Introduction and Epidemiology
Elbow stiffness, characterized by a restricted range of motion, significantly impacts an individual's ability to perform activities of daily living and vocational tasks. While seemingly a simple metric, the precise assessment of elbow flexion degrees is paramount for accurate diagnosis, prognostication, and guiding therapeutic interventions. A functional arc of elbow motion, generally accepted as 30 degrees of extension to 130 degrees of flexion, is necessary for most daily activities. A loss outside this range, particularly a significant flexion contracture or limitation in flexion, can render the limb functionally compromised.
The epidemiology of elbow stiffness is diverse, with post-traumatic causes being the most prevalent, accounting for over fifty percent of cases. These include fractures of the distal humerus, olecranon, radial head, and coronoid process, as well as dislocations and ligamentous injuries. Other etiologies comprise primary osteoarthritis, inflammatory arthropathies, heterotopic ossification, infection, burns, prolonged immobilization, and iatrogenic causes following surgery. The precise measurement of flexion and extension deficits, often quantified using goniometry, allows for objective assessment of the severity of contracture, tracking of progression, and determination of thresholds for intervention. For instance, a flexion contracture exceeding 30 degrees or an inability to achieve more than 100 degrees of flexion is often considered functionally debilitating and may warrant surgical consideration following failed non-operative management.
Pathophysiologically, elbow stiffness is broadly classified into intrinsic, extrinsic, and mixed etiologies. Intrinsic stiffness arises from intra-articular pathology, including articular cartilage degradation, intra-articular adhesions, osteochondral defects, and joint incongruity following malunion. Extrinsic stiffness is driven by extra-articular soft tissue contractures, primarily involving the anterior and posterior joint capsule, collateral ligament scarring, and heterotopic ossification. At the cellular level, post-traumatic extrinsic capsular contracture is characterized by fibroblastic proliferation, increased myofibroblast density, and elevated expression of transforming growth factor beta, leading to disorganized collagen deposition and decreased capsular compliance. Most clinical presentations feature a mixed etiology, necessitating a comprehensive surgical approach that addresses both intra-articular mechanical blocks and extra-articular soft tissue tethers.
Surgical Anatomy and Biomechanics
A thorough understanding of the complex anatomy and biomechanics of the elbow joint is foundational for safe and effective surgical intervention for stiffness.

Bony Anatomy
The elbow is a highly constrained trochoginglymoid joint comprising the humeroulnar, humeroradial, and proximal radioulnar articulations.
* Distal Humerus Features the trochlea medially, articulating with the greater sigmoid notch of the ulna, and the capitellum laterally, articulating with the radial head. The olecranon fossa posteriorly and coronoid fossa anteriorly accommodate the olecranon and coronoid processes during full extension and flexion, respectively. Osteophytes, loose bodies, or malunion in these fossae are common causes of mechanical block to motion.
* Proximal Ulna The olecranon forms the proximal posterior aspect, while the coronoid process forms the anterior portion of the trochlear notch. Impingement of the olecranon tip in the olecranon fossa or the coronoid in the coronoid fossa is a frequent cause of restricted terminal motion.
* Radial Head Articulates with the capitellum and the radial notch of the ulna. Its rotation is critical for pronation and supination, and its congruity affects flexion and extension kinematics.
Ligamentous Anatomy
The collateral ligaments are critical for elbow stability, and their integrity must be preserved during arthrolysis where possible.
* Medial Collateral Ligament Complex Composed of anterior, posterior, and transverse bundles. The anterior bundle originates from the anterior inferior surface of the medial epicondyle and inserts on the sublime tubercle of the coronoid. It is the primary stabilizer against valgus stress throughout the entire range of motion. The posterior bundle is taut in extreme flexion and often requires release or excision in severe flexion contractures.
* Lateral Collateral Ligament Complex Includes the lateral ulnar collateral ligament, radial collateral ligament, annular ligament, and accessory lateral collateral ligament. The lateral ulnar collateral ligament originates from the lateral epicondyle and inserts on the supinator crest of the ulna. It is the primary stabilizer against posterolateral rotatory instability.
Musculature
The primary movers of the elbow are vital for restoring motion post-arthrolysis.
* Flexors Brachialis, biceps brachii, and brachioradialis. The brachialis muscle and its underlying capsule can become densely scarred and contracted anteriorly, acting as a primary tether contributing to flexion loss.
* Extensors Triceps brachii. The triceps tendon and posterior capsule frequently adhere to the olecranon fossa, limiting terminal extension.
* Pronators and Supinators Pronator teres, pronator quadratus, supinator, and biceps brachii.
Neurovascular Structures
Safe execution of capsular releases requires precise knowledge of the neurovascular relationships.
* Ulnar Nerve Courses posterior to the medial epicondyle within the cubital tunnel. It is highly susceptible to traction injury during restoration of flexion and is frequently encased in scar tissue or heterotopic ossification in post-traumatic stiffness.
* Radial Nerve Pierces the lateral intermuscular septum to enter the anterior compartment, coursing between the brachialis and brachioradialis. It is at risk during anterior capsulectomy from the lateral side.
* Median Nerve and Brachial Artery Course anterior to the brachialis muscle. While protected by the brachialis during anterior capsular release, severe contractures alter normal tissue planes, increasing the risk of iatrogenic injury.
Indications and Contraindications
The decision to proceed with operative intervention for elbow stiffness relies on a careful assessment of the functional deficit, the underlying etiology, and the exhaustion of non-operative modalities. A minimum of six months of dedicated non-operative management, including static progressive splinting and physical therapy, is generally recommended before considering surgical arthrolysis, allowing the inflammatory phase of tissue healing to subside and scar tissue to mature.
Operative intervention is indicated when the functional arc of motion remains compromised despite compliance with non-operative protocols, particularly when the deficit interferes with the patient's occupation or activities of daily living. Furthermore, the presence of distinct mechanical blocks, such as large intra-articular loose bodies, prominent osteophytes impinging within the olecranon or coronoid fossae, or mature heterotopic ossification bridging the joint, serves as a strong indication for surgery, as these pathologies are refractory to conservative management.
Contraindications must be strictly observed to prevent catastrophic outcomes. Active joint infection precludes elective arthrolysis. Severe articular destruction, such as advanced post-traumatic osteoarthritis with complete loss of cartilage space, is a relative contraindication for simple soft-tissue release, as motion gained will likely be painful; such patients are better served by interposition arthroplasty or total elbow arthroplasty depending on age and functional demands. Poor patient compliance is an absolute contraindication, as the success of the procedure relies entirely on rigorous, painful postoperative rehabilitation.
| Parameter | Operative Indications | Non Operative Indications | Absolute Contraindications |
|---|---|---|---|
| Duration of Symptoms | > 6 months of failed conservative therapy | < 6 months post-injury or surgery | N/A |
| Functional Deficit | Arc of motion < 100 degrees or outside 30-130 range | Minimal deficit not impacting daily activities | N/A |
| Mechanical Blocks | Intra-articular loose bodies, mature heterotopic ossification, osteophytes | Absence of distinct bony blocks | N/A |
| Splinting Response | Plateaued or failed response to static progressive splinting | Continued objective improvement with splinting | N/A |
| Joint Status | Maintained articular congruity with adequate cartilage space | Mild articular changes | Active joint infection, severe articular destruction |
| Patient Factors | Highly motivated, compliant with rigorous rehabilitation | Poor compliance, inability to tolerate aggressive therapy | Medical instability, active non-compliance |
Pre Operative Planning and Patient Positioning
Clinical Evaluation and Imaging Modalities
Comprehensive preoperative planning begins with a meticulous clinical examination. The exact degrees of active and passive flexion, extension, pronation, and supination must be recorded using a goniometer. The end-feel of the joint should be assessed; a firm, abrupt stop suggests a bony block, whereas a rubbery, gradual stop indicates soft tissue contracture. A thorough neurologic examination is mandatory, with specific attention to ulnar nerve function, as subclinical ulnar neuropathy is prevalent in stiff elbows and dictates the need for concurrent ulnar nerve decompression or transposition.
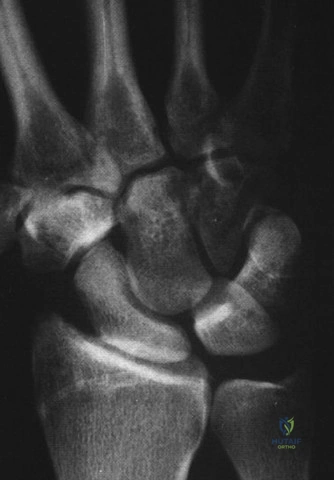
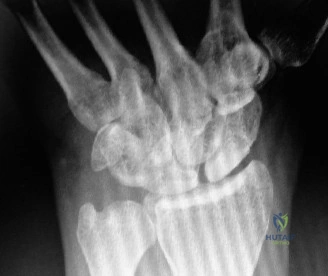
Standard anteroposterior and lateral radiographs are the initial imaging modality to assess overall joint congruity, joint space narrowing, and the presence of heterotopic ossification or hardware. However, a non-contrast Computed Tomography scan with three-dimensional reconstructions is the gold standard for preoperative planning in the stiff elbow. The CT scan precisely delineates the location and volume of heterotopic ossification, identifies osteophytes within the coronoid and olecranon fossae, and clarifies complex post-traumatic malunions. If ligamentous instability or severe soft tissue pathology is suspected, Magnetic Resonance Imaging may be utilized, though it is less commonly required than CT.
Patient Positioning and Operating Room Setup
Patient positioning is dictated by the planned surgical approach and surgeon preference. The lateral decubitus position is highly favored for both open and arthroscopic elbow arthrolysis. The patient is placed in the lateral decubitus position with the operative arm supported over a padded post or an articulating arm holder. This setup allows circumferential access to the elbow, facilitating both medial and lateral approaches without repositioning, and permits gravity to assist in joint distraction during arthroscopy.
Alternatively, the supine position with the arm draped across the chest can be utilized, particularly for isolated lateral or posterior approaches. A sterile tourniquet is applied high on the brachium to ensure a bloodless surgical field, which is critical for identifying neurovascular structures and delineating tissue planes during extensive capsular releases.
Detailed Surgical Approach and Technique
The surgical management of elbow stiffness involves a systematic release of contracted structures and excision of mechanical blocks. The choice of approach depends on the location of the pathology. Open arthrolysis remains the workhorse for severe, multi-compartmental stiffness, particularly in the presence of heterotopic ossification or altered neurovascular anatomy.
The Lateral Column Approach
The lateral column approach, popularized by Mansat and Morrey, is highly versatile and allows access to the anterior and posterior compartments from a single incision.
1. Incision and Superficial Dissection A longitudinal incision is made over the lateral supracondylar ridge, extending distally to the radial head. The interval between the extensor carpi radialis longus and the extensor digitorum communis is developed.
2. Anterior Capsulectomy The brachialis and extensor carpi radialis longus are elevated anteriorly off the humerus. This exposes the anterior capsule. The radial nerve is protected by the brachialis muscle belly. The anterior capsule is sharply excised from lateral to medial. It is crucial to perform a capsulectomy (excision) rather than a capsulotomy (incision) to prevent recurrence.
3. Posterior Decompression The triceps is elevated posteriorly off the lateral intermuscular septum. The posterior capsule is excised, and the olecranon fossa is cleared of fibrotic tissue and osteophytes using a rongeur or high-speed burr. The tip of the olecranon can be resected if it impinges within the fossa.
4. Ligament Preservation Throughout the dissection, the origin of the lateral ulnar collateral ligament at the lateral epicondyle must be strictly preserved to prevent posterolateral rotatory instability.
The Medial Approach
A medial approach is indicated when there is severe medial heterotopic ossification, medial collateral ligament contracture, or concurrent ulnar neuropathy requiring intervention.
1. Ulnar Nerve Management The incision is made posterior to the medial epicondyle. The ulnar nerve is immediately identified, neurolysed, and mobilized. Depending on the extent of the release and preoperative symptoms, the nerve is either decompressed in situ or transposed anteriorly.
2. Medial Capsular Release The flexor-pronator mass is elevated anteriorly to expose the medial aspect of the anterior capsule. The anterior band of the medial collateral ligament must be identified and protected. The posterior bundle of the medial collateral ligament, which is often contracted in severe flexion deficits, is selectively released or excised.
3. Over the Top Release In cases of severe global stiffness, a medial approach can be combined with a lateral approach, or an "over the top" anterior capsulectomy can be completed from the medial side after protecting the median nerve and brachial artery.
The Posterior Universal Approach
For extensive heterotopic ossification encompassing the entire joint, or when previous posterior incisions exist, a posterior universal approach is utilized. This involves a midline posterior incision with the creation of full-thickness medial and lateral fasciocutaneous flaps. This provides access to both the medial and lateral columns, allowing for ulnar nerve transposition, bilateral capsular releases, and extensive heterotopic ossification excision through a single skin incision. The triceps can be mobilized via a triceps-reflecting (Bryan-Morrey) or triceps-splitting approach, though minimizing triceps detachment is preferred to facilitate immediate postoperative active extension.
Arthroscopic Arthrolysis Principles
Arthroscopic release is an advanced technique indicated for mild to moderate intrinsic and extrinsic stiffness, particularly when pathology is localized to the anterior or posterior compartments without significant heterotopic ossification or extra-articular altered anatomy. It involves sequential establishment of proximal anteromedial, proximal anterolateral, and posterior portals. The anterior capsule is resected using a shaver and radiofrequency wand, taking care to stay strictly on the capsular side to avoid the anterior neurovascular bundle. The olecranon fossa is cleared of osteophytes, and the olecranon tip can be resected arthroscopically. While offering the benefits of reduced surgical trauma and potentially faster initial rehabilitation, arthroscopic arthrolysis requires significant expertise and carries a steep learning curve regarding neurovascular safety.
Complications and Management
The surgical treatment of elbow stiffness is fraught with potential complications, necessitating meticulous surgical technique and vigilant postoperative care. The altered anatomy resulting from trauma and dense scar tissue significantly increases the risk profile compared to routine elbow surgery.
| Complication | Estimated Incidence | Pathophysiology and Risk Factors | Prevention and Salvage Strategies |
|---|---|---|---|
| Ulnar Neuropathy | 5% to 15% | Traction injury during flexion restoration, encasement in scar/HO, thermal injury during arthroscopy. | Prophylactic decompression or transposition during open release. Postoperative observation for transient neuropraxia; revision neurolysis for persistent deficits. |
| Recurrent Stiffness | 10% to 20% | Inadequate primary release, failure of postoperative rehabilitation, excessive surgical trauma leading to robust scar formation. | Complete capsulectomy (not capsulotomy), meticulous hemostasis, immediate aggressive postoperative CPM and splinting. Revision arthrolysis for refractory cases. |
| Iatrogenic Instability | 2% to 5% | Inadvertent transection of the anterior bundle of the MCL or the LUCL during capsular resection. | Precise anatomical identification of collateral origins. Repair with suture anchors or ligament reconstruction with autograft if transection occurs intraoperatively. |
| Heterotopic Ossification Recurrence | 5% to 10% | Incomplete excision of immature HO, severe initial trauma, concomitant traumatic brain injury. | Delay surgery until HO is radiographically mature. Postoperative prophylaxis with Indomethacin or single-dose localized radiation therapy. |
| Deep Infection | 1% to 3% | Prolonged operative time, extensive soft tissue dissection, compromised local soft tissue envelope from prior trauma. | Meticulous soft tissue handling, perioperative intravenous antibiotics. Management requires aggressive irrigation and debridement, targeted antibiotics, and potential hardware removal if present. |
| Hematoma Formation | 3% to 8% | Extensive capsulectomy leaving dead space, inadequate hemostasis post-tourniquet deflation. | Deflate tourniquet prior to closure to achieve pinpoint hemostasis. Use of closed suction drains for 24-48 hours postoperatively. |
Post Operative Rehabilitation Protocols
The surgical procedure represents only the first phase of treatment; the ultimate success of an elbow arthrolysis is entirely dependent on the postoperative rehabilitation protocol. The primary goal is to maintain the range of motion achieved in the operating room while managing pain and inflammation.
Immediate postoperative pain control is paramount. The use of an indwelling regional anesthetic catheter (such as a supraclavicular or infraclavicular brachial plexus block) for the first 48 to 72 hours allows for aggressive, painless mobilization during the critical early inflammatory phase.
Continuous Passive Motion machines are frequently deployed immediately in the recovery room or on postoperative day one. While the long-term superiority of Continuous Passive Motion over active therapy is debated in the literature, it serves to prevent early intra-articular adhesion formation and helps evacuate intra-articular hematoma. The Continuous Passive Motion machine is typically used for 20 to 22 hours a day during the inpatient stay.
Active and active-assisted range of motion exercises are initiated under the guidance of a specialized hand or upper extremity therapist. Gravity-assisted exercises and overhead stretches are highly effective. Strengthening exercises are strictly avoided in the early phases (first 4 to 6 weeks) to prevent excessive muscle co-contraction and exacerbation of inflammation, which can drive recurrent stiffness.
Upon discharge, or at the 2 to 3-week postoperative mark, patients are transitioned to a static progressive splinting program. Turnbuckle splints or custom-molded static progressive orthoses are utilized to apply a low-load, prolonged stretch to the maturing collagen of the healing capsule. Patients alternate between flexion and extension splinting regimens, typically wearing the splints during sleep and for several hours during the day, adjusting the tension to a level of tolerable stretch rather than acute pain. This splinting regimen is often maintained for 3 to 6 months postoperatively until the range of motion plateaus.
Summary of Key Literature and Guidelines
The academic foundation for the management of the stiff elbow is built upon several landmark studies that dictate current surgical and rehabilitative paradigms.
Morrey et al. established the biomechanical parameters of the functional arc of motion (100 degrees of flexion-extension, 100 degrees of pronation-supination), which remains the standard metric for determining surgical indications and defining successful outcomes. Their work underscored that small gains in terminal extension are less functionally significant than achieving adequate flexion for activities of daily living.
The lateral column approach for open arthrolysis was heavily refined and popularized by Mansat and Morrey. Their seminal papers demonstrated that an extensive anterior and posterior capsulectomy could be safely performed through a single lateral incision, yielding reproducible improvements in the arc of motion with a low complication rate, provided the lateral ulnar collateral ligament was respected.
Jupiter and Ring contributed significantly to the understanding of complex post-traumatic stiffness, particularly following distal humerus fractures. Their research highlighted the necessity of addressing intra-articular hardware malposition and restoring articular congruity concurrently with soft tissue release. They also emphasized the utility of the posterior universal approach for global joint access in the setting of severe heterotopic ossification.
In the realm of arthroscopic management, O'Driscoll and colleagues defined the safe zones and portals for elbow arthroscopy. Their guidelines on capsular release techniques, particularly the "tenting" of the anterior capsule to protect the neurovascular bundle during resection, are foundational for surgeons performing arthroscopic arthrolysis. Current consensus guidelines suggest that while arthroscopy is highly effective for localized contractures and loose body removal, open arthrolysis remains the gold standard for severe stiffness, extensive heterotopic ossification, and cases involving significant ulnar neuropathy requiring transposition.
Detailed Chapters & Topics
Dive deeper into specialized chapters regarding wrist-cases-4
