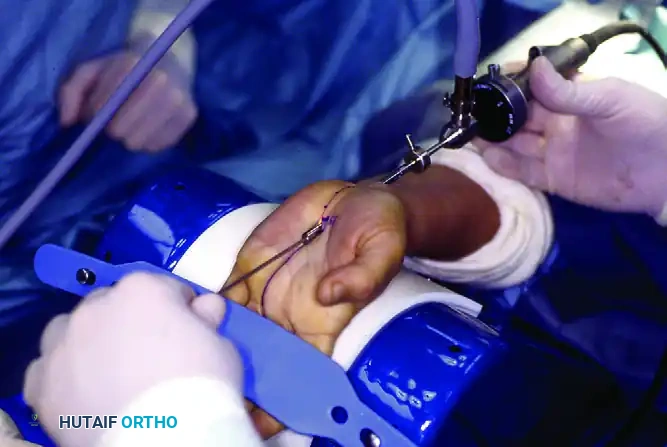
Ulnar Nerve Decompression at Guyon's Canal: An Intraoperative Masterclass
Key Takeaway
This masterclass details ulnar nerve decompression at Guyon's Canal, from intricate anatomy to real-time surgical execution. Fellows learn patient positioning, precise incision, meticulous neurovascular bundle dissection, and management of various compressive pathologies. We cover critical pearls, potential pitfalls, and comprehensive postoperative rehabilitation, ensuring optimal patient outcomes and surgical proficiency.
Alright team, gather around. Today, we're going to perform a decompression of the ulnar nerve at Guyon's Canal. This is a common yet intricate procedure, and understanding the nuances is paramount to achieving excellent patient outcomes. This isn't just about cutting; it's about respecting the anatomy, anticipating challenges, and executing with precision.
Understanding the Pathology: Ulnar Nerve Entrapment at the Wrist
The ulnar nerve, as you know, is a critical component of hand function. When patients present with symptoms of ulnar nerve dysfunction, our first task is to precisely identify the site of compression. While the cubital tunnel at the elbow is the most common site, Guyon's canal at the wrist is the second most frequent location for ulnar nerve entrapment.
Symptoms can be purely motor, purely sensory, or a combination of both, depending entirely on where and how the nerve is being compressed. This is where your detailed anatomical knowledge becomes indispensable.
Comprehensive Surgical Anatomy of the Ulnar Nerve at the Wrist
Let's review the critical anatomy we'll encounter. In the distal half of the forearm, the ulnar nerve is closely accompanied by the ulnar artery on its lateral side, forming a neurovascular bundle. Proximally, before the nerve even reaches the wrist, it gives off a crucial dorsal sensory branch. This branch provides sensation to the dorsum of the wrist and the ulnar side of the hand. It's vital to remember that this dorsal cutaneous branch usually bifurcates before the nerve enters Guyon's canal, which has significant implications for our incision planning.
The main trunk of the ulnar nerve then continues into the hand, passing directly through Guyon's canal.
Guyon's Canal: A Detailed Look
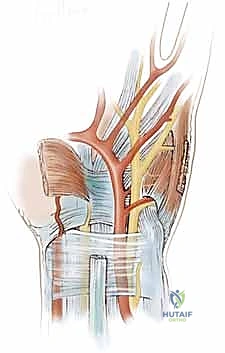
Guyon's canal itself is a triangular, fibro-osseous tunnel situated at the base of the ulnar side of the palm. It measures approximately 4 cm in length, extending from the proximal edge of the palmar carpal ligament to the fibrous edge of the hypothenar muscles. This space functions as a physiologic tunnel with distinct anatomical borders:
- Lateral Wall: Formed by the hook of the hamate and the robust transverse carpal ligament.
- Medial Wall: Composed of the pisiform bone and the attachments of the pisohamate ligament.
- Floor: Primarily the transverse carpal ligament and the pisohamate ligament.
- Roof: The palmar carpal ligament, which is a superficial thickening of the deep fascia, and the palmaris brevis muscle.
Both the ulnar nerve and the ulnar artery, along with their accompanying veins, pass through this canal to enter the hand.

FIG 1 • A. Anatomic landmarks of the distal ulnar tunnel (Guyon’s canal).
Ulnar Nerve Branches within Guyon's Canal: The Zone System
To better correlate clinical symptoms with the specific pathology, we divide Guyon's canal into three distinct zones:
-
Zone 1 (Proximal): This zone, about 3 cm in length, is the area proximal to the bifurcation of the ulnar nerve into its motor and sensory branches. Compression here typically results in a combined motor and sensory loss because the nerve is still undivided. Common culprits in Zone 1 include fractures of the hook of the hamate or ganglion cysts originating from the pisotriquetral joint. Idiopathic compression can also occur due to thickening of the proximal fibrous ligament at the canal's entrance.
-
Zone 2 (Motor Branch): Located next to Zone 3, this zone encompasses the deep motor branch of the ulnar nerve. This motor branch, along with the deep branch of the ulnar artery, courses dorsoradially within the tunnel, passing between the abductor digiti quinti and the flexor digiti quinti brevis, eventually perforating the opponens digiti quinti. It then follows the deep volar arch across the palm to innervate a wide array of intrinsic hand muscles:
- The three intrinsic muscles of the small finger: abductor digiti quinti, flexor digiti quinti brevis, and opponens digiti quinti.
- The third and fourth lumbricales.
- All volar and dorsal interossei.
- The adductor pollicis.
- The deep head of the flexor pollicis brevis.
Compression in Zone 2 causes pure motor loss to all these ulnar-innervated muscles in the hand. Ganglions, particularly from the pisotriquetral joint, and fractures of the hook of the hamate are the most common etiologic factors.
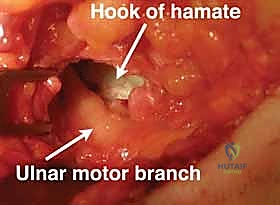
FIG 1 • C. The proximity of the motor branch of the ulnar nerve to the hook of the hamate as seen during excision of the hook.
Critical Note: Due to the motor branch's close proximity to the hook of the hamate, it is unfortunately easy to damage this nerve segment during excision of the hamate hook. Extreme caution is warranted.
- Zone 3 (Sensory Branch): Situated ulnar to Zone 2, this zone encompasses the superficial or sensory branch of the bifurcated ulnar nerve. This superficial branch supplies the palmaris brevis muscle and provides sensation to the hypothenar eminence, the small finger, and the ulnar side of the ring finger. Compression here typically causes pure sensory loss in this distribution, but usually spares motor function. Common causes include aneurysm or thrombosis of the ulnar artery, and synovial inflammation.
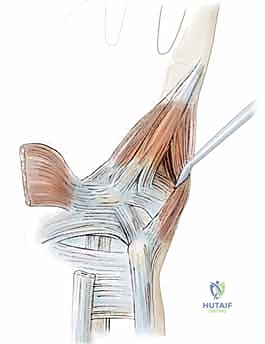
FIG 1 • B. Location of the three zones. Zone 1 is proximal to the bifurcation; zone 2 encompasses the motor branch; zone 3 is the region surrounding the sensory branch.
Nerve Anomalies that Can Confuse Diagnosis:
- Martin-Gruber anastomosis: In the forearm, fibers destined for the intrinsic hand muscles are carried within the median nerve and then cross over to join the ulnar nerve in the middle of the forearm. If present, this anomaly means that even with a high ulnar nerve injury (proximal to the anastomosis), some intrinsic muscle function may be preserved, complicating localization.
- Riche-Cannieu anastomosis: This connection between the median and ulnar nerves occurs in the palm. Similar to Martin-Gruber, it can allow some intrinsic function to remain even with an ulnar nerve injury at the wrist.
Pathogenesis and Etiology of Compression
The causes of ulnar nerve compression in Guyon's canal are diverse. Repeated blunt trauma, such as from power tools, gripping, or hammering with the palm, can lead to thrombosis or aneurysm of the ulnar artery, subsequently compressing the nerve—a condition known as "hypothenar hammer syndrome." Direct, sustained pressure, like that experienced during cycling or prolonged typing with wrist extension, can also be causative.

FIG 2 • A. Ulnar artery thrombosis.
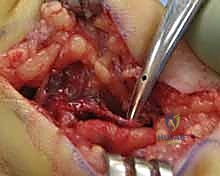
FIG 2 • B. Resected thrombosed segment.
Other etiologies include:
* Soft Tissue Masses: Ganglia (from the pisotriquetral joint or other carpal joints), lipomas, or other benign tumors. These are responsible for a significant percentage (32% to 48%) of ulnar tunnel syndromes.
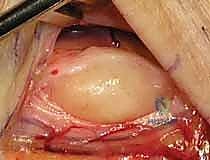
FIG 2 • C. Hypothenar mass as a cause of compression of the ulnar nerve at the wrist.
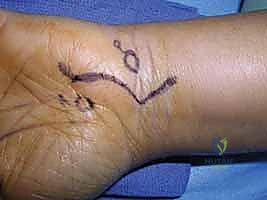
FIG 2 • D. Lipoma causing compression of the nerve.
* Anomalous Muscle Bellies: Such as an accessory abductor digiti minimi or hypertrophy of the palmaris brevis. These account for about 16% of cases.
* Osteological Issues: Fractures of the hook of the hamate or distal radius fractures (due to swelling or malunion).
* Inflammatory Conditions: Synovitis secondary to rheumatoid arthritis, gout, tenosynovitis, or edema from burns.
* Iatrogenic Causes: Compression following tendon or muscle transfers (e.g., Huber opponensplasty).
* Vascular Conditions: Ulnar artery thrombosis or pseudoaneurysm.
* Coexistent Carpal Tunnel Syndrome: Compression at Guyon's canal can occur simultaneously with carpal tunnel syndrome, often resolving after carpal tunnel decompression.
* Systemic Conditions: Diabetes, alcoholism, or hypothyroidism can predispose to neuropathies.
* Double-Crush Syndrome: A proximal lesion (e.g., at the cubital tunnel or cervical spine) can make the nerve more susceptible to compression distally at Guyon's canal.
Clinical Evaluation: History and Physical Examination
A thorough clinical evaluation is paramount. Always remember, the ulnar nerve can be compressed at multiple levels: the cervical spine, the thoracic outlet, the elbow (cubital tunnel), or the wrist (Guyon's canal).
Clinical History:
* Presenting Symptoms: Can range from mild, transient paresthesias in the ring and small fingers to severe intrinsic muscle atrophy and clawing of these digits.
* Pain: Patients may report severe pain at the elbow or wrist radiating into the hand, or even proximally into the shoulder and neck.
* Functional Impairment: Difficulty with fine motor tasks, clumsiness when opening jars or turning doorknobs. Early fatigue or weakness with repetitive hand motions.
* Environmental Factors: Cold intolerance in the ring and small fingers, especially in certain climates or work conditions.
* Symptom Pattern: Determine if symptoms are transient or continuous, related to work, sleep, or recreation. Elicit duration and any possible relation to trauma.
* Occupational History: Ask about vibration exposure, repetitive blunt trauma, prolonged wrist extension (typing, cycling).
Physical Examination:
* Proximal to Distal Approach: Always begin the examination at the neck and shoulder, systematically moving down the affected extremity to the elbow and then the wrist.
* Neck: Pain on neck movement mimicking symptoms suggests cervical disc disease.
* Shoulder/Brachial Plexus: Palpate the plexus, assess shoulder motion for brachial plexus pathology or Pancoast tumor. Assess provocative maneuvers for thoracic outlet syndrome.
* Arm: Look for masses on the medial side of the arm (soft tissue tumor, hemorrhage).
* Elbow: Note any deformity, palpate the ulnar nerve in the cubital tunnel, and assess for abnormal mobility (subluxation). Assess strength of the flexor carpi ulnaris and flexor digitorum profundus (to the ring and small fingers) to help differentiate cubital tunnel from Guyon's canal compression, as these are innervated proximal to the wrist.
* Forearm and Wrist: Palpate the course of the nerve in the forearm all the way to the wrist.
* Tinel's/Phalen's: A positive Tinel's sign (eliciting paresthesias with percussion) or Phalen's sign (wrist flexion for 60 seconds) over the ulnar nerve at the wrist is often found.
* Tenderness: Tenderness over the hook of the hamate is a particularly important finding, suggesting fracture or a mass in Zone 2.
* Hand:
* Sensory Function: Assess sensation in the ulnar nerve distribution (hypothenar eminence, small finger, ulnar half of ring finger). Semmes-Weinstein monofilament testing may be abnormal, but often normal early. Two-point discrimination usually becomes abnormal only late in the disease course.
* Motor Function/Intrinsic Muscles:
* Ask the patient to cross the long finger over the index finger (crossed finger test) to assess interossei.
* Abductor Digiti Quinti (ADQ): This is one of the two muscles that can be accurately tested in the hand for ulnar nerve function. Palpate or visualize its belly.
* First Dorsal Interosseous (FDI): The other accurately testable intrinsic muscle.
* Froment's Sign: Assess weakness of thumb pinch. A positive Froment's sign occurs if the patient must flex the thumb interphalangeal joint (via the median-innervated flexor pollicis longus) to maintain a strong pinch, indicating adductor pollicis weakness.
Imaging and Other Diagnostic Studies
- Radiographs: Mandatory for ulnar nerve compression to rule out skeletal pathology and multi-level entrapment.
- Hand and Wrist: Standard AP, lateral, and oblique views, plus carpal tunnel views. Look for hook of hamate fractures, carpal dislocations, soft tissue masses, or calcifications.
- Elbow: Abnormal anatomy (valgus deformity), bone spurs, shallow olecranon groove, osteochondromas, destructive lesions.
- Neck: If cervical disc disease is suspected, rule out cervical ribs.
- Chest: If Pancoast tumor or tuberculosis is suspected.
- Ultrasonography: Useful for detecting cysts or masses in Guyon's canal and can assess ulnar nerve diameter at the elbow, though less specific for Guyon's.
- MRI: Not always necessary, but invaluable for further delineation of soft tissue masses (lipomas, ganglions), visualization of fractures, aneurysms, congenital abnormalities, or fibrous bands compressing the nerve.
- Electromyography (EMG) and Nerve Conduction Studies (NCS): These are critical to confirm the specific area(s) of entrapment and document the extent of pathology.
- Motor and Sensory Conduction Velocities: More useful in recent entrapments.
- EMG: Useful in chronic neuropathies, showing axonal degeneration (e.g., fibrillation potentials, fasciculations), and assessing motor unit morphology and recruitment patterns. It also helps expand the differential diagnosis by checking muscle membrane integrity.
- Conduction Velocity Short-Segment Stimulation (Inching Technique): Increases sensitivity and improves localization by pinpointing the exact site of blockage.
Nonoperative Management
Conservative treatment is most successful for transient paresthesias.
* Patient Education: Crucial for understanding the condition and modifying activities.
* Activity Modification: Avoiding vibrating or power tools, repetitive blunt trauma, prolonged wrist extension (typing, cycling).
* Ergonomic Correction: Adjusting workstations to maintain a neutral wrist position.
* Wrist Splinting: In a neutral position, especially at night.
* Medications: Nonsteroidal anti-inflammatory drugs (NSAIDs) for nerve irritation. Oral vitamin B6 supplements for mild symptoms (6-12 weeks trial).
Indications for Surgical Management
Surgical intervention is indicated when:
* Paresthesias persist or worsen despite adequate conservative treatment.
* Abnormal nerve conduction studies or EMGs confirm significant entrapment.
* There are any signs of motor changes (weakness, atrophy).
* In cases of immediate, complete ulnar nerve injury secondary to a wrist fracture: the fracture should be reduced as soon as possible. If ulnar nerve function does not improve within 24-36 hours following satisfactory reduction, immediate exploration and decompression are warranted.
Preoperative Planning: The Roadmap to Success
Before we even think about making an incision, meticulous planning is essential.
Confirming the Diagnosis
- EMG/NCS and Imaging: The diagnosis must be confirmed with electrodiagnostic studies and/or imaging (MRI) to precisely localize the compression and rule out other pathologies.
- Differential Diagnosis Review: Always consider the broad differential:
- Cervical disc disease
- Brachial plexus abnormalities, thoracic outlet syndrome, Pancoast tumor
- Elbow abnormalities, cubital tunnel syndrome, epicondylitis
- Systemic conditions: infections, tumors, diabetes mellitus, hypothyroidism, rheumatoid diseases, alcoholism
- Wrist fractures
- Ulnar artery aneurysms or thrombosis at the wrist
Patient Positioning and Setup
Our patient is already positioned, but let's review the setup.
- Supine Position: The patient is supine on the operating table.
- Armboard Extension: The affected arm is extended on a specialized hand table or armboard, ensuring full access to the wrist and distal forearm. We need to ensure the arm is comfortably abducted and externally rotated, allowing for optimal visualization and instrument maneuverability.
- Tourniquet Placement: A pneumatic tourniquet is placed high on the upper arm, above the elbow. We'll inflate it to 250 to 265 mm Hg just before the incision to ensure a bloodless field, which is crucial for nerve identification and protection.
- Draping: The arm is draped to the shoulder, allowing for full range of motion of the wrist and fingers during the procedure, if needed, and to ensure sterility.
Intraoperative Execution: Ulnar Nerve Exploration and Decompression of Guyon’s Canal
Alright fellows, let's scrub in. We're aiming to explore and decompress the ulnar nerve from the distal forearm, through Guyon's canal, and into the hand, addressing all three zones.
Step 1: Anatomical Landmarks and Incision Planning
First, let's re-identify our key landmarks.
* Pisiform: Palpate and mark the pisiform bone. This is our medial anchor.
* Hook of Hamate: The hook of the hamate is located approximately 1 cm distal and lateral to the pisiform. This is our lateral anchor.
Now, let's plan our incision. Precision here is critical to avoid nerve injury and minimize scar contracture.
- Curvilinear Incision: We will make a curvilinear incision.
- Distal Start: Begin distally in the interval between the pisiform and the hook of the hamate.
- Proximal Extension: Cross the wrist in a gentle zigzag fashion, extending proximally to just beyond the distal wrist flexion crease.
- Radial Border of FCU: Continue the proximal extension along the radial border of the flexor carpi ulnaris (FCU) tendon.
TECH FIG 1 • A. Curvilinear incision for decompression of the ulnar nerve at Guyon’s canal.
Surgical Warning: The incision should not be carried ulnarly over the hypothenar eminence. This is to avoid injury to the palmar cutaneous branch of the ulnar nerve, which can cause painful neuromas or sensory deficits. Furthermore, the zigzag pattern over the wrist crease is essential to prevent longitudinal scar contracture, which can limit wrist motion postoperatively.
Step 2: Skin and Subcutaneous Dissection
- Initial Dissection: Using a #15 blade, make a precise skin incision along our markings.
- Subcutaneous Layer: Carefully dissect through the subcutaneous tissue. You'll encounter the palmaris brevis muscle just beneath the skin in the hypothenar region. We will incise this muscle and the overlying fibrous tissue as we proceed.
- Hemostasis: Maintain meticulous hemostasis with bipolar cautery to ensure a clear field. Avoid excessive cautery near the nerve.
Step 3: Proximal Nerve Identification and Distal Tracing (Zone 1 Decompression)
Now, we'll begin our deep dissection, working from proximal to distal. This approach is safer as the nerve is less compressed and typically easier to identify proximally.
- Identify Ulnar Nerve Proximally: Carefully identify the ulnar nerve proximal to the distal wrist flexor retinaculum, along the radial border of the FCU tendon. It lies just ulnar to the ulnar artery. Use fine dissecting scissors and blunt dissection with a nerve hook or small blunt probe.
- Neurovascular Bundle: Once identified, gently trace the neurovascular bundle distally. It will lead us directly to the point where it enters Guyon’s canal beneath the palmar carpal ligament.
- Decompressing Zone 1: We need to incise the palmar carpal ligament, the palmaris brevis muscle, and any other constricting fibrous tissue forming the roof of Zone 1. Use a small, blunt-tipped dissecting scissor or a scalpel with the blade facing away from the nerve.
- Technique: Introduce a nerve hook or a small, blunt dissector under the ligament to protect the nerve, then incise the ligament longitudinally. Extend this incision proximally as far as necessary to ensure complete decompression of Zone 1.
- Reflecting FCU and Pisohamate Ligament: Reflect the flexor carpi ulnaris tendon radially if necessary, and carefully incise the pisohamate ligament, which forms part of the medial wall and floor of the canal. This opens up the canal and allows for better visualization.
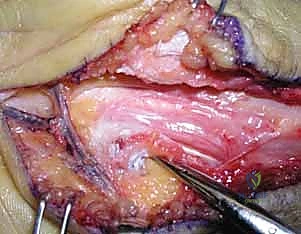
TECH FIG 1 • B. Decompression of the ulnar nerve along its entire course through Guyon’s canal.
Step 4: Examination of the Ulnar Artery and Nerve
With the canal opened, we can now thoroughly examine the neurovascular bundle.
- Ulnar Artery Assessment: Carefully inspect the ulnar artery for any signs of thickening, thrombosis, or aneurysm. If thrombosis or an aneurysm (as seen in hypothenar hammer syndrome) is present, this may require a vascular surgeon's consultation for resection and possible reconstruction, or simply ligation if collateral flow is sufficient.
- Ulnar Nerve Assessment: Examine the ulnar nerve along its entire course for any intra- or extraneural tumors (e.g., schwannoma, neurolemmoma), anomalous muscle bellies, or ganglion cysts.
Step 5: Exploration of the Canal Floor and Zone-Specific Decompression (Zones 2 & 3)
Now, we'll continue our meticulous dissection distally, ensuring complete decompression through Zones 2 and 3, and identifying the nerve branches.
- Floor Exploration: Further explore the floor of the canal to identify any hidden masses, ganglions, or anomalous muscles that might be causing compression. These must be carefully excised.
- Ganglion Excision: If a ganglion cyst is present, meticulously dissect it from the surrounding tissues, tracing its stalk to its origin (often the pisotriquetral joint) and excising it completely.
- Anomalous Muscles/Lipomas: Excise any hypertrophic or anomalous muscle bellies or lipomas.
- Identifying and Protecting Branches: This is perhaps the most delicate part of the procedure.
- Hypothenar Branches: Identify the ulnar nerve branches supplying the hypothenar muscles (abductor digiti quinti, flexor digiti quinti brevis, opponens digiti quinti). These typically arise from the deep motor branch.
- Palmaris Brevis Branch: The superficial sensory branch gives off a small branch to the palmaris brevis muscle.
- Deep Motor Branch (Zone 2): Carefully trace the deep motor branch as it dives dorsoradially. This is the segment most vulnerable during hamate hook excision. Ensure it is completely free of compression from any fibrous bands or the fibrous arch of the hypothenar muscles.
- Superficial Sensory Branch (Zone 3): Trace the superficial sensory branch distally. Ensure it is decompressed from any overlying structures.
Surgical Warning: When excising the hook of the hamate (if indicated for fracture or impingement), extreme care must be taken to protect the deep motor branch of the ulnar nerve. It lies in very close proximity. Use fine instruments and visualize clearly. Consider using a small, curved osteotome or a rongeur, always protecting the nerve with a broad retractor.
Step 6: Final Inspection and Irrigation
- Complete Decompression: Once all potential compressive structures (ligaments, fibrous bands, muscles, masses, vascular anomalies) have been addressed, visually confirm that the entire
REFERENCES
References 1. Agarwal Sk, Schneider Lb, Ahmad Bk. Clinical Usefulness Of Ulnar Motor Responses Recording From First Dorsal Interosseous. Muscle Nerve 1995;18:1043.
-
Aguiar Ph, Bor-Seng-Shu E, Gomes-Pinto F, Et Al. Surgical Management Of Guyon’S Canal Syndrome, An Ulnar Nerve Entrapment At The Wrist: Report Of Two Cases. Arq Neuropsiquiatr 2001;59:106–111.
-
Bartels Rh, Grotenhuis Ja, Kauer Jm. The Arcade Of Struthers: An Anatomical Study. Acta Neurochir (Wien) 2003;145:295–300.
-
Beekman R, Schoemaker Mc, Van Der Plas Jp, Et Al. Diagnostic Value Of High-Resolution Sonography In Ulnar Neuropathy At The Elbow. Neurology 2004;62:767–773.
-
Beekman R, Van Der Plas Jp, Uitdehaag Bm, Et Al. Clinical, Electrodiagnostic, And Sonographic Studies In Ulnar Neuropathy At The Elbow. Muscle Nerve 2004;30:202–208.
-
Beekman R, Wokke Jh, Schoemaker Mc, Et Al. Ulnar Neuropathy At The Elbow: Follow-Up And Prognostic Factors Determining Outcome. Neurology 2004;63:1675–1680.
-
Bradshaw Dy, Shefner Jm. Ulnar Neuropathy At The Elbow. Neurol Clin 1999;17:447–461.
-
Buzzard Ef. Some Varieties Of Toxic And Traumatic Ulnar Neuritis. Lancet 1922;1:317.
-
Campbell Ww. Ulnar Neuropathy At The Elbow. Muscle Nerve 2000;23:450–452.
-
Cooke Ra. Hypothenar Hammer Syndrome: A Discrete Syndrome To Be Distinguished From Hand–Arm Vibration Syndrome. Occup Med (Lond) 2003;53:320–324.
-
Postoperatively, patients are placed into a protective splint for about 2 weeks to prevent excessive wrist flexion and extension.
-
Sutures are removed at 10 to 14 days after surgery, at which time gentle active range of motion is started, as well as scar care.
-
The wrist splint should be continued for 2 to 3 more weeks to prevent scar thickening, which is common in this area.
-
Silicone or otoform is helpful to prevent hard, firm scars.
OUTCOMES
- Symptoms can be expected to improve in all cases, with fewer than 20% of patients complaining of slight persistent numbness after the surgery. 14
- The most common cause of failure of surgery is failure in diagnosis, followed by inadequate decompression of all of the branches of the ulnar nerve.
COMPLICATIONS
- Laceration of the ulnar nerve or artery (or both)
-
Inadequate decompression
-
Injury to the ulnar artery
-
Feindel W, J Stratford J. Cubital tunnel compression in tardy ulnar palsy. Can Med Assoc J 1958;78:351–353.
-
Gelberman RH. Ulnar tunnel syndrome. In: Gelberman RH, ed. Operative Nerve Repair and Reconstruction. Philadelphia: JB Lippincott, 1991:1131–1143.
-
Gross MS, Gelberman RH. The anatomy of the distal ulnar tunnel. Clin Orthop Relat Res 1985;196:238–247.
-
Murata K, Shih JT, Tsai TM. Causes of ulnar tunnel syndrome: a retrospective study of 31 subjects. J Hand Surg Am 2003;28:647–651.
-
Pribyl CR, Moneim MS. Anomalous hand muscle found in Guyon’s canal at exploration for ulnar artery thrombosis: a case report. Clin Orthop Relat Res 1994;306 : 120–123.
-
Silver MA, Gelberman RH, Gellman H, et al. Carpal tunnel syndrome: Associated abnormalities in ulnar nerve function and the effect of carpal tunnel release on these abnormalities. J Hand Surg Am 1985;10:710–713.
-
Szabo RM, Steinberg DR. Nerve entrapment syndromes in the wrist. J Am Acad Orthop Surg 1994;2:115–123.
You Might Also Like