Limb Reconstruction: Restoring Function for Challenges Near and Far
Key Takeaway
In this comprehensive guide, we discuss everything you need to know about Limb Reconstruction: Restoring Function for Challenges Near and Far. Limb reconstruction, rooted in Ilizarov's tension-stress effect, regenerates living tissue and bone through distraction osteogenesis. This involves precise, slow callus distraction (e.g., 1mm/day), requiring optimal stability, blood supply, and timing. Enhancing stability is crucial, utilizing methods like increasing wire tension, multiplanar half-pin placement, and employing near and far positions for external fixator rings.
Comprehensive Introduction and Patho-Epidemiology
The field of limb reconstruction represents one of the most profound intersections of biological potential and biomechanical engineering in orthopedic surgery. When subjected to slow, steady traction under the appropriate physiological and mechanical conditions, living tissue becomes metabolically activated and is able to regenerate. This foundational concept, known as the "tension-stress effect," was famously described by Professor Gavril Abramovich Ilizarov working in Kurgan, Western Siberia, in the early 1950s. His pioneering work fundamentally shifted the paradigm of how orthopedic surgeons approach complex deformities, bone loss, and limb length discrepancies. By harnessing the body's intrinsic capacity for intramembranous ossification under tension, Ilizarov developed highly successful techniques that remain the gold standard in modern reconstructive practice.

Distraction osteogenesis (DO) is the biological process that underpins limb lengthening and deformity correction. It is characterized by the mechanical induction of new bone formation between the surfaces of a surgically created osteotomy—more accurately termed a corticotomy, as the preservation of the medullary blood supply is paramount. The process is highly dependent on an intricate cascade of cellular events, driven by mechanotransduction. As tension is applied across the healing callus, mesenchymal stem cells are directed toward an osteogenic lineage rather than a chondrogenic one. This results in the direct formation of woven bone parallel to the vector of distraction. Concurrently, the tension-stress effect induces profound neoangiogenesis, driven by the upregulation of vascular endothelial growth factor (VEGF) and bone morphogenetic proteins (BMPs), ensuring the hyperemic environment necessary for massive tissue generation.

Epidemiologically, the demand for limb reconstruction spans a vast spectrum of pathology, from congenital anomalies to high-energy trauma sequelae. In the pediatric population, conditions such as fibular hemimelia, proximal focal femoral deficiency (PFFD), and congenital pseudarthrosis of the tibia present severe, progressive challenges that require multi-staged reconstructive strategies throughout the child's growth. In adults, the epidemiology shifts heavily toward post-traumatic conditions, including infected non-unions, malunions, and massive segmental bone defects resulting from open fractures or tumor resections. The global burden of road traffic accidents and high-velocity trauma ensures a steady influx of patients requiring complex limb salvage procedures, making mastery of these techniques an absolute necessity for the modern trauma and reconstructive surgeon.

The success of distraction osteogenesis relies on two non-negotiable pillars: absolute mechanical stability and the meticulous maintenance of the biological envelope (blood supply). If the fixation construct is excessively rigid, the mechanotransductive signaling fails, leading to delayed consolidation. Conversely, if the construct is too unstable, shear forces predominate, leading to fibrocartilage formation and ultimate non-union. Furthermore, the maximum safe distraction possible per anatomical segment is anecdotally and clinically recognized as approximately 20% of the original length of the bone being lengthened. Pushing beyond this physiological limit exponentially increases the risk of severe neurovascular compromise, joint subluxation, and devastating soft tissue contractures, reminding the surgeon that we are lengthening not just bone, but the entire functional limb unit.
Detailed Surgical Anatomy and Biomechanics
A profound, three-dimensional understanding of cross-sectional anatomy is the absolute prerequisite for the safe application of external fixators and the execution of complex osteotomies. The concept of "safe corridors" or "safe zones" dictates where transfixing wires and half-pins can be inserted without catastrophic injury to major neurovascular bundles. In the thigh, the safe zones are notoriously narrow due to the complex fascial compartments, the superficial femoral artery in Hunter’s canal, and the sciatic nerve posteriorly. Consequently, femoral external fixation often relies heavily on monolateral half-pin constructs or hybrid systems that utilize arches rather than full rings proximally, avoiding the medial neurovascular structures and allowing for patient comfort and perineal hygiene.


In the leg, the tibia provides a more forgiving anatomical landscape, but it is not without its traps. The common peroneal nerve winding around the fibular neck, the anterior tibial artery piercing the interosseous membrane, and the posterior tibial neurovascular bundle in the deep posterior compartment must be meticulously mapped in the surgeon's mind. Wire insertion must follow a strict protocol of drilling only through bone; soft tissues must be traversed by pushing the wire through with a mallet to avoid winding nerves or vessels around the spinning drill bit. Furthermore, the fibula must be addressed in any tibial lengthening or major deformity correction. Failure to stabilize the proximal and distal tibiofibular joints with transverse syndesmotic wires or screws will result in proximal migration of the fibular head (endangering the peroneal nerve) or distal migration of the lateral malleolus (destabilizing the ankle mortise).

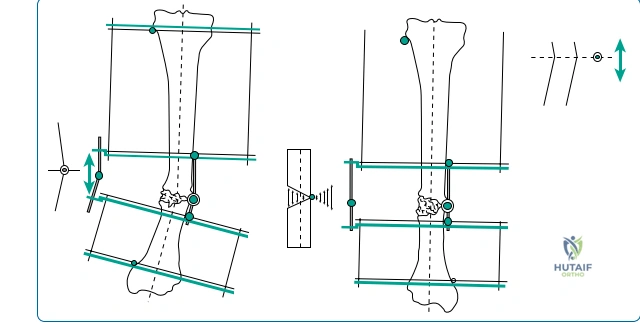
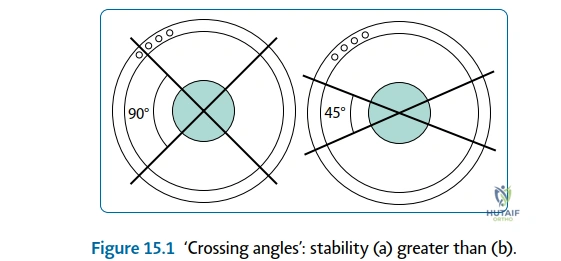
The biomechanics of the Ilizarov circular fixator represent a masterclass in structural engineering applied to human biology. The system derives its stability from the tensioning of small-diameter (typically 1.5 mm or 1.8 mm) smooth or olive wires across rigid rings. When tensioned to 90–130 kg, these wires exhibit a non-linear stiffness curve; they are compliant under low loads (providing the micromotion necessary to stimulate osteogenesis) but become highly rigid under high loads (preventing shear at the osteotomy site). The stability of the construct can be manipulated by altering the ring diameter (smaller rings are stiffer), the wire crossing angle (orthogonal 90-degree crossings provide maximum multi-planar stability), and the distance between the rings and the bone.

The advent of hexapod circular fixators, such as the Taylor Spatial Frame (TSF), introduced the principles of the Stewart-Gough platform to orthopedic surgery. These devices utilize six telescopic struts connecting two rings, allowing for simultaneous, multi-planar correction of angulation, translation, rotation, and length. Biomechanically, hexapod systems provide a highly stable, rigid construct that is exceptionally well-suited for complex, multi-apical deformities. However, the surgeon must understand that the biomechanical demands change as the treatment progresses. During the distraction phase, axial micromotion is beneficial. During the consolidation phase, the construct must be rigid enough to protect the nascent regenerate bone from bending moments until corticalization is radiographically confirmed in at least three out of four cortices.
Exhaustive Indications and Contraindications
The indications for limb reconstruction techniques are broad, encompassing almost every subspecialty of orthopedics, from pediatric orthopedics to orthopedic oncology. The decision to utilize external fixation (circular or monolateral) versus internal lengthening devices (intramedullary magnetic nails) depends heavily on the specific pathology, the quality of the soft tissue envelope, the presence of active infection, and the magnitude of the deformity.

In the realm of trauma, the Ilizarov method remains the undisputed champion for the management of infected non-unions and massive segmental bone defects. The technique of bone transport allows the surgeon to resect necrotic, infected bone back to bleeding, healthy margins (often creating defects of 5 to 15 centimeters) and subsequently transport a healthy intercalary segment to dock with the target site. This simultaneously eradicates the infection and restores limb length. In congenital deformities, limb reconstruction is indicated for severe length discrepancies (typically greater than 3-4 cm) that cannot be managed with shoe lifts or contralateral epiphysiodesis.
Despite the power of these techniques, there are absolute and relative contraindications that the prudent surgeon must respect. Poor patient compliance is perhaps the most critical relative contraindication. Limb reconstruction is a grueling psychological and physical marathon for the patient, requiring daily pin site care, multiple strut adjustments, and aggressive, painful physical therapy. A patient lacking the psychological resilience or social support to endure a 6-to-12-month treatment course will inevitably suffer catastrophic complications.


| Category | Indications | Contraindications |
|---|---|---|
| Trauma & Post-Trauma | Infected non-unions, segmental bone defects, malunions, complex periarticular fractures. | Active systemic sepsis, unsalvageable neurovascular injury (indication for amputation). |
| Congenital & Pediatric | PFFD, fibular hemimelia, radial clubhand, achondroplasia, Blount's disease. | Open physes (for intramedullary nails crossing the physis), severe metabolic bone disease (e.g., severe Osteogenesis Imperfecta). |
| Oncology & Infection | Post-tumor resection defects, chronic osteomyelitis requiring massive debridement. | Terminal prognosis with short life expectancy, active untreated malignancy at the osteotomy site. |
| Patient Factors | High motivation, good social support, realistic expectations. | Severe psychiatric illness, active substance abuse, non-compliance, severe peripheral vascular disease. |
Pre-Operative Planning, Templating, and Patient Positioning
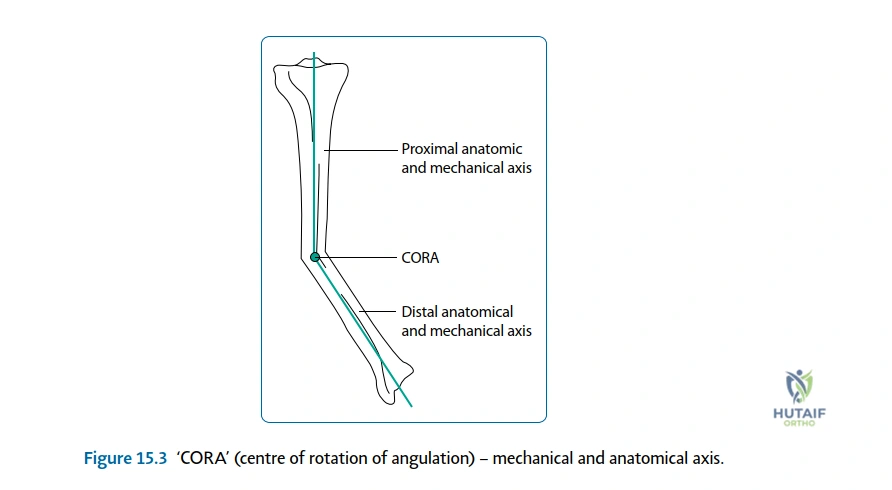
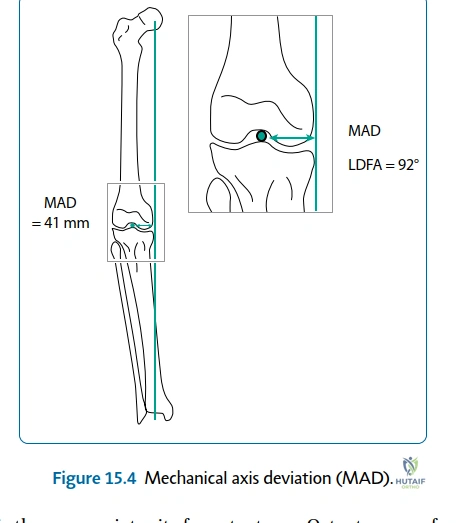
The success of any limb reconstruction procedure is dictated long before the patient enters the operating theater; it is won or lost in the meticulous pre-operative planning phase. Deformity analysis relies on the principles elucidated by Dror Paley, focusing on the Mechanical Axis Deviation (MAD) and the Center of Rotation of Angulation (CORA). Full-length, standing, weight-bearing radiographs of both lower extremities (from hip to ankle) are mandatory. The surgeon must systematically evaluate the joint orientation angles (e.g., mLDFA, MPTA, LDTA) to identify whether the deformity is femoral, tibial, or a combination of both.


Once the CORA is identified, the surgeon must apply the osteotomy rules. Rule 1 states that if the osteotomy and the mechanical hinge are placed at the CORA, the mechanical axis will realign without translation. Rule 2 states that if the osteotomy is placed away from the CORA, but the hinge remains at the CORA, the mechanical axis will realign, but a translation will occur at the osteotomy site. Rule 3 dictates that if both the osteotomy and the hinge are placed away from the CORA, a translation deformity will be induced. Understanding these geometric principles is essential for planning the level of the corticotomy, especially when dealing with periarticular deformities where placing the osteotomy exactly at the CORA might compromise fixation.

In the era of modern limb reconstruction, software-assisted planning has become the standard of care. Hexapod systems require the precise input of radiographic parameters (mounting parameters and deformity parameters) into proprietary web-based software to generate a customized strut-adjustment schedule. The surgeon must meticulously measure the AP and lateral translation, angulation, and axial rotation. Errors in inputting the "reference fragment" or the "mounting parameters" (the position of the reference ring relative to the bone) will result in a completely erroneous correction pathway, potentially worsening the deformity.

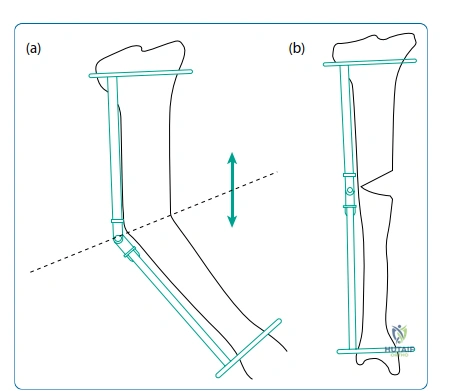
Patient positioning in the operating room must facilitate unobstructed fluoroscopic imaging in both the AP and lateral planes from the hip to the ankle. A radiolucent operative table is mandatory. For femoral lengthening or deformity correction, the patient is typically positioned supine with a bump under the ipsilateral hip to correct external rotation. The C-arm must be able to swing freely to obtain true orthogonal views without moving the limb, as maintaining the limb in a static, anatomical position is critical when applying the reference wires or determining the mechanical axis intra-operatively using the electrocautery cord technique.
Step-by-Step Surgical Approach and Fixation Technique
The surgical execution of limb reconstruction demands a synthesis of delicate tissue handling and robust biomechanical construction. The procedure generally begins with the application of the fixation device, whether it be an external circular frame or an internal lengthening nail. For external fixation, the application of the "reference wire" is the most critical step. This smooth 1.8 mm wire is driven parallel to the joint line (e.g., parallel to the tibial plateau for a proximal tibial frame). The reference ring is then mounted to this wire, establishing the anatomical baseline for the entire construct. Subsequent wires and half-pins are added to build the proximal and distal blocks, ensuring multi-planar stability. Hydroxyapatite-coated half-pins are strongly recommended to enhance osseointegration and reduce the incidence of pin loosening during prolonged treatments.


The creation of the corticotomy is a defining moment in the operation. Unlike a traditional osteotomy, a corticotomy aims to sever the rigid cortical bone while meticulously preserving the periosteal and endosteal blood supply. This is typically achieved through a minimally invasive approach. Multiple drill holes are made through the near cortex, traversing the medullary canal to breach the far cortex, using a 4.8 mm drill bit under fluoroscopic guidance. A sharp osteotome is then inserted, and a twist of the surgeon's wrist completes the fracture. The surgeon must audibly and tactilely confirm the completion of the corticotomy by rotating the proximal and distal segments; any residual cortical tethering will prevent distraction and lead to premature consolidation.


Innovation in limb lengthening has dramatically shifted toward fully implantable intramedullary lengthening nails (e.g., PRECICE, STRYDE). These devices utilize an internal magnetic motor driven by an external remote controller. The surgical technique for internal lengthening requires meticulous reaming of the medullary canal, often utilizing rigid reamers over a centrally placed guidewire to ensure the nail sits perfectly within the mechanical axis. Venting drill holes are placed at the planned osteotomy site prior to reaming to prevent fat embolism syndrome. Blocking screws (Poller screws) are frequently employed adjacent to the osteotomy to narrow the medullary canal and prevent the nail from translating or angulating within the metaphyseal bone, ensuring the bone lengthens strictly along the axis of the nail.



Following the corticotomy and fixation, regardless of the method used, the surgical sites are copiously irrigated. Skin tension around external fixator pins must be meticulously released with a scalpel to prevent necrosis, which is the primary nidus for pin site infections. The incisions are closed in a layered fashion. Intra-operative testing of the distraction mechanism is highly recommended. The surgeon should acutely distract the frame or nail by 1-2 mm to confirm that the osteotomy is completely free and that the mechanical components are functioning flawlessly before returning the bone ends to their resting apposition.
Complications, Incidence Rates, and Salvage Management
Limb reconstruction is a high-stakes endeavor, and the complication profile is extensive. Complications are so ubiquitous in this field that Paley famously categorized them not merely as complications, but as "problems" (requiring non-operative intervention), "obstacles" (requiring operative intervention but not affecting the final outcome), and true "complications" (affecting the final outcome). Pin site infection is the most common problem, occurring in up to 80% of patients undergoing external fixation. These are classified using the Checketts-MacKburney system. Grades 1-3 represent superficial soft tissue infections manageable with oral antibiotics and local care. Grades 4-6 involve deep bony infection or pin loosening, necessitating surgical removal of the pin, curettage of the tract, and replacement of the pin at a different site to maintain construct stability.


Joint contractures represent a severe obstacle, particularly during extensive lengthenings (greater than 5 cm). As the bone lengthens, the surrounding soft tissues—muscles, fascia, nerves, and vessels—must stretch. The muscles spanning two joints (e.g., the gastrocnemius, the rectus femoris) are particularly vulnerable. Equinus contracture of the ankle during tibial lengthening or knee flexion contracture during femoral lengthening can become permanent if not aggressively managed. Salvage management includes intensive physical therapy, dynamic splinting, botulinum toxin injections, and, if necessary, surgical release (e.g., percutaneous Achilles tendon lengthening or strayer procedure).

Regenerate failure is a catastrophic complication that can manifest as either premature consolidation or delayed/non-union. Premature consolidation occurs when the bone heals faster than it is being distracted, often due to a delay in initiating distraction, a distraction rate that is too slow, or an incomplete corticotomy. Salvage requires a return to the operating room for a re-corticotomy. Conversely, poor regenerate formation (hypotrophic callus) results from excessive instability, a distraction rate that is too fast, or compromised biology. Salvage management includes slowing the rate of distraction, implementing a "concertina" technique (alternating compression and distraction to stimulate the callus), or ultimately, bone grafting the defect.


| Complication Type | Incidence Rate | Prevention & Salvage Management |
|---|---|---|
| Pin Site Infection | 60% - 80% | Prevention: Meticulous skin release, daily chlorhexidine care. Salvage: Oral antibiotics, pin removal/exchange for deep sepsis. |
| Joint Contracture | 20% - 40% | Prevention: Aggressive daily PT, extending frames across joints. Salvage: Botulinum toxin, surgical soft tissue releases (TAL). |
| Premature Consolidation | 5% - 10% | Prevention: Ensure complete corticotomy intra-op, adhere to latency timing. Salvage: Surgical re-corticotomy. |
| Delayed Consolidation | 10% - 15% | Prevention: Preserve endosteal/periosteal blood supply, optimize frame stability. Salvage: Slow distraction rate, concertina technique, bone grafting. |
| Axial Deviation | 10% - 20% | Prevention: Use of blocking screws (internal), orthogonal wire placement (external). Salvage: Frame modification, acute correction via hexapod software. |
Phased Post-Operative Rehabilitation Protocols
The post-operative management of a limb reconstruction patient is as critical as the surgical execution. The process is divided into distinct, highly regulated phases: Latency, Distraction, Consolidation, and Remodeling. The Latency phase is the period immediately following surgery before distraction begins. This allows for the resolution of the acute inflammatory phase and the initiation of the soft callus formation. For metaphyseal corticotomies in healthy pediatric patients, latency is typically 5 days. In adults, or in diaphyseal bone with compromised blood supply, the latency period is extended to 7–10 days. Premature distraction will tear the fragile vascular buds, leading to non-union.
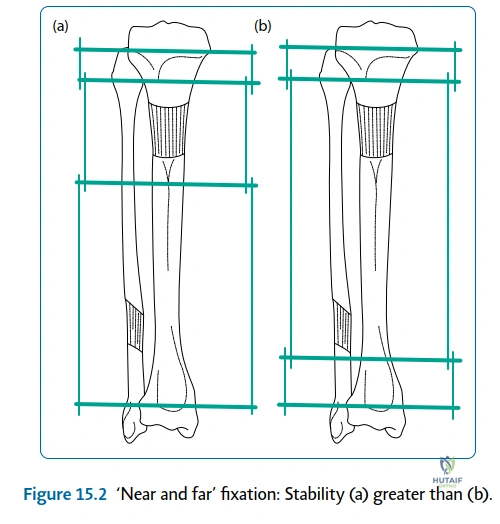
The Distraction phase is where the mechanical induction of bone occurs. The gold standard rate of distraction, as established by Ilizarov, is 1 mm per day. However, the rhythm of distraction is equally critical. Distracting 1 mm once a day is inferior to distracting 0.25 mm four times a day. High-frequency, small-increment distraction provides a smoother continuous tension curve, which is more favorable for angiogenesis and osteogenesis while causing less pain and soft tissue spasm. The surgeon must monitor the regenerate weekly with radiographs. If the regenerate appears hyperdense or is consolidating too quickly, the rate may be increased to 1.5 mm/day. If the regenerate is lucent or tapering (the "hourglass" sign), the rate must be slowed to 0.5 mm/day or temporarily halted.
Once the goal length or alignment is achieved, the Consolidation phase begins. The fixator or nail must remain in place to act as a load-sharing device while the woven bone of the regenerate remodels into mature, lamellar cortical bone. This phase is notoriously lengthy. A reliable heuristic is that consolidation takes approximately 30 to 40 days per centimeter of lengthening. During this time, progressive weight-bearing is strongly encouraged, as axial loading stimulates corticalization through Wolff's Law. Frame removal is only considered when plain radiographs demonstrate solid corticalization of at least three of the four cortices (anterior, posterior, medial, lateral) on orthogonal views.


Physical therapy is the cornerstone of the entire process. From post-operative day one, patients must engage in aggressive, active and active-assisted range of motion exercises for the joints above and below the osteotomy. Weight-bearing is dictated by the construct; circular frames typically allow immediate weight-bearing as tolerated, which is vital for bone healing. Internal magnetic nails have specific weight-bearing restrictions based on the diameter of the nail and the internal mechanism (e.g., early titanium nails required strict non-weight-bearing, while newer stainless steel iterations allow for partial loading). The rehabilitation team must remain vigilant for signs of nerve stretch injuries, particularly peroneal nerve palsy during tibial lengthening, which presents as a subtle loss of great toe extension before progressing to a full foot drop.
Summary of Landmark Literature and Clinical Guidelines
The academic foundation of limb reconstruction rests heavily on the voluminous, groundbreaking publications of G.A. Ilizarov in the late 1980s and early 1990s. His seminal papers in Clinical Orthopaedics and Related Research (CORR) elucidated the biological principles of tension-stress, the vital importance of preserving the medullary blood supply during corticotomy, and the optimal rate and rhythm of distraction. These principles remain virtually unchanged and form the absolute core guidelines for any surgeon attempting these procedures today.

Following Ilizarov, the work of Dror Paley revolutionized the geometric understanding of deformity correction. His textbook, Principles of Deformity Correction, introduced the concepts of MAD and CORA, shifting the field from an intuitive art to a precise mathematical science. Paley's osteotomy rules are now universally accepted clinical guidelines, ensuring that surgeons do not inadvertently create secondary translation deformities while attempting to correct angular ones. Furthermore, the integration of Stewart-Gough platform mathematics into hexapod fixators (pioneered by the Taylor brothers) represents a landmark leap in our ability to manage complex, multi-planar deformities simultaneously.
In recent years, the literature has heavily focused on the transition from external to internal lengthening devices. Systematic reviews and meta-analyses comparing circular frames to magnetic intramedullary nails (e.g., PRECICE) have consistently demonstrated that internal lengthening offers significantly lower rates of superficial infection, improved patient comfort, and faster recovery of joint range of motion. However, clinical guidelines still mandate the use of external fixation for cases involving active infection, massive bone defects requiring transport, or deformities too close to the joint line to accommodate an intramedullary device. The modern orthopedic surgeon must therefore remain fluent in both the historical techniques of Ilizarov and the cutting-edge innovations of internal magnetic lengthening, applying each judiciously to restore function to the most challenging of limbs.
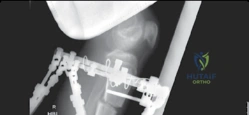
Clinical & Radiographic Imaging Archive









