Comprehensive Introduction and Patho-Epidemiology
Welcome, fellows and colleagues, to the operating theater. Today, we are undertaking a meticulous exploration of a common yet profoundly debilitating condition: hallux rigidus, or degenerative arthritis of the first metatarsophalangeal (MTP) joint. This procedure, a first MTP hemiarthroplasty utilizing a metallic proximal phalangeal prosthesis (such as the BioPro implant), remains a highly effective cornerstone in our surgical armamentarium for managing advanced cases. Our definitive goal is the restoration of pain-free, functional motion to the great toe, thereby allowing our patients to return to their demanding daily activities and athletic pursuits without the constant, limiting burden of forefoot pain and altered gait mechanics.
Hallux rigidus is a complex clinical entity that can arise from a multitude of etiologies. While primary osteoarthritis is the most frequent culprit, we must also maintain a high index of suspicion for systemic inflammatory arthritides (such as rheumatoid arthritis or gout), or less commonly, the sequelae of septic arthritis. Post-traumatic hallux rigidus is another distinct presentation, often developing insidiously after an intra-articular fracture, a severe crush injury, or a significant turf toe injury that critically compromises the ligamentous stabilizers and vascular supply of the joint. Furthermore, underlying biomechanical factors play an outsized role in the pathogenesis. A hypermobile first ray, a structurally long first metatarsal, or metatarsus primus elevatus can all contribute to repetitive dorsal impingement of the proximal phalangeal base against the metatarsal head during the terminal stance phase of gait. This repetitive microtrauma accelerates cartilage degeneration, leading to the characteristic dorsal osteophyte formation.
The progressive pathophysiology of hallux rigidus is characterized by a predictable sequence of chondral fibrillation, subchondral sclerosis, and marginal osteophytosis. As the dorsal osteophytes coalesce, they create a physical block to dorsiflexion, effectively jamming the joint and exacerbating the destruction of the remaining articular cartilage. This mechanical block not only causes localized pain but also forces the patient to supinate the foot during gait to offload the medial column, leading to secondary kinetic chain issues, including lateral metatarsalgia, midfoot arthritis, and even proximal knee or hip pathology. Understanding this cascading effect is crucial for appreciating the value of a motion-preserving procedure over a static fusion in appropriately selected candidates.
To standardize our communication and surgical planning, we rely heavily on established classification systems. The Hattrup and Johnson classification, alongside the more contemporary Coughlin and Shurnas grading system, provides a reliable framework:
* Grade I: Characterized by mild to moderate osteophyte formation with preservation of the joint space and minimal pain at the extremes of motion.
* Grade II: Demonstrates moderate joint space narrowing, significant dorsal and lateral osteophytes, and pain that occurs throughout the arc of motion, often with a noticeable decrease in dorsiflexion.
* Grade III: Represents severe joint space narrowing or complete obliteration, extensive osteophytosis, subchondral cysts, and constant pain with any degree of motion.
* Grade IV (Coughlin and Shurnas): Identical radiographic findings to Grade III, but distinguished by the presence of severe pain even at rest or during mid-arc motion, indicating near-total joint destruction.
Detailed Surgical Anatomy and Biomechanics
A profound mastery of the surgical anatomy of the first MTP joint is non-negotiable for the orthopedic surgeon. The first MTP joint is a highly complex, dynamic articulation involving the convex head of the first metatarsal, the concave base of the hallux proximal phalanx, and the critical sesamoid apparatus embedded within the plantar soft tissues.
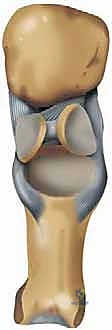
The osteology of the first ray dictates its kinematic function. The first metatarsal head is unique; its articular surface extends further dorsally than plantarly to accommodate the vast arc of dorsiflexion required during the toe-off phase of normal gait. The plantar aspect of the metatarsal head features two distinct longitudinal grooves separated by the crista, which articulate with the medial (tibial) and lateral (fibular) sesamoids. The base of the proximal phalanx, which serves as the recipient site for our hemiarthroplasty implant, must be meticulously prepared to ensure orthogonal seating of the prosthesis. The sesamoids themselves act as a fulcrum for the flexor hallucis brevis (FHB), increasing its mechanical advantage and absorbing weight-bearing forces.
The ligamentous structures of the first MTP joint provide essential static stability and must be fiercely protected during our surgical approach. The medial and lateral collateral ligaments originate from the epicondyles of the metatarsal head and fan out to insert on the base of the proximal phalanx and the margins of the plantar plate. Preservation of these ligaments during the subperiosteal dissection is paramount; iatrogenic disruption will inevitably lead to postoperative instability, varus/valgus drift, and ultimate failure of the arthroplasty. The plantar plate itself is a dense, fibrocartilaginous structure that intimately connects with the intersesamoid ligament, the metatarsosesamoid ligaments, and the phalangeosesamoid ligaments, forming a robust hammock that resists dorsal subluxation of the phalanx.
The musculotendinous units crossing the joint drive the dynamic "windlass mechanism" described by Hicks. The Flexor Hallucis Brevis (FHB) encapsulates the sesamoids within its medial and lateral heads before inserting on the plantar base of the proximal phalanx. The Flexor Hallucis Longus (FHL) courses centrally between the sesamoids to insert on the distal phalanx, providing powerful terminal plantarflexion. Dorsally, the Extensor Hallucis Longus (EHL) and Extensor Hallucis Brevis (EHB) provide dorsiflexion. The abductor hallucis and adductor hallucis provide dynamic transverse plane stability. During our bone resection of the proximal phalangeal base, we must be exquisitely careful not to resect too much bone, which would detach the FHB insertion and result in a devastating loss of push-off strength and a potential cock-up deformity.
Neurovascular risks in this region demand meticulous surgical technique. The dorsomedial cutaneous nerve, a branch of the superficial peroneal nerve, is the most critical structure encountered during the standard dorsomedial approach. It lies precariously in the subcutaneous tissues directly over the operative field. Blunt dissection and gentle, continuous retraction are required to prevent neurapraxia or complete transection, which can result in a highly symptomatic, recalcitrant neuroma. The proper plantar digital nerves are generally protected by the plantar plate during dorsal approaches, but extreme care must be taken when passing instruments plantarly around the metatarsal head.
Exhaustive Indications and Contraindications
The decision to proceed with a first MTP hemiarthroplasty requires a nuanced understanding of the patient's pathology, functional demands, and the limitations of the prosthesis. While arthrodesis remains the gold standard for end-stage hallux rigidus due to its predictability and durability, hemiarthroplasty offers the distinct advantage of motion preservation, which is highly valued by many patients, particularly those who wish to wear a variety of footwear (including modest heels) or engage in activities requiring a supple forefoot.
Indications for hemiarthroplasty are generally centered around patients with symptomatic Grade II or Grade III hallux rigidus who have failed exhaustive non-operative management. Specifically, candidates should have greater than 50% loss of the metatarsal head articular cartilage, rendering them poor candidates for an isolated cheilectomy. The ideal candidate has preserved motion at the interphalangeal (IP) joint and an intact, relatively disease-free metatarsosesamoid articulation. Hemiarthroplasty is particularly advantageous for patients who adamantly refuse arthrodesis, provided they understand the potential for future revision.
Contraindications must be strictly adhered to in order to prevent catastrophic failures. Active or recent localized infection is an absolute contraindication. Severe osteopenia or osteoporosis precludes the use of a press-fit or stemmed implant, as the bone stock will be insufficient to support the prosthesis, leading to rapid subsidence and loosening. Furthermore, severe degenerative changes within the metatarsosesamoid joint represent a significant contraindication; a proximal phalangeal hemiarthroplasty does not address plantar pain originating from sesamoid arthritis, and these patients will continue to suffer postoperatively.
Indications and Contraindications Matrix
| Parameter | Indications for Hemiarthroplasty | Contraindications for Hemiarthroplasty |
|---|---|---|
| Pathology Grade | Symptomatic Grade II or III Hallux Rigidus | Grade IV (Complete ankylosis/severe deformity) |
| Cartilage Status | >50% loss of metatarsal head cartilage | Isolated dorsal impingement (Cheilectomy preferred) |
| Sesamoid Complex | Intact, asymptomatic metatarsosesamoid joint | Severe metatarsosesamoid arthritis or ankylosis |
| Bone Quality | Adequate trabecular bone stock | Severe osteopenia, osteoporosis, or avascular necrosis |
| Patient Factors | Strong desire for motion preservation | High-impact athletes, laborers, unrealistic expectations |
| Infection Status | No history of prior joint infection | Active local or systemic infection; recent osteomyelitis |
| Prior Surgery | Failed prior cheilectomy | Prior failed arthroplasty with massive bone loss |
Prior to any surgical intervention, we must ensure that all non-operative modalities have been thoroughly exhausted. This includes footwear modifications (stiff-soled shoes, rocker bottoms, wide toe boxes), functional orthotics with Morton's extensions or carbon fiber turf-toe plates, aggressive pharmacologic management with NSAIDs, and intra-articular corticosteroid or hyaluronic acid injections. Only when these measures fail to provide acceptable quality of life should surgical intervention be entertained.
Pre-Operative Planning, Templating, and Patient Positioning
Meticulous preoperative planning is the foundation of a successful hemiarthroplasty. The clinical evaluation must differentiate between functional hallux rigidus (where pain and limitation occur only at the extremes of dorsiflexion due to impingement) and structural hallux rigidus (where the joint space is globally narrowed, and pain is present throughout the arc of motion). A positive grind test—eliciting crepitus and pain with axial loading and rotation of the phalanx—confirms advanced intra-articular degeneration.
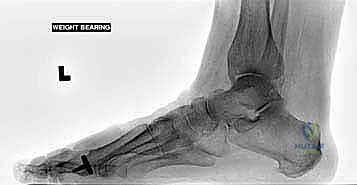
Radiographic evaluation requires high-quality, weight-bearing anteroposterior (AP), lateral, and oblique views of the foot, supplemented by axial sesamoid views. We scrutinize these images for the extent of joint space narrowing, the size and location of osteophytes, the presence of subchondral cysts, and the overall alignment of the first ray (assessing for concurrent hallux valgus or varus). The sesamoid view is critical; if the joint space between the sesamoids and the metatarsal head is obliterated, hemiarthroplasty is likely to fail in relieving plantar pain. Advanced imaging, such as MRI or fine-cut CT, is reserved for cases where avascular necrosis of the metatarsal head is suspected, or when occult sesamoid pathology cannot be definitively ruled out on plain films.
Implant selection and templating are performed using the weight-bearing AP and lateral radiographs. Our preferred implant, the BioPro cobalt chrome proximal phalangeal hemiarthroplasty, requires careful sizing. The goal is to select an implant that provides maximum cortical coverage of the resected phalangeal base without overhanging, which could impinge on adjacent soft tissues or the second toe. We template to ensure the stem length is appropriate for the medullary canal of the phalanx and that the resection depth will not compromise the FHB insertion. The operating room must be equipped not only with the full hemiarthroplasty system but also with backup equipment for arthrodesis (plates, screws, joint preparation tools) should intraoperative findings reveal inadequate bone stock or severe sesamoid disease precluding arthroplasty.
Patient positioning is straightforward but requires attention to detail. The patient is placed supine on the operating table. A well-padded thigh or calf tourniquet is applied to ensure a completely bloodless surgical field, which is absolutely essential for identifying the cutaneous nerves and performing precise bone cuts. The foot is positioned at the very edge of the bed to allow for unimpeded maneuverability of the saw and broaches. Following the administration of intravenous antibiotics, a regional anesthetic block (such as an ankle block or a popliteal sciatic nerve block) is performed to preemptively manage postoperative pain, providing a smooth transition into the recovery phase.
Step-by-Step Surgical Approach and Fixation Technique
With the tourniquet inflated and the field meticulously prepped, we commence the operative masterclass.
Surgical Approach and Initial Exposure
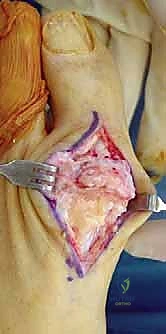
My initial incision is a longitudinal dorsomedial approach, centered directly over the first MTP joint, extending approximately 3 to 4 centimeters proximal and distal to the joint line. This specific trajectory provides unparalleled visualization of the dorsal osteophytes while minimizing the risk of adherence between the skin incision and the underlying extensor tendons. Immediately upon incising the dermis, we utilize blunt dissection techniques—using fine hemostats or a blunt periosteal elevator—to identify and mobilize the dorsomedial cutaneous nerve. This nerve is gently retracted either dorsally or plantarly, depending on its exact anatomical course, and protected throughout the entirety of the procedure.
Once the neurovascular structures are secured, we identify the Extensor Hallucis Longus (EHL) tendon. The extensor retinaculum is incised, and the EHL is retracted laterally. We then perform a robust, longitudinal capsulotomy slightly medial to the EHL tendon. It is imperative to leave a substantial, full-thickness cuff of capsular tissue on both the medial and lateral aspects. This tissue will be essential for a secure, watertight closure at the conclusion of the case, which prevents postoperative hematoma formation and provides an additional layer of static stability to the joint.
Comprehensive Cheilectomy and Joint Decompression
Using a sharp periosteal elevator, we execute a meticulous subperiosteal dissection, exposing the dorsal, medial, and lateral aspects of the metatarsal head, as well as the dorsal base of the proximal phalanx. I cannot overstate the importance of remaining strictly subperiosteal during this phase to absolutely preserve the origins and insertions of the medial and lateral collateral ligaments.


With the joint fully exposed, we begin the comprehensive cheilectomy. Using a combination of a rongeur, sharp osteotomes, and a sagittal saw, we systematically resect all marginal osteophytes. The dorsal exostosis on the metatarsal head is resected flush with the native dorsal cortex. We meticulously debride the medial and lateral gutters, ensuring no bony impingement remains. A crucial, often overlooked step is the release of the sesamoids. We pass a Freer elevator plantarly to ensure the sesamoids glide freely within their articular grooves; if they are bound by adhesions, a careful intra-articular release is performed.
Phalangeal Resection and Implantation
Attention is now turned to the base of the proximal phalanx. The joint is plantarflexed to present the articular surface. Using an oscillating microsaw, we perform a precise resection of the proximal phalangeal base. The cut must be perfectly orthogonal to the long axis of the proximal phalanx in both the sagittal and coronal planes. Typically, only 2 to 3 millimeters of bone are resected—just enough to remove the eburnated articular surface and create a flat bed for the prosthesis. Resecting too much bone is a critical error; it will detach the insertion of the Flexor Hallucis Brevis (FHB) and the plantar plate, leading to a catastrophic loss of flexor power and a highly unstable joint.
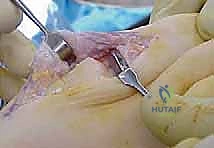
Following the resection, we utilize the specific instrumentation provided by the implant manufacturer. A starter awl is used to breach the medullary canal of the phalanx, taking care to centralize the entry point. Sequential broaching is then performed to prepare the canal for the stem of the prosthesis. The broach should achieve a snug, press-fit engagement within the diaphyseal bone.
We then insert a trial prosthesis. With the trial in place, we rigorously assess the joint. The great toe should rest in neutral alignment without varus or valgus deviation. We take the joint through a full, passive range of motion. We expect to achieve at least 70 to 80 degrees of dorsiflexion and 20 to 30 degrees of plantarflexion without impingement or subluxation. If the joint feels excessively tight, further soft tissue release or a slightly deeper bone resection may be required. Once satisfied with the trialing, the definitive cobalt chrome implant is impacted into place. A final fluoroscopic image is obtained to confirm orthogonal seating and appropriate sizing. The capsule is then repaired with heavy absorbable sutures in an interrupted fashion, followed by standard closure of the subcutaneous tissues and skin.
Complications, Incidence Rates, and Salvage Management
While first MTP hemiarthroplasty yields excellent outcomes in appropriately selected patients, it is not immune to complications. As academic surgeons, we must be intimately familiar with the potential failure modes, their incidence, and the definitive salvage pathways. The complication profile of hemiarthroplasty differs significantly from arthrodesis, primarily revolving around implant survivorship and soft tissue balancing.
Aseptic loosening and implant subsidence are the most significant long-term concerns. Subsidence typically occurs if the implant is undersized, if the patient has unrecognized osteopenia, or if the patient returns to high-impact activities prematurely. Subsidence leads to a recurrence of joint jamming, pain, and a loss of the achieved range of motion. Reactive synovitis and osteolysis secondary to wear debris (metallosis) are less common with modern cobalt chrome implants compared to historical silicone variants, but they remain a documented mode of late failure.
Soft tissue complications include persistent stiffness, which can occur if the initial cheilectomy was inadequate or if the patient fails to adhere to the postoperative mobilization protocol. Iatrogenic nerve injury to the dorsomedial cutaneous nerve results in a painful neuroma, which can be far more debilitating than the original arthritis. Infection, while rare (incidence <1-2%), is a devastating complication that necessitates immediate implant removal, aggressive debridement, and placement of an antibiotic spacer.
Complications and Management Strategies
| Complication | Estimated Incidence | Etiology/Risk Factors | Salvage / Management Strategy |
|---|---|---|---|
| Aseptic Loosening/Subsidence | 5 - 10% (Long-term) | Poor bone stock, undersized implant, high impact activity | Revision to Arthrodesis (often requiring structural bone graft) |
| Persistent Stiffness | 5 - 15% | Inadequate cheilectomy, poor rehab compliance, capsular scarring | Aggressive physical therapy, manipulation under anesthesia (rarely), arthroscopic lysis of adhesions |
| Nerve Injury / Neuroma | 2 - 5% | Retraction injury or transection of dorsomedial cutaneous nerve | Conservative (gabapentin, injections); Surgical excision and proximal burying of the nerve stump |
| Deep Infection | < 2% | Immunocompromise, poor wound healing, hematogenous spread | Explantation, aggressive I&D, IV antibiotics, delayed arthrodesis |
| Transfer Metatarsalgia | 3 - 8% | Altered gait mechanics, shortening of the 1st ray | Orthotic management, metatarsal pads; rarely requires Weil osteotomies of lesser rays |
When a hemiarthroplasty definitively fails, the gold standard salvage procedure is conversion to a first MTP arthrodesis. This is technically demanding due to the bone void created by the implant stem and the initial phalangeal resection. After explantation and meticulous debridement of any metallosis or fibrous tissue, the joint surfaces must be prepared down to bleeding subchondral bone. Because of the bone loss, structural interpositional bone grafting (using autograft from the iliac crest or calcaneus, or robust allograft) is almost universally required to restore the length of the first ray and maintain the functional biomechanics of the forefoot. Fixation is typically achieved with a robust dorsal plate and interfragmentary screw construct.
Phased Post-Operative Rehabilitation Protocols
The success of a motion-preserving procedure like a hemiarthroplasty is inextricably linked to the quality of the postoperative rehabilitation. Unlike an arthrodesis, where immobilization is the goal, hemiarthroplasty requires a delicate balance between protecting the surgical wound and initiating early motion to prevent capsular contracture.
Phase I: Immediate Post-Operative (Days 0-14)
The primary goals in the first two weeks are wound healing, edema control, and pain management. The patient is placed in a rigid postoperative shoe or a controlled ankle motion (CAM) boot. Weight-bearing is restricted to heel-touch or flat-foot weight-bearing only; active push-off through the hallux is strictly prohibited to protect the capsular repair and allow the bone-implant interface to stabilize. The patient is instructed to keep the foot elevated above heart level for the majority of the day to mitigate swelling.
Phase II: Early Mobilization and ROM (Weeks 2-6)
At the two-week mark, sutures are removed provided the incision is fully healed. This phase marks the critical initiation of joint mobilization. Patients transition to a supportive, stiff-soled athletic shoe. We begin aggressive, active and passive range of motion exercises for the first MTP joint. Patients are instructed to manually grasp the great toe and perform controlled dorsiflexion and plantarflexion stretches multiple times a day. Physical therapy is often formally initiated here, utilizing modalities such as soft tissue massage to prevent adherence of the extensor tendons to the surgical scar, and joint mobilizations to maximize the capsular excursion.
Phase III: Strengthening and Return to Function (Weeks 6-12)
By six weeks, the capsular tissues have achieved significant tensile strength, and the implant should be stable. The focus shifts to restoring the dynamic strength of the flexor and extensor mechanisms. Resistance band exercises are incorporated to strengthen the FHB and EHL. Gait training is paramount; patients are coached to actively engage the windlass mechanism and push off through the great toe, correcting the supinated, antalgic gait pattern they likely developed preoperatively.
Phase IV: Long-Term Maintenance (Months 3+)
Patients can gradually return to higher-impact activities and varied footwear as tolerated. It is crucial to counsel patients that maximum medical improvement—where swelling completely subsides and maximum ROM is achieved—can take up to 6 to 12 months. We recommend the continued use of supportive footwear and custom orthotics for heavy physical exertion to protect the longevity of the prosthesis.
Summary of Landmark Literature and Clinical Guidelines
The literature surrounding first MTP hemiarthroplasty is extensive and provides a robust evidence base for its continued use in modern orthopedic practice. The conceptual foundation was laid by Townley and Taranow, who popularized the metallic hemiarthroplasty as a durable alternative to the earlier, highly problematic silicone implants that were plagued by catastrophic fragmentation and severe foreign-body giant-cell reactions (silicone synovitis).
Long-term outcome studies specifically evaluating the BioPro cobalt chrome implant have demonstrated highly favorable survivorship and patient satisfaction. A landmark retrospective review with over a decade of follow-up showed that over 85% of patients maintained excellent pain relief and functional range of motion, with a radiographic survivorship exceeding 90%. These studies consistently highlight that while radiographic lucencies may occasionally appear around the stem, they do not always correlate with clinical failure or the need for revision, provided the implant remains stable and the patient is asymptomatic.
The debate between hemiarthroplasty and arthrodesis for advanced hallux rigidus remains a prominent topic in foot and ankle literature. Prospective randomized controlled trials (RCTs) comparing the two modalities generally show that both provide excellent pain relief. Arthrodesis reliably scores higher in terms of absolute predictability and lower revision rates over a 15-year horizon. However, hemiarthroplasty consistently outperforms arthrodesis in patient-reported outcome measures (PROMs) related to footwear flexibility and the ability to perform specific tasks requiring forefoot dorsiflexion (e.g., kneeling, lunging).
Current clinical guidelines from major orthopedic societies suggest that while arthrodesis is the definitive treatment for Grade III and IV hallux rigidus, modern metallic hemiarthroplasty is a highly validated, evidence-based alternative for the active patient with Grade II or III disease who possesses adequate bone stock and places a premium on joint motion. Future directions in the field are focused on advanced biomaterials, such as pyrocarbon implants, and kinematically designed prostheses that aim to more perfectly replicate the complex, multi-axial center of rotation of the native first MTP joint.
Detailed Chapters & Topics
Dive deeper into specialized chapters regarding first-metatarsophalangeal-joint-hemiarthroplasty
