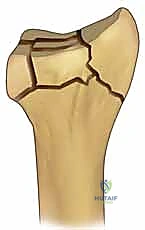
Flexor Hallucis Longus Tendon Transfer for Chronic Peroneal Tendon Tears: An Intraoperative Masterclass
Key Takeaway
This masterclass guides fellows through FHL transfer for chronic peroneal tendon tears. We cover patient selection, meticulous surgical anatomy, precise intraoperative steps including Hunter rod placement and FHL harvest, and the Pulvertaft weave. Critical pearls, complication avoidance, and structured postoperative rehabilitation are emphasized for optimal patient outcomes in complex cases.
Welcome, fellows, to the operating theater. Today, we're tackling a challenging, yet incredibly rewarding procedure: the reconstruction of chronic peroneal tendon tears using a Flexor Hallucis Longus (FHL) tendon transfer. This isn't a simple primary repair; we're dealing with advanced pathology, often in active, middle-aged individuals who've endured significant pain and instability, frequently after failed previous interventions. Our goal is to provide dynamic stabilization to the ankle and restore the critical eversion function of the peroneal tendons, which is often severely compromised.
Understanding the Pathology and Patient Profile
These patients typically present with chronic lateral ankle pain, tenderness, swelling, and a profound sense of lateral ankle instability. Manual muscle testing often reveals considerable weakness and pain with inversion and eversion compared to the contralateral limb. They are often active individuals who refuse to wear a brace full-time or accept a hindfoot fusion, making a reconstructive procedure essential for their quality of life.
The underlying pathology is usually not an isolated acute tear, but rather chronic fissuring, longitudinal splitting, and degeneration of both the peroneus brevis and longus tendons. Histologic evaluation often shows chronic wear with cystic and myxoid degeneration. This advanced state means direct repair is often not viable, necessitating a tendon transfer. Our specific technique involves inserting the FHL into the residual stump of the peroneus brevis tendon, effectively sacrificing the distal peroneus longus portion which is often too scarred to serve as a viable insertion point.
Differential Diagnosis
Before we even consider surgery, we must rule out other causes of chronic lateral ankle pain:
* Fibular fracture or stress fracture
* Lateral process fracture of the talus
* Syndesmosis or subtalar sprains
* Ankle instability involving the anterior talofibular or calcaneofibular ligaments
* Impingement lesions
* Osteochondral lesions of the talus
* Tarsal coalition
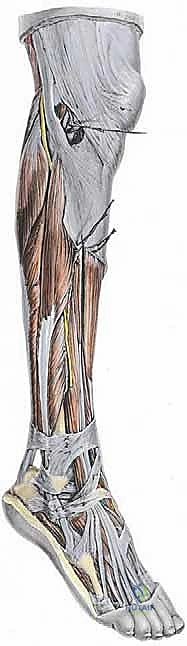
Comprehensive Surgical Anatomy
A thorough understanding of the anatomy is paramount for success and complication avoidance.
Peroneal Tendons and Retinacula
The peroneus brevis and longus tendons descend posterior to the lateral malleolus.
* The peroneus brevis is typically closer to the lateral malleolus, originating from the distal two-thirds of the lateral fibula and inserting onto the base of the fifth metatarsal.
* The peroneus longus lies directly posterior to the brevis, originating from the proximal two-thirds of the lateral fibula and inserting into the medial cuneiform and base of the first metatarsal.
* Both tendons are tethered at the level of the lateral malleolus by the superior peroneal retinaculum (SPR), a strong band of deep fascia extending from the tip of the lateral malleolus to the calcaneus. Distally, the inferior peroneal retinaculum provides further stability.
* The most common location for longitudinal peroneus brevis tears is within the fibular groove, where it can be mechanically impinged.

Neurovascular Structures in the Lateral Ankle
- Sural Nerve: This sensory nerve is a critical structure to protect. It runs subcutaneously, typically posterior to the peroneal tendons, and provides sensation to the lateral aspect of the foot and ankle. It's particularly vulnerable in the distal aspect of our lateral incision. Preoperative assessment for pre-existing sural nerve damage from prior surgeries is crucial.
- Superficial Peroneal Nerve: While less directly exposed in this approach, its branches can be at risk with overly aggressive retraction or incisions extending too anteriorly.
Flexor Hallucis Longus (FHL) Tendon
The FHL is our chosen motor for transfer due to its excellent strength (3.6% of total ankle strength, compared to the peroneus brevis's 2.6%) and its in-phase muscle activity, making it a synergistic choice.
* Origin: Posterior fibula, interosseous membrane, and posterior intermuscular septum.
* Course: It descends through the deep posterior compartment, passing posterior to the talus, through a groove on the posterior aspect of the sustentaculum tali, and then courses obliquely across the plantar aspect of the foot to insert into the base of the distal phalanx of the great toe.
* Neurovascular Supply: The FHL is innervated by the tibial nerve (a branch of the sciatic nerve) and supplied by the posterior tibial artery. These structures lie in close proximity in the deep posterior compartment and must be protected during FHL harvest.
Osteology and Alignment
We must assess the alignment of the entire lower extremity, including the hip, knee, tibia, ankle, hindfoot, and forefoot. A fixed hindfoot varus deformity, if present, may need to be corrected concurrently, as it can predispose to peroneal pathology and lead to failure of the transfer.
Preoperative Planning and Patient Positioning
Preoperative planning is not merely a formality; it's a blueprint for success.
Imaging Review
- Weight-bearing ankle and foot radiographs: Review for degenerative changes, malalignment (especially hindfoot varus), fractures, and any existing hardware from previous surgeries.
- MRI of the involved ankle: This is invaluable. It demonstrates chronic thickening, fissuring, scarring, and stenosis of the remaining peroneal structures. We'll look for tears within the tendon substance and fluid in the sheaths, which are hallmarks of chronic tendinopathy. Associated ankle pathology, such as osteochondral lesions or ligamentous instability, must also be identified.
Physical Examination Review
- Re-evaluate muscle strength and balance, particularly inversion and eversion.
- Perform a single heel rise test to assess hindfoot alignment.
- Anterior drawer test to check for anterior talofibular ligament integrity and calcaneofibular ligament.
- Crucially, confirm a fully functional FHL tendon. Manual muscle testing for FHL strength is mandatory.
Patient Positioning
We'll position the patient supine on the operating table. While some prefer a pure lateral decubitus, we find a lazy lateral position to be ideal for accessing both the lateral and medial aspects of the ankle and foot. This is achieved by placing saline bags or a beanbag under the ipsilateral hip, allowing the affected limb to be slightly internally rotated and easily draped free. The leg is prepped and draped from the mid-thigh to the toes, allowing full mobility of the ankle and foot. A pneumatic thigh tourniquet will be applied to ensure a bloodless field, which is critical for meticulous dissection in scarred tissues. This two-stage procedure requires the patient to be positioned identically for both stages.
Stage 1: Débridement and Hunter Rod Insertion
Alright, team, let's begin Stage 1. We're focusing on meticulous débridement of the diseased peroneal tendons and preparing the sheath for the Hunter rod.
Step 1: Incision and Initial Dissection
Surgeon: "Scalpel, please. We're making a longitudinal incision centered over the course of the peroneal tendons. I'm starting approximately 1 cm posterior and proximal to the tip of the fibula, extending distally towards the base of the fifth metatarsal. Remember, precision is key here, especially in previously operated fields."
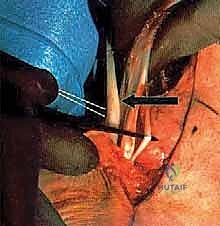
Surgical Warning: "Fellows, be acutely aware of the sural nerve in the distal aspect of this incision. It runs subcutaneously, just posterior to our incision line. We'll perform careful, sharp dissection through the skin and subcutaneous tissue, using small, gentle sweeps of the scalpel or electrocautery, always looking for the nerve. If the patient has had prior surgery, the nerve may be scarred or displaced. We want to identify and protect it throughout."
Surgeon: "As we deepen our dissection, you'll immediately notice the extensive scar tissue. This is typical in multiply-operated patients. We need to meticulously dissect through this dense, fibrotic tissue to identify the underlying peroneal sheath and tendons. This requires patience and a good understanding of the anatomy under distorted conditions."
Step 2: Peroneal Sheath Identification and Débridement
Surgeon: "Now that we've navigated through the superficial scar, we're looking for the peroneal sheath. It may be thickened and adherent. Once identified, I'll incise the sheath proximally, through the superior peroneal retinaculum, all the way up to the musculotendinous junction. Distally, we'll open the sheath as far as needed to expose the entire pathological segment of the tendons."
Surgeon: "This is a critical step: thorough débridement. We're removing all remaining, non-viable peroneal tendon tissue and the scarred, stenotic tendon sheath remnants. Use a combination of sharp dissection and fine rongeurs to remove any osteophytes or sharp bony ridges within the fibular groove that could impinge on the future tendon transfer. We want a clean, smooth bed for our Hunter rod."
Surgical Warning: "Adequate débridement is non-negotiable. If we leave behind diseased or scarred tissue, it can lead to persistent pain and compromise the gliding function of our future FHL transfer."
Step 3: Hunter Rod Insertion
Surgeon: "With the sheath thoroughly débrided, we're ready for the Hunter rod. I'll take a 6-mm Hunter rod now. We're going to insert this rod into the newly formed bed of the peroneal sheath. The purpose of this rod is to create a smooth, gliding tunnel for our FHL transfer in three months' time, allowing tissue ingrowth to form a new, vascularized sheath."
Surgeon: "I'm advancing the rod proximally into the sheath. Distally, we need to secure it. I'll suture the distal end of the Hunter rod to the remaining stump of the peroneus brevis tendon. We use a nonabsorbable suture for this, typically a 2-0 or 3-0 braided polyester, to ensure the rod remains firmly in place and doesn't migrate. The proximal end of the rod will remain free within the sheath."
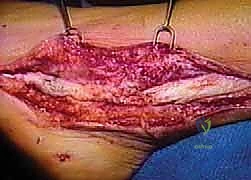
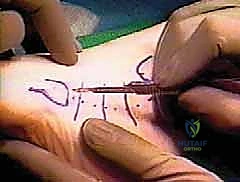
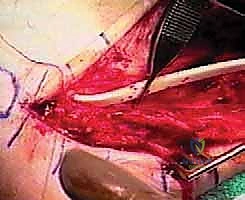

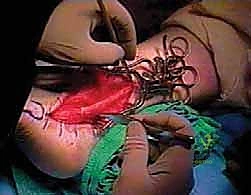
Surgical Warning: "Using a nonabsorbable suture for distal fixation of the Hunter rod is crucial. An absorbable suture risks early rod displacement, which would jeopardize the formation of the gliding tunnel."
Surgeon: "Finally, we'll trim any redundancy from the peroneal sheath and meticulously close it over the Hunter rod using fine absorbable sutures. This ensures the rod is well-contained and promotes the formation of a smooth, new tendon sheath."
Surgeon: "We'll then close the subcutaneous tissue and skin in layers. A bulky Jones dressing will be applied. That concludes Stage 1. The patient will return in approximately three months for Stage 2, allowing sufficient time for the Hunter rod to create a mature gliding tunnel."
Stage 2: FHL Harvest and Transfer
Welcome back for Stage 2, fellows. Three months have passed, and our Hunter rod has done its job, creating a fantastic gliding tunnel. Now, we're going to harvest the FHL and transfer it into its new home.
Step 1: FHL Harvest (Medial Incision)
Surgeon: "We'll begin with the FHL harvest. For this, we'll make a separate incision along the medial border of the midfoot, starting just above the level of the abductor hallucis muscle, extending from the navicular to the head of the first metatarsal. This allows us excellent access to the FHL tendon."
Surgeon: "Once through the skin and subcutaneous tissue, identify the fascia of the abductor hallucis muscle. We'll incise this fascia and carefully reflect the abductor muscle plantarly. This exposes the deeper structures."
Surgeon: "Now, I'll place a small Weitlaner retractor to maintain exposure. We need to reflect the flexor hallucis brevis plantarward as well. Sometimes, releasing the origin of this muscle can improve exposure without significant morbidity. We're looking for the FHL and FDL tendons within this second muscle layer of the foot, deep to the fat pad that overlies the neurovascular structures."
Surgical Warning: "During FHL exposure, extreme caution is necessary to protect the neurovascular structures that sit just plantar to the long tendons. These include the medial plantar nerve and artery. Stay within the second muscle layer, deep to the fat pad, to minimize risk."
Surgeon: "To confirm we have the FHL, I'm placing a finger over the lateral aspect of the short flexors and will ask my assistant to gently plantarflex and dorsiflex the hallux interphalangeal joint. You should see the FHL tendon moving distinctly. Once confirmed, we'll release the FHL as far distally as possible, generally at the level of the midshaft of the first metatarsal. It's crucial to maintain an adequate distal stump of the FHL – at least 1-2 cm – for tenodesis."
Surgeon: "Now, we need to tenodese the distal stump of the FHL to the adjacent FDL tendon. We'll do this with all five toes held in a neutral posture. This prevents a 'floating' great toe and maintains some function. Use a nonabsorbable suture, typically a 3-0, for this tenodesis."
Surgeon: "Finally, I'll tag the proximal stump of the harvested FHL with a long, strong nonabsorbable suture. This will help us retrieve it easily later."
Step 2: Hunter Rod Exchange and FHL Tendon Transfer
Surgeon: "Now, let's turn our attention back to the lateral side. We'll make a small, precise incision at the proximal aspect of our original lateral incision, staying just proximal to the lateral malleolus. This is where the proximal end of our Hunter rod is located."
Surgeon: "Through this proximal lateral incision, we'll identify the FHL tendon in the deep posterior compartment. With gentle traction on our tagging suture, we can pull the FHL tendon into this lateral incision. You can see it clearly now."
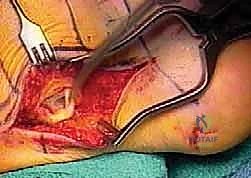
Surgeon: "Next, we'll attach the proximal end of the FHL to the proximal aspect of the Hunter rod using a strong, temporary suture. This creates a continuous 'train' from the FHL to the Hunter rod."
Surgeon: "Now for the exchange. I'll release the Hunter rod from its distal suture site, the one we placed in Stage 1. Then, with gentle, steady traction on the distal end of the Hunter rod, we'll pull it distally, allowing the FHL tendon to smoothly slide into the newly formed tendon sheath. This is a critical moment – ensure no kinking or twisting of the FHL as it enters its new tunnel."
Surgeon: "Once the FHL has passed through, we'll make a small distal incision directly over the distal suture site of the original Hunter rod and the remaining stump of the peroneus brevis. This exposes our target for the FHL insertion."
Step 3: FHL to Peroneus Brevis Tenodesis (Pulvertaft Weave)
Surgeon: "Now, we'll attach the transferred FHL to the remaining stump of the peroneus brevis tendon. We're going to use a Pulvertaft weave for this, which provides a robust, broad area of contact and promotes excellent healing."
Surgeon: "I'll create three slits in the peroneus brevis stump, approximately 1 cm apart. Then, I'll weave the FHL tendon through these slits, alternating directions. After weaving it through, I'll fold the end of the FHL back on itself and suture it securely to itself and to the brevis stump using multiple nonabsorbable sutures, typically 2-0 or 3-0 braided polyester. The goal is a secure, tensioned repair, ensuring the ankle is in a neutral or slightly everted position during the final tensioning."
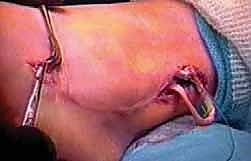
Surgeon: "After securing the weave, we'll check the tension by gently dorsiflexing and plantarflexing the ankle. The FHL should feel taut and provide dynamic eversion without over-tensioning. Once satisfied with the tension and stability, we'll close the incisions in layers: deep fascia, subcutaneous tissue, and skin. Again, a bulky Jones dressing will be applied."
Pearls and Pitfalls
General Considerations
- Patient Selection: This procedure is for chronic tendinosis of both peroneal tendons that have failed previous surgical repair. It's not for acute tears.
- Concomitant Pathology: Always address additional pathology such as ligament instability (e.g., ATFL/CFL reconstruction) or a fixed hindfoot varus deformity during the first stage of reconstruction. Ignoring these will compromise your transfer.
Incision
- Sural Nerve Protection: This is paramount. The sural nerve is subcutaneous and approximately 1 cm posterior to the peroneal tendons. Meticulous, layer-by-layer dissection is required. Preoperative assessment for existing nerve damage from prior surgeries helps manage patient expectations. Staying directly over the course of the peroneal tendons generally keeps you safe.
Hunter Rod Placement
- Adequate Débridement: Do not compromise on débriding all diseased peroneal tendon tissue and surrounding scar. Any residual pathology can hinder the gliding of the FHL.
- Nonabsorbable Suture: Always use a nonabsorbable suture to attach the Hunter rod distally to the peroneus brevis stump. This prevents rod displacement and ensures the formation of a robust gliding tunnel.
FHL Harvest
- Correct Tendon Identification: Double-check that you are harvesting the FHL and not the FDL. The FHL specifically moves the great toe.
- Neurovascular Protection: Be extremely careful of the neurovascular structures (medial plantar nerve and artery) in the medial midfoot. Stay deep to the fat pad, within the second muscle layer.
- Distal FHL Stump Tenodesis: Tenodese the distal stump of the FHL to the FDL tendon with all five toes held in a neutral position. This prevents a "floating" great toe deformity and maintains some flexor function for the hallux.
FHL Transfer and Tenodesis
- Smooth Tunnel: Ensure the Hunter rod has created a smooth, unscarred tunnel. If there's any resistance during rod removal or FHL advancement, investigate for adhesions or residual scar tissue.
- Proper Tensioning: The FHL transfer must be tensioned correctly. Too loose, and it won't provide adequate dynamic stability; too tight, and it can cause pain or rupture. Aim for neutral or slight eversion with the ankle in neutral dorsiflexion.
- Pulvertaft Weave: This technique provides the strongest repair for tendon-to-tendon tenodesis. Ensure multiple passes and secure suturing.
Postoperative Rehabilitation and Complication Management
Postoperative care is as crucial as the surgery itself for a successful outcome.
Stage 1 Postoperative Care (Hunter Rod Insertion)
- Initial Immobilization: Patients are placed in a bulky Jones dressing for the first 2 weeks.
- Early Mobilization & Weight-Bearing: After 2 weeks, the dressing is removed, and patients are allowed to bear weight as tolerated in a removable short-leg walking boot.
- Range of Motion (ROM): Patients are instructed to remove the boot four times a day to perform active and passive range-of-motion exercises of the ankle and hindfoot in all planes of motion. This prevents stiffness and promotes early sheath formation around the rod.
Stage 2 Postoperative Care (FHL Transfer)
- Initial Immobilization: Again, a bulky Jones-type dressing is applied for 2 weeks.
- Non-Weight Bearing (NWB): The patient is then advanced to a removable short-leg cast walker but remains non–weight-bearing for the first 4 weeks post-transfer. This protects the delicate tendon repair.
- Partial Weight Bearing (PWB): From week 4 to week 8, the patient progresses to partial weight bearing in the removable cast walker.
- Early ROM: Active and passive range-of-motion exercises of the ankle and hindfoot in all planes of motion are initiated.
- Transition to Brace & Therapy: At 8 weeks, the patient is advanced to an ankle stirrup, and formal physical therapy for functional rehabilitation of the ankle begins. This therapy focuses on concentric and eccentric muscle strengthening, endurance training with particular attention to the newly transferred FHL and remaining peroneal musculature, and proprioceptive training.
- Full Weight-Bearing & Return to Activity: At 12 to 14 weeks, based on strength and clinical progress, the patient transitions out of the stirrup. Proprioceptive exercises are a long-term, essential part of the rehabilitation program to improve dynamic stability. Functional bracing or taping may be useful for "at-risk" activities initially.
Potential Complications and Management
- Wound Complications: Hematoma, infection, or dehiscence. Meticulous hemostasis, sterile technique, and careful wound closure are paramount. If infection occurs, aggressive débridement and targeted antibiotics are necessary.
- Sural Nerve Injury: This can manifest as numbness, tingling, or neuropathic pain in the lateral foot. Prevention through careful dissection is key. If identified intraoperatively, direct repair or grafting may be considered. Postoperatively, nerve blocks, neuromodulators, or even neurolysis may be required for persistent symptoms.
- Chronic Pain: Despite a technically successful transfer, some patients may experience persistent pain, especially those with workers' compensation claims or extensive pre-existing psychological factors. Thorough preoperative counseling and realistic expectation setting are vital. Multi-modal pain management and continued physical therapy are often necessary.
- Hardware Failure/Tendon Rupture: While rare with a Pulvertaft weave, improper tensioning or early, aggressive activity can lead to failure. Revision surgery would involve re-harvesting a new motor unit or exploring alternative reconstructive options.
- Great Toe Deformity (Floating Toe): This occurs if the distal FHL stump is not adequately tenodesed to the FDL. Revision surgery to perform the tenodesis may be required.
Outcomes
Published data from experienced surgeons on this technique has shown promising results. In a series of 8-year follow-up patients, most reported complete relief of preoperative symptoms and a return to pre-injury levels of activity, with a high rate of excellent to good results. While one patient with workers' compensation had continued pain and required an AFO, the overall success rate is encouraging for this challenging patient population.
This procedure, while complex, offers a robust solution for patients suffering from devastating chronic peroneal tendon pathology. By adhering to meticulous surgical technique, understanding the intricate anatomy, and committing to a comprehensive rehabilitation protocol, we can significantly improve their function and quality of life. Thank you, fellows, for your attention and excellent assistance today.
REFERENCES
-
Lamm BM, Myers DT, Dombek M, et al. Magnetic resonance imaging and surgical correlation of peroneus brevis tears. J Foot Ankle Surg 2004;43:30–36.
-
Sammarco GJ, DiRaimondo CV. Chronic peroneus brevis tendon lesions. Foot Ankle 1989;9:163–170.
-
Sobel M, Geppert MJ, Hannafin JA, et al. Microvascular anatomy of the peroneal tendons. Foot Ankle 1992;13:469–472.
-
Sobel M, Geppert MJ, Olson EJ, et al. The dynamics of peroneus brevis tendon splits: a proposed mechanism, technique of diagnosis, and classification of injury. Foot Ankle 1992;13:413–422.
-
Sobel M, Levy ME, Bohne WH. Congenital variations of the peroneus quartus muscle: an anatomic study. Foot Ankle 1990;11:81–89.
-
Zammit J, Singh D. The peroneus quartus muscle: anatomy and clinical relevance. J Bone Joint Surg Br 2003;85B:1134–1137.
-
Wapner KL, Parekh SG, Pedowitz DI, et al. Reconstruction of chronic peroneal tendon ruptures with staged Hunter rods and a flexor hallucis longus transfer. Tech Foot Ankle Surg 2005;4:202–206.
-
Wapner KL, Taras J, Lin SS, et al. Staged reconstruction for chronic rupture of both peroneal tendons using Hunter rod and flexor hallucis longus tendon transfer: a long-term follow-up study. Foot Ankle Int 2006;27:591–597.
- Bassett FH III, Speer KP. Longitudinal rupture of the peroneal tendons. Am J Sports Med 1993;21:354–357.
-
Beck E. Operative treatment of recurrent dislocation of the peroneal tendons. Arch Orthop Trauma Surg 1981;98:247–250.
-
Brage ME, Hansen ST Jr. Traumatic subluxation/dislocation of the peroneal tendons. Foot Ankle 1992;13:423–431.
-
Burman M. Stenosing tendovaginitis of the foot and ankle; studies with special reference to the stenosing tendovaginitis of the peroneal tendons of the peroneal tubercle. AMA Arch Surg 1953;67: 686–698.
-
Cox D, Paterson FW. Acute calcific tendinitis of peroneus longus. J Bone Joint Surg Br 1991;73B:342.
-
Edwards ME. The relations of the peroneal tendons to the fibula, calcaneus and cuboideum. Am J Anat 1928;42:213–253.
-
Gray JM, Alpar EK. Peroneal tenosynovitis following ankle sprains. Injury 2001;32:487–489.
-
Kojima Y, Kataoka Y, Suzuki S, et al. Dislocation of the peroneal tendons in neonates and infants. Clin Orthop Relat Res 1991; 266:180–184.