Orthopedic Foot And Ank Review | Dr Hutaif Foot & Ankle -...
Key Takeaway
Looking for accurate information on Orthopedic MCQS online 012 FOOT AND ANKLE? For avulsion fractures of the calcaneus, immediate open reduction and internal fixation is the best treatment. Nonsurgical management often **failed to provide** adequate healing, leaving a weak Achilles tendon and high complication rates. Percutaneous Kirschner wire fixation also **failed to provide** stable fixation against the powerful Achilles tendon, making it unsuitable for this type of injury.
Orthopedic Foot And Ank Review | Dr Hutaif Foot & Ankle -...
Comprehensive 100-Question Exam
00:00
Start Quiz
Question 1
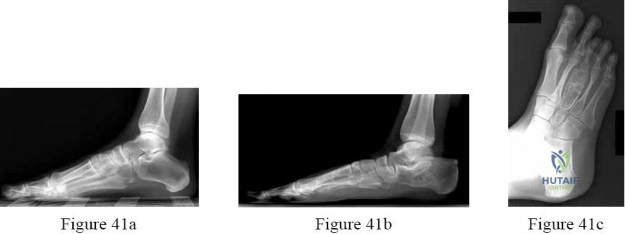
A 45-year-old female presents with a painful bunion. Radiographs demonstrate a hallux valgus angle (HVA) of 35 degrees and an intermetatarsal angle (IMA) of 16 degrees. Clinical examination reveals profound hypermobility at the first tarsometatarsal (TMT) joint. What is the most appropriate surgical treatment?
Explanation
Question 2
A 60-year-old male complains of severe pain and stiffness in his right big toe. Examination reveals significantly limited dorsiflexion and pain at the extremes of motion. Radiographs demonstrate large dorsal osteophytes and near-complete joint space narrowing of the first MTP joint, consistent with Grade 3 hallux rigidus. Which of the following is considered the gold standard surgical treatment?
Explanation
Question 3
When comparing early functional rehabilitation protocols to traditional cast immobilization for acute Achilles tendon ruptures treated nonoperatively, which of the following statements is most accurate?
Explanation
Question 4
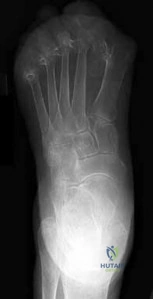
A 55-year-old female presents with a progressive flatfoot deformity. She is unable to perform a single-limb heel rise on the affected side. Radiographs demonstrate talonavicular uncoverage of 40% and a Meary's angle of 15 degrees apex plantar. The hindfoot deformity is correctable passively. Which stage of posterior tibial tendon dysfunction (PTTD) does this represent?
Explanation
Question 5
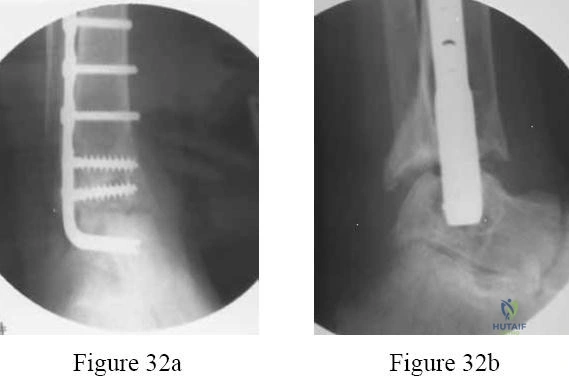
A 22-year-old athlete requires surgical intervention for chronic lateral ankle instability after failing 6 months of physical therapy. A modified Broström procedure with a Gould modification is performed. What specific structure is mobilized and advanced to augment the primary ligament repair in the Gould modification?
Explanation
Question 6
A 30-year-old male has an osteochondral lesion of the medial talar dome measuring 1.2 cm x 1.0 cm. He has failed 6 months of conservative management. What is the most appropriate initial surgical treatment?
Explanation
Question 7
In the evaluation of an intra-articular calcaneus fracture, the Sanders classification is utilized. What specific anatomical finding defines a Sanders Type III fracture?
Explanation
Question 8
A patient sustained a Hawkins Type III talar neck fracture following a high-energy motor vehicle accident. What does this classification imply regarding the displacement of the talus?
Explanation
Question 9
During the radiographic evaluation of a suspected midfoot injury, what finding is considered pathognomonic for a Lisfranc injury?
Explanation
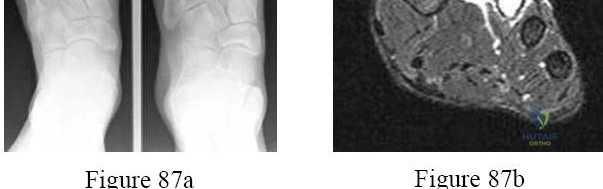
Question 10
A 60-year-old diabetic male presents with a warm, swollen, erythematous foot. His pedal pulses are bounding. Radiographs demonstrate periarticular fragmentation, subluxation, and bony debris at the tarsometatarsal joints. Which stage of the Eichenholtz classification does this clinical and radiographic picture represent?
Explanation
Question 11
When evaluating a patient with a hindfoot cavovarus deformity, the Coleman block test is performed. If the hindfoot varus corrects to neutral when the first metatarsal is allowed to drop off the block, what is the primary biomechanical driver of the varus deformity?
Explanation
Question 12
A 24-year-old elite collegiate basketball player suffers a Zone 2 proximal fifth metatarsal fracture. To minimize the risk of nonunion and expedite his return to play, what is the recommended treatment?
Explanation
Question 13
Surgical release of the plantar fascia for recalcitrant plantar fasciitis involves releasing only the medial one-third to one-half of the fascia. Releasing the entire plantar fascia significantly increases the biomechanical risk of developing which of the following complications?
Explanation
Question 14
A patient is diagnosed with a Morton's neuroma based on a positive Mulder's click and burning forefoot pain. Anatomically, which intermetatarsal web space is most commonly affected by this condition?
Explanation
Question 15
In the context of Tarsal Tunnel Syndrome, compression of the tibial nerve occurs deep to the flexor retinaculum. The first branch of the lateral plantar nerve, which can become entrapped and cause symptoms mimicking severe chronic heel pain, is anatomically known as:
Explanation
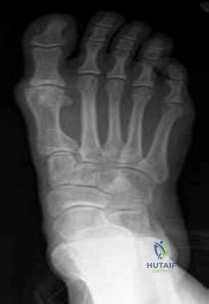
Question 16
A 45-year-old male presents with posterior heel pain. MRI confirms severe insertional Achilles tendinosis with a Haglund's deformity. Surgical debridement is planned. If the debridement requires detachment of greater than 50% of the Achilles tendon insertion, what is the most appropriate adjunct procedure?
Explanation
Question 17
During the operative fixation of a pronation-external rotation ankle fracture, the syndesmosis is evaluated fluoroscopically. Which radiographic parameter on a standard AP or mortise view is the most reliable indicator of syndesmotic widening?
Explanation
Question 18
When managing a highly comminuted distal tibia pilon fracture (AO/OTA 43-C3) with significant soft tissue injury, standard protocol involves a staged approach (spanning external fixation followed by delayed ORIF). What is the primary rationale for this delay?
Explanation
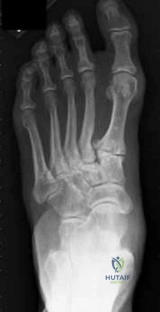
Question 19
A professional wide receiver sustains a severe hyperextension injury to his first MTP joint (Turf Toe). MRI reveals a complete rupture of the plantar plate with proximal retraction of the sesamoid apparatus. What is the most appropriate management?
Explanation
Question 20
A 20-year-old collegiate dancer presents with localized, recalcitrant pain directly plantar to the first metatarsal head. Imaging demonstrates a fragmented and nonunited tibial sesamoid. After 6 months of failed conservative management, what is the surgical treatment of choice?
Explanation
Question 21
A 60-year-old female presents with progressive flattening of her left foot. Examination reveals a flexible hindfoot valgus and inability to perform a single-limb heel rise. Radiographs show >40% talonavicular uncoverage on the AP view. What procedure is indicated in addition to flexor digitorum longus (FDL) transfer and medializing calcaneal osteotomy to address the specific deformity seen on the AP radiograph?
Explanation
Question 22
A 22-year-old man presents with a right cavovarus foot deformity. On the Coleman block test, the hindfoot varus corrects to neutral when the lateral border of the foot is placed on the block while the first metatarsal is allowed to drop off. What is the primary driver of this patient's hindfoot deformity?
Explanation
Question 23
A 25-year-old male athlete presents with deep ankle pain 6 months after an inversion injury. MRI reveals a 1.2 cm^2 osteochondral lesion of the medial talar dome with intact overlying cartilage. He has failed non-operative management. What is the most appropriate next step in treatment?

Explanation
Question 24
A 45-year-old female presents with a painful bunion. Weight-bearing radiographs show a hallux valgus angle (HVA) of 45 degrees, an intermetatarsal angle (IMA) of 18 degrees, and hypermobility at the first tarsometatarsal (TMT) joint. What is the most appropriate surgical intervention?
Explanation
Question 25
A 58-year-old man complains of dorsal forefoot pain with push-off during walking. Examination reveals restricted first MTP joint dorsiflexion, with pain at the extremes of motion. Radiographs demonstrate a dorsal osteophyte, joint space narrowing, but preservation of the plantar joint space (Coughlin and Shurnas Grade 2). What is the initial surgical procedure of choice if conservative care fails?

Explanation
Question 26
A 50-year-old overweight male presents with posterior heel pain. Examination reveals a tender, bulbous enlargement at the Achilles insertion. Radiographs show a large dorsal calcaneal exostosis (Haglund's deformity) and intratendinous calcification. Non-operative management for 6 months has failed. MRI shows tendinosis involving 60% of the tendon width at the insertion. What is the most appropriate surgical management?
Explanation
Question 27
A 28-year-old soccer player sustains a twisting injury to his ankle. Radiographs show a spiral fracture of the proximal third of the fibula. An external rotation stress view shows widening of the medial clear space to 6 mm. Which of the following structures is most likely to be completely disrupted?

Explanation
Question 28
A 40-year-old construction worker falls from a ladder, sustaining a closed, displaced intra-articular calcaneus fracture. The primary fracture line on the coronal CT scan divides the posterior facet into two pieces. Which of the following describes a Sanders Type II fracture?
Explanation
Question 29
A 30-year-old involved in a motor vehicle collision sustains a Hawkins Type III talar neck fracture. What does this classification imply regarding the displacement and the blood supply to the talar body?
Explanation
Question 30
A 22-year-old offensive lineman sustains an axial load to a plantarflexed foot. Weight-bearing radiographs demonstrate a 3 mm diastasis between the bases of the first and second metatarsals without any visible fractures. What is the recommended definitive treatment for this pure ligamentous injury in a high-level athlete?

Explanation
Question 31
A 24-year-old professional football player hyperextends his great toe on artificial turf. He has severe pain, ecchymosis, and inability to bear weight. MRI shows a complete tear of the plantar plate with proximal retraction of the sesamoids. What is the most appropriate management?
Explanation
Question 32
A 60-year-old diabetic patient presents with a warm, swollen, erythematous left foot. Radiographs reveal fragmentation and periarticular debris around the midfoot, with subluxation of the tarsometatarsal joints. Skin is intact. Inflammatory markers are mildly elevated. What is the appropriate initial management?

Explanation
Question 33
A 26-year-old skier presents with a snapping sensation at the posterolateral ankle. Examination reveals the peroneal tendons dislocating anteriorly over the lateral malleolus with resisted dorsiflexion and eversion. Conservative treatment has failed. Surgical exploration reveals a shallow fibular groove and an incompetent superior peroneal retinaculum (SPR). What is the standard surgical procedure?
Explanation
Question 34
A 45-year-old woman complains of sharp, burning pain in the plantar aspect of her forefoot, radiating to the third and fourth toes. Symptoms worsen with tight shoes. A Mulder's click is positive. The most likely diagnosis involves entrapment of a nerve beneath which of the following structures?
Explanation
Question 35
A 14-year-old boy presents with frequent ankle sprains and a rigid flatfoot. Radiographs show a "C-sign" on the lateral view and an irregular subtalar joint. Which type of tarsal coalition does this patient most likely have, and which imaging modality is best to confirm it?

Explanation
Question 36
A 21-year-old collegiate basketball player sustains a fracture of the fifth metatarsal base. Radiographs show a transverse fracture at the metaphyseal-diaphyseal junction extending into the intermetatarsal (4-5) articulation. This is a Zone 2 injury. To minimize the risk of nonunion and allow early return to play, what is the best treatment?
Explanation
Question 37
A 20-year-old male track athlete complains of vague, aching pain in the dorsal midfoot that is worse with sprinting. Radiographs are negative. An MRI reveals a linear signal abnormality in the central third of the navicular. CT scan confirms an incomplete sagittal fracture. What is the most appropriate initial treatment?
Explanation
Question 38
A 45-year-old active man presents with asymmetric anterior ankle pain. Radiographs demonstrate asymmetric narrowing of the medial ankle joint space with a varus tibial plafond angle. The lateral joint space is preserved. Hindfoot motion is normal. What is the primary rationale for performing a supramalleolar osteotomy in this patient?
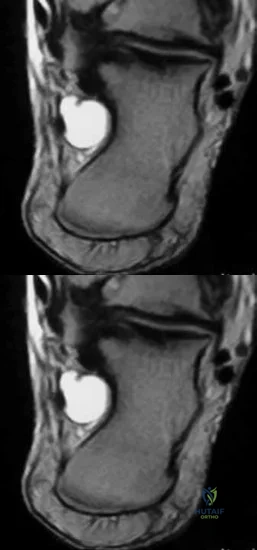
Explanation
Question 39
In a high-energy tibial pilon fracture, CT imaging is routinely obtained for preoperative planning. The classic three-fragment pattern involves a medial fragment, a posterior fragment, and an anterolateral fragment. The anterolateral fragment is typically attached to which of the following ligaments?
Explanation
Question 40
A 55-year-old diabetic male presents with an ulcer under his first metatarsal head and a swollen foot. It is critical to differentiate osteomyelitis from acute Charcot arthropathy. On MRI, which finding is most specific for osteomyelitis over acute Charcot neuroarthropathy?
Explanation
Question 41
A 55-year-old female presents with medial ankle pain and a progressively flattening arch. She has pain with single-limb heel rise but is able to perform it weakly. Passively, her hindfoot corrects to neutral. What is the most appropriate surgical intervention if conservative management fails?
Explanation
Question 42
A 28-year-old male sustains a Hawkins Type III talar neck fracture following a motor vehicle collision. Which of the following best describes the disruption of blood supply and the associated risk of avascular necrosis (AVN)?
Explanation
Question 43
A 22-year-old football player sustains an axial load to a plantarflexed foot. Weight-bearing radiographs reveal a 3 mm diastasis between the base of the first and second metatarsals. What is the most appropriate definitive management?
Explanation
Question 44
A 62-year-old male undergoes surgical debridement for severe insertional Achilles tendinopathy. During the procedure, 60% of the tendon insertion is resected to remove calcifications and degenerative tissue. What is the most appropriate next step in management?
Explanation
Question 45
A 19-year-old collegiate basketball player sustains a fracture at the metaphyseal-diaphyseal junction of the fifth metatarsal. He wishes to return to play as soon as possible. What is the recommended treatment?
Explanation
Question 46
A 58-year-old poorly controlled diabetic presents with a red, hot, swollen unilateral foot. Radiographs show periarticular fragmentation and debris at the midfoot. Which of the following tests is most specific for differentiating acute Charcot neuroarthropathy from osteomyelitis?
Explanation
Question 47
A 24-year-old marathon runner presents with vague dorsal midfoot pain. A CT scan confirms an incomplete, non-displaced stress fracture of the tarsal navicular in the sagittal plane. What is the most appropriate initial management?
Explanation
Question 48
A 72-year-old thin female with rheumatoid arthritis and low functional demands presents with severe, bone-on-bone ankle osteoarthritis. She has preserved subtalar and midfoot motion. What is the primary advantage of total ankle arthroplasty (TAA) over ankle arthrodesis in this patient?
Explanation
Question 49
A professional football player sustains a hyperdorsiflexion injury to the 1st MTP joint. Clinical examination reveals absent push-off strength and a positive Lachman test of the MTP joint. MRI shows a complete disruption of the plantar plate with proximal retraction of the sesamoids. What is the most appropriate management?
Explanation
Question 50
A 16-year-old male presents with bilateral progressive cavovarus feet. Examination shows weak tibialis anterior and peroneus brevis muscles, with a strong peroneus longus and tibialis posterior. A Coleman block test normalizes the hindfoot varus. What is the primary driver of this patient's deformity?
Explanation
Question 51
A 35-year-old roofer falls 15 feet, sustaining a closed, displaced intra-articular calcaneus fracture (Sanders Type III). He is scheduled for ORIF via an extensile lateral approach. Which of the following patient factors is the strongest contraindication to this surgical approach?
Explanation
Question 52
A 25-year-old female presents with persistent ankle pain 6 months after an inversion sprain. MRI reveals an anterolateral osteochondral lesion of the talus (OCLT) measuring 0.8 cm squared. The cartilage is intact but soft on probing during arthroscopy. What is the most appropriate surgical treatment?
Explanation
Question 53
A 25-year-old male presents with severe midfoot pain after a football injury. He states another player fell on his heel while his foot was plantarflexed. Radiographs reveal a widening of the space between the 1st and 2nd metatarsal bases with a small osseous fragment visible in the interspace.
What is the most likely mechanism of this injury?

Explanation
Question 54
A 14-year-old male presents with recurrent ankle sprains and a rigid, painful flatfoot. A lateral weight-bearing radiograph demonstrates a continuous, C-shaped bony contour extending from the talar dome to the sustentaculum tali. What is the most likely diagnosis and appropriate initial management?
Explanation
Question 55
A 55-year-old female presents with Stage IIB adult-acquired flatfoot deformity. Clinical exam demonstrates a flexible hindfoot valgus and significant forefoot abduction (too many toes sign). Radiographs show greater than 30% uncovering of the talonavicular joint. Which of the following procedures is essential to correct her deformity in addition to a flexor digitorum longus transfer and medial displacement calcaneal osteotomy?
Explanation
Question 56
A 60-year-old male with poorly controlled diabetes presents with a red, hot, swollen right foot. There are no open ulcers or portals of entry. Radiographs show fragmentation and debris at the tarsometatarsal joints. What is the most appropriate initial management?
Explanation
Question 57
A surgeon is performing a minimally invasive percutaneous repair of an acute Achilles tendon rupture. Which nerve is at the highest risk of iatrogenic injury during this procedure, and in what anatomical zone?
Explanation
Question 58
A 25-year-old male presents with chronic ankle pain. MRI reveals an anterolateral osteochondral lesion of the talus (OLT) measuring 1.1 cm squared. He has failed 6 months of conservative management. What is the most appropriate primary surgical treatment?
Explanation
Question 59
A 35-year-old construction worker sustains a Sanders type III calcaneus fracture after a fall from a ladder. The surgeon elects to use an extensile lateral approach for open reduction and internal fixation. Which structure is elevated within the full-thickness subperiosteal flap and must be protected?
Explanation
Question 60
A 22-year-old elite collegiate basketball player sustains a Zone 2 fracture of the proximal fifth metatarsal. To minimize nonunion risk and expedite return to play, what is the treatment of choice?
Explanation
Question 61
During open reduction and internal fixation of a pronation-external rotation ankle fracture, the surgeon is evaluating the syndesmosis. What intraoperative step provides the most reliable assessment to ensure anatomic reduction of the syndesmosis?
Explanation
Question 62
A 40-year-old female complains of burning pain in her third webspace, exacerbated by wearing narrow shoes. Examination reveals a painful click when compressing the metatarsal heads (Mulder's sign). The pathogenesis of this condition involves perineural fibrosis caused by compression against which structure?
Explanation
Question 63
A 65-year-old female with end-stage post-traumatic ankle arthritis desires a total ankle arthroplasty (TAA). Which of the following conditions is considered an absolute contraindication for TAA?
Explanation
Question 64
When performing a Scarf osteotomy for correction of moderate to severe hallux valgus, which of the following is a unique and recognized complication specific to the geometry of this osteotomy?
Explanation
Question 65
A 30-year-old male sustains a Hawkins Type III talar neck fracture following a high-energy motor vehicle collision. What is the approximate risk of avascular necrosis (AVN) for this injury, and what is the primary arterial supply to the talar body?
Explanation
Question 66
A competitive skier presents with lateral ankle pain and a snapping sensation behind the lateral malleolus after a sudden dorsiflexion and inversion injury. Radiographs show a small "fleck sign" avulsed from the posterolateral fibula. What is the primary stabilizing structure injured in this condition?
Explanation
Question 67
A 45-year-old male with chronic, recalcitrant plantar fasciitis undergoes an open complete release of the plantar fascia after failing 12 months of conservative care. What is a recognized biomechanical complication of releasing the entire plantar fascia?
Explanation
Question 68
A 55-year-old diabetic male has a chronic, full-thickness neuropathic ulcer beneath the first metatarsal head. The ulcer probes to bone. No retained hardware is present. Which imaging modality provides the highest sensitivity and specificity for diagnosing osteomyelitis in this setting?
Explanation
Question 69
A 22-year-old football player sustains an external rotation injury to his ankle and has a positive squeeze test. He is diagnosed with an acute syndesmotic sprain. Which ligament is considered the strongest component of the inferior tibiofibular syndesmotic complex?
Explanation
Question 70
A 28-year-old male with Charcot-Marie-Tooth disease presents with a progressive cavovarus foot deformity. A Coleman block test is performed, and the hindfoot corrects from a varus to a neutral position. What does this test signify about the primary driver of his deformity?
Explanation
Question 71
A 24-year-old professional athlete hyperextends his great toe on artificial turf. MRI confirms a Grade 3 turf toe injury with proximal migration of the sesamoids. Complete disruption of which structure is characteristic of this grade of injury?
Explanation
Question 72
A 20-year-old female track athlete complains of vague, aching midfoot pain that worsens with running. CT imaging demonstrates a partial, non-displaced dorsal cortical stress fracture in the central third of the navicular. What is the most appropriate initial management?
Explanation
Question 73
A 28-year-old male presents with bilateral cavovarus feet. A Coleman block test is performed, and the hindfoot corrects to a neutral alignment. Which of the following is the most appropriate primary osseous surgical procedure?
Explanation
None
