Orthopedic Pediatric Review | Dr Hutaif Pediatric Ortho -...
Key Takeaway
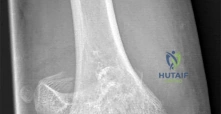
Your ultimate guide to ORTHOPEDIC MCQS ONLINE PEDIATRIC 016 starts here. A headneck junction offset refers to any deviation from optimal anatomical alignment at the craniocervical junction, where the skull meets the upper spine. In pediatric orthopaedics, understanding this offset is vital for assessing structural integrity, potential neurological implications, and risk factors for conditions or injuries, including those related to trauma and athletic activity.
Orthopedic Pediatric Review | Dr Hutaif Pediatric Ortho -...
Comprehensive 100-Question Exam
00:00
Start Quiz
Question 1
A 6-week-old female is being treated with a Pavlik harness for Developmental Dysplasia of the Hip (DDH).
At her 2-week follow-up, the parents report she is not kicking her left leg as much. On examination, she has decreased active extension of the left knee, though passive range of motion is normal. What is the most likely cause of this finding?
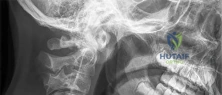
Explanation
Question 2
A 13-year-old obese male with a stable left Slipped Capital Femoral Epiphysis (SCFE) undergoes in situ pinning with a single cannulated screw.
Six months postoperatively, he develops severe, constant hip pain and a significantly restricted range of motion in all planes. Radiographs demonstrate concentric joint space narrowing without hardware failure. What is the most likely diagnosis?
Explanation
Question 3
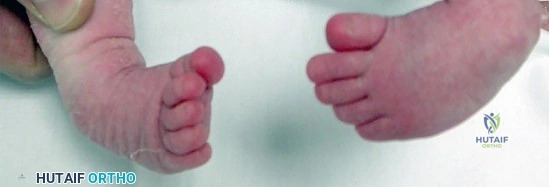
An infant with idiopathic clubfoot is being treated with the Ponseti method of serial casting.
The forefoot has been successfully abducted to 60 degrees, and the heel is in valgus. However, the foot remains in 20 degrees of equinus. What is the most appropriate next step in management?

Explanation
Question 4
A 5-year-old boy presents with an extension-type Gartland III supracondylar humerus fracture after a fall.
On examination, his hand is well-perfused (pink) with brisk capillary refill, but the radial pulse is absent. What is the most appropriate initial management?
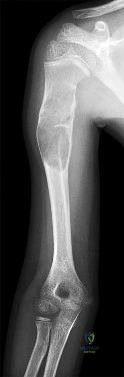
Explanation
Question 5
A 4-year-old child sustains a mildly displaced (<2mm) lateral condyle fracture of the humerus, which is treated non-operatively in a long arm cast. Three months later, radiographs reveal a frank nonunion of the lateral condyle. If left untreated, what late neurological complication is most characteristic of this condition?
Explanation
Question 6
A 7-year-old boy is diagnosed with Legg-Calvé-Perthes disease. Anteroposterior radiographs of the pelvis demonstrate that exactly 50% of the lateral pillar height is maintained on the affected side. According to the Herring lateral pillar classification, into which group does this patient fall?
Explanation
Question 7
A 4-year-old boy presents to the emergency department with acute right hip pain, a severe limp, and a refusal to bear weight. His temperature is 38.6°C. Laboratory workup reveals a WBC count of 13,500/mm³ and an ESR of 45 mm/hr. According to the Kocher criteria, what is the approximate statistical probability that this child has septic arthritis of the hip?
Explanation
Question 8
A newborn is diagnosed with congenital scoliosis secondary to a fully segmented hemivertebra at T8.
Which of the following is the most appropriate routine screening protocol to order next to evaluate for frequently associated anomalies?
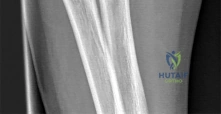
Explanation
Question 9
In a 6-year-old child with spastic quadriplegic cerebral palsy (GMFCS Level V), routine hip surveillance is indicated. What is the most important, standardized radiographic parameter used to monitor the progression of hip displacement in this population?
Explanation
Question 10
A 3-year-old girl, who is at the 95th percentile for weight and began walking at 9 months of age, presents with progressive bilateral genu varum.
Radiographs reveal an abrupt medial beaking of the proximal tibial metaphysis and a metaphyseal-diaphyseal angle (Drennan's angle) of 18 degrees. What is the most likely diagnosis?
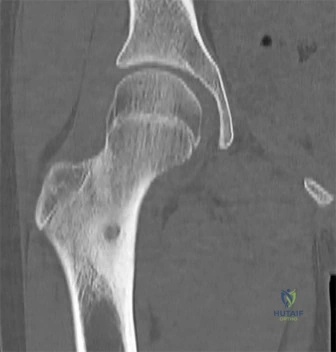
Explanation
Question 11
A 5-year-old boy with blue sclerae, multiple previous fractures, and mild short stature is diagnosed with Osteogenesis Imperfecta Type I. Which of the following gene mutations is most commonly responsible for this condition?
Explanation
Question 12
A 3-year-old boy presents with progressive bowing of the lower extremities, short stature, and a waddling gait. Laboratory studies reveal a normal serum calcium, profoundly low serum phosphate, elevated alkaline phosphatase, and normal parathyroid hormone levels. What is the primary pathophysiology underlying his condition?
Explanation
Question 13
A 13-year-old girl sustains an ankle injury during a soccer match. Radiographs reveal an isolated Salter-Harris III fracture of the anterolateral distal tibial epiphysis (Tillaux fracture). Which of the following describes the anatomical sequence of distal tibial physeal closure that predisposes adolescents to this specific fracture pattern?
Explanation
Question 14
A 14-year-old boy complains of a painful, rigid flatfoot and a history of recurrent ankle sprains. Physical examination demonstrates severe restriction of subtalar motion and peroneal spasticity. A 45-degree internal oblique radiograph of the foot reveals an 'anteater nose' sign. Which of the following is the most likely diagnosis?
Explanation
Question 15
A 12-year-old elite Little League pitcher complains of progressively worsening pain in his throwing shoulder during the late cocking phase. Radiographs show widening and sclerosis of the proximal humeral physis. What is the primary pathophysiology of this condition (Little League Shoulder)?
Explanation
Question 16
An 8-year-old Japanese girl presents with a painless, palpable 'clunk' on the lateral side of her left knee during terminal extension. MRI confirms a discoid lateral meniscus. Which specific variant of a discoid meniscus is characterized by an absent posterior meniscotibial attachment, leading to hypermobility and snapping?
Explanation
Question 17
A 3-year-old boy sustains a closed, isolated, midshaft femur fracture after a fall from a playground structure.
Radiographs show 1.5 cm of overriding. What is the most widely accepted definitive management for this patient?
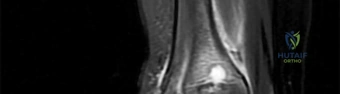
Explanation
Question 18
A 15-year-old female gymnast presents with persistent lower back pain. Lateral radiographs of the lumbar spine reveal a pars interarticularis defect at L5 and a forward translation of L5 on S1. The superior endplate of S1 is divided into four equal parts, and the posterior cortex of L5 sits over the second quartile. According to the Meyerding classification, what is the grade of this spondylolisthesis?
Explanation
Question 19
A 7-year-old boy undergoes closed reduction and percutaneous pinning of a displaced supracondylar humerus fracture.
Six hours postoperatively, he is crying uncontrollably on the ward and requires escalating doses of IV opioids. Which of the following is the most reliable early clinical indicator of compartment syndrome in this pediatric patient?
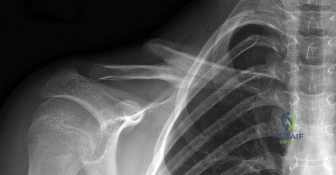
Explanation
Question 20
An 8-month-old infant with homozygous achondroplasia presents with witnessed episodes of central sleep apnea, hyperreflexia, and generalized hypotonia. What is the most likely anatomic cause of these severe neurological symptoms?
Explanation
Question 21
A 12-year-old obese male presents with severe left hip pain and is completely unable to bear weight, even with the assistance of crutches. Radiographs confirm a severe left Slipped Capital Femoral Epiphysis (SCFE). Which of the following best describes his classification and the associated risk of the most catastrophic complication?
Explanation
Question 22
An 18-month-old female with late-presenting Developmental Dysplasia of the Hip (DDH) undergoes closed reduction and spica casting in the operating room. To minimize the risk of iatrogenic avascular necrosis (AVN) of the femoral head, which of the following extreme positions must be strictly avoided during casting?
Explanation
Question 23
A 9-year-old boy is diagnosed with Legg-Calvé-Perthes disease. Radiographs demonstrate that less than 50% of the lateral pillar height is maintained. Based on the Herring Lateral Pillar Classification, which of the following is true regarding his prognosis and management?
Explanation
Question 24
A 4-year-old boy previously treated for idiopathic clubfoot with the Ponseti method presents with a relapsed deformity. Gait analysis reveals dynamic supination of the foot during the swing phase. Passive range of motion demonstrates a fully correctable deformity. What is the most appropriate definitive management?
Explanation
Question 25
A 3-year-old female presents with progressive unilateral genu varum. Standing lower extremity radiographs are obtained. Measurement of the metaphyseal-diaphyseal angle (Drennan's angle) is most predictive of progression to infantile Blount's disease when it exceeds what threshold?
Explanation
Question 26
A 6-year-old boy sustains a completely displaced, extension-type supracondylar humerus fracture (Gartland Type III). Upon presentation, his hand is pale and pulseless. Following closed reduction and percutaneous pinning in the operating room, the hand becomes warm and pink with a capillary refill of 2 seconds, but the radial pulse remains unpalpable. What is the most appropriate next step in management?
Explanation
Question 27
A 7-year-old non-ambulatory child with spastic quadriplegic cerebral palsy presents for a routine evaluation. Pelvic radiographs demonstrate a Reimers Migration Percentage of 45% bilaterally. He is currently painless. What is the most appropriate treatment recommendation?
Explanation
Question 28
A newborn is evaluated for congenital scoliosis. Which of the following radiographic vertebral anomalies carries the highest risk for rapid, unrelenting curve progression and typically requires early in situ spinal fusion?
Explanation
Question 29
A 3-year-old presents with a 2-day history of right hip pain, refusal to bear weight, and a temperature of 38.8°C. According to the updated Kocher criteria by Caird et al., which laboratory value was added as a strong independent predictor for septic arthritis of the hip?
Explanation
Question 30
A 13-year-old male presents with recurrent ankle sprains and a rigid, painful flatfoot. Radiographs show an elongated anterior process of the calcaneus resembling an "anteater's nose" on the lateral view. What is the most likely diagnosis?
Explanation
Question 31
A 5-year-old boy with Osteogenesis Imperfecta (Type III) is being treated with intravenous bisphosphonates. By what specific mechanism do bisphosphonates decrease the fracture rate in these patients?
Explanation
Question 32
An 8-year-old, 35 kg boy sustains a transverse midshaft fracture of the right femur. He is treated with titanium elastic nails (TENs). What is the most common complication associated with this surgical treatment?
Explanation
Question 33
A 13-year-old female sustains a fracture of the anterolateral aspect of her distal tibial epiphysis after an external rotation injury. This fracture pattern (Tillaux fracture) occurs specifically due to the asymmetrical closure of the distal tibial physis. In what sequence does the normal distal tibial physis close?
Explanation
Question 34
An 8-year-old girl presents with a painless "clunking" in her lateral knee during flexion and extension. MRI demonstrates a Wrisberg-variant discoid lateral meniscus. What anatomical structure is characteristically absent in this variant?
Explanation
Question 35
A 4-year-old boy presents with profound bilateral genu varum, frontal bossing, and short stature. Laboratory evaluation reveals a normal serum calcium, significantly decreased serum phosphate, elevated alkaline phosphatase, and normal parathyroid hormone levels. A mutation in the PHEX gene is confirmed. What is the primary pathophysiologic defect in this disorder?
Explanation
Question 36
A 5-year-old child sustains a minimally displaced (<2 mm) lateral condyle fracture of the humerus. If left completely untreated and progressing to a nonunion, what is the most likely long-term complication?
Explanation
Question 37
An 18-month-old male is evaluated for congenital pseudarthrosis of the tibia (CPT). Examination reveals anterolateral bowing of the affected leg. Which genetic condition is most strongly associated with this finding?
Explanation
Question 38
A 9-year-old male presents with acute shoulder pain after throwing a baseball. Radiographs reveal a pathologic fracture through a centrally located, lytic, expansile bone lesion in the proximal humeral metaphysis. A "fallen leaf" sign is noted. What is the most appropriate initial management?
Explanation
Question 39
A newborn is diagnosed with achondroplasia. Which zone of the epiphyseal physis (growth plate) is primarily affected by the genetic mutation underlying this condition?
Explanation
Question 40
A 9-year-old boy presents with a limp and groin pain. Radiographs demonstrate Legg-Calvé-Perthes disease classified as Lateral Pillar B. He has maintained good range of motion. What is the most appropriate surgical treatment to prevent femoral head deformation in this patient?
Explanation
Question 41
A 6-year-old boy falls from monkey bars and sustains a widely displaced posterolateral Gartland type III supracondylar humerus fracture. Which of the following neurologic deficits is most likely to be observed on physical examination?
Explanation
Question 42
A 4-year-old girl is evaluated for severe bowing of her left leg. Radiographs reveal a prominent physeal step-off with depression of the medial tibial plateau, consistent with Langenskiöld stage IV infantile Blount's disease. What is the most appropriate management?
Explanation
Question 43
A 5-year-old boy presents with a 2-day history of right hip pain and inability to bear weight. His temperature is 38.8°C (101.8°F), WBC count is 14,000/mm3, ESR is 55 mm/hr, and CRP is 3.5 mg/dL. Radiographs of the hip are normal. What is the most appropriate next step in management?
Explanation
Question 44
A 12-year-old boy with a BMI in the 99th percentile presents with left knee pain and an inability to bear weight on his left leg. Radiographs confirm a severe Slipped Capital Femoral Epiphysis (SCFE). Which of the following factors is the greatest predictor for the development of avascular necrosis (AVN) in this patient?
Explanation
Question 45
A 6-week-old female undergoes a screening hip ultrasound for breech presentation. The alpha angle is 45 degrees, and the beta angle is 80 degrees. According to the Graf classification, what is the most appropriate initial management?
Explanation
Question 46
A 4-year-old boy with a history of idiopathic clubfoot treated successfully with the Ponseti method presents with a relapsed deformity. Gait analysis shows dynamic supination of the foot during the swing phase. Passive range of motion demonstrates a fully correctable deformity. What is the most appropriate surgical intervention?
Explanation
Question 47
A 3-year-old boy sustains an isolated midshaft femur fracture. Radiographs demonstrate 1.5 cm of shortening and 10 degrees of varus angulation. What is the most appropriate definitive management?
Explanation
Question 48
A 13-year-old girl sustains an ankle injury during a soccer game. Radiographs reveal a Salter-Harris type III fracture of the anterolateral aspect of the distal tibial epiphysis (Tillaux fracture). This fracture pattern is primarily caused by an avulsion of which of the following structures?
Explanation
Question 49
A 12-year-old boy presents with a history of recurrent ankle sprains and a rigid, painful flatfoot. Radiographs demonstrate an "anteater nose" sign.
Which radiographic view is most sensitive for confirming the exact location of the most likely coalition?
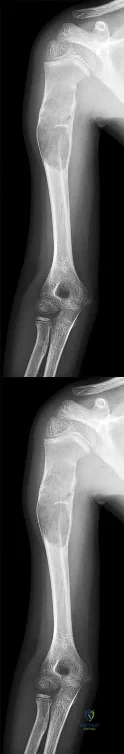
Explanation
Question 50
A 10-year-old boy with known Legg-Calvé-Perthes disease presents with increasing hip pain and stiffness. An arthrogram demonstrates "hinge abduction" with lateral subluxation of the femoral head against the acetabular rim during hip abduction. What is the most appropriate surgical treatment?
Explanation
Question 51
A newborn infant is noted to have severe anterolateral bowing of the right tibia. There are no fractures present on initial radiographs. The infant is at highest risk for developing congenital pseudarthrosis of the tibia (CPT). Which of the following genetic conditions is most strongly associated with this finding?
Explanation
Question 52
A 14-year-old elite baseball pitcher complains of insidious onset right shoulder pain during the cocking phase of throwing. Radiographs reveal widening and irregularity of the proximal humeral physis. What is the most appropriate initial management?
Explanation
Question 53
A 5-year-old boy is brought to the emergency department after a low-speed motor vehicle collision. He is neurologically intact with no neck pain. Lateral cervical spine radiographs show 3 mm of anterior translation of C2 on C3. The Swischuk line passes 1 mm anterior to the anterior aspect of the posterior arch of C3. What is the most appropriate management?
Explanation
Question 54
An 11-year-old boy complains of intermittent left knee pain after playing basketball. MRI reveals a 1.5 cm stable osteochondritis dissecans (OCD) lesion on the lateral aspect of the medial femoral condyle. What is the most important factor predicting successful non-operative healing of this lesion?
Explanation
Question 55
A 6-year-old girl presents with a painless "clunking" in her right knee. She has no history of trauma. MRI confirms the presence of a Wrisberg variant discoid lateral meniscus. This specific variant is characterized by the absence of which of the following structures?
Explanation
Question 56
A 7-year-old child with spastic quadriplegic cerebral palsy is evaluated during routine hip surveillance. Radiographs demonstrate a Reimers Migration Percentage of 45% in the right hip. The patient is non-ambulatory (GMFCS Level V) but experiences pain with diapering. What is the most recommended treatment?
Explanation
Question 57
A 2-month-old infant is diagnosed with congenital muscular torticollis, presenting with a right sternocleidomastoid mass and the chin rotated to the left. Which of the following screening evaluations is strictly recommended for this infant?
Explanation
Question 58
A 4-year-old boy with blue sclerae has sustained six fractures over the past two years with minimal trauma. Genetic testing confirms Osteogenesis Imperfecta (OI). The fundamental pathophysiology of his disease involves a defect in the synthesis of which of the following?
Explanation
Question 59
A 5-year-old girl undergoes closed reduction and percutaneous pinning for a Gartland type III supracondylar humerus fracture. Postoperatively, the radial pulse is completely absent, but her hand is warm, pink, and demonstrates brisk capillary refill (<2 seconds). What is the most appropriate management?
Explanation
Question 60
A 12-year-old boy presents with a 3-week history of right hip pain and a limp. He is unable to bear weight on the right leg, even with crutches. Radiographs confirm a Slipped Capital Femoral Epiphysis (SCFE). According to the Loder classification, what is the most significant prognostic factor associated with this specific presentation?
Explanation
Question 61
An 8-year-old boy is diagnosed with Legg-Calve-Perthes disease. Radiographs show greater than 50% collapse of the lateral pillar of the femoral head. According to the Herring lateral pillar classification, what is his stage and expected prognosis?
Explanation
Question 62
A 4-week-old female with an irreducible but dilatable left developmental dysplasia of the hip (DDH) is placed in a Pavlik harness. After 4 weeks of strictly compliant wear, dynamic ultrasound shows the hip remains completely dislocated. What is the most appropriate next step in management?
Explanation
Question 63
A 3-year-old girl presents with progressive bilateral genu varum. Radiographs reveal a prominent medial metaphyseal beak and a sharp diaphyseal-metaphyseal angle. Which of the following is the most accurate statement regarding the suspected underlying pathology?
Explanation
Question 64
A 6-year-old boy sustains a severe extension-type supracondylar humerus fracture. On examination, the hand is pink and warm with normal capillary refill, but the radial pulse is not palpable.
What is the most appropriate initial management?
Explanation
Question 65
An infant born with idiopathic clubfoot is treated with the Ponseti method. After successful sequential casting and a percutaneous Achilles tenotomy, the foot is placed in a foot abduction orthosis. The parents ask what the most common cause of future deformity recurrence is. What is the correct response?
Explanation
Question 66
A 4-year-old child with a history of multiple low-energy fractures, distinct blue sclerae, and dentinogenesis imperfecta is evaluated in the orthopedic clinic. Genetic testing reveals an autosomal dominant mutation. This systemic condition is primarily caused by a quantitative or qualitative defect in which of the following?
Explanation
Question 67
A 4-year-old boy previously treated for idiopathic clubfoot with the Ponseti method presents with a dynamic supination deformity during the swing phase of gait. Passive ankle dorsiflexion is 15 degrees. What is the most appropriate surgical management?
Explanation
Question 68
An 8-year-old boy is diagnosed with Legg-Calvé-Perthes disease. Anteroposterior radiographs demonstrate greater than 50% loss of the lateral pillar height. According to the Herring classification, which group does this represent and what is the expected outcome?
Explanation
Question 69
A 10-year-old girl with spastic diplegic cerebral palsy is found to have a Reimers migration percentage of 55% bilaterally. She is asymptomatic but has progressive subluxation. What is the most appropriate surgical intervention?
Explanation
Question 70
A 14-year-old obese male presents with a stable slipped capital femoral epiphysis (SCFE) of the left hip. He undergoes in situ pinning. Which of the following conditions represents the strongest indication for prophylactic pinning of the asymptomatic contralateral hip?
Explanation
Question 71
A 3-year-old boy presents with persistent bowing of the legs. Radiographs reveal medial metaphyseal beaking and a metaphyseal-diaphyseal angle of 18 degrees. What is the most appropriate initial management for this patient?
Explanation
Question 72
A 2.5-year-old girl presents with a limp. Clinical examination and radiographs confirm a unilaterally dislocated left hip (Developmental Dysplasia of the Hip). What is the most appropriate definitive management?
Explanation
Question 73
A 7-year-old boy sustains a completely displaced extension-type supracondylar humerus fracture. On neurological examination, he is unable to flex the interphalangeal joint of the thumb and the distal interphalangeal joint of the index finger. Which nerve is injured?
Explanation
None
