Open Hip Dislocation: How Fascia Lata Autograft Restores Stability
Key Takeaway
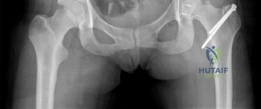
We review everything you need to understand about Open Hip Dislocation: How Fascia Lata Autograft Restores Stability. A 25-year-old female with left hip posterior femoroacetabular impingement received treatment via surgical hip dislocation. The procedure involved posterior wall rim trimming and labral reconstruction using a fascia lata autograft. This intervention successfully addressed chronic posterior hip pain and associated labral pathology stemming from a prominent posterior acetabular wall.
Introduction and Epidemiology
Hip instability encompasses a complex spectrum of pathology ranging from subtle microinstability to frank macroinstability and recurrent dislocation. Historically, the hip was considered an inherently stable enarthrodial joint, relying primarily on its deep bony architecture. However, the evolution of hip preservation surgery has elucidated the critical role of the capsuloligamentous complex in maintaining joint kinematics and stability. Iatrogenic capsular insufficiency, often secondary to un-repaired or aggressively resected capsule during hip arthroscopy, has emerged as a primary driver of postoperative instability. Furthermore, high-energy trauma, connective tissue disorders (such as Ehlers-Danlos or Marfan syndrome), and developmental dysplasia of the hip (DDH) contribute to the epidemiological burden of this condition.
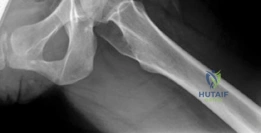
When conservative measures and arthroscopic interventions fail, or when the capsular tissue is fundamentally deficient, open surgical hip dislocation combined with capsular reconstruction becomes the definitive salvage procedure. The utilization of a fascia lata autograft to reconstruct the iliofemoral ligament and restore the anterior capsular restraint is a biomechanically sound and clinically validated technique. This procedure leverages the robust tensile properties of the iliotibial tract to recreate the primary checkrein against anterior translation and excessive external rotation. The open approach, pioneered by Ganz, allows for unparalleled 360-degree visualization of the femoral head and acetabulum while meticulously preserving the retinacular vascular supply, ensuring safe dislocation and precise anatomical graft placement.
Surgical Anatomy and Biomechanics
Osteology and Articular Geometry
The hip joint is a highly constrained ball-and-socket joint. The acetabulum is a hemispherical construct oriented in approximately 15 to 20 degrees of anteversion and 40 to 45 degrees of inclination. The femoral head is oriented in 15 degrees of anteversion relative to the femoral condyles. The inherent stability provided by the bony anatomy is augmented by the acetabular labrum, a fibrocartilaginous ring that deepens the socket by 21 percent and creates a fluid seal, enhancing the suction hydrostatic effect.
The Capsuloligamentous Complex
The capsule is reinforced by three primary ligaments. The iliofemoral ligament (Y-ligament of Bigelow) is the thickest and most robust ligament in the human body. Originating from the anterior inferior iliac spine (AIIS) and the adjacent acetabular rim, it bifurcates into a medial (descending) and lateral (transverse) arm, inserting along the intertrochanteric line. It is the primary restraint to anterior translation and external rotation in extension. The pubofemoral ligament limits abduction and external rotation, while the ischiofemoral ligament restricts internal rotation in extension.
Fascia Lata Autograft Properties
The fascia lata, specifically the iliotibial band (ITB), is an ideal autograft for capsular reconstruction. It is a dense, longitudinally oriented connective tissue structure. Biomechanical studies demonstrate that a tubularized or doubled fascia lata graft possesses an ultimate tensile load and stiffness that closely approximates or exceeds the native iliofemoral ligament. The graft acts as a static restraint, effectively neutralizing anterior shear forces and preventing the femoral head from subluxating anteriorly during the extremes of extension and external rotation.
Vascular Supply and the Ganz Principle
The fundamental principle of open surgical hip dislocation is the preservation of the medial circumflex femoral artery (MCFA). The deep branch of the MCFA courses posterior to the obturator externus and anterior to the superior gemellus, perforating the capsule at the level of the superior retinaculum to supply the femoral head. By utilizing a digastric trochanteric flip osteotomy and maintaining the integrity of the external rotators, the MCFA is protected, allowing for safe anterior dislocation of the femoral head without inducing avascular necrosis (AVN).
Indications and Contraindications
The decision to proceed with an open hip dislocation and fascia lata autograft reconstruction requires a rigorous clinical and radiographic evaluation. This is a salvage procedure reserved for profound instability where local tissue is insufficient for primary repair.
| Clinical Scenario | Operative Indications | Non Operative Indications |
|---|---|---|
| Iatrogenic Instability | Symptomatic anterior subluxation/dislocation post-arthroscopy with MRI-confirmed capsular defect. | Asymptomatic capsular defect; initial presentation amenable to physical therapy focusing on dynamic stabilizers. |
| Traumatic Dislocation | Recurrent instability despite concentric reduction; irreducible dislocation; incarcerated intra-articular fragments. | First-time traumatic dislocation with concentric closed reduction and stable examination under anesthesia. |
| Connective Tissue Disorders | Recurrent macroinstability failing extensive conservative management; debilitating pain affecting activities of daily living. | Generalized hypermobility without focal hip pain or subluxation; lack of dedicated physical therapy trial. |
| Osteoarthritis | Tönnis Grade 0 or 1 with primary instability symptoms. | Tönnis Grade 2 or 3 (Relative to Absolute Contraindication - Total Hip Arthroplasty preferred). |
| Soft Tissue Envelope | Intact abductor mechanism; adequate fascia lata tissue available for harvest. | Active local or systemic infection; severe abductor deficiency; previously harvested or compromised ipsilateral IT band. |
Absolute Contraindications
Absolute contraindications include active joint infection, advanced osteoarthritis (Tönnis Grade 3) where arthroplasty is the definitive standard of care, and severe medical comorbidities precluding major orthopedic surgery.
Relative Contraindications
Relative contraindications include moderate osteoarthritis (Tönnis Grade 2), advanced age, and active smoking, which significantly increases the risk of trochanteric osteotomy nonunion and graft failure.
Pre Operative Planning and Patient Positioning
Radiographic and Advanced Imaging
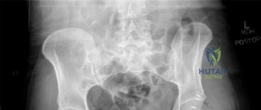
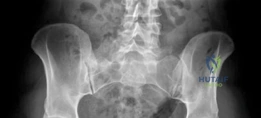
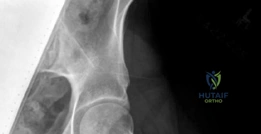
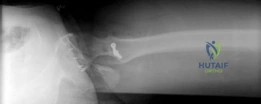
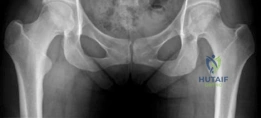
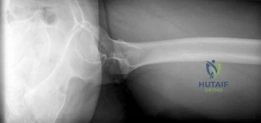
Standard preoperative imaging must include an anteroposterior (AP) pelvis, cross-table lateral, and false-profile view of the affected hip. These evaluate for dysplasia, impingement morphology (cam/pincer), and degenerative changes.
Magnetic Resonance Arthrography (MRA) is the gold standard for evaluating the capsuloligamentous complex. Extravasation of contrast anteriorly often delineates the size and location of the capsular defect. MRA also assesses labral integrity, chondral damage, and the viability of the femoral head. A 3D computed tomography (CT) scan is highly recommended to quantify femoral anteversion and acetabular version, as unrecognized osseous malorientation (e.g., severe femoral retroversion) will predispose the reconstruction to failure if not addressed concurrently with a derotational osteotomy.
Patient Positioning
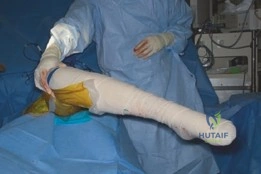
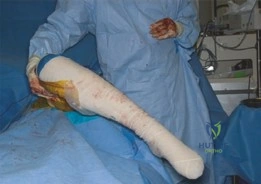
The patient is placed in the lateral decubitus position on a radiolucent Jackson table or standard operating table with a beanbag. The pelvis must be rigidly secured with anterior and posterior supports to prevent rolling during the procedure, which could disorient the surgeon's perception of version. All bony prominences are meticulously padded. The entire lower extremity is prepped and draped free to allow for full range of motion, which is critical for intraoperative assessment of stability and graft tensioning.
Equipment and Instrumentation
Standard instrumentation for a Ganz surgical dislocation is required, including an oscillating saw with a thin blade for the trochanteric osteotomy, specialized retractors (e.g., Hohmann and Cobra retractors), and a sterile femoral distractor. For the capsular reconstruction, 5.0 mm or 5.5 mm titanium or PEEK suture anchors double-loaded with high-tensile suture are utilized for the acetabular side. On the femoral side, interference screws (7.0 mm to 8.0 mm) or robust suture anchors are prepared.
Detailed Surgical Approach and Technique
The Gibson Interval and Exposure
A longitudinal incision is made centered over the greater trochanter, extending proximally towards the posterior superior iliac spine and distally along the femoral shaft. The fascia lata is incised in line with the skin incision. The Gibson interval—between the gluteus maximus (inferior gluteal nerve) and the gluteus medius (superior gluteal nerve)—is developed. The gluteus maximus is retracted posteriorly, exposing the short external rotators and the posterior border of the gluteus medius.
Trochanteric Flip Osteotomy
To preserve the MCFA, a digastric trochanteric flip osteotomy is performed. The vastus lateralis origin is identified, and a small cuff is left attached to the trochanteric fragment. An oscillating saw is used to create an osteotomy from the posterior border of the greater trochanter, exiting anteriorly just proximal to the vastus lateralis ridge. The thickness of the fragment should be approximately 1.5 cm. The osteotomized trochanter, with the attached gluteus medius and minimus, is flipped anteriorly. The underlying capsule is meticulously exposed by elevating the gluteus minimus off the superior capsule.
Capsulotomy and Joint Evaluation
A Z-shaped capsulotomy is typically performed, though in cases of severe capsular deficiency, the surgeon may encounter a massive defect with dense scar tissue. The remaining capsular edges are tagged with heavy non-absorbable sutures. The hip is dislocated anteriorly by externally rotating and flexing the leg. The ligamentum teres is sharply excised if intact. The femoral head and acetabulum are inspected for chondral defects, and any concurrent intra-articular pathology (e.g., labral tears, cam lesions) is addressed at this stage.
Fascia Lata Autograft Harvest
Attention is turned to the distal aspect of the primary incision or a separate lateral thigh incision. A rectangular strip of the iliotibial band is harvested. The dimensions depend on the defect but typically measure 4 to 5 cm in width and 10 to 12 cm in length. Care is taken to avoid violating the underlying vastus lateralis muscle belly. The graft is taken to the back table, cleared of adventitial tissue, and either tubularized using a running locking whipstitch (e.g., Krackow technique) with high-tensile suture or left as a broad patch, depending on the reconstruction strategy.
Acetabular Preparation and Fixation
The anterior acetabular rim is prepared with a burr to create a bleeding bony bed, enhancing graft incorporation. Two to three suture anchors (typically 5.0 mm) are placed along the anterior and superior acetabular rim, corresponding to the anatomical origin of the iliofemoral ligament (extending from the AIIS to the superior rim). The sutures are passed through the proximal end of the fascia lata graft and tied securely, ensuring broad contact between the graft and the decorticated bone.
Femoral Preparation and Graft Tensioning
The hip is reduced back into the acetabulum. The femoral insertion site is prepared along the intertrochanteric line. A trough or bone sockets are created depending on the fixation method (anchors vs. interference screws). The distal end of the graft is passed over the anterior femoral neck.
Crucially, the graft must be tensioned correctly. The hip is placed in 10 to 15 degrees of extension and neutral rotation. The graft is pulled distally into the femoral sockets or over the anchor footprints and secured. Over-tensioning will restrict physiological motion and lead to early joint degeneration, while under-tensioning will fail to restore stability.
Closure and Osteotomy Fixation
Once the graft is secured, the hip is taken through a dynamic range of motion to confirm stability and assess for impingement. The native remnant capsule, if present, is imbricated over the graft. The trochanteric flip osteotomy is reduced and fixed using two or three 4.5 mm fully threaded cortical screws directed medially and slightly proximally toward the lesser trochanter. The fascia lata defect from the harvest site is partially closed if possible, avoiding compartment syndrome, and the remainder of the wound is closed in layers over a suction drain.
Complications and Management
Open hip dislocation and capsular reconstruction is a technically demanding procedure with a distinct complication profile. Meticulous surgical technique is paramount to mitigate these risks.

| Complication | Incidence | Etiology and Risk Factors | Management and Salvage Strategy |
|---|---|---|---|
| Avascular Necrosis (AVN) | < 1% | Violation of the deep branch of the MCFA during approach or excessive retractor placement. | Early stage: Core decompression. Late stage with collapse: Total Hip Arthroplasty (THA). |
| Trochanteric Nonunion | 2% - 5% | Poor fixation, premature weight-bearing, smoking, overtightening of the abductors. | Revision internal fixation with bone grafting; tension band wiring if fragmented. |
| Heterotopic Ossification (HO) | 5% - 15% | Extensive muscle dissection, bone dust from osteotomy, lack of prophylaxis. | Prophylaxis with Indomethacin or single-fraction radiation. Surgical excision if symptomatic and mature. |
| Graft Failure / Recurrent Instability | 3% - 8% | Under-tensioning, unrecognized bony malversion, early aggressive rehabilitation. | Revision reconstruction, correction of underlying bony deformity (osteotomy), or THA. |
| Sciatic Nerve Neuropraxia | 1% - 3% | Excessive posterior retraction, extreme positioning, direct compression. | Usually transient. Observation, gabapentinoids, and ankle-foot orthosis (AFO) if foot drop is present. |
| Stiffness / Adhesive Capsulitis | 5% - 10% | Over-tensioning of the graft, prolonged immobilization, excessive scar formation. | Aggressive physical therapy, intra-articular corticosteroid injections, arthroscopic lysis of adhesions. |
Post Operative Rehabilitation Protocols
Rehabilitation following fascia lata autograft capsular reconstruction is a delicate balance between protecting the healing graft and preventing debilitating arthrofibrosis. The protocol must be strictly adhered to and tailored to the individual patient's tissue quality and fixation security.
Phase 1 Immediate Post Operative (Weeks 0 to 6)
The primary goal is graft protection and osteotomy healing.
* Weight Bearing: Touch-down weight bearing (TDWB) or 20 pounds flat-foot weight bearing with bilateral crutches.
* Range of Motion: Motion is restricted to prevent stress on the anterior reconstruction. Flexion is limited to 90 degrees. Extension is strictly limited to 0 degrees (no hyperextension). External rotation is limited to 0 degrees (neutral).
* Bracing: An abduction brace with an extension stop is often utilized for the first 4 weeks, particularly in non-compliant patients or those with profound preoperative instability.
* Exercises: Isometric quadriceps, hamstring, and gluteal sets. Gentle passive and active-assisted ROM within the restricted limits. No active abduction to protect the trochanteric osteotomy.
Phase 2 Intermediate Phase (Weeks 6 to 12)
The focus shifts to restoring physiological kinematics and progressing weight bearing.
* Weight Bearing: Radiographic confirmation of early trochanteric union is required before progressing. Weight bearing is advanced by 25% body weight per week until full weight bearing is achieved.
* Range of Motion: Gradual progression of extension and external rotation. The goal is to achieve full symmetrical ROM by week 12.
* Exercises: Initiate active abduction and core strengthening. Closed kinetic chain exercises (e.g., mini-squats, leg presses) are introduced. Pool therapy is highly beneficial in this phase.
Phase 3 Advanced Strengthening (Weeks 12 to 24)
- Weight Bearing: Full weight bearing without assistive devices. Normal gait mechanics must be established.
- Exercises: Progressive resistance training. Focus on abductor and external rotator endurance. Proprioceptive and balance training (e.g., BOSU ball, single-leg stance) are emphasized to restore dynamic joint stability.
Phase 4 Return to Activity (Months 6+)
- Criteria for Progression: Pain-free full ROM, abductor strength at least 90% of the contralateral side, and successful completion of functional testing.
- Exercises: Sport-specific drills, plyometrics, and agility training. Return to high-impact or contact sports is generally delayed until 9 to 12 months postoperatively and is dependent on the surgeon's discretion and the patient's functional recovery.
Summary of Key Literature and Guidelines
The literature supporting open capsular reconstruction with fascia lata autograft highlights its efficacy as a salvage procedure for the multiply operated or grossly unstable hip.
Ganz et al. established the foundation for this intervention with their landmark description of the surgical dislocation approach, proving that the hip could be safely dislocated without compromising the retinacular blood supply. This approach revolutionized the treatment of intra-articular hip pathology and provided the necessary exposure for complex reconstructions.
Subsequent biomechanical studies, notably by Myers et al. and Philippon's group, quantified the structural properties of the native capsule and various graft options. They demonstrated that the iliotibial band possesses superior ultimate failure loads compared to the native anterior capsule, making it the autograft of choice.
Clinical outcome studies have consistently shown significant improvements in patient-reported outcome measures (PROMs), such as the modified Harris Hip Score (mHHS) and the Non-Arthritic Hip Score (NAHS), following capsular reconstruction. Matsuda and other hip preservation specialists have published series demonstrating that restoring the anatomical footprint of the iliofemoral ligament effectively eliminates apprehension and recurrent subluxation in the vast majority of patients.
However, the literature also emphasizes a critical caveat: capsular reconstruction will inevitably fail if underlying bony pathomorphology is ignored. Guidelines dictate that surgeons must concurrently address severe femoral retroversion, acetabular dysplasia, or cam impingement. Failure to correct these osseous drivers of instability subjects the fascia lata graft to supraphysiological shear forces, leading to attenuation and recurrent dislocation. Therefore, comprehensive preoperative 3D imaging and a holistic approach to joint biomechanics remain the cornerstone of successful surgical management.
