Endoscopic Plantar Fasciotomy: A Masterclass in Minimally Invasive Heel Pain Relief
Key Takeaway
Master Endoscopic Plantar Fasciotomy (EPF) for chronic heel pain. This immersive guide details patient selection, precise anatomy, advanced surgical techniques, and critical pearls for optimal outcomes. Learn step-by-step execution, from incision to fascia release, emphasizing neurovascular protection and effective post-op rehabilitation for rapid recovery and lasting relief.
Comprehensive Introduction and Patho-Epidemiology
Endoscopic Plantar Fasciotomy (EPF) represents a paradigm shift in the surgical management of recalcitrant plantar heel pain. Since its inception, this minimally invasive technique has revolutionized the treatment algorithm for chronic plantar fasciitis, offering a sophisticated alternative to traditional open releases. Open procedures, while historically effective, are frequently fraught with prolonged recovery times, significant postoperative morbidity, painful scarring, and a higher propensity for wound healing complications. In stark contrast, EPF leverages advanced endoscopic visualization to achieve a highly selective, precise partial release of the plantar fascia. This masterclass chapter delineates the exhaustive preoperative, intraoperative, and postoperative protocols required to execute this procedure with uncompromising precision, ensuring optimal patient outcomes and rapid return to function.
To master the surgical intervention, one must first possess a profound understanding of the underlying patho-epidemiology. Plantar fasciitis is the most ubiquitous cause of inferior heel pain, affecting approximately 10% of the general population over their lifetime. It accounts for over one million patient visits annually in the United States alone. While the nomenclature implies a primary inflammatory process ("-itis"), rigorous histological analyses of surgical specimens have unequivocally demonstrated that the condition is more accurately classified as a "fasciosis." The pathology is characterized by a non-inflammatory, degenerative process involving myxoid degeneration, microtearing of the collagen matrix, angiofibroblastic proliferation, and subsequent necrosis at the fascial origin on the medial calcaneal tuberosity. This degenerative cascade is typically mechanically induced, resulting from repetitive microtrauma that overwhelms the tissue's intrinsic reparative capacity.
The clinical presentation is highly stereotyped, though diagnostic vigilance remains paramount. Patients classically describe an insidious onset of sharp, localized pain directly over the plantar medial calcaneal tuberosity. The pathognomonic symptom is "first-step" pain—excruciating discomfort upon initiating weight-bearing after a period of rest, particularly upon rising in the morning. This pain typically attenuates with initial ambulation as the fascia stretches, only to exacerbate following prolonged standing or intense physical exertion. Upon physical examination, palpable soft tissue swelling and exquisite point tenderness at the medial fascial insertion are invariably present. Dorsiflexion of the toes, which engages the windlass mechanism, often exacerbates the pain by increasing tension across the compromised fascial origin.
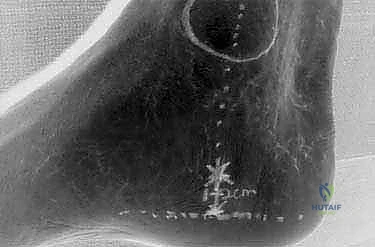
Diagnostic imaging serves to corroborate the clinical diagnosis and meticulously exclude confounding pathologies. Non-weight-bearing lateral radiographs are routinely obtained to rule out calcaneal stress fractures, unicameral bone cysts, giant cell tumors, or other occult osseous abnormalities. While plantar calcaneal osteophytes (spurs) are visualized in up to 50% of symptomatic patients, they are an incidental finding associated with the origin of the flexor digitorum brevis, not the plantar fascia itself, and are not the primary nociceptive source. High-resolution ultrasonography has emerged as the gold standard for initial imaging due to its cost-effectiveness and dynamic capabilities. A fascial thickness exceeding 4.0 to 4.5 mm, coupled with hypoechogenicity and loss of normal fibrillar architecture, is highly diagnostic. Magnetic Resonance Imaging (MRI) is reserved for atypical presentations, providing unparalleled soft-tissue contrast to evaluate for marrow edema, fascial ruptures, or deep soft-tissue neoplasms.
Detailed Surgical Anatomy and Biomechanics
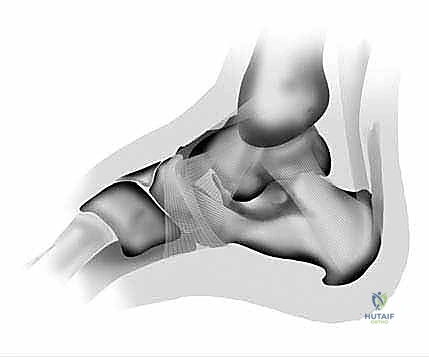
A masterful execution of an Endoscopic Plantar Fasciotomy demands an intimate, three-dimensional comprehension of the plantar foot's complex functional anatomy. The plantar fascia is a formidable, multilayered aponeurotic structure composed of dense, longitudinally oriented type I collagen fibers. It is anatomically partitioned into three distinct bands: the medial, central, and lateral bands. The central band is the thickest and most structurally significant, originating from the medial process of the calcaneal tuberosity. As it courses distally, it broadens and divides into five distinct slips that insert into the base of the proximal phalanges, the plantar plates, and the flexor tendon sheaths.
Biomechanically, the plantar fascia is the primary static stabilizer of the longitudinal arch. During the propulsive phase of the gait cycle, dorsiflexion of the metatarsophalangeal joints tightly winds the plantar fascia around the metatarsal heads. This action, famously described by Hicks as the "windlass mechanism," shortens the distance between the calcaneus and the metatarsals, elevating the medial longitudinal arch, inverting the hindfoot, and externally rotating the tibia. This transforms the foot into a rigid lever for efficient forward propulsion. The surgical objective of EPF is to selectively release only the medial one-third to one-half of the fascia (primarily the medial band and the medial aspect of the central band). Preserving the lateral structures is absolutely critical to maintaining the integrity of the lateral column and preventing catastrophic arch collapse or iatrogenic cuboid syndrome.
Navigating the neurovascular landscape of the plantar heel is the most treacherous aspect of this procedure. The surgical field is bordered by several critical "red zones" that must be meticulously respected. The medial plantar nerve and artery course deep and slightly medial to the abductor hallucis muscle; an overly aggressive medial or deep dissection risks catastrophic transection. Laterally, the lateral plantar nerve and its branches are vulnerable if the instrumentation strays beyond the fascial margins.
Of paramount importance is the first branch of the lateral plantar nerve, commonly known as Baxter's nerve. This nerve courses transversely between the deep fascia of the abductor hallucis and the medial aspect of the quadratus plantae muscle. Entrapment of Baxter's nerve can perfectly mimic recalcitrant plantar fasciitis and must be differentiated preoperatively. Furthermore, the flexor digitorum brevis (FDB) muscle lies immediately dorsal (deep) to the plantar fascia. During the endoscopic release, the visualization of the distinct, red muscle belly of the FDB serves as the definitive anatomical endpoint, confirming a complete fascial release while ensuring the surgeon has not violated the deeper neurovascular plane.
Exhaustive Indications and Contraindications
The decision to proceed with surgical intervention must be the culmination of a rigorous, algorithmic approach to patient management. Plantar fasciitis is inherently self-limiting in the vast majority of cases, with conservative modalities yielding a success rate exceeding 90%. Therefore, surgery is strictly reserved for a highly selected cohort of patients who have demonstrated true chronicity and refractoriness. A comprehensive understanding of the indications and contraindications is the foundation of surgical success and patient safety.
The absolute primary indication for Endoscopic Plantar Fasciotomy is recalcitrant plantar fasciitis that has unequivocally failed a structured, exhaustive regimen of conservative therapy for a minimum of 6 to 12 months. This conservative protocol must have included, at minimum: aggressive Achilles and plantar fascia specific stretching, formal physical therapy, nonsteroidal anti-inflammatory drugs (NSAIDs), custom orthotic management, night splinting, and judicious use of corticosteroid injections (limited to 2-3 maximum to avoid iatrogenic rupture). Additionally, advanced modalities such as Extracorporeal Shockwave Therapy (ESWT) or Platelet-Rich Plasma (PRP) injections should have been considered or attempted. The patient must exhibit severe, persistent pain that significantly impairs their activities of daily living and diminishes their overall quality of life.
Contraindications must be meticulously ruled out to prevent surgical failure and exacerbation of underlying pathology. A thorough differential diagnosis is crucial. Conditions such as tarsal tunnel syndrome, radiculopathy (L5-S1), calcaneal stress fractures, and systemic inflammatory arthropathies (e.g., Ankylosing Spondylitis, Rheumatoid Arthritis) must be excluded. Operating on a patient with undiagnosed Baxter's nerve entrapment without addressing the nerve compression will result in persistent postoperative pain. Furthermore, patients presenting with acute plantar fascia rupture are not candidates for EPF, as the structural integrity is already compromised, and further release will precipitate arch collapse.
Clinical Decision Matrix
| Category | Specific Criteria | Rationale |
|---|---|---|
| Absolute Indications | Failure of >6-12 months of structured conservative care | Ensures natural history of spontaneous resolution is respected |
| MRI or Ultrasound confirmed fascial thickening (>4.5mm) | Objective confirmation of degenerative fascial pathology | |
| Severe impairment of ADLs and Quality of Life | Justifies the inherent risks of surgical intervention | |
| Relative Indications | Failure of advanced modalities (ESWT, PRP) | Demonstrates absolute refractoriness of the tissue |
| Concomitant mild Achilles contracture | May require simultaneous gastrocnemius recession | |
| Absolute Contraindications | Active local or systemic infection | Risk of deep space plantar infection or osteomyelitis |
| Acute plantar fascia rupture | High risk of iatrogenic flatfoot deformity and lateral column overload | |
| Isolated Baxter's Nerve Entrapment | Requires targeted neurolysis, not fascial release | |
| Systemic inflammatory arthropathy (e.g., Reiter's, AS) | Pain is driven by systemic enthesopathy, not mechanical overload | |
| Relative Contraindications | Severe obesity (BMI > 40) | Increased risk of postoperative arch collapse and altered biomechanics |
| Pre-existing severe pes planus | Fascial release may further destabilize the medial column |
Pre-Operative Planning, Templating, and Patient Positioning
Meticulous preoperative planning and flawless operating room setup are non-negotiable prerequisites for a safe and efficient Endoscopic Plantar Fasciotomy. The procedure requires specialized instrumentation and a highly specific spatial orientation to navigate the constrained plantar anatomy safely. Prior to the day of surgery, the surgeon must review all imaging modalities, specifically noting the thickness of the fascia, the presence of any anatomical variants, and the exact location of the calcaneal spur, if present, to mentally template the trajectory of the endoscopic cannula.
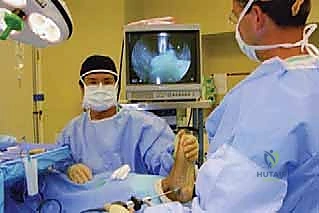
Patient positioning is critical for optimal access and visualization. The patient is placed in the supine position on the operating table. A small, firm bump is placed under the ipsilateral hip of the operative side. This slight elevation internally rotates the lower extremity, neutralizing the natural external rotation of the hip and bringing the medial aspect of the foot into a direct, perpendicular line of sight for the surgeon. The operative foot is then elevated and secured on a specialized foot prop or a well-padded Mayo stand. This elevation allows the surgeon to comfortably manipulate instruments from both the medial and lateral aspects of the foot simultaneously, maintaining a consistent, ergonomic posture throughout the case. A pneumatic tourniquet is applied to the distal calf or thigh, depending on surgeon preference, to ensure a completely bloodless field, which is critical for endoscopic visualization.
Anesthetic management is tailored to facilitate both intraoperative stability and postoperative comfort. While general anesthesia is a viable option, a regional approach utilizing a popliteal sciatic nerve block combined with intravenous monitored anesthesia care (MAC) is highly preferred. This provides profound intraoperative analgesia, promotes a bloodless field via sympathetic blockade, and offers extended postoperative pain control, allowing for early, comfortable mobilization. Standard perioperative antibiotic prophylaxis, typically 1 gram of intravenous cefazolin, is administered 30 minutes prior to tourniquet inflation to mitigate the risk of surgical site infection.
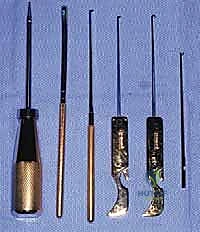
The instrumentation must be rigorously checked prior to incision. The standard EPF setup utilizes a specialized slotted cannula system, such as the Instratek Endotrac System. This system includes a blunt plantar fascia elevator, a slotted cannula, a conical obturator, and specialized disposable retrograde and antegrade cutting knives (hook and triangle configurations). A standard 4.0-mm, 30-degree short arthroscope is utilized. The 30-degree angle is crucial, as it allows the surgeon to rotate the light cord and peer "around the corner" to inspect the deep margins of the released fascia and verify the integrity of the lateral band. Additionally, sterile cotton-tipped applicators, slightly fluffed using a Bovie scratch pad, are essential for mechanically sweeping away the inevitable lobules of plantar fat that will herniate into the slotted cannula and obscure the visual field.
Step-by-Step Surgical Approach and Fixation Technique
The surgical execution of the Endoscopic Plantar Fasciotomy is an exercise in precise spatial awareness and controlled tissue release. The limb is exsanguinated with an Esmarch bandage, and the tourniquet is inflated to 250 mm Hg. The establishment of the surgical portals dictates the trajectory of the entire procedure; misplaced portals can lead to incomplete release or catastrophic neurovascular injury.
Establishing the Medial Portal and Working Plane
The medial incision site is meticulously mapped. The primary landmark is the medial malleolus. An imaginary line is drawn bisecting the medial malleolus vertically. The incision is placed along this line, approximately 1.5 to 2.0 cm superior to the junction of the plantar keratinized and dorsal non-keratinized skin, directly anterior and plantar to the medial calcaneal tuberosity. A #15 blade is used to make a precise 8-mm vertical skin incision. It is imperative to incise only the skin and superficial dermis. Blunt tenotomy scissors are then employed to carefully dissect through the subcutaneous adipose tissue, spreading parallel to the skin to expose the glistening white superficial fascia of the abductor hallucis muscle.
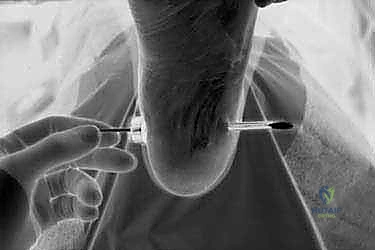
Once the medial deep fascia is visualized, the blunt plantar fascia elevator is introduced. The elevator is directed laterally and slightly distally, creating a subcutaneous working plane strictly plantar to the plantar fascia. The surgeon must rely heavily on tactile feedback; a distinct, firm resistance is felt as the elevator glides beneath the rigid aponeurosis. The elevator is swept back and forth to clear a pathway for the cannula.
Next, the slotted cannula, with the conical obturator locked in place, is introduced into this newly created tunnel. The assembly is advanced firmly from medial to lateral, maintaining a trajectory parallel to the plantar aspect of the foot. As the obturator traverses the plantar space, the surgeon palpates the lateral aspect of the foot. Once the tip of the obturator tents the lateral skin, a 5-mm vertical stab incision is made directly over the prominence. The obturator and cannula are then advanced through the lateral portal. The obturator is removed, leaving the slotted cannula bridging the medial and lateral aspects of the foot, with the open slot directed dorsally (deep) toward the plantar fascia.
Endoscopic Visualization and Fascial Release
The 4.0-mm, 30-degree arthroscope is introduced through the medial portal. Initially, the visual field is often obscured by a "white out" phenomenon caused by plantar fat herniating into the cannula slot. The assistant introduces a fluffed cotton-tipped applicator from the lateral portal, mechanically sweeping the fat dorsally and clearing the slot. This maneuver reveals the glistening, longitudinally oriented, dense white fibers of the plantar fascia.
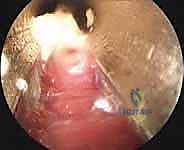
With the medial band clearly identified, the release commences. A disposable triangle knife is introduced through the lateral portal. The blade is visualized endoscopically as it engages the medial edge of the plantar fascia. Under direct, magnified vision, the surgeon draws the knife medially, transecting the fascial fibers. The release is typically performed in layers, utilizing both retrograde and antegrade cutting motions to ensure a controlled depth of penetration.

The critical endpoint of the release is the visualization of the flexor digitorum brevis (FDB) muscle belly. As the final layers of the medial and central bands are transected, the distinct, red, striated muscle tissue of the FDB will immediately herniate into the surgical field. This visual confirmation is the hallmark of a complete and safe release. The surgeon must meticulously verify that only the medial one-third to one-half of the fascia has been transected. The scope is rotated to inspect the lateral aspect of the cannula slot, ensuring the lateral band remains pristine and intact to preserve lateral column stability.
Once hemostasis is confirmed and the release is deemed satisfactory, the cannula is withdrawn. The medial and lateral portals are thoroughly irrigated with sterile saline. The skin incisions are closed with simple interrupted non-absorbable sutures, typically 4-0 nylon or Prolene. A sterile, bulky compressive dressing is applied prior to tourniquet deflation to minimize postoperative hematoma formation.
Complications, Incidence Rates, and Salvage Management
While Endoscopic Plantar Fasciotomy is celebrated for its minimally invasive nature and high success rates (frequently cited between 85% and 95%), it is not devoid of complications. A comprehensive understanding of potential adverse events is required for prompt recognition and effective salvage management. The most significant complications stem from technical errors, specifically over-resection of the fascia or loss of anatomical orientation.
The most dreaded biomechanical complication is lateral column overload, often manifesting as iatrogenic cuboid syndrome or lateral midfoot pain. This occurs when the surgeon inadvertently transects the lateral band of the plantar fascia, completely obliterating the windlass mechanism and destabilizing the longitudinal arch. This shifts abnormal biomechanical stress to the calcaneocuboid joint and the lateral metatarsals. Management of lateral column pain begins conservatively with rigid custom orthotics featuring a lateral wedge, taping techniques, and extended immobilization. In refractory cases, surgical salvage may necessitate complex midfoot fusions, such as a calcaneocuboid arthrodesis, to restore stability.
Neurological complications, though rare, can be devastating. Injury to the medial plantar nerve or its branches can occur if the medial portal is placed too deeply or if the cutting knife is aggressively driven beyond the medial border of the abductor hallucis. Similarly, the lateral plantar nerve is at risk during the creation of the lateral portal. Postoperative nerve entrapment due to aggressive scarring around the release site is also a recognized phenomenon. Management includes aggressive physical therapy, desensitization, gabapentinoids, and in severe cases, open surgical neurolysis.
Complication Profile and Management Strategy
| Complication | Estimated Incidence | Pathophysiology | Salvage / Management Strategy |
|---|---|---|---|
| Lateral Column Overload | 2% - 5% | Complete transection of lateral band; loss of arch support | Custom orthotics (lateral posting), CAM boot, rarely calcaneocuboid fusion |
| Transient Neurapraxia | 1% - 3% | Traction injury or localized edema affecting medial/lateral plantar nerves | Observation, NSAIDs, Gabapentin; typically resolves in 3-6 months |
| Recalcitrant Heel Pain | 5% - 10% | Incomplete release of the medial band; misdiagnosis (e.g., Baxter's nerve) | Re-evaluation (MRI), targeted corticosteroid injection, revision open surgery |
| Superficial Infection | < 1% | Portal site contamination | Oral antibiotics, local wound care; usually resolves rapidly |
| Deep Space Infection | < 0.1% | Introduction of pathogens into plantar fascial space | Emergent open I&D, IV antibiotics, wound vac therapy |
| Plantar Fascia Rupture | < 1% | Aggressive early weight-bearing before tissue healing | Immobilization in plantarflexion, extended non-weight bearing |
Phased Post-Operative Rehabilitation Protocols
The postoperative rehabilitation protocol following an Endoscopic Plantar Fasciotomy is meticulously phased to balance the need for early mobilization with the biological imperative of tissue healing. Unlike open procedures that require prolonged non-weight-bearing to protect large incisions, the minimally invasive nature of EPF allows for a dramatically accelerated recovery timeline. However, patient compliance is critical to prevent premature stress on the healing fascial stump.
Phase I: Immediate Postoperative Period (Weeks 0-2)
The primary goals during this phase are to control edema, manage pain, and protect the surgical site. The patient is placed in a rigid Controlled Ankle Motion (CAM) walker boot immediately postoperatively. Weight-bearing as tolerated (WBAT) is permitted, but patients are strongly advised to limit ambulation to essential household distances. The bulky compressive dressing remains intact until the first postoperative visit at approximately 10 to 14 days. Elevation of the limb above the level of the heart and regular application of ice behind the knee or at the ankle (avoiding the surgical site directly) are emphasized to mitigate swelling.
Phase II: Transitional Mobilization and Stretching (Weeks 2-6)
At the two-week mark, the sutures are removed. If the incisions are fully healed, the patient is transitioned out of the CAM boot and into a supportive, rigid-soled athletic shoe equipped with a custom or high-quality prefabricated orthotic featuring a deep heel cup and robust arch support. This is a critical transition period. Physical therapy is initiated, focusing heavily on aggressive, sustained stretching of the Achilles tendon and the gastrocnemius-soleus complex. Because the plantar fascia and the Achilles tendon are anatomically linked via the calcaneal paratenon, resolving any equinus contracture is vital to reducing tension on the healing plantar structures. Gentle cross-friction massage over the portal sites is introduced to prevent restrictive scar tissue formation.
Phase III: Return to Function and High-Impact Activity (Weeks 6-12)
By week six, most patients report a significant reduction in their preoperative pain levels. The focus of rehabilitation shifts toward strengthening the intrinsic musculature of the foot (e.g., towel scrunches, marble pickups) to provide dynamic support to the longitudinal arch, compensating for the partially released static fascia. Proprioceptive training and gradual reintroduction of impact activities are initiated under the guidance of a physical therapist. Return to high-impact sports, such as distance running or competitive athletics, is typically permitted between 10 and 12 weeks, contingent upon the patient demonstrating pain-free ambulation, full range of motion, and adequate intrinsic foot strength.
Summary of Landmark Literature and Clinical Guidelines
The evolution and validation of Endoscopic Plantar Fasciotomy are deeply rooted in robust clinical literature. The procedure was pioneered and popularized in the early 1990s by Barrett and Day, who published the seminal early series demonstrating the feasibility, safety, and rapid recovery associated with the two-portal endoscopic technique. Their initial cadaveric studies meticulously mapped the endoscopic anatomy, establishing the safety zones that dictate modern portal placement.
Subsequent high-level evidence has consistently supported the efficacy of EPF. A landmark prospective, randomized controlled trial by Macmull et al. compared EPF directly with open plantar fasciotomy. The study demonstrated that while both techniques provided equivalent long-term pain relief at one year, the EPF cohort exhibited statistically significant superiority in short-term outcomes, including reduced postoperative pain scores, faster return to normal footwear, and an accelerated return to work.
Furthermore, long-term follow-up studies, such as those by Jerosch et al., have confirmed the durability of the procedure, with patient satisfaction rates remaining above 85% at five to ten years postoperatively. These studies also highlighted the critical importance of the partial release technique; cohorts in which a complete fascial release was performed demonstrated an unacceptably high incidence of lateral column pain and arch destabilization.
Current clinical guidelines from major orthopedic and podiatric societies position Endoscopic Plantar Fasciotomy as a first-line surgical intervention for recalcitrant plantar fasciitis that has failed exhaustive conservative management. The literature unequivocally dictates that the success of the procedure is entirely dependent on strict patient selection, precise endoscopic execution, and adherence to a structured, orthotic-supported postoperative rehabilitation protocol. When performed by a skilled surgeon respecting these tenets, EPF remains the gold standard for minimally invasive heel pain relief.
