Endoscopic Retrocalcaneal Decompression for Haglund Syndrome: A Masterclass
Key Takeaway
Join us for an immersive masterclass on endoscopic retrocalcaneal decompression for Haglund syndrome. We'll meticulously cover comprehensive surgical anatomy, precise patient positioning, and a granular, real-time breakdown of the intraoperative steps. Fellows will learn critical techniques for bony and soft tissue resection, managing potential pitfalls, and optimizing postoperative rehabilitation, ensuring excellent patient outcomes and a rapid return to activity.
Welcome, fellows, to the operating theater. Today, we are undertaking a masterclass on a common yet frequently debilitating condition: Haglund syndrome, classically characterized by the triad of retrocalcaneal bursitis, an enlarged posterosuperior calcaneal tuberosity, and frequently, insertional Achilles tendinopathy. While historically managed with extensive open exposures that mandated prolonged recovery and carried significant risks of wound breakdown, our modern approach will be entirely endoscopic. I favor this technique for its drastically reduced soft tissue morbidity, excellent cosmetic outcome, preservation of the Achilles tendon insertion, and expedited functional recovery. Let us begin our deep dive into the mastery of endoscopic retrocalcaneal decompression.
Comprehensive Introduction and Patho-Epidemiology
Before we make any incisions or establish our portals, a thorough understanding of the underlying pathology, historical context, and epidemiological factors is paramount for any orthopedic surgeon. Patrick Haglund first described the eponymous deformity in 1928, noting an enlarged posterior superior border of the os calcis in patients presenting with posterior heel pain. This bony prominence, universally referred to as a Haglund exostosis or "pump bump," serves as the primary mechanical irritant in this complex regional pain syndrome. However, to view Haglund syndrome merely as an osseous deformity is a gross oversimplification; it is a dynamic, multi-structural impingement syndrome.
The epidemiology of Haglund syndrome reveals a strong predilection for active individuals, particularly runners, and those who frequently wear footwear with rigid heel counters—hence the colloquial term "pump bump" associated with high-heeled shoes. It frequently presents in middle-aged adults, though elite athletes in their twenties and thirties are also commonly afflicted due to repetitive microtrauma. The pathogenesis is driven by a repetitive cycle of mechanical compression and friction. During the gait cycle, particularly in terminal stance and push-off where the ankle is driven into hyperdorsiflexion, the posterosuperior calcaneus rotates posteriorly and superiorly, compressing the retrocalcaneal bursa against the anterior fibers of the Achilles tendon.
Over time, this constant friction and impingement lead to a cascade of pathological changes. The retrocalcaneal bursa, normally a thin, friction-reducing synovial sac, becomes acutely inflamed, hypertrophied, and fibrotic. The continuous pressure against the anterior aspect of the Achilles tendon induces microvascular ischemia and mechanical wear, ultimately resulting in insertional Achilles tendinopathy. This tendinopathy is characterized histologically by mucoid degeneration, disorganized collagen architecture, microtears, and reactive neovascularization within the tendon substance.
The paradigm shift towards endoscopic management represents one of the most significant advancements in foot and ankle surgery over the last two decades. Open procedures, while effective at removing the bony prominence, often require partial or complete detachment of the Achilles tendon, necessitating complex reattachment with suture anchors and mandating a grueling, months-long postoperative immobilization period. The open approach is also fraught with wound healing complications due to the tenuous vascular supply of the posterior heel skin. Conversely, the endoscopic approach allows for a complete osseous and soft tissue decompression while leaving the Achilles tendon footprint entirely undisturbed, thereby minimizing surgical trauma and accelerating the biological timeline for rehabilitation.
Detailed Surgical Anatomy and Biomechanics
Osteology of the Posterior Calcaneus
The calcaneus is the largest of the tarsal bones, and its posterior tuberosity serves as the critical lever arm for the gastroc-soleus complex. The posterior surface of the calcaneus is divided into three distinct facets: superior, middle, and inferior. The Achilles tendon inserts primarily into the middle facet, while the inferior facet is continuous with the plantar fascia. The superior facet, which is normally smooth and slopes anteriorly, is the site of the Haglund deformity. In afflicted patients, this posterosuperior aspect develops an abnormal, hyperplastic prominence that projects directly into the retrocalcaneal space.
Biomechanically, the shape of the calcaneus dictates the degree of impingement. When the ankle dorsiflexes, the Achilles tendon is drawn tightly across the posterosuperior calcaneal angle. If this angle is excessively prominent, it acts as a fulcrum, increasing the tensile and compressive loads on the anterior tendon fibers. Radiographically, we attempt to quantify this prominence using several metrics. The Fowler-Philip angle, measured between the inferior surface of the calcaneus and the posterior surface, was historically considered abnormal if greater than 75 degrees. However, modern literature suggests that the parallel pitch lines—where the bony prominence extends above a line drawn parallel to the inferior calcaneal border—are a more reliable indicator of a pathological Haglund deformity.
Despite these radiographic measurements, it is critical to remember that Haglund syndrome is a clinical diagnosis. A patient may possess a radiographically prominent posterosuperior calcaneus yet remain entirely asymptomatic. Conversely, a patient with a relatively normal-appearing calcaneus on a lateral radiograph may experience severe impingement if their retrocalcaneal bursa is severely hypertrophied or if their specific biomechanics (e.g., rigid cavus foot) predispose them to hyperdorsiflexion impingement. Therefore, the surgeon must treat the patient's clinical impingement, not merely the radiographic angle.
Soft Tissue Envelope and the Achilles Complex
The Achilles tendon is the largest and strongest tendon in the human body, formed by the confluence of the gastrocnemius and soleus aponeuroses. As it descends towards its insertion, the tendon fibers rotate approximately 90 degrees, with the gastrocnemius fibers inserting laterally and the soleus fibers inserting medially. The insertion footprint on the middle facet of the calcaneal tuberosity is broad, crescent-shaped, and extends further distally than many junior surgeons realize. Understanding the exact boundaries of this footprint is crucial during endoscopic bone resection to avoid iatrogenic detachment.
Intimately associated with the tendon insertion is the retrocalcaneal bursa. This is a true, anatomically constant synovial bursa located between the anterior surface of the distal Achilles tendon and the posterosuperior surface of the calcaneus. Its physiological function is to provide a frictionless gliding mechanism during ankle range of motion. In Haglund syndrome, this bursa transforms from a microscopic fluid-filled sac into a thick, inflamed, and highly vascularized mass of hypertrophic tissue that obliterates the retrocalcaneal space and directly contributes to the patient's pain profile.
Anterior to the retrocalcaneal bursa lies Kager's fat pad, a triangular mass of adipose tissue bordered by the Achilles tendon posteriorly, the flexor hallucis longus anteriorly, and the calcaneus inferiorly. During our endoscopic approach, Kager's fat pad can frequently prolapse into our visual field. While a small amount of this fat pad may be debrided to improve visualization, aggressive resection should be avoided, as it plays a role in the vascular supply to the anterior Achilles tendon and contributes to the normal biomechanics of the posterior ankle.
Neurovascular Topography
As we plan our portal placement, maintaining a profound respect for the regional neurovascular anatomy is non-negotiable. The most critical structure at risk during retrocalcaneal endoscopy is the sural nerve. This nerve courses distally along the posterolateral aspect of the calf, piercing the deep fascia approximately 10 to 15 centimeters proximal to the calcaneal insertion. At the level of the ankle, it runs subcutaneously, intimately associated with the lateral border of the Achilles tendon, before curving anteriorly below the lateral malleolus.
Injury to the sural nerve—whether via direct transection, traction neuropraxia, or entrapment in portal scar tissue—can result in debilitating dysesthesia, painful neuroma formation, or bothersome numbness along the lateral aspect of the foot. To mitigate this risk, our lateral portal must be placed with extreme precision: slightly anterior to the palpable lateral border of the Achilles tendon, yet strictly posterior to the anticipated course of the sural nerve. Furthermore, all portal development must be performed using strictly blunt dissection techniques.
Also located in the posterolateral subcutaneous tissues is the lesser saphenous vein, which typically runs just superficial and slightly anterior to the sural nerve. While less critical than the nerve, transection of this vein can lead to troublesome postoperative hematoma and swelling. On the medial side of the ankle, the tibial nerve and the posterior tibial artery and vein are located deep to the flexor retinaculum within the tarsal tunnel. Fortunately, these major structures are located significantly anterior and deep to our operative field and are generally not at risk during standard retrocalcaneal bursoscopy, provided the surgeon maintains proper spatial orientation and does not stray aggressively anterior to Kager's triangle.
Exhaustive Indications and Contraindications
Patient selection is the absolute cornerstone of a successful surgical outcome. Surgery is strictly reserved for patients who present with chronic, debilitating posterior heel pain that has proven recalcitrant to a comprehensive, exhaustive course of nonoperative management. Clinically, these patients will demonstrate point tenderness directly over the retrocalcaneal bursa and the anterior aspect of the Achilles tendon insertion. The pain is reliably reproduced or exacerbated by passive forced dorsiflexion of the ankle, which mechanically recreates the impingement.
Nonoperative management must be exhausted before offering surgical intervention. This typically includes a minimum of three to six months of targeted therapies. Core conservative modalities include nonsteroidal anti-inflammatory medications (NSAIDs), rigorous shoe wear modification (transitioning to open-backed shoes or utilizing heel lifts to plantarflex the ankle and decrease Achilles tension), and structured physical therapy. Therapy should focus on eccentric loading of the gastroc-soleus complex, modalities such as extracorporeal shockwave therapy (ESWT), and aggressive stretching. I must emphasize a critical surgical warning: local injections of corticosteroids into the retrocalcaneal space, while potentially offering transient symptomatic relief, carry a profound risk of inducing necrosis within the Achilles tendon substance, predisposing it to catastrophic micro- or macro-rupture. We vehemently avoid them.
When conservative measures fail, endoscopic decompression is indicated for isolated Haglund deformity, retrocalcaneal bursitis, and mild to moderate insertional Achilles tendinopathy. However, if preoperative imaging or clinical examination reveals massive intratendinous calcifications, severe degenerative tearing involving more than 50% of the tendon's cross-sectional area, or frank avulsion of the tendon footprint, an endoscopic approach alone is insufficient. These complex cases mandate an open approach for formal tendon debridement, detachment, osseous resection, and subsequent robust reattachment using suture anchors, often augmented with a flexor hallucis longus (FHL) transfer.
| Category | Endoscopic Retrocalcaneal Decompression |
|---|---|
| Primary Indications | - Chronic retrocalcaneal bursitis failing >6 months of conservative care. - Symptomatic Haglund exostosis with clinical impingement. - Mild to moderate insertional Achilles tendinopathy (<25-30% tendon involvement). - "Pump bump" pain limiting daily activities or athletic participation. |
| Absolute Contraindications | - Active local or systemic infection. - Severe insertional Achilles tendinopathy requiring detachment and repair (involving >50% of the tendon). - Large, intratendinous calcific spurring requiring open excision. - Acute or chronic Achilles tendon rupture. |
| Relative Contraindications | - Significant peripheral vascular disease or severe neuropathy. - Previous extensive open surgery in the retrocalcaneal space (due to distorted anatomy and scarring). - Morbid obesity (complicating portal placement and postoperative rehabilitation). - Active smoking (significantly increases risk of delayed healing and non-union). |
Pre-Operative Planning, Templating, and Patient Positioning
Advanced Imaging Modalities
Thorough preoperative planning relies heavily on high-quality imaging to confirm the diagnosis, quantify the deformity, and critically assess the integrity of the Achilles tendon. Our initial evaluation always begins with plain radiography. A lateral, weight-bearing foot radiograph is indispensable. It clearly demonstrates the osseous morphology of the calcaneus, allowing us to identify the Haglund exostosis. We routinely evaluate the parallel pitch lines and the Fowler-Philip angle to objectify the prominence. Furthermore, plain films are crucial for identifying intratendinous calcifications or large dorsal calcaneal spurs extending into the tendon substance, which might alter our surgical plan from endoscopic to open.
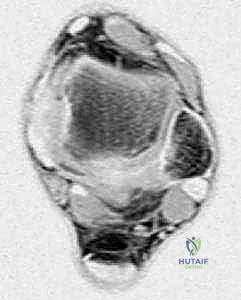
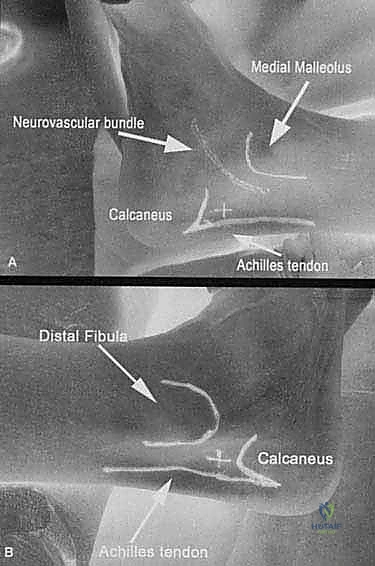
FIG 1 • A. Preoperative lateral foot film showing a prominent Haglund exostosis and obliteration of the retrocalcaneal recess.
While radiographs define the bone, Magnetic Resonance Imaging (MRI) is our gold standard for soft tissue evaluation and is mandatory before proceeding with endoscopic decompression. A non-contrast MRI beautifully delineates the presence of fluid within the retrocalcaneal bursa, confirming active bursitis. More importantly, it provides a high-resolution assessment of the Achilles tendon. We meticulously evaluate the sagittal and axial T2-weighted sequences for intratendinous signal changes, fusiform thickening, or partial tearing. If the MRI demonstrates that the insertional tendinopathy is severe, with degenerative changes encompassing a large portion of the tendon footprint, the patient is counseled that an open procedure with potential augmentation may be required.
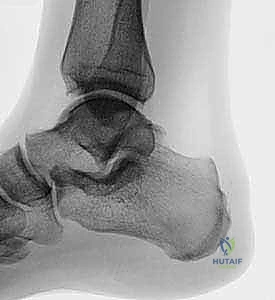
FIG 1 • B. Preoperative MRI demonstrating high T2 signal indicating severe retrocalcaneal bursitis and mild insertional tendinopathy, ideal for endoscopic intervention.
Anesthesia and Patient Positioning
For this procedure, we typically utilize general anesthesia or a robust regional block (such as a popliteal sciatic nerve block combined with a saphenous nerve block), depending on patient comorbidities and anesthesiologist preference. Today, we will execute this masterclass with the patient in the supine position. While some surgeons advocate for the prone position, the supine setup offers distinct advantages: it simplifies airway management for the anesthesia team, facilitates faster operating room turnover, and, most importantly, allows the surgeon to control the foot and ankle dynamically against their own torso.
Once anesthetized, a high thigh tourniquet is applied over generous padding. The operative limb is exsanguinated using an Esmarch bandage, and the tourniquet is inflated to 300 mmHg. A bloodless field is not a luxury in foot and ankle endoscopy; it is an absolute necessity. Even minor capillary bleeding can completely obscure the small retrocalcaneal working space.
The patient's foot is positioned at the very distal edge of the operating table. This specific placement allows me to stand at the foot of the bed and place the plantar aspect of the patient's foot against my abdomen or chest. This ergonomic setup provides incredibly stable control of the limb and frees both of my hands for simultaneous instrument manipulation. To facilitate portal access, the lower leg rests on a firm, padded cylindrical bump, approximately 12 inches long and 4 inches in diameter, placed just proximal to the Achilles insertion. This elevates the heel off the bed, providing ample clearance for the handles of the arthroscope and motorized instruments, and allows for unimpeded, controlled dorsiflexion and plantarflexion throughout the case. Finally, a mini C-arm fluoroscopy unit is draped and brought into the field, positioned to provide perfect lateral imaging of the calcaneus when required.
Step-by-Step Surgical Approach and Fixation Technique
Portal Placement and Safe Zones
Alright, fellows, let us scrub in. The limb has been prepped and draped in standard sterile fashion. The success of this operation hinges on the first five minutes: establishing precise, safe portals. We utilize a two-portal technique, creating a lateral and a medial portal flanking the Achilles tendon.
We begin laterally. Palpate the lateral border of the Achilles tendon and the superior aspect of the calcaneal tuberosity. The lateral portal is established at the level of the superior aspect of the calcaneus, just anterior to the Achilles tendon. Using a #15 blade, I make a precise, vertical skin incision no larger than 1 cm. A vertical orientation is critical; transverse incisions risk transecting the vertically oriented sural nerve.
Once the skin is incised, we immediately discard the scalpel. Take a small curved hemostat and begin blunt dissection through the subcutaneous adipose tissue. Spread, do not cut. Direct the tips of the hemostat medially and slightly anteriorly, aiming for the retrocalcaneal space. By spreading the tissues, we gently push the sural nerve and lesser saphenous vein out of harm's way. You will feel a distinct, tactile "pop" or loss of resistance as the hemostat breaches the thickened wall of the retrocalcaneal bursa. Once the path is established, introduce a blunt arthroscopic trocar into the space to further dilate the tract.
Remove the trocar and insert a 4.0-mm, 30-degree arthroscope through the lateral portal. Connect the inflow fluid (normal saline) and clear the initial debris. You will immediately see the inflamed, hypertrophic synovial tissue of the bursa. Now, to establish the medial portal, we utilize the transillumination technique. Dim the operating room lights and direct the arthroscope medially against the skin. The bright light will transilluminate the medial soft tissues, allowing you to identify an avascular safe zone, perfectly mirroring the lateral portal, just anterior to the medial border of the Achilles tendon. Make a vertical skin incision here, followed by the exact same meticulous blunt dissection with a hemostat until you visualize the tip of your clamp entering the arthroscopic field. Introduce a blunt trocar, and your working medial portal is established.
Endoscopic Debridement and Bursal Resection
With our portals established, the first objective is to clear the visual field. The retrocalcaneal space is typically filled with a dense, hypervascular mass of inflamed bursal tissue that obscures the bony anatomy. Introduce a 3.5-mm or 4.5-mm full-radius arthroscopic shaver through the medial portal.
Systematically resect all hypertrophied bursal tissue. I typically work from a posteromedial to posterolateral direction, utilizing the shaver on an oscillating setting. As you clear the bursa, the anatomy will begin to reveal itself. Superiorly, you will identify the yellowish, lobulated fat of Kager's triangle. Inferiorly, the hard, white surface of the posterosuperior calcaneal prominence will become visible. Posteriorly, the anterior fibers of the Achilles tendon will come into view. It is imperative to meticulously clean the anterior surface of the Achilles tendon to assess for any macroscopic fraying or partial tearing that may require debridement, but be extremely careful not to aggressively shave the tendon substance itself. We want a panoramic view of the entire retrocalcaneal space before commencing bone work.
Osseous Resection and Decompression
Once the soft tissue is cleared, we transition to the definitive osseous decompression. Remove the shaver and introduce a 4.0-mm or 4.5-mm hooded arthroscopic burr through the medial portal. The orientation of the burr hood is the most critical safety mechanism in this procedure. The open, cutting window of the burr must always face anteriorly, towards the calcaneus. The smooth, protective hood must always face posteriorly, resting against the anterior surface of the Achilles tendon. This protects the tendon from catastrophic iatrogenic injury.

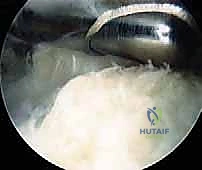
TECH FIG 2 • Intraoperative view demonstrating the arthroscopic burr resecting the posterosuperior calcaneal prominence. Note the hood protecting the posterior soft tissues.
Begin resecting the posterosuperior calcaneal prominence. I prefer a sweeping motion, moving the burr from medial to lateral across the width of the calcaneus. You will feel the burr bite into the cortical bone, revealing the softer cancellous bone beneath. The goal is not merely to flatten the prominence, but to create a smooth, gentle concavity that slopes away from the Achilles tendon.
You must carry the resection distally right up to the true footprint of the Achilles tendon insertion. This is often further distal than anticipated. Failure to resect adequately distal is the most common cause of persistent impingement. Similarly, you must ensure adequate decompression both medially and laterally, eliminating the entire width of the Haglund exostosis.

TECH FIG 3 • Arthroscopic view post-resection, showing a widened retrocalcaneal space and a completely decompressed anterior Achilles tendon.
Throughout the resection, dynamically test the ankle. By placing the patient's foot against my torso, I can passively drive the ankle into maximum dorsiflexion while visualizing the retrocalcaneal space endoscopically. If the anterior Achilles tendon still contacts the calcaneus during forced dorsiflexion, further bone resection is mandated.
Once visually satisfied, we bring in the mini C-arm. A perfect lateral fluoroscopic image is obtained to objectively confirm the adequacy of the resection. We are looking for the complete obliteration of the Fowler-Philip prominence and the establishment of a smooth, flat or slightly concave surface that parallels the anterior border of the Achilles tendon. Pay close attention to the medial and lateral borders on fluoroscopy to ensure no residual "dog ears" or sharp ridges of bone remain, which could act as new stress risers.

TECH FIG 4 • A. Intraoperative fluoroscopy confirming the start of the osseous resection.
TECH FIG 4 • B. Final intraoperative lateral fluoroscopic view demonstrating adequate, smooth resection of the Haglund deformity.
Once confirmed, thoroughly irrigate the retrocalcaneal space to remove all bone debris, which can cause severe postoperative pain and heterotopic ossification if left behind. Close the portals with simple interrupted non-absorbable sutures, and apply a sterile, bulky compressive dressing.
Complications, Incidence Rates, and Salvage Management
While endoscopic retrocalcaneal decompression boasts a significantly lower morbidity profile compared to open techniques, it is not without risk. A profound understanding of potential complications, their incidence, and salvage strategies is essential for the master surgeon. The most feared complications are neurological injury and iatrogenic tendon damage.
Sural nerve injury is the most common specific complication associated with this procedure, with literature reporting an incidence ranging from 2% to 7%. This typically occurs during the establishment of the lateral portal if sharp dissection is utilized or if the portal is placed too far posteriorly. Injury can range from transient neuropraxia due to traction, to complete transection resulting in a painful neuroma. Prevention via meticulous blunt dissection is paramount. If a symptomatic neuroma develops postoperatively, initial management includes desensitization therapy and gabapentinoids; recalcitrant cases may require surgical excision of the neuroma and burying the proximal nerve stump into deep muscle or bone.
Iatrogenic injury to the Achilles tendon is a catastrophic complication. This can occur if the burr is oriented incorrectly, allowing the cutting flutes to engage the tendon fibers, or if the surgeon aggressively resects
