Orthopedic Foot And Ank Review | Dr Hutaif Foot & Ankle -...
Comprehensive 100-Question Exam
00:00
Start Quiz
Question 1
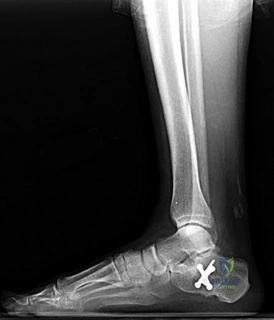
A 32-year-old male sustains a Hawkins Type II fracture of the talar neck following a motor vehicle collision. Which of the following sources of blood supply is most likely to remain intact, often providing the sole remaining perfusion to the talar body?
Explanation
Question 2
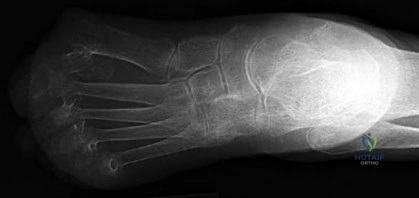
A 24-year-old rugby player sustains an axial load to a plantarflexed foot. Radiographs reveal a 'fleck sign' adjacent to the base of the second metatarsal. The primary injured ligament connects which two osseous structures?
Explanation
Question 3
A 45-year-old female presents with severe bunion pain. Weight-bearing radiographs demonstrate a hallux valgus angle (HVA) of 42 degrees, an intermetatarsal angle (IMA) of 18 degrees, and clinical hypermobility of the first tarsometatarsal (TMT) joint. Which of the following procedures is most appropriate to effectively correct the deformity and minimize recurrence?
Explanation
Question 4
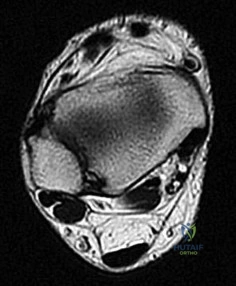
A 38-year-old recreational athlete sustains an acute, closed Achilles tendon rupture. He opts for nonoperative management. According to recent high-level evidence, which rehabilitation protocol yields a re-rupture rate most comparable to operative treatment?
Explanation
Question 5
A 60-year-old female presents with a progressive, flexible flatfoot deformity and inability to perform a single-leg heel raise. Examination shows severe hindfoot valgus and >40% uncovering of the talonavicular joint. She reports lateral ankle impingement pain. According to the Johnson and Strom classification modified by Myerson, what is the most appropriate surgical management if conservative treatment fails?
Explanation
Question 6
When performing an extensile lateral approach for open reduction and internal fixation of a displaced intra-articular calcaneus fracture, the surgical flap must be carefully elevated as a full-thickness layer to the periosteum to prevent necrosis. Which artery provides the primary blood supply to the apex of this lateral flap?
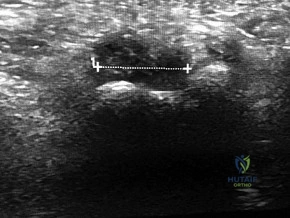
Explanation
Question 7
A 55-year-old patient with poorly controlled diabetes mellitus presents with a red, hot, and swollen left foot. Radiographs show periarticular osteopenia, fragmentation of bone, and early subluxation at the midtarsal joints. Infection has been definitively ruled out. According to the Eichenholtz classification, what stage is this, and what is the standard initial management?
Explanation
Question 8
In the setting of a complex ankle fracture, the anterior inferior tibiofibular ligament (AITFL) is typically attached to specific osseous landmarks. An avulsion fracture of the anterolateral distal tibia by the AITFL is eponymously known as which of the following?
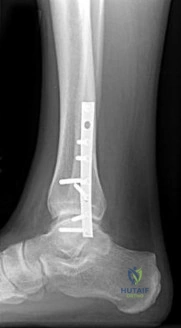
Explanation
Question 9
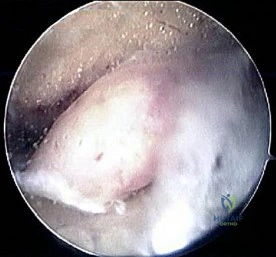
A 26-year-old male sustains an inversion ankle sprain while his foot is maximally plantarflexed. He later develops persistent deep ankle pain. MRI reveals an osteochondral lesion of the talus. Based on the mechanism of injury, where is the lesion most likely located and what is its typical morphology?
Explanation
Question 10
A 42-year-old runner complains of chronic medial heel pain radiating to the plantar aspect of the foot. Examination reveals maximal tenderness over the medial tuberosity of the calcaneus, exacerbated by palpation distal to the abductor hallucis. Entrapment of the first branch of the lateral plantar nerve (Baxter's nerve) is suspected. This nerve typically courses between which two muscle bellies?
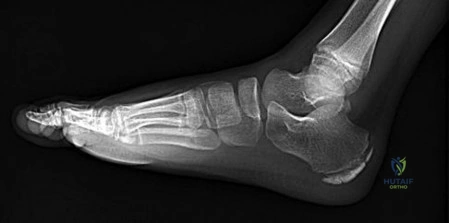
Explanation
Question 11
A 20-year-old male with Charcot-Marie-Tooth disease presents with a symptomatic bilateral cavovarus foot deformity. A Coleman block test is performed, which normalizes his hindfoot varus. Which of the following muscle imbalances is the primary driver initiating the plantarflexed first ray in this specific deformity?
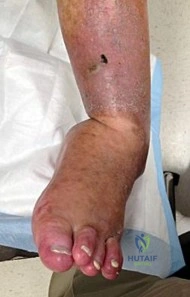
Explanation
Question 12
A professional American football player forcibly hyperextends his first metatarsophalangeal (MTP) joint during a tackle. MRI confirms a complete rupture of the plantar plate (Grade III turf toe injury). Which of the following describes the most common anatomical site of failure in a complete plantar plate rupture requiring surgical repair?
Explanation
Question 13
A 28-year-old professional basketball player sustains a fracture at the base of the fifth metatarsal. Radiographs show a transverse fracture at the metaphyseal-diaphyseal junction extending into the 4th-5th intermetatarsal articulation (Zone 2). What is the recommended treatment to minimize nonunion and expedite return to play in this elite athlete?
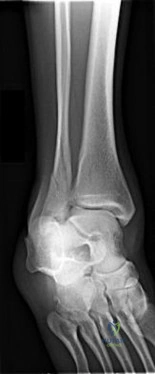
Explanation
Question 14
A 30-year-old skier presents with lateral ankle pain and a snapping sensation behind the lateral malleolus after a fall. The injury occurred during forced ankle dorsiflexion and eversion. Radiographs show a thin cortical flake of bone avulsed from the posterolateral border of the fibula. What is the most likely diagnosis?
Explanation
Question 15
A 58-year-old male presents with dorsal first MTP joint pain. Radiographs demonstrate advanced joint space narrowing, large dorsal osteophytes, and subchondral sclerosis. Clinically, he has severe pain at the extremes of motion AND during the mid-arc of motion (Coughlin and Shurnas Grade 4 hallux rigidus). Which surgical procedure is considered the most reliable gold standard for this patient?
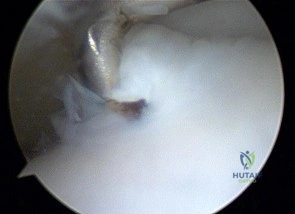
Explanation
Question 16
A 14-year-old boy presents with a history of recurrent ankle sprains and a painful, rigid flatfoot. Examination reveals restricted subtalar motion and peroneal spasticity. Lateral radiographs reveal a continuous bony contour forming a 'C-sign'. Which of the following describes the most likely anatomic location of the pathology?
Explanation
Question 17
A 25-year-old male sustains a severe crush injury to his foot and develops compartment syndrome. The human foot is traditionally described as having nine anatomical compartments. Which of the following structures is exclusively located within the calcaneal compartment?
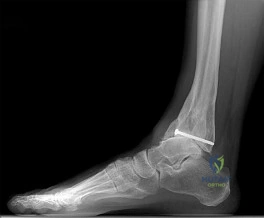
Explanation
Question 18
Total Ankle Arthroplasty (TAA) has become an increasingly popular alternative to ankle arthrodesis for end-stage ankle osteoarthritis. According to current guidelines, which of the following is generally considered an ABSOLUTE contraindication for TAA?
Explanation
Question 19
A 21-year-old track athlete presents with insidious onset of vague midfoot pain. Examination reveals point tenderness over the dorsal 'N-spot'. CT scan confirms a navicular stress fracture. This fracture typically originates in which specific region of the navicular due to a vascular watershed area and maximum shear stress?
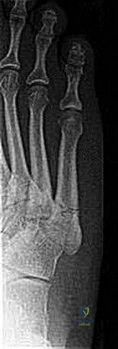
Explanation
Question 20
During the surgical repair of an acute syndesmotic injury (high ankle sprain) without a medial malleolus fracture, the surgeon places a syndesmotic screw. Historically, teaching dictated fixing the syndesmosis with the ankle in maximal dorsiflexion to prevent overtightening. What anatomical characteristic of the talus was the basis for this traditional teaching, even though recent studies show anatomical reduction is the true determinant of postoperative motion?
Explanation
Question 21
A 45-year-old male presents with chronic lateral foot and ankle pain 18 months after sustaining a closed, displaced intra-articular calcaneus fracture treated nonoperatively. He reports difficulty wearing standard closed shoes. Physical examination reveals limited subtalar motion and tenderness inferior to the lateral malleolus. What is the most likely pathophysiologic cause of his current symptoms?
Explanation
Question 22
A 55-year-old female presents with a painful, progressive flatfoot deformity. Examination reveals an inability to perform a single-limb heel rise and significant flexible hindfoot valgus. Weight-bearing radiographs demonstrate a talonavicular coverage angle of 45 degrees and uncovering of the talar head. Which of the following surgical strategies is most appropriate for this stage of deformity?
Explanation
Question 23
A surgeon is performing a minimally invasive percutaneous repair of an acute Achilles tendon rupture. To minimize the risk of iatrogenic nerve injury during suture passage, the surgeon must be acutely aware of the course of the sural nerve. At approximately what distance proximal to the calcaneal insertion does the sural nerve typically cross the lateral border of the Achilles tendon?
Explanation
Question 24
A 62-year-old patient with poorly controlled type 2 diabetes presents with a globally swollen, erythematous, and warm right foot. Pedal pulses are palpable. Radiographs reveal fragmentation, periarticular debris, and subluxation at the tarsometatarsal joints. What is the most appropriate initial management?
Explanation
Question 25
A 22-year-old female with Charcot-Marie-Tooth disease presents with bilateral cavovarus feet. A Coleman block test is performed, and her hindfoot varus completely corrects to a neutral alignment when the first metatarsal is allowed to drop off the block. What does this finding dictate regarding surgical planning?
Explanation
Question 26
A 21-year-old collegiate basketball player sustains a fracture of the fifth metatarsal. Radiographs show a transverse fracture at the metaphyseal-diaphyseal junction involving the fourth-fifth intermetatarsal articulation. He is treated with intramedullary screw fixation. To minimize the risk of nonunion or construct failure, which of the following is the most critical technical factor regarding the screw?
Explanation
Question 27
A 19-year-old cross-country runner presents with insidious onset dorsal midfoot pain. Plain radiographs are negative. A CT scan confirms an incomplete, non-displaced stress fracture of the dorsal cortex of the tarsal navicular. Why is this specific anatomic region highly susceptible to nonunion?
Explanation
Question 28
A 28-year-old male sustains an acute distal tibiofibular syndesmotic injury. During surgical stabilization, the surgeon meticulously evaluates the individual syndesmotic ligaments. Which of the following ligaments provides the greatest resistance to lateral displacement of the fibula and is mechanically the strongest?
Explanation
Question 29
A 58-year-old male presents with dorsal foot pain and stiffness of the great toe. Examination shows palpable dorsal osteophytes and pain exclusively at the extremes of motion. Radiographs demonstrate <50% joint space narrowing with preservation of the plantar joint space (Coughlin Grade 2 Hallux Rigidus). What is the most appropriate initial surgical intervention if conservative measures fail?
Explanation
Question 30
A 22-year-old American football lineman sustains an acute hyperextension injury to his first MTP joint. MRI confirms a complete tear of the plantar plate. During surgical repair, where is the most common anatomic location of the plantar plate disruption?
Explanation
Question 31
A 10-year-old boy presents with a history of recurrent lateral ankle sprains and a rigid flatfoot. Oblique radiographs of the foot demonstrate an elongated anterior process of the calcaneus, commonly known as the 'anteater nose' sign. Which of the following is the most likely diagnosis?
Explanation
Question 32
Osteochondral lesions of the talus (OLTs) have distinct morphologic characteristics based on their location. Which of the following descriptions classically characterizes an anterolateral OLT?
Explanation
Question 33
A 45-year-old female presents with pain in the second webspace, radiating into the toes. Clinical examination reveals pain upon lateral compression of the forefoot accompanied by a palpable click (Mulder's sign). She undergoes surgical excision through a dorsal approach. Which of the following is a known risk specific to the dorsal approach compared to the plantar approach for this pathology?
Explanation
Question 34
A 26-year-old skier presents with snapping over the lateral malleolus after an acute eversion injury. Examination confirms subluxation of the peroneal tendons with resisted eversion. Surgical management involves repair of the superior peroneal retinaculum (SPR). To which structure must the SPR be anatomically reattached?
Explanation
Question 35
A 68-year-old male with end-stage ankle osteoarthritis is being evaluated for a Total Ankle Arthroplasty (TAA). Which of the following represents an absolute contraindication to performing a TAA rather than an ankle arthrodesis in this patient?
Explanation
Question 36
A 38-year-old male sustains a high-energy pilon fracture. CT imaging demonstrates significant comminution, but distinct fracture fragments are identifiable. The anterolateral distal tibial articular fragment, often avulsed during the injury, is attached to which ligament?
Explanation
Question 37
A 50-year-old runner undergoes a complete surgical release of the plantar fascia for recalcitrant plantar fasciitis. Post-operatively, she reports relief of her heel pain but develops new-onset, severe pain along the lateral border of her midfoot. What is the most likely biomechanical cause of this new symptom?
Explanation
Question 38
A 25-year-old equestrian falls from a horse, sustaining a subtle Lisfranc injury with instability of the first, second, and third tarsometatarsal (TMT) joints. The surgeon opts for open reduction and internal fixation utilizing dorsal spanning plates rather than transarticular screws. What is the primary biomechanical and biologic advantage of using dorsal spanning plates in this scenario?
Explanation
Question 39
A 14-year-old female presents with insidious onset forefoot pain localized to the second metatarsophalangeal (MTP) joint. Radiographs demonstrate sclerosis, flattening, and early fragmentation of the second metatarsal head. What is the most likely diagnosis?
Explanation
Question 40
A 40-year-old roofer falls from a height and sustains a displaced intra-articular calcaneus fracture. He undergoes Open Reduction Internal Fixation (ORIF) via an extensile lateral approach. Postoperatively, he complains of numbness over the lateral aspect of his heel and foot. Which nerve was most likely injured during the surgical approach?
Explanation
Question 41
A 55-year-old female presents with a progressive flatfoot deformity. Examination reveals a flexible hindfoot valgus and inability to perform a single-leg heel raise. Weight-bearing radiographs show more than 30% uncovering of the talonavicular joint on the AP view. Which of the following surgical interventions is most appropriate for this Stage IIb posterior tibial tendon dysfunction?
Explanation
Question 42
A 22-year-old collegiate football lineman presents with severe pain at the base of the great toe after being tackled with his foot planted in extreme dorsiflexion. MRI confirms a complete tear of the plantar plate complex with proximal retraction of the sesamoids. What is the most appropriate management for this athlete?
Explanation
Question 43
A 20-year-old track athlete presents with insidious onset of vague dorsal midfoot pain. CT scan reveals an incomplete stress fracture of the tarsal navicular located in the central third of the bone. What anatomical feature primarily predisposes the navicular to stress fractures in this specific region?
Explanation
Question 44
A 19-year-old professional basketball player sustains an acute, displaced fracture at the metaphyseal-diaphyseal junction of the fifth metatarsal. To minimize the risk of nonunion and expedite return to play, intramedullary screw fixation is planned. What is the optimal entry point for accurately placing the screw in the medullary canal?
Explanation
Question 45
A 55-year-old female presents with progressive flattening of her left medial longitudinal arch. On examination, she is unable to perform a single-leg heel rise. Weight-bearing radiographs demonstrate >40% talonavicular uncoverage and an abnormally high talus-first metatarsal angle. Which of the following surgical procedures is most appropriate for this stage of posterior tibial tendon dysfunction (Stage IIb)?
Explanation
Question 46
During an extensile lateral approach for open reduction and internal fixation of a displaced intra-articular calcaneus fracture, protecting the primary blood supply to the apex of the corner flap is critical. Which of the following arteries is primarily responsible for perfusing this flap?
Explanation
Question 47
A 22-year-old professional basketball player presents with lateral foot pain after landing awkwardly. Radiographs reveal an acute, non-displaced fracture at the metaphyseal-diaphyseal junction of the fifth metatarsal (Zone 2). What is the recommended treatment to minimize the risk of nonunion and allow the fastest return to play?
Explanation
Question 48
A 40-year-old male is undergoing open reduction and internal fixation of a bimalleolar equivalent ankle fracture. Intraoperatively, the Cotton test demonstrates syndesmotic instability. On an AP and Mortise radiograph, what is the normal limit for the tibiofibular clear space when evaluating reduction?
Explanation
Question 49
When performing a minimally invasive repair of an acute Achilles tendon rupture, care must be taken to avoid injury to the sural nerve. At what approximate distance proximal to the calcaneal insertion does the sural nerve typically cross the lateral border of the Achilles tendon?
Explanation
Question 50
A 60-year-old poorly controlled diabetic male presents with an acutely swollen, red, and warm right foot. He denies trauma, and his pedal pulses are bounding. Inflammatory markers are mildly elevated. Radiographs show early fragmentation and debris at the midfoot. What is the most appropriate immediate management?
Explanation
Question 51
A 52-year-old avid runner presents with worsening great toe pain. Examination reveals less than 10 degrees of dorsiflexion and significant pain through the mid-arc of motion. Radiographs demonstrate severe joint space narrowing, subchondral sclerosis, and large circumferential osteophytes at the first metatarsophalangeal (MTP) joint. What is the most definitive and reliable surgical treatment?
Explanation
Question 52
A 19-year-old track athlete experiences vague dorsal midfoot pain for three months. A CT scan confirms a non-displaced stress fracture of the tarsal navicular. In which anatomic zone of the navicular do these stress fractures most commonly occur due to an area of relative avascularity?
Explanation
Question 53
In patients with Charcot-Marie-Tooth (CMT) disease, a classic cavovarus foot deformity develops due to specific muscle imbalances. Which of the following combinations best describes the primary overpowering muscle forces driving the plantarflexed first ray and hindfoot varus?
Explanation
Question 54
A surgeon is performing a dorsal approach for the excision of a recurrent Morton's neuroma in the third web space. To gain adequate exposure and successfully identify and resect the neuroma, which of the following structures MUST be transected?
Explanation
Question 55
A 28-year-old male develops severe foot pain and tense swelling following a severe crush injury. Compartment syndrome of the foot is suspected. Among the nine recognized fascial compartments of the foot, the calcaneal compartment contains which of the following vital structures?
Explanation
Question 56
A 13-year-old male sustains an external rotation injury to his ankle. Radiographs show a Salter-Harris III fracture of the anterolateral distal tibia (Tillaux fracture). This fracture pattern is primarily due to the avulsion pull of which of the following ligaments?
Explanation
Question 57
A 60-year-old male is undergoing surgery for chronic insertional Achilles tendinopathy with a large Haglund's deformity. During debridement through a central tendon-splitting approach, it is determined that 65% of the Achilles tendon insertion must be detached and excised to adequately remove the degenerative tissue. What is the most appropriate next step in management?
Explanation
Question 58
A 68-year-old female with end-stage post-traumatic ankle osteoarthritis is being evaluated for a total ankle arthroplasty (TAA). Which of the following conditions represents an absolute contraindication to performing a TAA in this patient?
Explanation
Question 59
According to the Lauge-Hansen classification of ankle fractures, a Supination-External Rotation (SER) mechanism predictably injures structures in a sequential order. What represents Stage 3 of this injury pattern?
Explanation
Question 60
A 24-year-old sprinter presents with acute plantar first MTP joint pain after forcefully pushing off the starting blocks. Radiographs reveal a radiolucency through the tibial sesamoid. Which of the following radiographic characteristics best distinguishes an acute sesamoid fracture from a congenital bipartite sesamoid?
Explanation
Question 61
A 52-year-old female presents with a progressive, painful flatfoot deformity. Clinical examination reveals an inability to perform a single-leg heel rise. Weight-bearing radiographs show a flexible hindfoot valgus and greater than 30% uncovering of the talonavicular joint with forefoot abduction. What is the most appropriate surgical management for this Stage IIb posterior tibial tendon dysfunction?
Explanation
Question 62
A 40-year-old construction worker falls from a height and sustains a severely displaced, joint-depressed calcaneus fracture. The surgeon elects to perform an open reduction and internal fixation via an extensile lateral approach. Which of the following is the most common postoperative complication associated with this specific surgical approach?
Explanation
Question 63
A 35-year-old recreational basketball player suffers an acute Achilles tendon rupture. Based on high-level level I evidence (e.g., the Willits trial) comparing operative repair versus non-operative management with early functional rehabilitation, what is the expected outcome profile?
Explanation
Question 64
A 58-year-old male with long-standing, poorly controlled type II diabetes presents with a red, hot, swollen left foot. He denies trauma. Pulses are bounding, and sensation to monofilament testing is absent. Radiographs demonstrate marked periarticular fragmentation, subchondral debris, and subluxation at the tarsometatarsal joints. According to the Eichenholtz classification, what stage of Charcot neuroarthropathy does this represent?
Explanation
Question 65
A 21-year-old collegiate soccer player sustains a twisting injury to his foot and is diagnosed with an acute diaphyseal/metaphyseal junction fracture of the fifth metatarsal (Zone 2, Jones fracture). Given his desire to return to elite-level sports, what is the gold standard of treatment?
Explanation
Question 66
A 28-year-old female presents with chronic ankle pain following recurrent sprains. MRI reveals an osteochondral lesion of the talus (OCD). Which of the following best describes the characteristics and mechanism of a posteromedial talar dome lesion?
Explanation
Question 67
A patient with Charcot-Marie-Tooth disease presents with a bilateral cavovarus foot deformity. A Coleman block test is performed on the right foot, and the hindfoot varus corrects completely to a neutral alignment. What does this clinical finding indicate?
Explanation
Question 68
A 68-year-old male presents with severe pain in his first metatarsophalangeal (MTP) joint, particularly during toe-off. Examination reveals pain throughout the mid-range of motion. Radiographs demonstrate >50% joint space narrowing, a dorsal ring of osteophytes, and subchondral cysts (Coughlin/Shurnas Grade 4 Hallux Rigidus). What is the most reliable definitive surgical treatment?
Explanation
Question 69
A professional American football lineman sustains a severe hyperextension injury to his great toe. Clinical exam shows marked swelling, ecchymosis, and a gross lack of resistance to passive MTP dorsiflexion. MRI confirms a complete rupture of the plantar plate with proximal retraction of the sesamoids. What is the most appropriate management?
Explanation
Question 70
A 45-year-old female complains of burning and tingling in the plantar aspect of her foot, which worsens after standing. Examination reveals a positive Tinel's sign posterior to the medial malleolus. If an MRI is ordered and identifies a space-occupying lesion compressing the posterior tibial nerve, what is the most common etiology in this specific location?
Explanation
Question 71
A 22-year-old skier experiences a sudden 'popping' sensation behind his lateral malleolus after forced dorsiflexion and eversion of his ankle. Examination reveals tenderness and visible swelling over the peroneal tendons, which subluxate anteriorly with active eversion. Which of the following is the most common anatomic variant of the superior peroneal retinaculum (SPR) injury in this condition?
Explanation
Question 72
A 30-year-old male presents to the emergency department after a twisting injury to his ankle. Radiographs show a widened medial clear space and an isolated proximal third fibula fracture (Maisonneuve fracture). Given the location of the proximal fibula fracture, which nerve is at greatest risk of associated injury?
Explanation
Question 73
A 12-year-old boy presents with a painful, rigid flatfoot and a history of recurrent ankle sprains. Peroneal spasticity is noted on examination. Oblique radiographs of the foot demonstrate an elongated anterior process of the calcaneus approaching the navicular. What is the classic radiographic name for this finding?
Explanation
Question 74
A 55-year-old runner has chronic insertional Achilles tendinopathy with a prominent Haglund deformity and extensive intratendinous calcification. Conservative management has failed. During surgery, aggressive debridement of the diseased tendon is necessary. At what threshold of Achilles tendon detachment/debridement is augmentation with a flexor hallucis longus (FHL) transfer generally recommended?
Explanation
Question 75
According to the Lauge-Hansen classification system, what is the typical progression of osseous and ligamentous injury in a Supination-External Rotation (SER) ankle fracture?
Explanation
None
Detailed Chapters & Topics
Dive deeper into specialized chapters regarding orthopedic-mcqs-online-015-foot-and-ankle-e
