Superficial Radial Nerve Injury: A Clinical Case Study on Diagnosis in the Anatomical Snuffbox
Key Takeaway
Superficial radial nerve (SRN) injury is diagnosed via meticulous sensory assessment in its distribution, especially the dorsal thumb web space. Intact radial nerve motor function rules out deeper involvement. Key diagnostic tests include two-point discrimination, light touch, and pinprick sensation, comparing with the contralateral hand to confirm isolated sensory loss after wrist laceration.
Patient Presentation and History
Mechanism of Injury and Demographics
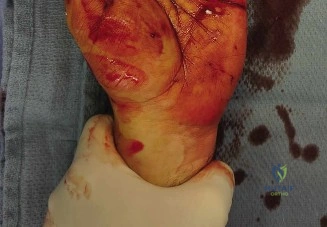
A 34-year-old right-hand dominant male presented to the emergency department following an acute traumatic incident involving a fall onto broken glass during a domestic do-it-yourself project. The mechanism of injury involved a direct, high-velocity impact of the volar-radial aspect of the left forearm and wrist against a fixed, sharp glass edge, resulting in a laceration to the dorsoradial aspect of the left wrist. Specifically, the wound was localized precisely over the anatomical snuffbox. The injury occurred approximately two hours prior to the initial emergency department presentation, placing the patient well within the optimal golden window for acute primary microsurgical intervention.
The patient reported immediate, sharp, and localized pain at the site of the laceration, accompanied by brisk, pulsatile bleeding which he managed independently with direct, sustained manual pressure. Concurrently with the laceration, the patient noted an immediate onset of profound paresthesia described as a "pins and needles" sensation, rapidly progressing to complete anesthesia over the dorsal aspect of the first web space, the dorsal thumb, and the radial aspect of the index finger. This immediate neurological deficit following a sharp penetrating injury is the hallmark presentation of a complete nerve transection, classifying the injury anatomically and physiologically as a Sunderland Grade V neurotmesis.
Comorbidities and Functional Demands
A thorough review of the patient's past medical history revealed well-controlled essential hypertension, managed effectively with a daily dose of lisinopril. He possessed no known drug allergies and had no prior surgical history, specifically lacking any prior orthopedic or plastic surgical interventions on either upper extremity. He is a non-smoker, which is a favorable prognostic indicator for microvascular and peripheral nerve regeneration, and he consumes alcohol on a socially infrequent basis. His tetanus immunization status was confirmed to be up to date, mitigating the immediate risk of Clostridium tetani infection from the contaminated glass mechanism.
From a functional and occupational standpoint, the patient is employed as an Information Technology professional. This occupation necessitates high-level fine motor dexterity, repetitive keystroke actions, and significant bimanual computer utilization. While his right hand is dominant, the functional integrity of his non-dominant left hand is critical for his bimanual occupational tasks, as well as his reported high-demand leisure activities, which include competitive road cycling. The potential for a painful neuroma in the superficial radial nerve distribution—a highly exposed area during cycling grip—poses a significant threat to his quality of life and functional independence, thereby elevating the urgency and precision required for surgical management.
Clinical Examination Findings
Upon initial assessment in the trauma bay, the patient was hemodynamically stable, afebrile, and in mild distress secondary to localized pain and anxiety regarding his functional deficits.
Inspection
The primary zone of injury was systematically evaluated following the removal of the patient's improvised compressive dressing. A 3-centimeter, clean-edged, linear laceration was identified, coursing obliquely across the anatomical snuffbox of the left wrist. The laceration extended from the dorsal-radial aspect of the distal radius, angling distally and volarly towards the apex of the first web space.
While no active, pulsatile arterial hemorrhage was observed at the time of inspection, a significant, organized hematoma was present within the subcutaneous tissues surrounding the wound margins, indicating substantial recent hemorrhage likely originating from the cephalic vein or a dorsal branch of the radial artery. There was no gross deformity of the radiocarpal joint, distal radioulnar joint, or the metacarpals to suggest an underlying displaced fracture or carpal dislocation. Skin color, temperature, and turgor proximal and distal to the laceration appeared symmetric to the contralateral extremity, indicating macroscopically intact peripheral perfusion. No significant tense swelling of the hand or forearm compartments was noted, rendering acute compartment syndrome highly unlikely at this early clinical stage.
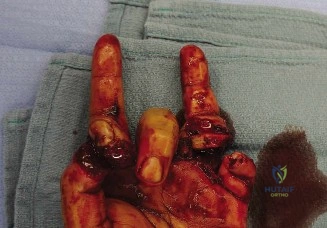
Palpation
Gentle palpation revealed exquisite point tenderness localized strictly to the laceration margins and the immediate underlying soft tissue envelope. Deep palpation of the anatomical snuffbox floor (the scaphoid waist and trapezium) was deferred to avoid disrupting potential underlying hemostasis, but gentle compression over the distal radius and first metacarpal elicited no bony crepitus or step-offs, further lowering the clinical suspicion for an occult osseous injury.
A distinct, strongly positive Tinel's sign was elicited precisely at the proximal margin of the laceration. Percussion at this site reproduced a sharp, electric shock-like sensation radiating distally into the dorsal thumb and first web space, confirming the exact anatomical level of the superficial radial nerve disruption. Capillary refill was brisk, occurring in under two seconds in all digits of the left hand. Both radial and ulnar arterial pulses were strong, bounding, and symmetrically palpable at the volar wrist crease. Due to the organized hematoma, definitive manual palpation for retained radiopaque or radiolucent foreign bodies was obscured.
Range of Motion and Tendon Assessment
A comprehensive assessment of the musculotendinous units traversing the injury zone was conducted to rule out concomitant tendon lacerations.
* Wrist Kinematics: Active and passive range of motion of the radiocarpal and midcarpal joints were full and pain-free in flexion, extension, ulnar deviation, and radial deviation.
* First Dorsal Compartment: Active thumb abduction (Abductor Pollicis Longus) and extension at the metacarpophalangeal joint (Extensor Pollicis Brevis) were intact and symmetric to the contralateral side, indicating preservation of the first dorsal extensor compartment.
* Third Dorsal Compartment: Active retropulsion and extension of the thumb interphalangeal joint (Extensor Pollicis Longus) were robust. The EPL tendon could be visibly and palpably observed bowing across the anatomical snuffbox during active extension, confirming its structural continuity.
* Digital Extensors: Full active and passive range of motion was observed in all metacarpophalangeal and interphalangeal joints of the index through small fingers, with no extensor lag, confirming the integrity of the Extensor Digitorum Communis, Extensor Indicis Proprius, and Extensor Digiti Minimi.
Neurological and Vascular Assessment
The neurological examination was the cornerstone of the diagnostic process, necessitating a highly granular evaluation of the radial nerve and its terminal arborizations.
- Motor Function Assessment (Posterior Interosseous Nerve): Motor function of the deep branch of the radial nerve (PIN) was evaluated to ensure the injury was isolated to the superficial sensory branch. Wrist extension against resistance was strong and symmetric, confirming the integrity of the Extensor Carpi Radialis Longus and Brevis. Finger extension at the MCP joints and thumb retropulsion were fully intact against maximal manual resistance, confirming that the motor fascicles of the radial nerve, which diverge from the superficial sensory branch proximal to the supinator muscle (arcade of Frohse), were completely uninjured.
- Sensory Function Assessment (Superficial Radial Nerve): Sensory mapping was performed using static two-point discrimination and Semmes-Weinstein monofilament testing. The patient exhibited complete anesthesia (inability to perceive the 6.65 monofilament) over the dorsal aspect of the first web space, the dorsal skin of the thumb up to the interphalangeal joint, and the dorsal-radial aspect of the proximal phalanx of the index finger. Sensation in the autonomous zones of the median nerve (volar tip of the index finger) and ulnar nerve (volar tip of the small finger) was perfectly preserved, exhibiting normal static two-point discrimination of 4 millimeters.
- Vascular Assessment: An Allen's test was performed to assess the patency of the superficial and deep palmar arches. The test demonstrated rapid reperfusion of the hand from both the radial and ulnar arteries independently, confirming excellent collateral circulation. Despite the proximity of the radial artery as it dives dorsally through the anatomical snuffbox, the strong distal perfusion and lack of expanding pulsatile hematoma suggested the artery was either uninjured or had sustained a minor adventitial injury that had spontaneously thrombosed.
Imaging and Diagnostics
While the diagnosis of a superficial radial nerve transection in the setting of an open laceration is primarily clinical, judicious utilization of imaging modalities is mandatory to rule out concomitant injuries, specifically retained foreign bodies and occult fractures, which would fundamentally alter the surgical approach and preoperative templating.
Radiographic Evaluation
Standard orthogonal radiographs of the left wrist and hand were obtained, including posteroanterior, lateral, and scaphoid-specific oblique views. The primary indication for plain radiography in this specific clinical scenario was the mechanism of injury: a fall onto broken glass. Glass is inherently radiopaque on standard musculoskeletal radiographs, regardless of lead content, due to its physical density relative to surrounding soft tissues.
The radiographic series demonstrated normal osseous alignment with no evidence of acute fracture, subluxation, or carpal instability. The Gilula's arcs were smooth and unbroken. The scaphoid and radial styloid—the bony floors of the anatomical snuffbox—were fully intact. Crucially, meticulous inspection of the soft tissue shadows on all views revealed no evidence of radiopaque foreign bodies within the subcutaneous tissues or deep fascial planes.
High Resolution Ultrasonography
Given the clean nature of the laceration and the definitive clinical exam, advanced imaging is not strictly mandatory for diagnosis. However, high-frequency musculoskeletal ultrasonography (utilizing a 15-18 MHz linear array transducer) is an invaluable adjunct in the acute trauma setting.
In this case, bedside ultrasonography was utilized to map the proximal and distal stumps of the superficial radial nerve. Sonographic evaluation demonstrated a distinct discontinuity of the fascicular architecture of the SRN approximately 1.5 centimeters proximal to its bifurcation into the lateral and medial terminal branches. The proximal stump appeared slightly edematous, while the distal stump was retracted by approximately 8 millimeters. Furthermore, color Doppler ultrasound was utilized to trace the radial artery through the snuffbox; it demonstrated normal triphasic flow with no evidence of pseudoaneurysm, intimal flap, or extravasation, confirming the structural integrity of the arterial wall.
Magnetic Resonance Imaging Indications
Magnetic Resonance Imaging (MRI) is generally not indicated in the acute management of a sharp, open nerve transection where the site of injury is visually obvious and primary exploration is planned. The role of MRI, specifically high-resolution MR neurography, is reserved for delayed presentations, closed traction injuries, or cases where the exact level of the lesion is clinically ambiguous. In such scenarios, MR neurography can identify nerve root avulsions, neuromas-in-continuity, or extensive Wallerian degeneration. For this acute presentation, MRI would delay definitive surgical management without providing actionable data that would alter the immediate surgical plan.
Differential Diagnosis
The presentation of a dorsal wrist laceration with localized pain and sensory deficits requires a systematic differentiation of the injured anatomical structures within the specific zone of trauma.
| Pathological Entity | Clinical Presentation | Diagnostic Differentiators | Imaging and Procedural Findings |
|---|---|---|---|
| Superficial Radial Nerve Transection | Complete anesthesia over dorsal first web space and dorsal thumb. Positive Tinel's sign at laceration. Intact motor function of thumb/wrist. | Sensory deficit perfectly matches the autonomous zone of the SRN. No motor loss. Mechanism involves sharp, superficial trauma. | Ultrasound shows fascicular discontinuity of the SRN. Direct surgical exploration confirms complete epineurial and fascicular disruption. |
| Radial Artery Laceration | Pulsatile bleeding, rapidly expanding hematoma. Potential diminished capillary refill in thumb/index finger if collateral flow is poor. | Often presents with profound hemorrhage. Allen's test may show delayed radial reperfusion. Sensory deficits are absent unless concomitant nerve injury exists. | Doppler ultrasound shows flow disruption, pseudoaneurysm, or extravasation. Angiography (rarely needed acutely) shows dye leak. |
| Extensor Pollicis Longus Tendon Laceration | Inability to actively retropulse or extend the thumb interphalangeal joint. Weakness in thumb extension. | Loss of active IP joint extension. The EPL tendon is not palpable or visible bowing across the snuffbox during attempted extension. | Ultrasound demonstrates tendon discontinuity and retraction. Plain films are normal. Surgical exploration reveals severed tendon ends. |
Surgical Decision Making and Classification
The decision to proceed with operative intervention in this patient was absolute and unambiguous. The clinical diagnosis of a complete transection of the superficial radial nerve (Sunderland Grade V / Seddon Neurotmesis) in a young, highly functional, and demanding patient necessitates acute microsurgical repair.
Rationale for Operative Intervention
The superficial radial nerve is a purely sensory nerve, but its anatomical location renders it highly susceptible to trauma and, more importantly, to the development of exquisitely painful neuromas following injury. A neuroma forms when regenerating axonal sprouts escape the confines of the epineurium and grow chaotically into the surrounding scar tissue. In the dorsoradial aspect of the wrist, a neuroma is subjected to constant mechanical irritation from clothing, watch bands, and normal daily activities (such as gripping a bicycle handlebar or typing).
Conservative management (wound closure without nerve repair) guarantees the formation of an end-bulb neuroma, leading to chronic neuropathic pain, allodynia, and hyperalgesia, which can be profoundly debilitating. Primary microsurgical neurorrhaphy serves two critical purposes:
1. It provides a conduit for axonal regeneration, offering the best possible chance for the restoration of protective and potentially discriminative sensation in the first web space.
2. It acts as the most effective prophylaxis against the formation of a symptomatic, disorganized neuroma by directing regenerating axons into the distal nerve stump rather than surrounding soft tissues.
Timing and Classification of Repair
The injury occurred two hours prior to presentation. This falls within the optimal window for acute primary repair (within 72 hours). Acute primary repair is superior to delayed repair because the anatomical landmarks are preserved, tissue planes are not yet obscured by dense fibrotic scar tissue, and the nerve ends have not undergone significant retraction or neuroma formation, thereby allowing for a tension-free direct coaptation.
The injury is classified as a sharp, clean transection. Unlike crush injuries or high-velocity gunshot wounds, which require delayed repair to allow the zone of injury to demarcate, a sharp glass laceration typically has a very narrow zone of trauma. This allows for minimal debridement of the nerve stumps and facilitates a direct, end-to-end epineurial repair without the immediate need for interpositional nerve grafting.
Surgical Technique and Intervention
The patient was taken to the operating room on an emergent basis. The procedure was performed under regional anesthesia (supraclavicular brachial plexus block) supplemented with intravenous sedation, allowing for optimal patient comfort and profound regional sympathectomy, which aids in vasodilation and tissue perfusion.
Patient Positioning and Preparation
The patient was positioned supine on the operating table with the left upper extremity extended onto a radiolucent hand table. A well-padded pneumatic tourniquet was applied to the proximal brachium. The entire left upper extremity, from the fingertips to the axilla, was meticulously prepped with chlorhexidine gluconate and draped in a standard sterile orthopedic fashion. The arm was exsanguinated using an Esmarch bandage, and the tourniquet was inflated to 250 mmHg to ensure a bloodless surgical field, which is an absolute prerequisite for microvascular and peripheral nerve surgery.
Surgical Approach and Exploration
The surgical approach utilized the existing traumatic laceration. To gain adequate proximal and distal exposure, the linear laceration was extended longitudinally using a lazy-S incision pattern. This geometric incision prevents the formation of a linear, restrictive scar contracture across the radiocarpal joint line.
Skin flaps were elevated with meticulous preservation of the subdermal vascular plexus. The subcutaneous tissues were dissected using tenotomy scissors and bipolar electrocautery. The hematoma within the anatomical snuffbox was carefully evacuated and irrigated with warm sterile saline.
The initial dissection focused on identifying normal anatomical landmarks outside the immediate zone of injury. The cephalic vein, which frequently courses in close proximity to the SRN, was identified and carefully mobilized. The first and third dorsal compartment tendons (APL, EPB, and EPL) were visually inspected and confirmed to be completely intact, corroborating the preoperative clinical examination. Deep in the snuffbox, the radial artery was identified and traced; it was found to be uninjured, with no adventitial disruption.

Nerve Identification and Preparation
The superficial radial nerve was identified proximally as it emerged from beneath the brachioradialis tendon. It was traced distally into the zone of injury. The proximal stump was identified and mobilized circumferentially for approximately 2 centimeters to alleviate any inherent tension. The distal stump was similarly identified and mobilized. The transection was noted to be complete, occurring approximately 2 centimeters proximal to the nerve's bifurcation into its terminal dorsal digital branches.
Operating loupes (4.5x magnification) were utilized for the initial macroscopic dissection, after which the operating microscope was brought into the field for the definitive nerve preparation and repair. Under high-power magnification, the nerve ends were inspected. The glass laceration had created a relatively clean cut, but a 1-millimeter segment of damaged epineurium and protruding, disorganized fascicles was noted on both stumps.
Using a sharp, micro-surgical diamond knife and a sterile wooden tongue depressor as a cutting block, the proximal and distal nerve stumps were serially sectioned (trimmed) by fractions of a millimeter until healthy, pouting, well-vascularized fascicles were visualized, and normal intraneural architecture (the "mushrooming" effect) was confirmed.
Microsurgical Epineurial Repair
Following adequate preparation, the nerve ends were brought into approximation. A blue silastic background material was placed deep to the nerve to enhance visual contrast and prevent inadvertent suturing to the underlying soft tissues.
The repair was performed using a standard epineurial neurorrhaphy technique. The fascicular topography was carefully aligned by matching the longitudinal epineurial blood vessels (vasa nervorum) and the size/orientation of the internal fascicles.
Two primary stay sutures of 9-0 monofilament nylon on a spatulated micro-needle were placed at the 180-degree and 360-degree positions (the medial and lateral poles of the nerve). These sutures were tied with precise tension—tight enough to approximate the epineurium without causing any buckling or overriding of the internal fascicles. Once the stay sutures were secured, the anterior epineurial wall was repaired with three additional interrupted 9-0 nylon sutures. The nerve was then flipped using the stay sutures, and the posterior epineurial wall was repaired in an identical fashion.
A total of eight epineurial sutures were placed. The coaptation site was inspected under maximum magnification to ensure no fascicles were extruding through the epineurial repair line. The repair was deemed to be entirely tension-free through a full arc of wrist motion. As an adjunct to the suture repair, a thin layer of autologous fibrin glue was applied circumferentially around the coaptation site to seal the epineurium and prevent axonal escape.
Closure and Hemostasis
Prior to closure, the pneumatic tourniquet was deflated. Meticulous hemostasis was achieved using micro-bipolar electrocautery to prevent postoperative hematoma formation, which can lead to excessive fibrosis and constrict the regenerating nerve. The wound was copiously irrigated. The skin was closed loosely with interrupted 4-0 non-absorbable monofilament sutures (nylon) to allow for dependent drainage of any residual serosanguinous fluid.
Post Operative Protocol and Rehabilitation
The success of a peripheral nerve repair is as dependent upon the postoperative rehabilitation protocol as it is upon the technical precision of the microsurgery. The rehabilitation program is phased, focusing initially on protecting the repair and subsequently on maximizing functional recovery and sensory re-education.
Phase I Immediate Postoperative Protection (Weeks 0 to 3)
In the operating room, a bulky, non-compressive soft dressing was applied, followed by a custom-molded thermoplastic volar wrist splint. The splint immobilized the wrist in 20 degrees of extension and included a thumb spica component to immobilize the thumb metacarpophalangeal and carpometacarpal joints. This specific positioning is critical; it places the superficial radial nerve in a relaxed state, entirely offloading the micro-sutured coaptation site.
During this phase, the patient was instructed to maintain strict elevation of the extremity above the level of the heart to minimize interstitial edema. Active and passive range of motion of the uninvolved digits (index through small fingers) was strongly encouraged to prevent joint stiffness and maintain tendon glide. The patient was explicitly instructed to avoid any composite wrist and thumb flexion, which would place catastrophic longitudinal tension on the healing nerve.
Phase II Mobilization and Nerve Gliding (Weeks 4 to 8)
At the three-week postoperative mark, the skin sutures were removed. The wound demonstrated excellent primary intention healing with no signs of erythema or dehiscence. The static splint was transitioned to a removable orthosis, to be worn during sleep and high-risk activities.
Supervised hand therapy was initiated. The primary focus shifted to gentle, progressive active and active-assisted range of motion of the wrist and thumb. Meticulous nerve gliding exercises were introduced. These exercises are designed to prevent the superficial radial nerve from adhering to the surrounding scar tissue bed. Gliding exercises must be performed within a pain-free arc of motion to avoid traction injuries to the delicate regenerating axons.
During this phase, the patient's neurological status was serially monitored by tracking the advancement of the Tinel's sign. Axonal regeneration typically occurs at a rate of approximately 1 millimeter per day (or 1 inch per month) following the initial latency period of Wallerian degeneration. The distal progression of the Tinel's sign serves as a clinical biomarker for successful axonal sprouting across the repair site.
Phase III Sensory Re-education and Desensitization (Weeks 8 and Beyond)
As regenerating axons begin to reach the distal sensory end organs in the skin of the first web space, the brain receives novel, often disorganized afferent signals. This can manifest as hypersensitivity, dysesthesia, or altered perception of touch.
A rigorous sensory re-education program was instituted. This involves cortical remapping techniques. The patient utilized various textures (cotton, silk, velcro) to stimulate the reinnervated skin while visually observing the stimulus, thereby helping the somatosensory cortex accurately interpret the new signals.
Simultaneously, a desensitization protocol was employed to manage any hyperalgesia at the surgical incision site. This included fluidotherapy, light massage, and vibration therapy. Strengthening exercises for the wrist and hand musculature were gradually integrated as the patient's pain tolerance improved and normal kinematics were restored.
The patient was advised that maximal sensory recovery following a peripheral nerve transection can take up to 12 to 18 months. While normal, pre-injury two-point discrimination is rarely fully restored in adults, the primary goal—restoration of protective sensation and the prevention of a debilitating neuroma—is highly achievable with strict adherence to the rehabilitation protocol.
Clinical Pearls and Pitfalls
Clinical Pearls
- High Index of Suspicion: Always assume a superficial radial nerve injury in any laceration over the dorsoradial wrist or anatomical snuffbox until definitively proven otherwise through meticulous sensory examination. The SRN is the most commonly injured nerve in the upper extremity due to superficial lacerations.
- Microscopic Preparation is Paramount: The most critical step in nerve repair is the preparation of the stumps. Inadequate resection of traumatized epineurium and fascicles will result in a barrier of scar tissue that prevents axonal crossing, leading to a failed repair and neuroma formation. Always resect back to healthy, pouting fascicles.
- Tension is the Enemy: A nerve repair must be completely tension-free. Tension across the coaptation site causes ischemia of the intrinsic vasa nervorum, leading to fibroblast proliferation, scarring, and failure of regeneration. If a tension-free repair cannot be achieved with primary approximation, interpositional nerve grafting (e.g., using a medial antebrachial cutaneous nerve autograft) is absolutely indicated.
- Topographical Alignment: While the SRN is primarily sensory, aligning the fascicular architecture based on surface blood vessels prevents cross-innervation of different sensory territories, which can complicate cortical remapping and sensory re-education.
Clinical Pitfalls
- Failure to Examine Before Anesthesia: The most common pitfall in peripheral nerve trauma is failing to perform and document a comprehensive neurological examination prior to the administration of local anesthetics or regional blocks. Once the patient is blocked, the diagnostic window is closed.
- Over-reliance on Imaging: While ultrasound is helpful, negative imaging does not rule out a nerve injury. The diagnosis is fundamentally clinical. Do not delay surgical exploration of a highly suspicious wound based on equivocal imaging.
- Inadequate Hemostasis: Closing a nerve repair over an active bleeding site will result in a hematoma. Blood is highly irritating to peripheral nerves and promotes dense perineurial fibrosis, which acts as a mechanical barrier to axonal regeneration and causes tethering of the nerve.
- Neglecting Postoperative Therapy: The surgeon's job does not end in the operating room. Failing to prescribe and monitor a structured sensory re-education and desensitization program will result in suboptimal functional outcomes, even with a technically perfect microsurgical repair. The brain must be retrained to
