Pediatric Orthopedic MCQs: Osteogenesis Imperfecta & SMA Comprehensive Review
Key Takeaway
This interactive board review contains 100 randomly selected orthopedic surgery questions with clinical images, immediate feedback, and detailed references.
Pediatric Orthopedic MCQs: Osteogenesis Imperfecta & SMA Comprehensive Review
Comprehensive 100-Question Exam
00:00
Start Quiz
Question 1
A 10-year-old boy presents with a history of recurrent fractures, blue sclerae, and opalescent teeth. Genetic testing reveals a mutation in COL1A1. Which of the following best describes the fundamental defect in the collagen synthesis pathway for this patient?
Explanation
Question 2
A 6-year-old girl with Spinal Muscular Atrophy (SMA) Type II presents for evaluation of progressive scoliosis. She is currently receiving intrathecal Nusinersen therapy. What is the mechanism of action of this medication?
Explanation
Question 3
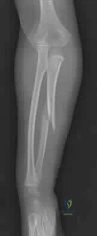
A 12-year-old male with Osteogenesis Imperfecta develops a painful, rapidly enlarging mass over his right femur following a minor trauma. Radiographs show a massive, dense ossification surrounding the femoral shaft. Genetic testing would most likely reveal a mutation in which of the following genes?
Explanation
Question 4
A 14-year-old non-ambulatory male with SMA Type II has a 75-degree progressive neuromuscular scoliosis and significant pelvic obliquity. He is scheduled for a posterior spinal fusion from T2 to the pelvis. He has been receiving intrathecal therapies for his SMA. Which specific surgical modification is most critical to consider during this procedure?
Explanation
Question 5
A 3-year-old girl with severe Osteogenesis Imperfecta (Sillence Type III) presents with marked anterolateral bowing of both femurs, interfering with her ability to stand in braces. Which of the following is the most appropriate surgical management for her deformities?
Explanation
Question 6
Spinal Muscular Atrophy (SMA) is characterized by the progressive degeneration of which of the following structures?
Explanation
Question 7
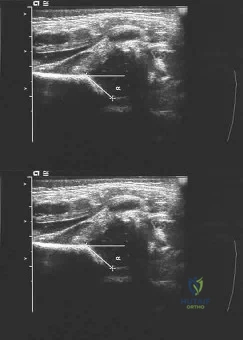
A 7-year-old child with Osteogenesis Imperfecta Type IV has been on intravenous pamidronate therapy for 3 years. Which of the following radiographic findings is a direct consequence of this pharmacological treatment?
Explanation
Question 8
You are evaluating a 4-year-old boy recently diagnosed with SMA. His parents state he can sit independently if placed in position, but he has never been able to stand or walk. Based on this clinical milestone, which type of SMA does he have, and what is the expected lifespan?
Explanation
Question 9
Which of the following factors plays the most significant role in determining the phenotypic severity of Spinal Muscular Atrophy (SMA) in patients with an SMN1 gene mutation?
Explanation
Question 10
A 15-year-old girl with Osteogenesis Imperfecta Type I presents with progressive hearing loss. What is the most common etiology of hearing impairment in patients with OI?
Explanation
Question 11
An 8-year-old boy with severe SMA Type II presents with unilateral right hip dislocation. He has an asymptomatic windswept pelvic deformity and does not walk. He sits in a customized wheelchair. What is the most appropriate management for his right hip dislocation?
Explanation
Question 12
A 6-month-old infant is evaluated for multiple fractures with no clear history of trauma. Radiographs show multiple healing fractures of different ages, osteopenia, and wormian bones in the skull. Which of the following clinical findings would most strongly support a diagnosis of Osteogenesis Imperfecta over non-accidental trauma?
Explanation
Question 13
In Osteogenesis Imperfecta, treatment with bisphosphonates reduces fracture frequency and increases bone mineral density. However, long-term use has been associated with which of the following orthopedic complications?
Explanation
Question 14
A 9-year-old boy with OI Type III presents with a new onset of occipital headaches, hyperreflexia, and subjective weakness in his upper extremities. What is the most critical next step in evaluation?
Explanation
Question 15
The medication Zolgensma (Onasemnogene abeparvovec) is an FDA-approved gene therapy for SMA. What is its mechanism of action?
Explanation
Question 16
A 10-year-old girl with OI Type IV undergoes bilateral femoral osteotomies and telescoping intramedullary rod insertion. Two years later, radiographs show that the male (distal) portion of the rod has migrated proximally out of the distal epiphysis. Which complication of telescoping rods does this represent?
Explanation
Question 17
A patient with Osteogenesis Imperfecta presents with severe dentinogenesis imperfecta (DI). DI is most frequently associated with which mutation and which classification of OI?
Explanation
Question 18
In patients with SMA, neuromuscular scoliosis often presents early and progresses rapidly. What is the typical curve pattern and sagittal profile associated with SMA scoliosis?
Explanation
Question 19
A 1-year-old infant is suspected of having a lethal form of Osteogenesis Imperfecta. They have multiple in utero fractures, 'crumpled' long bones, and an extremely soft skull. According to the Sillence classification, which type of OI does this infant have?
Explanation
Question 20
You are evaluating a 5-year-old male with SMA Type II. He presents with bilateral knee flexion contractures of 40 degrees and equinovarus foot deformities. He is non-ambulatory. What is the primary indication for surgical intervention for lower extremity contractures in non-ambulatory SMA patients?
Explanation
Question 21
A 4-year-old child with Spinal Muscular Atrophy Type II is scheduled for a posterior spinal fusion for progressive neuromuscular scoliosis. During the induction of anesthesia, which of the following agents is strictly contraindicated due to a specific severe adverse effect?
Explanation
Question 22
A 10-year-old boy presents with forearm deformity and restricted pronosupination. Radiographs reveal calcification of the interosseous membrane and a history of hyperplastic callus formation following a previous femur fracture. Which genetic mutation is most likely responsible for this specific phenotype?
Explanation
Question 23
A 6-year-old patient with SMA Type II requires surgical stabilization for a progressive 80-degree neuromuscular scoliosis. The patient is currently receiving Nusinersen (Spinraza) therapy. What specific surgical consideration must be addressed during the spinal fusion?
Explanation
Question 24
A 14-year-old patient with Osteogenesis Imperfecta Type IV complains of new-onset occipital headaches, hyperreflexia, sleep apnea, and swallowing difficulties. Which of the following is the most appropriate next diagnostic step?
Explanation
Question 25
A non-ambulatory 8-year-old child with SMA Type II presents with unilateral hip subluxation noted on a routine surveillance radiograph. The patient is completely pain-free, tolerates sitting well, and has a symmetrical, level pelvis. What is the most appropriate management for this hip subluxation?
Explanation
Question 26
A 7-year-old with OI Type III underwent placement of Fassier-Duval telescoping rods in both femurs 2 years ago. He now presents with anterior thigh pain. Radiographs reveal proximal migration of the female rod component out of the bone and into the gluteal soft tissues. What is the most common technical error leading to this specific complication?

Explanation
Question 27
Spinal Muscular Atrophy is primarily caused by a homozygous deletion or mutation in the SMN1 gene. The clinical severity of the disease, which distinguishes between Types I, II, III, and IV, is most closely and inversely correlated with which of the following factors?
Explanation
Question 28
A 3-year-old child with severe Osteogenesis Imperfecta is started on cyclical intravenous Pamidronate. Which of the following best describes the cellular mechanism of action of this medication?
Explanation
Question 29
A 2-year-old with SMA Type II is being evaluated for orthotic management to aid in supported standing. Which of the following is the primary goal of standing programs and lower extremity orthoses in a non-ambulatory child with SMA?
Explanation
Question 30
A histomorphometric analysis of an iliac crest bone biopsy from a patient with severe Osteogenesis Imperfecta (Type III) would most likely demonstrate which of the following findings compared to a healthy, age-matched control?
Explanation
Question 31
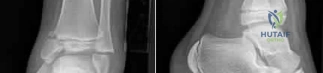
Onasemnogene abeparvovec (Zolgensma) is a transformative therapeutic option for patients with SMA. What is the specific mechanism of action of this therapy?
Explanation
Question 32
A patient diagnosed with Osteogenesis Imperfecta Type VI is noted to have a paradoxically poor response to bisphosphonate therapy and exhibits an isolated mineralization defect on bone histology that mimics osteomalacia. Which gene is most likely mutated in this patient?
Explanation
Question 33
A 5-year-old with SMA Type II presents with a progressive thoracolumbar neuromuscular scoliosis measuring 35 degrees. The child is a functional sitter. What is the most appropriate role for a Thoracolumbosacral Orthosis (TLSO) in the management of this patient?
Explanation
Question 34
The Sofield-Millar operation remains a foundational concept in the surgical management of severe long bone deformities in Osteogenesis Imperfecta. What does this classic procedure fundamentally entail?
Explanation
Question 35
In a patient with Spinal Muscular Atrophy Type II undergoing evaluation for posterior spinal fusion, which preoperative pulmonary function test parameters are the most critical predictors of postoperative extubation success and respiratory complications?
Explanation
Question 36
Dentinogenesis imperfecta (DI) is a common manifestation of certain types of Osteogenesis Imperfecta. Which of the following accurately describes the dental findings and its most common associated OI types?
Explanation
Question 37
A 12-year-old non-ambulatory male with SMA Type II presents with bilateral 30-degree knee flexion contractures and 20-degree hip flexion contractures. His parents inquire about surgical release to allow him to lie completely flat in bed. He currently has no pain and sits comfortably in his wheelchair. What is the most appropriate recommendation?
Explanation
Question 38
Blue sclerae, a hallmark clinical finding in many patients with Osteogenesis Imperfecta (especially Type I), are primarily attributed to which of the following physiological alterations?
Explanation
Question 39
Spinal Muscular Atrophy primarily causes weakness through the degeneration of which specific neural structures?
Explanation
Question 40
While bisphosphonates (antiresorptive agents) are the standard of care for severe Osteogenesis Imperfecta, recent research has explored anabolic agents to increase bone formation. Which of the following drugs represents an anabolic approach by acting as a monoclonal antibody against sclerostin?
Explanation
Question 41
A 10-year-old boy with Spinal Muscular Atrophy (SMA) Type II is scheduled for a posterior spinal fusion to correct a severe, progressive neuromuscular scoliosis. He is currently receiving Nusinersen (Spinraza) therapy. What specific surgical modification must be planned to facilitate his ongoing medical treatment?
Explanation
Question 42
A 5-year-old boy with Osteogenesis Imperfecta (OI) presents with bowing of the bilateral femurs.
He undergoes placement of telescoping intramedullary rods (Fassier-Duval). What is the most common mechanical complication associated with this specific type of implant?

Explanation
Question 43
Which of the following genetic profiles determines the phenotypic severity of Spinal Muscular Atrophy in a patient with a homozygous deletion of the SMN1 gene?
Explanation
Question 44
A 14-year-old female with Osteogenesis Imperfecta has been treated with intravenous pamidronate for 10 years. Radiographs of her distal femur reveal multiple transverse radiodense lines.
What is the mechanism of action of this medication in producing these lines?

Explanation
Question 45
A 7-year-old non-ambulatory child with SMA Type II presents with an asymptomatic, unilateral dislocated hip. Pelvic obliquity is minimal. What is the most appropriate management for this hip?
Explanation
Question 46
A 3-year-old child presents with frequent fractures, blue sclerae, and hyperplastic callus formation following a recent tibia fracture. Genetic analysis reveals a mutation in the IFITM5 gene. Which type of Osteogenesis Imperfecta does this patient have?
Explanation
Question 47
During preoperative evaluation for scoliosis surgery in a 12-year-old with SMA Type II, the pulmonologist performs spirometry. Which of the following pulmonary function test findings indicates an increased risk of prolonged postoperative mechanical ventilation?
Explanation
Question 48
A patient with severe Osteogenesis Imperfecta (Type III) develops progressive upper motor neuron signs, hyperreflexia, and lower cranial nerve deficits. What is the most likely diagnosis?
Explanation
Question 49
A 2-month-old infant is diagnosed with SMA Type I (Werdnig-Hoffmann disease). The parents ask about Onasemnogene abeparvovec (Zolgensma). What is the mechanism of this therapy?
Explanation
Question 50
A 10-year-old girl with SMA Type II presents with severe, collapsing neuromuscular scoliosis.
When planning a posterior spinal fusion for this patient, what is the most appropriate distal foundation to prevent future deformity?
Explanation
Question 51
Which of the following anesthetic complications is most highly associated with patients who have Osteogenesis Imperfecta?
Explanation
Question 52
A 4-year-old boy with SMA Type II is undergoing surgical release of severe bilateral knee flexion contractures. The anesthesiologist asks about muscle relaxant precautions. Why is succinylcholine absolutely contraindicated in this patient?
Explanation
Question 53
A newborn presents with hypotonia, multiple congenital fractures, and profound osteopenia on radiographs. Genetic testing confirms a mutation affecting type I collagen synthesis. The primary biochemical defect in classical Osteogenesis Imperfecta usually involves the substitution of which amino acid in the collagen triple helix?
Explanation
Question 54
A 16-year-old male with Osteogenesis Imperfecta Type VI presents with a femur fracture. He has a known SERPINF1 mutation. How does the pathophysiology and medical management of Type VI differ from classical OI (Types I-IV)?
Explanation
Question 55
Which of the following accurately describes the pathology of the dental abnormalities commonly seen in classical Osteogenesis Imperfecta?
Explanation
Question 56
An 8-year-old girl with SMA Type III (Kugelberg-Welander disease) presents to the clinic. Based on her SMA classification, what is her expected maximum lifetime motor milestone?
Explanation
Question 57
A 15-year-old with severe OI has experienced multiple long bone fractures despite years of maximum-dose IV bisphosphonate therapy. The multidisciplinary team considers switching to Denosumab. What is the mechanism of action of Denosumab?
Explanation
Question 58
You are examining an infant with multiple rib fractures in various stages of healing. You are trying to differentiate non-accidental trauma from Osteogenesis Imperfecta. Which skull radiograph finding strongly suggests Osteogenesis Imperfecta over abuse?
Explanation
Question 59
A 6-year-old patient with SMA Type II undergoes bilateral soft tissue releases for severe equinovarus foot deformities. Postoperatively, she is braced. What is the most critical physiological reason why surgical release of contractures in non-ambulatory SMA patients often yields poor functional outcomes?
Explanation
Question 60
In a patient with Osteogenesis Imperfecta undergoing intramedullary rodding of the femur, which of the following osteotomy principles is critical to prevent the "Z-effect" or loss of fixation?
Explanation
Question 61
A newborn presents with a soft, fragile calvarium, a small thoracic cage, and severe bowing of all extremities. Radiographs reveal multiple fractures in various stages of healing, including "accordion" ribs. The infant succumbs to respiratory failure within 24 hours. According to the Sillence classification, what is the most likely fundamental genetic defect?
Explanation
Question 62
A 3-year-old child with Spinal Muscular Atrophy (SMA) Type II is being evaluated for motor milestones. The severity of the clinical phenotype in SMA is primarily determined by the copy number of which of the following genes?
Explanation
Question 63
A 5-year-old boy with Osteogenesis Imperfecta Type III has been receiving cyclic intravenous pamidronate therapy.
Radiographs demonstrate horizontal sclerotic bands in the metaphyses. What is the primary cellular mechanism of action of this medication?

Explanation
Question 64
A 7-year-old non-ambulatory child with Spinal Muscular Atrophy Type II presents for a routine orthopedic follow-up. Pelvic radiographs reveal a painless, complete lateral dislocation of the left hip. The child has no difficulty sitting in his wheelchair. What is the most appropriate management?
Explanation
Question 65
A 14-year-old girl with Osteogenesis Imperfecta Type IV is scheduled for posterior spinal fusion for a progressive 75-degree thoracic scoliotic curve. During preoperative planning, the surgeon must account for which characteristic intraoperative challenge specific to OI?
Explanation
Question 66
A 6-year-old boy with SMA Type II requires surgical intervention for a progressive 80-degree neuromuscular scoliosis with 20 degrees of pelvic obliquity. He is scheduled for magnetically controlled growing rods. Which of the following is a critical surgical principle regarding spinal instrumentation in this specific population?
Explanation
Question 67
A 15-year-old boy with severe Osteogenesis Imperfecta (Type III) presents with worsening occipital headaches, hyperreflexia in the lower extremities, and fine motor clumsiness in the hands. Which of the following is the most appropriate next step in diagnosis?
Explanation
Question 68
A 4-year-old girl with Osteogenesis Imperfecta Type III requires surgical stabilization of a recurrent femur fracture. The surgeon elects to use a Fassier-Duval intramedullary nail.
What is the primary biomechanical advantage of this device compared to a standard Rush rod?

Explanation
Question 69
A 6-month-old infant is newly diagnosed with SMA Type I. The family is counseled regarding Onasemnogene abeparvovec (Zolgensma) therapy. What is the fundamental mechanism of this treatment?
Explanation
Question 70
A 6-month-old infant presents to the ED with a spiral fracture of the femur. The parents, who both have normal physical exams, claim the infant rolled off a low bed. Radiographs reveal the femur fracture and multiple classic metaphyseal lesions (corner fractures) of the distal tibias. Which of the following strongly supports non-accidental trauma rather than Osteogenesis Imperfecta?
Explanation
Question 71
An 8-year-old patient with SMA Type III is prescribed Risdiplam. By what mechanism does this medication improve the patient's muscle function?
Explanation
Question 72
A 6-year-old boy with Osteogenesis Imperfecta Type III presents with brownish-blue, opalescent teeth that exhibit significant wear and enamel flaking. This dental abnormality is a result of a defect in which of the following structures?
Explanation
Question 73
In patients with untreated SMA Type I and II, what is the most common cause of early mortality, dictating the need for aggressive proactive management?
Explanation
Question 74
A 10-year-old with Osteogenesis Imperfecta Type IV undergoes an osteotomy to correct severe anterior bowing of the tibia. Which of the following best characterizes the expected bone healing process in this patient compared to a healthy, age-matched child?
Explanation
Question 75
A 12-year-old boy with SMA Type II presents for posterior spinal fusion. During anesthetic induction, which of the following medications must be strictly avoided due to the risk of severe, life-threatening hyperkalemia?
Explanation
Question 76
If a bone biopsy is taken from the iliac crest of a patient with severe Osteogenesis Imperfecta (Type III), which of the following histologic findings is most expected?
Explanation
Question 77
A 4-month-old infant is brought to the clinic for delayed motor milestones. Examination reveals severe hypotonia, a weak cry, "bell-shaped" chest, absent deep tendon reflexes, and distinct fasciculations of the tongue. The mother reports feeling diminished fetal movements during the third trimester. What is the most likely diagnosis?
Explanation
Question 78
A 25-year-old woman with a history of mild Osteogenesis Imperfecta (Type I) presents for an orthopedic evaluation of a recent Colles fracture. Which of the following extraskeletal manifestations is most frequently associated with her condition and often becomes symptomatic during adulthood?
Explanation
Question 79
A 14-year-old girl is diagnosed with mild Osteogenesis Imperfecta (Type I) after sustaining multiple fractures from minor trauma. Genetic analysis reveals a premature stop codon in one allele of COL1A1. What is the precise biochemical consequence of this mutation?
Explanation
Question 80
Children with Spinal Muscular Atrophy have a high incidence of fragility fractures. Which of the following principles should strictly guide the orthopedic management of a femur fracture in a non-ambulatory SMA patient?
Explanation
Question 81
A 9-year-old boy with a history of multiple fractures presents with a painless, limited range of motion in his right forearm. Radiographs reveal calcification of the interosseous membrane and a history of hyperplastic callus formation following previous fractures.
Genetic testing is most likely to show a mutation in which of the following genes?

Explanation
Question 82
Spinal Muscular Atrophy (SMA) is an autosomal recessive neuromuscular disorder caused by a mutation in the SMN1 gene. Which of the following genetic factors serves as the primary determinant for the phenotypic severity of the disease in these patients?
Explanation
Question 83
A 5-year-old girl with severe Osteogenesis Imperfecta (OI) is receiving intravenous pamidronate infusions to increase bone mineral density and reduce fracture frequency. Which of the following best describes the molecular mechanism of action of this medication?
Explanation
Question 84
A 10-year-old boy with SMA Type II presents with severe, progressive paralytic scoliosis measuring 85 degrees. He is currently receiving intrathecal Nusinersen therapy every 4 months. When planning posterior spinal fusion for this patient, which critical technical modification must be considered?
Explanation
Question 85
An infant diagnosed with SMA Type I receives Onasemnogene abeparvovec (Zolgensma) at 2 months of age. What is the mechanism by which this therapy provides a therapeutic benefit?
Explanation
Question 86
A 14-year-old with Osteogenesis Imperfecta Type IV presents with hyperreflexia, ataxia, and a new-onset headache exacerbated by coughing. Which of the following imaging modalities is the most appropriate next step in evaluation?
Explanation
Question 87
A 6-year-old child with Osteogenesis Imperfecta undergoes bilateral femur Sofield-Millar osteotomies stabilized with Fassier-Duval telescoping rods. Which of the following is the most common complication specifically associated with this type of instrumentation?
Explanation
Question 88
A 7-year-old girl with SMA Type II, who is a non-ambulator and utilizes a customized wheelchair, is found to have an asymptomatic, unilateral dislocated hip on routine radiographic screening. What is the most appropriate orthopedic management?
Explanation
Question 89
Which type of Osteogenesis Imperfecta, according to the Sillence classification, is characterized by extreme bone fragility, multiple intrauterine fractures, severe skeletal deformities, and is generally lethal in the perinatal period?

Explanation
Question 90
A pediatric patient with Spinal Muscular Atrophy Type II is evaluated in the clinic. Without disease-modifying therapies, what is the maximum expected motor milestone this patient will achieve during their natural history?
Explanation
Question 91
A 12-year-old with multiple fractures has a bone biopsy that demonstrates a distinctive 'fish-scale' lamellation pattern under polarized light microscopy. The patient has shown no clinical improvement with prolonged bisphosphonate therapy. This presentation is most consistent with a mutation in which gene?
Explanation
Question 92
A 4-year-old boy with SMA is prescribed Risdiplam. Which of the following accurately describes the administration and mechanism of this medication?
Explanation
Question 93
Osteogenesis Imperfecta Types I and III represent two different clinical severities of the disease. Which of the following best contrasts the underlying collagen defect between classical Type I and classical Type III OI?
Explanation
Question 94
A 5-year-old child with SMA Type II requires general anesthesia for the placement of a gastrostomy tube. The anesthesiologist must strictly avoid which of the following agents to prevent a life-threatening complication?
Explanation
Question 95
A 6-year-old boy with severe Osteogenesis Imperfecta presents with teeth that are opalescent, severely worn, and appear brown-blue. The underlying pathophysiology of this dental manifestation is due to a defect primarily affecting which tooth structure?
Explanation
Question 96
A 10-year-old girl with SMA Type II presents with an increasingly collapsing spine.
A custom Thoracolumbosacral Orthosis (TLSO) is prescribed. What is the primary expectation regarding the use of this brace?

Explanation
Question 97
A 3-year-old child is being evaluated for multiple fractures. The differential diagnosis includes Osteogenesis Imperfecta (OI) and Non-Accidental Trauma (NAT). Which of the following radiographic findings is highly specific for NAT and NOT typically seen in OI?
Explanation
Question 98
In patients with Spinal Muscular Atrophy, the primary pathological process affecting the nervous system is characterized by which of the following?
Explanation
Question 99
A 2-year-old boy with OI Type III receives his first intravenous infusion of pamidronate. Within 24 hours, he develops a fever of 38.5°C, myalgia, and vomiting. What is the most appropriate management of these symptoms?
Explanation
Question 100
Which of the following cellular processes accurately describes how a fracture heals in a patient with classical Osteogenesis Imperfecta (Type I, III, or IV)?
Explanation
None
