Capsular Interposition Arthroplasty for Hallux Rigidus: An Operative Masterclass
Key Takeaway
Welcome, fellows, to an immersive operative masterclass on capsular interposition arthroplasty for hallux rigidus. We'll meticulously navigate the first MTP joint, from precise incision and anatomical dissection to meticulous tissue balancing and hardware application. This procedure aims to restore pain-free motion in end-stage arthritis, emphasizing crucial neurovascular protection and optimal long-term function. Prepare for a granular, real-time walkthrough, addressing every critical step and potential pitfall.
Introduction and Epidemiology
Hallux rigidus refers to progressive degenerative osteoarthritis of the first metatarsophalangeal joint. This condition is characterized by insidious onset of pain, progressively decreased range of motion, and the formation of prominent periarticular osteophytes, particularly along the dorsal aspect of the metatarsal head. As the most common arthritic condition of the foot, hallux rigidus affects approximately 1 in 45 individuals over the age of 50, with a slight predilection for female patients.
The pathogenesis of progressive first metatarsophalangeal joint cartilage degeneration remains multifactorial and, in many cases, idiopathic. Most orthopedic literature attributes hallux rigidus to biomechanical disturbances or local anatomic pathology that leads to repetitive microtrauma, shear stress on the articular cartilage, and subsequent deterioration of the chondral surface. Recognized etiologies include prior intra-articular trauma, osteochondritis dissecans, and inflammatory arthritides such as rheumatoid arthritis or crystalline arthropathy.

Primary osteoarthritis is frequently associated with specific anatomic variants. Factors such as a structurally long first metatarsal, a flattened metatarsal head, metatarsus primus elevatus, generalized pes planovalgus, or hallux valgus interphalangeus are often identified in patients presenting with end-stage arthritis of the first metatarsophalangeal joint. A long first metatarsal, in particular, alters the kinematics of the first ray during the terminal stance phase of gait, correlating strongly with the development of hallux rigidus due to increased compressive forces across the joint.
Initially, the natural history of hallux rigidus involves pain localized to the dorsal aspect of the great toe metatarsophalangeal joint. Loss of motion in the early stages is minimal but becomes clinically apparent during activities requiring maximum dorsiflexion, such as running or ascending stairs. Over several years, the degree of joint involvement and the loss of sagittal plane motion increase significantly. In the end stage of the disease process, the first metatarsophalangeal joint will lose nearly all functional motion. Unlike hallux valgus, a significant varus or valgus deformity is usually not associated with primary hallux rigidus.

Paradoxically, pain may stabilize or even decrease as massive osteophytes form to auto-fuse and stabilize the joint. However, the progression of osteophytes and joint space narrowing observed on weight-bearing radiographs does not always correlate linearly with the severity of patient symptoms.
Surgical Anatomy and Biomechanics
Osteology and Articular Geometry
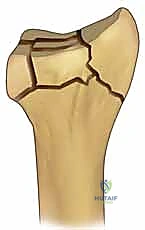
The first metatarsophalangeal joint is a highly complex diarthrodial joint composed of the first metatarsal head and the proximal articulating base of the proximal phalanx. The metatarsal head is inherently asymmetric, featuring a larger radius of curvature dorsally than plantarly, which creates a cam effect during sagittal plane motion. Pathology in hallux rigidus is limited primarily to this joint, with the hallmark lesion being a prominent dorsal osteophyte on the metatarsal head that physically blocks the proximal phalanx from gliding dorsally.

Soft Tissue Restraints and the Sesamoid Complex
The joint is encapsulated by the dorsal joint capsule, which is often thickened and contracted in hallux rigidus. Medial and lateral collateral ligaments provide coronal and transverse plane stability. Plantarly, the joint is supported by the highly specialized plantar plate-sesamoid-flexor hallucis brevis tendon complex. The medial (tibial) and lateral (fibular) sesamoids are embedded within the tendons of the flexor hallucis brevis and articulate with the plantar facets of the first metatarsal head. The sesamoids function to increase the mechanical advantage of the intrinsic flexors and protect the flexor hallucis longus tendon, which glides between them.

Biomechanics of the First Ray
Normal gait requires approximately 65 to 75 degrees of dorsiflexion at the first metatarsophalangeal joint during the terminal stance and pre-swing phases. This motion is inextricably linked to the windlass mechanism described by Hicks. As the hallux dorsiflexes, the plantar fascia is wound around the first metatarsal head, elevating the medial longitudinal arch, plantarflexing the first metatarsal, and locking the midtarsal joints to create a rigid lever for propulsion.

In hallux rigidus, the dorsal osteophyte and contracted capsule restrict this critical dorsiflexion. Consequently, the windlass mechanism is disrupted. Patients frequently adopt an avoidance gait, transferring weight laterally to the lesser metatarsals, which can result in transfer metatarsalgia, lateral column overload, and secondary pathologies such as plantar fasciitis or Achilles tendinopathy.
Indications and Contraindications
Surgical management of hallux rigidus is dictated by the severity of the disease, typically graded using the Coughlin and Shurnas clinical-radiographic classification system. While arthrodesis remains the gold standard for end-stage (Grade 3 and 4) hallux rigidus due to its predictable pain relief and durability, capsular interpositional arthroplasty serves as a critical motion-preserving alternative.
Capsular interpositional arthroplasty is primarily indicated for active patients with Grade 3 or early Grade 4 hallux rigidus who explicitly desire preservation of joint motion and refuse arthrodesis. It is particularly useful in patients who wish to continue wearing shoes with a slight heel or participate in activities that require sagittal plane flexibility, such as yoga or certain martial arts.

Contraindications to capsular interpositional arthroplasty include severe inflammatory arthropathy (e.g., advanced rheumatoid arthritis), active infection, profound osteopenia or avascular necrosis of the metatarsal head, and significant concurrent sesamoid arthritis. If the plantar plate and sesamoid complex are rigidly fused to the metatarsal head, motion preservation will fail, and arthrodesis is mandated.
Summary of Operative and Non Operative Indications
| Disease Stage (Coughlin and Shurnas) | Clinical and Radiographic Findings | Non Operative Management | Operative Management Options |
|---|---|---|---|
| Grade 1 | Mild pain at extremes of ROM; mild dorsal osteophyte; normal joint space. | Stiff-soled shoes, NSAIDs, intra-articular corticosteroid injection. | Cheilectomy. |
| Grade 2 | Moderate pain; restricted ROM; dorsal osteophyte; mild to moderate joint space narrowing. | Carbon fiber inserts, Morton's extension, activity modification. | Cheilectomy, Moberg osteotomy. |
| Grade 3 | Constant pain; significant stiffness; severe joint space narrowing; extensive periarticular osteophytes. | Rocker-bottom shoes, custom orthoses, chronic pain management. | Capsular Interpositional Arthroplasty, Arthrodesis. |
| Grade 4 | Pain throughout entire ROM; complete loss of joint space; loose bodies; sesamoid arthritis. | Rigid orthoses, accommodative footwear. | Arthrodesis (Gold Standard), Resection Arthroplasty (Keller). |
Pre Operative Planning and Patient Positioning
Clinical Evaluation
A meticulous history and physical examination are paramount. The typical history includes insidious swelling around the first metatarsophalangeal joint. Patients frequently complain of a progressive increase in the physical size of the joint, often erroneously attributing this to a bunion deformity.
Physical examination should begin with gait analysis to identify an antalgic or lateral-loading avoidance gait. Inspection will reveal a prominent, tender dorsal osteophyte. Upon palpation, the dorsal cutaneous nerve may exhibit Tinel's sign due to mechanical irritation over the exostosis.

Range of motion testing typically demonstrates limited dorsiflexion with a hard, mechanical block due to the abutment of the proximal phalanx articular surface against the metatarsal head osteophyte. Compensatory hyperextension of the hallucal interphalangeal joint is frequently observed in long-standing disease as the body attempts to recreate toe-off mechanics.
The axial compression test (grind test) is crucial; stabilizing the first metatarsal while compressing and rotating the proximal phalanx against the metatarsal head will elicit pain proportional to the degree of central cartilage degradation. Additionally, the Thomassen sign should be evaluated: with the ankle held in neutral, dorsiflexion of the metatarsophalangeal joint is measured. A positive result (decreased motion compared to resting plantarflexion) is suggestive of a stenosing flexor hallucis longus tenosynovitis, which must be addressed intraoperatively.
Radiographic Evaluation
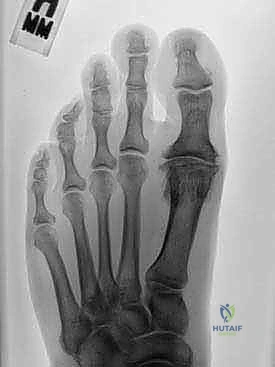
Standard weight-bearing radiographs of the foot are mandatory. The anteroposterior view evaluates joint space narrowing, subchondral sclerosis, and the presence of lateral osteophytes or loose bodies. The lateral view is critical for assessing the size of the dorsal osteophyte and the degree of metatarsus primus elevatus. An axial sesamoid view must be obtained to evaluate the articulation between the sesamoids and the plantar metatarsal head; severe sesamoid arthritis is a relative contraindication to motion-preserving surgery.

Patient Positioning and Anesthesia
The procedure is typically performed under regional anesthesia (popliteal or ankle block) combined with monitored anesthesia care or general anesthesia. The patient is positioned supine on the operating table. A small bump is placed under the ipsilateral hip to internally rotate the leg to a neutral position, bringing the first ray pointing directly toward the ceiling. A well-padded thigh or calf tourniquet is applied to ensure a bloodless surgical field, which is critical for identifying and preserving the delicate dorsal capsular structures required for the interpositional flap.
Detailed Surgical Approach and Technique
Incision and Superficial Dissection
A dorsal longitudinal incision is made centered over the first metatarsophalangeal joint, extending from the mid-shaft of the first metatarsal to the mid-shaft of the proximal phalanx. The incision is carried through the skin and subcutaneous tissues. Meticulous hemostasis is maintained.

During the superficial dissection, the dorsomedial cutaneous nerve (a branch of the superficial peroneal nerve) and the extensor hallucis longus tendon must be identified and protected. The extensor hallucis longus tendon is typically retracted laterally, while the extensor hallucis brevis tendon can be retracted laterally or utilized later if an extensor brevis interposition is planned.
Capsular Exposure and Cheilectomy
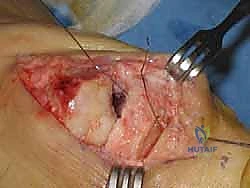
The dorsal capsule is exposed. In a standard capsular interpositional arthroplasty, a U-shaped capsulotomy is performed, with the base of the flap left attached to the base of the proximal phalanx. This dorsal capsular flap is carefully elevated and reflected distally, exposing the degenerative joint.

The joint is inspected, and a comprehensive cheilectomy is performed. Using an oscillating saw or sharp osteotome, the dorsal 25% to 30% of the metatarsal head is resected. The cut should begin just dorsal to the remaining viable articular cartilage and angle proximally to remove the entire dorsal exostosis, creating a smooth dorsal contour. Medial and lateral periarticular osteophytes are resected using a rongeur and smoothed with a rasp.
Joint Debridement and Soft Tissue Release
Following the cheilectomy, the joint is distracted. The central articular surface of the metatarsal head is typically devoid of cartilage. Any loose bodies are removed. A critical step in restoring motion is the release of the plantar plate and sesamoid complex. A McGlamry elevator or Freer elevator is passed plantarly to free the sesamoids from any fibrous adhesions to the plantar aspect of the metatarsal head. If the flexor hallucis longus is tethered, a fractional lengthening or tenolysis may be performed.

At this stage, the joint should dorsiflex to at least 70 degrees passively. If motion remains restricted, further bony resection or plantar release is required.
Flap Preparation and Interposition
The success of the capsular interpositional arthroplasty relies on the interposition of viable tissue to prevent bone-on-bone articulation. If the local dorsal capsule is robust, the proximally based U-shaped flap is utilized. Alternatively, as described by Hamilton, the extensor hallucis brevis tendon can be transected proximally, left attached distally, and woven into the joint space. In cases of severe capsular deficiency, allograft tissues (such as acellular dermal matrix) or autografts (gracilis tendon) may be utilized.

The chosen interpositional tissue is advanced into the joint space, covering the denuded articular surface of the metatarsal head.
Fixation of the Interpositional Flap
The flap must be securely anchored plantarly to prevent dorsal migration during range of motion. This is accomplished using either transosseous bone tunnels or suture anchors.
If using bone tunnels, two small drill holes are made from the dorsal aspect of the metatarsal neck exiting plantarly near the articular margin. Sutures attached to the distal end of the capsular flap are passed through these tunnels and tied dorsally over a bone bridge.

Alternatively, small biocomposite suture anchors can be placed at the plantar-articular junction of the metatarsal head. The sutures are passed through the leading edge of the interpositional flap and tied, effectively resurfacing the metatarsal head with the soft tissue flap.
Final Assessment and Closure
Once the flap is secured, the joint is taken through a full range of motion to ensure the interpositional tissue remains stable and does not impinge. The extensor hallucis longus tendon is allowed to return to its anatomic position. The extensor retinaculum and superficial tissues are closed in layers using absorbable suture. The skin is closed with non-absorbable monofilament or subcuticular absorbable sutures. A compressive, bulky soft dressing is applied to control postoperative edema.
Complications and Management
While capsular interpositional arthroplasty can provide excellent pain relief and motion preservation, it is technically demanding and carries a distinct complication profile. The most common cause of failure is the progression of degenerative joint disease or insufficient initial bony resection, leading to recurrent pain and stiffness.

Transfer metatarsalgia is a recognized complication, particularly if excessive bone is resected from the metatarsal head, effectively shortening the first ray and transferring ground reaction forces to the lesser metatarsals. Conversely, failure to adequately release the plantar plate can lead to persistent stiffness and recurrent dorsal impingement.
Summary of Common Complications and Salvage Strategies
| Complication | Estimated Incidence | Etiology | Salvage and Management Strategy |
|---|---|---|---|
| Recurrent Pain / Progression of OA | 10% - 15% | Ongoing cartilage wear; failure of the interpositional flap; inadequate initial cheilectomy. | Conversion to first MTP joint arthrodesis. Usually requires structural bone graft if prior resection was extensive. |
| Transfer Metatarsalgia | 5% - 10% | Shortening of the first ray due to excessive metatarsal head resection; elevation of the first metatarsal. | Conservative: Custom orthotics with metatarsal pads. Operative: Weil osteotomies of lesser metatarsals or first MTP arthrodesis. |
| Joint Stiffness | 5% - 12% | Inadequate release of the plantar plate/sesamoid complex; poor postoperative rehabilitation compliance. | Aggressive physical therapy, dynamic splinting. Rarely requires secondary surgical release. |
| Nerve Injury (Neuritis) | 2% - 5% | Iatrogenic injury or traction to the dorsomedial cutaneous nerve during exposure. | Desensitization therapy, gabapentinoids. Surgical exploration and nerve burying if a symptomatic neuroma forms. |
| Flap Necrosis / Infection | < 2% | Ischemia of the capsular flap; standard surgical site infection risks. | Oral or IV antibiotics. Debridement. If joint is destroyed, staged arthrodesis. |
Post Operative Rehabilitation Protocols
The postoperative rehabilitation protocol following capsular interpositional arthroplasty must balance the need for soft tissue healing of the anchored flap with the absolute necessity of early motion to prevent capsular scarring and joint stiffness.
Phase 1: Tissue Healing (Weeks 0 to 2)
The patient is placed in a rigid postoperative shoe or controlled ankle motion (CAM) boot. Weight-bearing is restricted to heel-touch or strict non-weight-bearing based on the surgeon's assessment of flap fixation security. The bulky compressive dressing remains intact until the first postoperative visit. Elevation and strict edema control are emphasized.
Phase 2: Early Motion (Weeks 2 to 6)
At the two-week mark, sutures are removed. The patient is transitioned to weight-bearing as tolerated in a stiff-soled surgical shoe. The critical component of this phase is the initiation of aggressive, passive, and active-assisted range of motion exercises. Patients are instructed to manually distract the proximal phalanx and perform plantarflexion and dorsiflexion exercises multiple times daily. Failure to initiate motion in this window invariably leads to a stiff, painful joint.















You Might Also Like