Post-Traumatic Elbow Contracture: Diagnosis & Management of Heterotopic Ossification

Key Takeaway
Severe post-traumatic elbow stiffness often results from heterotopic ossification (HO), where bone forms in soft tissues after injury or surgery. Diagnosis involves detailed patient history, clinical examination, and advanced imaging like CT scans with 3D reconstructions to precisely map HO and plan effective surgical management, restoring essential range of motion.
Patient Presentation and Initial Evaluation
A 48-year-old right-hand dominant male presented to our clinic with a chief complaint of progressively worsening right elbow stiffness and pain, significantly impacting his daily activities and work. His history dates back eight months prior, following a high-energy motor vehicle accident in which he sustained a comminuted right distal humerus fracture (AO/OTA 13-C2) and an ipsilateral radial head fracture.
The initial injury was managed surgically with open reduction and internal fixation of the distal humerus using a dual-plate construct (medial and lateral columns) and excision of the radial head due to comminution that was deemed unreconstructable. Post-operatively, he was immobilized in a long-arm splint for three weeks, followed by a referral for physical therapy. Despite diligent adherence to the physical therapy regimen for five months, his elbow range of motion plateaued and then progressively deteriorated.
At presentation, he reported an inability to fully extend or flex his elbow, making tasks such as reaching for objects overhead, grooming, and working at a computer extremely difficult. He described the pain as a dull ache at rest, intensifying to a sharp, restrictive pain at the end-range of attempted motion. He denied any acute trauma since the initial injury.
His past medical history is notable for well-controlled hypertension and a 20-pack-year smoking history, which he quit six months prior. He has no history of head trauma or burns. His occupation involves manual labor, making functional elbow motion critical for his livelihood.
Inspection
On visual inspection, the right elbow demonstrated significant soft tissue scarring consistent with his prior surgical incision, extending along the posterior aspect of the distal arm and elbow. There was mild efferent swelling but no overt erythema or signs of active infection. The carrying angle appeared subtly altered, favoring a slight valgus deformity, though this was difficult to ascertain definitively given the contracture. Marked atrophy of the triceps and forearm musculature was evident compared to the contralateral limb. No skin tenting or open wounds were present.
Palpation
Palpation revealed a firm, non-tender mass along the posterior-medial aspect of the elbow, extending from the distal humerus to the proximal ulna, suggestive of heterotopic ossification. Tenderness was elicited over the medial and lateral epicondyles with deep palpation. The ulnar nerve groove felt thickened and somewhat immobile at the cubital tunnel. There was no palpable joint effusion. The surgical hardware appeared well-seated, with no signs of prominence or superficial irritation.
Range of Motion
Active and passive range of motion measurements were performed, demonstrating severe limitations. The flexion-extension arc was from 70 degrees of extension deficit to 105 degrees of flexion. This represents a severely restricted arc of 35 degrees. Both extension and flexion had a hard, bony end-feel. Forearm rotation was also compromised, with pronation limited to 45 degrees and supination limited to 30 degrees. These limitations were likely secondary to capsular and soft tissue contracture, as well as the radial head excision and subsequent radioulnar scarring.
Neurological and Vascular Assessment
Neurological examination of the right upper extremity revealed mild paresthesia in the ulnar nerve distribution affecting the small finger and ulnar half of the ring finger. Sensation to light touch and two-point discrimination was diminished in this area. Motor strength testing demonstrated mild weakness of the flexor carpi ulnaris and the interossei (Grade 4/5), consistent with mild ulnar neuropathy. The median and radial nerves were intact with no motor or sensory deficits. Radial and ulnar pulses were 2+ bilaterally, and capillary refill was brisk, indicating intact distal perfusion.
Introduction and Epidemiology
Post-traumatic elbow contracture represents a formidable challenge in orthopedic surgery, frequently complicated by the development of heterotopic ossification. The elbow joint is notoriously prone to stiffness following trauma due to its highly congruent osseous anatomy, the intimate proximity of its capsuloligamentous structures to the joint axis, and a robust fibroblastic response to injury.
Heterotopic ossification is defined as the formation of mature, lamellar bone in non-osseous tissues, most commonly within muscles, joint capsules, and fascial planes. In the context of elbow trauma, the incidence of heterotopic ossification varies significantly based on the severity of the injury. Simple elbow dislocations carry a relatively low risk (approximately 3 percent), whereas complex instability patterns, such as the terrible triad of the elbow, or high-energy intra-articular distal humerus fractures (AO/OTA Type 13-C), can exhibit heterotopic ossification rates approaching 30 to 40 percent.
The pathophysiology of heterotopic ossification involves the inappropriate differentiation of pluripotent mesenchymal stem cells into osteoblasts. This osteoinductive cascade is triggered by local tissue hypoxia, profound inflammatory responses, and the release of bone morphogenetic proteins, specifically BMP-2 and BMP-4, from the fracture hematoma and traumatized muscle. Systemic factors also play a critical role; patients with concomitant traumatic brain injury or severe burns exhibit a markedly amplified osteogenic response, likely mediated by systemic neurohumoral factors and accelerated osteoblastogenesis.
In the clinical vignette presented, the patient exhibits classic risk factors for profound post-traumatic stiffness and heterotopic ossification, including a high-energy mechanism, comminuted intra-articular fractures requiring extensive surgical exposure, delayed mobilization (three weeks of immobilization), and radial head excision. The presence of a hard, bony end-feel combined with ulnar neuropathy strongly suggests that the heterotopic bone has bridged the ulnohumeral articulation and encroached upon the cubital tunnel.
Surgical Anatomy and Biomechanics
A profound understanding of elbow anatomy and kinematics is a prerequisite for executing a safe and effective contracture release. The elbow is a highly constrained hinge (ginglymus) joint, though it permits a complex interplay of flexion, extension, and forearm rotation.
The primary stabilizers of the elbow include the highly congruent ulnohumeral articulation, the medial collateral ligament complex, and the lateral collateral ligament complex. The anterior band of the medial collateral ligament is the primary restraint to valgus stress, originating from the anteroinferior surface of the medial epicondyle and inserting onto the sublime tubercle of the ulna. The lateral ulnar collateral ligament is the primary restraint to posterolateral rotatory instability, originating from the lateral epicondyle and inserting onto the supinator crest of the ulna.
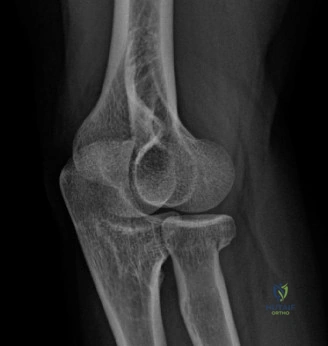
The functional arc of elbow motion, as described by Morrey, requires 30 to 130 degrees of flexion and 50 degrees of both pronation and supination to perform 90 percent of activities of daily living. The patient in our vignette, possessing an arc of only 70 to 105 degrees, is severely functionally debilitated.
In the setting of post-traumatic contracture, the joint capsule undergoes predictable pathologic changes. The anterior capsule typically thickens and contracts, limiting extension. Conversely, the posterior capsule, along with the posterior band of the medial collateral ligament, becomes fibrotic and limits flexion. Heterotopic ossification frequently develops within these capsular planes, particularly in the posterior-medial compartment between the olecranon and the medial epicondyle, directly adjacent to the ulnar nerve.
The intimate relationship of the neurovascular structures to the joint capsule dictates the surgical approach. The ulnar nerve traverses posterior to the medial epicondyle through the cubital tunnel, roofed by Osborne's fascia. In post-traumatic settings, the normal anatomic planes are frequently obliterated by scar tissue and heterotopic bone, tethering the nerve and rendering it highly susceptible to iatrogenic injury during dissection or subsequent mechanical stretch following the restoration of flexion. The radial nerve crosses the radiocapitellar joint anteriorly, placing it at risk during anterior capsulectomy or lateral heterotopic ossification excision.
Indications and Contraindications
The decision to proceed with operative intervention for post-traumatic elbow contracture and heterotopic ossification requires a careful assessment of the patient's functional deficit, the maturity of the heterotopic bone, and the exhaustion of non-operative modalities.
Historically, surgical excision of heterotopic ossification was delayed for 12 to 18 months until the bone was deemed metabolically mature, as indicated by a normalized serum alkaline phosphatase and a quiescent triphasic technetium-99m bone scan. However, contemporary literature supports earlier intervention (typically 6 to 9 months post-injury) once the radiographic appearance of the heterotopic ossification demonstrates sharp, well-corticated margins on computed tomography, and the patient's range of motion has definitively plateaued despite aggressive therapy. Early intervention prevents secondary articular cartilage degradation and progressive capsular contracture.
| Clinical Scenario | Operative Indications | Non-Operative Indications |
|---|---|---|
| Functional Deficit | Arc of motion less than 100 degrees; inability to perform ADLs | Functional arc preserved (30-130 degrees); minimal ADL impact |
| Therapy Response | Plateau in ROM despite 4-6 months of compliant, aggressive static progressive splinting and PT | Continued measurable improvement with physical therapy and splinting |
| HO Maturity | Well-corticated, trabeculated bone on CT; stable ROM for 3-4 months | Immature, fluffy, ill-defined ossification on radiographs |
| Neurologic Status | Progressive ulnar, median, or radial neuropathy secondary to HO compression | Intact neurovascular examination |
| Patient Factors | Compliant patient, optimized comorbidities, motivated for intense post-op rehab | Active infection, severe CRPS, non-compliant patient, active systemic illness |
Absolute contraindications to surgical release include active local or systemic infection and a patient unwilling or unable to participate in the rigorous postoperative rehabilitation protocol. Relative contraindications include severe, active Complex Regional Pain Syndrome, which can be exacerbated by surgical trauma, and profound articular destruction where an interposition arthroplasty or total elbow arthroplasty might be more appropriate than a simple contracture release.
Pre Operative Planning and Patient Positioning
Thorough preoperative planning is paramount to anticipate the location of heterotopic bone, identify retained hardware that may require removal, and map the trajectory of critical neurovascular structures.
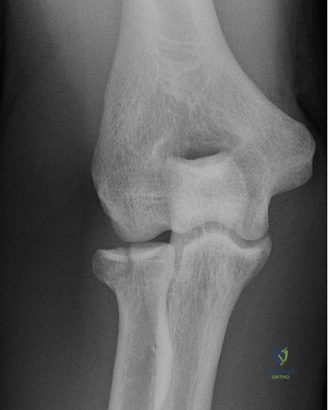
Standard orthogonal radiographs (anteroposterior and lateral) provide a baseline assessment of joint congruity, hardware position, and the gross extent of heterotopic ossification. However, a high-resolution Computed Tomography scan with three-dimensional reconstructions is the gold standard and an absolute requirement. The 3D CT scan allows the surgeon to precisely map the location of the heterotopic bone, distinguishing between extra-articular bridging bone and intra-articular osseous blocks. In our patient, the CT scan would explicitly define the posterior-medial mass and its relationship to the cubital tunnel and the medial column hardware.
Electromyography and nerve conduction studies are highly recommended in patients presenting with neurologic symptoms. Given our patient's clinical signs of ulnar neuropathy, an EMG/NCS will confirm the baseline severity of the compression, document any subclinical involvement of other nerves, and provide medicolegal protection.
Preoperative planning must also include a strategy for heterotopic ossification prophylaxis to prevent recurrence. The standard of care involves either non-steroidal anti-inflammatory drugs (typically Indomethacin 75mg sustained-release daily for 3 to 6 weeks) or localized external beam radiation therapy (a single dose of 700 to 800 cGy administered within 24 hours preoperatively or 48 hours postoperatively).
For patient positioning, the lateral decubitus position is generally preferred for extensive open elbow contracture releases. The patient is placed in the lateral decubitus position with the operative arm supported over an L-bar or a padded post. This position allows unobstructed access to both the medial and lateral compartments of the elbow, facilitates gravity-assisted retraction, and provides excellent visualization of the posterior structures. A sterile tourniquet is applied high on the brachium to ensure a bloodless field during the critical neurovascular dissection phases.
Detailed Surgical Approach and Technique
The surgical management of severe post-traumatic elbow contracture requires a meticulous, systematic approach. The goal is to sequentially address the anatomical structures limiting motion while preserving joint stability and protecting neurovascular elements. A universal posterior incision is the workhorse approach, allowing access to both the medial and lateral aspects of the joint through full-thickness fasciocutaneous flaps.
Approach Selection and Incision
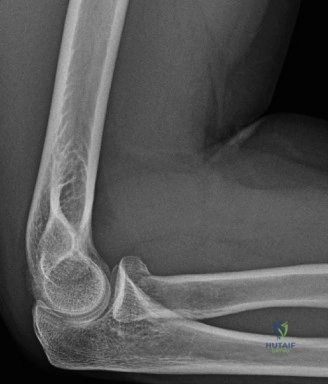
A longitudinal midline posterior incision is utilized, typically incorporating the previous surgical scar to minimize the risk of skin necrosis. The incision extends from the distal third of the humerus, curving slightly lateral to the tip of the olecranon, and continuing distally along the subcutaneous border of the ulna. Full-thickness fasciocutaneous flaps are elevated medially and laterally. It is critical to maintain the integrity of these flaps to preserve the vascular supply to the skin.
Ulnar Nerve Management
The absolute first step in the deep dissection is the identification, neurolysis, and protection of the ulnar nerve. Given the patient's preoperative ulnar neuropathy and the presence of posterior-medial heterotopic ossification, the nerve is at extreme risk. The nerve is located proximally in the arm, where the anatomy is relatively undisturbed, and traced distally into the cubital tunnel.
The nerve must be carefully dissected free from the encasing scar tissue and any impinging heterotopic bone. The arcade of Struthers, the medial intermuscular septum, Osborne's fascia, and the deep aponeurosis of the flexor carpi ulnaris must be sequentially released. Once fully mobilized, the nerve is protected with a vessel loop. In cases of preoperative neuropathy or significant osseous deformity requiring extensive medial dissection, an anterior subcutaneous or submuscular transposition is routinely performed to relieve tension on the nerve during postoperative flexion.
Contracture Release and Heterotopic Ossification Excision
Following ulnar nerve management, a sequential release is performed based on the specific limitations in range of motion.
To address the flexion deficit (limited to 105 degrees in our patient), the posterior compartment is accessed. The triceps can be mobilized using a triceps-reflecting approach (Bryan-Morrey) or through paratricipital windows if the extensor mechanism allows sufficient retraction. The posterior capsule is excised. The posterior band of the medial collateral ligament, which is often contracted and thickened, is released.
Attention is then directed to the posterior-medial heterotopic ossification mass. Using osteotomes, rongeurs, and a high-speed burr, the heterotopic bone is meticulously excised. Care must be taken to distinguish the heterotopic bone from the native medial epicondyle and the sublime tubercle to avoid iatrogenic destabilization of the anterior band of the medial collateral ligament.
To address the extension deficit (70-degree contracture), the anterior compartment must be accessed. This is typically achieved through lateral and medial column windows. On the lateral side, the extensor origin is elevated from the lateral epicondyle (Kocher interval between the anconeus and extensor carpi ulnaris). The anterior capsule is identified and completely excised from the anterior humerus down to the radiocapitellar joint. The brachialis muscle is elevated off the anterior capsule to protect the median nerve and brachial artery, which lie immediately anterior to the muscle belly.
In our patient, the radial head was previously excised. The proximal radioulnar space must be inspected for heterotopic ossification or dense fibrotic scarring that may be tethering the radius to the ulna, explaining his severe rotational deficits (pronation 45 degrees, supination 30 degrees). Any bridging bone in the radial neck region must be resected to restore forearm rotation.
Closure and Hemostasis
Once the release and heterotopic ossification excision are complete, the joint is taken through a full range of motion to confirm the removal of all mechanical blocks. The tourniquet is deflated prior to closure to ensure meticulous hemostasis, as postoperative hematoma is a significant risk factor for recurrent heterotopic ossification and stiffness. A closed suction drain is placed deep within the joint space. The extensor origin and triceps intervals are meticulously repaired, and the skin is closed in a layered fashion.
Complications and Management
Surgical release of the stiff elbow is a complex procedure with a recognized complication profile. Careful preoperative optimization and meticulous surgical technique are required to mitigate these risks.
| Complication | Incidence | Etiology and Risk Factors | Management and Salvage Strategies |
|---|---|---|---|
| Recurrent HO / Stiffness | 10 - 20% | Inadequate initial resection, failure of prophylaxis, postoperative hematoma, poor rehab compliance | Optimization of secondary prophylaxis (XRT + Indomethacin), aggressive static progressive splinting, revision excision if severely symptomatic after 6-12 months |
| Ulnar Neuropathy | 5 - 15% | Iatrogenic traction, failure to adequately decompress, postoperative hematoma compression | Prompt evaluation; if progressive motor deficit, consider early re-exploration and anterior transposition. If mild sensory, observe with gabapentinoids |
| Iatrogenic Instability | 2 - 5% | Over-resection of the anterior band of MCL or LUCL during HO excision | Intraoperative recognition requires immediate ligamentous repair or reconstruction (e.g., palmaris longus autograft). Postoperative recognition requires hinged bracing and potential delayed reconstruction |
| Infection (Deep) | 1 - 3% | Prolonged operative time, extensive soft tissue dissection, compromised fasciocutaneous flaps | Aggressive surgical debridement, hardware removal if unneeded, culture-directed intravenous antibiotics |
| Postoperative Hematoma | 5 - 10% | Extensive bleeding from raw osseous surfaces after HO excision, inadequate hemostasis | Evacuation if causing severe pain, skin compromise, or neurologic compression. Prevention via drain placement and meticulous intraoperative hemostasis |

Ulnar neuropathy remains one of the most concerning complications. Even with meticulous neurolysis, the nerve can become ischemic or stretched as the elbow achieves new ranges of flexion postoperatively. Routine transposition in high-risk cases significantly reduces this complication.
Recurrent stiffness is often a result of patient guarding due to pain. Therefore, comprehensive perioperative pain management, including regional anesthesia (such as an indwelling supraclavicular or axillary nerve block catheter) for the first few postoperative days, is essential to allow for immediate, painless motion.
Post Operative Rehabilitation Protocols
The success of an elbow contracture release is intrinsically linked to the postoperative rehabilitation protocol. Surgery merely resets the anatomical potential for motion; rehabilitation secures it.
In the immediate postoperative phase (Days 0 to 3), the arm is typically placed in a bulky compressive dressing with an anterior plaster slab maintaining the elbow in maximal extension, as extension is notoriously the most difficult motion to regain and maintain. Regional analgesia via an indwelling catheter facilitates early mobilization. Continuous Passive Motion machines were historically utilized, but modern protocols favor early active and active-assisted range of motion exercises initiated within 24 to 48 hours postoperatively.
During Weeks 1 to 4, the focus shifts to aggressive edema control and frequent, daily range of motion exercises. The patient is transitioned to a static progressive or dynamic splinting program. A common regimen involves alternating between an extension splint worn at night and a flexion splint worn during specific periods of the day. Turnbuckle splints allow the patient to dial in progressive tension to stretch the maturing collagen fibers of the healing joint capsule.
Prophylaxis against heterotopic ossification must be strictly administered during this phase. If radiation therapy was utilized, it is completed within 48 hours. If pharmacological prophylaxis is chosen, Indomethacin (75mg sustained-release daily) is continued for a minimum of three to six weeks, provided there are no gastrointestinal or renal contraindications.
From Weeks 4 to 12, strengthening exercises are gradually introduced, but the primary emphasis remains on maximizing the functional arc of motion. Maximum medical improvement following an open contracture release is typically not achieved until 6 to 12 months postoperatively.
Summary of Key Literature and Guidelines
The management of post-traumatic elbow contracture and heterotopic ossification is guided by several foundational studies and evolving clinical guidelines.
The classification of heterotopic ossification about the elbow is most commonly described using the Hastings and Graham system. This classification categorizes heterotopic ossification based on clinical limitations and radiographic appearance:
* Class I: Radiographic presence of HO without functional limitation.
* Class II: HO causing limitation in the flexion/extension arc (IIA), pronation/supination (IIB), or both (IIC).
* Class III: Complete bony ankylosis preventing flexion/extension (IIIA), pronation/supination (IIIB), or both (IIIC).
Our patient presents with a severe Class IIC moving towards Class III given the rigid bony end-feel and profound multiaxial restrictions.
Morrey's seminal work on the functional arc of motion remains the benchmark for evaluating surgical success. Achieving an arc from 30 degrees of extension to 130 degrees of flexion is the primary goal, as this restores the patient's ability to position the hand in space for feeding, hygiene, and occupational tasks.
Jupiter and Ring have extensively published on the outcomes of surgical release following distal humerus fractures. Their data underscores that while functional motion can be reliably restored, patients rarely achieve normal, symmetric motion compared to the contralateral limb. They also highlight the critical importance of secure initial fracture fixation to allow for early mobilization, which is the most effective prophylaxis against contracture.
Recent consensus guidelines regarding the timing of heterotopic ossification excision have shifted the paradigm from waiting for metabolic maturity (as defined by bone scans) to radiographic maturity (defined by well-corticated margins on CT). Studies have demonstrated that earlier excision (6 to 9 months) yields equivalent or superior functional outcomes compared to delayed excision (18+ months), while significantly reducing the duration of patient disability and minimizing secondary joint degeneration. Prophylaxis with either NSAIDs or radiation therapy is universally recommended following excision, with recent meta-analyses showing equivalent efficacy between the two
