Mastering Foot & Ankle Interventions: Essential Ankle Surgery Insights
Key Takeaway
Your ultimate guide to Mastering Foot & Ankle Interventions: Essential Ankle Surgery Insights starts here. Ankle arthrodesis is a foot ankle int indicated for severe arthropathy, failed arthroplasty, or avascular necrosis of the talus. This surgical procedure fuses the ankle joint into a specific functional position (e.g., 0° dorsiflexion, 0-5° valgus, 5-10° external rotation). It aims to relieve pain but results in altered walking mechanics and increased energy expenditure.
Comprehensive Introduction and Patho-Epidemiology
End-stage ankle arthritis presents a profound clinical challenge, exacting a functional and economic toll on patients that is frequently compared to the disability associated with end-stage hip or knee arthropathy. However, the patho-epidemiology of ankle arthritis diverges significantly from that of the larger weight-bearing joints. While primary osteoarthritis dominates the epidemiological landscape of the hip and knee, the ankle joint is uniquely resistant to primary degenerative changes. Consequently, approximately seventy to eighty percent of ankle arthritis cases are post-traumatic in etiology, stemming from prior rotational ankle fractures, recurrent ligamentous instability, or intra-articular pilon fractures. This post-traumatic predilection means that patients presenting with end-stage ankle arthropathy are often significantly younger and possess higher functional demands than their counterparts requiring hip or knee reconstruction.
The historical evolution of surgical interventions for the arthritic ankle has been characterized by a perpetual tension between joint-sacrificing stability and joint-preserving mobility. For decades, ankle arthrodesis has stood as the gold standard for alleviating the intractable pain of tibiotalar degeneration. By converting a painful, arthritic articulation into a solid, painless osseous block, arthrodesis provides reliable, durable relief. However, this relief comes at the biomechanical cost of sacrificing native tibiotalar kinematics, thereby increasing the compensatory burden placed upon the adjacent subtalar, transverse tarsal, and midfoot articulations. This biomechanical compromise has driven the parallel evolution of Total Ankle Arthroplasty (TAA), which seeks to preserve motion and protect adjacent joints, though historically plagued by higher complication and revision rates compared to fusion.
Furthermore, the management of ankle pathology rarely exists in an isolated osseous vacuum. The surrounding soft tissue envelope, particularly the tendinous structures, frequently exhibits concomitant pathology that must be addressed to achieve optimal surgical outcomes. Surgery for Achilles tendinopathy and peroneal tendinopathy frequently serve as critical adjunctive procedures. A contracted Achilles tendon can exert deleterious deforming forces on the midfoot following an ankle fusion, while degenerative peroneal tendons can exacerbate lateral column instability. Therefore, a comprehensive understanding of foot and ankle interventions requires the surgeon to seamlessly integrate osseous reconstruction with meticulous soft-tissue balancing.
This chapter provides an exhaustive, highly technical exploration of ankle interventions, with a primary focus on the nuanced execution of ankle arthrodesis. We will navigate the complex decision-making matrix required to optimize patient outcomes, detailing the precise surgical anatomy, biomechanical imperatives, and advanced fixation techniques that define modern orthopedic foot and ankle surgery. By mastering these principles, the orthopedic surgeon can reliably navigate the myriad challenges presented by the arthritic and dysfunctional ankle.

Detailed Surgical Anatomy and Biomechanics
A profound mastery of the osseous geometry and ligamentous restraints of the ankle is the absolute prerequisite for any successful surgical intervention. The ankle, or talocrural joint, is a highly congruent, modified hinge joint formed by the distal tibia, the medial and lateral malleoli, and the talar dome. The talus itself is a unique osseous structure; it is largely devoid of muscular attachments, relying entirely on its articular geometry and complex ligamentous tethers for stability, and is covered by articular cartilage over approximately sixty percent of its surface area. The talar dome is wider anteriorly than posteriorly, a geometric reality that dictates the inherent stability of the joint in dorsiflexion as the wider anterior dome wedges into the tibial mortise, tensioning the syndesmotic ligaments.
The ligamentous anatomy of the ankle is traditionally divided into the lateral collateral complex, the medial deltoid complex, and the distal tibiofibular syndesmosis. The lateral complex, comprising the anterior talofibular ligament (ATFL), the calcaneofibular ligament (CFL), and the posterior talofibular ligament (PTFL), primarily resists inversion and anterior translation of the talus. The robust medial deltoid ligament, divided into superficial and deep components, is the primary restraint to valgus tilting and lateral talar excursion. The syndesmosis, consisting of the anterior inferior tibiofibular ligament (AITFL), posterior inferior tibiofibular ligament (PITFL), transverse ligament, and interosseous membrane, maintains the integrity of the mortise. Disruption of any of these complexes alters the contact mechanics of the tibiotalar joint; a mere one millimeter of lateral talar shift can reduce the tibiotalar contact area by up to forty-two percent, exponentially increasing peak contact stresses and precipitating rapid cartilaginous degeneration.
Understanding the normal range of motion and kinematics of the ankle is vital for both joint-preserving and joint-sacrificing procedures. The native ankle joint demonstrates a complex, multi-planar axis of rotation that changes dynamically throughout the arc of motion. Normal physiological range of motion requires dorsiflexion of 0°–20° and plantarflexion of 0°–45°. During normal gait, approximately 10° of dorsiflexion is required during the terminal stance phase to allow the tibia to advance over the plantigrade foot, while 15° to 20° of plantarflexion is utilized during the pre-swing phase for propulsion. When performing an ankle arthrodesis, the surgeon is permanently eliminating this crucial arc of motion.
Consequently, the precise position of the fused ankle is the single most critical determinant of a successful clinical outcome. The universally accepted, non-negotiable position of arthrodesis is defined by three strict parameters: 1. Neutral flexion (0° of dorsiflexion/plantarflexion), 2. 0°–5° of valgus, and 3. 5°–10° of external rotation. Neutral sagittal alignment is paramount; even slight plantarflexion (equinus) results in a functionally longer limb, causing a recurvatum thrust at the knee and severe midfoot overloading, while excessive dorsiflexion leads to a peg-leg gait and heel ulceration. The 0°–5° of valgus is critical because it unlocks the transverse tarsal joint (talonavicular and calcaneocuboid joints), allowing the midfoot to remain flexible and accommodate uneven terrain. Conversely, a varus malunion rigidly locks the midfoot, leading to rapid lateral column overload and adjacent joint arthritis. Finally, the 5°–10° of external rotation mirrors the normal transmalleolar axis and tibial torsion, allowing the foot to clear the contralateral limb during the swing phase of gait.

Exhaustive Indications and Contraindications
The decision to proceed with operative intervention, specifically ankle arthrodesis versus arthroplasty, requires a meticulous synthesis of patient-specific variables, osseous integrity, and functional expectations. The primary indication for ankle arthrodesis is an end-stage arthropathy failing comprehensive conservative management, which typically includes activity modification, non-steroidal anti-inflammatory drugs, rigid ankle-foot orthoses (AFOs), and intra-articular corticosteroid or orthobiologic injections. When these modalities fail to provide acceptable pain relief and functional capacity, surgical intervention is warranted. Arthrodesis remains the most reliable procedure for eliminating pain and providing a stable, durable construct, particularly in young, high-demand laborers or patients with profound deformity.
Beyond primary or post-traumatic osteoarthritis, there are several complex clinical scenarios where ankle arthrodesis remains the undisputed treatment of choice. These include the salvage of a failed total ankle arthroplasty, where significant bone loss and compromised soft tissue envelopes make revision arthroplasty untenable. Tumor reconstruction, requiring massive osseous resection and stabilization, also heavily relies on arthrodesis, often utilizing massive structural allografts or custom metallic cages. Furthermore, arthrodesis is the definitive solution for the sequelae of severe joint infection, particularly tuberculosis or pyogenic arthritis, once the infectious burden has been definitively eradicated.
In patients with profound structural or neurological compromise, arthrodesis offers unparalleled stability. Avascular necrosis (AVN) of the talus, particularly when involving greater than fifty percent of the talar body, frequently leads to catastrophic collapse of the tibiotalar joint. In such cases, a standard tibiotalar fusion may be insufficient, necessitating a tibiotalocalcaneal (TTC) arthrodesis to bypass the necrotic bone. Similarly, patients with neuropathic joints (Charcot arthropathy) or severe neurological conditions resulting in flaccid or spastic instability (e.g., severe Charcot-Marie-Tooth disease, post-polio syndrome, or severe cerebral palsy) require the rigid stabilization that only a robust fusion construct can provide.
Conversely, absolute and relative contraindications must be rigorously respected to prevent catastrophic surgical failures. Active, untreated infection of the ankle joint or surrounding soft tissues is an absolute contraindication to definitive internal fixation and arthrodesis; these must be staged with aggressive debridement, antibiotic spacers, and systemic therapy prior to definitive fusion. A critical relative contraindication is the presence of severe, pre-existing degeneration of the subtalar and midfoot joints. Because an ankle fusion transfers immense biomechanical stress to these adjacent joints, pre-existing arthritis in the subtalar or talonavicular joints will rapidly accelerate and become highly symptomatic post-operatively. In such scenarios, a pantalar arthrodesis or consideration for total ankle arthroplasty (if other criteria are met) must be entertained.
| Parameter | Ankle Arthrodesis (Fusion) | Total Ankle Arthroplasty (TAA) |
|---|---|---|
| Primary Indications | High-demand laborers, severe deformity, failed TAA, AVN of talus, neuropathic joints, neuro-instability, post-infection sequelae. | Low-demand patients, older age (>60), preserved adjacent joint function, minimal coronal/sagittal deformity. |
| Absolute Contraindications | Active local or systemic infection, critical limb ischemia, uncorrectable soft tissue defects. | Active infection, Charcot arthropathy, severe AVN of talus, absent motor function, severe uncorrectable deformity. |
| Relative Contraindications | Severe adjacent joint (subtalar/midfoot) arthritis, bilateral ankle arthritis (due to severe gait impairment). | High BMI, high-impact activities/labor, prior deep joint infection, significant osteoporosis. |
| Expected Outcomes | Reliable pain relief, permanent loss of tibiotalar motion, increased stress on adjacent joints. | Preservation of motion, protection of adjacent joints, risk of polyethelene wear and aseptic loosening. |
Pre-Operative Planning, Templating, and Patient Positioning
Meticulous pre-operative planning is the cornerstone of a successful ankle reconstruction. The clinical evaluation must extend beyond the ankle joint itself to include a comprehensive assessment of the entire lower extremity mechanical axis, from the hip to the forefoot. The surgeon must evaluate the flexibility of the subtalar and transverse tarsal joints, as rigid adjacent joints will poorly tolerate the altered biomechanics of an ankle fusion. A thorough vascular assessment, including palpable pulses and potentially Ankle-Brachial Indices (ABI) or Doppler ultrasonography, is mandatory, as the anterior and lateral surgical approaches rely on robust perfusion for primary wound healing. Neurological assessment is equally critical, particularly evaluating the function of the superficial and deep peroneal nerves, which are at risk during surgical exposure.
Radiographic evaluation begins with high-quality, weight-bearing anteroposterior, lateral, and mortise views of the ankle, supplemented by weight-bearing views of the foot to assess the longitudinal arch and midfoot integrity. Advanced imaging is almost universally required in contemporary practice. Computed Tomography (CT) is invaluable for assessing the exact location and volume of subchondral cysts, determining the remaining viable bone stock, and evaluating the presence of adjacent joint arthrosis that may not be fully appreciated on plain radiographs. Magnetic Resonance Imaging (MRI) is less commonly utilized for routine arthrodesis planning but becomes critical when assessing the viability of the talus (ruling out AVN) or evaluating concomitant soft tissue pathology, such as severe Achilles or peroneal tendinopathy that may require simultaneous surgical management.
Digital or physical templating is a non-negotiable step in the pre-operative workflow. The surgeon must determine the method of joint preparation (e.g., flat cuts versus contouring of the native joint surfaces) and select the appropriate fixation construct. Templating allows the surgeon to anticipate the need for structural bone grafting, particularly in cases of severe coronal plane deformity or post-traumatic bone loss, to prevent unacceptable shortening of the limb. The surgeon must mentally rehearse achieving the optimal position: 1. Neutral flexion, 2. 0°–5° valgus, and 3. 5°–10° external rotation. Anticipating the trajectory of the fixation screws, particularly the "home run" screw from the posterior tibia into the talar neck, ensures maximum bony purchase and biomechanical compression.
Patient positioning in the operating room dictates the ease of surgical exposure and the accuracy of intra-operative fluoroscopy. For an anterior approach, the patient is positioned supine with a bump under the ipsilateral hip to internally rotate the leg to a neutral position, counteracting the natural external rotation of the hip. A radiolucent triangle or bump is placed under the calf to allow the heel to float freely, facilitating manipulation of the ankle into the desired position of fusion. A sterile tourniquet is typically applied to the proximal thigh. The fluoroscopy unit (C-arm) must be positioned to allow unhindered, orthogonal views of the ankle joint without compromising the sterile field. For transfibular or lateral approaches, the patient is positioned in the lateral decubitus position, utilizing a beanbag and rigid pelvic positioners to ensure absolute stability during aggressive osseous resection and compression.

Step-by-Step Surgical Approach and Fixation Technique
The Anterior Surgical Approach
The anterior approach to the ankle is widely favored for primary ankle arthrodesis as it provides excellent, direct visualization of the entire tibiotalar articulation and allows for the preservation of the medial and lateral malleoli, which contribute to rotational stability. The incision is typically centered over the anterior ankle joint, approximately 10 to 15 centimeters in length, following the interval between the extensor hallucis longus (EHL) and the tibialis anterior tendons. Meticulous superficial dissection is critical to identify and protect the superficial peroneal nerve, which frequently crosses the operative field. Deep dissection requires mobilization of the neurovascular bundle (deep peroneal nerve and anterior tibial artery), which is carefully retracted laterally with the EHL and extensor digitorum longus (EDL).
Once the joint capsule is incised and elevated, the surgeon is presented with the arthritic tibiotalar joint. Joint preparation is the most critical technical step; incomplete cartilage removal is the primary culprit in nonunion. Utilizing a combination of osteotomes, curettes, and high-speed burrs, the surgeon meticulously removes all remaining articular cartilage down to bleeding, healthy subchondral bone. It is imperative to preserve the subchondral bone plate as much as possible to prevent subsidence of the talus into the tibial metaphysis. The contour of the native joint (the talar dome and tibial plafond) is often maintained to maximize the bony contact area, though flat saw cuts can be utilized in cases of severe deformity to realign the mechanical axis. Once the surfaces are prepared, the subchondral bone is aggressively fenestrated or "feathered" with a small drill or osteotome to release marrow elements and osteoprogenitor cells into the fusion site, promoting robust osteogenesis.
Fixation Strategies and Biomechanics
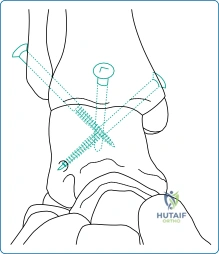
Following meticulous joint preparation and the introduction of local autograft or allograft material, the ankle is provisionally reduced into the optimal position: neutral dorsiflexion, 0°–5° of valgus, and 5°–10° of external rotation. Provisional fixation is achieved with stout Kirschner wires. The surgeon must visually and fluoroscopically verify this position, ensuring the foot is plantigrade relative to the tibia. Once the position is confirmed, definitive fixation is applied. The historical gold standard, and still the most widely used technique, is the three-screw construct utilizing large-fragment (6.5mm or 7.3mm) cannulated screws.
The first screw, often termed the "home run" screw, is typically directed from the posterior aspect of the distal tibia, across the fusion site, and into the dense bone of the talar neck. This screw provides immense compression and resists plantarflexion forces. A second screw is directed from the medial malleolus into the lateral aspect of the talar body, and a third screw is passed from the lateral distal tibia (or through the fibula if a transfibular approach was used) into the medial talar body. This crossing screw configuration creates a highly stable, biomechanically rigid construct that resists multi-planar torsional and bending forces. In cases of osteoporotic bone, revision surgery, or significant bone loss, the surgeon may opt for an anterior locking plate system. These anatomically contoured plates provide rigid fixed-angle stability and allow for robust compression across the fusion site, significantly reducing the risk of hardware failure or loss of reduction in compromised host bone.
Adjunctive Soft Tissue Management
During the surgical intervention, the surgeon must frequently address concomitant soft tissue pathology to ensure the long-term success of the osseous reconstruction. If the patient presents with a severe equinus contracture that prevents achieving neutral dorsiflexion, a percutaneous or open Achilles tendon lengthening (surgery for Achilles tendinopathy/contracture) is mandatory. Forcing the ankle into neutral against a tight Achilles tendon will result in massive compressive forces on the anterior skin flap, leading to catastrophic wound necrosis, and will place excessive strain on the posterior fixation hardware. Similarly, if a lateral transfibular approach is utilized, the surgeon has direct access to the peroneal tendons. Surgery for peroneal tendinopathy, including tenosynovectomy, repair of longitudinal tears, or tenodesis, should be performed concurrently to eliminate lateral pain generators and restore lateral column balance.
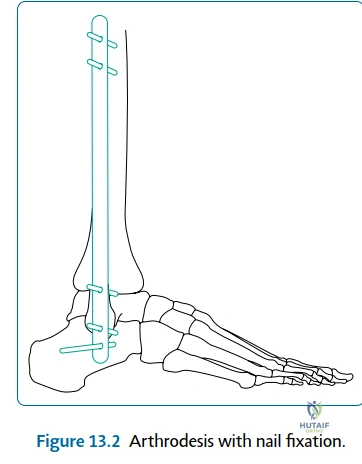
Complications, Incidence Rates, and Salvage Management
Despite meticulous surgical technique and advanced fixation modalities, ankle arthrodesis carries a distinct profile of complications that the orthopedic surgeon must be prepared to manage. The most concerning osseous complication is nonunion (failure of fusion). Historically, and in optimal patient populations, the rate of nonunion is reported at less than 2%. However, in high-risk cohorts—specifically active tobacco smokers, patients with poorly controlled diabetes mellitus, those with profound neuropathy, or those undergoing revision surgery—the nonunion rate can approach 10% to 20%. Nonunions may be asymptomatic, presenting merely as a radiographic lucency, or highly symptomatic, presenting with hardware breakage, recurrent pain, and progressive deformity. Management of a symptomatic nonunion requires a revision arthrodesis, often necessitating the removal of broken hardware, aggressive debridement of fibrous tissue, the use of structural bone grafts (autocrest or allograft), and enhanced fixation, frequently transitioning from screws to rigid plating or an intramedullary TTC nail.
Malunion is an entirely iatrogenic complication resulting from a failure to achieve or maintain the strict positional parameters during surgery. As previously discussed, an equinus malunion results in a recurvatum thrust at the knee and severe midfoot pain, while a varus malunion rigidly locks the transverse tarsal joint, leading to lateral column overload and rapid adjacent joint arthrosis. The treatment for a symptomatic malunion is a challenging corrective osteotomy through the prior fusion mass, realignment of the foot, and rigid re-fixation. This is a technically demanding procedure with a higher risk of subsequent nonunion and wound complications.
The most insidious and inevitable long-term complication of a successful ankle arthrodesis is the development of adjacent joint arthritis. By eliminating motion at the tibiotalar joint, the biomechanical forces of gait are obligatorily transferred to the subtalar, talonavicular, and calcaneocuboid joints. Long-term outcome studies demonstrate that nearly 100% of patients will develop radiographic evidence of adjacent joint arthrosis within 10 to 20 years post-operatively, though clinical symptoms do not always correlate directly with radiographic severity. When conservative management (custom orthotics, bracing, injections) fails to control the pain of adjacent joint arthritis, the salvage procedure involves extending the fusion to include the affected joints, culminating in a subtalar or triple arthrodesis, which further stiffens the foot and alters gait mechanics.
Wound healing complications and deep infections are particularly devastating in foot and ankle surgery due to the tenuous soft tissue envelope. Anterior approaches are prone to delayed healing or dehiscence, particularly if the soft tissues were subjected to excessive retraction or if an equinus contracture was not adequately released. Superficial wound breakdowns can often be managed with local wound care and oral antibiotics. However, a deep infection communicating with the fusion site or hardware requires immediate, aggressive surgical intervention. This entails operative debridement, removal of all hardware (if the fusion is not yet solid, provisional stabilization with an external fixator may be required), placement of antibiotic-impregnated cement spacers, and a prolonged course of culture-directed intravenous antibiotics.
| Complication | Estimated Incidence | Risk Factors | Salvage / Management Strategy |
|---|---|---|---|
| Nonunion (Failure of Fusion) | < 2% (Optimal); up to 20% (High-risk) | Smoking, Diabetes, AVN, Revision surgery, Inadequate cartilage removal. | Revision arthrodesis, bone grafting (autograft/allograft), rigid plate/nail fixation, bone stimulators. |
| Malunion (Varus/Equinus) | 5% - 10% | Poor intra-operative fluoroscopy, failure to release tight Achilles. | Corrective intra-articular or extra-articular osteotomy, realignment, and re-fixation. |
| Adjacent Joint Arthritis | > 80% at 15-20 years | Natural biomechanical consequence of a fused tibiotalar joint. | Custom orthotics/rocker-bottom shoes, intra-articular injections, extension of fusion (Subtalar/Triple). |
| Deep Joint Infection | 1% - 3% | Immunocompromised state, prior soft tissue trauma, prolonged operative time. | Radical irrigation and debridement, hardware removal, antibiotic spacers, external fixation. |

Phased Post-Operative Rehabilitation Protocols
The post-operative rehabilitation following an ankle arthrodesis is a protracted process that demands strict patient compliance and close clinical monitoring. The biological reality of achieving solid osseous union across the dense cortical and subchondral bone of the distal tibia and talus dictates a conservative approach to weight-bearing. The rehabilitation protocol is generally divided into four distinct phases, tailored to the radiographic evidence of healing and the patient's clinical progression.
Phase I encompasses the immediate post-operative period, from day zero to approximately two to three weeks. The primary goals during this phase are wound healing, edema control, and pain management. The patient is placed in a bulky, well-padded posterior splint or a rigid bivalved cast in the operating room. Strict, absolute non-weight bearing (NWB) is mandated. Patients are instructed to keep the operative extremity elevated above the level of the heart as much as possible to mitigate the significant dependent edema characteristic of foot and ankle surgery. Chemical deep vein thrombosis (DVT) prophylaxis is strongly considered during this period of immobility, particularly in patients with additional risk factors.
Phase II begins at the two-to-three-week mark, coinciding with the first post-operative clinic visit and suture removal. If the surgical incisions are well-healed, the patient is transitioned into a rigid, removable Controlled Ankle Motion (CAM) boot or a short-leg fiberglass cast. The strict non-weight bearing status is maintained. The advantage of a removable CAM boot is that it allows the patient to perform gentle, passive range-of-motion exercises of the toes and, crucially, the knee and hip, preventing proximal joint stiffness and muscle atrophy. However, the boot must remain locked and worn at all times, especially during sleep, to protect the fragile, early fibrocartilaginous callus forming at the fusion site.
Phase III represents the critical transition to progressive weight bearing, typically initiated between six and eight weeks post-operatively, entirely contingent upon radiographic evidence of healing. Orthogonal radiographs must demonstrate bridging trabecular bone across at least two, and preferably three, cortices of the fusion site. Once this radiographic milestone is achieved, the patient
Clinical & Radiographic Imaging Archive



