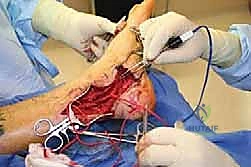
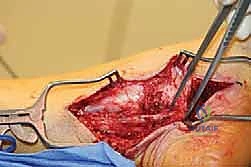
Revision Nerve Decompression and Barrier Procedures for Adhesive Neuralgia
Key Takeaway
Join us in the OR for an immersive masterclass on revision nerve decompression and barrier procedures for adhesive neuralgia. We'll meticulously dissect the posterior tibial, saphenous, superficial peroneal, and sural nerves, focusing on comprehensive anatomy, precise intraoperative techniques, and critical pearls for managing scarred nerves. Learn patient positioning, surgical approaches, and the intricate vein wrap procedure to prevent recurrence.
Welcome to the operating theater, fellows. Today, we're tackling a challenging, yet incredibly rewarding, condition: adhesive neuralgia. This isn't your standard nerve release; we're dealing with nerves scarred down to surrounding tissues, often after prior surgery or trauma. Our goal is to meticulously free these nerves and, in some cases, employ a barrier procedure to prevent recurrence. This requires patience, precision, and a deep understanding of regional anatomy.
Understanding Adhesive Neuralgia: Definition and Pathogenesis
Adhesive neuritis describes the persistent, often debilitating pain emanating from a peripheral nerve that has become tethered or scarred to its surrounding soft tissues. The nerve's natural gliding mechanism, essential for accommodating the dynamic range of motion of the foot and ankle, is severely compromised. This leads to mechanical irritation, impaired nerve conduction, and often a chronic inflammatory state within the epineurium.
While any peripheral nerve in the lower extremity can be affected, the posterior tibial nerve is overwhelmingly the most common culprit, particularly after a prior tarsal tunnel release. The initial surgery, intended to decompress the nerve, can paradoxically lead to a cycle of inflammation and subsequent scar formation, entrapping the very nerve we sought to liberate. Other common etiologies include direct trauma, severe contusions, stretch injuries, surgery on adjacent tendons, or the resection of tumors or cysts. The critical factor is often where the nerve naturally rounds a bend or courses under a retinaculum, making these areas inherently vulnerable to adhesion formation.
The Landscape of Lower Extremity Nerve Entrapment
Let's review the key nerves susceptible to adhesive neuralgia in the lower extremity:
- Posterior Tibial Nerve: This is our primary focus today. It's a continuation of the sciatic nerve, coursing along the medial leg within a discrete retinacular tunnel alongside the posterior tibial artery and vein. As it rounds the medial malleolus, it typically bifurcates into the medial and lateral plantar nerves. The lancinate ligament obliquely crosses this region, a notorious site for primary and recurrent compression. Furthermore, the calcaneal branches, usually one or two, can split from the main trunk or the lateral plantar nerve, and are frequently constricted within the medial soft tissues. More distally, the nerves dive under the abductor hallucis muscle, whose thick lateral fascial covering can become a significant source of mechanical compression.
- Risks: Tarsal tunnel release, trauma, adjacent tendon surgery, tumor/cyst resection.
- Clinical Pearl: The "double crush" phenomenon, where a more proximal nerve compression (e.g., radiculopathy) exacerbates a distal entrapment, is a crucial consideration.
- Saphenous Nerve: This superficial nerve travels anteromedially with the great saphenous vein.
- Risks: Open reduction and internal fixation (ORIF) of the ankle joint, medial malleolus fractures, triple arthrodesis, or any medial ankle surgery, including arthroscopy.
- Superficial Peroneal Nerve: Located in the anterolateral aspect of the leg, it often travels within its own sheath between the anterior intermuscular septum and the lateral muscle compartment fascia. Its most common site of constriction is where it emerges from the deep fascia of the peroneal muscle, typically above the ankle joint, becoming subcutaneous and splitting into two main branches. Its anatomical course in this region is highly variable.
- Risks: Prior surgery or injury to the anterolateral aspect of the leg, especially arthroscopic portals or ORIF of lateral malleolus fractures.
- Sural Nerve: Found in the lateral aspect of the foot and ankle.
- Risks: Surgery on the posterior calcaneus (Haglund deformity), calcaneus fractures, peroneal tendinitis, triple arthrodesis, insertional Achilles tendinitis, and surgery on the base of the fifth metatarsal where it drapes over the bone.
- Deep Peroneal Nerve: This nerve lies along the anterolateral border of the tibia as it approaches the ankle, nestled between the extensor digitorum longus and tibialis anterior muscles. It provides a muscle branch to the extensor digitorum brevis and may send branches to the sinus tarsi before innervating the first web space distally.
- Risks: Entrapment at the anterior ankle retinaculum.
The Pathophysiology of Adhesion
The essential pathophysiology involves the formation of dense scar and fibrinous tissue adhering directly to the nerve epineurium. This scar tissue acts as a mechanical impediment, restricting the nerve's normal longitudinal and transverse excursion during joint motion. This physical impingement can directly impede nerve conduction and compromise the intrinsic vascularity of the nerve, leading to ischemia and further dysfunction. The constant mechanical pull on the nerve, particularly with extremes of limb position, is a profound irritant, manifesting as the characteristic neuralgic pain. The decision to perform a simple nerve release versus a more extensive epineurolysis remains a judgment call, often guided by the gross appearance of the nerve intraoperatively.
Preoperative Planning: Setting the Stage for Success
Fellows, remember, success in revision surgery begins long before the first incision. This is a revision nerve procedure, carrying an inherently greater risk for intrinsic nerve damage, accompanying vessel damage, and prolonged, meticulous dissection.
Patient Assessment and Differential Diagnosis
A thorough patient history is paramount. Patients typically present with a clear event leading to their nerve issues, often a prior surgery. We must differentiate between true adhesive neuralgia and an inadequate initial decompression or an entirely different pathology. A comprehensive medical history, particularly regarding diabetes or other metabolic neuropathies, is essential. Any proximal symptoms, such as sciatica or pain radiating into the posterior thigh, warrant careful evaluation with electromyography (EMG) and nerve conduction studies (NCS) to rule out lumbosacral pathology or a "double crush" syndrome.
On physical examination, assess for gait abnormalities, varus or valgus deformities, and vascular status (dorsal pedal pulses, capillary refill). Palpate for joint issues, synovitis, arthritis, or a palpable mass (ganglion cyst, neurilemmoma). Tinel's sign, elicited by direct percussion over the suspected impingement site, can help pinpoint the area of maximal irritation. For the posterior tibial nerve, palpation around the lancinate ligament and abductor fascia is key, often provoking pain. Increased sensitivity with passive dorsiflexion and eversion of the foot is a hallmark finding, indicating mechanical strain on the nerve adhesions. This mechanical irritation with motion is a strong prognostic indicator for surgical intervention.
Differential Diagnosis Checklist:
* Intrinsic nerve damage (e.g., crush injury)
* Systemic neuropathy (e.g., diabetic neuropathy, leprosy)
* Peripheral vascular disease
* Posterior tibial tendinitis
* Rheumatoid arthritis
* Space-occupying lesions: Ganglion cyst, lipoma, neurilemmoma, giant cell tumor of the tendon sheath, abscess/infection
* Spinal or nerve root pathology (radiculopathy)
* Fracture or malalignment (varus/valgus foot/ankle)
* Tarsal coalition
* Plantar fasciitis
Nonoperative Management Considerations
Before considering surgery, a trial of nonoperative management is usually warranted. This often includes:
* Immobilization: A walker boot or cast can provide significant relief by reducing mechanical strain on the nerve.
* Pharmacologic Management: Anticonvulsants (pregabalin, gabapentin), tricyclic antidepressants (amitriptyline), and benzodiazepines (clonazepam) can modulate neuropathic pain. Referral to a pain management specialist is often beneficial. Systemic anti-inflammatories can help, especially if an arthritic or synovitic component contributes to nerve irritation.
* Topical Agents: Lidocaine patches or gels, ketamine, or anti-inflammatory creams can provide localized relief for superficial nerves. Capsaicin cream can also be effective by modulating nerve signaling.
Imaging and Diagnostic Studies
No single radiologic study is confirmatory for adhesive neuralgia. Their primary role is to rule out alternative pathologies.
* Plain Radiographs: Essential to exclude fracture, severe malalignment, tarsal coalition, arthritis, or bone cysts.
* MRI: May discern underlying mechanical insults such as tendinitis, ganglion cysts, or tumors.
*
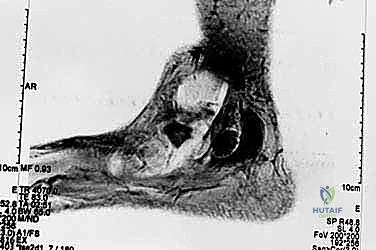
* FIG 1 • MRI of cyst formation along the tibial nerve.
* Ultrasonography: Offers a dynamic assessment similar to MRI, but its diagnostic utility is highly dependent on operator experience.
* EMG and NCS: Crucial for ruling out systemic neuropathy or more proximal lumbosacral pathology. While they may not always confirm tarsal tunnel nerve compression, they are vital for comprehensive evaluation.
Operating Room Setup and Patient Positioning
For these procedures, we need a meticulously prepared environment.
* Tourniquet: We will apply a tourniquet to the proximal thigh. However, I rarely inflate it initially. The ability to identify engorged vessels against scarred tissue without a bloodless field often makes dissection easier. We'll only inflate if severe, uncontrollable bleeding occurs.
* Magnification: Loupe magnification, typically 2.0x, is usually sufficient. For particularly intricate cases or if a more extensive epineurolysis is anticipated, microscopic magnification should be readily available.
* Microsurgical Instruments: Ensure a dedicated microsurgical set is on hand, including fine dissecting scissors, nerve hooks, and micro-forceps. We'll also need finer sutures, such as 8-0 nylon or Prolene, for potential repair of small vascular branches.
* OR Table: A table that allows for elevation and tilting (Trendelenburg position) is helpful to reduce venous congestion in the limb, further aiding visualization.
* Patient Positioning: The patient will be placed supine. We'll use a bean bag positioner or a bump under the contralateral hip. This allows for optimal access to the medial aspect of the foot and ankle, which is our primary operative field. Ensure all bony prominences are meticulously padded to prevent pressure injuries during what can be a lengthy procedure.
* Preoperative Vascular Assessment: Always document a good dorsal pedal pulse before surgery. If there's any doubt, or if the pulse is non-palpable, a preoperative vascular consultation is essential to assess for any compromise.
Intraoperative Masterclass: Revision Nerve Release
Fellows, this is where the art of nerve surgery truly comes into play. The revision nerve release is the most crucial and often the most challenging part of these procedures. The amount and density of scar tissue vary widely, dictating the pace and difficulty of our dissection. Patience is paramount.
The Incision: Navigating Scarred Terrain
- Skin Incision: We will typically utilize the line of the original incision, extending it both proximally and distally to ensure adequate exposure. In cases where the original incision was directed plantar-ward (perhaps for an associated plantar fascia release), and the bulk of the symptoms are related to medial plantar nerve entrapment by the abductor fascia, our revision incision may need to curve anteriorly, angling away from the original cut. The skin in this region is generally well-vascularized, and sharp angles rarely pose healing problems. Remember, an extensile exposure is always preferable to struggling in a confined space.
- Initial Superficial Dissection: The initial skin incision should be superficial, especially distally where the nerve moves more medially and superficially near the lancinate ligament. We want to avoid inadvertently transecting superficial nerve branches or encountering unexpected scar tissue immediately.
Meticulous Deep Dissection: Unveiling the Nerve
-
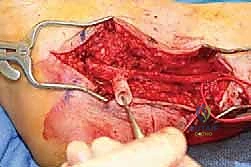
Accessing the Tarsal Tunnel: Once through the skin and subcutaneous tissue, we begin our deep dissection. I prefer to start more proximally in "virgin" tissue, away from the densest scar. This allows us to identify the normal anatomy of the posterior tibial nerve and its accompanying vessels before encountering the scarred segment. This proximal identification provides a critical roadmap.
- Blunt Dissection: Using a combination of dissection scissors and gentle blunt clearing, we'll carefully visualize the fascia overlying the flexor digitorum longus tendon. Look for a characteristic band of yellow fat; this often marks the location of the tarsal tunnel beneath the deep fascia.
- Fascial Incision: Now, carefully incise the deep fascia of the tarsal tunnel. This release should extend both proximally and distally, ensuring complete decompression of the nerve and its branches.
- Nerve Isolation: With the fascia released, we can begin to isolate the posterior tibial nerve.
-
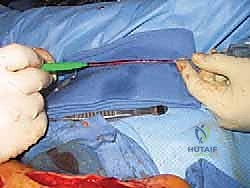
Managing the Neurovascular Bundle: The posterior tibial nerve is intimately associated with a complex venous plexus and the posterior tibial artery and veins.
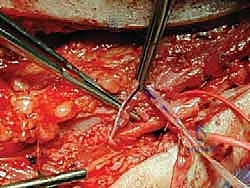
* TECH FIG 1 • Dissection of the tarsal tunnel is facilitated by the bipolar forceps.
* Venous Plexus: The posterior tibial nerve often has a dense venous plexus surrounding it. This can be stripped away gently, but anticipate some bleeding. Larger vessels will send small branches directly to the nerve; these may require careful cauterization or, if larger, ligation with fine suture.
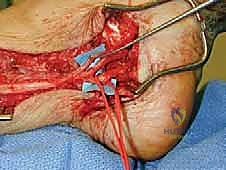
* Separation of Structures: Meticulously separate the nerve from the artery and veins. This is where patience pays off.
* Tourniquet Strategy: As I mentioned, I prefer not to inflate the tourniquet unless severe bleeding occurs. The vessels, when full, are often easier to identify and differentiate from nerve tissue within the scar. However, if persistent or vigorous bleeding, particularly from the venous plexus around the medial plantar nerve, obscures our view, a brief inflation of the tourniquet may be necessary to achieve better dissection and cauterization.
* Vessel Loops: Small vessel loops are invaluable here. They allow us to gently retract the vessels and manipulate the nerves without direct trauma, providing better visualization of the scarred planes.
Distal Decompression and Epineurolysis
- Extending the Release: Our dissection must extend proximally above the ankle joint and distally beyond the lancinate ligament and, critically, under the abductor hallucis muscle.
- Abductor Fascia Release: The abductor hallucis muscle can be remarkably thick and restrictive to the medial and lateral plantar nerves. Using a small hemostat or a blunt dissector, gently slide it along the nerve's course, ensuring a complete release of the investing abductor fascia. You should feel the soft tissues "yield easily" as the nerve is freed.
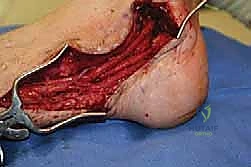
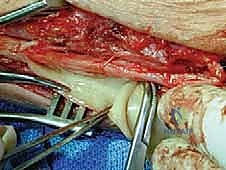
* TECH FIG 3 • Typical scarring of the medial plantar nerve as it courses under the abductor fascia.
- Epineurolysis Decision: Once the nerve is completely decompressed from extrinsic compression and scar, we assess its intrinsic health. If the nerve appears grossly scarred but then "blanches" or appears healthy after the extrinsic release, a formal epineurolysis (incision of the epineurium) may not be necessary. However, if the nerve remains constricted or discolored, an epineurolysis may be considered to free the internal fascicles. There are no conclusive studies definitively guiding this decision; it remains a judgment call based on intraoperative findings and the surgeon's experience.
Pearls and Pitfalls During Nerve Release
- Pitfall: Inadvertent nerve injury from aggressive dissection or thermal damage from cautery.
- Pearl: Always identify the nerve proximally in virgin tissue first. Use bipolar cautery on a low setting, keeping it away from the nerve. Maintain constant visualization of the nerve and its branches.
- Pitfall: Incomplete release, leading to persistent symptoms.
- Pearl: Ensure complete release of all compressive structures: lancinate ligament, abductor fascia, and any other fibrous bands. Follow the nerve and its branches distally until they are entirely free. Use a nerve hook to gently lift and inspect the nerve's entire circumference.
- Pitfall: Significant bleeding obscuring the field.
- Pearl: Have vessel loops ready. Use local pressure with sponges. If necessary, inflate the tourniquet for a brief period to gain control, but deflate as soon as possible to allow for vessel identification.
- Pitfall: Missing an associated pathology (e.g., small ganglion cyst intimately associated with the nerve).
- Pearl: Be thorough. Explore the entire length of the nerve and surrounding tissues. If MRI suggested a lesion, confirm its presence or absence.
The Barrier Procedure: Vein Wrap Technique
Once the nerve is meticulously decompressed, the critical next step is to prevent the recurrence of adhesions. One effective barrier procedure is the autologous vein wrap. This utilizes a segment of the patient's own saphenous vein to encase the freed nerve, providing a biological, non-constrictive barrier against scar ingrowth.
Harvesting the Saphenous Vein
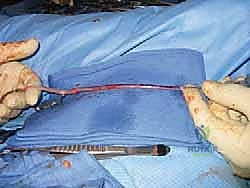
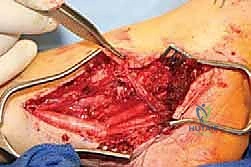
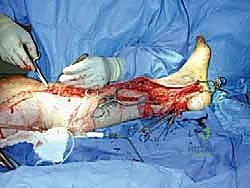
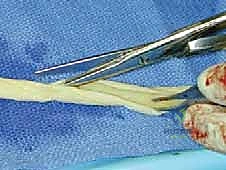
- Harvest Site: We'll harvest a segment of the great saphenous vein from the ipsilateral lower extremity, typically from the thigh or knee region.
- Incision: This can be done via multiple skip incisions or a single, longer incision, depending on the required length and surgeon preference. For maximum length, extending to the knee region is often ideal. If you're less familiar with vein harvest, don't hesitate to consult with our cardiovascular surgical technicians; they perform these daily.
* Image: Saphenous vein harvest.
3. Side Branch Ligation: As we harvest the vein, meticulously ligate all small side branch vessels. This is crucial to allow for later
Additional Intraoperative Imaging & Surgical Steps
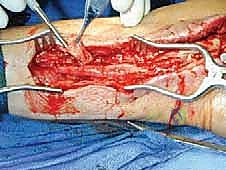
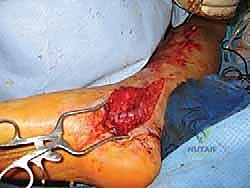
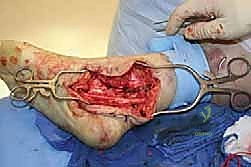
REFERENCES
-
Easley ME, Schon LC. Peripheral nerve vein wrapping for intractable lower extremity pain. Foot Ankle Int 2000;21:492–500.
-
Kinoshita M, Okuda R, Morkikawa J, et al. The dorsiflexion-eversion test for diagnosis of tarsal tunnel syndrome. J Bone Joint Surg Am 2001;83A:1835–1839.
-
Schon LC, Anderson CD, Easley ME, et al. Surgical treatment of chronic lower extremity neuropathic pain. Clin Orthop Relat Res 2001;289:156–164.

You Might Also Like