The Painful Total Hip Arthroplasty: Etiology, Anatomy, Biomechanics, and Management
Key Takeaway
A painful total hip arthroplasty demands a systematic evaluation, differentiating mechanical failure, infection (PJI), biological reactions, and anatomical issues. Causes include aseptic loosening, component malposition, leg length discrepancy, abductor dysfunction, and nerve impingement. Thorough understanding of anatomy and biomechanics is critical for diagnosis and effective management in orthopedic practice.
Introduction and Epidemiology
Total hip arthroplasty represents one of the most successful surgical interventions in orthopedic surgery, profoundly improving quality of life and restoring biomechanical function for millions of patients globally. With increasing surgical volume and an aging demographic, the prevalence of both primary and revision total hip arthroplasty continues to rise exponentially. While the vast majority of patients experience excellent long term outcomes, a significant subset develops persistent or new onset pain following the index procedure, necessitating a comprehensive understanding of its etiology, diagnostic workup, and management. A painful total hip arthroplasty is a complex diagnostic and therapeutic challenge, demanding a systematic algorithmic approach to differentiate mechanical failure from biological reactions, periprosthetic joint infection, or extrinsic referred pathology. This comprehensive review outlines the intrinsic and extrinsic causes of the painful total hip arthroplasty and provides a structured framework for clinical evaluation and surgical management, targeting orthopedic surgeons and trainees.
Epidemiologically, patient satisfaction rates following primary total hip arthroplasty are exceptionally high, frequently exceeding 90 percent in long term registries. However, approximately 10 to 20 percent of patients report some degree of dissatisfaction or persistent pain postoperatively. The incidence of revision total hip arthroplasty is projected to increase substantially over the next decade. Aseptic loosening, periprosthetic joint infection, instability, and periprosthetic fractures remain the leading indications for revision burden. Furthermore, the recognition of adverse local tissue reactions secondary to mechanically assisted crevice corrosion and trunnionosis has added a layer of complexity to the epidemiological landscape of the painful hip. Understanding the precise underlying etiology is paramount to successful surgical salvage, as empirical revision without a definitive diagnosis is associated with unacceptably high failure rates.
Surgical Anatomy and Biomechanics
A thorough understanding of the pertinent surgical anatomy and biomechanics is fundamental to both primary total hip arthroplasty success and the differential diagnosis of a painful hip. Failure to restore native biomechanics frequently manifests as persistent pain and functional deficit.
Bony Anatomy
The acetabulum is a hemispherical socket providing articulation for the femoral head. Proper reaming and component placement are critical for stability and avoiding impingement. The target safe zone typically dictates an inclination of 40 to 45 degrees and anteversion of 15 to 20 degrees. Deviations from this safe zone can lead to edge loading, accelerated polyethylene wear, and component instability. The femoral canal accepts the prosthetic stem, and the proximal femur dictates offset and leg length. Calcar preservation and appropriate stem sizing are crucial to prevent subsidence and proximal stress shielding, which can manifest as thigh pain.
Muscular Anatomy
The abductor complex, comprising the gluteus medius and minimus, is paramount for coronal plane pelvic stability during the stance phase of gait. Injury, avulsion, or dysfunction secondary to fatty atrophy can lead to a Trendelenburg gait and debilitating lateral hip pain. The superior gluteal nerve innervates these muscles and is highly vulnerable during posterior or direct lateral surgical approaches. The adductor group contributes to medial stability. Iliopsoas impingement on an anteriorly prominent or under anteverted acetabular component is a well documented cause of anterior groin pain, particularly during active hip flexion. The external rotators, including the piriformis and obturator internus, are critical landmarks and dynamic stabilizers.
Neurovascular Anatomy
The sciatic nerve is the most vulnerable neural structure in posterior approaches, typically lying deep to the short external rotators. It is at risk of indirect stretch injury, particularly during significant leg lengthening, or direct iatrogenic trauma. The femoral nerve is vulnerable anteriorly, particularly with aggressive retractor placement over the anterior acetabular rim. The lateral femoral cutaneous nerve possesses a highly variable anatomical course and is prone to injury with direct anterior approaches, leading to meralgia paresthetica. Vascular structures, including the external iliac and femoral vessels anteriorly, and the superior and inferior gluteal arteries posterolaterally, dictate safe zones for acetabular screw placement.
Biomechanical Principles

Leg length discrepancy can lead to severe gait abnormalities, compensatory lumbar radiculopathy, and nerve stretch injuries. Restoration of femoral offset is equally critical; insufficient offset decreases the abductor lever arm, exponentially increasing the joint reaction force required to maintain a level pelvis. This increased joint reaction force accelerates bearing surface wear and causes abductor fatigue, presenting clinically as trochanteric pain. Conversely, excessive offset can lead to trochanteric bursitis and increased stress transfer to the femoral stem interface. The center of rotation must be restored to its native anatomical position. Superior and lateral displacement of the center of rotation increases the body weight lever arm, thereby increasing the joint reaction force and the risk of aseptic loosening.
Indications and Contraindications
The management of a painful total hip arthroplasty hinges on identifying a definitive etiology. Surgical intervention is indicated when a clear, addressable intrinsic mechanical or biological failure is identified. Revision surgery in the absence of a clear diagnosis is strongly contraindicated.
| Indication Category | Operative Indications for Revision | Non Operative Indications and Observation |
|---|---|---|
| Infectious | Acute or chronic periprosthetic joint infection meeting diagnostic criteria | Superficial incisional infection without deep joint involvement |
| Mechanical | Aseptic loosening with progressive radiolucency or component subsidence | Stable, asymptomatic radiolucencies in isolated Gruen zones |
| Biological | Severe adverse local tissue reaction with pseudotumor or abductor necrosis | Mild, asymptomatic trunnionosis without soft tissue compromise |
| Instability | Recurrent dislocation secondary to component malposition or soft tissue failure | Single index dislocation with identifiable and avoidable provoking mechanism |
| Impingement | Refractory iliopsoas impingement on a prominent acetabular shell | Mild anterior groin pain resolving with targeted physical therapy |
| Extrinsic | None | Lumbar radiculopathy, spinal stenosis, vascular claudication |
| Periprosthetic | Vancouver B2, B3, and C periprosthetic femoral fractures | Stable Vancouver A or B1 fractures amenable to protected weight bearing |
Contraindications to surgical revision include extreme medical comorbidities precluding safe anesthesia, active systemic bacteremia (until cleared), and the absence of a definitive diagnosis for the pain. Extrinsic causes of pain, such as lumbar spine pathology, greater trochanteric pain syndrome, and complex regional pain syndrome, must be ruled out and managed non operatively or by the appropriate subspecialist.
Pre Operative Planning and Patient Positioning
Thorough preoperative planning is the cornerstone of successful management for the painful total hip arthroplasty. The diagnostic algorithm must be exhaustive, moving from non invasive to invasive modalities.
Diagnostic Algorithm for the Painful Hip
The initial evaluation begins with a detailed history, focusing on the onset, character, and location of the pain. Start up pain radiating to the groin is highly suggestive of aseptic loosening of the femoral or acetabular component. Pain that is constant, nocturnal, or present since the index operation raises a high index of suspicion for periprosthetic joint infection.
Serological evaluation is mandatory for every painful arthroplasty. Erythrocyte sedimentation rate and C reactive protein are the first line screening tools. If these inflammatory markers are elevated, or if clinical suspicion remains high despite normal values, an image guided joint aspiration is required. Synovial fluid must be sent for cell count with manual differential, aerobic and anaerobic cultures, and alpha defensin testing.
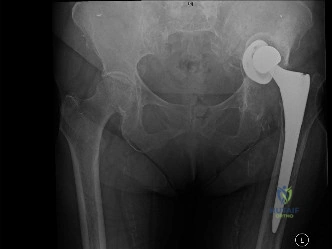
Radiographic evaluation includes a low anteroposterior pelvis, cross table lateral, and full length femur radiographs. Serial radiographs are invaluable for assessing progressive radiolucencies, osteolysis in DeLee and Charnley zones for the acetabulum, and Gruen zones for the femur. Component migration, subsidence, or pedestal formation at the distal stem tip indicate loss of fixation.
Advanced imaging is utilized when standard radiographs are equivocal. Computed tomography is excellent for evaluating osteolysis volume, component version, and occult periprosthetic fractures. Metal artifact reduction sequence magnetic resonance imaging is the gold standard for diagnosing adverse local tissue reactions, pseudotumors, and abductor tendon avulsions.
Templating and Bone Loss Classification
Once the etiology is identified and revision is indicated, precise preoperative templating is required. The surgeon must anticipate the need for component extraction and subsequent bone loss. Acetabular bone loss is typically classified using the Paprosky classification system, which evaluates the structural integrity of the superior dome, medial wall, and ischium to guide reconstruction options (e.g., hemispherical cups, augments, or custom triflange constructs). Femoral bone loss is similarly classified, dictating the choice between metaphyseal engaging stems, diaphyseal splined tapered stems, or tumor megaprostheses.
Patient Positioning and Room Setup
Patient positioning depends on the selected surgical approach and surgeon preference. The lateral decubitus position is most commonly utilized for revision hip arthroplasty, providing excellent access for the posterior approach and extended trochanteric osteotomy. The patient is secured using a pelvic positioner or peg board, ensuring the anterior superior iliac spines are perfectly vertical to allow for accurate intraoperative assessment of component version. The supine position on a radiolucent table may be preferred if an anterior approach is utilized, facilitating intraoperative fluoroscopy for component positioning and leg length assessment.
Detailed Surgical Approach and Technique
The surgical management of a painful total hip arthroplasty often necessitates complex revision techniques. The posterior approach is considered the workhorse for revision surgery due to its extensile nature and excellent visualization of both the femur and acetabulum.
The Extended Trochanteric Osteotomy
When addressing a well fixed femoral stem in the setting of infection, or when managing severe proximal femoral deformity, an extended trochanteric osteotomy is frequently required. This technique provides unparalleled exposure to the femoral diaphysis, facilitates safe cement and component extraction, and allows for direct correction of proximal femoral remodeling.
The technique involves measuring the anticipated length of the osteotomy, typically 12 to 15 centimeters distal to the tip of the greater trochanter, ensuring the osteotomy extends beyond the distal extent of the porous coating of the existing stem. Multiple drill holes are placed along the posterolateral femur to act as stress risers. An oscillating saw is used to connect the drill holes, completing the posterior and distal transverse cuts. Broad, flexible osteotomes are then carefully advanced from posterior to anterior, levering the anterolateral cortical fragment open like a book, maintaining the robust muscular attachments of the gluteus medius and vastus lateralis to preserve blood supply.
Component Extraction Strategies
Safe extraction of components without catastrophic bone loss is a critical skill. For the acetabulum, specialized explant systems utilizing hemispherical blades that match the outer diameter of the cup are employed to disrupt the bone implant interface. If screws are present, they must be meticulously removed; stripped screw heads may require the use of a high speed carbide burr.
Femoral stem extraction depends on the fixation method. Cementless stems with proximal porous coating can often be disrupted using flexible osteotomes passed along the implant bone interface. Fully porous coated stems or heavily integrated stems often necessitate an extended trochanteric osteotomy. Cemented stems require removal of the implant followed by meticulous extraction of the cement mantle using ultrasonic tools, segmented osteotomes, and specialized drills, under frequent fluoroscopic guidance to prevent cortical perforation.
Acetabular and Femoral Reconstruction
Following extraction and thorough debridement of all pseudotumors, metallosis, or infected tissue, reconstruction begins. Acetabular reconstruction aims to achieve rigid primary stability and restore the true center of rotation. In cases of massive uncontained defects, highly porous titanium augments or structural allografts are utilized in conjunction with a multi hole jumbo cup.
Femoral reconstruction in the revision setting frequently relies on modular, fluted, tapered titanium stems. These implants achieve diaphyseal fixation bypassing the compromised proximal metaphysis. The modularity allows for independent adjustment of leg length and version after the distal stem is rigidly fixed. The extended trochanteric osteotomy fragment is then reduced around the new stem and secured using multiple heavy duty cables.
Complications and Management
Revision total hip arthroplasty for a painful joint carries a significantly higher complication profile compared to primary arthroplasty. The altered anatomy, compromised soft tissue envelope, and prolonged operative times contribute to this elevated risk.
| Complication | Estimated Incidence | Prevention and Salvage Strategy |
|---|---|---|
| Intraoperative Fracture | 5 to 15 Percent | Prophylactic cabling prior to stem impaction. Bypass fractures with a stem extending two cortical diameters past the defect. |
| Recurrent Dislocation | 10 to 20 Percent | Utilize large diameter femoral heads, dual mobility constructs, or constrained liners in patients with profound abductor deficiency. |
| Periprosthetic Joint Infection | 3 to 8 Percent | Meticulous dead space management. Use of antibiotic loaded cement spacers in two stage revisions. Intravenous antibiotics based on intraoperative cultures. |
| Nerve Injury (Sciatic/Femoral) | 1 to 3 Percent | Careful retractor placement. Avoid excessive leg lengthening (limit to less than 2 to 3 centimeters). Immediate exploration if direct transection is suspected. |
| Subsidence of Femoral Stem | 2 to 5 Percent | Achieve rigid diaphyseal scratch fit. Utilize intraoperative fluoroscopy to confirm adequate cortical contact of fluted tapered stems. |
| Trochanteric Nonunion | 2 to 10 Percent | Meticulous handling of the extended trochanteric osteotomy fragment. Rigid fixation with multiple cables. Strict adherence to postoperative weight bearing restrictions. |
Management of these complications requires a high index of suspicion and prompt intervention. Recurrent instability may necessitate a return to the operating room for revision of modular components to adjust version, or the escalation of constraint to a dual mobility or fully constrained articulation. Intraoperative fractures recognized during the procedure must be addressed immediately with cerclage wiring, strut allografts, or bypass with a longer diaphyseal engaging stem.
Post Operative Rehabilitation Protocols
Rehabilitation following surgical management of a painful total hip arthroplasty is highly individualized, dictated by the complexity of the reconstruction, the quality of the host bone, and the specific surgical techniques employed.
In cases where an extended trochanteric osteotomy is performed, or massive structural allografts are utilized, patients are typically restricted to toe touch or flat foot weight bearing (approximately 20 pounds) on the operative extremity for six to eight weeks to prevent catastrophic subsidence and allow for osteotomy union. Active abduction is strictly prohibited during this initial phase to protect the trochanteric repair and the gluteus medius insertion.
Standard posterior dislocation precautions (avoiding hip flexion past 90 degrees, internal rotation, and adduction across the midline) are universally applied unless an anterior approach was utilized. Deep vein thrombosis prophylaxis is mandatory, utilizing pharmacological agents such as low molecular weight heparin, direct oral anticoagulants, or aspirin, stratified by the patient's individual risk profile and mobility status. Progression to full weight bearing and active resistance exercises is permitted only after radiographic evidence of component stability and osteotomy healing is confirmed at the six to eight week follow up interval.
Summary of Key Literature and Guidelines
The management of the painful total hip arthroplasty is heavily guided by established literature and consensus guidelines. The Musculoskeletal Infection Society criteria represent the gold standard for diagnosing periprosthetic joint infection, utilizing a combination of major criteria (sinus tract, identical organisms on multiple cultures) and minor criteria (elevated serum inflammatory markers, elevated synovial white blood cell count, positive alpha defensin).
The classification of bone loss is predicated on the foundational work of Paprosky, whose acetabular and femoral defect classifications dictate the reconstructive algorithm and predict the likelihood of achieving biological fixation. Furthermore, the management of adverse local tissue reactions relies on guidelines established by the American Association of Hip and Knee Surgeons, which emphasize the role of serial metal ion testing (cobalt and chromium) and metal artifact reduction sequence magnetic resonance imaging in asymptomatic and symptomatic patients with metal on metal or modular taper constructs.
The technique and outcomes of the extended trochanteric osteotomy are deeply rooted in the classic literature by Younger and colleagues, demonstrating its efficacy in achieving reliable component extraction and high rates of subsequent osteotomy union when performed with meticulous surgical technique. Mastery of this literature is essential for any orthopedic surgeon undertaking the complex task of evaluating and revising the painful total hip arthroplasty.
