First Metatarsal Surgery: Expert Solutions for Foot & Ankle Pain

Key Takeaway
Looking for accurate information on First Metatarsal Surgery: Expert Solutions for Foot & Ankle Pain? The midfoot bridges the hindfoot and forefoot, facilitating adduction and abduction. It includes intercuneiform, naviculocuneiform, and tarsalmetatarsal (TMT) joints. These joints are vital for foot biomechanics, with the fi rst metatarsal playing a significant role in forefoot stability and weight-bearing during the gait cycle, particularly at the first TMT joint.
Comprehensive Introduction and Patho-Epidemiology
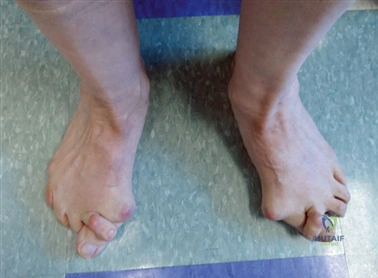
First metatarsal pathology encompasses a broad spectrum of debilitating conditions, ranging from hallux valgus and hallux rigidus to complex deformities associated with systemic arthropathies and neuromuscular disorders. As the principal weight-bearing axis of the medial forefoot, the first ray is subjected to immense biomechanical forces during the propulsive phase of the human gait cycle. Any structural or functional perturbation within this complex osteoligamentous network inevitably leads to altered load distribution, progressive deformity, and significant functional impairment. The surgical management of these conditions requires an exhaustive understanding of both local first ray anatomy and global foot and ankle kinematics.

Epidemiologically, hallux valgus alone affects nearly 23% of adults aged 18 to 65 years and over 35% of individuals older than 65 years, with a pronounced predilection for the female demographic. This gender disparity is classically attributed to a combination of intrinsic ligamentous laxity, hormonal influences, and extrinsic factors such as constrictive, narrow-toebox footwear with elevated heels. However, modern orthopedic consensus increasingly acknowledges the polygenic, hereditary nature of first ray deformities. Patients frequently exhibit a positive family history, suggesting an underlying genetic predisposition to metatarsus primus varus, hypermobility of the first tarsometatarsal (TMT) joint, or anomalous articular morphology.
The pathophysiology of first metatarsal disorders is fundamentally rooted in biomechanical failure. In the context of hallux valgus, the initial destabilization often occurs at the first TMT joint or the metatarsophalangeal (MTP) joint, leading to medial deviation of the first metatarsal and lateral subluxation of the proximal phalanx. As the deformity progresses, the intrinsic musculature—specifically the adductor hallucis—gains a mechanical advantage, further exacerbating the valgus drift and pronation of the hallux. Concurrently, the sesamoid apparatus remains tethered to the transverse metatarsal ligament, resulting in relative lateral subluxation of the sesamoids as the metatarsal head drifts medially.
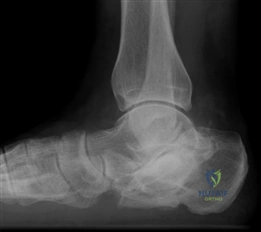
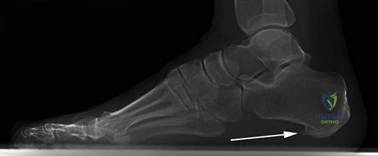
Conversely, hallux rigidus represents a degenerative cascade characterized by osteophyte formation, dorsal impingement, and progressive loss of sagittal plane motion at the first MTP joint. While trauma and inflammatory arthropathies can precipitate this condition, the most common etiology is idiopathic, often linked to an elevated or elongated first metatarsal (metatarsus primus elevatus), which alters the joint's instant center of rotation and accelerates articular wear. Recognizing these distinct pathophysiological pathways is paramount for the orthopedic surgeon, as it dictates the selection of joint-sparing osteotomies versus joint-sacrificing arthrodesis.
Detailed Surgical Anatomy and Biomechanics
Global Foot and Ankle Biomechanics
A profound mastery of first metatarsal surgery requires an appreciation of the global biomechanical environment of the lower extremity. The complex bony and ligamentous anatomy of the foot and ankle allows multiple foot positions and motion in three axes of rotation. The gait cycle is composed of a stance and swing phase, the mechanics of which are influenced by critical soft-tissue contributions. The midfoot serves as an indispensable bridge between the hindfoot and forefoot and is stabilized by robust longitudinal and transverse arches.
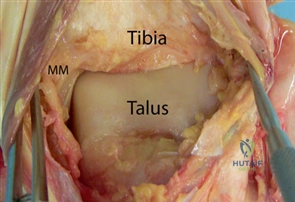
The ankle joint, an articulation between the tibial plafond, medial malleolus, lateral malleolus, and talus, is responsible for the majority of sagittal plane motion: dorsiflexion (10–23°) and plantarflexion (23–48°). Due to the trapezoidal shape of the talar dome, the mortise widens and the ankle becomes inherently more stable in dorsiflexion. The medial deltoid ligament complex acts as the main stabilizer of the ankle during stance, resisting lateral translation and valgus forces (talar tilt), while the lateral ligamentous complex acts as a primary restraint to varus forces. Proximal to this, the distal tibiofibular joint—consisting of the convex distal fibula and the concave incisura fibularis—allows the fibula to externally rotate approximately 2° during normal gait. Along with the syndesmotic ligaments, this articulation provides crucial stability against lateral talar translation.

Hindfoot and Midfoot Kinematics
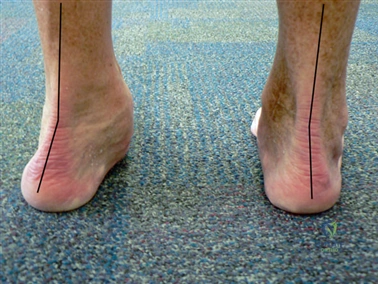
The hindfoot biomechanics are equally critical to forefoot function. The subtalar joint functions primarily in inversion and eversion. Limited eversion accommodation contributes significantly to the disability derived from even a mild cavovarus foot deformity, directly overloading the lateral border of the foot and subsequently altering the windlass mechanism of the first ray.
The transverse tarsal joint (Chopart joint), comprising the talonavicular (TN) and calcaneocuboid (CC) articulations, is paramount for providing stability to the hindfoot and midfoot to produce a rigid lever at toe-off. During heel strike, these joints are supple and their axes are parallel, allowing the foot to adapt to uneven terrain. As the stance phase progresses toward toe-off, hindfoot inversion causes these axes to become divergent and lock, providing essential stiffness to the longitudinal arch. Failure of the posterior tibial tendon to invert the hindfoot and lock the transverse tarsal joints is the primary biomechanical etiology for the lack of a heel rise in patients with posterior tibial tendon dysfunction (PTTD). This collapse dramatically increases the load on the first metatarsal, frequently precipitating secondary hallux valgus or midfoot arthritis.
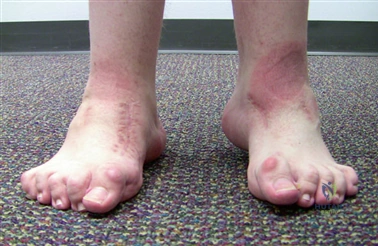
First Ray Specific Anatomy
The first ray functions as an independent biomechanical column consisting of the medial cuneiform and the first metatarsal. The first TMT joint is a complex, kidney-shaped articulation that exhibits primary motion in the sagittal and coronal planes. Hypermobility at this joint is a highly debated topic, yet it remains a critical consideration in the surgical planning of Lapidus arthrodesis. The vascular supply to the first metatarsal head is tenuous, supplied primarily by the first dorsal metatarsal artery and the plantar medial and lateral arteries. The intraosseous blood supply enters the metatarsal neck and travels proximally; thus, aggressive lateral soft-tissue stripping combined with a distal osteotomy poses a well-documented risk of avascular necrosis (AVN).
The sesamoid complex, embedded within the flexor hallucis brevis (FHB) tendons, acts as a fulcrum to increase the mechanical advantage of the intrinsic flexors. The tibial (medial) and fibular (lateral) sesamoids articulate with the plantar facets of the first metatarsal head, separated by the crista. In severe hallux valgus, the metatarsal head pronates and drifts medially off the sesamoid apparatus, leading to erosion of the crista and intractable pain. Surgical realignment must restore this delicate sesamoid-metatarsal relationship to ensure long-term success and prevent recurrence.
Exhaustive Indications and Contraindications
The decision to proceed with surgical intervention for first metatarsal pathology must be grounded in a thorough clinical evaluation, radiographic assessment, and a clear understanding of the patient's functional demands. Non-operative management—including shoe wear modification, orthoses, NSAIDs, and targeted corticosteroid injections—must be exhausted prior to considering surgical reconstruction.
When conservative measures fail, the choice of procedure is dictated by the severity of the deformity, the presence of degenerative joint disease, and the stability of the first TMT joint. Distal osteotomies (e.g., Chevron) are generally reserved for mild to moderate deformities with an intermetatarsal angle (IMA) less than 13 degrees. Diaphyseal osteotomies (e.g., Scarf) offer greater translational correction for moderate to severe deformities. Proximal procedures, such as the Lapidus arthrodesis, are indicated for severe deformities (IMA > 15 degrees), clinical hypermobility of the first TMT joint, or recurrent hallux valgus. For hallux rigidus, joint-sparing procedures like cheilectomy are indicated for early-stage disease, while first MTP arthrodesis remains the gold standard for end-stage arthritis.

| Surgical Procedure | Primary Indications | Absolute Contraindications | Relative Contraindications |
|---|---|---|---|
| Distal Osteotomy (Chevron) | Mild-moderate HV (IMA < 13°, HVA < 30°); Congruent MTP joint; No TMT hypermobility. | Severe degenerative MTP arthritis; Active infection; Severe peripheral vascular disease (PVD). | Osteopenia; High-demand athletes (requires careful consideration of fixation). |
| Diaphyseal Osteotomy (Scarf) | Moderate-severe HV (IMA 13-20°); Need for plantarflexion/shortening correction. | Narrow metatarsal diaphysis (risk of troughing); Severe MTP arthritis. | Advanced age with poor bone stock; Heavy smoking history. |
| TMT Arthrodesis (Lapidus) | Severe HV (IMA > 15°); First ray hypermobility; Recurrent HV; Medial column instability. | Open physes (in pediatric patients); Active midfoot infection. | Non-compliant patients (unable to maintain NWB status); Severe midfoot arthrosis. |
| First MTP Arthrodesis | End-stage hallux rigidus; Severe rheumatoid forefoot deformity; Salvage for failed HV surgery. | Active local infection; Critical limb ischemia. | Pre-existing severe interphalangeal (IP) joint arthritis (can lead to IP overload). |
| Cheilectomy | Coughlin/Shurnas Grade 1 or 2 hallux rigidus; Dorsal impingement pain with preserved plantar cartilage. | Grade 4 hallux rigidus (diffuse joint space narrowing); Severe angular deformity. | Systemic inflammatory arthropathy (e.g., Rheumatoid arthritis). |
Pre-Operative Planning, Templating, and Patient Positioning
Clinical and Radiographic Evaluation
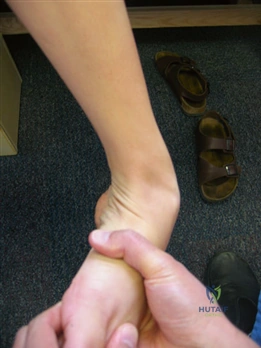
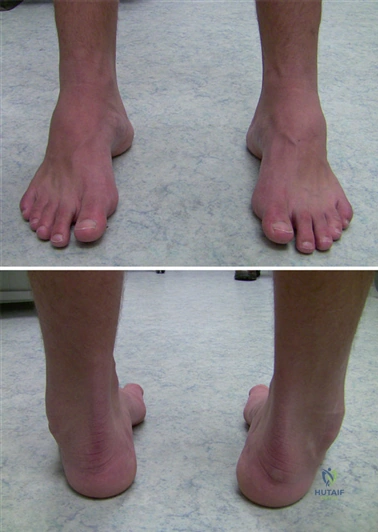
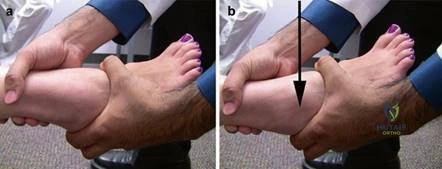
Meticulous pre-operative planning begins with a comprehensive physical examination. The surgeon must assess the vascular status (palpation of dorsalis pedis and posterior tibial pulses, capillary refill) and neurologic function. The Silfverskiöld test is utilized to evaluate for isolated gastrocnemius contracture, which can exacerbate forefoot overload and may necessitate a concomitant gastrocnemius recession. First ray mobility is assessed in the sagittal plane by stabilizing the lesser metatarsals and translating the first metatarsal head dorsally and plantarly; excessive excursion suggests TMT hypermobility.
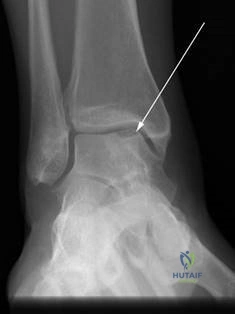
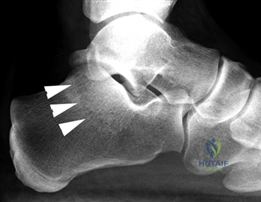
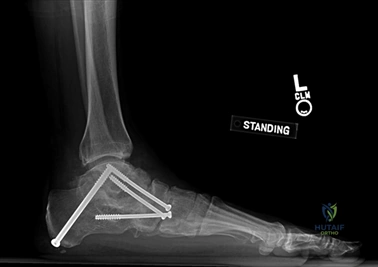
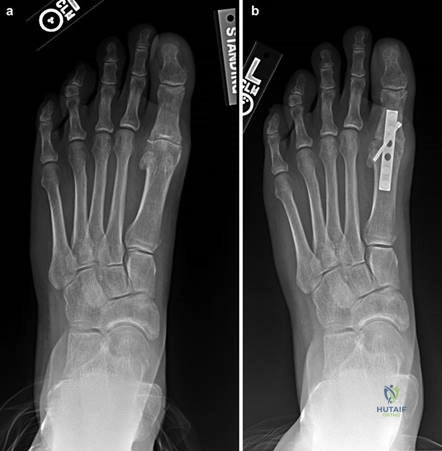
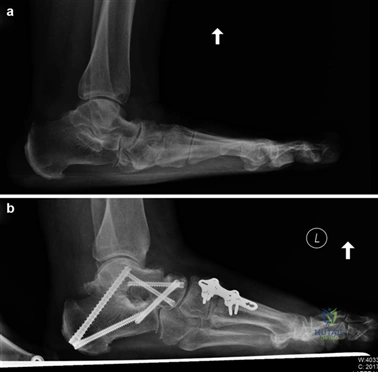
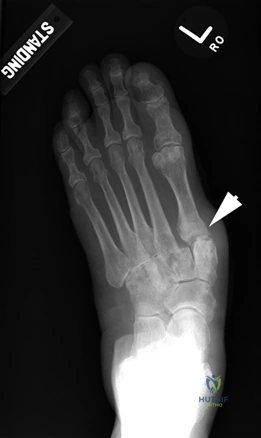
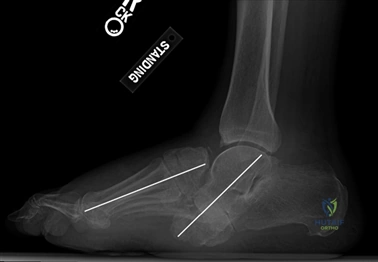
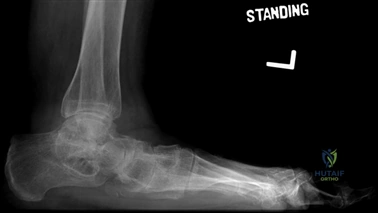
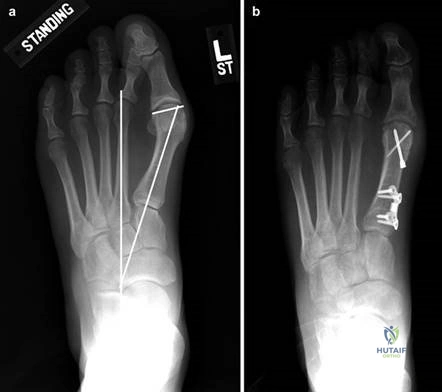
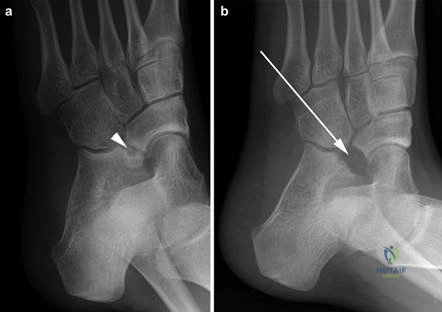
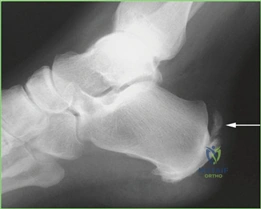
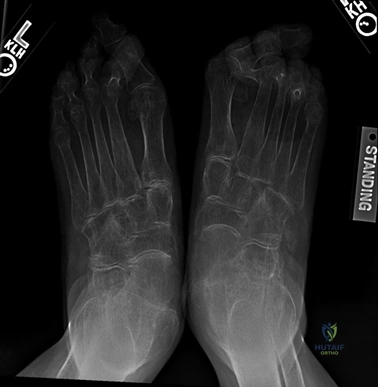
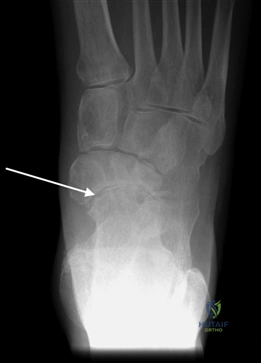
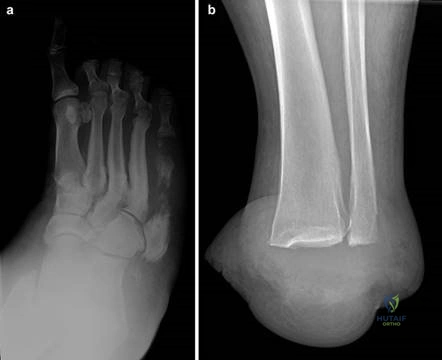
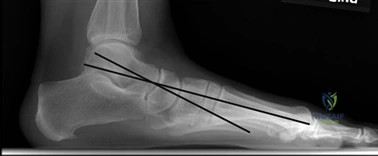
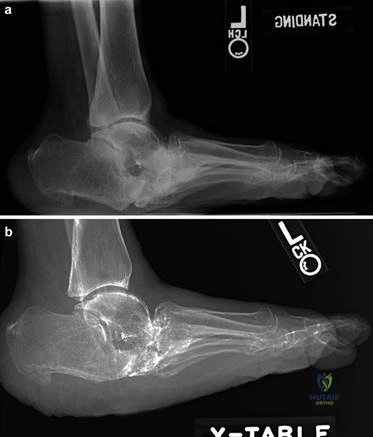
Weight-bearing anteroposterior (AP), lateral, and sesamoid axial radiographs are mandatory. On the AP view, the surgeon measures the Hallux Valgus Angle (HVA, normal < 15°), the Intermetatarsal Angle (IMA, normal < 9°), and the Distal Metatarsal Articular Angle (DMAA). The lateral view is scrutinized for Meary's angle (talo-first metatarsal angle) to identify midfoot collapse, as well as the presence of dorsal osteophytes indicative of hallux rigidus. The sesamoid axial view is critical for assessing the degree of sesamoid subluxation and the integrity of the crista.
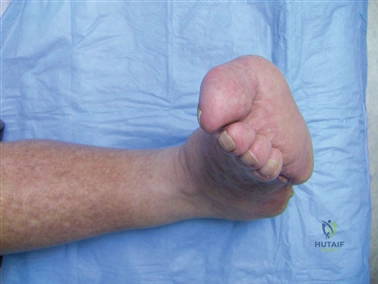
Digital Templating and Patient Positioning
Digital templating software is employed to determine the center of rotation of angulation (CORA) and to simulate the proposed osteotomy or fusion. This allows the surgeon to anticipate the degree of translation required, the potential for metatarsal shortening, and the appropriate size of fixation hardware. For a Lapidus procedure, templating helps calculate the exact wedge of bone to be resected from the medial cuneiform and first metatarsal base to achieve the desired multiplanar correction.
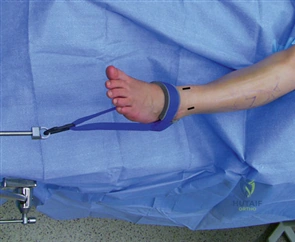
The patient is typically positioned supine on the operating table. A bump is placed under the ipsilateral hip to internally rotate the leg, bringing the foot into a neutral, upward-facing position, which greatly facilitates access to the medial column. A pneumatic tourniquet is placed either at the thigh or the calf, depending on surgeon preference and the planned proximal extent of the procedure. Intravenous prophylactic antibiotics are administered within one hour of incision, and a regional ankle block or popliteal sciatic nerve block is frequently utilized to provide preemptive analgesia and minimize volatile anesthetic requirements.
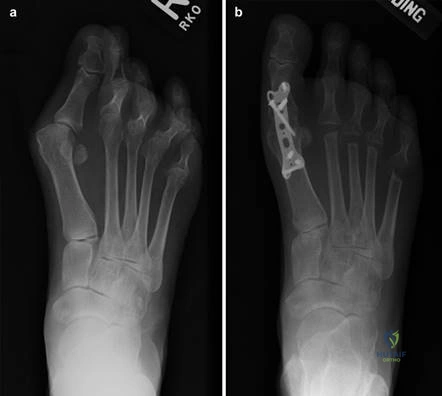
Step-by-Step Surgical Approach and Fixation Technique
The Modified Chevron Osteotomy
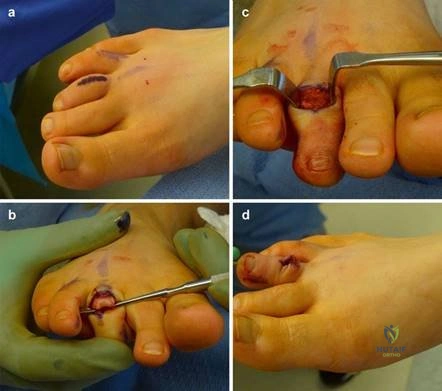
The modified distal Chevron osteotomy is a powerful tool for mild to moderate hallux valgus. A medial longitudinal incision is made centered over the first MTP joint. Dissection is carried down to the joint capsule, taking care to protect the dorsal medial cutaneous nerve. A midline or L-shaped capsulotomy is performed, exposing the medial eminence. The medial eminence is resected parallel to the medial border of the foot, preserving the sagittal groove to avoid disrupting the articular surface.
A V-shaped osteotomy is then created in the metatarsal neck with an apex angle of approximately 60 degrees. The apex is positioned centrally within the metatarsal head, and the limbs exit dorsally and plantarly. The capital fragment is translated laterally by 30-50% of the metatarsal shaft width. If the DMAA is increased, a medial closing wedge can be incorporated into the osteotomy. The osteotomy is provisionally stabilized with a Kirschner wire, and definitive fixation is achieved using one or two headless compression screws directed from dorsal-proximal to plantar-distal. The medial capsule is then imbricated to correct the soft-tissue imbalance, and the skin is closed in layers.
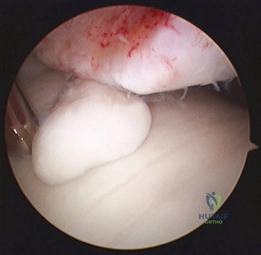
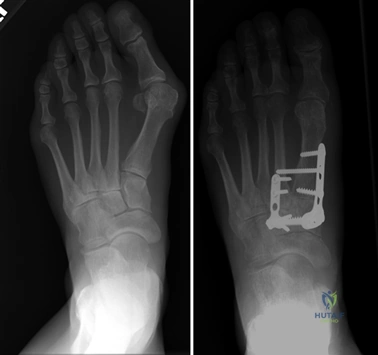
The Lapidus Arthrodesis (First TMT Fusion)
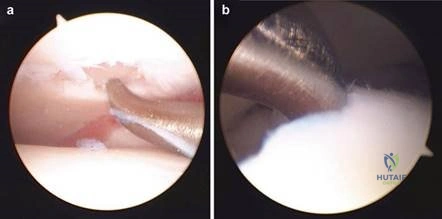
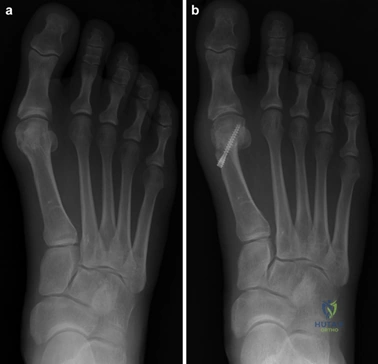
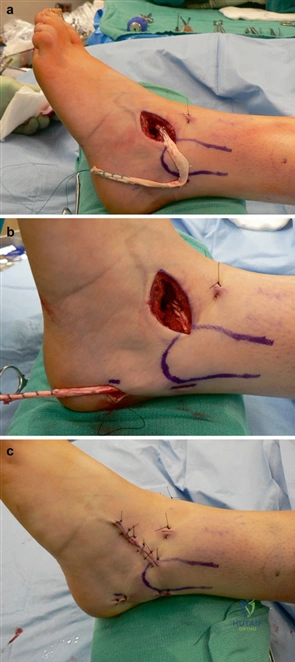
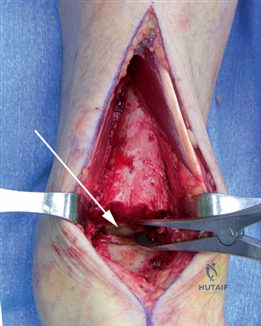
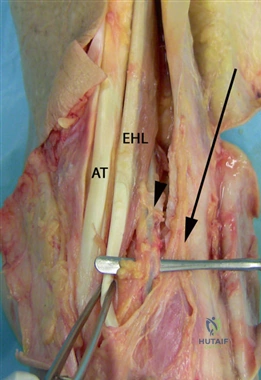
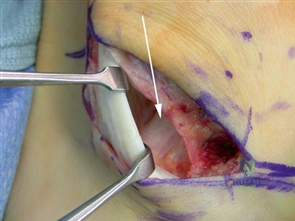
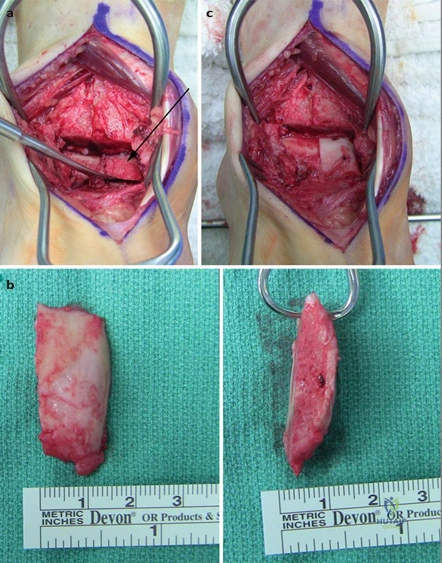
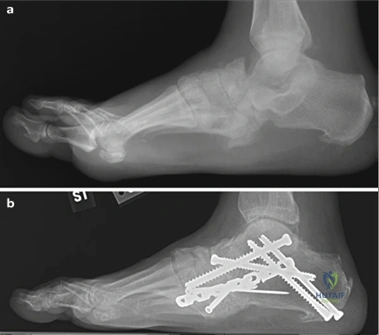
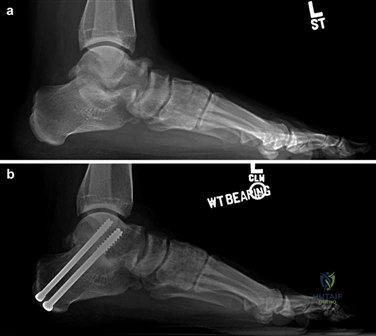
For severe deformities or hypermobility, the Lapidus procedure provides robust stabilization of the medial column. A dorsal or medial incision is utilized over the first TMT joint. The extensor hallucis longus (EHL) is retracted dorsally, and the tibialis anterior tendon is identified and protected at its insertion on the medial cuneiform and first metatarsal base. The TMT joint capsule is incised, and the joint is thoroughly debrided of all articular cartilage using a combination of osteotomes, curettes, and a high-speed burr.
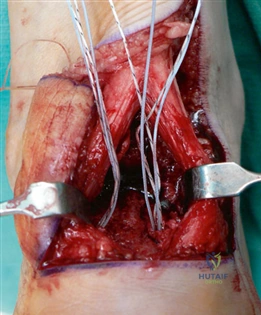
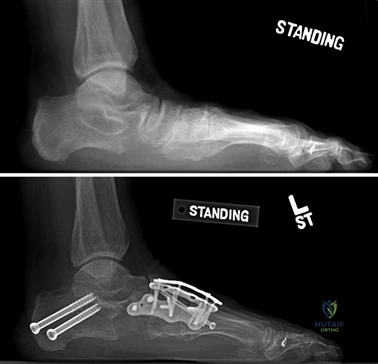
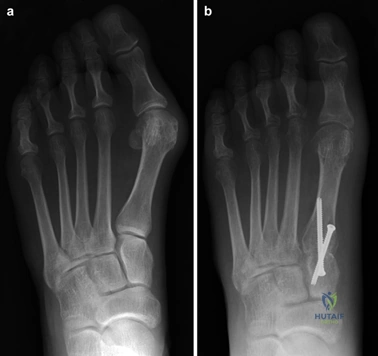
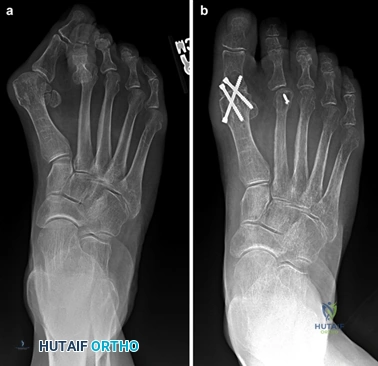
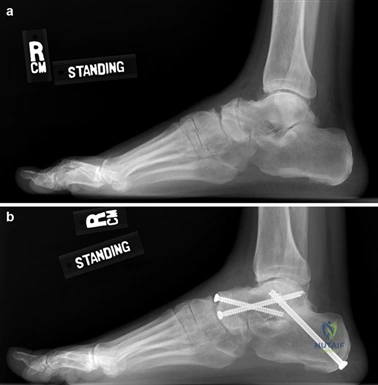
To achieve multiplanar correction, the surgeon must address the sagittal, coronal, and transverse planes. The first metatarsal is plantarflexed to restore the longitudinal arch, rotated out of pronation to realign the sesamoids, and translated laterally to close the IMA. Subchondral drilling or feathering is performed to optimize the biological environment for fusion. Fixation is traditionally achieved with two or three crossed solid or cannulated screws (typically 3.5mm or 4.0mm). Recently, plantar or medial locking plates have gained immense popularity due to their superior biomechanical construct, allowing for earlier weight-bearing. Bone graft or orthobiologics may be packed into the arthrodesis site to stimulate osteogenesis.
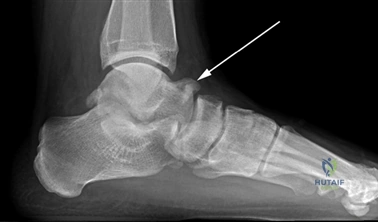
First MTP Arthrodesis
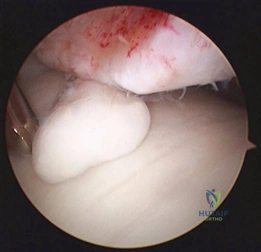
In cases of end-stage hallux rigidus, first MTP arthrodesis yields excellent, predictable outcomes. A dorsal longitudinal incision is made just medial to the EHL tendon. The joint is exposed, and aggressive cheilectomy is performed to remove all dorsal, medial, and lateral osteophytes. The remaining articular cartilage on the metatarsal head and the base of the proximal phalanx is resected using cup-and-cone reamers, which allow for infinite adjustment of the joint position prior to fixation.
Positioning of the fusion is the most critical step of the operation. The hallux must be positioned in 10-15 degrees of valgus, 15-20 degrees of dorsiflexion relative to the first metatarsal, and neutral rotation. Excessive dorsiflexion causes shoe impingement, while insufficient dorsiflexion leads to vaulting during gait and interphalangeal joint arthritis. Fixation is most reliably achieved using a pre-contoured dorsal locking plate combined with a lag screw crossing the fusion interface.
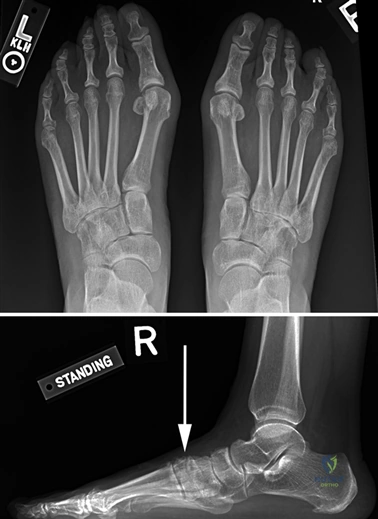
Complications, Incidence Rates, and Salvage Management
Despite meticulous surgical technique, complications in first metatarsal surgery are well-documented. Surgeons must be prepared to identify and manage these adverse events promptly to optimize patient outcomes.
| Complication | Estimated Incidence | Etiology / Risk Factors | Salvage Management / Treatment |
|---|---|---|---|
| Recurrence of Deformity | 10 - 15% | Under-correction of IMA; Failure to address frontal plane rotation; Unrecognized hypermobility. | Revision osteotomy; Conversion to Lapidus arthrodesis; Soft-tissue re-balancing. |
| Hallux Varus | 2 - 8% | Over-resection of medial eminence; Over-tightening of medial capsule; Aggressive lateral release. | Early: Taping/splinting. Late: EHB tendon transfer; Medial capsule release; MTP Arthrodesis. |
| Avascular Necrosis (AVN) | 1 - 3% | Extensive lateral soft-tissue stripping combined with distal osteotomy; Disruption of 1st dorsal metatarsal artery. | Protected weight-bearing; Bone stimulators. Severe collapse requires MTP Arthrodesis. |
| Nonunion (Lapidus/MTP) | 3 - 10% | Inadequate cartilage resection; Poor fixation construct; Patient non-compliance; Smoking. | Revision arthrodesis with structural bone grafting and robust locking plate fixation. |
| Transfer Metatarsalgia | 5 - 15% | Excessive shortening or dorsal elevation of the first metatarsal (malunion). | Orthotic management (metatarsal pads); Weil osteotomies of lesser metatarsals; Plantarflexing 1st TMT revision. |
| Hardware Irritation | 10 - 20% | Prominent screw heads or dorsal plates under thin soft-tissue envelope. | Symptomatic hardware removal after radiographic confirmation of complete union. |

Avascular necrosis of the metatarsal head is a devastating complication primarily associated with distal osteotomies. It presents with insidious onset of pain, swelling, and eventual radiographic collapse of the articular surface. Prevention is paramount and relies on preserving the plantar-lateral soft tissue attachments during the lateral release. If symptomatic AVN occurs and progresses to joint destruction, the definitive salvage procedure is a first MTP arthrodesis, often requiring structural bone grafting to restore metatarsal length.
Hallux varus, characterized by medial deviation of the hallux, is an iatrogenic complication that is deeply frustrating for both the surgeon and the patient. It is typically the result of a "staged" error: over-resection of the medial eminence past the sagittal sulcus, combined with over-plication of the medial capsule and complete transection of the lateral collateral ligament. Flexible deformities can occasionally be managed with an extensor hallucis brevis (EHB) tenodesis, while rigid deformities inevitably require arthrodesis.
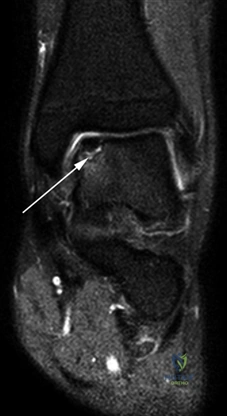
Phased Post-Operative Rehabilitation Protocols
The post-operative rehabilitation following first metatarsal surgery is dictated by the specific procedure performed, the stability of the fixation construct, and the biological healing requirements of the osteotomy or arthrodesis. A standardized, phased approach ensures protection of the surgical site while mitigating the risks of joint stiffness and disuse atrophy.
Phase 1: Maximum Protection (Weeks 0 - 2)
Immediately post-operatively, the foot is placed in a bulky, compressive Jones dressing with a posterior splint to maintain the ankle in neutral and protect the forefoot. For distal osteotomies (e.g., Chevron), patients are typically allowed heel-touch or flat-foot weight-bearing in a rigid post-operative shoe. For proximal osteotomies or Lapidus arthrodesis, strict non-weight-bearing (NWB) with crutches or a knee scooter is traditionally mandated to prevent sheer forces across the fusion site. Elevation of the limb above the level of the heart is strictly enforced to minimize edema and promote wound healing. At the two-week mark, sutures are removed, and clinical alignment is assessed.

Phase 2: Controlled Loading and Early Motion (Weeks 2 - 6)
During this phase, patients transition to a Controlled Ankle Motion (CAM) boot. For distal osteotomies, progressive weight-bearing to tolerance is permitted. Crucially, active and passive range of motion (ROM) exercises of the first MTP joint are initiated to prevent capsular adhesions. The patient is instructed to manually plantarflex and dorsiflex the hallux multiple times daily. For Lapidus patients, NWB is generally maintained until 4 to 6 weeks, though recent literature utilizing robust plantar plating constructs has pushed for earlier protected weight-bearing. Radiographs are obtained at 6 weeks to assess for early callus formation and maintenance of alignment.
Phase 3: Transition and Strengthening (Weeks 6 - 12)
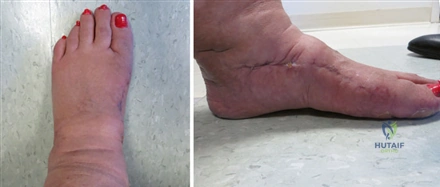
Upon radiographic confirmation of bridging trabecular bone, patients are weaned from the CAM boot into a stiff-soled athletic shoe with a wide toe box. Physical therapy is formally initiated, focusing on intrinsic foot muscle strengthening, restoration of the windlass mechanism, and proprioceptive training. Aggressive MTP joint mobilization is continued. Patients are counseled that mild to moderate swelling is expected and may persist for up to 6 months post-operatively.
Phase 4: Return to High-Level Activity (Weeks 12+)
By 12 weeks, the osteotomy or fusion site should be solidly united. Patients are cleared for high-impact activities, running, and jumping, provided they have regained adequate strength and have no pain with provocative testing. Shoe wear restrictions are gradually lifted, though patients are continually advised against the chronic use of narrow, high-heeled footwear to prevent late recurrence of angular deformities.
Summary of Landmark Literature and Clinical Guidelines
The evolution of first metatarsal surgery is deeply rooted in decades of rigorous clinical research and biomechanical studies. The American Orthopaedic Foot & Ankle Society (AOFAS) frequently updates clinical practice guidelines based on the latest evidence-based medicine.
The seminal work by Mann and Coughlin in the late 20th century established the foundational understanding of the pathophysiology of hallux valgus and the critical importance of the intermetatarsal angle in dictating surgical decision-making. Their long-term follow-up studies on the Chevron osteotomy validated its efficacy for mild to moderate deformities, demonstrating high patient satisfaction and low recurrence rates when indications were strictly adhered to.
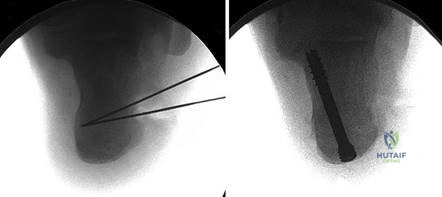
Regarding the Lapidus procedure, Myerson's extensive publications revolutionized the approach to the hypermobile first ray. His studies highlighted that failure to address the apex of the deformity at the TMT joint in severe cases inevitably leads to recurrence. More recently, Coetzee et al. published landmark papers evaluating the biomechanical superiority of multiplanar correction and modern locking plate technology in Lapidus arthrodesis, significantly reducing the historical nonunion rates and allowing for accelerated rehabilitation protocols.
For hallux rigidus, Coughlin and Shurnas developed the definitive clinical and radiographic grading system that remains the international standard for guiding treatment. Their research definitively proved that while cheilectomy provides excellent relief for Grades 1 and 2, first MTP arthrodesis is the only reliable, long-term solution for Grade 3 and 4 disease. These landmark studies form the bedrock of modern foot and ankle surgical training, ensuring that orthopedic surgeons approach first metatarsal pathology with a nuanced, evidence-based perspective.
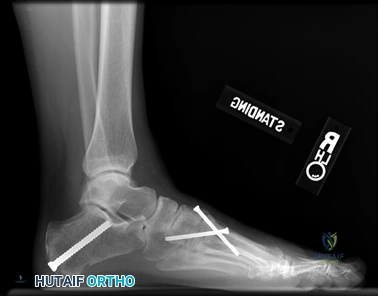
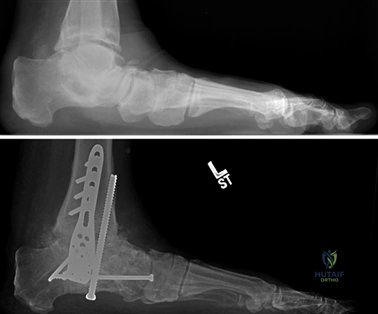
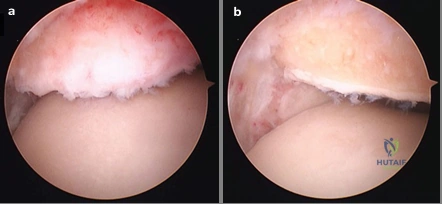
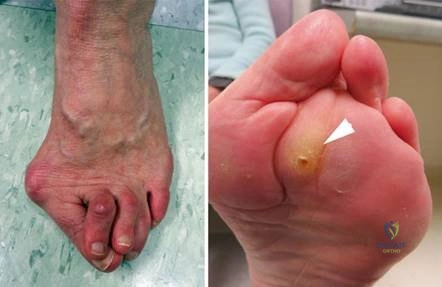
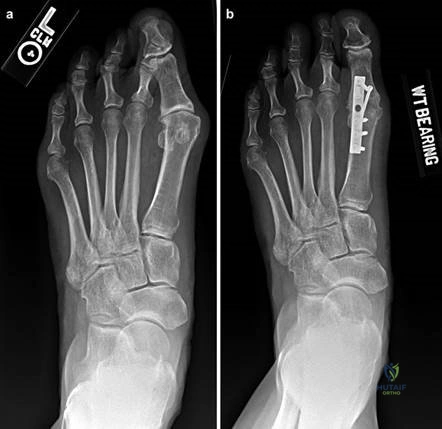
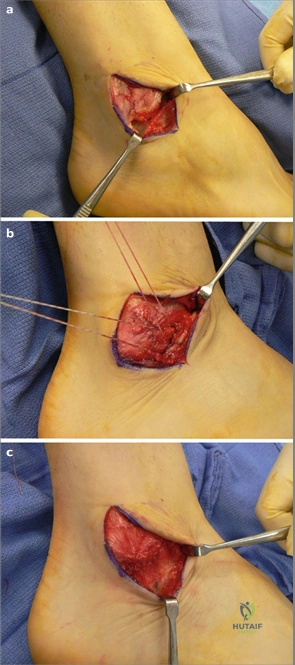
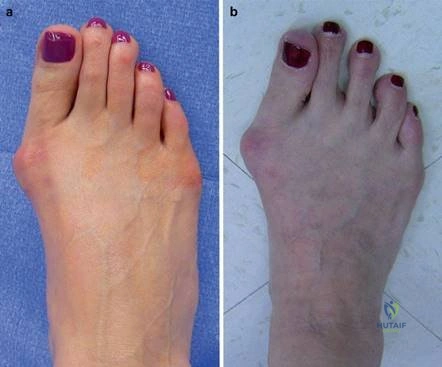
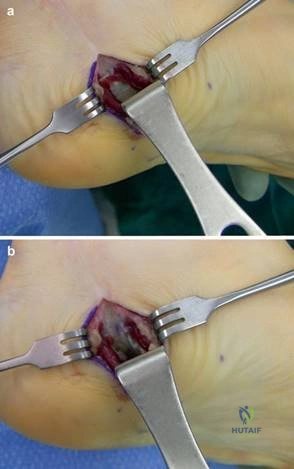
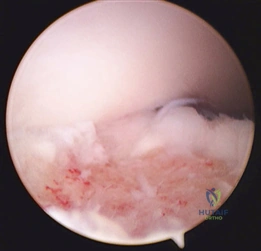
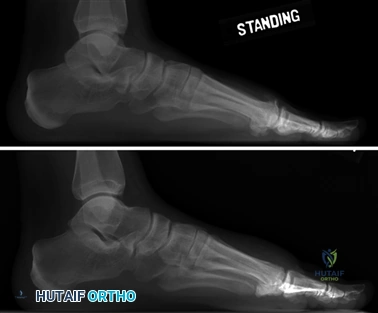
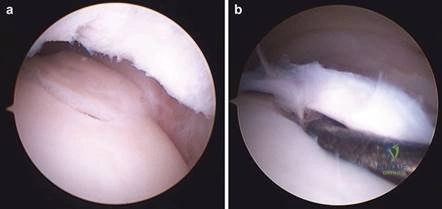
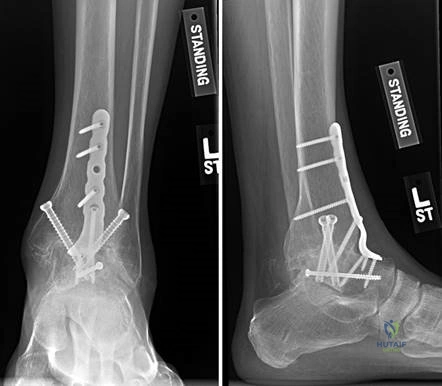
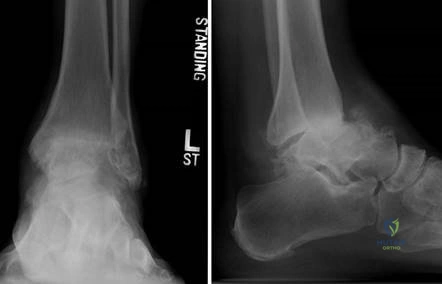
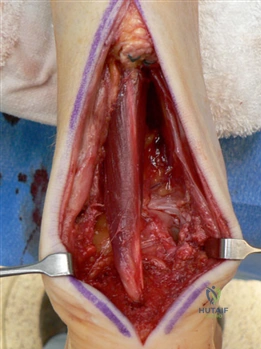
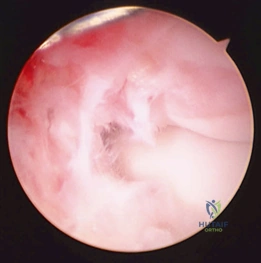
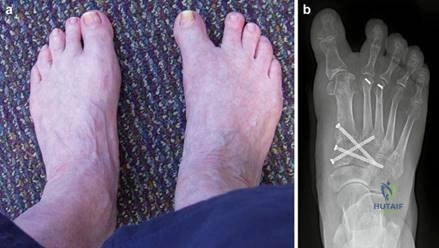
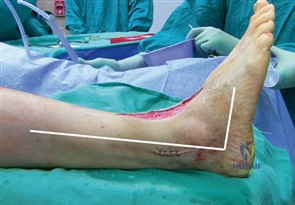
Clinical & Radiographic Imaging Archive