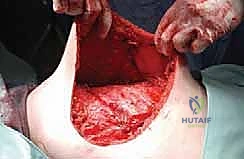
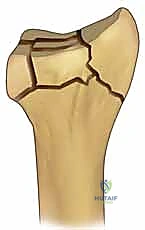
Moberg Osteotomy & Cheilectomy: A Masterclass in Hallux Rigidus Correction
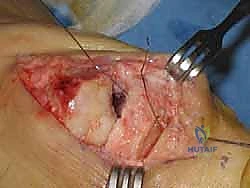
Key Takeaway
This masterclass provides an exhaustive, immersive guide to the Moberg osteotomy and concomitant cheilectomy for hallux rigidus. As your scrubbed-in instructor, we'll navigate comprehensive surgical anatomy, meticulous preoperative planning, and granular intraoperative execution. Learn critical pearls, pitfalls, and strategies for complication management, ensuring optimal outcomes for patients suffering from this debilitating condition. Master the art of restoring MTP joint function.
Introduction and Epidemiology
Hallux rigidus represents a progressive, degenerative osteoarthritis of the first metatarsophalangeal joint. The condition is characterized by a significant functional limitation of motion, predominantly restricting dorsiflexion. Historically referred to by various nomenclature including hallux limitus and dorsal bunion, hallux rigidus is the most common osteoarthritic condition of the foot. Epidemiological data indicates that hallux rigidus affects approximately three percent of the adult population, with a higher prevalence observed in females compared to males. The condition frequently presents bilaterally, though symptom severity may be asymmetric.
The primary surgical intervention discussed herein is the dorsal closing wedge osteotomy of the proximal phalanx, initially popularized by Erik Moberg. Originally described for adolescent patients with hallux rigidus, Moberg subsequently expanded the indications to include adult patients experiencing functional limitations due to restricted dorsiflexion. In contemporary orthopedic practice, the Moberg osteotomy is rarely performed in isolation; it is almost universally executed in conjunction with a dorsal cheilectomy. The fundamental objective of the Moberg osteotomy is not to increase the total arc of motion of the first metatarsophalangeal joint, but rather to translate the existing arc of motion dorsally, thereby restoring functional dorsiflexion required for normal gait kinematics.

Pathogenesis and Natural History
The primary etiology of idiopathic hallux rigidus remains incompletely understood, though it is widely considered multifactorial. A well-documented causative factor is localized trauma, with hallux rigidus frequently developing sequelae to fractures, severe sprains, or crush injuries affecting the first ray. Furthermore, repetitive microtrauma is hypothesized to induce cumulative injury to the articular cartilage over time, precipitating a cascade of degenerative changes. Systemic inflammatory arthropathies, including rheumatoid arthritis and crystalline arthropathies such as gout, can also precipitate degeneration of the first metatarsophalangeal joint, clinically mimicking the idiopathic variant.
The natural history of hallux rigidus demonstrates a higher incidence in adults compared to adolescents. While generalized degenerative changes radiographically progress with advancing age, the correlation between radiographic severity and clinical symptomatology is often non-linear. Patients typically describe an insidious onset of activity-related pain, localized swelling, and progressive stiffness. Limitation of dorsiflexion directly impairs the terminal stance phase of gait, leading to profound difficulties with running, ascending inclines, and utilizing footwear with elevated heels.

Surgical Anatomy and Biomechanics
A comprehensive understanding of the osseous and soft tissue anatomy of the first metatarsophalangeal joint is requisite for successful execution of the Moberg osteotomy. The articulation involves the convex articular surface of the first metatarsal head and the concave base of the proximal phalanx, augmented plantarly by the sesamoid complex and the plantar plate.
Osteology and Articular Wear Patterns
In the setting of hallux rigidus, dorsiflexion is mechanically obstructed by the formation of a prominent dorsal osteophyte on the first metatarsal head. Concurrently, a corresponding osteophyte or ossicle frequently develops on the dorsal aspect of the proximal phalanx base. The articular cartilage erosion exhibits a highly characteristic topographic pattern. Chondral denudation is predominantly observed on the dorsal aspect of the articular surface of the first metatarsal head and, to a lesser degree, on the dorsal base of the proximal phalanx.
Crucially, the medial and plantar aspects of the metatarsophalangeal joint, including the sesamoid articulation, are typically spared until the end stages of the disease process. This specific wear pattern provides the anatomical rationale for joint-sparing procedures such as the cheilectomy and Moberg osteotomy, which rely on the preservation of the viable plantar cartilage for weight-bearing articulation.

Biomechanical Alterations in Hallux Rigidus
Normal gait requires approximately 65 to 75 degrees of dorsiflexion at the first metatarsophalangeal joint to engage the windlass mechanism and allow for efficient toe-off. In hallux rigidus, the dorsal osteophyte creates a mechanical block, while concomitant contracture of the plantar capsule further tethers the joint.
When a patient attempts to dorsiflex the hallux against this mechanical block, painful impingement occurs. To compensate for this restricted motion, patients often adopt adaptive gait strategies, such as walking with a supinated forefoot to unload the medial column. This compensatory mechanism frequently results in transfer metatarsalgia, lateral foot pain, and the development of adventitial calluses under the lesser metatarsal heads. Rarely, compensatory hyperextension of the interphalangeal joint may develop.
The Moberg osteotomy alters the biomechanics of the hallux by resecting a dorsal wedge of bone from the proximal phalanx. By closing this wedge, the distal aspect of the phalanx is elevated. This structural modification effectively shifts the functional arc of motion dorsally. While the absolute total degrees of motion remain unchanged, the arc is repositioned into a more functional range, allowing the hallux to clear the ground during the swing phase and accommodate the terminal stance phase of gait without impinging the dorsal articular surfaces.

Indications and Contraindications
The selection of appropriate surgical candidates is the most critical determinant of success for the Moberg osteotomy. The procedure is indicated for patients with symptomatic hallux rigidus who have failed exhaustive conservative management and possess specific clinical and radiographic characteristics. The Coughlin and Shurnas classification system is universally utilized to grade the severity of hallux rigidus and guide surgical decision-making.
The Moberg osteotomy, combined with cheilectomy, is primarily indicated for Grade 1 and Grade 2 hallux rigidus. In highly selected cases of Grade 3 disease, where the plantar half of the metatarsal head cartilage remains pristine and the primary complaint is a lack of dorsiflexion rather than mid-range pain, a Moberg osteotomy may be considered. It is strictly contraindicated in Grade 4 disease, which is characterized by complete joint space obliteration, severe pain throughout the entire arc of motion, and advanced sesamoid arthritis.

Operative and Non Operative Management Parameters
| Management Strategy | Indications and Clinical Scenarios | Modalities and Techniques |
|---|---|---|
| Non-Operative | Initial presentation, Grade 1-3 hallux rigidus, poor surgical candidates, mild symptomatology. | Rigid Morton extension orthotics, carbon fiber shoe inserts, rocker-bottom footwear modifications, NSAIDs, intra-articular corticosteroid injections. |
| Operative Joint Sparing | Grade 1 and 2, select Grade 3. Pain primarily at terminal dorsiflexion. Intact plantar cartilage. Failed conservative care. | Cheilectomy alone (older patients with impingement), Cheilectomy with Moberg Osteotomy (active patients requiring functional dorsiflexion shift). |
| Operative Joint Sacrificing | Grade 3 with mid-range pain, Grade 4 hallux rigidus, inflammatory arthropathies, severe sesamoid arthritis, salvage of failed prior surgery. | First MTP Arthrodesis (Gold Standard), Interpositional Arthroplasty, Total Joint Arthroplasty (select older, lower-demand patients). |

Pre Operative Planning and Patient Positioning
Thorough preoperative planning relies on high-quality, weight-bearing radiographic evaluation. Standard imaging protocols must include weight-bearing anteroposterior, lateral, and lateral oblique views of the foot. An axial sesamoid view is highly recommended to evaluate the articular integrity of the metatarsosesamoid articulation.
On the lateral radiograph, the surgeon must quantify the size of the dorsal metatarsal osteophyte and assess the joint space. The AP radiograph is utilized to evaluate for any concomitant hallux valgus deformity, as a Moberg osteotomy does not address transverse plane pathology. If significant hallux valgus is present, alternative or additional osteotomies must be planned.

Anesthesia and Positioning Protocols
The procedure is typically performed in an outpatient ambulatory surgery setting. Regional anesthesia, specifically an ankle block or popliteal sciatic nerve block, combined with monitored anesthesia care or general anesthesia, provides excellent intraoperative conditions and postoperative analgesia.
The patient is positioned supine on the operating table. A small bump may be placed under the ipsilateral hip to internally rotate the lower extremity, bringing the first ray into a neutral, directly vertical position facing the surgeon. A well-padded pneumatic tourniquet is applied to either the proximal calf or the ankle, depending on surgeon preference and the patient's vascular status. The lower extremity is prepped and draped in standard sterile fashion. Intraoperative fluoroscopy should be available to confirm the osteotomy trajectory and hardware placement.

Detailed Surgical Approach and Technique
The execution of the Moberg osteotomy requires meticulous soft tissue handling and precise osseous resection to prevent complications such as intra-articular fracture or nonunion.
Surgical Incision and Soft Tissue Dissection
A standard dorsal or dorsomedial longitudinal incision is utilized, extending from the mid-shaft of the first metatarsal to the interphalangeal joint of the hallux. Subcutaneous dissection is performed carefully to identify and protect the dorsal medial cutaneous nerve branches.
The extensor hallucis longus tendon is identified within its sheath. The tendon may be mobilized and retracted either medially or laterally, depending on the exposure required. A longitudinal capsulotomy is performed in line with the skin incision. Subperiosteal dissection is utilized to expose the dorsal aspect of the first metatarsal head and the dorsal base of the proximal phalanx.

Execution of the Cheilectomy
Before addressing the proximal phalanx, the metatarsal head must be prepared. The dorsal osteophyte is identified. Using a microsagittal saw or a sharp osteotome, the dorsal one-third of the metatarsal head is resected. The resection plane should begin just dorsal to the intact plantar articular cartilage and angle proximally to lie flush with the dorsal metatarsal shaft.
Following the primary resection, rongeurs and a rasp are utilized to smooth the medial and lateral borders of the metatarsal head, removing any overhanging osteophytes that could contribute to capsular impingement. The joint is thoroughly irrigated, and any loose bodies are excised. The joint is then taken through a range of motion to assess the improvement in dorsiflexion. If dorsiflexion remains inadequate despite an aggressive cheilectomy, the Moberg osteotomy is initiated.

The Moberg Osteotomy Proximal Phalanx Resection
Exposure is shifted distally to the proximal phalanx. The periosteum over the dorsal aspect of the proximal phalanx is elevated. The osteotomy site is planned approximately one to two millimeters distal to the articular surface of the proximal phalanx base.
Using a microsagittal saw, the proximal cut is made parallel to the articular surface. The cut is directed from dorsal to plantar, stopping short of the plantar cortex. It is imperative to leave the plantar cortex intact to serve as a stabilizing hinge.
The distal cut is then made, starting two to four millimeters distal to the first cut on the dorsal cortex, angling proximally to intersect the first cut at the plantar cortex. This creates a dorsal-based wedge. The size of the dorsal wedge dictates the degree of elevation; typically, a two to three millimeter wedge is sufficient.

Osteotomy Reduction and Hardware Fixation
Once the wedge of bone is carefully removed using a small curette or Freer elevator, the osteotomy is closed by applying a dorsiflexion force to the distal phalanx. The intact plantar hinge should bend, allowing the dorsal cortices to appose flushly.
Fixation of the osteotomy can be achieved through various modalities based on surgeon preference. Common techniques include:
* Two crossed 0.045-inch or 0.062-inch Kirschner wires.
* A dorsal titanium staple.
* A single or double low-profile titanium screw (e.g., 2.0 mm or 2.4 mm) placed from dorsal-distal to plantar-proximal.
* Heavy non-absorbable transosseous sutures.
Following rigid fixation, the joint is again taken through a range of motion. The surgeon should note a clinically significant increase in resting dorsiflexion and an improved functional arc. Intraoperative fluoroscopy is utilized to confirm the hardware position, ensure the osteotomy is fully closed, and verify that no hardware penetrates the articular surface.

Capsular Management and Wound Closure
The surgical site is copiously irrigated. The capsule is closed over the joint using an absorbable suture. It is critical not to over-tighten the dorsal capsule, as this could negate the dorsiflexion gained from the procedure. The extensor hallucis longus tendon is allowed to fall back into its anatomic position. The subcutaneous tissues are closed, followed by skin closure utilizing non-absorbable sutures or staples. A bulky, compressive sterile dressing is applied to control postoperative edema.

Complications and Management
While the Moberg osteotomy is generally highly successful when indicated correctly, complications can arise from technical errors or progression of the underlying degenerative disease. Careful surgical technique and appropriate patient selection mitigate these risks.
The most specific complication related to the Moberg osteotomy is the creation of a "cock-up" toe deformity. This occurs when an excessively large dorsal wedge is resected, resulting in over-elevation of the distal phalanx. This leads to shoe wear impingement dorsally and a failure of the hallux to purchase the ground during the stance phase of gait.

Common Surgical Complications and Salvage Strategies
| Complication | Estimated Incidence | Etiology and Clinical Presentation | Salvage and Management Strategies |
|---|---|---|---|
| Recurrent Stiffness / Undercorrection | 10% - 15% | Inadequate cheilectomy, insufficient wedge size, aggressive capsular closure, poor postoperative rehab. | Aggressive physical therapy, intra-articular injections. Revision surgery or conversion to arthrodesis. |
| Cock-Up Toe Deformity (Overcorrection) | < 5% | Resection of a wedge larger than 4mm, complete fracture of the plantar hinge leading to dorsal translation. | Conservative: shoe modification. Operative: revision osteotomy with plantarflexion structural grafting or arthrodesis. |
| Progression of Osteoarthritis | 20% - 30% (Long term) | Natural history of the degenerative joint disease. Pain shifts from terminal dorsiflexion to mid-arc motion. | Conversion to first MTP joint arthrodesis. |
| Hardware Prominence / Irritation | 5% - 10% | Prominent K-wires or staple bridges causing dorsal skin irritation and shoe impingement. | Hardware removal once radiographic union is confirmed (typically after 3-4 months). |
| Nonunion / Delayed Union | < 2% | Thermal necrosis from saw, poor fixation construct, patient non-compliance, smoking. | Prolonged immobilization, bone stimulator. Revision with bone grafting and rigid internal fixation. |

Post Operative Rehabilitation Protocols
The postoperative rehabilitation protocol is designed to protect the osteotomy site while encouraging early motion to prevent capsular scarring and joint stiffness.
During Phase 1 (Weeks 0 to 2), the patient is placed in a rigid, hard-soled postoperative shoe or a controlled ankle motion boot. Weight-bearing is permitted strictly through the heel and lateral border of the foot to avoid loading the first ray. The initial bulky dressing remains intact until the first postoperative visit. Elevating the extremity is heavily emphasized to minimize edema and promote wound healing.

During Phase 2 (Weeks 2 to 6), sutures are removed. Radiographs are obtained to confirm maintenance of osteotomy reduction. The patient is transitioned to a supportive athletic shoe as swelling permits. Active and passive range of motion exercises for the first metatarsophalangeal joint are initiated immediately. Physical therapy is often prescribed to focus on plantarflexion stretching and active dorsiflexion strengthening. The patient is instructed to perform manual distraction and dorsal/plantar glides to prevent capsular adhesions.
During Phase 3 (Weeks 6 and beyond), radiographic union is typically evident. The patient is cleared to gradually resume normal activities, including high-impact exercises and running, as tolerated by pain and swelling. Continued daily range of motion exercises are encouraged for up to six months postoperatively to maximize the functional outcome.
Summary of Key Literature and Guidelines
The academic foundation for the Moberg osteotomy is rooted in its biomechanical rationale. Moberg's original 1979 publication highlighted that while the osteotomy does not reverse arthritic changes, it fundamentally alters the kinematics of the joint to favor the dorsiflexion required for ambulation.
Subsequent literature has consistently demonstrated that combining a dorsal closing wedge osteotomy with a cheilectomy yields superior functional scores in active patients compared to cheilectomy alone. Studies by Thomas and Smith, as well as Citibati et al., have shown high patient satisfaction rates (frequently exceeding 85%) when applied strictly to Grade 1 and Grade 2 hallux rigidus.
Academic consensus dictates that surgeons must explicitly counsel patients that the Moberg osteotomy is a joint-sparing, but not joint-curing, procedure. The underlying degenerative process may continue, and patients must be aware that conversion to a first metatarsophalangeal joint arthrodesis may be required in the future if mid-arc pain develops due to progressive articular cartilage loss. Nonetheless, as an intermediate intervention, the Moberg osteotomy remains a highly effective, biomechanically sound procedure for restoring functional gait in the symptomatic hallux rigidus patient.

Clinical & Radiographic Imaging

















You Might Also Like