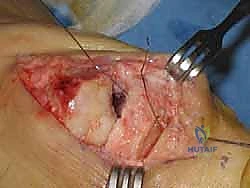
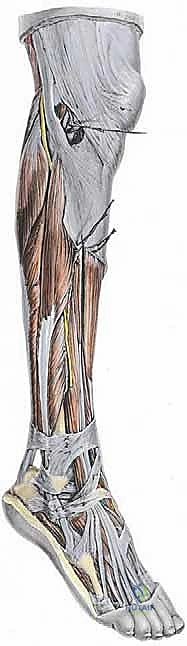
Forearm Osteotomy and Exostosis Excision for Multiple Hereditary Exostoses: An Intraoperative Masterclass
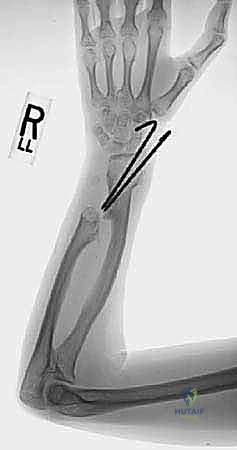
Key Takeaway
This masterclass guides orthopaedic fellows through forearm osteotomy and exostosis excision for Multiple Hereditary Exostoses (MHE). We cover detailed anatomy, meticulous surgical steps from incision to hardware, and critical pearls for managing complex deformities and preventing complications. Master the techniques for improved function and alignment in affected patients.
Introduction and Epidemiology
Multiple hereditary exostoses (MHE), initially documented by Boyer in 1814, is a complex familial skeletal dysplasia characterized by an autosomal dominant mode of inheritance. The condition exhibits exceptionally high penetrance (approximately 96%) and variable expressivity. Also referred to in the literature as multiple osteochondromatosis, diaphyseal aclasis, or metaphyseal aclasis, MHE presents profound reconstructive challenges in pediatric orthopedic surgery due to multi-planar deformities and asynchronous physeal growth.
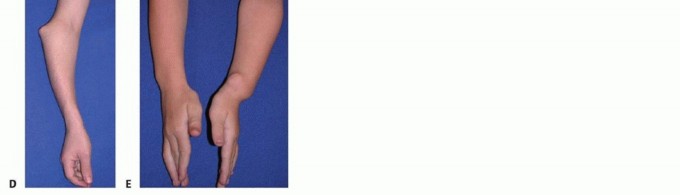
The primary genetic pathophysiology involves loss-of-function mutations in the tumor suppressor genes EXT-1 (chromosome 8q24) and EXT-2 (chromosome 11p11-12). These genes encode glycosyltransferases essential for the biosynthesis of heparan sulfate. A deficiency in heparan sulfate disrupts the Indian Hedgehog (IHH) and parathyroid hormone-related protein (PTHrP) signaling pathways at the physis, leading to premature chondrocyte hypertrophy and aberrant peripheral physeal growth. Approximately 10% to 20% of MHE cases represent de novo spontaneous mutations with no prior family history. The general population prevalence is estimated to be 1 in 50,000. Diagnosis typically occurs between 2 and 3 years of age, as exostoses rarely ossify sufficiently to be palpable or radiographically evident before age two. By age 12, penetrance is virtually complete.
Osteochondromas arise from the peripheral aspect of the growth plate (the perichondrial ring of Ranvier) in bones undergoing endochondral ossification. They consist of a bony stalk—whose medullary cavity is distinctly continuous with that of the host bone—covered by a hyaline cartilage cap.
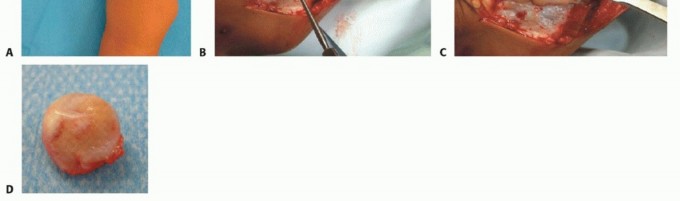
As longitudinal growth proceeds, these lesions migrate diaphyseally away from the physis. The aberrant proliferation of chondroblasts and subsequent defective metaphyseal remodeling yield the two hallmark clinical features of MHE: skeletal metaphyseal exostoses and significant retardation of longitudinal bone growth. Upon reaching skeletal maturity and physeal closure, osteochondromas typically become quiescent. Any subsequent enlargement, new onset of pain, or increasing cartilage cap thickness (typically >1.5 cm in adults on MRI) mandates immediate oncologic workup to exclude malignant transformation to secondary peripheral chondrosarcoma, a complication occurring in 1% to 5% of the MHE population.
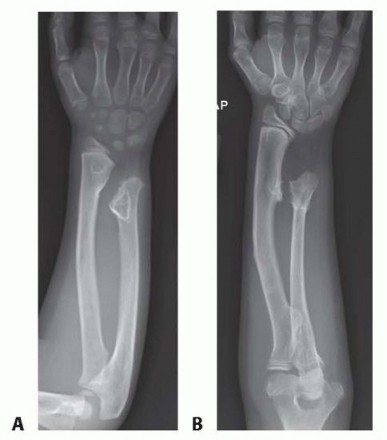
Forearm deformity is a prominent and debilitating manifestation, occurring in 30% to 60% of MHE patients. The paired-bone anatomy of the forearm makes it uniquely susceptible to asynchronous longitudinal growth. Because 80% of ulnar longitudinal growth occurs at the distal physis—which is disproportionately affected by osteochondromata—the ulna frequently becomes tethered and shortened. This relative ulnar shortening forces the continuously growing radius to bow (typically convex dorsoradially), increases ulnar variance, alters the radial articular angle, and invariably leads to progressive radial head subluxation or frank dislocation.
Surgical Anatomy and Biomechanics
A rigorous understanding of the normal kinematics and biomechanics of the pediatric forearm is an absolute prerequisite for conceptualizing the pathogenesis of MHE deformities and executing complex reconstructive osteotomies.
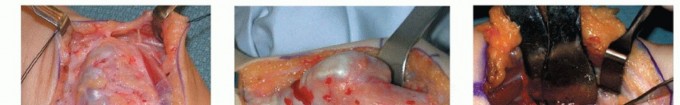
The forearm functions mechanically as a complex, dynamic joint. Pronation and supination require near-anatomic alignment of the radius and ulna, coupled with the uncompromised integrity of the proximal radioulnar joint (PRUJ), distal radioulnar joint (DRUJ), and the intervening interosseous membrane (IOM). The mechanical axis of forearm rotation is oblique, extending from the center of the radial head proximally to the fovea of the ulnar head distally. The ulna acts as a stable, relatively fixed swivel hinge around which the radius rotates. Even minor multi-planar axial deformities, asymmetric shortening, or ligamentous contractures can severely restrict this rotational arc.
The Interosseous Membrane and Tethering Effect
The interosseous membrane is a robust ligamentous complex, primarily comprising the central band, accessory bands, and the distal oblique bundle. Its primary biomechanical role is the transmission of axial loads from the radius to the ulna, while also providing critical longitudinal and transverse stability to the PRUJ and DRUJ. In the context of MHE, an osteochondroma arising from the distal ulna exerts a profound tethering effect.
Because the radius and ulna are tightly bound by the IOM, the retardation of ulnar growth directly dictates radial morphology. As the radius continues its longitudinal growth against the unyielding, shortened ulna, it is subjected to compressive forces that induce bowing. This bowing fundamentally alters the functional axis of rotation, creating a mechanical block to pronation and supination. Furthermore, the relative overgrowth of the radius drives the carpus into ulnar deviation, pathologically increasing the radial articular angle. Proximally, the continued longitudinal thrust of the radius against a fixed ulnar length exerts superiorly directed sheer forces on the radiocapitellar joint. This chronic stress attenuates the annular ligament, ultimately precipitating radial head subluxation and subsequent dislocation.
Radiocarpal and Radioulnar Kinematics
In a physiologically normal wrist, approximately 80% of the axial load is transmitted through the radiocarpal articulation and 20% through the ulnocarpal articulation via the triangular fibrocartilage complex (TFCC). In MHE, severe negative ulnar variance radically disrupts this load distribution. The radius assumes nearly 100% of the axial load, leading to altered carpal kinematics, adaptive carpal instability (carpal slip), and a high propensity for long-term degenerative osteoarthritis. Restoring the relative lengths of the radius and ulna is therefore paramount to reestablishing normal load transmission across the radiocarpal and ulnocarpal axes.
Indications and Contraindications
Surgical intervention for MHE forearm deformities is dictated by the magnitude of the deformity, the trajectory of progression, the degree of functional impairment, and the status of the radiocapitellar joint. The Masada classification remains the universally accepted framework for categorizing these deformities and establishing a surgical algorithm.
Masada Classification System
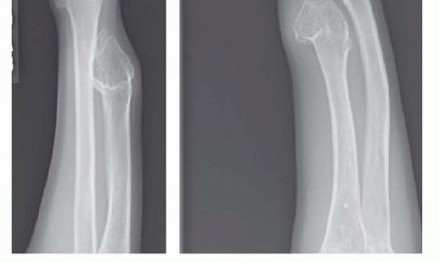
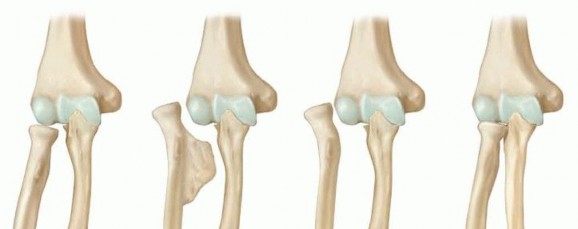
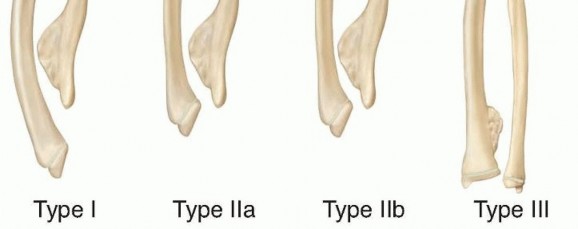
- Type I: The most common variant. Characterized by an osteochondroma of the distal ulna causing primary ulnar shortening and secondary radial bowing. The radial head remains anatomically located.
- Type IIa: Characterized by ulnar shortening with radial head dislocation. The primary osteochondroma is located at the proximal radius, directly impinging on the PRUJ.
- Type IIb: Characterized by ulnar shortening with radial head dislocation. The primary osteochondroma is located at the distal ulna, causing severe tethering and proximal failure (dislocation).
- Type III: Characterized by an osteochondroma of the distal radius causing relative radial shortening and positive ulnar variance (less common).
Patient Selection Criteria
Operative management is generally indicated for progressive deformity, significant loss of forearm rotation (typically <50 degrees of pronation/supination), intractable pain, and impending or frank radial head subluxation/dislocation. The timing of intervention remains a subject of academic debate. Early excision of distal ulnar lesions is advocated by some to decompress the tethering effect and prevent irreversible radial head dislocation. However, definitive reconstructive osteotomies are often delayed until the patient is closer to skeletal maturity to mitigate the high risk of recurrence inherent in the growing skeleton.
| Parameter | Operative Indications | Non Operative Indications |
|---|---|---|
| Pain | Persistent, mechanically reproducible pain | Asymptomatic |
| Range of Motion | Progressive, functionally limiting loss of pronation/supination | Maintained functional arc of motion |
| Radial Head | Subluxation or dislocation (Masada Type II) | Stable, radiographically well-located radial head |
| Ulnar Variance | Severe negative variance with ulnar carpal shift | Mild variance, stable and aligned carpus |
| Aesthetics | Severe clinical deformity causing psychosocial distress | Mild bowing, acceptable clinical appearance |
| Skeletal Maturity | Rapidly progressive deformity in an immature patient | Skeletally mature with non-progressive, mild deformity |
Contraindications to complex reconstructive osteotomies include asymptomatic patients with stable, congruent joints, active osteomyelitis or soft tissue infection, and a compromised soft tissue envelope that would preclude safe distraction osteogenesis or rigid internal fixation.
Pre Operative Planning and Patient Positioning
Meticulous preoperative planning is the cornerstone of successful forearm reconstruction in MHE. The surgical strategy must be highly individualized, with overriding goals including complete excision of offending osteochondromas, precise restoration of ulnar length, correction of radial diaphyseal bowing, and concentric reduction of the radiocapitellar joint.
Clinical and Radiographic Evaluation
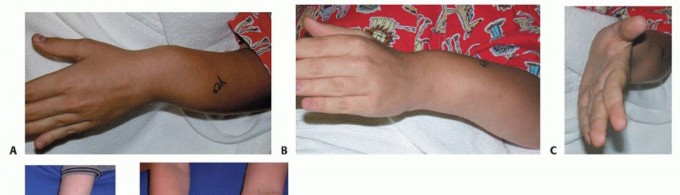
A comprehensive clinical evaluation must document the precise arc of pronation and supination, wrist flexion/extension, and elbow range of motion. A highly detailed neurovascular examination is critical; massive proximal radius osteochondromas frequently cause mass effect and compression neuropathies of the posterior interosseous nerve (PIN).
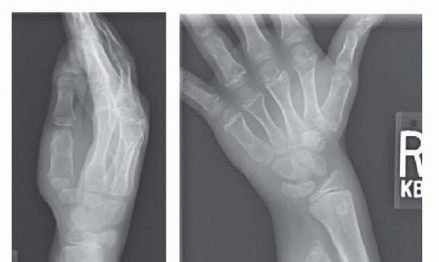
Standard orthogonal radiographs (true AP and lateral) of the wrist, forearm, and elbow are mandatory. Bilateral imaging is strongly recommended to establish the patient's baseline anatomy, acknowledging that MHE is typically a bilateral, albeit asymmetric, disease. Critical radiographic parameters to quantify include:
* Ulnar Variance: Measured as the distance between the distal articular surface of the ulna and the lunate fossa of the radius.
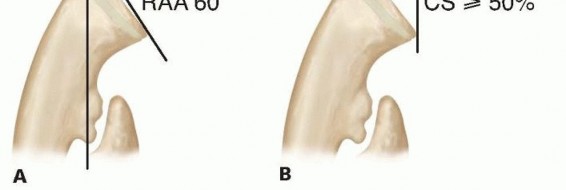
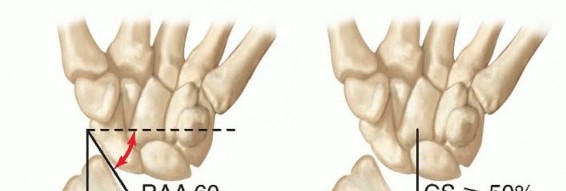
* Radial Articular Angle (RAA): The normal RAA is typically 15 to 30 degrees. In MHE, this angle pathologically increases due to distal ulnar tethering and relative radial overgrowth.
* Maximum Radial Bowing: The magnitude and exact diaphyseal apex of the radial bow must be calculated to dictate the site of a potential corrective radial osteotomy.
Advanced cross-sectional imaging (MRI or CT) is reserved for specific indications. MRI is invaluable when an osteochondroma exhibits rapid growth, pain, or atypical features, allowing precise measurement of the cartilaginous cap to rule out malignant transformation. 3D CT reconstructions are highly beneficial for mapping the exact spatial relationship of a dislocated radial head to the capitellum and planning multi-planar corrective osteotomies.
Surgical Templating
Preoperative templating dictates the choice between acute lengthening and distraction osteogenesis for the ulna. If the ulnar discrepancy is less than 1.5 to 2.0 cm, acute lengthening utilizing an interpositional structural bone graft (iliac crest autograft or structural allograft) and rigid plate fixation is generally feasible. For discrepancies exceeding 2.0 cm, gradual lengthening via distraction osteogenesis utilizing a unilateral or circular external fixator is the gold standard. This gradual approach mitigates excessive tension on the neurovascular bundles and the soft tissue envelope.
Patient Positioning
The patient is positioned supine on the operating table with the affected extremity extended onto a radiolucent hand table. A well-padded pneumatic tourniquet is applied high on the brachium. The C-arm fluoroscopy unit is positioned either parallel or perpendicular to the hand table, ensuring unhindered, dynamic access for true AP and lateral imaging of the entire forearm axis, from the distal humerus to the carpus.
Detailed Surgical Approach and Technique
The surgical management of MHE forearm deformities frequently necessitates a multi-stage, multi-level procedure performed under a single anesthetic event. The logical sequence of reconstruction typically proceeds as follows: osteochondroma excision, ulnar osteotomy and lengthening, radial corrective osteotomy (if indicated), and radial head reduction.
Excision of Osteochondromas
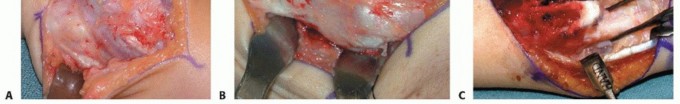
The initial surgical phase requires the meticulous, extra-periosteal excision of the osteochondromas that are mechanically tethering growth or creating a physical block to rotation.
For distal ulnar lesions, a longitudinal incision is centered over the subcutaneous border of the distal ulna. The internervous plane between the extensor carpi ulnaris (ECU) and flexor carpi ulnaris (FCU) is developed. The periosteum overlying the osteochondroma is incised and sharply elevated. It is imperative to excise the lesion flush with the normal cortical contour of the host diaphysis or metaphysis. The entire cartilaginous cap, including the perichondrial ring, must be radically excised to minimize the risk of local recurrence. Meticulous care is required to identify and protect the dorsal sensory branch of the ulnar nerve during this distal dissection.
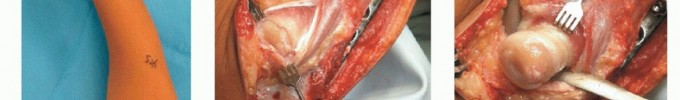
For proximal radial lesions, a modified volar Henry or dorsal Thompson approach is utilized, dictated by the precise anatomical location of the exostosis. The Thompson approach exploits the internervous plane between the extensor carpi radialis brevis (ECRB, radial nerve proper) and the extensor digitorum communis (EDC, posterior interosseous nerve). Identification, neurolysis, and protection of the PIN represent the most critical and hazardous steps of this approach. The supinator muscle is carefully elevated off the proximal radius to expose the base of the exostosis.
Ulnar Lengthening Osteotomy
Following the excision of the distal ulnar exostosis, attention is directed to the ulnar lengthening procedure.
Distraction Osteogenesis Technique:
If gradual lengthening is indicated, a unilateral external fixator is utilized. Hydroxyapatite-coated half-pins are inserted into the proximal and distal ulnar segments under strict fluoroscopic guidance. Proximal pins are placed carefully to avoid the ulnar nerve, which courses posterior to the medial epicondyle. Distal pins must be placed to avoid violating the DRUJ and to protect the dorsal sensory branch of the ulnar nerve.
Once the pins are secured to the external fixator rail, a diaphyseal or metaphyseal osteotomy is executed. A subperiosteal exposure is achieved, and the osteotomy is performed utilizing a multiple drill-hole technique followed by completion with a sharp osteotome. Alternatively, a low-speed oscillating saw with copious chilled saline irrigation may be used to prevent thermal necrosis of the bone ends. The fixator is then tested for stability and unimpeded distraction.
Acute Lengthening Technique:
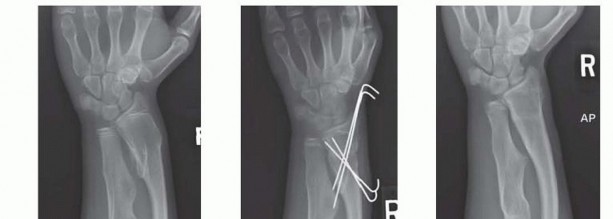
For acute lengthening, the osteotomy is performed in a biologically respectful manner. A lamina spreader is utilized to distract the osteotomy site until the templated ulnar variance is achieved (aiming for neutral or slightly negative variance). A pre-contoured dynamic compression plate or locking compression plate (LCP) is applied. A structural tricortical iliac crest bone graft is precisely fashioned to fit the defect and secured with the plate to provide immediate structural continuity.
Radial Corrective Osteotomy
In patients presenting with severe radial bowing (typically >20 degrees) that mechanically precludes normal pronation-supination or prevents the indirect reduction of a dislocated radial head, a formal corrective radial osteotomy is mandated.
Through a volar Henry approach (utilizing the internervous plane between the brachioradialis and flexor carpi radialis), the apex of the radial diaphyseal deformity is exposed. A closing wedge or opening wedge osteotomy is executed based on preoperative templating. A closing wedge osteotomy is inherently more stable and provides excellent bone-to-bone contact, but results in slight radial shortening—a factor that must be mathematically accounted for during the ulnar lengthening phase. The osteotomy is rigidly stabilized with a volar locking plate.
Radial Head Reduction
In Masada Type II deformities, the radial head is subluxated or frankly dislocated. Frequently, the act of restoring ulnar length and correcting radial bowing will result in the spontaneous, indirect reduction of the radial head, mediated by the tethering effect of the intact interosseous membrane pulling the radius proximally and ulnarly.
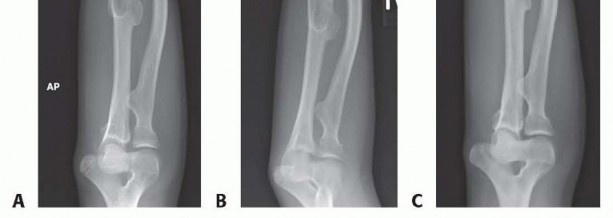
If the radial head remains stubbornly dislocated following ulnar and radial osteotomies, an open reduction is required. This is achieved via a lateral approach to the elbow (the Kocher interval, between the anconeus and ECU). The radiocapitellar joint is meticulously cleared of fibrotic tissue and the interposed joint capsule, allowing the radial head to be concentrically reduced. If the annular ligament is found to be incompetent or absent, a formal reconstruction (such as the Bell-Tawse procedure utilizing a slip of the triceps tendon or a palmaris longus autograft) may be necessary to confer dynamic stability.
Complications and Management
Surgical reconstruction of the forearm in the setting of MHE is fraught with potential complications. These arise from the severely altered local anatomy, the necessity of multi-level surgical intervention, and the inherent reliance on regenerate bone healing in distraction osteogenesis or the incorporation of massive structural grafts.
Pin tract infections represent the most frequent complication associated with distraction osteogenesis. Delayed union or nonunion of the ulnar osteotomy site (the docking site) can occur, particularly if the distraction rate exceeds the biological capacity of the regenerate (typically >1 mm/day) or if the periosteal sleeve is excessively stripped during the initial surgical exposure.
Iatrogenic nerve injuries pose a significant risk. The posterior interosseous nerve (PIN) is highly vulnerable during the excision of proximal radial osteochondromas and during proximal radial osteotomies. The dorsal sensory branches of the ulnar and radial nerves are at risk during distal half-pin placement and distal surgical approaches.
Recurrence of deformity is a well-documented and frustrating complication, especially when surgical intervention is undertaken in very young children with substantial remaining physeal growth potential. The cartilaginous cap must be completely and radically excised to prevent local recurrence of the primary osteochondroma.
| Complication | Estimated Incidence | Prevention and Salvage Strategies |
|---|---|---|
| Pin Tract Infection | 20% - 40% | Prevention: Meticulous pin site care, low-tension skin incisions, pre-drilling. Salvage: Oral antibiotics, aggressive local wound care; rarely requires premature pin removal. |
| Delayed Union / Nonunion | 10% - 15% | Prevention: Preserve the periosteal sleeve, maintain optimal distraction rate (1 mm/day). Salvage: Halt distraction, compress the non-union site ("accordion technique"); secondary bone grafting and internal fixation if persistent. |
| Nerve Injury (PIN / Sensory) | 2% - 5% | Prevention: Careful internervous dissection, avoid excessive or prolonged retraction. Salvage: Most are neuropraxias that resolve spontaneously; formal microsurgical exploration is mandated if complete transection is suspected. |
| Recurrence of Deformity | 15% - 30% | Prevention: Complete marginal excision of the cartilage cap; delay definitive osteotomies until near skeletal maturity if clinically feasible. Salvage: Revision osteotomy and repeat lengthening if the patient becomes symptomatic. |
| Loss of Forearm Rotation | 10% - 20% | Prevention: Rigid fixation, early mobilization, accurate restoration of the radial bow and RAA. Salvage: Intensive physical therapy; hardware removal if plates are impinging on the PRUJ or DRUJ. |
Post Operative Rehabilitation Protocols
The postoperative rehabilitation protocol must be rigorously tailored to the specific type of surgical intervention performed (acute lengthening with internal fixation versus gradual distraction osteogenesis).
Distraction Osteogenesis Protocol
If a unilateral external fixator is utilized, the latency phase commences immediately postoperatively and is maintained for 5 to 7 days to allow for initial fracture hematoma organization and early soft callus formation. Following latency, the distraction phase is initiated at a standard rate of 1 mm per day, optimally divided into four 0.25 mm increments to provide continuous, low-tension histogenesis.
During the distraction phase, aggressive, supervised physical therapy is mandatory. Active and active-assisted range of motion exercises for the elbow, wrist, and digits are instituted daily to prevent debilitating joint contractures. The patient and family are extensively educated on meticulous pin site care protocols utilizing chlorhexidine or sterile saline solutions.
Once the templated ulnar length is achieved, the consolidation phase begins. The external fixator is locked and remains in place as a static neutralization device. Serial orthogonal radiographs are obtained every 3 to 4 weeks to assess the maturation of the regenerate bone. The fixator is removed only when robust, circumferential corticalization of the regenerate bone is radiographically confirmed on at least three out of four cortices. The consolidation phase typically requires twice the duration of the distraction phase.
Acute Lengthening and Internal Fixation Protocol
For patients undergoing acute lengthening with rigid plate fixation and structural bone grafting, the forearm is immobilized in a well-padded, long-arm bulky dressing or bivalved cast for the initial 10 to 14 days to allow for acute soft tissue healing and edema subsidence.
At the first postoperative clinic visit, sutures are removed, and the patient is transitioned to a custom-molded, removable Munster splint or a long-arm cast. Gentle active range of motion of the elbow and wrist is initiated. Pronation and supination are advanced cautiously to avoid imparting excessive rotational torque on the plate and structural graft construct. Progressive resistance and strengthening exercises are strictly delayed until definitive radiographic evidence of graft incorporation and osteotomy union is observed, typically occurring between 8 to 12 weeks postoperatively. Return to full unrestricted activities, heavy lifting, or contact sports may require 6 months or longer, contingent upon complete radiographic healing.
Summary of Key Literature and Guidelines
The surgical management of forearm deformities in MHE has evolved significantly, heavily guided by several landmark academic studies. The classification system proposed by Masada et al. in 1989 remains the foundational cornerstone for categorizing these deformities and establishing operative indications. Their seminal work highlighted the direct biomechanical correlation between distal ulnar osteochondromas, subsequent ulnar shortening, and the eventual proximal failure resulting in radial head dislocation.
Waters et al. extensively evaluated the long-term outcomes of ulnar lengthening and early excision
You Might Also Like