
Orthopedic Trauma Review | Dr Hutaif Trauma & Fractures -...
Comprehensive 100-Question Exam
00:00
Start Quiz
Question 1
A 34-year-old male is brought to the trauma bay after a motorcycle accident. He is hypotensive (BP 75/40 mmHg) and tachycardic (HR 130). Primary survey reveals an 'open book' pelvic fracture. A pelvic binder is immediately applied to reduce pelvic volume and control hemorrhage. To achieve optimal reduction and biomechanical stability to tamponade bleeding, the binder must be centered over which of the following anatomic landmarks?
Explanation
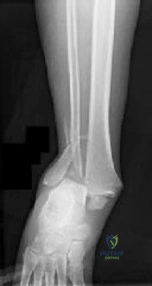
Question 2
A 28-year-old male sustains a high-energy Pauwels type III (vertical) femoral neck fracture. Biomechanical studies comparing fixation methods for this specific highly-unstable fracture pattern demonstrate that which of the following constructs provides the greatest resistance to vertical shear forces and subsequent varus collapse?
Explanation
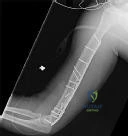
Question 3
A 42-year-old male is undergoing open reduction and internal fixation of a bicondylar tibial plateau fracture (Schatzker VI). The surgeon plans a standard posteromedial approach to directly reduce and buttress a displaced posteromedial fragment. The surgical interval for this approach involves mobilizing and retracting which two structures?
Explanation
Question 4
A 30-year-old male sustains a Gustilo-Anderson IIIB open fracture of the middle third of the tibia with a 6 cm anterior soft tissue defect exposing bone void of periosteum. Following thorough serial debridement and skeletal stabilization, which of the following is the most appropriate local muscle flap for coverage of this specific defect?
Explanation
Question 5
A 45-year-old male is involved in a motor vehicle collision and sustains a complex acetabular fracture.
On the obturator oblique radiograph, the 'spur sign' is distinctly visible. According to the Letournel and Judet classification, this radiographic finding is pathognomonic for which of the following acetabular fracture patterns?
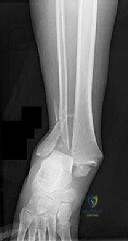
Explanation
Question 6
A 25-year-old snowboarder sustains a Hawkins type II talar neck fracture and undergoes urgent ORIF. At 8 weeks postoperatively, an AP radiograph of the ankle demonstrates a subchondral radiolucent band in the talar dome, known as the Hawkins sign. What is the clinical significance of this finding?
Explanation
Question 7
A 38-year-old roofer falls from a height and sustains a severely displaced intra-articular calcaneus fracture. The surgeon opts for open reduction and internal fixation utilizing an extensile lateral approach. The full-thickness fasciocutaneous flap elevated in this approach receives its primary blood supply from which of the following vessels?
Explanation
Question 8
The standard of care for high-energy tibial pilon fractures usually involves temporary application of a spanning external fixator followed by delayed definitive ORIF 10-14 days later. What is the primary rationale for staging the surgical management of this injury?
Explanation
Question 9
A 22-year-old male sustains a closed, distal-third spiral humeral shaft fracture (Holstein-Lewis) during an arm-wrestling match. On initial presentation, he exhibits a dense radial nerve palsy. Closed reduction is performed and a coaptation splint is applied. Post-reduction examination confirms the radial nerve palsy is persistent and unchanged. Based on AAOS guidelines, what is the most appropriate management of the radial nerve?
Explanation
Question 10
A 55-year-old female undergoes volar locking plate fixation for a displaced intra-articular distal radius fracture. Six months postoperatively, she returns complaining of a sudden inability to actively flex the interphalangeal joint of her thumb. This complication is most closely associated with which of the following surgical technique errors?
Explanation
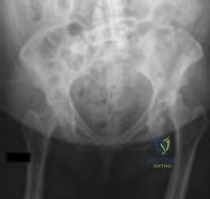
Question 11
A 20-year-old college athlete falls onto an outstretched hand and sustains a fracture of the proximal pole of the scaphoid. This fracture pattern carries a high risk of nonunion and avascular necrosis due to the scaphoid's retrograde blood supply. Which of the following arteries provides the primary blood supply to the proximal pole of the scaphoid?
Explanation
Question 12
A 40-year-old male is involved in a high-speed motor vehicle collision. Radiographs and CT scan of his right knee reveal an intra-articular, coronal plane fracture of the lateral femoral condyle. What is the eponym for this specific fracture pattern, and what is the optimal trajectory for lag screw fixation?
Explanation
Question 13
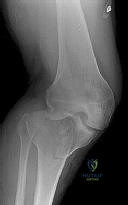
A 28-year-old male sustains a closed comminuted midshaft tibia fracture. Eight hours later, he complains of worsening pain out of proportion to the injury, unrelieved by intravenous opioids. His blood pressure is 110/70 mmHg. Intracompartmental pressure testing of the anterior compartment yields a measurement of 45 mmHg. What is the patient's Delta P (ΔP), and what is the indicated treatment?
Explanation
Question 14
The Mangled Extremity Severity Score (MESS) is a clinical tool historically utilized to help guide the difficult decision between amputation and limb salvage in severe lower extremity trauma. Which of the following variables is NOT a scored component of the MESS criteria?
Explanation
Question 15
A 35-year-old male polytrauma patient presents with closed bilateral femoral shaft fractures, multiple rib fractures, and bilateral pulmonary contusions. Initial arterial blood gas evaluation shows a pH of 7.21, base excess of -8, and lactate of 5.0 mmol/L. According to the principles of Damage Control Orthopedics (DCO), what is the most appropriate initial management for his femur fractures?
Explanation
Question 16
A 45-year-old farmer catches his leg in a tractor mechanism, sustaining a Gustilo-Anderson type IIIA open tibia fracture heavily contaminated with soil and manure. According to current evidence-based guidelines for open fracture management in farm injuries, which of the following intravenous antibiotic regimens is most traditionally appropriate for initial prophylaxis?
Explanation
Question 17
A 25-year-old female presents to the trauma bay after a high-speed skiing accident.
Examination reveals a clinically obvious posterior knee dislocation. The joint is urgently reduced in the emergency department. Post-reduction, the extremity is warm, but pulses are slightly asymmetric. An Ankle-Brachial Index (ABI) is calculated to be 0.85. What is the most appropriate next step in management?
Explanation
Question 18
A 32-year-old competitive cyclist falls directly onto his right shoulder, sustaining a midshaft clavicle fracture. Which of the following radiographic or clinical findings is considered an absolute indication for open reduction and internal fixation rather than nonoperative management?
Explanation
Question 19
A 29-year-old football player sustains a hyperplantarflexion injury to his midfoot. Weight-bearing radiographs reveal a 3 mm diastasis between the base of the first and second metatarsals. The primary ligamentous stabilizer disrupted in this injury (the Lisfranc ligament) courses between which two osseous structures?
Explanation
Question 20
A 22-year-old male sustains a low-velocity civilian gunshot wound to the right thigh, resulting in a comminuted midshaft femur fracture. The entrance and exit wounds are 1 cm in diameter with no gross contamination or active bleeding. Compartments are soft, and distal pulses are intact. What is the most appropriate management of this injury?
Explanation
Question 21
A 35-year-old man presents with a posterior hip dislocation and associated posterior wall acetabular fracture after a motor vehicle collision. Closed reduction is performed in the emergency department. The post-reduction CT scan reveals a 40% posterior wall defect with a significant area of marginal impaction. What is the most critical step during open reduction and internal fixation to ensure a congruent joint and minimize post-traumatic arthritis?
Explanation
Question 22
A 28-year-old hypotensive male is brought in after a motorcycle crash. A pelvic binder is immediately applied. Radiographs show a widened symphysis pubis and disrupted sacroiliac joints bilaterally, consistent with an Anteroposterior Compression (APC) Type III injury. FAST scan is negative. Despite 2 units of uncrossmatched blood and crystalloid resuscitation, his blood pressure remains 75/40 mmHg. What is the most appropriate next step in management?
Explanation
Question 23
A 22-year-old male sustains a vertical, displaced basicervical femoral neck fracture (Pauwels Type III) during a sporting event. Which of the following factors has been shown in recent literature to be the most critical in decreasing the rate of nonunion and osteonecrosis in this specific patient population?
Explanation
Question 24
In the setting of a completely displaced subtrochanteric femur fracture, the proximal fragment is typically displaced into flexion, abduction, and external rotation due to muscular pull. Which muscle group is primarily responsible for the external rotation deformity of the proximal fragment?
Explanation
Question 25
A 65-year-old woman on long-term alendronate therapy presents with a 3-month history of a dull, aching pain in her right thigh. Radiographs reveal lateral cortical thickening and a transverse radiolucent line in the subtrochanteric region of the right femur.
What is the recommended standard of care for this patient?

Explanation
Question 26
A 45-year-old male sustains a high-energy varus injury to his knee, resulting in a medial tibial plateau fracture with a large posteromedial fragment (Schatzker IV). Which of the following surgical approaches is most appropriate for direct visualization and optimal mechanical buttress plating of the posteromedial fragment?
Explanation
Question 27
A 30-year-old male is admitted with a closed midshaft tibia fracture treated with casting. Twelve hours later, he complains of severe, escalating leg pain out of proportion to the injury, unrelieved by intravenous opioids. On examination, he has pain with passive stretch of the hallux and a tense calf. When utilizing intra-compartmental pressure monitoring, what is the most definitive diagnostic threshold indicating acute compartment syndrome that requires immediate fasciotomy?
Explanation
Question 28
A 42-year-old female presents with a high-energy intra-articular distal tibia fracture (Pilon, AO/OTA 43-C3) with severe soft tissue swelling, fracture blisters, and a significantly shortened extremity. What is the gold standard initial management protocol for this injury?
Explanation
Question 29
During open reduction and internal fixation of a Weber C ankle fracture, the surgeon performs a Cotton test to assess the integrity of the syndesmosis. Which of the following intraoperative radiographic findings during the test indicates dynamic syndesmotic instability requiring fixation?
Explanation
Question 30
A 28-year-old male sustains a talar neck fracture following a fall from a height. Radiographs demonstrate a displaced fracture of the talar neck with subluxation of the subtalar joint, but the tibiotalar joint remains congruous. According to the Hawkins classification, what is the fracture type and the historically associated risk of avascular necrosis (AVN) of the talar body?
Explanation
Question 31
In the evaluation and surgical planning of a displaced intra-articular calcaneus fracture, the Sanders classification is highly prognostic. This classification is primarily based on the number of articular fracture lines and their location on which specific imaging view?
Explanation
Question 32
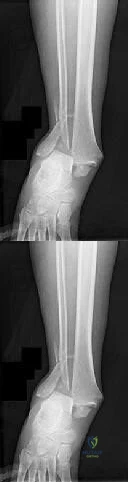
A 24-year-old football player sustains a hyperplantarflexion injury to his midfoot. Radiographs show widening of the space between the base of the first and second metatarsals, indicative of a Lisfranc injury.
The critical Lisfranc ligament, disrupted in this injury, connects which two osseous structures?
Explanation
Question 33
A 45-year-old male sustains an isolated scapula body fracture with involvement of the extra-articular glenoid neck after a high-speed fall. Which of the following radiographic parameters is a generally accepted indication for operative internal fixation of an extra-articular scapular neck fracture?
Explanation
Question 34
A 32-year-old female presents with a closed spiral fracture of the distal third of the humeral shaft resulting from a fall. On physical examination, she is unable to actively extend her wrist or her metacarpophalangeal joints. What is the most appropriate initial management of this injury?
Explanation
Question 35
A 29-year-old female falls onto an outstretched hand and sustains a coronal shear fracture of the capitellum that extends medially to include a large portion of the trochlea (McKee modification of Bryan and Morrey Type IV). What is the optimal surgical approach to address this specific, complex fracture pattern?
Explanation
Question 36
A 36-year-old male is struck by a heavy metal pipe on the forearm while defending himself. Radiographs reveal a displaced, short oblique fracture of the distal third of the radius with associated widening and disruption of the distal radioulnar joint (DRUJ). This specific injury pattern is best described as a:
Explanation
Question 37
The "terrible triad" of the elbow is a complex instability pattern comprising an elbow dislocation, a radial head fracture, and a coronoid fracture. During open surgical reconstruction of this injury, what is the most widely accepted and biomechanically sound sequence of repair to restore elbow stability?
Explanation
Question 38
A 27-year-old man sustains a severe open tibia fracture following a motorcycle crash. Operative exploration reveals extensive soft tissue stripping, muscle necrosis, and a large segmental soft tissue defect over the anterior leg with exposed, devascularized bone. The vascular surgeon confirms that distal pulses are palpable and major arteries are intact, but the orthopedic and plastic surgeons agree that a free muscle flap will be required for adequate coverage. According to the Gustilo-Anderson classification, what is the grade of this open fracture?
Explanation
Question 39
A 55-year-old female presents with a displaced intra-articular fracture of the distal radius. Radiographs demonstrate a fracture characterized by a volar marginal articular fragment (involving the lunate facet) that has displaced proximally and volarly along with the entire carpus. Which of the following internal fixation constructs is biomechanically optimal to prevent loss of reduction of this specific, highly unstable fragment?
Explanation
Question 40
A 34-year-old male is brought to the trauma bay after a severe high-speed motor vehicle collision. He has closed, bilateral comminuted femoral shaft fractures, a grade III spleen laceration, pulmonary contusions, and a moderate traumatic brain injury. His admission labs show a lactate of 5.5 mmol/L, pH of 7.20, and a base excess of -8. Under the principles of Damage Control Orthopedics (DCO), what is the most appropriate initial orthopedic management for his bilateral femur fractures?
Explanation
Question 41
A 35-year-old male sustains a high-energy trauma resulting in a distal femur fracture. CT scan reveals a coronal plane fracture of the lateral femoral condyle. Which of the following is the most appropriate surgical approach and fixation strategy for this specific fracture pattern?
Explanation
Question 42
A 45-year-old man presents with a subtrochanteric femoral fracture. The proximal fragment is typically flexed, abducted, and externally rotated. Which muscle group is primarily responsible for the external rotation of the proximal fragment?
Explanation
Question 43
A 28-year-old female is brought to the ED after a motor vehicle collision. She is hemodynamically unstable. A pelvic binder is applied.
Radiographs show a widened symphysis pubis > 2.5 cm and disruption of the anterior sacroiliac ligaments, but intact posterior sacroiliac ligaments. According to the Young-Burgess classification, what type of injury is this, and what is the most common primary source of bleeding?
Explanation
Question 44
A 32-year-old man sustained a talar neck fracture 8 weeks ago. He is being followed up in the clinic. Radiographs reveal a subchondral radiolucent band in the dome of the talus. What does this finding (Hawkins sign) indicate?
Explanation
Question 45
A 24-year-old male sustains a closed tibial shaft fracture. Two hours post-admission, he complains of severe pain out of proportion to the injury. On examination, pain is exacerbated by passive stretch of the toes. Intracompartmental pressure testing is performed. Which of the following pressure readings is the most widely accepted absolute indication for a four-compartment fasciotomy?
Explanation
Question 46
A 30-year-old male presents with a closed, isolated spiral fracture of the distal third of the humeral shaft (Holstein-Lewis fracture). On examination, he is unable to extend his wrist or fingers. What is the most appropriate initial management for the nerve injury?
Explanation
Question 47
A 42-year-old female pedestrian is struck by a car. Radiographs of her knee show a split-depression fracture of the lateral tibial plateau. According to the Schatzker classification, what is the type of this fracture?
Explanation
Question 48
A 40-year-old roofer falls from a height and sustains a closed, displaced intra-articular calcaneus fracture. Surgery is planned using an extensile lateral approach. Which of the following nerves is at greatest risk of iatrogenic injury during this specific surgical approach?
Explanation
Question 49
A 50-year-old man is involved in a high-speed MVC. AP pelvis and Judet views show an acetabular fracture.
The obturator oblique view shows disruption of the iliopectineal line, and the iliac oblique view shows an intact ilioischial line. Which of the following fracture patterns is most consistent with these radiographic findings?

Explanation
Question 50
A 35-year-old female falls on an outstretched hand and presents with elbow pain and instability. Radiographs confirm an elbow dislocation, radial head fracture, and coronoid fracture. Which of the following is the most appropriate sequence of surgical reconstruction for this 'terrible triad' injury?
Explanation
Question 51
A 28-year-old male motorcyclist sustains an open midshaft tibial fracture. The wound is 12 cm long with extensive soft tissue stripping and visible muscle necrosis, but there is adequate periosteal coverage and the soft tissue can be approximated without a flap. According to the Gustilo-Anderson classification, what is the grade of this open fracture?
Explanation
Question 52
A 22-year-old man falls on an outstretched hand. He has anatomic snuffbox tenderness. Radiographs show a fracture through the proximal pole of the scaphoid. This fracture is at high risk of avascular necrosis (AVN). Which of the following best describes the primary blood supply to the scaphoid?
Explanation
Question 53
A 45-year-old male falls from a ladder and sustains a high-energy tibial pilon fracture with severe soft tissue swelling and fracture blisters. What is the most appropriate initial management?
Explanation
Question 54
A 6-year-old boy falls off monkey bars. Radiographs show a fracture of the proximal third of the ulna with an associated dislocation of the radial head. According to the Bado classification, what is the most common type of Monteggia fracture-dislocation?
Explanation
Question 55
A 72-year-old female presents with a 4-part proximal humerus fracture after a fall.
Which of the following factors most significantly increases the risk of avascular necrosis (AVN) of the humeral head in this setting?

Explanation
Question 56
A 68-year-old female with a 10-year history of alendronate use presents with sudden, atraumatic thigh pain. Radiographs reveal a transverse fracture of the lateral cortex of the subtrochanteric femur with a focal periosteal reaction ('beaking'). What is the pathophysiological mechanism behind this fracture?
Explanation
Question 57
A 25-year-old football player sustains a forced plantar flexion injury to his midfoot. He has plantar ecchymosis and pain over the tarsometatarsal joints. Weight-bearing radiographs show 3 mm of widening between the bases of the 1st and 2nd metatarsals. Which ligament is primarily injured, and what structures does it connect?
Explanation
Question 58
A 30-year-old male sustains a femoral neck fracture in a high-speed MVC. The fracture is oriented nearly vertically (Pauwels Type III, 70 degrees). Which of the following biomechanical forces predominates at the fracture site, making internal fixation challenging?
Explanation
Question 59
A 55-year-old female presents with a wrist injury after a fall. Radiographs show a fracture of the distal radius with a displaced volar articular lip and volar subluxation of the carpus. Which of the following is the most accurate diagnosis and recommended treatment?
Explanation
Question 60
A 24-year-old male cyclist falls and sustains a midshaft clavicle fracture. Which of the following is an absolute indication for immediate operative management (ORIF) of this fracture?
Explanation
Question 61
The Lower Extremity Assessment Project (LEAP) evaluated outcomes following severe lower extremity trauma resulting in a mangled limb. Which of the following statements most accurately reflects the findings of this multicenter study?
Explanation
Question 62
A 28-year-old male sustains a Hawkins Type III fracture of the talar neck. At 8 weeks post-operative follow-up, an AP radiograph of the ankle reveals a subchondral radiolucent band across the talar dome (Hawkins sign). What does this radiographic finding indicate?
Explanation
Question 63
In a polytraumatized patient presenting with a closed femoral shaft fracture, which of the following is considered an absolute indication for Damage Control Orthopedics (DCO) using external fixation rather than Early Total Care (ETC) with intramedullary nailing?
Explanation
Question 64
A 65-year-old female presents with the inability to actively flex her thumb interphalangeal joint 6 months after open reduction and internal fixation of a distal radius fracture with a volar locking plate. What is the most likely etiology of her new deficit?
Explanation
Question 65
During an extensile lateral approach for the fixation of a displaced intra-articular calcaneus fracture, the surgeon elevates a full-thickness subperiosteal flap.
To prevent wound edge necrosis, this flap relies primarily on blood supply from which of the following vessels?

Explanation
Question 66
A 30-year-old male is undergoing open reduction of a posterior wall acetabular fracture via a Kocher-Langenbeck approach. The surgeon limits splitting of the gluteus maximus and avoids dissecting more than 5 cm proximal to the greater sciatic notch. This maneuver is specifically performed to protect which of the following nerves?
Explanation
Question 67
A 22-year-old male presents with a comminuted midshaft tibia fracture and pain out of proportion to the injury. His blood pressure is 110/70 mmHg. Intracompartmental pressure measurements of the lower leg are obtained. What pressure threshold indicates the need for emergent four-compartment fasciotomies?
Explanation
Question 68
A 45-year-old male sustains an acetabular fracture after a motor vehicle collision. AP and Judet views show disruption of the iliopectineal line with an intact ilioischial line. Which of the following best describes this fracture pattern?
Explanation
Question 69
A 25-year-old polytrauma patient with bilateral femoral shaft fractures and a severe pulmonary contusion is evaluated for definitive fracture fixation versus damage control orthopedics (DCO). Which of the following physiological parameters is the most reliable indicator of adequate resuscitation for safe early total care?
Explanation
Question 70
A 30-year-old male falls from a height and sustains a Hawkins Type III talar neck fracture. Which of the following best describes the disruption of blood supply leading to the near 100% rate of avascular necrosis in this specific fracture pattern?
Explanation
Question 71
A 22-year-old male presents with a closed distal-third spiral humeral shaft fracture (Holstein-Lewis) following an arm-wrestling match. On examination, he has an absent brachioradialis reflex and inability to extend his wrist. What is the most appropriate initial management?
Explanation
Question 72
A 40-year-old farmer sustains an open tibial shaft fracture with massive soft tissue stripping and gross soil contamination after his leg is caught in a tractor. According to the updated guidelines for severe agricultural open fractures, which empiric antibiotic regimen should be initiated immediately?
Explanation
Question 73
A 28-year-old male with a closed tibial shaft fracture reports severe, unrelenting leg pain out of proportion to his injury. His blood pressure is 110/70 mmHg. Which of the following intracompartmental pressure readings is an absolute indication for emergency four-compartment fasciotomy?
Explanation
Question 74
A hemodynamically unstable 35-year-old male with an APC-III pelvic ring injury remains hypotensive (BP 70/40 mmHg) despite pelvic binder application, activation of a massive transfusion protocol, and a negative FAST exam. What is the most appropriate next step in acute management?
Explanation
None
Detailed Chapters & Topics
Dive deeper into specialized chapters regarding orthopedic-mcqs-trauma-0018
