Comprehensive Introduction and Patho-Epidemiology
The first metatarsophalangeal joint (MTPJ) is a critical biomechanical fulcrum in the human foot, essential for normal ambulation, balance, and weight transfer during the terminal stance phase of gait. Pathology affecting this joint is ubiquitous in orthopedic practice, encompassing a broad spectrum of conditions from hallux rigidus and hallux valgus to inflammatory arthropathies and post-traumatic degenerative joint disease. Understanding the surgical options for the first MTPJ requires a profound appreciation of both the natural history of these conditions and the biomechanical demands placed upon the medial column of the foot.
Hallux rigidus, characterized by progressive osteophyte formation and articular cartilage degeneration, is the most common osteoarthritic condition of the foot. Epidemiological studies suggest it affects approximately 10% of the adult population, with a predilection for females and a bimodal age distribution peaking in the third and sixth decades. The etiology is multifactorial, involving a combination of repetitive microtrauma, altered foot biomechanics (such as metatarsus primus elevatus), genetic predisposition, and occasionally, frank osteochondral defects. As the dorsal articular surface degrades and dorsal osteophytes proliferate, patients experience a mechanical block to dorsiflexion, leading to pain, altered gait kinematics, and subsequent transfer lesions across the lesser metatarsals.

Conversely, hallux valgus presents a complex three-dimensional deformity involving lateral deviation and pronation of the proximal phalanx, medial deviation of the first metatarsal, and lateral subluxation of the sesamoid apparatus. While mild-to-moderate deformities are often managed with joint-sparing osteotomies, severe deformities with concomitant degenerative changes necessitate definitive joint-sacrificing procedures. Furthermore, systemic inflammatory conditions, such as rheumatoid arthritis, frequently target the first MTPJ, causing profound capsular attenuation, erosive articular destruction, and severe multi-planar instability.
The surgical armamentarium for first MTPJ pathology is extensive, ranging from joint-preserving procedures like cheilectomy and corrective osteotomies to definitive salvage operations such as arthrodesis and arthroplasty. The selection of the optimal procedure is predicated on a meticulous evaluation of the patient's physiological age, activity level, disease severity, and the presence of adjacent joint pathology. Arthrodesis remains the gold standard for end-stage disease, providing predictable pain relief and functional restoration, though joint-sparing options like cheilectomy offer excellent outcomes for early-to-mid-stage hallux rigidus.

Detailed Surgical Anatomy and Biomechanics
Osteology and Articular Anatomy
The first MTPJ is a complex diarthrodial joint formed by the articulation of the convex first metatarsal head and the concave base of the proximal phalanx. The metatarsal head is unique, possessing a larger dorsal-to-plantar dimension than medial-to-lateral, which accommodates the extensive sagittal plane motion required during gait. Plantarly, the metatarsal head features two longitudinal grooves separated by a central ridge (the crista), which articulate with the medial (tibial) and lateral (fibular) sesamoids. The sesamoids are embedded within the tendons of the flexor hallucis brevis (FHB) and serve to increase the mechanical advantage of the intrinsic flexors while protecting the flexor hallucis longus (FHL) tendon that glides between them.

Ligamentous and Capsular Structures
Stability of the first MTPJ is conferred by a robust capsuloligamentous complex. The proper collateral ligaments originate from the medial and lateral epicondyles of the metatarsal head and insert onto the plantar-medial and plantar-lateral aspects of the proximal phalanx base. The accessory collateral ligaments fan out plantarly to insert into the plantar plate and the sesamoid complex. The plantar plate itself is a thick, fibrocartilaginous structure that resists hyperextension and provides a congruent articulating surface for the metatarsal head. The dynamic stabilizers include the abductor hallucis medially, the adductor hallucis laterally, the extensor hallucis longus (EHL) and brevis (EHB) dorsally, and the FHL and FHB plantarly.

Biomechanics and Kinematics
The biomechanics of the foot and ankle dictate the functional requirements of the first MTPJ. Normal ambulation requires a complex interplay of joint motions. As established in fundamental orthopedic principles, the standard functional ranges of motion (ROM) for the foot and ankle complex are:
* Subtalar joint inversion: 10°
* Subtalar joint eversion: 5°
* Transverse tarsal joint adduction: 20°
* Transverse tarsal joint abduction: 10°
* Combined foot supination: 30°
* Combined foot pronation: 15°
* First metatarsophalangeal joint flexion: 30°
* First metatarsophalangeal joint extension: 60°
The 60 degrees of first MTPJ extension is absolutely critical for the "Windlass mechanism," first described by Hicks. During the heel-off phase of gait, dorsiflexion of the hallux winds the plantar fascia around the metatarsal head, pulling the calcaneus toward the metatarsal heads, elevating the longitudinal arch, and locking the midtarsal joints. This converts the foot into a rigid lever for effective forward propulsion. Loss of this extension, as seen in hallux rigidus, forces the patient to supinate the foot and roll off the lateral border, leading to lateral column overload, transfer metatarsalgia, and altered proximal joint kinematics.

Exhaustive Indications and Contraindications
The decision-making algorithm for first MTPJ surgery hinges on an accurate diagnosis, radiographic staging (such as the Coughlin and Shurnas classification for hallux rigidus), and a thorough understanding of the patient's functional demands. Given the large number of adjacent joints in the foot and ankle, it can be useful to localize the exact source of pain with a diagnostic intra-articular injection of local anesthetic. This is particularly crucial when differentiating first MTPJ pain from sesamoiditis, interdigital neuroma, or tarsometatarsal (TMT) joint arthrosis.

Cheilectomy is primarily indicated for early to moderate hallux rigidus (Coughlin and Shurnas Grades 1 and 2, and select Grade 3 cases) where the pathology is predominantly dorsal. The goal is to resect the dorsal osteophytes and the dorsal 30% of the metatarsal head to decompress the joint and restore dorsiflexion. It is contraindicated in advanced joint space narrowing, inflammatory arthropathy, or when pain is present throughout the entire arc of motion (indicating global articular destruction).
First MTPJ arthrodesis is the definitive, gold-standard procedure for end-stage hallux rigidus (Grade 3 and 4), severe hallux valgus with degenerative changes, inflammatory arthritis, neuromuscular deformities, and salvage of failed prior first ray surgery. Arthrodesis provides predictable pain relief and a stable medial column. Contraindications are relatively few but include active infection, severe vascular compromise, and ipsilateral interphalangeal (IP) joint arthritis (as a fused MTPJ will increase stress on the IP joint, exacerbating symptoms).

| Surgical Procedure | Primary Indications | Absolute Contraindications | Relative Contraindications |
|---|---|---|---|
| Cheilectomy | Coughlin Grade 1-2 Hallux Rigidus; Dorsal impingement pain; Preserved plantar articular cartilage. | Advanced joint space collapse; Inflammatory arthritis; Pain in mid-arc of motion. | Significant metatarsus primus elevatus; Severe hallux valgus. |
| Arthrodesis | Coughlin Grade 3-4 Hallux Rigidus; Severe/recurrent Hallux Valgus; Rheumatoid arthritis; Salvage of failed arthroplasty. | Active local infection; Severe peripheral arterial disease; Inadequate soft tissue coverage. | Symptomatic ipsilateral IP joint arthritis; Non-compliant patient (NWB restrictions). |
| Arthroplasty (Silicone/Metallic) | Low-demand, elderly patients with end-stage arthritis; Patients refusing arthrodesis. | Young, active, high-demand patients; Prior joint infection; Significant bone loss. | Severe osteopenia; Uncorrectable malalignment. |

Pre-Operative Planning, Templating, and Patient Positioning
Clinical and Radiographic Evaluation
Meticulous preoperative planning is the cornerstone of successful first MTPJ surgery. The clinical examination must assess the vascular status (palpation of dorsalis pedis and posterior tibial pulses, with ABIs if indicated), neurological function, and the quality of the soft tissue envelope. The range of motion of the first MTPJ, IP joint, and first TMT joint must be documented. Pain elicited only at terminal dorsiflexion suggests dorsal impingement amenable to cheilectomy, whereas pain throughout the arc of motion or crepitus suggests global joint destruction requiring arthrodesis.
Radiographic evaluation demands standard weight-bearing anteroposterior (AP), lateral, and sesamoid axial views of the foot. On the AP view, the surgeon must evaluate the joint space, the presence of medial/lateral osteophytes, the hallux valgus angle (HVA), and the intermetatarsal angle (IMA). The lateral view is critical for assessing the size of the dorsal osteophyte, the sagittal alignment of the first metatarsal, and the presence of IP joint arthritis. Templating is particularly important for arthrodesis to determine the size of the fixation hardware and to plan the optimal fusion angles.

Patient Positioning and Setup
The patient is typically positioned supine on the operating table. A bump may be placed under the ipsilateral hip to internally rotate the leg, bringing the foot into a neutral, upward-facing position, which greatly facilitates exposure of the medial column. A thigh or calf tourniquet is applied based on surgeon preference and patient vascular status. Intravenous antibiotics are administered 30 minutes prior to inflation. The foot and ankle are prepped and draped in a standard sterile fashion, ensuring the toes are exposed to allow for intraoperative assessment of alignment and rotation.

Step-by-Step Surgical Approach and Fixation Technique
The Dorsal Approach to the First MTPJ
The standard approach for both cheilectomy and arthrodesis is a dorsal longitudinal incision. The incision is centered over the first MTPJ, extending approximately 3 cm proximal and 3 cm distal to the joint line, situated just medial to the EHL tendon. Careful subcutaneous dissection is performed to protect the dorsomedial cutaneous nerve (a branch of the superficial peroneal nerve) and the proper digital nerve to the medial hallux. The EHL tendon is mobilized and retracted laterally. A longitudinal capsulotomy is then performed, exposing the dorsal aspect of the metatarsal head and the base of the proximal phalanx.

Technique: First MTPJ Cheilectomy
For a cheilectomy, the joint is maximally plantarflexed to expose the dorsal metatarsal head. Using a microsagittal saw or an osteotome, the dorsal osteophyte and the dorsal 25% to 30% of the metatarsal head are resected. The cut should be angled slightly plantarly from distal to proximal to ensure a smooth transition and prevent a new ridge from forming. Marginal osteophytes on the medial, lateral, and phalangeal sides are excised using a rongeur. The joint is then aggressively irrigated, and the surgeon must confirm that at least 60 to 70 degrees of passive dorsiflexion is achieved without impingement. The capsule is closed meticulously to prevent EHL bowstringing.

Technique: First MTPJ Arthrodesis
Arthrodesis requires meticulous joint preparation and rigid internal fixation. The principles of foot and ankle arthrodesis dictate that all cartilage and subchondral bone must be removed down to bleeding, healthy cancellous bone.
- Joint Preparation: After exposing the joint, the collateral ligaments are released to allow for severe plantarflexion and complete exposure of the articular surfaces. Cartilage is removed using either flat cuts with a saw or, more commonly, cup-and-cone reamers. Cup-and-cone reamers are advantageous as they preserve bone stock, allow for multi-planar micro-adjustments of the fusion angle, and maximize the cancellous surface area for osteogenesis. Subchondral drilling or feathering with an osteotome is performed to enhance marrow egress and vascularity.
- Positioning: Positioning is the most critical step of the procedure. The ideal position for arthrodesis is:
- Valgus: 10° to 15° of valgus (matching the contralateral side, allowing the toe to sit adjacent to the second toe without impingement).
- Dorsiflexion: 10° to 15° of dorsiflexion relative to the floor, or roughly 15° to 20° relative to the axis of the first metatarsal. This allows the IP joint to rest comfortably on the ground during weight-bearing and accommodates a standard shoe heel.
- Rotation: Neutral rotation, ensuring the toenail is facing directly upwards.
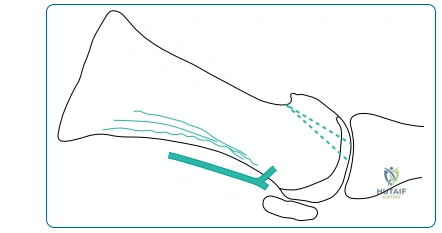
- Fixation: Once provisional fixation with Kirschner wires is achieved and the position is confirmed both clinically (by simulating weight-bearing with a flat plate against the foot) and fluoroscopically, definitive fixation is applied. The modern gold standard construct is a combination of a solid interfragmentary lag screw (typically a 3.5mm or 4.0mm screw placed from plantarmedial-distal to dorsolateral-proximal) combined with a low-profile dorsal titanium neutralization plate. This construct provides superior biomechanical stability, resisting both bending and torsional forces, thereby maximizing union rates.

Complications, Incidence Rates, and Salvage Management
Despite high success rates, first MTPJ surgery is not without complications. The surgeon must be acutely aware of potential pitfalls and possess the technical acumen to manage them effectively.
Nonunion (pseudoarthrosis) is the most significant complication following arthrodesis, with reported rates ranging from 5% to 10%. Risk factors include smoking, diabetes, inadequate fixation, and technical errors such as failing to adequately prepare the joint surfaces. Fortunately, many nonunions are asymptomatic and require no intervention. Symptomatic nonunions necessitate revision surgery, which often involves taking down the pseudoarthrosis, utilizing structural autograft or allograft (such as an iliac crest bone graft) to restore length, and applying more robust fixation.
Malunion is arguably more problematic than nonunion, as it directly alters foot biomechanics. Excessive dorsiflexion leads to dorsal shoe wear irritation and transfer metatarsalgia beneath the lesser metatarsal heads due to a lack of medial column weight-bearing. Excessive plantarflexion results in excessive pressure on the tip of the hallux and rapid degeneration of the IP joint. Varus malalignment causes the hallux to rub against the medial shoe counter, while excessive valgus causes impingement against the second toe. Revision for malunion requires a corrective closing or opening wedge osteotomy through the fusion mass.

| Complication | Estimated Incidence | Etiology / Risk Factors | Salvage / Management Strategy |
|---|---|---|---|
| Nonunion | 5% - 10% | Smoking, poor bone prep, inadequate fixation stability. | If asymptomatic: Observe. If symptomatic: Revision arthrodesis with bone graft and rigid plating. |
| Malunion | 5% - 8% | Intraoperative positioning error; failure to simulate weight-bearing. | Corrective osteotomy through the fusion mass; realign and re-fixate. |
| Hardware Irritation | 10% - 15% | Prominent dorsal plate; thin soft tissue envelope. | Hardware removal after radiographic confirmation of solid union (typically >6 months). |
| Transfer Metatarsalgia | 5% - 12% | First ray shortening; excessive dorsiflexion of the fusion. | Orthotics with metatarsal pads; rarely requires lesser metatarsal Weil osteotomies. |
| IP Joint Degeneration | 10% - 20% (Long-term) | Excessive plantarflexion of fusion; pre-existing IP joint disease. | Rocker-bottom shoe modifications; IP joint arthrodesis (rarely required). |

Phased Post-Operative Rehabilitation Protocols
The postoperative rehabilitation protocol must be tailored to the specific procedure performed, balancing the need for early mobilization to prevent stiffness with the necessity of protecting the repair or fusion site.
Post-Cheilectomy Protocol
Following a cheilectomy, the primary goal is the rapid restoration of motion to prevent capsular scarring and recurrence of stiffness.
* Weeks 0-2: The patient is placed in a stiff-soled postoperative shoe and is allowed to weight-bear as tolerated on the heel and lateral border of the foot. Elevation is emphasized to control edema.
* Weeks 2-6: Sutures are removed at 2 weeks. Aggressive passive and active range of motion exercises of the first MTPJ are initiated immediately. Patients are encouraged to perform manual stretching into dorsiflexion multiple times a day. Transition to comfortable, wide-toe-box footwear is permitted as swelling subsides.
* Weeks 6+: Return to normal activities and sports is allowed as tolerated. Maximum medical improvement regarding range of motion may take up to 6 to 12 months.

Post-Arthrodesis Protocol
Arthrodesis requires strict protection of the fixation construct until biological union occurs.
* Weeks 0-2: The patient is immobilized in a bulky Jones dressing and a posterior splint or a rigid cast boot. Weight-bearing is restricted to heel-touch or strict non-weight-bearing with crutches, depending on bone quality and fixation strength.
* Weeks 2-6: Sutures are removed. The patient is transitioned to a controlled ankle motion (CAM) boot. Heel-weight-bearing or flat-foot weight-bearing in the boot is initiated. No roll-off is permitted.
* Weeks 6-10: Radiographs are obtained to assess for bridging trabecular bone. If clinical and radiographic signs of union are present, the patient is gradually transitioned into a stiff-soled athletic shoe or a shoe with a rocker-bottom modification.
* Months 3-6: Progressive return to higher-impact activities. Swelling may persist for up to a year, and patients should be counseled accordingly.

Summary of Landmark Literature and Clinical Guidelines
The surgical management of the first MTPJ is heavily guided by landmark literature that has shaped modern orthopedic consensus. The seminal work by Coughlin and Shurnas established the most widely utilized clinical and radiographic grading system for hallux rigidus, directly linking the grade of disease to the recommended surgical intervention. Their long-term outcomes studies demonstrated that cheilectomy provides excellent results for Grades 1 and 2, with over 85% of patients reporting significant pain relief and improved function at 10-year follow-up.

For first MTPJ arthrodesis, the biomechanical studies by Brodsky et al. and Politi et al. fundamentally changed fixation strategies. They demonstrated that the combination of an interfragmentary lag screw and a dorsal neutralization plate provides statistically significant superior stiffness and load-to-failure compared to crossed screws or Kirschner wires alone. This has directly correlated with a reduction in clinical nonunion rates in modern series.
Furthermore, comparative studies evaluating arthrodesis versus synthetic arthroplasty (such as silicone implants) have consistently shown that while arthroplasty may preserve some motion, arthrodesis provides superior long-term pain relief, lower revision rates, and better restoration of the medial column's weight-bearing capacity. Consequently, clinical guidelines from major orthopedic societies strongly favor arthrodesis over arthroplasty for young, active patients and those with severe deformity or bone loss. Understanding this literature is paramount for the orthopedic surgeon to provide evidence-based, patient-specific care for first MTPJ pathology.

Clinical & Radiographic Imaging Archive



















Detailed Chapters & Topics
Dive deeper into specialized chapters regarding surgery-of-the-foot
