Mastering Tendon Transfers for Median Nerve Palsy: An Operative Guide
Key Takeaway
Welcome to the operating theater, fellows. Today, we're tackling median nerve palsy with precision tendon transfers. This masterclass will guide you through the intricate anatomy, meticulous preoperative planning, and granular intraoperative execution of FDS, ADM, and EIP transfers. We'll cover critical pearls, pitfalls, and comprehensive postoperative management, ensuring you master restoration of thumb opposition and hand function.
Comprehensive Introduction and Patho-Epidemiology
The surgical restoration of function in a hand afflicted by median nerve palsy represents one of the most profound interventions in reconstructive hand surgery. This is not merely an exercise in moving musculotendinous units; it is a complex biomechanical orchestration aimed at returning to the patient the fundamental abilities to pinch, grasp, and interact meaningfully with their environment. The median nerve, often termed the "eye of the hand" due to its critical sensory supply to the radial digits, also serves as the primary motor conduit for thumb opposition and extrinsic flexion of the radial digits. When this nerve is compromised, the resulting functional deficit is devastating, severely crippling the hand's prehensile capabilities. Our goal in this definitive masterclass is to provide a highly professional, immersive, and granular exploration of these intricate tendon transfer procedures, detailing every nuance from preoperative biomechanical assessment to intraoperative execution.
The etiology of median nerve palsy is broad and dictates both the timing and the specific reconstructive strategy employed. In the pediatric population, we frequently encounter congenital or developmental anomalies such as lipofibrohamartoma of the median nerve, or progressive demyelinating conditions like Charcot-Marie-Tooth disease, which unfortunately exhibits a predilection for both the median and ulnar nerves. These pediatric presentations often manifest with insidious, progressive deficits that require careful longitudinal monitoring before surgical intervention is deemed appropriate. Congenital thumb hypoplasia, particularly types II and IIIA, often presents with profound thenar hypoplasia mimicking isolated median nerve motor palsy, necessitating transfers like the Huber (abductor digiti minimi) to restore palmar abduction and opposition.
Conversely, adult etiologies are predominantly traumatic, neoplastic, or compressive in nature. Acute lacerations at the wrist (often secondary to glass injuries or suicide attempts) or proximal forearm (associated with fractures or penetrating trauma) present with immediate, profound sensory and motor deficits. High median nerve injuries, though statistically rarer than their distal counterparts, share similar traumatic etiologies but present a vastly more complex reconstructive challenge due to the loss of extrinsic flexors and pronators. Chronic compressive neuropathies, most ubiquitously severe carpal tunnel syndrome, present an insidious clinical course. These patients progress over months or years, often ignoring the gradual decline in nerve function until profound, irreversible thenar atrophy and loss of opposition have occurred, rendering primary nerve decompression insufficient for functional recovery.
Understanding the pathophysiology of denervation is critical for surgical decision-making. Following a complete nerve transection or severe axonotmesis, the target musculature undergoes progressive atrophy. The motor endplates remain viable for a finite period, generally considered to be 12 to 18 months in adults. If nerve regeneration (either spontaneous or post-neurorrhaphy) does not reach the target muscle within this critical window, irreversible fibrosis and fatty infiltration occur, rendering the muscle permanently non-contractile. In such scenarios, or when proximal nerve injuries make timely regeneration biologically impossible, tendon transfers become the primary reconstructive modality. We must meticulously evaluate the timeline of the injury to determine whether we are performing an "early" transfer (to act as an internal splint while awaiting nerve recovery) or a "late" definitive transfer for irreversible paralysis.
Detailed Surgical Anatomy and Biomechanics
Mastery of tendon transfer surgery is predicated upon an exhaustive understanding of the surgical anatomy and the complex biomechanics of the hand. The median nerve's course through the upper extremity is fraught with potential sites of compression and vulnerability. Entering the forearm between the humeral and ulnar heads of the pronator teres, the nerve gives off critical motor branches to the flexor carpi radialis, palmaris longus, and flexor digitorum superficialis (FDS). Identifying this proximal interval is paramount when addressing high median nerve injuries or when harvesting proximal donor muscles.
Distal to the pronator teres, the anterior interosseous nerve (AION) branches off, traveling along the interosseous membrane to innervate the flexor pollicis longus (FPL), the flexor digitorum profundus (FDP) to the index and long fingers, and the pronator quadratus. A lesion specifically affecting the AION results in the classic inability to form an "OK" sign, while preserving thenar function and sensation. As the main trunk of the median nerve continues distally, it lies nestled in the fascial plane between the FDS and FDP. Approximately 5 centimeters proximal to the wrist crease, it gives off the palmar cutaneous branch, which travels superficial to the transverse carpal ligament to provide sensation to the thenar eminence. Recognizing the origin and course of this branch is vital during volar forearm incisions to avoid painful neuromas.
The biomechanics of thumb opposition represent a marvel of evolutionary engineering. Opposition is not a single, simple movement, but rather a complex, multi-planar synergy consisting of palmar abduction, flexion, and pronation of the first metacarpal at the trapeziometacarpal (CMC) joint. The abductor pollicis brevis (APB) is the primary driver of palmar abduction and internal rotation (pronation). The opponens pollicis (OP) further assists in pronation and flexion of the metacarpal, while the superficial head of the flexor pollicis brevis (FPB) contributes to metacarpophalangeal (MCP) flexion and palmar abduction. It is crucial to remember the high incidence of dual innervation; the deep head of the FPB is frequently innervated by the deep motor branch of the ulnar nerve (Riche-Cannieu anastomosis). This anatomical variant explains why some patients with complete median nerve palsy retain a surprising degree of thumb flexion and weak opposition.
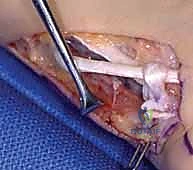
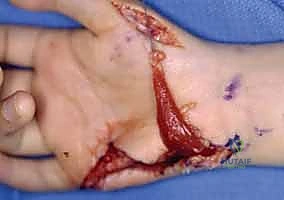
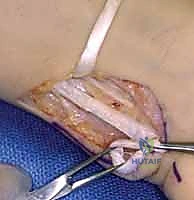
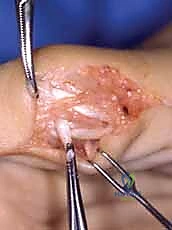
When selecting donor muscles, a profound understanding of their native anatomy, excursion, and neurovascular supply is mandatory. The FDS of the ring finger, our preferred donor for opponensplasty, offers excellent excursion (approximately 3-4 cm) and strength. However, its harvest requires meticulous dissection in the distal forearm to protect the adjacent ulnar neurovascular bundle and the underlying FDP tendons. Alternatively, the extensor indicis proprius (EIP) provides a reliable, expendable donor with a vector that naturally promotes pronation when routed around the ulnar border of the wrist. Harvesting the EIP necessitates careful identification on the dorsum of the hand, recognizing its position ulnar to the extensor digitorum communis (EDC) tendon of the index finger, while meticulously preserving the dorsal sensory branches of the radial nerve.
Exhaustive Indications and Contraindications
The decision to proceed with a tendon transfer for median nerve palsy requires a rigorous, multifaceted evaluation of the patient's biological, mechanical, and psychological status. Tendon transfers are indicated primarily when there is an irreversible loss of motor function that significantly impairs the patient's activities of daily living or occupational capabilities. In the context of low median nerve palsy, the absolute indication is the loss of thumb opposition—specifically the inability to palmar abduct and pronate the thumb to achieve pulp-to-pulp pinch with the ulnar digits. For high median nerve palsy, the indications expand to include the loss of active flexion of the interphalangeal joint of the thumb (FPL), the distal interphalangeal joints of the index and long fingers (FDP), and active forearm pronation.
Timing plays a critical role in the indication algorithm. "Early" tendon transfers may be indicated in high-energy proximal injuries where the anticipated time for nerve regeneration exceeds the viability window of the distal motor endplates (typically >12-18 months). In these scenarios, an early opponensplasty acts as an "internal splint," preventing severe adduction contractures of the first web space and maintaining cortical representation of thumb opposition while awaiting potential nerve recovery. Conversely, "late" transfers are indicated for established, irreversible deficits, such as those seen in neglected severe carpal tunnel syndrome, end-stage Charcot-Marie-Tooth disease, or failed nerve reconstructions.
Contraindications to tendon transfer surgery must be respected to avoid catastrophic functional failures. The most absolute contraindication is a stiff, contracted joint. A transferred tendon possesses only a fraction of its original force and cannot overcome rigid capsular contractures. Therefore, full passive range of motion (PROM) of the thumb CMC and MCP joints is a strict prerequisite. If the first web space is contracted, it must be released—often requiring a Z-plasty, release of the adductor pollicis fascia, or even a trapeziometacarpal capsulotomy—prior to or concurrently with the tendon transfer. Furthermore, the selected donor muscle must possess adequate strength, graded at least M4 on the Medical Research Council (MRC) scale. Transferring a weak muscle will inevitably lead to a weak, non-functional result.
| Category | Specific Factors | Clinical Implications |
|---|---|---|
| Indications (Low Palsy) | Irreversible loss of APB/OP function; Severe thenar atrophy from chronic CTS; Failure of nerve repair > 1 year. | Primary goal is restoration of palmar abduction and pronation for pinch. |
| Indications (High Palsy) | Loss of FPL, FDP (index/long), and pronation; Proximal nerve injuries with prolonged recovery time. | Requires multiple transfers (e.g., BR to FPL, FDP tenodesis, Opponensplasty). |
| Absolute Contraindications | Stiff/contracted thumb CMC or MCP joints; Severe first web space adduction contracture. | Tendons cannot move stiff joints. Requires pre-op therapy or concurrent release. |
| Relative Contraindications | Donor muscle strength < M4; Progressive neurologic disease (e.g., ALS); Poor patient compliance/cognition. | Weak donors fail. Progressive diseases require careful timing and patient counseling. |
Patient compliance and cognitive capacity are frequently overlooked but represent vital relative contraindications. The postoperative rehabilitation protocol following a tendon transfer is rigorous and demands active patient participation for motor relearning and cortical remapping. A patient who is unable or unwilling to adhere to strict splinting protocols and structured hand therapy is at a high risk for transfer rupture, severe adhesions, or failure to integrate the transferred muscle into functional movement patterns. Comprehensive preoperative counseling regarding expectations and the arduous rehabilitation process is therefore mandatory.
Pre-Operative Planning, Templating, and Patient Positioning
Thorough preoperative planning is the bedrock upon which successful tendon transfer surgery is built. The clinical examination must be exhaustive, moving beyond mere diagnosis to a granular assessment of available biomechanical capital. We begin by meticulously documenting the passive range of motion of all relevant joints. The thumb must be easily passively placed into full opposition without resistance. If a supination contracture of the thumb metacarpal exists, it must be addressed. We then systematically evaluate potential donor muscles using the MRC grading system. In cases of isolated median nerve palsy, the radial and ulnar nerve-innervated musculature provides a wealth of potential donors. However, in combined nerve injuries (e.g., median and ulnar palsy, or brachial plexus injuries), the donor pool is severely restricted, requiring highly creative and complex reconstructive strategies.
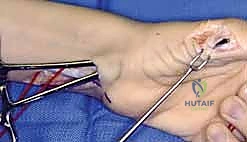
Diagnostic studies, while secondary to the clinical exam, provide essential confirmatory data. Electrodiagnostic studies (EMG/NCS) are invaluable for confirming the extent of denervation and, critically, for assessing the subclinical involvement of potential donor muscles, particularly in systemic neuropathies or compression syndromes. Plain radiographs of the hand and wrist are routinely obtained to rule out underlying osteoarthritis, particularly at the thumb CMC joint. Performing an opponensplasty in the presence of severe basal joint arthritis may exacerbate pain and lead to a poor functional outcome; in such cases, a concurrent CMC arthroplasty or arthrodesis must be considered.
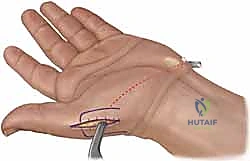
The selection of the specific donor tendon and its routing vector is the true "art" of opponensplasty. For profound loss of opposition, the ideal vector of pull originates from the region of the pisiform, directing the thumb into palmar abduction and pronation. The FDS of the ring finger, routed around the flexor carpi ulnaris (FCU) or through a window in the transverse carpal ligament, perfectly replicates this vector. Alternatively, the EIP transfer (Burkhalter) routed around the ulnar aspect of the wrist provides an excellent vector for pronation, though slightly less palmar abduction than the FDS. For patients with severe carpal tunnel syndrome requiring simultaneous release and transfer, the Camitz procedure (palmaris longus extended with palmar fascia, transferred to the APB) is an elegant, local option, though it primarily restores palmar abduction rather than true pronatory opposition.
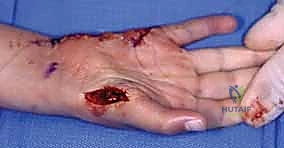
Patient positioning and operating room setup must facilitate unimpeded access and precise execution. The patient is positioned supine with the operative extremity extended on a radiolucent hand table. A pneumatic tourniquet is applied high on the brachium and inflated to 250 mmHg (or appropriately above systolic pressure) following exsanguination to ensure a pristine, bloodless surgical field. This is non-negotiable for the meticulous dissection of fine neurovascular structures and the precise tensioning of tendon weaves. The entire upper extremity is prepped and draped to allow full visualization of the resting cascade of the hand. The surgeon and assistant must utilize loupe magnification (minimum 2.5x, preferably 3.5x to 4.5x) to safely navigate the intricate fascial planes and neurovascular bundles of the distal forearm and hand.
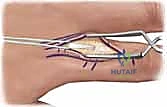
Step-by-Step Surgical Approach and Fixation Technique
The intraoperative execution of an opponensplasty demands meticulous tissue handling, precise routing, and exact tensioning. We will detail the authors' preferred technique: the transfer of the ring finger Flexor Digitorum Superficialis (FDS) to the thumb, utilizing the Flexor Carpi Ulnaris (FCU) as a pulley (modified Bunnell/Riordan technique).
Phase 1: Donor Harvest (FDS of the Ring Finger)
The procedure commences with a transverse or lazy-S incision in the distal palmar crease over the A1 pulley of the ring finger. The subcutaneous tissues are carefully parted to expose the flexor tendon sheath. The A1 pulley is incised longitudinally. Using blunt hook retractors, the FDS tendon is isolated. It is imperative to confirm the identity of the FDS by applying traction and observing proximal interphalangeal (PIP) joint flexion, distinguishing it from the underlying FDP. Once confirmed, the FDS slips are divided as far distally as possible, often requiring division of the chiasm of Camper to maximize tendon length.
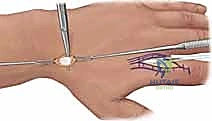
A second, longitudinal or curvilinear incision is made in the volar distal forearm, extending proximally from the wrist crease along the ulnar border of the palmaris longus. The antebrachial fascia is incised, and the FDS muscle belly to the ring finger is identified. Gentle traction on the distal cut end in the palm allows the surgeon to identify the correct tendon in the forearm. The FDS tendon is then carefully withdrawn into the forearm wound. Meticulous care must be taken during this withdrawal to ensure the tendon does not drag adjacent lumbrical muscle tissue or traumatize the median nerve.

Phase 2: Pulley Creation and Tendon Routing
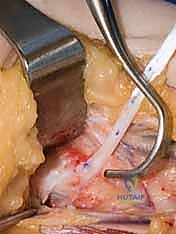
To achieve the optimal vector for opposition (palmar abduction and pronation), the transfer must pull from the ulnar aspect of the wrist, near the pisiform. We utilize the FCU tendon as a dynamic pulley. Through the forearm incision, the FCU tendon is isolated. A longitudinal slit is created in the ulnar half of the FCU tendon, approximately 3-4 cm proximal to its insertion on the pisiform. The harvested FDS tendon is passed through this slit from radial to ulnar, creating a functional loop that directs the vector of pull toward the pisiform.
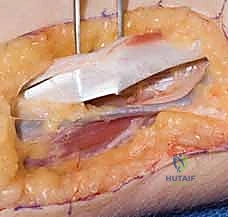
Next, a generous subcutaneous tunnel must be created from the FCU pulley across the palm to the insertion site on the thumb. A longitudinal incision is made over the radial aspect of the thumb MCP joint, exposing the insertion of the APB and the extensor mechanism. A large curved tendon passer or Kelly clamp is passed from the thumb incision, subcutaneously across the palm, to the forearm incision. This tunnel must be wide and superficial to the palmar fascia to prevent any mechanical tethering or bowstringing of the transferred tendon. The FDS tendon is grasped and smoothly drawn through the tunnel to the thumb.
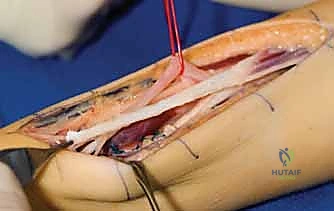
Phase 3: Insertion and Tensioning
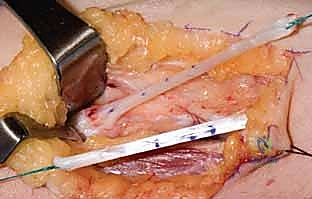
The insertion technique dictates the specific biomechanical outcome. For robust palmar abduction and pronation, we prefer a dual insertion technique (modified Riordan). The FDS tendon is split longitudinally into two slips. One slip is woven through the tendinous insertion of the APB. The second slip is routed dorsally over the APB and woven into the Extensor Pollicis Longus (EPL) tendon over the proximal phalanx. This dual insertion provides a balanced force that abducts the metacarpal while simultaneously extending the IP joint and pronating the entire ray.
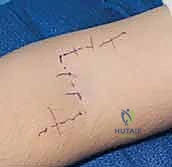
Tensioning is the most critical and unforgiving step of the procedure. The "art" of tensioning requires the surgeon to set the resting length of the muscle-tendon unit to optimize its position on the Blix curve (length-tension relationship). The wrist is positioned in neutral (0 degrees of flexion/extension). The thumb is placed into maximum palmar abduction and full opposition (pulp of the thumb touching the pulp of the long or ring finger). With the thumb held rigidly in this position, maximal tension is applied to the FDS tendon, pulling it completely taut.
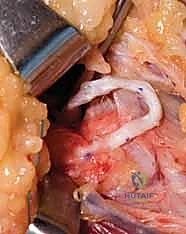
While maintaining this maximal tension, the tendon slips are secured to the APB and EPL using a Pulvertaft weave technique, utilizing 3-0 or 4-0 non-absorbable braided sutures (e.g., Ethibond or Ticron). A minimum of three passes through the recipient tendon is required for biomechanical security. Following fixation, the tourniquet is deflated, and hemostasis is achieved. The tenodesis effect is then tested: passively extending the wrist should cause the thumb to automatically sweep into opposition, while flexing the wrist should allow the thumb to fall into extension and adduction. If the thumb does not oppose with wrist extension, the transfer is too loose and must be re-tensioned.
High Median Nerve Additions
In cases of high median nerve palsy, restoring thumb and finger flexion is required concurrently. The Brachioradialis (BR) is the premier donor for restoring thumb flexion. The BR is harvested in the mid-forearm, aggressively mobilized by releasing its fascial attachments proximally to increase excursion, and woven into the FPL tendon using a Pulvertaft weave. Tensioning here is also critical; the thumb IP joint should rest in slight flexion when the wrist is neutral. To restore index and long finger flexion, we perform a side-to-side tenodesis. The denervated FDP tendons of the index and long fingers are sutured to the intact, ulnar nerve-innervated FDP tendons of the ring and small fingers in the distal forearm, ensuring a harmonious, cascading flexion of all four digits when the ulnar FDPs contract.
Complications, Incidence Rates, and Salvage Management
Despite meticulous surgical technique, tendon transfers for median nerve palsy carry a recognized profile of complications. Understanding these risks, their incidence, and the appropriate salvage strategies is essential for the operating surgeon. Intraoperative complications are relatively rare but can be devastating. Iatrogenic injury to the ulnar neurovascular bundle during FDS harvest, or injury to the radial sensory nerve during EIP harvest, must be avoided through disciplined dissection and the use of loupe magnification. Inadequate mobilization of the donor muscle, particularly the brachioradialis, will result in insufficient excursion and a functionally poor outcome.
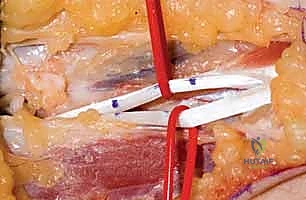
Early postoperative complications primarily revolve around the mechanical failure of the transfer or wound healing issues. Rupture of the tendon anastomosis occurs in approximately 1-3% of cases, almost exclusively due to patient non-compliance with the immobilization protocol or a premature return to heavy lifting. If a rupture is identified within the first few weeks (evidenced by a sudden loss of the restored function and an absent tenodesis effect), immediate surgical re-exploration and repair are mandated. Infection and hematoma formation are mitigated by meticulous intraoperative hemostasis, the use of closed suction drains if necessary, and perioperative prophylactic antibiotics.
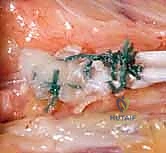
Late complications are more insidious and often relate to the biological healing response and the accuracy of intraoperative tensioning. Adhesion formation along the course of the transferred tendon, particularly where it passes through the fascial pulley or the subcutaneous tunnel, is the most common cause of a suboptimal result. Patients present with restricted excursion despite strong muscle contraction. If intensive hand therapy fails to resolve the adhesions after 4-6 months, a surgical tenolysis may be indicated. Conversely, if the transfer was tensioned too loosely, or if the tendon stretches out over time, the patient will exhibit a weak, incomplete opposition. In such cases, surgical revision to shorten and re-tension the transfer is required.
| Complication Type | Specific Issue | Estimated Incidence | Salvage / Management Strategy |
|---|---|---|---|
| Intraoperative | Nerve injury (Ulnar during FDS; Radial during EIP) | < 1% | Primary microsurgical repair; meticulous prevention is key. |
| Early Post-Op | Tendon Rupture / Pull-out | 1 - 3% | Immediate surgical re-exploration and re-weaving. |
| Early Post-Op | Hematoma / Deep Infection | < 2% | Evacuation, debridement, targeted IV antibiotics. |
| Late Post-Op | Severe Adhesions restricting excursion | 10 - 15% | Aggressive hand therapy; Surgical tenolysis at 4-6 months if refractory. |
| Late Post-Op | Transfer stretch-out (Under-tensioning) | 5 - 10% | Surgical revision to shorten and re-tension the transfer. |
| Late Post-Op | Joint Contracture (Over-tensioning) | 2 - 5% | Prolonged splinting; rarely requires surgical lengthening. |
In the unfortunate event of a catastrophic failure of the tendon transfer—due to irreversible donor muscle weakness, massive scarring, or recurrent rupture—salvage procedures must be considered to provide a stable, functional pinch. The ultimate salvage procedure for a failed opponensplasty is a trapeziometacarpal (CMC) joint arthrodesis. By fusing the thumb metacarpal in a position of palmar abduction and slight pronation, the surgeon provides a rigid, stable post against which the intact ulnar-innervated digits can pinch. While this sacrifices CMC motion, it reliably restores powerful key pinch and grasp, significantly improving hand function in the severely compromised patient.
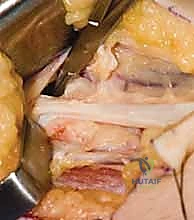
Phased Post-Operative Rehabilitation Protocols
The surgical procedure itself represents only half of the reconstructive journey; the subsequent rehabilitation is equally critical to the ultimate functional outcome. A meticulously executed tendon transfer can easily be ruined by an inappropriate or non-compliant postoperative regimen. The rehabilitation protocol must be phased, structured, and closely supervised by a specialized certified hand therapist (CHT). The immediate postoperative phase (Weeks 0 to 3 or 4) prioritizes the protection of the delicate
Clinical & Radiographic Imaging Archive