Pediatric Orthopaedics: Comprehensive MCQ Question Bank & Exam Prep
Comprehensive 100-Question Exam
00:00
Start Quiz
Question 1
A 13-year-old obese male presents with left groin and knee pain that has been worsening over 6 months. Radiographs reveal a severe chronic Slipped Capital Femoral Epiphysis (SCFE). He undergoes in situ percutaneous pinning. What is the most significant recognized mechanical risk factor for developing chondrolysis in this patient?
Explanation
Question 2
A 4-week-old infant with idiopathic clubfoot is being treated with the Ponseti method. After 5 weeks of serial casting, the cavus, adductus, and varus deformities have completely resolved. However, passive ankle dorsiflexion is only 5 degrees. What is the next most appropriate step in management?
Explanation
Question 3
A 7-year-old child with spastic quadriplegic cerebral palsy (GMFCS Level V) is evaluated for hip pain and difficulty with perineal hygiene. An AP pelvis radiograph demonstrates a Reimers' migration index of 65% bilaterally. What is the most appropriate surgical intervention to stabilize the hips?
Explanation
Question 4
A 6-week-old female infant, born in a breech presentation, is evaluated for Developmental Dysplasia of the Hip (DDH). A coronal ultrasound of the hip is performed. The alpha angle is measured at 40 degrees and the beta angle at 80 degrees. According to the Graf classification, what is the diagnosis and the most appropriate management?
Explanation
Question 5
A 13-year-old male presents with rigid, painful flat feet and recurrent ankle sprains. On examination, he demonstrates restricted subtalar motion and peroneal spasticity. Radiographs demonstrate an 'anteater nose' sign. Which of the following is the most likely diagnosis?
Explanation
Question 6
A 6-year-old child sustains a widely displaced, extension-type supracondylar humerus fracture. On presentation to the emergency department, the hand is pink, warm, and has a brisk capillary refill, but the radial pulse is entirely non-palpable. What is the most appropriate initial step in the management of this patient?
Explanation
Question 7
An 8-year-old boy is diagnosed with Legg-Calvé-Perthes disease. During the fragmentation stage, the treating orthopaedist assesses the radiographs for 'head-at-risk' signs described by Catterall. Which of the following is considered a Catterall 'head-at-risk' sign?
Explanation
Question 8
A 4-year-old child with achondroplasia presents with progressive weakness in all four extremities, new-onset hyperreflexia, and frequent episodes of central sleep apnea. What is the most appropriate imaging study to evaluate the underlying cause of these symptoms?
Explanation

Question 9
A 3-year-old obese female presents with bilateral bowing of the legs. Standing AP radiographs show a sharp varus angulation at the proximal tibial metaphyses. The metaphyseal-diaphyseal angle (Drennan's angle) is measured at 18 degrees bilaterally. What is the most appropriate management?
Explanation
Question 10
A 5-year-old child is evaluated for a painless waddling gait. AP pelvis radiographs reveal a decreased neck-shaft angle and a Hilgenreiner Epiphyseal Angle (HEA) of 65 degrees. A triangular fragment of bone is visible in the inferior aspect of the femoral neck. What is the recommended treatment for this condition?
Explanation
Question 11
A 6-year-old girl complains of a painful, audible 'popping' sensation in her lateral knee when walking. MRI confirms the presence of a discoid lateral meniscus. Which specific variant of a discoid meniscus lacks normal posterior coronary ligament attachments, directly causing this 'snapping knee' syndrome?
Explanation
Question 12
A newborn infant presents with severe radial deviation of both wrists. Radiographs confirm bilateral absent radii. Physical examination reveals that the thumbs are present bilaterally. Laboratory evaluation shows a profoundly low platelet count. Which of the following is the most likely diagnosis?
Explanation
Question 13
A 14-year-old boy sustains an ankle injury. Radiographs show a Salter-Harris III fracture of the anterolateral aspect of the distal tibial epiphysis. This fracture pattern (juvenile Tillaux fracture) is caused by an avulsion force from which of the following ligaments?
Explanation
Question 14
A 10-year-old boy falls off his bicycle and presents with knee hemarthrosis. Radiographs reveal a Meyers and McKeever Type II fracture of the tibial eminence. Which of the following best describes the anatomical displacement in this fracture pattern?
Explanation
Question 15
A 12-year-old competitive gymnast presents with severe low back pain and radicular pain radiating down her posterior left leg. Lateral radiographs demonstrate a Meyerding Grade IV isthmic spondylolisthesis at L5-S1 with a slip angle of 55 degrees. What is the most appropriate surgical treatment?
Explanation
Question 16
A 10-year-old boy with known mutations in the EXT1 gene is followed for multiple bone lesions. He presents with a rapidly enlarging, painful mass on his proximal tibia. He is at highest risk for developing which of the following malignancies?
Explanation
Question 17
A 4-year-old boy presents with a 2-day history of right hip pain and a limp, now refusing to bear weight completely. His temperature is 38.6°C (101.5°F), WBC count is 14,500/mm³, ESR is 45 mm/hr, and CRP is elevated. According to the Kocher criteria, what is the approximate predictive probability of septic arthritis in this patient?
Explanation
Question 18
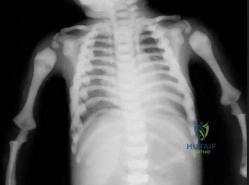
A 6-month-old infant presents with multiple fractures of varying ages, blue sclerae, and generalized osteopenia. Genetic testing reveals a mutation in the COL1A1 gene. Which of the following is the primary mechanism of action of the most commonly prescribed class of medications (bisphosphonates) used to treat this condition?
Explanation
Question 19
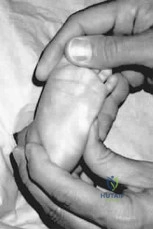
A 2-year-old child presents with an anterolateral bowing deformity of the left tibia. Radiographs demonstrate a diaphyseal fracture with sclerotic, tapered ends that has failed to heal. This condition, congenital pseudarthrosis of the tibia (CPT), is most highly associated with which of the following systemic disorders?
Explanation
Question 20
A 12-year-old male presents with acute severe groin pain after jumping off a swing. He is completely unable to bear weight, even with crutch assistance. Radiographs demonstrate a Slipped Capital Femoral Epiphysis (SCFE). What is the approximate risk of avascular necrosis (AVN) in this type of SCFE compared to a 'stable' slip?
Explanation
Question 21
What radiographic parameter is considered the most reliable and predictive marker for the risk of hip dislocation in a non-ambulatory child with Cerebral Palsy (GMFCS Level IV or V)?
Explanation
Question 22
An 18-month-old female presents with an untreated, late-diagnosed Developmental Dysplasia of the Hip (DDH). Open reduction and a pelvic osteotomy are planned to improve anterolateral acetabular coverage. Which of the following pelvic osteotomies utilizes the pubic symphysis as its primary hinge?
Explanation
Question 23
A 7-year-old boy is diagnosed with Legg-Calvé-Perthes disease. According to the Herring Lateral Pillar Classification, which of the following findings places him in Group C and predicts the poorest clinical outcome?
Explanation
Question 24
Which of the following patients presenting with a unilateral Slipped Capital Femoral Epiphysis (SCFE) has the strongest absolute indication for prophylactic in situ pinning of the contralateral hip?
Explanation
Question 25
A 2-year-old girl presents with progressive bowing of her left leg. Standing full-length radiographs demonstrate a marked varus deformity isolated to the proximal tibia. Which of the following radiographic parameters is most strongly predictive of progression to true infantile Blount's disease rather than physiological bowing?
Explanation
Question 26
A 4-month-old infant with molecularly confirmed achondroplasia is being evaluated. What is the most common cause of sudden, unexpected infant death in patients with this skeletal dysplasia?
Explanation
Question 27
In the evaluation of pediatric developmental (isthmic) spondylolisthesis at L5-S1, which of the following spinopelvic parameters is most strongly associated with an increased risk of severe slip progression?
Explanation
Question 28
A 2.5-year-old boy treated successfully in infancy for a right idiopathic clubfoot using the Ponseti method returns to the clinic. His parents report worsening of his foot shape over the last 3 months, and admit to discontinuing the foot abduction orthosis. Examination reveals dynamic supination and recurrent equinus. What is the most appropriate initial management?
Explanation
Question 29
A 12-year-old boy complains of recurrent left lateral ankle sprains and a painful, rigid flatfoot. Physical examination reveals spasm of the peroneal tendons. Which radiographic view is best to properly identify a calcaneonavicular coalition (the 'anteater nose' sign)?
Explanation
Question 30
A 2-year-old girl is brought in for a locked interphalangeal joint of her right thumb. Her mother reports a small nodule at the base of the thumb on the volar surface. Active extension is absent, but passive extension is painful and yields a palpable click. What is the most appropriate initial management?
Explanation
Question 31
A 6-year-old boy sustains a severe Gartland Type III supracondylar humerus fracture. Upon arrival, his hand is pale and pulseless. After closed reduction and percutaneous pinning, the radial pulse remains unpalpable, but the hand becomes pink, warm, and has a capillary refill of less than 2 seconds. What is the next best step in management?
Explanation
Question 32
A 4-year-old child with Osteogenesis Imperfecta (OI) type III is treated with intravenous pamidronate. What is the primary cellular mechanism of action by which this medication improves bone density and reduces fracture burden in this patient population?
Explanation
Question 33
A 14-year-old boy presents with progressive mid-back pain. Lateral radiographs of his thoracic spine reveal rigid hyperkyphosis. According to the Sorensen criteria for classical Scheuermann's disease, what is the required radiographic threshold regarding vertebral body wedging?
Explanation
Question 34
Congenital Pseudarthrosis of the Tibia (CPT) is a notoriously difficult condition to treat and is characterized by bowing and spontaneous fractures that fail to heal. The condition has the strongest genetic and clinical association with a mutation on which chromosome?
Explanation
Question 35
A 6-year-old girl complains of a painful 'clunk' and a snapping sensation on the lateral aspect of her right knee when moving from flexion to extension. MRI confirms a Watanabe Type III (Wrisberg variant) discoid lateral meniscus. What specific anatomical deficiency characterizes this specific variant?
Explanation
Question 36
Pediatric hip fractures are rare and associated with a high rate of complications. According to the Delbet classification, which fracture type is associated with the highest rate of avascular necrosis (AVN) of the femoral head?
Explanation
Question 37
Proximal Focal Femoral Deficiency (PFFD), also known as Congenital Femoral Deficiency, presents with marked limb length discrepancy, external rotation, and flexion at the hip. It is most commonly associated with which of the following intra-articular knee anomalies?
Explanation
Question 38
A 7-year-old girl presents with severe torticollis, neck pain, and a 'cock-robin' head position three weeks after undergoing a tonsillectomy. Radiographs show an increased atlantodens interval. In the pathogenesis of Grisel's syndrome, what is the primary mechanism leading to this atlantoaxial subluxation?
Explanation
Question 39
A 12-year-old boy with Duchenne Muscular Dystrophy (DMD) has lost independent ambulation and presents with a progressive neuromuscular scoliosis of 28 degrees. When counseling the family regarding posterior spinal fusion to the pelvis, what are the standard criteria for proceeding with surgery to optimize outcomes and minimize prohibitive respiratory complications?
Explanation
Question 40
Madelung deformity is a congenital wrist deformity characterized by premature closure of the volar-ulnar aspect of the distal radial physis. It frequently presents bilaterally in adolescent females. This specific deformity is the hallmark skeletal manifestation of Léri-Weill dyschondrosteosis, which is caused by a mutation in which gene?
Explanation
Question 41
A 6-week-old female is treated with a Pavlik harness for an ultrasonographically confirmed irreducible right hip dislocation. At the 2-week follow-up, the parents report the infant is no longer kicking her right leg. Examination reveals absent active knee extension on the right, but active ankle dorsiflexion and plantarflexion are preserved. Ultrasound confirms the hip remains dislocated. What is the most appropriate next step in management?
Explanation
Question 42
An 8.5-year-old boy presents with a 4-month history of a painless limp. Radiographs demonstrate fragmentation of the capital femoral epiphysis with >50% maintenance of the lateral pillar height. He has 15 degrees of abduction and a 10-degree flexion contracture. Based on his age and radiographic classification, which treatment provides the best long-term radiographic outcome?
Explanation
Question 43
A 6-year-old boy sustains a Gartland type III extension supracondylar humerus fracture. On presentation, his hand is pink and warm, but the radial pulse is non-palpable. Urgent closed reduction and percutaneous pinning are performed. Postoperatively, the fracture is anatomically aligned on fluoroscopy, but the radial pulse remains absent. Capillary refill is 2 seconds and the hand remains warm. What is the most appropriate management?
Explanation
Question 44
A newborn male presents with bilateral radial longitudinal deficiency (absent radii and absent thumbs). A chromosomal breakage test using diepoxybutane is positive. If left untreated, what is the most common cause of mortality associated with this patient's underlying diagnosis?
Explanation
Question 45
A 14-year-old boy presents with chronic, insidious-onset left hindfoot pain and recurrent ankle sprains. Examination shows a rigid, flat foot with severely restricted subtalar motion and peroneal spasticity. A lateral radiograph of the foot demonstrates the 'anteater nose' sign. Which anatomical structures are abnormally connected?
Explanation
Question 46
A 2-year-old boy presents with a completely displaced, atraumatic fracture of the middle/distal third of the tibia. Radiographs show dysplastic, tapered bone ends at the fracture site. He has 7 café-au-lait spots measuring >5mm. Which of the following is the most important surgical principle in achieving primary osseous union for this condition?
Explanation
Question 47
A 14-year-old female gymnast presents with severe lower back pain radiating down the posterior aspect of both thighs. Radiographs demonstrate a Grade III L5-S1 isthmic spondylolisthesis. Her pelvic incidence is 75 degrees and her slip angle is 50 degrees. She has failed 6 months of conservative management. What is the most appropriate surgical treatment?
Explanation
Question 48
A 5-year-old child with a history of multiple low-energy fractures, easy bruising, and blue sclerae is diagnosed with Osteogenesis Imperfecta type I. Genetic testing is most likely to reveal a defect in the synthesis or structure of which of the following?
Explanation
Question 49
A 9-year-old male presents with bilateral knee pain and a waddling gait. He is in the 10th percentile for weight and 5th percentile for height. Radiographs reveal bilateral slipped capital femoral epiphyses (SCFE). Given the patient's age and bilateral presentation, an endocrine workup is initiated. Which of the following conditions is most commonly associated with this presentation?
Explanation
Question 50
A 9-year-old boy (Tanner stage I) sustains a complete mid-substance tear of the anterior cruciate ligament (ACL) while playing soccer. He has recurrent episodes of instability despite extensive physical therapy and bracing. To minimize the risk of growth arrest and severe angular deformity, which of the following ACL reconstruction techniques is most appropriate for this patient?
Explanation
Question 51
A 12-year-old girl with primary hypothyroidism presents with a stable left Slipped Capital Femoral Epiphysis (SCFE) and undergoes in situ pinning. Her right hip is currently asymptomatic and radiographically normal. What is the most appropriate management regarding her contralateral right hip?
Explanation
Question 52
A 3-month-old infant is being treated with a Pavlik harness for developmental dysplasia of the hip (DDH). At the 2-week follow-up, the mother reports the infant is not kicking the left leg as much. On examination, the infant exhibits absent active knee extension on the left. What is the most appropriate next step in management?
Explanation
Question 53
An 8-year-old boy is diagnosed with Legg-Calvé-Perthes disease. Radiographs demonstrate exactly 50% loss of lateral pillar height. According to the Herring lateral pillar classification and patient age, which treatment has been shown to provide the best long-term radiographic outcome (Stulberg I or II)?
Explanation
Question 54
A 6-year-old girl sustains an extension-type Gartland III supracondylar humerus fracture. Examination reveals an inability to actively flex the interphalangeal joint of the thumb and the distal interphalangeal joint of the index finger. Which nerve is most likely injured?
Explanation
Question 55
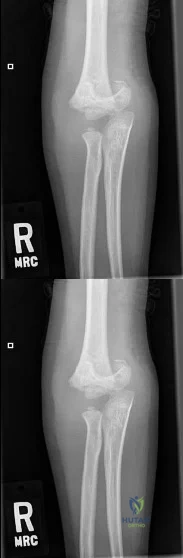
A 14-year-old boy presents with an ankle injury after an external rotation force.
Radiographs demonstrate a Salter-Harris III fracture of the anterolateral distal tibia (Tillaux fracture). Which of the following describes the normal sequence of distal tibial physeal closure that explains this fracture pattern?
Explanation
Question 56
A 6-month-old infant is noted to have a left thoracic curve of 25 degrees on a supine radiograph. The rib-vertebral angle difference (RVAD) of Mehta is measured at 28 degrees. What is the most likely clinical course and appropriate management?
Explanation
Question 57
A 2-year-old boy with neurofibromatosis type 1 (NF1) presents with pronounced anterolateral bowing of the left tibia and a frank pseudarthrosis on radiographs. What is the most definitive surgical management strategy to achieve long-term union?
Explanation
Question 58
A 4-year-old child with achondroplasia presents to the clinic with progressive weakness in the lower extremities, hyperreflexia, and new-onset central sleep apnea. What is the most critical anatomical region to evaluate urgently with an MRI?
Explanation
Question 59
A 4-year-old boy, previously treated successfully with the Ponseti method for idiopathic clubfoot, presents with dynamic supination of the foot during the swing phase of gait. Passive range of motion of the ankle and subtalar joints is normal. What is the most appropriate surgical treatment?
Explanation
Question 60
A 12-year-old boy complains of recurrent ankle sprains and rigid, painful flatfeet. A lateral radiograph demonstrates an elongated lateral process of the talus projecting toward the navicular. What is the most likely diagnosis?
Explanation
Question 61
A 5-year-old boy with Sillence Type III osteogenesis imperfecta sustains a recurrent mid-diaphyseal femur fracture. His previous fracture was treated non-operatively and healed with significant anterolateral bowing. What is the optimal surgical management for his current fracture to prevent future deformities?
Explanation
Question 62
What is the primary cause of cubitus varus deformity following closed reduction and percutaneous pinning of a Gartland type III supracondylar humerus fracture?
Explanation
Question 63
A 4-year-old child with developmental dysplasia of the hip (DDH) is scheduled for an innominate osteotomy. Which of the following osteotomies hinges at the pubic symphysis to redirect the entire acetabulum, requiring a complete cut through the ilium from the sciatic notch to the anterior inferior iliac spine?
Explanation
Question 64
A 6-week-old female is treated with a Pavlik harness for developmental dysplasia of the hip (DDH). At the 3-week follow-up, she exhibits decreased active extension of the knee on the affected side but cries when the leg is manipulated. What is the most likely cause of this clinical finding?
Explanation
Question 65
A 6-year-old boy presents with a displaced Gartland type III supracondylar humerus fracture. After closed reduction and percutaneous pinning, the hand is pink, warm, and has a capillary refill of 2 seconds, but the radial pulse remains absent on Doppler ultrasound. What is the most appropriate next step in management?
Explanation
Question 66
An 8-year-old boy presents with a progressive limp and hip pain. Radiographs demonstrate sclerosis and fragmentation of the proximal femoral epiphysis consistent with Legg-Calve-Perthes disease. Which of the following radiographic findings in the lateral pillar classification is most predictive of a poor long-term outcome?
Explanation
Question 67
An 11-year-old girl with end-stage renal disease and renal osteodystrophy undergoes in situ percutaneous pinning for a left slipped capital femoral epiphysis (SCFE). Her right hip is completely asymptomatic and radiographically normal. What is the most appropriate management for the right hip?
Explanation
Question 68
A 9-year-old boy weighing 55 kg (121 lbs) sustains a midshaft femoral fracture. The surgeon considers intramedullary fixation using titanium elastic nails (TENs). Which complication is most highly associated with this choice of implant in this specific patient compared to alternative fixation methods?
Explanation
Question 69
A 14-year-old boy presents with rigid flat feet and recurrent ankle sprains. Examination shows restricted subtalar motion and peroneal spasticity. A CT scan confirms a talocalcaneal coalition. Which non-operative management is typically considered the most effective initial step?
Explanation
Question 70
A newborn is evaluated for a congenital right lower extremity deformity. Clinical examination reveals an anteromedial tibial bow, a deep skin dimple over the anterior tibia, an absent lateral ray of the foot, and significant limb length discrepancy. What is the most likely diagnosis?
Explanation
Question 71
A 3-year-old child presents with progressive bilateral genu varum. Radiographs demonstrate a prominent medial metaphyseal beak of the proximal tibia with a metaphyseal-diaphyseal angle (Drennan's angle) of 20 degrees. What is the most appropriate initial management?
Explanation
Question 72
A 14-year-old girl sustains an ankle injury while playing soccer. Radiographs reveal a Salter-Harris III fracture of the anterolateral distal tibial epiphysis. What is the primary mechanism causing this specific fracture pattern?
Explanation
Question 73
A 2-month-old infant boy presents with his head tilted to the right and chin rotated to the left. A firm, painless, non-pulsatile mass is palpable in the right side of the neck. Ultrasound confirms a fibrotic mass within the sternocleidomastoid muscle. What is the most common associated musculoskeletal condition that must be screened for in this patient?
Explanation
None
Detailed Chapters & Topics
Dive deeper into specialized chapters regarding pediatric-orthopaedic-mcqs-online-bank-1
