Clinical Diagnosis & Imaging of Elbow Adhesive Capsulitis: An Orthopedic Case Study
Key Takeaway
Elbow adhesive capsulitis is diagnosed through a comprehensive clinical evaluation, revealing progressive, symmetrical global motion restriction and a firm capsular end-feel. Predisposing factors like diabetes are considered. Imaging, primarily MRI, confirms capsular thickening and inflammation while ruling out other pathologies, making it crucial for a definitive diagnosis.
Patient Presentation and History
Demographics and Comorbidities
A 48-year-old right-hand dominant male presented to the Orthopedic Trauma Clinic with a 9-month history of progressive left elbow pain and severe stiffness. His medical history is highly relevant, marked by well-controlled Type 2 Diabetes Mellitus (HbA1c 6.8%) and primary hypothyroidism, both managed medically. The intersection of these endocrinopathies is a critical predisposing factor in the pathogenesis of fibrotic joint disorders. Diabetes mellitus, in particular, accelerates the accumulation of advanced glycation end-products within the collagen matrix of the joint capsule, leading to pathological cross-linking, decreased capsular compliance, and subsequent fibroblastic proliferation. Hypothyroidism further alters collagen metabolism and extracellular matrix turnover, creating a systemic environment primed for capsular contracture following even minimal provocation.
Mechanism of Injury and Symptom Progression
There was no preceding high-energy trauma, fracture, or dislocation identified by the patient. However, he recounted a minor "jarring" injury to his left elbow approximately 10 months prior while lifting a moderately heavy box. Fearing an occult fracture, he self-immobilized the extremity in a commercial sling for two weeks. This period of absolute immobilization served as the mechanical catalyst for the ensuing capsular fibrosis.
The pain initially presented as a deep, poorly localized dull ache, exhibiting a characteristic nocturnal exacerbation and sharp pain with attempts at terminal range of motion. Over the subsequent months, the patient noted a gradual, insidious, and symmetrical restriction in both active and passive elbow flexion and extension. This global loss of motion significantly impacted his activities of daily living, specifically compromising dressing, personal hygiene, and his occupational tasks as a clerical worker. He denied any acute mechanical symptoms such as locking or catching, and reported no subjective instability or neurological symptoms such as paresthesias, numbness, or motor weakness in the distal extremity.
Prior Interventions and Clinical Course
Initial conservative management initiated by his primary care physician included a sustained course of oral non-steroidal anti-inflammatory drugs (NSAIDs) and a six-week trial of formal physical therapy. The physical therapy regimen focused heavily on aggressive passive stretching and modalities. However, this conservative approach provided minimal therapeutic benefit and arguably exacerbated his inflammatory pain cycle, leading to persistent and worsening functional limitations. He reported strict compliance with his diabetes and thyroid medication regimens throughout this period, ruling out acute metabolic dysregulation as a driver of his rapid symptom progression.
Clinical Examination Findings
Upon examination in the clinic, the patient was alert, cooperative, and in no acute distress. The examination was conducted systematically, comparing the affected left upper extremity to the contralateral right side.
Inspection and Palpation
Inspection of the left elbow revealed mild, global joint effusion without localized erythema, ecchymosis, or overt structural deformity. There were no visible skin lesions, prior surgical scars, or signs of superficial infection. Mild disuse atrophy was clinically evident in the left forearm musculature and the distal triceps belly compared to the contralateral limb, consistent with chronic offloading of the extremity.
Palpation elicited diffuse, non-focal tenderness around both the anterior and posterior aspects of the elbow joint, localizing primarily over the radiocapitellar and ulnohumeral joint lines. Crucially, no focal point tenderness was identified over the medial or lateral epicondyles, the olecranon process, or the radial head, effectively lowering the probability of epicondylitis or occult osseous injury. The ulnar nerve groove was palpated; it was non-tender, and the ulnar nerve was not subluxable during dynamic flexion and extension maneuvers, remaining stable within the cubital tunnel.
Range of Motion Assessment
The hallmark of the clinical examination was the profound restriction in the functional arc of motion. Range of motion (ROM) testing was performed using a standard goniometer.
- Left Elbow:
- Flexion Active 90 degrees, Passive 95 degrees (normal 140 to 150 degrees). The flexion endpoint was distinctively firm and highly provocative of pain.
- Extension Active -45 degrees, Passive -40 degrees (normal 0 to 5 degrees hyperextension). The extension endpoint was similarly firm, mechanical, and painful.
- Pronation Active 70 degrees, Passive 75 degrees (normal 80 to 90 degrees).
- Supination Active 60 degrees, Passive 65 degrees (normal 80 to 90 degrees).
- Right Elbow (contralateral): Demonstrated a full, pain-free range of motion (0 to 145 degrees flexion, 85 degrees pronation, 85 degrees supination).
The patient exhibited a classic "capsular pattern" of the elbow, characterized by a severe, nearly symmetrical loss of both flexion and extension, with a relative preservation of forearm rotation. The functional arc of the elbow, generally accepted as 30 to 130 degrees of flexion and 50 degrees of both pronation and supination, was severely compromised, explaining his profound functional deficits.
Neurological and Vascular Evaluation
A comprehensive distal neurovascular examination was performed to rule out compressive neuropathies, which frequently accompany complex elbow pathology.
* Motor Assessment: Intact motor strength graded at 5/5 in all muscle groups innervated by the radial, median, anterior interosseous, and ulnar nerves.
* Sensory Assessment: Intact light touch and pinprick sensation in all dermatomes distal to the elbow, including the autonomous zones of the median, ulnar, and superficial sensory radial nerves.
* Reflexes: Biceps, brachioradialis, and triceps deep tendon reflexes were graded 2+ bilaterally and were perfectly symmetrical.
* Vascular Assessment: Radial and ulnar arterial pulses were palpable, graded 2+, and symmetrical bilaterally. Capillary refill was brisk (under 2 seconds) in all digits. There were no clinical signs of venous congestion, deep vein thrombosis, or lymphatic obstruction.
Ligamentous Stability Testing
Despite the stiffness, an assessment of ligamentous integrity was carefully performed. Varus and valgus stress testing, executed at 30 degrees of flexion to unlock the olecranon from its fossa, as well as in full extension, revealed a firm endpoint with no demonstrable laxity. This indicated structurally intact medial ulnar collateral ligament and lateral collateral ligament complexes. Posterolateral rotatory instability testing was negative, though inherently limited by the patient's restricted extension and guarding.
Imaging and Diagnostics
Plain Radiography Evaluation
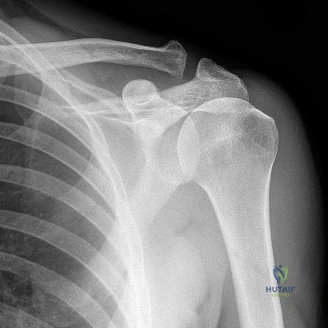
Standard orthogonal anteroposterior and lateral radiographic views of the left elbow were obtained in the clinic. The interpretation of these radiographs is critical in differentiating primary adhesive capsulitis from post-traumatic arthrofibrosis or degenerative joint disease.
The radiographs revealed no evidence of acute fracture, chronic non-union, malunion, dislocation, or subluxation. The ulnohumeral and radiocapitellar joint spaces were well-maintained without evidence of asymmetrical narrowing, subchondral sclerosis, or significant marginal osteophyte formation. Furthermore, there were no visible intra-articular loose bodies, and no evidence of heterotopic ossification within the anterior or posterior soft tissue envelopes. The absence of these osseous abnormalities strongly supported a purely soft-tissue driven pathology, pointing directly toward intrinsic capsular contracture.
Advanced Cross Sectional Imaging
To definitively evaluate the soft tissue envelope, confirm the diagnosis of adhesive capsulitis, and rule out subtle chondral defects or occult loose bodies not visualized on plain films, a non-contrast Magnetic Resonance Imaging scan of the left elbow was ordered.
The MRI demonstrated marked thickening and abnormal signal intensity within the anterior and posterior joint capsule, characteristic of fibroblastic proliferation and edema. The anterior capsule measured approximately 4.5 millimeters in thickness (normal is typically less than 2 millimeters). There was a small to moderate reactive joint effusion. The articular cartilage overlying the capitellum, radial head, trochlea, and greater sigmoid notch was preserved, confirming the absence of advanced osteoarthritis. The collateral ligaments and common flexor and extensor origins were intact.

Computed Tomography and Templating Considerations
While a CT scan is often considered the gold standard for evaluating complex post-traumatic elbow stiffness—specifically to identify architectural distortion, subtle articular incongruity, and the precise anatomical location of heterotopic ossification—it was deemed unnecessary in this specific clinical scenario. The pristine nature of the plain radiographs, combined with the classic clinical presentation of primary adhesive capsulitis and the confirmatory MRI findings, rendered a CT scan clinically redundant. However, had there been any suspicion of an osseous block to motion, a 3D reconstructed CT would have been essential for preoperative templating and determining the necessity of an open osteocapsular arthroplasty versus an arthroscopic soft tissue release.
Differential Diagnosis
The diagnosis of a stiff elbow requires a meticulous differentiation between intra-articular and extra-articular etiologies, as well as distinguishing between primary capsular disease and secondary reactive fibrosis. The following table outlines the primary differential diagnoses considered for this patient.
| Condition | Pathophysiology | Key Clinical Findings | Radiographic Hallmarks |
|---|---|---|---|
| Primary Adhesive Capsulitis | Idiopathic fibroblastic proliferation and capsular contracture; highly associated with DM and thyroid dysfunction. | Global loss of active/passive ROM (capsular pattern); firm end-feel; insidious onset without major trauma. | Normal joint space; absence of osteophytes or heterotopic ossification; thickened capsule on MRI. |
| Post Traumatic Arthrofibrosis | Excessive scar tissue formation following intra-articular fracture, dislocation, or severe soft tissue trauma. | History of specific trauma/surgery; ROM loss correlates with the site of scarring; potential mechanical blocks. | May show healed fractures, surgical hardware, subtle malalignment, or post-traumatic osteophytes. |
| Elbow Osteoarthritis | Degenerative loss of articular cartilage, subchondral sclerosis, and marginal osteophyte formation. | Pain at end-range of motion; crepitus; catching/locking from loose bodies; history of repetitive microtrauma. | Joint space narrowing, subchondral cysts, osteophytes (especially olecranon/coronoid), loose bodies. |
| Heterotopic Ossification | Ectopic bone formation within soft tissues, often following neurotrauma, burns, or direct high-energy elbow trauma. | Rigid, abrupt block to motion; palpable bony mass; history of severe trauma or prolonged intubation. | Distinct radiopaque bone formation within the muscles or capsule on plain films and CT scans. |
| Inflammatory Arthropathy | Systemic autoimmune destruction of the joint (e.g., Rheumatoid Arthritis) leading to synovitis and secondary stiffness. | Polyarticular involvement; morning stiffness; boggy synovitis; potential ligamentous laxity/instability. | Periarticular osteopenia, symmetrical joint space narrowing, marginal erosions. |
In this patient, the insidious onset, lack of major trauma, perfectly preserved joint spaces on radiography, and the presence of significant endocrine comorbidities definitively pointed toward Primary Adhesive Capsulitis, effectively ruling out post-traumatic, degenerative, and osseous etiologies.
Surgical Decision Making and Classification
Indications for Operative Intervention
The management of elbow adhesive capsulitis typically begins with a robust non-operative protocol, including physical therapy, NSAIDs, and intra-articular corticosteroid injections. However, surgical intervention is strongly indicated when a patient experiences a persistent, unacceptable deficit in their functional arc of motion despite a minimum of six months of dedicated conservative management.
In this case, the patient had endured nine months of progressive stiffness. His range of motion (95 degrees of flexion to -40 degrees of extension) fell drastically outside the functional arc required for basic activities of daily living (30 to 130 degrees). The chronicity of his symptoms, the failure of non-operative modalities, and the severe impact on his occupational capacity provided clear indications for surgical release.
Classification of Elbow Stiffness
To guide surgical planning, the stiffness was classified. According to the Kay classification of elbow stiffness, this patient presented with Type I stiffness: soft tissue contracture without intra-articular osseous pathology or heterotopic ossification. This classification is vital as it dictates the surgical approach. Type I stiffness is highly amenable to arthroscopic capsular release, whereas Types II through V (involving articular changes, hardware, or heterotopic ossification) often necessitate complex open arthrolysis.
Operative Strategy Arthroscopic Versus Open Release
The decision between an open and arthroscopic approach for elbow capsular release hinges on the surgeon's experience, the presence of ulnar neuropathy, and the exact anatomical location of the contracture.
An open column procedure (typically a lateral or medial over-the-top approach) provides excellent visualization of the capsule and allows for concurrent management of heterotopic ossification or hardware removal. However, it is associated with higher postoperative morbidity, greater incisional pain, and a theoretically higher risk of recurrent fibrosis due to the larger surgical trauma.
Conversely, arthroscopic capsular release offers the advantages of minimal soft tissue disruption, superior illumination and magnification of intra-articular structures, decreased postoperative pain, and the ability to initiate immediate aggressive postoperative rehabilitation. Given that this patient had isolated soft tissue capsular contracture without ulnar nerve symptoms or osseous blocks, an arthroscopic global capsular release (anterior and posterior capsulectomy) was deemed the optimal, least morbid intervention.
Surgical Technique and Intervention
Patient Positioning and Setup
The patient was brought to the operating room and placed under general anesthesia. A supplemental ultrasound-guided supraclavicular regional nerve block was administered by the anesthesia team. This block is a critical component of the procedure, as it provides profound perioperative analgesia, minimizes the requirement for systemic narcotics, and allows for immediate, painless continuous passive motion in the recovery room.
The patient was positioned in the lateral decubitus position on a beanbag. The operative left arm was supported over a padded L-bar post, allowing the elbow to hang freely at 90 degrees of flexion. A non-sterile tourniquet was placed high on the brachium. The arm was prepped and draped in a standard sterile orthopedic fashion. Prior to inflation of the tourniquet, the anatomical landmarks—including the medial and lateral epicondyles, the olecranon, the radial head, and the course of the ulnar nerve—were meticulously demarcated with a surgical marker.
Surgical Approach and Portal Placement
Arthroscopy of the stiff elbow demands extreme precision in portal placement due to the altered anatomical relationships caused by capsular contracture and reduced joint volume. The joint was initially insufflated with 15 to 20 milliliters of sterile normal saline via a lateral soft spot puncture to distend the capsule and displace the neurovascular structures anteriorly.
The initial viewing portal established was the proximal anteromedial portal. An incision was made 2 centimeters proximal and 1 centimeter anterior to the medial epicondyle. Blunt dissection with a hemostat was performed down to the capsule to protect the medial antebrachial cutaneous nerve. A blunt trocar was introduced, aiming towards the radial head, maintaining contact with the anterior humerus to avoid injury to the median nerve and brachial artery.
Once intra-articular access was confirmed, a diagnostic sweep revealed severe, diffuse synovitis and a thick, fibrotic anterior capsule. Under direct intra-articular visualization, the proximal anterolateral portal was established using an outside-in spinal needle localization technique, ensuring safe distance from the radial nerve.
Capsular Reduction and Tissue Management
The core of the surgical intervention for adhesive capsulitis is not a traditional fracture reduction or the application of a fixation construct, but rather the systematic, controlled excision of the pathological fibrotic tissue—a true capsulectomy rather than a simple capsulotomy.
Working through the proximal anterolateral portal with a 4.5-millimeter aggressive oscillating shaver and a radiofrequency ablation wand, an anterior capsulectomy was initiated. The fibrotic capsule was systematically resected starting from the lateral gutter, moving medially across the anterior joint line. The resection was carried proximally to expose the anterior humeral cortex and distally to the level of the radiocapitellar joint.
A critical technical pearl during this phase is the identification of the brachialis muscle fibers. The anterior capsule must be completely excised until the red, healthy fibers of the brachialis muscle are clearly visualized across the entire anterior compartment. This ensures a complete release and allows the brachialis to act as a dynamic interpositional graft, preventing readhesion of the joint surfaces. Extreme caution was exercised as the resection proceeded medially to avoid thermal or mechanical injury to the median nerve and brachial artery, which lie immediately anterior to the brachialis.
Posterior Compartment Decompression
Following the completion of the anterior capsulectomy, attention was turned to the posterior compartment. The anterior portals were left open to allow fluid egress and prevent excessive extravasation.
A direct posterior portal and a posterolateral portal were established. Diagnostic arthroscopy of the posterior compartment revealed a similarly thickened posterior capsule and fibrotic bands tethering the olecranon within the olecranon fossa.
A thorough posterior capsulectomy was performed. The fibrotic tissue within the olecranon fossa was debrided, and the posterior band of the medial ulnar collateral ligament was carefully evaluated. In cases of severe flexion contracture, the posterior band of the MUCL often requires fractional release; however, in this patient, the posterior capsulectomy and debridement of the olecranon fossa yielded a highly satisfactory restoration of flexion. The triceps tendon was mobilized off the posterior humerus to ensure unrestricted excursion.
Post Release Stability Assessment
Following the global capsular release, the arthroscope was removed, and the joint was evacuated of fluid. A dynamic clinical examination under anesthesia was performed to assess the results of the tissue management.
The patient's range of motion was dramatically improved. Passive flexion was restored to 140 degrees, and passive extension was restored to 0 degrees (full extension). Pronation and supination remained full. Varus and valgus stress testing was repeated, confirming that the collateral ligaments remained structurally sound and the joint was completely stable. The surgical portals were closed with simple non-absorbable sutures, and a bulky, soft compressive dressing was applied with the elbow resting in full extension.
Post Operative Protocol and Rehabilitation
Immediate Postoperative Phase and Analgesia
The success of an arthroscopic capsular release is intrinsically tied to the postoperative rehabilitation protocol. The immediate goal is to maintain the range of motion achieved in the operating room while managing the inevitable inflammatory response.
Due to the indwelling supraclavicular regional catheter, the patient awoke completely pain-free. While in the Post-Anesthesia Care Unit, the patient's arm was immediately placed into a Continuous Passive Motion machine. The CPM was programmed to cycle slowly from 0 degrees of extension to 140 degrees of flexion. The patient was instructed to utilize the CPM for a minimum of 18 to 20 hours per day during the first week.
Early Mobilization and Dynamic Splinting
Upon discharge on postoperative day one, the patient was prescribed a robust multimodal oral pain regimen, including scheduled NSAIDs (Indomethacin 75mg sustained release daily) not only for analgesia but also as prophylaxis against heterotopic ossification.
Formal physical therapy commenced on postoperative day two. The initial phase (Weeks 0 to 2) focused on aggressive active-assisted and passive range of motion exercises. Edema control was managed with compressive sleeves and cryotherapy.
By week three, static progressive splinting was initiated. The patient was fitted with custom-molded orthoses: an extension splint worn primarily at night to combat the natural tendency of the elbow to rest in flexion, and a flexion splint worn during specific intervals during the day. The use of turnbuckle splints allowed the patient to apply a low-load, prolonged stretch to the healing tissues, which is biomechanically superior to high-load, brief stretching in modifying collagen cross-linking.
Long Term Rehabilitation Goals
From weeks six through twelve, the rehabilitation protocol transitioned toward strengthening and functional integration. Progressive resistance exercises were introduced for the biceps, triceps, and forearm musculature. The patient was educated that maximal medical improvement following a stiff elbow release often takes up to six to nine months. Continuous compliance with a daily home stretching program was emphasized as mandatory to prevent recurrent contracture. By the four-month postoperative mark, the patient had successfully returned to all clerical duties and activities of daily living with a maintained functional arc of 5 degrees of extension to 135 degrees of flexion.
Clinical Pearls and Pitfalls
Surgical Pearls
- Preoperative Optimization: Strict glycemic control in diabetic patients prior to surgery is paramount. Elevated HbA1c levels correlate directly with a higher incidence of recurrent postoperative stiffness and poor wound healing.
- Meticulous Portal Placement: The altered anatomy of a stiff elbow makes portal placement hazardous. Always distend the joint maximally before establishing the first portal, and strongly consider using an outside-in needle localization technique for all subsequent portals to protect the radial and ulnar nerves.
- Capsulectomy Over Capsulotomy: Simply incising the capsule (capsulotomy) is insufficient and carries a high rate of recurrence. A complete capsulectomy, revealing the healthy fibers of the brachialis muscle anteriorly and the triceps posteriorly, is required to achieve lasting mobility.
- Prophylactic Ulnar Nerve Evaluation: While not transposed in this case, the ulnar nerve must be carefully evaluated preoperatively. If preoperative ulnar nerve symptoms exist, or if significant gains in flexion are anticipated that may place the nerve under tension, an open in-situ decompression or anterior transposition should be performed concurrently.
Avoidance of Complications
- Iatrogenic Neurological Injury: The most devastating complication of elbow arthroscopy is nerve injury. The radial nerve is at extreme risk during the establishment of the anterolateral portals and during lateral capsulectomy. Keeping the shaver blades facing the joint and away from the capsule when not actively resecting is a critical safety measure.
- Inadequate Posterior Release: Surgeons frequently focus heavily on the anterior capsule to restore extension but neglect the posterior compartment. Failure to clear the olecranon fossa and release the posterior capsule will result in persistent deficits in terminal flexion.
- Rehabilitation Failure: The surgery is only 50% of the treatment. Failure to implement a rigorous, immediately instituted, and well-managed postoperative pain and continuous passive motion protocol will almost certainly result in recurrent arthrofibrosis and a failed procedure. Clear, repetitive patient counseling regarding the grueling nature of the postoperative rehabilitation is essential before offering surgical intervention.
