gluteus maximus was bluntly split in line with its fibers. The short external rotators (piriformis, superior gemellus, obturator internus, inferior gemellus) and the quadratus femoris were identified, tagged with heavy non-absorbable suture, and released from their insertion on the greater trochanter to expose the posterior capsule. A T-shaped capsulotomy was performed, and the hip was gently dislocated via internal rotation and flexion.
Acetabular Preparation and Component Implantation
The femoral neck was osteotomized using an oscillating saw based on the preoperative templating measurements, typically 1 to 1.5 cm proximal to the lesser trochanter. The acetabulum was then exposed using sequential retractor placement. The labrum and prominent osteophytes were excised to identify the true bony margins of the acetabulum, including the transverse acetabular ligament, which serves as a critical landmark for version.
Sequential hemispherical reaming was performed, starting with a small reamer to medialize down to the radiographic teardrop (cotyloid fossa), followed by progressively larger reamers to achieve a hemispherical construct. The subchondral bone was preserved to provide rigid support for the uncemented cup. A highly porous titanium multi-hole acetabular shell was impacted into place with a target orientation of 40-45° of abduction and 15-20° of anteversion. Excellent initial press-fit stability was achieved, and two supplementary cancellous screws were placed into the posterosuperior quadrant (the "safe zone") to augment fixation. A highly cross-linked polyethylene liner was then impacted into the shell.
Femoral Preparation and Diaphyseal Fixation
Attention was then turned to the femur. The proximal femur was elevated and the canal was opened with a box osteotome. Sequential cylindrical reaming of the diaphysis was performed. This is the most critical step when utilizing an AML stem. The surgeon must ream precisely to the planned diameter; under-reaming risks an intraoperative catastrophic longitudinal fracture of the femoral shaft during stem impaction, while over-reaming compromises the scratch fit, leading to subsidence and failure of ingrowth.
Once the diaphysis was appropriately prepared, the metaphyseal region was broached to accommodate the proximal geometry of the stem. The definitive extensively porous-coated AML stem was then introduced and impacted. The surgeon noted the characteristic change in pitch (the "ping") as the stem seated and achieved its rigid diaphyseal interference fit. Trial heads and necks were utilized to assess leg length, offset, and stability. The hip was taken through a full range of motion, demonstrating no impingement and excellent stability in the extremes of flexion/internal rotation and extension/external rotation. The definitive CoCr femoral head was impacted onto the trunnion.
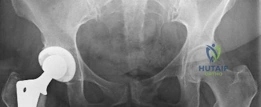
The intraoperative and immediate postoperative AP radiograph demonstrates excellent alignment of the components. The acetabular cup is appropriately inclined, and the AML stem is centered within the femoral canal, demonstrating a tight diaphyseal fit without evidence of cortical fracture.
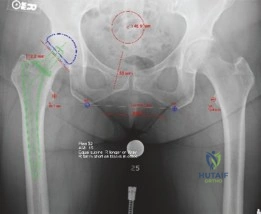
The postoperative lateral radiograph confirms appropriate version of the acetabular component and central placement of the femoral stem within the medullary canal. The robust porous coating is visible engaging the diaphyseal cortices.
Strict Post-Operative Protocol and Rehabilitation Stages
Immediate Post-Operative Management
Given the patient's complex medical history, specifically her prior myocardial infarction, she was admitted to the surgical telemetry unit for continuous cardiac monitoring. Postoperative hemoglobin and hematocrit were closely monitored, and her fluid status was meticulously managed to avoid fluid overload and secondary heart failure.
For venous thromboembolism (VTE) prophylaxis, a multidisciplinary discussion with her cardiologist dictated a tailored approach. Given her CAD, she was placed on a regimen of aspirin 81 mg twice daily for 4 weeks, combined with mechanical sequential compression devices (SCDs) and early mobilization.
Pain management utilized a multimodal, opioid-sparing protocol. This included scheduled oral acetaminophen, a short course of selective NSAIDs (weighing the cardiovascular risks), and gabapentin to address neuropathic pain pathways. Intravenous opioids were strictly reserved for severe breakthrough pain to minimize the risk of respiratory depression and postoperative delirium.
Progressive Weight-Bearing and Functional Milestones
Despite the use of an uncemented stem, modern arthroplasty principles dictate that if rigid initial fixation is achieved intraoperatively, the patient is allowed weight-bearing as tolerated (WBAT) immediately on postoperative day zero.
Physical therapy was initiated within hours of surgery. The patient was educated on strict posterior hip precautions for the first 6 weeks to prevent posterior dislocation:
1. No hip flexion past 90 degrees.
2. No internal rotation of the operative leg.
3. No adduction of the operative leg past the midline.
By postoperative day 2, the patient was successfully clearing physical therapy milestones, including independent transfers, ambulation of over 150 feet with a standard walker, and the ability to navigate a standard flight of stairs. She was subsequently discharged to her home with home health physical therapy.
High-Yield Clinical Pearls and Pitfalls
Pearls for Extensively Porous-Coated Stems
- The Concept of "Spot Welds": Over the first 6 to 12 months postoperatively, successful osteointegration of an extensively porous-coated stem can be visualized radiographically by the formation of "spot welds"—areas of dense endosteal bone bridging directly to the porous coating, typically seen at the distal extent of the porous coating.
- Diaphyseal Engagement: The AML stem's success is entirely dependent on diaphyseal engagement. The surgeon must ensure at least 4 to 5 cm of intimate contact between the cylindrical stem and the cortical bone of the isthmus.
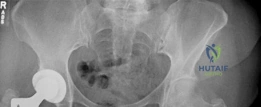
This follow-up radiograph demonstrates the classic appearance of an extensively porous-coated stem that has achieved biologic fixation. Notice the absence of radiolucent lines around the diaphyseal portion of the stem, indicating a lack of fibrous tissue interposition.
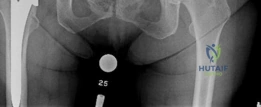
A closer, magnified view of the distal stem highlights the subtle endosteal condensation and "spot weld" formation at the transition zone of the porous coating, confirming rigid, long-term biologic integration.
Pitfalls and Complication Avoidance
- Intraoperative Fracture: The most feared complication during the insertion of a cylindrical, extensively coated stem is an intraoperative longitudinal fracture of the proximal femur or diaphysis. This occurs due to the massive hoop stresses generated during impaction if the canal is under-reamed. Prophylactic cerclage cabling of the proximal femur prior to stem impaction is a widely utilized technique to mitigate this risk, especially in Dorr Type A bone.
- Thigh Pain: A classic complication specific to stiff (CoCr), diaphyseal-engaging stems is anterior thigh pain. This is caused by a modulus mismatch between the ultra-stiff metal stem and the relatively elastic host bone. The rigid stem transfers stress preferentially to the distal tip, causing localized micro-motion and pain during weight-bearing. While this often resolves over 1-2 years as the bone remodels, it can be a significant source of patient dissatisfaction. Modern stem designs have largely shifted towards tapered titanium wedges to reduce this modulus mismatch and eliminate thigh pain.
- Stress Shielding: As previously discussed, the rigid distal fixation deprives the proximal femur of mechanical loading. Over a decade, this can lead to severe proximal bone resorption (calcar round-off). If revision surgery ever becomes necessary for infection or wear, the lack of proximal bone stock makes the revision procedure exponentially more complex.
